Therapeutic Effects of Phytochemicals and Medicinal Herbs on Chemotherapy-Induced Peripheral Neuropathy
Abstract
:1. Introduction
2. Phytochemicals and Medicinal Herbs against Vincristine-Induced Peripheral Neuropathy
2.1. Acorus calamus
2.2. Auraptenol
2.3. Butea monosperma
2.4. Cannabinoids
2.5. Ginkgo biloba L.
2.6. Ocimum sanctum L.
2.7. Xylopic Acid
3. Phytochemicals and Medicinal Herbs against Cisplatin-Induced Peripheral Neuropathy
3.1. Curcumin
3.2. Ginkgo biloba L.
3.3. Salvia officinalis
3.4. Walnut
4. Phytochemicals and Medicinal Herbs against Oxaliplatin-Induced Peripheral Neuropathy
4.1. Curcumin
4.2. Rutin and Quercetin
4.3. Camellia sinensis (Green Tea)
4.4. Gyeryongtongrac-Bang (Guilongtongluofang in Chinese)
4.5. Gyejigachulbu-Tang (Keishikajutsubuto in Japanese)
4.6. Jesengsingi-Hwan (Goshajinkigan in Japanese)
4.7. Hwanggiomul-Tang (Ogikeishigomotsuto in Japanese)
5. Phytochemicals and Medicinal Herbs against Paclitaxel-Induced Peripheral Neuropathy
5.1. Cannabidiol
5.2. Verticinone
5.3. Jesengshingi-Hwan
5.4. Jakyakgamcho-Tang (Shakuyakukanzoto in Japanese)
6. Conclusions and Perspectives
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Miltenburg, N.C.; Boogerd, W. Chemotherapy-induced neuropathy: A comprehensive survey. Cancer Treat. Rev. 2014, 40, 872–882. [Google Scholar] [CrossRef] [PubMed]
- Jaggi, A.S.; Singh, N. Mechanisms in cancer-chemotherapeutic drugs-induced peripheral neuropathy. Toxicology 2012, 291, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Egan, M.; Burke, E.; Meskell, P.; MacNeela, P.; Dowling, M. Quality of life and resilience related to chemotherapy-induced peripheral neuropathy in patients post treatment with platinums and taxanes. J. Res. Nurs. 2015, 20, 385–398. [Google Scholar] [CrossRef]
- Visovsky, C.; Collins, M.; Abbott, L.; Aschenbrenner, J.; Hart, C. Putting evidence into practice: Evidence-based interventions for chemotherapy-induced peripheral neuropathy. Clin. J. Oncol. Nurs. 2007, 11, 901–913. [Google Scholar] [CrossRef] [PubMed]
- Cavaletti, G. Chemotherapy-induced peripheral neurotoxicity (cipn): What we need and what we know. J. Peripher. Nerv. Syst. 2014, 19, 66–76. [Google Scholar] [CrossRef] [PubMed]
- Beijers, A.J.; Vreugdenhil, G.; Oerlemans, S.; Eurelings, M.; Minnema, M.C.; Eeltink, C.M.; van de Poll-Franse, L.V.; Mols, F. Chemotherapy-induced neuropathy in multiple myeloma: Influence on quality of life and development of a questionnaire to compose common toxicity criteria grading for use in daily clinical practice. Support. Care Cancer 2016, 24, 2411–2420. [Google Scholar] [CrossRef] [PubMed]
- Park, S.B.; Goldstein, D.; Krishnan, A.V.; Lin, C.S.; Friedlander, M.L.; Cassidy, J.; Koltzenburg, M.; Kiernan, M.C. Chemotherapy-induced peripheral neurotoxicity: A critical analysis. CA A Cancer J. Clin. 2013, 63, 419–437. [Google Scholar] [CrossRef] [PubMed]
- Argyriou, A.A.; Kyritsis, A.P.; Makatsoris, T.; Kalofonos, H.P. Chemotherapy-induced peripheral neuropathy in adults: A comprehensive update of the literature. Cancer Manag. Res. 2014, 6, 135–147. [Google Scholar] [CrossRef] [PubMed]
- Smith, J.A.; Benbow, S.J. Meeting report: Inaugural chemotherapy-induced peripheral neuropathy symposium—Santa Barbara, CA, February 2015. Cancer Res. 2015, 75, 3696–3698. [Google Scholar] [CrossRef] [PubMed]
- Cavaletti, G.; Zanna, C. Current status and future prospects for the treatment of chemotherapy-induced peripheral neurotoxicity. Eur. J. Cancer 2002, 38, 1832–1837. [Google Scholar] [CrossRef]
- Cavaletti, G.; Frigeni, B.; Lanzani, F.; Mattavelli, L.; Susani, E.; Alberti, P.; Cortinovis, D.; Bidoli, P. Chemotherapy-induced peripheral neurotoxicity assessment: A critical revision of the currently available tools. Eur. J. Cancer 2010, 46, 479–494. [Google Scholar] [CrossRef] [PubMed]
- Cavaletti, G.; Cornblath, D.R.; Merkies, I.S.; Postma, T.J.; Rossi, E.; Frigeni, B.; Alberti, P.; Bruna, J.; Velasco, R.; Argyriou, A.A.; et al. The chemotherapy-induced peripheral neuropathy outcome measures standardization study: From consensus to the first validity and reliability findings. Ann. Oncol. 2013, 24, 454–462. [Google Scholar] [CrossRef] [PubMed]
- Hausheer, F.H.; Schilsky, R.L.; Bain, S.; Berghorn, E.J.; Lieberman, F. Diagnosis, management, and evaluation of chemotherapy-induced peripheral neuropathy. Semin. Oncol. 2006, 33, 15–49. [Google Scholar] [CrossRef] [PubMed]
- Grothey, A. Clinical management of oxaliplatin-associated neurotoxicity. Clin. Colorectal Cancer 2005, 5 (Suppl. 1), S38–S46. [Google Scholar] [CrossRef] [PubMed]
- Kushlaf, H.A. Emerging toxic neuropathies and myopathies. Neurol. Clin. 2011, 29, 679–687. [Google Scholar] [CrossRef] [PubMed]
- Kuncl, R.W.; George, E.B. Toxic neuropathies and myopathies. Curr. Opin. Neurol. 1993, 6, 695–704. [Google Scholar] [CrossRef] [PubMed]
- Flatters, S.J.; Xiao, W.H.; Bennett, G.J. Acetyl-l-carnitine prevents and reduces paclitaxel-induced painful peripheral neuropathy. Neurosci. Lett. 2006, 397, 219–223. [Google Scholar] [CrossRef] [PubMed]
- Cavaletti, G. Calcium and magnesium prophylaxis for oxaliplatin-related neurotoxicity: Is it a trade-off between drug efficacy and toxicity? Oncologist 2011, 16, 1667–1668. [Google Scholar] [CrossRef] [PubMed]
- Ta, L.E.; Schmelzer, J.D.; Bieber, A.J.; Loprinzi, C.L.; Sieck, G.C.; Brederson, J.D.; Low, P.A.; Windebank, A.J. A novel and selective poly(adp-ribose) polymerase inhibitor ameliorates chemotherapy-induced painful neuropathy. PLoS ONE 2013, 8, e54161. [Google Scholar] [CrossRef] [PubMed]
- Wolf, S.; Barton, D.; Kottschade, L.; Grothey, A.; Loprinzi, C. Chemotherapy-induced peripheral neuropathy: Prevention and treatment strategies. Eur. J. Cancer 2008, 44, 1507–1515. [Google Scholar] [CrossRef] [PubMed]
- Ceresa, C.; Cavaletti, G. Drug transporters in chemotherapy induced peripheral neurotoxicity: Current knowledge and clinical implications. Curr. Med. Chem. 2011, 18, 329–341. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Cao, S.E.; Tian, J.; Liu, G.; Zhang, X.; Li, P. Auraptenol attenuates vincristine-induced mechanical hyperalgesia through serotonin 5-ht1a receptors. Sci. Rep. 2013, 3, 3377. [Google Scholar] [CrossRef] [PubMed]
- Ward, S.J.; McAllister, S.D.; Kawamura, R.; Murase, R.; Neelakantan, H.; Walker, E.A. Cannabidiol inhibits paclitaxel-induced neuropathic pain through 5-HT(1A) receptors without diminishing nervous system function or chemotherapy efficacy. Br. J. Pharmacol. 2014, 171, 636–645. [Google Scholar] [CrossRef] [PubMed]
- Al Moundhri, M.S.; Al-Salam, S.; Al Mahrouqee, A.; Beegam, S.; Ali, B.H. The effect of curcumin on oxaliplatin and cisplatin neurotoxicity in rats: Some behavioral, biochemical, and histopathological studies. J. Med. Toxicol. 2013, 9, 25–33. [Google Scholar] [CrossRef] [PubMed]
- Azevedo, M.I.; Pereira, A.F.; Nogueira, R.B.; Rolim, F.E.; Brito, G.A.; Wong, D.V.; Lima-Junior, R.C.; de Albuquerque Ribeiro, R.; Vale, M.L. The antioxidant effects of the flavonoids rutin and quercetin inhibit oxaliplatin-induced chronic painful peripheral neuropathy. Mol. Pain 2013, 9, 53. [Google Scholar] [CrossRef] [PubMed]
- Xu, F.Z.; Xu, S.Z.; Wang, L.J.; Chen, C.T.; Zhou, X.Q.; Lu, Y.Z.; Zhang, H.H. Antinociceptive efficacy of verticinone in murine models of inflammatory pain and paclitaxel induced neuropathic pain. Biol. Pharm. Bull. 2011, 34, 1377–1382. [Google Scholar] [CrossRef] [PubMed]
- Ameyaw, E.O.; Woode, E.; Boakye-Gyasi, E.; Abotsi, W.K.; Kyekyeku, J.O.; Adosraku, R.K. Anti-allodynic and anti-hyperalgesic effects of an ethanolic extract and xylopic acid from the fruits of Xylopia aethiopica in murine models of neuropathic pain. Pharm. Res. 2014, 6, 172–179. [Google Scholar]
- Muthuraman, A.; Singh, N. Attenuating effect of hydroalcoholic extract of Acorus calamus in vincristine-induced painful neuropathy in rats. J. Nat. Med. 2011, 65, 480–487. [Google Scholar] [CrossRef] [PubMed]
- Thiagarajan, V.R.; Shanmugam, P.; Krishnan, U.M.; Muthuraman, A.; Singh, N. Antinociceptive effect of Butea monosperma on vincristine-induced neuropathic pain model in rats. Toxicol. Ind. Health 2013, 29, 3–13. [Google Scholar] [CrossRef] [PubMed]
- Park, H.J.; Lee, H.G.; Kim, Y.S.; Lee, J.Y.; Jeon, J.P.; Park, C.; Moon, D.E. Ginkgo biloba extract attenuates hyperalgesia in a rat model of vincristine-induced peripheral neuropathy. Anesthesia Analg. 2012, 115, 1228–1233. [Google Scholar] [CrossRef] [PubMed]
- Ozturk, G.; Anlar, O.; Erdogan, E.; Kosem, M.; Ozbek, H.; Turker, A. The effect of ginkgo extract EGb761 in cisplatin-induced peripheral neuropathy in mice. Toxicol. Appl. Pharmacol. 2004, 196, 169–175. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.S.; Kim, Y.T.; Jeon, E.K.; Won, H.S.; Cho, Y.S.; Ko, Y.H. Effect of green tea extracts on oxaliplatin-induced peripheral neuropathy in rats. BMC Complement. Altern. Med. 2012, 12, 124. [Google Scholar] [CrossRef] [PubMed]
- Kaur, G.; Jaggi, A.S.; Singh, N. Exploring the potential effect of Ocimum sanctum in vincristine-induced neuropathic pain in rats. J. Brachial Plex. Peripher. Nerve Inj. 2010, 5, 3. [Google Scholar] [CrossRef] [PubMed]
- Namvaran-Abbas-Abad, A.; Tavakkoli, F. Antinociceptive effect of salvia extract on cisplatin-induced hyperalgesia in mice. Neurophysiology 2012, 43, 452–458. [Google Scholar] [CrossRef]
- Shabani, M.; Nazeri, M.; Parsania, S.; Razavinasab, M.; Zangiabadi, N.; Esmaeilpour, K.; Abareghi, F. Walnut consumption protects rats against cisplatin-induced neurotoxicity. Neurotoxicology 2012, 33, 1314–1321. [Google Scholar] [CrossRef] [PubMed]
- Ahn, B.S.; Kim, S.K.; Kim, H.N.; Lee, J.H.; Lee, J.H.; Hwang, D.S.; Bae, H.; Min, B.I.; Kim, S.K. Gyejigachulbu-tang relieves oxaliplatin-induced neuropathic cold and mechanical hypersensitivity in rats via the suppression of spinal glial activation. Evid. Based Complement. Altern. Med. 2014, 2014, 436482. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Zhu, G.; Han, L.; Liu, J.; Ma, T.; Yu, H. Clinical study on the prevention of oxaliplatin-induced neurotoxicity with guilongtongluofang: Results of a randomized, double-blind, placebo-controlled trial. Evid. Based Complement. Altern. Med. 2013, 2013, 541217. [Google Scholar] [CrossRef] [PubMed]
- Sima, L.; Pan, L. Influence of chinese herb ah on chemotherapy-induced peripheral neuropathy. Ann. Oncol. 2009, 20, 46. [Google Scholar]
- Hidaka, T.; Shima, T.; Nagira, K.; Ieki, M.; Nakamura, T.; Aono, Y.; Kuraishi, Y.; Arai, T.; Saito, S. Herbal medicine shakuyaku-kanzo-to reduces paclitaxel-induced painful peripheral neuropathy in mice. Eur. J. Pain 2009, 13, 22–27. [Google Scholar] [CrossRef] [PubMed]
- Fujii, K.; Okamoto, S.; Saitoh, K.; Sasaki, N.; Takano, M.; Tanaka, S.; Kudoh, K.; Kita, T.; Tode, T.; Kikuchi, Y. The efficacy of shakuyaku-kanzo-to for peripheral nerve dysfunction in paclitaxel combination chemotherapy for epithelial ovarian carcinoma. Gan To Kagaku Ryoho. Cancer Chemother. 2004, 31, 1537–1540. [Google Scholar]
- Ushio, S.; Egashira, N.; Sada, H.; Kawashiri, T.; Shirahama, M.; Masuguchi, K.; Oishi, R. Goshajinkigan reduces oxaliplatin-induced peripheral neuropathy without affecting anti-tumour efficacy in rodents. Eur. J. Cancer 2012, 48, 1407–1413. [Google Scholar] [CrossRef] [PubMed]
- Kono, T.; Suzuki, Y.; Mizuno, K.; Miyagi, C.; Omiya, Y.; Sekine, H.; Mizuhara, Y.; Miyano, K.; Kase, Y.; Uezono, Y. Preventive effect of oral goshajinkigan on chronic oxaliplatin-induced hypoesthesia in rats. Sci. Rep. 2015, 5, 16078. [Google Scholar] [CrossRef] [PubMed]
- Bahar, M.A.; Andoh, T.; Ogura, K.; Hayakawa, Y.; Saiki, I.; Kuraishi, Y. Herbal medicine goshajinkigan prevents paclitaxel-induced mechanical allodynia without impairing antitumor activity of paclitaxel. Evid. Based Complement. Altern. Med. 2013. [Google Scholar] [CrossRef] [PubMed]
- Kono, T.; Mamiya, N.; Chisato, N.; Ebisawa, Y.; Yamazaki, H.; Watari, J.; Yamamoto, Y.; Suzuki, S.; Asama, T.; Kamiya, K. Efficacy of goshajinkigan for peripheral neurotoxicity of oxaliplatin in patients with advanced or recurrent colorectal cancer. Evid. Based Complement. Altern. Med. 2011, 2011, 418481. [Google Scholar] [CrossRef] [PubMed]
- Kono, T.; Hata, T.; Morita, S.; Munemoto, Y.; Matsui, T.; Kojima, H.; Takemoto, H.; Fukunaga, M.; Nagata, N.; Shimada, M.; et al. Goshajinkigan oxaliplatin neurotoxicity evaluation (gone): A phase 2, multicenter, randomized, doubleblind, placebocontrolled trial of goshajinkigan to prevent oxaliplatininduced neuropathy. Cancer Chemother. Pharmacol. 2013, 72, 1283–1290. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, N.; Hosokawa, T.; Ishikawa, T.; Yagi, N.; Kokura, S.; Naito, Y.; Nakanishi, M.; Kokuba, Y.; Otsuji, E.; Kuroboshi, H.; et al. Efficacy of goshajinkigan for oxaliplatin-induced peripheral neuropathy in colorectal cancer patients. J. Oncol. 2013, 2013, 139740. [Google Scholar] [CrossRef] [PubMed]
- Hosokawa, A.; Ogawa, K.; Ando, T.; Suzuki, N.; Ueda, A.; Kajiura, S.; Kobayashi, Y.; Tsukioka, Y.; Horikawa, N.; Yabushita, K.; et al. Preventive effect of traditional japanese medicine on neurotoxicity of folfox for metastatic colorectal cancer: A multicenter retrospective study. Anticancer Res. 2012, 32, 2545–2550. [Google Scholar] [PubMed]
- Yamamoto, T.; Murai, T.; Ueda, M.; Katsuura, M.; Oishi, M.; Miwa, Y.; Okamoto, Y.; Uejima, E.; Taguchi, T.; Noguchi, S.; et al. Clinical features of paclitaxel-induced peripheral neuropathy and role of gosya-jinki-gan. Gan To kagaku ryoho. Cancer Chemother. 2009, 36, 89–92. [Google Scholar]
- Jordan, M.A. Mechanism of action of antitumor drugs that interact with microtubules and tubulin. Curr. Med. Chem. Anti-Cancer Agent. 2002, 2, 1–17. [Google Scholar] [CrossRef]
- Verstappen, C.C.; Koeppen, S.; Heimans, J.J.; Huijgens, P.C.; Scheulen, M.E.; Strumberg, D.; Kiburg, B.; Postma, T.J. Dose-related vincristine-induced peripheral neuropathy with unexpected off-therapy worsening. Neurology 2005, 64, 1076–1077. [Google Scholar] [CrossRef] [PubMed]
- Sharma, V.; Singh, I.; Chaudhary, P. Acorus calamus (the healing plant): A review on its medicinal potential, micropropagation and conservation. Nat. Prod. Res. 2014, 28, 1454–1466. [Google Scholar] [CrossRef] [PubMed]
- Shah, P.D.; Ghag, M.; Deshmukh, P.B.; Kulkarni, Y.; Joshi, S.V.; Vyas, B.A.; Shah, D.R. Toxicity study of ethanolic extract of Acorus calamus rhizome. Int. J. Green Pharm. 2014, 6, 38–44. [Google Scholar] [CrossRef]
- Li, H.; Dai, Y.; Zhang, H.; Xie, C. Pharmacological studies on the chinese drug radix Angelicae dahuricae. Zhongguo Zhong Yao Za Zhi 1991, 16, 560–562, 576. [Google Scholar] [PubMed]
- Nie, H.; Shen, Y.J. Effect of essential oil of radix Angelicae dahuricae on beta-endorphin, acth, no and proopiomelanocortin of pain model rats. Zhongguo Zhong Yao Za Zhi 2002, 27, 690–693. [Google Scholar] [PubMed]
- Yuan, C.S.; Mehendale, S.R.; Wang, C.Z.; Aung, H.H.; Jiang, T.; Guan, X.; Shoyama, Y. Effects of Corydalis yanhusuo and Angelicae dahuricae on cold pressor-induced pain in humans: A controlled trial. J. Clin. Pharmacol. 2004, 44, 1323–1327. [Google Scholar] [CrossRef] [PubMed]
- Akram, M.; Akhtar, N.; Asif, H.M.; Shah, P.A.; Saeed, T.; Mahmood, A.; Malik, N.S. Butea monosperma lam.: A review. J. Med. Plants Res. 2011, 5, 3994–3996. [Google Scholar]
- Madhavi, A. An overview of Butea monosperma (flame of forest). World J. Pharm. Pharm. Sci. 2013, 3, 307–319. [Google Scholar]
- Rahn, E.J.; Hohmann, A.G. Cannabinoids as pharmacotherapies for neuropathic pain: From the bench to the bedside. Neurotherapeutics 2009, 6, 713–737. [Google Scholar] [CrossRef] [PubMed]
- Nagarkatti, P.; Pandey, R.; Rieder, S.A.; Hegde, V.L.; Nagarkatti, M. Cannabinoids as novel anti-inflammatory drugs. Future Med. Chem. 2009, 1, 1333–1349. [Google Scholar] [CrossRef] [PubMed]
- Rahn, E.J.; Makriyannis, A.; Hohmann, A.G. Activation of cannabinoid cb1 and cb2 receptors suppresses neuropathic nociception evoked by the chemotherapeutic agent vincristine in rats. Br. J. Pharmacol. 2007, 152, 765–777. [Google Scholar] [CrossRef] [PubMed]
- Velasco, G.; Hernandez-Tiedra, S.; Davila, D.; Lorente, M. The use of cannabinoids as anticancer agents. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2016, 64, 259–266. [Google Scholar] [CrossRef] [PubMed]
- Isah, T. Rethinking Ginkgo biloba L.: Medicinal uses and conservation. Pharm. Rev. 2015, 9, 140–148. [Google Scholar] [CrossRef] [PubMed]
- Jiang, W.; Qiu, W.L.; Wang, Y.S.; Cong, Q.; Edwards, D.; Ye, B.; Xu, C.J. Ginkgo may prevent genetic-associated ovarian cancer risk: Multiple biomarkers and anticancer pathways induced by ginkgolide b in brca1-mutant ovarian epithelial cells. Eur. J. Cancer Prev. 2011, 20, 508–517. [Google Scholar] [CrossRef] [PubMed]
- Marques, F.; Azevedo, F.; Johansson, B.; Oliveira, R. Stimulation of DNA repair in saccharomyces cerevisiae by Ginkgo biloba leaf extract. Food Chem. Toxicol. 2011, 49, 1361–1366. [Google Scholar] [CrossRef] [PubMed]
- Esmekaya, M.A.; Aytekin, E.; Ozgur, E.; Guler, G.; Ergun, M.A.; Omeroglu, S.; Seyhan, N. Mutagenic and morphologic impacts of 1.8 ghz radiofrequency radiation on human peripheral blood lymphocytes (hPBLs) and possible protective role of pre-treatment with Ginkgo biloba (EGb 761). Sci. Total Environ. 2011, 410, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Biggs, M.L.; Sorkin, B.C.; Nahin, R.L.; Kuller, L.H.; Fitzpatrick, A.L. Ginkgo biloba and risk of cancer: Secondary analysis of the ginkgo evaluation of memory (gem) study. Pharmacoepidemiol. Drug Saf. 2010, 19, 694–698. [Google Scholar] [CrossRef] [PubMed]
- Pattanayak, P.; Behera, P.; Das, D.; Panda, S.K. Ocimum sanctum linn. A reservoir plant for therapeutic applications: An overview. Pharm. Rev. 2010, 4, 95–105. [Google Scholar] [CrossRef] [PubMed]
- Kelm, M.A.; Nair, M.G.; Strasburg, G.M.; DeWitt, D.L. Antioxidant and cyclooxygenase inhibitory phenolic compounds from Ocimum sanctum linn. Phytomedicine 2000, 7, 7–13. [Google Scholar] [CrossRef]
- Prakash, J.; Gupta, S.K. Chemopreventive activity of Ocimum sanctum seed oil. J. Ethnopharmacol. 2000, 72, 29–34. [Google Scholar] [CrossRef]
- Igwe, S.A.; Afonne, J.C.; Ghasi, S.I. Ocular dynamics of systemic aqueous extracts of Xylopia aethiopica (african guinea pepper) seeds on visually active volunteers. J. Ethnopharm. 2003, 86, 139–142. [Google Scholar] [CrossRef]
- Adaramoye, O.A.; Sarkar, J.; Singh, N.; Meena, S.; Changkija, B.; Yadav, P.P.; Kanojiya, S.; Sinha, S. Antiproliferative action of Xylopia aethiopica fruit extract on human cervical cancer cells. Phytother. Res. 2011, 25, 1558–1563. [Google Scholar] [CrossRef] [PubMed]
- Choumessi, A.T.; Danel, M.; Chassaing, S.; Truchet, I.; Penlap, V.B.; Pieme, A.C.; Asonganyi, T.; Ducommun, B.; Valette, A. Characterization of the antiproliferative activity of Xylopia aethiopica. Cell Div. 2012, 7, 8. [Google Scholar] [CrossRef] [PubMed]
- Cavalcanti, B.C.; Bezerra, D.P.; Magalhaes, H.I.; Moraes, M.O.; Lima, M.A.; Silveira, E.R.; Camara, C.A.; Rao, V.S.; Pessoa, C.; Costa-Lotufo, L.V. Kauren-19-oic acid induces DNA damage followed by apoptosis in human leukemia cells. J. Appl. Toxicol. 2009, 29, 560–568. [Google Scholar] [CrossRef] [PubMed]
- Karasawa, T.; Steyger, P.S. An integrated view of cisplatin-induced nephrotoxicity and ototoxicity. Toxicol. Lett. 2015, 237, 219–227. [Google Scholar] [CrossRef] [PubMed]
- Tsang, R.Y.; Al-Fayea, T.; Au, H.J. Cisplatin overdose: Toxicities and management. Drug Saf. 2009, 32, 1109–1122. [Google Scholar] [CrossRef] [PubMed]
- Ataie, A.; Sabetkasaei, M.; Haghparast, A.; Moghaddam, A.H.; Kazeminejad, B. Neuroprotective effects of the polyphenolic antioxidant agent, curcumin, against homocysteine-induced cognitive impairment and oxidative stress in the rat. Pharmacol. Biochem. Behav. 2010, 96, 378–385. [Google Scholar] [CrossRef] [PubMed]
- Attia, H.N.; Al-Rasheed, N.M.; Al-Rasheed, N.M.; Maklad, Y.A.; Ahmed, A.A.; Kenawy, S.A. Protective effects of combined therapy of gliclazide with curcumin in experimental diabetic neuropathy in rats. Behav. Pharmacol. 2012, 23, 153–161. [Google Scholar] [CrossRef] [PubMed]
- Kandhare, A.D.; Raygude, K.S.; Ghosh, P.; Ghule, A.E.; Bodhankar, S.L. Therapeutic role of curcumin in prevention of biochemical and behavioral aberration induced by alcoholic neuropathy in laboratory animals. Neurosci. Lett. 2012, 511, 18–22. [Google Scholar] [CrossRef] [PubMed]
- Ravindran, J.; Prasad, S.; Aggarwal, B.B. Curcumin and cancer cells: How many ways can curry kill tumor cells selectively? AAPS J. 2009, 11, 495–510. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Lazaro, M. Anticancer and carcinogenic properties of curcumin: Considerations for its clinical development as a cancer chemopreventive and chemotherapeutic agent. Mol. Nutr. Food Res. 2008, 52 (Suppl 1), S103–S127. [Google Scholar] [CrossRef] [PubMed]
- Sharma, R.A.; Euden, S.A.; Platton, S.L.; Cooke, D.N.; Shafayat, A.; Hewitt, H.R.; Marczylo, T.H.; Morgan, B.; Hemingway, D.; Plummer, S.M.; et al. Phase i clinical trial of oral curcumin: Biomarkers of systemic activity and compliance. Clin. Cancer Res. 2004, 10, 6847–6854. [Google Scholar] [CrossRef] [PubMed]
- Kunnumakkara, A.B.; Guha, S.; Krishnan, S.; Diagaradjane, P.; Gelovani, J.; Aggarwal, B.B. Curcumin potentiates antitumor activity of gemcitabine in an orthotopic model of pancreatic cancer through suppression of proliferation, angiogenesis, and inhibition of nuclear factor-kappab-regulated gene products. Cancer Res. 2007, 67, 3853–3861. [Google Scholar] [CrossRef] [PubMed]
- Dance-Barnes, S.T.; Kock, N.D.; Moore, J.E.; Lin, E.Y.; Mosley, L.J.; D’Agostino, R.B., Jr.; McCoy, T.P.; Townsend, A.J.; Miller, M.S. Lung tumor promotion by curcumin. Carcinogenesis 2009, 30, 1016–1023. [Google Scholar] [CrossRef] [PubMed]
- National Toxicology Program. NTP toxicology and carcinogenesis studies of turmeric oleoresin (cas no. 8024-37-1) (major component 79%–85% curcumin, cas no. 458-37-7) in F344/N rats and B6C3F1 mice (feed studies). Nat. Toxicol. Program. Tech. Rep. Ser. 1993, 427, 1–275. [Google Scholar]
- Miroddi, M.; Navarra, M.; Quattropani, M.C.; Calapai, F.; Gangemi, S.; Calapai, G. Systematic review of clinical trials assessing pharmacological properties of salvia species on memory, cognitive impairment and alzheimer’s disease. CNS Neurosci. Ther. 2014, 20, 485–495. [Google Scholar] [CrossRef] [PubMed]
- Perry, N.B.; Anderson, R.E.; Brennan, N.J.; Douglas, M.H.; Heaney, A.J.; McGimpsey, J.A.; Smallfield, B.M. Essential oils from dalmatian sage (Salvia officinalis L.): Variations among individuals, plant parts, seasons, and sites. J. Agric. Food Chem. 1999, 47, 2048–2054. [Google Scholar] [CrossRef] [PubMed]
- Abu-Darwish, M.S.; Cabral, C.; Ferreira, I.V.; Goncalves, M.J.; Cavaleiro, C.; Cruz, M.T.; Al-bdour, T.H.; Salgueiro, L. Essential oil of common sage (Salvia officinalis L.) from jordan: Assessment of safety in mammalian cells and its antifungal and anti-inflammatory potential. BioMed Res. Int. 2013, 2013, 538940. [Google Scholar] [CrossRef] [PubMed]
- Vujosevic, M.; Blagojevic, J. Antimutagenic effects of extracts from sage (Salvia officinalis) in mammalian system in vivo. Acta Vet. Hung. 2004, 52, 439–443. [Google Scholar] [CrossRef] [PubMed]
- Keshavarz, M.; Bidmeshkipour, A.; Mostafaie, A.; Mansouri, K.; Mohammadi-Motlagh, H.R. Anti tumor activity of Salvia officinalis is due to its anti-angiogenic, anti-migratory and anti-proliferative effects. Yakhteh 2011, 12, 477–482. [Google Scholar]
- Hardman, W.E.; Ion, G.; Akinsete, J.A.; Witte, T.R. Dietary walnut suppressed mammary gland tumorigenesis in the c(3)1 tag mouse. Nutr. Cancer 2011, 63, 960–970. [Google Scholar] [CrossRef] [PubMed]
- Hardman, W.E.; Ion, G. Suppression of implanted mda-mb 231 human breast cancer growth in nude mice by dietary walnut. Nutr. Cancer 2008, 60, 666–674. [Google Scholar] [CrossRef] [PubMed]
- Davis, P.A.; Vasu, V.T.; Gohil, K.; Kim, H.; Khan, I.H.; Cross, C.E.; Yokoyama, W. A high-fat diet containing whole walnuts (Juglans regia) reduces tumour size and growth along with plasma insulin-like growth factor 1 in the transgenic adenocarcinoma of the mouse prostate model. Br. J. Nutr. 2012, 108, 1764–1772. [Google Scholar] [CrossRef] [PubMed]
- Reiter, R.J.; Tan, D.X.; Manchester, L.C.; Korkmaz, A.; Fuentes-Broto, L.; Hardman, W.E.; Rosales-Corral, S.A.; Qi, W.B. A walnut-enriched diet reduces the growth of lncap human prostate cancer xenografts in nude mice. Cancer Investig. 2013, 31, 365–373. [Google Scholar] [CrossRef] [PubMed]
- Nagel, J.M.; Brinkoetter, M.; Magkos, F.; Liu, X.; Chamberland, J.P.; Shah, S.; Zhou, J.R.; Blackburn, G.; Mantzoros, C.S. Dietary walnuts inhibit colorectal cancer growth in mice by suppressing angiogenesis. Nutrition 2012, 28, 67–75. [Google Scholar] [CrossRef] [PubMed]
- Becouarn, Y.; Ychou, M.; Ducreux, M.; Borel, C.; Bertheault-Cvitkovic, F.; Seitz, J.F.; Nasca, S.; Nguyen, T.D.; Paillot, B.; Raoul, J.L.; et al. Phase ii trial of oxaliplatin as first-line chemotherapy in metastatic colorectal cancer patients. J. Clin. Oncol. 1998, 16, 2739–2744. [Google Scholar] [PubMed]
- Graham, J.; Muhsin, M.; Kirkpatrick, P. Oxaliplatin. Nat. Rev. Drug Discov. 2004, 3, 11–12. [Google Scholar] [CrossRef] [PubMed]
- Pasetto, L.M.; D’Andrea, M.R.; Rossi, E.; Monfardini, S. Oxaliplatin-related neurotoxicity: How and why? Crit. Rev. Oncol. Hemat. 2006, 59, 159–168. [Google Scholar] [CrossRef] [PubMed]
- Waseem, M.; Parvez, S. Neuroprotective activities of curcumin and quercetin with potential relevance to mitochondrial dysfunction induced by oxaliplatin. Protoplasma 2016, 253, 417–430. [Google Scholar] [CrossRef] [PubMed]
- Morand, C.; Manach, C.; Crespy, V.; Remesy, C. Respective bioavailability of quercetin aglycone and its glycosides in a rat model. BioFactors 2000, 12, 169–174. [Google Scholar] [CrossRef] [PubMed]
- Raygude, K.S.; Kandhare, A.D.; Ghosh, P.; Ghule, A.E.; Bodhankar, S.L. Evaluation of ameliorative effect of quercetin in experimental model of alcoholic neuropathy in rats. Inflammopharmacology 2012, 20, 331–341. [Google Scholar] [CrossRef] [PubMed]
- Ruiz, P.A.; Braune, A.; Haller, D.R. Quercetin inhibits tnf-induced irf-1 but not nf-kappa b recruitment to the ip-10 gene promoter in intestinal epithelial cells through the modulation of histone acetyl transferase activity. Gastroenterology 2006, 130, A693–A693. [Google Scholar]
- Ferry, D.R.; Smith, A.; Malkhandi, J.; Fyfe, D.W.; DeTakats, P.G.; Anderson, D.; Baker, J.; Kerr, D.J. Phase i clinical trial of the flavonoid quercetin: Pharmacokinetics and evidence for in vivo tyrosine kinase inhibition. Clin. Cancer Res. 1996, 2, 659–668. [Google Scholar] [PubMed]
- Zaveri, N.T. Green tea and its polyphenolic catechins: Medicinal uses in cancer and noncancer applications. Life Sci. 2006, 78, 2073–2080. [Google Scholar] [CrossRef] [PubMed]
- Khan, N.; Mukhtar, H. Cancer and metastasis: Prevention and treatment by green tea. Cancer Metast. Rev. 2010, 29, 435–445. [Google Scholar] [CrossRef] [PubMed]
- Nakachi, K.; Suemasu, K.; Suga, K.; Takeo, T.; Imai, K.; Higashi, Y. Influence of drinking green tea on breast cancer malignancy among japanese patients. Jpn. J. Cancer Res. 1998, 89, 254–261. [Google Scholar] [CrossRef] [PubMed]
- Saville, M.W.; Lietzau, J.; Pluda, J.M.; Feuerstein, I.; Odom, J.; Wilson, W.H.; Humphrey, R.W.; Feigal, E.; Steinberg, S.M.; Broder, S.; et al. Treatment of hiv-associated kaposi’s sarcoma with paclitaxel. Lancet 1995, 346, 26–28. [Google Scholar] [CrossRef]
- Bharadwaj, R.; Yu, H. The spindle checkpoint, aneuploidy, and cancer. Oncogene 2004, 23, 2016–2027. [Google Scholar] [CrossRef] [PubMed]
- Grisold, W.; Cavaletti, G.; Windebank, A.J. Peripheral neuropathies from chemotherapeutics and targeted agents: Diagnosis, treatment, and prevention. Neuro-Oncology 2012, 14, 45–54. [Google Scholar] [CrossRef] [PubMed]
- Campos, A.C.; Moreira, F.A.; Gomes, F.V.; del Bel, E.A.; Guimaraes, F.S. Multiple mechanisms involved in the large-spectrum therapeutic potential of cannabidiol in psychiatric disorders. Philos. Trans. R. Soc. B 2012, 367, 3364–3378. [Google Scholar] [CrossRef] [PubMed]
- Mechoulam, R.; Parker, L.A.; Gallily, R. Cannabidiol: An overview of some pharmacological aspects. J. Clin. Pharmacol. 2002, 42 (Suppl. 1), 11S–19S. [Google Scholar] [CrossRef] [PubMed]
- Andoh, T.; Kitamura, R.; Fushimi, H.; Komatsu, K.; Shibahara, N.; Kuraishi, Y. Effects of goshajinkigan, hachimijiogan, and rokumigan on mechanical allodynia induced by paclitaxel in mice. J. Tradit. Complement. Med. 2014, 4, 293–297. [Google Scholar] [CrossRef] [PubMed]
- Materazzi, S.; Fusi, C.; Benemei, S.; Pedretti, P.; Patacchini, R.; Nilius, B.; Prenen, J.; Creminon, C.; Geppetti, P.; Nassini, R. Trpa1 and trpv4 mediate paclitaxel-induced peripheral neuropathy in mice via a glutathione-sensitive mechanism. Pflugers Arch. Eur. J. Physiol. 2012, 463, 561–569. [Google Scholar] [CrossRef] [PubMed]
- Alessandri-Haber, N.; Dina, O.A.; Joseph, E.K.; Reichling, D.B.; Levine, J.D. Interaction of transient receptor potential vanilloid 4, integrin, and src tyrosine kinase in mechanical hyperalgesia. J. Neurosci. 2008, 28, 1046–1057. [Google Scholar] [CrossRef] [PubMed]
- Goswami, C. Trpv1-tubulin complex: Involvement of membrane tubulin in the regulation of chemotherapy-induced peripheral neuropathy. J. Neurochem. 2012, 123, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Gauchan, P.; Andoh, T.; Kato, A.; Kuraishi, Y. Involvement of increased expression of transient receptor potential melastatin 8 in oxaliplatin-induced cold allodynia in mice. Neurosci. Lett. 2009, 458, 93–95. [Google Scholar] [CrossRef] [PubMed]
- Mizuno, K.; Kono, T.; Suzuki, Y.; Miyagi, C.; Omiya, Y.; Miyano, K.; Kase, Y.; Uezono, Y. Goshajinkigan, a traditional japanese medicine, prevents oxaliplatin-induced acute peripheral neuropathy by suppressing functional alteration of trp channels in rat. J. Pharmacol. Sci. 2014, 125, 91–98. [Google Scholar] [CrossRef] [PubMed]
- Matsumura, Y.; Yokoyama, Y.; Hirakawa, H.; Shigeto, T.; Futagami, M.; Mizunuma, H. The prophylactic effects of a traditional japanese medicine, goshajinkigan, on paclitaxel-induced peripheral neuropathy and its mechanism of action. Mol. Pain 2014, 10, 61. [Google Scholar] [CrossRef] [PubMed]
- Bifulco, M.; Malfitano, A.M.; Pisanti, S.; Laezza, C. Endocannabinoids in endocrine and related tumours. Endocr. Relat. Cancer 2008, 15, 391–408. [Google Scholar] [CrossRef] [PubMed]
- McKallip, R.J.; Lombard, C.; Fisher, M.; Martin, B.R.; Ryu, S.H.; Grant, S.; Nagarkatti, P.S.; Nagarkatti, M. Targeting cb2 cannabinoid receptors as a novel therapy to treat malignant lymphoblastic disease. Blood 2002, 100, 627–634. [Google Scholar] [CrossRef] [PubMed]
- Li, R.; Wang, H.; Bekele, B.N.; Yin, Z.; Caraway, N.P.; Katz, R.L.; Stass, S.A.; Jiang, F. Identification of putative oncogenes in lung adenocarcinoma by a comprehensive functional genomic approach. Oncogene 2006, 25, 2628–2635. [Google Scholar] [CrossRef] [PubMed]
- Ramer, R.; Rohde, A.; Merkord, J.; Rohde, H.; Hinz, B. Decrease of plasminogen activator inhibitor-1 may contribute to the anti-invasive action of cannabidiol on human lung cancer cells. Pharm. Res. 2010, 27, 2162–2174. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.M.; Lehky, T.J.; Brell, J.M.; Dorsey, S.G. Discovering cytokines as targets for chemotherapy-induced painful peripheral neuropathy. Cytokine 2012, 59, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Chiurchiu, V.; Leuti, A.; Maccarrone, M. Cannabinoid signaling and neuroinflammatory diseases: A melting pot for the regulation of brain immune responses. J. Neuroimmune Pharmacol. 2015, 10, 268–280. [Google Scholar] [CrossRef] [PubMed]
| Phytochemical | Dose | Chemotherapy | Effects | Refs. |
|---|---|---|---|---|
Auraptenol 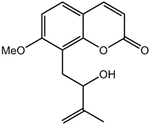 | 0.05–0.8 mg/kg | Vincristine in mice | Suppresses mechanical hyperalgesia and alteration of behavioral and biochemical changes | [22] |
Cannabidiol  | 2.5–10 mg/kg | Paclitaxel in mice | Inhibits neuropathic pain through 5-HT1A receptor signaling without diminishing chemothferapy efficacy or nervous system function | [23] |
Curcumin  | 10 mg/kg | Cisplatin or oxaliplatin in rats | Reverses the alterations of neurotensin levels in the plasma, protects the sciatic nerve from injury, and reduces drug absorption in the sciatic nerve | [24] |
Rutin  & quercetin 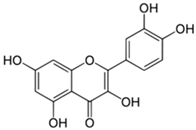 | 25–100 mg/kg | Oxaliplatin in rats | prevent the shrinkage of neurons and inhibit edema | [25] |
Verticinone 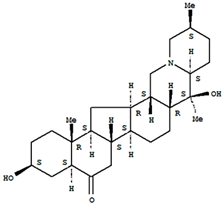 | 1.5–3 mg/kg | Paclitaxel in rats | Has a relatively constant analgesic effect; the analgesic effect of morphine was decreased after repeated medication | [26] |
Xylopic acid  | 10–100 mg/kg | Vincristine in rats | Has anti-allodynic and anti-hyperalgesic properties | [27] |
| Herbs | Dose | Chemotherapy | Effects | Refs. |
|---|---|---|---|---|
| Acorus calamus | 100–200 mg/kg | Vincristine in rats | Attenuates symptoms of neuropathy through serotonin 5-HT1A receptors | [28] |
| Butea monosperma | 200–400 mg/kg | Vincristine in rats | Reverses alterations of behavioral, biochemical, and histopathological changes | [29] |
| Ginkgo biloba L. | 50–150 mg/kg | Vincristine in rats | Decreases paw-withdrawal frequency to cold stimuli and increases the threshold to mechanical stimuli Suppresses NF-κB activation and production of TNF-α and NO Inhibits axonal degradation Improves axonal transportation | [30] |
| 100–200 mg/kg | Cisplatin in rats, mice, guinea pigs | Protects the inner ear from ototoxicity | [31] | |
| Camellia sinensis | 300 mg/kg | Oxaliplatin in rats | Alleviates mechanical allodynia and thermal hyperalgesia, but does not prevent morphometric or electrophysiological alterations | [32] |
| Ocimum sanctum | 100–200 mg/kg | Vincristine in rats | Attenuates neurotoxicity with the decline in calcium levels and oxidative stress | [33] |
| Salvia officinalis | 100 mg/kg | Cisplatin in mice, | Suppresses a second phase of cisplatin-enhanced pain in the formalin test | [34] |
| Walnut | 6% of diet | Cisplatin in rats | Inhibits an alteration in performance of hippocampus- and cerebellum-related behaviors | [35] |
| Xylopia aethiopica | 30–300 mg/kg | Vincristine in rats | Has anti-allodynic and anti-hyperalgesic properties | [27] |
| Herbal Formula | Herbs Composition | Chemotherapy | Effects | Refs. |
|---|---|---|---|---|
| Gyejigachulbu-Tang | Aconiti tuber, Atractylodis lanceae rhizome, Cinnamomi cortex, Glycyrrhizae radix, Paeoniae radix, Zingiberis rhizoma, Zizyphi fructus | Oxaliplatin in rats | Attenuates cold and mechanical allodynia Suppresses spinal glia activation | [36] |
| Gyeryongtongrac-Bang | Ramulus cinnamomi, Earthworm, Radix astragali, Safflower, Radix angelicae sinensis, Ligusticum, Spatholobus, Radix paeoniae alba, Rhizoma curcumae, Licorice | Oxaliplatin in a randomized, double-blind, placebo-controlled trial | Prevents sensory neurotoxicity and delays its onset | [37] |
| Hwanggiomul-Tang | Zingiberis hizome, Jujubae fructus, Paeonia alba radix, Cinnamomi cortex, Astragalus membranaceus radix | A case study of oxaliplatin-treated 59-year-old man with recurrent colon cancer | Prevents chronic cumulative neurotoxicity | [38] |
| Jakyakgamcho-Tang | Paeoniae radix, Glycyrrhizae radix | Paclitaxel in mice | Relieves allodynia and a hyperalgesia | [39] |
| A retrospective case analysis investigated 23 patients with ovarian cancer treated with paclitaxel and carboplatin combination chemotherapy | Reduces pain in epithelial ovarian carcinoma | [40] | ||
| Jesengsingi-Hwan | Achyranthis bidentatae radix, Alismatis rhizome, Aconiti tuber, Cinnamomi cortex, Corni fructus, Dioscorea opposita rhizoma, Plantaginis semen, Poria alba, Moutan cortex, Rehmannia viride radix | Oxaliplatin in rats | Reduces peripheral neuropathy without influence on anti-cancer potency Ameliorates abnormal sensations and histological damage to the sciatic nerve | [41,42] |
| Paclitaxel in mice | Inhibits mechanical allodynia | [43] | ||
| Oxaliplatin in a placebo-controlled double-blind randomized study | Delays onset of grade 2 or greater peripheral neurotoxicity without impairing FOLFOX efficacy with an acceptable safety margin | [44,45] | ||
| Prevents exacerbation of peripheral neuropathy | [46,47] | |||
| A clinical trial enrolling 82 patients | Reduces peripheral neuropathy | [48] |
© 2016 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, G.; Kim, S.K. Therapeutic Effects of Phytochemicals and Medicinal Herbs on Chemotherapy-Induced Peripheral Neuropathy. Molecules 2016, 21, 1252. https://doi.org/10.3390/molecules21091252
Lee G, Kim SK. Therapeutic Effects of Phytochemicals and Medicinal Herbs on Chemotherapy-Induced Peripheral Neuropathy. Molecules. 2016; 21(9):1252. https://doi.org/10.3390/molecules21091252
Chicago/Turabian StyleLee, Gihyun, and Sun Kwang Kim. 2016. "Therapeutic Effects of Phytochemicals and Medicinal Herbs on Chemotherapy-Induced Peripheral Neuropathy" Molecules 21, no. 9: 1252. https://doi.org/10.3390/molecules21091252
APA StyleLee, G., & Kim, S. K. (2016). Therapeutic Effects of Phytochemicals and Medicinal Herbs on Chemotherapy-Induced Peripheral Neuropathy. Molecules, 21(9), 1252. https://doi.org/10.3390/molecules21091252






