The Role of Omega-3 Fatty Acids in Developmental Psychopathology: A Systematic Review on Early Psychosis, Autism, and ADHD
Abstract
1. Introduction
2. Results
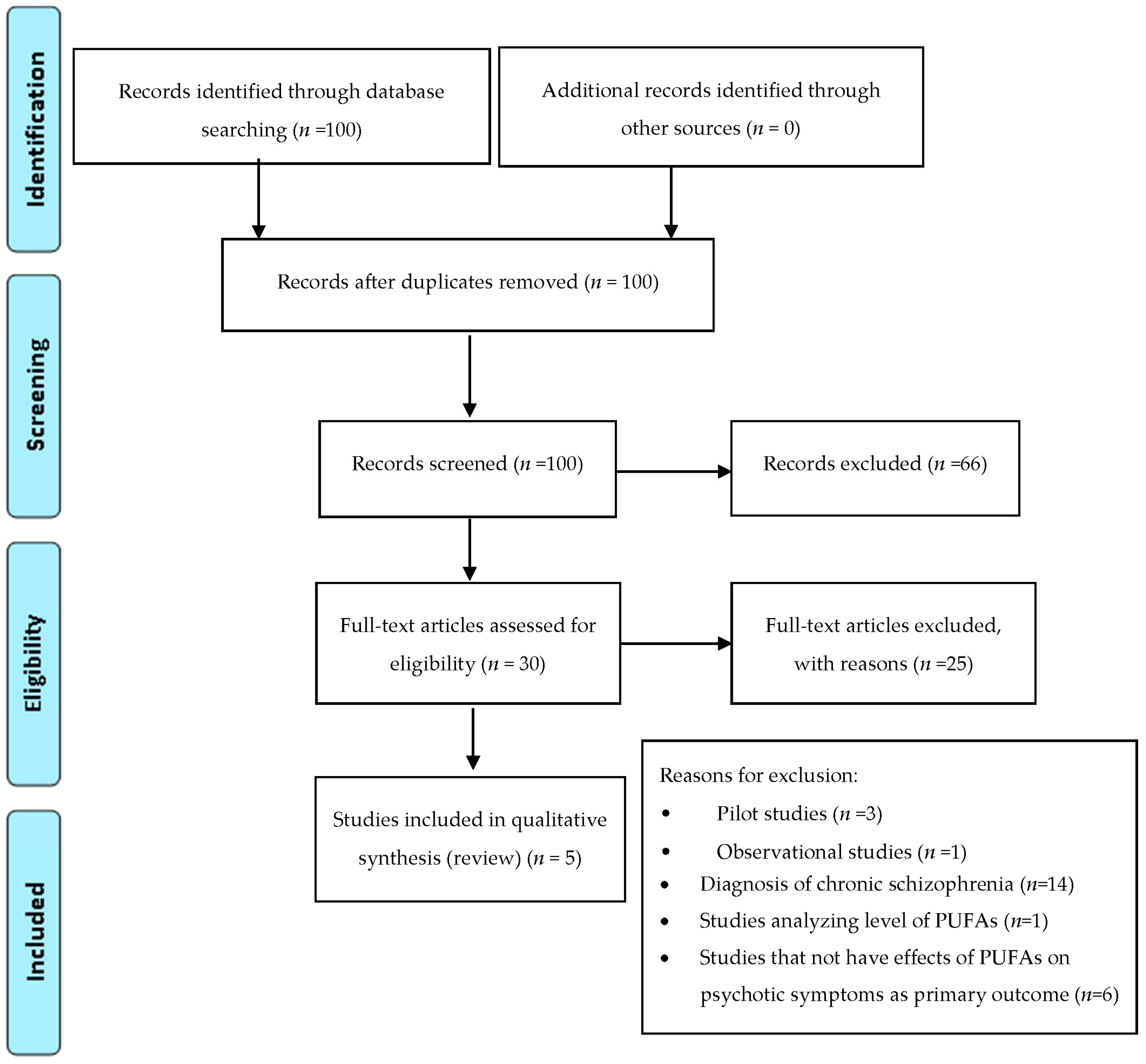
2.1. Omega-3 in Psychosis
2.1.1. Ultra-high-risk Patients
2.1.2. First Episode Psychosis
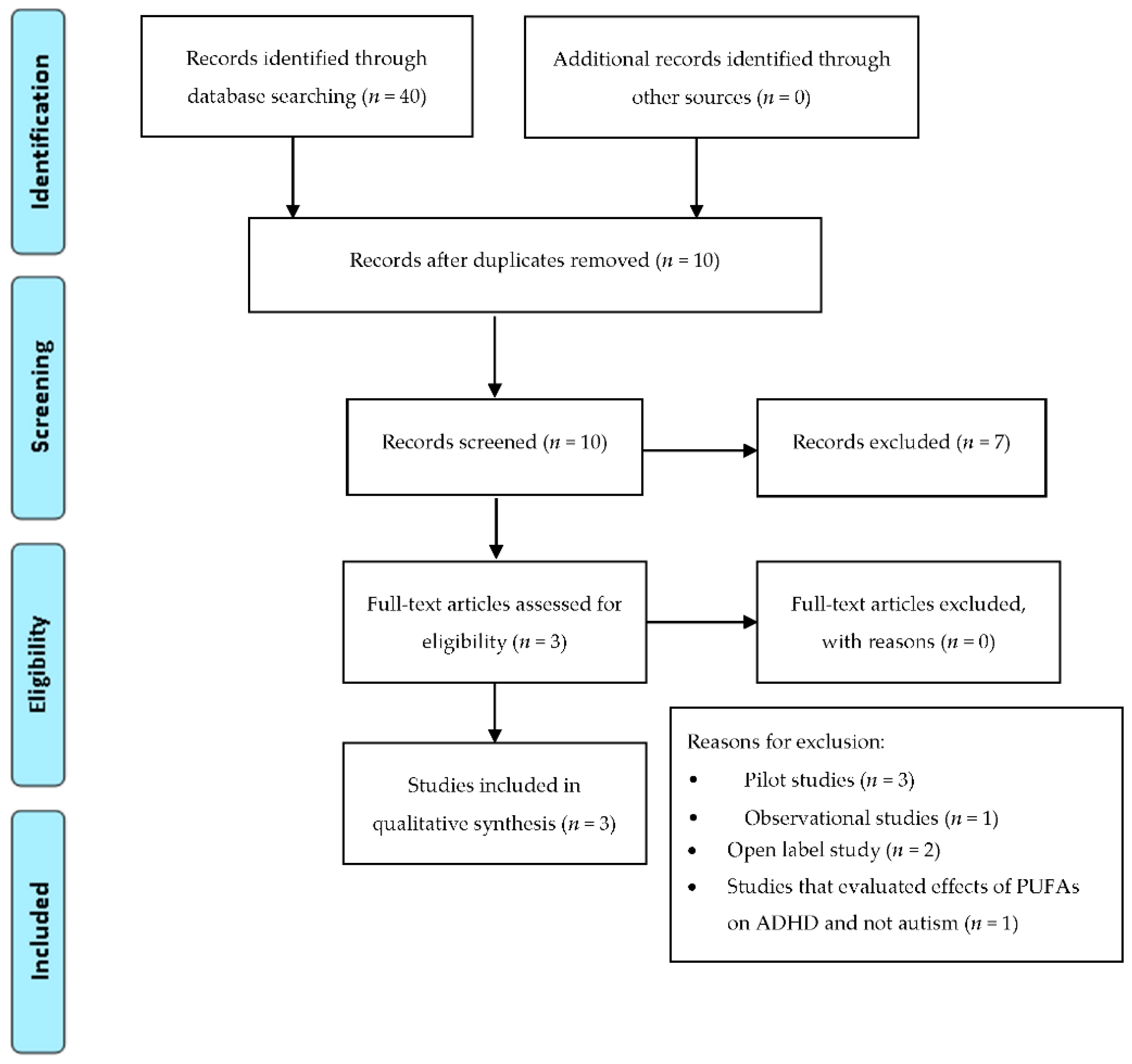
2.2. Omega-3 and Autism
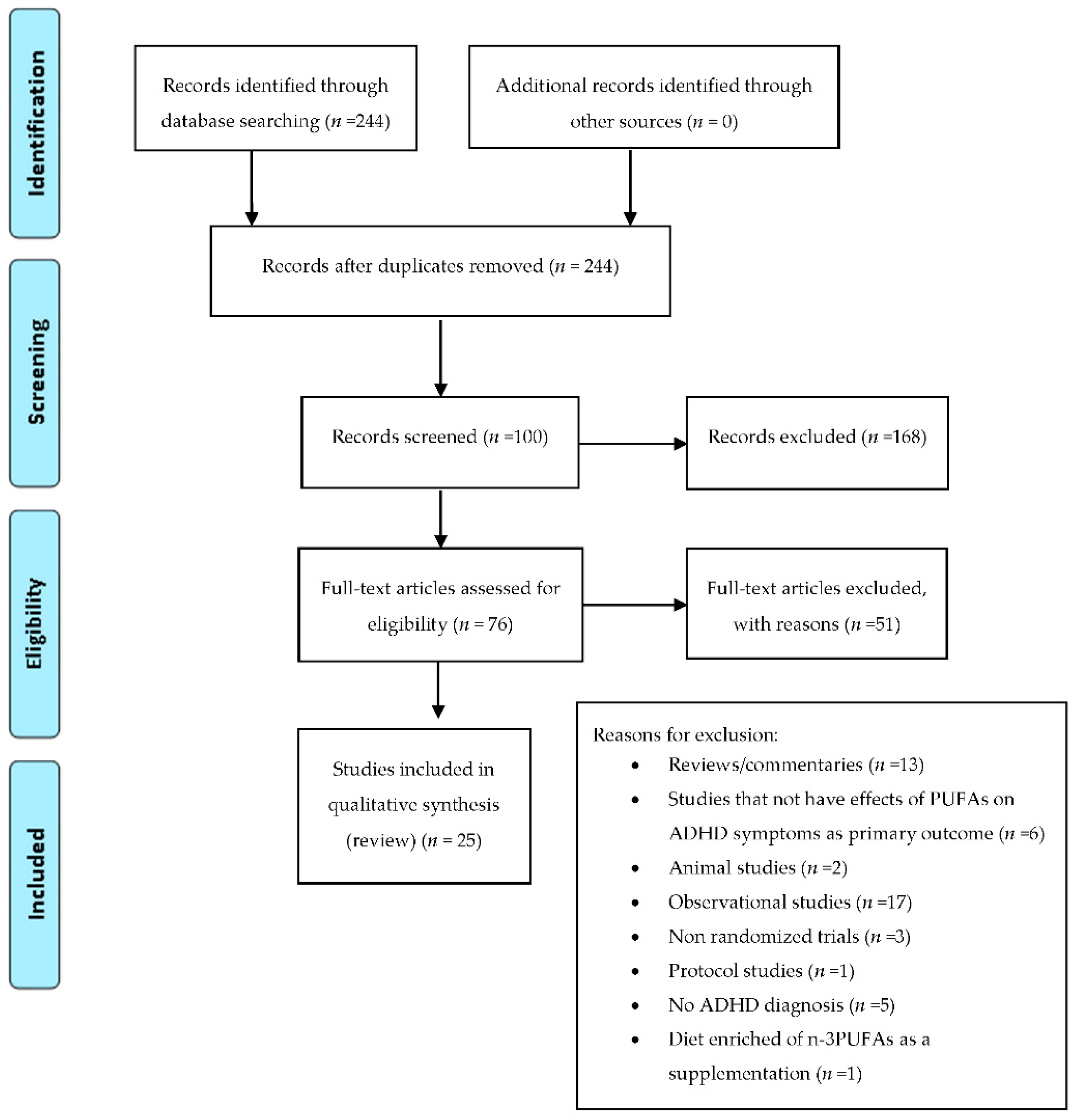
2.3. Omega-3 in ADHD
3. Conclusions and Future Directions
4. Material and Methods
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Baxter, A.J.; Patton, G.; Scott, K.M.; Kate, M.; Degenhardt, L.; Whiteford, H.A. Global Epidemiology of Mental Disorders: What Are We Missing? PLoS ONE 2013, 8, e65514. [Google Scholar] [CrossRef] [PubMed]
- Logan, A.C.; Jacka, F.N. Nutritional psychiatry research: An emerging discipline and its intersection with global urbanization, environmental challenges and the evolutionary mismatch. J. Phys. Anthropol. 2014, 33, 22. [Google Scholar] [CrossRef] [PubMed]
- McNamara, R.K.; Vannest, J.J.; Valentine, C.J. Role of perinatal long-chain omega-3 fatty acids in cortical circuit maturation: Mechanisms and implications for psychopathology. World J. Psychiatry 2015, 5, 15–34. [Google Scholar] [CrossRef] [PubMed]
- Innis, S.M. Perinatal biochemistry and physiology of long-chain polyunsaturated fatty acids. J. Pediatr. 2003, 143, S1–S8. [Google Scholar] [CrossRef]
- Kiecolt-Glaser, J.K.; Preacher, K.J.; MacCallum, R.C.; Atkinson, C.; Malarkey, W.; Glaser, R. Chronic stress and age-related increases in the proinflammatory cytokine IL-6. Proc. Natl. Acad. Sci. USA 2003, 100, 9090–9095. [Google Scholar] [CrossRef] [PubMed]
- Das, U.N. Biological significance of essential fatty acids. J. Assoc. Phys. India 2006, 54, 309–319. [Google Scholar]
- Lauritzen, L.; Brambilla, P.; Mazzocchi, A.; Harsløf, L.; Ciappolino, V.; Agostoni, C. DHA Effects in Brain Development and Function. Nutrients 2016, 8, 6. [Google Scholar] [CrossRef] [PubMed]
- Carver, J.D.; Benford, V.J.; Han, B.; Cantor, A.B. The relationship between age and the fatty acid composition of cerebral cortex and erythrocytes in human subjects. Brain Res. Bull. 2001, 56, 79–85. [Google Scholar] [CrossRef]
- Herrera, E. Implications of dietary fatty acids during pregnancy on placental, fetal and postnatal development—A review. Placenta 2002, 23 (Suppl. A), S9–S19. [Google Scholar] [CrossRef] [PubMed]
- Jørgensen, M.H.; Nielsen, P.K.; Michaelsen, K.; Lund, P.; Lauritzen, L. The composition of polyunsaturated fatty acids in erythrocytes of lactating mothers and their infants. Matern. Child Nutr. 2006, 2, 29–39. [Google Scholar] [CrossRef] [PubMed]
- European Food Safety Authority. The Panel on Dietetic Products, Nutrition and Allergies on a re-quest from Mead Johnson Nutritionals. Scientific opinion on DHA and ARA and visual development. EFSA J. 2009, 941, 1–14. [Google Scholar]
- Browning, L.M.; Walker, C.G.; Mander, A.P.; West, A.; Madden, J.; Gambell, J.; Young, S.; Wang, L.; Jebb, S.; Calder, P. Incorporation of eicosapentaenoic and docosahexaenoic acids into lipid pools when given as supplements providing doses equivalent to typical intakes of oily fish. Am. J. Clin. Nutr. 2012, 96, 748–758. [Google Scholar] [CrossRef] [PubMed]
- Mischoulon, D.; Freeman, M.P. Omega-3 fatty acids in psychiatry. Psychiatr. Clin. N. Am. 2013, 36, 15–23. [Google Scholar] [CrossRef] [PubMed]
- Ross, B.M.; Seguin, J.; Sieswerda, L.E. Omega-3 fatty acids as treatments for mental illness: Which disorder and which fatty acid? Lipids Health Dis. 2007, 6, 21. [Google Scholar] [CrossRef] [PubMed]
- Hallahan, B.; Garland, M.R. Essential fatty acids and mental health. Br. J. Psychiatry 2005, 186, 275–277. [Google Scholar] [CrossRef] [PubMed]
- Assisi, A.; Banzi, R.; Buonocore, C.; Capasso, F.; Muzio, V.D.; Michelacci, F.; Renzo, D.; Tafuri, G.; Trotta, F.; Vitocolonna, M.; et al. Fish oil and mental health: The role of n-3 long-chain polyunsaturated fatty acids in cognitive development and neurological disorders. Int. Clin. Psychopharmacol. 2006, 21, 319–336. [Google Scholar] [CrossRef] [PubMed]
- De la Presa Owens, S.; Innis, S.M. Docosahexaenoic and arachidonic acid prevent a decrease in dopaminergic and serotoninergic neurotransmitters in frontal cortex caused by a linoleic and α-linolenic acid deficient diet in formula-fed piglets. J. Nutr. 1999, 129, 2088–2093. [Google Scholar] [PubMed]
- Galli, C.; Trzeciak, H.I.; Paoletti, R. Effects of essential fatty acid deficiency on myelin and various subcellular structures in rat brain. J. Neurochem. 1972, 19, 1863–1867. [Google Scholar] [CrossRef] [PubMed]
- Yehuda, S.; Rabinovitz, S.; Carasso, R.L.; Mostofsky, D.I. The role of polyunsaturated fatty acids in restoring the aging neuronal membrane. Neurobiol. Aging 2002, 23, 843–853. [Google Scholar] [CrossRef]
- Haag, M. Essential Fatty Acids and the Brain. Can. J. Psychiatry 2003, 48, 195–203. [Google Scholar] [CrossRef] [PubMed]
- Colangelo, L.A.; He, K.; Whooley, M.A.; Daviglus, M.; Liu, K. Higher dietary intake of long-chain ω-3 polyunsaturated fatty acids is inversely associated with depressive symptoms in women. Nutrition 2009, 25, 1011–1019. [Google Scholar] [CrossRef] [PubMed]
- Sinn, N.; Milte, C.; Howe, P.R.C. Oiling the brain: A review of randomized controlled trials of omega-3 fatty acids in psychopathology across the lifespan. Nutrients 2010, 2, 128–170. [Google Scholar] [CrossRef] [PubMed]
- Sinclair, A.J.; Begg, D.; Mathai, M.; Weisinger, R.S. Omega 3 fatty acids and the brain: Review of studies in depression. Asia Pac. J. Clin. Nutr. 2007, 16 (Suppl. S1), 391–397. [Google Scholar] [PubMed]
- McNamara, R.K.; Jandacek, R.; Rider, T.; Tso, P.; Hahn, C.; Richtand, N.; Stanford, K. Abnormalities in the fatty acid composition of the postmortem orbitofrontal cortex of schizophrenic patients: Gender differences and partial normalization with antipsychotic medications. Schizophr. Res. 2007, 91, 37–50. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.M.; Evans, D.R.; Gunna, V.; Scheffer, R.; Parikh, V.; Mahadik, S. Reduced erythrocyte membrane essential fatty acids and increased lipid peroxides in schizophrenia at the never-medicated first-episode of psychosis and after years of treatment with antipsychotics. Schizophr. Res. 2002, 58, 1–10. [Google Scholar] [CrossRef]
- Reddy, R.D.; Keshavan, M.S.; Yao, J.K. Reduced red blood cell membrane essential polyunsaturated fatty acids in first episode schizophrenia at neuroleptic-naive baseline. Schizophr. Bull. 2004, 30, 901–911. [Google Scholar] [CrossRef] [PubMed]
- Hoen, W.P.; Lijmer, J.G.; Duran, M.; Wanders, R.; van Beveren, N.; de Haan, L. Red blood cell polyunsaturated fatty acids measured in red blood cells and schizophrenia: A meta-analysis. Psychiatry Res. 2013, 207, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Sliwinski, S.; Croonenberghs, J.; Christophe, A.; Deboutte, D.; Maes, M. Polyunsaturated fatty acids: Do they have a role in the pathophysiology of autism? Neuro Endocrinol. Lett. 2006, 27, 465–471. [Google Scholar] [PubMed]
- Hawkey, E.; Nigg, J.T. Omega-3 fatty acid and ADHD: Blood level analysis and meta-analytic extension of supplementation trials. Clin. Psychol. Rev. 2014, 34, 496–505. [Google Scholar] [CrossRef] [PubMed]
- Tesei, A.; Crippa, A.; Ceccarelli, S.B.; Mauri, M.; Molteni, M.; Agostoni, C.; Nobile, M. The potential relevance of docosahexaenoic acid and eicosapentaenoic acid to the etiopathogenesis of childhood neuropsychiatric disorders. Eur. Child Adolesc. Psychiatry 2016, 26, 1011–1030. [Google Scholar] [CrossRef] [PubMed]
- Colter, A.L.; Cutler, C.; Meckling, K.A. Fatty acid status and behavioural symptoms of Attention Deficit Hyperactivity Disorder in adolescents: A case-control study. Nutr. J. 2008, 7, 8. [Google Scholar] [CrossRef] [PubMed]
- Crippa, A.; Agostoni, C.; Mauri, M.; Mauri, M.; Molteni, M.; Nobile, M. Polyunsaturated Fatty Acids Are Associated with Behavior but Not with Cognition in Children with and without ADHD: An Italian study. J. Atten. Disord. 2016. [Google Scholar] [CrossRef] [PubMed]
- Stevens, L.J.; Zentall, S.S.; Deck, J.L.; Abate, M.; Watkins, B.; Lipp, S.; Burgess, J. Essential fatty acid metabolism in boys with attention-deficit hyperactivity disorder. Am. J. Clin. Nutr. 1995, 62, 761–768. [Google Scholar] [PubMed]
- Mueser, K.T.; McGurk, S.R. Schizophrenia. Lancet 2004, 363, 2063–2072. [Google Scholar] [CrossRef]
- Whiteford, H.A.; Degenhardt, L.; Rehm, J.; Baxter, A.; Ferrari, A.; Erskine, H.; Charlson, F.; Norman, R.; Flaxman, A.; Johns, N.; et al. Global burden of disease attributable to mental and substance use disorders: Findings from the Global Burden of Disease Study 2010. Lancet 2013, 382, 1575–1586. [Google Scholar] [CrossRef]
- Van Os, J.; Linscott, R.J.; Myin-Germeys, I.; Delespaul, P.; Krabbendam, L. A systematic review and meta-analysis of the psychosis continuum: Evidence for a psychosis proneness-persistence-impairment model of psychotic disorder. Psychol. Med. 2009, 39, 179–195. [Google Scholar] [CrossRef] [PubMed]
- McGlashan, T.H. Commentary: Progress, issues, and implications of prodromal research: An inside view. Schizophr. Bull. 2003, 29, 851–858. [Google Scholar] [CrossRef] [PubMed]
- Ruhrmann, S.; Schultze-Lutter, F.; Salokangas, R.K.R.; Heinimaa, M.; Linszen, D.; Dingemans, P.; Birchwood, M.; Patterson, P.; Juckel, G.; Heinz, A.; et al. Prediction of psychosis in adolescents and young adults at high risk: Results from the prospective European prediction of psychosis study. Arch. Gen. Psychiatry 2010, 67, 241–251. [Google Scholar] [CrossRef] [PubMed]
- Yung, A.R.; Phillips, L.J.; Yuen, H.P.; Francey, S.; McFarlane, C.; Hallgren, M.; McGorry, P. Psychosis prediction: 12-month follow up of a high-risk (“prodromal”) group. Schizophr. Res. 2003, 60, 21–32. [Google Scholar] [CrossRef]
- Miller, T.J.; McGlashan, T.H.; Rosen, J.L.; Somjee, L.; Markovich, P.; Stein, K.; Woods, S. Prospective diagnosis of the initial prodrome for schizophrenia based on the Structured Interview for Prodromal Syndromes: Preliminary evidence of interrater reliability and predictive validity. Am. J. Psychiatry 2002, 159, 863–865. [Google Scholar] [CrossRef] [PubMed]
- Fusar-Poli, P. Prodromal psychosis: Diagnosis and treatment. Curr. Pharm. Des. 2012, 18, 337. [Google Scholar] [CrossRef] [PubMed]
- Stafford, M.R.; Jackson, H.; Mayo-Wilson, E.; Morrison, A.; Kendall, T. Early interventions to prevent psychosis: Systematic review and meta-analysis. BMJ 2013, 346, f185. [Google Scholar] [CrossRef] [PubMed]
- Evans, D.R.; Parikh V, V.; Khan, M.M.; Coussons, C.; Buckley, P.; Mahadik, S. Red blood cell membrane essential fatty acid metabolism in early psychotic patients following antipsychotic drug treatment. Prostaglandins Leukot. Essent. Fat. Acids 2003, 69, 393–399. [Google Scholar] [CrossRef]
- Glen, A.I.; Glen, E.M.; Horrobin, D.F.; Vaddadi, K.; Spellman, M.; Morse-Fisher, N.; Ellis, K.; Skinner, F. A red cell membrane abnormality in a subgroup of schizophrenic patients: Evidence for two diseases. Schizophr. Res. 1994, 12, 53–61. [Google Scholar] [CrossRef]
- Horrobin, D.F. The membrane phospholipid hypothesis as a biochemical basis for the neurodevelopmental concept of schizophrenia. Schizophr. Res. 1998, 30, 193–208. [Google Scholar] [CrossRef]
- Amminger, G.P.; Schäfer, M.R.; Papageorgiou, K.; Klier, C.; Cotton, S.; Harrigan, S.; Mackinnon, A.; McGorry, P.; Berger, G. Long-Chain ω-3 Fatty Acids for Indicated Prevention of Psychotic Disorders. Arch. Gen. Psychiatry 2010, 67, 146–154. [Google Scholar] [CrossRef] [PubMed]
- Emsley, R.; Myburgh, C.; Oosthuizen, P.; van Rensburg, S.J. Randomized, placebo-controlled study of ethyl-eicosapentaenoic acid as supplemental treatment in schizophrenia. Am. J. Psychiatry 2002, 159, 1596–1598. [Google Scholar] [CrossRef] [PubMed]
- Mellor, J.E.; Laugharne, J.D.; Peet, M. Schizophrenic symptoms and dietary intake of n-3 fatty acids. Schizophr. Res. 1995, 18, 85–86. [Google Scholar] [CrossRef]
- Schlögelhofer, M.; Amminger, G.P.; Schaefer, M.R.; Fusar-Poli, P.; Smesny, S.; Mcgorry, P.; Berger, G.; Mossaheb, N. Polyunsaturated fatty acids in emerging psychosis: A safer alternative? Early Interv. Psychiatry 2014, 8, 199–208. [Google Scholar] [CrossRef] [PubMed]
- McGorry, P.D.; Nelson, B.; Markulev, C.; Yuen, H.; Schäfer, M.; Mossaheb, N.; Schlögelhofer, M.; Smesny, S.; Hickie, I.; Berger, G. Effect of ω-3 Polyunsaturated Fatty Acids in Young People at Ultrahigh Risk for Psychotic Disorders. JAMA Psychiatry 2017, 74, 19. [Google Scholar] [CrossRef] [PubMed]
- Amminger, G.P.; Chanen, A.M.; Ohmann, S.; Klier, C.M.; Mossaheb, N.; Bechdolf, A.; Nelson, B.; Thompson, A.; McGorry, P.D.; Yung, A.R.; et al. Omega-3 Fatty Acid Supplementation in Adolescents with Borderline Personality Disorder and Ultra-High Risk Criteria for Psychosis: A Post Hoc Subgroup Analysis of a Double-Blind, Randomized Controlled Trial. Can. J. Psychiatry 2013, 58, 402–408. [Google Scholar] [CrossRef] [PubMed]
- Amminger, G.P.; Schäfer, M.R.; Schlögelhofer, M.; Klier, C.; McGorry, P. Longer-term outcome in the prevention of psychotic disorders by the Vienna omega-3 study. Nat. Commun. 2015, 6, 7934. [Google Scholar] [CrossRef] [PubMed]
- Smesny, S.; Milleit, B.; Hipler, U.-C.; Milleit, C.; Schäfer, M.; Klier, C.; Holub, M.; Holzer, I.; Berger, G.; Otto, M.; Nenadic, I. Omega-3 fatty acid supplementation changes intracellular phospholipase A2 activity and membrane fatty acid profiles in individuals at ultra-high risk for psychosis. Mol. Psychiatry 2014, 19, 317–324. [Google Scholar] [CrossRef] [PubMed]
- Pawełczyk, T.; Grancow-Grabka, M.; Kotlicka-Antczak, M.; Trafalska, E.; Pawełczyk, A. A randomized controlled study of the efficacy of six-month supplementation with concentrated fish oil rich in omega-3 polyunsaturated fatty acids in first episode schizophrenia. J. Psychiatr. Res. 2016, 73, 34–44. [Google Scholar] [CrossRef] [PubMed]
- Berger, G.E.; Proffitt, T.-M.; McConchie, M.; Yuen, H.; Wood, S.; Amminger, G.; Brewer, W.; McGorry, P. Ethyl-eicosapentaenoic acid in first-episode psychosis: A randomized, placebo-controlled trial. J. Clin. Psychiatry 2007, 68, 1867–1875. [Google Scholar] [CrossRef] [PubMed]
- Berger, G.E.; Wood, S.J.; Wellard, R.M.; Proffitt, T.; McConchie, M.; Amminger, G.; Jackson, G.; Velakoulis, D.; Pantelis, C.; McGorry, P. Ethyl-Eicosapentaenoic Acid in First-Episode Psychosis. A 1H-MRS Study. Neuropsychopharmacology 2008, 33, 2467–2473. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, K.; Wang, W.; Kang, U.J. The role of glutathione in dopaminergic neuronal survival. J. Neurochem. 1997, 69, 1850–1858. [Google Scholar] [CrossRef] [PubMed]
- Dringen, R. Metabolism and functions of glutathione in brain. Prog. Neurobiol. 2000, 62, 649–671. [Google Scholar] [CrossRef]
- Irving, C.B.; Mumby-Croft, R.; Joy, L.A. Polyunsaturated fatty acid supplementation for schizophrenia. In The Cochrane Database of Systematic Reviews; Irving, C.B., Ed.; John Wiley & Sons, Ltd.: Chichester, UK, 2006; p. CD001257. [Google Scholar]
- Freeman, M.P.; Hibbeln, J.R.; Wisner, K.L.; Davis, J.; Mischoulon, D.; Peet, M.; Keck, P.; Marangell, L.; Richardson, A.; Lake, J.; et al. Omega-3 fatty acids: Evidence basis for treatment and future research in psychiatry. J. Clin. Psychiatry 2006, 67, 1954–1967. [Google Scholar] [CrossRef] [PubMed]
- Fusar-Poli, P.; Berger, G. Eicosapentaenoic Acid Interventions in Schizophrenia. J. Clin. Psychopharmacol. 2012, 32, 179–185. [Google Scholar] [CrossRef] [PubMed]
- Chen, A.T.; Chibnall, J.T.; Nasrallah, H.A. A meta-analysis of placebo-controlled trials of omega-3 fatty acid augmentation in schizophrenia: Possible stage-specific effects. Ann. Clin. Psychiatry 2015, 27, 289–296. [Google Scholar] [PubMed]
- Akter, K.; Gallo, D.A.; Martin, S.A.; Myronyuk, N.; Roberts, R.; Stercula, K.; Raffa, R. A review of the possible role of the essential fatty acids and fish oils in the aetiology, prevention or pharmacotherapy of schizophrenia. J. Clin. Pharm. Ther. 2012, 37, 132–139. [Google Scholar] [CrossRef] [PubMed]
- Kelly, C.; Hadjinicolaou, A.V.; Holt, C.; Agius, M.; Zaman, R. Meta-analysis of medical and non-medical treatments of the prodromal phase of psychotic illness in at-risk mental states. Psychiatr. Danub. 2010, 22 (Suppl. S1), S56–S62. [Google Scholar] [PubMed]
- Preti, A.; Cella, M. Randomized-controlled trials in people at ultra high risk of psychosis: A review of treatment effectiveness. Schizophr. Res. 2010, 123, 30–36. [Google Scholar] [CrossRef] [PubMed]
- Souaiby, L.; Gaillard, R.; Krebs, M.-O. Durée de psychose non traitée: État des lieux et analyse critique. Encephale 2016, 42, 361–366. [Google Scholar] [CrossRef] [PubMed]
- Marshall, M.; Rathbone, J. Early intervention for psychosis. In The Cochrane Database of Systematic Reviews; Marshall, M., Ed.; John Wiley & Sons, Ltd.: Chichester, UK, 2011; p. CD004718. [Google Scholar]
- Müller, H.; Wießmann, T.; Bechdolf, A. Interventionen bei Personen mit erhöhtem Psychoserisiko: Eine aktuelle Übersicht über randomisiert kontrollierte Studien. Fortschr. Neurol. Psychiatr. 2012, 80, 570–579. [Google Scholar] [CrossRef] [PubMed]
- Van der Gaag, M.; Smit, F.; Bechdolf, A.; French, P.; Linszen, D.; Yung, A.; McGorry, P.; Cuijpers, P. Preventing a first episode of psychosis: Meta-analysis of randomized controlled prevention trials of 12 month and longer-term follow-ups. Schizophr. Res. 2013, 149, 56–62. [Google Scholar] [CrossRef] [PubMed]
- Mazahery, H.; Stonehouse, W.; Delshad, M.; Kruger, M.; Conlon, C.; Beck, K.; von Hurst, P. Relationship between Long Chain n-3 Polyunsaturated Fatty Acids and Autism Spectrum Disorder: Systematic Review and Meta-Analysis of Case-Control and Randomised Controlled Trials. Nutrients 2017, 9, 155. [Google Scholar] [CrossRef] [PubMed]
- Bent, S.; Hendren, R.L.; Zandi, T.; Law, K.; Choi, J.; Widjaja, F.; Kalb, L.; Nestle, J.; Law, P. Internet-Based, Randomized, Controlled Trial of Omega-3 Fatty Acids for Hyperactivity in Autism. J. Am. Acad. Child Adolesc. Psychiatry 2014, 53, 658–666. [Google Scholar] [CrossRef] [PubMed]
- Voigt, R.G.; Mellon, M.W.; Katusic, S.K.; Weaver, A.; Matern, D.; Mellon, B.; Jensen, C.; Barbaresi, W. A Randomized, Double-Blind, Placebo-Controlled Trial of Dietary Docosahexaenoic Acid (DHA) Supplementation in Children with Autism. J. Pediatr. Gastroenterol. Nutr. 2013, 58, 1. [Google Scholar] [CrossRef] [PubMed]
- Yui, K.; Koshiba, M.; Nakamura, S.; Kobayashi, Y. Effects of Large Doses of Arachidonic Acid Added to Docosahexaenoic Acid on Social Impairment in Individuals With Autism Spectrum Disorders. J. Clin. Psychopharmacol. 2012, 32, 200–206. [Google Scholar] [CrossRef] [PubMed]
- Horvath, A.; Łukasik, J.; Szajewska, H. ω-3 Fatty Acid Supplementation Does Not Affect Autism Spectrum Disorder in Children: A Systematic Review and Meta-Analysis. J. Nutr. 2017, 147, 367–376. [Google Scholar] [CrossRef] [PubMed]
- Anand, P.; Sachdeva, A. Effect of Poly Unsaturated Fatty Acids Administration on Children with Attention Deficit Hyperactivity Disorder: A Randomized Controlled Trial. J. Clin. Diagn. Res. 2016, 10, OC01–OC05. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.; Ostlund, S.; Fransson, G.; Kadesjö, B.; Gillberg, C. Omega-3/omega-6 fatty acids for attention deficit hyperactivity disorder: A randomized placebo-controlled trial in children and adolescents. J. Atten. Disord. 2009, 12, 394–401. [Google Scholar] [CrossRef] [PubMed]
- Salehi, B.; Mohammadbeigi, A.; Sheykholeslam, H.; Moshiri, E.; Dorreh, F. Omega-3 and Zinc supplementation as complementary therapies in children with attention-deficit/hyperactivity disorder. J. Res. Pharm. Pract. 2016, 5, 22–26. [Google Scholar] [CrossRef] [PubMed]
- Behdani, F.; Hebrani, P.; Naseraee, A.; Haghighi, M.; Akhavanrezayat, A. Does omega-3 supplement enhance the therapeutic results of methylphenidate in attention deficit hyperactivity disorder patients? J. Res. Med. Sci. 2013, 18, 653–658. [Google Scholar] [PubMed]
- Bos, D.J.; Oranje, B.; Veerhoek, E.S.; van Diepen, R.; Weusten, J.; Demmelmair, H.; Koletzko, B.; De Sain-Van Der Velden, M.G.; Eilander, A.; Hoeksma, M.; et al. Reduced Symptoms of Inattention after Dietary Omega-3 Fatty Acid Supplementation in Boys with and without Attention Deficit/Hyperactivity Disorder. Neuropsychopharmacology 2015, 40, 2298–2306. [Google Scholar] [CrossRef] [PubMed]
- Bélanger, S.A.; Vanasse, M.; Spahis, S.; Sylvestre, M.; Lippé, S.; L'heureux, F.; Ghadirian, P.; Vanasse, C.; Levy, E. Omega-3 fatty acid treatment of children with attention-deficit hyperactivity disorder: A randomized, double-blind, placebo-controlled study. Paediatr. Child Health 2009, 14, 89–98. [Google Scholar] [CrossRef] [PubMed]
- Gustafsson, P.A.; Birberg-Thornberg, U.; Duchén, K.; Landgren, M.; Malmberg, K.; Pelling, H.; Strandvik, B.; Karlsson, T. EPA supplementation improves teacher-rated behaviour and oppositional symptoms in children with ADHD. Acta Paediatr. 2010, 99, 1540–1549. [Google Scholar] [CrossRef] [PubMed]
- Kean, J.D.; Sarris, J.; Scholey, A.; Silberstein, R.; Downey, L.; Stough, C. Reduced inattention and hyperactivity and improved cognition after marine oil extract (PCSO-524®) supplementation in children and adolescents with clinical and subclinical symptoms of attention-deficit hyperactivity disorder (ADHD): A randomised, double-blind, placebo-controlled trial. Psychopharmacology 2017, 234, 403–420. [Google Scholar] [CrossRef] [PubMed]
- Manor, I.; Magen, A.; Keidar, D.; Rosen, S.; Tasker, H.; Cohen, T.; Richter, Y.; Zaaroor-Regev, D.; Manor, Y.; Weizman, A. The effect of phosphatidylserine containing Omega3 fatty-acids on attention-deficit hyperactivity disorder symptoms in children: A double-blind placebo-controlled trial, followed by an open-label extension. Eur. Psychiatry 2012, 27, 335–342. [Google Scholar] [CrossRef] [PubMed]
- Milte, C.M.; Parletta, N.; Buckley, J.D.; Buckley, J.; Coates, A.; Young, R.; Howe, P. Increased Erythrocyte Eicosapentaenoic Acid and Docosahexaenoic Acid Are Associated With Improved Attention and Behavior in Children With ADHD in a Randomized Controlled Three-Way Crossover Trial. J. Atten. Disord. 2015, 19, 954–964. [Google Scholar] [CrossRef] [PubMed]
- Milte, C.M.; Parletta, N.; Buckley, J.D.; Coates, A.; Young, R.; Howe, P. Eicosapentaenoic and docosahexaenoic acids, cognition, and behavior in children with attention-deficit/hyperactivity disorder: A randomized controlled trial. Nutrition 2012, 28, 670–677. [Google Scholar] [CrossRef] [PubMed]
- Vaisman, N.; Kaysar, N.; Zaruk-Adasha, Y.; Pelled, D.; Brichon, G.; Zwingelstein, G.; Bodennec, J. Correlation between changes in blood fatty acid composition and visual sustained attention performance in children with inattention: Effect of dietary n-3 fatty acids containing phospholipids. Am. J. Clin. Nutr. 2008, 87, 1170–1180. [Google Scholar] [PubMed]
- Widenhorn-Müller, K.; Schwanda, S.; Scholz, E.; Spitzer, M.; Bode, H. Effect of supplementation with long-chain ω-3 polyunsaturated fatty acids on behavior and cognition in children with attention deficit/hyperactivity disorder (ADHD): A randomized placebo-controlled intervention trial. Prostaglandins Leukot. Essent. Fat. Acids 2014, 91, 49–60. [Google Scholar] [CrossRef] [PubMed]
- Assareh, M.; Davari Ashtiani, R.; Khademi, M.; Jazayeri, S.; Rai, A.; Nikoo, M. Efficacy of Polyunsaturated Fatty Acids (PUFA) in the Treatment of Attention Deficit Hyperactivity Disorder. J. Atten. Disord. 2017, 21, 78–85. [Google Scholar] [CrossRef] [PubMed]
- Barragán, E.; Breuer, D.; Döpfner, M. Efficacy and Safety of Omega-3/6 Fatty Acids, Methylphenidate, and a Combined Treatment in Children With ADHD. J. Atten. Disord. 2017, 21, 433–441. [Google Scholar] [CrossRef] [PubMed]
- Hariri, M.; Djazayery, A.; Djalali, M.; Saedisomeolia, A.; Rahimi, A.; Abdolahian, E. Effect of n-3 supplementation on hyperactivity, oxidative stress and inflammatory mediators in children with attention-deficit-hyperactivity disorder. Malays. J. Nutr. 2012, 18, 329–335. [Google Scholar] [PubMed]
- Matsudaira, T.; Gow, R.V.; Kelly, J.; Murphy, C.; Potts, L.; Sumich, A.; Ghebremeskel, K.; Crawford, M.; Taylor, E. Biochemical and Psychological Effects of Omega-3/6 Supplements in Male Adolescents with Attention-Deficit/Hyperactivity Disorder: A Randomized, Placebo-Controlled, Clinical Trial. J. Child Adolesc. Psychopharmacol. 2015, 25, 775–782. [Google Scholar] [CrossRef] [PubMed]
- Stevens, L.; Zhang, W.; Peck, L.; Kuczek, T.; Grevstad, N.; Mahon, A.; Zentall, S.S.; Eugene Arnold, L.; Burgess, J.R. EFA supplementation in children with inattention, hyperactivity, and other disruptive behaviors. Lipids 2003, 38, 1007–1021. [Google Scholar] [CrossRef] [PubMed]
- Sinn, N.; Bryan, J. Effect of Supplementation with Polyunsaturated Fatty Acids and Micronutrients on Learning and Behavior Problems Associated with Child ADHD. J. Dev. Behav. Pediatr. 2007, 28, 82–91. [Google Scholar] [CrossRef] [PubMed]
- Sinn, N.; Bryan, J.; Wilson, C. Cognitive effects of polyunsaturated fatty acids in children with attention deficit hyperactivity disorder symptoms: A randomised controlled trial. Prostaglandins Leukot. Essent. Fat. Acids 2008, 78, 311–326. [Google Scholar] [CrossRef] [PubMed]
- Dubnov-Raz, G.; Khoury, Z.; Wright, I.; Raz, R.; Berger, I. The effect of α-linolenic acid supplementation on ADHD symptoms in children: A randomized controlled double-blind study. Front. Hum. Neurosci. 2014, 8, 780. [Google Scholar] [CrossRef] [PubMed]
- Raz, R.; Carasso, R.L.; Yehuda, S. The influence of short-chain essential fatty acids on children with attention-deficit/hyperactivity disorder: A double-blind placebo-controlled study. J. Child Adolesc. Psychopharmacol. 2009, 19, 167–177. [Google Scholar] [CrossRef] [PubMed]
- Dashti, N.; Hekmat, H.; Soltani, H.R.; Rahimdel, A.; Javaherchian, M. Comparison of therapeutic effects of omega-3 and methylphenidate (ritalin(®)) in treating children with attention deficit hyperactivity disorder. Iran. J. Psychiatry Behav. Sci. 2014, 8, 7–11. [Google Scholar] [PubMed]
- Perera, H.; Jeewandara, K.C.; Seneviratne, S.; Guruge, C. Combined ω3 and ω6 Supplementation in Children With Attention-Deficit Hyperactivity Disorder (ADHD) Refractory to Methylphenidate Treatment. J. Child Neurol. 2012, 27, 747–753. [Google Scholar] [CrossRef] [PubMed]
- Voigt, R.G.; Llorente, A.M.; Jensen, C.L.; Fraley, J.; Berretta, M.; Heird, W. A randomized, double-blind, placebo-controlled trial of docosahexaenoic acid supplementation in children with attention-deficit/hyperactivity disorder. J. Pediatr. 2001, 139, 189–196. [Google Scholar] [CrossRef] [PubMed]
- Campoy, C.; Escolano-Margarit, M.V.; Anjos, T.; Szajewska, H.; Uauy, R. Omega 3 fatty acids on child growth, visual acuity and neurodevelopment. Br. J. Nutr. 2012, 107, S85–S106. [Google Scholar] [CrossRef] [PubMed]
- Innis, S.M. Fatty acids and early human development. Early Hum. Dev. 2007, 83, 761–766. [Google Scholar] [CrossRef] [PubMed]
- Agostoni, C.; Mazzocchi, A.; Leone, L.; Ciappolino, V.; Delvecchio, G.; Altamura, C.; Brambilla, P. The first model of keeping energy balance and optimal psycho affective development: Breastfed infants. J. Affect. Disord. 2017, 224, 10–15. [Google Scholar] [CrossRef] [PubMed]
- Clandinin, M.T.; Chappell, J.E.; Leong, S.; Heim, T.; Swyer, P.; Chance, G. Extrauterine fatty acid accretion in infant brain: Implications for fatty acid requirements. Early Hum. Dev. 1980, 4, 131–138. [Google Scholar] [CrossRef]
- Martinez, M. Tissue levels of polyunsaturated fatty acids during early human development. J. Pediatr. 1992, 120, S129–S138. [Google Scholar] [CrossRef]
- Innis, S.M. Omega-3 Fatty acids and neural development to 2 years of age: Do we know enough for dietary recommendations? J. Pediatr. Gastroenterol. Nutr. 2009, 48 (Suppl. S1), S16–S24. [Google Scholar] [CrossRef] [PubMed]
- Williams, C.; Birch, E.E.; Emmett, P.M.; Northstone, K. Stereoacuity at age 3.5 y in children born full-term is associated with prenatal and postnatal dietary factors: A report from a population-based cohort study. Am. J. Clin. Nutr. 2001, 73, 316–322. [Google Scholar] [PubMed]
- Bloch, M.H. Qawasmi A Omega-3 fatty acid supplementation for the treatment of children with attention-deficit/hyperactivity disorder symptomatology: Systematic review and meta-analysis. J. Am. Acad. Child Adolesc. Psychiatry 2011, 50, 991–1000. [Google Scholar] [CrossRef] [PubMed]
- Sonuga-Barke, E.J.S.; Brandeis, D.; Cortese, S.; Daley, D.; Ferrin, M.; Holtmann, M.; Stevenson, J.; Danckaerts, M.; van der Oord, S. Nonpharmacological Interventions for ADHD: Systematic Review and Meta-Analyses of Randomized Controlled Trials of Dietary and Psychological Treatments. Am. J. Psychiatry 2013, 170, 275–289. [Google Scholar] [CrossRef] [PubMed]
- Puri, B.K.; Martins, J.G. Which polyunsaturated fatty acids are active in children with attention-deficit hyperactivity disorder receiving PUFA supplementation? A fatty acid validated meta-regression analysis of randomized controlled trials. Prostaglandins Leukot. Essent. Fat. Acids 2014, 90, 179–189. [Google Scholar] [CrossRef] [PubMed]
- Richardson, A.J.; Montgomery, P. The Oxford-Durham study: A randomized, controlled trial of dietary supplementation with fatty acids in children with developmental coordination disorder. Pediatrics 2005, 115, 1360–1366. [Google Scholar] [CrossRef] [PubMed]
| Ultra Hight Risk Psychosis | |||||
| Study | N. Sample | N-PUFA Assessed Daily Amounts | Duration (Weeks) | Outcome Measures | Major Finding |
| [46] | 76 of 81 participants (93.8%) completed the intervention (aged 13–25) | MONO 1.2 g/day (EPA 700 mg + DHA 480 mg) or PLACEBO + 7.6 mg Vit E | 12 + 40 of follow up | Primary outcome transition to psychosis Secondary outcomes included symptomatic and functional changes | A significant reduction in ω-3 PUFAs group of positive symptoms, negative symptoms, and general symptoms and improved functioning compared with placebo. |
| [51] | 15 | MONO 1.2 g (EPA + DHA) day OR PLACEBO | 12 | PANSS, MADRS GAF Udvalg for Kliniske Undersøgelser (SCALE for SIDE EFFECTS) | ω-3 PUFA significantly improved functioning and reduced psychiatric symptoms, compared with placebo. Side effects did not differ between the treatment groups |
| [50] | 304 (aged between 13 and 40 years) | MONO 1.4 g (EPA + DHA) or PLACEBO + CBCM | 24 | Transition to psychosis status at 6 months BPRS SANS MADRS YMRS SOFAS GF: S GF: R | ω-3 PUFAs are not effective under conditions where good quality, evidence-based psychosocial treatment is available |
| First episode Psychosis | |||||
| Study | N. Sample | N-PUFA Assessed Daily Amounts | Duration (Weeks) | Outcome Measures | Major Finding |
| [55] | ADD ON 2 g EPA OR PLACEBO | 80 FEP but only 69 were eligible for analysis | 12 | Primary outcome PANSS GAF CGI Secondary outcome measures: tolerability measures and cumulative anti psychotic dose | EPA no efficacy on specific psychotic symptoms |
| [54] | 71 (aged 16–35) | ADD ON 2.2 g/day (EPA + DHA) or PLACEBO | 26 | PANSS | Significant differences between the study arms regarding total PANSS score change favoring ω-3 PUFA. |
| ADHD | |||||
| Study | N. Sample | N-PUFA Assessed Daily Amounts | Duration (Weeks) | Outcome Measures | Major Finding |
| [75] | 50 | ADD ON ATX + 180 mg EPA + 120 mg DHA OR ATX | 16 | KSAD S-PLCPRS | Study group had greater but not statistically significant (p = 0.08) reduction in CPRS ADHD scores. |
| [88] | 40 | ADD ON MPH + 241 mg DHA + 33 mg EPA + 180 mg omega 6 per day OR MPH + placebo | 10 | ADHD-RS Side-Effect questionnaire | ADHD-RS scores decreased significantly within both groups but total score and scores of inattention, hyperactivity, and impulsivity were not significantly different between the groups. |
| [89] | 90 | ADD ON 558 mg EPA + 174 mg DHA + 60 mg GLA per day OR MPH + 558 mg EPA + 174 mg DHA + 60 mg GLA per day OR MPH | 48 | ADHD-RS CGI-S | No significant differences between MPH + Omega-3/6 and MPH alone. Significant differences between Omega-3/6 and MPH + Omega-3/6 in ADHD Total score and Hyperactivity-Impulsivity indicating a stronger effect for combined treatment compared with Omega-3/6. |
| [78] | 69 | ADD ON MPH + 240 mg DHA + 360 mg EPA per day OR MPH + placebo | 8 | ADHD-RS | Both groups had a significant improvement of ADHD symptoms but there was no significant difference between them. |
| [79] | 40 | MONO 650 mg DHA + 650 mg EPA per day OR placebo (margarine) | 16 | fMRI scan with a Go-No-Go task; CBCL; SWAN | Scores on CBCL attention problems were reduced in comparison with placebo (p < 0.001). No effect of EPA/DHA on Go-No-Go task or on fMRI measures. |
| [80] | 26 | MONO 20–25 mg/kg EPA + 8.5 − 10.5 mg/kg DHA per day OR placebo (sunflower oil) | 8 | SWAN CPRS-L CPT Go-No-Go test | CPRS subscales measuring symptoms of inattention and impulsivity showed a significant improvement in both groups; study group showed a greater but not statistically significant improvement. |
| [97] | 85 | MONO 1 g omega 3 per day OR MPH OR placebo | 4 | CPRS CTRS KBIT (for IQ) | Significant association between treatment with MPH or omega 3 and improvement in hyperactivity-impulsivity and combined subtypes. No significant association between treatment with placebo and improvement. |
| [95] | 17 | MONO 1 g ALA per day OR placebo (lactose) | 8 | MOXO-CPT CPRS CTRS | No significant differences between groups in the changes from pre- to post-supplementation values on CPRS, CTRS and MOXO-CPT |
| [81] | 92 | MONO 500 mg EPA + 2.7 mg DHA and 10 mg Vitamin E per day OR placebo (rape seed oil and medium-chain triglycerides) | 15 | CPRS CTRS | Supplementation improved CTRS inattention/cognitive subscale (p = 0.04) but not Conners’ total score. In oppositional children (n = 48) CTRS total score improved ≥25% in 48% of the children in study group vs. 9% for placebo (p = 0.001). |
| [90] | 103 | ADD ON Ritalin + 635 mg EPA + 195 mg DHA + 100 mg other omega 3 fatty acids per day OR Ritalin + placebo (olive oil) | 8 | ASQ-P | Significant improvement from week in ASQ-P scores of the omega-3 group. |
| [76] | 64 | MONO 558 mg EPA + 174 mg DHA + 60 mg GLA per day OR placebo (olive oil) | 12 | ADHD-RS CGI-S | Improvement on CGI-S in the study group significantly greater than in the placebo group. More than half of all children did not respond to treatment. However, 26% in the study group responded versus 7% in the placebo group. |
| [83] | 147 | MONO 300 mg PS and 120 mg EPA + DHA (EPA/DHA ratio of 2:1) per day OR placebo (cellulose) | 15 | CPRS CTRS SDQ CHQ-PF50 | Significant reduction in the Restless/Impulsive subscale of CPRS and in Parental Emotional Impact subscale of the CHQ in the study group compared to placebo group. |
| [91] | 76 | MONO 558 mg EPA + 174 mg DHA + 60 mg GLA + 9.6 mg vitamin E per day OR placebo (medium chain triglycerides) | 12 | CTRS CPRS BIS | LC-PUFA supplementation did not improve ADHD symptoms at 12 weeks follow-up. |
| [84] | 87 | MONO 1109 mg EPA + 108 mg DHA + Vitamine E per day or 264 mg EPA, 1032 mg DHA + Vitamine E per day OR placebo (safflower oil) | 48 | word reading and spelling subtests from WIAT-III Vocabulary subtest from WISC-III CPRS TEA-ch Go/No-go | No significant treatment effects for literacy, cognition or parent-reported behavior. |
| [85] | 87 ADHD | MONO 1109 mg EPA + 108 mg DHA + Vitamine E per day OR 264 mg EPA + 1032 mg DHA + Vitamine E per day OR placebo (safflower oil) | 16 | word reading and spelling subtests from WIAT-III Vocabulary subtest from WISC-III CPRS TEA-ch Go/No-go | No significant treatment effects for literacy, cognition or parent-reported behavior. |
| [98] | 94 | ADD ON 592.74 mg omega 3 + 361.5 mg omega 6 per day + MPH OR placebo (sunflower oil) + MPH | 24 | 11-item checklist completed by the parents. | Significant improvement in the study group compared with the placebo group (p < 0.01) at 12 weeks in restlessness, aggressiveness, completing work and academic performance. Significant improvement became evident at 24 weeks (p < 0.05) also for inattention, impulsiveness, and cooperation with parents and teachers. |
| [96] | 63 | MONO 480 mg LA + 120 mg ALA + 190 mg mineral oil + 10 mg a-tocopherol per day OR placebo (vitamin c) | 7 | DSM-IV questionnaire for ADHD Abbreviated CPRS/CTRS TOVA | Both groups ameliorated some of the symptoms, but no significant differences were found between the groups in any of variables explored |
| [77] | 150 | ADD ON Ritalin + 100–400 mg EPA per day depending on weight OR Ritalin + 22 mg zinc sulfate OR Ritalin + placebo (sugar) | 8 | CPRS CTRS | A significant decreasing trend in all three groups was observed. No significant differences between groups on average Conners’ scores at Week 8. |
| [92] | 50 | MONO 480 mg DHA + 80 mg EPA + 40 mg AA + 96 mg GLA per day OR placebo (olive oil) | 16 | ASQ-Parents/Teachers DBD-Parents/Teachers CPT WJ-R | ASQ: Significant decrease from baseline within both placebo and PUFA group but no treatment effect. DBD: For conduct problems rated by parents and for attention symptoms rated by teachers, study group showed significant improvement over the placebo group. |
| [86] | 60 | MONO 156 mg EPA + 95 mg DHA containing 300 mg PL-omega 3 per day OR 153 mg EPA + 96 mg DHA containing FO OR placebo (rapeseed oil) | 12 | TOVA ASQ CBCL 4–18 | Total TOVA score was significantly affected by the treatments: PL-omega 3 > FO > placebo. The proportion of subjects with normative scores in the PL-omega-3 group (11/18) was statistically different from that of the placebo group (3/21), but not from the FO group (7/21). The PL-omega-3 and, to a limited extent, the FO group significantly improved the executive functioning in almost all TOVA-adjusted variables compared with placebo |
| [99] | 54 | ADD ON MPH + 345 mg DHA per day OR MPH + not specified placebo | 16 | TOVA Children’s Color Trails Test CBCL CPRS | No statistically significant improvement in any measure of ADHD symptoms. |
| [87] | 95 | MONO 600 mg EPA + 120 mg DHA + 15 mg of vitamin E per day OR Placebo (olive oil) | 16 | DISYPS-II CBCL TRF HAWIK IV KITAP 6–10 years TAP 10–18 years | Omega-3 improved working memory function, but had no effect on other cognitive measures and on DISYPS-II, CBCL or TRF. |
| Elevated ADHD Symptoms | |||||
| Study | N. Sample | N-PUFA Assessed Daily Amounts | Duration (Weeks) | Outcome Measures | Major Finding |
| [82] | 112 | MONO 21.9/29.2 mg EPA + 16.5/22 mg DHA + 300/400 mg natural mono-unsaturated olive oil + 0.675/0.9 mg vitamin E per day depending on age OR placebo (olive oil, lecithin, coconut oil and β-carotene) | 14 | CPRS COMPASS cognitive battery TOVA BRUMS EEG CGI | No significant difference between treatment groups on CPRS. Significant treatment effects on CPRS scores of hyperactivity, attention, learning and probability of ADHD for children who did not meet criteria for combined hyperactivity and inattention. Significant improvements in the study group on delayed working memory between baseline and Week 8. |
| [93] | 104 | MONO 558 mg EPA + 174 mg DHA+ 60 mg GLA + 10.8 mg vitamin E per day, alone or associated with a multivitamin/mineral supplement OR placebo (palm oil) | 15 | CPRS CTRS | CPRS: Significant improvements in the PUFA groups (combined) compared with placebo on core ADHD symptoms (inattention, hyperactivity, and impulsivity) and on ratings of oppositional behavior CTRS: No significant results. |
| [94] | 109 | MONO 558 mg EPA + 174 mg DHA+ 60 mg GLA + 10.8 mg vitamin E per day, alone or associated with a multivitamin/mineral supplement OR placebo (palm oil) | 15 | CPRS CTRS Creature-Counting test Short form of WISC-III Inspection time Rey Auditory-Verbal Learning Test Knock and Tap NEPSY subtest Stroop color–word test | Creature Counting: Over 15 weeks, there was a significant improvement in the PUFA groups compared to placebo. |
| Autism | |||||
| Study | N. Sample | N-PUFA Assessed Daily Amounts | Duration (Weeks) | Outcome Measures | Major Finding |
| [71] | 57 | 1.3 g of ω-3 PUFA per day OR placebo | 6 | the change in hyperactivity on the Aberrant Behavior Checklist (ABC-H, parent and teacher) Secondary outcomes included changes in the other subscales of the ABC and the Social Responsiveness Scale (SRS). | Children in the omega-3 fatty acid group had a greater reduction in hyperactivity, but the difference was not statistically significant. This study found statistically significant improvements in the ω-3 PUFA group in the stereotypy and lethargy subscales of the ABC. |
| [72] | 48 | DHA supplementation of 200 mg/day OR placebo. | 26 | The primary outcome measure was a significant positive response on the Clinical Global Impressions-Improvement (CGI-I) scale. Secondary outcome measures were changes in behavior or development noted on the Aberrant Behavior Checklist (ABC), the Behavior Assessment Scale for Children (BASC), and the Child Development Inventory (CDI) | The DHA group was not rated as improved in core symptoms of autism compared to the placebo group on the CGI-I. Parents (but not teachers) provided a higher average rating of social skills on the BASC for the children in the placebo group compared to the DHA group Teachers (but not parents) provided a higher average rating of functional communication on the BASC for the children in the DHA group compared to the placebo group |
| [73] | 13 | 240 mg of ARA-enriched triglyceride (40 mg/capsule each of ARA and DHA, and 0.16 mg/capsule of astaxanthin). The usual daily doses of this capsule were 6 capsules (240 mg). The placebo was an identical capsule containing olive oil. | 16 | The outcome measures were the Social Responsiveness Scale and the Aberrant Behavior Checklist-Community. | This supplementation regimen significantly improved Aberrant Behavior Checklist-Community-measured social withdrawal and Social Responsiveness Scale-measured communication. |
| Diagnosis | Positive Results | Negative Results | Positive Results Without Statistical Significance |
|---|---|---|---|
| Ultra Hight Risk Psychosis | [46,51] | [50] | |
| First psychosis episode | [54] | [55] | |
| ADHD | [76,79,81,83,86,90,98] | [84,85,87,91,95,99] | [75,77,78,80,88,89,92,96,97] |
| Elevated ADHD symptoms | [93,94] | [82] | |
| Autism | [73] | [72] | [71] |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Agostoni, C.; Nobile, M.; Ciappolino, V.; Delvecchio, G.; Tesei, A.; Turolo, S.; Crippa, A.; Mazzocchi, A.; Altamura, C.A.; Brambilla, P. The Role of Omega-3 Fatty Acids in Developmental Psychopathology: A Systematic Review on Early Psychosis, Autism, and ADHD. Int. J. Mol. Sci. 2017, 18, 2608. https://doi.org/10.3390/ijms18122608
Agostoni C, Nobile M, Ciappolino V, Delvecchio G, Tesei A, Turolo S, Crippa A, Mazzocchi A, Altamura CA, Brambilla P. The Role of Omega-3 Fatty Acids in Developmental Psychopathology: A Systematic Review on Early Psychosis, Autism, and ADHD. International Journal of Molecular Sciences. 2017; 18(12):2608. https://doi.org/10.3390/ijms18122608
Chicago/Turabian StyleAgostoni, Carlo, Maria Nobile, Valentina Ciappolino, Giuseppe Delvecchio, Alessandra Tesei, Stefano Turolo, Alessandro Crippa, Alessandra Mazzocchi, Carlo A. Altamura, and Paolo Brambilla. 2017. "The Role of Omega-3 Fatty Acids in Developmental Psychopathology: A Systematic Review on Early Psychosis, Autism, and ADHD" International Journal of Molecular Sciences 18, no. 12: 2608. https://doi.org/10.3390/ijms18122608
APA StyleAgostoni, C., Nobile, M., Ciappolino, V., Delvecchio, G., Tesei, A., Turolo, S., Crippa, A., Mazzocchi, A., Altamura, C. A., & Brambilla, P. (2017). The Role of Omega-3 Fatty Acids in Developmental Psychopathology: A Systematic Review on Early Psychosis, Autism, and ADHD. International Journal of Molecular Sciences, 18(12), 2608. https://doi.org/10.3390/ijms18122608







