Wearing Effect of Implant Steel Drills and Tappers for the Preparation of the Bone Osteotomies: An Infrared Thermal Analysis and Energy Dispersive Spectroscopy-Scanning Electron Microscopy (EDS-SEM) Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Drills and Bone Tappers Evaluated
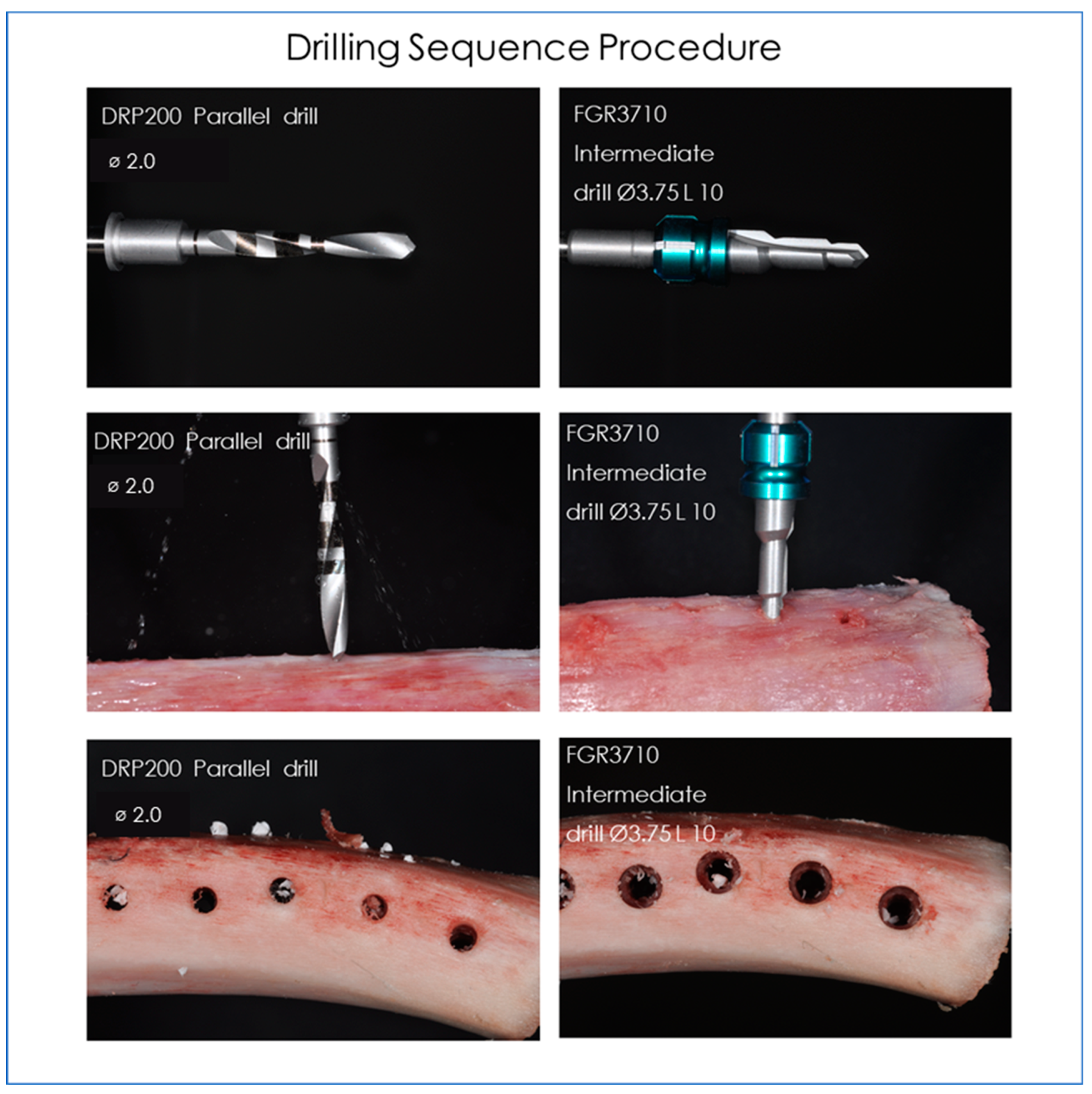
- FGR3710 Intermediate drill Ø3.75 L 10 (Dental Tech, Misinto MB, Italy).
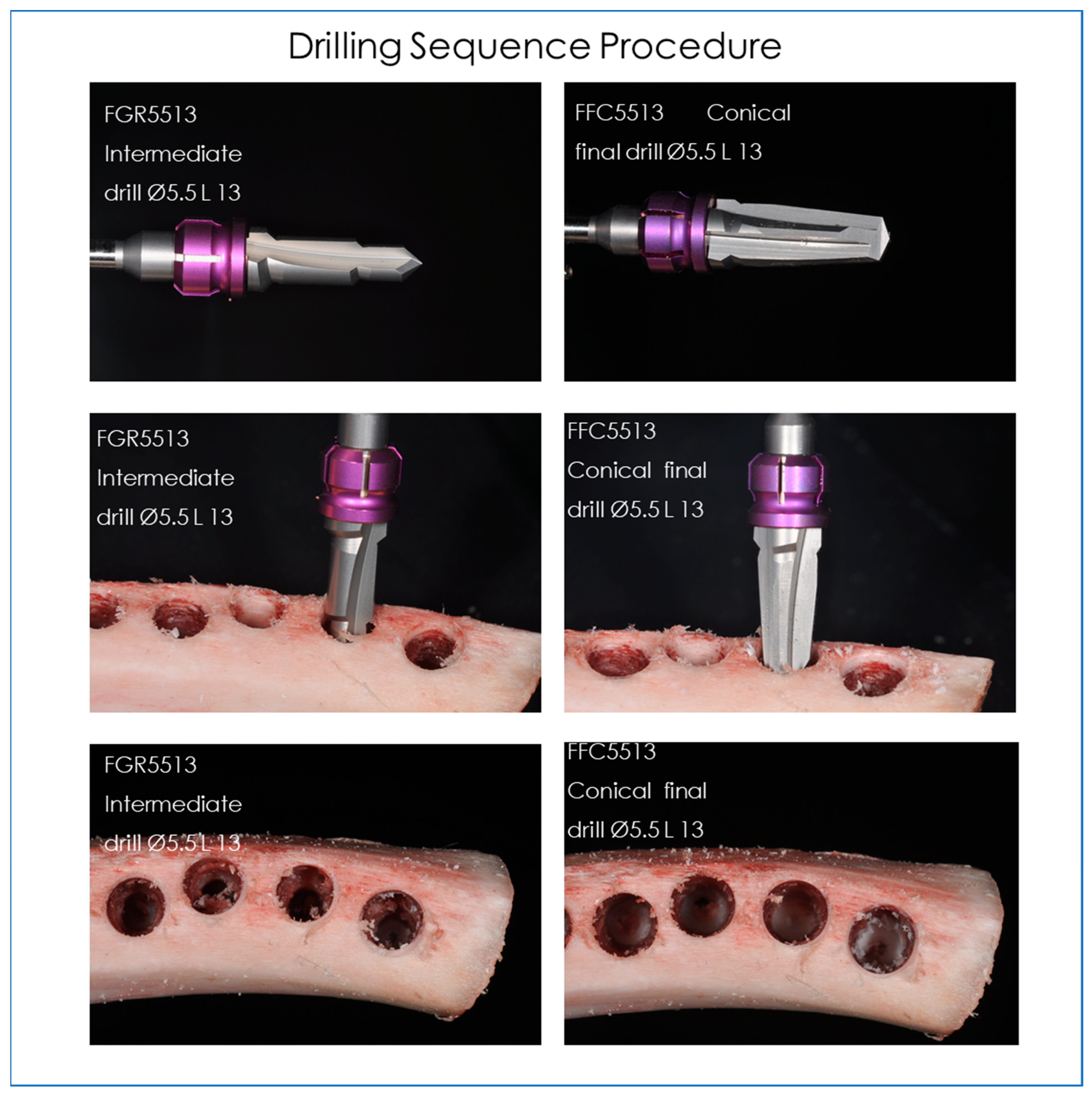
- FGR5513 Intermediate drill Ø5.5 L 13 (Dental Tech, Misinto MB, Italy).
- FFC3710 Conical final drill Ø3.75 L 10 (Dental Tech, Misinto MB, Italy).
- FFC5513 Conical final drill Ø5.5 L 13 (Dental Tech, Misinto MB, Italy).
- DRP200 Parallel drill Ø2,0 (Dental Tech, Misinto MB, Italy).
- DRP450 Parallel drill Ø4,5 (Dental Tech, Misinto MB, Italy).
- MKN3710 Conical tapper Ø3.75 L 10 (Dental Tech, Misinto MB, Italy).
- MKN3711 Conical tapper Ø3.75 L 11.5 (Dental Tech, Misinto MB, Italy).
- MKN3713 Conical tapper Ø3.75 L 13 (Dental Tech, Misinto MB, Italy).
- MKN3714 Conical tapper Ø3.75 L 14.5 (Dental Tech, Misinto MB, Italy).
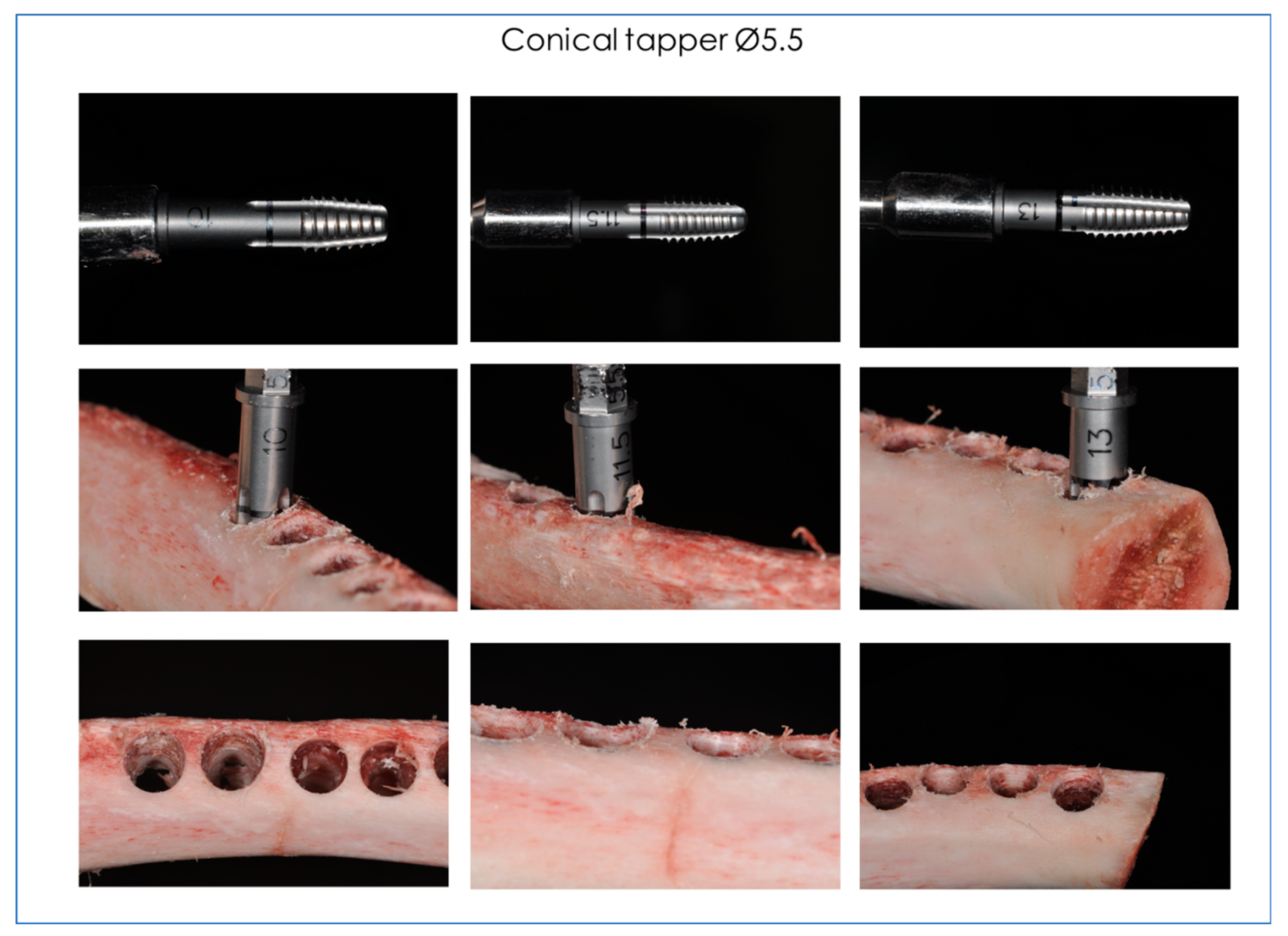
- MSL5510 Conical tapper Ø5.5 L 10 (Dental Tech, Misinto MB, Italy).
- MSL5511 Conical tapper Ø5.5 L 11.5 (Dental Tech, Misinto MB, Italy).
- MSL5513 Conical tapper Ø5.5 L 13 (Dental Tech, Misinto MB, Italy).
2.2. Infrared Thermographic Measurements
2.3. EDS-SEM Observations
2.4. Statistical Evaluation
3. Results
3.1. Infrared Thermography Measurements
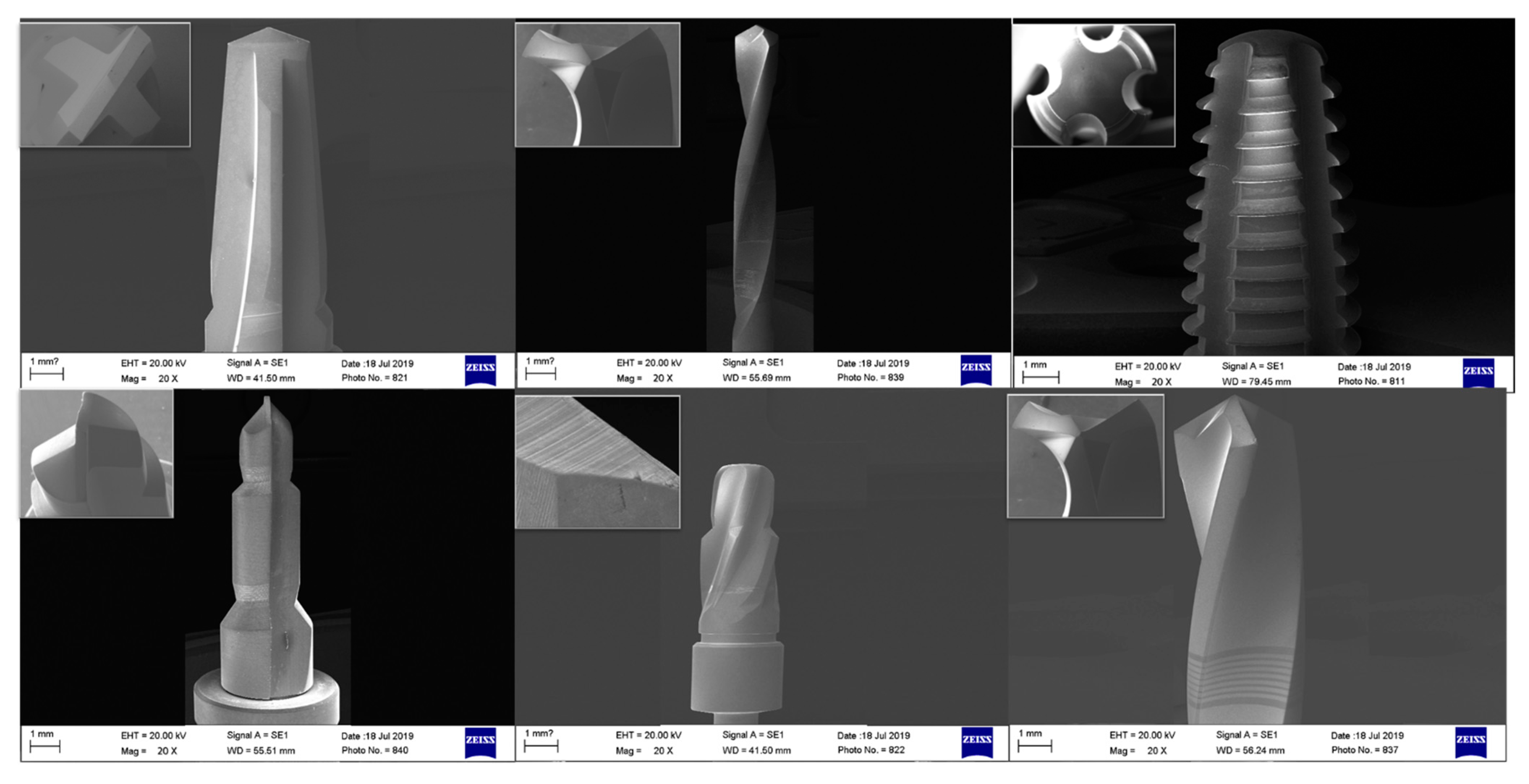
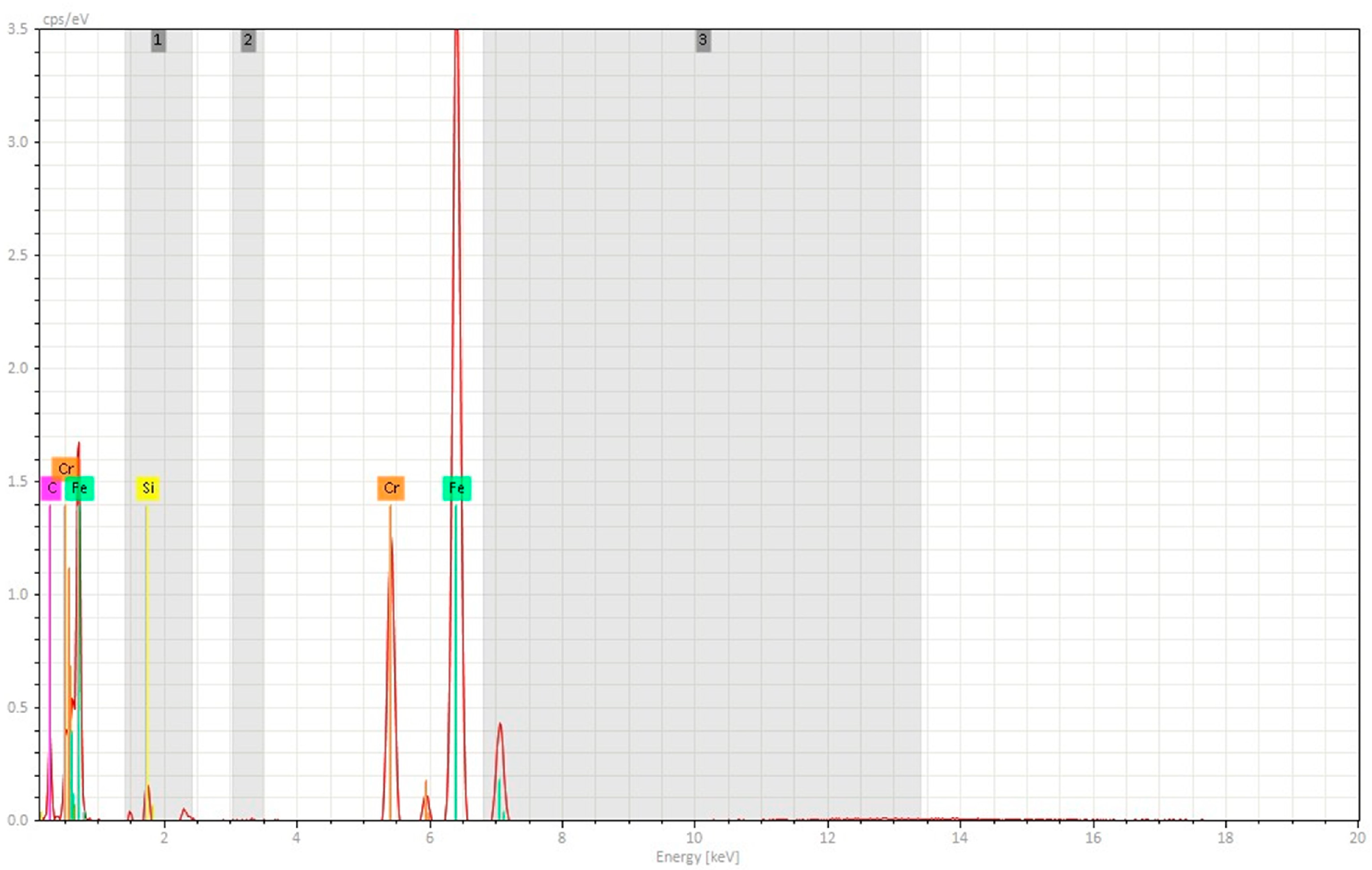
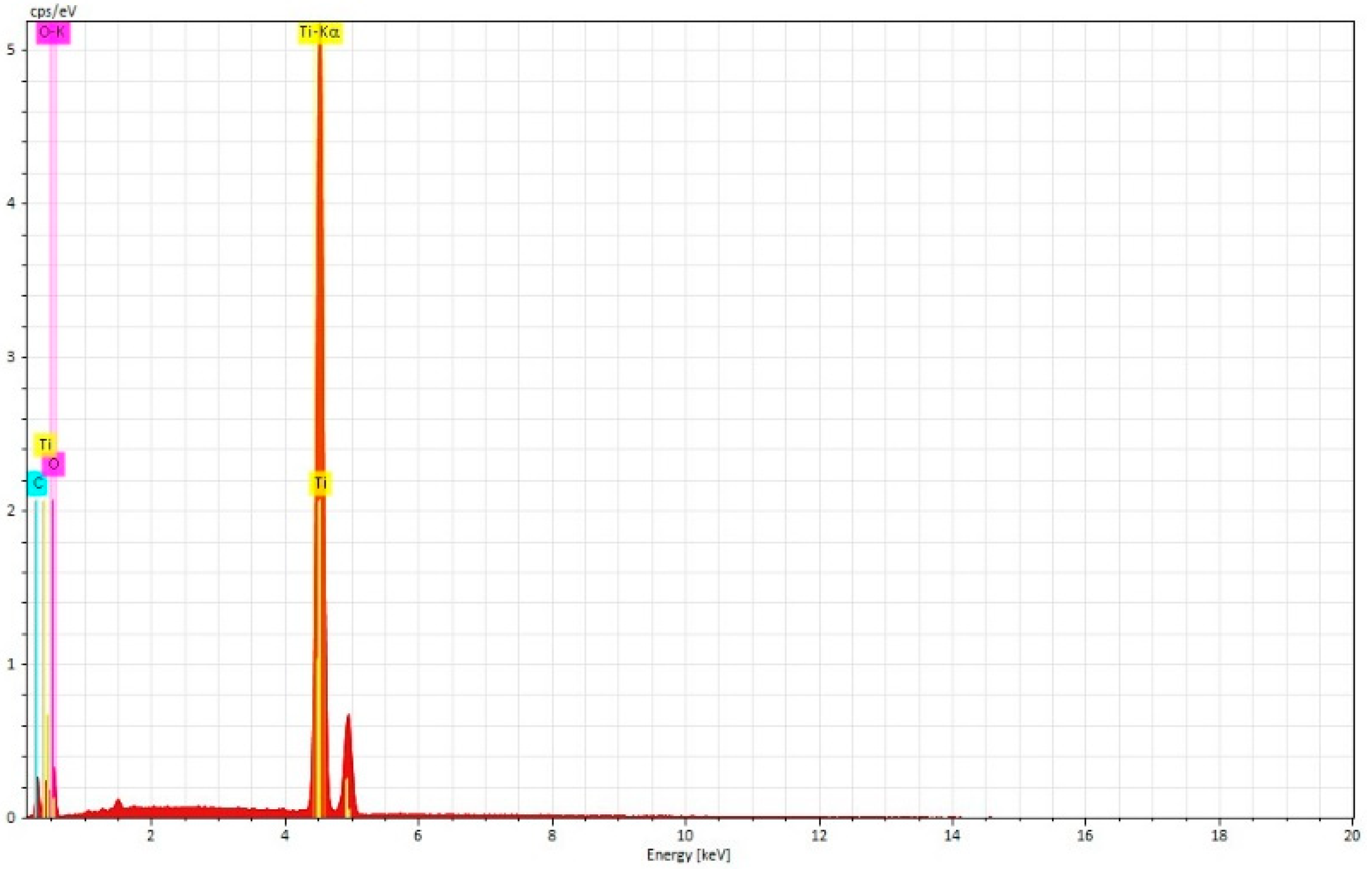
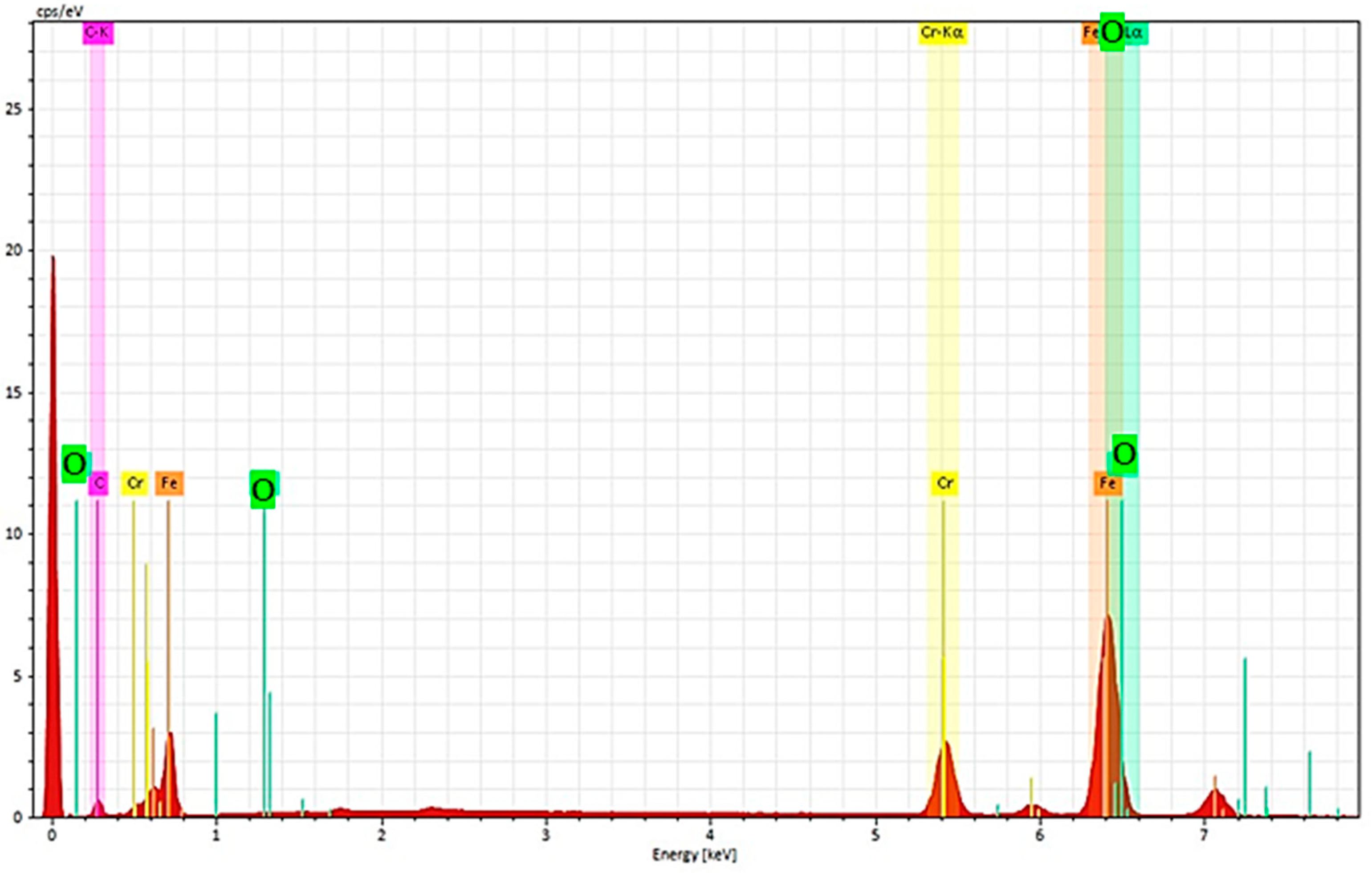
3.2. Scanning Electron Microscopy-EDS Analysis
3.2.1. Non-Sterilized Drill and Conical Tapper
3.2.2. Used and Sterilized Drill and Conical Tapper
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Albrektsson, T.; Berglundh, T.; Lindhe, J. Osseointegration: Historic Background and Current Concepts. Clin. Periodontol. Implant. Dent. 2003, 4, 809–820. [Google Scholar]
- Bilhan, H.; Geckili, O.; Mumcu, E.; Bozdag, E.; Sünbüloğlu, E.; Kutay, O. Influence of Surgical Technique, Implant Shape and Diameter on the Primary Stability in Cancellous Bone: What Influences Primary Stability in Cancellous Bone. J. Oral Rehabil. 2010, 37, 900–907. [Google Scholar] [CrossRef] [PubMed]
- Arys, A.; Philippart, C.; Dourov, N.; He, Y.; Le, Q.T.; Pireaux, J.J. Analysis of Titanium Dental Implants after Failure of Osseointegration: Combined Histological, Electron Microscopy, and X-ray Photoelectron Spectroscopy Approach. J. Biomed. Mater. Res. 1998, 43, 300–312. [Google Scholar] [CrossRef]
- Scarano, A.; Piattelli, A.; Assenza, B.; Carinci, F.; Di Donato, L.; Romani, G.L.; Merla, A. Infrared Thermographic Evaluation of Temperature Modifications Induced during Implant Site Preparation with Cylindrical versus Conical Drills. Clin. Implant Dent. Relat. Res. 2011, 13, 319–323. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Lorusso, F.; Noumbissi, S. Infrared Thermographic Evaluation of Temperature Modifications Induced during Implant Site Preparation with Steel vs. Zirconia Implant Drill. J. Clin. Med. 2020, 9, 148. [Google Scholar] [CrossRef] [Green Version]
- Sener, B.C.; Dergin, G.; Gursoy, B.; Kelesoglu, E.; Slih, I. Effects of Irrigation Temperature on Heat Control in Vitro at Different Drilling Depths. Clin. Oral Implant. Res. 2009, 20, 294–298. [Google Scholar] [CrossRef]
- Benington, I.C.; Biagioni, P.A.; Briggs, J.; Sheridan, S.; Lamey, P.-J. Thermal Changes Observed at Implant Sites during Internal and External Irrigation: Thermal Changes at Implant Sites during Irrigation. Clin. Oral Implant. Res. 2002, 13, 293–297. [Google Scholar] [CrossRef]
- Lucchiari, N.; Frigo, A.C.; Stellini, E.; Coppe, M.; Berengo, M.; Bacci, C. In Vitro Assessment with the Infrared Thermometer of Temperature Differences Generated During Implant Site Preparation: The Traditional Technique Versus the Single-Drill Technique: Heat with Traditional and Single-Bur Drilling. Clin. Implant. Dent. Relat. Res. 2016, 18, 182–191. [Google Scholar] [CrossRef]
- Ozcan, M.; Salimov, F.; Temmerman, A.; Turer, O.U.; Alkaya, B.; Haytac, M.C. The Evaluation of Different Osteotomy Drilling Speed Protocols on Cortical Bone Temperature, Implant Stability and Bone Healing: An Experimental Study in an Animal Model. J. Oral Implant. 2022, 48, 3–8. [Google Scholar] [CrossRef]
- Tur, D.; Giannis, K.; Unger, E.; Mittlböck, M.; Rausch-Fan, X.; Strbac, G.D. Thermal Effects of Various Drill Materials during Implant Site Preparation—Ceramic vs. Stainless Steel Drills: A Comparative in Vitro Study in a Standardised Bovine Bone Model. Clin. Oral Implant. Res. 2021, 32, 154–166. [Google Scholar] [CrossRef]
- Cattoni, F.; Merlone, A.; Broggi, R.; Manacorda, M.; Vinci, R. Computer-Assisted Prosthetic Planning and Implant Design with Integrated Digital Bite Registration: A Treatment Protocol. J. Biol. Regul. Homeost. Agents 2021, 35, 11–29. [Google Scholar] [CrossRef] [PubMed]
- Merlone, A.; Tetè, G.; Cantile, N.; Manacorda, M.; Cattoni, F. Minimally Invasive Digital Implant-Prosthetic Procedure in “All on 4” Rehabilitation in Patients with Special Needs: A Three-Year Follow-Up. J. Biol. Regul. Homeost. Agents 2021, 35, 71–85. [Google Scholar] [CrossRef] [PubMed]
- Cattoni, F.; Chirico, L.; Merlone, A.; Manacorda, M.; Vinci, R.; Gherlone, E.F. Digital Smile Designed Computer-Aided Surgery versus Traditional Workflow in “All on Four” Rehabilitations: A Randomized Clinical Trial with 4-Years Follow-Up. Int. J. Environ. Res. Public Health 2021, 18, 3449. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Petrini, M.; Mastrangelo, F.; Noumbissi, S.; Lorusso, F. The Effects of Liquid Disinfection and Heat Sterilization Processes on Implant Drill Roughness: Energy Dispersion X-ray Microanalysis and Infrared Thermography. J. Clin. Med. 2020, 9, 1019. [Google Scholar] [CrossRef] [Green Version]
- Scarano, A.; Carinci, F.; Lorusso, F.; Festa, F.; Bevilacqua, L.; Santos de Oliveira, P.; Maglione, M. Ultrasonic vs Drill Implant Site Preparation: Post-Operative Pain Measurement Through VAS, Swelling and Crestal Bone Remodeling: A Randomized Clinical Study. Materials 2018, 11, 2516. [Google Scholar] [CrossRef] [Green Version]
- Oh, T.-J.; Yoon, J.; Misch, C.E.; Wang, H.-L. The Causes of Early Implant Bone Loss: Myth or Science? J. Periodontol. 2002, 73, 322–333. [Google Scholar] [CrossRef] [PubMed]
- Misch, C.E.; Dietsh-Misch, F.; Hoar, J.; Beck, G.; Hazen, R.; Misch, C.M. A Bone Quality–Based Implant System: First Year of Prosthetic Loading. J. Oral Implant. 1999, 25, 185–197. [Google Scholar] [CrossRef]
- Misch, C.E.; Qu, Z.; Bidez, M.W. Mechanical Properties of Trabecular Bone in the Human Mandible: Implications for Dental Implant Treatment Planning and Surgical Placement. J. Oral Maxillofac. Surg. 1999, 57, 700–706. [Google Scholar] [CrossRef]
- Norton, M.R.; Gamble, C. Bone Classification: An Objective Scale of Bone Density Using the Computerized Tomography Scan: Bone Classification: An Objective Scale of Bone Density Using the Computerized Tomography Scan. Clin. Oral Implant. Res. 2001, 12, 79–84. [Google Scholar] [CrossRef]
- Bubeck, K.A.; García-López, J.; Maranda, L.S. In Vitro Comparison of Cortical Bone Temperature Generation between Traditional Sequential Drilling and a Newly Designed Step Drill in the Equine Third Metacarpal Bone. Veter-Comp. Orthop. Traumatol. 2009, 22, 442–447. [Google Scholar] [CrossRef]
- Chacon, G.E.; Bower, D.L.; Larsen, P.E.; McGlumphy, E.A.; Beck, F.M. Heat Production by 3 Implant Drill Systems after Repeated Drilling and Sterilization. J. Oral Maxillofac. Surg. 2006, 64, 265–269. [Google Scholar] [CrossRef] [PubMed]
- Sharawy, M.; Misch, C.E.; Weller, N.; Tehemar, S. Heat Generation during Implant Drilling: The Significance of Motor Speed. J. Oral Maxillofac. Surg. 2002, 60, 1160–1169. [Google Scholar] [CrossRef] [Green Version]
- Gronkiewicz, K.; Majewski, P.; Wisniewska, G.; Pihut, M.; Loster, B.W.; Majewski, S. Experimental Research on the Possibilities of Maintaining Thermal Conditions within the Limits of the Physiological Conditions during Intraoral Preparation of Dental Implants. J. Physiol. Pharmacol. 2009, 60 (Suppl. 8), 123–127. [Google Scholar] [PubMed]
- Ercoli, C.; Funkenbusch, P.D.; Lee, H.-J.; Moss, M.E.; Graser, G.N. The Influence of Drill Wear on Cutting Efficiency and Heat Production during Osteotomy Preparation for Dental Implants: A Study of Drill Durability. Int. J. Oral Maxillofac. Implant. 2004, 19, 335–349. [Google Scholar]
- Oliveira, N.; Alaejos-Algarra, F.; Mareque-Bueno, J.; Ferrés-Padró, E.; Hernández-Alfaro, F. Thermal Changes and Drill Wear in Bovine Bone during Implant Site Preparation. A Comparative in Vitro Study: Twisted Stainless Steel and Ceramic Drills: Thermal Changes and Drill Wear in Bovine Bone. Clin. Oral Implant. Res. 2012, 23, 963–969. [Google Scholar] [CrossRef] [PubMed]
- Möhlhenrich, S.C.; Modabber, A.; Steiner, T.; Mitchell, D.A.; Hölzle, F. Heat Generation and Drill Wear during Dental Implant Site Preparation: Systematic Review. Br. J. Oral Maxillofac. Surg. 2015, 53, 679–689. [Google Scholar] [CrossRef]
- Stelzle, F.; Frenkel, C.; Riemann, M.; Knipfer, C.; Stockmann, P.; Nkenke, E. The Effect of Load on Heat Production, Thermal Effects and Expenditure of Time during Implant Site Preparation—An Experimental Ex Vivo Comparison between Piezosurgery and Conventional Drilling. Clin. Oral Implant. Res. 2014, 25, e140–e148. [Google Scholar] [CrossRef]
- Sumer, M.; Misir, A.F.; Telcioglu, N.T.; Guler, A.U.; Yenisey, M. Comparison of Heat Generation during Implant Drilling Using Stainless Steel and Ceramic Drills. J. Oral Maxillofac. Surg. 2011, 69, 1350–1354. [Google Scholar] [CrossRef]
- Harder, S.; Egert, C.; Wenz, H.J.; Jochens, A.; Kern, M. Influence of the Drill Material and Method of Cooling on the Development of Intrabony Temperature during Preparation of the Site of an Implant. Br. J. Oral Maxillofac. Surg. 2013, 51, 74–78. [Google Scholar] [CrossRef]
- Koo, K.-T.; Kim, M.-H.; Kim, H.-Y.; Wikesjö, U.M.E.; Yang, J.-H.; Yeo, I.-S. Effects of Implant Drill Wear, Irrigation, and Drill Materials on Heat Generation in Osteotomy Sites. J. Oral Implant. 2015, 41, e19–e23. [Google Scholar] [CrossRef]
- Möhlhenrich, S.C.; Abouridouane, M.; Heussen, N.; Modabber, A.; Klocke, F.; Hölzle, F. Influence of Bone Density and Implant Drill Diameter on the Resulting Axial Force and Temperature Development in Implant Burs and Artificial Bone: An in Vitro Study. Oral Maxillofac. Surg. 2016, 20, 135–142. [Google Scholar] [CrossRef] [PubMed]
- Gehrke, S.A.; Aramburú Júnior, J.S.; Pérez-Albacete Martínez, C.; Ramirez Fernandez, M.P.; Maté Sánchez de Val, J.E.; Calvo-Guirado, J.L. The Influence of Drill Length and Irrigation System on Heat Production during Osteotomy Preparation for Dental Implants: An Ex Vivo Study. Clin. Oral Implant. Res. 2018, 29, 772–778. [Google Scholar] [CrossRef] [PubMed]
- Oh, J.-H.; Fang, Y.; Jeong, S.-M.; Choi, B.-H. The Effect of Low-Speed Drilling without Irrigation on Heat Generation: An Experimental Study. J. Korean Assoc. Oral Maxillofac. Surg. 2016, 42, 9. [Google Scholar] [CrossRef] [Green Version]
- Gehrke, S.A.; Guirado, J.L.C.; Bettach, R.; Fabbro, M.D.; Martínez, C.P.-A.; Shibli, J.A. Evaluation of the Insertion Torque, Implant Stability Quotient and Drilled Hole Quality for Different Drill Design: An in Vitro Investigation. Clin. Oral Implant. Res. 2018, 29, 656–662. [Google Scholar] [CrossRef]
- Guazzi, P.; Grandi, T.; Grandi, G. Implant Site Preparation Using a Single Bur versus Multiple Drilling Steps: 4-Month Post-Loading Results of a Multicenter Randomised Controlled Trial. Eur. J. Oral Implant. 2015, 8, 283–290. [Google Scholar]


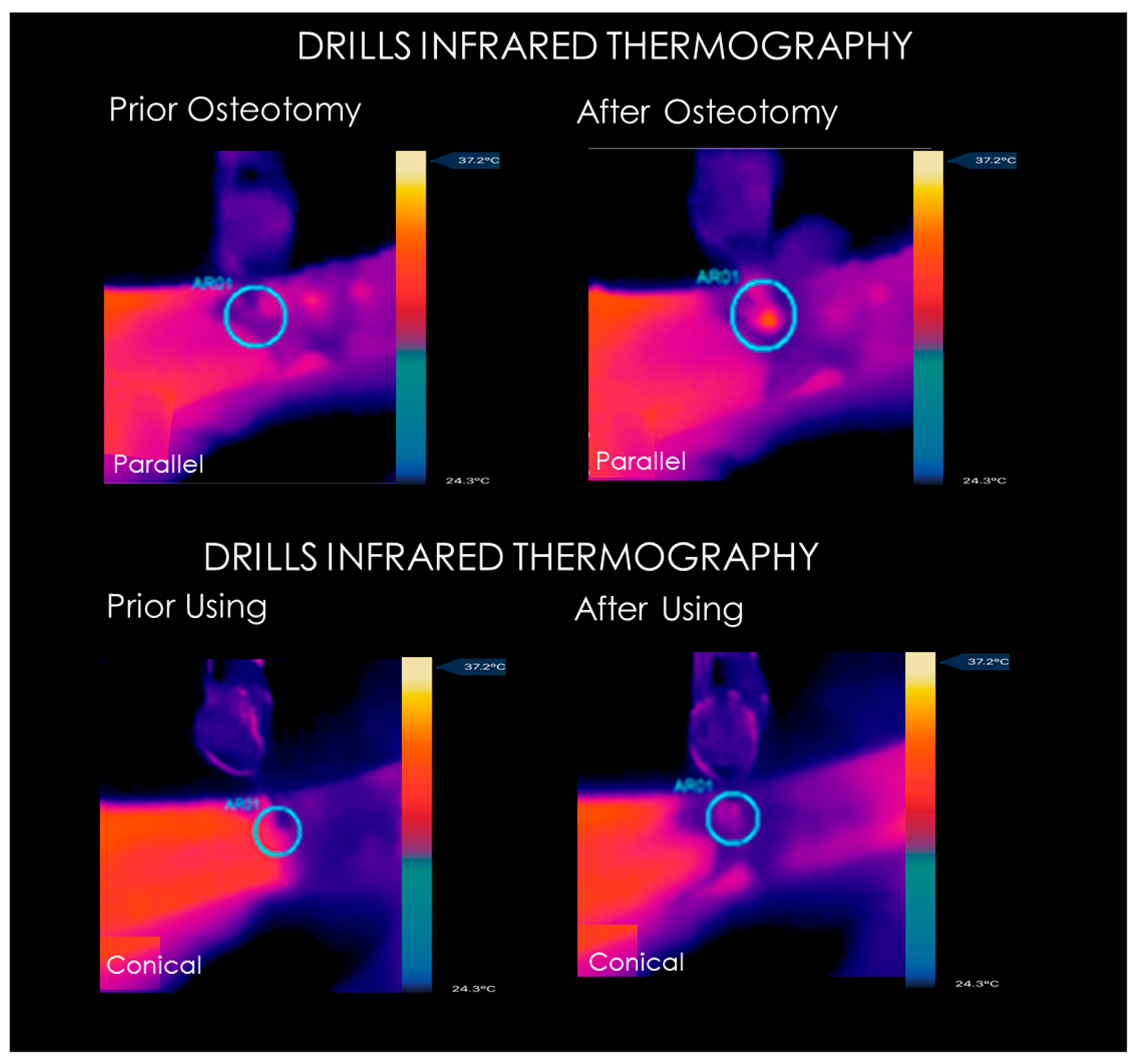




| Drill Bone Temperature (°C). | Baseline | FGR3710 | FGR5513 | FFC3710 | FFC5513 | DRP200 | DRP450 | CTK425 |
|---|---|---|---|---|---|---|---|---|
| 1st osteotomy | 37.0 ± 0.10 °C | 38.6 ± 0.66 | 40.96 ± 0.59 | 39.01 ± 0.51 | 41.12 ± 0.47 | 38.59 ± 0.73 | 39.37 ± 0.63 | 39.25 ± 0.55 |
| After 30th osteotomy | 37.0 ± 0.13 °C | 39.01 ± 0.56 | 41.83 ± 0.56 | 39.37 ± 1.12 | 41.97 ± 0.51 | 39.01 ± 0.56 | 39.89 ± 0.71 | 39.71 ± 0.63 |
| p-value | / | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 |
| TapperBone Temperature (°C) | Baseline | MKN3710 | MKN3711 | MKN3713 | MKN3714 | MSL5510 | MSL5511 | MSL5513 |
|---|---|---|---|---|---|---|---|---|
| 1st osteotomy | 37.0 ± 0.14 °C | 38.1 ± 0.5 | 38.3 ± 0.47 | 38.3 ± 0.50 | 38.5 ± 0.45 | 38.2 ± 0.46 | 38.4 ± 0.57 | 38. 8± 0.66 |
| After 30th osteotomy | 37.0 ± 0.12 °C | 38.1 ± 0.5 | 38.3 ± 0.47 | 38.3 ± 0.50 | 38.5 ± 0.45 | 38.2 ± 0.46 | 38.4 ± 0.57 | 38.8 ± 0.66 |
| p-value | / | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 | * p > 0.05 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lorusso, F.; Gehrke, S.A.; Festa, F.; Scarano, A. Wearing Effect of Implant Steel Drills and Tappers for the Preparation of the Bone Osteotomies: An Infrared Thermal Analysis and Energy Dispersive Spectroscopy-Scanning Electron Microscopy (EDS-SEM) Study. Prosthesis 2022, 4, 679-694. https://doi.org/10.3390/prosthesis4040054
Lorusso F, Gehrke SA, Festa F, Scarano A. Wearing Effect of Implant Steel Drills and Tappers for the Preparation of the Bone Osteotomies: An Infrared Thermal Analysis and Energy Dispersive Spectroscopy-Scanning Electron Microscopy (EDS-SEM) Study. Prosthesis. 2022; 4(4):679-694. https://doi.org/10.3390/prosthesis4040054
Chicago/Turabian StyleLorusso, Felice, Sergio Alexandre Gehrke, Felice Festa, and Antonio Scarano. 2022. "Wearing Effect of Implant Steel Drills and Tappers for the Preparation of the Bone Osteotomies: An Infrared Thermal Analysis and Energy Dispersive Spectroscopy-Scanning Electron Microscopy (EDS-SEM) Study" Prosthesis 4, no. 4: 679-694. https://doi.org/10.3390/prosthesis4040054
APA StyleLorusso, F., Gehrke, S. A., Festa, F., & Scarano, A. (2022). Wearing Effect of Implant Steel Drills and Tappers for the Preparation of the Bone Osteotomies: An Infrared Thermal Analysis and Energy Dispersive Spectroscopy-Scanning Electron Microscopy (EDS-SEM) Study. Prosthesis, 4(4), 679-694. https://doi.org/10.3390/prosthesis4040054










