Blood-Transfusion Risk Factors after Intramedullary Nailing for Extracapsular Femoral Neck Fracture in Elderly Patients
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Sample
2.3. Surgical Technique, Intervention, and Blood-Transfusion Criteria
2.4. Risk Factors and Outcome Measurements
2.5. Statistical Analysis
3. Results
3.1. Patients
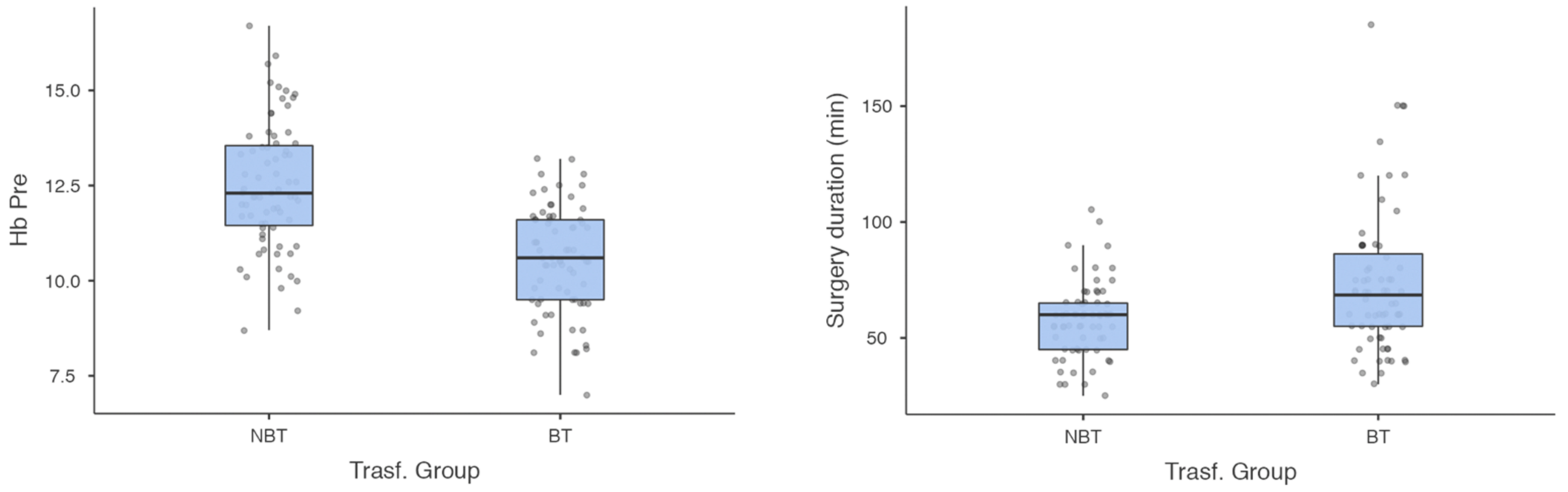
3.2. Group Comparisons
3.3. Relative-Risk Parameters
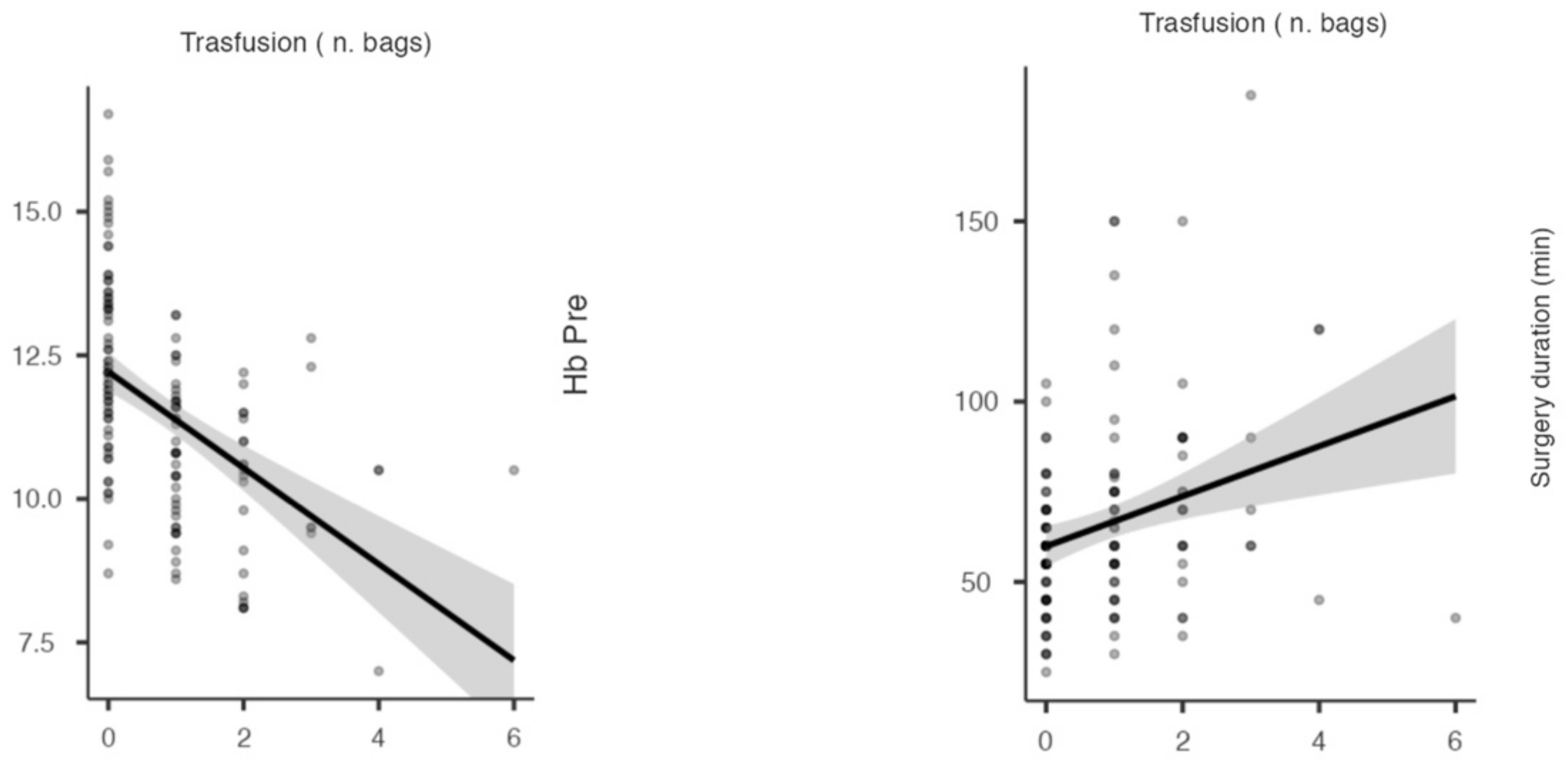
3.4. Cohort-Parameter Correlation
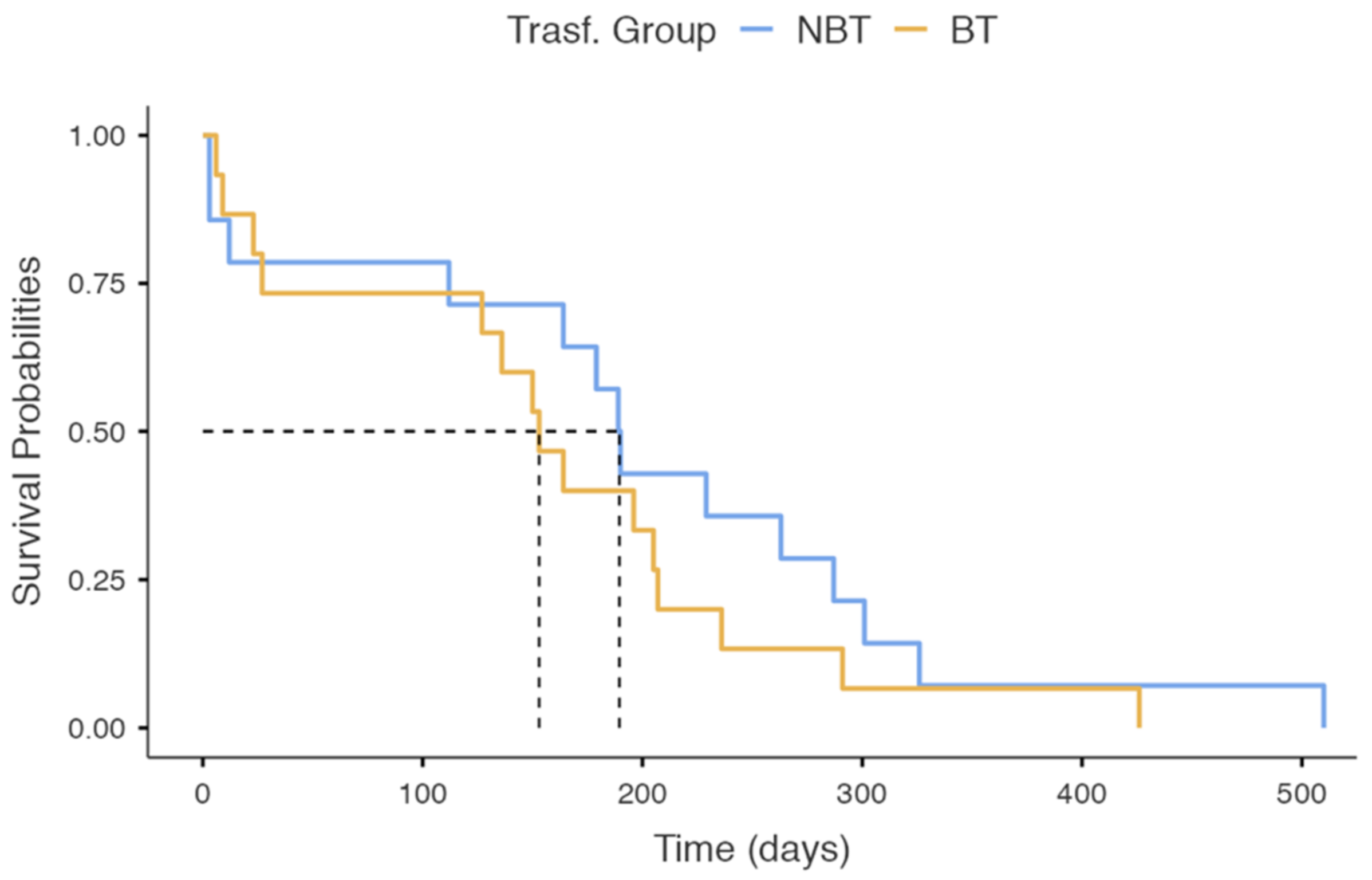
3.5. Survival Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bastard, C. Femoral neck fracture. Rev. Prat. 2019, 69, 1124–1128. [Google Scholar] [PubMed]
- Clegg, A.; Young, J.; Iliffe, S.; Rikkert, M.O.; Rockwood, K. Frailty in Elderly People. Lancet 2013, 381, 752–762. [Google Scholar] [CrossRef] [PubMed]
- Keene, G.S.; Parker, M.J.; Pryor, G.A. Mortality and Morbidity after Hip Fractures. BMJ 1993, 307, 1248–1250. [Google Scholar] [CrossRef] [PubMed]
- Sambrook, P.; Cooper, C. Osteoporosis. Lancet 2006, 367, 2010–2018. [Google Scholar] [CrossRef]
- Pillai, A.; Eranki, V.; Shenoy, R.; Hadidi, M. Age Related Incidence and Early Outcomes of Hip Fractures: A Prospective Cohort Study of 1177 Patients. J. Orthop. Surg. Res. 2011, 6, 5. [Google Scholar] [CrossRef] [PubMed]
- Lamb, J.N.; Panteli, M.; Pneumaticos, S.G.; Giannoudis, P.V. Epidemiology of Pertrochanteric Fractures: Our Institutional Experience. Eur. J. Trauma Emerg. Surg. 2014, 40, 225–232. [Google Scholar] [CrossRef]
- Hoffmann, M.F.; Khoriaty, J.D.; Sietsema, D.L.; Jones, C.B. Outcome of Intramedullary Nailing Treatment for Intertrochanteric Femoral Fractures. J. Orthop. Surg. Res. 2019, 14, 360. [Google Scholar] [CrossRef]
- Roberts, K.C.; Brox, W.T.; Jevsevar, D.S.; Sevarino, K. Management of Hip Fractures in the Elderly. J. Am. Acad. Orthop. Surg. 2015, 23, 131–137. [Google Scholar] [CrossRef]
- Florschutz, A.V.; Langford, J.R.; Haidukewych, G.J.; Koval, K.J. Femoral Neck Fractures: Current Management. J. Orthop. Trauma 2015, 29, 121–129. [Google Scholar] [CrossRef] [PubMed]
- Bennett-Guerrero, E.; Zhao, Y.; O’Brien, S.M.; Ferguson, T.B.; Peterson, E.D.; Gammie, J.S.; Song, H.K. Variation in Use of Blood Transfusion in Coronary Artery Bypass Graft Surgery. JAMA 2010, 304, 1568. [Google Scholar] [CrossRef]
- Testa, G.; Vescio, A.; Zuccalà, D.; Petrantoni, V.; Amico, M.; Russo, G.I.; Sessa, G.; Pavone, V. Diagnosis, Treatment and Prevention of Sarcopenia in Hip Fractured Patients: Where We Are and Where We Are Going: A Systematic Review. JCM 2020, 9, 2997. [Google Scholar] [CrossRef]
- Avola, M.; Mangano, G.R.A.; Testa, G.; Mangano, S.; Vescio, A.; Pavone, V.; Vecchio, M. Rehabilitation Strategies for Patients with Femoral Neck Fractures in Sarcopenia: A Narrative Review. JCM 2020, 9, 3115. [Google Scholar] [CrossRef] [PubMed]
- Lakstein, D.; Hendel, D.; Haimovich, Y.; Feldbrin, Z. Changes in the Pattern of Fractures of the Hip in Patients 60 Years of Age and Older between 2001 and 2010: A Radiological Review. Bone Jt. J. 2013, 95-B, 1250–1254. [Google Scholar] [CrossRef] [PubMed]
- Dai, C.-Q.; Wang, L.-H.; Zhu, Y.-Q.; Xu, G.-H.; Shan, J.-B.; Huang, W.-C.; Wei, L.-H.; Zhou, F.-L.; Li, Y. Risk Factors of Perioperative Blood Transfusion in Elderly Patients with Femoral Intertrochanteric Fracture. Medicine 2020, 99, e19726. [Google Scholar] [CrossRef] [PubMed]
- Luangwaranyoo, A.; Suksintharanon, M.; Tangadulrat, P.; Iamthanaporn, K.; Hongnaparak, T.; Yuenyongviwat, V. Factors for Blood Transfusions Following Hemi Hip Arthroplasty for Patients With Femoral Neck Fracture. Geriatr. Orthop. Surg. Rehabil. 2020, 11, 215145932097299. [Google Scholar] [CrossRef] [PubMed]
- Nagra, N.S.; van Popta, D.; Whiteside, S.; Holt, E.M. An Analysis of Postoperative Hemoglobin Levels in Patients with a Fractured Neck of Femur. Acta Orthop. Traumatol. Turc. 2016, 50, 507–513. [Google Scholar] [CrossRef]
- Wang, J.-Q.; Chen, L.-Y.; Jiang, B.-J.; Zhao, Y.-M. Development of a Nomogram for Predicting Blood Transfusion Risk After Hemiarthroplasty for Femoral Neck Fractures in Elderly Patients. Med. Sci. Monit. 2020, 26, e920255-1–e920255-7. [Google Scholar] [CrossRef] [PubMed]
- D’Amore, T.; Loewen, M.; Gorczyca, M.T.; Judd, K.; Ketz, J.P.; Soles, G.; Gorczyca, J.T. Rethinking Strategies for Blood Transfusion in Hip Fracture Patients. OTA Int. Open Access J. Orthop. Trauma 2020, 3, e083. [Google Scholar] [CrossRef] [PubMed]
- Jang, S.-Y.; Cha, Y.-H.; Yoo, J.-I.; Oh, T.; Kim, J.-T.; Park, C.H.; Choy, W.-S.; Ha, Y.-C.; Koo, K.-H. Blood Transfusion for Elderly Patients with Hip Fracture: A Nationwide Cohort Study. J. Korean Med. Sci. 2020, 35, e313. [Google Scholar] [CrossRef] [PubMed]
- Goh, E.L.; Lerner, R.G.; Achten, J.; Parsons, N.; Griffin, X.L.; Costa, P.M.L. Complications Following Hip Fracture: Results from the World Hip Trauma Evaluation Cohort Study. Injury 2020, 51, 1331–1336. [Google Scholar] [CrossRef] [PubMed]
- Kamiloski, V. Analysis of the Hemoglobin Level Drop in Patients with Hip Fracture After Admission. ACC 2017, 56, 645–649. [Google Scholar] [CrossRef] [PubMed]
- Zheng, H.; Zhang, Y.; Wang, H.; Sun, T.; Sun, Q. Comparison of Perioperative Hidden Blood Loss for Intertrochanteric Fractures in the Elderly by Different Intramedullary Fixations: A Randomized Controlled Study Protocol. Medicine 2020, 99, e21666. [Google Scholar] [CrossRef] [PubMed]
- Cai, L.; Wang, T.; Di, L.; Hu, W.; Wang, J. Comparison of Intramedullary and Extramedullary Fixation of Stable Intertrochanteric Fractures in the Elderly: A Prospective Randomised Controlled Trial Exploring Hidden Perioperative Blood Loss. BMC Musculoskelet. Disord. 2016, 17, 475. [Google Scholar] [CrossRef] [PubMed]
- Luo, X.; He, S.; Li, Z.; Li, Q. Quantification and Influencing Factors of Perioperative Hidden Blood Loss during Intramedullary Fixation for Intertrochanteric Fractures in the Elderly. Arch. Orthop. Trauma Surg. 2020, 140, 1339–1348. [Google Scholar] [CrossRef]
- Greenhalgh, M.S.; Gowers, B.T.V.; Iyengar, K.P.; Adam, R.F. Blood Transfusions and Hip Fracture Mortality—A Retrospective Cohort Study. J. Clin. Orthop. Trauma 2021, 21, 101506. [Google Scholar] [CrossRef]
- Arshi, A.; Lai, W.C.; Iglesias, B.C.; McPherson, E.J.; Zeegen, E.N.; Stavrakis, A.I.; Sassoon, A.A. Blood Transfusion Rates and Predictors Following Geriatric Hip Fracture Surgery. HIP Int. 2021, 31, 272–279. [Google Scholar] [CrossRef] [PubMed]
- von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for Reporting Observational Studies. Epidemiology 2007, 18, 800–804. [Google Scholar] [CrossRef] [PubMed]
- Carson, J.L.; Guyatt, G.; Heddle, N.M.; Grossman, B.J.; Cohn, C.S.; Fung, M.K.; Gernsheimer, T.; Holcomb, J.B.; Kaplan, L.J.; Katz, L.M.; et al. Clinical Practice Guidelines From the AABB: Red Blood Cell Transfusion Thresholds and Storage. JAMA 2016, 316, 2025. [Google Scholar] [CrossRef]
- Yombi, J.C.; Putineanu, D.C.; Cornu, O.; Lavand’homme, P.; Cornette, P.; Castanares-Zapatero, D. Low Haemoglobin at Admission Is Associated with Mortality after Hip Fractures in Elderly Patients. Bone Jt. J. 2019, 101-B, 1122–1128. [Google Scholar] [CrossRef]
- Carson, J.L. Perioperative Blood Transfusion and Postoperative Mortality. JAMA 1998, 279, 199. [Google Scholar] [CrossRef]
- Johnston, P.; Wynn-Jones, H.; Chakravarty, D.; Boyle, A.; Parker, M.J. Is Perioperative Blood Transfusion a Risk Factor for Mortality or Infection After Hip Fracture? J. Orthop. Trauma 2006, 20, 675–679. [Google Scholar] [CrossRef] [PubMed]
- Brunskill, S.J.; Millette, S.L.; Shokoohi, A.; Pulford, E.; Doree, C.; Murphy, M.F.; Stanworth, S. Red Blood Cell Transfusion for People Undergoing Hip Fracture Surgery. Cochrane Database Syst. Rev. 2015, 4, CD009699. [Google Scholar] [CrossRef] [PubMed]
- Gregersen, M.; Damsgaard, E.M.; Borris, L.C. Blood Transfusion and Risk of Infection in Frail Elderly after Hip Fracture Surgery: The TRIFE Randomized Controlled Trial. Eur. J. Orthop. Surg. Traumatol. 2015, 25, 1031–1038. [Google Scholar] [CrossRef]
- Hart, A.; Khalil, J.A.; Carli, A.; Huk, O.; Zukor, D.; Antoniou, J. Blood Transfusion in Primary Total Hip and Knee Arthroplasty. Incidence, Risk Factors, and Thirty-Day Complication Rates. J. Bone Jt. Surg. 2014, 96, 1945–1951. [Google Scholar] [CrossRef] [PubMed]
- Tüzün, H.Y.; Bilekli, A.B.; Erşen, Ö. The Factors That Affect Blood Loss in Intertrochanteric Fractures Treated with Proximal Femoral Nail in the Elderly. Eur. J. Trauma Emerg. Surg. 2022, 48, 1879–1884. [Google Scholar] [CrossRef] [PubMed]
- Hou, G.; Zhou, F.; Tian, Y.; Ji, H.; Zhang, Z.; Guo, Y.; Lv, Y. Predicting the Need for Blood Transfusions in Elderly Patients with Pertrochanteric Femoral Fractures. Injury 2014, 45, 1932–1937. [Google Scholar] [CrossRef] [PubMed]
- Fazal, M.A.; Bagley, C.; Garg, P. Predictors for Perioperative Blood Transfusion in Elderly Patients with Extra Capsular Hip Fractures Treated with Cephalo-Medullary Nailing. Chin. J. Traumatol. 2018, 21, 16–19. [Google Scholar] [CrossRef] [PubMed]
- Adunsky, A.; Lichtenstein, A.; Mizrahi, E.; Arad, M.; Heim, M. Blood Transfusion Requirements in Elderly Hip Fracture Patients. Arch. Gerontol. Geriatr. 2003, 36, 75–81. [Google Scholar] [CrossRef]
- Desai, S.; Wood, K.; Marsh, J.; Bryant, D.; Abdo, H.; Lawendy, A.-R.; Sanders, D. Factors Affecting Transfusion Requirement after Hip Fracture: Can We Reduce the Need for Blood? Can. J. Surg. 2014, 57, 342–348. [Google Scholar] [CrossRef]
- Walsh, M.; Preston, C.; Bong, M.; Patel, V.; Di Cesare, P.E. Relative Risk Factors for Requirement of Blood Transfusion after Total Hip Arthroplasty. J. Arthroplast. 2007, 22, 1162–1167. [Google Scholar] [CrossRef]
- Shelton, C.; White, S. Anaesthesia for Hip Fracture Repair. BJA Educ. 2020, 20, 142–149. [Google Scholar] [CrossRef] [PubMed]
- Chen, D.X.; Yang, L.; Ding, L.; Li, S.Y.; Qi, Y.N.; Li, Q. Perioperative Outcomes in Geriatric Patients Undergoing Hip Fracture Surgery with Different Anesthesia Techniques: A Systematic Review and Meta-Analysis. Medicine 2019, 98, e18220. [Google Scholar] [CrossRef] [PubMed]
- Basques, B.A.; Bohl, D.D.; Golinvaux, N.S.; Samuel, A.M.; Grauer, J.G. General versus Spinal Anaesthesia for Patients Aged 70 Years and Older with a Fracture of the Hip. Bone Jt. J. 2015, 97-B, 689–695. [Google Scholar] [CrossRef]
- Borghi, B.; Casati, A.; Iuorio, S.; Celleno, D.; Michael, M.; Serafini, P.; Pusceddu, A.; Fanelli, G. Frequency of Hypotension and Bradycardia during General Anesthesia, Epidural Anesthesia, or Integrated Epidural-General Anesthesia for Total Hip Replacement. J. Clin. Anesth. 2002, 14, 102–106. [Google Scholar] [CrossRef] [PubMed]
- Sessler, D.I.; Warner, D.S.; Warner, M.A. Temperature Monitoring and Perioperative Thermoregulation. Anesthesiology 2008, 109, 318–338. [Google Scholar] [CrossRef] [PubMed]
- Dillon, M.F.; Collins, D.; Rice, J.; Murphy, P.G.; Nicholson, P.; Mac Elwaine, J. Preoperative Characteristics Identify Patients with Hip Fractures at Risk of Transfusion. Clin. Orthop. Relat. Res. 2005, 439, 201–206. [Google Scholar] [CrossRef] [PubMed]
- Hasan, O.; Barkat, R.; Rabbani, A.; Rabbani, U.; Mahmood, F.; Noordin, S. Charlson Comorbidity Index Predicts Postoperative Complications in Surgically Treated Hip Fracture Patients in a Tertiary Care Hospital: Retrospective Cohort of 1045 Patients. Int. J. Surg. 2020, 82, 116–120. [Google Scholar] [CrossRef] [PubMed]
- Quach, L.H.; Jayamaha, S.; Whitehouse, S.L.; Crawford, R.; Pulle, C.R.; Bell, J.J. Comparison of the Charlson Comorbidity Index with the ASA Score for Predicting 12-Month Mortality in Acute Hip Fracture. Injury 2020, 51, 1004–1010. [Google Scholar] [CrossRef] [PubMed]
- Haugan, K.; Klaksvik, J.; Foss, O.A. 30-Day Mortality in Patients after Hip Fracture Surgery: A Comparison of the Charlson Comorbidity Index Score and ASA Score Used in Two Prediction Models. Injury 2021, 52, 2379–2383. [Google Scholar] [CrossRef]
- Guo, J.; Zhang, Y.; Hou, Z. Intramedullary Fixation Does Not Cause a Large Amount of Hidden Blood Loss in Elderly Patients with Intertrochanteric Fractures. CIA 2021, 16, 475–486. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.-H.; Chien, J.-T.; Hung, J.-P.; Hong, C.-K.; Tsai, T.-Y.; Yang, C.-C. Unstable Intertrochanteric Fractures Are Associated with a Greater Hemoglobin Drop during the Perioperative Period: A Retrospective Case Control Study. BMC Musculoskelet. Disord. 2020, 21, 244. [Google Scholar] [CrossRef] [PubMed]
- Ma, J.; Kuang, M.; Fan, Z.; Xing, F.; Zhao, Y.; Zhang, L.; Chen, H.; Han, C.; Ma, X. Comparison of Clinical Outcomes with InterTan vs Gamma Nail or PFNA in the Treatment of Intertrochanteric Fractures: A Meta-Analysis. Sci. Rep. 2017, 7, 15962. [Google Scholar] [CrossRef]
- Thamyongkit, S.; MacKenzie, J.S.; Sirisreetreerux, N.; Shafiq, B.; Hasenboehler, E.A. Outcomes after Unstable Pertrochanteric Femur Fracture: Intermediate versus Long Cephalomedullary Nails. Eur. J. Trauma Emerg. Surg. 2020, 46, 963–968. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.-H.; Kim, N.Y. Can Early Surgery Reduce the Need to Packed Red Blood Cell Transfusion in Elderly Patients with Intertrochanteric Femur Fractures? Injury 2021, 52, 3047–3050. [Google Scholar] [CrossRef] [PubMed]
- Mattisson, L.; Lapidus, L.J.; Enocson, A. What Is the Influence of a Delay to Surgery >24 Hours on the Rate of Red Blood Cell Transfusion in Elderly Patients With Intertrochanteric or Subtrochanteric Hip Fractures Treated With Cephalomedullary Nails? J. Orthop. Trauma 2018, 32, 403–407. [Google Scholar] [CrossRef] [PubMed]
- Shokoohi, A.; Stanworth, S.; Mistry, D.; Lamb, S.; Staves, J.; Murphy, M.F. The Risks of Red Cell Transfusion for Hip Fracture Surgery in the Elderly: The Risks of Red Cell Transfusion for Hip. Vox Sang. 2012, 103, 223–230. [Google Scholar] [CrossRef] [PubMed]
- Scharman, C.D.; Burger, D.; Shatzel, J.J.; Kim, E.; DeLoughery, T.G. Treatment of Individuals Who Cannot Receive Blood Products for Religious or Other Reasons. Am. J. Hematol. 2017, 92, 1370–1381. [Google Scholar] [CrossRef] [PubMed]
- Cuenca, J.; García-Erce, J.A.; Martínez, A.A.; Solano, V.M.; Molina, J.; Muñoz, M. Role of Parenteral Iron in the Management of Anaemia in the Elderly Patient Undergoing Displaced Subcapital Hip Fracture Repair: Preliminary Data. Arch. Orthop. Trauma Surg. 2005, 125, 342–347. [Google Scholar] [CrossRef]
- Rowlands, M.; Forward, D.P.; Sahota, O.; Moppett, I.K. The Effect of Intravenous Iron on Postoperative Transfusion Requirements in Hip Fracture Patients: Study Protocol for a Randomized Controlled Trial. Trials 2013, 14, 288. [Google Scholar] [CrossRef]
- Xing, F.; Chen, W.; Long, C.; Huang, F.; Wang, G.; Xiang, Z. Postoperative Outcomes of Tranexamic Acid Use in Geriatric Trauma Patients Treated with Proximal Femoral Intramedullary Nails: A Systematic Review and Meta-Analysis. Orthop. Traumatol. Surg. Res. 2020, 106, 117–126. [Google Scholar] [CrossRef] [PubMed]
| Patients (M:F) | Age (Range) | BMI | Hb | INR | Hospital Stay | Time To Surgery | Surgery Duration | Anesthesia (GA/CSEA) | ASA | CCI | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Group NBT | 71 (24:47) | 80.2 ± 10.7 (65–94) | 26.5 ± 5.9 (15.4–44.4) | 12.5 ± 1.67 (8.7–16.7) | 1.1 ± 0.12 (0.9–1.4) | 10.8 ± 4 (5–24) | 2.4 ± 1.6 (0–8) | 57.8 ± 16.2 (25–105) | 9/62 | 2.8 ± 0.6 (1–5) | 5.21 ± 2.1 (1–10) |
| Group BT | 72 (17:55) | 82.9 ± 7.6 (65–99) | 26.1 ± 5.1 (12.9–39.1) | 10.6 ± 1.4 (7.0–13.2) | 1.1 ± 0.16 (0.9–1.6) | 11.4 ± 5.3 (5–39) | 2.3 ± 2 (0–9) | 73.3 ± 31.2 (30–185) | 11/61 | 2.8 ± 0.5 (2–4) | 5.78 ± 2.4 (2–12) |
| NBT vs. BT | 0.17 | 0.07 | 0.65 | <0.001 | 0.88 | 0.44 | 0.64 | <0.001 | 0.65 | 0.81 | 0.19 |
| RR (95% C.I.) | 1.43 (0.8, 2.4) | 1.52 (0.9, 2.5) | 1.0 (0.77, 1.4) | 1.03 (0.9, 1.7) | 0.91 (0.49, 1.4) | 1.16 (0.45, 2.8) | 0.74 (0.5, 1.1) | 1.37 (0.80, 2.3) | 1.05 (0.9, 1.2) | 0.96 (0.55, 1.6) | 0.82 (0.62, 1.1) |
| PCC (p) | 0.07 (0.64) | 0.08 (0.33) | −0.033 (0.70) | −0.49 (<0.001) | −0.02 (0.89) | 0.16 (0.06) | −0.07 (0.41) | 0.28 (0.001) | 0.11 (0.17) | 0.02 (0.74) | 0.16 (0.10) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Testa, G.; Montemagno, M.; Vescio, A.; Micali, G.; Perrotta, R.; Lacarrubba, F.; Avitabile, T.; Basile, G.; Pavone, V. Blood-Transfusion Risk Factors after Intramedullary Nailing for Extracapsular Femoral Neck Fracture in Elderly Patients. J. Funct. Morphol. Kinesiol. 2023, 8, 27. https://doi.org/10.3390/jfmk8010027
Testa G, Montemagno M, Vescio A, Micali G, Perrotta R, Lacarrubba F, Avitabile T, Basile G, Pavone V. Blood-Transfusion Risk Factors after Intramedullary Nailing for Extracapsular Femoral Neck Fracture in Elderly Patients. Journal of Functional Morphology and Kinesiology. 2023; 8(1):27. https://doi.org/10.3390/jfmk8010027
Chicago/Turabian StyleTesta, Gianluca, Marco Montemagno, Andrea Vescio, Giuseppe Micali, Rosario Perrotta, Francesco Lacarrubba, Teresio Avitabile, Guido Basile, and Vito Pavone. 2023. "Blood-Transfusion Risk Factors after Intramedullary Nailing for Extracapsular Femoral Neck Fracture in Elderly Patients" Journal of Functional Morphology and Kinesiology 8, no. 1: 27. https://doi.org/10.3390/jfmk8010027
APA StyleTesta, G., Montemagno, M., Vescio, A., Micali, G., Perrotta, R., Lacarrubba, F., Avitabile, T., Basile, G., & Pavone, V. (2023). Blood-Transfusion Risk Factors after Intramedullary Nailing for Extracapsular Femoral Neck Fracture in Elderly Patients. Journal of Functional Morphology and Kinesiology, 8(1), 27. https://doi.org/10.3390/jfmk8010027







