New Insights into Dietary Pterostilbene: Sources, Metabolism, and Health Promotion Effects
Abstract
1. Introduction
2. Potential Dietary Sources of PTS
Biosynthesis and Nutraceutical Availability
3. Analytical Aspects
4. Pharmacokinetics
4.1. Absorption
4.2. Distribution
4.3. Metabolism
4.4. Excretion
4.5. Toxicity
5. Major Pathways Associated with PTS
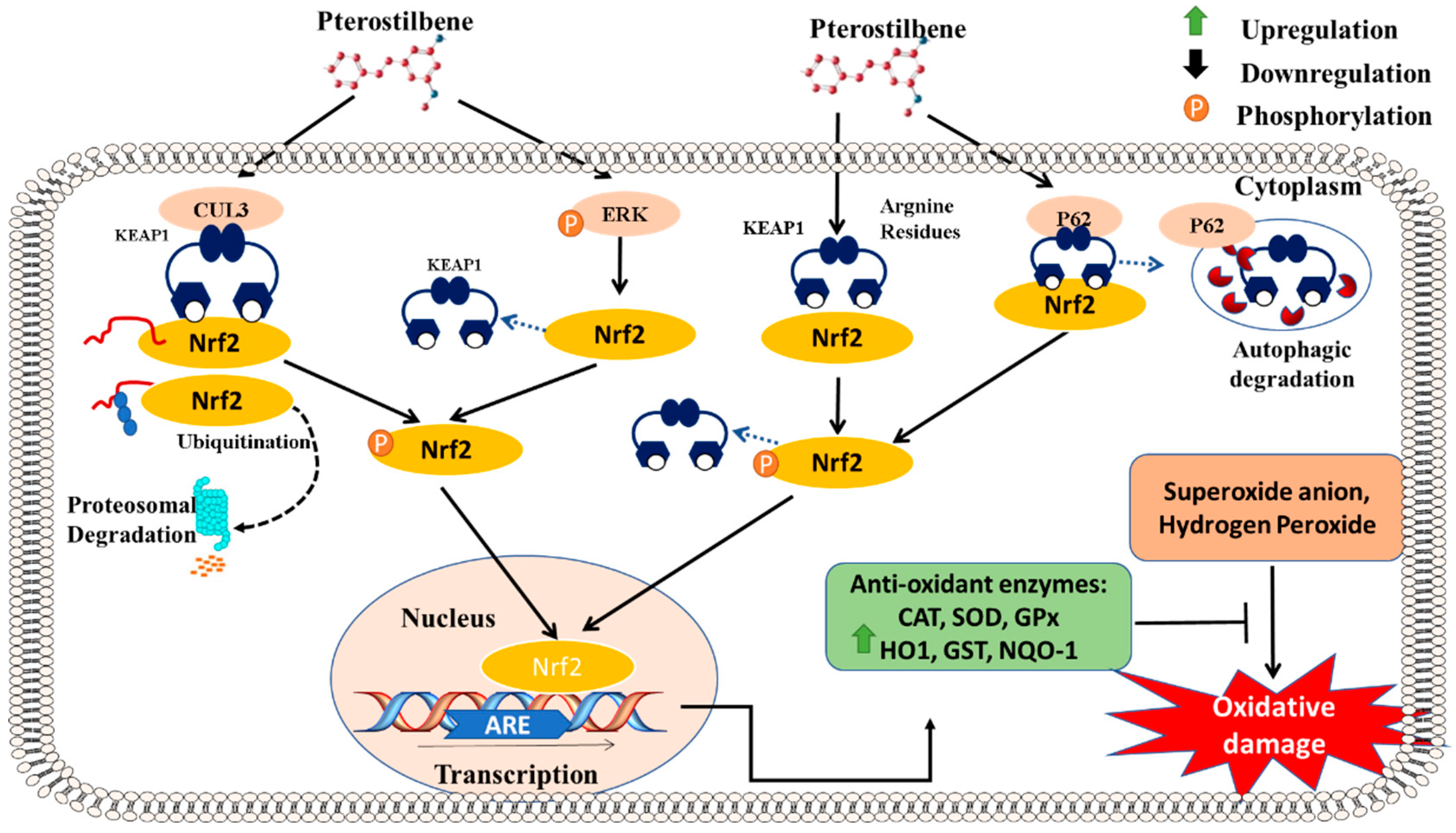
5.1. Antioxidative Pathway: Activation of Nrf2 Signaling
5.2. Pro- and Anti-Apoptotic Pathways
5.3. Anti-Inflammatory Pathway
6. Therapeutic Properties of PTS
6.1. Anti-Cancer Activity of PTS
6.2. Anti-Diabetic Activity of PTS
6.3. Therapeutic Effect of PTS in Liver Diseases
6.4. Effects of PTS on Diseases of the Central Nervous System
6.5. Effects of PTS on Cardiovascular Diseases
6.6. Effects of PTS on Aging
6.7. Antibacterial Effect of PTS
6.8. Therapeutic Effects of PTS against COVID-19 Infection
7. Enhancement of PTS Bioavailability
8. Conclusions and Future Prospects
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data availability Statement
Acknowledgments
Conflicts of Interest
References
- Wang, P.; Sang, S. Metabolism and Pharmacokinetics of Resveratrol and Pterostilbene. Biofactors 2018, 44, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Estrela, J.M.; Ortega, A.; Mena, S.; Rodriguez, M.L.; Asensi, M. Pterostilbene: Biomedical Applications. Crit. Rev. Clin. Lab. Sci. 2013, 50, 65–78. [Google Scholar] [CrossRef] [PubMed]
- Kosuru, R.; Rai, U.; Prakash, S.; Singh, A.; Singh, S. Promising Therapeutic Potential of Pterostilbene and Its Mechanistic Insight Based on Preclinical Evidence. Eur. J. Pharmacol. 2016, 789, 229–243. [Google Scholar] [CrossRef] [PubMed]
- Kapetanovic, I.M.; Muzzio, M.; Huang, Z.; Thompson, T.N.; McCormick, D.L. Pharmacokinetics, Oral Bioavailability, and Metabolic Profile of Resveratrol and Its Dimethylether Analog, Pterostilbene, in Rats. Cancer Chemother. Pharmacol. 2011, 68, 593–601. [Google Scholar] [CrossRef]
- Langcake, P.; Cornford, C.A.; Pryce, R.J. Identification of Pterostilbene as a Phytoalexin from Vitis Vinifera Leaves. Phytochemistry 1979, 18, 1025–1027. [Google Scholar] [CrossRef]
- Rodríguez-Bonilla, P.; López-Nicolás, J.M.; Méndez-Cazorla, L.; García-Carmona, F. Development of a Reversed Phase High Performance Liquid Chromatography Method Based on the Use of Cyclodextrins as Mobile Phase Additives to Determine Pterostilbene in Blueberries. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2011, 879, 1091–1097. [Google Scholar] [CrossRef]
- McCormack, D.; McFadden, D. A Review of Pterostilbene Antioxidant Activity and Disease Modification. Oxid. Med. Cell Longev. 2013, 2013, 575482. [Google Scholar] [CrossRef]
- Remsberg, C.M.; Yáñez, J.A.; Ohgami, Y.; Vega-Villa, K.R.; Rimando, A.M.; Davies, N.M. Pharmacometrics of Pterostilbene: Preclinical Pharmacokinetics and Metabolism, Anticancer, Antiinflammatory, Antioxidant and Analgesic Activity. Phytother. Res. 2008, 22, 169–179. [Google Scholar] [CrossRef]
- Chan, E.W.C.; Wong, C.W.; Tan, Y.H.; Foo, J.P.Y.; Wong, S.K.; Chan, H.T. Resveratrol and Pterostilbene: A Comparative Overview of Their Chemistry, Biosynthesis, Plant Sources and Pharmacological Properties. J. App. Pharm. Sci. 2019, 9, 124–129. [Google Scholar] [CrossRef]
- Rimando, A.M.; Pan, Z.; Polashock, J.J.; Dayan, F.E.; Mizuno, C.S.; Snook, M.E.; Liu, C.-J.; Baerson, S.R. In Planta Production of the Highly Potent Resveratrol Analogue Pterostilbene via Stilbene Synthase and O-Methyltransferase Co-Expression. Plant Biotechnol. J. 2012, 10, 269–283. [Google Scholar] [CrossRef]
- Rimando, A.M.; Kalt, W.; Magee, J.B.; Dewey, J.; Ballington, J.R. Resveratrol, Pterostilbene, and Piceatannol in Vaccinium Berries. J. Agric. Food Chem. 2004, 52, 4713–4719. [Google Scholar] [CrossRef] [PubMed]
- Sobolev, V.S.; Khan, S.I.; Tabanca, N.; Wedge, D.E.; Manly, S.P.; Cutler, S.J.; Coy, M.R.; Becnel, J.J.; Neff, S.A.; Gloer, J.B. Biological Activity of Peanut (Arachis Hypogaea) Phytoalexins and Selected Natural and Synthetic Stilbenoids. J. Agric. Food Chem. 2011, 59, 1673–1682. [Google Scholar] [CrossRef] [PubMed]
- Aiyer, H.S.; Warri, A.M.; Woode, D.R.; Hilakivi-Clarke, L.; Clarke, R. Influence of Berry Polyphenols on Receptor Signaling and Cell-Death Pathways: Implications for Breast Cancer Prevention. J. Agric. Food Chem. 2012, 60, 5693–5708. [Google Scholar] [CrossRef] [PubMed]
- Adrian, M.; Jeandet, P.; Douillet-Breuil, A.C.; Tesson, L.; Bessis, R. Stilbene Content of Mature Vitis Vinifera Berries in Response to UV-C Elicitation. J. Agric. Food Chem. 2000, 48, 6103–6105. [Google Scholar] [CrossRef] [PubMed]
- Duke, S.O. Benefits of Resveratrol and Pterostilbene to Crops and Their Potential Nutraceutical Value to Mammals. Agriculture 2022, 12, 368. [Google Scholar] [CrossRef]
- Valletta, A.; Iozia, L.M.; Leonelli, F. Impact of Environmental Factors on Stilbene Biosynthesis. Plants 2021, 10, 90. [Google Scholar] [CrossRef]
- Sarig, P.; Zutkhi, Y.; Monjauze, A.; Lisker, N.; Ben-Arie, R. Phytoalexin Elicitation in Grape Berries and Their Susceptibility ToRhizopus Stolonifer. Physiol. Mol. Plant Pathol. 1997, 50, 337–347. [Google Scholar] [CrossRef]
- Douillet-Breuil, A.C.; Jeandet, P.; Adrian, M.; Bessis, R. Changes in the Phytoalexin Content of Various Vitis Spp. in Response to Ultraviolet C Elicitation. J. Agric. Food Chem. 1999, 47, 4456–4461. [Google Scholar] [CrossRef]
- Shrikanta, A.; Kumar, A.; Govindaswamy, V. Resveratrol Content and Antioxidant Properties of Underutilized Fruits. J. Food Sci. Technol. 2015, 52, 383–390. [Google Scholar] [CrossRef]
- Martínez-Márquez, A.; Morante-Carriel, J.A.; Ramírez-Estrada, K.; Cusidó, R.M.; Palazon, J.; Bru-Martínez, R. Production of Highly Bioactive Resveratrol Analogues Pterostilbene and Piceatannol in Metabolically Engineered Grapevine Cell Cultures. Plant Biotechnol. J. 2016, 14, 1813–1825. [Google Scholar] [CrossRef]
- Jeong, Y.J.; An, C.H.; Woo, S.G.; Jeong, H.J.; Kim, Y.-M.; Park, S.-J.; Yoon, B.D.; Kim, C.Y. Production of Pinostilbene Compounds by the Expression of Resveratrol O-Methyltransferase Genes in Escherichia coli. Enzym. Microb. Technol. 2014, 54, 8–14. [Google Scholar] [CrossRef] [PubMed]
- Tsai, H.-Y.; Ho, C.-T.; Chen, Y.-K. Biological Actions and Molecular Effects of Resveratrol, Pterostilbene, and 3’-Hydroxypterostilbene. J. Food Drug Anal. 2017, 25, 134–147. [Google Scholar] [CrossRef] [PubMed]
- Ruiz, M.J.; Fernández, M.; Picó, Y.; Mañes, J.; Asensi, M.; Carda, C.; Asensio, G.; Estrela, J.M. Dietary Administration of High Doses of Pterostilbene and Quercetin to Mice Is Not Toxic. J. Agric. Food Chem. 2009, 57, 3180–3186. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; You, Y.; Lu, J.; Chen, X.; Yang, Z. Recent Advances in Synthesis, Bioactivity, and Pharmacokinetics of Pterostilbene, an Important Analog of Resveratrol. Molecules 2020, 25, 5166. [Google Scholar] [CrossRef]
- Yeo, S.C.M.; Ho, P.C.; Lin, H.-S. Pharmacokinetics of Pterostilbene in Sprague-Dawley Rats: The Impacts of Aqueous Solubility, Fasting, Dose Escalation, and Dosing Route on Bioavailability. Mol. Nutr. Food Res. 2013, 57, 1015–1025. [Google Scholar] [CrossRef]
- Bethune, S.J.; Schultheiss, N.; Henck, J.-O. Improving the Poor Aqueous Solubility of Nutraceutical Compound Pterostilbene through Cocrystal Formation. Cryst. Growth Des. 2011, 11, 2817–2823. [Google Scholar] [CrossRef]
- Choo, Q.-Y.; Yeo, S.C.M.; Ho, P.C.; Tanaka, Y.; Lin, H.-S. Pterostilbene Surpassed Resveratrol for Anti-Inflammatory Application: Potency Consideration and Pharmacokinetics Perspective. J. Funct. Foods 2014, 11, 352–362. [Google Scholar] [CrossRef]
- Manach, C.; Scalbert, A.; Morand, C.; Rémésy, C.; Jiménez, L. Polyphenols: Food Sources and Bioavailability. Am. J. Clin. Nutr. 2004, 79, 727–747. [Google Scholar] [CrossRef]
- McCormack, D.; McFadden, D. Pterostilbene and Cancer: Current Review. J. Surg. Res. 2012, 173, e53–e61. [Google Scholar] [CrossRef]
- Obrador, E.; Salvador-Palmer, R.; Jihad-Jebbar, A.; López-Blanch, R.; Dellinger, T.H.; Dellinger, R.W.; Estrela, J.M. Pterostilbene in Cancer Therapy. Antioxidants 2021, 10, 492. [Google Scholar] [CrossRef]
- Riche, D.M.; McEwen, C.L.; Riche, K.D.; Sherman, J.J.; Wofford, M.R.; Deschamp, D.; Griswold, M. Analysis of Safety from a Human Clinical Trial with Pterostilbene. J. Toxicol. 2013, 2013, 463595. [Google Scholar] [CrossRef] [PubMed]
- Elango, B.; Devibalan, S.; Veerapazham, T.; Palanisamy, R.; Paulmurugan, R.; Mohanram, R. Therapeutic Potential of Pterostilbene against Pancreatic β-Cell Apoptosis through Nrf2 Mechanism. Br. J. Pharmacol. 2014, 171, 1747–1757. [Google Scholar] [CrossRef]
- Chen, R.-J.; Kuo, H.-C.; Cheng, L.-H.; Lee, Y.-H.; Chang, W.-T.; Wang, B.-J.; Wang, Y.-J.; Cheng, H.-C. Apoptotic and Nonapoptotic Activities of Pterostilbene against Cancer. Int. J. Mol. Sci. 2018, 19, 287. [Google Scholar] [CrossRef] [PubMed]
- Bhakkiyalakshmi, E.; Dineshkumar, K.; Karthik, S.; Sireesh, D.; Hopper, W.; Paulmurugan, R.; Ramkumar, K.M. Pterostilbene-Mediated Nrf2 Activation: Mechanistic Insights on Keap1:Nrf2 Interface. Bioorg. Med. Chem. 2016, 24, 3378–3386. [Google Scholar] [CrossRef] [PubMed]
- Xu, J.; Liu, J.; Li, Q.; Mi, Y.; Zhou, D.; Meng, Q.; Chen, G.; Li, N.; Hou, Y. Pterostilbene Alleviates Aβ1-42 -Induced Cognitive Dysfunction via Inhibition of Oxidative Stress by Activating Nrf2 Signaling Pathway. Mol. Nutr. Food Res. 2021, 65, e2000711. [Google Scholar] [CrossRef]
- Sireesh, D.; Ganesh, M.-R.; Dhamodharan, U.; Sakthivadivel, M.; Sivasubramanian, S.; Gunasekaran, P.; Ramkumar, K.M. Role of Pterostilbene in Attenuating Immune Mediated Devastation of Pancreatic Beta Cells via Nrf2 Signaling Cascade. J. Nutr. Biochem. 2017, 44, 11–21. [Google Scholar] [CrossRef] [PubMed]
- Bhakkiyalakshmi, E.; Sireesh, D.; Sakthivadivel, M.; Sivasubramanian, S.; Gunasekaran, P.; Ramkumar, K.M. Anti-Hyperlipidemic and Anti-Peroxidative Role of Pterostilbene via Nrf2 Signaling in Experimental Diabetes. Eur. J. Pharmacol. 2016, 777, 9–16. [Google Scholar] [CrossRef]
- Shen, H.; Rong, H. Pterostilbene Impact on Retinal Endothelial Cells under High Glucose Environment. Int. J. Clin. Exp. Pathol. 2015, 8, 12589–12594. [Google Scholar]
- Zhang, H.; Chen, Y.; Chen, Y.; Ji, S.; Jia, P.; Xu, J.; Li, Y.; Wang, T. Pterostilbene Attenuates Liver Injury and Oxidative Stress in Intrauterine Growth–Retarded Weanling Piglets. Nutrition 2021, 81, 110940. [Google Scholar] [CrossRef]
- Chiou, Y.-S.; Tsai, M.-L.; Nagabhushanam, K.; Wang, Y.-J.; Wu, C.-H.; Ho, C.-T.; Pan, M.-H. Pterostilbene Is More Potent than Resveratrol in Preventing Azoxymethane (AOM)-Induced Colon Tumorigenesis via Activation of the NF-E2-Related Factor 2 (Nrf2)-Mediated Antioxidant Signaling Pathway. J. Agric. Food Chem. 2011, 59, 2725–2733. [Google Scholar] [CrossRef]
- Sirerol, J.A.; Feddi, F.; Mena, S.; Rodriguez, M.L.; Sirera, P.; Aupí, M.; Pérez, S.; Asensi, M.; Ortega, A.; Estrela, J.M. Topical Treatment with Pterostilbene, a Natural Phytoalexin, Effectively Protects Hairless Mice against UVB Radiation-Induced Skin Damage and Carcinogenesis. Free Radic. Biol. Med. 2015, 85, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Perecko, T.; Drabikova, K.; Lojek, A.; Ciz, M.; Ponist, S.; Bauerova, K.; Nosal, R.; Harmatha, J.; Jancinova, V. The Effects of Pterostilbene on Neutrophil Activity in Experimental Model of Arthritis. Biomed. Res. Int. 2013, 2013, 106041. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.-R.; Li, S.; Lin, C.-C. Effect of Resveratrol and Pterostilbene on Aging and Longevity. Biofactors 2018, 44, 69–82. [Google Scholar] [CrossRef] [PubMed]
- Alosi, J.A.; McDonald, D.E.; Schneider, J.S.; Privette, A.R.; McFadden, D.W. Pterostilbene Inhibits Breast Cancer in Vitro through Mitochondrial Depolarization and Induction of Caspase-Dependent Apoptosis. J. Surg. Res. 2010, 161, 195–201. [Google Scholar] [CrossRef] [PubMed]
- Mannal, P.; McDonald, D.; McFadden, D. Pterostilbene and Tamoxifen Show an Additive Effect against Breast Cancer in Vitro. Am. J. Surg. 2010, 200, 577–580. [Google Scholar] [CrossRef]
- Chakraborty, A.; Gupta, N.; Ghosh, K.; Roy, P. In Vitro Evaluation of the Cytotoxic, Anti-Proliferative and Anti-Oxidant Properties of Pterostilbene Isolated from Pterocarpus Marsupium. Toxicol. Vitr. 2010, 24, 1215–1228. [Google Scholar] [CrossRef]
- Mh, P.; Yh, C.; V, B.; K, N.; Ct, H. Pterostilbene Induces Apoptosis and Cell Cycle Arrest in Human Gastric Carcinoma Cells. J. Agric. Food Chem. 2007, 55, 7777–7785. [Google Scholar] [CrossRef]
- McCormack, D.E.; Mannal, P.; McDonald, D.; Tighe, S.; Hanson, J.; McFadden, D. Genomic Analysis of Pterostilbene Predicts Its Antiproliferative Effects against Pancreatic Cancer In Vitro and In Vivo. J. Gastrointest. Surg. 2012, 16, 1136–1143. [Google Scholar] [CrossRef]
- Zhang, L.; Zhou, G.; Song, W.; Tan, X.; Guo, Y.; Zhou, B.; Jing, H.; Zhao, S.; Chen, L. Pterostilbene Protects Vascular Endothelial Cells against Oxidized Low-Density Lipoprotein-Induced Apoptosis in Vitro and in Vivo. Apoptosis 2012, 17, 25–36. [Google Scholar] [CrossRef]
- Zhang, L.; Cui, L.; Zhou, G.; Jing, H.; Guo, Y.; Sun, W. Pterostilbene, a Natural Small-Molecular Compound, Promotes Cytoprotective Macroautophagy in Vascular Endothelial Cells. J. Nutr. Biochem. 2013, 24, 903–911. [Google Scholar] [CrossRef]
- Özdaş, S.; Taştekin, B.; Gürgen, S.G.; Özdaş, T.; Pelit, A.; Erkan, S.O.; Tuhanioğlu, B.; Gülnar, B.; Görgülü, O. Pterostilbene Protects Cochlea from Ototoxicity in Streptozotocin-Induced Diabetic Rats by Inhibiting Apoptosis. PLoS ONE 2020, 15, e0228429. [Google Scholar] [CrossRef] [PubMed]
- Dvorakova, M.; Landa, P. Anti-inflammatory activity of natural stilbenoids: A review. Pharmacol. Res. 2017, 124, 126–145. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Fan, C.; Yu, L.; Yang, Y.; Jiang, S.; Ma, Z.; Hu, W.; Li, T.; Yang, Z.; Tian, T.; et al. Pterostilbene Exerts an Anti-Inflammatory Effect via Regulating Endoplasmic Reticulum Stress in Endothelial Cells. Cytokine 2016, 77, 88–97. [Google Scholar] [CrossRef] [PubMed]
- Paul, S.; Rimando, A.M.; Lee, H.J.; Ji, Y.; Reddy, B.S.; Suh, N. Anti-Inflammatory Action of Pterostilbene Is Mediated through the P38 Mitogen-Activated Protein Kinase Pathway in Colon Cancer Cells. Cancer Prev. Res. 2009, 2, 650–657. [Google Scholar] [CrossRef] [PubMed]
- Lim, Y.R.I.; Preshaw, P.M.; Lim, L.P.; Ong, M.M.A.; Lin, H.-S.; Tan, K.S. Pterostilbene Complexed with Cyclodextrin Exerts Antimicrobial and Anti-Inflammatory Effects. Sci. Rep. 2020, 10, 9072. [Google Scholar] [CrossRef] [PubMed]
- Cichocki, M.; Paluszczak, J.; Szaefer, H.; Piechowiak, A.; Rimando, A.M.; Baer-Dubowska, W. Pterostilbene Is Equally Potent as Resveratrol in Inhibiting 12-O-Tetradecanoylphorbol-13-Acetate Activated NFkappaB, AP-1, COX-2, and INOS in Mouse Epidermis. Mol. Nutr. Food Res. 2008, 52 Suppl. S1, S62–S70. [Google Scholar] [CrossRef]
- Yan, W.; Ren, D.; Feng, X.; Huang, J.; Wang, D.; Li, T.; Zhang, D. Neuroprotective and Anti-Inflammatory Effect of Pterostilbene against Cerebral Ischemia/Reperfusion Injury via Suppression of COX-2. Front. Pharmacol. 2021, 12, 770329. [Google Scholar] [CrossRef]
- Liu, H.; Wu, X.; Luo, J.; Wang, X.; Guo, H.; Feng, D.; Zhao, L.; Bai, H.; Song, M.; Liu, X.; et al.; et al. Pterostilbene Attenuates Astrocytic Inflammation and Neuronal Oxidative Injury after Ischemia-Reperfusion by Inhibiting NF-ΚB Phosphorylation. Front. Immunol. 2019, 10, 2408. [Google Scholar] [CrossRef]
- Yang, H.; Hua, C.; Yang, X.; Fan, X.; Song, H.; Peng, L.; Ci, X. Pterostilbene Prevents LPS-Induced Early Pulmonary Fibrosis by Suppressing Oxidative Stress, Inflammation and Apoptosis in Vivo. Food Funct. 2020, 11, 4471–4484. [Google Scholar] [CrossRef]
- Rui, Z.; Zhang, L.; Li, X.; Han, J.; Yuan, Y.; Ding, H.; Liu, Y.; Ding, X. Pterostilbene Exert an Anti-Arthritic Effect by Attenuating Inflammation, Oxidative Stress, and Alteration of Gut Microbiota. J. Food. Biochem. 2022, 46, e14011. [Google Scholar] [CrossRef]
- Azzolini, M.; Mattarei, A.; La Spina, M.; Fanin, M.; Chiodarelli, G.; Romio, M.; Zoratti, M.; Paradisi, C.; Biasutto, L. New Natural Amino Acid-Bearing Prodrugs Boost Pterostilbene’s Oral Pharmacokinetic and Distribution Profile. Eur. J. Pharm. Biopharm. 2017, 115, 149–158. [Google Scholar] [CrossRef] [PubMed]
- Rimando, A.; Cuendet, M.; Desmarchelier, C.; Mehta, R.; Pezzuto, J.; Duke, S. Cancer Chemopreventive and Antioxidant Activities of Pterostilbene, a Naturally Occurring Analogue of Resveratrol. J. Agric. Food Chem. 2002, 50, 3453–3457. [Google Scholar] [CrossRef] [PubMed]
- Su, C.-M.; Lee, W.-H.; Wu, A.T.H.; Lin, Y.-K.; Wang, L.-S.; Wu, C.-H.; Yeh, C.-T. Pterostilbene Inhibits Triple-Negative Breast Cancer Metastasis via Inducing MicroRNA-205 Expression and Negatively Modulates Epithelial-to-Mesenchymal Transition. J. Nutr. Biochem. 2015, 26, 675–685. [Google Scholar] [CrossRef] [PubMed]
- Kong, Y.; Chen, G.; Xu, Z.; Yang, G.; Li, B.; Wu, X.; Xiao, W.; Xie, B.; Hu, L.; Sun, X.; et al. Pterostilbene Induces Apoptosis and Cell Cycle Arrest in Diffuse Large B-Cell Lymphoma Cells. Sci. Rep. 2016, 6, 37417. [Google Scholar] [CrossRef] [PubMed]
- Xie, B.; Xu, Z.; Hu, L.; Chen, G.; Wei, R.; Yang, G.; Li, B.; Chang, G.; Sun, X.; Wu, H.; et al. Pterostilbene Inhibits Human Multiple Myeloma Cells via ERK1/2 and JNK Pathway In Vitro and In Vivo. Int. J. Mol. Sci. 2016, 17, 1927. [Google Scholar] [CrossRef] [PubMed]
- Suh, N.; Paul, S.; Hao, X.; Simi, B.; Xiao, H.; Rimando, A.M.; Reddy, B.S. Pterostilbene, an Active Constituent of Blueberries, Suppresses Aberrant Crypt Foci Formation in the Azoxymethane-Induced Colon Carcinogenesis Model in Rats. Clin. Cancer Res. 2007, 13, 350–355. [Google Scholar] [CrossRef]
- Chatterjee, K.; Mukherjee, S.; Vanmanen, J.; Banerjee, P.; Fata, J.E. Dietary Polyphenols, Resveratrol and Pterostilbene Exhibit Antitumor Activity on an HPV E6-Positive Cervical Cancer Model: An in Vitro and in Vivo Analysis. Front. Oncol. 2019, 9, 352. [Google Scholar] [CrossRef]
- Tam, K.-W.; Ho, C.-T.; Tu, S.-H.; Lee, W.-J.; Huang, C.-S.; Chen, C.-S.; Wu, C.-H.; Lee, C.-H.; Ho, Y.-S. α-Tocopherol Succinate Enhances Pterostilbene Anti-Tumor Activity in Human Breast Cancer Cells in Vivo and in Vitro. Oncotarget 2017, 9, 4593–4606. [Google Scholar] [CrossRef]
- Benlloch, M.; Obrador, E.; Valles, S.L.; Rodriguez, M.L.; Sirerol, J.A.; Alcácer, J.; Pellicer, J.A.; Salvador, R.; Cerdá, C.; Sáez, G.T.; et al. Pterostilbene Decreases the Antioxidant Defenses of Aggressive Cancer Cells In Vivo: A Physiological Glucocorticoids- and Nrf2-Dependent Mechanism. Antioxid. Redox. Signal. 2016, 24, 974–990. [Google Scholar] [CrossRef]
- Wang, D.; Guo, H.; Yang, H.; Wang, D.; Gao, P.; Wei, W. Pterostilbene, An Active Constituent of Blueberries, Suppresses Proliferation Potential of Human Cholangiocarcinoma via Enhancing the Autophagic Flux. Front. Pharmacol. 2019, 10, 1238. [Google Scholar] [CrossRef]
- Huynh, T.-T.; Lin, C.-M.; Lee, W.-H.; Wu, A.T.H.; Lin, Y.-K.; Lin, Y.-F.; Yeh, C.-T.; Wang, L.-S. Pterostilbene Suppressed Irradiation-Resistant Glioma Stem Cells by Modulating GRP78/MiR-205 Axis. J. Nutr. Biochem. 2015, 26, 466–475. [Google Scholar] [CrossRef] [PubMed]
- Pari, L.; Satheesh, M.A. Effect of Pterostilbene on Hepatic Key Enzymes of Glucose Metabolism in Streptozotocin- and Nicotinamide-Induced Diabetic Rats. Life Sci. 2006, 79, 641–645. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Ren, S.; Ji, Y.; Liang, Y. Pterostilbene Ameliorates Nephropathy Injury in Streptozotocin-Induced Diabetic Rats. Pharmacology 2019, 104, 71–80. [Google Scholar] [CrossRef]
- Grover, J.K.; Vats, V.; Yadav, S. Effect of Feeding Aqueous Extract of Pterocarpus Marsupium on Glycogen Content of Tissues and the Key Enzymes of Carbohydrate Metabolism. Mol. Cell Biochem. 2002, 241, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.-F.; Liu, M.-L.; Cheng, A.-C.; Tsai, M.-L.; Ho, C.-T.; Liou, W.-S.; Pan, M.-H. Pterostilbene Inhibits Dimethylnitrosamine-Induced Liver Fibrosis in Rats. Food Chem. 2013, 138, 802–807. [Google Scholar] [CrossRef] [PubMed]
- Aguirre, L.; Palacios-Ortega, S.; Fernández-Quintela, A.; Hijona, E.; Bujanda, L.; Portillo, M.P. Pterostilbene Reduces Liver Steatosis and Modifies Hepatic Fatty Acid Profile in Obese Rats. Nutrients 2019, 11, 961. [Google Scholar] [CrossRef]
- Kim, H.; Seo, K.-H.; Yokoyama, W. Chemistry of Pterostilbene and Its Metabolic Effects. J. Agric. Food Chem. 2020, 68, 12836–12841. [Google Scholar] [CrossRef]
- Zhan, J.; Hu, T.; Shen, J.; Yang, G.; Ho, C.-T.; Li, S. Pterostilbene Is More Efficacious than Hydroxystilbenes in Protecting Liver Fibrogenesis in a Carbon Tetracholride-Induced Rat Model. J. Funct. Foods 2021, 84, 104604. [Google Scholar] [CrossRef]
- Fan, X.; Wang, L.; Huang, J.; Lv, H.; Deng, X.; Ci, X. Pterostilbene Reduces Acetaminophen-Induced Liver Injury by Activating the Nrf2 Antioxidative Defense System via the AMPK/Akt/GSK3β Pathway. CPB 2018, 49, 1943–1958. [Google Scholar] [CrossRef]
- Blueberry Supplementation Enhances Signaling and Prevents Behavioral Deficits in an Alzheimer Disease Model: Nutritional Neuroscience. Volume 6. No. 3. Available online: https://www.tandfonline.com/doi/abs/10.1080/1028415031000111282 (accessed on 5 May 2022).
- Yang, Y.; Wang, J.; Li, Y.; Fan, C.; Jiang, S.; Zhao, L.; Di, S.; Xin, Z.; Wang, B.; Wu, G.; et al. HO-1 Signaling Activation by Pterostilbene Treatment Attenuates Mitochondrial Oxidative Damage Induced by Cerebral Ischemia Reperfusion Injury. Mol. Neurobiol. 2015, 53, 2339–2353. [Google Scholar] [CrossRef]
- Chang, J.; Rimando, A.; Pallas, M.; Camins, A.; Porquet, D.; Reeves, J.; Shukitt-Hale, B.; Smith, M.A.; Joseph, J.A.; Casadesus, G. Low-Dose Pterostilbene, but Not Resveratrol, Is a Potent Neuromodulator in Aging and Alzheimer’s Disease. Neurobiol. Aging 2012, 33, 2062–2071. [Google Scholar] [CrossRef] [PubMed]
- Lacerda, D.; Türck, P.; Campos-Carraro, C.; Hickmann, A.; Ortiz, V.; Bianchi, S.; Belló-Klein, A.; de Castro, A.L.; Bassani, V.L.; da Rosa Araujo, A.S. Pterostilbene Improves Cardiac Function in a Rat Model of Right Heart Failure through Modulation of Calcium Handling Proteins and Oxidative Stress. Appl. Physiol. Nutr. Metab. 2020, 45, 987–995. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Kang, J.; Xie, C.; Burris, R.; Ferguson, M.E.; Badger, T.M.; Nagarajan, S. Dietary Blueberries Attenuate Atherosclerosis in Apolipoprotein E-Deficient Mice by Upregulating Antioxidant Enzyme Expression. J. Nutr. 2010, 140, 1628–1632. [Google Scholar] [CrossRef] [PubMed]
- Ahmet, I.; Spangler, E.; Shukitt-Hale, B.; Juhaszova, M.; Sollott, S.J.; Joseph, J.A.; Ingram, D.K.; Talan, M. Blueberry-Enriched Diet Protects Rat Heart from Ischemic Damage. PLoS ONE 2009, 4, e5954. [Google Scholar] [CrossRef]
- Yang, G.; Sun, J.; Lu, K.; Shan, S.; Li, S.; Sun, C. Pterostilbene Coupled with Physical Exercise Effectively Mitigates Collagen-Induced Articular Synovial by Correcting the PI3K/Akt/NF-ΚB Signal Pathway. J. Agric. Food Chem. 2021, 69, 13821–13830. [Google Scholar] [CrossRef]
- Elsherbini, A.M.; Sheweita, S.A.; Sultan, A.S. Pterostilbene as a Phytochemical Compound Induces Signaling Pathways Involved in the Apoptosis and Death of Mutant P53-Breast Cancer Cell Lines. Nutr. Cancer 2021, 73, 1976–1984. [Google Scholar] [CrossRef]
- Priego, S.; Feddi, F.; Ferrer, P.; Mena, S.; Benlloch, M.; Ortega, A.; Carretero, J.; Obrador, E.; Asensi, M.; Estrela, J.M. Natural Polyphenols Facilitate Elimination of HT-29 Colorectal Cancer Xenografts by Chemoradiotherapy: A Bcl-2- and Superoxide Dismutase 2-Dependent Mechanism. Mol. Cancer Ther. 2008, 7, 3330–3342. [Google Scholar] [CrossRef]
- Paul, S.; DeCastro, A.J.; Lee, H.J.; Smolarek, A.K.; So, J.Y.; Simi, B.; Wang, C.X.; Zhou, R.; Rimando, A.M.; Suh, N. Dietary Intake of Pterostilbene, a Constituent of Blueberries, Inhibits the β-Catenin/P65 Downstream Signaling Pathway and Colon Carcinogenesis in Rats. Carcinogenesis 2010, 31, 1272–1278. [Google Scholar] [CrossRef]
- Ferrer, P.; Asensi, M.; Segarra, R.; Ortega, A.; Benlloch, M.; Obrador, E.; Varea, M.T.; Asensio, G.; Jordá, L.; Estrela, J.M. Association between Pterostilbene and Quercetin Inhibits Metastatic Activity of B16 Melanoma. Neoplasia 2005, 7, 37–47. [Google Scholar] [CrossRef]
- Mena, S.; Rodríguez, M.L.; Ponsoda, X.; Estrela, J.M.; Jäättela, M.; Ortega, A.L. Pterostilbene-Induced Tumor Cytotoxicity: A Lysosomal Membrane Permeabilization-Dependent Mechanism. PLoS ONE 2012, 7, e44524. [Google Scholar] [CrossRef]
- Tsai, M.-L.; Lai, C.-S.; Chang, Y.-H.; Chen, W.-J.; Ho, C.-T.; Pan, M.-H. Pterostilbene, a Natural Analogue of Resveratrol, Potently Inhibits 7,12-Dimethylbenz[a]Anthracene (DMBA)/12-O-Tetradecanoylphorbol-13-Acetate (TPA)-Induced Mouse Skin Carcinogenesis. Food Funct. 2012, 3, 1185–1194. [Google Scholar] [CrossRef] [PubMed]
- Wen, W.; Lowe, G.; Roberts, C.M.; Finlay, J.; Han, E.S.; Glackin, C.A.; Dellinger, T.H. Pterostilbene, a Natural Phenolic Compound, Synergizes the Antineoplastic Effects of Megestrol Acetate in Endometrial Cancer. Sci. Rep. 2017, 7, 12754. [Google Scholar] [CrossRef] [PubMed]
- Wen, W.; Lowe, G.; Roberts, C.M.; Finlay, J.; Han, E.S.; Glackin, C.A.; Dellinger, T.H. Pterostilbene Suppresses Ovarian Cancer Growth via Induction of Apoptosis and Blockade of Cell Cycle Progression Involving Inhibition of the STAT3 Pathway. Int. J. Mol. Sci. 2018, 19, 1983. [Google Scholar] [CrossRef]
- Riche, D.M.; Riche, K.D.; Blackshear, C.T.; McEwen, C.L.; Sherman, J.J.; Wofford, M.R.; Griswold, M.E. Pterostilbene on Metabolic Parameters: A Randomized, Double-Blind, and Placebo-Controlled Trial. Evid. Based Complement. Altern. Med. 2014, 2014, 459165. [Google Scholar] [CrossRef]
- Guo, L.; Tan, K.; Wang, H.; Zhang, X. Pterostilbene Inhibits Hepatocellular Carcinoma through P53/SOD2/ROS-Mediated Mitochondrial Apoptosis. Oncol. Rep. 2016, 36, 3233–3240. [Google Scholar] [CrossRef] [PubMed]
- Wang, R.; Xu, Z.; Tian, J.; Liu, Q.; Dong, J.; Guo, L.; Hai, B.; Liu, X.; Yao, H.; Chen, Z.; et al. Pterostilbene Inhibits Hepatocellular Carcinoma Proliferation and HBV Replication by Targeting Ribonucleotide Reductase M2 Protein. Am. J. Cancer Res. 2021, 11, 2975–2989. [Google Scholar] [PubMed]
- Qian, Y.-Y.; Liu, Z.-S.; Yan, H.-J.; Yuan, Y.-F.; Levenson, A.S.; Li, K. Pterostilbene Inhibits MTA1/HDAC1 Complex Leading to PTEN Acetylation in Hepatocellular Carcinoma. Biomed. Pharmacother. 2018, 101, 852–859. [Google Scholar] [CrossRef]
- Baquer, N.Z.; Gupta, D.; Raju, J. Regulation of Metabolic Pathways in Liver and Kidney during Experimental Diabetes: Effects of Antidiabetic Compounds. Indian J. Clin. Biochem. 1998, 13, 63–80. [Google Scholar] [CrossRef]
- Satheesh, M.A.; Pari, L. The Antioxidant Role of Pterostilbene in Streptozotocin-Nicotinamide-Induced Type 2 Diabetes Mellitus in Wistar Rats. J. Pharm. Pharmacol. 2010, 58, 1483–1490. [Google Scholar] [CrossRef]
- Dornadula, S.; Thiruppathi, S.; Palanisamy, R.; Umapathy, D.; Suzuki, T.; Mohanram, R.K. Differential Proteomic Profiling Identifies Novel Molecular Targets of Pterostilbene against Experimental Diabetes. J. Cell. Physiol. 2019, 234, 1996–2012. [Google Scholar] [CrossRef]
- Acharya, J.D.; Ghaskadbi, S.S. Protective Effect of Pterostilbene against Free Radical Mediated Oxidative Damage. BMC Complement. Altern. Med. 2013, 13, 238. [Google Scholar] [CrossRef] [PubMed]
- Schuppan, D.; Afdhal, N.H. Liver Cirrhosis. Lancet 2008, 371, 838–851. [Google Scholar] [CrossRef]
- Tsai, H.-Y.; Shih, Y.-Y.; Yeh, Y.-T.; Huang, C.-H.; Liao, C.-A.; Hu, C.-Y.; Nagabhushanam, K.; Ho, C.-T.; Chen, Y.-K. Pterostilbene and Its Derivative 3’-Hydroxypterostilbene Ameliorated Nonalcoholic Fatty Liver Disease Through Synergistic Modulation of the Gut Microbiota and SIRT1/AMPK Signaling Pathway. J. Agric. Food Chem. 2022, 70, 4966–4980. [Google Scholar] [CrossRef] [PubMed]
- Joseph, J.A.; Fisher, D.R.; Cheng, V.; Rimando, A.M.; Shukitt-Hale, B. Cellular and Behavioral Effects of Stilbene Resveratrol Analogues: Implications for Reducing the Deleterious Effects of Aging. J. Agric. Food Chem. 2008, 56, 10544–10551. [Google Scholar] [CrossRef]
- Song, Z.; Han, S.; Pan, X.; Gong, Y.; Wang, M. Pterostilbene Mediates Neuroprotection against Oxidative Toxicity via Oestrogen Receptor α Signalling Pathways. J. Pharm. Pharmacol. 2015, 67, 720–730. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Fan, C.; Wang, B.; Ma, Z.; Wang, D.; Gong, B.; Di, S.; Jiang, S.; Li, Y.; Li, T.; et al. Pterostilbene Attenuates High Glucose-Induced Oxidative Injury in Hippocampal Neuronal Cells by Activating Nuclear Factor Erythroid 2-Related Factor 2. Biochim. Biophys. Acta Mol. Basis Dis. 2017, 1863, 827–837. [Google Scholar] [CrossRef] [PubMed]
- Poulose, S.M.; Thangthaeng, N.; Miller, M.G.; Shukitt-Hale, B. Effects of Pterostilbene and Resveratrol on Brain and Behavior. Neurochem. Int. 2015, 89, 227–233. [Google Scholar] [CrossRef]
- Sinha, K.; Chaudhary, G.; Kumar Gupta, Y. Protective Effect of Resveratrol against Oxidative Stress in Middle Cerebral Artery Occlusion Model of Stroke in Rats. Life Sci. 2002, 71, 655–665. [Google Scholar] [CrossRef]
- Zhang, F.; Shi, J.-S.; Zhou, H.; Wilson, B.; Hong, J.-S.; Gao, H.-M. Resveratrol Protects Dopamine Neurons against Lipopolysaccharide-Induced Neurotoxicity through Its Anti-Inflammatory Actions. Mol. Pharmacol. 2010, 78, 466–477. [Google Scholar] [CrossRef]
- Kosuru, R.; Kandula, V.; Rai, U.; Prakash, S.; Xia, Z.; Singh, S. Pterostilbene Decreases Cardiac Oxidative Stress and Inflammation via Activation of AMPK/Nrf2/HO-1 Pathway in Fructose-Fed Diabetic Rats. Cardiovasc. Drugs Ther. 2018, 32, 147–163. [Google Scholar] [CrossRef]
- Mechanisms of atherosclerosis--a review. Adv. Nephrol. Necker Hosp. 1990, 19, 79–86.
- Park, E.-S.; Lim, Y.; Hong, J.-T.; Yoo, H.-S.; Lee, C.-K.; Pyo, M.-Y.; Yun, Y.-P. Pterostilbene, a Natural Dimethylated Analog of Resveratrol, Inhibits Rat Aortic Vascular Smooth Muscle Cell Proliferation by Blocking Akt-Dependent Pathway. Vasc. Pharmacol. 2010, 53, 61–67. [Google Scholar] [CrossRef] [PubMed]
- Hou, Y.; Xie, G.; Miao, F.; Ding, L.; Mou, Y.; Wang, L.; Su, G.; Chen, G.; Yang, J.; Wu, C. Pterostilbene Attenuates Lipopolysaccharide-Induced Learning and Memory Impairment Possibly via Inhibiting Microglia Activation and Protecting Neuronal Injury in Mice. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2014, 54, 92–102. [Google Scholar] [CrossRef] [PubMed]
- Porquet, D.; Casadesús, G.; Bayod, S.; Vicente, A.; Canudas, A.M.; Vilaplana, J.; Pelegrí, C.; Sanfeliu, C.; Camins, A.; Pallàs, M.; et al. Dietary Resveratrol Prevents Alzheimer’s Markers and Increases Life Span in SAMP8. AGE 2013, 35, 1851–1865. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Deng, R.; Hua, X.; Zhang, L.; Lu, F.; Coursey, T.G.; Pflugfelder, S.C.; Li, D.-Q. Blueberry Component Pterostilbene Protects Corneal Epithelial Cells from Inflammation via Anti-Oxidative Pathway. Sci. Rep. 2016, 6, 19408. [Google Scholar] [CrossRef]
- Wilson, M.A.; Shukitt-Hale, B.; Kalt, W.; Ingram, D.K.; Joseph, J.A.; Wolkow, C.A. Blueberry Polyphenols Increase Lifespan and Thermotolerance in Caenorhabditis Elegans. Aging Cell 2006, 5, 59–68. [Google Scholar] [CrossRef]
- Peng, C.; Zuo, Y.; Kwan, K.M.; Liang, Y.; Ma, K.Y.; Chan, H.Y.E.; Huang, Y.; Yu, H.; Chen, Z.-Y. Blueberry Extract Prolongs Lifespan of Drosophila Melanogaster. Exp. Gerontol. 2012, 47, 170–178. [Google Scholar] [CrossRef]
- Joseph, J.A.; Denisova, N.A.; Arendash, G.; Gordon, M.; Diamond, D.; Shukitt-Hale, B.; Morgan, D. Blueberry Supplementation Enhances Signaling and Prevents Behavioral Deficits in an Alzheimer Disease Model. Nutr. Neurosci. 2003, 6, 153–162. [Google Scholar] [CrossRef]
- Majeed, M.; Majeed, S.; Jain, R.; Mundkur, L.; Rajalakshmi, H.; Lad, P.S.; Neupane, P. An Open-Label Single-Arm, Monocentric Study Assessing the Efficacy and Safety of Natural Pterostilbene (Pterocarpus Marsupium) for Skin Brightening and Antiaging Effects. Clin. Cosmet. Investig. Dermatol. 2020, 13, 105–116. [Google Scholar] [CrossRef]
- Vaňková, E.; Paldrychová, M.; Kašparová, P.; Lokočová, K.; Kodeš, Z.; Maťátková, O.; Kolouchová, I.; Masák, J. Natural Antioxidant Pterostilbene as an Effective Antibiofilm Agent, Particularly for Gram-Positive Cocci. World J. Microbiol. Biotechnol. 2020, 36, 101. [Google Scholar] [CrossRef]
- Shih, Y.-H.; Tsai, P.-J.; Chen, Y.-L.; Pranata, R.; Chen, R.-J. Assessment of the Antibacterial Mechanism of Pterostilbene against Bacillus Cereus through Apoptosis-like Cell Death and Evaluation of Its Beneficial Effects on the Gut Microbiota. J. Agric. Food Chem. 2021, 69, 12219–12229. [Google Scholar] [CrossRef] [PubMed]
- Lee, W.X.; Basri, D.F.; Ghazali, A.R. Bactericidal Effect of Pterostilbene Alone and in Combination with Gentamicin against Human Pathogenic Bacteria. Molecules 2017, 22, 463. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.-C.; Tseng, C.-H.; Wang, P.-W.; Lu, P.-L.; Weng, Y.-H.; Yen, F.-L.; Fang, J.-Y. Pterostilbene, a Methoxylated Resveratrol Derivative, Efficiently Eradicates Planktonic, Biofilm, and Intracellular MRSA by Topical Application. Front. Microbiol. 2017, 8, 1103. [Google Scholar] [CrossRef] [PubMed]
- ter Ellen, B.M.; Dinesh Kumar, N.; Bouma, E.M.; Troost, B.; van de Pol, D.P.I.; van der Ende-Metselaar, H.H.; Apperloo, L.; van Gosliga, D.; van den Berge, M.; Nawijn, M.C.; et al. Resveratrol and Pterostilbene Inhibit SARS-CoV-2 Replication in Air–Liquid Interface Cultured Human Primary Bronchial Epithelial Cells. Viruses 2021, 13, 1335. [Google Scholar] [CrossRef] [PubMed]
- Lin, S.-C.; Ho, C.-T.; Chuo, W.-H.; Li, S.; Wang, T.T.; Lin, C.-C. Effective Inhibition of MERS-CoV Infection by Resveratrol. BMC Infect. Dis. 2017, 17, 144. [Google Scholar] [CrossRef]
- Das, A.; Pandita, D.; Jain, G.K.; Agarwal, P.; Grewal, A.S.; Khar, R.K.; Lather, V. Role of Phytoconstituents in the Management of COVID-19. Chem. Biol. Interact. 2021, 341, 109449. [Google Scholar] [CrossRef] [PubMed]
- Kelleni, M.T. Resveratrol-Zinc Nanoparticles or Pterostilbene-Zinc: Potential COVID-19 Mono and Adjuvant Therapy. Biomed Pharmacother. 2021, 139, 111626. [Google Scholar] [CrossRef]
- Hsieh, Y.-H.; Chen, C.W.S.; Schmitz, S.-F.H.; King, C.-C.; Chen, W.-J.; Wu, Y.-C.; Ho, M.-S. Candidate Genes Associated with Susceptibility for SARS-Coronavirus. Bull. Math. Biol. 2010, 72, 122–132. [Google Scholar] [CrossRef]
- Hu, W.; Yu, H.; Zhou, X.; Li, M.; Xiao, L.; Ruan, Q.; Huang, X.; Li, L.; Xie, W.; Guo, X.; et al. Topical Administration of Pterostilbene Accelerates Burn Wound Healing in Diabetes through Activation of the HIF1α Signaling Pathway. Burns 2021, 48, 1452–1461. [Google Scholar] [CrossRef]
- Bofill, L.; Barbas, R.; de Sande, D.; Font-Bardia, M.; Ràfols, C.; Albertí, J.; Prohens, R. A Novel, Extremely Bioavailable Cocrystal of Pterostilbene. Cryst. Growth Des. 2021, 21, 2315–2323. [Google Scholar] [CrossRef]
- Schultheiss, N.; Bethune, S.; Henck, J.-O. Nutraceutical Cocrystals: Utilizing Pterostilbene as a Cocrystal Former. CrystEngComm 2010, 12, 2436–2442. [Google Scholar] [CrossRef]
- Zhao, X.; Shi, A.; Ma, Q.; Yan, X.; Bian, L.; Zhang, P.; Wu, J. Nanoparticles Prepared from Pterostilbene Reduce Blood Glucose and Improve Diabetes Complications. J. Nanobiotechnol. 2021, 19, 191. [Google Scholar] [CrossRef] [PubMed]
- Liu, K.-F.; Liu, Y.-X.; Dai, L.; Li, C.-X.; Wang, L.; Liu, J.; Lei, J.-D. A Novel Self-Assembled PH-Sensitive Targeted Nanoparticle Platform Based on Antibody–4arm-Polyethylene Glycol–Pterostilbene Conjugates for Co-Delivery of Anticancer Drugs. J. Mater. Chem. B 2018, 6, 656–665. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Chen, J.; Qin, Y.; Jiang, B.; Zhang, T. Zein/Fucoidan-Based Composite Nanoparticles for the Encapsulation of Pterostilbene: Preparation, Characterization, Physicochemical Stability, and Formation Mechanism. Int. J. Biol. Macromol. 2020, 158, 461–470. [Google Scholar] [CrossRef]
- Romio, M.; Morgese, G.; Trachsel, L.; Babity, S.; Paradisi, C.; Brambilla, D.; Benetti, E.M. Poly(2-Oxazoline)–Pterostilbene Block Copolymer Nanoparticles for Dual-Anticancer Drug Delivery. Biomacromolecules 2018, 19, 103–111. [Google Scholar] [CrossRef]
- Sun, Y.; Xia, Z.; Zheng, J.; Qiu, P.; Zhang, L.; McClements, D.J.; Xiao, H. Nanoemulsion-Based Delivery Systems for Nutraceuticals: Influence of Carrier Oil Type on Bioavailability of Pterostilbene. J. Funct. Foods 2015, 13, 61–70. [Google Scholar] [CrossRef]
- Ansari, M.; Sadarani, B.; Majumdar, A. Colon Targeted Beads Loaded with Pterostilbene: Formulation, Optimization, Characterization and in Vivo Evaluation. Saudi Pharm. J. 2019, 27, 71–81. [Google Scholar] [CrossRef]



| Source | Concentration Range | Reference |
|---|---|---|
| Blueberries | 9.9–15.1 mg/kg of fresh weight | [13] |
| Blueberries | 15 µg/100 g of weight | [11] |
| Vaccinium berries | 99–520 ng/g of dry sample in Vaccinium ashei and V. stamineum | [11] |
| Fungal infected grapes | 0.2–4.7 mg/g of fresh weight | [14] |
| Rabbit-eye blueberry | 99–151 ng/g of dry sample | [11] |
| Deerberries | 520 ng/g of dry sample | [11] |
| Peanut | NA | [12] |
| Disease Condition | Experimental Model | Effect of Pterostilbene | Reference |
|---|---|---|---|
| Cancer | Endometrial cancer xenograft model | Reduced weight and volume of tumor | [61] |
| DMBA-induced mammary alveolar precancerous lesions in mice | Reduced lesions | [62] | |
| MDA-MB-231 (breast cancer) xenograft model | Suppressed tumor growth | [63] | |
| UVB-induced skin cancer in mice | Nrf2-dependent antioxidant response | [41] | |
| Hematological cancer xenograft model | (a) Increased caspase activation (b) Reduced cell proliferation | [64,65] | |
| Azoxymethane-induced colon cancer model | Reduced iNOS levels and attenuated crypt formation | [66] | |
| MIA PaCa-2 xenograft model | Inhibited tumor growth and prominent central necrosis | [48] | |
| HPV-E6-positive cervical cancer mouse model | (a) Increased apoptosis (b) Downregulated E6 and VEGF expression | [67] | |
| Breast cancer xenograft mouse model | When coupled with Vitamin E: (a) Inhibited Akt (b) Downregulated cell-cycle proteins | [68] | |
| Melanoma xenograft mouse model | ACTH downregulation led to decreased Nrf2-mediated defenses | [69] | |
| Large B-cell lymphoma xenograft mouse model | (a) Reduced mitochondrial membrane potential (b) Increased apoptosis | [64] | |
| Biliary cancer xenograft mouse model | (a) Inhibited proliferation (b) Induced autophagy | [70] | |
| Multiple myeloma mouse xenograft | (a) Inhibited cell progression (b) Increased ROS production for apoptosis (c) Improved extracellular-signal- regulated kinases 1/2 and c-Jun N-terminal kinase signaling | [65] | |
| Xenograft of glioma stem cells in mice | Attenuated GRP78, suppressing tumorogenesis | [71] | |
| Diabetes | STZ-induced diabetic rats | Protected rats from ototoxicity through the inhibition of apoptosis | [51] |
| STZ- and Nicotinamide-induced diabetic rats | (a) Increased hepatic glycolytic enzyme hexokinase (b) Reduced the levels of glycogenic enzymes and enhanced peripheral utilization of glucose | [72] | |
| STZ-induced diabetic rats | (a) Regulated NF-κB signal pathway and inhibited oxidative stress and inflammation (b) Improved renal damage | [73] | |
| STZ-induced diabetic mouse | (a) Normalized plasma VLDL, LDL, and HDL (b) Reduced lipid peroxidation | [36] | |
| Diabetic rats | (a) Enhanced the peripheral utilization of glucose (b) Elevated the levels of hepatic hexokinase and hepatic phosphofructokinase | [74] | |
| Liver injury | Dimethyl nitrosamine-induced rats with liver fibrosis | (a) Hepatoprotective activities (b) Inhibited TGF-b1/Smad signaling | [75] |
| Zucker rats with liver steatosis | (a) Reduced insulin and hepatic triacylglycerol levels (b) Improved fatty acid profile | [76] | |
| Hamsters with a High-fat diet supplemented with 8% blueberry by-product | (a) Low plasma LDL (b) Increased phosphorylation of adenosine monophosphate-activated protein kinase | [77] | |
| Hypercholesterolemic hamsters | Cytoprotective macroautophagy | [7] | |
| CCl4-stimulated hepatic fibrosis rat models | (a) Reduced levels of α-smooth muscle cell actin, desmins, MMP2, and MMP9 (b) Downregulated pro-fibrogenesis through the suppression of TGF-β1 in liver tissue | [78] | |
| Acetaminophen-exposed rats | Suppressed Acetaminophen-induced oxidative stress | [79] | |
| Diseases of the Central Nervous System | Amyloid precursor protein (APP)/Presenilin 1 (PS1) SERCA mouse model with Alzheimer’s disease | Reduced amyloid-beta content Improved pathological changes | [80] |
| Common carotid artery occlusion mouse model to study cerebral ischemia/reperfusion injury | Upregulated antioxidant activity through HO-1 | [81] | |
| SAMP8-Alzheimer’s disease mouse model | Increased peroxisome proliferator-activated receptor-α expression | [82] | |
| Middle cerebral artery occlusion rodent model | (a) Suppressed the swelling and disintegration of cells and attenuated the infiltration of macrophages and monocytes (b) Attenuated the degranulation of polymorphonuclear leukocytes in neural tissue | [57] | |
| Cardiovascular disease | Monocrotaline-treated rats with reduced cardiac function | (a) Prevented reduction in stroke volume and cardiac output (b) Reduced lipid peroxidation and total phospholamban (c) Increased SERCA expression in the right ventricle | [83] |
| Apo-lipoprotein-E-deficient mice | Reduced atherosclerosis by inhibiting lipid peroxidation and enhanced antioxidants | [84] | |
| Fischer-344 rat model of coronary artery ligation | Reduced myocardial infarction size by 22% | [85] | |
| Arthritis | Bovine type II collagen-stimulated rat arthritis model | Reduced pathological process of arthritis when coupled with physical exercise | [86] |
| Freund’s adjuvant (CFA)-induced arthritis rat model | (a) Alleviated the swelling of paw and reduced arthritic score (b) Improved body weight | [60] | |
| Injection of heat-killed Mycobacterium butyricum in Lewis rats | Lowered number of neutrophils, thereby downregulating neutrophil oxidative burst | [42] |
| Clinical Trial | Subjects | The Drug Used/Diet | Status | Findings | Reference |
|---|---|---|---|---|---|
| Studying the Effects of ElevATP on Body Composition and Athletic Performance of Healthy Individuals | Healthy 18–35-year-old males | ElevATP with and without caffeine and Vitamins | Completed | Improved strength and power output in the lower body | ClinicalTrials.gov Identifier: NCT02819219 |
| Study of Pharmacokinetics and Safety of Basis™ in Subjects with Acute Kidney Injury | Patients with Acute Kidney Injury | Basis | Completed | Nicotinamide riboside with pterostilbene increased whole-blood NAD + levels | ClinicalTrials.gov Identifier: NCT03176628 |
| Effect of PTS on Cholesterol and Hypertension | Patients with hyperlipidemia and increased Blood Pressure | 1. PTS (low dosage of 50 mg and high dosage of 125 mg) 2. Low dose combination of PTS and grape extract (50 mg + 100 mg) | Completed | PTS increased LDL and reduced blood pressure in adults [95] | ClinicalTrials.gov Identifier: NCT01267227 |
| Evaluating Safety and Benefits of Basis™ Among Elderly Subjects | 60–80-year-old healthy subjects | Basis™ | Completed | Yet to be published | ClinicalTrials.gov Identifier: NCT02678611 |
| A Trial of Nicotinamide/PTS Supplement in Amyotrophic Lateral Sclerosis | Patients with Amyotrophic Lateral Sclerosis | EH301 (nicotinamide riboside/PTS) | Recruiting | Yet to be published | ClinicalTrials.gov Identifier: NCT05095571 |
| Effect of Blueberries in Postmenopausal Women with Elevated Blood Pressure for Improving Vascular Endothelial Function | Postmenopausal women with elevated blood pressure, hypertension, and endothelial dysfunction | Blueberry powder | Active Phase 2 Phase 3 | Yet to be published | ClinicalTrials.gov Identifier: NCT03370991 |
| Supplementing Wild Blueberries to Study Cardiovascular Health in Middle-aged/Older Men | 45- to 70-year-old men with hypertension and endothelial dysfunction | Blueberry powder | Recruiting Phase 1 Phase 2 | Yet to be published | ClinicalTrials.gov Identifier: NCT04530916 |
| Effect of High-intensity Training and Daily Consumption of Basis™ on Muscle Metabolism and Exercise | 18- to 25-year-old healthy men | NRPT (125 mg nicotinamide riboside and 25 mg PTS) | Phase 1 | Yet to be published | ClinicalTrials.gov Identifier: NCT04050358 |
| Study of Treating Megestrol Acetate with or without PTS in Patients with Endometrial Cancer Undergoing Hysterectomy | Women with Atypical Endometrial Hyperplasia and Endometrial Carcinoma | Megestrol Acetate with or without PTS | Recruiting Phase 2 | Yet to be published | ClinicalTrials.gov Identifier: NCT03671811 |
| Protection of Basis™ in Acute Kidney Injury | Patients with Acute Kidney Injury | Nicotinamide riboside + PTS | Recruiting Phase 2 | Yet to be published | ClinicalTrials.gov Identifier: NCT04342975 |
| Studying the Benefit of Supplementation with Short-term Curcumin and Multi-polyphenol | Non-smokers in good health not taking medications or dietary supplements | Polyresveratrol supplementation (100 mg of trans-PTS, 100 mg of curcumin phytosome, 100 mg of quercetin phytosome, 100 mg of green tea phytosome, and 100 mg of trans-resveratrol) | Unknown | Not Published | ClinicalTrials.gov Identifier: NCT02998918 |
| Studying effects of Nicotinamide Riboside and PTS on Muscle Regeneration in Elderly Humans | 55- to 80-year- old individuals | Nicotinamide riboside/PTS-NRPT (500 mg/100 mg twice daily) | Completed | Not published | ClinicalTrials.gov Identifier: NCT03754842 |
| Evaluating Sirtuin Supplements to Benefit Elderly Trauma Patients to study recovery of function | Individuals 65 years and older presenting to trauma bay | Nicotinamide riboside and PTS | Unknown | Not published | ClinicalTrials.gov Identifier: NCT03635411 |
| Effects of a Seven-day BASIS™ Supplementation on Menopausal Syndrome, Estradiol levels and Measurements of the Urinary Vitamin B3 | Women 35 years or older | BASIS™ | Completed | Not published | ClinicalTrials.gov Identifier: NCT04841499 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nagarajan, S.; Mohandas, S.; Ganesan, K.; Xu, B.; Ramkumar, K.M. New Insights into Dietary Pterostilbene: Sources, Metabolism, and Health Promotion Effects. Molecules 2022, 27, 6316. https://doi.org/10.3390/molecules27196316
Nagarajan S, Mohandas S, Ganesan K, Xu B, Ramkumar KM. New Insights into Dietary Pterostilbene: Sources, Metabolism, and Health Promotion Effects. Molecules. 2022; 27(19):6316. https://doi.org/10.3390/molecules27196316
Chicago/Turabian StyleNagarajan, Sanjushree, Sundhar Mohandas, Kumar Ganesan, Baojun Xu, and Kunka Mohanram Ramkumar. 2022. "New Insights into Dietary Pterostilbene: Sources, Metabolism, and Health Promotion Effects" Molecules 27, no. 19: 6316. https://doi.org/10.3390/molecules27196316
APA StyleNagarajan, S., Mohandas, S., Ganesan, K., Xu, B., & Ramkumar, K. M. (2022). New Insights into Dietary Pterostilbene: Sources, Metabolism, and Health Promotion Effects. Molecules, 27(19), 6316. https://doi.org/10.3390/molecules27196316







