Comparison of Two Low-Profile Prosthetic Retention System Interfaces: Preliminary Data of an In Vitro Study
Abstract
:1. Introduction
1.1. Background
1.2. Aim
2. Results
3. Discussion
4. Materials and Methods
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Feine, J.S.; E Carlsson, G.; A Awad, M.; Chehade, A.; Duncan, W.J.; Gizani, S.; Head, T.; Heydecke, G.; Lund, J.P.; MacEntee, M.; et al. The McGill consensus statement on overdentures. Mandibular two-implant overdentures as first choice standard of care for edentulous patients. Gerodontology 2002, 19, 601–602. [Google Scholar]
- Awad, M.A.; Rashid, F.; Feine, J.S. The effect of mandibular 2-implant overdentures on oral health-related quality of life: An international multi centre study. Clin. Oral Implants Res. 2014, 25, 46–51. [Google Scholar] [CrossRef] [PubMed]
- Sadowsky, S.J. Mandibular implant-retained overdentures: A literature review. J. Prosthet. Dent. 2001, 86, 468–473. [Google Scholar] [CrossRef] [PubMed]
- Bakke, M.; Holm, B.; Gotfredsen, K. Masticatory function and patient satisfaction with implant-supported mandibular overdentures: A prospective 5-year study. Int. J. Prosthodont. 2002, 15, 575–581. [Google Scholar] [PubMed]
- The Glossary of Prosthodontic Terms. J. Prosthet. Dent. 2005, 94, 10–92. [CrossRef] [PubMed]
- Cune, M.; Van Kampen, F.; Van Der Bilt, A.; Bosman, F. Patient satisfaction and preference with magnet, bar-clip, and ball-socket retained mandibular implant overdentures: A cross-over clinical trial. J. Prosthet. Dent. 2005, 94, 471. [Google Scholar] [CrossRef]
- Kobayashi, M.; Srinivasan, M.; Ammann, P.; Perriard, J.; Ohkubo, C.; Muller, F.; Belser, U.C.; Schimmel, M. Effects of in vitro cyclic dislodging on retentive force and removal torque of three overdenture attachment systems. Clin. Oral Implants Res. 2014, 25, 426–434. [Google Scholar] [CrossRef]
- Rutkunas, V.; Mizutani, H.; Takahashi, H.; Iwasaki, N. Wear simulation effects on overdenture stud attachments. Dent. Mater. J. 2011, 30, 845–853. [Google Scholar] [CrossRef]
- Srinivasan, M.; Schimmel, M.; Badoud, I.; Ammann, P.; Herrmann, F.R.; Muller, F. Influence of implant angulation and cyclic dislodging on the retentive force of two different overdenture attachments - an in vitro study. Clin. Oral Implants Res. 2016, 27, 604–611. [Google Scholar] [CrossRef]
- Alsabeeha, N.H.; Payne, A.G.; Swain, M.V. Attachment systems for mandibular two-implant overdentures: A review of in vitro investigations on retention and wear features. Int. J. Prosthodont. 2009, 22, 429–440. [Google Scholar]
- Kim, H.-Y.; Lee, J.-Y.; Shin, S.-W.; Bryant, S.R. Attachment systems for mandibular implant overdentures: A systematic review. J. Adv. Prosthodont. 2012, 4, 197–203. [Google Scholar] [CrossRef] [PubMed]
- Prasad, D.; Prasad, D.; Buch, M. Selection of attachment systems in fabricating an implant supported overdenture. J. Dent. Implant. 2014, 4, 176. [Google Scholar] [CrossRef]
- Naert, I.; Alsaadi, G.; Quirynen, M. Prosthetic aspects and patient satisfaction with two-implant-retained mandibular overdentures: A 10-year randomized clinical study. Int. J. Prosthodont. 2004, 17, 401–410. [Google Scholar] [CrossRef] [PubMed]
- Sadowsky, S.J.; Caputo, A.A. Effect of anchorage systems and extension base contact on load transfer with mandibular implant-retained overdentures. J. Prosthet. Dent. 2000, 84, 327–334. [Google Scholar] [CrossRef] [PubMed]
- Evtimovska, E.; Masri, R.; Driscoll, C.F.; Romberg, E. The Change in Retentive Values of Locator Attachments and Hader Clips over Time. J. Prosthodont. 2009, 18, 479–483. [Google Scholar] [CrossRef]
- Bramanti, E.; Cervino, G.; Lauritano, F.; Fiorillo, L.; D’Amico, C.; Sambataro, S.; Denaro, D.; Famà, F.; Ierardo, G.; Polimeni, A.; et al. FEM and Von Mises Analysis on Prosthetic Crowns Structural Elements: Evaluation of Different Applied Materials. Sci. World J. 2017, 2017, 1–7. [Google Scholar] [CrossRef]
- Bramanti, E. Oral health-related quality of life in partially edentulous patients before and after implant therapy: A 2-year longitudinal study. Oral Implant. 2013, 6, 37–42. [Google Scholar] [CrossRef]
- Cicciù, M.; Beretta, M.; Risitano, G.; Maiorana, C. Cemented-retained vs screw-retained implant restorations: An investigation on 1939 dental implants. Minerva Stomatol. 2008, 57, 167–179. [Google Scholar]
- Stefano, D.; De Stefano, R. Psychological Factors in Dental Patient Care: Odontophobia. Medicina 2019, 55, 678. [Google Scholar] [CrossRef]
- Germano, F.; Bramanti, E.; Arcuri, C.; Cecchetti, F.; Cicciù, M. Atomic force microscopy of bacteria from periodontal subgingival biofilm: Preliminary study results. Eur. J. Dent. 2013, 7, 152–158. [Google Scholar] [CrossRef]
- Wichmann, M.G.; Kuntze, W. Wear behavior of precision attachments. Int. J. Prosthodont. 1999, 12, 409–414. [Google Scholar] [PubMed]
- Besimo, C.E.; Guarneri, A. In vitro retention force changes of prefabricated attachments for overdentures. J. Oral Rehabilitation 2003, 30, 671–678. [Google Scholar] [CrossRef] [PubMed]
- Chaves, C.; De Souza, R.; Cunha, T.; Vecchia, M.; Ribeiro, A.; Bruniera, J.; Silva-Sousa, Y. Preliminary In Vitro Study on O-Ring Wear in Mini-Implant–Retained Overdentures. Int. J. Prosthodont. 2016, 29, 357–359. [Google Scholar] [CrossRef] [PubMed] [Green Version]
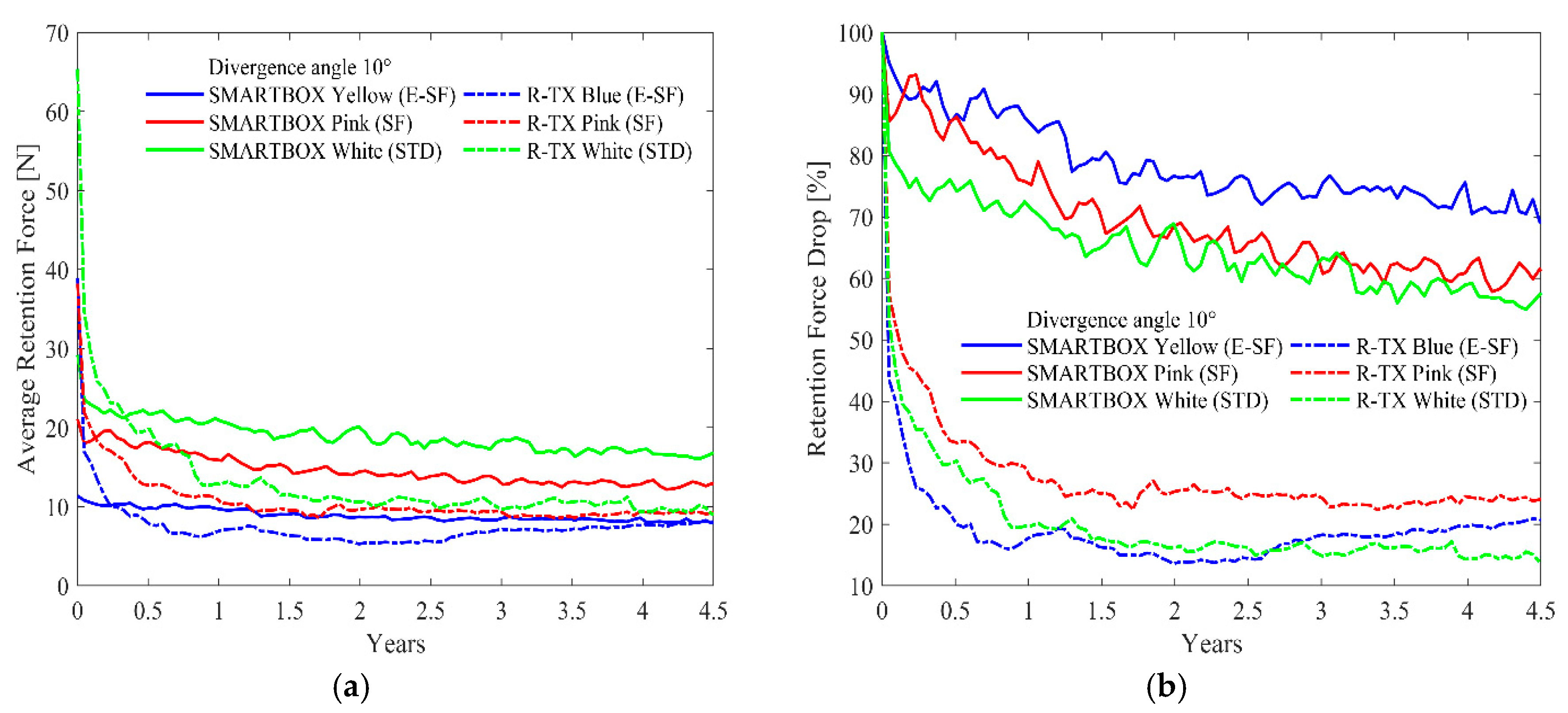
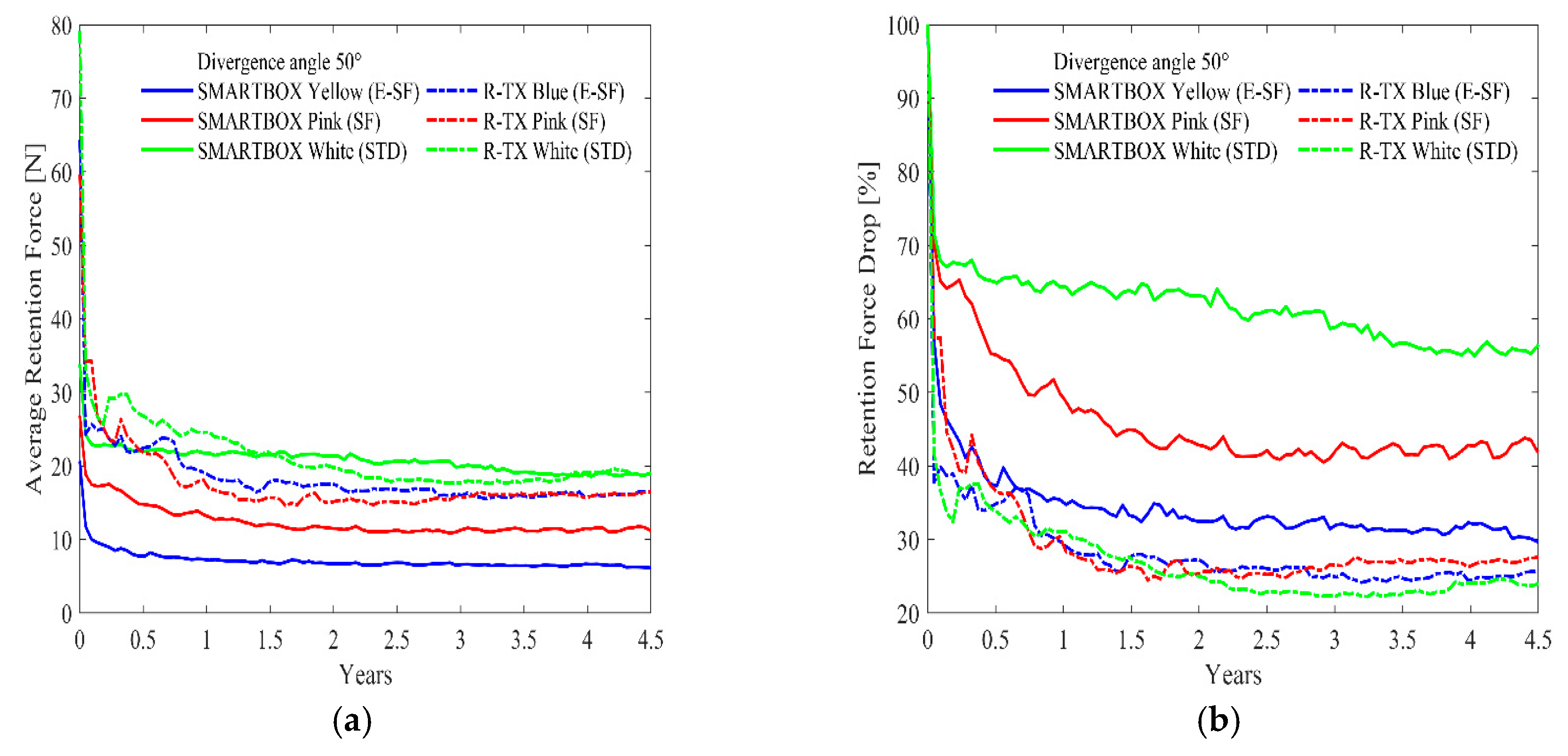


| Cap Class | OT EQUATOR® SMART BOX | LOCATOR® R-TX |
|---|---|---|
| Extra-Soft (E-SF) | Yellow (0.60 kg) | Blue (0.68 Kg) |
| Soft (SF) | Pink (1.20 kg) | Pink (1.36 kg) |
| Standard (STD) | White (1.80 kg) | White (2.27 kg) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cervino, G.; Montanari, M.; Santonocito, D.; Nicita, F.; Baldari, R.; De Angelis, C.; Storni, G.; Fiorillo, L. Comparison of Two Low-Profile Prosthetic Retention System Interfaces: Preliminary Data of an In Vitro Study. Prosthesis 2019, 1, 54-60. https://doi.org/10.3390/prosthesis1010007
Cervino G, Montanari M, Santonocito D, Nicita F, Baldari R, De Angelis C, Storni G, Fiorillo L. Comparison of Two Low-Profile Prosthetic Retention System Interfaces: Preliminary Data of an In Vitro Study. Prosthesis. 2019; 1(1):54-60. https://doi.org/10.3390/prosthesis1010007
Chicago/Turabian StyleCervino, Gabriele, Marco Montanari, Dario Santonocito, Fabiana Nicita, Riccardo Baldari, Claudio De Angelis, Gianni Storni, and Luca Fiorillo. 2019. "Comparison of Two Low-Profile Prosthetic Retention System Interfaces: Preliminary Data of an In Vitro Study" Prosthesis 1, no. 1: 54-60. https://doi.org/10.3390/prosthesis1010007
APA StyleCervino, G., Montanari, M., Santonocito, D., Nicita, F., Baldari, R., De Angelis, C., Storni, G., & Fiorillo, L. (2019). Comparison of Two Low-Profile Prosthetic Retention System Interfaces: Preliminary Data of an In Vitro Study. Prosthesis, 1(1), 54-60. https://doi.org/10.3390/prosthesis1010007








