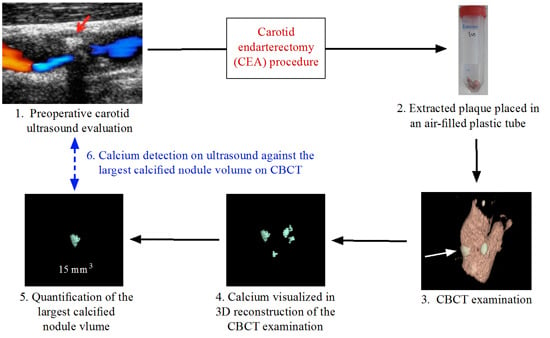
Atherosclerotic Calcification Detection: A Comparative Study of Carotid Ultrasound and Cone Beam CT
Abstract
:1. Introduction
2. Results
2.1. Clinical Characteristics
| Baseline | Study Population (n = 88) |
|---|---|
| Age (years), mean (SD) Females, n (%) | 70 (7), 29 (33) |
| Systolic blood pressure (mmHg), mean (SD) | 147 (22.6) |
| Diastolic blood pressure (mmHg), mean (SD) | 78 (12) |
| Total cholesterol (mmol/L), mean (SD) | 4.61 (1.03) |
| LDL (mmol/L), mean (SD) | 2.60 (0.92) |
| HDL (mmol/L), mean (SD) | 1.27 (0.48) |
| Creatinine (μmol/L), mean (SD) | 84 (25) |
| HBA1c (mmol/mol), mean (SD) | 52.5 (12.7) |
| Symptomatic carotid stenosis, n (%) | 73 (83) |
| Prior myocardial infarction, n (%) | 14 (16) |
| Current angina pectoris, n (%) | 7 (8) |
| Heart failure, n (%) | 1 (1.1) |
| Previous stroke (>6 months to the present evaluation), n (%) | 14 (16) |
| Claudication (lower extremity artery disease), n (%) | 10 (11.4) |
| Any previous revascularization for ischemia, n (%) | 24 (27.3) |
| Current smoker, n (%) | 9 (10.2) |
| Diabetes, n (%) | 29 (33) |
| Lipid lowering medicine, n (%) | 82 (93.2) |
| Platelet inhibiting or anticoagulation medicine, n (%) | 88 (100) |
| Blood pressure reducing medicine, n (%) | 84 (95.5) |
2.2. Carotid Calcification: Ultrasound vs. Cone Beam CT (CBCT)
| Subgroups | Arteries n | <8 mm3 Calcification Volumes on CBCT, n (%) | p |
|---|---|---|---|
| Age | |||
| <75 | 68 | 18 (26.5) | |
| ≥75 | 26 | 4 (15.3) | 0.21 |
| Gender | |||
| Female | 30 | 7 (23.3) | |
| Male | 64 | 15 (23.4) | 0.99 |
| Symptomatic | 79 | 20 (25.3) | |
| Asymptomatic | 15 | 2 (13.3) | 0.31 |
| Current smoker | |||
| Yes | 10 | 4 (40.0) | |
| No | 84 | 18 (21.4) | 0.19 |
| Diabetes | |||
| Yes | 31 | 8 (25.8) | |
| No | 63 | 14 (22.2) | 0.60 |
| Previous stroke | |||
| Yes | 17 | 2 (11.8) | |
| No | 77 | 20 (26.0) | 0.21 |
| Previous MI | |||
| Yes | 15 | 3 (20.0) | |
| No | 79 | 19 (24.0) | 0.73 |
| Statin therapy | |||
| Yes | 87 | 21 (24.1) | |
| No | 7 | 1 (14.3) | 0.55 |
| Degree of stenosis | |||
| 50%–69% | 6 | 0 (0) | |
| 70%–99% | 85 | 20 (23.5) | |
| Near-occlusion | 3 | 2 (66.7) | 0.08 |
| CBCT\Ultrasound | Total Arteries, n | Calcification on CBCT | Calcification on US | US Sensitivity | US Specificity |
|---|---|---|---|---|---|
| Calcification | 94 | 93 | 82 | 88.20% | 100% |
| Calcification ≥8 mm3 | 72 | 72 | 69 | 96% | N/A |
| Calcification <8 mm3 | 22 | 21 | 13 | 62% | 100% |
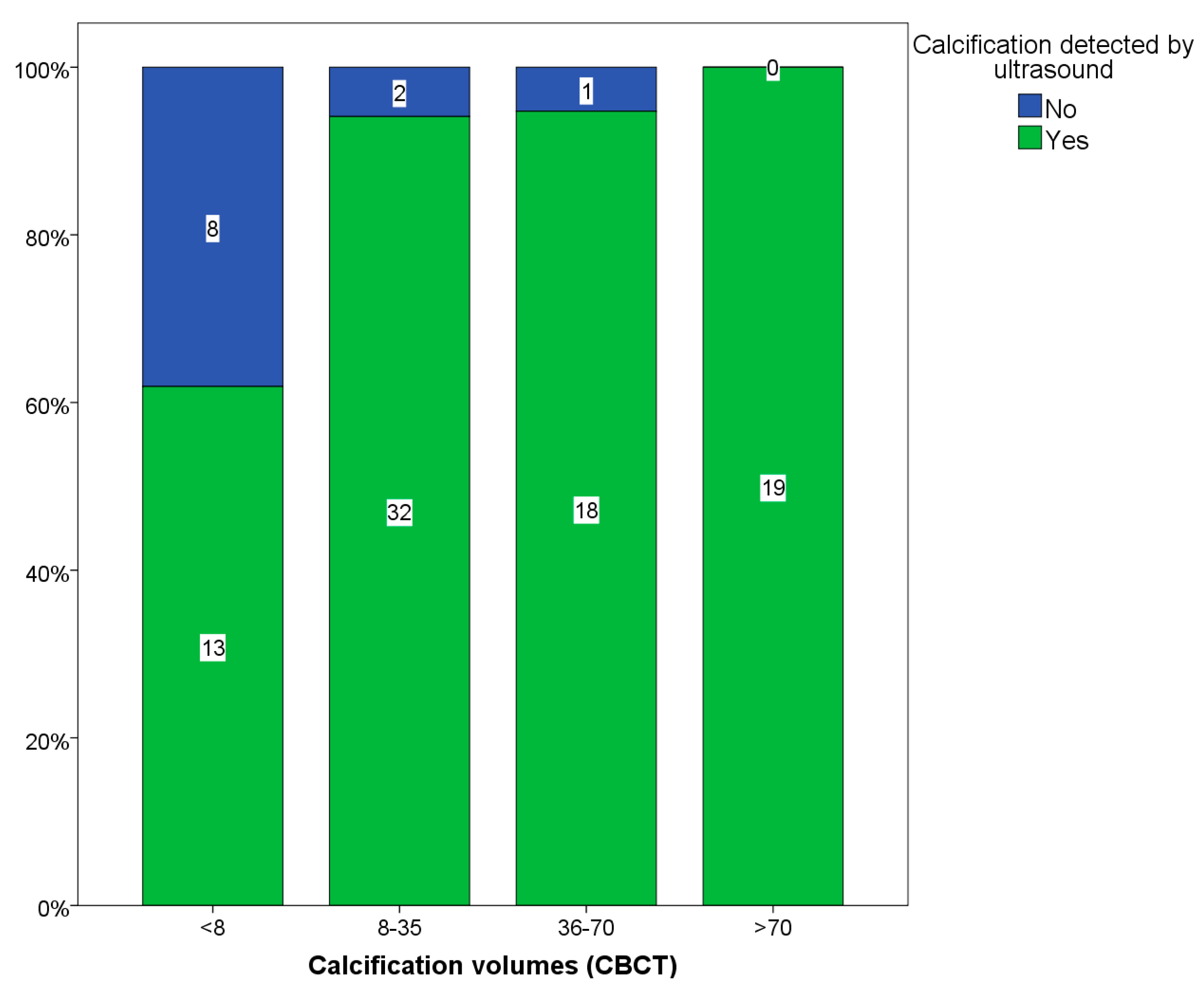
2.3. Carotid Calcification vs. Symptoms
2.4. Reproducibility Analyses
3. Discussion
3.1. Findings
3.2. Data Interpretation
3.3. Clinical Implications
3.4. Study Limitations
4. Experimental Section
4.1. Subjects
4.2. Ultrasound Examination
4.3. Carotid Ultrasound Analysis
4.4. Carotid Endarterectomy (CEA)
4.5. CBCT
4.6. Statistics
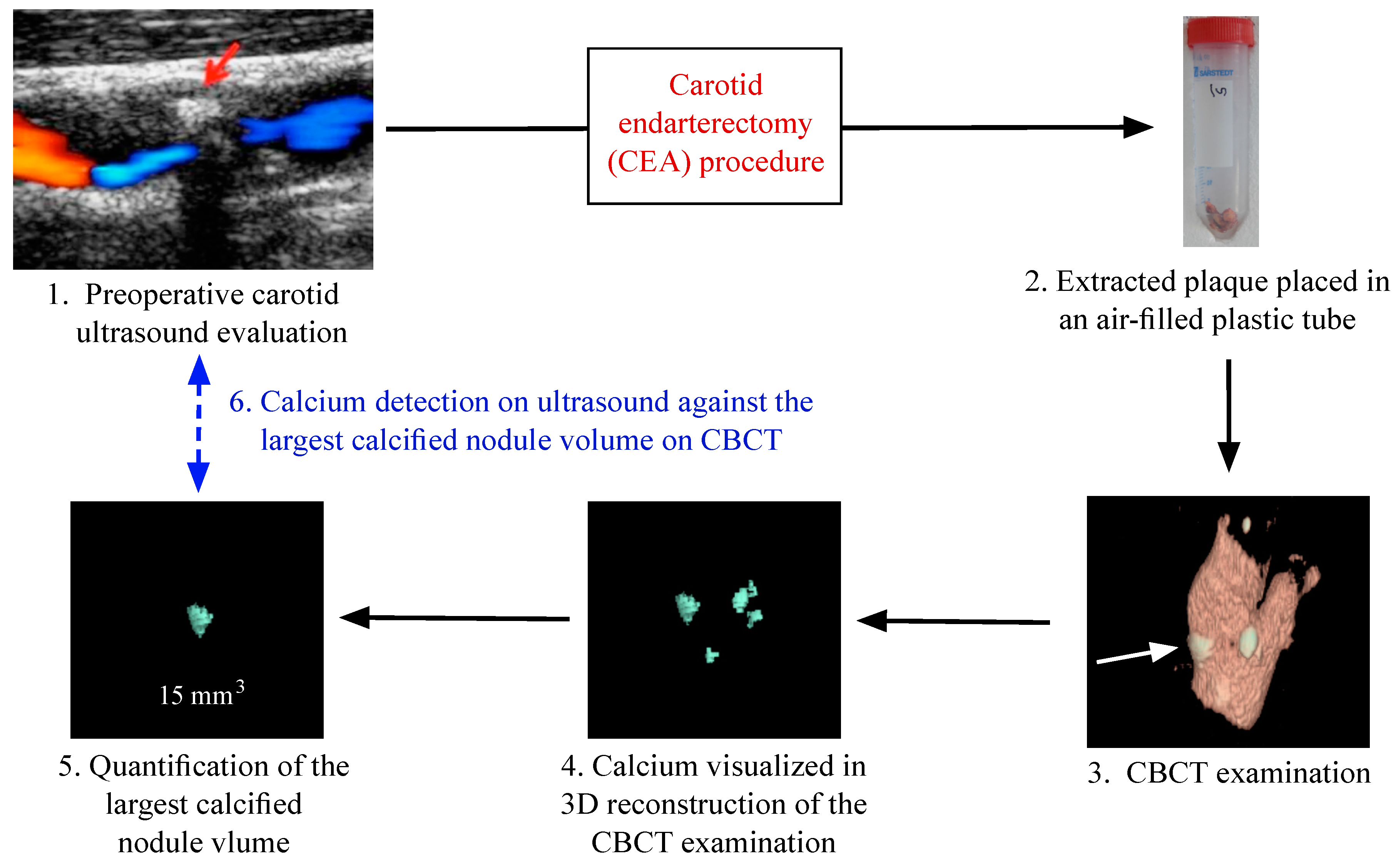
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Grau, A.J.; Weimar, C.; Buggle, F.; Heinrich, A.; Goertler, M.; Neumaier, S.; Glahn, J.; Brandt, T.; Hacke, W.; Diener, H.-C.; et al. Risk factors, outcome, and treatment in subtypes of ischemic stroke: The German Stroke Data Bank. Stroke J. Cereb. Circ. 2001, 32, 2559–2566. [Google Scholar] [CrossRef]
- Chaturvedi, S.; Bruno, A.; Feasby, T.; Holloway, R.; Benavente, O.; Cohen, S.N.; Cote, R.; Hess, D.; Saver, J.; Spence, J.D.; et al. Carotid endarterectomy—An evidence-based review: Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 2005, 65, 794–801. [Google Scholar] [CrossRef] [PubMed]
- Hashimoto, H.; Tagaya, M.; Niki, H.; Etani, H. Computer-assisted analysis of heterogeneity on B-mode imaging predicts instability of asymptomatic carotid plaque. Cerebrovasc. Dis. 2009, 28, 357–364. [Google Scholar] [CrossRef] [PubMed]
- Slevin, M.; Wang, Q.; Font, M.A.; Luque, A.; Juan-Babot, O.; Gaffney, J.; Kumar, P.; Kumar, S.; Badimon, L.; Krupinski, J. Atherothrombosis and plaque heterology: Different location or a unique disease? Pathobiol. J. Immunopathol. Mol. Cell. Boil. 2008, 75, 209–225. [Google Scholar] [CrossRef] [PubMed]
- Garoff, M.; Johansson, E.; Ahlqvist, J.; Jaghagen, E.L.; Arnerlöv, C.; Wester, P. Detection of calcifications in panoramic radiographs in patients with carotid stenoses ≥50%. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2014, 117, 385–391. [Google Scholar] [CrossRef] [PubMed]
- Huang, H.; Virmani, R.; Younis, H.; Burke, A.P.; Kamm, R.D.; Lee, R.T. The impact of calcification on the biomechanical stability of atherosclerotic plaques. Circulation 2001, 103, 1051–1056. [Google Scholar] [CrossRef] [PubMed]
- Nandalur, K.R.; Baskurt, E.; Hagspiel, K.D.; Finch, M.; Phillips, C.D.; Bollampally, S.R.; Kramer, C.M. Carotid artery calcification on CT may independently predict stroke risk. AJR Am. J. Roentgenol. 2006, 186, 547–552. [Google Scholar] [CrossRef] [PubMed]
- Kwee, R.M. Systematic review on the association between calcification in carotid plaques and clinical ischemic symptoms. J. Vasc. Surg. 2010, 51, 1015–1025. [Google Scholar] [CrossRef] [PubMed]
- Garoff, M.; Johansson, E.; Ahlqvist, J.; Arnerlöv, C.; Levring Jäghagen, E.; Wester, P. Calcium quantity in carotid plaques: Detection in panoramic radiographs and association with degree of stenosis. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2015, 120, 269–274. [Google Scholar] [CrossRef] [PubMed]
- Ibrahimi, P.; Jashari, F.; Nicoll, R.; Bajraktari, G.; Wester, P.; Henein, M.Y. Coronary and carotid atherosclerosis: How useful is the imaging? Atherosclerosis 2013, 231, 323–333. [Google Scholar] [CrossRef] [PubMed]
- Ababneh, B.; Rejjal, L.; Pokharel, Y.; Nambi, V.; Wang, X.; Tung, C.H.; Han, R.I.; Talyor, A.A.; Kougias, P.; Lumsden, A.B.; et al. Distribution of calcification in carotid endarterectomy tissues: Comparison of micro-computed tomography imaging with histology. Vasc. Med. 2014, 19, 343–350. [Google Scholar] [CrossRef] [PubMed]
- Miralles, M.; Merino, J.; Busto, M.; Perich, X.; Barranco, C.; Vidal-Barraquer, F. Quantification and characterization of carotid calcium with multi-detector CT-angiography. Eur. J. Vasc. Endovasc. Surg. 2006, 32, 561–567. [Google Scholar] [CrossRef] [PubMed]
- Lal, B.K.; Hobson, R.W., 2nd.; Pappas, P.J.; Kubicka, R.; Hameed, M.; Chakhtoura, E.Y.; Jamil, Z.; Padber, F.T., Jr.; Haser, P.B.; Durán, W.N. Pixel distribution analysis of B-mode ultrasound scan images predicts histologic features of atherosclerotic carotid plaques. J. Vasc. Surg. 2002, 35, 1210–1217. [Google Scholar] [CrossRef] [PubMed]
- Denzel, C.; Lell, M.; Maak, M.; Höckl, M.; Balzer, K.; Müller, K.M.; Fellner, C.; Fellner, F.A.; Lang, W. Carotid artery calcium: Accuracy of a calcium score by computed tomography—An in vitro study with comparison to sonography and histology. Eur. J. Vasc. Endovasc. Surg. 2004, 28, 214–220. [Google Scholar] [CrossRef] [PubMed]
- Setacci, C.; Chisci, E.; Setacci, F.; Iacoponi, F.; de Donato, G.; Rossi, A. Siena carotid artery stenting score: A risk modelling study for individual patients. Stroke 2010, 41, 1259–1265. [Google Scholar] [CrossRef] [PubMed]
- Elias-Smale, S.E.; Odink, A.E.; Wieberdink, R.G.; Hofman, A.; Hunink, M.G.; Krestin, G.P.; Koudstaal, P.J.; Breteler, M.B.; van der Lugt, A.; Witteman, J.C.M. Carotid, aortic arch and coronary calcification are related to history of stroke: The Rotterdam study. Atherosclerosis 2010, 212, 656–660. [Google Scholar] [CrossRef] [PubMed]
- Bajraktari, G.; Nicoll, R.; Ibrahimi, P.; Jashari, F.; Schmermund, A.; Henein, M.Y. Coronary calcium score correlates with estimate of total plaque burden. Int. J. Cardiol. 2013, 167, 1050–1052. [Google Scholar] [CrossRef] [PubMed]
- Nicoll, R.; Henein, M.Y. Arterial calcification: Friend or foe? Int. J. Cardiol. 2013, 167, 322–327. [Google Scholar] [CrossRef] [PubMed]
- Ibrahimi, P.; Jashari, F.; Bajraktari, G.; Wester, P.; Henein, M.Y. Ultrasound assessment of carotid plaque echogenicity response to statin therapy: A systematic review and meta-analysis. Int. J. Mol. Sci. 2015, 16, 10734–10747. [Google Scholar] [CrossRef] [PubMed]
- Henein, M.; Granåsen, G.; Wiklund, U.; Schmermund, A.; Guerci, A.; Erbel, R.; Raggi, P. High dose and long-term statin therapy accelerate coronary artery calcification. Int. J. Cardiol. 2015, 184, 581–586. [Google Scholar] [CrossRef] [PubMed]
- Hansen, F.; Bergqvist, D.; Lindblad, B.; Lindh, M.; Matzsch, T.; Lanne, T. Accuracy of duplex sonography before carotid endarterectomy—A comparison with angiography. Eur. J. Vasc. Endovasc. Surg. 1996, 12, 331–336. [Google Scholar] [CrossRef]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jashari, F.; Ibrahimi, P.; Johansson, E.; Ahlqvist, J.; Arnerlöv, C.; Garoff, M.; Jäghagen, E.L.; Wester, P.; Henein, M.Y. Atherosclerotic Calcification Detection: A Comparative Study of Carotid Ultrasound and Cone Beam CT. Int. J. Mol. Sci. 2015, 16, 19978-19988. https://doi.org/10.3390/ijms160819978
Jashari F, Ibrahimi P, Johansson E, Ahlqvist J, Arnerlöv C, Garoff M, Jäghagen EL, Wester P, Henein MY. Atherosclerotic Calcification Detection: A Comparative Study of Carotid Ultrasound and Cone Beam CT. International Journal of Molecular Sciences. 2015; 16(8):19978-19988. https://doi.org/10.3390/ijms160819978
Chicago/Turabian StyleJashari, Fisnik, Pranvera Ibrahimi, Elias Johansson, Jan Ahlqvist, Conny Arnerlöv, Maria Garoff, Eva Levring Jäghagen, Per Wester, and Michael Y. Henein. 2015. "Atherosclerotic Calcification Detection: A Comparative Study of Carotid Ultrasound and Cone Beam CT" International Journal of Molecular Sciences 16, no. 8: 19978-19988. https://doi.org/10.3390/ijms160819978
APA StyleJashari, F., Ibrahimi, P., Johansson, E., Ahlqvist, J., Arnerlöv, C., Garoff, M., Jäghagen, E. L., Wester, P., & Henein, M. Y. (2015). Atherosclerotic Calcification Detection: A Comparative Study of Carotid Ultrasound and Cone Beam CT. International Journal of Molecular Sciences, 16(8), 19978-19988. https://doi.org/10.3390/ijms160819978