Restrictions in the Ankle Sagittal- and Frontal-Plane Range of Movement during Simulated Walking with Different Types of Orthoses
Abstract
1. Introduction
2. Material and Method
2.1. Orthoses and Measurement Set-Up
2.2. Simulation of Walking
2.3. Statistical Analysis
3. Results
4. Discussion
Acknowledgements
Author Contributions
Conflicts of Interest
References
- Valderrabano, V.; Hintermann, B.; Horisberger, M.; Fung, T.S. Ligamentous posttraumatic ankle osteoarthritis. Am. J. Sports Med. 2006, 34, 612–620. [Google Scholar] [CrossRef] [PubMed]
- Waterman, B.R.; Owens, B.D.; Davey, S.; Zacchilli, M.A.; Belmont, P.J., Jr. The epidemiology of ankle sprains in the United States. J. Bone Joint Surg. Am. 2010, 92, 2279–2284. [Google Scholar] [CrossRef] [PubMed]
- Hølmer, P.; Søndergaard, L.; Konradsen, L.; Nielsen, P.T.; Jørgensen, L.N. Epidemiology of sprains in the lateral ankle and foot. Foot Ankle Int. 1994, 15, 72–74. [Google Scholar] [CrossRef] [PubMed]
- Gribble, P.A.; Bleakley, C.M.; Caulfield, B.M.; Docherty, C.L.; Fourchet, F.; Fong, D.T.-P.; McKeon, P.O. 2016 consensus statement of the International Ankle Consortium: Prevalence, impact and long-term consequences of lateral ankle sprains. Br. J. Sports Med. 2016, 50, 1493–1495. [Google Scholar] [CrossRef] [PubMed]
- Petersen, W.; Rembitzki, I.V.; Koppenburg, A.G.; Ellermann, A.; Liebau, C.; Brüggemann, G.P.; Best, R. Treatment of acute ankle ligament injuries: A systematic review. Arch. Orthop. Trauma Surg. 2013, 133, 1129–1141. [Google Scholar] [CrossRef] [PubMed]
- Fong, D.T.-P.; Chan, Y.-Y.; Mok, K.-M.; Yung, P.S.; Chan, K.-M. Understanding acute ankle ligamentous sprain injury in sports. BMC Sports Sci. Med. Rehabil. 2009, 1, 14. [Google Scholar] [CrossRef] [PubMed]
- Giza, E.; Shin, E.C.; Wong, S.E.; Acevedo, J.I.; Mangone, P.G.; Olson, K.; Anderson, M.J. Arthroscopic suture anchor repair of the lateral ligament ankle complex: A cadaveric study. Am. J. Sports Med. 2013, 41, 2567–2572. [Google Scholar] [CrossRef] [PubMed]
- Wenny, R.; Duscher, D.; Meytap, E.; Weninger, P.; Hirtler, L. Dimensions and attachments of the ankle ligaments: Evaluation for ligament reconstruction. Anat. Sci. Int. 2015, 90, 161–171. [Google Scholar] [CrossRef] [PubMed]
- Ribbans, W.J.; Garde, A. Tibialis posterior tendon and deltoid and spring ligament injuries in the elite athlete. Foot Ankle Clin. 2013, 18, 255–291. [Google Scholar] [CrossRef] [PubMed]
- Crim, J.R.; Beals, T.C.; Nickisch, F.; Schannen, A.; Saltzman, C.L. Deltoid ligament abnormalities in chronic lateral ankle instability. Foot Ankle Int. 2011, 32, 873–878. [Google Scholar] [PubMed]
- Hintermann, B.; Boss, A.; Schäfer, D. Arthroscopic findings in patients with chronic ankle instability. Am. J. Sports Med. 2002, 30, 402–409. [Google Scholar] [CrossRef] [PubMed]
- Hintermann, B.; Valderrabano, V.; Boss, A.; Trouillier, H.H.; Dick, W. Medial ankle instability. Am. J. Sports Med. 2004, 32, 183–190. [Google Scholar] [CrossRef] [PubMed]
- Ferran, N.A.; Maffulli, N. Epidemiology of sprains of the lateral ankle ligament complex. Foot Ankle Clin. 2006, 11, 659–662. [Google Scholar] [CrossRef] [PubMed]
- Leumann, A.; Tsaknis, R.; Wiewiorski, M.; Valderrabano, V. Das akute Supinationstrauma des oberen Sprunggelenkes—Eine Bagatelle? Schweiz Med. Forum 2008, 8, 214–216. [Google Scholar]
- McCriskin, B.J.; Cameron, K.L.; Orr, J.D.; Waterman, B.R. Management and prevention of acute and chronic lateral ankle instability in athletic patient populations. World J. Orthop. 2015, 6, 161–171. [Google Scholar] [CrossRef] [PubMed]
- Van Rijn, R.M.; Van Os, A.G.; Bernsen, R.M.; Luijsterburg, P.A.; Koes, B.W.; Bierma-Zeinstra, S.M. What is the clinical course of acute ankle sprains? A systematic literature review. Am. J. Med. 2008, 121. [Google Scholar] [CrossRef] [PubMed]
- Kerkhoffs, G.; Rowe, B.H.; Assendelft, W.; Kelly, K.; Struijs, P.; Van Dijk, C. Immobilisation and functional treatment for acute lateral ankle ligament injuries in adults. Cochrane Database Syst. Rev. 2002, 3. [Google Scholar] [CrossRef]
- Struijs, P.A.; Kerkhoffs, G.M. Ankle sprain. BMJ Clin. Evid. 2010. [Google Scholar] [PubMed Central]
- Rosenbaum, D.; Becker, H. Ankle orthotic devices. Review, areas of application, and scientific results. Orthopade 1999, 28, 559–564. [Google Scholar] [CrossRef] [PubMed]
- Cottrell, J.A.; Turner, J.C.; Arinzeh, T.L.; O’Connor, J.P. The Biology of Bone and Ligament Healing. Foot Ankle Clin. 2016, 21, 739–761. [Google Scholar] [CrossRef] [PubMed]
- Ozeki, S.; Yasuda, K.; Kaneda, K.; Yamakoshi, K.; Yamanoi, T. Simultaneous strain measurement with determination of a zero strain reference for the medial and lateral ligaments of the ankle. Foot Ankle Int. 2002, 23, 825–832. [Google Scholar] [CrossRef] [PubMed]
- Cawley, P.W.; France, E.P. Biomechanics of the lateral ligaments of the ankle: An evaluation of the effects of axial load and single plane motions on ligament strain patterns. Foot Ankle 1991, 12, 92–99. [Google Scholar] [CrossRef] [PubMed]
- Bürgi, S.; Roost, J.; Hitz, M.R.; Schwilch, P.; Taylor, W.R.; Lorenzetti, S. A fast testing method to objectively quantify the stiffness of stability boots. Appl. Bion. Biomech. 2015, 595708. [Google Scholar] [CrossRef] [PubMed]
- Best, R.; Böhle, C.; Schiffer, T.; Petersen, W.; Ellermann, A.; Brueggemann, G.P.; Liebau, C. Early functional outcome of two different orthotic concepts in ankle sprains: A randomized controlled trial. Arch. Orthop. Trauma Surg. 2015, 135, 993–1001. [Google Scholar] [CrossRef] [PubMed]
- Mattacola, C.G.; Dwyer, M.K. Rehabilitation of the ankle after acute sprain or chronic instability. J. Athl. Train. 2002, 37, 413–429. [Google Scholar] [PubMed]
- Knupp, M.; Lang, T.H.; Zwicky, L.; Lötscher, P.; Hintermann, B. Chronic ankle instability (medial and lateral). Clin. Sports Med. 2015, 34, 679–688. [Google Scholar] [CrossRef] [PubMed]
- Knupp, M.; Valderrabano, V.; Hintermann, B. Anatomical and biomechanical aspects of total ankle replacement. Orthopade 2006, 35, 489–494. [Google Scholar] [CrossRef] [PubMed]
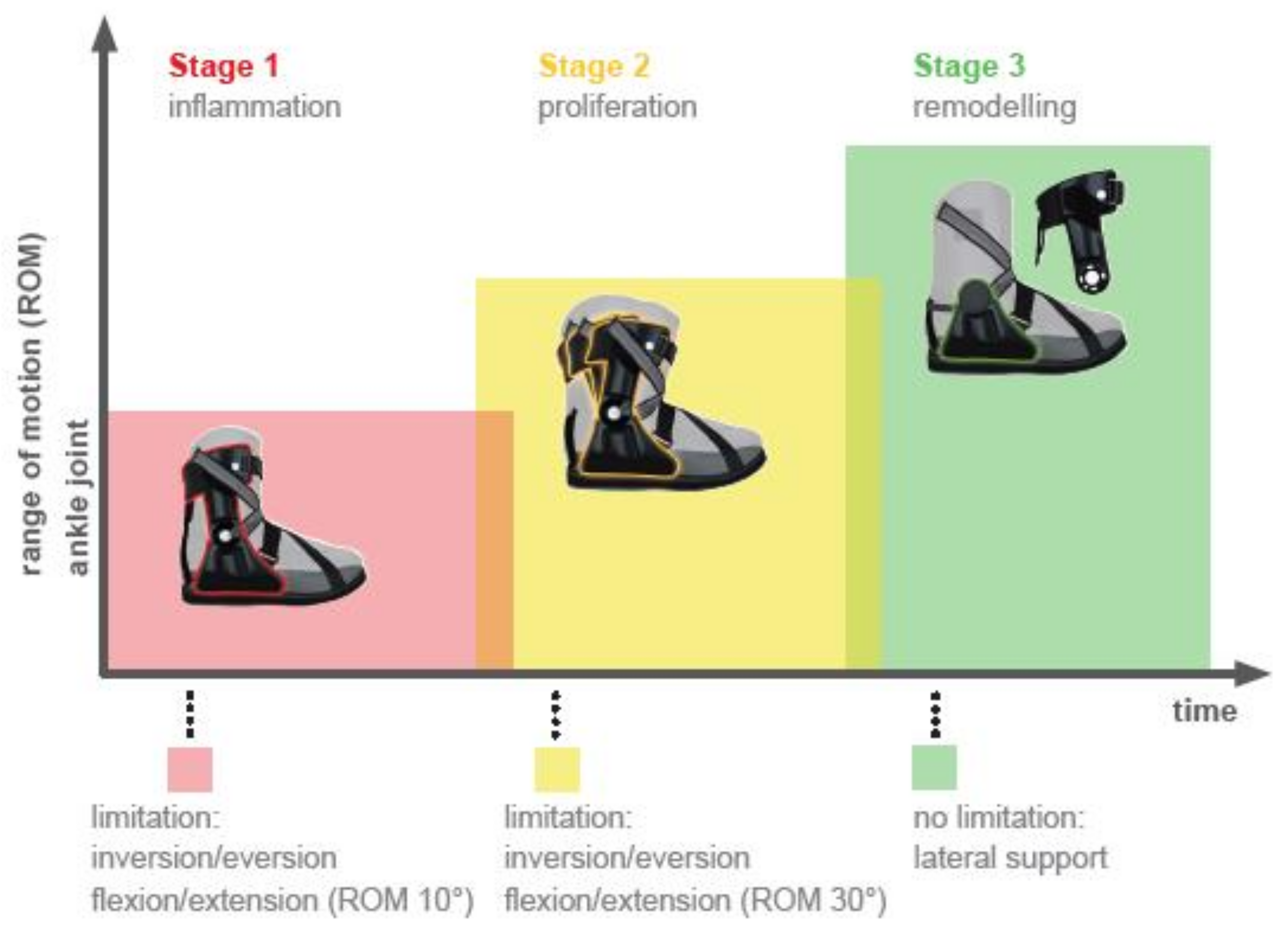


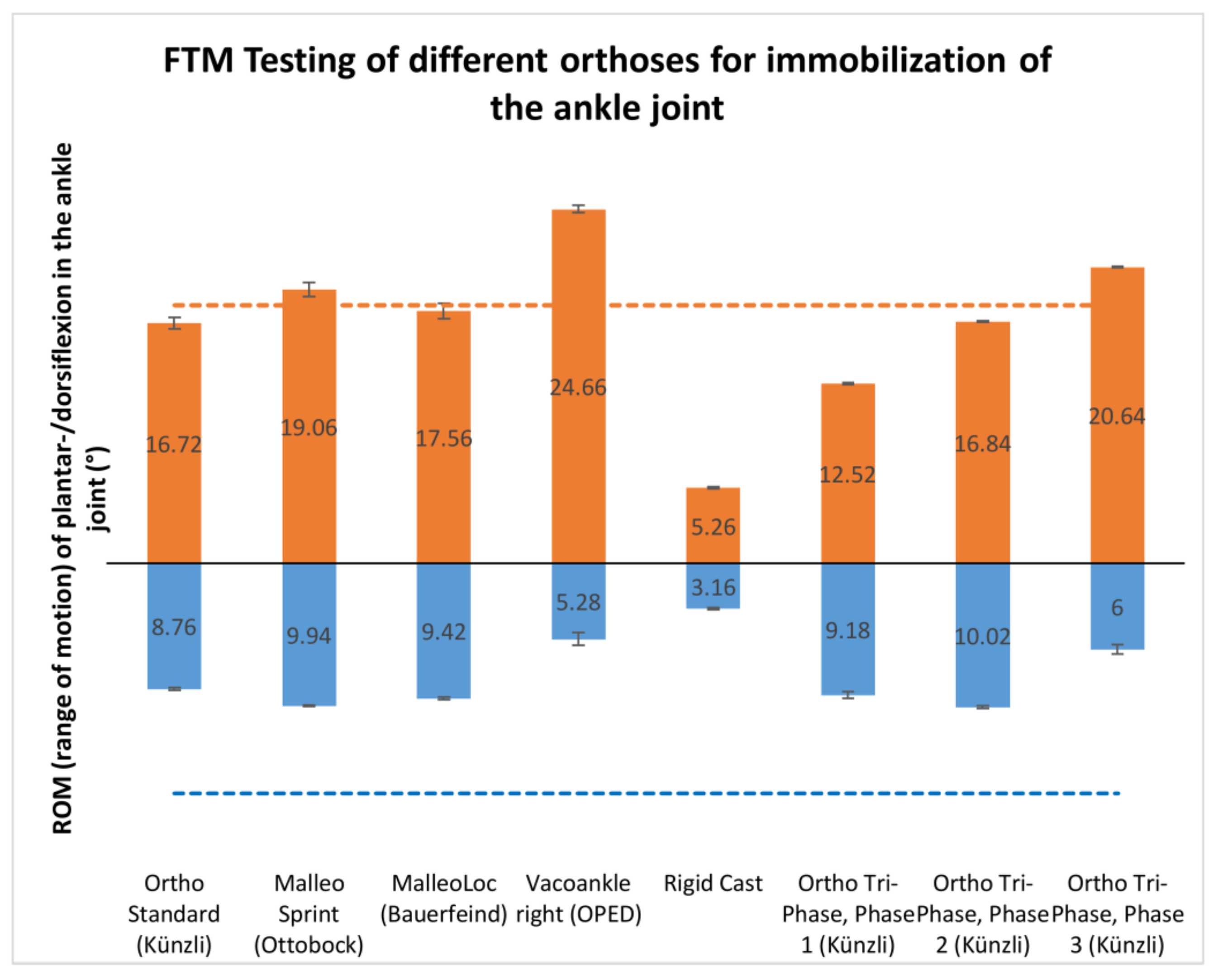
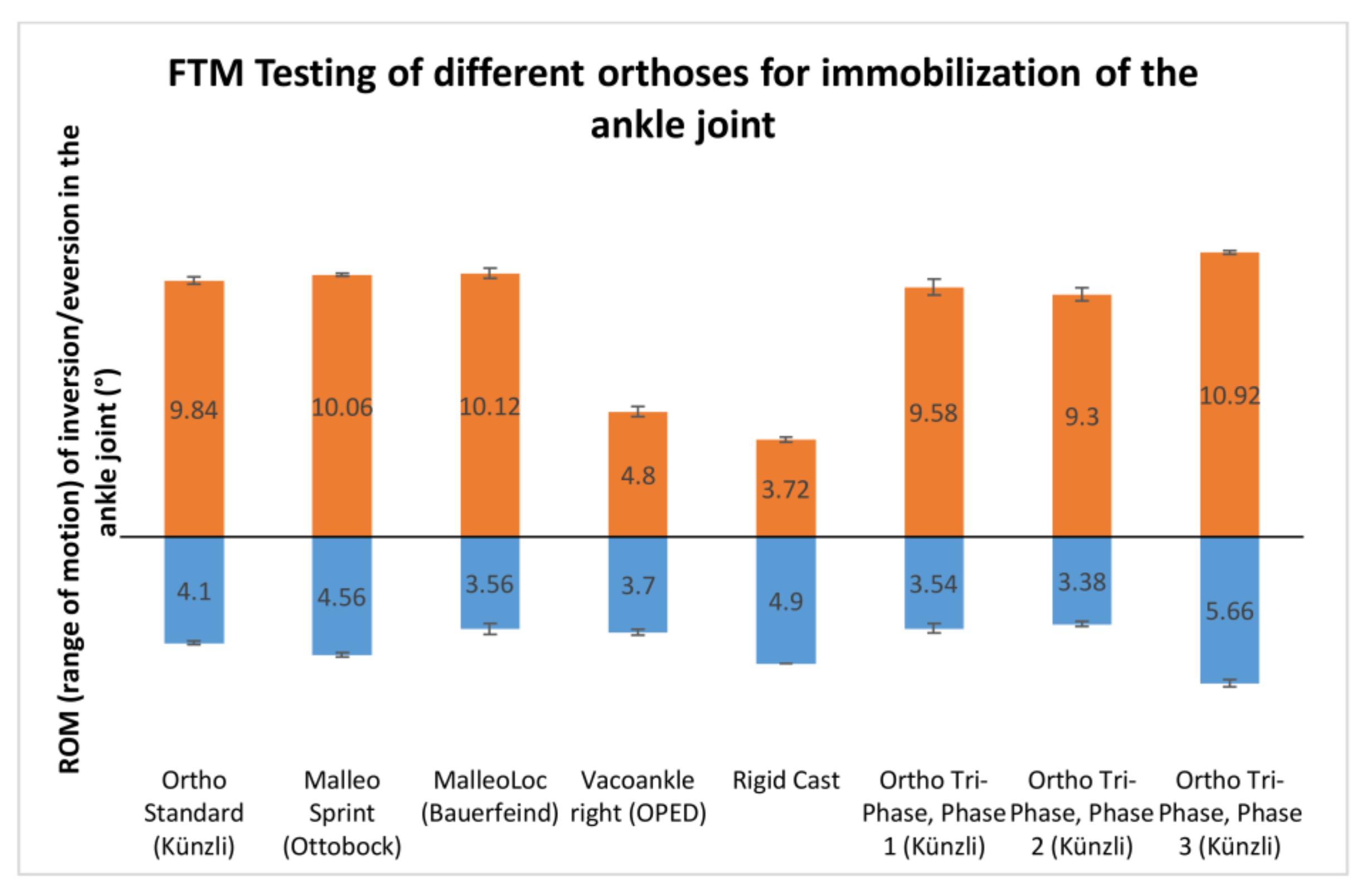
| Dorsiflexion | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Plantarflexion | Ortho Standard (Künzli) | MalleoSprint (Ottobock) | MalleoLoc (Bauerfeind) | VACOankle (OPED) | Rigid Cast | Ortho Tri-Phase 1 (Künzli) | Ortho Tri-Phase 2 (Künzli) | Ortho Tri-Phase 3 (Künzli) | |
| Ortho Standard (Künzli) | 0.000 | 0.034 | 0.000 | 0.000 | 0.000 | 1.000 | 0.000 | ||
| MalleoSprint (Ottobock) | 0.000 | 0.000 | 0.000 | 0.000 | 0.003 | 0.000 | 0.000 | ||
| MalleoLoc (Bauerfeind) | 0.016 | 0.152 | 0.000 | 0.000 | 0.000 | 0.139 | 0.000 | ||
| VACOankle right (OPED) | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | ||
| Rigid Cast | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | ||
| Ortho Tri-Phase Phase 1 (Künzli) | 0.666 | 0.003 | 1.000 | 0.000 | 0.000 | 0.000 | 0.000 | ||
| Ortho Tri-Phase Phase 2 (Künzli) | 0.000 | 1.000 | 0.042 | 0.000 | 0.000 | 0.001 | 0.000 | ||
| Ortho Tri-Phase Phase 3 (Künzli) | 0.000 | 0.000 | 0.000 | 0.006 | 0.000 | 0.000 | 0.000 | ||
| Inversion | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Eversion | Ortho Standard (Künzli) | MalleoSprint (Ottobock) | MalleoLoc (Bauerfeind) | VACOankle (OPED) | Rigid Cast | Ortho Tri-Phase 1 (Künzli) | Ortho Tri-Phase 2 (Künzli) | Ortho Tri-Phase 3 (Künzli) | |
| Ortho Standard (Künzli) | 1.000 | 1.000 | 0.000 | 0.000 | 1.000 | 0.004 | 0.000 | ||
| MalleoSprint (Ottobock) | 0.000 | 1.000 | 0.000 | 0.000 | 0.016 | 0.000 | 0.000 | ||
| MalleoLoc (Bauerfeind) | 0.000 | 0.000 | 0.000 | 0.000 | 0.004 | 0.000 | 0.000 | ||
| VACOankle right (OPED) | 0.001 | 0.000 | 1.000 | 0.000 | 0.000 | 0.000 | 0.000 | ||
| Rigid Cast | 0.000 | 0.010 | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | ||
| Ortho Tri-Phase Phase 1 (Künzli) | 0.000 | 0.000 | 1.000 | 1.000 | 0.000 | 1.000 | 0.000 | ||
| Ortho Tri-Phase Phase 2 (Künzli) | 0.000 | 0.000 | 1.000 | 0.020 | 0.000 | 1.000 | 0.000 | ||
| Ortho Tri-Phase Phase 3 (Künzli) | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | 0.000 | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Thiele, F.; Schuhmacher, S.; Schwaller, C.; Plüss, S.; Rhiner, J.; List, R.; Lorenzetti, S. Restrictions in the Ankle Sagittal- and Frontal-Plane Range of Movement during Simulated Walking with Different Types of Orthoses. J. Funct. Morphol. Kinesiol. 2018, 3, 21. https://doi.org/10.3390/jfmk3020021
Thiele F, Schuhmacher S, Schwaller C, Plüss S, Rhiner J, List R, Lorenzetti S. Restrictions in the Ankle Sagittal- and Frontal-Plane Range of Movement during Simulated Walking with Different Types of Orthoses. Journal of Functional Morphology and Kinesiology. 2018; 3(2):21. https://doi.org/10.3390/jfmk3020021
Chicago/Turabian StyleThiele, Frank, Sebastian Schuhmacher, Christoph Schwaller, Stefan Plüss, Joël Rhiner, Renate List, and Silvio Lorenzetti. 2018. "Restrictions in the Ankle Sagittal- and Frontal-Plane Range of Movement during Simulated Walking with Different Types of Orthoses" Journal of Functional Morphology and Kinesiology 3, no. 2: 21. https://doi.org/10.3390/jfmk3020021
APA StyleThiele, F., Schuhmacher, S., Schwaller, C., Plüss, S., Rhiner, J., List, R., & Lorenzetti, S. (2018). Restrictions in the Ankle Sagittal- and Frontal-Plane Range of Movement during Simulated Walking with Different Types of Orthoses. Journal of Functional Morphology and Kinesiology, 3(2), 21. https://doi.org/10.3390/jfmk3020021






