Isx9 Regulates Calbindin D28K Expression in Pancreatic β Cells and Promotes β Cell Survival and Function
Abstract
1. Introduction
2. Results
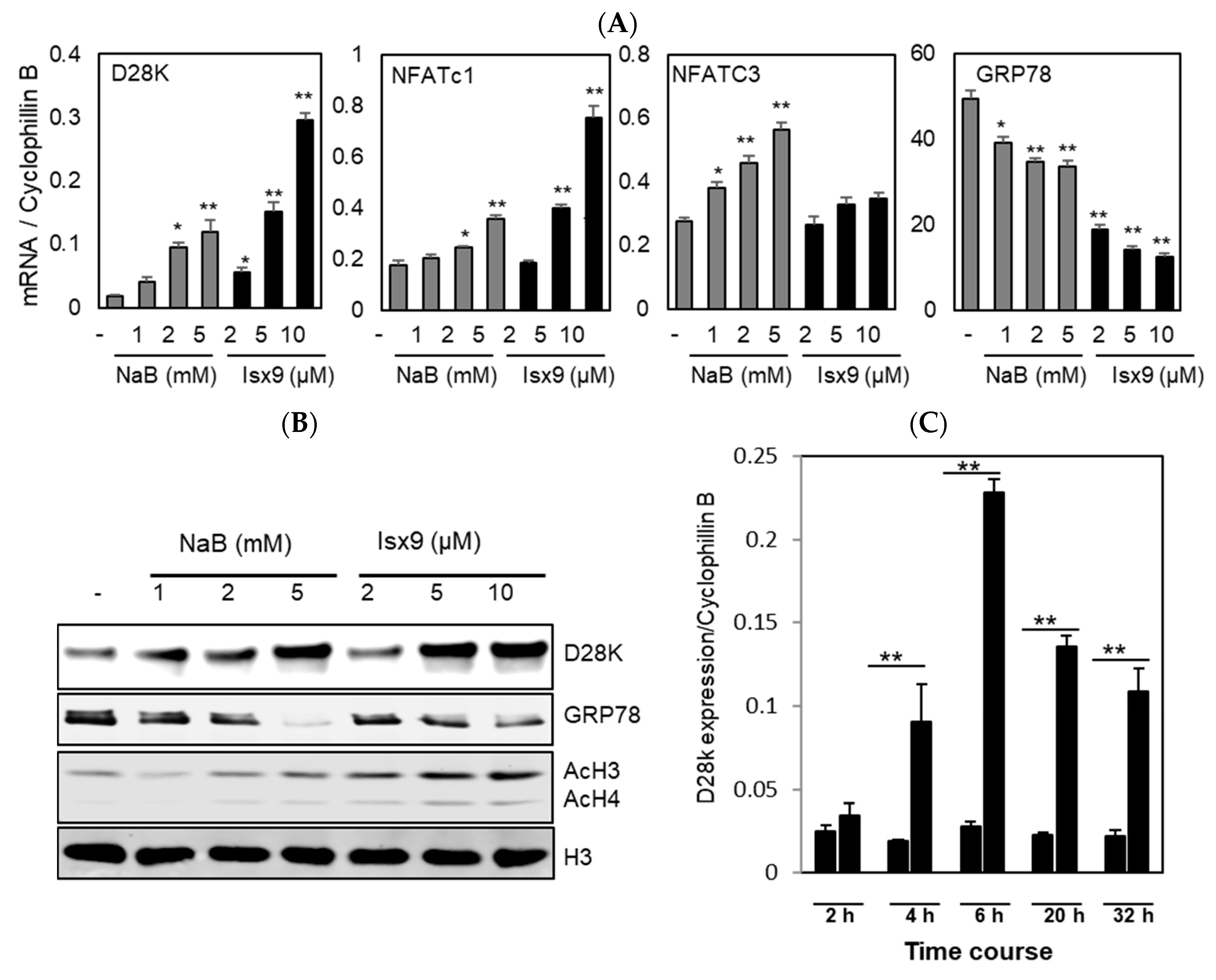
2.1. Isx9 Increases Expression Levels of NFAT and D28K
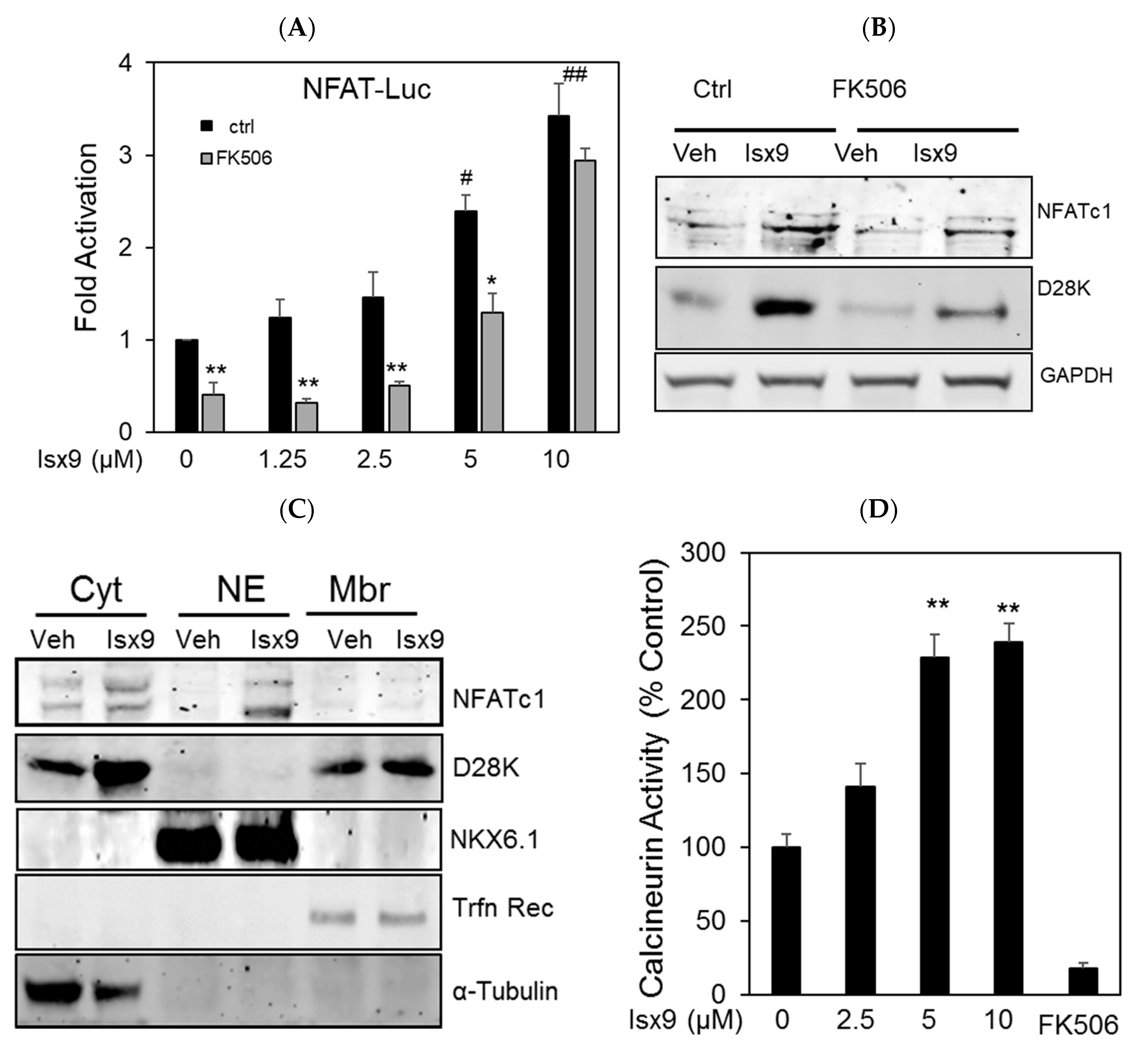
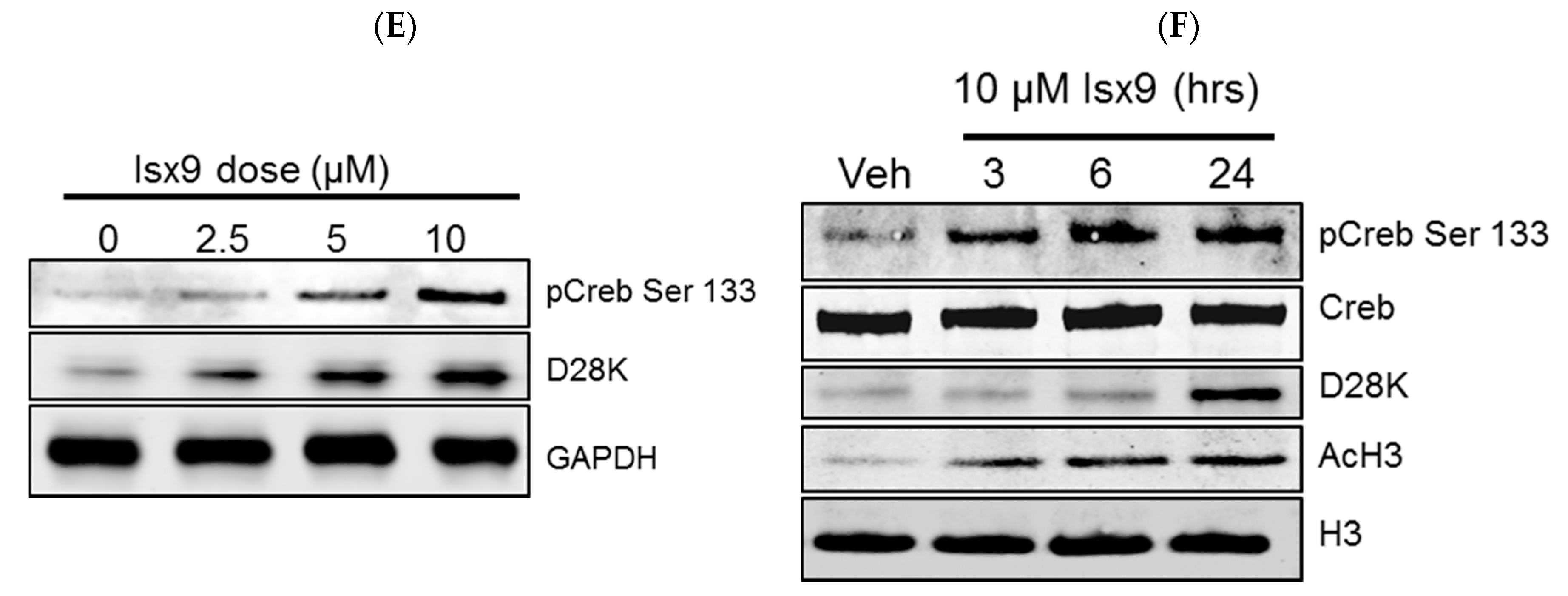
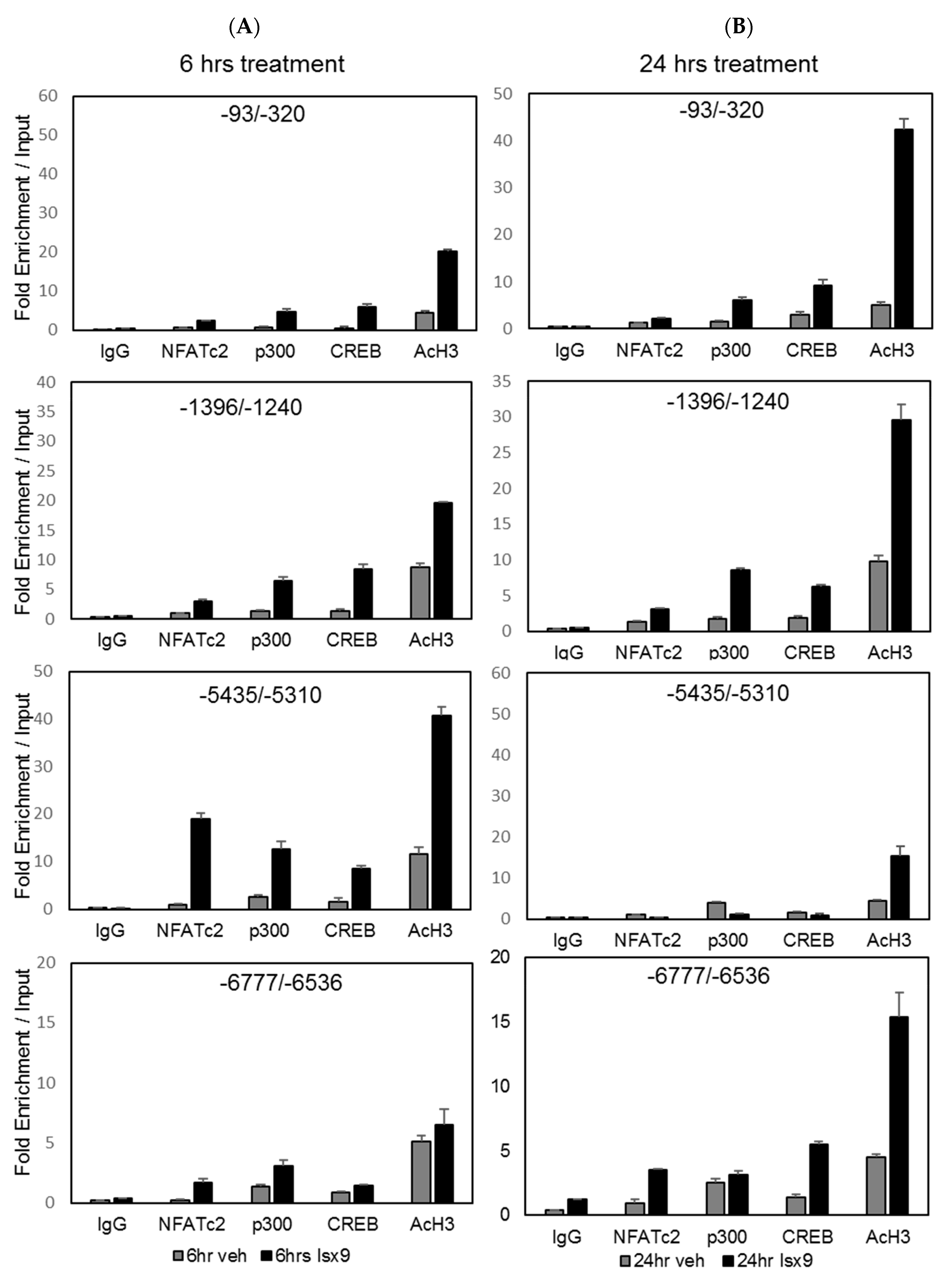
2.2. Isx9 Increases NFAT Transcriptional Activity and Recruitment of the Transcriptional Complex
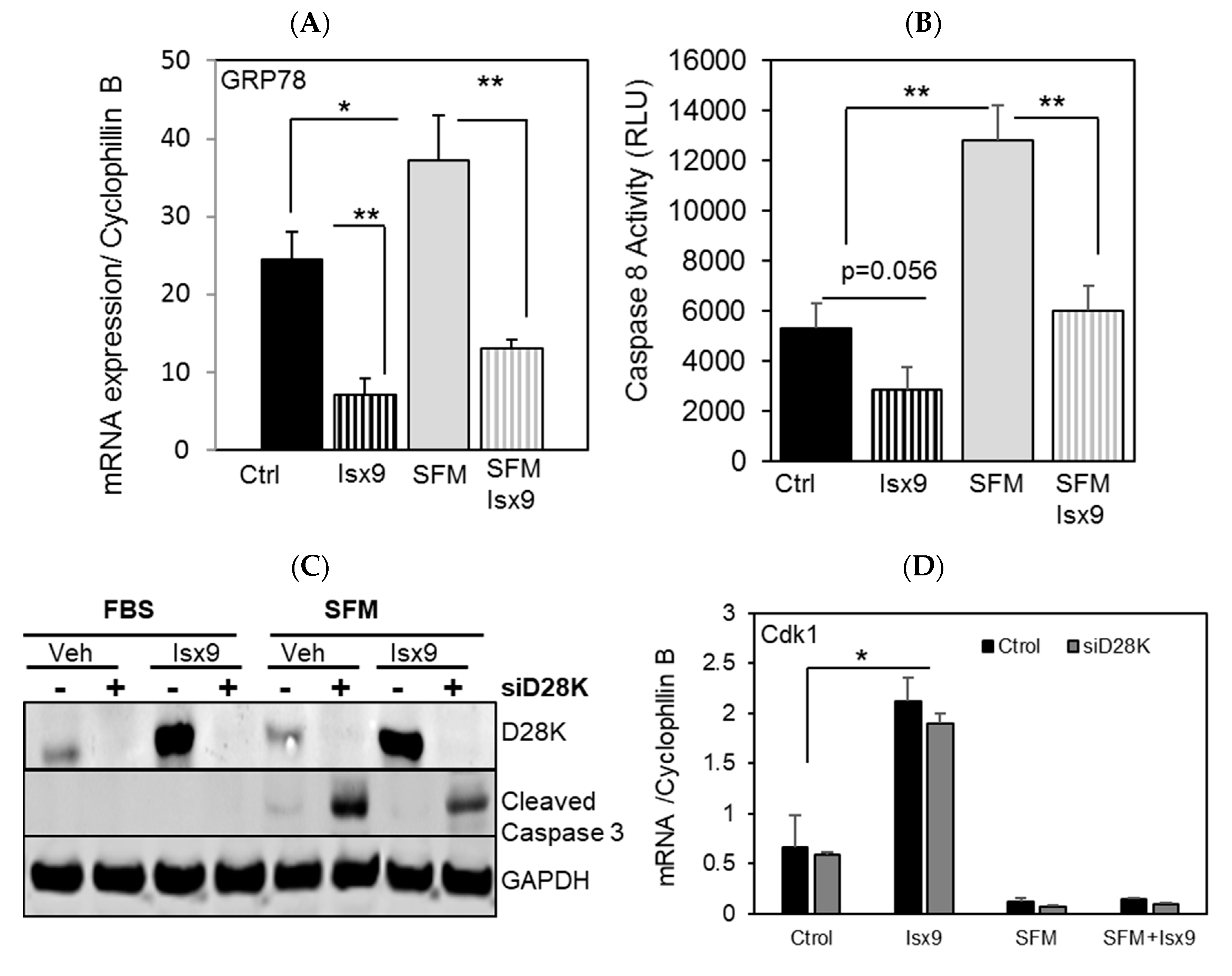
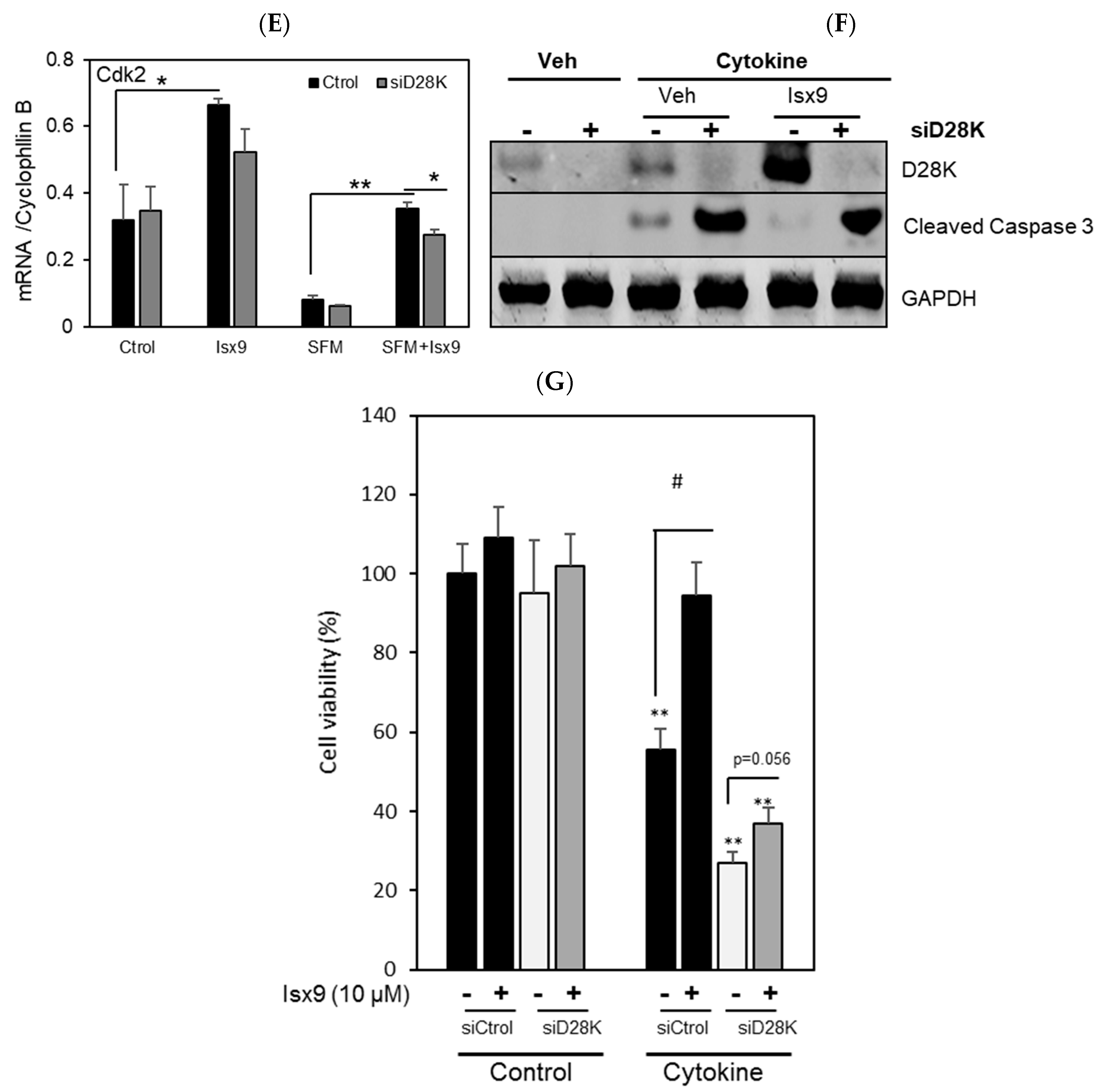
2.3. Isx9 Protects β Cells against Apoptosis through Upregulation of D28K
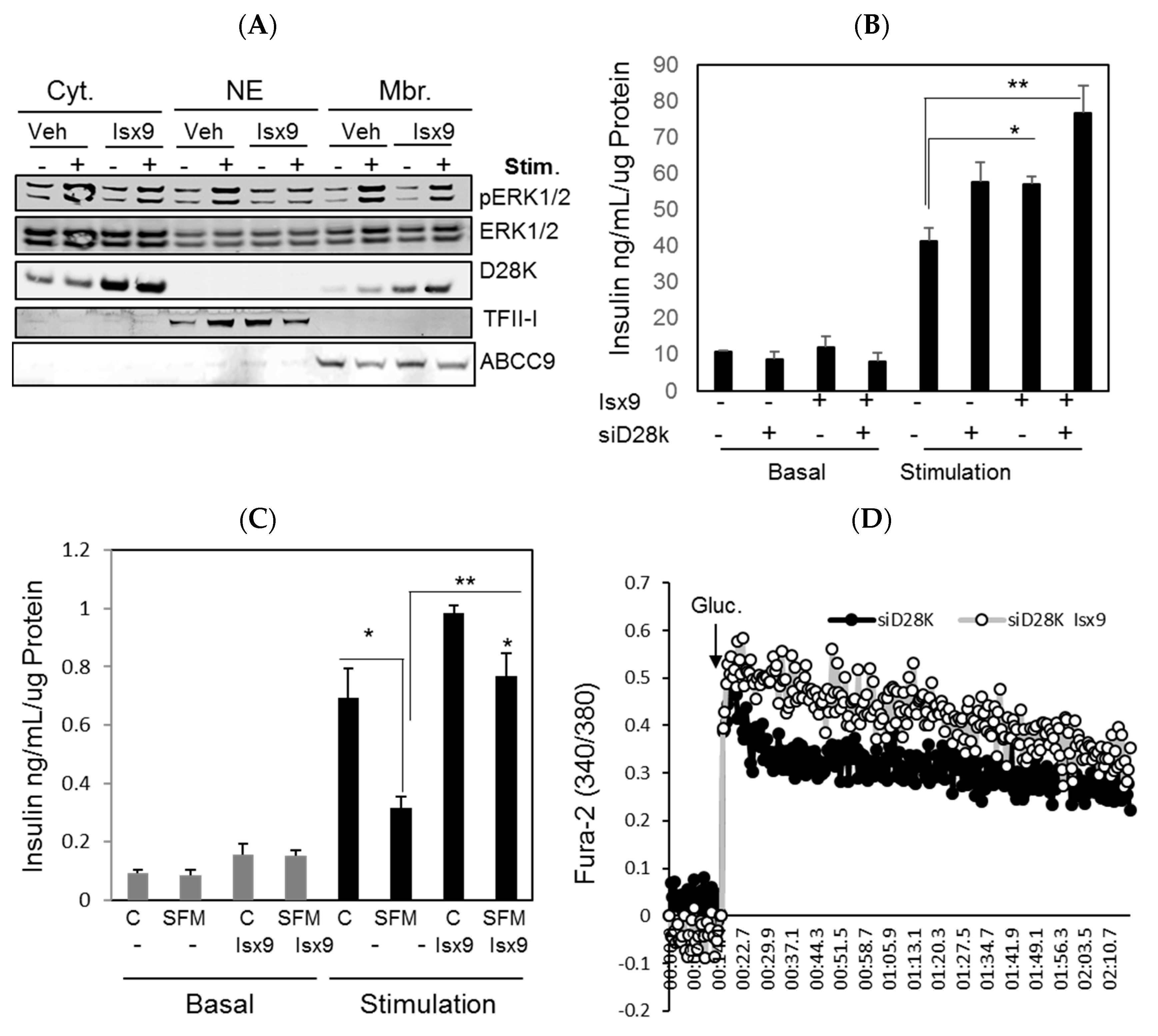
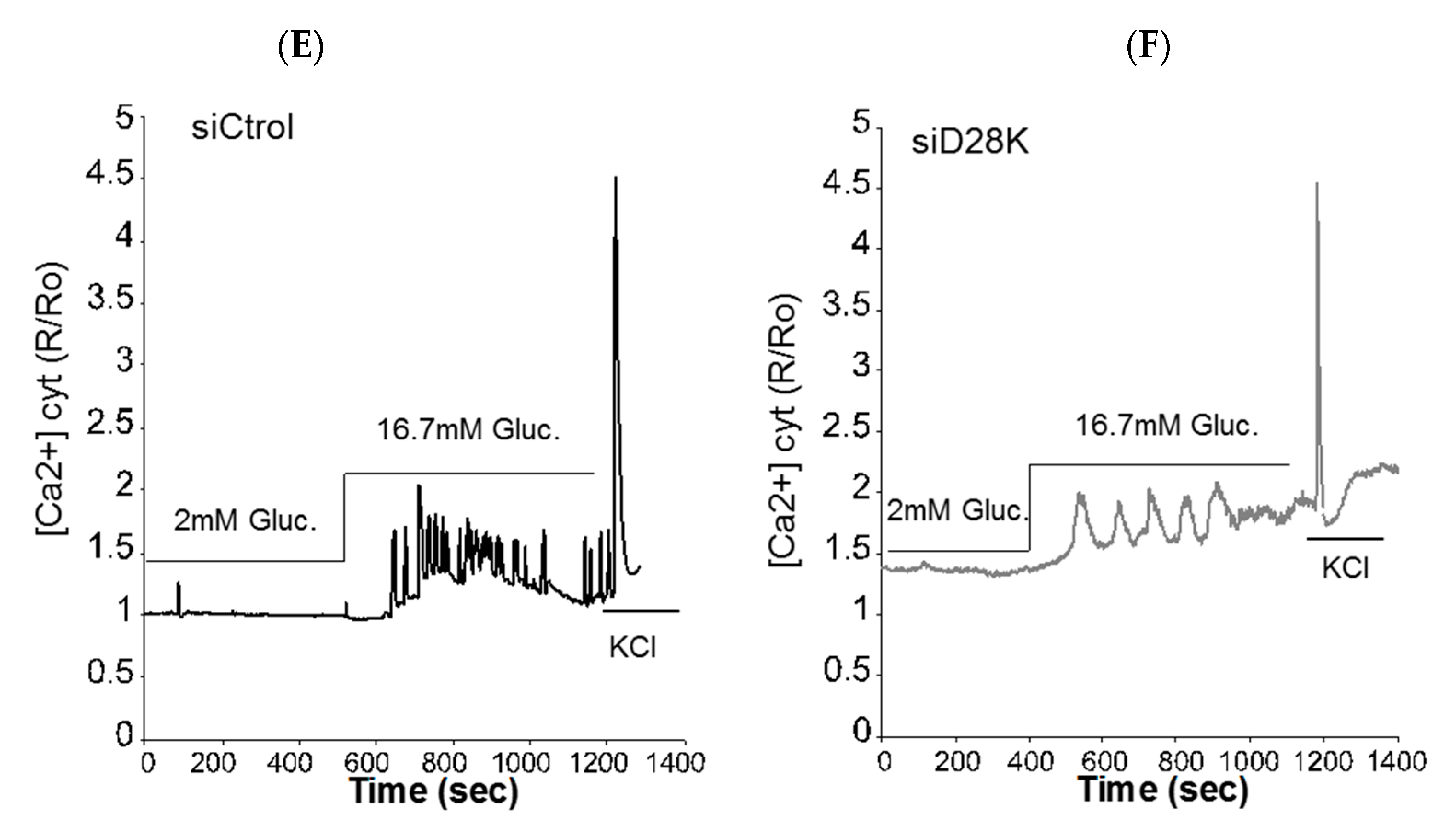
2.4. Isx9 Protects against SFM-Induced β Cell Dysfunction
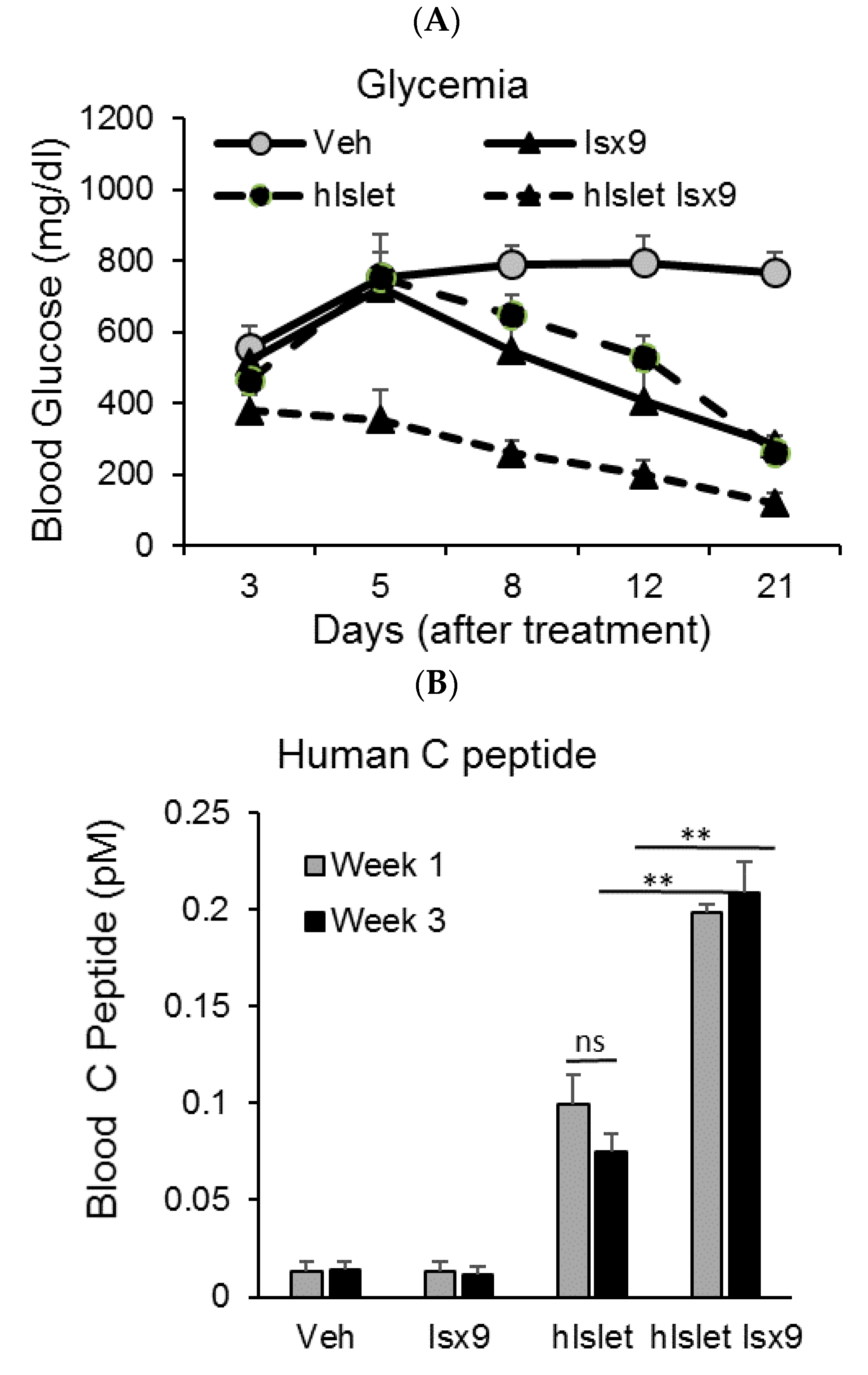
2.5. Isx9 Effect on Human Islet Survival and Function after Transplantation in a Diabetic Mouse Model
3. Discussion
4. Materials and Methods
4.1. Cell Culture and Preparation of Mouse Islets
4.2. Immunofluorescence and Confocal Microscopy
4.3. Western Blotting and Antibodies
4.4. Luciferase Assays
4.5. Chromatin Immunoprecipitation (ChIP) Assays
4.6. RNA Isolation and qPCR
4.7. Calbindin D28K siRNA Knockdown
4.8. Insulin Secretion Assay
4.9. Calcineurin Activity
4.10. Calcium Measurement
4.11. Cell Viability Assay
4.12. Mouse Studies
4.13. Statistics
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Atkinson, M.A.; Eisenbarth, G.S. Type 1 diabetes: New perspectives on disease pathogenesis and treatment. Lancet 2001, 358, 221–229. [Google Scholar] [CrossRef]
- Matveyenko, A.V.; Butler, P.C. Relationship between beta-cell mass and diabetes onset. Diabetes Obes. Metab. 2008, 10, 23–31. [Google Scholar] [CrossRef] [PubMed]
- Henquin, J.C.; Dufrane, D.; Nenquin, M. Nutrient control of insulin secretion in isolated normal human islets. Diabetes 2006, 55, 3470–3477. [Google Scholar] [CrossRef] [PubMed]
- Szollosi, A.; Nenquin, M.; Aguilar-Bryan, L.; Bryan, J.; Henquin, J.C. Glucose stimulates Ca2+ influx and insulin secretion in 2-week-old beta-cells lacking ATP-sensitive K+ channels. J. Biol. Chem. 2007, 282, 1747–1756. [Google Scholar] [CrossRef] [PubMed]
- Klee, C.B.; Ren, H.; Wang, X. Regulation of the calmodulin-stimulated protein phosphatase, calcineurin. J. Biol. Chem. 1998, 273, 13367–13370. [Google Scholar] [CrossRef] [PubMed]
- Crabtree, G.R.; Olson, E.N. NFAT signaling: Choreographing the social lives of cells. Cell 2002, 109, S67–S79. [Google Scholar] [CrossRef]
- Lawrence, M.C.; Borenstein-Auerbach, N.; McGlynn, K.; Kunnathodi, F.; Shahbazov, R.; Syed, I.; Kanak, M.; Takita, M.; Levy, M.F.; Naziruddin, B. NFAT targets signaling molecules to gene promoters in pancreatic beta-cells. Mol. Endocrinol. 2015, 29, 274–288. [Google Scholar] [CrossRef] [PubMed]
- Heit, J.J.; Apelqvist, A.A.; Gu, X.; Winslow, M.M.; Neilson, J.R.; Crabtree, G.R.; Kim, S.K. Calcineurin/NFAT signalling regulates pancreatic beta-cell growth and function. Nature 2006, 443, 345–349. [Google Scholar] [CrossRef] [PubMed]
- Lawrence, M.C.; McGlynn, K.; Park, B.H.; Cobb, M.H. ERK1/2-dependent activation of transcription factors required for acute and chronic effects of glucose on the insulin gene promoter. J. Biol. Chem. 2005, 280, 26751–26759. [Google Scholar] [CrossRef] [PubMed]
- Hajibeigi, A.; Dioum, E.M.; Guo, J.; Oz, O.K. Identification of novel regulatory NFAT and TFII-I binding elements in the calbindin-D28k promoter in response to serum deprivation. Biochem. Biophys. Res. Commun. 2015, 465, 414–420. [Google Scholar] [CrossRef] [PubMed]
- Lambers, T.T.; Mahieu, F.; Oancea, E.; Hoofd, L.; de Lange, F.; Mensenkamp, A.R.; Voets, T.; Nilius, B.; Clapham, D.E.; Hoenderop, J.G.; et al. Calbindin-D28K dynamically controls TRPV5-mediated Ca2+ transport. EMBO J. 2006, 25, 2978–2988. [Google Scholar] [CrossRef] [PubMed]
- Oz, O.K.; Hajibeigi, A.; Howard, K.; Cummins, C.L.; van Abel, M.; Bindels, R.J.; Word, R.A.; Kuro-o, M.; Pak, C.Y.; Zerwekh, J.E. Aromatase deficiency causes altered expression of molecules critical for calcium reabsorption in the kidneys of female mice. J. Bone Miner. Res. 2007, 22, 1893–1902. [Google Scholar] [CrossRef] [PubMed]
- Sooy, K.; Schermerhorn, T.; Noda, M.; Surana, M.; Rhoten, W.B.; Meyer, M.; Fleischer, N.; Sharp, G.W.; Christakos, S. Calbindin-D(28k) controls [Ca(2+)](i) and insulin release. Evidence obtained from calbindin-d(28k) knockout mice and beta cell lines. J. Biol. Chem. 1999, 274, 34343–34349. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.; Obukhov, A.G.; Shen, Q.; Liu, Y.; Dhawan, P.; Nowycky, M.C.; Christakos, S. Calbindin-D28k decreases L-type calcium channel activity and modulates intracellular calcium homeostasis in response to K+ depolarization in a rat beta cell line RINr1046-38. Cell Calcium 2006, 39, 475–485. [Google Scholar] [CrossRef] [PubMed]
- Rabinovitch, A.; Suarez-Pinzon, W.L.; Sooy, K.; Strynadka, K.; Christakos, S. Expression of calbindin-D(28k) in a pancreatic islet beta-cell line protects against cytokine-induced apoptosis and necrosis. Endocrinology 2001, 142, 3649–3655. [Google Scholar] [CrossRef] [PubMed]
- Phillips, R.G.; Meier, T.J.; Giuli, L.C.; McLaughlin, J.R.; Ho, D.Y.; Sapolsky, R.M. Calbindin D28K gene transfer via herpes simplex virus amplicon vector decreases hippocampal damage in vivo following neurotoxic insults. J. Neurochem. 1999, 73, 1200–1205. [Google Scholar] [CrossRef] [PubMed]
- Guo, Q.; Christakos, S.; Robinson, N.; Mattson, M.P. Calbindin D28k blocks the proapoptotic actions of mutant presenilin 1: Reduced oxidative stress and preserved mitochondrial function. Proc. Natl. Acad. Sci. USA 1998, 95, 3227–3232. [Google Scholar] [CrossRef] [PubMed]
- Kook, S.Y.; Jeong, H.; Kang, M.J.; Park, R.; Shin, H.J.; Han, S.H.; Son, S.M.; Song, H.; Baik, S.H.; Moon, M.; et al. Crucial role of calbindin-D28k in the pathogenesis of Alzheimer’s disease mouse model. Cell Death Differ. 2014, 21, 1575–1587. [Google Scholar] [CrossRef] [PubMed]
- Bellido, T.; Huening, M.; Raval-Pandya, M.; Manolagas, S.C.; Christakos, S. Calbindin-D28k is expressed in osteoblastic cells and suppresses their apoptosis by inhibiting caspase-3 activity. J. Biol. Chem. 2000, 275, 26328–26332. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Porta, A.; Peng, X.; Gengaro, K.; Cunningham, E.B.; Li, H.; Dominguez, L.A.; Bellido, T.; Christakos, S. Prevention of glucocorticoid-induced apoptosis in osteocytes and osteoblasts by calbindin-D28k. J. Bone Miner. Res. 2004, 19, 479–490. [Google Scholar] [CrossRef] [PubMed]
- Eizirik, D.L.; Darville, M.I. beta-cell apoptosis and defense mechanisms: Lessons from type 1 diabetes. Diabetes 2001, 50, S64–S69. [Google Scholar] [CrossRef] [PubMed]
- Susin, S.A.; Lorenzo, H.K.; Zamzami, N.; Marzo, I.; Snow, B.E.; Brothers, G.M.; Mangion, J.; Jacotot, E.; Costantini, P.; Loeffler, M.; et al. Molecular characterization of mitochondrial apoptosis-inducing factor. Nature 1999, 397, 441–446. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, R.N.; Bruning, J.C.; Winnay, J.N.; Postic, C.; Magnuson, M.A.; Kahn, C.R. Tissue-specific knockout of the insulin receptor in pancreatic beta cells creates an insulin secretory defect similar to that in type 2 diabetes. Cell 1999, 96, 329–339. [Google Scholar] [CrossRef]
- Shirakawa, J.; Fernandez, M.; Takatani, T.; El Ouaamari, A.; Jungtrakoon, P.; Okawa, E.R.; Zhang, W.; Yi, P.; Doria, A.; Kulkarni, R.N. Insulin Signaling Regulates the FoxM1/PLK1/CENP-A Pathway to Promote Adaptive Pancreatic beta Cell Proliferation. Cell Metab. 2017, 25, 868–882. [Google Scholar] [CrossRef] [PubMed]
- Kawamori, D.; Shirakawa, J.; Liew, C.W.; Hu, J.; Morioka, T.; Duttaroy, A.; Burkey, B.; Kulkarni, R.N. GLP-1 signalling compensates for impaired insulin signalling in regulating beta cell proliferation in betaIRKO mice. Diabetologia 2017, 60, 1442–1453. [Google Scholar] [CrossRef] [PubMed]
- Winnay, J.N.; Solheim, M.H.; Dirice, E.; Sakaguchi, M.; Noh, H.L.; Kang, H.J.; Takahashi, H.; Chudasama, K.K.; Kim, J.K.; Molven, A.; et al. PI3-kinase mutation linked to insulin and growth factor resistance in vivo. J. Clin. Investig. 2016, 126, 1401–1412. [Google Scholar] [CrossRef] [PubMed]
- Schneider, J.W.; Gao, Z.; Li, S.; Farooqi, M.; Tang, T.S.; Bezprozvanny, I.; Frantz, D.E.; Hsieh, J. Small-molecule activation of neuronal cell fate. Nat. Chem. Biol. 2008, 4, 408–410. [Google Scholar] [CrossRef] [PubMed]
- Dioum, E.M.; Osborne, J.K.; Goetsch, S.; Russell, J.; Schneider, J.W.; Cobb, M.H. A small molecule differentiation inducer increases insulin production by pancreatic beta cells. Proc. Natl. Acad. Sci. USA 2011, 108, 20713–20718. [Google Scholar] [CrossRef] [PubMed]
- Kalwat, M.A.; Huang, Z.; Wichaidit, C.; McGlynn, K.; Earnest, S.; Savoia, C.; Dioum, E.M.; Schneider, J.W.; Hutchison, M.R.; Cobb, M.H. Isoxazole Alters Metabolites and Gene Expression, Decreasing Proliferation and Promoting a Neuroendocrine Phenotype in beta-Cells. ACS Chem. Biol. 2016, 11, 1128–1136. [Google Scholar] [CrossRef] [PubMed]
- Emamaullee, J.A.; Shapiro, A.M. Interventional strategies to prevent beta-cell apoptosis in islet transplantation. Diabetes 2006, 55, 1907–1914. [Google Scholar] [CrossRef] [PubMed]
- Geiss, G.K.; Bumgarner, R.E.; Birditt, B.; Dahl, T.; Dowidar, N.; Dunaway, D.L.; Fell, H.P.; Ferree, S.; George, R.D.; Grogan, T.; et al. Direct multiplexed measurement of gene expression with color-coded probe pairs. Nat. Biotechnol. 2008, 26, 317–325. [Google Scholar] [CrossRef] [PubMed]
- Gill, R.K.; Christakos, S. Identification of sequence elements in mouse calbindin-D28k gene that confer 1,25-dihydroxyvitamin D3- and butyrate-inducible responses. Proc. Natl. Acad. Sci. USA 1993, 90, 2984–2988. [Google Scholar] [CrossRef] [PubMed]
- Eberhard, C.E.; Fu, A.; Reeks, C.; Screaton, R.A. CRTC2 is required for beta-cell function and proliferation. Endocrinology 2013, 154, 2308–2317. [Google Scholar] [CrossRef] [PubMed]
- Arias, J.; Alberts, A.S.; Brindle, P.; Claret, F.X.; Smeal, T.; Karin, M.; Feramisco, J.; Montminy, M. Activation of cAMP and mitogen responsive genes relies on a common nuclear factor. Nature 1994, 370, 226–229. [Google Scholar] [CrossRef] [PubMed]
- Vo, N.; Goodman, R.H. CREB-binding protein and p300 in transcriptional regulation. J. Biol. Chem. 2001, 276, 13505–13508. [Google Scholar] [CrossRef] [PubMed]
- Screaton, R.A.; Conkright, M.D.; Katoh, Y.; Best, J.L.; Canettieri, G.; Jeffries, S.; Guzman, E.; Niessen, S.; Yates, J.R., 3rd; Takemori, H.; et al. The CREB coactivator TORC2 functions as a calcium- and cAMP-sensitive coincidence detector. Cell 2004, 119, 61–74. [Google Scholar] [CrossRef] [PubMed]
- Assmann, A.; Hinault, C.; Kulkarni, R.N. Growth factor control of pancreatic islet regeneration and function. Pediatr. Diabetes 2009, 10, 14–32. [Google Scholar] [CrossRef] [PubMed]
- Maestre, I.; Jordan, J.; Calvo, S.; Reig, J.A.; Cena, V.; Soria, B.; Prentki, M.; Roche, E. Mitochondrial dysfunction is involved in apoptosis induced by serum withdrawal and fatty acids in the beta-cell line INS-1. Endocrinology 2003, 144, 335–345. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.L.; Chan, P.C.; Wang, S.H.; Pan, Y.R.; Chen, H.C. Elevated expression of protein kinase C delta induces cell scattering upon serum deprivation. J. Cell Sci. 2010, 123, 2901–2913. [Google Scholar] [CrossRef] [PubMed]
- Jimenez-Palomares, M.; Lopez-Acosta, J.F.; Villa-Perez, P.; Moreno-Amador, J.L.; Munoz-Barrera, J.; Fernandez-Luis, S.; Heras-Pozas, B.; Perdomo, G.; Bernal-Mizrachi, E.; Cozar-Castellano, I. Cyclin C stimulates beta-cell proliferation in rat and human pancreatic beta-cells. Am. J. Physiol. Endocrinol. Metab. 2015, 308, E450–E459. [Google Scholar] [CrossRef] [PubMed]
- Goodyer, W.R.; Gu, X.; Liu, Y.; Bottino, R.; Crabtree, G.R.; Kim, S.K. Neonatal beta cell development in mice and humans is regulated by calcineurin/NFAT. Dev. Cell 2012, 23, 21–34. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.Y.; Lee, J.H.; Merrins, M.J.; Gavrilova, O.; Bisteau, X.; Kaldis, P.; Satin, L.S.; Rane, S.G. Loss of Cyclin-dependent Kinase 2 in the Pancreas Links Primary beta-Cell Dysfunction to Progressive Depletion of beta-Cell Mass and Diabetes. J. Biol. Chem. 2017, 292, 3841–3853. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, G.V.; McCulloch, C.A. Serum deprivation induces apoptotic cell death in a subset of Balb/c 3T3 fibroblasts. J. Cell Sci. 1994, 107, 1169–1179. [Google Scholar] [PubMed]
- Voccoli, V.; Mazzoni, F.; Garcia-Gil, M.; Colombaioni, L. Serum-withdrawal-dependent apoptosis of hippocampal neuroblasts involves Ca++ release by endoplasmic reticulum and caspase-12 activation. Brain Res. 2007, 1147, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Nicotera, P.; Orrenius, S. The role of calcium in apoptosis. Cell Calcium 1998, 23, 173–180. [Google Scholar] [CrossRef]
- Jung, E.M.; An, B.S.; Choi, K.C.; Jeung, E.B. Apoptosis- and endoplasmic reticulum stress-related genes were regulated by estrogen and progesterone in the uteri of calbindin-D(9k) and -D(28k) knockout mice. J. Cell. Biochem. 2012, 113, 194–203. [Google Scholar] [CrossRef] [PubMed]
- Oz, S.; Tsemakhovich, V.; Christel, C.J.; Lee, A.; Dascal, N. CaBP1 regulates voltage-dependent inactivation and activation of Ca(V)1.2 (L-type) calcium channels. J. Biol. Chem. 2011, 286, 13945–13953. [Google Scholar] [CrossRef] [PubMed]
- Bernardo, A.S.; Hay, C.W.; Docherty, K. Pancreatic transcription factors and their role in the birth, life and survival of the pancreatic beta cell. Mol. Cell. Endocrinol. 2008, 294, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Odom, D.T.; Koo, S.H.; Conkright, M.D.; Canettieri, G.; Best, J.; Chen, H.; Jenner, R.; Herbolsheimer, E.; Jacobsen, E.; et al. Genome-wide analysis of cAMP-response element binding protein occupancy, phosphorylation, and target gene activation in human tissues. Proc. Natl. Acad. Sci. USA 2005, 102, 4459–4464. [Google Scholar] [CrossRef] [PubMed]
- Khan, S.; Jena, G.B. Protective role of sodium butyrate, a HDAC inhibitor on beta-cell proliferation, function and glucose homeostasis through modulation of p38/ERK MAPK and apoptotic pathways: Study in juvenile diabetic rat. Chem. Biol. Interact. 2014, 213, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Imhof, A.; Yang, X.J.; Ogryzko, V.V.; Nakatani, Y.; Wolffe, A.P.; Ge, H. Acetylation of general transcription factors by histone acetyltransferases. Curr. Biol. 1997, 7, 689–692. [Google Scholar] [CrossRef]
- Lee, D.Y.; Hayes, J.J.; Pruss, D.; Wolffe, A.P. A positive role for histone acetylation in transcription factor access to nucleosomal DNA. Cell 1993, 72, 73–84. [Google Scholar] [CrossRef]
- Zentner, G.E.; Henikoff, S. Regulation of nucleosome dynamics by histone modifications. Nat. Struct. Mol. Biol. 2013, 20, 259–266. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.M.; Chao, J.R.; Chen, W.; Kuo, M.L.; Yen, J.J.; Yang-Yen, H.F. The antiapoptotic gene mcl-1 is up-regulated by the phosphatidylinositol 3-kinase/Akt signaling pathway through a transcription factor complex containing CREB. Mol. Cell. Biol. 1999, 19, 6195–6206. [Google Scholar] [CrossRef] [PubMed]
- Vidakovic, M.; Grdovic, N.; Dinic, S.; Mihailovic, M.; Uskokovic, A.; Arambasic Jovanovic, J. The Importance of the CXCL12/CXCR4 Axis in Therapeutic Approaches to Diabetes Mellitus Attenuation. Front. Immunol. 2015, 6, 403. [Google Scholar] [PubMed]
- Ricordi, C.; Strom, T.B. Clinical islet transplantation: Advances and immunological challenges. Nat. Rev. Immunol. 2004, 4, 259–268. [Google Scholar] [CrossRef] [PubMed]
- Rangel, E.B. Tacrolimus in pancreas transplant: A focus on toxicity, diabetogenic effect and drug-drug interactions. Exp. Opin. Drug Metab. Toxicol. 2014, 10, 1585–1605. [Google Scholar] [CrossRef] [PubMed]
- Vandewalle, A.; Tourneur, E.; Bens, M.; Chassin, C.; Werts, C. Calcineurin/NFAT signaling and innate host defence: A role for NOD1-mediated phagocytic functions. Cell Commun. Signal. 2014, 12, 8. [Google Scholar] [CrossRef] [PubMed]
- Lawrence, M.C.; McGlynn, K.; Shao, C.; Duan, L.; Naziruddin, B.; Levy, M.F.; Cobb, M.H. Chromatin-bound mitogen-activated protein kinases transmit dynamic signals in transcription complexes in beta-cells. Proc. Natl. Acad. Sci. USA 2008, 105, 13315–13320. [Google Scholar] [CrossRef] [PubMed]
- Sutton, R.; Peters, M.; McShane, P.; Gray, D.W.; Morris, P.J. Isolation of rat pancreatic islets by ductal injection of collagenase. Transplantation 1986, 42, 689–691. [Google Scholar] [CrossRef] [PubMed]
- Kalwat, M.A.; Wichaidit, C.; Nava Garcia, A.Y.; McCoy, M.K.; McGlynn, K.; Hwang, I.H.; MacMillan, J.B.; Posner, B.A.; Cobb, M.H. Insulin promoter-driven Gaussia luciferase-based insulin secretion biosensor assay for discovery of beta-cell glucose-sensing pathways. ACS Sens. 2016, 1, 1208–1212. [Google Scholar] [CrossRef] [PubMed]
- Wauson, E.M.; Zaganjor, E.; Lee, A.Y.; Guerra, M.L.; Ghosh, A.B.; Bookout, A.L.; Chambers, C.P.; Jivan, A.; McGlynn, K.; Hutchison, M.R.; et al. The G protein-coupled taste receptor T1R1/T1R3 regulates mTORC1 and autophagy. Mol. Cell 2012, 47, 851–862. [Google Scholar] [CrossRef] [PubMed]
- De Marchi, U.; Thevenet, J.; Hermant, A.; Dioum, E.; Wiederkehr, A. Calcium co-regulates oxidative metabolism and ATP synthase-dependent respiration in pancreatic beta cells. J. Biol. Chem. 2014, 289, 9182–9194. [Google Scholar] [CrossRef] [PubMed]
- Boss, C.; De Marchi, U.; Hermant, A.; Conrad, M.; Sizzano, F.; Palini, A.; Wiederkehr, A.; Bouche, N. Encapsulation of Insulin-Secreting Cells Expressing a Genetically Encoded Fluorescent Calcium Indicator for Cell-Based Sensing In Vivo. Adv. Healthc. Mater. 2017, 6, 1600869. [Google Scholar] [CrossRef] [PubMed]
- Al-Nasiry, S.; Geusens, N.; Hanssens, M.; Luyten, C.; Pijnenborg, R. The use of Alamar Blue assay for quantitative analysis of viability, migration and invasion of choriocarcinoma cells. Hum. Reprod. 2007, 22, 1304–1309. [Google Scholar] [CrossRef] [PubMed]

© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pujol, J.B.; Heikkila, E.; Savoia, C.; Hajibeigi, A.; De Marchi, U.; Battiprolu, P.K.; Öz, O.K.; Dioum, E.H.M. Isx9 Regulates Calbindin D28K Expression in Pancreatic β Cells and Promotes β Cell Survival and Function. Int. J. Mol. Sci. 2018, 19, 2542. https://doi.org/10.3390/ijms19092542
Pujol JB, Heikkila E, Savoia C, Hajibeigi A, De Marchi U, Battiprolu PK, Öz OK, Dioum EHM. Isx9 Regulates Calbindin D28K Expression in Pancreatic β Cells and Promotes β Cell Survival and Function. International Journal of Molecular Sciences. 2018; 19(9):2542. https://doi.org/10.3390/ijms19092542
Chicago/Turabian StylePujol, Julien B., Eija Heikkila, Claudia Savoia, Asghar Hajibeigi, Umberto De Marchi, Pavan K. Battiprolu, Orhan K. Öz, and El Hadji M. Dioum. 2018. "Isx9 Regulates Calbindin D28K Expression in Pancreatic β Cells and Promotes β Cell Survival and Function" International Journal of Molecular Sciences 19, no. 9: 2542. https://doi.org/10.3390/ijms19092542
APA StylePujol, J. B., Heikkila, E., Savoia, C., Hajibeigi, A., De Marchi, U., Battiprolu, P. K., Öz, O. K., & Dioum, E. H. M. (2018). Isx9 Regulates Calbindin D28K Expression in Pancreatic β Cells and Promotes β Cell Survival and Function. International Journal of Molecular Sciences, 19(9), 2542. https://doi.org/10.3390/ijms19092542





