Anti-Inflammatory Activity of Natural Products
Abstract
:1. Introduction
2. Review Articles of Natural Non-Plant Materials
3. Review Articles on Natural Plant Materials
4. Active Anti-Inflammatory Plant Extracts, Essential Oils, Juices and Powders
5. Selected Reports of Single Natural Products with Anti-Inflammatory Activities
6. Concluding Remarks
Conflicts of Interest
References
- Artis, D.; Spits, H. The biology of innate lymphoid cells. Nature 2015, 517, 293–301. [Google Scholar] [CrossRef] [PubMed]
- Isailovic, N.; Daigo, K.; Mantovani, A.; Selmi, C. Interleukin-17 and innate immunity in infections and chronic inflammation. J. Autoimmun. 2015, 60, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Pedraza-Alva, G.; Pérez-Martínez, L.; Valdez-Hernández, L.; Meza-Sosa, K.F.; Ando-Kuri, M. Negative regulation of the inflammasome: Keeping inflammation under control. Immunol. Rev. 2015, 265, 231–257. [Google Scholar] [CrossRef] [PubMed]
- Lucas, S.M.; Rothwell, N.J.; Gibson, R.M. The role of inflammation in CNS injury and disease. Br. J. Pharmacol. 2006, 147, S232–S240. [Google Scholar] [CrossRef] [PubMed]
- Rock, K.L.; Lai, J.J.; Kono, H. Innate and adaptive immune responses to cell death. Immunol. Rev. 2011, 243, 191–205. [Google Scholar] [CrossRef] [PubMed]
- Fernandes, J.V.; Cobucci, R.N.; Jatobá, C.A.; Fernandes, T.A.; de Azevedo, J.W.; de Araújo, J.M. The role of the mediators of inflammation in cancer development. Pathol. Oncol. Res. 2015, 21, 527–534. [Google Scholar] [CrossRef] [PubMed]
- Heppner, F.L.; Ransohoff, R.M.; Becher, B. Immune attack: The role of inflammation in Alzheimer disease. Nat. Rev. Neurosci. 2015, 16, 358–372. [Google Scholar] [CrossRef] [PubMed]
- Loane, D.J.; Kumar, A. Microglia in the TBI brain: The good, the bad, and the dysregulated. Exp. Neurol. 2016, 275, 316–327. [Google Scholar] [CrossRef] [PubMed]
- Waisman, A.; Liblau, R.S.; Becher, B. Innate and adaptive immune responses in the CNS. Lancet Neurol. 2015, 14, 945–955. [Google Scholar] [CrossRef]
- Vignali, D.A.; Kuchroo, V.K. IL-12 family cytokines: immunological playmakers. Nat. Immun. 2012, 13, 722–728. [Google Scholar] [CrossRef] [PubMed]
- Montgomery, S.L.; Bowers, W.J. Tumor necrosis factor-alpha and the roles it plays in homeostatic and degenerative processes within the central nervous system. J. Neuroimmune. Pharmacol. 2012, 7, 42–59. [Google Scholar] [CrossRef] [PubMed]
- Zelová, H.; Hošek, J. TNF-α signalling and inflammation: interactions between old acquaintances. Inflamm. Res. 2013, 62, 641–651. [Google Scholar] [CrossRef] [PubMed]
- Fenton, M.J. Review: Transcriptional and post-transcriptional regulation of interleukin 1 gene expression. Int. J. Immunopharmacol. 1992, 14, 401–411. [Google Scholar] [CrossRef]
- Rider, P.; Carmi, Y.; Voronov, E.; Apte, R.N. Interleukin-1α. Semin. Immunol. 2013, 25, 430–438. [Google Scholar] [CrossRef] [PubMed]
- Langrish, C.L.; McKenzie, B.S.; Wilson, N.J.; de Waal Malefyt, R.; Kastelein, R.A.; Cua, D.J. IL-12 and IL-23: master regulators of innate and adaptive immunity. Immunol. Rev. 2004, 202, 96–105. [Google Scholar] [CrossRef] [PubMed]
- Duvallet, E.; Semerano, L.; Assier, E.; Falgarone, G.; Boissier, M.C. Interleukin-23: A key cytokine in inflammatory diseases. Ann. Med. 2011, 43, 503–511. [Google Scholar] [CrossRef] [PubMed]
- Sabat, R. IL-10 family of cytokines. Cytokine Growth Factor Rev. 2010, 21, 315–324. [Google Scholar] [CrossRef] [PubMed]
- Ng, T.H.; Britton, G.J.; Hill, E.V.; Verhagen, J.; Burton, B.R.; Wraith, D.C. Regulation of adaptive immunity; The role of interleukin-10. Front. Immunol. 2013, 31, 129. [Google Scholar] [CrossRef] [PubMed]
- Kwilasz, A.J.; Grace, P.M.; Serbedzija, P.; Maier, S.F.; Watkins, L.R. The therapeutic potential of interleukin-10 in neuroimmune diseases. Neuropharmacology 2015, 96, 55–69. [Google Scholar] [CrossRef] [PubMed]
- Goetzl, E.J.; An, S.; Smith, W.L. Specificity of expression and effects of eicosanoid mediators in normal physiology and human diseases. FASEB J. 1995, 9, 1051–1058. [Google Scholar] [PubMed]
- Leff, J.A.; Busse, W.W.; Pearlman, D.; Bronsky, E.A.; Kemp, J.; Hendeles, L.; Dockhorn, R.; Kundu, S.; Zhang, J.; Seidenberg, B.C.; et al. Montelukast, a leukotriene-receptor antagonist, for the treatment of mild asthma and exercise-induced bronchoconstriction. N. Engl. J. Med. 1998, 339, 147–152. [Google Scholar] [CrossRef] [PubMed]
- Peters-Golden, M.; Henderson, W.R. Leukotrienes. N. Engl. J. Med. 2007, 357, 1841–1854. [Google Scholar] [CrossRef] [PubMed]
- Zhao, J.; Quyyumi, A.A.; Patel, R.; Zafari, A.M.; Veledar, E.; Onufrak, S.; Shallenberger, L.H.; Jones, L.; Vaccarino, V. Sex-specific association of depression and a haplotype in leukotriene A4 hydrolase gene. Psychosom. Med. 2009, 71, 691–696. [Google Scholar] [CrossRef] [PubMed]
- Moncada, S.; Bolanos, J.P. Nitric oxide, cell bioenergetics and neurodegeneration. J. Neurochem. 2006, 97, 1676–1689. [Google Scholar] [CrossRef] [PubMed]
- Rayet, B.; Gélinas, C. Aberrant rel/nfkb genes and activity in human cancer. Oncogene 1999, 18, 6938–6947. [Google Scholar] [CrossRef] [PubMed]
- Oeckinghaus, A.; Hayden, M.S.; Ghosh, S. Crosstalk in NF-κB signaling pathways. Nat. Immunol. 2011, 12, 695–708. [Google Scholar] [CrossRef] [PubMed]
- Ling, J.; Kumar, R. Crosstalk between NFkB and glucocorticoid signaling: A potential target of breast cancer therapy. Cancer Lett. 2012, 322, 119–126. [Google Scholar] [CrossRef] [PubMed]
- Khalifa, A.B. Herbs: Nature's Pharmacy, 1st ed.; Arab Cultural Center: Casablanca, Morocco, 2004; pp. 286–288. [Google Scholar]
- Lindequist, U.; Niedermeyer, T.H.J.; Jülich, W.D. The pharmacological potential of mushrooms. Evid. Based Complement. Altern. Med. 2005, 2, 285–299. [Google Scholar] [CrossRef] [PubMed]
- Elsayed, E.A.; El Enshasy, H.; Wadaan, M.A.M.; Aziz, R. Mushrooms: A potential natural source of anti-inflammatory compounds for medical applications. Mediat. Inflamm. 2014. [Google Scholar] [CrossRef] [PubMed]
- Ngai, P.H.K.; Zhao, Z.; Ng, T.B. Agrocybin, an antifungal peptide from the edible mushroom Agrocybe cylindracea. Peptides 2005, 26, 191–196. [Google Scholar] [CrossRef] [PubMed]
- Rosa, L.H.; Souza-Fagundes, E.M.; Machado, K.M.G.; Alves, T.M.A.; Martins-Filho, O.A.; Romanha, A.J.; Oliveira, R.C.; Rosa, C.A.; Zani, C.L. Cytotoxic, immunosuppressive and trypanocidal activities of agrocybin, a polyacetylene produced by Agrocybe perfecta (Basidiomycota). World J. Microb. Biot. 2006, 22, 539–545. [Google Scholar] [CrossRef]
- U.S. National Library of Medicine, National Center for Biotechnology Information: Agrocybin (PubChem CID 11004). Available online: https://pubchem.ncbi.nlm.nih.gov/compound/Agrocybin#section=Top (accessed on 30 September 2016).
- Yaghoobi, R.; Kazerouni, A.; Kazerouni, O. Evidence for clinical use of honey in wound healing as an anti-bacterial, anti-inflammatory anti-oxidant and anti-viral agent: A review. Jundishapur J. Nat. Pharm. Prod. 2013, 8, 100–104. [Google Scholar] [CrossRef] [PubMed]
- Vallianou, N.G.; Gounari, P.; Skourtis, A.; Panagos, J.; Kazazis, C. Honey and its anti-inflammatory, anti-bacterial and anti-oxidant properties. Gen. Med. 2014, 2. [Google Scholar] [CrossRef]
- Deharo, E.; Ginsburg, H. Analysis of additivity and synergism in the anti-plasmodial effect of purified compounds from plant extracts. Malar. J. 2011, 10. [Google Scholar] [CrossRef] [PubMed]
- Umar, M.I.; Asmawi, M.Z.; Sadikun, A.; Abdul Majid, A.M.S.; Atangwho, I.J.; Ahamed, M.B.K.; Altaf, R.; Ahmad, A. Multi-constituent synergism is responsible for anti-inflammatory effect of Azadirachta indica leaf extract. Pharm. Biol. 2014, 52, 1411–1422. [Google Scholar] [CrossRef] [PubMed]
- Hammer, K.D.; Hillwig, M.L.; Solco, A.K.; Dixon, P.M.; Delate, K.; Murphy, P.A.; Wurtele, E.S.; Birt, D.F. Inhibition of prostaglandin E2 production by anti-inflammatory Hypericum perforatum extracts and constituents in RAW 264.7 mouse macrophage cells. J. Agric. Food Chem. 2007, 55, 7323–7331. [Google Scholar] [CrossRef] [PubMed]
- Perez, S.G.; Zavala, M.S.; Arias, L.G.; Ramos, M.L. Anti-inflammatory activity of some essential oils. J. Essent. Oil Res. 2011, 23, 38–44. [Google Scholar] [CrossRef]
- Sharopov, F.; Braun, M.S.; Gulmurodov, I.; Khalifaev, D.; Isupov, S.; Wink, M. Antimicrobial, antioxidant, and anti-inflammatory activities of essential oils of selected aromatic plants from Tajikistan. Foods 2015, 4, 645–653. [Google Scholar] [CrossRef]
- Nasri, S.; Anoush, M.; Khatami, N. Evaluation of analgesic and anti-inflammatory effects of fresh onion juice in experimental animals. Afr. J. Pharm. Pharmacol. 2012, 6, 1679–1684. [Google Scholar]
- Jayanthi, M.K.; Dhar, M. Anti-inflammatory effects of Allium sativum (garlic) in experimental rats. Biomedicine 2011, 31, 84–89. [Google Scholar]
- Zakaria, Z.A.; Sulaiman, M.R.; Arifah, A.K.; Mat Jais, A.M.; Somchit, M.N.; Kirisnaveni, K.; Punnitharrani, D.; Safarul, M.; Fatimah, C.A.; Johari, R. The anti-inflammatory and antipyretic activities of Corrchorus olotorius in rats. J. Pharm. Toxicol. 2006, 1, 139–146. [Google Scholar]
- Islam, M.R.; Mannan, M.A.; Kabir, M.H.B.; Islam, A.; Olival, K.J. Analgesic, anti-inflammatory and antimicrobial effects of ethanol extracts of mango leaves. J. Bangladesh Agril. Univ. 2010, 8, 239–244. [Google Scholar] [CrossRef]
- Li, C.; Wang, M.H. Anti-inflammatory effect of the water fraction from hawthorn fruit on LPS-stimulated RAW 264.7 cells. Nutr. Res. Pract. 2011, 5, 101–106. [Google Scholar] [CrossRef] [PubMed]
- Abu-Gharbieh, E.; Shehab, N.G.; Khan, S.A. Anti-inflammatory and gastroprotective activities of the aqueous extract of Micromeria fruticosa (L.) Druce ssp Serpyllifolia in mice. Pak. J. Pharm. Sci. 2013, 26, 799–803. [Google Scholar] [PubMed]
- Falcão, H.S.; Lima, I.O.; Santos, V.L.; Dantas, H.F.; Diniz, M.F.F.M.; Barbosa-Filho, J.M.; Batista, L.M. Review of the plants with anti-inflammatory activity studied in Brazil. Braz. J. Pharmacog. 2005, 15, 381–391. [Google Scholar] [CrossRef]
- Watzl, B. Anti-inflammatory effects of plant-based foods and of their constituents. Int. J. Vitam. Nutr. Res. 2008, 78, 293–298. [Google Scholar] [CrossRef] [PubMed]
- Aravindaram, K.; Yang, N.S. Anti-inflammatory plant natural products for cancer therapy. Planta Med. 2010, 76, 1103–1117. [Google Scholar] [CrossRef] [PubMed]
- Arya, V.; Arya, M.L. A review on anti-inflammatory plant barks. Int. J. PharmTech Res. 2011, 3, 899–908. [Google Scholar]
- Shah, B.N.; Seth, A.K.; Maheshwari, K.M. A review on medicinal plants as a source of anti-inflammatory agents. Res. J. Med. Plant. 2011, 5, 101–115. [Google Scholar] [CrossRef]
- Beg, S.; Swain, S.; Hasan, H.; Abul Barkat, M.; Hussain, S. Systematic review of herbals as potential anti-inflammatory agents: Recent advances, current clinical status and future perspectives. Pharmacogn. Rev. 2011, 5, 120–137. [Google Scholar] [CrossRef] [PubMed]
- Lucas, L.; Russell, A.; Keast, R. Molecular mechanisms of inflammation. Anti-inflammatory benefits of virgin olive oil and the phenolic compound oleocanthal. Curr. Pharm. Des. 2011, 17, 754–768. [Google Scholar] [CrossRef]
- Sengupta, R.; Sheorey, S.D.; Hinge, M.A. Analgesic and anti-inflammatory plants: an updated review. Int. J. Pharm. Sci. Rev. Res. 2012, 12, 114–119. [Google Scholar]
- Shilpi, J.A.; Islam, M.E.; Billah, M.; Islam, K.M.D.; Sabrin, F.; Uddin, S.J.; Nahar, L.; Sarker, S.D. Antinociceptive, anti-inflammatory, and antipyretic activity of mangrove plants: A mini review. Adv. Pharmacol. Sci. 2012, 576086. [Google Scholar] [CrossRef] [PubMed]
- Kumar, S.; Bajwa, B.S.; Kuldeep, S.; Kalia, A.N. Anti-inflammatory activity of herbal plants: A review. Int. J. Adv. Pharm. Biol. Chem. 2013, 2, 272–281. [Google Scholar]
- Wei, W.C.; Sung, P.J.; Duh, C.Y.; Chen, B.W.; Sheu, J.H.; Yang, N.S. Anti-inflammatory activities of natural products isolated from soft corals of Taiwan between 2008 and 2012. Mar. Drugs 2013, 11, 4083–4126. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.C.; Hou, M.F.; Huang, H.W.; Chang, F.R.; Yeh, C.C.; Tang, J.Y.; Chang, H.W. Marine algal natural products with anti-oxidative, anti-inflammatory, and anti-cancer properties. Cancer Cell Int. 2013, 13. [Google Scholar] [CrossRef] [PubMed]
- Bajpai, S.; Pathak, R.; Hussain, T. Anti-inflammatory activity of ethnobotanical plants used as traditional medicine: A review. Res. Rev. J. Bot.Sci. 2014, 3, 8–18. [Google Scholar]
- Fürst, R.; Zündorf, I. Plant-derived anti-inflammatory compounds: Hopes and disappointments regarding the translation of preclinical knowledge into clinical progress. Mediat. Inflamm. 2014, 146832. [Google Scholar] [CrossRef] [PubMed]
- Schäfer, G.; Kaschula, C.H. The immunomodulation and anti-Inflammatory effects of garlic organosulfur compounds in cancer chemoprevention. Anticancer Agents Med. Chem. 2014, 14, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Arreola, R.; Quintero-Fabián, S.; López-Roa, R.I.; Flores-Gutiérrez, E.O.; Reyes-Grajeda, J.P.; Carrera Quintanar, L.; Ortuño-Sahagún, D. Immunomodulation and anti-Inflammatory effects of garlic compounds. J. Immunol. Res. 2015. [Google Scholar] [CrossRef] [PubMed]
- Bhagyasri, Y.; Lavakumar, V.; Divya Sree, M.S.; Ashok Kumar, C.K. An overview on anti-inflammatory activity of Indian herbal plants. Int. J. Res. Pharm. Nano Sci. 2015, 4, 1–9. [Google Scholar]
- González, Y.; Torres-Mendoza, D.; Jones, G.E.; Fernandez, P.L. Marine diterpenoids a potential anti-inflammatory agents. Mediators Inflamm. 2015, 263543. [Google Scholar] [CrossRef] [PubMed]
- Parhiz, H.; Roohbakhsh, A.; Soltani, F.; Ramin Rezaee, R.; Iranshahi, M. Antioxidant and anti-inflammatory properties of the citrus flavonoids hesperidin and hesperetin: An updated review of their molecular mechanisms and experimental models. Phytother. Res. 2015, 29, 323–331. [Google Scholar] [CrossRef] [PubMed]
- Karunaweera1, N.; Raju, R.; Gyengesi, E.; Münch, G. Plant polyphenols as inhibitors of NF-kB induced cytokine production—A potential anti-inflammatory treatment for Alzheimer’s disease? Front. Mol. Neurosci. 2015, 8. [Google Scholar] [CrossRef]
- Cheung, R.C.F.; Ng, T.B.; Wong, J.H.; Chen, Y.; Chan, W.Y. Marine natural products with anti-inflammatory activity. Appl. Microbiol. Biotechnol. 2016, 100, 1645–1666. [Google Scholar] [CrossRef] [PubMed]
- Maione, F.; Russo, R.; Khan, H.; Mascolo, N. Medicinal plants with anti-inflammatory activities. Nat. Prod. Res. 2016, 30, 1343–1353. [Google Scholar] [CrossRef] [PubMed]
- Stohs, S.J.; Bagchi, D. Antioxidant, anti-inflammatory, and chemoprotective properties of Acacia catechu heartwood extracts. Phytother. Res. 2015, 29, 818–824. [Google Scholar] [CrossRef] [PubMed]
- Mascolo, N.; Autore, G.; Capasso, F.; Menghini, A.; Fasulo, M.P. Biological screening of Italian medicinal plants for anti-inflammatory activity. Phytother. Res. 1987, 1, 28–31. [Google Scholar] [CrossRef]
- Badilla, B.; Mora, G.; Poveda, L.J. Anti-inflammatory activity of aqueous extracts of five Costa Rican medicinal plants in Sprague-Dawley rats. Rev. Siol. Trop. 1999, 47, 723–727. [Google Scholar]
- Chan, K.; Islam, M.W.; Kamil, M.; Radhakrishnan, R.; Zakaria, M.N.M.; Habibullah, M.; Attas, A. The analgesic and anti-inflammatory effects of Portulaca oleracea L. subsp. Sativa (Haw.) Celak. J. Ethnopharmacol. 2000, 73, 445–451. [Google Scholar] [CrossRef]
- Kim, Y.O.; Lee, S.W.; Na, S.W.; Park, H.R.; Son, E.S. Anti-inflammatory effects of Portulaca oleracea L. on the LPS-induced RAW 264.7 cells. J. Med. Plants Res. 2015, 9, 407–411. [Google Scholar]
- Agyare, C.; Baiden, E.; Apenteng, J.A.; Boakye, Y.D.; Adu-Amoah, L. Anti-infective and anti-inflammatory properties of Portulaca oleracea L. Donn. J. Med. Plnt. Res. 2015, 2, 2041–2064. [Google Scholar]
- Baricevic, D.; Sosa, S.; Della Loggia, R.; Tubaro, A.; Simonovska, B.; Krasna, A.; Zupancic, A. Topical anti-inflammatory activity of Salvia officinalis L. leaves: the relevance of ursolic acid. J. Ethnopharmacol. 2001, 75, 125–132. [Google Scholar] [CrossRef]
- Qnais, E.Y.; Abu-Dieyeh, M.; Abdulla, F.A.; Abdalla, S.S. The antinociceptive and anti-inflammatory effects of Salvia officinalis leaf aqueous and butanol extracts. Pharm. Biol. 2010, 48, 1149–1156. [Google Scholar] [CrossRef] [PubMed]
- Boukhary, R.; Raafat, K.; Ghoneim, A.I.; Aboul-Ela, M.; El-Lakany, A. Anti-Inflammatory and antioxidant activities of Salvia fruticosa: An HPLC determination of phenolic contents. Evid. Based Complement. Altern. Med. 2016, 2016, 7178105. [Google Scholar]
- Owoyele, B.V.; Adebukola, O.M.; Funmilayo, A.A.; Soladoye, A.O. Anti-inflammatory activities of ethanolic extract of Carica papaya leaves. Inflammopharmacology 2008, 16, 168–173. [Google Scholar] [CrossRef] [PubMed]
- Choudhary, M.I.; Jalil, A.S.; Nawaz, S.A.; Khan, K.M.; Tareen, R.B.; Atta-ur-Rahman. Antiinflammatory and lipoxygenase inhibitory compounds from Vitex agnus-castus. Phytother. Res. 2009, 23, 1336–1339. [Google Scholar] [CrossRef] [PubMed]
- Loizzo, M.R.; Menichini, F.; Conforti, F.; Tundis, R.; Bonesi, M.; Saab, A.M.; Statti, G.A.; de Cindio, B.; Houghton, P.J.; Menichini, F.; et al. Chemical analysis, antioxidant, antiinflammatory and anticholinesterase activities of Origanum ehrenbergii Boiss and Origanum syriacum L. essential oils. Food Chem. 2009, 117, 174–180. [Google Scholar] [CrossRef]
- Jaijoy, K.; Soonthornchareonnon, N.; Panthong, A.; Sireeratawong, S. Anti-inflammatory and analgesic activities of the water extract from the fruit of Phyllanthus emblica Linn. Int. J. Appl. Res. Nat. Prod. 2010, 3, 28–35. [Google Scholar]
- Huang, Y.S.; Ho, S.C. Polymethoxy flavones are responsible for the anti-inflammatory activity of citrus fruit peel. Food Chem. 2010, 119, 868–873. [Google Scholar] [CrossRef]
- Rahman, M.; Chowdhury, J.A.; Habib, R.; Saha, B.K.; Salauddin, A.D. Islam, M.K. Anti-inflammatory, anti-arthritic and analgesic activity of the alcoholic extract of the plant Urginea indica Kunth. Int. J. Pharm. Sci. Res. 2011, 2, 2915–2919. [Google Scholar]
- Ravipati, A.S.; Zhang, L.; Koyyalamudi, S.R.; Jeong, S.J.; Reddy, N.; Bartlett, J.; Smith, P.T.; Shanmugam, K.; Münch, G.; Wu, M.J.; et al. Antioxidant and anti-inflammatory activities of selected Chinese medicinal plants and their relation with antioxidantcontent. BMC Complement. Altern. Med. 2012, 12. [Google Scholar] [CrossRef] [PubMed]
- Diaz, P.; Jeong, S.C.; Lee, S.; Khoo, C.; Koyyalamudi, S.R. Antioxidant and anti-inflammatory activities of selected medicinal plants and fungi containing phenolic and flavonoid compounds. Chin. Med. 2012, 7. [Google Scholar] [CrossRef] [PubMed]
- Yasmeen, N.; Sujatha, K. Evaluation of anti-inflammatory activity of ethanolic whole plant extract of Desmodium gangeticum L. Int. J. Phytomed. 2013, 5, 347–349. [Google Scholar]
- Saravana, K.K.; Nagaveni, P.; Anitha, K.; Mahaboob, S.T.M. Evaluation of anti-inflammatory activity on Vitex negundo Linn. J. Drug Deliv. Ther. 2013, 3, 41–44. [Google Scholar]
- Komalavalli, K.; Nithya, P.Y.; Sabapathy, M.; Mohan, V.R. Antiinflammatory activity of whole plant of Sonerila tinnevelliensis Fischer (Melastomataceae). Int. J. Pharmacol. Res. 2013, 3, 74–76. [Google Scholar]
- Yousuf, P.H.; Noba, N.Y.; Shohel, M.; Bhattacherjee, R.; Das, B.K. Analgesic, anti-inflammatory and antipyretic effect of Mentha spicata (Spearmint). Br. J. Pharm. Res. 2013, 3, 854–864. [Google Scholar] [CrossRef]
- Prudente, A.S.; Loddi, A.M.V.; Duarte, M.R.; Santos, A.R.S.; Pochapski, M.T.; Pizzolatti, M.G.; Hayashi, S.S.; Campos, F.R.; Pontarolo, R.; Fabio, A.; et al. Pre-clinical anti-inflammatory aspects of a cuisine and medicinal millennial herb: Malva sylvestris L. Food Chem. Toxicol. 2013, 58, 324–331. [Google Scholar] [CrossRef] [PubMed]
- Fezai, M.; Senovilla, L.; Jemaà, M.; Ben-Attia, M. Analgesic, anti-Inflammatory and anticancer activities of extra virgin olive oil. J. Lipids 2013, 129736. [Google Scholar] [CrossRef] [PubMed]
- Rosillo, M.A.; Alcaraz, M.J.; Sánchez-Hidalgo, M.; Fernández-Bolaños, J.G.; Alarcón-de-la-Lastra, C.; Ferrándiz, M.L. Anti-inflammatory and joint protective effects of extra-virgin olive-oil polyphenol extract in experimental arthritis. J. Nutr. Biochem. 2014, 25, 1275–1281. [Google Scholar] [CrossRef] [PubMed]
- Benso, B.; Rosalen, P.L.; Severino Matias Alencar, S.M.; Murata, R.M. Malva sylvestris inhibits inflammatory response in oral human cells. An in vitro infection model. PLoS ONE 2015, 10. [Google Scholar] [CrossRef] [PubMed]
- Kaladhar, D.S.V.G.K.; Swathi, S.K.; Varahalarao, V.; Nagendra, S.Y. Evaluation of anti-inflammatory and anti-proliferative activity of Abutilon indicum L. plant ethanolic leaf extract on lung cancer cell line A549 for system network studies. J. Cancer Sci. Ther. 2014, 6, 188–194. [Google Scholar]
- Tag, H.M.; Kelany, O.E.; Tantawy, H.M.; Fahmy, A.A. Potential anti-inflammatory effect of lemon and hot pepper extracts on adjuvant-induced arthritis in mice. J. Basic Appl. Zoo. 2014, 67, 149–157. [Google Scholar] [CrossRef]
- Adebayo, S.A.; Dzoyem, J.P.; Shai, L.J.; Eloff, J.N. The anti-inflammatory and antioxidant activity of 25 plant species used traditionally to treat pain in southern African. BMC Complement. Altern. Med. 2015, 15. [Google Scholar] [CrossRef] [PubMed]
- Serafini, M.R.; de Oliveira Barreto, E.; de Almeida Brito, F.; Almeida dos Santos, J.P.; dos Santos Lima, B.; Banderó Walker, C.I.; Amaral da Silva, F.; Quintans-Junior, L.J.; Gelain, D.P.; de Souza Araújo, A.A. Anti-inflammatory property and redox profile of the leaves extract from Morinda citrifolia L. J. Med. Plants Res. 2015, 9, 693–701. [Google Scholar]
- Da Costa, G.A.; Morais, M.G.; Saldanha, A.A.; Assis Silva, I.C.; Aleixo, A.A.; Ferreira, J.M.; Soares, A.C.; Duarte-Almeida, J.M.; Lima, L.A. Antioxidant, antibacterial, cytotoxic, and anti-inflammatory potential of the leaves of Solanum lycocarpum A. St. Hil. (Solanaceae). Evid. Based Complement. Altern. Med. 2015, 2015, 315987. [Google Scholar]
- Gupta, A.; Chaphalkar, S.R. Terpenoids from three medicinal plants and their potential anti-inflammatory and immunosuppressive activity on human whole blood and peripheral blood mononuclear cells. Asian J. Ethnopharmacol. Med. Foods 2016, 2, 13–17. [Google Scholar]
- Medicherla, K.; Ketkar, A.; Sahu, B.D.; Sudhakar, G.; Sistla, R. Rosmarinus officinalis L. extract ameliorates intestinal inflammation through MAPKs/NF-κB signaling in a murine model of acute experimental colitis. Food Funct. 2016, 7, 3233–3243. [Google Scholar] [CrossRef] [PubMed]
- Walker, J.; Reichelt, K.V.; Obst, K.; Widder, S.; Hans, J.; Krammer, G.E.; Ley, J.P.; Somoza, V. Identification of an anti-inflammatory potential of Eriodictyon angustifolium compounds in human gingival fibroblasts. Food Funct. 2016, 7, 3046–3055. [Google Scholar] [CrossRef] [PubMed]
- Ghate, N.B.; Das, A.; Chaudhuri, D.; Panja, S.; Mandal, N. Sundew plant, a potential source of anti-inflammatory agents, selectively induces G2/M arrest and apoptosis in MCF-7 cells through upregulation of p53 and Bax/Bcl-2 ratio. Cell Death Discov. 2016, 2. [Google Scholar] [CrossRef] [PubMed]
- Lachkar, N.; Al-Sobarry, M.; El Hajaji, H.; Lamkinsi, T.; Lachkar, M.; Cherrah, Y.; Alaoui, K. Anti-inflammatory and antioxidant effect of Ceratonia siliqua L. methanol barks extract. J. Chem. Pharm. Res. 2016, 8, 202–210. [Google Scholar]
- Campana, P.R.; Mansur, D.S.; Gusman, G.S.; Ferreira, D.; Teixeira, M.M.; Braga, F.C. Anti-TNF-α activity of Brazilian medicinal plants and compounds from Ouratea semiserrata. Phytother. Res. 2015, 29, 1509–1515. [Google Scholar] [CrossRef] [PubMed]
- Riedel, R.; Marrassini, C.; Anesini, C.; Gorzalczany, S. Anti-inflammatory and antinociceptive activity of Urera aurantiaca. Phytother. Res. 2015, 29, 59–66. [Google Scholar] [CrossRef] [PubMed]
- Uto, T.; Tung, N.H.; Taniyama, R.; Miyanowaki, T.; Morinaga, O.; Shoyama, Y. Anti-inflammatory activity of constituents isolated from aerial part of Angelica acutiloba kitagawa. Phytother. Res. 2015, 29, 1956–1963. [Google Scholar] [CrossRef] [PubMed]
- Iii Colado-Velázquez, J.; Mailloux-Salinas, P.; Medina-Contreras, J.; Cruz-Robles, D.; Bravo, G. Effect of Serenoa repens on oxidative stress, inflammatory and growth factors in obese Wistar rats with benign prostatic hyperplasia. Phytother. Res. 2015, 29, 1525–1531. [Google Scholar] [CrossRef] [PubMed]
- Kumar, R.; Gupta, Y.K.; Singh, S.; Arunraja, S. Picrorhiza kurroa inhibits experimental arthritis through inhibition of pro-inflammatory cytokines, angiogenesis and MMPs. Phytother. Res. 2016, 30, 112–119. [Google Scholar] [CrossRef] [PubMed]
- Rtibi, K.; Selmi, S.; Jabri, M.A.; Mamadou, G.; Limas-Nzouzi, N.; Sebai, H.; El-Benna, J.; Marzouki, L.; Eto, B.; Amri, M. Effects of aqueous extracts from Ceratonia siliqua L. pods on small intestinal motility in rats and jejunal permeability in mice. RSC Adv. 2016, 6, 44345–44353. [Google Scholar] [CrossRef]
- Rtibi, K.; Jabri, M.A.; Selmi, S.; Sebai, H.; Amri, M.; El-Benna, J.; Marzouki, L. Ceratonia siliqua leaves exert a strong ROS scavenging effect in human neutrophils, inhibit myeloperoxydase in vitro and protect against intestinal fluid and electrolytes secretion in rats. RSC Adv. 2016, 6, 65483–65493. [Google Scholar] [CrossRef]
- Campbell, W.C.; Fisher, M.H.; Stapley, E.O.; Albers-Schonberg, G.; Jacob, T.A. Ivermectin: A potent new antiparasitic agent. Science 1983, 221, 823–828. [Google Scholar] [CrossRef] [PubMed]
- Gupta, M.B.; Bhalla, T.N.; Gupta, G.P.; Mitra, C.R.; Bhargava, K.P. Anti-inflammatory activity of natural products (I) Triterpenoids. Eur. J. Pharmacol. 1969, 6, 67–70. [Google Scholar] [CrossRef]
- Guardia, T.; Rotelli, A.E.; Juarez, A.O.; Pelzer, L.E. Anti-inflammatory properties of plant flavonoids. Effects of rutin, quercetin and hesperidin on adjuvant arthritis in rat. Il Farmaco 2001, 56, 683–687. [Google Scholar] [CrossRef]
- Bose, S.; Laha, B.; Banerjee, S. Anti-inflammatory activity of isolated allicin from garlic with post-acoustic waves and microwave radiation. J. Adv. Pharm. Edu. Res. 2013, 3, 512–515. [Google Scholar]
- Silva, R.O.; Salvadori, M.S.; Sousa, F.B.M.; Santos, M.S.; Carvalho, N.S.; Sousa, D.P.; Gomes, B.S.; Oliveira, F.A.; Barbosa, A.L.R.; Freitas, R.M.; et al. Evaluation of the anti-inflammatory and antinociceptive effects of myrtenol, a plant-derived monoterpene alcohol, in mice. Flavour Fragr. J. 2014, 29, 184–192. [Google Scholar] [CrossRef]
- Thao, N.P.; Luyen, B.T.T.; Koo, J.E.; Kim, S.; Koh, Y.S.; Thanh, N.V.; Cuong, N.X.; Kiem, P.V.; Minh, C.V.; Kim, H.Y. In vitro anti-inflammatory components isolated from the carnivorous plant Nepenthes mirabilis (Lour.) Rafarin. Pharm. Biol. 2016, 54, 588–594. [Google Scholar] [CrossRef] [PubMed]
- Navarrete, S.; Alarcón, M.; Palomo, I. Aqueous extract of tomato (Solanum lycopersicum L.) and ferulic acid reduce the expression of TNF-α and IL-1β in LPS-activated macrophages. Molecules 2015, 20, 15319–15329. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.; Kwak, J.H.; Pyo, S. Inhibition of LPS-induced inflammatory mediators by 3-hydroxyanthranilic acid in macrophages through suppression of PI3K/NF-κB signaling pathways. Food Funct. 2016, 7, 3073–3082. [Google Scholar] [CrossRef] [PubMed]
- Aquino, R.; De Feo, V.; De Simone, F.; Pizza, C.; Cirino, C. Plant metabolites. New compounds and antiinflammatory activity of Uncaria tomentosa. J. Nat. Prod. 1991, 54, 453–459. [Google Scholar] [CrossRef] [PubMed]
- Checker, R.; Sandur, S.K.; Sharma, D.; Patwardhan, R.S.; Jayakumar, S.; Kohli, V.; Sethi, G.; Aggarwal, B.B.; Sainis, K.B. Potent anti-inflammatory activity of ursolic acid, a triterpenoid antioxidant, is mediated through suppression of NF-kB, AP-1 and NF-AT. PLoS ONE 2012, 7. [Google Scholar] [CrossRef] [PubMed]
- Yesilada, E.; Tanaka, S.; Sezik, E.; Tabata, M. Isolation of an anti-inflammatory principle from the juice of Ecballium elaterium. J. Nat. Prod. 1988, 51, 504–508. [Google Scholar] [CrossRef] [PubMed]
- Yesilada, E.; Tanaka, S.; Tabata, M.; Sezik, E. Antiinflammatory effects of the fruit juice of Ecballium elaterium on edemas in mice. Phytother. Res. 1989, 3, 75–76. [Google Scholar] [CrossRef]
- Jayaprakasam, B.; Seeram, N.P.; Nair, M.G. Anticancer and antiinflammatory activities of cucurbitacins from Cucurbita andreana. Cancer Lett. 2003, 189, 11–16. [Google Scholar] [CrossRef]
- Oliveira, T.T.; Campos, K.M.; Cerqueira-Lima, A.T.; Brasil Carneiro, T.C.; da Silva Velozo, E.; Alexandrino Ribeiro Melo, I.C.; Abrantes Figueiredo, E.; de Jesus Oliveira, E.; Silva Amorim de Vasconcelos, D.F.; Pontes-de-Carvalho, L.C.; et al. Potential therapeutic effect of Allium cepa L. and quercetin in a murine model of Blomia Tropicalis induced asthma. DARU J. Pharm. Sci. 2015, 23. [Google Scholar] [CrossRef] [PubMed]
- Shin, J.H.; Ryu, J.H.; Kang, M.J.; Hwang, C.R.; Han, J.; Kang, D. Short-term heating reduces the anti-inflammatory effects of fresh raw garlic extracts on the LPS-induced production of NO and pro-inflammatory cytokines by downregulating allicin activity in RAW 264.7 macrophages. Food Chem. Toxicol. 2013, 58, 545–551. [Google Scholar] [CrossRef] [PubMed]
- Rufino, A.T.; Ribeiro, M.; Judas, F.; Salgueiro, L.; Lopes, M.C.; Cavaleiro, C.; Mendes, A.F. Anti-inflammatory and chondroprotective activity of (+)-α-pinene: structural and enantiomeric selectivity. J. Nat. Prod. 2014, 77, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, S.; Tajima, M.; Tsukada, M.; Tabata, M. A comparative study of anti-inflammatory activities of the enantiomers, shikonin and alkannin. J. Nat. Prod. 1986, 49, 466–469. [Google Scholar] [CrossRef] [PubMed]
- Peng, X.; Nie, Y.; Wu, J.; Huang, Q.; Cheng, Y. Juglone prevents metabolic endotoxemia-induced hepatitis and neuroinflammation via suppressing TLR4/NF-κB signaling pathway in high-fat diet rats. Biochem. Biophys. Res. Commun. 2015, 462, 245–250. [Google Scholar] [CrossRef] [PubMed]

| Main Theme of the Article | Major Method(s) of Testing | Major Active Materials/Compounds | Main Effects on Inflammation * | Ref. |
|---|---|---|---|---|
| Brazilian plants | Inflammation induction in rats and mice (e.g., by carrageenan) | Plants parts, various extracts, chromatographic fractions | Significant inhibition of COX and 5-LOX activity; reduction in edema volume | [47] |
| Plant-based foods | Plant-based food consumption in humans | Carotenoids, flavonoids, phenolic acids, monoterpenes, sulfides | Reduction in C-reactive protein (CRP) and IL-6 levels; inhibition of NFκB | [48] |
| Plant natural products | Various in vitro and in vivo models of inflammation (e.g., lipopolysaccharide [LPS]-induced) and cancer | Polyphenols, capsaicin, curcumin, ascorbic acid, indol-3-carbinol, geraniol, sulphoraphane, gingerol, lycopene, deoxyelephantophin | Significant reduction in cytokines levels; inhibition of COX-2, iNOS, NFκB and STAT (signal transducers and activators of transcription) activity | [49] |
| Plant barks | Various inflammation models in vivo (e.g., carrageenan-induced paw edema) | Various extracts, oleanolic acid, polyphenols, coumarin, β-amyrin, ursolic acid, β-sitosterol | Significant inhibition of COX and iNOS activity; attenuation of paw edema | [50] |
| Medicinal plants (General) | Various inflammation models in vivo (e.g., carrageenan-induced paw edema) | Various extracts; ambrosanolide, betulinic acid, ardisiaquinone G, polyphenols and others | Inhibition of COX, iNOS, 5-LOX and PLA2 activity; attenuation of paw edema | [51] |
| Herbal drugs (medicinal plants) | Various in vitro and in vivo (animals) models of inflammation; clinical trials in humans including safety and efficacy measures | Detailed compound families (e.g., alkaloids, glycosides, terpenoids, resins, essential oils, fatty acids, flavonoids, polysaccharides, phenolic compounds, steroids, cannabinoids, glycoproteins) | Significant reduction in cytokines, LTs, PGs and NO levels; inhibition of COX, iNOS, 5-LOX, PLA2 and NFκB activity; in humans: analgesic effects in different pain states, reduction of edema, attenuation of inflammatory measures | [52] |
| Virgin olive oil | Various in vitro and in vivo models of inflammation; clinical trials in humans | The phenolic compound oleocanthal | Reduction in cytokines, CRP, LTs, and PGs levels; inhibition of COX, iNOS, 5-LOX and NFκB activity | [53] |
| Medicinal plants | Various in vitro and in vivo models of inflammation | Whole plant or parts; alkaloids, glycosides, essential oils, fatty acids, flavonoids, nyctanthic acid, phyllanthin, and many others | Analgesic effects and reduction of inflammatory measures | [54] |
| Mangrove plants | Various in vitro and in vivo models of inflammation | Various extracts, pure compounds such as: agallochaol O, eugenol, mimosol D, calophyllolide | Reduction in cytokines, LTs, NO and PGs levels; inhibition of COX, iNOS, 5-LOX and NFκB activity | [55] |
| Herbal plants | Various in vitro and in vivo models of inflammation | Various extracts, plants parts, resins | Significant reduction in cytokines, LTs, NO and PGs levels; inhibition of COX, iNOS and 5-LOX activity | [56] |
| Marine natural products from soft corals | Various in vitro and in vivo models of inflammation (e.g., LPS-induced inflammation) | Sesquiterpenoids, diterpenoids, steroids, ceramide, cerebrosides, and many others (a comprehensive review with 339 structures) | Reduction in cytokines, NO and PGs levels; inhibition of COX and iNOS activity | [57] |
| Marine natural products of algal origin | Various in vitro and in vivo models of inflammation (e.g., LPS-induced inflammation) | Various extracts and pure compounds such as neorogioltriol, (12Z)-cis-maneonene-D | Reduction in IL-6, TNF-α, NO and PGs levels; inhibition of COX, iNOS, NFκB and STAT activity | [58] |
| Ethnobotanical plants | Carrageenan-induced paw edema | Various extracts | Significant reduction in edema volume; effects were similar to those of other anti-inflammatory drugs such as valdecoxib, sulindac, aspirin, diclofenac, ibuprofen, phenylbutazone and indomethacin | [59] |
| Plant-derived compounds | Various in vitro and in vivo models of inflammation; pre-clinical tests and clinical trials in humans | Curcumin, colchicine, resveratrol, capsaicin, epigallocatechin-3-gallate, quercetin | Reduction in cytokines, LTs and PGs levels; inhibition of COX-2, 5-LOX and NFκB activity; in humans: attenuation of inflammatory measures such as CRP, IL-1β, IL-6, and TNF-α | [60] |
| Active organosulfur compounds in garlic | Various in vitro and in vivo animals models (LPS-induced inflammation); studies in human volunteers and pre-clinical studies | Ajoene, diallyl sulfide, diallyl disulfide, allylmethyl sulfide, S-allyl cysteine, alliin, allicin | Anti-inflammatory: reduction in PGs, NO, IL-1β, IL6 and TNF-α levels; increase in IL-10 levels; inhibition of COX-2, iNOS and NFκB activity Pro-inflammatory: opposite effects of the mentioned above | [61] |
| Active organosulfur compounds and extracts of garlic | Various in vitro and in vivo animals models (e.g., LPS-induced inflammation); studies in humans | Aqueous, oil, chloroform and n-hexane extracts, as well as compounds in previous raw | Anti-inflammatory: reduction in IL-1β, IL-6 and TNF-α levels; increase in IL-10 levels; inhibition of NFκB activity Pro-inflammatory: increase in NO, IFN-γ and TNF-α levels | [62] |
| Indian medicinal plants | Various in vitro and in vivo models | Polyphenols, lignans, anthraquinones, flavonoids, alkaloids, terpenoids, saponins, polysaccharides | Reduction in TNF-α and other cytokines levels; inhibition of PLA2 activity; general–anti-inflammatory, analgesic and anti-allergic effects | [63] |
| Marine diterpenoids | Various in vitro and in vivo models (e.g., LPS-induced inflammation) | Eunicellane, briarane, cembrane and other diterpenoids | Significant reduction in IL-6, TNF-α, NO, PGs and LTs levels; significant inhibition of COX-2, iNOS, 5-LOX and NFκB activity, some of the effects were comparable to those of anti-inflammatory drugs such as indomethacin | [64] |
| Citrus flavonoids | Various in vitro and in vivo animal models (e.g., LPS-induced inflammation), healthy human volunteers | Hesperidin and hesperetin—two major flavonoids of citrus | Reduction in IL-1β, IL-6, TNF-α, NO and PGs levels; inhibition of COX-2, iNOS and NFκB activity; reduction in plasma CRP levels in humans | [65] |
| Plant polyphenols | Various in vitro and in vivo animal models (e.g., LPS-induced inflammation) | Plant polyphenols such as curcumin, apigenin, quercetin, E-cinnamaldehyde and E-resveratrol | Reduction in IL-1β, IL-6, TNF-α, NO and PGs levels; inhibition of COX-2, iNOS and NFκB activity | [66] |
| Marine natural products | Various in vitro and in vivo animal models (e.g., LPS or carrageenan-induced inflammation) | Detailed structures of 35 marine compounds such as steroids, fatty acids, diterpenes, sesquiterpenoids, alkaloids and polysaccharides | Significant reduction in IL-1β, IL-6, TNF-α, NO and PGs levels; significant inhibition of COX-2, iNOS and NFκB activity | [67] |
| Medicinal plants | Various in vitro and in vivo animal models (e.g., LPS-induced inflammation) | Isogarcinol, andrograpanin, hinokitiol, tectorigenin, α-iso-cubebene, schisantherin A, psoralidin, formosumone A, isofraxidin, maslinic acid, mangiferin | Reduction in IL-1β, IL-6, TNF-α, NO and PGs levels; inhibition of COX-2 and iNOS activity | [68] |
| Acacia catechu (Mimosaceae); in most reviewed studies extracts of A. catechu were combined with extracts of Scutellaria baicalensis | LPS-induced inflammation in vitro (cell lines and primary cells); arachidonic acid-induced inflammation and edema in mice ear; randomized, double-blind trial in patients with osteoarthritis | Catethin, epicatechin, flavonoids | In-vitro studies in cells—a mixture of A. catechu and S. baicalensis significantly reduced mRNA levels of COX, IL-1β, TNF-α and IL-6, and decreased the activity of NF-κB in LPS-stimulated cells; ear edema in mice—a mixture of A. catechu and S. baicalensis significantly attenuated COX and 5-LOX activity in the ear; osteoarthritis patients—a blend of A. catechu and S. baicalensis extracts (500 mg/day) led to a significant reduction in joint pain intensity (the effect was stronger than that of naproxen 440 mg/day) and, on the other hand, significantly increased plasma levels of IL-1β and TNF-α | [69] |
| Extracting Solvent(s) | Major Method(s) of Testing | Plant Species | Main Effects on Inflammation * | Ref. |
|---|---|---|---|---|
| 80% EtOH in H2O | Carrageenan-induced paw edema in rats (for assessing inflammation) | 75 species of medicinal plants that grow in Italy | Four species caused a significant reduction in paw edema similar to that seen under treatment with indomethacin. Other species exerted a less prominent edema-reducing effect | [70] |
| H2O | Carrageenan-induced paw edema in rats | Five species of Costa Rican medicinal plants: Loasa speciciosa, Loasa triphylla, Urtica leptuphylla, Urera baccifera, Chaptalia nutans | Four species caused a significant reduction in paw edema, similar to that seen under treatment with indomethacin | [71] |
| 10% EtOH in H2O | Hot-plate method for assessing analgesia; carrageenan-induced paw edema | Portulaca oleracea L. subsp. sativa (Haw.) Celak | A significant reduction in paw edema and an analgesic effect, similar to that of diclofenac | [72] |
| H2O | LPS-induced inflammation in a macrophage cell line (RAW 264.7 cells) | Portulaca oleracea L. | A significant reduction in IL-6, TNF-α, NO and PGE2 levels; decrease in iNOS expression; effects were more prominent than those of indomethacin | [73] |
| 70% MeOH in H2O | Carrageenan-induced paw edema in chicks | Portulaca oleracea L. | A significant dose-dependent reduction in paw edema which was stronger than that seen under treatment with aspirin | [74] |
| n-Hexane, CHCl3, MeOH | Croton oil-induced ear edema in mice | Salvia officinalis L. (main active component is ursolic acid) | n-Hexane and CHCl3 extracts prominently reduced ear edema; MeOH extract had a weak effect while the essential oil was ineffective; the significant effect of ursolic acid was 2-fold stronger in reducing the edema than indomethacin | [75] |
| H2O, n-BuOH | Hot-plate method in mice; cotton pellet granuloma and carrageenan-induced paw edema in rats | Salvia officinalis L. | The H2O and BuOH extracts had a marked analgesic effect; both extracts significantly and dose-dependently reduced pellet granuloma and paw edema-effects were comparable to those of indomethacin | [76] |
| CHCl3, MeOH, EtOAc, n-BuOH | Carrageenan-induced paw edema in mice | Salvia fruticosa | A significant reduction in paw edema similar to that seen under treatment with diclofenac | [77] |
| H2O | Carrageenan-induced paw edema and yeast-induced pyrexia in rats | Corchorus olitorius | A significant reduction in paw edema which was stronger than that of aspirin; attenuation of hyperthermia (fever) | [43] |
| EtOH | Carrageenan-induced paw edema and cotton pellet-induced granuloma in rats | Carica papaya | A significant reduction in paw edema and pellet granuloma; effects were similar to those of indomethacin | [78] |
| MeOH | In-vitro assays for measuring neutrophils inflammation and lipoxygenase activity | Vitex agnus-castus; 10 compounds were extracted | Three compounds had a significant anti-inflammatory activity; two compounds inhibited the activity of lipoxygenase | [79] |
| Essential oils | LPS-induced inflammation in RAW 264.7 cells | Origanum ehrenbergii Boiss, Origanum syriacum L. | O. ehrenbergii caused a significant decrease in NO production | [80] |
| H2O | Ethyl phenylpropiolate and arachidonic acid-induced ear edema, carrageenan-induced paw edema, and cotton pellet-induced granuloma in rats | Phyllanthus emblica Linn. | Significant inhibition of ear inflammation and a reduction in paw edema and pellet granuloma—effects were similar to those of aspirin; the extract exerted an analgesic effect | [81] |
| MeOH | LPS-induced inflammation in RAW 264.7 cells | Citrus paradis, C. limon (L.) Bur, C. kotokan Hayata, C. sinensis (L.) Osbec, C. reticulata Blanco, C. reticulata x C. sinensis, C. tankan Hayata | A significant, dose-dependent reduction in PGE2 and NO levels; a significant decrease in COX-2 and iNOS expression | [82] |
| MeOH | Acetic acid-induced writhing in mice; carrageenan-induced paw edema in rats | Mangifera indica | A non-significant reduction in paw edema; a significant analgesic effect similar to that of diclofenac | [44] |
| MeOH | Hot-plate method in mice; cotton pellet granuloma and carrageenan-induced paw edema in rats | Urginea indica Kunth | Anti-inflammatory and analgesic effects, a significant reduction in paw edema; effects were similar to those of ibuprofen | [83] |
| 70% MeOH in H2O, then, in different solvents | LPS-induced inflammation in RAW 264.7 cells | Crataegus pinnatifida Bunge var. typica Schneider | The aqueous extract caused a significant reduction in NO levels; and, a significant dose-dependent decrease in COX-2, IL-1β, IL-6 and TNF-α expression | [45] |
| H2O, EtOH | Inflammation induced by LPS and INF-γ in RAW 264.7 cells | 40 Chinese plant species | Several extracts caused a significant reduction in NO and TNF-α levels | [84] |
| H2O, EtOH | Inflammation induced by LPS and INF-γ in J774A.1 cells | 13 Chinese plant species and two fungi | Some extracts caused a significant reduction in NO and TNF-α levels | [85] |
| EtOH | Carrageenan-induced paw edema in rats | Desmodium gangeticum | A significant reduction in paw edema | [86] |
| n-Hexane, EtOAc, CHCl3, EtOH | Cotton pellet granuloma and carrageenan-induced paw edema in rats | Vitex negundo Linn; only the ethanolic extract was tested for biological activity | A significant decrease in paw edema and a modest reduction in pellet granuloma; effects were similar to those of indomethacin | [87] |
| EtOH | Carrageenan-induced paw edema in rats | Sonerila tinnevelliensis Fischer | A significant decrease in paw edema which was similar to that of indomethacin | [88] |
| MeOH | Hot-plate test & acetic acid-induced writhing in mice; carrageenan-induced paw edema in rats; yeast-induced pyrexia in rats | Mentha spicata L. | Significant dose-dependent analgesic effect, anti-inflammatory effect (reduction in paw edema) and antipyretic effect; effects were similar to those of reference drugs such as ketorolac and paracetamol | [89] |
| H2O | Carrageenan-induced paw edema in mice | Micromeria fruticosa | A significant reduction in paw edema; effect was similar to that of indomethacin | [46] |
| EtOH | 12-O-tetradecanoylphorbol-acetate-induced ear edema in mice | Malva sylvestris L | A significant dose-dependent reduction in ear edema; a decrease in IL-1β levels and leukocytes migration to the tissue; effects were less potent than those of dexamethasone | [90] |
| Extra virgin olive oil | Acetic acid-induced writhing and formalin tests in mice; carrageenan-induced paw edema in rats | Olea europaea | A significant analgesic effect similar to that of aspirin; a significant reduction in paw edema similar to that seen under treatment with dexamethasone | [91] |
| 80% MOH in H2O | Collagen-induced arthritis in mice | Polyphenol extract of extra virgin olive oil (Olea europaea) | A significant reduction in joint edema and bone loss; a significant decline in leukocytes migration; a decrease in PGE2, IL-1β, IL-6 and TNF-α levels; a significant reduction in COX-2 expression and NFκB activity, among other anti-inflammatory effects | [92] |
| EtOH and fractionation with n-hexane, CHCl3, EtOAc | Aggregatibacter actinomycetemcomitans-induced infection and inflammation in human oral cells (in vitro model) | Malva sylvestris | A significant reduction in protein levels of multiple pro-inflammatory mediators (e.g., IL-1β, IL-6, IL-8) and a decrease in their gene expression | [93] |
| EtOH | Assessment of 5-LOX activity in lung cancer cell line A549 | Abutilon indicum L. | A significant reduction in 5-LOX activity | [94] |
| EtOH | Adjuvant-induced arthritis in mice | Citrus x limon, Capsicum annuum L. | A significant decrease in CRP, IL-1β, IL-6 and TNF-α levels; a significant reduction in arthritis | [95] |
| Acetone | LPS-induced inflammation in RAW 264.7 cells; assessment of 15-LOX activity | 25 South African plant species | A significant reduction in NO levels; significant inhibition of 15-LOX activity | [96] |
| H2O | Carrageenan-induced paw edema in mice | Morinda citrifolia L. | A significant reduction in TNF-α levels; a significant decline in leukocytes migration; effects were comparable to those of indomethacin | [97] |
| EtOH and fractionation with n-hexane, CH2Cl2, EtOAc | Carrageenan-induced paw edema in mice | Solanum lycocarpum A. St. Hil. | A significant reduction in paw edema which was similar to that seen under treatment with indomethacin | [98] |
| EtOH then petroleum ether | Human peripheral blood cells stimulated with different antigens | Azadirachta indica, Acacia catechu, Salmalia malabarica (terpenoids were extracted) | A significant dose-dependent reduction in NO levels; a decrease in leukocytes count | [99] |
| MeOH | LPS-induced inflammation in RAW 264.7 cells; dextran sulfate sodium-induced colitis in mice | Rosmarinus officinalis L. | A significant dose-dependent decrease in nitrites, IL-6 and TNF-α levels; a significant reduction in COX-2 and iNOS expression; a significant decline in NFκB activity, among other inflammatory markers that were attenuated | [100] |
| 90% EtOH in H2O | LPS-induced inflammation in human gingival fibroblasts | Eriodictyon angustifolium, 8 active compounds were extracted | A significant reduction in IL-6, IL-8 and MCP-1 levels | [101] |
| 70% MeOH in H2O | LPS-induced inflammation in RAW 264.7 cells | Drosera burmannii Vahl. (insectivorous herb, sundew) | A significant dose-dependent decrease in nitrites and TNF-α levels; a significant dose-dependent reduction in COX-2 and iNOS expression | [102] |
| n-Hexane, CH2Cl2, EtOAc, MeOH | Carrageenan and experimental trauma-induced paw edema in mice and rats | Ceratonia siliqua L. | A significant dose-dependent reduction in paw edema which was similar to that seen under treatment with indomethacin | [103] |
| EtOH, acetone | LPS-induced release of TNF-α in THP-1 cells | Fourteen non-toxic extracts derived from six plants: Cuphea carthagenensis (Lythraceae), Echinodorus grandiflorus (Alismataceae), Mansoa hirsuta (Bignoniaceae), Ouratea semiserrata (Ochnaceae), Ouratea spectabilis and Remijia ferruginea (Rubiaceae); three non-toxic active compounds were extracted from O. semiserrata: epicatechin, lanceoloside A and rutin | Seven active extracts significantly reduced (>80% inhibition) TNF-α production. The effects of the extracts were comparable to that of dexamethasone (0.1 μM); epicatechin, lanceoloside A and rutin significantly decreased the release of TNF-α by approximately 67%, 65% and 42%, respectively | [104] |
| CH2Cl2, EtOAc, MeOH | Ear edema in mice; carrageenan-induced paw edema in rats; acetic acid-induced abdominal writhing and alteration of vascular permeability in mice | Urera aurantiaca Wedd. (Urticaceae) | A significant reduction in ear edema and myeloperoxidase activity in mice and rats (effects were less potent than those of indomethacin); a significant decrease in vascular permeability in mice (effect was comparable to that of indomethacin); a significant anti-nociceptive effect in mice which was comparable to that of indomethacin | [105] |
| MeOH | LPS-induced inflammation in RAW 264 cells | Angelica acutiloba | A significant decrease in NO, PGE2, IL-6 and TNF-α levels; a significant increase in heme oxygenase-1 expression, suggesting enhanced anti-inflammatory activity | [106] |
| H2O, EtOH | A testosterone-induced benign prostatic hyperplasia model in obese rats | Serenoa repens | A significant reduction in IL-1β, IL-6, NO and TNF-α levels | [107] |
| EtOH in H2O | Formaldehyde and adjuvant-induced Arthritis in rats | Picrorhiza kurroa | A significant reduction in synovial expression of IL-1β, IL-6 and TNF-α; a significant decrease in paw edema; a significant decline in NO levels and leukocytes infiltration to the inflamed joints; all the effects were comparable to those of indomethacin | [108] |
| Compound(s) | Major Method(s) of Testing | Plants with High Concentration of the Compound(s) | Main Effects on Inflammation | Ref. |
|---|---|---|---|---|
| Triterpenes: α/β-amyrin acetate, nimbin, filicene, oleanolic acid | Carrageenan and formaldehyde-induced paw edema in rats | Thymus serpyllum, Syzygium aromaticum, Salvia triloba, Rosmarinus officinalis, Origanum majorana, Ligustrum lucidum, Lavandula latifolia | A significant reduction in edema volume; effects were comparable to those of hydrocortisone | [112] |
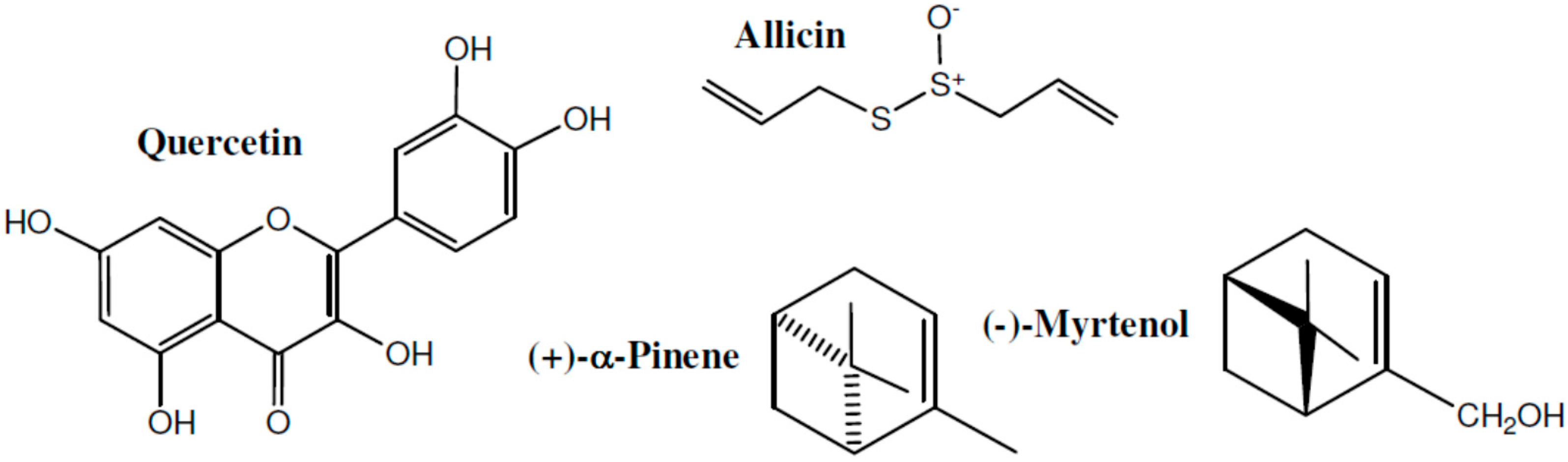
| Quercetin | Adjuvant and carrageenan-induced arthritis in rats (acute and chronic designs) | Allium cepa, Camellia sinensis, Hypericum perforatum, Podophyllum peltatum | A significant reduction in edema volume both in the acute and chronic models; effects were comparable to those of phenylbutazone | [113] |
| Allicin | Carrageenan-induced paw edema in rats | Allium sativum (garlic) | A significant reduction in edema volume which was similar to that of diclofenac | [114] |
| (−)-Myrtenol | Various models in mice: paw edema induced by various compounds, and, carrageenan-induced peritonitis (inflammation); acetic acid-induced writhing, hot-plate test, and, paw licking induced by formalin, glutamate, and capsaicin (nociception) | Tanacetum vulgare, Aralia cachemirica | A significant reduction in edema volume comparable to that of indomethacin; a significant decrease in IL-1β levels; a significant decline in leukocytes count; an significant analgesic effect which was comparable to that of morphine in most tests | [115] |
| Various terpenes and polyphenols | Inflammation induced by LPS in bone marrow derived dendritic cells | Nepenthes mirabilis (Lour.) Rafarin (Carnivorous plant) | A significant reduction in IL-6, IL-12 and TNF-α levels | [116] |
| Ferulic acid | LPS-induced inflammation in macrophages (in-vitro) | Solanum lycopersicum L. (Tomato) | A significant decrease in IL-1β and TNF-α expression; a significant reduction in NFκB activity | [117] |
| 3-Hydroxyanthranilic acid | LPS-induced inflammation in RAW 264.7 cells and in mouse peritoneal macrophages | Hibiscus tilliaceus | A significant decrease in NO, IL-1β, IL-6 and TNF-α expression; a significant increase in IL-10 expression; a significant reduction in NFκB activity | [118] |
© 2016 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Azab, A.; Nassar, A.; Azab, A.N. Anti-Inflammatory Activity of Natural Products. Molecules 2016, 21, 1321. https://doi.org/10.3390/molecules21101321
Azab A, Nassar A, Azab AN. Anti-Inflammatory Activity of Natural Products. Molecules. 2016; 21(10):1321. https://doi.org/10.3390/molecules21101321
Chicago/Turabian StyleAzab, Abdullatif, Ahmad Nassar, and Abed N. Azab. 2016. "Anti-Inflammatory Activity of Natural Products" Molecules 21, no. 10: 1321. https://doi.org/10.3390/molecules21101321
APA StyleAzab, A., Nassar, A., & Azab, A. N. (2016). Anti-Inflammatory Activity of Natural Products. Molecules, 21(10), 1321. https://doi.org/10.3390/molecules21101321






