What Do We Know about Opioids and the Kidney?
Abstract
:1. Introduction
2. Why Has Opioid Use Increased?
3. Context of Renal Failure from Opioid Use
4. Incidence of Renal Failure from Opioid Use
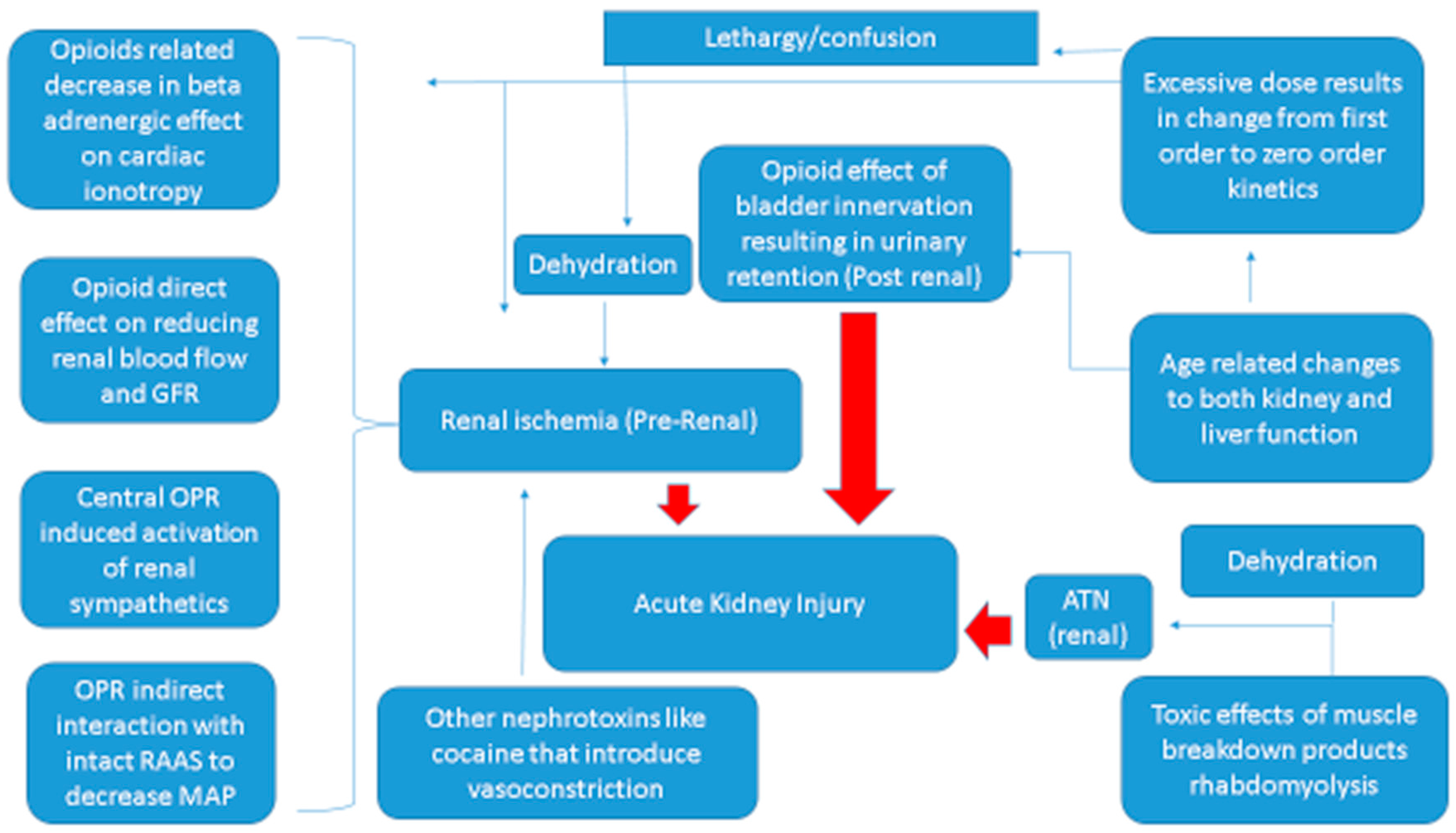
5. Mechanisms of Kidney Damage with Opioid Use
5.1. Enhancing Para-Sympathetics and Reducing Sympathetic Effect
5.2. Opioid and the Renin–Angiotensin–Aldosterone System (RAAS) and Anti-Diuretic Hormone (ADH)
5.3. Dehydration
5.4. Rhabdomyolysis and AKI with Opioids
5.5. Opioid-Related Urinary Retention
6. Clinical Events and Treatment of AKI Due to Opioids
7. Treatment
8. Other Clinical Findings with Opioid-Induced AKI
9. Chronic Kidney Disease and opioids
9.1. Opioids Use Leading to CKD
9.2. Heroin Nephropathy: Focal and Segmental Glomerulosclerosis (FSGS), Apol1 and HIV
9.3. CKD Due to Amyloidosis from Skin Popping with Opioids
10. Multiple Classes of Pain Medication Use and CKD
11. Use of Opioids in CKD
12. Changes with Elderly
13. Safe Use of Opioids in Those with Chronic Kidney Disease
14. Conclusions
Author Contributions
Conflicts of Interest
References
- Hernandez, S.H.; Nelson, L.S. Prescription drug abuse: Insight into the epidemic. Clin. Pharmacol. Ther. 2010, 88, 307–317. [Google Scholar] [CrossRef] [PubMed]
- Manchikanti, L.; Singh, A. Therapeutic opioids: A ten-year perspective on the complexities and complications of the escalating use, abuse, and nonmedical use of opioids. Pain Phys. 2008, 11, 63–88. [Google Scholar]
- Martins, S.S.; Sampson, L.; Cerdá, M.; Galea, S. Worldwide prevalence and trends in unintentional drug overdose: A systematic review of the literature. Am. J. Public Health 2015, 105, 29–49. [Google Scholar] [CrossRef] [PubMed]
- Ihongbe, T.O.; Masho, S.W. Prevalence, correlates and patterns of heroin use among young adults in the United States. Addict. Behav. 2016, 63, 74–81. [Google Scholar] [CrossRef] [PubMed]
- Cerda, M.; Ransome, Y.; Keyes, K.M.; Koenen, K.C.; Tracy, M.; Tardiff, K.J.; Vlahov, D.; Galea, S. Prescription opioid mortality trends in New York City, 1990–2006: Examining the emergence of an epidemic. Drug Alcohol. Depend. 2013, 132, 53–62. [Google Scholar] [CrossRef] [PubMed]
- Havens, J.R.; Young, A.M.; Havens, C.E. Nonmedical prescription drug use in a nationally representative sample of adolescents: Evidence of greater use among rural adolescents. Arch. Pediatr. Adolesc. Med. 2011, 165, 250–255. [Google Scholar] [CrossRef] [PubMed]
- Wu, L.T.; Woody, G.E.; Yang, C.; Blazer, D.G. Subtypes of nonmedical opioid users: Results from the national epidemiologic survey on alcohol and related conditions. Drug Alcohol Depend. 2010, 112, 69–80. [Google Scholar] [CrossRef] [PubMed]
- Novick, T.; Liu, Y.; Alvanzo, A.; Zonderman, A.B.; Evans, M.K.; Crews, D.C. Lifetime cocaine and opiate use and chronic kidney disease. Am. J. Nephrol. 2016, 44, 447–453. [Google Scholar] [CrossRef] [PubMed]
- Barbosa-Leiker, C.; McPherson, S.; Daratha, K.; Alicic, R.; Short, R.; Dieter, B.; Chaytor, N.; Roll, J.; Tuttle, K.R. Association between prescription opioid use and biomarkers of kidney disease in US adults. Kidney Blood Press Res. 2016, 41, 365–373. [Google Scholar] [CrossRef] [PubMed]
- Novick, T.; Kuo, Y.F.; Raji, M.A.; Chen, N.W.; Hasan, H.; Goodwin, J.S. Trends in opioid prescriptions among part D medicare recipients from 2007 to 2012. Am. J. Med. 2016, 129, 21–30. [Google Scholar]
- Christensen, K.; Doblhammer, G.; Rau, R.; Vaupel, J.W. Ageing populations: The challenges ahead. Lancet 2009, 374, 1196–1208. [Google Scholar] [CrossRef]
- Mallappallil, M.; Friedman, E.A.; Delano, B.G.; McFarlane, S.I.; Salifu, M.O. Chronic kidney disease in the elderly: Evaluation and management. Clin. Pract. 2014, 11, 525–535. [Google Scholar] [CrossRef] [PubMed]
- Campbell, C.I.; Weisner, C.; Leresche, L.; Ray, G.T.; Saunders, K.; Sullivan, M.D.; Banta-Green, C.J.; Merrill, J.O.; Silverberg, M.J.; Boudreau, D.; et al. Age and gender trends in long-term opioid analgesic use for noncancer pain. Am. J. Public Health 2010, 100, 2541–2547. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.I.; Walsh, D.; Brito-Dellan, N. Opioid and adjuvant analgesics: Compared and contrasted. Am. J. Hosp. Palliat. Care 2011, 28, 378–383. [Google Scholar] [CrossRef] [PubMed]
- Porubsky, S.; Kuppe, C.; Maier, T.; Birk, H.W.; Wörnle, M.; Moeller, M.J.; Floege, J.; Gröne, H.J. Renal lipidosis in patients enrolled in a methadone substitution program. Arch. Pathol. Lab Med. 2014, 138, 689–693. [Google Scholar] [CrossRef] [PubMed]
- Davis, M.P.; Srivastava, M. Demographics, assessment and management of pain in the elderly. Drugs Aging 2003, 20, 23–57. [Google Scholar] [CrossRef] [PubMed]
- Brouwer, B.A.; de Greef, B.T.; Hoeijmakers, J.G.; Geerts, M.; van Kleef, M.; Merkies, I.S.; Faber, C.G. Neuropathic pain due to small fiber neuropathy in aging: Current management and future prospects. Drugs Aging 2015, 32, 611–621. [Google Scholar] [CrossRef] [PubMed]
- Mercadante, S.; Ferrera, P.; Villari, P.; Casuccio, A. Opioid escalation in patients with cancer pain: The effect of age. J. Pain Sympt. Manag. 2006, 32, 413–419. [Google Scholar] [CrossRef] [PubMed]
- Nolin, T.D.; Naud, J.; Leblond, F.A.; Pichette, V. Emerging evidence of the impact of kidney disease on drug metabolism and transport. Clin. Pharmacol. Ther. 2008, 83, 898–903. [Google Scholar] [CrossRef] [PubMed]
- Feng, G.; Luo, Q.; Guo, E.; Yao, Y.; Yang, F.; Zhang, B.; Li, L. Multiple organ dysfunction syndrome, an unusual complication of heroin intoxication: A case report and review of literature. Int. J. Clin. Exp. Pathol. 2015, 8, 11826–11830. [Google Scholar] [PubMed]
- Zhao, A.; Tan, M.; Maung, A.; Salifu, M.; Mallappallil, M. Rhabdomyolysis and acute kidney injury requiring dialysis as a result of concomitant use of atypical neuroleptics and synthetic cannabinoids. Case Rep. Nephrol. 2015, 2015, 235982. [Google Scholar] [CrossRef] [PubMed]
- Melli, G.; Chaudhry, V.; Cornblath, D.R. Rhabdomyolysis: An evaluation of 475 hospitalized patients. Medicine 2005, 84, 377–385. [Google Scholar] [CrossRef] [PubMed]
- Gangahar, D. A case of rhabdomyolysis associated with severe opioid withdrawal. Am. J. Addict. 2015, 24, 400–402. [Google Scholar] [CrossRef] [PubMed]
- Schultz, J.J.; Hsu, A.K.; Gross, G.J. Ischemic preconditioning and morphine-induced cardioprotection involve the delta δ-opioid receptor in the intact rat heart. J. Mol. Cell Cardiol. 1997, 29, 2187–2195. [Google Scholar] [CrossRef] [PubMed]
- Pepe, S.; van den Brink, O.W.; Lakatta, E.G.; Xiao, R.P. Cross-talk of opioid peptide receptor and β-adrenergic receptor signalling in the heart. Cardiovasc. Res. 2004, 63, 414–422. [Google Scholar] [CrossRef] [PubMed]
- Kuczeriszka, M.; Lipkowski, A.W.; Sadowski, J.; Kompanowska-Jezierska, E. An endomorphine analog ([d-Ala(2)]-Endomorphin 2, TAPP) lowers blood pressure and enhances tissue nitric oxide in anesthetized rats. Pharmacol. Rep. 2016, 68, 616–619. [Google Scholar] [CrossRef] [PubMed]
- Frithiof, R.; Rundgren, M. Activation of central opioid receptors determines the timing of hypotension during acute hemorrhage-induced hypovolemia in conscious sheep. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2006, 291, R987–R996. [Google Scholar] [CrossRef] [PubMed]
- Schenk, H.D.; Radke, J.; Ensink, F.B.; Drobnik, L.; Kettler, D.; Sonntag, H.; Hellige, G.; Bretschneider, H.J. Interactions between renal and general hemodynamics in fentanyl, droperidol, ketamine, thiopental and in peridural anesthesia—Animal studies. Anaesthesiol. Reanim. 1995, 20, 60–70. [Google Scholar] [PubMed]
- Mutoh, J.; Ohsawa, M.; Hisa, H. Effect of naloxone on ischemic acute kidney injury in the mouse. Neuropharmacology 2013, 71, 10–18. [Google Scholar] [CrossRef] [PubMed]
- Mercatello, A. Changes in renal function induced by anesthesia. Ann. Fr. Anesth. Reanim. 1990, 9, 507–524. [Google Scholar] [CrossRef]
- Burchardi, H.; Kaczmarczyk, G. The effect of anaesthesia on renal function. Eur. J. Anaesthesiol. 1994, 11, 163–168. [Google Scholar] [PubMed]
- Priano, L.L.; Vatner, S.F. Morphine effects on cardiac output and regional blood flow distribution in conscious dogs. Anesthesiology 1981, 55, 236–243. [Google Scholar] [CrossRef] [PubMed]
- Mousa, S.A.; Shaqura, M.; Schäper, J.; Huang, W.; Treskatsch, S.; Habazettl, H.; Abdul-Khaliq, H.; Schäfer, M. Identification of μ- and κ-opioid receptors as potential targets to regulate parasympathetic, sympathetic, and sensory neurons within rat intracardiac ganglia. J. Comp. Neurol. 2010, 518, 3836–3847. [Google Scholar] [CrossRef] [PubMed]
- Staessen, J.; Fiocchi, R.; Bouillon, R.; Fagard, R.; Hespel, P.; Lijnen, P.; Moerman, E.; Amery, A. Effects of opioid antagonism on the haemodynamic and hormonal responses to exercise. Clin. Sci. 1988, 75, 293–300. [Google Scholar] [CrossRef] [PubMed]
- Badzynska, B.; Lipkowski, A.W.; Olszyński, K.H.; Sadowski, J. Different blood pressure responses to opioids in 3 rat hypertension models: Role of the baseline status of sympathetic and renin–angiotensin systems. Can. J. Physiol. Pharmacol. 2016. [Google Scholar] [CrossRef]
- Stotts, N.A.; Arai, S.R.; Cooper, B.A.; Nelson, J.E.; Puntillo, K.A. Predictors of thirst in intensive care unit patients. J. Pain Sympt. Manag. 2015, 49, 530–538. [Google Scholar] [CrossRef] [PubMed]
- Lal, J.; Atkinson, J. Involvement of the renin–angiotensin system in the dipsogenic effect of morphine. Arch. Int. Pharmacodyn. Ther. 1985, 278, 273–291. [Google Scholar] [PubMed]
- Ikonomov, O.C.; Stoynev, A.G.; Kurtev, I.V. Effect of morphine withdrawal on food and water intake, urine output and electrolyte excretion in the rat: Participation of the renin–aldosterone–system in renal excretory changes. Acta Physiol. Hung. 1984, 63, 137–146. [Google Scholar] [PubMed]
- Roncal-Jimenez, C.A.; García-Trabanino, R.; Wesseling, C.; Johnson, R.J. Mesoamerican nephropathy or global warming nephropathy? Blood Purif. 2016, 41, 135–138. [Google Scholar] [CrossRef] [PubMed]
- Roncal Jimenez, C.A.; Ishimoto, T.; Lanaspa, M.A.; Rivard, C.J.; Nakagawa, T.; Ejaz, A.A.; Cicerchi, C.; Inaba, S.; Le, M.; Miyazaki, M.; et al. Fructokinase activity mediates dehydration-induced renal injury. Kidney Int. 2014, 86, 294–302. [Google Scholar] [CrossRef] [PubMed]
- Chau, D.L.; Walker, V.; Pai, L.; Cho, L.M. Opiates and elderly: Use and side effects. Clin. Interv. Aging 2008, 3, 273–278. [Google Scholar] [CrossRef] [PubMed]
- Dray, A.; Metsch, R. Opioid receptor subtypes involved in the central inhibition of urinary bladder motility. Eur. J. Pharmacol. 1984, 104, 47–53. [Google Scholar] [CrossRef]
- DeGroot, J.F.; Coggeshall, R.E.; Carlton, S.M. The reorganization of mu opioid receptors in the rat dorsal horn following peripheral axotomy. Neurosci. Lett. 1997, 233, 113–116. [Google Scholar] [CrossRef]
- Durant, P.A.; Yaksh, T.L. Drug effects on urinary bladder tone during spinal morphine-induced inhibition of the micturition reflex in unanesthetized rats. Anesthesiology 1988, 68, 325–334. [Google Scholar] [CrossRef] [PubMed]
- Malinovsky, J.M.; Le Normand, L.; Lepage, J.Y.; Malinge, M.; Cozian, A.; Pinaud, M.; Buzelin, J.M. The urodynamic effects of intravenous opioids and ketoprofen in humans. Anesth. Analg. 1998, 87, 456–461. [Google Scholar] [PubMed]
- Brown, C.V.; Rhee, P.; Chan, L.; Evans, K.; Demetriades, D.; Velmahos, G.C. Preventing renal failure in patients with rhabdomyolysis: Do bicarbonate and mannitol make a difference? J. Trauma 2004, 56, 1191–1196. [Google Scholar] [CrossRef] [PubMed]
- Anonymous. Manual of symbols, equations & definitions in pharmacokinetics. J. Clin. Pharmacol. 1982, 22, 1–23. [Google Scholar]
- Zhang, L.; Kang, Y.; Fu, P.; Cao, Y.; Shi, Y.; Liu, F.; Hu, Z.; Su, B.; Tang, W.; Qin, W. Myoglobin clearance by continuous venous-venous haemofiltration in rhabdomyolysis with acute kidney injury: A case series. Injury 2012, 43, 619–623. [Google Scholar] [CrossRef] [PubMed]
- Nolin, T.D.; Aronoff, G.R.; Fissell, W.H.; Jain, L.; Madabushi, R.; Reynolds, K.; Zhang, L.; Huang, S.M.; Mehrotra, R.; Flessner, M.F.; et al. Pharmacokinetic assessment in patients receiving continuous RRT: Perspectives from the Kidney Health Initiative. Clin. J. Am. Soc. Nephrol. 2015, 10, 159–164. [Google Scholar] [CrossRef] [PubMed]
- Kulacoglu, H.; Dener, C.; Kama, N.A. Urinary retention after elective cholecystectomy. Am. J. Surg. 2001, 182, 226–229. [Google Scholar] [CrossRef]
- Dolin, S.J.; Cashman, J.N. Tolerability of acute postoperative pain management: Nausea, vomiting, sedation, pruritus, and urinary retention. Evidence from published data. Br. J. Anaesth. 2005, 95, 584–591. [Google Scholar] [CrossRef] [PubMed]
- Lau, H.; Lam, B. Management of postoperative urinary retention: A randomized trial of in-out versus overnight catheterization. ANZ J. Surg. 2004, 74, 658–661. [Google Scholar] [CrossRef] [PubMed]
- Fernandez, R.S.; Griffiths, R.D. Duration of short-term indwelling catheters—A systematic review of the evidence. J. Wound Ostomy Cont. Nurs. 2006, 33, 145–513. [Google Scholar] [CrossRef]
- Gallo, S.; DuRand, J.; Pshon, N. A study of naloxone effect on urinary retention in the patient receiving morphine patient-controlled analgesia. Orthop. Nurs. 2008, 27, 111–115. [Google Scholar] [CrossRef] [PubMed]
- Parker, R.K.; Holtmann, B.; White, P.F. Patient-controlled epidural analgesia: Interactions between nalbuphine and hydromorphone. Anesth. Anal. 1997, 84, 757–763. [Google Scholar] [CrossRef]
- Paton, W.D. The action of morphine and related substances on contraction and on acetylcholine output of coaxially stimulated guinea-pig ileum. Br. J. Pharmacol. Chemother. 1957, 12, 119–127. [Google Scholar] [CrossRef] [PubMed]
- Zhou, P.L.; Li, Y.L.; Yan, L.D.; Yong, Z.; Yu, G.; Dong, H.J.; Yan, H.; Su, R.B.; Gong, Z.H. Effect of thienorphine on intestinal transit and isolated guinea-pig ileum contraction. World J. Gastroenterol. 2013, 19, 1444–1450. [Google Scholar] [CrossRef] [PubMed]
- Darke, S.; Duflou, J.; Torok, M. The comparative toxicology and major organ pathology of fatal methadone and heroin toxicity cases. Drug Alcohol. Depend. 2010, 106, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Sreepada Rao, T.K.; Nicastri, A.D.; Friedman, E.A. Renal consequences of narcotic abuse. Adv. Nephrol. Necker Hosp. 1977, 7, 261–290. [Google Scholar] [PubMed]
- Friedman, E.A.; Rao, T.K.; Nicastri, A.D. Heroin-associated nephropathy. Nephron 1974, 13, 421–426. [Google Scholar] [CrossRef] [PubMed]
- Rao, T.K.; Nicastri, A.D.; Friedman, E.A. Natural history of heroin-associated nephropathy. N. Engl. J. Med. 1974, 290, 19–23. [Google Scholar] [CrossRef] [PubMed]
- Friedman, E.A.; Rao, T.K. Why does uremia in heroin abusers occur predominantly among blacks? JAMA 1983, 250, 2965–2966. [Google Scholar] [CrossRef] [PubMed]
- Friedman, E.A.; Tao, T.K. Disappearance of uremia due to heroin-associated nephropathy. Am. J. Kidney Dis. 1995, 25, 689–693. [Google Scholar] [CrossRef]
- Hamilton, R.J.; Perrone, J.; Hoffman, R.; Henretig, F.M.; Karkevandian, E.H.; Marcus, S.; Shih, R.D.; Blok, B.; Nordenholz, K. A descriptive study of an epidemic of poisoning caused by heroin adulterated with scopolamine. J. Toxicol. Clin. Toxicol. 2000, 38, 597–608. [Google Scholar] [CrossRef] [PubMed]
- Dettmeyer, R.B.; Preuss, J.; Wollersen, H.; Burkhard, M. Heroin-associated nephropathy. Expert Opin. Drug Saf. 2005, 4, 19–28. [Google Scholar] [CrossRef] [PubMed]
- Rao, T.K.; Filippone, E.J.; Nicastri, A.D.; Landesman, S.H.; Frank, E.; Chen, C.K.; Friedman, E.A. Associated focal and segmental glomerulosclerosis in the acquired immunodeficiency syndrome. N. Engl. J. Med. 1984, 310, 669–673. [Google Scholar] [CrossRef] [PubMed]
- Kopp, J.B.; Nelson, G.W.; Sampath, K.; Johnson, R.C.; Genovese, G.; An, P.; Friedman, D.; Briggs, W.; Dart, R.; Korbet, S.; et al. APOL1 genetic variants in focal segmental glomerulosclerosis and HIV-associated nephropathy. J. Am. Soc. Nephrol. 2011, 22, 2129–2137. [Google Scholar] [CrossRef] [PubMed]
- Lan, X.; Rao, T.K.; Chander, P.N.; Skorecki, K.; Singhal, P.C. Apolipoprotein L1 (APOL1) Variants (Vs) a possible link between Heroin-associated Nephropathy (HAN) and HIV-associated Nephropathy (HIVAN). Front. Microbiol. 2015, 6, 571. [Google Scholar] [CrossRef] [PubMed]
- Neugarten, J.; Gallo, G.R.; Buxbaum, J.; Katz, L.A.; Rubenstein, J.; Baldwin, D.S. Amyloidosis in subcutaneous heroin abusers “skin poppers’ amyloidosis”. Am. J. Med. 1986, 81, 635–640. [Google Scholar] [CrossRef]
- Moran, C.P.; Courtney, A.E. Managing acute and chronic renal stone disease. Practitioner 2016, 260, 17–20. [Google Scholar] [PubMed]
- Welk, B.K.; Teichman, J.M. Pharmacological management of renal colic in the older patient. Drugs Aging 2007, 24, 891–900. [Google Scholar] [CrossRef] [PubMed]
- Barratt, D.T.; Bandak, B.; Klepstad, P.; Dale, O.; Kaasa, S.; Christrup, L.L.; Tuke, J.; Somogyi, A.A. Genetic, pathological and physiological determinants of transdermal fentanyl pharmacokinetics in 620 cancer patients of the EPOS study. Pharmacogenet. Genom. 2014, 24, 185–194. [Google Scholar] [CrossRef] [PubMed]
- Davies, G.; Kingswood, C.; Street, M. Pharmacokinetics of opioids in renal dysfunction. Clin. Pharmacokinet. 1996, 31, 410–422. [Google Scholar] [CrossRef] [PubMed]
- Won, A.B.; Lapane, K.L.; Vallow, S.; Schein, J.; Morris, J.N.; Lipsitz, L.A. Persistent nonmalignant pain and analgesic prescribing patterns in elderly nursing home residents. J. Am. Geriatr. Soc. 2004, 52, 867–874. [Google Scholar] [CrossRef] [PubMed]
- Linnebur, S.A.; O’Connell, M.B.; Wessell, A.M.; McCord, A.D.; Kennedy, D.H.; DeMaagd, G.; Dent, L.A.; Splinter, M.Y.; Biery, J.C.; Chang, F.; et al. Pharmacy practice, research, education, and advocacy for older adults. Pharmacotherapy 2005, 25, 1396–1430. [Google Scholar] [CrossRef] [PubMed]
- Tegeder, I.; Lotsch, J.; Geisslinger, G. Pharmacokinetics of opioids in liver disease. Clin. Pharmacokinet. 1999, 37, 17–40. [Google Scholar] [CrossRef] [PubMed]
- Lindeman, R.D.; Tobin, J.; Shock, N.W. Longitudinal studies on the rate of decline in renal function with age. J. Am. Geriatr. Soc. 1985, 33, 278–285. [Google Scholar] [CrossRef] [PubMed]
- American Geriatrics Society Panel on Pharmacological Management of Persistent Pain in Older Persons. Pharmacological management of persistent pain in older persons. J. Am. Geriatr. Soc. 2009, 57, 1331–1346. [Google Scholar]
- Grond, S.; Sablotzki, A. Clinical pharmacology of tramadol. Clin. Pharmacokinet. 2004, 43, 879–923. [Google Scholar] [CrossRef] [PubMed]
- Skinner-Robertson, S.; Fradette, C.; Bouchard, S.; Mouksassi, M.S.; Varin, F. Pharmacokinetics of tramadol and O-desmethyltramadol enantiomers following administration of extended-release tablets to elderly and young subjects. Drugs Aging 2015, 32, 1029–1043. [Google Scholar] [CrossRef] [PubMed]
- Yue, Q.Y.; Alm, C.; Svensson, J.O.; Säwe, J. Quantification of the O- and N-demethylated and the glucuronidated metabolites of codeine relative to the debrisoquine metabolic ratio in urine in ultrarapid, rapid, and poor debrisoquine hydroxylators. Ther. Drug Monit. 1997, 19, 539–542. [Google Scholar] [CrossRef] [PubMed]
- Davison, S.N. Pain in hemodialysis patients: Prevalence, cause, severity, and management. Am. J. Kidney Dis. 2003, 42, 1239–1247. [Google Scholar] [CrossRef] [PubMed]
- Wyne, A.; Rai, R.; Cuerden, M.; Clark, W.F.; Suri, R.S. Opioid and benzodiazepine use in end-stage renal disease: A systematic review. Clin. J. Am. Soc. Nephrol. 2011, 6, 326–333. [Google Scholar] [CrossRef] [PubMed]
- King, S.; Forbes, K.; Hanks, G.W.; Ferro, C.J.; Chambers, E.J. A systematic review of the use of opioid medication for those with moderate to severe cancer pain and renal impairment: A European Palliative Care Research Collaborative opioid guidelines project. Palliat. Med. 2011, 25, 525–552. [Google Scholar] [CrossRef] [PubMed]
- Kurella, M.; Bennett, W.M.; Chertow, G.M. Analgesia in patients with ESRD: A review of available evidence. Am. J. Kidney Dis. 2003, 42, 217–228. [Google Scholar] [CrossRef]
- Murtagh, F.E.; Chai, M.O.; Donohoe, P.; Edmonds, P.M.; Higginson, I.J. The use of opioid analgesia in end-stage renal disease patients managed without dialysis: Recommendations for practice. J. Pain Palliat. Care Pharmacother. 2007, 21, 5–16. [Google Scholar] [CrossRef] [PubMed]
| Type of Opioid | Dose in Milligrams |
|---|---|
| I. Exogenous | - |
| A. Natural | - |
| Morphine | 10 |
| Morphine esters | - |
| Morphine diacetate also called heroin | 2.5 |
| B. Semi-synthetic | - |
| Hydromorphone | 7.5 |
| Hydrocodone | 10 |
| Oxycodone | 6.5 |
| Oxymorphone | 10 |
| Buprenorphine (partial agonist) | 0.4 |
| C. Synthetic | - |
| Fentanyl (Intramuscular/Intravenous) | 0.1 |
| Meperidine (pethidine) | 300 |
| Levorphanol | 1.25 |
| Methodone | 2.5 |
| Dextropropoxyphene | 130 |
| Tramadol (also blocks reuptake of monoamines) | 200 |
| II. Endogenous | - |
| About 20 identified: includes endorphins, enkephalins, dynorphins, endomorphins | - |
| Pure Agonists |
| Have no ceiling effect for analgesia. |
| Example: morphine and fentanyl |
| Agonist-Antagonists |
| Partial agonists are those drugs that have with lower efficacy to bind to the mu receptor. |
| Mixed agonist-antagonists are those drugs that have agonist effects at one opioid receptor and antagonist effects at another. |
| These are made to be less addictive. |
| Drugs in this category have a ceiling effect for analgesia. |
| Example: buprenorphine |
| Pure Antagonists |
| Compete for the mu receptor and block it; they are used to reverse opioid effects especially in the setting of respiratory depression. This effect may not last long and repeat treatments may be needed to keep opioids from competing andbinding to the vacant receptor. |
| Example: naloxone |
| Anti-Diuretic Hormone (ADH) | Opioids Decrease ADH Effect |
|---|---|
| Diuretics | When added to diuretics, opioids lead to increased diuretic effect/toxicity. |
| Anti-cholinergics | In general opioids present a 2%–20% risk of urinary retention, with increased risk if benign prostatic hypertrophy is present. Risk is further increased if anti-cholinergics are used. |
| β-blockers | If combined with β-blockers, bradycardia can be enhanced. |
| Blood Pressure | Enhance parasympathetic effect and oppose noradrenergic effect: Opioids can lead to a clinical decrease in blood pressure. |
| Non-dihydropyridine Calcium channel blockers | If combined with non-dihydropyridine calcium channel blockers, bradycardia can be enhanced. |
| Constipation | Due to decreased acetylcholine release in the gut from opioids. |
| Central nervous system (CNS) depressants (alcohol/benzodiazepenes etc.) | Opioids interact with other CNS depressants for additive effect. |
| Desmopressin | Opioids can enhance the effect of desmopressin. |
| Magnesium sulphate | With magnesium sulphate CNS depression can be increased. |
| Sodium polystyrene sulfonate | Use with caution in the setting of hyperkalemia with renal failure; (with constipation caution is needed regarding use of potassium resin exchangers in the gut). |
| Drug | Use in End Stage Renal Disease (ESRD) and Chronic Kidney Disease |
|---|---|
| Morphine | ESRD: Use with caution and start with small doses as metabolites accumulate and may have delayed respiratory depression; pruritus may be difficult to control. Up to 47% can be removed with HD despite being protein bound (MW 668 dalton; 35% protein bound, Vd = 1–6 L/kg). |
| CKD: Starting oral dose is 25%–50%; start low dose and titrate slowly with longer dosing intervals as metabolites may accumulate with a delayed effect of respiratory depression. | |
| Drug interactions: nimodipine augments morphine’s analgesic effect via unknown mechanisms. May need small doses of morphine when using nimodipine. | |
| Diamorphine (Heroin/morpine diacetate) | Not medically used in USA as quickly addictive. |
| ESRD: Use with caution due to accumulation of metabolites (MW 369; not protein bound; easily crosses into brain; pro-drug converted to morphine and metabolites). | |
| CKD: Use with caution due to accumulation of metabolites. | |
| Codeine | ESRD: Significant accumulation of metabolites ; start at 50% of dose with increased interval of dosing and carefully titrate (MW 299; Vd = 2.6 L/kg; 90% excreted by kidneys). |
| CKD: GFR < 50 mL/min: start at 75% dose with increased interval and carefully titrate due to accumulation of metabolites. | |
| Tramadol | ESRD: As it is dialyzed out administer on day of HD; increased interval of dosing to 12 h may be needed (MW 263; Vd 2.6–2.9 L/kg; 20% protein bound). |
| CKD: For GFR < 30 mL/min, increase dosing interval to 12 h; avoid the use of extended release; for GFR > 30 m/min, use with caution. | |
| Can have symptoms of urinary frequency and urinary tract infection; metabolized in liver, metabolites excreted via kidney. | |
| Oxymorphone | ESRD: No clear data of use (MW 301; Vd 3 L/kg). |
| CKD: eGFR > 50 mL/min reduce starting dose 50% and increase dosing frequency for titration; bioavailability increases with CKD. | |
| Thromobtic thrombocytopenic purpura and acute kidney injury (AKI) noted when the tablets are crushed and intravenously administered as in injection with drug abusers. | |
| Hydromorphone | ESRD: Limited information with fluctuating levels may be difficult to use due to removal of drug; clearance with HD 105 mL/min with change in drug level of 55% with one treatment of HD; parent drug is removed but metabolites may persist and accumulate; (MW 285; Vd 1.2 L/kg; 8%–19% protein bound). |
| Oxycodone | ESRD: Use with caution; limited information case reports (MW 315; Vd 2.6 L/kg; 45% protein bound). |
| CKD: Serum concentration increases 50% if GFR < 60 mL/min. | |
| Limited information suggests starting at one-third the usual starting dose and increasing interval between dosing as half life increases. | |
| Drug interaction: Conivaptan: could increase concentration of CYP3A4 substrate. | |
| Buprenorphine | ESRD: May be used with caution, limited information (MW 467; Vd 188–335 L/kg; 96% protein bound). Transdermal route may be satisfactory. |
| CKD: May be used with CKD. | |
| Methodone | ESRD: Dose at 75% normal dose; lipophilic and minimal clearance with HD with less than 15% change in levels); methodone clearance with HD is about 17–19 mL/min (MW 345; 85%–90% protein bound; Vd 1–8 L/kg). |
| CKD: eGFR > 10 mL/min no change in dose needed. | |
| If QTc prolonged on EKG, an alternate drug may be needed. | |
| Drug interaction: Conivaptan: could increase concentration ofCYP3A4 substrate. | |
| Fentanyl | ESRD: Transdermal patch suggested to not be used with ESRD (MW 336; lipophilic; Vd 4 L/kg). |
| CKD: Reduce dose by 50%; limited information on other forms besides transdermal route; lipophilic and protein bound; free fraction increases with acidosis. | |
| Conivaptan: Could increase concentration of the CYP3A4 substrate. |
© 2017 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mallappallil, M.; Sabu, J.; Friedman, E.A.; Salifu, M. What Do We Know about Opioids and the Kidney? Int. J. Mol. Sci. 2017, 18, 223. https://doi.org/10.3390/ijms18010223
Mallappallil M, Sabu J, Friedman EA, Salifu M. What Do We Know about Opioids and the Kidney? International Journal of Molecular Sciences. 2017; 18(1):223. https://doi.org/10.3390/ijms18010223
Chicago/Turabian StyleMallappallil, Mary, Jacob Sabu, Eli A. Friedman, and Moro Salifu. 2017. "What Do We Know about Opioids and the Kidney?" International Journal of Molecular Sciences 18, no. 1: 223. https://doi.org/10.3390/ijms18010223
APA StyleMallappallil, M., Sabu, J., Friedman, E. A., & Salifu, M. (2017). What Do We Know about Opioids and the Kidney? International Journal of Molecular Sciences, 18(1), 223. https://doi.org/10.3390/ijms18010223





