Why Some People Are Hesitant to Receive COVID-19 Boosters: A Systematic Review
Abstract
1. Introduction
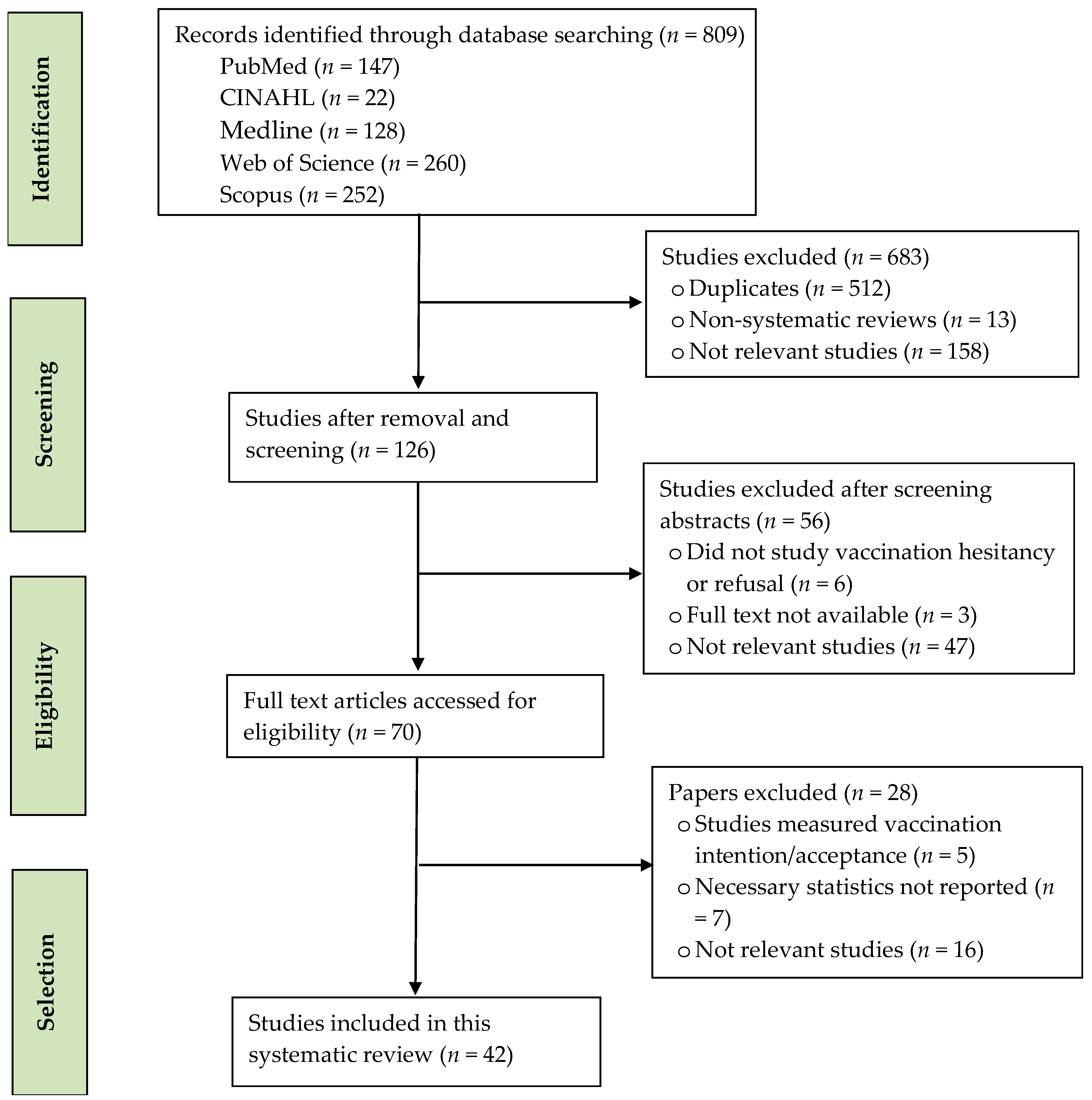
2. Methodology
2.1. Inclusion Criteria
2.2. Search Strategy
3. Results
3.1. Study Characteristics
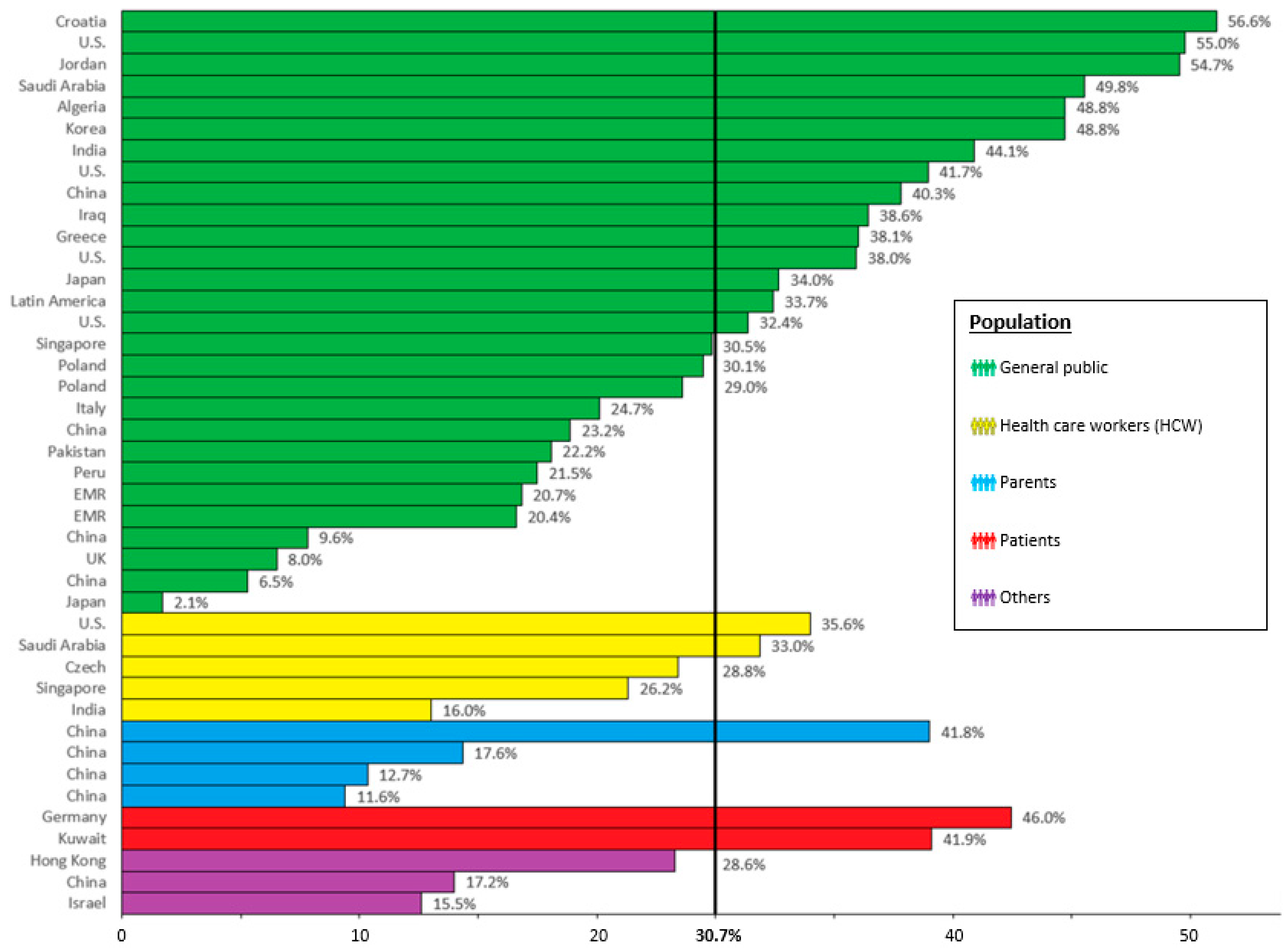
3.2. COVID-19 Booster Vaccination Hesitancy Rate
3.3. Predictors of COVID-19 Booster Vaccine Hesitancy
3.3.1. Demographic
3.3.2. Geographical Factors
3.3.3. Adverse Events
3.3.4. Perceived Benefits/Efficacy
3.3.5. Perceived Susceptibility
3.3.6. Perceived Severity
3.3.7. History of COVID-19 Infection
3.3.8. Vaccination Status
3.3.9. Vaccination Recommendations
3.3.10. Health Status
3.3.11. Knowledge and Information
3.3.12. Skepticism/Distrust/Conspiracy Theory
3.3.13. Vaccine Type
3.3.14. Miscellaneous Determinants
4. Discussion
4.1. Demographic Factors
4.2. Booster Vaccine Hesitancy Model
4.3. Limitations and Future Research
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization. WHO Coronavirus (COVID-19) Dashboard. 2023. Available online: https://worldhealthorg.shinyapps.io/covid/ (accessed on 16 January 2023).
- Batra, K.; Sharma, M.; Dai, C.-L.; Khubchandani, J. COVID-19 Booster Vaccination Hesitancy in the United States: A Multi-Theory-Model (MTM)-Based National Assessment. Vaccines 2022, 10, 758. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. COVID-19 Vaccinations in the United States. 2023. Available online: https://covid.cdc.gov/covid-data-tracker/#vaccinations_vacc-people-onedose-pop-total (accessed on 16 January 2023).
- Kowalski, E.; Stengel, A.; Schneider, A.; Goebel-Stengel, M.; Zipfel, S.; Graf, J. How to Motivate SARS-CoV-2 Convalescents to Receive a Booster Vaccination? Influence on Vaccination Willingness. Vaccines 2022, 10, 455. [Google Scholar] [CrossRef]
- Noh, Y.; Kim, J.H.; Yoon, D.; Choe, Y.J.; Choe, S.A.; Jung, J.; Lee, S.W.; Shin, J.Y. Predictors of COVID-19 booster vaccine hesitancy among fully vaccinated adults in Korea: A nationwide cross-sectional survey. Epidemiol. Health 2022, 44, e2022061. [Google Scholar] [CrossRef]
- Zhou, Y.; Li, G.X.; Zhao, T.S.; Du, J.; Zhang, W.X.; Xie, M.Z.; Chen, L.Y.; Zeng, J.; Wang, C.; Liu, B.; et al. Parents’ willingness to vaccinate themselves and their children with the booster vaccine against SARS-CoV-2: A cross-sectional study in Puyang city, China. J. Med. Virol. 2022, 95, e28256. [Google Scholar] [CrossRef]
- Al-Qerem, W.; Al Bawab, A.Q.; Hammad, A.; Ling, J.; Alasmari, F. Willingness of the Jordanian Population to Receive a COVID-19 Booster Dose: A Cross-Sectional Study. Vaccines 2022, 10, 410. [Google Scholar] [CrossRef]
- Lounis, M.; Bencherit, D.; Rais, M.A.; Riad, A. COVID-19 Vaccine Booster Hesitancy (VBH) and Its Drivers in Algeria: National Cross-Sectional Survey-Based Study. Vaccines 2022, 10, 621. [Google Scholar] [CrossRef]
- Folcarelli, L.; Miraglia del Giudice, G.; Corea, F.; Angelillo, I.F. Intention to Receive the COVID-19 Vaccine Booster Dose in a University Community in Italy. Vaccines 2022, 10, 146. [Google Scholar] [CrossRef]
- Paul, E.; Fancourt, D. Predictors of uncertainty and unwillingness to receive the COVID-19 booster vaccine: An observational study of 22,139 fully vaccinated adults in the UK. Lancet Reg. Health-Eur. 2022, 14, 100317. [Google Scholar] [CrossRef]
- Wang, R.; Qin, C.; Du, M.; Liu, Q.; Tao, L.; Liu, J. The association between social media use and hesitancy toward COVID-19 vaccine booster shots in China: A web-based cross-sectional survey. Hum. Vaccines Immunother. 2022, 18, 2065167. [Google Scholar] [CrossRef]
- Bendezu-Quispe, G.; Caira-Chuquineyra, B.; Fernandez-Guzman, D.; Urrunaga-Pastor, D.; Herrera-Añazco, P.; Benites-Zapata, V.A. Factors Associated with Not Receiving a Booster Dose of COVID-19 Vaccine in Peru. Vaccines 2022, 10, 1183. [Google Scholar] [CrossRef]
- Seboka, B.T.; Moeed, A.; Najeeb, H.; Saleem, A.; Asghar, M.S.; Rafi, H.M.; Khattak, A.K.; Bilal, Z. Willingness and Perceptions Regarding COVID-19 Vaccine Booster Dose in Pakistani Vaccinated Population: A Cross-Sectional Survey. Front. Public Health 2022, 10, 911518. [Google Scholar]
- MacDonald, N.E.; Eskola, J.; Liang, X.; Chaudhuri, M.; Dube, E.; Gellin, B.; Goldstein, S.; Larson, H.; Manzo, M.L.; Reingold, A.; et al. Vaccine hesitancy: Definition, scope and determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef]
- United Nations Children’s Fund. Over 20 Million Children Worldwide Missed out on Measles Vaccine Annually in past 8 Years, Creating a Pathway to Current Global Outbreaks—UNICEF. Press Release, 25th April, 2019. 2019. Available online: https://www.unicef.org/press-releases/over-20-million-children-worldwide-missed-out-measles-vaccine-annuallypast-8-years (accessed on 17 January 2023).
- World Health Organization. UNICEF and WHO Warn of ‘Perfect Storm’ of Conditions for Measles Outbreaks, Affecting Children. WHO. 2022. Available online: https://www.who.int/news/item/27-04-2022-unicef-andwho-warn-of–perfect-storm–of-conditions-for-measles-outbreaks–affectingchildren (accessed on 16 January 2023).
- Abdelmoneim, S.A.; Sallam, M.; Hafez, D.M.; Elrewany, E.; Mousli, H.M.; Hammad, E.M.; Elkhadry, S.W.; Adam, M.F.; Ghobashy, A.A.; Naguib, M.; et al. COVID-19 Vaccine Booster Dose Acceptance: Systematic Review and Meta-Analysis. Trop. Med. Infect. Dis. 2022, 7, 298. [Google Scholar] [CrossRef]
- Iguacel, I.; Álvarez-Najar, J.P.; Vásquez, P.D.C.; Alarcón, J.; Orte, M.; Samatán, E.; Martínez-Jarreta, B. Citizen Stance towards Mandatory COVID-19 Vaccination and Vaccine Booster Doses: A Study in Colombia, El Salvador and Spain. Vaccines 2022, 10, 781. [Google Scholar] [CrossRef]
- Wirawan, G.B.S.; Harjana, N.P.A.; Nugrahani, N.W.; Januraga, P.P. Health Beliefs and Socioeconomic Determinants of COVID-19 Booster Vaccine Acceptance: An Indonesian Cross-Sectional Study. Vaccines 2022, 10, 724. [Google Scholar] [CrossRef]
- Wu, F.; Yuan, Y.; Deng, Z.; Yin, D.; Shen, Q.; Zeng, J.; Xie, Y.; Xu, M.; Yang, M.; Jiang, S.; et al. Acceptance of COVID-19 booster vaccination based on the protection motivation theory: A cross-sectional study in China. J. Med. Virol. 2022, 94, 4115–4124. [Google Scholar] [CrossRef]
- Galanis, P.; Vraka, I.; Katsiroumpa, A.; Siskou, O.; Konstantakopoulou, O.; Katsoulas, T.; Mariolis-Sapsakos, T.; Kaitelidou, D. Predictors of Willingness of the General Public to Receive a Second COVID-19 Booster Dose or a New COVID-19 Vaccine: A Cross-Sectional Study in Greece. Vaccines 2022, 10, 1061. [Google Scholar] [CrossRef]
- Chenchula, S.; Karunakaran, P.; Sharma, S.; Chavan, M. Current evidence on efficacy of COVID-19 booster dose vaccination against the Omicron variant: A systematic review. J. Med. Virol. 2022, 94, 2969–2976. [Google Scholar] [CrossRef]
- Deng, J.; Ma, Y.; Liu, Q.; Du, M.; Liu, M.; Liu, J. Comparison of the Effectiveness and Safety of Heterologous Booster Doses with Homologous Booster Doses for SARS-CoV-2 Vaccines: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2022, 19, 10752. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, e1–e34. [Google Scholar] [CrossRef]
- Urrunaga-Pastor, D.; Fernandez-Guzman, D.; Caira-Chuquineyra, B.; Herrera-Añazco, P.; Benites-Zapata, V.A.; Bendezu-Quispe, G. Prevalence and factors associated with not receiving the booster dose of the COVID-19 vaccine in adults in Latin America and the Caribbean. Travel Med. Infect. Dis. 2022, 50, 102409. [Google Scholar] [CrossRef]
- Abouzid, M.; Ahmed, A.A.; El-Sherif, D.M.; Alonazi, W.B.; Eatmann, A.I.; Alshehri, M.M.; Saleh, R.N.; Ahmed, M.H.; Aziz, I.A.; Abdelslam, A.E.; et al. Attitudes toward receiving COVID-19 booster dose in the Middle East and North Africa (MENA) region: A cross-sectional study of 3041 fully vaccinated participants. Vaccines 2022, 10, 1270. [Google Scholar] [CrossRef] [PubMed]
- Abullais, S.S.; Arora, S.; Parveen, S.; Mahmood, S.E.; Baba, S.M.; Khalid, I.; Khader, M.A.; Elgib, M.F.A. Perceptions, motivation factors, and barriers to a COVID-19 booster immunization in a subpopulation of KSA: A cross-sectional study. Medicine 2022, 101, e31669. [Google Scholar] [CrossRef] [PubMed]
- Achrekar, G.C.; Batra, K.; Urankar, Y.; Batra, R.; Iqbal, N.; Choudhury, S.A.; Hooda, D.; Khan, R.; Arora, S.; Singh, A.; et al. Assessing COVID-19 booster hesitancy and its correlates: An early evidence from India. Vaccines 2022, 10, 1048. [Google Scholar] [CrossRef]
- Al-Qerem, W.; Jarab, A.; Hammad, A.; Alsajri, A.H.; Al-Hishma, S.W.; Ling, J.; Alabdullah, A.S.; Salama, A.; Mosleh, R. Knowledge, Attitudes, and Practices of Adult Iraqi Population Towards COVID-19 Booster Dose: A Cross-Sectional Study. Patient Prefer. Adherence 2022, 16, 1525–1537. [Google Scholar] [CrossRef]
- Babicki, M.; Mastalerz-Migas, A. Attitudes of Poles towards the COVID-19 Vaccine Booster Dose: An Online Survey in Poland. Vaccines 2022, 10, 68. [Google Scholar] [CrossRef] [PubMed]
- Bennett, N.G.; Bloom, D.E.; Ferranna, M. Factors underlying COVID-19 vaccine and booster hesitancy and refusal, and incentivizing vaccine adoption. PLoS ONE 2022, 17, e0274529. [Google Scholar] [CrossRef]
- Chrissian, A.A.; Oyoyo, U.E.; Patel, P.; Beeson, W.L.; Loo, L.K.; Tavakoli, S.; Dubov, A. Impact of COVID-19 vaccine-associated side effects on health care worker absenteeism and future booster vaccination. Vaccine 2022, 40, 3174–3181. [Google Scholar] [CrossRef]
- De Giorgio, A.; Kuvačić, G.; Maleš, D.; Vecchio, I.; Tornali, C.; Ishac, W.; Ramaci, T.; Barattucci, M.; Milavić, B. Willingness to Receive COVID-19 Booster Vaccine: Associations between Green-Pass, Social Media Information, Anti-Vax Beliefs, and Emotional Balance. Vaccines 2022, 10, 481. [Google Scholar] [CrossRef]
- Ghazy, R.M.; Abdou, M.S.; Awaidy, S.; Sallam, M.; Elbarazi, I.; Youssef, N.; Fiidow, O.A.; Mehdad, S.; Hussein, M.F.; Adam, M.F.; et al. Acceptance of COVID-19 Vaccine Booster Doses Using the Health Belief Model: A Cross-Sectional Study in Low-Middle- and High-Income Countries of the East Mediterranean Region. Int. J. Environ. Res. Public Health 2022, 19, 12136. [Google Scholar] [CrossRef]
- Huang, L.L.; Yang, Y.P.; Mao, H.P.; Hu, W.W.; Jiang, Y.H.; Jiesisibieke, Z.L.; Tung, T.H. Parental hesitancy towards vaccinating their children with a booster dose against COVID-19: Real-world evidence from Taizhou, China. J. Infect. Public Health 2022, 15, 1006–1012. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.S.R.; Nguyen, T.X.T.; Lal, S.; Watanapongvanich, S.; Kadoya, Y. Hesitancy towards the Third Dose of COVID-19 Vaccine among the Younger Generation in Japan. Int. J. Environ. Res. Public Health 2022, 19, 7041. [Google Scholar] [CrossRef]
- Klugar, M.; Riad, A.; Mohanan, L.; Pokorná, A. COVID-19 Vaccine Booster Hesitancy (VBH) of Healthcare Workers in Czechia: National Cross-Sectional Study. Vaccines 2021, 9, 1437. [Google Scholar] [CrossRef]
- Koh, S.W.C.; Tan, H.M.; Lee, W.H.; Mathews, J.; Young, D. COVID-19 Vaccine Booster Hesitancy among Healthcare Workers: A Retrospective Observational Study in Singapore. Vaccines 2022, 10, 464. [Google Scholar] [CrossRef] [PubMed]
- Lennon, R.P.; Block Jr, R.; Schneider, E.C.; Zephrin, L.; Shah, A.; Collaborative, T.A.A.R. and 2021 COVID Group. Underserved population acceptance of combination influenza-COVID-19 booster vaccines. Vaccine 2022, 40, 562–567. [Google Scholar] [CrossRef]
- Luk, T.T.; Lui, J.H.T.; Wang, M.P. Efficacy, Usability, and Acceptability of a Chatbot for Promoting COVID-19 Vaccination in Unvaccinated or Booster-Hesitant Young Adults: Pre-Post Pilot Study. J. Med. Internet Res. 2022, 24, e39063. [Google Scholar] [CrossRef] [PubMed]
- Ma, L.; Yang, J.; Zhang, T.; Han, X.; Huang, Q.; Yang, Y.; Feng, L.; Yang, W.; Wang, C. Willingness toward COVID-19 vaccination, coadministration with other vaccines and receive a COVID-19 vaccine booster: A cross-sectional study on the guardians of children in China. Hum. Vaccines Immunother. 2022, 18, 2049169. [Google Scholar] [CrossRef]
- Motta, M. The Correlates & Public Health Consequences of Prospective Vaccine Hesitancy among Individuals Who Received COVID-19 Vaccine Boosters in the U.S. Vaccines 2022, 10, 1791. [Google Scholar] [CrossRef]
- Qin, C.; Yan, W.; Tao, L.; Liu, M.; Liu, J. The Association between Risk Perception and Hesitancy toward the Booster Dose of COVID-19 Vaccine among People Aged 60 Years and Older in China. Vaccines 2022, 10, 1112. [Google Scholar] [CrossRef]
- Qin, C.; Wang, R.; Tao, L.; Liu, M.; Liu, J. Association Between Risk Perception and Acceptance for a Booster Dose of COVID-19 Vaccine to Children Among Child Caregivers in China. Front. Public Health 2022, 10, 834572. [Google Scholar] [CrossRef]
- Rzymski, P.; Poniedziałek, B.; Fal, A. Willingness to Receive the Booster COVID-19 Vaccine Dose in Poland. Vaccines 2021, 9, 1286. [Google Scholar] [CrossRef] [PubMed]
- Shehab, M.; Alrashed, F.; Alfadhli, A. COVID-19 Vaccine Booster Dose Willingness among Patients with Inflammatory Bowel Disease on Infliximab and Vedolizumab: A Cross-Sectional Study. Vaccines 2022, 10, 1166. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Dai, H.; Wang, P.; Zhang, X.; Cui, D.; Huang, Y.; Zhang, J.; Xiang, T. Will People Accept a Third Booster Dose of the COVID-19 Vaccine? A Cross-Sectional Study in China. Front. Public Health 2022, 10, 914950. [Google Scholar] [CrossRef] [PubMed]
- Talmy, T.; Nitzan, I. Rapid rollout and initial uptake of a booster COVID-19 vaccine among Israel defense forces soldiers. J. Prev. 2022, 44, 1–14. [Google Scholar] [CrossRef]
- Tan, K.Y.K.; Soh, A.S.E.; Ong, B.W.L.; Chen, M.I.; Griva, K. Determining the Prevalence and Correlates of COVID-19 Booster Vaccine Hesitancy in the Singapore Population Following the Completion of the Primary Vaccination Series. Vaccines 2022, 10, 1088. [Google Scholar] [CrossRef]
- Vellappally, S.; Naik, S.; Alsadon, O.; Al-Kheraif, A.A.; Alayadi, H.; Alsiwat, A.J.; Kumar, A.; Hashem, M.; Varghese, N.; Thomas, N.G.; et al. Perception of COVID-19 Booster Dose Vaccine among Healthcare Workers in India and Saudi Arabia. Int. J. Environ. Res. Public Health 2022, 19, 8942. [Google Scholar] [CrossRef]
- Yadete, T.; Batra, K.; Netski, D.M.; Antonio, S.; Patros, M.J.; Bester, J.C. Assessing Acceptability of COVID-19 Vaccine Booster Dose among Adult Americans: A Cross-Sectional Study. Vaccines 2021, 9, 1424. [Google Scholar] [CrossRef]
- Yoshida, M.; Kobashi, Y.; Kawamura, T.; Shimazu, Y.; Nishikawa, Y.; Omata, F.; Zhao, T.; Yamamoto, C.; Kaneko, Y.; Nakayama, A.; et al. Factors Associated with COVID-19 Vaccine Booster Hesitancy: A Retrospective Cohort Study, Fukushima Vaccination Community Survey. Vaccines 2022, 10, 515. [Google Scholar] [CrossRef]
- Zhou, M.; Liu, L.; Gu, S.Y.; Peng, X.Q.; Zhang, C.; Wu, Q.F.; Xu, X.P.; You, H. Behavioral Intention and Its Predictors toward COVID-19 Booster Vaccination among Chinese Parents: Applying Two Behavioral Theories. Int. J. Environ. Res. Public Health 2022, 19, 7520. [Google Scholar] [CrossRef]
- Surie, D.; DeCuir, J.; Zhu, Y.; Gaglani, M.; Ginde, A.A.; Douin, D.J.; Talbot, H.K.; Casey, J.D.; Mohr, N.M.; Zepeski, A.; et al. Early Estimates of Bivalent mRNA Vaccine Effectiveness in Preventing COVID-19–Associated Hospitalization Among Immunocompetent Adults Aged ≥65 Years—IVY Network, 18 States, September 8–November 30, 2022. Morb. Mortal. Wkly. Rep. 2022, 71, 1625–1630. [Google Scholar] [CrossRef]
- Tenforde, M.W.; Weber, Z.A.; Natarajan, K.; Klein, N.P.; Kharband, A.B.; Stenehjem, E.; Embi, P.J.; Reese, S.E.; Naleway, A.L.; Grannis, S.J.; et al. Early Estimates of Bivalent mRNA Vaccine Effectiveness in Preventing COVID-19–Associated Emergency Department or Urgent Care Encounters and Hospitalizations Among Immunocompetent Adults—VISION Network, Nine States, September–November 2022. Morb. Mortal. Wkly. Rep. 2022, 71, 1616–1624. [Google Scholar] [CrossRef]
- Danabal, K.G.M.; Magesh, S.S.; Saravanan, S.; Gopichandran, V. Attitude towards COVID 19 vaccines and vaccine hesitancy in urban and rural communities in Tamil Nadu, India–a community based survey. BMC Health Serv. Res. 2021, 21, 994. [Google Scholar] [CrossRef] [PubMed]
- Wiysonge, C.S.; Ndwandwe, D.; Ryan, J.; Jaca, A.; Batouré, O.; Anya, B.P.M.; Cooper, S. Vaccine hesitancy in the era of COVID-19: Could lessons from the past help in divining the future? Hum. Vaccines Immunother. 2022, 18, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Schmid, P.; Rauber, D.; Betsch, C.; Lidolt, G.; Denker, M.L. Barriers of influenza vaccination intention and behavior—A systematic review of influenza vaccine hesitancy, 2005–2016. PLoS ONE 2017, 12, e0170550. [Google Scholar] [CrossRef]
- Frew, P.M.; Lutz, C.S. Interventions to increase pediatric vaccine uptake: An overview of recent findings. Hum. Vaccines Immunother. 2017, 13, 2503–2511. [Google Scholar] [CrossRef]
| Database | Search Terms (Boolean Operators) | #Records |
|---|---|---|
| PubMed | (((((((((((booster[Title]) AND (hesitancy)) OR (refusal)) OR (delay)) OR (decline)) OR (reluctance)) OR (unwillingness)) AND (covid-19)) OR (coronavirus)) OR (2019-ncov)) OR (sars-cov-2)) OR (cov-19) | 147 |
| CINAHL | TI booster AND TX (hesitancy or refusal or delay or decline or reluctance or unwillingness) AND TX (covid-19 or coronavirus or 2019-ncov or sars-cov-2 or cov-19) | 22 |
| Medline | TI booster AND TX (hesitancy or refusal or delay or decline or reluctance or unwillingness) AND TX (covid-19 or coronavirus or 2019-ncov or sars-cov-2 or cov-19) | 128 |
| Web of Science | ((((((((((TI=(booster)) AND ALL=(hesitancy)) OR ALL=(refusal)) OR ALL=(delay)) OR ALL=(decline)) OR ALL=(reluctance)) AND ALL=(unwillingness)) AND ALL=(covid-19)) OR ALL=(coronavirus)) OR ALL=(2019-ncov)) OR ALL=(sars-cov-2) OR ALL=(cov-19) | 260 |
| Scopus | Title (booster) AND ALL (hesitancy) OR (refusal) OR (delay) OR (decline) OR (reluctance) OR (unwillingness) AND ALL (covid-19) OR (coronavirus) OR (2019-ncov) OR (sars-cov-2) OR cov-19 | 252 |
| Author(s) | Year of Publication | Data Collection Year | Country/Region | CBVH % | Population | Sample Size | Sampling Technique | Study Design | Predictors of CBVH |
|---|---|---|---|---|---|---|---|---|---|
| Abouzid et al. [26] | 2022 | 2021 | EMR nations of Egypt, Iraq, Palestine, Saudi Arabia Sudan | 20.4 | General public | 3041 | NR | C-S survey | Safety uncertainties, opinions that the booster dose is unnecessary, side effects associated with previous COVID-19 vaccines, history of COVID-19 infection, influenza-unvaccinated individuals, females, normal body mass index, country |
| Abullais et al. [27] | 2022 | 2021 | Saudi Arabia | 49.8 | General public | 520 | RS | C-S survey | Vaccine allergy, only a single dose of the COVID-19 vaccination, private hospital usage |
| Achrekar et al. [28] | 2022 | 2021–2022 | India | 44.1 | General public | 687 | NR | C-S survey | Unvaccinated with the primary series, low income, rural residents, not living with vulnerable individuals, family/friend history of COVID-19 infection |
| Al-Qerem et al. [7] | 2022a | 2021 | Jordan | 54.7 | General public | 915 | NR | C-S survey | Income (medium), perceived susceptibility, post-vaccine symptoms, government mandate |
| Al-Qerem et al. [29] | 2022b | 2022 | Iraq | 38.6 | General public | 754 | NR | C-S survey | Age (younger), education (low), low knowledge about COVID-19, did not know someone who had died due to COVID-19, low perceived susceptibility, low perceived severity, high perceived seriousness of COVID-19, low side effects from previous COVID-19 vaccination doses, received a COVID vaccine due to government mandate, low adherence to protective practices against COVID-19, vaccine brand (AstraZeneca vs. Sinopharm) |
| Babicki et al. [30] | 2022 | 2021 | Poland | 30.1 | General public | 1528 | NR | C-S survey | Lack of confidence in the effectiveness of the booster dose, experienced adverse events following vaccination, family/friend experienced adverse events following vaccination, fear of future complications |
| Batra et al. [2] | 2022 | 2021 | U.S. | 41.7 | General public | 501 | NR | C-S survey | Unvaccinated with the primary series, younger, single or never married, education (low), Republicans, low vaccine literacy, low vaccine confidence, low behavioral confidence |
| Bendezu-Quispe et al. [12] | 2022 | 2022 | Peru | 21.5 | General public | 20,814 | RS | C-S survey | Gender, age (under 75 years), education, employed, history of COVID-19 infection, living in a town or rural area |
| Bennett et al. [31] | 2022 | 2021 | U.S. | 32.4 | General public | 3497 | NR | C-S survey | Age; ethnicity; education; rural residents; non-Democrats; household member at least 60 years of age; knew someone who had been hospitalized or died of COVID-19; knew someone with severe vaccine side effects; belief that one’s health is in God’s hands; lack trust in the government, CDC, or health care system; lack trust in COVID-19 vaccine efficacy |
| Chrissian et al. [32] | 2022 | 2021 | U.S. | 35.6 | HCW | 2491 | NR | C-S survey | Age (younger), education (lower), Moderna vaccine recipient, missed work due to vaccine-related symptoms, would not recommend vaccine to family or friends |
| De Giorgio et al. [33] | 2022 | 2021 | Croatia | 56.63 | General public | 1003 | NR | C-S survey | Vaccine information source (social networks, general internet blogs/forums, and friends/acquaintances), low optimism about the future |
| Folcarelli et al. [9] | 2022 | 2021 | Italy | 24.7 | General public | 615 | NR | C-S survey | Need additional information regarding the booster dose, no friends or family diagnosed with COVID-19, not having received information regarding the booster dose from official government organization, lower self-rated health status |
| Galanis et al. [21] | 2022 | 2022 | Greece | 38.1 | General public | 815 | NR | C-S survey | Concerns about side effects, concerns about effectiveness, opinion that further vaccination is unnecessary |
| Ghazy et al. [34] | 2022 | 2022 | EMR | 20.67 | General public | 2327 | NR | C-S survey | Beliefs that booster doses have no benefit, severe side effects from prior doses |
| Huang et al. [35] | 2022 | 2022 | China | 41.8 | Parent | 514 | NR | C-S survey | Gender (mother), parental belief in need for booster, parental attitude toward booster, presence of people around parents hesitant about booster vaccines for children |
| Khan et al. [36] | 2022 | 2022 | Japan | 34 | General public | 2912 | NR | C-S survey | Gender (men), age (younger), subjective health status, future anxiety, marital status, have children, household income and assets, myopic (i.e., present-focused) view of future |
| Klugar et al. [37] | 2021 | 2021 | Czech Republic | 28.8 | HCW | 3454 | NR | C-S survey | Gender (female), pregnant, age (young), allied health professionals, prior infection, previously unvaccinated, previously sought medical care for COVID-19 |
| Koh et al. [38] | 2022 | 2021 | Singapore | 26.2 | HCW | 891 | NR | C-S survey | First-dose hesitant, vaccine dose (booster vs. first dose), occupation (administrative staff vs. ancillary, medical, or nursing) |
| Kowalski et al. [4] | 2022 | 2021 | Germany | 46 | COVID-19 patients | 224 | NR | C-S survey | Age (younger), nationality (foreign), income (low), low trust in vaccination effectiveness, fear of negative vaccination side effects, low trust in the governmental pandemic management, low subjective informativeness about SARS-CoV-2, support of conspiracy theories |
| Lennon et al. [39] | 2022 | 2021 | U.S. | 55 | General public | 12,887 | NR | C-S survey | Gender (female), ethnicity (Black, Native American), residency (rural) |
| Lounis et al. [8] | 2022 | 2022 | Algeria | 48.8 | General public | 787 | NR | C-S survey | Gender (female), age (younger), HCW, education (high: postgraduate degrees), history of COVID-19 infection, regret after vaccine, belief vaccines are not efficient |
| Luk et al. [40] | 2022 | 2021 | Hong Kong | 28.6 | Students | 290 | NR | C-S survey | eHealth literacy, perceived danger of COVID-19 |
| Ma et al. [41] | 2022 | 2021 | China | 17.63 | Parents | 9424 | NR | C-S survey | Education (higher), occupation (housewives vs. other occupations), occupation (service workers vs. other occupations) |
| Motta et al. [42] | 2022 | 2022 | U.S. | General public | 1551 | NR | C-S survey | Concerns about missing work for vaccination, unconvinced that additional boosters are necessary | |
| Noh et al. [5] | 2022 | 2021 | Korea | 48.8 | General public and parents | 2993 | NR | C-S survey | For self: gender (women), age (younger), education (low), brand (Moderna or mRNA-1273), experienced serious adverse events following previous COVID-19 vaccination, concerns about safety, doubts about efficacy For children: parent with children aged < 18 years, younger, higher education, Pfizer (BNT162b2), history of COVID-19 infection |
| Paul and Fancourt [10] | 2022 | 2021 | U.K. | 8 | General public | 22,139 | NR | C-S survey | Healthy adults, perceived susceptibility, perceived severity, low compliance with COVID-19 government guidelines during periods of strict restrictions, education (lower), socio-economic (lower), age (lower: below 45 years) |
| Qin et al. [43] | 2022a | 2022 | China | 17.2 | 60 years or older | 3321 | RS | C-S survey | Belief that they were ineligible for vaccination due to certain illnesses, concerns about vaccine safety, belief that booster shots are unnecessary, limitation on their movements, low perceived susceptibility, perceived benefit (low to moderate), perceived barriers (moderate to high) |
| Qin et al. [44] | 2022b | 2021 | China | 11.56 | Parents | 1724 | NR | C-S survey | Belief that vaccination process is complicated and time wasting, vaccine safety uncertainty, vaccine efficacy uncertainty, belief that booster is unnecessary |
| Rzymski et al. [45] | 2021 | 2021 | Poland | 29 | General public | 2427 | NR | C-S survey | Age (young), gender (male), absence of immunosuppression, no chronic disease, history of COVID-19 infection after 1st dose, never had influenza vaccination, prior booster side effects, fear of booster |
| Seboka et al. [13] | 2022 | 2022 | Pakistan | 22.2 | General public | 787 | NR | C-S survey | Unwillingness to pay for the booster, partial vaccination, safety concerns due to prior side effects of doses, belief that COVID-19 is similar to seasonal flu, belief in natural immunity, vaccine brand (AstraZeneca) |
| Shehab et al. [46] | 2022 | 2022 | Kuwait | 41.9 | Patients | 499 | NR | C-S survey | Vaccine type (AstraZeneca), biologic therapy |
| Sun et al. [47] | 2022 | 2021 | China | 9.61 | General public | 1062 | NR | C-S survey | low perceived risk of COVID-19 infection, worried about the rapid mutation of SARS-CoV-2, belief that the vaccine is ineffective, worried about side effects |
| Talmy and Nitzan [48] | 2022 | 2021 | Israel | 15.5 | Army | 1157 | NR | C-S survey | Below-average cognitive function score |
| Tan et al. [49] | 2022 | 2021 | Singapore | 30.5 | General public | 1552 | NR | C-S survey | Education (tertiary), lower COVID-19 threat perception, lower perceived benefits, higher perceived concerns, decreased need for booster vaccination, lower benefit/concerns differential score |
| Urrunaga-Pastor et al. [25] | 2022 | 2022 | Latin America and the Caribbean | 33.7 | General public | 154,841 | RS | C-S survey | Age (under 75 years), education (lower), having no or 1 to 2 comorbidities, town resident, has food insecurity, depressive symptoms, has had COVID-19 |
| Vellappally et al. [50] | 2022 | 2022 | India and Saudi Arabia | 16 and 33 | HCW | 530 and 303 | NR | C-S survey | India: concerns about vaccine effectiveness, concerns about probable long-term side effects Saudi Arabia: concerns about not knowing enough about the vaccination, concerns about probable long-term side effects |
| Wang et al. [11] | 2022 | 2021 | China | 6.5 | General public | 3119 | RS | C-S survey | Unemployment, low monthly income, low scores of knowledge, low level of cues to action, low perceived importance of social media, official social media use, traditional media use |
| Wu et al. [20] | 2022 | 2021 | China | 23.2 | General public | 8229 | NR | C-S survey | High perceived severity, response cost (risk), low perceived susceptibility, low response efficacy (benefit), low self-efficacy |
| Yadete et al. [51] | 2021 | 2021 | U.S. | 38 | General public | 2138 | NR | C-S survey | Single or never married, less educated, lives in the southern region of the U.S., unvaccinated, did not intend to have their children vaccinated, very little to no trust in the COVID-19 vaccine information given by public health/government agencies, low vaccine confidence, low vaccine literacy |
| Yoshida et al. [52] | 2022 | 2021 | Japan | 2.1 | General public | 2439 | NR | C-S survey | Age (younger), concerns about adverse reactions, experience of adverse reactions, concern about the efficacy of the COVID-19 vaccine, higher antibody levels |
| Zhou, M. et al. [53] | 2022 | 2021 | China | 12.7 | Parents | 1602 | RS | C-S survey | Response cost/risk |
| Zhou, Y. et al. [6] | 2022 | 2021 | China | 40.3 | General public | 1536 | NR | C-S survey | Younger, less educated, less healthy, unsure of vaccines’ efficacy and adverse events |
| Themes | Determinants of CBVH |
|---|---|
| Demographic | Increases CBVH Age Younger [4,5,6,8,29,32,36,37,45,52] Younger: below 45 years of age [2,10] Under 75 years of age [12,25] Parent with children aged <18 years [5] Younger parent [5] Education Lower level [5,6,10,25,32,51] With some high school [2] Less than postgraduate [12] Higher level [8,41] High: tertiary education [49] Parent with higher education [5] Gender Females [5,8,26,37,39] Mothers [35] Pregnant women [37] Males [36,45] Occupation HCWs vs. other [8] Administrative staff vs. ancillary, medical, and nursing [38] Allied health professions vs. other HCWs [37] Housewives vs. those with other occupations [41] Service workers vs. those with other occupations [41] Income Low [4,10,11,28] Medium [7] High household income among young adults [36] |
| Demographic | Ethnicity Black [31,39] Native American [39] Employment Unemployed [11] Employed [12] Other demographic Marital status (single or never married) [2,51] Nationality (foreign) [4] Decreases CBVH Age Aged 65 and older [31] Household member is at least 60 years of age [31] Education College degree [31] Low [29] Gender Female [12] Income High household income and assets [36] Ethnicity Asian and Hispanic [31] Other demographic Marital status (married) [36] Having children [36] |
| Geographical | Increases CBVH Country: (Saudi Arabia) [26] Living in a rural area [12,28,31,39] Living in a town [25] Living in a town compared to living in the city [12] Living in a southern region of the U.S. [51] |
| Adverse events | Increases CBVH Fear of booster side effects [4,21,45,47] Severity of side effects associated with previous COVID-19 vaccine [26,34] Knowledge of someone whose vaccine side effects were severe [31] Safety concerns due to side effects after previous doses [13] Concerns about possible long-term side effects of booster vaccines [50] Fear of future complications of boosters [30] Concerns about adverse reactions to booster vaccines [6,52] Personal experience of adverse events following vaccination [30] Family or friend’s experience of adverse events following vaccination [30] Experience of adverse reactions such as nausea [52] Experience of serious adverse events following previous COVID-19 vaccination [5] Post-vaccine mild or no symptom [7] Receipt of medical care following the COVID-19 vaccine primer doses [37] Uncertainty about the vaccine safety [26,44] Concern about vaccine safety [5,43] Higher perceived concerns about boosters [49] High response cost (i.e., adverse effects of boosters may interfere with daily activities) [20,53] Missing work due to vaccine-related symptoms [32] Decreases CBVH Low side effects associated with previous COVID-19 vaccine [29] |
| Perceived benefit/efficacy | Increases CBVH Lack of confidence in the effectiveness of the booster dose [2,30,51] Lack trust in the efficacy of the vaccine [4,31] Concerns about the efficacy of the vaccine [8,21,47,50,52] Uncertainty about COVID-19 vaccine’s efficacy [5,6,44] Beliefs that booster doses have no benefit [34] Lower perceived benefits of booster vaccines [49] Lower benefit/concerns differential score [49] Perceived benefit (low to moderate) [43] Decreases CBVH High response efficacy/benefit [20] |
| Perceived susceptibility | Increases CBVH Adults who believed they would not be infected with COVID-19 in the next 6 months [29] Seniors aged 60 years and older with a low perceived susceptibility [43] Adults with a low perceived susceptibility [20,47] Fully vaccinated adults who felt less stress about catching COVID-19 [10] Adults who had lower perceived risk of contracting COVID-19 [49] Decreases CBVH Adults who were categorized in the high-level group of developing COVID-19 complications [7] |
| Perceived severity | Increases CBVH Low perceived severity of COVID-19 [29,40] Low levels of current stress about becoming seriously ill from COVID-19 [10] High perceived severity [20] |
| History of COVID-19 infection | Increases CBVH History of COVID-19 infection [8,12,25,37] History of COVID-19 infection after at least one dose [26,45] No family/friends tested positive for COVID-19 [9,28] Did not personally know someone who had died due to COVID-19 [29] Parents with history of COVID-19 infection [5] Decreases CBVH Knew someone who had been hospitalized or died of COVID-19 [31] |
| Vaccination status | Increases CBVH Unvaccinated with the primary series [2,28,37,51] Partial vaccination with the primary series [13] People with a single COVID-19 vaccine dose vs. two or more doses [27] Never had influenza vaccination [26,45] Parents who were unwilling to vaccinate their children [51] |
| Booster vaccine recommendation or mandate | Increases CBVH Would not recommend vaccine to family or friends [32] Low level of cues to action (i.e., vaccination recommendation from physicians, family members, or community workers) [11] Decreases CBVH Received primary series of COVID-19 vaccine due to imposed laws [7,29] |
| Medical conditions and health status | Increases CBVH Poor self-rated health status [6] Lower self-rated health status after the second dose of COVID-19 vaccination [9] 1 to 2 comorbidities [25] Depressive symptoms [25] People with allergy to vaccine [27] Good self-rated health status [10] Absence of immunosuppression [45] No chronic diseases [25,45] Normal body mass index [26] Belief in natural immunity [13] Higher antibody levels [52] Not living with vulnerable individuals [28] Below-average cognitive function scores [48] Decreases CBVH Good self-rated health status [36] Higher anxiety about the future [36] |
| Knowledge/information | Increases CBVH Low knowledge about COVID-19 [29] Low knowledge of COVID-19 vaccine [11] Low vaccine literacy [2,51] Low eHealth literacy [40] Concerns about not knowing enough about the vaccine [50] Want additional information regarding the booster dose [9] Did not receive information regarding the booster dose from an official government organization [9] Low subjective informativeness about SARS-CoV-2 [4] Belief that certain illnesses made them ineligible for vaccination [43] |
| Skepticism/distrust/conspiracy theories | Increases CBVH Belief that the booster dose is unnecessary [21,26,35,43,44,49] Skeptical of the need for boosters [42] Distrust in the government, CDC, and health care system [31] Low trust in the governmental pandemic management [4] Very little to no trust in the COVID-19 vaccine information provided by public health or government agencies [51] Supports conspiracy theories [4] Belief that one’s health is in God’s hands [31] Belief that COVID-19 is similar to the seasonal flu [13] |
| Vaccine type and treatments | Increases CBVH Moderna vs. Pfizer [32] Moderna vs. other vaccines [5] Pfizer vs. other vaccines [5] AstraZeneca vs. other vaccines [13,46] Biologic therapy (patients receiving vedolizumab) [46] Decreases CBVH AstraZeneca vs. Sinopharm [29] |
| Miscellaneous determinants | Increases CBVH Political affiliation (Republicans) in the United States [2] Non-Democrats who did not vote for President Biden in the United States [31] Low level of adherence to protective practices against COVID-19 [29] Low compliance with COVID-19 government guidelines during periods of strict restrictions (e.g., lockdowns) [10] Low behavioral confidence (i.e., a lack of certainty in regard to receiving the vaccine booster) [2] Less optimistic about the future [33] More myopic view of the future (i.e., less concerned about future consequences) [36] Experiencing food insecurity [25] Perceived barriers (moderate to high) [43] Low level of cues to action [11] Worried about the rapid mutation of SARS-CoV-2 [47] Concerns about missing work to vaccinate [42] Vaccine information source (social networks, general internet blogs/forums, and friends/acquaintances) [33] Traditional media use [11] Social influence (presence of people around them hesitant about children receiving booster vaccines) [35] Vaccine dose (booster vs. first dose) [38] First dose-hesitant [38] Belief that the vaccination process is complicated and time wasting [44] Unwillingness to pay for the booster [13] Visitor of a private hospital [27] Decreases CBVH High perceived importance of social media [11] High self-efficacy [20] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Limbu, Y.B.; Huhmann, B.A. Why Some People Are Hesitant to Receive COVID-19 Boosters: A Systematic Review. Trop. Med. Infect. Dis. 2023, 8, 159. https://doi.org/10.3390/tropicalmed8030159
Limbu YB, Huhmann BA. Why Some People Are Hesitant to Receive COVID-19 Boosters: A Systematic Review. Tropical Medicine and Infectious Disease. 2023; 8(3):159. https://doi.org/10.3390/tropicalmed8030159
Chicago/Turabian StyleLimbu, Yam B., and Bruce A. Huhmann. 2023. "Why Some People Are Hesitant to Receive COVID-19 Boosters: A Systematic Review" Tropical Medicine and Infectious Disease 8, no. 3: 159. https://doi.org/10.3390/tropicalmed8030159
APA StyleLimbu, Y. B., & Huhmann, B. A. (2023). Why Some People Are Hesitant to Receive COVID-19 Boosters: A Systematic Review. Tropical Medicine and Infectious Disease, 8(3), 159. https://doi.org/10.3390/tropicalmed8030159







