Aloin Inhibits Müller Cells Swelling in a Rat Model of Thioacetamide-Induced Hepatic Retinopathy
Abstract
1. Introduction
2. Results
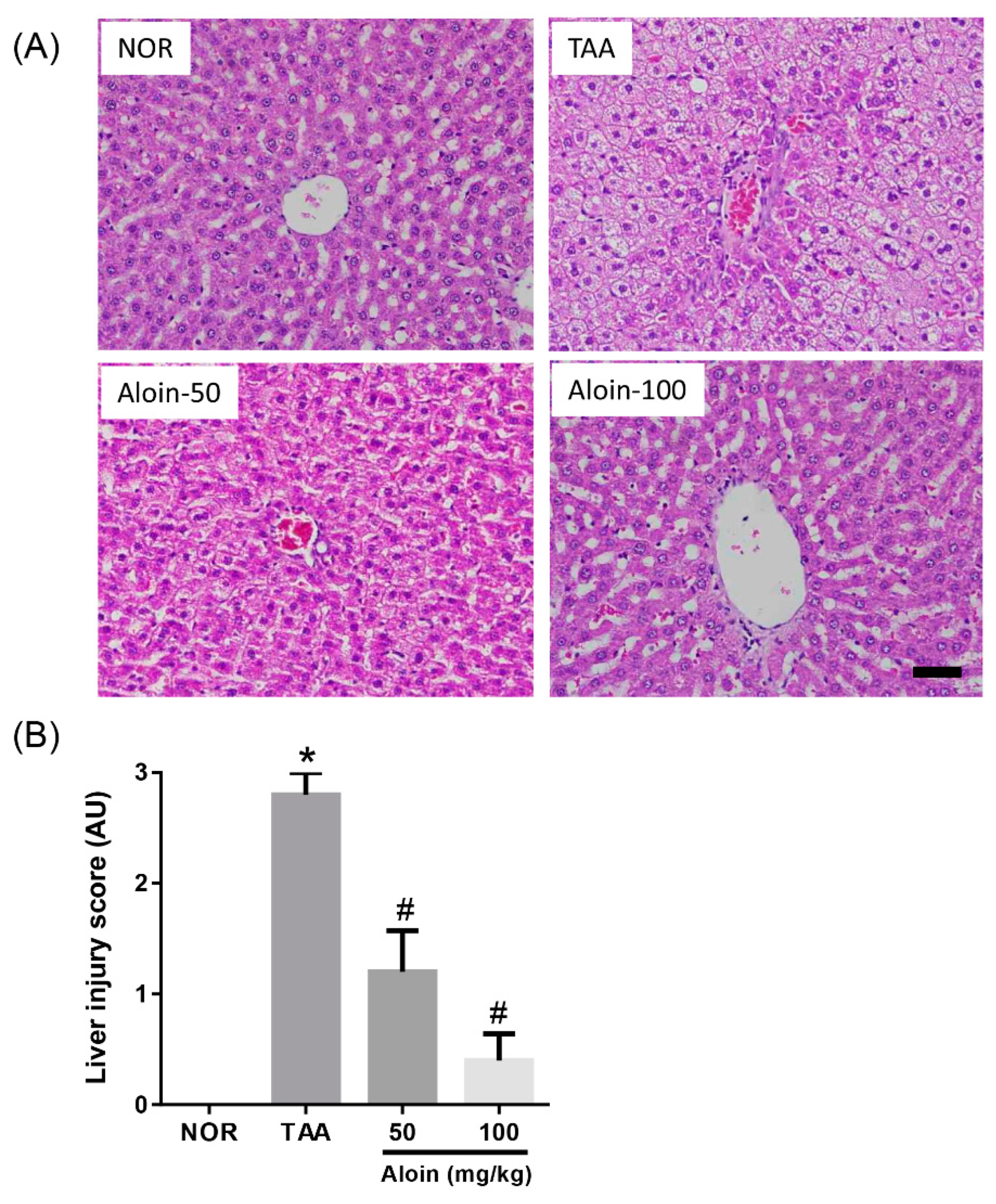
2.1. Histopathological Changes in Liver
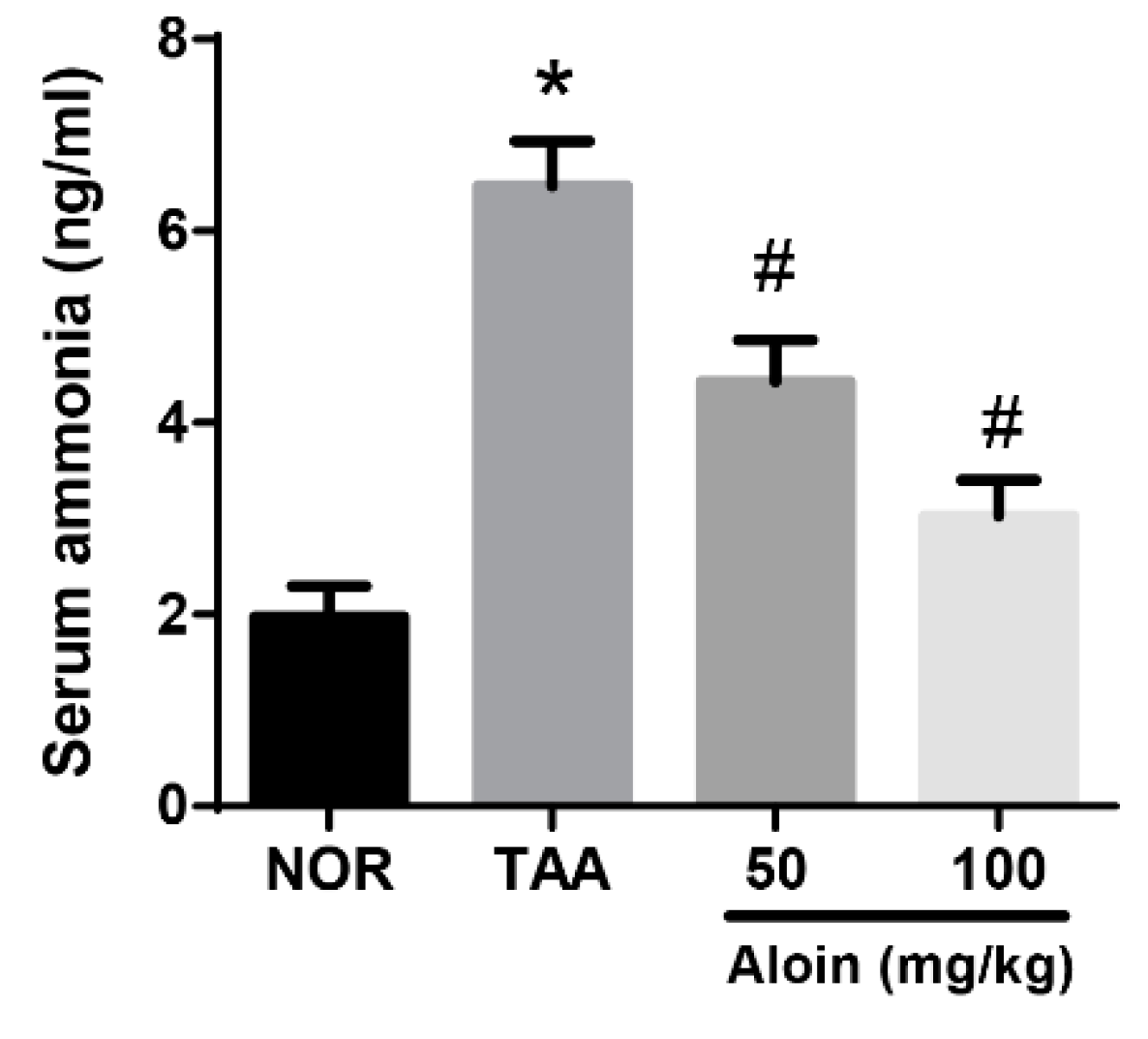
2.2. Serum Ammonia Levels
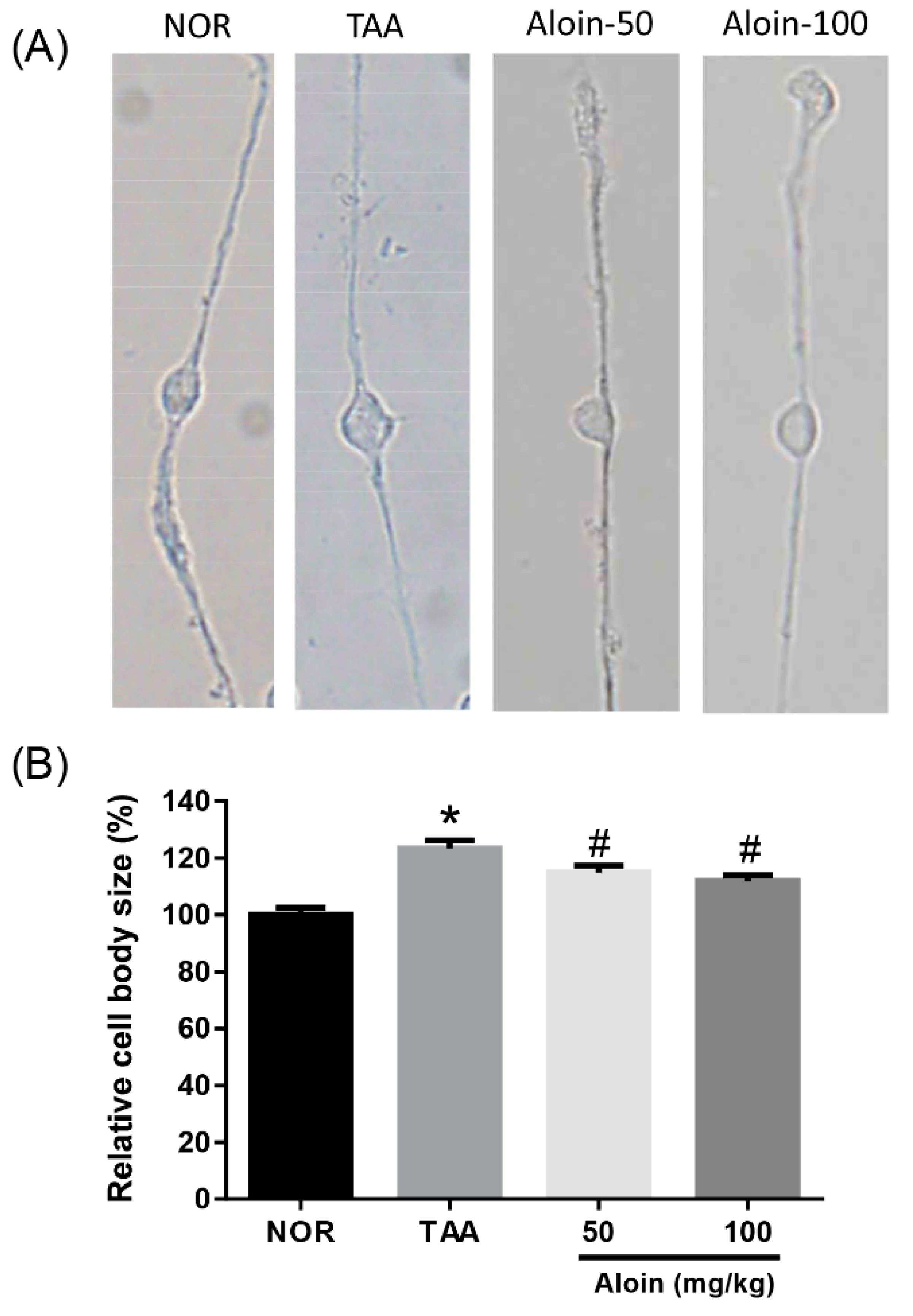
2.3. Müller Cell Swelling
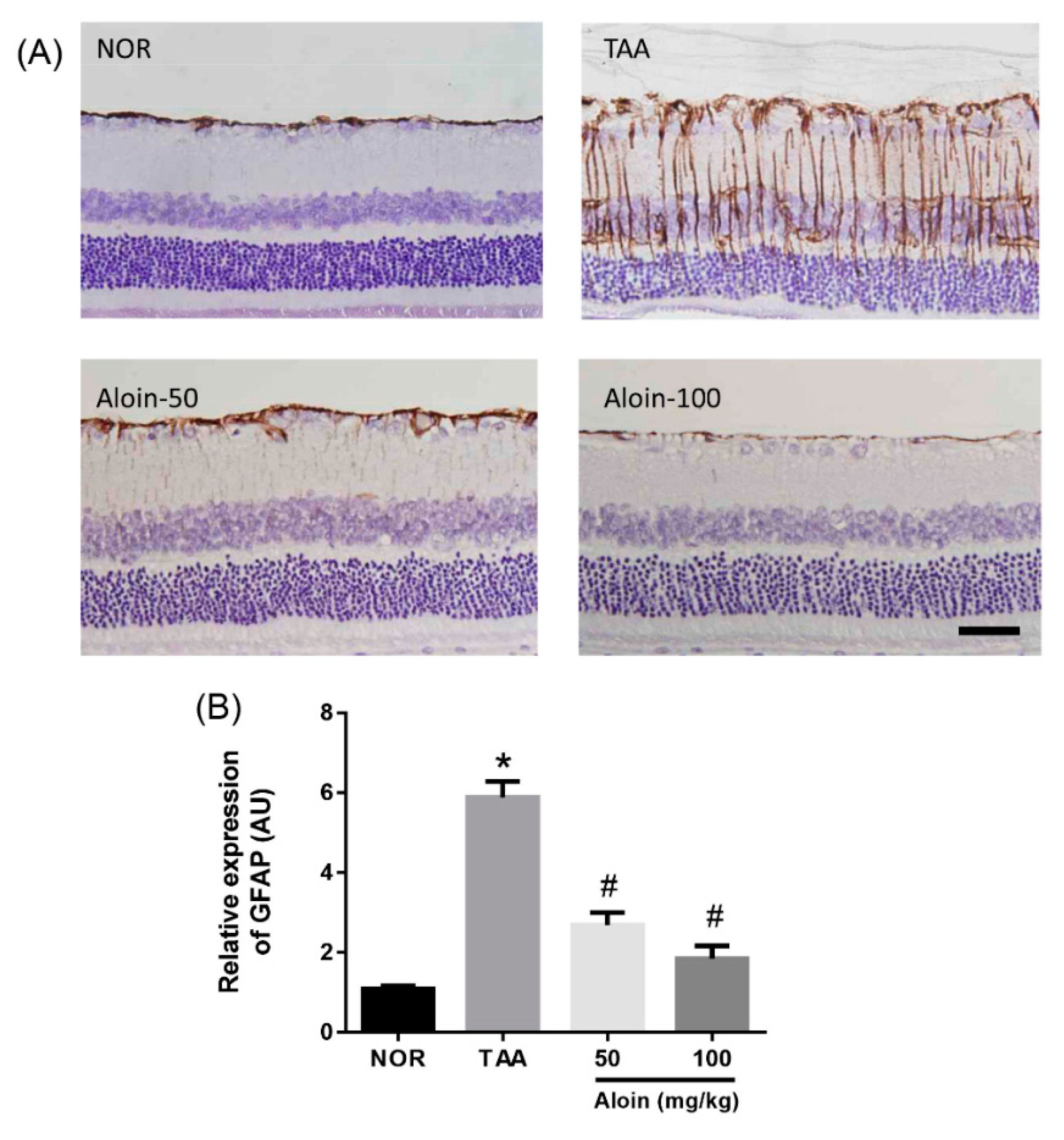
2.4. Müller Cell Activation
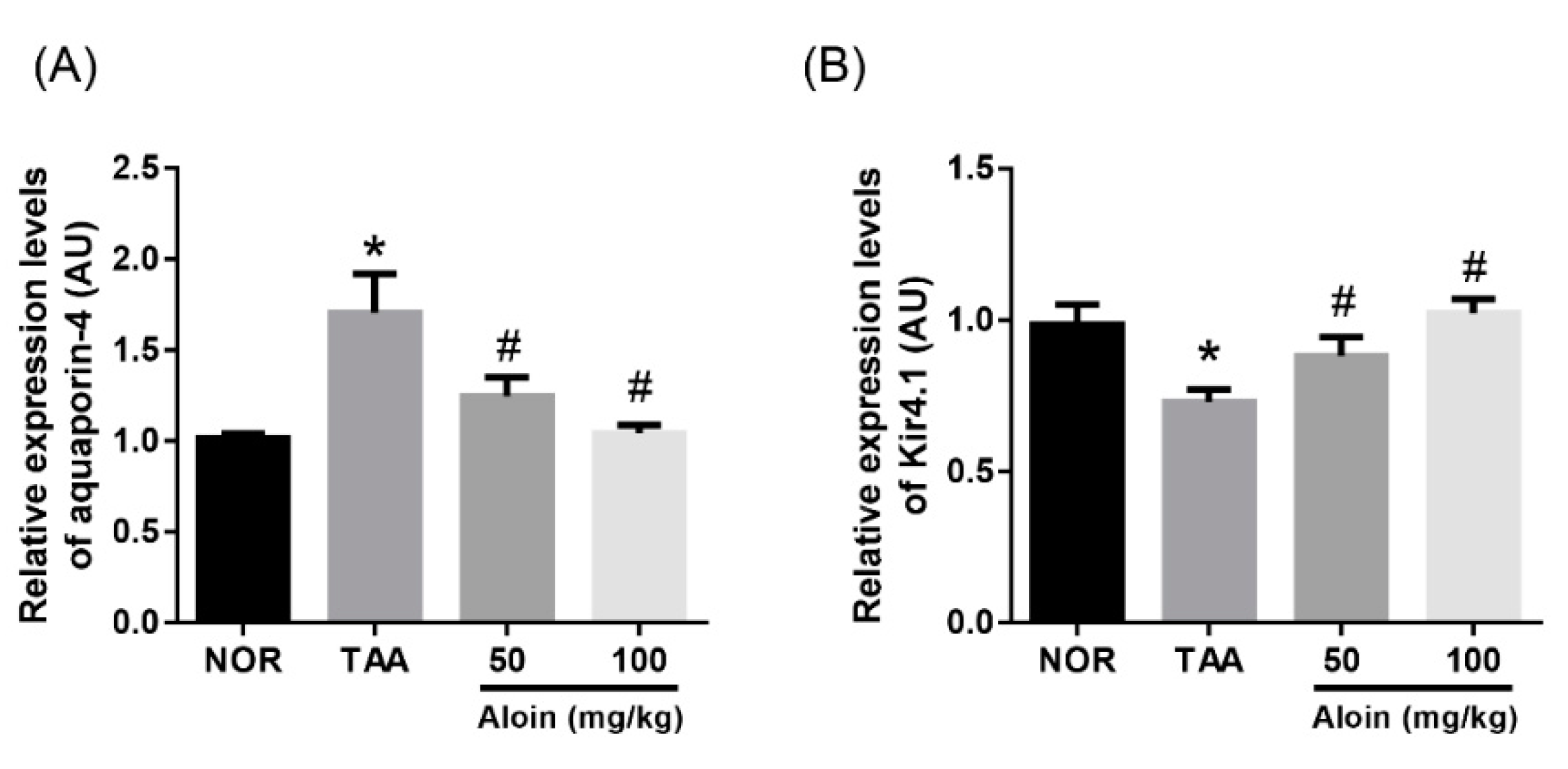
2.5. Retinal Gene Expression of Kir4.1 and Aquaporin-4
3. Discussion
4. Experimental Section
4.1. Animals and Experimental Design
4.2. Evaluation of Liver Injury
4.3. Isolation of Rat Retinal Müller Cells
4.4. Immunohistochemical Staining
4.5. Real-Time PCR
4.6. Statistical Analysis
Author Contributions
Funding
Conflicts of Interest
References
- Zhang, J.; Gao, S.; Duan, Z.; Hu, K.Q. Overview on acute-on-chronic liver failure. Front. Med. 2016, 10, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Duseja, A.; Singh, S.P. Toward a Better Definition of Acute-on-Chronic Liver Failure. J. Clin. Exp. Hepatol. 2017, 7, 262–265. [Google Scholar] [CrossRef] [PubMed]
- Elwir, S.; Rahimi, R.S. Hepatic Encephalopathy: An Update on the Pathophysiology and Therapeutic Options. J. Clin. Transl. Hepatol. 2017, 5, 142–151. [Google Scholar] [CrossRef] [PubMed]
- Reichenbach, A.; Fuchs, U.; Kasper, M.; el-Hifnawi, E.; Eckstein, A.K. Hepatic retinopathy: Morphological featuRes. of retinal glial (Müller) cells accompanying hepatic failure. Acta Neuropathol. 1995, 90, 273–281. [Google Scholar] [CrossRef] [PubMed]
- Uhlmann, S.; Uhlmann, D.; Hauss, J.; Reichenbach, A.; Wiedemann, P.; Faude, F. Recovery from hepatic retinopathy after liver transplantation. Graefe’s Arch. Clin. Exp. Ophthalmol. 2003, 241, 451–457. [Google Scholar] [CrossRef] [PubMed]
- Bringmann, A.; Wiedemann, P. Müller glial cells in retinal disease. Ophthalmologica 2012, 227, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Hassan, I.; Luo, Q.; Majumdar, S.; Dominguez, J.M., 2nd; Busik, J.V.; Bhatwadekar, A.D. Tumor Necrosis Factor Alpha (TNF-alpha) Disrupts Kir4.1 Channel Expression Resulting in Müller Cell Dysfunction in the Retina. Investig. Ophthalmol. Vis. Sci. 2017, 58, 2473–2482. [Google Scholar] [CrossRef] [PubMed]
- Kida, T.; Oku, H.; Horie, T.; Fukumoto, M.; Okuda, Y.; Morishita, S.; Ikeda, T. Implication of VEGF and aquaporin 4 mediating Müller cell swelling to diabetic retinal edema. Graefe’s Arch. Clin. Exp. Ophthalmol. 2017, 255, 1149–1157. [Google Scholar] [CrossRef] [PubMed]
- Vecino, E.; Rodriguez, F.D.; Ruzafa, N.; Pereiro, X.; Sharma, S.C. Glia-neuron interactions in the mammalian retina. Prog. Retin. Eye Res. 2016, 51, 1–40. [Google Scholar] [CrossRef] [PubMed]
- Rajasekaran, S.; Sivagnanam, K.; Subramanian, S. Antioxidant effect of Aloe vera gel extract in streptozotocin-induced diabetes in rats. Pharmacol. Rep. 2005, 57, 90–96. [Google Scholar] [PubMed]
- Grierson, D.S.; Afolayan, A.J. Antibacterial activity of some indigenous plants used for the treatment of wounds in the Eastern Cape, South Africa. J. Ethnopharmacol. 1999, 66, 103–106. [Google Scholar] [CrossRef]
- Devaraj, S.; Yimam, M.; Brownell, L.A.; Jialal, I.; Singh, S.; Jia, Q. Effects of Aloe vera supplementation in subjects with prediabetes/metabolic syndrome. Metab. Syndr. Relat. Disord. 2013, 11, 35–40. [Google Scholar] [CrossRef] [PubMed]
- Choi, H.C.; Kim, S.J.; Son, K.Y.; Oh, B.J.; Cho, B.L. Metabolic effects of aloe vera gel complex in obese prediabetes and early non-treated diabetic patients: Randomized controlled trial. Nutrition 2013, 29, 1110–1114. [Google Scholar] [CrossRef] [PubMed]
- Wintola, O.A.; Afolayan, A.J. Phytochemical constituents and antioxidant activities of the whole leaf extract of Aloe ferox Mill. Pharmacogn. Mag. 2011, 7, 325–333. [Google Scholar] [PubMed]
- Curto, E.M.; Labelle, A.; Chandler, H.L. Aloe vera: An in vitro study of effects on corneal wound closure and collagenase activity. Vet. Ophthalmol. 2014, 17, 403–410. [Google Scholar] [CrossRef] [PubMed]
- Atiba, A.; Wasfy, T.; Abdo, W.; Ghoneim, A.; Kamal, T.; Shukry, M. Aloe vera gel facilitates re-epithelialization of corneal alkali burn in normal and diabetic rats. Clin. Ophthalmol. 2015, 9, 2019–2026. [Google Scholar] [PubMed]
- Werawatganon, D.; Linlawan, S.; Thanapirom, K.; Somanawat, K.; Klaikeaw, N.; Rerknimitr, R.; Siriviriyakul, P. Aloe vera attenuated liver injury in mice with acetaminophen-induced hepatitis. BMC Complement. Altern. Med. 2014, 14, 229. [Google Scholar] [CrossRef] [PubMed]
- Can, A.; Akev, N.; Ozsoy, N.; Bolkent, S.; Arda, B.P.; Yanardag, R.; Okyar, A. Effect of Aloe vera leaf gel and pulp extracts on the liver in type-II diabetic rat models. Biol. Pharm. Bull. 2004, 27, 694–698. [Google Scholar] [CrossRef] [PubMed]
- Norikura, T.; Kennedy, D.O.; Nyarko, A.K.; Kojima, A.; Matsui-Yuasa, I. Protective effect of aloe extract against the cytotoxicity of 1,4-naphthoquinone in isolated rat hepatocytes involves modulations in cellular thiol levels. Pharmacol. Toxicol. 2002, 90, 278–284. [Google Scholar] [CrossRef] [PubMed]
- Arosio, B.; Gagliano, N.; Fusaro, L.M.; Parmeggiani, L.; Tagliabue, J.; Galetti, P.; De Castri, D.; Moscheni, C.; Annoni, G. Aloe-Emodin quinone pretreatment reduces acute liver injury induced by carbon tetrachloride. Pharmacol. Toxicol. 2000, 87, 229–233. [Google Scholar] [CrossRef] [PubMed]
- Cui, Y.; Ye, Q.; Wang, H.; Li, Y.; Xia, X.; Yao, W.; Qian, H. Aloin protects against chronic alcoholic liver injury via attenuating lipid accumulation, oxidative stress and inflammation in mice. Arch. Pharm. Res. 2014, 37, 1624–1633. [Google Scholar] [CrossRef] [PubMed]
- Chang, R.; Zhou, R.; Qi, X.; Wang, J.; Wu, F.; Yang, W.; Zhang, W.; Sun, T.; Li, Y.; Yu, J. Protective effects of aloin on oxygen and glucose deprivation-induced injury in PC12 cells. Brain Res. Bull. 2016, 121, 75–83. [Google Scholar] [CrossRef] [PubMed]
- Zhou, T.; Che, D.; Lan, Y.; Fang, Z.; Xie, J.; Gong, H.; Li, C.; Feng, J.; Hong, H.; Qi, W.; et al. Mesenchymal marker expression is elevated in Müller cells exposed to high glucose and in animal models of diabetic retinopathy. Oncotarget 2017, 8, 4582–4594. [Google Scholar] [PubMed]
- Eckstein, A.K.; Reichenbach, A.; Jacobi, P.; Weber, P.; Gregor, M.; Zrenner, E. Hepatic retinopathia. Changes in retinal function. Vis. Res. 1997, 37, 1699–1706. [Google Scholar] [CrossRef]
- Kashani, A.A. Hepatic retinopathia: Changes in retinal function. Vis. Res. 1999, 39, 2027–2029. [Google Scholar] [PubMed]
- Karl, A.; Wurm, A.; Pannicke, T.; Krugel, K.; Obara-Michlewska, M.; Wiedemann, P.; Reichenbach, A.; Albrecht, J.; Bringmann, A. Synergistic action of hypoosmolarity and glutamine in inducing acute swelling of retinal glial (Müller) cells. Glia 2011, 59, 256–266. [Google Scholar] [CrossRef] [PubMed]
- Toft-Kehler, A.K.; Skytt, D.M.; Svare, A.; Lefevere, E.; Van Hove, I.; Moons, L.; Waagepetersen, H.S.; Kolko, M. Mitochondrial function in Müller cells—Does it matter? Mitochondrion 2017, 36, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Madeira, M.H.; Boia, R.; Santos, P.F.; Ambrosio, A.F.; Santiago, A.R. Contribution of microglia-mediated neuroinflammation to retinal degenerative diseases. Mediat. Inflamm. 2015, 2015. [Google Scholar] [CrossRef] [PubMed]
- Ali, S.O.; Darwish, H.A.; Ismail, N.A. Modulatory effects of curcumin, silybin-phytosome and alpha-R-lipoic acid against thioacetamide-induced liver cirrhosis in rats. Chem. Biol. Interact. 2014, 216, 26–33. [Google Scholar] [CrossRef] [PubMed]
- Albrecht, J.; Gadamski, R.; Kuhrt, H.; Walski, M.; Reichenbach, A. Retinal gliopathy accompanying thioacetamide-induced liver insufficiency: Light and electron microscopic observations. Acta Neuropathol. 1998, 96, 57–66. [Google Scholar] [CrossRef] [PubMed]
- Parekh, P.J.; Balart, L.A. Ammonia and Its Role in the Pathogenesis of Hepatic Encephalopathy. Clin. Liver Dis. 2015, 19, 529–537. [Google Scholar] [CrossRef] [PubMed]
- Reichenbach, A.; Bringmann, A. Purinergic signaling in retinal degeneration and regeneration. Neuropharmacology 2016, 104, 194–211. [Google Scholar] [CrossRef] [PubMed]
- Bringmann, A.; Pannicke, T.; Biedermann, B.; Francke, M.; Iandiev, I.; Grosche, J.; Wiedemann, P.; Albrecht, J.; Reichenbach, A. Role of retinal glial cells in neurotransmitter uptake and metabolism. Neurochem. Chem. Int. 2009, 54, 143–160. [Google Scholar] [CrossRef] [PubMed]
- Verkman, A.S.; Smith, A.J.; Phuan, P.W.; Tradtrantip, L.; Anderson, M.O. The aquaporin-4 water channel as a potential drug target in neurological disorders. Expert. Opin. Ther. Targets 2017, 21, 1161–1170. [Google Scholar] [CrossRef] [PubMed]
- Siqueiros-Marquez, L.; Benard, R.; Vacca, O.; Charles-Messance, H.; Bolanos-Jimenez, R.; Guilloneau, X.; Sennlaub, F.; Montanez, C.; Sahel, J.A.; Rendon, A.; et al. Protection of Glial Müller Cells by Dexamethasone in a Mouse Model of Surgically Induced Blood-Retinal Barrier Breakdown. Investig. Ophthalmol. Vis. Sci. 2017, 58, 876–886. [Google Scholar]
- Nagelhus, E.A.; Horio, Y.; Inanobe, A.; Fujita, A.; Haug, F.M.; Nielsen, S.; Kurachi, Y.; Ottersen, O.P. Immunogold evidence suggests that coupling of K+ siphoning and water transport in rat retinal Müller cells is mediated by a coenrichment of Kir4.1 and AQP4 in specific membrane domains. Glia 1999, 26, 47–54. [Google Scholar] [CrossRef]
- Pannicke, T.; Iandiev, I.; Wurm, A.; Uckermann, O.; vom Hagen, F.; Reichenbach, A.; Wiedemann, P.; Hammes, H.P.; Bringmann, A. Diabetes alters osmotic swelling characteristics and membrane conductance of glial cells in rat retina. Diabetes 2006, 55, 633–639. [Google Scholar] [CrossRef] [PubMed]
- Pannicke, T.; Uckermann, O.; Iandiev, I.; Wiedemann, P.; Reichenbach, A.; Bringmann, A. Ocular inflammation alters swelling and membrane characteristics of rat Müller glial cells. J. Neuroimmunol. 2005, 161, 145–154. [Google Scholar] [CrossRef] [PubMed]
- Wurm, A.; Pannicke, T.; Iandiev, I.; Buhner, E.; Pietsch, U.C.; Reichenbach, A.; Wiedemann, P.; Uhlmann, S.; Bringmann, A. Changes in membrane conductance play a pathogenic role in osmotic glial cell swelling in detached retinas. Am. J. Pathol. 2006, 169, 1990–1998. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, H.; Ashkenazi, M.; Weizman, N.; Shahmurov, M.; Aeed, H.; Bruck, R. Curcumin ameliorates acute thioacetamide-induced hepatotoxicity. J. Gastroenterol. Hepatol. 2006, 21, 358–366. [Google Scholar] [CrossRef] [PubMed]
- Chen, T.M.; Subeq, Y.M.; Lee, R.P.; Chiou, T.W.; Hsu, B.G. Single dose intravenous thioacetamide administration as a model of acute liver damage in rats. Int. J. Exp. Pathol. 2008, 89, 223–231. [Google Scholar] [CrossRef] [PubMed]
- Lucas, D.R.; Newhouse, J.P. The toxic effect of sodium L-glutamate on the inner layers of the retina. AMA Arch. Ophthalmol. 1957, 58, 193–201. [Google Scholar] [CrossRef] [PubMed]
- Izumi, Y.; Matsukawa, M.; Benz, A.M.; Izumi, M.; Ishikawa, M.; Olney, J.W.; Zorumski, C.F. Role of ammonia in reversal of glutamate-mediated Müller cell swelling in the rat retina. Glia 2004, 48, 44–50. [Google Scholar] [CrossRef] [PubMed]
- Müller, A.; Machnik, F.; Zimmermann, T.; Schubert, H. Thioacetamide-induced cirrhosis-like liver lesions in rats—Usefulness and reliability of this animal model. Exp. Pathol. 1988, 34, 229–236. [Google Scholar] [CrossRef]
- Lee, Y.M.; Lee, Y.R.; Kim, C.S.; Jo, K.; Sohn, E.; Kim, J.S.; Kim, J. Cnidium officinale extract and butylidenephthalide inhibits retinal neovascularization in vitro and in vivo. BMC Complement. Altern. Med. 2016, 16, 231. [Google Scholar] [CrossRef] [PubMed]
Sample Availability: Samples of the compounds at amounts less than 1 mg are available from the authors. |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jung, E.; Kim, J. Aloin Inhibits Müller Cells Swelling in a Rat Model of Thioacetamide-Induced Hepatic Retinopathy. Molecules 2018, 23, 2806. https://doi.org/10.3390/molecules23112806
Jung E, Kim J. Aloin Inhibits Müller Cells Swelling in a Rat Model of Thioacetamide-Induced Hepatic Retinopathy. Molecules. 2018; 23(11):2806. https://doi.org/10.3390/molecules23112806
Chicago/Turabian StyleJung, Eunsoo, and Junghyun Kim. 2018. "Aloin Inhibits Müller Cells Swelling in a Rat Model of Thioacetamide-Induced Hepatic Retinopathy" Molecules 23, no. 11: 2806. https://doi.org/10.3390/molecules23112806
APA StyleJung, E., & Kim, J. (2018). Aloin Inhibits Müller Cells Swelling in a Rat Model of Thioacetamide-Induced Hepatic Retinopathy. Molecules, 23(11), 2806. https://doi.org/10.3390/molecules23112806






