Prevention of Type 2 Diabetes: The Role of Intermittent Fasting
Abstract
1. Introduction
1.1. Intermittent Fasting
Intermittent Fasting Schedules
1.2. Fasting for the Future
1.3. At the Core of Prediabetes and Type 2 Diabetes
1.3.1. Visceral Fat
1.3.2. Hepatic Steatosis
2. The Role of Intermittent Fasting in Combating Type 2 Diabetes Mellitus
2.1. What Is at Stake?
2.2. The Effects of Intermittent Fasting on HbA1c Levels
2.3. From Healthy to Prediabetes to Type 2 Diabetes Mellitus
2.4. Current Alternative Therapies for the Prevention of Type 2 Diabetes Mellitus
3. The Challenges to Overcome
3.1. Catching It Early
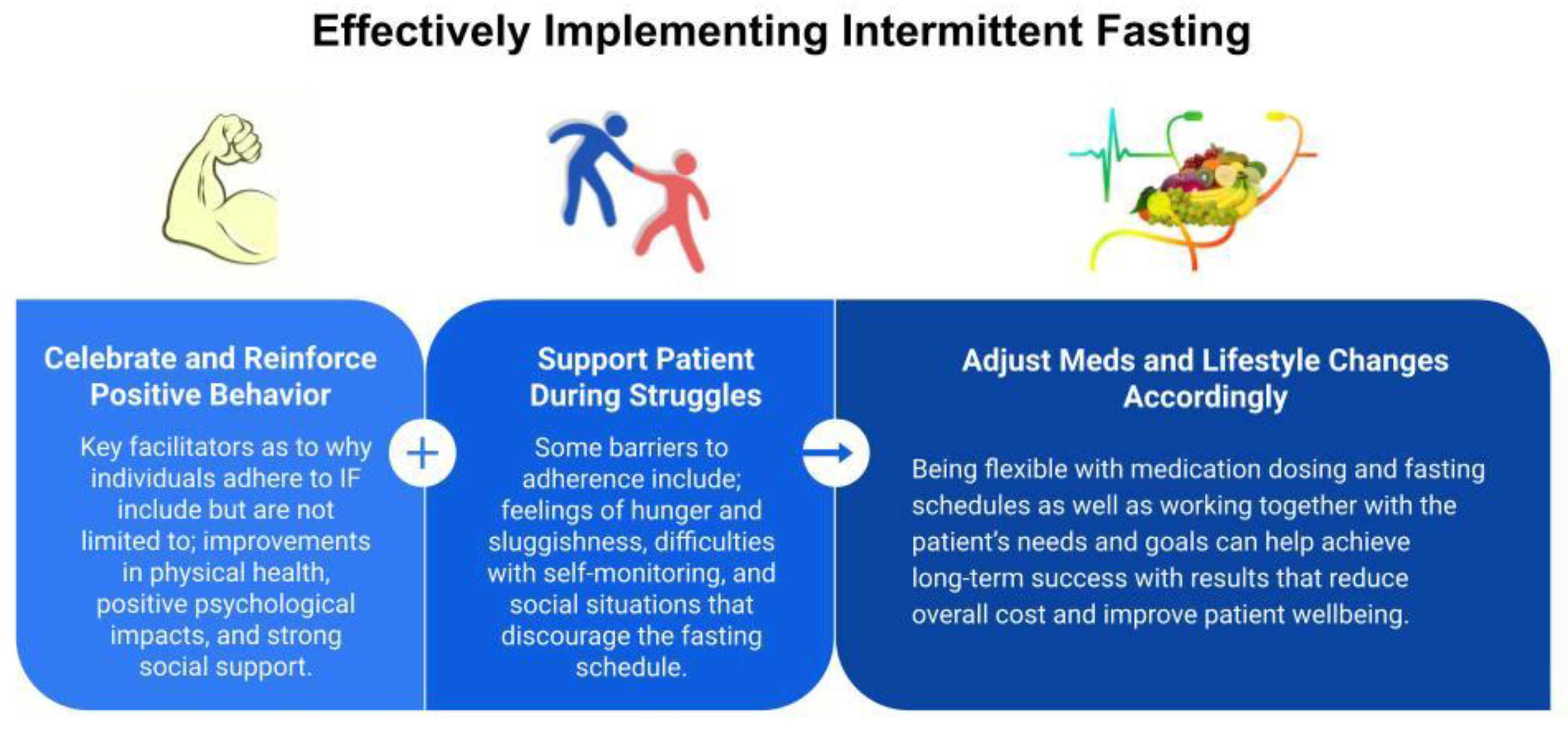
3.2. Implementing and Adhering to Intermittent Fasting
4. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Intermittent Fasting: What Is It, and How Does It Work? Available online: https://www.hopkinsmedicine.org/health/wellness-and-prevention/intermittent-fasting-what-is-it-and-how-does-it-work (accessed on 14 June 2023).
- Tinsley, G.M.; La Bounty, P.M. Effects of Intermittent Fasting on Body Composition and Clinical Health Markers in Humans. Nutr. Rev. 2015, 73, 661–674. [Google Scholar] [CrossRef] [PubMed]
- Seimon, R.V.; Roekenes, J.A.; Zibellini, J.; Zhu, B.; Gibson, A.A.; Hills, A.P.; Wood, R.E.; King, N.A.; Byrne, N.M.; Sainsbury, A. Do Intermittent Diets Provide Physiological Benefits over Continuous Diets for Weight Loss? A Systematic Review of Clinical Trials. Mol. Cell. Endocrinol. 2015, 418, 153–172. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Zhang, C.; Wang, H.; Ma, Z.; Liu, D.; Guan, X.; Liu, Y.; Fu, Y.; Cui, M.; Dong, J. Intermittent Fasting versus Continuous Calorie Restriction: Which Is Better for Weight Loss? Nutrients 2022, 14, 1781. [Google Scholar] [CrossRef] [PubMed]
- Gabel, K.; Kroeger, C.M.; Trepanowski, J.F.; Hoddy, K.K.; Cienfuegos, S.; Kalam, F.; Varady, K.A. Differential Effects of Alternate-Day Fasting Versus Daily Calorie Restriction on Insulin Resistance. Obesity 2019, 27, 1443–1450. [Google Scholar] [CrossRef]
- De Cabo, R.; Mattson, M.P. Effects of Intermittent Fasting on Health, Aging, and Disease. N. Engl. J. Med. 2019, 381, 2541–2551. [Google Scholar] [CrossRef]
- Redman, L.M.; Smith, S.R.; Burton, J.H.; Martin, C.K.; Il’yasova, D.; Ravussin, E. Metabolic Slowing and Reduced Oxidative Damage with Sustained Caloric Restriction Support the Rate of Living and Oxidative Damage Theories of Aging. Cell Metab. 2018, 27, 805–815.e4. [Google Scholar] [CrossRef]
- Wan, R.; Camandola, S.; Mattson, M.P. Intermittent Food Deprivation Improves Cardiovascular and Neuroendocrine Responses to Stress in Rats. J. Nutr. 2003, 133, 1921–1929. [Google Scholar] [CrossRef]
- Castello, L.; Froio, T.; Maina, M.; Cavallini, G.; Biasi, F.; Leonarduzzi, G.; Donati, A.; Bergamini, E.; Poli, G.; Chiarpotto, E. Alternate-Day Fasting Protects the Rat Heart against Age-Induced Inflammation and Fibrosis by Inhibiting Oxidative Damage and NF-KB Activation. Free Radic. Biol. Med. 2010, 48, 47–54. [Google Scholar] [CrossRef]
- Wan, R.; Camandola, S.; Mattson, M.P. Intermittent Fasting and Dietary Supplementation with 2-Deoxy-D-Glucose Improve Functional and Metabolic Cardiovascular Risk Factors in Rats. FASEB J. 2003, 17, 1133–1134. [Google Scholar] [CrossRef]
- Anson, R.M.; Guo, Z.; de Cabo, R.; Iyun, T.; Rios, M.; Hagepanos, A.; Ingram, D.K.; Lane, M.A.; Mattson, M.P. Intermittent Fasting Dissociates Beneficial Effects of Dietary Restriction on Glucose Metabolism and Neuronal Resistance to Injury from Calorie Intake. Proc. Natl. Acad. Sci. USA 2003, 100, 6216–6220. [Google Scholar] [CrossRef]
- Bough, K.J.; Valiyil, R.; Han, F.T.; Eagles, D.A. Seizure Resistance Is Dependent upon Age and Calorie Restriction in Rats Fed a Ketogenic Diet. Epilepsy Res. 1999, 35, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Gilbert, D.L.; Pyzik, P.L.; Freeman, J.M. The Ketogenic Diet: Seizure Control Correlates Better with Serum Beta-Hydroxybutyrate than with Urine Ketones. J. Child Neurol. 2000, 15, 787–790. [Google Scholar] [CrossRef] [PubMed]
- Kashiwaya, Y.; Takeshima, T.; Mori, N.; Nakashima, K.; Clarke, K.; Veech, R.L. D-Beta-Hydroxybutyrate Protects Neurons in Models of Alzheimer’s and Parkinson’s Disease. Proc. Natl. Acad. Sci. USA 2000, 97, 5440–5444. [Google Scholar] [CrossRef]
- Varady, K.A.; Hellerstein, M.K. Alternate-Day Fasting and Chronic Disease Prevention: A Review of Human and Animal Trials. Am. J. Clin. Nutr. 2007, 86, 7–13. [Google Scholar] [CrossRef]
- Arum, O.; Bonkowski, M.S.; Rocha, J.S.; Bartke, A. The Growth Hormone Receptor Gene-Disrupted Mouse Fails to Respond to an Intermittent Fasting Diet. Aging Cell 2009, 8, 756–760. [Google Scholar] [CrossRef] [PubMed]
- Kendrick, D.C. The Effects of Infantile Stimulation and Intermittent Fasting and Feeding on Life Span in the Black-Hooded Rat. Dev. Psychobiol. 1973, 6, 225–234. [Google Scholar] [CrossRef]
- Goodrick, C.L.; Ingram, D.K.; Reynolds, M.A.; Freeman, J.R.; Cider, N. Effects of Intermittent Feeding upon Body Weight and Lifespan in Inbred Mice: Interaction of Genotype and Age. Mech. Ageing Dev. 1990, 55, 69–87. [Google Scholar] [CrossRef]
- DeFronzo, R.A. From the Triumvirate to the Ominous Octet: A New Paradigm for the Treatment of Type 2 Diabetes Mellitus. Diabetes 2009, 58, 773–795. [Google Scholar] [CrossRef]
- Schwartz, S.S.; Epstein, S.; Corkey, B.E.; Grant, S.F.A.; Gavin, J.R.; Aguilar, R.B. The Time Is Right for a New Classification System for Diabetes: Rationale and Implications of the β-Cell-Centric Classification Schema. Diabetes Care 2016, 39, 179–186. [Google Scholar] [CrossRef]
- Gastaldelli, A.; Miyazaki, Y.; Pettiti, M.; Matsuda, M.; Mahankali, S.; Santini, E.; DeFronzo, R.A.; Ferrannini, E. Metabolic Effects of Visceral Fat Accumulation in Type 2 Diabetes. J. Clin. Endocrinol. Metab. 2002, 87, 5098–5103. [Google Scholar] [CrossRef]
- Kantartzis, K.; Machann, J.; Schick, F.; Fritsche, A.; Häring, H.-U.; Stefan, N. The Impact of Liver Fat vs. Visceral Fat in Determining Categories of Prediabetes. Diabetologia 2010, 53, 882–889. [Google Scholar] [CrossRef] [PubMed]
- Samuel, V.T.; Liu, Z.-X.; Qu, X.; Elder, B.D.; Bilz, S.; Befroy, D.; Romanelli, A.J.; Shulman, G.I. Mechanism of Hepatic Insulin Resistance in Non-Alcoholic Fatty Liver Disease. J. Biol. Chem. 2004, 279, 32345–32353. [Google Scholar] [CrossRef] [PubMed]
- Dokpuang, D.; Zhiyong Yang, J.; Nemati, R.; He, K.; Plank, L.D.; Murphy, R.; Lu, J. Magnetic Resonance Study of Visceral, Subcutaneous, Liver and Pancreas Fat Changes after 12 Weeks Intermittent Fasting in Obese Participants with Prediabetes. Diabetes Res. Clin. Pract. 2023, 202, 110775. [Google Scholar] [CrossRef] [PubMed]
- de Souza Marinho, T.; Ornellas, F.; Barbosa-da-Silva, S.; Mandarim-de-Lacerda, C.A.; Aguila, M.B. Beneficial Effects of Intermittent Fasting on Steatosis and Inflammation of the Liver in Mice Fed a High-Fat or a High-Fructose Diet. Nutrition 2019, 65, 103–112. [Google Scholar] [CrossRef] [PubMed]
- Deng, J.; Feng, D.; Jia, X.; Zhai, S.; Liu, Y.; Gao, N.; Zhang, X.; Li, M.; Lu, M.; Liu, C.; et al. Efficacy and Mechanism of Intermittent Fasting in Metabolic Associated Fatty Liver Disease Based on Ultraperformance Liquid Chromatography-Tandem Mass Spectrometry. Front. Nutr. 2022, 9, 838091. [Google Scholar] [CrossRef]
- Ezpeleta, M.; Gabel, K.; Cienfuegos, S.; Kalam, F.; Lin, S.; Pavlou, V.; Song, Z.; Haus, J.M.; Koppe, S.; Alexandria, S.J.; et al. Effect of Alternate Day Fasting Combined with Aerobic Exercise on Non-Alcoholic Fatty Liver Disease: A Randomized Controlled Trial. Cell Metab. 2023, 35, 56–70.e3. [Google Scholar] [CrossRef]
- Health and Economic Benefits of Diabetes Interventions|Power of Prevention. Available online: https://www.cdc.gov/chronicdisease/programs-impact/pop/diabetes.htm (accessed on 1 July 2023).
- Galaviz, K.I.; Narayan, K.M.V.; Lobelo, F.; Weber, M.B. Lifestyle and the Prevention of Type 2 Diabetes: A Status Report. Am. J. Lifestyle Med. 2015, 12, 4–20. [Google Scholar] [CrossRef]
- National Diabetes Statistics Report|Diabetes|CDC. Available online: https://www.cdc.gov/diabetes/data/statistics-report/index.html (accessed on 14 June 2023).
- American Diabetes Association. Economic Costs of Diabetes in the U.S. in 2017. Diabetes Care 2018, 41, 917–928. [Google Scholar] [CrossRef]
- Obermayer, A.; Tripolt, N.J.; Pferschy, P.N.; Kojzar, H.; Aziz, F.; Müller, A.; Schauer, M.; Oulhaj, A.; Aberer, F.; Sourij, C.; et al. Efficacy and Safety of Intermittent Fasting in People With Insulin-Treated Type 2 Diabetes (INTERFAST-2)-A Randomized Controlled Trial. Diabetes Care 2023, 46, 463–468. [Google Scholar] [CrossRef]
- Tagde, P.; Tagde, S.; Bhattacharya, T.; Tagde, P.; Akter, R.; Rahman, M.H. Multifaceted Effects of Intermittent Fasting on the Treatment and Prevention of Diabetes, Cancer, Obesity or Other Chronic Diseases. Curr. Diabetes Rev. 2022, 18, e131221198789. [Google Scholar] [CrossRef]
- Kunduraci, Y.E.; Ozbek, H. Does the Energy Restriction Intermittent Fasting Diet Alleviate Metabolic Syndrome Biomarkers? A Randomized Controlled Trial. Nutrients 2020, 12, 3213. [Google Scholar] [CrossRef] [PubMed]
- Carter, S.; Clifton, P.M.; Keogh, J.B. Effect of Intermittent Compared With Continuous Energy Restricted Diet on Glycemic Control in Patients With Type 2 Diabetes: A Randomized Noninferiority Trial. JAMA Netw. Open 2018, 1, e180756. [Google Scholar] [CrossRef] [PubMed]
- Wing, R.R.; Lang, W.; Wadden, T.A.; Safford, M.; Knowler, W.C.; Bertoni, A.G.; Hill, J.O.; Brancati, F.L.; Peters, A.; Wagenknecht, L. Benefits of Modest Weight Loss in Improving Cardiovascular Risk Factors in Overweight and Obese Individuals with Type 2 Diabetes. Diabetes Care 2011, 34, 1481–1486. [Google Scholar] [CrossRef] [PubMed]
- Guariguata, L.; Whiting, D.; Weil, C.; Unwin, N. The International Diabetes Federation Diabetes Atlas Methodology for Estimating Global and National Prevalence of Diabetes in Adults. Diabetes Res. Clin. Pract. 2011, 94, 322–332. [Google Scholar] [CrossRef]
- Harris, M.I.; Klein, R.; Welborn, T.A.; Knuiman, M.W. Onset of NIDDM Occurs at Least 4–7 Yr before Clinical Diagnosis. Diabetes Care 1992, 15, 815–819. [Google Scholar] [CrossRef]
- Ali, O. Genetics of Type 2 Diabetes. World J. Diabetes 2013, 4, 114–123. [Google Scholar] [CrossRef]
- Lyssenko, V.; Laakso, M. Genetic Screening for the Risk of Type 2 Diabetes. Diabetes Care 2013, 36, S120–S126. [Google Scholar] [CrossRef]
- Shaw, J. Diagnosis of Prediabetes. Med. Clin. N. Am. 2011, 95, 341–352. [Google Scholar] [CrossRef]
- Stern, M.P.; Williams, K.; Haffner, S.M. Identification of Persons at High Risk for Type 2 Diabetes Mellitus: Do We Need the Oral Glucose Tolerance Test? Ann. Intern. Med. 2002, 136, 575–581. [Google Scholar] [CrossRef]
- Sagesaka, H.; Sato, Y.; Someya, Y.; Tamura, Y.; Shimodaira, M.; Miyakoshi, T.; Hirabayashi, K.; Koike, H.; Yamashita, K.; Watada, H.; et al. Type 2 Diabetes: When Does It Start? J. Endocr. Soc. 2018, 2, 476–484. [Google Scholar] [CrossRef]
- Uusitupa, M.; Khan, T.A.; Viguiliouk, E.; Kahleova, H.; Rivellese, A.A.; Hermansen, K.; Pfeiffer, A.; Thanopoulou, A.; Salas-Salvadó, J.; Schwab, U.; et al. Prevention of Type 2 Diabetes by Lifestyle Changes: A Systematic Review and Meta-Analysis. Nutrients 2019, 11, 2611. [Google Scholar] [CrossRef]
- Knowler, W.C.; Barrett-Connor, E.; Fowler, S.E.; Hamman, R.F.; Lachin, J.M.; Walker, E.A.; Nathan, D.M. Diabetes Prevention Program Research Group Reduction in the Incidence of Type 2 Diabetes with Lifestyle Intervention or Metformin. N. Engl. J. Med. 2002, 346, 393–403. [Google Scholar] [CrossRef] [PubMed]
- Diabetes Prevention Program Research Group; Knowler, W.C.; Fowler, S.E.; Hamman, R.F.; Christophi, C.A.; Hoffman, H.J.; Brenneman, A.T.; Brown-Friday, J.O.; Goldberg, R.; Venditti, E.; et al. 10-Year Follow-up of Diabetes Incidence and Weight Loss in the Diabetes Prevention Program Outcomes Study. Lancet 2009, 374, 1677–1686. [Google Scholar] [CrossRef] [PubMed]
- Eriksson, J.; Lindström, J.; Valle, T.; Aunola, S.; Hämäläinen, H.; Ilanne-Parikka, P.; Keinänen-Kiukaanniemi, S.; Laakso, M.; Lauhkonen, M.; Lehto, P.; et al. Prevention of Type II Diabetes in Subjects with Impaired Glucose Tolerance: The Diabetes Prevention Study (DPS) in Finland. Study Design and 1-Year Interim Report on the Feasibility of the Lifestyle Intervention Programme. Diabetologia 1999, 42, 793–801. [Google Scholar] [CrossRef] [PubMed]
- Lindström, J.; Ilanne-Parikka, P.; Peltonen, M.; Aunola, S.; Eriksson, J.G.; Hemiö, K.; Hämäläinen, H.; Härkönen, P.; Keinänen-Kiukaanniemi, S.; Laakso, M.; et al. Sustained Reduction in the Incidence of Type 2 Diabetes by Lifestyle Intervention: Follow-up of the Finnish Diabetes Prevention Study. Lancet 2006, 368, 1673–1679. [Google Scholar] [CrossRef] [PubMed]
- Li, G.; Zhang, P.; Wang, J.; Gregg, E.W.; Yang, W.; Gong, Q.; Li, H.; Li, H.; Jiang, Y.; An, Y.; et al. The Long-Term Effect of Lifestyle Interventions to Prevent Diabetes in the China Da Qing Diabetes Prevention Study: A 20-Year Follow-up Study. Lancet 2008, 371, 1783–1789. [Google Scholar] [CrossRef]
- Chiasson, J.-L.; Josse, R.G.; Gomis, R.; Hanefeld, M.; Karasik, A.; Laakso, M. STOP-NIDDM Trail Research Group Acarbose for Prevention of Type 2 Diabetes Mellitus: The STOP-NIDDM Randomised Trial. Lancet 2002, 359, 2072–2077. [Google Scholar] [CrossRef]
- Buchanan, T.A.; Xiang, A.H.; Peters, R.K.; Kjos, S.L.; Marroquin, A.; Goico, J.; Ochoa, C.; Tan, S.; Berkowitz, K.; Hodis, H.N.; et al. Preservation of Pancreatic Beta-Cell Function and Prevention of Type 2 Diabetes by Pharmacological Treatment of Insulin Resistance in High-Risk Hispanic Women. Diabetes 2002, 51, 2796–2803. [Google Scholar] [CrossRef]
- DREAM (Diabetes REduction Assessment with ramipril and rosiglitazone Medication) Trial Investigators; Gerstein, H.C.; Yusuf, S.; Bosch, J.; Pogue, J.; Sheridan, P.; Dinccag, N.; Hanefeld, M.; Hoogwerf, B.; Laakso, M.; et al. Effect of Rosiglitazone on the Frequency of Diabetes in Patients with Impaired Glucose Tolerance or Impaired Fasting Glucose: A Randomised Controlled Trial. Lancet 2006, 368, 1096–1105. [Google Scholar] [CrossRef]
- Zinman, B.; Harris, S.B.; Neuman, J.; Gerstein, H.C.; Retnakaran, R.R.; Raboud, J.; Qi, Y.; Hanley, A.J.G. Low-Dose Combination Therapy with Rosiglitazone and Metformin to Prevent Type 2 Diabetes Mellitus (CANOE Trial): A Double-Blind Randomised Controlled Study. Lancet 2010, 376, 103–111. [Google Scholar] [CrossRef]
- Torgerson, J.S.; Hauptman, J.; Boldrin, M.N.; Sjöström, L. XENical in the Prevention of Diabetes in Obese Subjects (XENDOS) Study: A Randomized Study of Orlistat as an Adjunct to Lifestyle Changes for the Prevention of Type 2 Diabetes in Obese Patients. Diabetes Care 2004, 27, 155–161. [Google Scholar] [CrossRef] [PubMed]
- Marina, A.L.; Utzschneider, K.M.; Wright, L.A.; Montgomery, B.K.; Marcovina, S.M.; Kahn, S.E. Colesevelam Improves Oral but Not Intravenous Glucose Tolerance by a Mechanism Independent of Insulin Sensitivity and β-Cell Function. Diabetes Care 2012, 35, 1119–1125. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Handelsman, Y.; Goldberg, R.B.; Garvey, W.T.; Fonseca, V.A.; Rosenstock, J.; Jones, M.R.; Lai, Y.-L.; Jin, X.; Misir, S.; Nagendran, S.; et al. Colesevelam Hydrochloride to Treat Hypercholesterolemia and Improve Glycemia in Prediabetes: A Randomized, Prospective Study. Endocr. Pract. 2010, 16, 617–628. [Google Scholar] [CrossRef]
- Rosenstock, J.; Foley, J.E.; Rendell, M.; Landin-Olsson, M.; Holst, J.J.; Deacon, C.F.; Rochotte, E.; Baron, M.A. Effects of the Dipeptidyl Peptidase-IV Inhibitor Vildagliptin on Incretin Hormones, Islet Function, and Postprandial Glycemia in Subjects with Impaired Glucose Tolerance. Diabetes Care 2008, 31, 30–35. [Google Scholar] [CrossRef][Green Version]
- Rosenstock, J.; Klaff, L.J.; Schwartz, S.; Northrup, J.; Holcombe, J.H.; Wilhelm, K.; Trautmann, M. Effects of Exenatide and Lifestyle Modification on Body Weight and Glucose Tolerance in Obese Subjects with and without Pre-Diabetes. Diabetes Care 2010, 33, 1173–1175. [Google Scholar] [CrossRef] [PubMed]
- Astrup, A.; Carraro, R.; Finer, N.; Harper, A.; Kunesova, M.; Lean, M.E.J.; Niskanen, L.; Rasmussen, M.F.; Rissanen, A.; Rössner, S.; et al. Safety, Tolerability and Sustained Weight Loss over 2 Years with the Once-Daily Human GLP-1 Analog, Liraglutide. Int. J. Obes. 2012, 36, 843–854. [Google Scholar] [CrossRef]
- Dixon, J.B.; Zimmet, P.; Alberti, K.G.; Rubino, F. Bariatric Surgery: An IDF Statement for Obese Type 2 Diabetes. Diabet. Med. 2011, 28, 628–642. [Google Scholar] [CrossRef]
- de la Cruz-Muñoz, N.; Messiah, S.E.; Arheart, K.L.; Lopez-Mitnik, G.; Lipshultz, S.E.; Livingstone, A. Bariatric Surgery Significantly Decreases the Prevalence of Type 2 Diabetes Mellitus and Pre-Diabetes among Morbidly Obese Multiethnic Adults: Long-Term Results. J. Am. Coll. Surg. 2011, 212, 505–511; discussion 512–513. [Google Scholar] [CrossRef]
- Carlsson, L.M.S.; Peltonen, M.; Ahlin, S.; Anveden, Å.; Bouchard, C.; Carlsson, B.; Jacobson, P.; Lönroth, H.; Maglio, C.; Näslund, I.; et al. Bariatric Surgery and Prevention of Type 2 Diabetes in Swedish Obese Subjects. N. Engl. J. Med. 2012, 367, 695–704. [Google Scholar] [CrossRef]
- Zhuo, X.; Zhang, P.; Barker, L.; Albright, A.; Thompson, T.J.; Gregg, E. The Lifetime Cost of Diabetes and Its Implications for Diabetes Prevention. Diabetes Care 2014, 37, 2557–2564. [Google Scholar] [CrossRef]
- Vasavada, A.; Taub, L.F.M. Diabetes Mellitus Screening. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- US Preventive Services Task Force. Screening for Prediabetes and Type 2 Diabetes: US Preventive Services Task Force Recommendation Statement. JAMA 2021, 326, 736–743. [Google Scholar] [CrossRef] [PubMed]
- Kahn, R.; Alperin, P.; Eddy, D.; Borch-Johnsen, K.; Buse, J.; Feigelman, J.; Gregg, E.; Holman, R.R.; Kirkman, M.S.; Stern, M.; et al. Age at Initiation and Frequency of Screening to Detect Type 2 Diabetes: A Cost-Effectiveness Analysis. Lancet 2010, 375, 1365–1374. [Google Scholar] [CrossRef] [PubMed]
- Lambrinou, E.; Hansen, T.B.; Beulens, J.W. Lifestyle Factors, Self-Management and Patient Empowerment in Diabetes Care. Eur. J. Prev. Cardiol. 2019, 26, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Bartoli, E.; Fra, G.P.; Carnevale Schianca, G.P. The Oral Glucose Tolerance Test (OGTT) Revisited. Eur. J. Intern. Med. 2011, 22, 8–12. [Google Scholar] [CrossRef]
- Lu, J.; He, J.; Li, M.; Tang, X.; Hu, R.; Shi, L.; Su, Q.; Peng, K.; Xu, M.; Xu, Y.; et al. Predictive Value of Fasting Glucose, Postload Glucose, and Hemoglobin A1c on Risk of Diabetes and Complications in Chinese Adults. Diabetes Care 2019, 42, 1539–1548. [Google Scholar] [CrossRef]
- Selvin, E.; Wang, D.; Matsushita, K.; Grams, M.E.; Coresh, J. Prognostic Implications of Single-Sample Confirmatory Testing for Undiagnosed Diabetes: A Prospective Cohort Study. Ann. Intern. Med. 2018, 169, 156–164. [Google Scholar] [CrossRef]
- Ostendorf, D.M.; Caldwell, A.E.; Zaman, A.; Pan, Z.; Bing, K.; Wayland, L.T.; Creasy, S.A.; Bessesen, D.H.; MacLean, P.; Melanson, E.L.; et al. Comparison of Weight Loss Induced by Daily Caloric Restriction versus Intermittent Fasting (DRIFT) in Individuals with Obesity: Study Protocol for a 52-Week Randomized Clinical Trial. Trials 2022, 23, 718. [Google Scholar] [CrossRef]
- Dansinger, M.L.; Gleason, J.A.; Griffith, J.L.; Selker, H.P.; Schaefer, E.J. Comparison of the Atkins, Ornish, Weight Watchers, and Zone Diets for Weight Loss and Heart Disease Risk ReductionA Randomized Trial. JAMA 2005, 293, 43–53. [Google Scholar] [CrossRef]
- MacLean, P.S.; Wing, R.R.; Davidson, T.; Epstein, L.; Goodpaster, B.; Hall, K.D.; Levin, B.E.; Perri, M.G.; Rolls, B.J.; Rosenbaum, M.; et al. NIH Working Group Report: Innovative Research to Improve Maintenance of Weight Loss. Obesity 2015, 23, 7–15. [Google Scholar] [CrossRef]
- O’Connor, S.G.; Boyd, P.; Bailey, C.P.; Nebeling, L.; Reedy, J.; Czajkowski, S.M.; Shams-White, M.M. A Qualitative Exploration of Facilitators and Barriers of Adherence to Time-Restricted Eating. Appetite 2022, 178, 106266. [Google Scholar] [CrossRef]
- Vasim, I.; Majeed, C.N.; DeBoer, M.D. Intermittent Fasting and Metabolic Health. Nutrients 2022, 14, 631. [Google Scholar] [CrossRef] [PubMed]
| Schedule | Description | Possible Modifications |
|---|---|---|
| Daily (16:8) | All days of the week involve a 16 h fasting period of zero calories, followed by an 8 h window of ad libitum eating. | Certain dietary restrictions can be added to modify results, or the fasting period may be increased to 18 h. |
| Alternate-day (4:3) | Fasting is carried out every other day for a 24 h period and alternates with days of ad libitum eating. | The fasting days typically involve a 25% caloric intake compared to normal, but this can be decreased to complete zero-calorie fasting. |
| Whole-day (5:2) | Zero-calorie fasting is completed for two days out of the week, usually in between a few days of ad libitum eating. | While zero-calorie fasting is the standard, a modified decrease in caloric intake, such as 25% of normal, may be implemented based on individual capabilities. |
| Study | Country | N | Baseline BMI (kg/m2) | Intervention Period (Years) | RRR (%) | NNT |
|---|---|---|---|---|---|---|
| Diabetes Prevention Program [45] | USA | 3234 | 34.0 | 2.8 | 58 | 21 |
| Diabetes Prevention Study [47,48] | Finland | 523 | 31.0 | 4 | 39 | 22 |
| Da Qing [49] | China | 577 | 25.8 | 6 | 51 | 30 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Test, B.; Shubrook, J.H. Prevention of Type 2 Diabetes: The Role of Intermittent Fasting. Diabetology 2023, 4, 507-518. https://doi.org/10.3390/diabetology4040044
Test B, Shubrook JH. Prevention of Type 2 Diabetes: The Role of Intermittent Fasting. Diabetology. 2023; 4(4):507-518. https://doi.org/10.3390/diabetology4040044
Chicago/Turabian StyleTest, Bright, and Jay H. Shubrook. 2023. "Prevention of Type 2 Diabetes: The Role of Intermittent Fasting" Diabetology 4, no. 4: 507-518. https://doi.org/10.3390/diabetology4040044
APA StyleTest, B., & Shubrook, J. H. (2023). Prevention of Type 2 Diabetes: The Role of Intermittent Fasting. Diabetology, 4(4), 507-518. https://doi.org/10.3390/diabetology4040044








