Burden of Acute Respiratory Infections Among Under-Five Children in Relation to Household Wealth and Socioeconomic Status in Bangladesh
Abstract
1. Introduction
2. Methods
2.1. Data Sources
2.2. Measures
2.3. Data Analysis
3. Results
3.1. Sample Characteristics
3.2. Multivariable Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| ARIs | Acute Respiratory Infections |
| BDHS | Bangladesh Demographic and Health Survey |
| WASH | Water, sanitation and hygiene facilities |
Appendix A
| Fever (N = 30,731) | p-value | Dyspnoea (N = 11,354) | p-value | ||||
| No | Yes | No | Yes | ||||
| Maternal Indicators | |||||||
| Age | |||||||
| 15–19 | 15.2 | 15.5 (14.9–16.2) | 16.6 (15.9–17.4) | <0.001 | 16.9 (15.9–18.0) | 18.8 (17.6–20.1) | <0.001 |
| 20–24 | 32.5 | 32.0 (31.1–32.8) | 33.5 (32.5–34.6) | 33.8 (32.5–35.2) | 33.3 (31.7–34.8) | ||
| 25–29 | 27.0 | 27.2 (26.5–27.9) | 25.9 (24.9–26.8) | 26.0 (24.8–27.3) | 24.9 (23.4–26.4) | ||
| 30–34 | 25.3 | 25.3 (24.6–26.1) | 24.0 (23.1–24.9) | 23.2 (22.0–24.4) | 23.0 (21.8–24.4) | ||
| Residency | |||||||
| Urban | 29.2 | 21.2 (19.9–22.5) | 19.7 (18.3–21.2) | <0.001 | 21.1 (19.5–22.8) | 19.1 (17.5–20.8) | <0.001 |
| Rural | 70.8 | 78.8 (77.5–80.1) | 80.3 (78.8–81.7) | 78.9 (77.2–80.5) | 80.9 (79.2–82.5) | ||
| Region | |||||||
| Barisal | 11.4 | 6.1 (5.3–6.9) | 6.3 (5.5–7.2) | <0.001 | 6.1 (5.2–7.1) | 6.6 (5.5–7.8) | <0.001 |
| Chittagong | 17.9 | 19.8 (18.2–21.5) | 23.3 (21.4–25.4) | 22.7 (20.6–24.9) | 24.7 (22.4–27.1) | ||
| Dhaka | 20.6 | 33.4 (31.3–35.5) | 30.0 (27.8–32.4) | 30.8 (28.5–33.1) | 28.5 (26.1–31.1) | ||
| Khulna | 12.3 | 11.1 (10.0–12.3) | 8.6 (7.6–9.6) | 9.7 (8.6–11.0) | 9.6 (8.3–10.9) | ||
| Rajshahi | 18.7 | 18.2 (16.6–19.9) | 19.5 (17.7–21.4) | 19.7 (17.7–21.8) | 18.4 (16.4–20.6) | ||
| Rangpur | 13.2 | 8.5 (7.6–9.5) | 8.6 (7.6–9.7) | 8.1 (6.9–9.6) | 8.7 (7.5–10.0) | ||
| Sylhet | 6.0 | 3.1 (2.6–3.6) | 3.7 (3.0–4.6) | 2.9 (2.3–3.8) | 3.6 (2.8–4.6) | ||
| Literacy Level | |||||||
| No Education | 29.1 | 30.6 (29.5–31.8) | 30.3 (29.1–31.6) | <0.001 | 30.0 (28.5–31.5) | 31.9 (30.2–33.6) | <0.001 |
| Primary | 29.2 | 28.5 (27.6–29.3) | 29.9 (28.8–31.0) | 28.4 (27.1–29.7) | 32.3 (30.6–33.9) | ||
| Secondary | 34.0 | 33.6 (32.6–34.7) | 34.4 (33.1–35.7) | 35.1 (33.5–36.6) | 31.3 (29.7–33.0) | ||
| Higher | 7.7 | 7.3 (6.8–7.8) | 5.4 (4.9–5.9) | 6.6 (5.9–7.3) | 4.6 (3.9–5.3) | ||
| Religion | |||||||
| Islam | 90.0 | 90.4 (89.4–91.3) | 92.0 (91.0–93.0) | 0.021 | 91.4 (90.2–92.4) | 91.0 (89.6–92.2) | 0.014 |
| Other | 10.0 | 9.6 (8.7–10.6) | 8.0 (7.0–9.0) | 8.6 (7.6–9.8) | 9.0 (7.8–10.4) | ||
| Sanitation | |||||||
| Unimproved | 45.6 | 47.9 (46.6–49.2) | 49.3 (47.7–50.8) | 47.8 (46.0–49.6) | 51.6 (49.6–53.6) | ||
| Improved | 54.4 | 52.1 (50.8–53.4) | 50.7 (49.2–52.3) | 52.2 (50.4–54.0) | 48.4 (46.4–50.4) | ||
| Water | |||||||
| Unimproved | 6.8 | 7.0 (6.5–7.6) | 6.4 (5.7–7.1) | <0.001 | 6.3 (5.5–7.1) | 6.6 (5.5–7.3) | <0.001 |
| Improved | 93.2 | 93.0 (92.4–93.5) | 93.6 (92.9–94.3) | 93.7 (92.9–94.5) | 93.4 (92.2–95.8) | ||
| Cooking Fuel | |||||||
| Unclean | 89.0 | 88.0 (86.6–89.2) | 90.9 (89.6–92.0) | 88.8 (87.1–90.3) | 92.5 (91.1–93.6) | ||
| Clean | 11.0 | 12.0 (10.8–13.4) | 9.1 (8.0–10.4) | 11.2 (9.7–12.9) | 7.5 (6.4–8.9) | ||
| Wealth Quintile | |||||||
| Poorest | 20.0 | 20.3 (19.3–21.4) | 23.1 (21.9–24.4) | <0.001 | 20.9 (19.6–22.3) | 25.7 (24.0–27.5) | <0.001 |
| Poorer | 20.0 | 20.5 (19.7–21.3) | 20.6 (19.6–21.7) | 19.6 (18.4–20.9) | 22.1 (20.6–23.6) | ||
| Middle | 18.8 | 18.5 (17.8–19.3) | 19.8 (18.6–21.0) | 19.1 (17.8–20.5) | 19.3 (18.0–20.7) | ||
| Richer | 19.4 | 19.6 (18.8–20.5) | 19.0 (18.0–20.0) | 19.7 (18.5–21.0) | 17.5 (16.2–18.9) | ||
| Richest | 21.8 | 21.1 (19.9–22.2) | 17.5 (16.3–18.7) | 20.7 (19.2–22.3) | 15.4 (14.2–16.8) | ||
| Employment | |||||||
| Unemployed | 75.8 | 75.3 (74.0–76.6) | 75.1 (73.6–76.6) | 0.021 | 74.8 (73.0–76.6) | 76.9 (74.9–78.8) | 0.017 |
| Employed | 24.2 | 24.7 (23.4–26.0) | 24.9 (23.4–26.4) | 25.2 (23.4–27.0) | 23.1 (21.2–25.1) | ||
| Parity | |||||||
| 2 | 59.0 | 59.4 (58.4–60.4) | 58.1 (57.0–59.3) | 0.041 | 59.4 (57.9–60.9) | 57.9 (56.3–59.5) | 0.018 |
| 4 | 27.6 | 27.1 (26.4–27.9) | 28.5 (27.5–29.4) | 28.4 (27.2–29.7) | 27.6 (26.3–29.0) | ||
| 5 | 13.3 | 13.5 (12.8–14.2) | 13.4 (12.6–14.3) | 12.2 (11.2–13.2) | 14.5 (13.3–15.8) | ||
| Age of Child | |||||||
| 0–11 | 24.3 | 23.0 (22.3–23.7) | 27.3 (26.3–28.4) | <0.001 | 25.6 (24.4–26.9) | 32.0 (30.4–33.7) | 0.024 |
| 12–23 | 21.0 | 20.3 (19.5–21.1) | 23.4 (22.4–24.4) | 22.4 (21.1–23.7) | 23.5 (22.0–25.0) | ||
| 24–35 | 20.9 | 20.5 (19.8–21.2) | 19.7 (18.9–20.6) | 20.3 (19.1–21.5) | 18.7 (17.5–20.0) | ||
| 36–47 | 18.9 | 19.8 (19.1–20.5) | 16.5 (15.6–17.4) | 17.7 (16.6–18.9) | 14.4 (13.2–15.6) | ||
| 48–59 | 14.9 | 16.5 (15.8–17.2) | 13.0 (12.0–14.0) | 14.0 (12.7–15.4) | 11.4 (10.4–12.6) | ||
| Child’s Sex | |||||||
| Male | 50.9 | 51.1 (50.3–52.0) | 51.6 (50.5–52.6) | 0.128 | 51.3 (49.9–52.7) | 52.7 (51.0–54.3) | 0.191 |
| Female | 49.1 | 48.9 (48.0–49.7) | 48.4 (47.4–49.5) | 48.7 (47.3–50.1) | 47.3 (45.7–49.0) | ||
| Multicollinearity Test for Outcome 1 (Fever): | |
| Variable | VIF |
| Water | 8.91 |
| Parity | 8.23 |
| Age | 7.66 |
| Residency | 7.44 |
| Wealth | 6.96 |
| Child’s Sex | 5.69 |
| Region | 4.77 |
| Education | 4.43 |
| Sanitation | 3.80 |
| Fuel | 1.55 |
| Occupation | 1.34 |
| Religion | 1.13 |
| Multicollinearity test for outcome 2 (dyspnoea): | |
| Variable | VIF |
| Water | 8.46 |
| Parity | 7.16 |
| Age | 5.31 |
| Residency | 5.14 |
| Wealth | 4.96 |
| Child’s Sex | 4.12 |
| Region | 3.17 |
| Education | 3.23 |
| Sanitation | 2.17 |
| Fuel | 1.55 |
| Occupation | 1.32 |
| Religion | 1.13 |
References
- WB: Bangladesh Has 8th Highest Number of Poor People. Available online: https://www.dhakatribune.com/business/2016/10/04/wb-bangladesh-8th-highest-number-poor-people (accessed on 1 December 2018).
- Top 10 Disturbing Facts about Poverty in Bangladesh. Available online: https://borgenproject.org/10-facts-about-poverty-in-bangladesh/ (accessed on 1 December 2018).
- Koblinsky, M.; Anwar, I.; Mridha, M.K.; Chowdhury, M.E.; Botlero, R. Reducing Maternal Mortality and Improving Maternal Health: Bangladesh and MDG 5. J. Health Popul. Nutr. 2008, 26, 280–294. [Google Scholar] [CrossRef] [PubMed]
- Jolly, S.P.; Rahman, M.; Afsana, K.; Yunus, F.M.; Chowdhury, A.M.R. Evaluation of Maternal Health Service Indicators in Urban Slum of Bangladesh. PLoS ONE 2016, 11, e0162825. [Google Scholar] [CrossRef] [PubMed]
- Ruhul, A.M.; Fukuda, H.; Nakajima, K.; Takatorige, T.; Tatara, K. Public health services in Bangladesh with special reference to systems and trends of vital statistics. Environ. Health Prev. Med. 1999, 4, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Cockcroft, A.; Milne, D.; Oelofsen, M.; Karim, E.; Andersson, N. Health services reform in Bangladesh: Hearing the views of health workers and their professional bodies. BMC Health Serv. Res. 2011, 11, S8. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, S.; Hasan, M.Z.; Ahmed, M.W.; Dorin, F.; Sultana, M.; Islam, Z.; Mirelman, A.J.; Rehnberg, C.; Khan, J.A.M.; Chowdhury, M.E. Evaluating the implementation related challenges of Shasthyo Suroksha Karmasuchi (health protection scheme) of the government of Bangladesh: A study protocol. BMC Health Serv. Res. 2018, 18, 552. [Google Scholar] [CrossRef] [PubMed]
- Molla, A.A.; Chi, C. Who pays for healthcare in Bangladesh? An analysis of progressivity in health systems financing. Int. J. Equity Health 2017, 16, 167. [Google Scholar] [CrossRef] [PubMed]
- 33 Million Children in Bangladesh Live in Poverty. Available online: https://www.unicef.org/media/media_51925.html (accessed on 1 December 2018).
- Bouzid, M.; Cumming, O.; Hunter, P.R. What is the impact of water sanitation and hygiene in healthcare facilities on care seeking behaviour and patient satisfaction? A systematic review of the evidence from low-income and middle-income countries. BMJ Glob. Health 2018, 3, e000648. [Google Scholar] [CrossRef]
- Chard, A.N.; Trinies, V.; Moss, D.M.; Chang, H.H.; Doumbia, S.; Lammie, P.J.; Freeman, M.C. The impact of school water, sanitation, and hygiene improvements on infectious disease using serum antibody detection. PLoS Negl. Trop. Dis. 2018, 12, e0006418. [Google Scholar] [CrossRef]
- Dreibelbis, R.; Freeman, M.C.; Greene, L.E.; Saboori, S.; Rheingans, R. The Impact of School Water, Sanitation, and Hygiene Interventions on the Health of Younger Siblings of Pupils: A Cluster-Randomized Trial in Kenya. Am. J. Public Health 2014, 104, e91–e97. [Google Scholar] [CrossRef]
- Hutton, G. Global costs and benefits of reaching universal coverage of sanitation and drinking-water supply. J. Water Health 2013, 11, 1–12. [Google Scholar] [CrossRef]
- Water in Crisis—Spotlight Nepal. Available online: https://thewaterproject.org/water-crisis/water-in-crisis-nepal (accessed on 20 February 2018).
- Rahman, M.; Ashraf, S.; Unicomb, L.; Mainuddin, A.K.M.; Parvez, S.M.; Begum, F.; Das, K.K.; Naser, A.M.; Hussain, F.; Clasen, T.; et al. WASH Benefits Bangladesh trial: System for monitoring coverage and quality in an efficacy trial. Trials 2018, 19, 360. [Google Scholar] [CrossRef] [PubMed]
- Lin, A.; Ercumen, A.; Benjamin-Chung, J.; Arnold, B.F.; Das, S.; Haque, R.; Ashraf, S.; Parvez, S.M.; Unicomb, L.; Rahman, M.; et al. Effects of Water, Sanitation, Handwashing, and Nutritional Interventions on Child Enteric Protozoan Infections in Rural Bangladesh: A Cluster-Randomized Controlled Trial. Clin. Infect. Dis. 2018, 67, 1515–1522. [Google Scholar] [CrossRef] [PubMed]
- Raihan, M.J.; Farzana, F.D.; Sultana, S.; Haque, M.A.; Rahman, A.S.; Waid, J.L.; McCormick, B.; Choudhury, N.; Ahmed, T. Examining the relationship between socio-economic status, WASH practices and wasting. PLoS ONE 2017, 12, e0172134. [Google Scholar] [CrossRef] [PubMed]
- WHO, Bangladesh—Sustainable Development & Healthy Environment. Available online: http://www.whoban.org/sust_dev_mental_env.html (accessed on 1 December 2018).
- Simoes, E.A.F.; Cherian, T.; Chow, J.; Shahid-Salles, S.A.; Laxminarayan, R.; John, T.J. Acute Respiratory Infections in Children. In Disease Control Priorities in Developing Countries; Jamison, D.T., Breman, J.G., Measham, A.R., Alleyne, G., Claeson, M., Evans, D.B., Jha, P., Mills, A., Musgrove, P., Eds.; World Bank: Washington, DC, USA, 2006; ISBN 978-0-8213-6179-5. [Google Scholar]
- Liu, W.K.; Liu, Q.; Chen, D.H.; Liang, H.X.; Chen, X.K.; Chen, M.X.; Qiu, S.Y.; Yang, Z.Y.; Zhou, R. Epidemiology of Acute Respiratory Infections in Children in Guangzhou: A Three-Year Study. PLoS ONE 2014, 9, e96674. [Google Scholar] [CrossRef] [PubMed]
- Cutrera, R.; Baraldi, E.; Indinnimeo, L.; Miraglia Del Giudice, M.; Piacentini, G.; Scaglione, F.; Ullmann, N.; Moschino, L.; Galdo, F.; Duse, M. Management of acute respiratory diseases in the pediatric population: The role of oral corticosteroids. Ital. J. Pediatr. 2017, 43, 31. [Google Scholar] [CrossRef] [PubMed]
- Harerimana, J.-M.; Nyirazinyoye, L.; Thomson, D.R.; Ntaganira, J. Social, economic and environmental risk factors for acute lower respiratory infections among children under five years of age in Rwanda. Arch. Public Health 2016, 74, 19. [Google Scholar] [CrossRef] [PubMed]
- Selvaraj, K.; Chinnakali, P.; Majumdar, A.; Krishnan, I.S. Acute respiratory infections among under-5 children in India: A situational analysis. J. Nat. Sci. Biol. Med. 2014, 5, 15–20. [Google Scholar] [CrossRef] [PubMed]
- Nandasena, S.; Wickremasinghe, A.R.; Sathiakumar, N. Indoor air pollution and respiratory health of children in the developing world. World J. Clin. Pediatr. 2013, 2, 6–15. [Google Scholar] [CrossRef]
- Akinyemi, J.O.; Morakinyo, O.M. Household environment and symptoms of childhood acute respiratory tract infections in Nigeria, 2003–2013: A decade of progress and stagnation. BMC Infect. Dis. 2018, 18, 296. [Google Scholar] [CrossRef]
- Humans, I.W.G. on the E. of C.R. Exposure Data; International Agency for Research on Cancer: Lyon, France, 2010. [Google Scholar]
- Salje, H.; Gurley, E.S.; Homaira, N.; Ram, P.K.; Haque, R.; Petri, W.; Moss, W.J.; Luby, S.P.; Breysse, P.; Azziz-Baumgartner, E. Impact of neighborhood biomass cooking patterns on episodic high indoor particulate matter concentrations in clean fuel homes in Dhaka, Bangladesh. Indoor Air 2014, 24, 213–220. [Google Scholar] [CrossRef]
- Tanchangya, J.; Geater, A.F. Use of traditional cooking fuels and the risk of young adult cataract in rural Bangladesh: A hospital-based case-control study. BMC Ophthalmol. 2011, 11, 16. [Google Scholar] [CrossRef] [PubMed]
- North, C.M.; Valeri, L.; Hunt, P.W.; Mocello, A.R.; Martin, J.N.; Boum, Y.; Haberer, J.E.; Bangsberg, D.R.; Christiani, D.C.; Siedner, M.J. Cooking fuel and respiratory symptoms among people living with HIV in rural Uganda. ERJ Open Res. 2017, 3, 00094-2016. [Google Scholar] [CrossRef] [PubMed]
- Kilabuko, J.H.; Nakai, S. Effects of Cooking Fuels on Acute Respiratory Infections in Children in Tanzania. Int. J. Environ. Res. Public Health 2007, 4, 283–288. [Google Scholar] [CrossRef] [PubMed]
- Ghose, B.; Feng, D.; Tang, S.; Yaya, S.; He, Z.; Udenigwe, O.; Ghosh, S.; Feng, Z. Women’s decision-making autonomy and utilisation of maternal healthcare services: Results from the Bangladesh Demographic and Health Survey. BMJ Open 2017, 7, e017142. [Google Scholar] [CrossRef] [PubMed]
- National Institute of Population Research and Training, Mitra and Associates; ORC Macro. Bangladesh Demographic and Health Survey 2014; ORC Macro: Dhaka, Bangladesh, 2014.
- Nasreen, S.; Luby, S.P.; Brooks, W.A.; Homaira, N.; Mamun, A.A.; Bhuiyan, M.U.; Rahman, M.; Ahmed, D.; Abedin, J.; Rahman, M.; et al. Population-Based Incidence of Severe Acute Respiratory Virus Infections among Children Aged <5 Years in Rural Bangladesh, June–October 2010. PLoS ONE 2014, 9, e89978. [Google Scholar] [CrossRef] [PubMed]
- Chowdhury, A.H.; Hanifi, S.M.A.; Mia, M.N.; Bhuiya, A. Socioeconomic inequalities in under-five mortality in rural Bangladesh: Evidence from seven national surveys spreading over 20 years. Int. J. Equity Health 2017, 16, 197. [Google Scholar] [CrossRef] [PubMed]
- Bishwajit, G. Household wealth status and overweight and obesity among adult women in Bangladesh and Nepal. Obes. Sci. Pract. 2017, 3, 185–192. [Google Scholar] [CrossRef] [PubMed]
- Giashuddin, S.M.; Rahman, A.; Rahman, F.; Mashreky, S.R.; Chowdhury, S.M.; Linnan, M.; Shafinaz, S. Socioeconomic inequality in child injury in Bangladesh—Implication for developing countries. Int. J. Equity Health 2009, 8, 7. [Google Scholar] [CrossRef] [PubMed]
- Rahman, M.M.; Shahidullah, M. Risk factors for acute respiratory infections among the slum infants of Dhaka city. Bangladesh Med. Res. Counc. Bull. 2001, 27, 55–62. [Google Scholar] [PubMed]
- Kumar, S.G.; Majumdar, A.; Kumar, V.; Naik, B.N.; Selvaraj, K.; Balajee, K. Prevalence of acute respiratory infection among under-five children in urban and rural areas of puducherry, India. J. Nat. Sci. Biol. Med. 2015, 6, 3–6. [Google Scholar] [CrossRef]
- Holloway, K.A.; Karkee, S.B.; Tamang, A.; Gurung, Y.B.; Kafle, K.K.; Pradhan, R.; Reeves, B.C. Community intervention to promote rational treatment of acute respiratory infection in rural Nepal. Trop. Med. Int. Health 2009, 14, 101–110. [Google Scholar] [CrossRef] [PubMed]
- Khan, T.A.; Madni, S.A.; Zaidi, A.K.M. Acute respiratory infections in Pakistan: Have we made any progress? J. Coll. Phys. Surg. Pak. 2004, 14, 440–448. [Google Scholar]
- Chowdhury, F.; Sturm-Ramirez, K.; Mamun, A.A.; Iuliano, A.D.; Bhuiyan, M.U.; Chisti, M.J.; Ahmed, M.; Haider, S.; Rahman, M.; Azziz-Baumgartner, E. Factors driving customers to seek health care from pharmacies for acute respiratory illness and treatment recommendations from drug sellers in Dhaka city, Bangladesh. Patient Prefer. Adher. 2017, 11, 479–486. [Google Scholar] [CrossRef] [PubMed]
- Halder, A.K.; Luby, S.P.; Akhter, S.; Ghosh, P.K.; Johnston, R.B.; Unicomb, L. Incidences and Costs of Illness for Diarrhea and Acute Respiratory Infections for Children <5 Years of Age in Rural Bangladesh. Am. J. Trop. Med. Hyg. 2017, 96, 953–960. [Google Scholar] [PubMed]
- Gupta, R.P.-S.; de Wit, M.L.; McKeown, D. The impact of poverty on the current and future health status of children. Paediatr. Child Health 2007, 12, 667–672. [Google Scholar] [CrossRef] [PubMed]
- Yaya, S.; Hudani, A.; Udenigwe, O.; Shah, V.; Ekholuenetale, M.; Bishwajit, G. Improving Water, Sanitation and Hygiene Practices, and Housing Quality to Prevent Diarrhea among Under-Five Children in Nigeria. Trop. Med. Infect. Dis. 2018, 3, 41. [Google Scholar] [CrossRef] [PubMed]
- Onozuka, D.; Chaves, L.F. Climate Variability and Nonstationary Dynamics of Mycoplasma pneumoniae Pneumonia in Japan. PLoS ONE 2014, 9, e95447. [Google Scholar] [CrossRef] [PubMed]
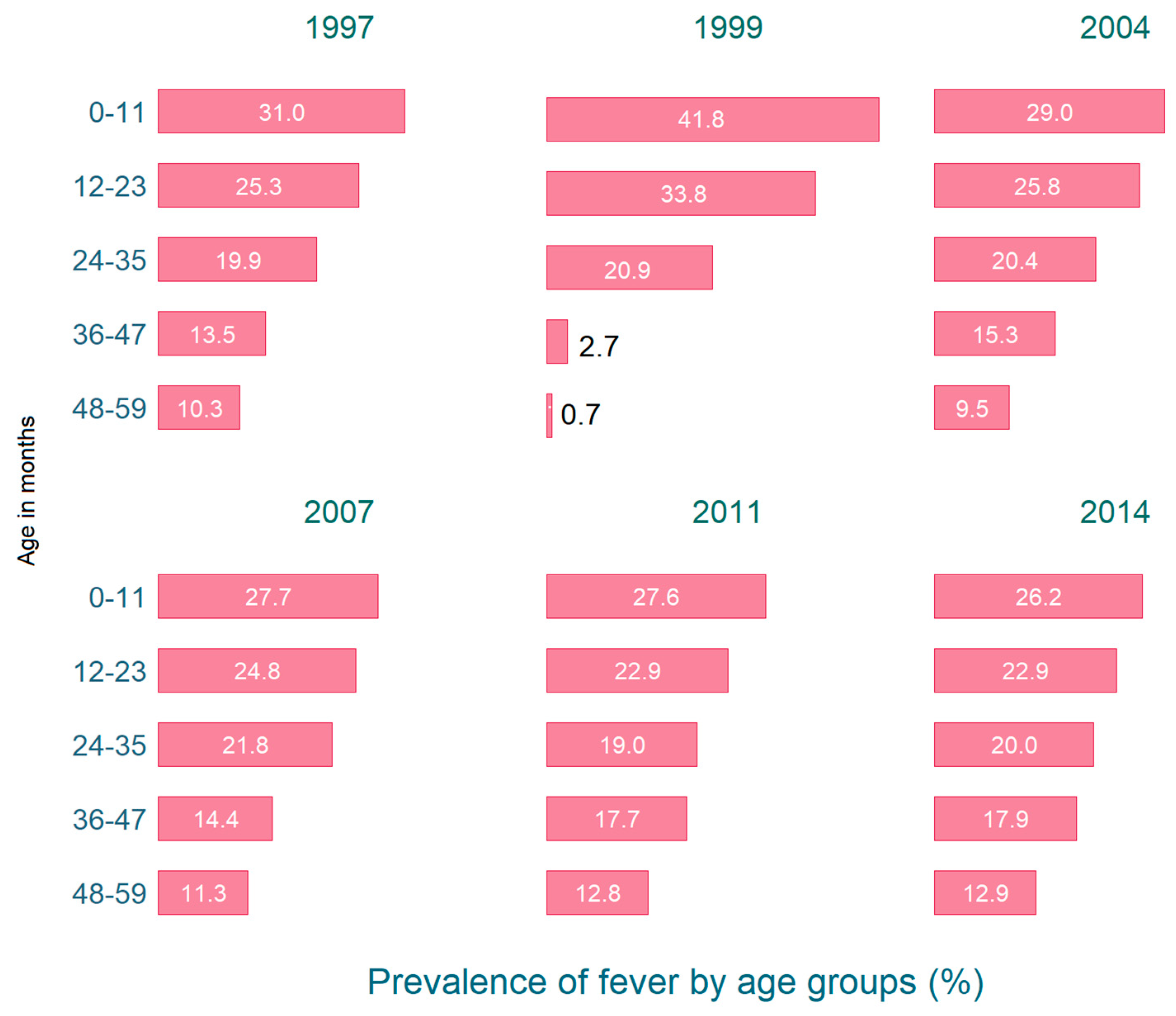
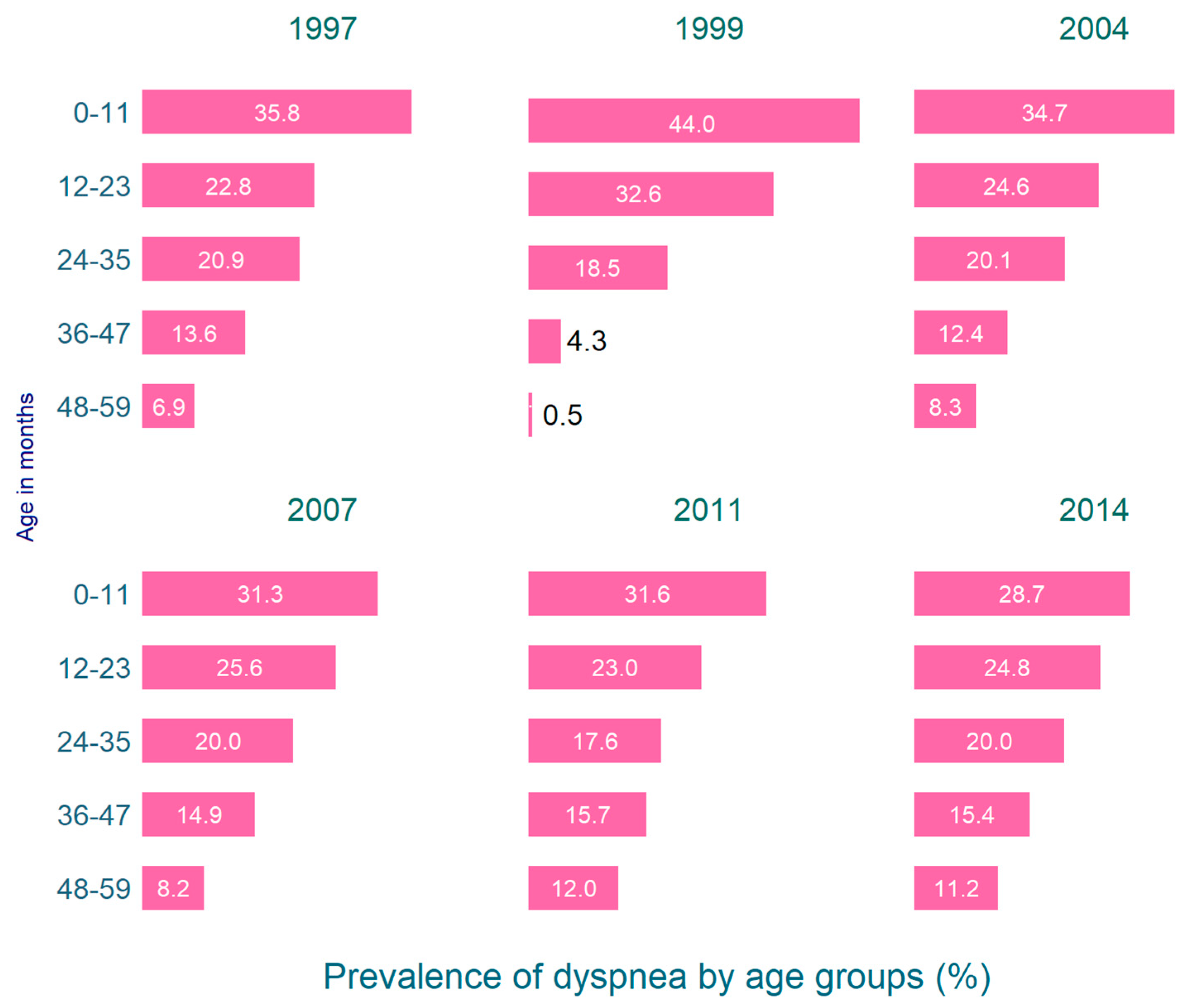
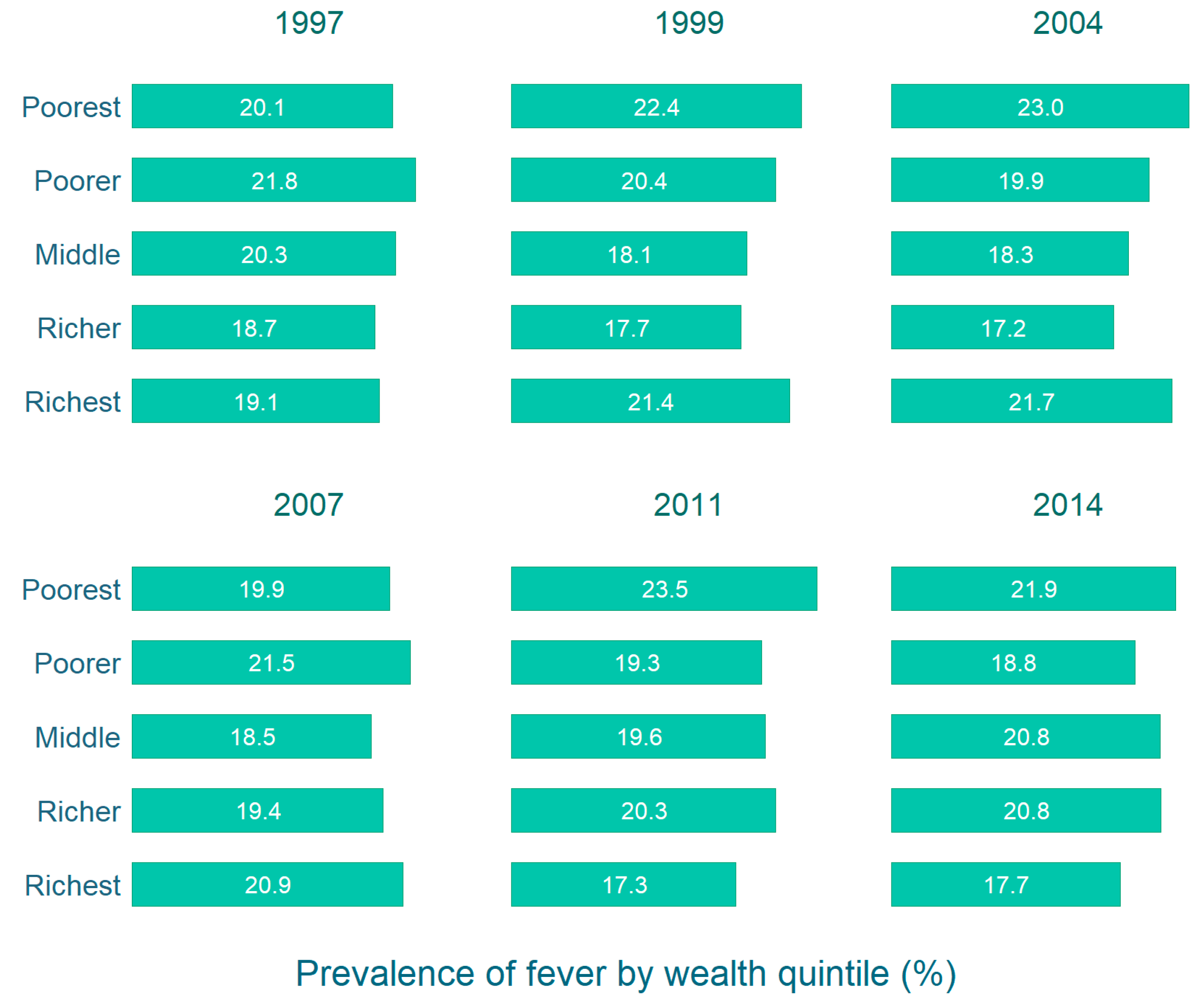
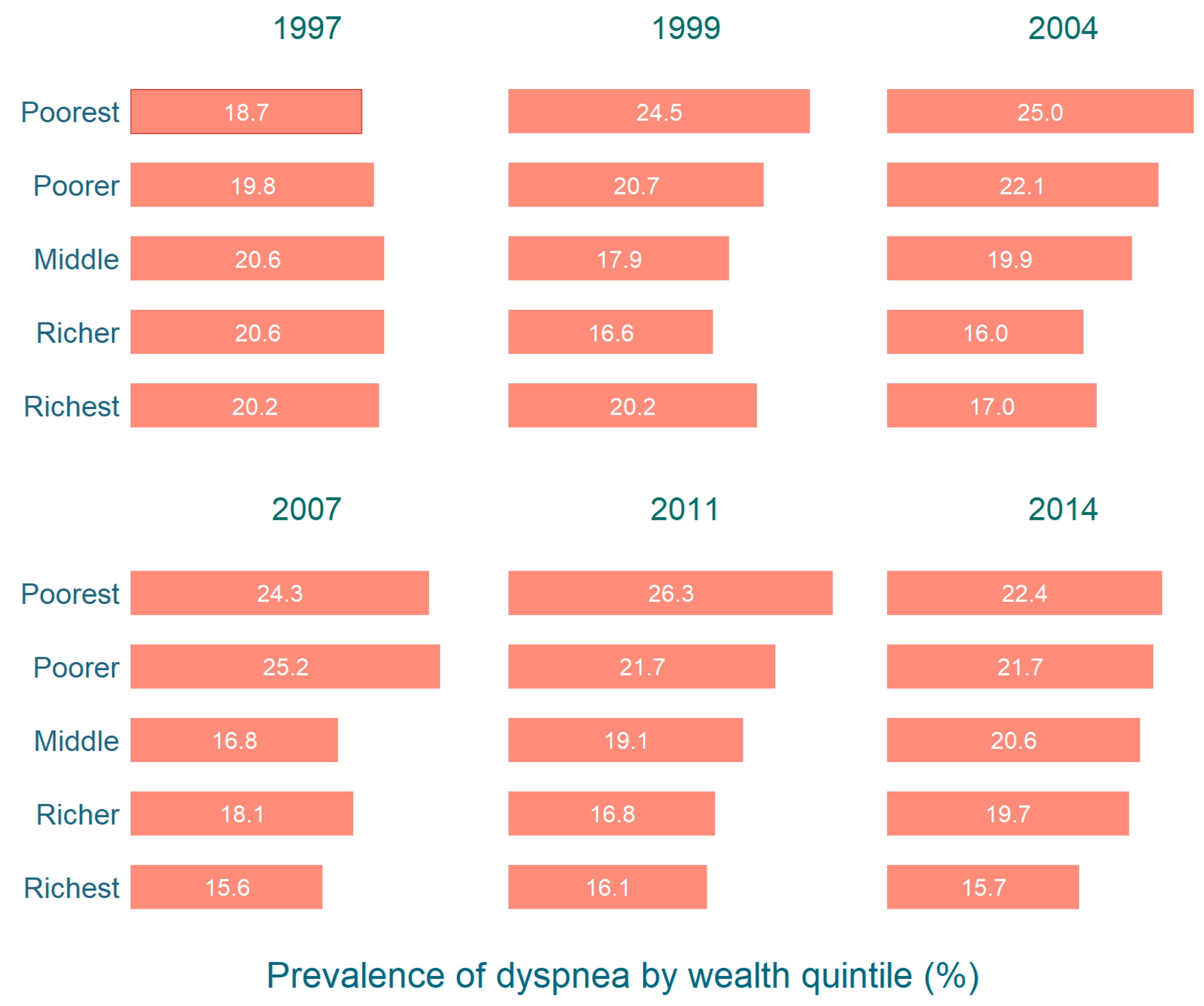
| Overall | Male | Female | |
|---|---|---|---|
| Age (15–19) | 1 | 1 | 1 |
| 20–24 | 1.041 | 0.932 | 1.166 |
| (0.923, 1.175) | (0.786, 1.105) | (0.981, 1.386) | |
| 25–29 | 0.945 | 0.886 | 1.019 |
| (0.831, 1.075) | (0.738, 1.064) | (0.849, 1.223) | |
| 30+ | 0.987 | 0.910 | 1.076 |
| (0.862, 1.131) | (0.750, 1.104) | (0.889, 1.303) | |
| Residency (Urban) | 1 | 1 | 1 |
| Rural | 0.889 * | 0.877 | 0.899 |
| (0.807, 0.980) | (0.765, 1.006) | (0.782, 1.032) | |
| Region (Barisal) | 1 | 1 | 1 |
| Chittagong | 1.133 | 1.458 *** | 0.895 |
| (0.980, 1.310) | (1.186, 1.794) | (0.728, 1.100) | |
| Dhaka | 0.965 | 1.161 | 0.813 |
| (0.831, 1.120) | (0.939, 1.436) | (0.658, 1.004) | |
| Khulna | 0.850 * | 0.958 | 0.765 * |
| (0.723, 0.999) | (0.759, 1.208) | (0.610, 0.960) | |
| Rajshahi | 1.163 * | 1.391 ** | 0.994 |
| (1.001, 1.352) | (1.123, 1.722) | (0.803, 1.230) | |
| Rangpur | 1.011 | 1.332 * | 0.766 * |
| (0.862, 1.185) | (1.063, 1.668) | (0.609, 0.963) | |
| Sylhet | 1.133 | 1.512 ** | 0.850 |
| (0.950, 1.352) | (1.179, 1.938) | (0.660, 1.095) | |
| Education (None) | 1 | 1 | 1 |
| Primary | 1.031 | 0.999 | 1.078 |
| (0.922, 1.153) | (0.855, 1.167) | (0.917, 1.269) | |
| Secondary | 1.013 | 0.907 | 1.144 |
| (0.902, 1.138) | (0.772, 1.066) | (0.967, 1.353) | |
| Higher | 0.809 * | 0.767 * | 0.853 |
| (0.679, 0.963) | (0.601, 0.979) | (0.664, 1.096) | |
| Religion (Islam) | 1 | 1 | 1 |
| Others | 0.894 | 0.773 | 0.960 |
| (0.689, 1.216) | (0.552, 1.121) | (0.781, 1.181) | |
| Sanitation (Unimproved) | 1 | 1 | 1 |
| Improved | 0.738 ** | 0.977 | 0.900 |
| (0.652, 0.932) | (0.854, 1.116) | (0.784, 1.032) | |
| Water (Unimproved) | 1 | 1 | 1 |
| Improved | 0.856 ** | 1.035 | 0.982 |
| (0.659, 0.988) | (0.975, 1.565) | (0.702, 1.639) | |
| Fuel (Unclean) | 1 | 1 | 1 |
| Clean | 0.830 ** | 0.817 | 0.938 |
| (0.593, 0.991) | (0.631, 1.150) | (0.749, 1.176) | |
| Employed (Yes) | 1 | 1 | 1 |
| No | 1.117 * | 1.231 ** | 1.002 |
| (1.016, 1.227) | (1.078, 1.405) | (0.874, 1.148) | |
| Wealth (Poorest) | 1 | 1 | 1 |
| Poorer | 0.947 | 0.869 | 1.035 |
| (0.835, 1.073) | (0.731, 1.034) | (0.863, 1.241) | |
| Middle | 0.940 | 0.855 | 1.019 |
| (0.825, 1.069) | (0.713, 1.025) | (0.846, 1.227) | |
| Richer | 0.869 * | 0.831 | 0.913 |
| (0.757, 0.998) | (0.685, 1.009) | (0.749, 1.114) | |
| Richest | 0.824 * | 0.748 * | 0.913 |
| (0.701, 0.968) | (0.593, 0.942) | (0.726, 1.147) | |
| Child’s Age (0–11 months) | 1 | 1 | 1 |
| 12–23 | 0.973 | 0.938 | 1.002 |
| (0.870, 1.088) | (0.801, 1.099) | (0.855, 1.173) | |
| 24–35 | 0.803 *** | 0.769 ** | 0.828 * |
| (0.715, 0.902) | (0.654, 0.905) | (0.701, 0.979) | |
| 36–47 | 0.772 *** | 0.713 *** | 0.838 * |
| (0.682, 0.873) | (0.599, 0.848) | (0.702, 1.000) | |
| 48–59 | 0.631 *** | 0.645 *** | 0.607 *** |
| (0.550, 0.725) | (0.533, 0.780) | (0.497, 0.743) | |
| Sex (Male) | |||
| Female | 0.911 | NA | NA |
| (0.705, 1.143) | |||
| Nagalekerke-R2 | 0.341 | 0.419 | 0.368 |
| Overall | Male | Female | |
|---|---|---|---|
| Age (15–19) | 1 | 1 | 1 |
| 20–24 | 0.802 | 0.828 | 0.774 |
| (0.666, 1.065) | (0.641, 1.068) | (0.587, 1.019) | |
| 25–29 | 0.888 | 0.679 ** | 0.934 |
| (0.643, 1.464) | (0.513, 0.898) | (0.694, 1.257) | |
| 30+ | 0.921 | 0.940 | 0.914 |
| (0.745, 1.139) | (0.698, 1.265) | (0.671, 1.243) | |
| Residency (Urban) | 1 | 1 | 1 |
| Rural | 0.900 | 1.020 | 0.777 * |
| (0.771, 1.051) | (0.823, 1.263) | (0.619, 0.975) | |
| Region (Barisal) | 1 | 1 | 1 |
| Chittagong | 1.020 | 1.131 | 0.923 |
| (0.812, 1.281) | (0.822, 1.557) | (0.664, 1.282) | |
| Dhaka | 0.983 | 1.150 | 0.839 |
| (0.774, 1.247) | (0.818, 1.616) | (0.598, 1.176) | |
| Khulna | 0.850 | 0.941 | 0.757 |
| (0.658, 1.098) | (0.656, 1.351) | (0.525, 1.092) | |
| Rajshahi | 0.770 * | 0.776 | 0.760 |
| (0.607, 0.976) | (0.554, 1.086) | (0.542, 1.067) | |
| Rangpur | 0.789 | 0.887 | 0.688 |
| (0.609, 1.022) | (0.618, 1.273) | (0.471, 1.003) | |
| Sylhet | 0.950 | 1.154 | 0.763 |
| (0.710, 1.272) | (0.775, 1.720) | (0.492, 1.183) | |
| Education (None) | 1 | 1 | 1 |
| Primary | 1.051 | 1.214 | 0.899 |
| (0.881, 1.254) | (0.952, 1.547) | (0.692, 1.167) | |
| Secondary | 0.823 * | 0.916 | 0.724 * |
| (0.683, 0.992) | (0.707, 1.187) | (0.551, 0.951) | |
| Higher | 0.584 * | 0.961 | 0.758 |
| (0.384, 0.890) | (0.639, 1.445) | (0.567, 1.013) | |
| Religion (Islam) | 1 | 1 | 1 |
| Others | 0.873 | 0.758 | 0.993 |
| (0.690, 1.105) | (0.547, 1.052) | (0.704, 1.401) | |
| Sanitation (Unimproved) | 1 | 1 | 1 |
| Improved | 0.724 ** | 1.009 | 0.836 |
| (0.595, 8.073) | (0.817, 1.244) | (0.672, 1.041) | |
| Water (Unimproved) | 1 | 1 | 1 |
| Improved | 0.820 * | 0.941 | 1.014 |
| (0.672, 0.949) | (0.714, 1.518) | (0.667, 1.544) | |
| Fuel (Unclean) | 1 | 1 | 1 |
| Clean | 0.682 ** | 0.635 * | 0.717 |
| (0.520, 0.894) | (0.433, 0.930) | (0.485, 1.060) | |
| Employed (Yes) | 1 | 1 | 1 |
| No | 0.987 | 0.953 | 1.021 |
| (0.848, 1.149) | (0.772, 1.177) | (0.818, 1.275) | |
| Wealth (Poorest) | 1 | 1 | 1 |
| Poorer | 1.162 | 1.067 | 1.279 |
| (0.953, 1.416) | (0.813, 1.400) | (0.954, 1.715) | |
| Middle | 1.030 | 0.882 | 1.210 |
| (0.838, 1.266) | (0.663, 1.173) | (0.892, 1.640) | |
| Richer | 0.849 * | 0.794 | 0.915 |
| (0.681, 0.960) | (0.583, 1.081) | (0.662, 1.265) | |
| Richest | 0.784 * | 0.740 | 0.842 |
| (0.605, 0.916) | (0.514, 1.067) | (0.579, 1.224) | |
| Child’s Age (0–11 months) | 1 | 1 | 1 |
| 12–23 | 0.873 | 0.760 * | 1.019 |
| (0.734, 1.038) | (0.596, 0.968) | (0.793, 1.308) | |
| 24–35 | 0.812 * | 0.704 ** | 0.951 |
| (0.676, 0.976) | (0.547, 0.907) | (0.725, 1.248) | |
| 36–47 | 0.661 *** | 0.521 *** | 0.863 |
| (0.540, 0.809) | (0.394, 0.690) | (0.641, 1.160) | |
| 48–59 | 0.639 *** | 0.600 ** | 0.693 * |
| (0.508, 0.804) | (0.439, 0.821) | (0.492, 0.978) | |
| Sex (Male) | |||
| Female | 0.946 | NA | NA |
| (0.835, 1.073) | |||
| Nagalekerke-R2 | 0.613 | 0.441 | 0.468 |
| Overall | Male | Female | |
|---|---|---|---|
| Age (15–19) | 1 | 1 | 1 |
| 20–24 | 1.035 | 0.997 | 1.067 |
| (0.802, 1.335) | (0.695, 1.431) | (0.740, 1.537) | |
| 25–29 | 1.133 | 0.879 | 1.560 * |
| (0.857, 1.498) | (0.597, 1.294) | (1.032, 2.358) | |
| 30+ | 1.321 | 1.037 | 1.711 * |
| (0.979, 1.782) | (0.680, 1.581) | (1.107, 2.644) | |
| Residency (Urban) | 1 | 1 | 1 |
| Rural | 0.955 | 0.972 | 0.911 |
| (0.772, 1.181) | (0.723, 1.307) | (0.666, 1.246) | |
| Region (Barisal) | 1 | 1 | 1 |
| Chittagong | 1.033 | 1.640 * | 0.592 * |
| (0.745, 1.430) | (1.058, 2.541) | (0.357, 0.982) | |
| Dhaka | 1.083 | 1.719 * | 0.664 |
| (0.770, 1.524) | (1.073, 2.754) | (0.394, 1.118) | |
| Khulna | 0.615 ** | 0.774 | 0.458 ** |
| (0.438, 0.862) | (0.493, 1.214) | (0.270, 0.778) | |
| Rajshahi | 0.915 | 1.122 | 0.702 |
| (0.654, 1.280) | (0.720, 1.749) | (0.414, 1.191) | |
| Rangpur | 0.819 | 1.261 | 0.489 * |
| (0.574, 1.170) | (0.774, 2.054) | (0.284, 0.844) | |
| Sylhet | 2.185 ** | 3.306 *** | 1.358 |
| (1.312, 3.638) | (1.670, 6.546) | (0.621, 2.970) | |
| Education (None) | 1 | 1 | 1 |
| Primary | 1.058 | 0.923 | 1.270 |
| (0.822, 1.363) | (0.649, 1.312) | (0.873, 1.847) | |
| Secondary | 1.138 | 1.028 | 1.337 |
| (0.876, 1.480) | (0.711, 1.484) | (0.911, 1.962) | |
| Higher | 0.892 | 1.282 | 0.653 |
| (0.619, 1.285) | (0.741, 2.220) | (0.392, 1.086) | |
| Religion (Islam) | 1 | 1 | 1 |
| Others | 0.792 | 0.699 | 0.844 |
| (0.588, 1.067) | (0.466, 1.050) | (0.540, 1.320) | |
| Sanitation (Unimproved) | 1 | 1 | 1 |
| Improved | 0.644 ** | 0.962 | 0.807 |
| (0.466, 0.890) | (0.712, 1.299) | (0.650, 1.003) | |
| Water (Unimproved) | 1 | 1 | 1 |
| Improved | 1.051 | 1.120 | 0.998 |
| (0.699, 1.580) | (0.648, 1.935) | (0.534, 1.863) | |
| Fuel (Unclean) | 1 | 1 | 1 |
| Clean | 0.648 * | 0.565 * | 0.716 |
| (0.464, 0.903) | (0.354, 0.901) | (0.439, 1.167) | |
| Employed (Yes) | 1 | 1 | 1 |
| No | 1.113 | 1.153 | 1.050 |
| (0.899, 1.379) | (0.855, 1.556) | (0.768, 1.435) | |
| Wealth (Poorest) | 1 | 1 | 1 |
| Poorer | 0.983 | 0.937 | 0.990 |
| (0.736, 1.312) | (0.619, 1.418) | (0.656, 1.494) | |
| Middle | 1.130 | 0.738 | 1.127 |
| (0.832, 1.537) | (0.487, 1.119) | (0.738, 2.933) | |
| Richer | 0.581 * | 0.695 | 0.999 |
| (0.352, 0.959) | (0.446, 1.081) | (0.643, 1.553) | |
| Richest | 0.592 * | 0.850 | 1.169 |
| (0.357, 0.980) | (0.624, 1.157) | (0.703, 1.946) | |
| Child’s Age (0–11 months) | 1 | 1 | 1 |
| 12–23 | 1.051 | 0.970 | 1.111 |
| (0.821, 1.345) | (0.685, 1.374) | (0.780, 1.583) | |
| 24–35 | 0.861 | 0.950 | 0.739 |
| (0.669, 1.107) | (0.664, 1.360) | (0.515, 1.062) | |
| 36–47 | 0.900 | 0.696 | 1.228 |
| (0.682, 1.189) | (0.481, 1.008) | (0.793, 1.902) | |
| 48–59 | 0.749 | 0.857 | 0.629 * |
| (0.552, 1.016) | (0.557, 1.317) | (0.404, 0.980) | |
| Sex (Male) | 1 | ||
| Female | 0.976 | NA | NA |
| (0.821, 1.161) | |||
| Nagalekerke-R2 | 0.374 | 0.280 | 0.412 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yaya, S.; Bishwajit, G. Burden of Acute Respiratory Infections Among Under-Five Children in Relation to Household Wealth and Socioeconomic Status in Bangladesh. Trop. Med. Infect. Dis. 2019, 4, 36. https://doi.org/10.3390/tropicalmed4010036
Yaya S, Bishwajit G. Burden of Acute Respiratory Infections Among Under-Five Children in Relation to Household Wealth and Socioeconomic Status in Bangladesh. Tropical Medicine and Infectious Disease. 2019; 4(1):36. https://doi.org/10.3390/tropicalmed4010036
Chicago/Turabian StyleYaya, Sanni, and Ghose Bishwajit. 2019. "Burden of Acute Respiratory Infections Among Under-Five Children in Relation to Household Wealth and Socioeconomic Status in Bangladesh" Tropical Medicine and Infectious Disease 4, no. 1: 36. https://doi.org/10.3390/tropicalmed4010036
APA StyleYaya, S., & Bishwajit, G. (2019). Burden of Acute Respiratory Infections Among Under-Five Children in Relation to Household Wealth and Socioeconomic Status in Bangladesh. Tropical Medicine and Infectious Disease, 4(1), 36. https://doi.org/10.3390/tropicalmed4010036






