Liposomes: Clinical Applications and Potential for Image-Guided Drug Delivery
Abstract
1. Introduction
2. Clinical Applications of Liposomes
2.1. Liposomal Formulations in Clinical Trials
2.1.1. Phase I
2.1.2. Phase II
2.1.3. Phase III
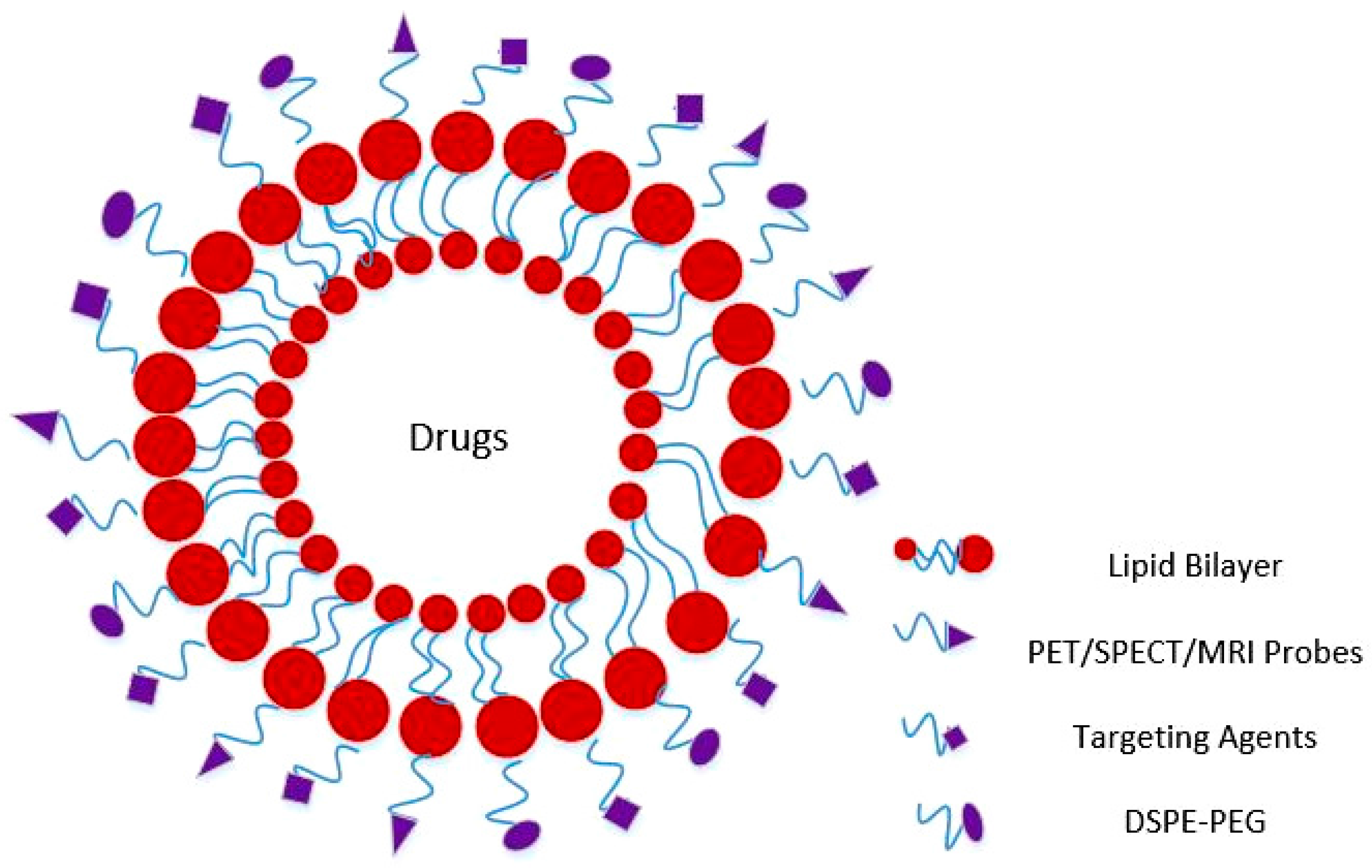
2.2. Liposomes and Image Guided Delivery
2.3. PET Imaging
2.4. SPECT Imaging
2.5. MRI Imaging
3. Conclusions
Conflicts of Interest
References
- Nagathihalli, N.S.; Castellanos, J.A.; Shi, C.; Beesetty, Y.; Reyzer, M.L.; Caprioli, R.; Chen, X.; Walsh, A.J.; Skala, M.C.; Moses, H.L.; et al. Signal transducer and activator of transcription 3, mediated remodeling of the tumor microenvironment results in enhanced tumor drug delivery in a mouse model of pancreatic cancer. Gastroenterology 2015, 149, 1932–1943. [Google Scholar] [CrossRef] [PubMed]
- Sriraman, S.K.; Aryasomayajula, B.; Torchilin, V.P. Barriers to drug delivery in solid tumors. Tissue Barriers 2014, 2, e29528. [Google Scholar] [CrossRef] [PubMed]
- Akhdar, H.; Legendre, C.; Aninat, C.; More, F. Anticancer drug metabolism: Chemotherapy resistance and new therapeutic approaches. In Topics on Drug Metabolism; Paxton, J., Ed.; InTech: Rijeka, Croatia, 2012; p. 6. [Google Scholar]
- Ernsting, M.J.; Murakami, M.; Roy, A.; Li, S.D. Factors controlling the pharmacokinetics, biodistribution and intratumoral penetration of nanoparticles. J. Control. Release 2013, 172, 782–794. [Google Scholar] [CrossRef] [PubMed]
- Phillips, W.T.; Bao, A.; Brenner, A.J.; Goins, B.A. Image-guided interventional therapy for cancer with radiotherapeutic nanoparticles. Adv. Drug Deliv. Rev. 2014, 76, 39–59. [Google Scholar] [CrossRef] [PubMed]
- Lembo, D.; Cavalli, R. Nanoparticulate delivery systems for antiviral drugs. Antivir. Chem. Chemother. 2010, 21, 53–70. [Google Scholar] [CrossRef] [PubMed]
- Massoud, T.F.; Gambhir, S.S. Molecular imaging in living subjects: Seeing fundamental biological processes in a new light. Genes Dev. 2003, 17, 545–580. [Google Scholar] [CrossRef] [PubMed]
- Ostro, M.J.; Cullis, P.R. Use of liposomes as injectable-drug delivery systems. Am. J. Hosp. Pharm. 1989, 46, 1576–1587. [Google Scholar] [PubMed]
- Caminade, A.M. Phosphorus dendrimers for nanomedicine. Chem. Commun. (Camb.) 2017, 53, 9830–9838. [Google Scholar] [CrossRef] [PubMed]
- Elbayoumi, T.A.; Torchilin, V.P. Current trends in liposome research. Methods Mol. Biol. 2010, 605, 1–27. [Google Scholar] [PubMed]
- Akbarzadeh, A.; Rezaei-Sadabady, R.; Davaran, S.; Joo, S.W.; Zarghami, N.; Hanifehpour, Y.; Samiei, M.; Kouhi, M.; Nejati-Koshki, K. Liposome: Classification, preparation, and applications. Nanoscale Res. Lett. 2013, 8, 102. [Google Scholar] [CrossRef] [PubMed]
- Malam, Y.; Loizidou, M.; Seifalian, A.M. Liposomes and nanoparticles: Nanosized vehicles for drug delivery in cancer. Trends Pharmacol. Sci. 2009, 30, 592–599. [Google Scholar] [CrossRef] [PubMed]
- Sercombe, L.; Veerati, T.; Moheimani, F.; Wu, S.Y.; Sood, A.K.; Hua, S. Advances and challenges of liposome assisted drug delivery. Front. Pharmacol. 2015, 6, 286. [Google Scholar] [CrossRef] [PubMed]
- Medina, O.; Zhu, Y.; Kairemo, K. Targeted liposomal drug delivery in cancer. Curr. Pharm. Des. 2004, 10, 2981–2989. [Google Scholar] [CrossRef] [PubMed]
- Torchilin, V. Recent advances with liposomes as pharmaceutical carriers. Nat. Rev. Drug Discov. 2005, 4, 145–160. [Google Scholar] [CrossRef] [PubMed]
- Harrington, K.J.; Rowlinson Busza, G.; Syrigos, K.N.; Uster, P.S.; Abra, R.M.; Stewart, J.S. Biodistribution and pharmacokinetics of 111In-DTPA-labelled pegylated liposomes in a human tumour xenograft model: Implications for novel targeting strategies. Br. J. Cancer 2000, 83, 232–238. [Google Scholar] [CrossRef] [PubMed]
- Yang, T.; Choi, M.-K.; Cui, F.-D.; Kim, J.; Chung, S.-J.; Shim, C.-K.; Kim, D.-D. Preparation and evaluation of paclitaxel-loaded pegylated immunoliposome. J. Control. Release 2007, 120, 169–177. [Google Scholar] [CrossRef] [PubMed]
- Klibanov, A.L.; Maruyama, K.; Torchilin, V.P.; Huang, L. Amphipathic polyethyleneglycols effectively prolong the circulation time of liposomes. FEBS Lett. 1990, 268, 235–237. [Google Scholar] [CrossRef]
- Klibanov, A.L.; Maruyama, K.; Beckerleg, A.M.; Torchilin, V.P.; Huang, L. Activity of amphipathic poly(ethylene glycol) 5000 to prolong the circulation time of liposomes depends on the liposome size and is unfavorable for immunoliposome binding to target. Biochim. Biophys. Acta 1991, 1062, 142–148. [Google Scholar] [CrossRef]
- Chow, T.-H.; Lin, Y.-Y.; Hwang, J.-J.; Wang, H.-E.; Tseng, Y.-L.; Pang, V.; Liu, R.-S.; Lin, W.-J.; Yang, C.-S.; Ting, G. Therapeutic efficacy evaluation of 111In-labeled pegylated liposomal vinorelbine in murine colon carcinoma with multimodalities of molecular imaging. J. Nucl. Med. 2009, 50, 2073–2081. [Google Scholar] [CrossRef] [PubMed]
- Immordino, M.L.; Dosio, F.; Cattel, L. Stealth liposomes: Review of the basic science, rationale, and clinical applications, existing and potential. Int. J. Nanomed. 2006, 1, 297–315. [Google Scholar]
- Soundararajan, A.; Dodd, G.; Bao, A.; Phillips, W.; McManus, L.; Prihoda, T.; Goins, B. Chemoradionuclide therapy with 186Re-labeled liposomal doxorubicin in combination with radiofrequency ablation for effective treatment of head and neck cancer in a nude rat tumor xenograft model. Radiology 2011, 261, 813–823. [Google Scholar] [CrossRef] [PubMed]
- Tseng, W.-C.; Huang, L. Liposome-based gene therapy. Pharm. Sci. Technol. Today 1998, 1, 206–213. [Google Scholar] [CrossRef]
- Allen, T.M.; Cullis, P.R. Liposomal drug delivery systems: From concept to clinical applications. Adv. Drug Deliv. Rev. 2013, 65, 36–48. [Google Scholar] [CrossRef] [PubMed]
- Fahr, A.; van Hoogevest, P.; May, S.; Bergstrand, N.; ML, S.L. Transfer of lipophilic drugs between liposomal membranes and biological interfaces: Consequences for drug delivery. Eur. J. Pharm. Sci. 2005, 26, 251–265. [Google Scholar] [CrossRef] [PubMed]
- Samad, A.; Sultana, Y.; Aqil, M. Liposomal drug delivery systems: An update review. Curr. Drug Deliv. 2007, 4, 297–305. [Google Scholar] [CrossRef] [PubMed]
- Madeira, C.; Mendes, R.D.; Ribeiro, S.C.; Boura, J.S.; Aires-Barros, M.R.; da Silva, C.L.; Cabral, J.M. Nonviral gene delivery to mesenchymal stem cells using cationic liposomes for gene and cell therapy. J. Biomed. Biotechnol. 2010, 2010, 735349. [Google Scholar] [CrossRef] [PubMed]
- Park, J.W. Liposome-based drug delivery in breast cancer treatment. Breast Cancer Res. 2002, 4, 95–99. [Google Scholar] [CrossRef] [PubMed]
- Koshkina, N.V.; Gilbert, B.E.; Waldrep, J.C.; Seryshev, A.; Knight, V. Distribution of camptothecin after delivery as a liposome aerosol or following intramuscular injection in mice. Cancer Chemother. Pharmacol. 1999, 44, 187–192. [Google Scholar] [CrossRef] [PubMed]
- Rogers, J.A.; Anderson, K.E. The potential of liposomes in oral drug delivery. Crit. Rev. Ther. Drug Carrier Syst. 1998, 15, 421–480. [Google Scholar] [CrossRef] [PubMed]
- Torchilin, V.P. Multifunctional, stimuli-sensitive nanoparticulate systems for drug delivery. Nat. Rev. Drug Discov. 2014, 13, 813–827. [Google Scholar] [CrossRef] [PubMed]
- Bulbake, U.; Doppalapudi, S.; Kommineni, N.; Khan, W. Liposomal formulations in clinical use: An updated review. Pharmaceutics 2017, 9, 12. [Google Scholar] [CrossRef] [PubMed]
- Barenholz, Y. Doxil®—The first fda-approved nano-drug: Lessons learned. J. Control. Release 2012, 160, 117–134. [Google Scholar] [CrossRef] [PubMed]
- Lasic, D.D.; Frederik, P.M.; Stuart, M.C.; Barenholz, Y.; McIntosh, T.J. Gelation of liposome interior. A novel method for drug encapsulation. FEBS Lett. 1992, 312, 255–258. [Google Scholar] [CrossRef]
- Haran, G.; Cohen, R.; Bar, L.K.; Barenholz, Y. Transmembrane ammonium sulfate gradients in liposomes produce efficient and stable entrapment of amphipathic weak bases. Biochim. Biophys. Acta 1993, 1151, 201–215. [Google Scholar] [CrossRef]
- Ohanian, M.; Kantarjian, H.M.; Ravandi, F.; Borthakur, G.; Garcia-Manero, G.; Andreeff, M.; Jabbour, E.; Konopleva, M.; Lim, M.; Pierce, S.; et al. Safety, pharmacokinetics, and efficacy of BP-100-1.01 (liposomal Grb-2 antisense oligonucleotide) in patients with refractory or relapsed acute myeloid leukemia (AML), philadelphia chromosome positive chronic myelogenous leukemia (CML), acute lymphoblastic leukemia (ALL), and myelodysplastic syndrome (MDS). Blood 2015, 126, 3801. [Google Scholar]
- Harper, B.W.; Krause-Heuer, A.M.; Grant, M.P.; Manohar, M.; Garbutcheon-Singh, K.B.; Aldrich-Wright, J.R. Advances in platinum chemotherapeutics. Chemistry 2010, 16, 7064–7077. [Google Scholar] [CrossRef] [PubMed]
- Clancy, J.P.; Dupont, L.; Konstan, M.W.; Billings, J.; Fustik, S.; Goss, C.H.; Lymp, J.; Minic, P.; Quittner, A.L.; Rubenstein, R.C.; et al. Phase II studies of nebulised arikace in cf patients with pseudomonas aeruginosa infection. Thorax 2013, 68, 818–825. [Google Scholar] [CrossRef] [PubMed]
- Semple, S.C.; Leone, R.; Wang, J.; Leng, E.C.; Klimuk, S.K.; Eisenhardt, M.L.; Yuan, Z.N.; Edwards, K.; Maurer, N.; Hope, M.J.; et al. Optimization and characterization of a sphingomyelin/cholesterol liposome formulation of vinorelbine with promising antitumor activity. J. Pharm. Sci. 2005, 94, 1024–1038. [Google Scholar] [CrossRef] [PubMed]
- Slingerland, M.; Guchelaar, H.J.; Rosing, H.; Scheulen, M.E.; van Warmerdam, L.J.; Beijnen, J.H.; Gelderblom, H. Bioequivalence of liposome-entrapped paclitaxel easy-to-use (LEP-ETU) formulation and paclitaxel in polyethoxylated castor oil: A randomized, two-period crossover study in patients with advanced cancer. Clin. Ther. 2013, 35, 1946–1954. [Google Scholar] [CrossRef] [PubMed]
- Boulikas, T. Clinical overview on lipoplatin: A successful liposomal formulation of cisplatin. Expert Opin. Investig. Drugs 2009, 18, 1197–1218. [Google Scholar] [CrossRef] [PubMed]
- Seiden, M.V.; Muggia, F.; Astrow, A.; Matulonis, U.; Campos, S.; Roche, M.; Sivret, J.; Rusk, J.; Barrett, E. A Phase II study of liposomal lurtotecan (OSI-211) in patients with topotecan resistant ovarian cancer. Gynecol. Oncol. 2004, 93, 229–232. [Google Scholar] [CrossRef] [PubMed]
- Prostaglandin E1 (liprostin) Treatment with Lower Limb Angioplasty for Peripheral Arterial Occlusive disease. Available online: https://clinicaltrials.gov/ct2/show/NCT00053716 (accessed on 2 October 2017).
- De Jonge, M.J.; Slingerland, M.; Loos, W.J.; Wiemer, E.A.; Burger, H.; Mathijssen, R.H.; Kroep, J.R.; den Hollander, M.A.; van der Biessen, D.; Lam, M.H.; et al. Early cessation of the clinical development of liplacis, a liposomal cisplatin formulation. Eur. J. Cancer 2010, 46, 3016–3021. [Google Scholar] [CrossRef] [PubMed]
- Wetzler, M.; Thomas, D.A.; Wang, E.S.; Shepard, R.; Ford, L.A.; Heffner, T.L.; Parekh, S.; Andreeff, M.; O’Brien, S.; Kantarjian, H.M. Phase I/II trial of nanomolecular liposomal annamycin in adult patients with relapsed/refractory acute lymphoblastic leukemia. Clin. Lymphoma Myeloma Leuk. 2013, 13, 430–434. [Google Scholar] [CrossRef] [PubMed]
- Kroemer, G.; Zitvogel, L.; Galluzzi, L. Victories and deceptions in tumor immunology: Stimuvax®. Oncoimmunology 2013, 2, e23687. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.; Ramanathan, R.K.; Zamboni, B.A.; Strychor, S.; Ramalingam, S.; Edwards, R.P.; Friedland, D.M.; Stoller, R.G.; Belani, C.P.; Maruca, L.J.; et al. Population pharmacokinetics of pegylated liposomal CKD-602 (S-CKD602) in patients with advanced malignancies. J. Clin. Pharmacol. 2012, 52, 180–194. [Google Scholar] [CrossRef] [PubMed]
- Wolf, P.; Müllegger, R.R.; Peter Soyer, H.; Hofer, A.; Smolle, J.; Horn, M.; Cerroni, L.; Hofmann-Wellenhof, R.; Kerl, H.; Maier, H.; et al. Topical treatment with liposomes containing T4 endonuclease V protects human skin in vivo from ultraviolet-induced upregulation of interleukin-10 and tumor necrosis factor-α. J. Investig. Dermatol. 2000, 114, 149–156. [Google Scholar] [CrossRef] [PubMed]
- Rose, P.G.; Smrekar, M.; Haba, P.; Fusco, N.; Rodriguez, M. A phase I study of oral topotecan and pegylated liposomal doxorubicin (Doxil) in platinum-resistant ovarian and peritoneal cancer. Am. J. Clin. Oncol. 2008, 31, 476–480. [Google Scholar] [CrossRef] [PubMed]
- Harrington, K.J.; Lewanski, C.R.; Northcote, A.D.; Whittaker, J.; Wellbank, H.; Vile, R.G.; Peters, A.M.; Stewart, J.S. Phase I-II study of pegylated liposomal cisplatin (SPI-077) in patients with inoperable head and neck cancer. Ann. Oncol. 2001, 12, 493–496. [Google Scholar] [CrossRef] [PubMed]
- Phase 3 Study of Thermodox with Radiofrequency Ablation (RFA) in Treatment of Hepatocellular Carcinoma (HCC). Available online: https://clinicaltrials.gov/ct2/show/NCT00617981 (accessed on 2 October 2017).
- Wang, R.; Billone, P.S.; Mullett, W.M. Nanomedicine in action: An overview of cancer nanomedicine on the market and in clinical trials. J. Nanomater. 2013, 2013, 12. [Google Scholar] [CrossRef]
- Strieth, S.; Dunau, C.; Kolbow, K.; Knuechel, R.; Michaelis, U.; Ledderose, H.; Eichhorn, M.E.; Strelczyk, D.; Tschiesner, U.; Wollenberg, B.; et al. Phase I clinical study of vascular targeting fluorescent cationic liposomes in head and neck cancer. Eur. Arch. Otorhinolaryngol. 2013, 270, 1481–1487. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, S.; Date, A.; Patravale, V.; Korting, H.C.; Roeder, A.; Weindl, G. Retinoids in the treatment of skin aging: An overview of clinical efficacy and safety. Clin. Interv. Aging 2006, 1, 327–348. [Google Scholar] [CrossRef] [PubMed]
- Kanasty, R.; Dorkin, J.R.; Vegas, A.; Anderson, D. Delivery materials for sirna therapeutics. Nat. Mater. 2013, 12, 967–977. [Google Scholar] [CrossRef] [PubMed]
- Chan, S.; Davidson, N.; Juozaityte, E.; Erdkamp, F.; Pluzanska, A.; Azarnia, N.; Lee, L.W. Phase III trial of liposomal doxorubicin and cyclophosphamide compared with epirubicin and cyclophosphamide as first-line therapy for metastatic breast cancer. Ann. Oncol. 2004, 15, 1527–1534. [Google Scholar] [CrossRef] [PubMed]
- Ma, M.K.; Zamboni, W.C.; Radomski, K.M.; Furman, W.L.; Santana, V.M.; Houghton, P.J.; Hanna, S.K.; Smith, A.K.; Stewart, C.F. Pharmacokinetics of irinotecan and its metabolites SN-38 and APC in children with recurrent solid tumors after protracted low-dose irinotecan. Clin. Cancer Res. 2000, 6, 813–819. [Google Scholar] [PubMed]
- Eichhorn, M.E.; Ischenko, I.; Luedemann, S.; Strieth, S.; Papyan, A.; Werner, A.; Bohnenkamp, H.; Guenzi, E.; Preissler, G.; Michaelis, U.; et al. Vascular targeting by endotag-1 enhances therapeutic efficacy of conventional chemotherapy in lung and pancreatic cancer. Int. J. Cancer 2010, 126, 1235–1245. [Google Scholar] [CrossRef] [PubMed]
- Zhigaltsev, I.V.; Maurer, N.; Akhong, Q.F.; Leone, R.; Leng, E.; Wang, J.; Semple, S.C.; Cullis, P.R. Liposome-encapsulated vincristine, vinblastine and vinorelbine: A comparative study of drug loading and retention. J. Control. Release 2005, 104, 103–111. [Google Scholar] [CrossRef] [PubMed]
- Absalon, M.; O’Brien, M.M.; Phillips, C.L.; Burns, K.C.; Mangino, J.; Mizukawa, B.; Breese, E.H.; Shah, R.; Perentesis, J.P. A Phase I/pilot study of CPX-351 for children, adolescents and young adults with recurrent or refractory hematologic malignancies. J. Clin. Oncol. 2016, 34, 10541. [Google Scholar]
- Ashizawa, A.T.; Cortes, J. Liposomal delivery of nucleic acid-based anticancer therapeutics: BP-100-1.01. Expert Opin. Drug Deliv. 2015, 12, 1107–1120. [Google Scholar] [CrossRef] [PubMed]
- Tari, A.M.; Gutierrez-Puente, Y.; Monaco, G.; Stephens, C.; Sun, T.; Rosenblum, M.; Belmont, J.; Arlinghaus, R.; Lopez-Berestein, G. Liposome-incorporated Grb2 antisense oligodeoxynucleotide increases the survival of mice bearing bcr-abl-positive leukemia xenografts. Int. J. Oncol. 2007, 31, 1243–1250. [Google Scholar] [PubMed]
- Wicki, A.; Witzigmann, D.; Balasubramanian, V.; Huwyler, J. Nanomedicine in cancer therapy: Challenges, opportunities, and clinical applications. J. Control. Release 2015, 200, 138–157. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, A.; Wang, Y.F.; Ahmad, I. Separation of liposome-entrapped mitoxantrone from nonliposomal mitoxantrone in plasma: Pharmacokinetics in mice. Methods Enzymol. 2005, 391, 176–185. [Google Scholar] [PubMed]
- Farrell, N.P. Platinum formulations as anticancer drugs clinical and pre-clinical studies. Curr. Top. Med. Chem. 2011, 11, 2623–2631. [Google Scholar] [CrossRef]
- Jakupec, M.A.; Galanski, M.; Keppler, B.K. Tumour-inhibiting platinum complexes—State of the art and future perspectives. Rev. Physiol. Biochem. Pharmacol. 2003, 146, 1–54. [Google Scholar] [PubMed]
- Chang, H.I.; Yeh, M.K. Clinical development of liposome-based drugs: Formulation, characterization, and therapeutic efficacy. Int. J. Nanomed. 2012, 7, 49–60. [Google Scholar]
- Tomkinson, B.; Bendele, R.; Giles, F.J.; Brown, E.; Gray, A.; Hart, K.; LeRay, J.D.; Meyer, D.; Pelanne, M.; Emerson, D.L. OSI-211, a novel liposomal topoisomerase I inhibitor, is active in scid mouse models of human aml and all. Leuk. Res. 2003, 27, 1039–1050. [Google Scholar] [CrossRef]
- Seetharamu, N.; Kim, E.; Hochster, H.; Martin, F.; Muggia, F. Phase II study of liposomal cisplatin (SPI-77) in platinum-sensitive recurrences of ovarian cancer. Anticancer Res. 2010, 30, 541–545. [Google Scholar] [PubMed]
- Meerum Terwogt, J.M.; Groenewegen, G.; Pluim, D.; Maliepaard, M.; Tibben, M.M.; Huisman, A.; ten Bokkel Huinink, W.W.; Schot, M.; Welbank, H.; Voest, E.E.; et al. Phase i and pharmacokinetic study of spi-77, a liposomal encapsulated dosage form of cisplatin. Cancer Chemother. Pharmacol. 2002, 49, 201–210. [Google Scholar] [CrossRef] [PubMed]
- Kim, E.S.; Lu, C.; Khuri, F.R.; Tonda, M.; Glisson, B.S.; Liu, D.; Jung, M.; Hong, W.K.; Herbst, R.S. A phase II study of stealth cisplatin (SPI-77) in patients with advanced non-small cell lung cancer. Lung Cancer 2001, 34, 427–432. [Google Scholar] [CrossRef]
- Colvin, O.M. An overview of cyclophosphamide development and clinical applications. Curr. Pharm. Des. 1999, 5, 555–560. [Google Scholar] [PubMed]
- Thomson, A.B.; Critchley, H.O.; Kelnar, C.J.; Wallace, W.H. Late reproductive sequelae following treatment of childhood cancer and options for fertility preservation. Best Pract. Res. Clin. Endocrinol. Metab. 2002, 16, 311–334. [Google Scholar] [CrossRef] [PubMed]
- Tripathi, D.N.; Jena, G.B. Astaxanthin inhibits cytotoxic and genotoxic effects of cyclophosphamide in mice germ cells. Toxicology 2008, 248, 96–103. [Google Scholar] [CrossRef] [PubMed]
- Papagiannaros, A.; Hatziantoniou, S.; Lelong-Rebel, I.H.; Papaioannou, G.T.; Dimas, K.; Demetzos, C. Antitumor activity of doxorubicin encapsulated in hexadecylphosphocholine (HePC) liposomes against human xenografts on scid mice. In Vivo 2006, 20, 129–135. [Google Scholar] [PubMed]
- Arif, K.; Ejaj, A.; Maroof, A.; Azmat, A.K.; Arun, C.; Fatima, N.; Gatoo, M.A.; Owais, M. Protective effect of liposomal formulation of tuftsin (a naturally occurring tetrapeptide) against cyclophosphamide-induced genotoxicity and oxidative stress in mice. Indian J. Biochem. Biophys. 2009, 46, 45–52. [Google Scholar] [PubMed]
- Abdella, E.M. Short-term comparative study of the cyclophosphamide genotoxicity administered free and liposome-encapsulated in mice. Iran. J. Cancer Prev. 2012, 5, 51–60. [Google Scholar] [PubMed]
- Wurz, G.T.; Kao, C.J.; Wolf, M.; DeGregorio, M.W. Tecemotide: An antigen-specific cancer immunotherapy. Hum. Vaccines Immunother. 2014, 10, 3383–3393. [Google Scholar] [CrossRef] [PubMed]
- Bradbury, P.A.; Shepherd, F.A. Immunotherapy for lung cancer. J. Thorac. Oncol. 2008, 3, S164–S170. [Google Scholar] [CrossRef] [PubMed]
- Stathopoulos, G.P.; Boulikas, T.; Vougiouka, M.; Deliconstantinos, G.; Rigatos, S.; Darli, E.; Viliotou, V.; Stathopoulos, J.G. Pharmacokinetics and adverse reactions of a new liposomal cisplatin (Lipoplatin): Phase I study. Oncol. Rep. 2005, 13, 589–595. [Google Scholar] [CrossRef] [PubMed]
- Boulikas, T.; Stathopoulos, G.P.; Volakakis, N.; Vougiouka, M. Systemic lipoplatin infusion results in preferential tumor uptake in human studies. Anticancer Res. 2005, 25, 3031–3039. [Google Scholar] [PubMed]
- Van der Geest, T.; Laverman, P.; Metselaar, J.M.; Storm, G.; Boerman, O.C. Radionuclide imaging of liposomal drug delivery. Expert Opin. Drug Deliv. 2016, 13, 1231–1242. [Google Scholar] [CrossRef] [PubMed]
- Xing, Y.; Zhao, J.; Conti, P.S.; Chen, K. Radiolabeled nanoparticles for multimodality tumor imaging. Theranostics 2014, 4, 290–306. [Google Scholar] [CrossRef] [PubMed]
- Seo, J.W.; Mahakian, L.M.; Tam, S.; Qin, S.; Ingham, E.S.; Meares, C.F.; Ferrara, K.W. The pharmacokinetics of Zr-89 labeled liposomes over extended periods in a murine tumor model. Nucl. Med. Biol. 2015, 42, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Mitra, A.; Nan, A.; Line, B.R.; Ghandehari, H. Nanocarriers for nuclear imaging and radiotherapy of cancer. Curr. Pharm. Des. 2006, 12, 4729–4749. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.; Zheng, J.; Gaddy, D.; Orcutt, K.D.; Leonard, S.; Geretti, E.; Hesterman, J.; Harwell, C.; Hoppin, J.; Jaffray, D.A.; et al. A gradient-loadable (64)Cu-chelator for quantifying tumor deposition kinetics of nanoliposomal therapeutics by positron emission tomography. Nanomedicine 2015, 11, 155–165. [Google Scholar] [CrossRef] [PubMed]
- Oku, N.; Yamashita, M.; Katayama, Y.; Urakami, T.; Hatanaka, K.; Shimizu, K.; Asai, T.; Tsukada, H.; Akai, S.; Kanazawa, H. Pet imaging of brain cancer with positron emitter-labeled liposomes. Int. J. Pharm. 2011, 403, 170–177. [Google Scholar] [CrossRef] [PubMed]
- Petersen, A.L.; Binderup, T.; Rasmussen, P.; Henriksen, J.R.; Elema, D.R.; Kjaer, A.; Andresen, T.L. 64Cu loaded liposomes as positron emission tomography imaging agents. Biomaterials 2011, 32, 2334–2341. [Google Scholar] [CrossRef] [PubMed]
- Zalutsky, M.R.; Noska, M.A.; Seltzer, S.E. Characterization of liposomes containing iodine-125-labeled radiographic contrast agents. Investig. Radiol. 1987, 22, 141–147. [Google Scholar] [CrossRef]
- Li, N.; Yu, Z.; Pham, T.T.; Blower, P.J.; Yan, R. A generic 89zr labeling method to quantify the in vivo pharmacokinetics of liposomal nanoparticles with positron emission tomography. Int. J. Nanomed. 2017, 12, 3281–3294. [Google Scholar] [CrossRef] [PubMed]
- Silindir, M.; Ozer, A.Y.; Erdogan, S. The use and importance of liposomes in positron emission tomography. Drug Deliv. 2012, 19, 68–80. [Google Scholar] [CrossRef] [PubMed]
- Wong, A.W.; Ormsby, E.; Zhang, H.; Seo, J.W.; Mahakian, L.M.; Caskey, C.F.; Ferrara, K.W. A comparison of image contrast with (64)Cu-labeled long circulating liposomes and (18)F-FDG in a murine model of mammary carcinoma. Am. J. Nucl. Med. Mol. Imaging 2013, 3, 32–43. [Google Scholar] [PubMed]
- Seo, J.W.; Qin, S.; Mahakian, L.M.; Watson, K.D.; Kheirolomoom, A.; Ferrara, K.W. Positron emission tomography imaging of the stability of Cu-64 labeled dipalmitoyl and distearoyl lipids in liposomes. J. Control. Release 2011, 151, 28–34. [Google Scholar] [CrossRef] [PubMed]
- Perez-Medina, C.; Abdel-Atti, D.; Zhang, Y.; Longo, V.A.; Irwin, C.P.; Binderup, T.; Ruiz-Cabello, J.; Fayad, Z.A.; Lewis, J.S.; Mulder, W.J.; et al. A modular labeling strategy for in vivo pet and near-infrared fluorescence imaging of nanoparticle tumor targeting. J. Nucl. Med. 2014, 55, 1706–1711. [Google Scholar] [CrossRef] [PubMed]
- Marik, J.; Tartis, M.S.; Zhang, H.; Fung, J.Y.; Kheirolomoom, A.; Sutcliffe, J.L.; Ferrara, K.W. Long-circulating liposomes radiolabeled with [18F]fluorodipalmitin ([18F]FDP). Nucl. Med. Biol. 2007, 34, 165–171. [Google Scholar] [CrossRef] [PubMed]
- Hansen, A.E.; Petersen, A.L.; Henriksen, J.R.; Boerresen, B.; Rasmussen, P.; Elema, D.R.; af Rosenschold, P.M.; Kristensen, A.T.; Kjaer, A.; Andresen, T.L. Positron emission tomography based elucidation of the enhanced permeability and retention effect in dogs with cancer using copper-64 liposomes. ACS Nano 2015, 9, 6985–6995. [Google Scholar] [CrossRef] [PubMed]
- Luo, D.; Goel, S.; Liu, H.J.; Carter, K.A.; Jiang, D.; Geng, J.; Kutyreff, C.J.; Engle, J.W.; Huang, W.C.; Shao, S.; et al. Intrabilayer (64)Cu labeling of photoactivatable, doxorubicin-loaded stealth liposomes. ACS Nano 2017, 11, 12482–12491. [Google Scholar] [CrossRef] [PubMed]
- Jensen, A.I.; Severin, G.W.; Hansen, A.E.; Fliedner, F.P.; Eliasen, R.; Parhamifar, L.; Kjaer, A.; Andresen, T.L.; Henriksen, J.R. Remote-loading of liposomes with manganese-52 and in vivo evaluation of the stabilities of 52MN-DOTA and 64Cu-DOTA using radiolabelled liposomes and pet imaging. J. Control. Release 2017, 269, 100–109. [Google Scholar] [CrossRef] [PubMed]
- Espinola, L.G.; Beaucaire, J.; Gottschalk, A.; Caride, V.J. Radiolabeled liposomes as metabolic and scanning tracers in mice. II. In-111 oxine compared with Tc-99m DTPA, entrapped in multilamellar lipid vesicles. J. Nucl. Med. 1979, 20, 434–440. [Google Scholar] [PubMed]
- Ogihara, I.; Kojima, S.; Jay, M. Differential uptake of gallium-67-labeled liposomes between tumors and inflammatory lesions in rats. J. Nucl. Med. 1986, 27, 1300–1307. [Google Scholar] [PubMed]
- Ogihara-Umeda, I.; Kojima, S. Increased delivery of gallium-67 to tumors using serum-stable liposomes. J. Nucl. Med. 1988, 29, 516–523. [Google Scholar] [PubMed]
- Ogihara-Umeda, I.; Kojima, S. Cholesterol enhances the delivery of liposome-encapsulated gallium-67 to tumors. Eur. J. Nucl. Med. 1989, 15, 612–617. [Google Scholar] [CrossRef] [PubMed]
- Ogihara-Umeda, I.; Sasaki, T.; Kojima, S.; Nishigori, H. Optimal radiolabeled liposomes for tumor imaging. J. Nucl. Med. 1996, 37, 326–332. [Google Scholar] [PubMed]
- Proffitt, R.T.; Williams, L.E.; Presant, C.A.; Tin, G.W.; Uliana, J.A.; Gamble, R.C.; Baldeschwieler, J.D. Tumor-imaging potential of liposomes loaded with In-111-NTA: Biodistribution in mice. J. Nucl. Med. 1983, 24, 45–51. [Google Scholar] [PubMed]
- Turner, A.F.; Presant, C.A.; Proffitt, R.T.; Williams, L.E.; Winsor, D.W.; Werner, J.L. In-111-labeled liposomes: Dosimetry and tumor depiction. Radiology 1988, 166, 761–765. [Google Scholar] [CrossRef] [PubMed]
- Kubo, A.; Nakamura, K.; Sammiya, T.; Katayama, M.; Hashimoto, T.; Hashimoto, S.; Kobayashi, H.; Teramoto, T. Indium-111-labelled liposomes: Dosimetry and tumour detection in patients with cancer. Eur. J. Nucl. Med. 1993, 20, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Oyen, W.J.; Boerman, O.C.; Storm, G.; van Bloois, L.; Koenders, E.B.; Claessens, R.A.; Perenboom, R.M.; Crommelin, D.J.; van der Meer, J.W.; Corstens, F.H. Detecting infection and inflammation with technetium-99m-labeled stealth liposomes. J. Nucl. Med. 1996, 37, 1392–1397. [Google Scholar] [PubMed]
- Boerman, O.C.; Storm, G.; Oyen, W.J.; van Bloois, L.; van der Meer, J.W.; Claessens, R.A.; Crommelin, D.J.; Corstens, F.H. Sterically stabilized liposomes labeled with indium-111 to image focal infection. J. Nucl. Med. 1995, 36, 1639–1644. [Google Scholar] [PubMed]
- Harrington, K.J.; Mohammadtaghi, S.; Uster, P.S.; Glass, D.; Peters, A.M.; Vile, R.G.; Stewart, J.S. Effective targeting of solid tumors in patients with locally advanced cancers by radiolabeled pegylated liposomes. Clin. Cancer Res. 2001, 7, 243–254. [Google Scholar] [PubMed]
- Basu, S.; Zhuang, H.; Torigian, D.A.; Rosenbaum, J.; Chen, W.; Alavi, A. Functional imaging of inflammatory diseases using nuclear medicine techniques. Semin. Nucl. Med. 2009, 39, 124–145. [Google Scholar] [CrossRef] [PubMed]
- Huang, F.Y.; Lee, T.W.; Kao, C.H.; Chang, C.H.; Zhang, X.; Lee, W.Y.; Chen, W.J.; Wang, S.C.; Lo, J.M. Imaging, autoradiography, and biodistribution of (188)Re-labeled pegylated nanoliposome in orthotopic glioma bearing rat model. Cancer Biother. Radiopharm. 2011, 26, 717–725. [Google Scholar] [CrossRef] [PubMed]
- De Vries, A.; Kok, M.B.; Sanders, H.M.; Nicolay, K.; Strijkers, G.J.; Grull, H. Multimodal liposomes for spect/mr imaging as a tool for in situ relaxivity measurements. Contrast Media Mol. Imaging 2012, 7, 68–75. [Google Scholar] [CrossRef] [PubMed]
- Ogawa, M.; Umeda, I.O.; Kosugi, M.; Kawai, A.; Hamaya, Y.; Takashima, M.; Yin, H.; Kudoh, T.; Seno, M.; Magata, Y. Development of 111in-labeled liposomes for vulnerable atherosclerotic plaque imaging. J. Nucl. Med. 2014, 55, 115–120. [Google Scholar] [CrossRef] [PubMed]
- Ito, K.; Hamamichi, S.; Asano, M.; Hori, Y.; Matsui, J.; Iwata, M.; Funahashi, Y.; Umeda, I.O.; Fujii, H. Radiolabeled liposome imaging determines an indication for liposomal anticancer agent in ovarian cancer mouse xenograft models. Cancer Sci. 2016, 107, 60–67. [Google Scholar] [CrossRef] [PubMed]
- Varga, Z.; Szigyarto, I.C.; Gyurko, I.; Doczi, R.; Horvath, I.; Mathe, D.; Szigeti, K. Radiolabeling and quantitative in vivo SPECT/CT imaging study of liposomes using the novel iminothiolane-99mTc-tricarbonyl complex. Contrast Media Mol. Imaging 2017, 2017, 4693417. [Google Scholar] [CrossRef] [PubMed]
- Awasthi, V.D.; Goins, B.; Klipper, R.; Phillips, W.T. Dual radiolabeled liposomes: Biodistribution studies and localization of focal sites of infection in rats. Nucl. Med. Biol. 1998, 25, 155–160. [Google Scholar] [CrossRef]
- Mougin-Degraef, M.; Bourdeau, C.; Jestin, E.; Sai-Maurel, C.; Bourgeois, M.; Saec, P.R.; Thedrez, P.; Gestin, J.F.; Barbet, J.; Faivre-Chauvet, A. Doubly radiolabeled liposomes for pretargeted radioimmunotherapy. Int. J. Pharm. 2007, 344, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Lamichhane, N.; Dewkar, G.K.; Sundaresan, G.; Mahon, R.N.; Zweit, J. [18F]-fluorinated carboplatin and [111In]-liposome for image-guided drug delivery. Int. J. Mol. Sci. 2017, 18, 1079. [Google Scholar] [CrossRef] [PubMed]
- Nakada, T. Clinical application of high and ultra high-field MRI. Brain Dev. 2007, 29, 325–335. [Google Scholar] [CrossRef] [PubMed]
- Langereis, S.; Geelen, T.; Grull, H.; Strijkers, G.J.; Nicolay, K. Paramagnetic liposomes for molecular MRI and MRI-guided drug delivery. NMR Biomed. 2013, 26, 728–744. [Google Scholar] [CrossRef] [PubMed]
- Ren, L.; Chen, S.; Li, H.; Zhang, Z.; Ye, C.; Liu, M.; Zhou, X. MRI-visible liposome nanovehicles for potential tumor-targeted delivery of multimodal therapies. Nanoscale 2015, 7, 12843–12850. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Gonzalez, R.; Estelrich, J.; Busquets, M.A. Liposomes loaded with hydrophobic iron oxide nanoparticles: Suitable T2 contrast agents for MRI. Int. J. Mol. Sci. 2016, 17, 1209. [Google Scholar] [CrossRef] [PubMed]
- Navon, G.; Panigel, R.; Valensin, G. Liposomes containing paramagnetic macromolecules as mri contrast agents. Magn. Reson. Med. 1986, 3, 876–880. [Google Scholar] [CrossRef] [PubMed]
- Ding, N.; Lu, Y.; Lee, R.J.; Yang, C.; Huang, L.; Liu, J.; Xiang, G. Folate receptor-targeted fluorescent paramagnetic bimodal liposomes for tumor imaging. Int. J. Nanomed. 2011, 6, 2513–2520. [Google Scholar] [CrossRef] [PubMed]
- De Smet, M.; Langereis, S.; van den Bosch, S.; Bitter, K.; Hijnen, N.M.; Heijman, E.; Grull, H. SPECT/CT imaging of temperature-sensitive liposomes for MR-image guided drug delivery with high intensity focused ultrasound. J. Control. Release 2013, 169, 82–90. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.R.; You, D.G.; Park, S.J.; Choi, K.S.; Um, W.; Kim, J.H.; Park, J.H.; Kim, Y.S. Mri monitoring of tumor-selective anticancer drug delivery with stable thermosensitive liposomes triggered by high-intensity focused ultrasound. Mol. Pharm. 2016, 13, 1528–1539. [Google Scholar] [CrossRef] [PubMed]
- Kneepkens, E.; Fernandes, A.; Nicolay, K.; Grull, H. Iron(III)-based magnetic resonance-imageable liposomal T1 contrast agent for monitoring temperature-induced image-guided drug delivery. Investig. Radiol. 2016, 51, 735–745. [Google Scholar] [CrossRef] [PubMed]
- Nordling-David, M.M.; Yaffe, R.; Guez, D.; Meirow, H.; Last, D.; Grad, E.; Salomon, S.; Sharabi, S.; Levi-Kalisman, Y.; Golomb, G.; et al. Liposomal temozolomide drug delivery using convection enhanced delivery. J. Control. Release 2017, 261, 138–146. [Google Scholar] [CrossRef] [PubMed]
- Shao, S.; Do, T.N.; Razi, A.; Chitgupi, U.; Geng, J.; Alsop, R.J.; Dzikovski, B.G.; Rheinstadter, M.C.; Ortega, J.; Karttunen, M.; et al. Design of hydrated porphyrin-phospholipid bilayers with enhanced magnetic resonance contrast. Small 2017, 13. [Google Scholar] [CrossRef] [PubMed]
Sample Availability: None. |
| Phase I | Phase II | Phase III | References | ||||
|---|---|---|---|---|---|---|---|
| Drug/Name | Agent/Target | Drug/Name | Agent/Target | Drug/Name | Agent/Target | ||
| 1 | BP1001 | Antisense protein/Grb-2 | Aroplatin | L-NDDP/Platinum | Arikace | Amikacin/Ribosomal inhibitor | [36,37,38] |
| 2 | INX-0125 | Sphingomyelin/cholesterol | LEP-ETU | Paclitaxel/microtubule | Lipoplatin | Cisplatin | [39,40,41] |
| 3 | INX-0076 | Topotecan Sphingosomes | OSI-211 | Lurtotecan/antineoplastic | Liprostin | PGE-I/Prostaglandin Receptor | [32,42,43] |
| 4 | LiPlaCis | Cisplatin/solid tumors | S-ANNA | Annamycin/TOPO II | Stimuvax | Tecemotide/Immunosuppressant | [44,45,46] |
| 5 | LEM-ETU | Mitoxantrone/TOPO II inhibitor | S-CKD602 | TOPO I inhibitor | TAN5 | T4 endonuclease V | [26,47,48] |
| 6 | SGT-53 | p-53 | SPI-077 | Cisplatin/ | Thermodox | Doxorubicin/antimitotic | [49,50,51] |
| 7 | LDF01 | Cationic liposomes/Microvessels | Tretnoin | Retinoids/Skin disease | MiR-122 | MicroRNA-122/HCV | [52,53,54] |
| 8 | Atu027 | siRNA/Solid tumors | Irinotecan SN-37 | Camptothecin/DNA damage | Cyclophosphamide | Nitrogen mustard/antineoplastic | [55,56,57] |
| 9 | Navelbine | Vinca alkaloid/Immunosuppressant | Taxol | Paclitaxel/microtubule | CPX-351 | Cytarabine:daunorubicin/DNA polymerase inhibitor | [58,59,60] |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lamichhane, N.; Udayakumar, T.S.; D’Souza, W.D.; Simone II, C.B.; Raghavan, S.R.; Polf, J.; Mahmood, J. Liposomes: Clinical Applications and Potential for Image-Guided Drug Delivery. Molecules 2018, 23, 288. https://doi.org/10.3390/molecules23020288
Lamichhane N, Udayakumar TS, D’Souza WD, Simone II CB, Raghavan SR, Polf J, Mahmood J. Liposomes: Clinical Applications and Potential for Image-Guided Drug Delivery. Molecules. 2018; 23(2):288. https://doi.org/10.3390/molecules23020288
Chicago/Turabian StyleLamichhane, Narottam, Thirupandiyur S. Udayakumar, Warren D. D’Souza, Charles B. Simone II, Srinivasa R. Raghavan, Jerimy Polf, and Javed Mahmood. 2018. "Liposomes: Clinical Applications and Potential for Image-Guided Drug Delivery" Molecules 23, no. 2: 288. https://doi.org/10.3390/molecules23020288
APA StyleLamichhane, N., Udayakumar, T. S., D’Souza, W. D., Simone II, C. B., Raghavan, S. R., Polf, J., & Mahmood, J. (2018). Liposomes: Clinical Applications and Potential for Image-Guided Drug Delivery. Molecules, 23(2), 288. https://doi.org/10.3390/molecules23020288





