Innovative Robotic Technologies and Artificial Intelligence in Pharmacy and Medicine: Paving the Way for the Future of Health Care—A Review
Abstract
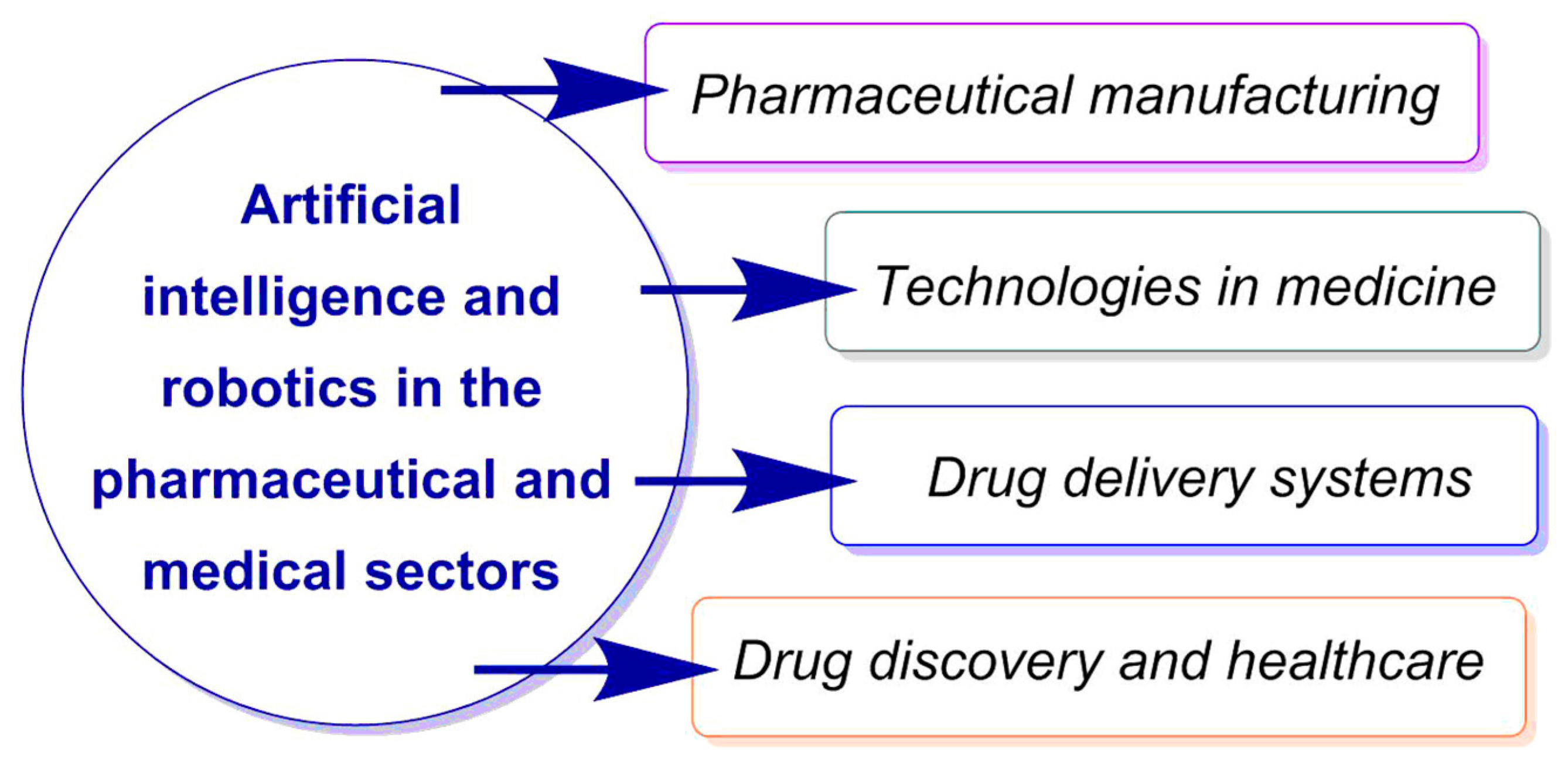
:1. Introduction
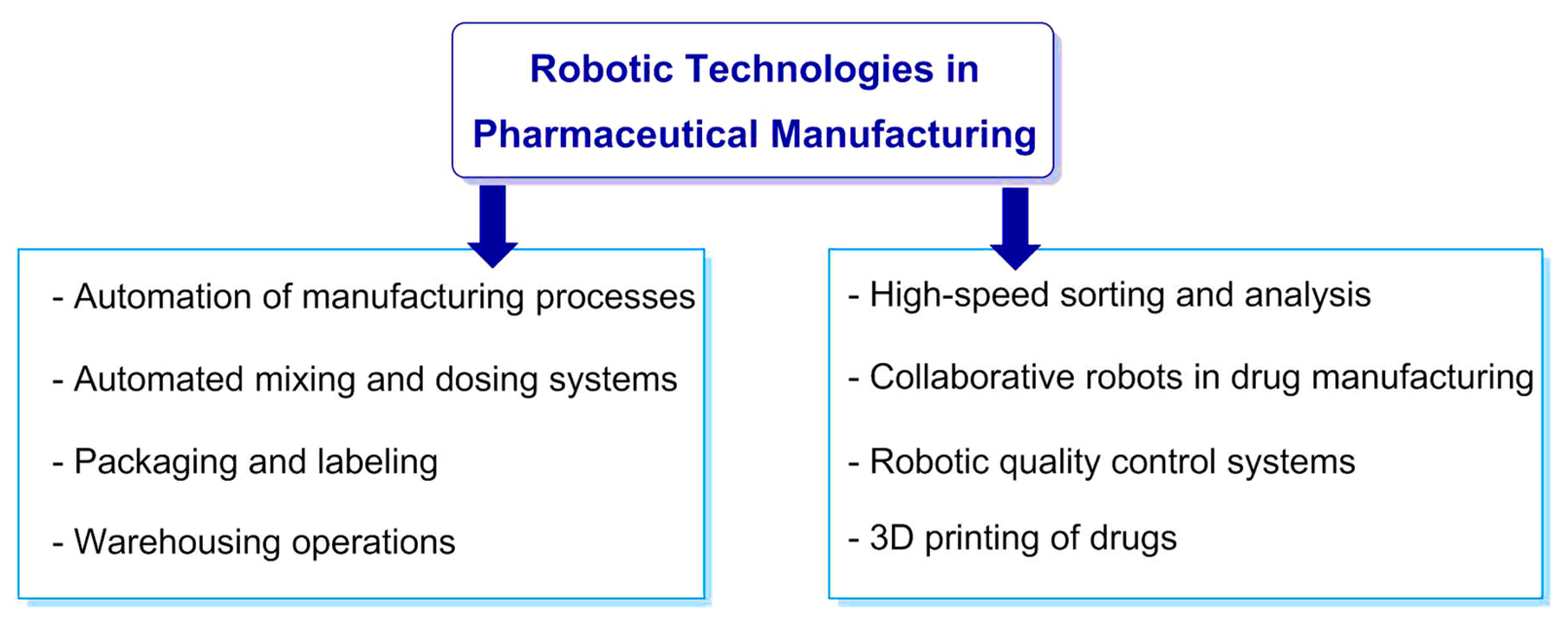
2. Robotic Technologies in Pharmaceutical Manufacturing
- Automation of manufacturing processes: Robots and automated systems are increasingly being used to perform a variety of tasks, including compounding, dosing, forming, and filling of medicinal products.
- Automated mixing and dosing systems allow for accurate dosing and mixing of drug components, which ensures product uniformity and reduces the risk of deviations from quality standards.
- Packaging and labeling: Robots can automatically package, label, and stack finished products, helping to increase efficiency and reduce labor costs.
- Warehousing operations: Robots can be used to automate the warehousing, shipping, and transportation processes of products, ensuring a high level of compliance and quality assurance.
- High-speed sorting and analysis: Robots can perform high-speed procedures such as component sorting or drug testing, increasing productivity and ensuring the accuracy of results.
- Collaborative robots (cobots) in drug manufacturing: Cobots work alongside human operators to perform tasks such as drug packaging and labeling, enhancing productivity while reducing the potential for errors.
- Robotic quality control systems: Advanced robotics and machine vision technologies are employed to inspect pharmaceutical products for defects, ensuring compliance with stringent quality standards and reducing the likelihood of product recalls. They can also monitor compliance of manufacturing processes with GMP (good manufacturing practice) standards.
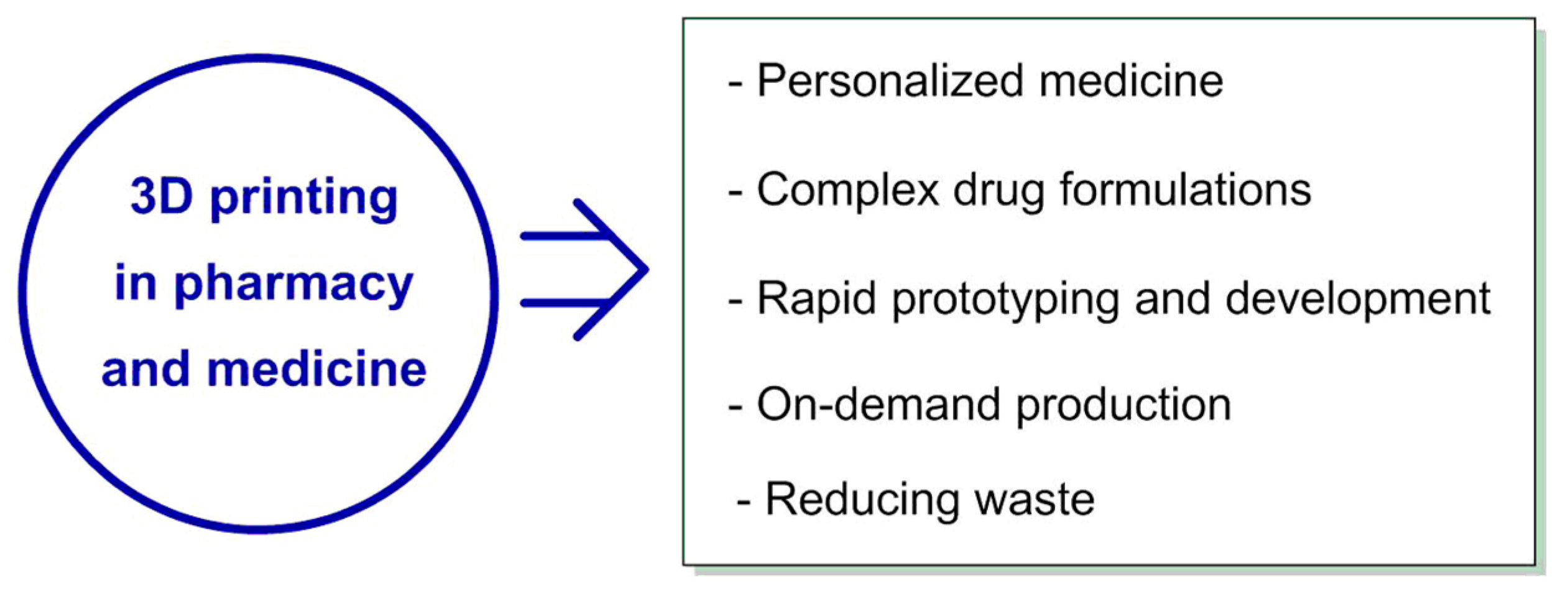
- 3D printing of drugs: The use of 3D printing in the field of drug production allows for the creation of personalized doses and forms of drugs that can take into account the individual needs of patients. Furthermore, 3D printing can help in the manufacture of complex tablet geometries, improving their solubility and bioavailability.
- Personalized medicine [44]: One of the most promising applications of 3D printing in drug production is the creation of personalized medications. With 3D printing, it is possible to tailor drugs to specific patients by adjusting the dosage, release profile, and even the combination of active pharmaceutical ingredients (APIs) based on individual needs. This can lead to more effective treatments and reduced side effects for patients.
- Complex drug formulations [45]: Three-dimensional printing enables the production of complex drug formulations that may be challenging for manufacture using traditional methods. For example, it can create multilayered tablets with different release profiles for each layer or intricate geometries that can affect the drug’s dissolution and absorption rates.
- Rapid prototyping and development [46]: Three-dimensional printing can significantly speed up the drug development process by allowing researchers to create and test new drug formulations and delivery systems. This can reduce the time and cost associated with bringing new medications to market.
- On-demand production [47,48]: Three-dimensional printing enables decentralized and on-demand drug production, allowing for smaller batch sizes and reduced inventory costs. This can be particularly beneficial where immediate access to medication is needed, such as in disaster relief or remote locations.
3. Robotic Drug Delivery Systems
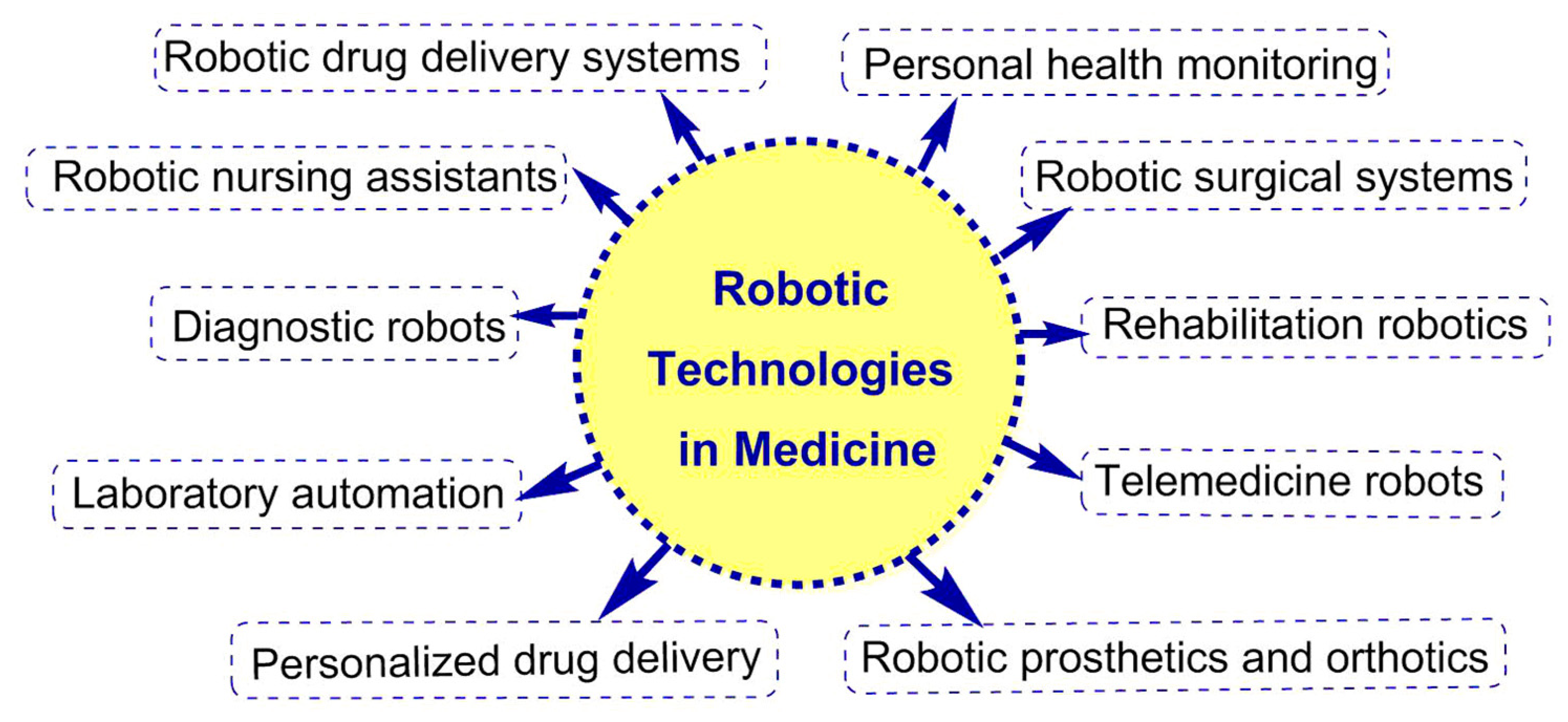
4. Robotic Technologies in Medicine
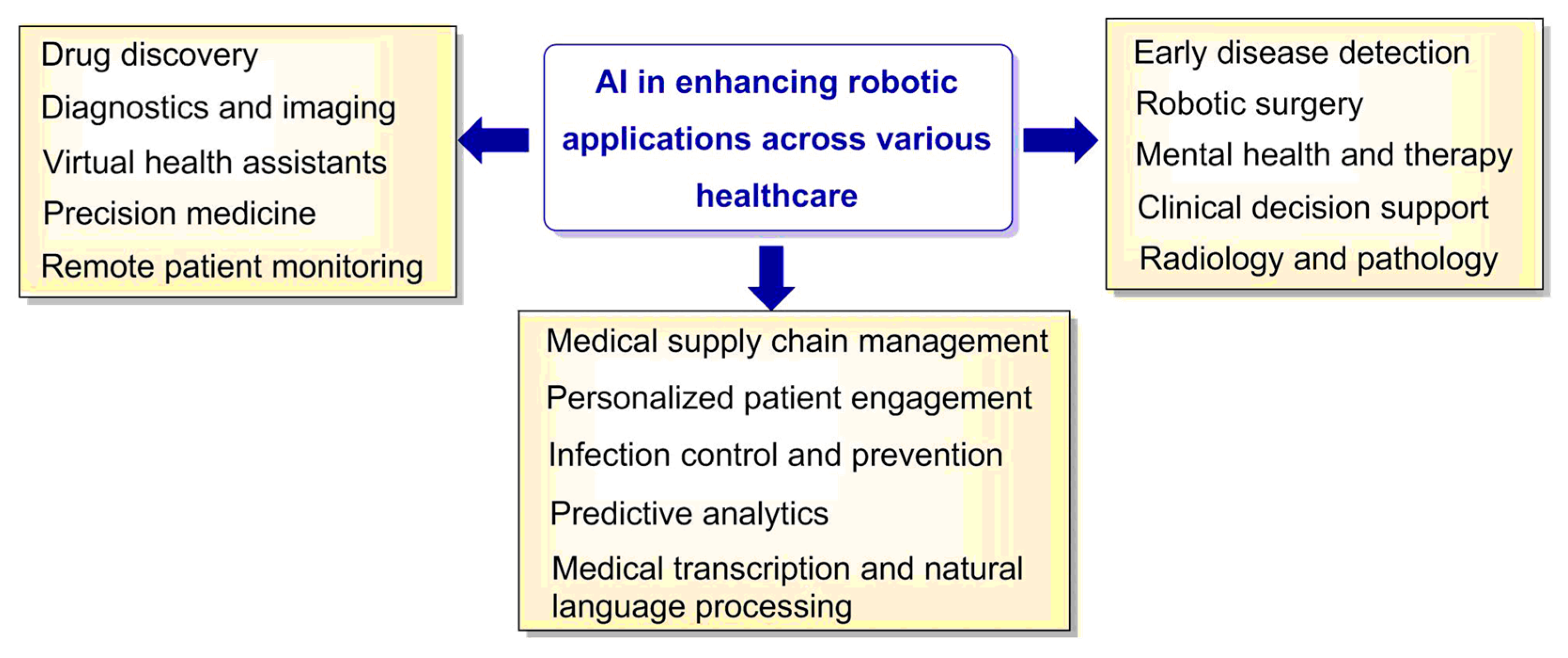
5. Artificial Intelligence and Robotics in Drug Discovery and Health Care
- Target identification: AI algorithms can analyze large datasets, such as genomic, proteomic, and metabolomic data, to identify potential drug targets and elucidate disease mechanisms [176]. This process enables researchers to better understand the molecular basis of diseases and pinpoint suitable targets for drug development.
- Compound screening: AI-driven virtual screening methods can identify promising drug candidates from vast libraries of compounds more efficiently than traditional high-throughput screening methods. AI algorithms can predict the biological activity, toxicity, and pharmacokinetic properties of potential drug candidates, thereby reducing the time and resources required for experimental validation [177].
- De novo drug design: AI can help design new drug molecules from scratch by leveraging deep learning techniques to predict the properties of potential compounds [178]. Generative adversarial networks (GANs) and other machine learning algorithms can create novel molecular structures with the desired biological activity and drug-like properties [179].
- Drug repurposing: AI can analyze existing drugs and their effects to identify new therapeutic uses, significantly reducing the time and cost of drug development. By analyzing the molecular profiles of approved drugs, AI can predict their potential efficacy in treating other diseases or conditions [180].
- Biomarker discovery: AI can analyze vast amounts of biological data to identify biomarkers that can be used for early disease detection, diagnosis, prognosis, or monitoring treatment response. These biomarkers can help tailor therapies to individual patients, leading to more effective treatments and better patient outcomes [181].
- Optimization of lead compounds: AI algorithms can optimize lead compounds by predicting the impact of chemical modifications on their pharmacological properties, such as potency, selectivity, and safety. This approach enables researchers to iteratively improve drug candidates before advancing to preclinical and clinical testing [182].
6. Ethical Considerations and Challenges in Implementing AI and Robotic Technologies in Health Care
7. Future Promising Technologies and Research Opportunities for Robotics Technologies and AI in Pharmacy and Medicine
8. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Alahmari, A.R.; Alrabghi, K.K.; Dighriri, I.M. An Overview of the Current State and Perspectives of Pharmacy Robot and Medication Dispensing Technology. Cureus 2022, 14, e28642. [Google Scholar] [CrossRef]
- Boyd, A.M.; Chaffee, B.W. Critical Evaluation of Pharmacy Automation and Robotic Systems: A Call to Action. Hosp. Pharm. 2019, 54, 4–11. [Google Scholar] [CrossRef]
- Rajpurkar, P.; Chen, E.; Banerjee, O.; Topol, E.J. AI in health and medicine. Nat. Med. 2022, 28, 31–38. [Google Scholar] [CrossRef]
- Naveed, M.A. Transforming Healthcare through Artificial Intelligence and Machine Learning. Pak. J. Health Sci. 2023, 4, 01. [Google Scholar]
- Jimenez, D. How Technology Could Transform Drug Research in 2022. Pharmaceutical Technology. 14 December 2021. Available online: https://www.pharmaceutical-technology.com/features/how-technology-could-transform-drug-research-in-2022/ (accessed on 22 February 2019).
- Dhatterwal, J.S.; Kaswan, K.S.; Kumar, N. Robotic Process Automation in Healthcare. In Confluence of Artificial Intelligence and Robotic Process Automation; Bhattacharyya, S., Banerjee, J.S., De, D., Eds.; Smart Innovation, Systems and Technologies; Springer: Singapore, 2023; Volume 335, pp. 157–175. [Google Scholar] [CrossRef]
- Morgan, A.A.; Abdi, J.; Syed, M.A.Q.; Kohen, G.E.; Barlow, P.; Vizcaychipi, M.P. Robots in Healthcare: A Scoping Review. Curr. Robot. Rep. 2022, 3, 271–280. [Google Scholar] [CrossRef]
- ROBOTNIK Applications of Robotics in Medicine Home Page. Available online: https://robotnik.eu/applications-of-robotics-in-medicine/ (accessed on 21 February 2023).
- INTEL Robotics in Healthcare: The Future of Robots in Medicine Home Page. Available online: https://www.intel.com/content/www/us/en/healthcare-it/robotics-in-healthcare.html (accessed on 21 February 2023).
- Chen, Z.; Li, J.; Wang, S.; Wang, J.; Ma, L. Flexible gait transition for six wheel-legged robot with unstructured terrains. Robot. Auton. Syst. 2022, 150, 103989. [Google Scholar] [CrossRef]
- Chen, Z.; Li, J.; Wang, J.; Wang, S.; Zhao, J.; Li, J. Towards Hybrid Gait Obstacle Avoidance for a Six Wheel-Legged Robot with Payload Transportation. J. Intell. Robot. Syst. 2021, 102, 60. [Google Scholar] [CrossRef]
- Morgan, B. The Future of Healthcare Personalization. Forbes. 3 May 2021. Available online: https://www.forbes.com/sites/blakemorgan/2021/05/03/the-future-of-healthcare-personalization/?sh=75fdd5e7e38f (accessed on 21 February 2023).
- Yamamoto, Y.; Kanayama, N.; Nakayama, Y.; Matsushima, N. Current Status, Issues and Future Prospects of Personalized Medicine for Each Disease. J. Pers. Med. 2022, 12, 444. [Google Scholar] [CrossRef]
- Rubinsztain, J. A New Kind of Help for Healthcare: Where Proven Science and New Technology Merge. Forbes. 2 August 2021. Available online: https://www.forbes.com/sites/forbestechcouncil/2021/08/02/a-new-kind-of-help-for-healthcare-where-proven-science-and-new-technology-merge/?sh=ec548695b215 (accessed on 21 February 2023).
- Soori, M.; Arezoo, B.; Dastres, R. Artificial Intelligence, Machine Learning and Deep Learning in Advanced Robotics, A Review. Cogn. Robot. 2023, 3, 54–70. [Google Scholar] [CrossRef]
- ABB Robotics Home Page. Available online: https://new.abb.com/products/robotics (accessed on 16 March 2023).
- ABB Robotics. Trends and Innovations. ABB Robotics. 2015. Available online: https://www.joanneum.at/fileadmin/user_upload/imported/ROBOTICS/news/150121_ABB_Vortrag_Joanneum_Research_externe_Version.pdf (accessed on 20 March 2023).
- Iqbal, J.; Khan, Z.H.; Khalid, A. Prospects of robotics in food industry. Food Sci. Technol. 2017, 37, 159–165. [Google Scholar] [CrossRef]
- KUKA Industrial Robots Home Page. Available online: https://www.kuka.com/en-de/products/robot-systems/industrial-robots (accessed on 16 March 2023).
- FANUC Delta Robots Home Page. Available online: https://www.fanuc.eu/ua/en/robots/robot-filter-page/delta-robots (accessed on 16 March 2023).
- UNIVERSAL ROBOTS Collaborative Robots from Universal Robots Home Page. Available online: https://www.universal-robots.com/products/ (accessed on 16 March 2023).
- STRYKER Advanced Digital Healthcare Home Page. Available online: https://www.stryker.com/us/en/portfolios/medical-surgical-equipment/advanced-digital-healthcare.html (accessed on 16 March 2023).
- STRYKER Mako Robotic-Arm Assisted Surgery Home Page. Available online: https://www.stryker.com/us/en/portfolios/orthopaedics/joint-replacement/mako-robotic-arm-assisted-surgery.html (accessed on 20 March 2023).
- SYNTEGON Pharma Packaging Solutions Home Page. Available online: https://www.syntegon.com/solutions/pharma-packaging-solutions/ (accessed on 16 March 2023).
- SYNTEGON Pharmaceutical Cleaning Systems Home Page. Available online: https://www.syntegon.com/solutions/pharma/pharmaceutical-cleaning-systems/ (accessed on 20 March 2023).
- YASKAWA Motoman Home Page. Available online: https://www.motoman.com/en-us (accessed on 16 March 2023).
- OMRON LD Series Autonomous Mobile Robots Home Page. Available online: https://automation.omron.com/en/mx/products/family/ld (accessed on 16 March 2023).
- Staubli TX2-60 Industrial Robot Range Home Page. Available online: https://www.staubli.com/tw/en/robotics/products/industrial-robots/tx2-60.html (accessed on 16 March 2023).
- DENSO vs. Robot Series Home Page. Available online: http://design.denso.com/en/works/works_008.html (accessed on 16 March 2023).
- Honeywell Products Home Page. Available online: https://sps.honeywell.com/us/en/products (accessed on 16 March 2023).
- IMA Pharma Home Page. Available online: https://ima.it/pharma/ (accessed on 16 March 2023).
- Azad, M.A.; Osorio, J.G.; Brancazio, D.; Hammersmith, G.; Klee, D.M.; Rapp, K.; Myerson, A. A compact, portable, re-configurable, and automated system for on-demand pharmaceutical tablet manufacturing. Int. J. Pharm. 2018, 539, 157–164. [Google Scholar] [CrossRef]
- Mehle, A.; Bukovec, M.; Likar, B.; Tomaževič, D. Print registration for automated visual inspection of transparent pharmaceutical capsules. Mach. Vis. Appl. 2016, 27, 1087–1102. [Google Scholar] [CrossRef]
- Vishwanatha, C.R.; Asha, V.; More, S.; Divya, C.; Keerthi, K.; Rohaan, S.P. A Survey on Defect Detection of Vials. In Proceedings of International Conference on Data Science and Applications; Lecture Notes in Networks and Systems; Springer: Singapore, 2023; Volume 551, pp. 171–186. [Google Scholar]
- Forcinio, H. Automating Quality Checks: Today’s inspection systems catch tinier flaws, manage data, and increasingly rely on artificial intelligence to further boost performance. Pharm. Technol. 2019, 31, 44–46. [Google Scholar]
- Liu, L.; Guo, F.; Zou, Z.; Duffy, V.G. Application, Development and Future Opportunities of Collaborative Robots (Cobots) in Manufacturing: A Literature Review. Int. J. Hum. Comput. Interact. 2022. [Google Scholar] [CrossRef]
- Saharan, V.A. Robotic Automation of Pharmaceutical and Life Science Industries. In Computer Aided Pharmaceutics and Drug Delivery; Saharan, V.A., Ed.; Springer: Singapore, 2022; pp. 381–414. [Google Scholar] [CrossRef]
- Wilkins, J. Automated pharmaceuticals. MHD Supply Chain. Solut. 2019, 49, 22–24. [Google Scholar]
- Bhatnagar, N. Role of Robotic Process Automation in Pharmaceutical Industries. In Advanced Machine Learning Technologies and Applications, Proceedings of the The International Conference on Advanced Machine Learning Technologies and Applications AMLTA 2019, Cairo, Egypt, 28–30 March 2019; Hassanien, A., Azar, A., Gaber, T., Bhatnagar, R.F., Tolba, M., Eds.; Advances in Intelligent Systems and Computing; Springer: Cham, Switzerland, 2020; Volume 921, pp. 497–504. [Google Scholar] [CrossRef]
- Tegally, H.; San, J.E.; Giandhari, J.; de Oliveira, T. Unlocking the efficiency of genomics laboratories with robotic liquid-handling. BMC Genom. 2020, 21, 729. [Google Scholar] [CrossRef]
- Jamroz, W.; Szafraniec, J.; Kurek, M.; Jachowicz, R. 3D Printing in Pharmaceutical and Medical—Recent Achievements and Challenges. Pharm. Res. 2018, 35, 176. [Google Scholar] [CrossRef]
- Khairuzzaman, A. Regulatory Perspectives on 3D Printing in Pharmaceuticals. In 3D Printing of Pharmaceuticals; Basit, A., Gaisford, S., Eds.; AAPS Advances in the Pharmaceutical Sciences Series; Springer: Cham, Switzerland, 2018; Volume 31, pp. 215–236. [Google Scholar] [CrossRef]
- Mathew, E.; Pitzanti, G.; Larrañeta, E.; Lamprou, D.A. 3D Printing of Pharmaceuticals and Drug Delivery Devices. Pharmaceutics 2020, 12, 266. [Google Scholar] [CrossRef]
- Beer, N.; Hegger, I.; Kaae, S.; De Bruin, M.L.; Genina, N.; Alves, T.L.; Hoebert, J.; Sporrong, S.K. Scenarios for 3D printing of personalized medicines—A case study. Explor. Res. Clin. Soc. Pharm. 2021, 4, 100073. [Google Scholar] [CrossRef]
- Lamichhane, S.; Bashyal, S.; Keum, T.; Noh, G.; Seo, J.E.; Bastola, R.; Choi, J.; Sohn, D.H.; Lee, S. Complex formulations, simple techniques: Can 3D printing technology be the Midas touch in pharmaceutical industry? Asian J. Pharm. Sci. 2019, 14, 465–479. [Google Scholar] [CrossRef]
- Norman, J.; Madurawe, R.D.; Moore, C.M.; Khan, M.A.; Khairuzzaman, A. A new chapter in pharmaceutical manufacturing: 3D—Printed drug products. Adv. Drug Deliv. Rev. 2017, 108, 39–50. [Google Scholar] [CrossRef]
- Aita, I.; Breitkreutz, J.; Quodbach, J. On-demand manufacturing of immediate release levetiracetam tablets using pressure-assisted microsyringe printing. Eur. J. Pharm. Biopharm. 2019, 134, 29–36. [Google Scholar] [CrossRef]
- Thakkar, R.; Pillai, A.R.; Zhang, J.; Zhang, Y.; Kulkarni, V.; Maniruzzaman, M. Novel On-Demand 3-Dimensional (3-D) Printed Tablets Using Fill Density as an Effective Release-Controlling Tool. Polymers 2020, 12, 1872. [Google Scholar] [CrossRef]
- Nyika, J.; Mwema, F.M.; Mahamood, R.M.; Akinlabi, E.T.; Jen, T.C. Advances in 3D printing materials processing-environmental impacts and alleviation measures. Adv. Mater. Process. Technol. 2022, 8, 1275–1285. [Google Scholar] [CrossRef]
- Choonara, Y.E.; du Toit, L.C.; Kumar, P.; Kondiah, P.P.D.; Pillay, V. 3D-printing and the effect on medical costs: A new era? Expert Rev. Pharmacoecon. Outcomes Res. 2016, 16, 23–32. [Google Scholar] [CrossRef]
- Weaver, E.; O’Hagan, C.; Lamprou, D.A. The sustainability of emerging technologies for use in pharmaceutical manufacturing. Expert Opin. Drug Deliv. 2022, 19, 861–872. [Google Scholar] [CrossRef]
- APRECIA Home Page. Available online: https://www.aprecia.com (accessed on 20 March 2023).
- SPRITAM Making Medicine Using 3D Printing Home Page. Available online: https://spritam.com/making-medicine-using-3d-printing/ (accessed on 20 March 2023).
- Wang, Z.; Han, X.; Chen, R.; Jingru, L.; Jing, G.; Hui, Z.; Liu, N.; Gao, X.; Zheng, A. Innovative color jet 3D printing of levetiracetam personalized paediatric preparations. Asian J. Pharm. Sci. 2021, 16, 374–386. [Google Scholar] [CrossRef]
- First 3D-printed pill. Nat. Biotechnol. 2015, 33, 1014. [CrossRef]
- Charoo, N.A.; Ali, S.F.B.; Mohamed, E.M.; Kuttolamadom, M.A.; Ozkan, T.; Khan, M.A.; Rahman, Z. Selective laser sintering 3D printing—An overview of the technology and pharmaceutical applications. Drug Dev. Ind. Pharm. 2020, 46, 869–877. [Google Scholar] [CrossRef]
- Parulski, C.; Jennotte, O.; Lechanteur, A.; Evrard, B. Challenges of fused deposition modeling 3D printing in pharmaceutical applications: Where are we now? Adv. Drug Deliv. Rev. 2021, 175, 113810. [Google Scholar] [CrossRef]
- Deshmane, S.; Kendre, P.; Mahajan, H.; Jain, S. Stereolithography 3D printing technology in pharmaceuticals: A review. Drug Dev. Ind. Pharm. 2021, 47, 1362–1372. [Google Scholar] [CrossRef]
- Robles-Martinez, P.; Xu, X.; Trenfield, S.J.; Awad, A.; Goyanes, A.; Telford, R.; Basit, A.W.; Gaisford, S. 3D Printing of a Multi-Layered Polypill Containing Six Drugs Using a Novel Stereolithographic Method. Pharmaceutics 2019, 11, 274. [Google Scholar] [CrossRef]
- Suárez-González, J.; Magariños-Triviño, M.; Díaz-Torres, E.; Cáceres-Pérez, A.R.; Santoveña-Estévez, A.; Fariña, J.B. Individualized orodispersible pediatric dosage forms obtained by molding and semi-solid extrusion by 3D printing: A comparative study for hydrochlorothiazide. J. Drug Deliv. Sci. Technol. 2021, 66, 102884. [Google Scholar] [CrossRef]
- Nano3D Biosciences Home Page. Available online: https://n3dbio.com (accessed on 20 March 2023).
- Ramadan, Q.; Zourob, M. 3D Bioprinting at the Frontier of Regenerative Medicine, Pharmaceutical, and Food Industries. Front. Med. Technol. 2021, 2, 607648. [Google Scholar] [CrossRef]
- Jung, M.; Ghamrawi, S.; Du, E.Y.; Gooding, J.J.; Kavallaris, M. Advances in 3D Bioprinting for Cancer Biology and Precision Medicine: From Matrix Design to Application. Adv. Healthc. Mater. 2022, 11, 2200690. [Google Scholar] [CrossRef]
- ExOne Home Page. Available online: https://www.exone.com (accessed on 26 March 2023).
- Freeman Technology. 3D Printing Drugs: Learning from the Pioneers; Freeman Technology: Tewkesbury, UK, 2019; Available online: https://staging.ondrugdelivery.com/wp-content/uploads/2019/08/Freeman-Tech.pdf (accessed on 26 March 2023).
- Wang, Y.; Müllertz, A.; Rantanen, J. Additive Manufacturing of Solid Products for Oral Drug Delivery Using Binder Jetting Three-Dimensional Printing. AAPS PharmSciTech 2022, 23, 196. [Google Scholar] [CrossRef]
- Simpson, I. Therapeutic delivery: Industry update covering November 2019. Ther. Deliv. 2020, 11, 217–224. [Google Scholar] [CrossRef]
- Paragon Medical Home Page. Available online: https://www.paragonmedical.com (accessed on 26 March 2023).
- Paragon Medical Pharmaceutical Technology and Drug Delivery Systems Home Page. Available online: https://www.paragonmedical.com/products/pharmaceutical-delivery/ (accessed on 26 March 2023).
- Elahpour, N.; Pahlevanzadeh, F.; Kharaziha, M.; Bakhsheshi-Rad, H.R.; Ramakrishna, S.; Berto, F. 3D printed microneedles for transdermal drug delivery: A brief review of two decades. Int. J. Pharm. 2021, 597, 120301. [Google Scholar] [CrossRef]
- Kulkarni, D.; Damiri, F.; Rojekar, S.; Zehravi, M.; Ramproshad, S.; Dhoke, D.; Musale, S.; Mulani, A.A.; Modak, P.; Paradhi, R.; et al. Recent Advancements in Microneedle Technology for Multifaceted Biomedical Applications. Pharmaceutics 2022, 14, 1097. [Google Scholar] [CrossRef]
- Xia, D.; Wood-Yang, A.J.; Prausnitz, M.R. Clearing away barriers to oral drug delivery. Sci. Robot. 2022, 7, eade3311. [Google Scholar] [CrossRef]
- Suhail, M.; Khan, A.; Rahim, M.A.; Naeem, A.; Fahad, M.; Badshah, S.F.; Jabar, A.; Janakiraman, A.K. Micro and nanorobot-based drug delivery: An overview. J. Drug Target. 2022, 30, 349–358. [Google Scholar] [CrossRef] [PubMed]
- Srinivasan, S.S.; Alshareef, A.; Hwang, A.V.; Kang, Z.; Kuosmanen, J.; Ishida, K.; Jenkins, J.; Liu, S.; Madani, W.A.M.; Lennerz, J.; et al. RoboCap: Robotic mucus-clearing capsule for enhanced drug delivery in the gastrointestinal tract. Sci. Robot. 2022, 7, eabp9066. [Google Scholar] [CrossRef] [PubMed]
- Cehajic-Kapetanovic, J.; Xue, K.; Edwards, T.L.; Meenink, T.C.; Beelen, M.J.; Naus, G.J.; de Smet, M.D.; MacLaren, R.E. First-in-Human Robot-Assisted Subretinal Drug Delivery Under Local Anesthesia. Am. J. Ophthalmol. 2022, 237, 104–113. [Google Scholar] [CrossRef] [PubMed]
- Nurgat, Z.A.; Alaboura, D.; Aljaber, R.; Mustafa, O.; Lawrence, V.; Mominah, M.; Al-Jazairi, A.S.; Al-Jedai, A. Real-World Experience of a Standalone Robotic Device for Batch Compounding of Small-Volume Parenteral Preparations. Hosp. Pharm. 2021, 56, 32–46. [Google Scholar] [CrossRef]
- Valdivia, P.C.; Robertson, A.R.; De Boer, N.K.H.; Marlicz, W.; Koulaouzidis, A. An Overview of Robotic Capsules for Drug Delivery to the Gastrointestinal Tract. J. Clin. Med. 2021, 10, 5791. [Google Scholar] [CrossRef]
- XACT Robotics Home Page. Available online: https://xactrobotics.com (accessed on 15 March 2023).
- Schonfeld, E.; Stienen, M.N.; Veeravagu, A. Future Perspective of Robot-Assisted Minimally Invasive Spine Surgery. In Technical Advances in Minimally Invasive Spine Surgery; Kim, J.S., Härtl, R., Wang, M.Y., Elmi-Terander, A., Eds.; Springer: Singapore, 2022; pp. 351–364. [Google Scholar] [CrossRef]
- Hale, C. XACT’s Needle-Guiding Robot Scores FDA Clearance for Ablation Procedures. Fierce Biotech. 19 May 2022. Available online: https://www.fiercebiotech.com/medtech/xacts-needle-guiding-robot-scores-fda-clearance-ablation-procedures (accessed on 15 March 2023).
- Mazidi, Z.; Javanmardi, S.; Naghib, S.M.; Mohammadpour, Z. Smart stimuli-responsive implantable drug delivery systems for programmed and on-demand cancer treatment: An overview on the emerging materials. Chem. Eng. J. 2022, 433, 134569. [Google Scholar] [CrossRef]
- Kar, A.; Ahamad, N.; Dewani, M.; Awasthi, L.; Patil, R.; Banerjee, R. Wearable and implantable devices for drug delivery: Applications and challenges. Biomaterials 2022, 283, 121435. [Google Scholar] [CrossRef]
- Tan, M.; Xu, Y.; Gao, Z.; Yuan, T.; Liu, Q.; Yang, R.; Zhang, B.; Peng, L. Recent Advances in Intelligent Wearable Medical Devices Integrating Biosensing and Drug Delivery. Adv. Mater. 2022, 34, 2108491. [Google Scholar] [CrossRef]
- Cao, N.; Marcus, A.; Altarawneh, L.; Kwon, S. Priority-based replenishment policy for robotic dispensing in central fill pharmacy systems: A simulation-based study. Health Care Manag. Sci. 2023, 26, 344–362. [Google Scholar] [CrossRef]
- Bagattini, Â.M.; Borges, J.L.A.; Riera, R.; de Carvalho, D.C.M.F. Automation of a tertiary hospital pharmacy drug dispensing system in a lower-middle-income country: A case study and preliminary results. Explor. Res. Clin. Soc. Pharm. 2022, 6, 100151. [Google Scholar] [CrossRef]
- ARXIUM FastPak Elite in Your Hospital Home Page. Available online: https://www.arxium.com/fastpak-elite-in-your-hospital/ (accessed on 15 March 2023).
- Garcia, L.; Kerns, G.; O’Reilley, K.; Okesanjo, O.; Lozano, J.; Narendran, J.; Broeking, C.; Ma, X.; Thompson, H.; Njapa Njeuha, P.; et al. The Role of Soft Robotic Micromachines in the Future of Medical Devices and Personalized Medicine. Micromachines 2022, 13, 28. [Google Scholar] [CrossRef] [PubMed]
- Feng, Y.; An, M.; Liu, Y.; Sarwar, M.T.; Yang, H. Advances in Chemically Powered Micro/Nanorobots for Biological Applications: A Review. Adv. Funct. Mater. 2023, 33, 2209883. [Google Scholar] [CrossRef]
- Aggarwal, M.; Kumar, S. The Use of Nanorobotics in the Treatment Therapy of Cancer and Its Future Aspects: A Review. Cureus 2022, 14, e29366. [Google Scholar] [CrossRef] [PubMed]
- Kolpashchikov, D.; Gerget, O.; Meshcheryakov, R. Robotics in Healthcare. In Handbook of Artificial Intelligence in Healthcare; Lim, C.P., Chen, Y.W., Vaidya, A., Mahorkar, C., Jain, L.C., Eds.; Intelligent Systems Reference Library; Springer: Cham, Switzerland, 2022; Volume 212, pp. 281–306. [Google Scholar] [CrossRef]
- Chandran, V.D.; Nam, S.; Hexner, D.; Bauman, W.A.; Pal, S. Comparison of the dynamics of exoskeletal-assisted and unassisted locomotion in an FDA-approved lower extremity device: Controlled experiments and development of a subject-specific virtual simulator. PLoS ONE 2023, 18, e0270078. [Google Scholar] [CrossRef]
- Akinyemi, T.O.; Omisore, O.M.; Chen, X.; Duan, W.; Du, W.; Yi, G.; Wang, L. Adapting Neural-Based Models for Position Error Compensation in Robotic Catheter Systems. Appl. Sci. 2022, 12, 10936. [Google Scholar] [CrossRef]
- Berczeli, M.; Legeza, P.; Lumsden, A. Catheter Robots in the Cardiovascular System. In Latest Developments in Medical Robotics Systems; Küçük, S., Ed.; IntechOpen: London, UK, 2021. [Google Scholar] [CrossRef]
- Piotin, M.; Blanc, R.; Turner, R.; Tomasello, A.; Ribo, M.; Galdámez, M.; Costalat, V.; Sourour, N.; Mordasini, P.; Killer-Oberpfalzer, M.; et al. P15 Evaluation of effectiveness and safety of the CorPath® GRX System in endovascular embolization procedures of cerebral aneurysms. J. Neurointerv. Surg. 2022, 14, A15. [Google Scholar]
- Bathirappan, K.; Pandurengan, D.B.; Nawaz, J.Y.A.; Arulrajan, J.R. Patient monitoring and medicine dispenser robot. In Proceedings of the 1st International Conference on Computational Intelligence in Engineering Systems, ICCIES 2021, AIP Conference Proceedings, Pandharpur, India, 25–26 June 2022; Volume 2494, p. 030004. [Google Scholar] [CrossRef]
- Cheney, D. Hero Pill Dispenser Review. Forbes HEALTH. 24 October 2022. Available online: https://www.forbes.com/health/healthy-aging/hero-pill-dispenser-review/ (accessed on 15 March 2023).
- Sumartojo, S.; Lugli, D. Lively robots: Robotic technologies in COVID-19. Soc. Cult. Geogr. 2022, 23, 1220–1237. [Google Scholar] [CrossRef]
- Gyles, C. Robots in medicine. Can. Vet. J. 2019, 60, 819–820. [Google Scholar]
- Greenwood, L. The Types of Medical Robots in Use Today and in the Future. Brainlab Journal. 22 November 2021. Available online: https://www.brainlab.com/journal/types-of-medical-robots-in-use-today-and-in-the-future/ (accessed on 15 March 2023).
- Deng, Z.; Guo, L.; Chen, X.; Wu, W. Smart Wearable Systems for Health Monitoring. Sensors 2023, 23, 2479. [Google Scholar] [CrossRef]
- Douissard, J.; Hagen, M.E.; Morel, P. The da Vinci Surgical System. In Bariatric Robotic Surgery; Domene, C., Kim, K., Vilallonga Puy, R., Volpe, P., Eds.; Springer: Cham, Switzerland, 2019; pp. 13–27. [Google Scholar] [CrossRef]
- Tamburella, F.; Lorusso, M.; Tramontano, M.; Fadlun, S.; Masciullo, M.; Scivoletto, G. Overground robotic training effects on walking and secondary health conditions in individuals with spinal cord injury: Systematic review. J. Neuroeng. Rehabil. 2022, 19, 27. [Google Scholar] [CrossRef]
- Alves, T.; Gonçalves, R.S.; Carbone, G. Serious games strategies with cable-driven robots for bimanual rehabilitation: A randomized controlled trial with Post-Stroke patients. Front. Robot. AI 2022, 9, 739088. [Google Scholar] [CrossRef]
- Koceska, N.; Koceski, S.; Beomonte Zobel, P.; Trajkovik, V.; Garcia, N. A Telemedicine Robot System for Assisted and Independent Living. Sensors 2019, 19, 834. [Google Scholar] [CrossRef] [PubMed]
- Matsumoto, S.; Moharana, S.; Devanagondi, N.; Oyama, L.C.; Riek, L.D. Iris: A Low-Cost Telemedicine Robot to Support Healthcare Safety and Equity During a Pandemic. In Pervasive Computing Technologies for Healthcare, Proceedings of the 15th EAI International Conference on Pervasive Computing Technologies for Healthcare, Pervasive Health 2021, Virtual, 6–8 December 2021; Lewy, H., Barkan, R., Eds.; Lecture Notes of the Institute for Computer Sciences, Social Informatics and Telecommunications Engineering; Springer: Cham, Switzerland, 2022; Volume 431, pp. 113–133. [Google Scholar] [CrossRef]
- Duan, F.; Li, W.; Tan, Y. Overview of Robots. In Intelligent Robot; Springer: Singapore, 2023; pp. 3–30. [Google Scholar] [CrossRef]
- Crunkhorn, A.; Andrews, E.; Fantini, C.; Highsmith, M.J.; Loftsgaarden, M.; Randolph, B.; Sall, J.; Webster, J. Management of Upper Limb Amputation Rehabilitation: Synopsis of the 2022 US Department of Veterans Affairs and US Department of Defense Clinical Practice Guideline for Acquired Amputation. Am. J. Phys. Med. Rehabil. 2023, 102, 245–253. [Google Scholar] [CrossRef] [PubMed]
- Herr, H. Pediatric Noodle® AFO from Kinetic Research. Orthologix E-NEWSLETTER. 5 February 2015. Available online: http://www.orthologix.com/enews/ClinicalUpdateWinter2015.html (accessed on 15 March 2023).
- Choo, Y.J.; Chang, M.C. Use of machine learning in the field of prosthetics and orthotics: A systematic narrative review. Prosthet. Orthot. Int. 2023, 47, 226–240. [Google Scholar] [CrossRef] [PubMed]
- Fikry, A.; Shafie, I.S.M.; Yusof, Y.L.M.; Mahamood, S.F.; Jamil, N. When Contactless Service Matters: The Use of Robotic Services in the Healthcare Sector. IEEE Eng. Manag. Rev. 2023, 51, 26–34. [Google Scholar] [CrossRef]
- Weng, Y.-H.; Hirata, Y. Design-Centered HRI Governance for Healthcare Robots. J. Healthc. Eng. 2022, 2022, 3935316. [Google Scholar] [CrossRef]
- Hamdeh, S.; Fathallah, J.; Zhang, H.; Charoen, A.; Altamimi, B.A.; Odufalu, F.-D.; Dave, D.; Sayed, A.E.; Glick, L.R.; Grisolano, S.; et al. Predictive Model for Positive Video Capsule Endoscopy in Iron Deficiency Anemia. Dig. Dis. Sci. 2023, 68, 3083–3091. [Google Scholar] [CrossRef]
- Lambiase, G.; Klottrup-Rees, K.; Lovelady, C.; Ali, S.; Shepherd, S.; Muroni, M.; Lindo, V.; James, D.C.; Dickman, M.J. An automated, low volume, and high-throughput analytical platform for aggregate quantitation from cell culture media. J. Chromatogr. A 2023, 1691, 463809. [Google Scholar] [CrossRef]
- Alterovitz, R.; Goldberg, K. Motion Planning in Medicine: Optimization and Simulation Algorithms for Image-Guided Procedures; Springer Tracts in Advanced Robotics; Springer: Berlin/Heidelberg, Germany, 2008. [Google Scholar] [CrossRef]
- Crawford, M. 6 Applications for Robotics in Medicine. The American Society of Mechanical Engineers. 14 September 2016. Available online: https://www.asme.org/topics-resources/content/top-6-robotic-applications-in-medicine (accessed on 15 August 2023).
- Kent, C. Drug dispensing goes digital. Pharmaceutical Technology. 20 May 2021. Available online: https://www.pharmaceutical-technology.com/features/robotic-drug-dispensing-digital-pharmacy/ (accessed on 16 August 2023).
- Schiraldi, E. Applying Robotic Process Automation in the Pharma Industry. Pharmaceutical Engineering. 18 April 2021. Available online: https://ispe.org/pharmaceutical-engineering/march-april-2021/applying-robotic-process-automation-pharma-industry (accessed on 16 August 2023).
- Böttger, S.; Çallar, T.; Schweikard, A.; Rückert, E. Medical robotics simulation framework for application-specific optimal kinematics. Curr. Dir. Biomed. Eng. 2019, 5, 145–148. [Google Scholar] [CrossRef]
- Walch, K. The Increasing Use of AI in the Pharmaceutical Industry. Forbes. 26 December 2020. Available online: https://www.forbes.com/sites/cognitiveworld/2020/12/26/the-increasing-use-of-ai-in-the-pharmaceutical-industry/?sh=71920b484c01 (accessed on 16 August 2023).
- Ayers, M.; Jayatunga, M.; Goldader, J.; Meier, C. Adopting AI in Drug Discovery. Biopharma. 29 March 2022. Available online: https://www.bcg.com/publications/2022/adopting-ai-in-pharmaceutical-discovery (accessed on 16 August 2023).
- Bhattamisra, S.K.; Banerjee, P.; Gupta, P.; Mayuren, J.; Patra, S.; Candasamy, M. Artificial Intelligence in Pharmaceutical and Healthcare Research. Big Data Cogn. Comput. 2023, 7, 10. [Google Scholar] [CrossRef]
- Hoppe, N.; Härting, R.C.; Rahmel, A. Potential Benefits of Artificial Intelligence in Healthcare. In Artificial Intelligence and Machine Learning for Healthcare; Lim, C.P., Vaidya, A., Chen, Y.W., Jain, V., Jain, L.C., Eds.; Intelligent Systems Reference Library; Springer: Cham, Switzerland, 2023; Volume 229, pp. 225–249. [Google Scholar] [CrossRef]
- Atomwise Home Page. Available online: https://www.atomwise.com (accessed on 5 April 2023).
- Johannsen, S.; Gierse, R.M.; Olshanova, A.; Smerznak, E.; Laggner, C.; Eschweiler, L.; Adeli, Z.; Hamid, R.; Alhayek, A.; Reiling, N.; et al. Not Every Hit-Identification Technique Works on 1-Deoxy-d-Xylulose 5-Phosphate Synthase (DXPS): Making the Most of a Virtual Screening Campaign. ChemMedChem 2023, e202200590. [Google Scholar] [CrossRef]
- Brown, P.; Merritt, A.; Skerratt, S.; Swarbrick, M.E. Recent trends in medicinal chemistry and enabling technologies. Highlights from the Society for Medicines Research Conference. Drugs Future 2023, 48, 211–219. [Google Scholar] [CrossRef]
- Ivanenkov, Y.A.; Polykovskiy, D.; Bezrukov, D.; Zagribelnyy, B.; Aladinskiy, V.; Kamya, P.; Aliper, A.; Ren, F.; Zhavoronkov, A. Chemistry42: An AI-Driven Platform for Molecular Design and Optimization. J. Chem. Inf. Model. 2023, 63, 695–701. [Google Scholar] [CrossRef] [PubMed]
- AIDOC Home Page. Available online: https://www.aidoc.com/ (accessed on 5 April 2023).
- Omiye, J.A.; Swaminathan, A.; Ross, E.G. AI in Surgery. In AI in Clinical Medicine: A Practical Guide for Healthcare Professionals; Byrne, M.F., Parsa, N., Greenhill, A.T., Chahal, D., Ahmad, O., Bagci, U., Eds.; Wiley: Hoboken, NJ, USA, 2023; pp. 282–297. [Google Scholar] [CrossRef]
- Milam, M.E.; Koo, C.W. The current status and future of FDA-approved artificial intelligence tools in chest radiology in the United States. Clin. Radiol. 2023, 78, 115–122. [Google Scholar] [CrossRef] [PubMed]
- Juyal, D.; Shingi, S.; Javed, S.A.; Padigela, H.; Shah, C.; Sampat, A.; Khosla, A.; Abel, J.; Taylor-Weiner, A. SC-MIL: Supervised Contrastive Multiple Instance Learning for Imbalanced Classification in Pathology. arXiv 2023, arXiv:2303.13405. [Google Scholar]
- TEMPUS Home Page. Available online: https://www.tempus.com (accessed on 5 April 2023).
- Deep Genomics Home Page. Available online: https://www.deepgenomics.com/platform/ (accessed on 5 April 2023).
- Mesko, B. The role of artificial intelligence in precision medicine. Expert Rev. Precis. Med. Drug Dev. 2017, 2, 239–241. [Google Scholar] [CrossRef]
- 23aANDME Home Page. Available online: https://www.23andme.com/dna-health-ancestry/ (accessed on 5 April 2023).
- Mala, J.D.; Reynold Pradeep, A. An Intelligent Virtual Medical Assistant for Healthcare Prediction. In Encyclopedia of Data Science and Machine Learning; Wang, J., Ed.; IGI Global: Hershey, PA, USA, 2023; pp. 870–886. [Google Scholar] [CrossRef]
- ADA Home Page. Available online: https://ada.com (accessed on 5 April 2023).
- Babylon 360 Home Page. Available online: https://www.babylonhealth.com/en-us/services/babylon-360 (accessed on 5 April 2023).
- Buoy Health Home Page. Available online: https://www.buoyhealth.com (accessed on 5 April 2023).
- Pathak, K.; Marwaha, J.S.; Tsai, T.C. The role of digital technology in surgical home hospital programs. NPJ Digit. Med. 2023, 6, 22. [Google Scholar] [CrossRef]
- Current Health Remote Patient Monitoring Home Page. Available online: https://www.currenthealth.com/products-page/product-remote-patient-monitoring/ (accessed on 5 April 2023).
- Quijano, Y.; Vicente, E.; Ferri, V.; Naldini, C.; Pizzuti, G.; Caruso, R. Robot-assisted Nissen fundoplication with the new HUGO™ Robotic assisted system: First worldwide report with system description, docking settings and video. Int. J. Surg. Case Rep. 2023, 106, 108178. [Google Scholar] [CrossRef] [PubMed]
- Nia, G.N.; Kaplanoglu, E.; Nasab, A. Evaluation of artificial intelligence techniques in disease diagnosis and prediction. Discov. Artif. Intell. 2023, 3, 5. [Google Scholar]
- Freenome Home Page. Available online: https://www.freenome.com (accessed on 5 April 2023).
- Closedloop Home Page. Available online: https://www.closedloop.ai/models/chronic-diseases (accessed on 5 April 2023).
- Woebot Health Home Page. Available online: https://woebothealth.com (accessed on 5 April 2023).
- Wysa Home Page. Available online: https://www.wysa.com (accessed on 5 April 2023).
- Talkspace Home Page. Available online: https://www.talkspace.com (accessed on 5 April 2023).
- Irmici, G.; Cè, M.; Caloro, E.; Khenkina, N.; Della Pepa, G.; Ascenti, V.; Martinenghi, C.; Papa, S.; Oliva, G.; Cellina, M. Chest X-ray in Emergency Radiology: What Artificial Intelligence Applications Are Available? Diagnostics 2023, 13, 216. [Google Scholar] [CrossRef] [PubMed]
- Butterfly Network Home Page. Available online: https://www.butterflynetwork.com (accessed on 13 April 2023).
- ENLITIC Home Page. Available online: https://enlitic.com/ai-in-radiology/ (accessed on 13 April 2023).
- Paige Home Page. Available online: https://paige.ai (accessed on 13 April 2023).
- Sezgin, E.; Hussain, S.-A.; Rust, S.; Huang, Y. Extracting Medical Information from Free-Text and Unstructured Patient-Generated Health Data Using Natural Language Processing Methods: Feasibility Study with Real-world Data. JMIR Form. Res. 2023, 7, e43014. [Google Scholar] [CrossRef]
- NUANCE Home Page. Available online: https://www.nuance.com/index.html (accessed on 13 April 2023).
- Deepscribe Home Page. Available online: https://www.deepscribe.ai (accessed on 13 April 2023).
- Cloud Healthcare API Home Page. Available online: https://cloud.google.com/healthcare-api (accessed on 13 April 2023).
- Zaman, S.B.; De Silva, N.; Goh, T.Y.; Evans, R.G.; Singh, R.; Singh, R.; Singh, A.; Singh, P.; Thrift, A.G. Design and development of a clinical decision support system for community health workers to support early detection and management of non-communicable disease. BMJ Innov. 2023, 9, 49–56. [Google Scholar] [CrossRef]
- van der Meijden, S.; de Hond, A.; Thoral, P.; Steyerberg, E.; Kant, I.; Cinà, G.; Arbous, M. Intensive Care Unit Physicians’ Perspectives on Artificial Intelligence–Based Clinical Decision Support Tools: Preimplementation Survey Study. JMIR Hum. Factors 2023, 10, e39114. [Google Scholar] [CrossRef]
- Wang, L.; Chen, X.; Zhang, L.; Li, L.; Huang, Y.; Sun, Y.; Yuan, X. Artificial intelligence in clinical decision support systems for oncology. Int. J. Med. Sci. 2023, 20, 79–86. [Google Scholar] [CrossRef]
- ORACLE Cerner Clinical Decision Support Home Page. Available online: https://www.cerner.com/gb/en/solutions/clinical-decision-support (accessed on 13 April 2023).
- ZS ZAIDYN™ Clinical Development Home Page. Available online: https://www.zs.com/products/zaidyn-platform/clinical-development (accessed on 13 April 2023).
- Kumar, A.; Mani, V.; Jain, V.; Gupta, H.; Venkatesh, V.G. Managing healthcare supply chain through artificial intelligence (AI): A study of critical success factors. Comput. Ind. Eng. 2023, 175, 108815. [Google Scholar] [CrossRef] [PubMed]
- GAUSS Surgical Home Page. Available online: http://gauss-surgical.squarespace.com (accessed on 13 April 2023).
- Swisslog Healthcare Home Page. Available online: https://www.swisslog-healthcare.com/en-gb/products (accessed on 13 April 2023).
- Omnicell Home Page. Available online: https://www.omnicell.com (accessed on 13 April 2023).
- Sathitakorn, O.; Jantarathaneewat, K.; Weber, D.J.; Apisarnthanarak, P.; Rutjanawech, S.; Apisarnthanarak, A. Efficacy of Environmental Cleaning Protocol Featuring Real-Time Feedback with and without PX-UV in Reducing the Contamination of Gram-Negative Microorganisms on High-Touch Surfaces in Four Intensive Care Units in Thailand. Antibiotics 2023, 12, 438. [Google Scholar] [CrossRef]
- Chatterjee, P.; Coppin, J.D.; Martel, J.A.; Williams, M.D.; Choi, H.; Stibich, M.; Simmons, S.; Passey, D.; Allton, Y.; Jinadatha, C. Assessment of microbial bioburden on portable medical equipment in a hospital setting. SAGE Open Med. 2023, 11, 20503121231162290. [Google Scholar] [CrossRef]
- Mehta, I.; Hsueh, H.Y.; Taghipour, S.; Li, W.; Saeedi, S. UV disinfection robots: A review. Robot. Auton. Syst. 2022, 161, 104332. [Google Scholar] [CrossRef]
- Kosa, G.; Morozov, O.; Lehmann, A.; Pargger, H.; Marsch, S.; Hunziker, P. Robots and Intelligent Medical Devices in the Intensive Care Unit: Vision, State of the Art, and Economic Analysis. IEEE Trans. Med. Robot. Bionics 2023, 5, 2–17. [Google Scholar] [CrossRef]
- Jolly, J. A study into the use of Surfacide® UV-C emitters in reducing hospital acquired infection rates at Royal Manchester Children’s Hospital. Infect. Dis. Health 2021, 26, S8. [Google Scholar] [CrossRef]
- Dev, S.; Wang, H.; Nwosu, C.S.; Jain, N.; Veeravalli, B.; John, D. A predictive analytics approach for stroke prediction using machine learning and neural networks. Healthc. Anal. 2022, 2, 100032. [Google Scholar] [CrossRef]
- Medial Earlysign Home Page. Available online: https://earlysign.com (accessed on 20 April 2023).
- Almutairi, N.; Vlahu-Gjorgievska, E.; Win, K.T. Persuasive features for patient engagement through mHealth applications in managing chronic conditions: A systematic literature review and meta-analysis. Inform. Health Soc. Care 2023, 48, 267–291. [Google Scholar] [CrossRef]
- Lark Home Page. Available online: https://www.lark.com (accessed on 20 April 2023).
- Wellframe Home Page. Available online: https://www.wellframe.com (accessed on 20 April 2023).
- GYANT Home Page. Available online: https://gyant.com (accessed on 20 April 2023).
- Vijayan, R.S.K.; Kihlberg, J.; Cross, J.B.; Poongavanam, V. Enhancing preclinical drug discovery with artificial intelligence. Drug Discov. Today 2022, 27, 967–984. [Google Scholar] [CrossRef] [PubMed]
- Murugan, N.A.; Priya, G.R.; Sastry, G.N.; Markidis, S. Artificial intelligence in virtual screening: Models versus experiments. Drug Discov. Today 2022, 27, 1913–1923. [Google Scholar] [CrossRef] [PubMed]
- Palazzesi, F.; Pozzan, A. Deep Learning Applied to Ligand-Based De Novo Drug Design. In Artificial Intelligence in Drug Design; Heifetz, A., Ed.; Methods in Molecular Biology; Humana: New York, NY, USA, 2022; Volume 2390, pp. 273–299. [Google Scholar] [CrossRef]
- Tripathi, S.; Augustin, A.I.; Dunlop, A.; Sukumaran, R.; Dheer, S.; Zavalny, A.; Haslam, O.; Austin, T.; Donchez, J.; Tripathi, P.K.; et al. Recent Advances and Application of Generative Adversarial Networks in Drug Discovery, Development, and Targeting. Artif. Intell. Life Sci. 2022, 2, 100045. [Google Scholar] [CrossRef]
- Quazi, S.; Fatima, Z. Role of Artificial Intelligence and Machine Learning in Drug Discovery and Drug Repurposing. In Structural and Functional Aspects of Biocomputing Systems for Data Processing; Vignesh, U., Parvathi, R., Goncalves, R., Eds.; IGI Global: Hershey, PA, USA, 2023; pp. 182–197. [Google Scholar] [CrossRef]
- Michelhaugh, S.A.; Januzzi, J.L. Using artificial intelligence to better predict and develop biomarkers. Clin. Lab. Med. 2023, 43, 99–114. [Google Scholar] [CrossRef]
- Talat, A.; Khan, A.U. Artificial intelligence as a smart approach to develop antimicrobial drug molecules: A paradigm to combat drug-resistant infections. Drug Discov. Today 2023, 28, 103491. [Google Scholar] [CrossRef]
- Benevolent Home Page. Available online: https://www.benevolent.com (accessed on 10 May 2023).
- Insilico Home Page. Available online: https://insilico.com (accessed on 10 May 2023).
- Exscientia Home Page. Available online: https://www.exscientia.ai (accessed on 10 May 2023).
- RECURSION Home Page. Available online: https://www.recursion.com (accessed on 10 May 2023).
- Schrodinger Home Page. Available online: https://www.schrodinger.com (accessed on 10 May 2023).
- ARIA Pharmaceuticals Home Page. Available online: https://ariapharmaceuticals.com (accessed on 10 May 2023).
- CYCLICA Home Page. Available online: https://cyclicarx.com (accessed on 10 May 2023).
- Bioxcel Therapeutics Home Page. Available online: https://www.bioxceltherapeutics.com (accessed on 10 May 2023).
- Numerate Home Page. Available online: http://www.numerate.com (accessed on 10 May 2023).
- A2A Pharmaceuticals Home Page. Available online: https://www.a2apharma.com (accessed on 10 May 2023).
- CLOUD Pharmaceuticals Home Page. Available online: https://www.cloudpharmaceuticals.com (accessed on 10 May 2023).
- Lantern Pharma Home Page. Available online: https://www.lanternpharma.com (accessed on 10 May 2023).
- OWKIN Home Page. Available online: https://owkin.com (accessed on 10 May 2023).
- Cerchia, C.; Lavecchia, A. New avenues in artificial-intelligence-assisted drug discovery. Drug Discov. Today 2023, 28, 103516. [Google Scholar] [CrossRef]
- King, M.R. The Future of AI in Medicine: A Perspective from a Chatbot. Ann. Biomed. Eng. 2023, 51, 291–295. [Google Scholar] [CrossRef]
- Kumar, K.; Kumar, P.; Deb, D.; Unguresan, M.-L.; Muresan, V. Artificial Intelligence and Machine Learning Based Intervention in Medical Infrastructure: A Review and Future Trends. Healthcare 2023, 11, 207. [Google Scholar] [CrossRef]
- Uunona, G.N.; Goosen, L. Leveraging Ethical Standards in Artificial Intelligence Technologies: A Guideline for Responsible Teaching and Learning Applications. In Handbook of Research on Instructional Technologies in Health Education and Allied Disciplines; Garcia, M., Cabrera, M.L., de Almeida, R., Eds.; IGI Global: Hershey, PA, USA, 2023; pp. 310–330. [Google Scholar] [CrossRef]
- Murdoch, B. Privacy and artificial intelligence: Challenges for protecting health information in a new era. BMC Med. Ethics 2021, 22, 122. [Google Scholar] [CrossRef]
- Lord, N. Healthcare Cybersecurity: Tips for Securing Private Health Data. Digital Guardian. 17 September 2020. Available online: https://www.digitalguardian.com/blog/healthcare-cybersecurity-tips-securing-private-health-data (accessed on 15 August 2023).
- Pino, L. Improving the Cybersecurity Posture of Healthcare in 2022; The U.S. Department of Health & Human Services: Washington, DC, USA, 2022. Available online: https://www.hhs.gov/blog/2022/02/28/improving-cybersecurity-posture-healthcare-2022.html (accessed on 16 August 2023).
- Di Nuovo, A.; Elliott, C.; Meese, H.; Vinanzi, S.; Zecca, M. Security and Privacy in Assistive Robotics: Cybersecurity Challenges for Healthcare; EPSRC UK-RAS Network: London, UK, 2023. [Google Scholar]
- Monoscalco, L.; Simeoni, R.; Maccioni, G.; Giansanti, D. Information Security in Medical Robotics: A Survey on the Level of Training, Awareness and Use of the Physiotherapist. Healthcare 2022, 10, 159. [Google Scholar] [CrossRef] [PubMed]
- Jain, S.; Doriya, R. Security framework to healthcare robots for secure sharing of healthcare data from cloud. Int. J. Inf. Technol. 2022, 14, 2429–2439. [Google Scholar] [CrossRef]
- Garcia-Perez, A.; Cegarra-Navarro, J.G.; Sallos, M.P.; Martinez-Caro, E.; Chinnaswamy, A. Resilience in healthcare systems: Cyber security and digital transformation. Technovation 2023, 121, 102583. [Google Scholar] [CrossRef]
- Besenyő, J.; Kovács, A.M. Healthcare Cybersecurity Threat Context and Mitigation Opportunities. Secur. Sci. J. 2023, 4, 83–101. [Google Scholar] [CrossRef]
- Englert, P. State of Cybersecurity for Medical Devices and Healthcare Systems; Securin, Health-ISAC; Finite State Press: Columbus, OH, USA, 2023. [Google Scholar]
- Smith, H. Clinical AI: Opacity, accountability, responsibility and liability. AI Soc. 2021, 36, 535–545. [Google Scholar] [CrossRef]
- Pasquale, F. When Medical Robots Fail: Malpractice Principles for an Era of Automation; Brookings Institution Press: Washington, DC, USA, 2020; Available online: https://www.brookings.edu/articles/when-medical-robots-fail-malpractice-principles-for-an-era-of-automation/ (accessed on 17 August 2023).
- Jasarevic, T. WHO Issues First Global Report on Artificial Intelligence (AI) in Health and Six Guiding Principles for Its Design and Use; World Health Organization: Geneva, Switzerland, 2021; Available online: https://www.who.int/news/item/28-06-2021-who-issues-first-global-report-on-ai-in-health-and-six-guiding-principles-for-its-design-and-use (accessed on 17 August 2023).
- Astromskė, K.; Peičius, E.; Astromskis, P. Ethical and legal challenges of informed consent applying artificial intelligence in medical diagnostic consultations. AI Soc. 2021, 36, 509–520. [Google Scholar] [CrossRef]
- Gesualdo, F.; Daverio, M.; Palazzani, L.; Dimitriou, D.; Diez-Domingo, J.; Fons-Martinez, J.; Jackson, S.; Vignally, P.; Rizzo, C.; Tozzi, A.E. Digital tools in the informed consent process: A systematic review. BMC Med. Ethics 2021, 22, 18. [Google Scholar] [CrossRef]
- Trafton, A. What is the Future of Robotics and AI in Healthcare? World Economic Forum. 10 March 2021. Available online: https://www.weforum.org/agenda/2021/03/why-robots-can-be-beneficial-in-healthcare/ (accessed on 17 August 2023).
- Denecke, K.; Baudoin, C.R. A Review of Artificial Intelligence and Robotics in Transformed Health Ecosystems. Front. Med. 2022, 9, 795957. [Google Scholar] [CrossRef]
- Spatharou, A.; Hieronimus, S.; Jenkins, J. Transforming Healthcare with AI: The Impact on the Workforce and Organizations. McKinsey & Company. 10 March 2020. Available online: https://www.mckinsey.com/industries/healthcare/our-insights/transforming-healthcare-with-ai (accessed on 17 August 2023).
- Ferrara, E. Fairness and Bias in Artificial Intelligence: A Brief Survey of Sources, Impacts, And Mitigation Strategies. arXiv 2023. [Google Scholar] [CrossRef]
- Giovanola, B.; Tiribelli, S. Beyond bias and discrimination: Redefining the AI ethics principle of fairness in healthcare machine-learning algorithms. AI Soc. 2023, 38, 549–563. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.-C.; Tamers, S.L.; Swanson, N. The Role of Technological Job Displacement in the Future of Work; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2022. Available online: https://blogs.cdc.gov/niosh-science-blog/2022/02/15/tjd-fow/ (accessed on 17 August 2023).
- Carrus, B.; Chowdhary, S.; Whiteman, R. Making Healthcare More Affordable through Scalable Automation. McKinsey & Company. 16 September 2020. Available online: https://www.mckinsey.com/capabilities/operations/our-insights/making-healthcare-more-affordable-through-scalable-automation (accessed on 17 August 2023).
- Servaty, R.; Kersten, A.; Brukamp, K.; Möhler, R.; Mueller, M. Implementation of robotic devices in nursing care. Barriers and facilitators: An integrative review. BMJ Open 2020, 10, e038650. [Google Scholar] [CrossRef] [PubMed]
- UL Solutions. Addressing Regulatory Considerations for Medical Robotic Devices; UL Solutions: Northbrook, IL, USA, 2017; Available online: https://library.ul.com/wp-content/uploads/sites/40/2017/08/BNG-UL17-Medical-Robots-White-Paper-080117-1.pdf (accessed on 17 August 2023).
- Dolic, Z.; Castro, R.; Moarcas, A. Robots in Healthcare: A Solution or a Problem? EPRS: European Parliamentary Research Service: Luxembourg, 2019. [Google Scholar] [CrossRef]
- Petersson, L.; Larsson, I.; Nygren, J.M.; Nilsen, P.; Neher, M.; Reed, J.E.; Tyskbo, D.; Svedberg, P. Challenges to implementing artificial intelligence in healthcare: A qualitative interview study with healthcare leaders in Sweden. BMC Health Serv. Res. 2022, 22, 850. [Google Scholar] [CrossRef] [PubMed]
- Willige, A. This Is What Healthcare Leaders See as the Future for Digital Health. World Economic Forum. 14 May 2021. Available online: https://www.weforum.org/agenda/2021/05/digital-health-telemedicine-telehealth-ai-digitalize-health-services/ (accessed on 17 August 2023).
- Deloitte US. The Future of Pharmacy. Available online: https://www2.deloitte.com/us/en/pages/life-sciences-and-health-care/articles/future-of-pharmacy-disruption-opportunities-challenges.html (accessed on 17 August 2023).
- Carney, S. Why AI in Healthcare Needs Human-Centered Design. Philips. 19 April 2021. Available online: https://www.philips.com/a-w/about/news/archive/blogs/innovation-matters/2021/20210419-why-ai-in-healthcare-needs-human-centered-design.html (accessed on 17 August 2023).



| Supplier Name, Country | Robotic Solutions for the Pharmaceutical Industry | Examples of Robotic Solutions |
|---|---|---|
| ABB Robotics, Switzerland | Robots are designed for tasks such as drug manufacturing, packaging, and quality control. | ABB’s FlexPicker robots [16,17,18] provide high-speed and precision handling for various pharmaceutical products. Its advanced vision system and software enable it to adapt quickly to different product shapes and sizes, making it suitable for a wide range of pharmaceutical manufacturing applications. |
| KUKA Robotics, Germany | Robots are utilized in various applications, such as drug manufacturing, assembly, and packaging. | The KR AGILUS robot (KUKA Robotics) series [19] is known for its speed, precision, and adaptability in handling delicate pharmaceutical products. Its advanced software and control systems allow for seamless integration with existing production lines and offer flexibility in programming for various tasks, such as drug manufacturing, assembly, and packaging. |
| FANUC Corporation, Japan | Robots are used for tasks such as drug dispensing, packaging, and assembly. | FANUC’s M-1iA robot series [20] is a family of high-speed, lightweight robots designed for the precision assembly and handling of small pharmaceutical components. These robots are equipped with FANUC’s proprietary software and control systems, which enable them to perform complex tasks with high accuracy and efficiency. |
| Universal Robots, Denmark | Specializes in collaborative robots (cobots), which can be easily programmed and adapted for drug packaging, labeling, and quality control. | The UR series of cobots [21] are known for their ease of use, flexibility, and safety features. These cobots are equipped with intuitive software that allows for easy programming and adaptation for tasks such as drug packaging, labeling, and quality control. |
| Stryker Corporation, USA | Robotic systems are used for tasks like precision drug dispensing and product assembly, helping to ensure accuracy and reduce human error. | The Mako Robotic-Arm Assisted Surgery System [22,23] is a robotic assisted surgery platform designed for precision drug dispensing and product assembly. This system is powered by advanced software that helps ensure accuracy and reduce human error during the manufacturing process. |
| Syntegon, Germany | Machines are used for tasks like filling, packaging, and labeling of pharmaceutical products. | The RAN series of robotic systems [24,25] are designed for high-speed, precise handling and packaging of various drug formats. These systems are equipped with advanced software and control systems that enable them to adapt to different product types and production requirements. |
| Yaskawa Motoman, Japan | Robotic systems are employed in the pharmaceutical industry for applications such as drug manufacturing, quality control, and packaging. | The Motoman GP series of robots are known for their precision and reliability in handling delicate pharmaceutical products [26]. |
| Omron Corporation, Japan | Robots are used in applications like drug manufacturing, assembly, and inspection. | Omron’s LD Mobile Robot series [27] is designed for material transportation and handling in pharmaceutical manufacturing facilities. |
| Stäubli Robotics, Switzerland | Robots are utilized for tasks such as drug manufacturing, packaging, and quality control. | Stäubli’s TX2 series of robots [28] are known for their cleanroom compatibility, making them suitable for use in sterile pharmaceutical production environments. Their advanced software and control systems ensure precise and efficient operation in various tasks, such as drug manufacturing, packaging, and quality control. |
| Denso Robotics, Japan | Robots are employed in the pharmaceutical industry for applications like drug manufacturing, packaging, and inspection. | Denso’s VS series of robots [29] are designed for high-speed and precision handling of pharmaceutical products, helping to improve productivity and quality. |
| Honeywell, USA | Offers automated solutions for the pharmaceutical industry, including production management, process monitoring, and quality control systems. | Automated storage and retrieval system (AS/RS), autonomous mobile robots (AMRs), and Pallet Accuglide™ conveyor [30]. |
| IMA Group, Italy | Automated solutions for packaging, dosing, labeling, and other manufacturing processes. | IMA Swiftpack SWIFTLIFT Tablet Elevator and continuous direct compression line [31]. |
| Robotic Technologies and Automated Systems | Application |
|---|---|
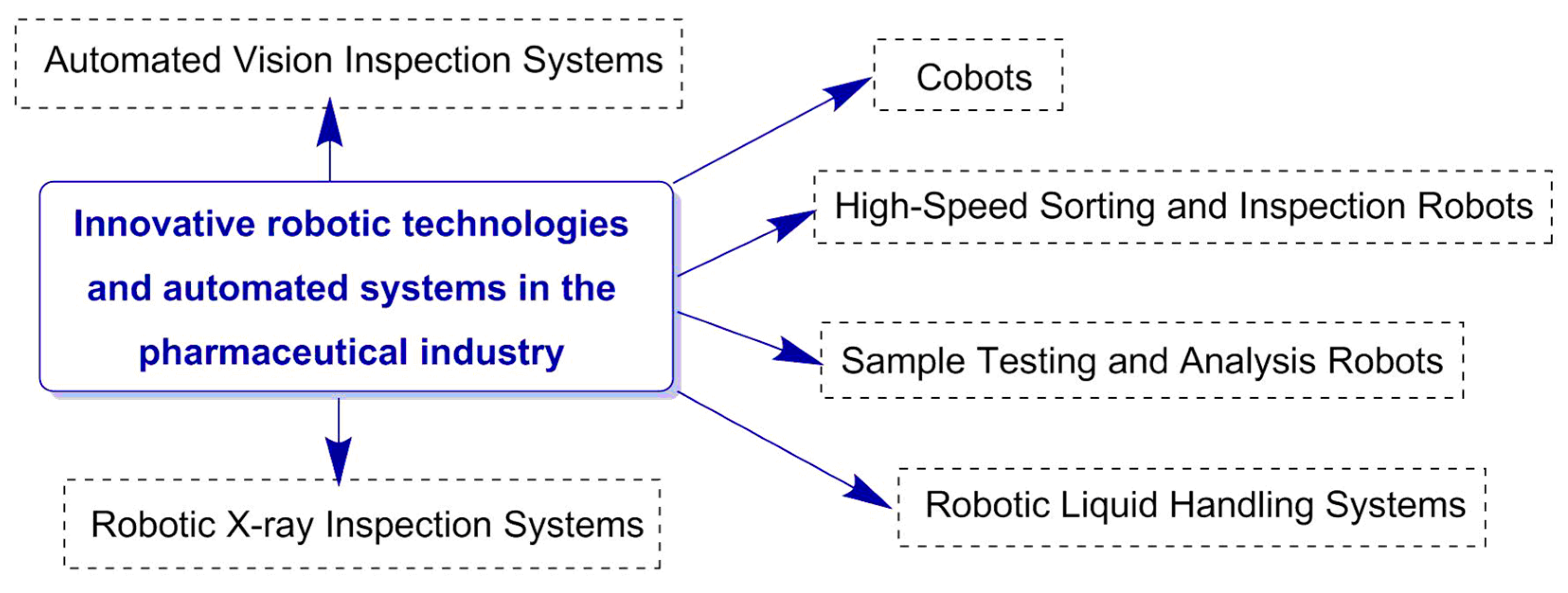
| Automated Vision Inspection Systems | Such systems use advanced cameras, sensors, and image processing software to inspect pharmaceutical products, such as tablets [32], capsules [33], and vials [34], for defects or inconsistencies. By automating the inspection process, these systems can quickly and accurately identify issues, such as incorrect labeling, damaged packaging, or improper tablet shapes and sizes, ensuring only high-quality products reach consumers [35]. |
| Collaborative Robots (Cobots) | Cobots [36,37], such as Universal Robots’ UR series, are designed to work alongside human operators in quality control processes. They can be easily programmed and adapted for tasks, such as drug packaging inspection, label verification, and quality control checks. Their advanced safety features ensure minimal risk to human operators while improving the overall efficiency of the quality control process. |
| High-Speed Sorting and Inspection Robots | Robots like ABB’s FlexPicker and KUKA’s KR AGILUS series are used for high-speed sorting and inspection of pharmaceutical products [37,38]. They can quickly and accurately sort products based on various criteria, such as size, shape, color, or weight, and identify any defects or inconsistencies in the process. |
| Sample Testing and Analysis Robots | These robotic systems [39] automate the process of collecting and analyzing samples from drug production batches. By using advanced sensors and analytical tools, they can quickly and accurately test samples for quality parameters, such as purity, potency, and stability, ensuring that products meet strict regulatory standards. |
| Robotic Liquid Handling Systems | These systems [40] are involved in the processes of transferring, measuring, and mixing liquids in the pharmaceutical manufacturing and quality control process. With high precision and accuracy, these robots ensure consistency in drug formulation and reduce the risk of human error, helping to maintain strict quality standards. |
| Robotic X-ray Inspection Systems | These systems [39] use advanced X-ray technology to inspect pharmaceutical products and packaging for defects, such as foreign particles, contaminants, or improper sealing. By automating this process, these robots can quickly and accurately identify issues, ensuring that only high-quality products reach the market. |
| Company/Research Institution, Country | Application of 3D Printing | 3D-Printed Pharmaceutical Product/Patented Technology |
|---|---|---|
| Aprecia Pharmaceuticals, USA | Aprecia is a pioneer in 3D printing for pharmaceuticals and developed the first FDA-approved 3D-printed drug, Spritam. The company’s proprietary ZipDose technology enables the creation of rapidly dissolving oral medications, which can improve patient adherence and make it easier for patients to take their medication. |
|
| FabRx, UK | FabRx focuses on developing 3D printing technologies for personalized medicine. The company researches various 3D printing methods, such as selective laser sintering (SLS) [56], fused deposition modeling (FDM) [57], and stereolithography (SLA) [58], to produce customized drug dosages and release profiles based on individual patients. |
|
| Nano3D Biosciences, USA | Nano3D Biosciences focuses on developing bioprinting technologies for drug discovery and development [61]. | Magnetic 3D bioprinting technology [62,63] can be used to create complex tissue structures for drug testing, which can help improve the efficiency and accuracy of drug development processes. |
| ExOne, USA | ExOne explores the use of its technology to create custom drug dosages and formulations, as well as drug delivery devices [64,65,66]. | Freeman technology [65]. |
| T3D Therapeutics, USA | T3D Therapeutics focuses on using 3D printing technology to create customized medications for the treatment of neurological disorders, such as Alzheimer’s disease. | Their 3D printing technology enables the precise control of drug release profiles, potentially improving treatment outcomes and reducing side effects for patients [67]. |
| Paragon Medical, USA | Paragon Medical focused on the development of 3D printing technologies for various industries, including pharmaceuticals [68]. | The company researches and develops new techniques for creating complex drug formulations, drug delivery devices, and personalized medications using 3D printing [69]. |
| Exaddon, North Carolina State University and the University of North Carolina, USA | Exaddon develops microneedles made from cooper that can be designed with varying shapes and sizes to control the release of drugs through the skin for delivery. | Exaddon technology for the printing of microneedles [70,71]. |
| Drug Delivery System | Application | Example of Drug Delivery Systems |
|---|---|---|
| Robot-assisted intravenous (IV) therapy | These systems for intravenous medications [76] help minimize human errors, improve safety, and reduce the risk of contamination during the preparation process. | RIVA (Robotic IV Automation) system from ARxIUM or the IV Compounding Robot from Aesynt |
| Capsule robots for gastrointestinal drug delivery | Capsule robots can provide external control to deliver drugs to specific locations within the gastrointestinal tract. These robots have the potential to improve drug absorption, reduce side effects, and enable targeted therapy for conditions such as inflammatory bowel disease or gastrointestinal tumors [74,77]. | RoboCap from Massachusetts Institute of Technology |
| Robotic needle guidance systems | Such systems can accurately position needles for drug injections or biopsies. These systems use advanced imaging and AI algorithms to improve accuracy, reduce complications, and shorten procedure times [78,79,80]. | Robotic needle guidance systems from XACT Robotics |
| Implantable drug delivery devices | Such devices can be remotely controlled to release drugs on demand or according to a predetermined schedule. Such devices have the potential to improve patient adherence, reduce the frequency of drug administration, and enable more precise dosing [81]. | LACRISERT from Bausch + Lomb |
| Wearable drug delivery systems | Systems can automatically administer drugs according to programmed schedules or in response to real-time physiological data. These devices can improve treatment outcomes by ensuring consistent drug delivery and reducing the burden on patients [82,83]. | Chrono Therapeutics’ SmartStop and the insulin delivery systems developed by Insulet and Tandem Diabetes Care |
| Robotic pharmacy dispensing systems | Automated pharmacy dispensing systems [84,85,86] help to improve the accuracy and efficiency of medication dispensing, reducing the risk of medication errors and freeing up pharmacy staff to focus on patient care. | The PillPick system from Swisslog Healthcare or the ARxIUM FastPak Elite |
| Soft robotic drug delivery systems | These systems can change shape and size to navigate through the body and deliver drugs to specific locations [87]. These flexible robots made from materials like hydrogels or elastomers can adapt to the body’s internal environment and minimize the risk of injury during drug delivery. | Millirobot from City University of Hong Kong and Shenzhen Institutes of Advanced Technology |
| Nanorobotic drug delivery | These systems use nanoscale robots to transport and release drugs within the body. These tiny robots can be engineered to respond to specific environmental stimuli, such as pH or temperature, ensuring targeted and controlled drug delivery [88,89]. | Nanobots for cancer treatment from Elan Pharmaceuticals, Merck’s Emend, and Wyeth’s Rapamune |
| Robotic exoskeletons for drug delivery | Robotic exoskeletons are being researched for drug delivery applications [90,91]. These wearable robotic devices could potentially administer medications directly into the bloodstream, bypassing the gastrointestinal system and improving bioavailability. | Robotic exoskeletons from ReWalk Robotics and Ekso Bionics |
| Robotic catheter systems | Robotic catheter systems enable precise navigation of catheters within the body to deliver drugs directly to targeted tissues or organs [92,93,94]. This can enhance the effectiveness of treatments while reducing systemic side effects. | Robotic catheter systems from Auris Health and Corindus Vascular Robotics |
| Robotic pill dispensers | Robotic pill dispensers use automation and artificial intelligence to dispense the right medications at the right time for patients [86,87]. These systems help improve patient adherence to treatment regimens and reduce the risk of medication errors [95,96]. | The Pillo Health or the Hero Medication Dispenser |
| Direction of Robotic Technology Applications | Application |
|---|---|
| Personal health monitoring | Wearable robotic devices, such as smartwatches or fitness trackers, monitor an individual’s vital signs, sleep patterns, and activity levels. This information can be used to provide personalized health insights and recommendations [100]. |
| Robotic surgery | Robotic surgical systems, such as the da Vinci Surgical System [101] by Intuitive Surgical, are used to perform minimally invasive procedures with greater precision and control. These systems provide enhanced visualization, improved dexterity, and increased accuracy, leading to shorter recovery times and reduced risk of complications for patients. |
| Rehabilitation robotics | Robotic devices are being used to support physical therapy and rehabilitation. Examples include exoskeletons like the ReWalk system [102], which assists individuals with spinal cord injuries in walking, and robotic devices like the InMotion Arm by Bionik Laboratories [103]. The latter helps patients regain upper limb function and can be used at home to support physical therapy and rehabilitation for patients recovering from stroke or other neurological conditions. These devices provide personalized therapy, enabling patients to receive tailored treatment in the comfort of their own homes. |
| Telemedicine robots | Telepresence robots [104,105,106], such as those developed by InTouch Health and Intuitive Surgical, enable healthcare professionals to remotely diagnose, consult, and treat patients. These robots use high-definition cameras and real-time communication systems to connect patients with healthcare providers, regardless of their physical location. |
| Robotic prosthetics and orthotics | Advanced prosthetic limbs, such as the DEKA Arm (also known as the “Luke Arm”) [107] and the BiOM T2 Ankle [108], use robotic technology to mimic natural limb movements and provide users with increased functionality and mobility [109]. |
| Robotic drug delivery systems | Innovative robotic drug delivery systems are being developed to improve the efficiency, safety, and patient experience in drug administration (see item 3). |
| Robotic nursing assistants | Robotic nursing assistants, such as Moxi by Diligent Robotics [110] and Robear by RIKEN [111], are designed to perform routine tasks like delivering medication, collecting lab samples, and assisting with patient transport. These robots help free up medical staff to focus on more complex patient care tasks. |
| Diagnostic robots | Robotic systems are being developed to aid in diagnostics. For example, the PillCam by Given Imaging [112] is a swallowable capsule camera that captures images of the gastrointestinal tract. Another example is the robotic catheter system by Auris Health [93], which aids in diagnosing and treating lung cancer. |
| Laboratory automation | Robotic systems like the Hamilton STAR and Tecan Freedom EVO [113] are used to automate laboratory processes, increasing efficiency, reducing human error, and improving the quality of data collected in medical research. |
| Personalized drug delivery | Robotic drug delivery systems like thosed discussed earlier can be tailored to individual patient needs, ensuring targeted and controlled drug delivery for optimal therapeutic outcomes. |
| Direction of AI and Robotics Applications | Application | Companies Working on These Solutions |
|---|---|---|
| Drug discovery | Analysis of large datasets and identification of potential drug candidates or targets, significantly speeding up the drug discovery process. | Atomwise [123,124], BenevolentAI [125], Insilico Medicine [126] |
| Diagnostics and imaging | Analysis of medical images, such as X-rays, MRIs, or CT scans and faster speed and accuracy of detection of abnormalities than human specialists. | Aidoc [127,128], Zebra Medical Vision [129], PathAI [130] |
| Precision medicine | Analysis of genetic, clinical, and lifestyle data to help tailor medical treatments to individual patients, improving outcomes and reducing side effects. | Tempus [131], Deep Genomics [132,133], 23andMe [134] |
| Virtual health assistants | AI-powered virtual health assistants [135], such as chatbots or voice assistants, to provide medical advice, answer health-related questions, and help schedule appointments. | Ada Health [136], Babylon Health [137], Buoy Health [138] |
| Remote patient monitoring | Analysis of data collected from wearable devices, alerting healthcare providers of any abnormalities, allowing for early intervention and improved patient care. | Biofourmis [139], Current Health [140] |
| Robotic surgery | Robotic surgical systems, such as the da Vinci Surgical System [101], enable surgeons to perform minimally invasive procedures with greater precision and control, leading to better patient outcomes. | Intuitive Surgical [101], Medtronic [141], Stryker [22,23] |
| Early disease detection | Prediction of the likelihood of diseases based on patient data and identification of early warning signs, facilitating early intervention and treatment [142]. | Freenome [143], ClosedLoop.ai [144] |
| Mental health and therapy | AI-driven chatbots and apps provide personalized support and therapy for individuals dealing with mental health issues, such as anxiety, depression, or post-traumatic stress disorder. | Woebot [145], Wysa [146], Talkspace [147] |
| Radiology and pathology | AI-based algorithms can help radiologists and pathologists interpret medical images, improving diagnostic accuracy and efficiency [148]. | Butterfly Network [149], Enlitic [150], Paige.AI [151] |
| Medical transcription and natural language processing | Transcription and analysis of spoken or written medical language, streamlining the documentation process and reducing the administrative burden on healthcare professionals [152]. | Nuance Communications [153], DeepScribe [154], Google Cloud Healthcare API [155] |
| Clinical decision support | AI-powered decision support tools help healthcare professionals make better-informed decisions, reducing errors and improving patient care [156,157]. | IBM Watson Health [158], Cerner [159], ZS [160] |
| Medical supply chain management | Optimization of the supply chain, helping to manage inventory and reduce waste [161]. | Gauss Surgical [162], Swisslog Healthcare [163], Omnicell [164] |
| Infection control and prevention | Robots equipped with UV-C light technology can be used to sanitize medical facilities, reducing the risk of hospital-acquired infections. | Xenex [165,166], UVD Robots [167,168], Surfacide [169] |
| Predictive analytics | AI-powered predictive analytics can be used to anticipate patient needs, optimize hospital resources, and identify high-risk patient populations [170]. | Medial EarlySign [171] |
| Personalized patient engagement | Creation of personalized care plans and interventions based on patient data, improving patient adherence to treatment and overall health outcomes [172]. | Lark Health [173], Wellframe [174], GYANT [175] |
| Company Name | Application of AI | Company Homepage |
|---|---|---|
| Atomwise | Structure-based drug design and compound screening to identify potential drug candidates | https://www.atomwise.com |
| BenevolentAI | Identification of drug targets, design of molecules, and optimization of drug candidates | https://www.benevolent.com |
| Insilico Medicine | Target identification, molecule generation, and drug repurposing | https://insilico.com |
| Exscientia | Design and optimization of drug candidates in a range of therapeutic areas | https://www.exscientia.ai |
| Recursion Pharmaceuticals | AI-based image analysis and machine learning to analyze cellular phenotypes for drug discovery and repurposing | https://www.recursion.com |
| Deep Genomics | Prediction of the effects of genetic mutations and development of therapies for genetic diseases | https://www.deepgenomics.com/platform/ |
| Schrödinger | Computational methods and AI for molecular modeling, design of novel compounds with desired properties, and optimization of existing drug candidates | https://www.schrodinger.com |
| ARIA Pharmaceuticals | AI-driven drug discovery for various therapeutic areas, leveraging large-scale data integration and machine learning algorithms to identify promising drug candidates | https://ariapharmaceuticals.com |
| Cyclica | In silico drug discovery using a combination of deep learning and molecular dynamics simulations to predict drug–target interactions, off-target effects, and ADMET properties | https://cyclicarx.com |
| BioXcel Therapeutics | Identification and development of innovative therapies by repurposing existing drugs and designing new drug candidates | https://www.bioxceltherapeutics.com |
| Numerate | Design, optimization, and validation of small molecule drug candidates, focusing on areas such as oncology, immunology, and metabolic diseases | http://www.numerate.com |
| A2A Pharmaceuticals | Design and development of novel drug candidates for difficult-to-drug targets, aiming to treat cancer, infectious diseases, and other conditions | https://www.a2apharma.com |
| Cloud Pharmaceuticals | Design and optimization of drug candidates, focusing on areas such as oncology, inflammation, and central nervous system disorders | https://www.cloudpharmaceuticals.com |
| Lantern Pharma | Identification and development of precision oncology therapies by repurposing existing drugs and discovering new drug candidates | https://www.lanternpharma.com |
| Owkin | Analysis of multimodal medical data, including imaging and omics data, to identify biomarkers and develop predictive models for drug discovery and personalized medicine | https://owkin.com |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stasevych, M.; Zvarych, V. Innovative Robotic Technologies and Artificial Intelligence in Pharmacy and Medicine: Paving the Way for the Future of Health Care—A Review. Big Data Cogn. Comput. 2023, 7, 147. https://doi.org/10.3390/bdcc7030147
Stasevych M, Zvarych V. Innovative Robotic Technologies and Artificial Intelligence in Pharmacy and Medicine: Paving the Way for the Future of Health Care—A Review. Big Data and Cognitive Computing. 2023; 7(3):147. https://doi.org/10.3390/bdcc7030147
Chicago/Turabian StyleStasevych, Maryna, and Viktor Zvarych. 2023. "Innovative Robotic Technologies and Artificial Intelligence in Pharmacy and Medicine: Paving the Way for the Future of Health Care—A Review" Big Data and Cognitive Computing 7, no. 3: 147. https://doi.org/10.3390/bdcc7030147
APA StyleStasevych, M., & Zvarych, V. (2023). Innovative Robotic Technologies and Artificial Intelligence in Pharmacy and Medicine: Paving the Way for the Future of Health Care—A Review. Big Data and Cognitive Computing, 7(3), 147. https://doi.org/10.3390/bdcc7030147






