Associations between the Presence of Granulomata and Disease Phenotype and Outcomes in Children Diagnosed with Crohn’s Disease
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Data Management
2.3. Disease Outcome Parameters
2.4. Data Analysis
3. Results
3.1. Patient Population
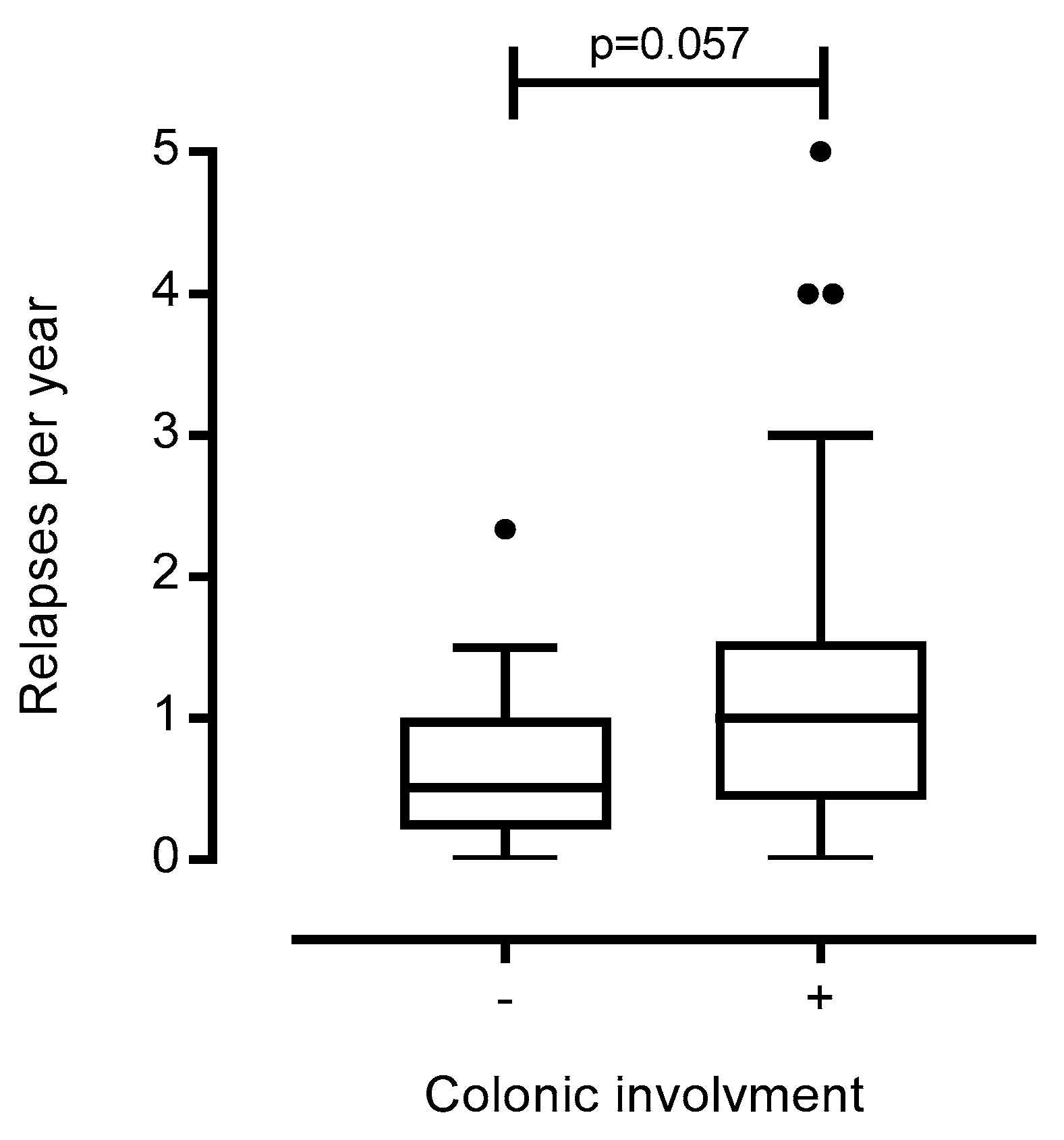
3.2. Disease Phenotype and Outcomes According to the Presence or Absence of Granuloma
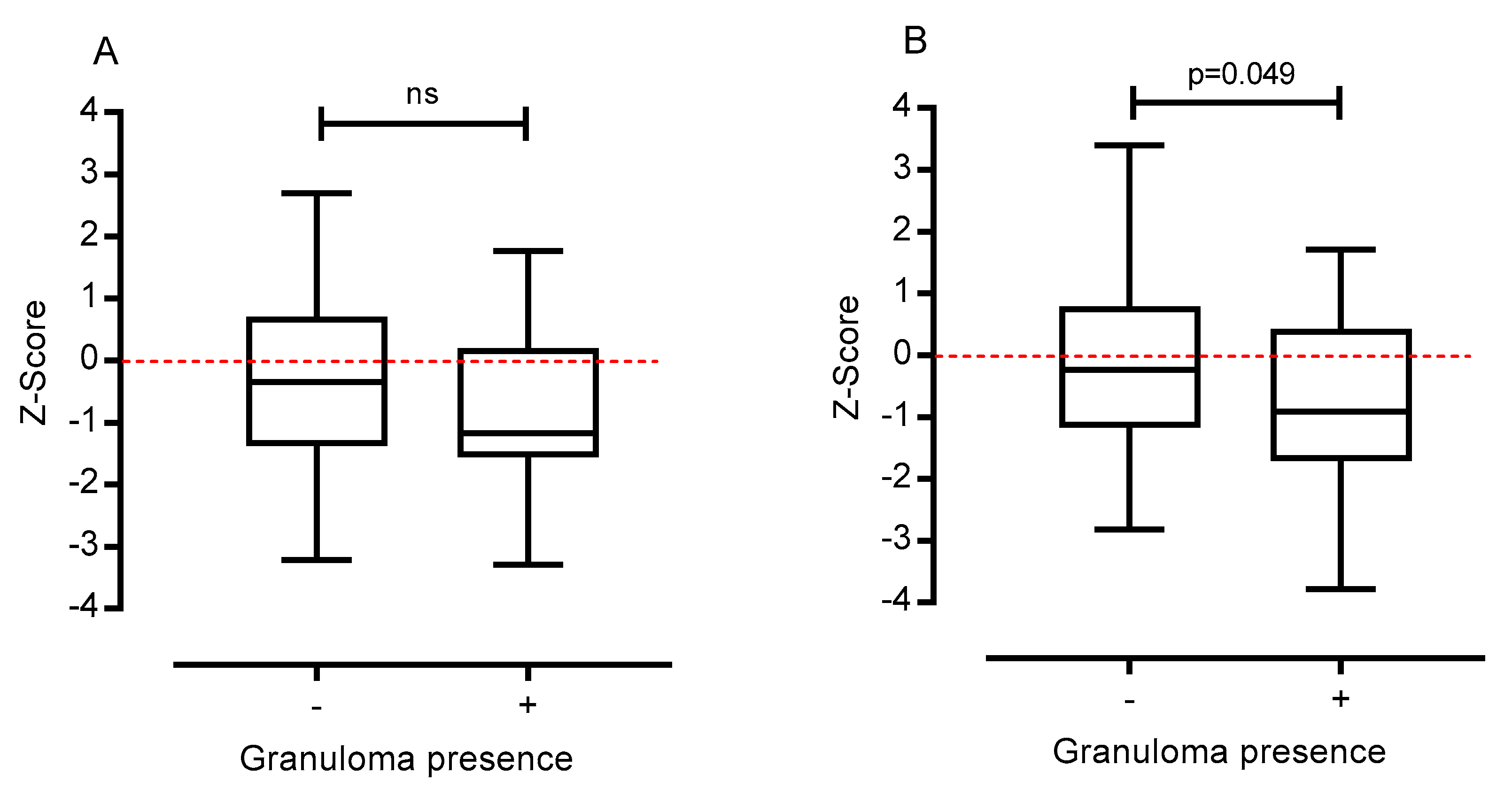
3.3. Nutrition
4. Discussion
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Loddo, I.; Romano, C. Inflammatory bowel disease: Genetics, epigenetics, and pathogenesis. Front. Immunol. 2015, 6, 551. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhang, Y.Z.; Li, Y.Y. Inflammatory bowel disease: Pathogenesis. World J. Gastroenterol. 2014, 20, 91–99. [Google Scholar] [CrossRef] [PubMed]
- Rosen, M.J.; Dhawan, A.; Saeed, S.A. Inflammatory Bowel Disease in Children and Adolescents. JAMA Pediatr. 2015, 169, 1053–1060. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sykora, J.; Pomahacova, R.; Kreslova, M.; Cvalinova, D.; Stych, P.; Schwarz, J. Current global trends in the incidence of pediatric-onset inflammatory bowel disease. World J. Gastroenterol. 2018, 24, 2741–2763. [Google Scholar] [CrossRef]
- Pigneur, B.; Seksik, P.; Viola, S.; Viala, J.; Beaugerie, L.; Girardet, J.P.; Ruemmele, F.M.; Cosnes, J. Natural history of Crohn’s disease: Comparison between childhood-and adult-onset disease. Inflamm. Bowel Dis. 2010, 16, 953–961. [Google Scholar] [CrossRef] [Green Version]
- Van Limbergen, J.; Russell, R.K.; Drummond, H.E.; Aldhous, M.C.; Round, N.K.; Nimmo, E.R.; Smith, L.; Gillett, P.M.; McGrogan, P.; Weaver, L.T.; et al. Definition of phenotypic characteristics of childhood-onset inflammatory bowel disease. Gastroenterology 2008, 135, 1114–1122. [Google Scholar] [CrossRef] [Green Version]
- Levine, A.; Koletzko, S.; Turner, D.; Escher, J.C.; Cucchiara, S.; de Ridder, L.; Kolho, K.L.; Veres, G.; Russell, R.K.; Paerregaard, A.; et al. ESPGHAN revised porto criteria for the diagnosis of inflammatory bowel disease in children and adolescents. J. Pediatr. Gastroenterol. Nutr. 2014, 58, 795–806. [Google Scholar] [CrossRef] [Green Version]
- Ruemmele, F.M.; Veres, G.; Kolho, K.L.; Griffiths, A.; Levine, A.; Escher, J.C.; Amil Dias, J.; Barabino, A.; Braegger, C.P.; Bronsky, J.; et al. Consensus guidelines of ECCO/ESPGHAN on the medical management of pediatric Crohn’s disease. J. Crohns Colitis 2014, 8, 1179–1207. [Google Scholar] [CrossRef] [Green Version]
- Freeman, H.J. Natural history and long-term clinical course of Crohn’s disease. World J. Gastroenterol. 2014, 20, 31–36. [Google Scholar] [CrossRef]
- Heresbach, D.; Alexandre, J.L.; Branger, B.; Bretagne, J.F.; Cruchant, E.; Dabadie, A.; Dartois-Hoguin, M.; Girardot, P.M.; Jouanolle, H.; Kerneis, J.; et al. Frequency and significance of granulomas in a cohort of incident cases of Crohn’s disease. Gut 2005, 54, 215–222. [Google Scholar] [CrossRef] [Green Version]
- Molnar, T.; Tiszlavicz, L.; Gyulai, C.; Nagy, F.; Lonovics, J. Clinical significance of granuloma in Crohn’s disease. World J. Gastroenterol. 2005, 11, 3118–3121. [Google Scholar] [CrossRef] [PubMed]
- De Matos, V.; Russo, P.A.; Cohen, A.B.; Mamula, P.; Baldassano, R.N.; Piccoli, D.A. Frequency and clinical correlations of granulomas in children with Crohn disease. J. Pediatr. Gastroenterol. Nutr. 2008, 46, 392–398. [Google Scholar] [CrossRef] [PubMed]
- Jevon, G.P.; Madhur, R. Endoscopic and histologic findings in pediatric inflammatory bowel disease. Gastroenterol. Hepatol. (N Y) 2010, 6, 174–180. [Google Scholar]
- Mazor, Y.; Karban, A.; Nesher, S.; Weiss, B.; Leshinsky-Silver, E.; Levine, A.; Eliakim, R. Granulomas in Crohn’s disease: Are newly discovered genetic variants involved? J. Crohns Colitis 2010, 4, 438–443. [Google Scholar] [CrossRef] [Green Version]
- Rothschild, B.; Rinawi, F.; Herman, Y.; Nir, O.; Shamir, R.; Assa, A. Prognostic significance of granulomas in children with Crohn’s disease. Scand. J. Gastroenterol. 2017, 52, 716–721. [Google Scholar] [CrossRef] [PubMed]
- Denoya, P.; Canedo, J.; Berho, M.; Allende, D.S.; Bennett, A.E.; Rosen, L.; Hull, T.; Wexner, S.D. Granulomas in Crohn’s disease: Does progression through the bowel layers affect presentation or predict recurrence? Colorectal Dis. 2011, 13, 1142–1147. [Google Scholar] [CrossRef]
- Markowitz, J.; Kahn, E.; Daum, F. Prognostic significance of epithelioid granulomas found in rectosigmoid biopsies at the initial presentation of pediatric Crohn’s disease. J. Pediatr. Gastroenterol. Nutr. 1989, 9, 182–186. [Google Scholar] [CrossRef]
- So, H.; Ye, B.D.; Park, Y.S.; Kim, J.; Kim, J.S.; Moon, W.; Lee, K.M.; Kim, Y.S.; Keum, B.; Kim, S.E.; et al. Gastric lesions in patients with Crohn’s disease in Korea: A multicenter study. Intest. Res. 2016, 14, 60–68. [Google Scholar] [CrossRef] [Green Version]
- Ramzan, N.N.; Leighton, J.A.; Heigh, R.I.; Shapiro, M.S. Clinical significance of granuloma in Crohn’s disease. Inflamm. Bowel Dis. 2002, 8, 168–173. [Google Scholar] [CrossRef]
- Hong, S.W.; Yoon, H.; Shin, C.M.; Park, Y.S.; Kim, N.; Lee, D.H.; Kim, J.S. Clinical Significance of Granulomas in Crohn’s Disease: A Systematic Review and Meta-analysis. J. Gastroenterol. Hepatol. 2019, 35, 364–373. [Google Scholar] [CrossRef]
- Johnson, C.M.; Hartman, D.J.; Ramos-Rivers, C.; Rao, B.B.; Bhattacharya, A.; Regueiro, M.; Schwartz, M.; Swoger, J.; Al Hashash, J.; Barrie, A.; et al. Epithelioid Granulomas Associate With Increased Severity and Progression of Crohn’s Disease, Based on 6-Year Follow-Up. Clin. Gastroenterol. Hepatol. 2018, 16, 900–907. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Watermeyer, G.; Thomson, S.R. Granulomas at initial diagnosis of Crohn’s disease signal a poor outcome. S. Afr. Med. J. 2015, 105, 480–483. [Google Scholar] [CrossRef] [PubMed]
| Overall Cohort (n = 94) | Granuloma Positive (n = 49) | Granuloma Negative (n = 45) | Significance | ||||
|---|---|---|---|---|---|---|---|
| Gender (Male) | 49 | (52.1) | 29 | (59.2) | 20 | (40.8) | NS |
| Age at diagnosis: | |||||||
| A1a (0 < 10 yrs) | 22 | (23.4) | 8 | (16.3) | 11 | (24.4) | NS |
| A1b (10 < 17 yrs) | 72 | (76.6) | 41 | (83.7) | 34 | (75.5) | NS |
| Disease location at diagnosis: | |||||||
| L1 ileum | 18 | (19.1) | 4 | (8.2) | 14 | (31.1) | p = 0.005 |
| L2 colonic | 24 | (25.5) | 15 | (30.6) | 9 | (20.0) | NS |
| L3 ileocolonic | 50 | (53.2) | 30 | (61.2) | 21 | (46.7) | NS |
| L4 isolated upper gut | 1 | (1.1) | 0 | (0.0) | 1 | (2.2) | NS |
| Upper gut involvement modifier | 40 | (42.6) | 26 | (53.1) | 14 | (31.1) | p = 0.032 |
| Disease behaviour: | |||||||
| B1 non-stricturing non-penetrating | 70 | (73.4) | 34 | (69.4) | 36 | (80.0) | NS |
| B2 stricturing | 19 | (20.2) | 10 | (20.4) | 9 | (20.0) | NS |
| B3 penetrating | 5 | (6.4) | 5 | (10.2) | 0 | (0.0) | NS |
| B2B3 stricturing and penetrating | 0 | (0.0) | 0 | (0.0) | 0 | (0.0) | - |
| p perianal modifier | 54 | (57.4) | 32 | (65.3) | 22 | (48.8) | NS |
| Extra-intestinal manifestation at diagnosis (yes) | 26 | (27.7) | 14 | (28.6) | 12 | (26.7) | NS |
| Surgery (yes) | 33 | (35.1) | 19 | (38.8) | 14 | (31.1) | NS |
| Ever used: | |||||||
| Biologics | 36 | (38.3) | 24 | (48.9) | 12 | (26.7) | p = 0.026 |
| Immunomodulators | 83 | (88.3) | 48 | (97.9) | 35 | (77.8) | p = 0.002 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Appleton, L.; Watt, E.; Jagger, F.; Hansen, R.; Gearry, R.B.; Day, A.S. Associations between the Presence of Granulomata and Disease Phenotype and Outcomes in Children Diagnosed with Crohn’s Disease. Gastrointest. Disord. 2020, 2, 164-170. https://doi.org/10.3390/gidisord2020017
Appleton L, Watt E, Jagger F, Hansen R, Gearry RB, Day AS. Associations between the Presence of Granulomata and Disease Phenotype and Outcomes in Children Diagnosed with Crohn’s Disease. Gastrointestinal Disorders. 2020; 2(2):164-170. https://doi.org/10.3390/gidisord2020017
Chicago/Turabian StyleAppleton, Laura, Euan Watt, Fiona Jagger, Richard Hansen, Richard B. Gearry, and Andrew S. Day. 2020. "Associations between the Presence of Granulomata and Disease Phenotype and Outcomes in Children Diagnosed with Crohn’s Disease" Gastrointestinal Disorders 2, no. 2: 164-170. https://doi.org/10.3390/gidisord2020017
APA StyleAppleton, L., Watt, E., Jagger, F., Hansen, R., Gearry, R. B., & Day, A. S. (2020). Associations between the Presence of Granulomata and Disease Phenotype and Outcomes in Children Diagnosed with Crohn’s Disease. Gastrointestinal Disorders, 2(2), 164-170. https://doi.org/10.3390/gidisord2020017






