Comparative Diagnostic Techniques for Cryptosporidium Infection
Abstract
:1. Introduction
2. Results and Discussion
2.1. Demographic Information of Study Subjects
| Sex | HIV-Positive Subjects (%) | HIV-Negative Subjects (%) | Control Subjects (%) | |
|---|---|---|---|---|
| Males 11 (6.1) | Males 34 (18.9) | Males 10 (5.6) | ||
| Female 24 (13.3) | Females 91 (50.6) | Female 10 (5.6) | ||
| 18–30 | 2 (1.1) | 8 (4.4) | 2 (1.1) | |
| 31–43 | 13 (7.2) | 34 (18.9) | 8 (4.4) | |
| 44–56 | 5 (2.8) | 11 (6.1) | 4 (2.2) | |
| 57–69 | 10 (5.6) | 31 (17.2) | 1 (0.56) | |
| 70–82 | 3 (1.7) | 25 (13.9) | 3 (1.7) | |
| 83–95 | 2 (1.1) | 16 (8.9) | 2 (1.1) | |
2.2. Detection of Cryptosporidium Oocysts: Microscopic Technique
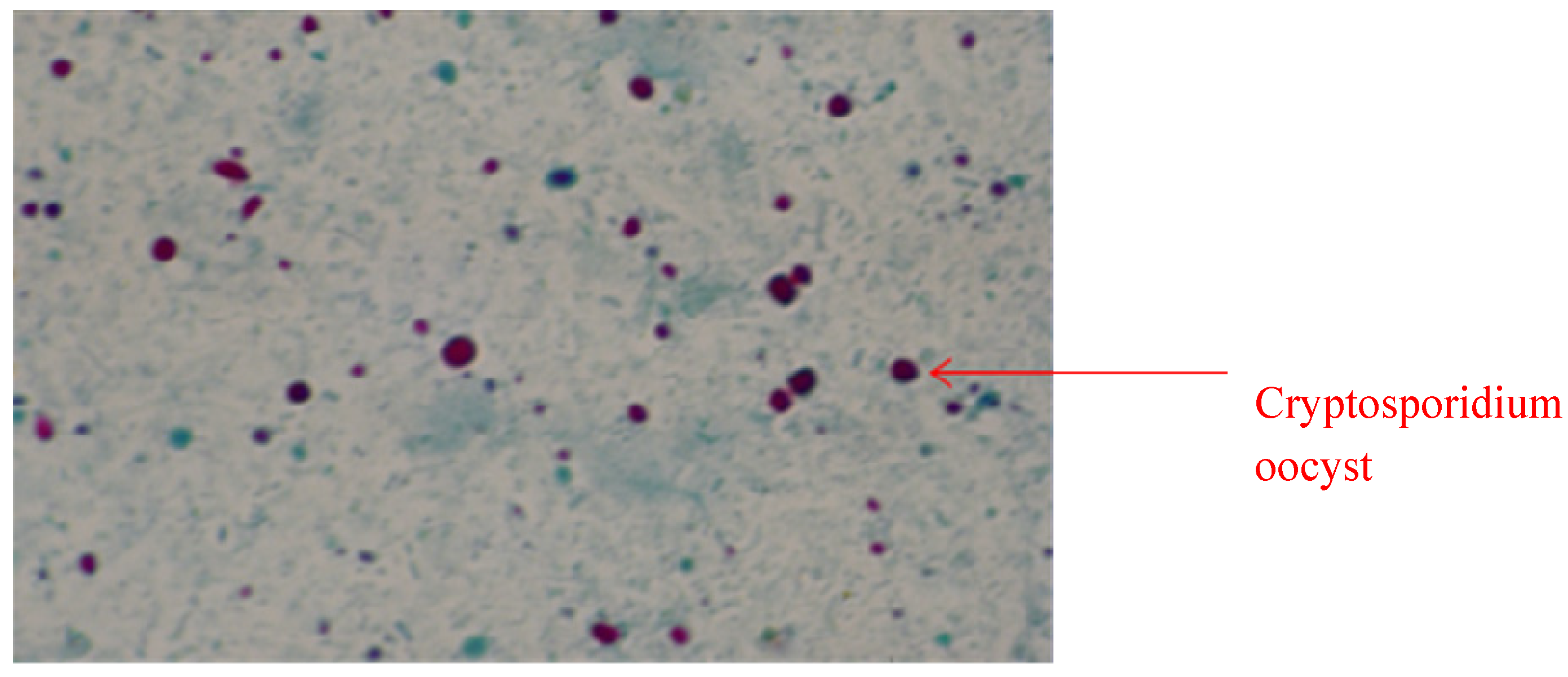
2.3. Detection of Cryptosporidium Oocysts: ELISA Assay Technique
2.4. Detection of Cryptosporidium Oocysts: PCR Amplification of Genomic DNA
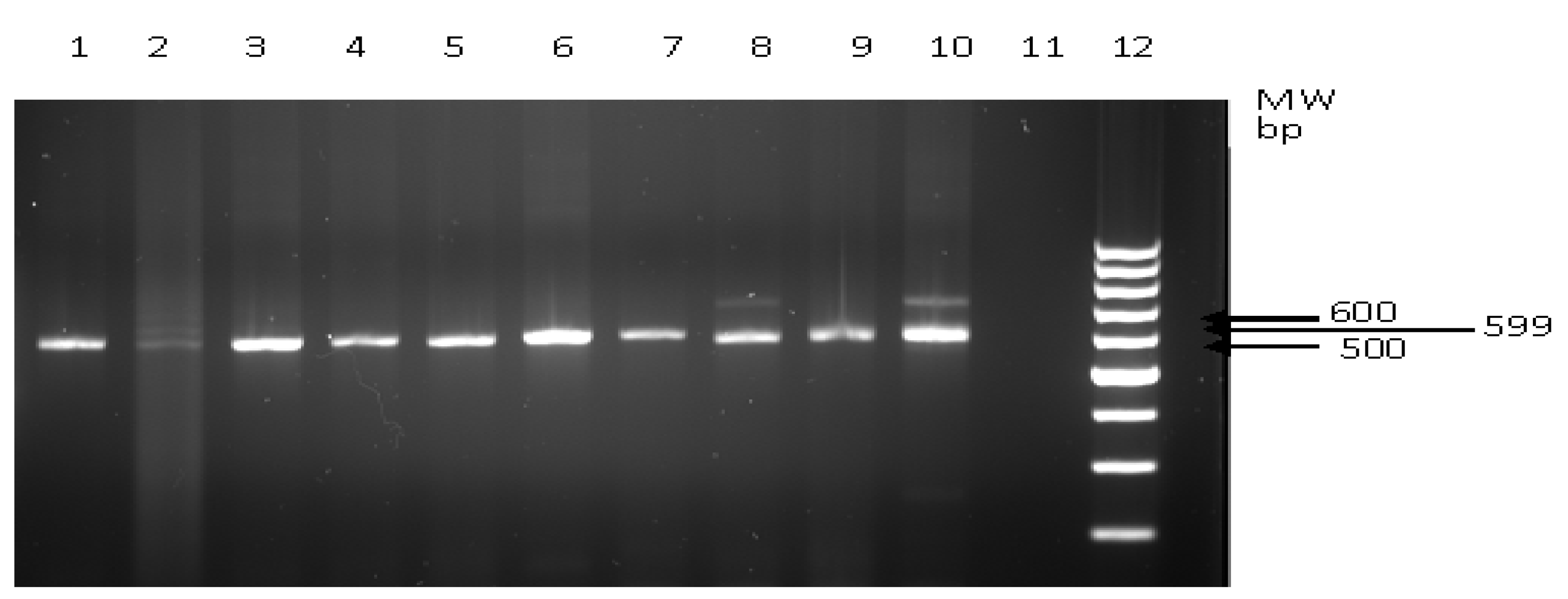
2.5. Comparative Evaluation of Cryptosporidium Detection Techniques
| TDiagnostic Techniques | HIV status | Cryptosporidium Incidence (%) | Sensitivity (%) | Specificity (%) | Positive Predictive Value (%) | Negative Predictive Value (%) |
|---|---|---|---|---|---|---|
| ZN | Positive | 13/35 (37.1) | 46.2 | 88.9 | 92.3 | 36.4 |
| Negative | 34/125 (27.2) | 32.3 | 96.6 | 96.9 | 30.1 | |
| sad-ELISA | Positive | 26/35 (74.3) | 92.3 | 36.4 | 46.2 | 88.9 |
| Negative | 96/125 (76.8) | 96.9 | 30.1 | 32.3 | 96.9 | |
| PCR | Positive | 23/35 (65.7) | 75.0 | 42.1 | 52.2 | 66.7 |
| Negative | 89/125 (71.2) | 96.9 | 32.6 | 79.5 | 77.8 |
3. Experimental
3.1. Patients and Control Subjects
3.2. Stool Specimens and Processing
3.3. Microscopic Examination of Cryptosporidium Oocysts
3.4. Cryptosporidium Specific Antigen Detection
3.5. PCR Assay for Cryptosporidium
3.6. PCR Amplification of Cryptosporidium DNA
3.7. Ethical Clearance
3.8. Statistical Analysis
4. Conclusions
Acknowledgments
Conflicts of Interest
References
- Cheng, A.C.; McDonald, J.R.M.D.; Nathan, M. Infectious diarrhoea in developed and developing countries. J. Clini. Gastroenterol. 2005, 39, 757–773. [Google Scholar] [CrossRef]
- Connelly, J.T.; Nugen, S.R.; Borejsza-Wysocki, W.; Durst, R.A.; Montagna, A.J. Human pathogenic Cryptosporidium species bioanalytical detection method with single oocyst detection capability. Anal. Bioanal. Chem. 2008, 36, 450–457. [Google Scholar]
- Weber, R.R.T.; Bryan, H.S.; Bishop, S.P.; Wahlquist, J.J.; Sullivan, D.D. Threshold of detection of Cryptosporidium oocysts in human stool specimens: evidence for low sensitivity of current diagnostic methods. J. Clin. Microbiol. 1991, 29, 1323–1327. [Google Scholar]
- Katanik, M.T.; Schneider, S.K.; Rosenblatt, J.E.; Hall, G.S.; Procop, G.W. Evaluation of Color PAC Giardia/Cryptosporidium rapid assay and ProSpecT Giardia/Cryptosporidium microplate assay for detection of Giardia and Cryptosporidium in fecal specimens. J. Clin. Microbiol. 2001, 39, 4523–4525. [Google Scholar] [CrossRef]
- Chappell, C.L.; Okhuysen, P.C. Cryptosporidiosis. Curr. Opin. Infect. Dis. 2002, 15, 523–527. [Google Scholar] [CrossRef]
- Higgins, J.A.; Fayer, R.; Trout, J.M.; Xiao, L.; Lal, A.A.; Kerby, S.; Jenkins, M.C. Real-time PCR for the detection of Cryptosporidium parvum. J. Microbiol. Meth. 2001, 47, 323–337. [Google Scholar] [CrossRef]
- Samie, A.; Bessong, P.O.; Obi, C.L.; Sevilleja, J.E.; Stroup, S.; Houpt, E.; Guerrant, R.L. Cryptosporidium species: Preliminary descriptions of the prevalence and genotype distribution among school children and hospital patients in the Venda region, Limpopo Province, South Afr. Exp. Parasitol. 2006, 114, 314–322. [Google Scholar] [CrossRef]
- Tumwine, J.K.; Kekitiinwa, A.; Nabukeera, N.; Akiyoshi, D.E.; Rich, S.M.; Widmer, G.; Feng, X.; Tzipori, S. Cryptosporidium parvum in children with diarrhoea in Mulago Hospital, Kampala, Ugand. Am. J. Trop. Med. Hyg. 2003, 68, 710–715. [Google Scholar]
- Morgan, U.M.; Pallant, L.; Dwyer, B.W.; Forbes, D.A.; Rich, G.; Thompson, R.C. Comparison of PCR and Microscopy for detection of Cryptosporidium parvum in human faecal specimens: Clinical trial. J. Clin. Microbiol. 1998, 36, 995–998. [Google Scholar]
- Bialek, R.; Binder, N.; Dietz, K.; Joachim, A.; Knobloch, J.; Zelck, U.E. Comparison of fluorescence, antigen and PCR assays to detect Cryptosporidium parvum in faecal specimens. Diagn. Microbiol. Infect. Dis. 2002, 43, 283–288. [Google Scholar] [CrossRef]
- Galen, R.S.; Gambino, S.R. Beyond Normality: The predictive value and efficiency of medical diagnosis. J. Infect. Dis. 1975, 157, 225–229. [Google Scholar]
- Vitaliano, A.C.; Caryn, B.; Jacqueline, R.; Lillia, C.; Charles, R.S.; Ynes, O.; Robert, H.; Lihua, X. Cryptosporidium species and subtypes and clinical manifestation in children in Peru. Emerg. Infect. Dis. 2008, 14, 1567–1574. [Google Scholar] [CrossRef]
- Nagamani, K.; Pavuluri, P.R.; Guaneshwari, M.; Prasanthi, K.; Raomi, N.K. Molecular characterization of Cryptosporidium. An emerging parasite. Indian J. Med. Microbiol. 2007, 25, 133–136. [Google Scholar] [CrossRef]
- Rym, E.; Mohamed, M.; Karim, A.; Rim, A.; Fethi, M.; Fakher, K.; Fracis, D.; Alda, B. Identification of Cryptosporidium species infecting humans in Tunisia. Am. J. Trop. Med. Hyg. 2007, 79, 702–705. [Google Scholar]
- Kumar, S.S.; Ananthan, S.; Sarvanan, P. Role of coccidian parasites in causation of diarrhoea in HIV infected patients in Chennai. Indian J. Med. Res. 2002, 116, 85–89. [Google Scholar]
- Stark, D.; Fotedar, R.; Hal, S.V.; Beebe, N.; Marriot, D.; Ells, J.T.; Harkness, J. Prevalence of enteric protozoa in human immunodeficiency virus (HIV)-positive and HIV-negative men who have sex with men from Sydney, Australia. Am. J. Trop. Med. Hyg. 2007, 76, 549–552. [Google Scholar]
- Oguntibeju, O.O. Prevalence of intestinal parasites in HIV-positive/AIDS patients. Malays. J. Med. Sci. 2006, 13, 68–73. [Google Scholar]
- Brandonisio, O.; Maggi, P.; Panaro, M.A.; Lisi, S.; Andriola, A.; Acquafredda, A.; Angarano, G. Intestinal protozoa in HIV-infected patients in Apulia, South Italy. Epidemiol. Infect. 1999, 123, 457–462. [Google Scholar] [CrossRef]
- Chintu, C.; Luo, C.; Baboo, S.; Med, M.; Khumalo-Ngwenya, B.; Mathewson, J.; DuPont, H.L.; Zumla, A. Intestinal parasites in HIV-seropositive Zambian children with diarrhoea. J. Trop. Paed. 1995, 41, 149–152. [Google Scholar] [CrossRef]
- Cotte, L.; Rabondonirina, M.; Piens, M.A.; Perrcard, M.M.; Trepo, C. Prevalence of intestinal protozoans in French patients infected with HIV. J. Acquir. Immune. Defic. Syndr. 1993, 6, 1024–1029. [Google Scholar]
- Sethi, S.; Sehgal, R.; Malla, N.; Mahajan, R.C. Cryptosporidiosis in a tertiary care hospital. Natl. Med. J. India 1999, 12, 207–209. [Google Scholar]
- Parija, S.C.; Shivaprakash, M.R.; Jayakeerthi, S.R. Evaluation of lacto-phenol cotton blue (LPCB) for detection of Cryptosporidium, Cyclospora and Isospora in the wet mount preparation of stool. Acta Trop. 2003, 85, 349–354. [Google Scholar] [CrossRef]
- Redlinger, T.V.; Corella-barud, J.; Graham, A.; Galindo, R.; Cardenas, V. Hyperendemic Cryptosporidium and Giadia in households lacking municipal sewer and water on the United State-Mexico border. Am. J. Trop. Med. Hyg. 2002, 66, 794–798. [Google Scholar]
- Casemore, D.P. The antibody response to Cryptosporidium: development of a serological test and its used in a study of immunologically normal persons. J. Clin. Infect. 2004, 14, 125–134. [Google Scholar] [CrossRef]
- Xiao, L.; Herd, R.P. Quantitation of Giardia cysts and Cryptosporidium oocysts in fecal sample by direct immunofluorescence assay. J. Clin. Microbiol. 1993, 31, 2944–2946. [Google Scholar]
- Alles, A.J. Prospective comparison of direct immunofluorescence and conventional staining methods for detection of Giardia and Cryptosporidium spp. in human fecal specimens. J. Clin. Microbiol. 1995, 33, 1632–1624. [Google Scholar]
- Weitzel, T.; Dittrich, S.; Möhl, I.; Adusu, E.; Jelinek, T. Evaluation of seven commercial antigen detection tests for Giardia and Cryptosporidium in stool samples. Clin. Microbiol. Infect. 2007, 13, 217–1217. [Google Scholar]
- Sample Availability: Cryptosporidium oocysts are available from the authors.
© 2014 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Omoruyi, B.E.; Nwodo, U.U.; Udem, C.S.; Okonkwo, F.O. Comparative Diagnostic Techniques for Cryptosporidium Infection. Molecules 2014, 19, 2674-2683. https://doi.org/10.3390/molecules19022674
Omoruyi BE, Nwodo UU, Udem CS, Okonkwo FO. Comparative Diagnostic Techniques for Cryptosporidium Infection. Molecules. 2014; 19(2):2674-2683. https://doi.org/10.3390/molecules19022674
Chicago/Turabian StyleOmoruyi, Beauty E., Uchechukwu U. Nwodo, Chukwuneke S. Udem, and Francis O. Okonkwo. 2014. "Comparative Diagnostic Techniques for Cryptosporidium Infection" Molecules 19, no. 2: 2674-2683. https://doi.org/10.3390/molecules19022674
APA StyleOmoruyi, B. E., Nwodo, U. U., Udem, C. S., & Okonkwo, F. O. (2014). Comparative Diagnostic Techniques for Cryptosporidium Infection. Molecules, 19(2), 2674-2683. https://doi.org/10.3390/molecules19022674




