Endemic Melioidosis in Southern China: Past and Present
Abstract
1. Introduction
2. History
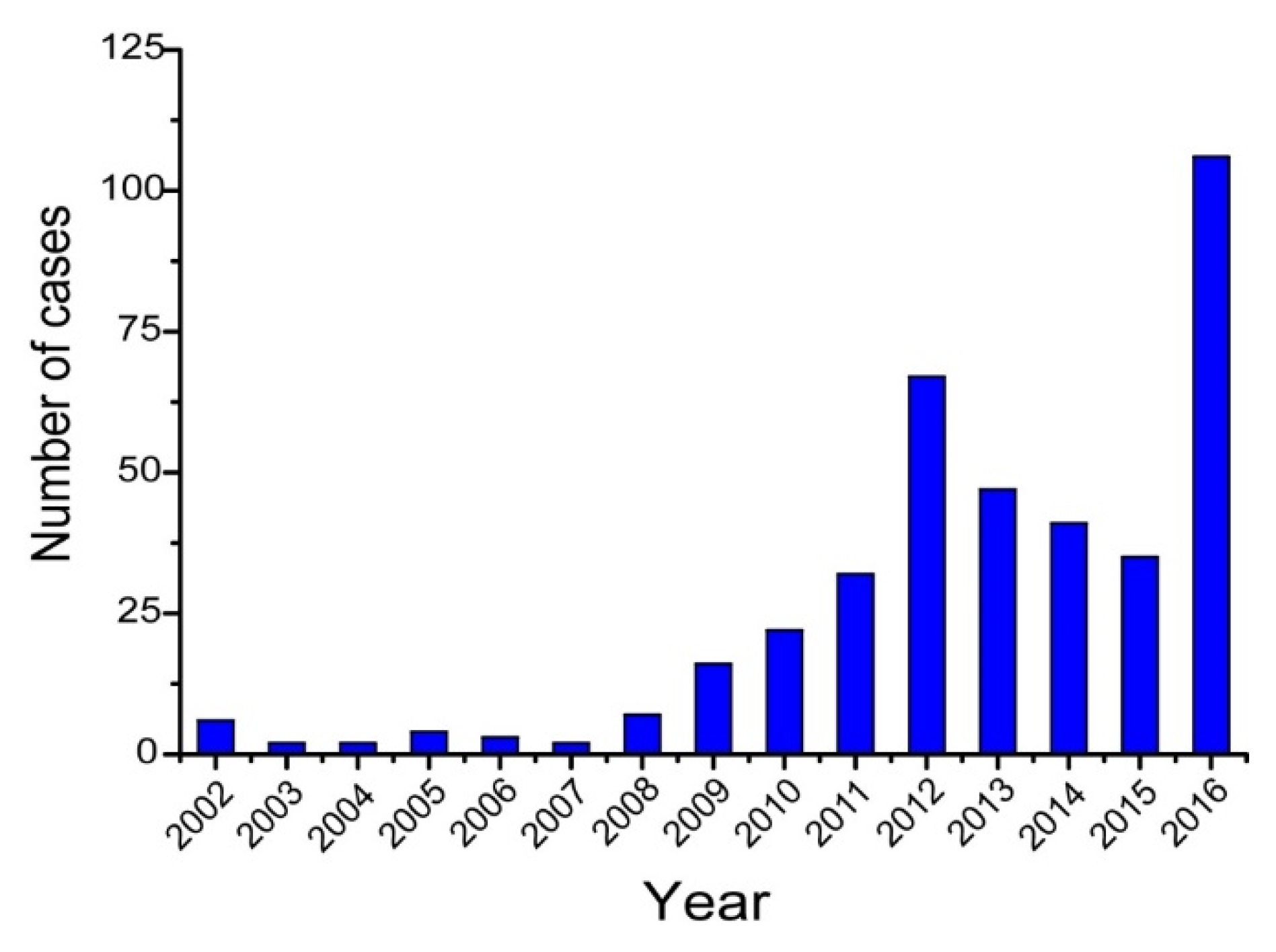
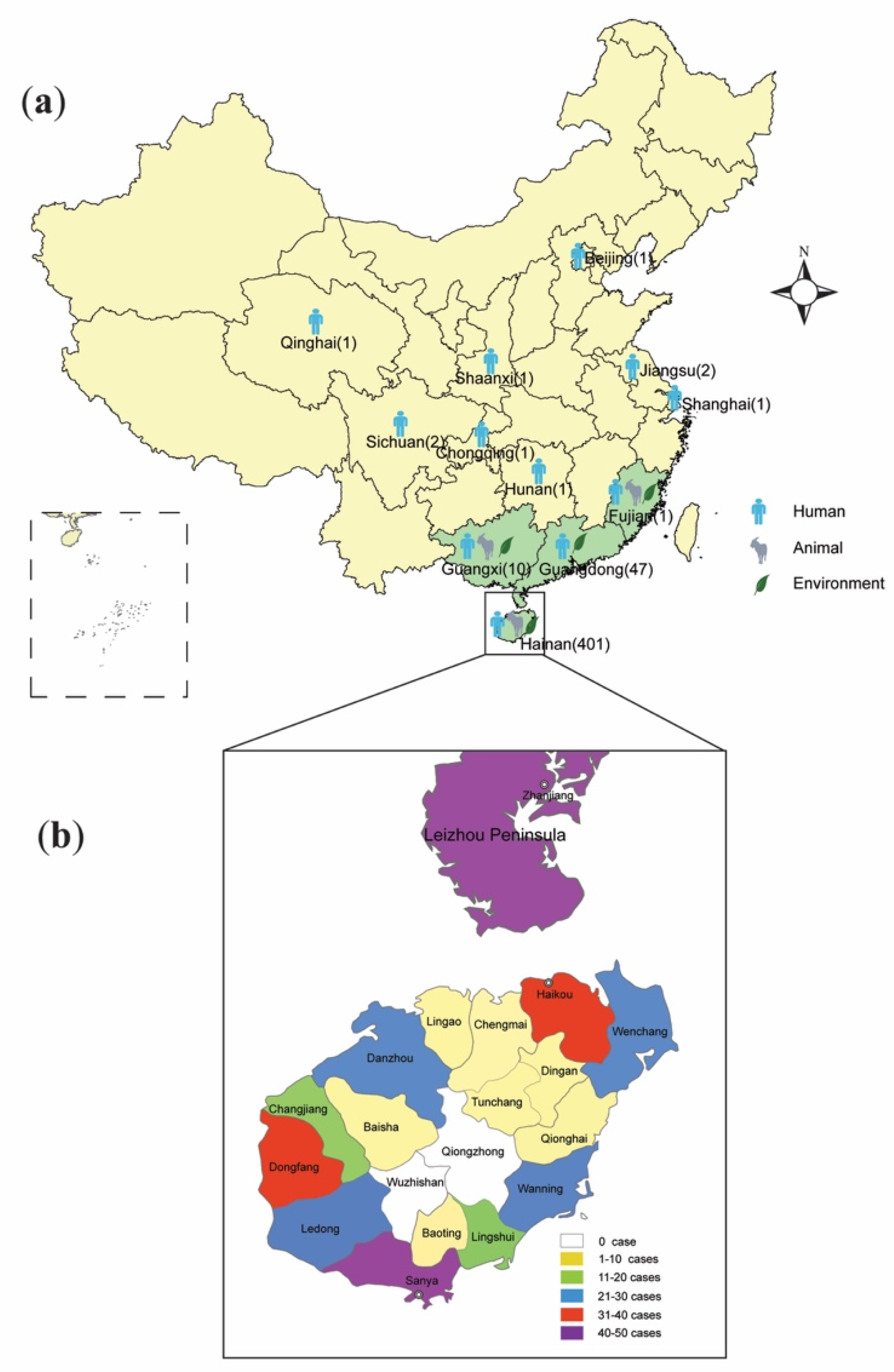
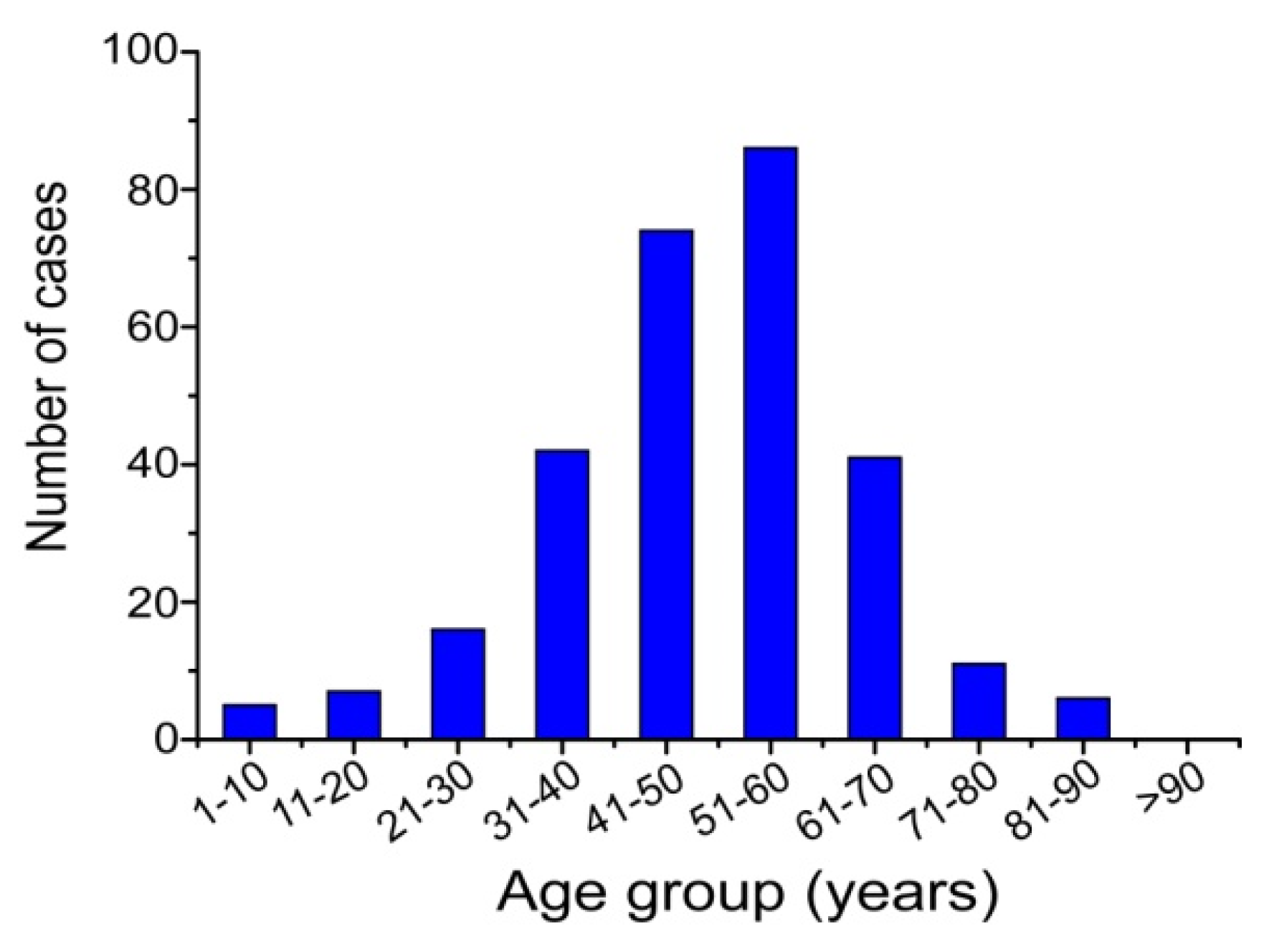
3. Review of Melioidosis Cases and Resurgence of the Disease in Hainan
4. Literature Review
5. Environmental and Molecular Investigations of B. pseudomallei in Hainan
5.1. Environmental Distribution of B. pseudomallei
5.2. Genetic Diversity of B. pseudomallei Isolates from Hainan
6. New Understanding of Melioidosis Epidemiology on Hainan
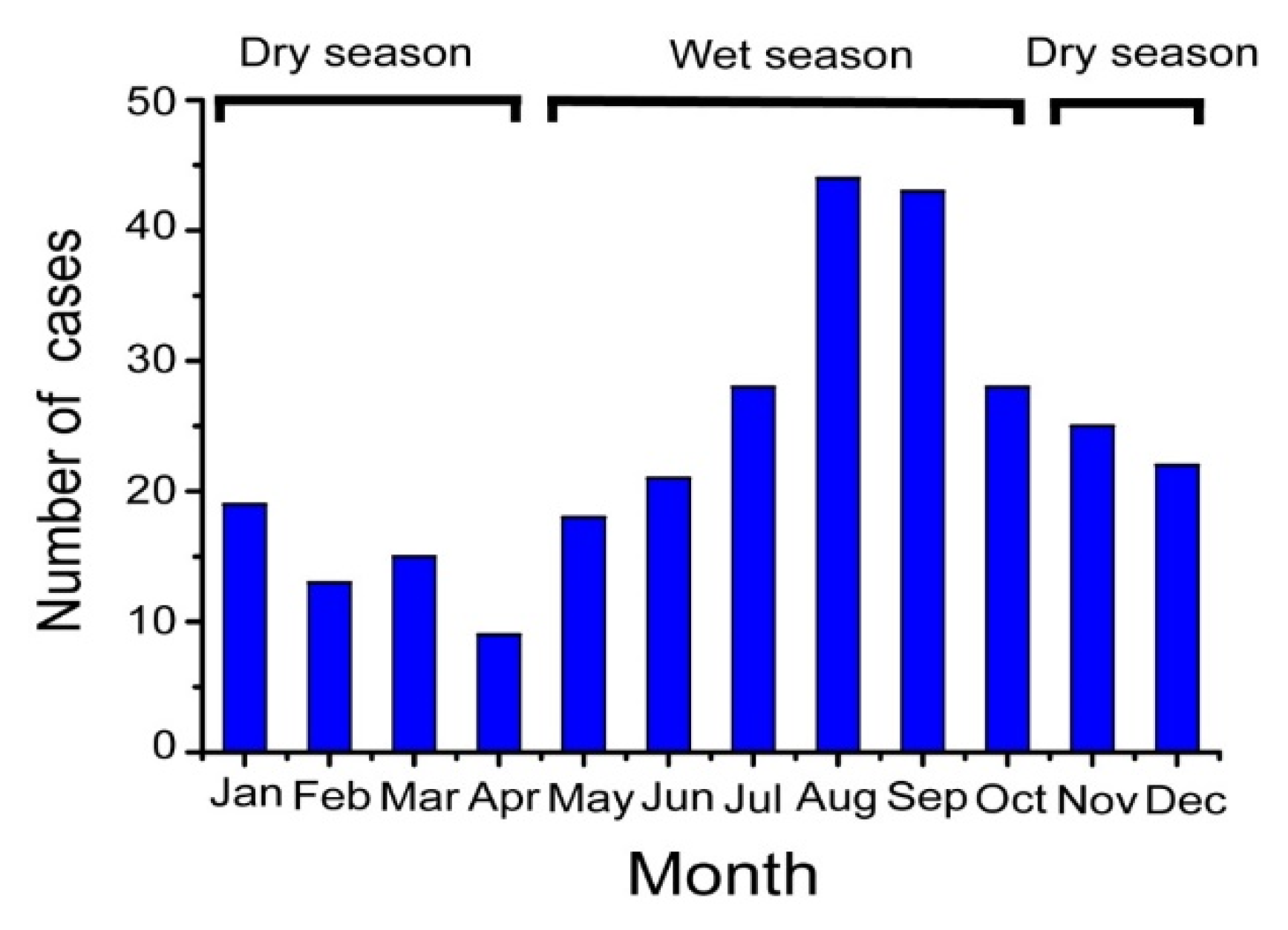
6.1. The Association between Typhoon and Case Clustering of Melioidosis
6.2. Disease Burden and Risk Analysis
7. Surveillance and Reporting of Melioidosis Cases in Mainland China
7.1. Human
7.2. Animals
7.3. Guidelines
8. Diagnosis and Treatment
9. Current and Future Challenges
10. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Wiersinga, W.J.; Currie, B.J.; Peacock, S.J. Melioidosis. N. Engl. J. Med. 2012, 367, 1035–1044. [Google Scholar] [CrossRef] [PubMed]
- Cheng, A.C.; Currie, B.J. Melioidosis: Epidemiology, pathophysiology, and management. Clin. Microbiol. Rev. 2005, 18, 383–416. [Google Scholar] [CrossRef] [PubMed]
- Currie, B.J. Melioidosis: Evolving concepts in epidemiology, pathogenesis, and treatment. Semin. Respir. Crit. Care Med. 2015, 36, 111–125. [Google Scholar] [CrossRef] [PubMed]
- Limmathurotsakul, D.; Golding, N.; Dance, D.A.; Messina, J.P.; Pigott, D.M.; Moyes, C.L.; Rolim, D.B.; Bertherat, E.; Day, N.P.; Peacock, S.J.; et al. Predicted global distribution of Burkholderia pseudomallei and burden of melioidosis. Nat. Microbiol. 2016, 1, 15008. [Google Scholar] [CrossRef] [PubMed]
- Yang, S. Melioidosis research in China. Acta Trop. 2000, 77, 157–165. [Google Scholar] [CrossRef]
- Mollaret, H.H. «L’affaire du jardin des plantes ou comment la mélioïdose fit son apparition en France. Med. Maladies Infect. 1988, 18, 643–654. (In French) [Google Scholar] [CrossRef]
- Li, L. Survey on endemic foci of melioidosis. Chin. J. Prev. Med. 1981, 15, 1–5. [Google Scholar]
- Li, L.; He, Y.W. Pseudomonas pseudomallei and melioidosis in China. Chin. Med. J. 1992, 105, 775–779. [Google Scholar] [PubMed]
- Yang, S.; Tong, S.; Lu, Z. Geographical distribution of Pseudomonas pseudomallei in China. Southeast Asian J. Trop. Med. Public Health 1995, 26, 636–638. [Google Scholar] [PubMed]
- Lu, Z.Z.; Zhang, W.D.; Mo, Z.S.; Wang, Y.X.; Fan, X.J.; Liang, J.Q.; Ouyang, X.M. Isolation of Pseudomonas pseudomallei from animals. Chin. J. Vet. Med. 1984, 2, 2–3. [Google Scholar]
- Li, L.; Lu, Z.; Han, O. Epidemiology of melioidosis in China. Chin. J. Epidemiol. 1994, 15, 292–295. [Google Scholar]
- Yang, S.; Tong, S.; Mo, C.; Jiang, Z.; Yang, S.; Ma, Y.; Lu, Z. Prevalence of human melioidosis on Hainan island in China. Microbiol. Immunol. 1998, 42, 651–654. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Xu, W.; Lu, S.; Jiang, J.; Zhou, J.; Shao, Z.; Liu, X.; Xu, L.; Xiong, Y.; Zheng, H.; et al. Landscape of emerging and re-emerging infectious diseases in China: Impact of ecology, climate, and behavior. Front. Med. 2018, 12, 3–22. [Google Scholar] [CrossRef] [PubMed]
- Lin, R.; Xie, C.; Chen, H.; Huang, Y. Clinical features and drug resistance analysis of melioidosis: 122 cases from Hainan. Guangdong Med. 2011, 32, 2303–2304. [Google Scholar]
- Wu, H.; Wang, X.; Huang, D. Laboratory culture and identification on a collection of 95 Burkholderia pseudomallei strains. Chin. J. Zoonoses 2013, 29, 730–732. [Google Scholar]
- Wang, X.M.; Zheng, X.; Wu, H.; Zhou, X.J.; Kuang, H.H.; Guo, H.L.; Xu, K.; Li, T.J.; Liu, L.L.; Li, W. Multilocus sequence typing of clinical isolates of Burkholderia pseudomallei collected in Hainan, a tropical island of southern China. Am. J. Trop. Med. Hyg. 2016, 95, 760–764. [Google Scholar] [CrossRef] [PubMed]
- Godoy, D.; Randle, G.; Simpson, A.J.; Aanensen, D.M.; Pitt, T.L.; Kinoshita, R.; Spratt, B.G. Multilocus sequence typing and evolutionary relationships among the causative agents of melioidosis and glanders, Burkholderia pseudomallei and Burkholderia mallei. J. Clin. Microbiol. 2003, 41, 2068–2079. [Google Scholar] [CrossRef] [PubMed]
- Tu, B.; Qin, E.; Zhao, M. A case of diabetes complicated with melioidosis septicemia. J. Clin. Res. 2011, 28, 2224. [Google Scholar]
- Jin, H.; Chen, X.; Pan, Y.; Zhou, C.; Gao, X.; Hu, B.; He, L. Analysis and appraisal of difficult cases: No. 76, Burkholderia pseudomallei infection with fever, cough, swelling and pain of the right knee joint and bilateral pleural effusion with left hydropneumothorax. Natl. Med. J. Chin. 2005, 85, 1287–1289. [Google Scholar] [CrossRef]
- Liu, Y.; Zhou, W.; Zhang, Z.; Si, J. One case of septicemia caused by Burkholderia pseudomallei. Lab. Med. Clin. 2016, 13, 575–576. [Google Scholar] [CrossRef]
- Fang, Y.; Chen, J.; Zhu, Y.; Mao, X. Source tracking for an imported case of melioidosis. J. Third Mil. Med. Univ. 2016, 38, 1224–1225. [Google Scholar]
- Li, Y.; Zhong, Y.; Liu, W.; Pu, Y.; Li, H.; Yan, Q.; Zou, M.; Guo, S. One death of sepsis caused by Burkholderia pseudomallei. Chin. J. Infect. Control. 2013, 12, 475–476. [Google Scholar] [CrossRef]
- Zhang, H. First imported and death case of melioidosis in Qinghai Province, China. Int. J. Lab. Med. 2015, 36, 1798–1799. [Google Scholar] [CrossRef]
- Yang, L.; Lu, J. A case of cutaneous melioidosis infection misdiagnosed as rash over 10 years. J. Third Mil. Med. Univ. 2014, 36, 552. [Google Scholar]
- Wang, Y. A case of melioidosis. J. Clin. Dermatol. 2014, 43, 163–164. [Google Scholar]
- Li, L.; Wang, C.; Liu, J.; Gu, X.; Liang, R.; Sun, H. A case of Burkholderia pseudomallei septicemia associated with periorbit abscess. Chin. J. Infect. Control. 2017, 16, 574–576. [Google Scholar] [CrossRef]
- Lin, R.; Chen, H.; Yun, W. Clinical analysis of 12 cases of melioidosis in Hainan Province, 2002–2005. Chin. J. Epidemiol. 2005, 26, 824. [Google Scholar]
- Chen, G.; Zeng, X.; Feng, X.; Liang, T.; Ke, S. Analysis of clinical feature and epidemiology investigation of melioidosis in Leizhou peninsula of Guangdong. Chin. J. Infect. Dis. 2006, 24, 406–409. [Google Scholar]
- Cai, D.; Jia, J.; Wu, T.; Su, L. Clinical analysis of 32 Pseudomonas pseudomallei pneumonia patients. Chin Trop. Med. 2006, 6, 620–621. [Google Scholar]
- Quan, H.; Fu, H.; Mo, C. Clinical analysis of 19 cases of type 2 diabetes mellitus complicated with septicemic melioidosis. Chin. J. Endocrinol. Metab. 2008, 24, 66–67. [Google Scholar] [CrossRef]
- He, X.; Jia, J. Clinical analysis of 25 cases of septicemic melioidosis. Chin. J. Modern Med. 2008, 18, 956–958. [Google Scholar]
- Cai, D.; Jia, J. Clinical features and drug resistance analysis of 104 melioidosis cases from Hainan. Chongqing Med. 2009, 38, 2362–2363. [Google Scholar]
- Zhong, Y.; Lin, H. Clinical features and follow-up of melioidosis: 40 cases in Hainan island. Chin. J. Lung Dis. 2014, 7, 55–57. [Google Scholar]
- Zhong, J.; Chen, R. Clinical analysis of 40 patients infected with Burkholderia pseudomallei in Sanya City. Chin. Trop. Med. 2014, 14, 1147–1149. [Google Scholar]
- Fang, Y.; Chen, H.; Li, Y.L.; Li, Q.; Ye, Z.J.; Mao, X.H. Melioidosis in Hainan, China: A restrospective study. Trans. R. Soc. Trop. Med. Hyg. 2015, 109, 636–642. [Google Scholar] [CrossRef] [PubMed]
- Zheng, X.; Wang, L.; Zhu, X.; Chen, H.; Wu, H.; Mai, W.; Li, W.; Xia, L. Preliminary study on incidence of melioidosis and molecular characteristics of clinical strains of Burkholderia pseudomallei after Typhoon Rammasun attack. Dis. Surveill. 2016, 31, 628–632. [Google Scholar] [CrossRef]
- Zhan, Y.; Wu, Y.; Li, Q.; Yu, A. Neuromelioidosis: A series of seven cases in Hainan province, China. J. Int. Med. Res. 2017, 45, 856–867. [Google Scholar] [CrossRef] [PubMed]
- Dong, S.; Lin, X.; Fu, S.; Wu, Q.; Xia, Q. Epidemiological features and clinical manifestations of melioidosis in 46 patients in Hainan. J. Pathog. Biol. 2017, 12, 579–582. [Google Scholar]
- Zou, W.; Li, J.; Deng, C.; Liu, L.; Li, S. Clinical features of 35 cases of melioidosis. Chin. J. Infect. Control 2018, 17, 146–150. [Google Scholar]
- Tang, Y.; Deng, J.; Zhang, J.; Zhong, X.; Qiu, Y.; Zhang, H.; Xu, H. Epidemiological and clinical features of melioidosis: A report of seven cases from southern inland China. Am. J. Trop. Med. Hyg. 2018, 985, 1296–1299. [Google Scholar] [CrossRef] [PubMed]
- Ma, G.; Zheng, D.; Cai, Q.; Yuan, Z. Prevalence of Burkholderia pseudomallei in Guangxi, China. Epidemiol. Infect. 2010, 138, 37–39. [Google Scholar] [CrossRef] [PubMed]
- One rare case of severe pneumonia caused by melioidosis infection in Putian. Sina Fujian, 27 November 2014. Available online: http://fj.sina.com.cn/news/s/2014-11-27/detail-iavxeafr5320356.shtml (accessed on 10 December 2018). (In Chinese).
- Fu, Z.; Lin, Y.; Wu, Q.; Xia, Q. Pediatric suppurative parotitis caused by Burkholderia pseudomallei. J. Venom. Anim. Toxins 2016, 22, 31. [Google Scholar] [CrossRef] [PubMed]
- Zou, W.; Jinghui, L.; Cao, Y.; Liu, F. Report of three cases of osteomyelitis caused by Burkholderia pseudomallei and literature review. Chin. J. Infect. Chemo. 2018, 18, 37–43. [Google Scholar] [CrossRef]
- Cai, X.J.; Huang, Y.J.; Fu, Y.H. A case on acute Burkholderia pseudomallei pericarditis. Chin. Med. J. 2016, 129, 2256. [Google Scholar] [CrossRef] [PubMed]
- Tan, G.; Li, J.; Chen, L.; Chen, X.; Zhang, S.; Ke, L.; Liu, J. Prostatic melioidosis rarely reported in China: Two cases report and literatures review. Int. J. Clin. Exp. Med. 2015, 8, 21830–21832. [Google Scholar] [PubMed]
- Li, X.Y.; Ke, B.X.; Chen, C.N.; Xiao, H.L.; Liu, M.Z.; Xiong, Y.C.; Bai, R.; Chen, J.D.; Ke, C.W. First co-infection case of melioidosis and Japanese encephalitis in China. BMC Infect. Dis. 2018, 18, 452. [Google Scholar] [CrossRef] [PubMed]
- Zheng, X.; Chen, H.; Zhu, X.; Cai, H.; Li, L.; Li, H.; You, X.; Ping, J.; Xia, L.; Li, W. Discovery of Burkholderia thailandensis isolated from melioidosis endemic areas of Hainan, China. Chin. J. Epidemiol. 2015, 36, 97–98. [Google Scholar]
- Lin, Y.; Wu, Q.; Liu, X.; Dong, S.; Wu, L.; Pei, H.; Xu, K.; Xia, Q. Molecular tracking investigation of melioidosis cases reveals regional endemicity in Hainan, China. Biomed. Rep. 2016, 5, 766–770. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Chen, H.; Li, H.; Li, W.; Xia, L.; Li, L.; Zheng, X.; Zhu, X. Molecular tracing investigation for one case of melioidosis in Hainan Island, China. Chin. J. Zoonoses 2018, 34, 673–676. [Google Scholar] [CrossRef]
- Dong, S.; Wu, L.; Long, F.; Wu, Q.; Liu, X.; Pei, H.; Xu, K.; Lu, Y.; Wang, Y.; Lin, Y.; et al. The prevalence and distribution of Burkholderia pseudomallei in rice paddy within Hainan, China. Acta Trop. 2018, 187, 165–168. [Google Scholar] [CrossRef] [PubMed]
- Fang, Y.; Zhu, P.; Li, Q.; Chen, H.; Li, Y.; Ren, C.; Hu, Y.; Tan, Z.; Gu, J.; Mao, X. Multilocus sequence typing of 102 Burkholderia pseudomallei strains isolated from China. Epidemiol. Infect. 2016, 144, 1917–1923. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Xia, L.; Zhu, X.; Li, W.; Du, X.; Wu, D.; Hai, R.; Shen, X.; Liang, Y.; Cai, H.; et al. Burkholderia pseudomallei sequence type 562 in China and Australia. Emerg. Infect. Dis. 2015, 21, 166–168. [Google Scholar] [CrossRef] [PubMed]
- Price, E.P.; Sarovich, D.S.; Smith, E.J.; MacHunter, B.; Harrington, G.; Theobald, V.; Hall, C.M.; Hornstra, H.M.; McRobb, E.; Podin, Y.; et al. Unprecedented melioidosis cases in northern Australia caused by an Asian Burkholderia pseudomallei strain identified by using large-scale comparative genomics. Appl. Environ. Microbiol. 2016, 82, 954–963. [Google Scholar] [CrossRef] [PubMed]
- Fang, Y.; Huang, Y.; Li, Q.; Chen, H.; Yao, Z.; Pan, J.; Gu, J.; Tang, B.; Wang, H.G.; Yu, B.; et al. First genome sequence of a Burkholderia pseudomallei isolate in China, strain BPC006, obtained from a melioidosis patient in Hainan. J. Bacteriol. 2012, 194, 6604–6605. [Google Scholar] [CrossRef] [PubMed]
- Song, L.; Yu, Y.; Feng, L.; He, J.; Wang, T.; Zhu, H.; Duan, Q. Draft genome sequence of Burkholderia pseudomallei strain 350105, isolated in Hainan, China, in 1976. Genome Announc. 2015, 3. [Google Scholar] [CrossRef] [PubMed]
- Chou, D.W.; Chung, K.M.; Chen, C.H.; Cheung, B.M. Bacteremic melioidosis in southern Taiwan: Clinical characteristics and outcome. J. Formos Med. Assoc. 2007, 106, 1013–1022. [Google Scholar] [CrossRef]
- Huang, Y.; Nie, X.; Huang, M.; Li, Y.; Chen, H.; Guo, X. Study on characteristics and epidemiology of Burkholderia pseudomallei in Zhanjiang area. Chin. Infect. Control. 2008, 7, 268–271. [Google Scholar]
- Hu, C.; Jia, W. Diabetes in China: Epidemiology and genetic risk factors and their clinical utility in personalized medication. Diabetes 2018, 67, 3–11. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.; Wu, J.; Ding, C.; Cui, Y.; Zhou, Y.; Li, Y.; Deng, M.; Wang, C.; Xu, K.; Ren, J.; et al. Epidemiological features of and changes in incidence of infectious diseases in China in the first decade after the SARS outbreak: An observational trend study. Lancet Infect. Dis. 2017, 17, 716–725. [Google Scholar] [CrossRef]
- Fan, C.; Li, Z.; Zhou, J.; Wen, W.; Chen, S.; Zhu, Y. Case report: A death of rhesus monkey caused by Burkholderia pseudomallei infection. Chin. J. Zoonoses 1994, 10, 64. [Google Scholar]
- Chen, H.; Zhu, L. Separation of Burkholderia pseudomallei from dead dolphin. Chin. J. Zoonoses 2007, 23, 1269–1270. [Google Scholar]
- Tao, L.; Peng, H.; Wei, Z.; Lan, M.; Li, J.; Qin, R.; Zhou, Y.; Chen, Z.; Yang, W. Diagnosis and treatment for Burkholderia pseudomallei infection in Boer Goats. Chin. J. Zoonoses 2011, 47, 39–40. [Google Scholar]
- Anuntagool, N.; Naigowit, P.; Petkanchanapong, V.; Aramsri, P.; Panichakul, T.; Sirisinha, S. Monoclonal antibody-based rapid identification of Burkholderia pseudomallei in blood culture fluid from patients with community-acquired septicaemia. J. Med. Microbiol. 2000, 49, 1075–1078. [Google Scholar] [CrossRef] [PubMed]
- Trinh, T.T.; Hoang, T.S.; Tran, D.A.; Trinh, V.T.; Gohler, A.; Nguyen, T.T.; Hoang, S.N.; Krumkamp, R.; Nguyen, L.T.N.; May, J.; et al. A simple laboratory algorithm for diagnosis of melioidosis in resource-constrained areas: A study from north-central Vietnam. Clin. Microbiol. Infect. 2018, 24, e81–e84. [Google Scholar] [CrossRef] [PubMed]
- Cai, D.; Jia, J.; Wu, T.; Su, L. Analysis of 15 cases of melioidosis misdiagnosed as pulmonary tuberculosis. Chin. J. Misdiagn. 2006, 6, 2135–2136. [Google Scholar]
- Lu, L.; Zhao, C.; Sun, Q. Misdiagnosis of a case of human glanders. Chin. J. Mult Organ. Dis Eld. 2004, 3, 184. [Google Scholar]
- Kai, C.; Jie, L.; Huan, X.; Min, L.; Fengling, Z.; Jin, L.; Dayong, G.; Shaoli, D.; Ming, C.; Weiping, L. Human infection with Burkholderia thailandensis, China, 2013. Emerg. Infect. Dis. 2017, 23, 1416–1418. [Google Scholar]
- Dance, D.A.B.; Sarovich, D.; Price, E.P.; Limmathurotsakul, D.; Currie, B.J. Human infection with Burkholderia thailandensis, China, 2013. Emerg. Infect. Dis. 2018, 24, 953–954. [Google Scholar] [CrossRef] [PubMed]
- Chenyang, J.; Hu, C.; Fang, Y.; Mao, X. Drug resistance spectrum of clinical Burkholderia pseudomallei strains in China and related mechanism. J. Third Mil. Med. Univ. 2016, 38, 1220–1223. [Google Scholar] [CrossRef]
- Hinjoy, S.; Hantrakun, V.; Kongyu, S.; Kaewrakmuk, J.; Wangrangsimakul, T.; Jitsuronk, S.; Saengchun, W.; Bhengsri, S.; Akarachotpong, T.; Thamthitiwat, S.; et al. Melioidosis in Thailand: Present and future. Trop. Med. Infect. Dis. 2018, 3, 38. [Google Scholar] [CrossRef] [PubMed]
- Trinh, T.T.; Nguyen, L.D.N.; Nguyen, T.V.; Tran, C.X.; Le, A.V.; Nguyen, H.V.; Assig, K.; Lichtenegger, S.; Wagner, G.E.; Do, C.D.; et al. Melioidosis in Vietnam: Recently improved recognition but still an uncertain disease burden after almost a century of reporting. Trop. Med. Infect. Dis. 2018, 3, 39. [Google Scholar] [CrossRef] [PubMed]
| Presentation | Number of Cases | Percentage (%) |
|---|---|---|
| Septicaemia | 153 | 55.2 |
| Pneumonia | 149 | 53.8 |
| Musculoskeletal or soft tissue abscess | 57 | 20.6 |
| Genitourinary or prostatic infection | 18 | 6.5 |
| Brain infection | 9 | 3.3 |
| Internal organ (liver, kidney or splenic) abscess | 8 | 2.9 |
| Pyogenic arthritis | 5 | 1.8 |
| Upper gastrointestinal hemorrhage | 4 | 1.4 |
| Neck abscess | 4 | 1.4 |
| Suppurative parotitis | 3 | 1.1 |
| Infected aortic aneurysm | 3 | 1.1 |
| Orbital abscess | 3 | 1.1 |
| Suppurative pharyngitis | 3 | 1.1 |
| Year of Report | Location of Infection | Duration of Study | Number of Cases 1 | Outcome | Reference |
|---|---|---|---|---|---|
| 1992 | Hainan & Guangdong | 1975–1992 | 3 | 1 Survived/2 Died | [8] |
| 1998 | Hainan | 1995–1996 | 8 | 4 Survived/2 Died/2 Unknown | [12] |
| 2005 | Hainan | 2002–2005 | 12 | 4 Survived/8 Died | [27] |
| 2006 | Guangdong | 1990–2005 | 44 | 19 Survived/25 Died | [28] |
| 2006 | Hainan | 1996–2005 | 32 | 21 Survived/3 Died/9 treatment withdrawn | [29] |
| 2008 | Hainan | 2002–2006 | 19 | 12 Survived/7 Died | [30] |
| 2008 | Hainan | 2000–2007 | 25 | 9 Survived/6 Died/10 treatment withdrawn | [31] |
| 2009 | Hainan | 2000–2009 | 104 | 72 Survived/15 Died/17 treatment withdrawn | [32] |
| 2011 | Hainan | 2002–2008 | 122 | 81 Survived/19 Died/22 treatment withdrawn | [14] |
| 2013 | Hainan | 2007–2012 | 95 | 65 Survived/30 Died | [15] |
| 2014 | Hainan | 2009–2012 | 40 | 34 Survived/6 Died | [33] |
| 2014 | Hainan | 2010–2013 | 40 | 6 Survived /10 Died/24 Unknown | [34] |
| 2015 | Hainan | 2002–2014 | 170 | 124 Survived/46 Died | [35] |
| 2016 | Hainan | 2003–2014 | 60 | 32 Survived/26 Died/2 Unknown | [16] |
| 2016 | Hainan | Jul–Sep 2014 | 16 | 8 Survived/8 Died | [36] |
| 2017 | Hainan | 2002–2015 | 7 | 5 Survived (4 had nervous system sequelae) /1 Died/1 treatment withdrawn | [37] |
| 2017 | Hainan | 2000–2012 | 46 | 33 Survived/13 Died | [38] |
| 2018 | Hainan | 2012–2017 | 35 | 26 Survived/7 Died/2 treatment withdrawn | [39] |
| 2018 | Guangxi | 2006–2015 | 7 | All Survived | [40] |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zheng, X.; Xia, Q.; Xia, L.; Li, W. Endemic Melioidosis in Southern China: Past and Present. Trop. Med. Infect. Dis. 2019, 4, 39. https://doi.org/10.3390/tropicalmed4010039
Zheng X, Xia Q, Xia L, Li W. Endemic Melioidosis in Southern China: Past and Present. Tropical Medicine and Infectious Disease. 2019; 4(1):39. https://doi.org/10.3390/tropicalmed4010039
Chicago/Turabian StyleZheng, Xiao, Qianfeng Xia, Lianxu Xia, and Wei Li. 2019. "Endemic Melioidosis in Southern China: Past and Present" Tropical Medicine and Infectious Disease 4, no. 1: 39. https://doi.org/10.3390/tropicalmed4010039
APA StyleZheng, X., Xia, Q., Xia, L., & Li, W. (2019). Endemic Melioidosis in Southern China: Past and Present. Tropical Medicine and Infectious Disease, 4(1), 39. https://doi.org/10.3390/tropicalmed4010039




