SLAC and SNAC Wrist: The Top Five Things That General Radiologists Need to Know
Abstract
1. Introduction
2. The Top 5 Things That General Radiologists Need to Know
2.1. Definition—Pathogenesis
2.2. Clinical Picture and Physical Examination
2.3. Imaging Diagnosis
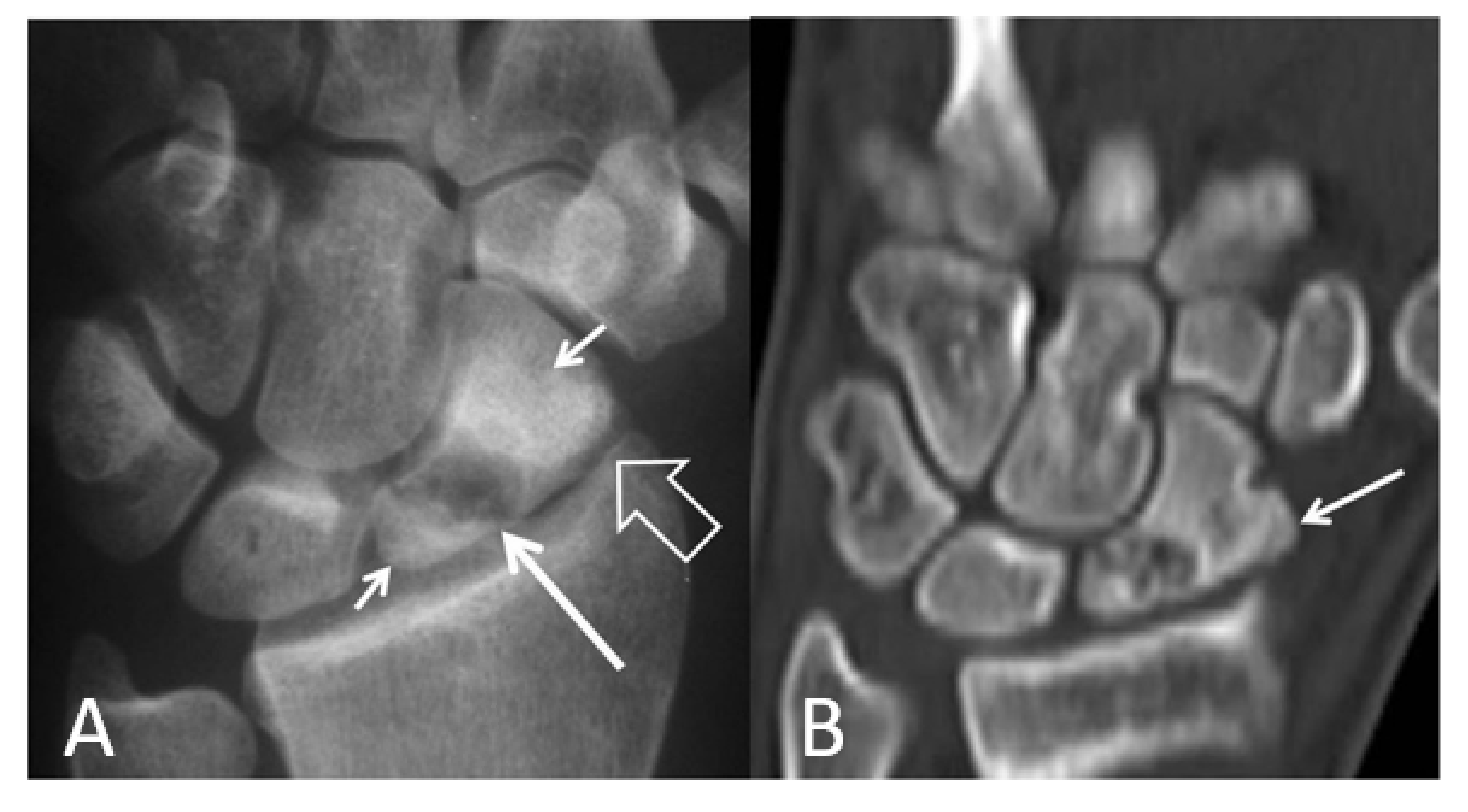
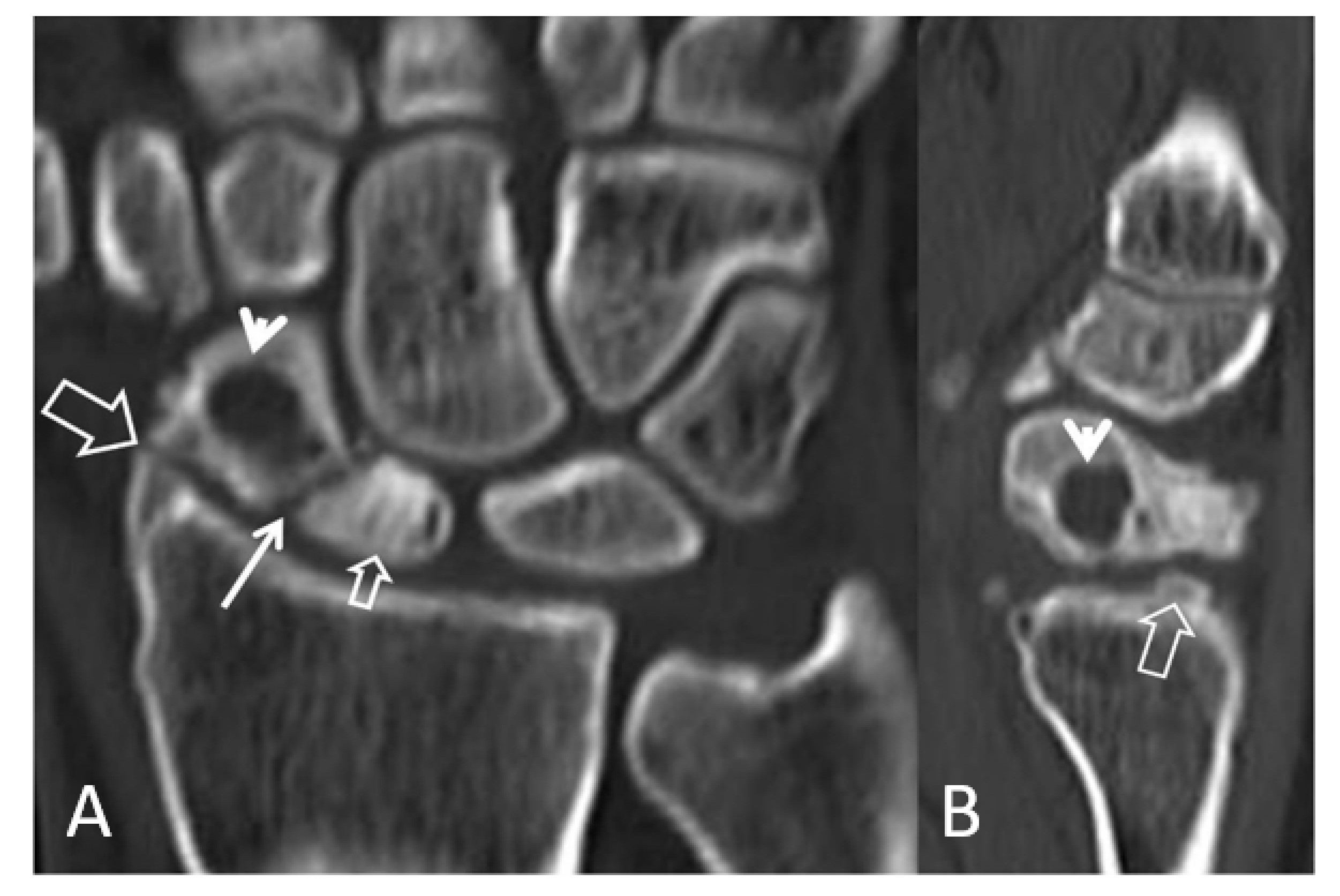
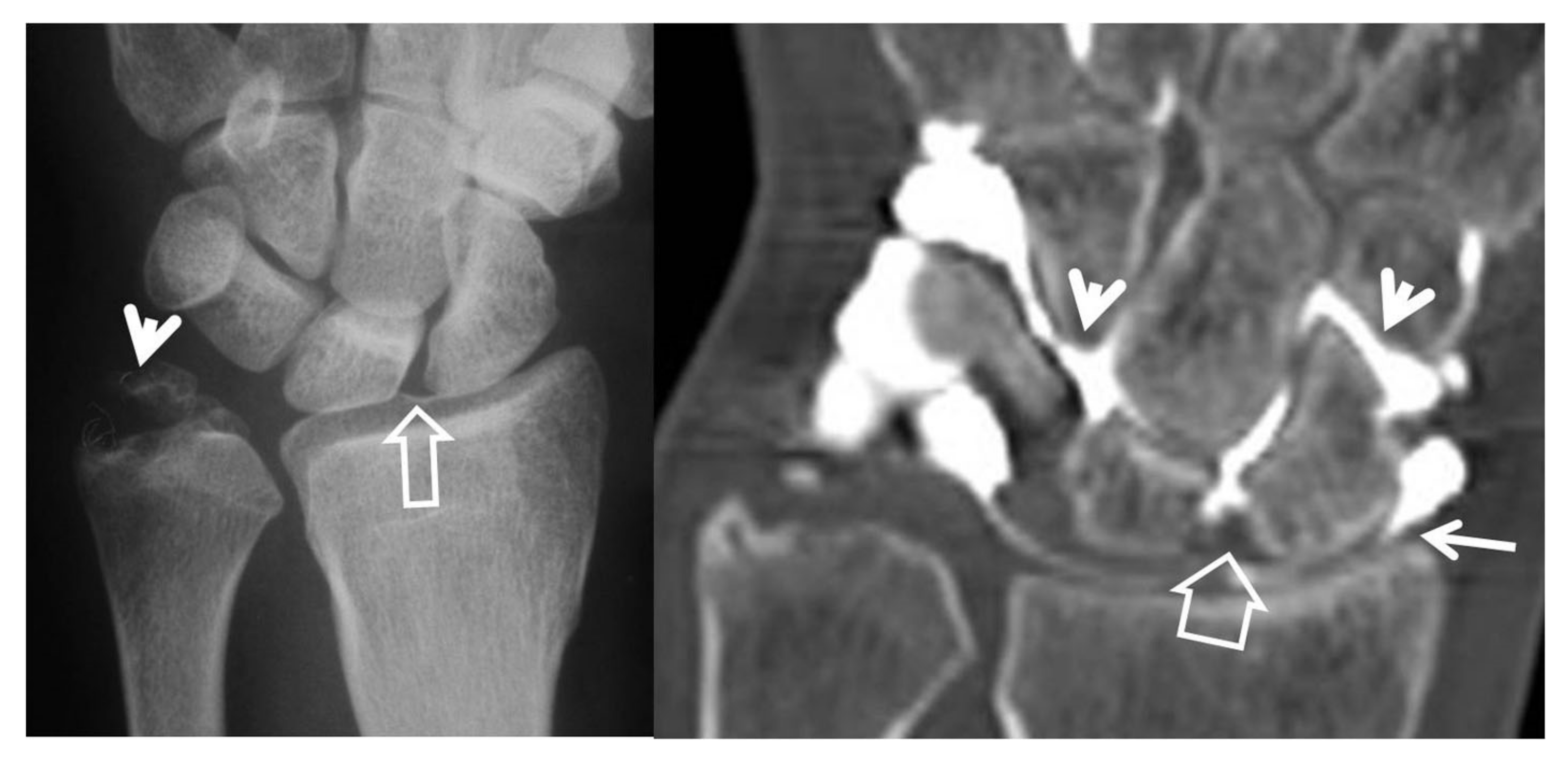
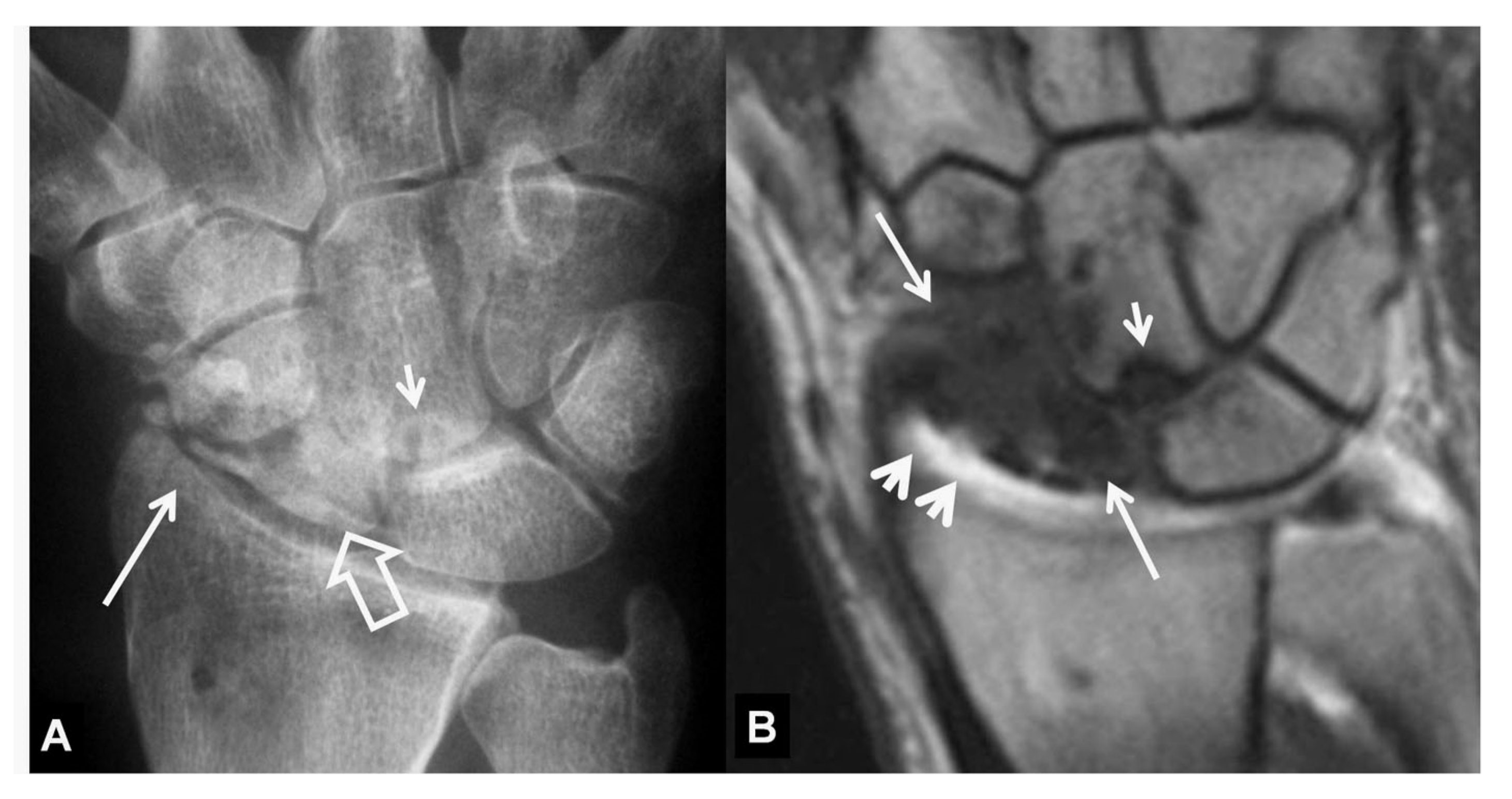
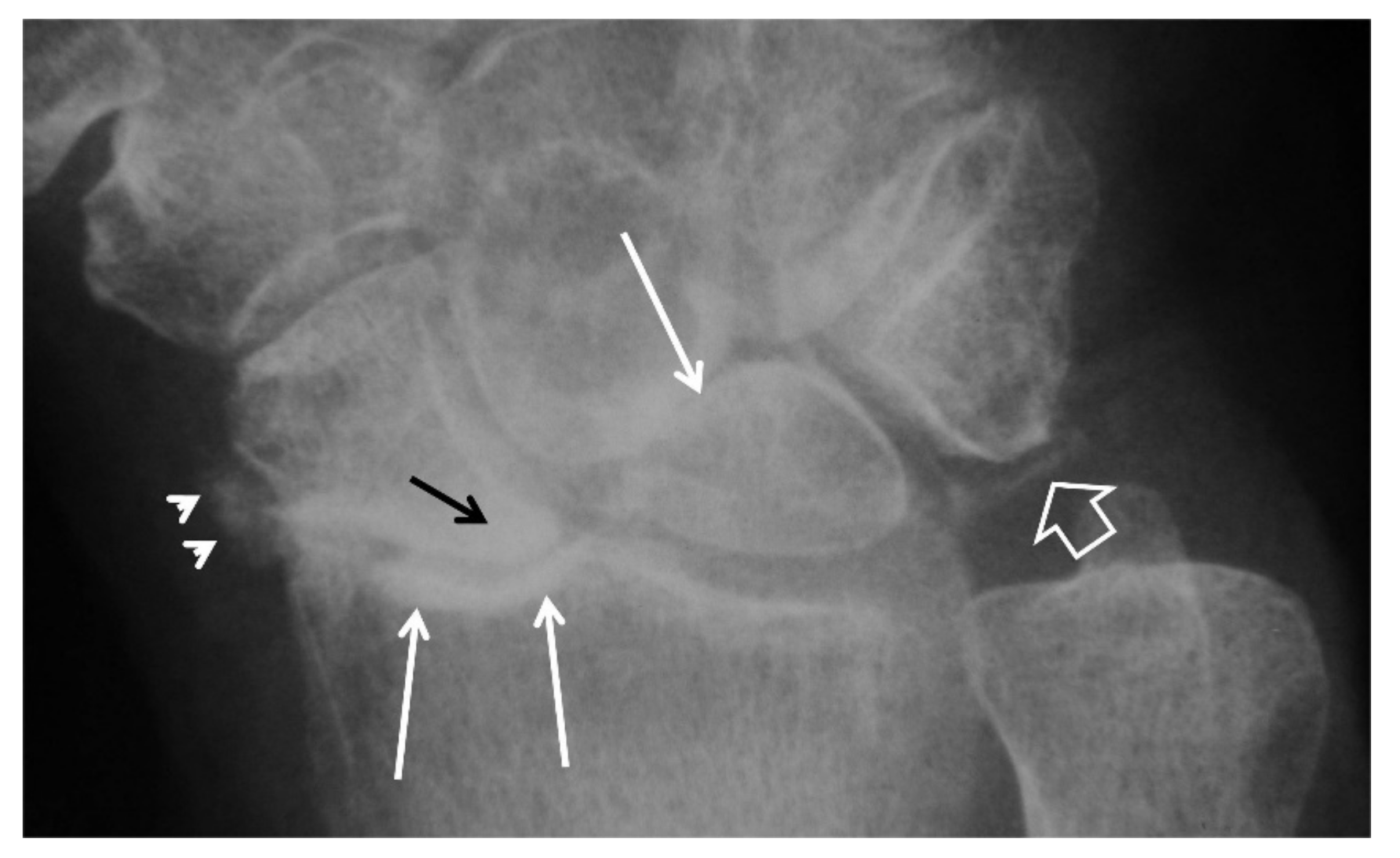
2.3.1. Radiographs
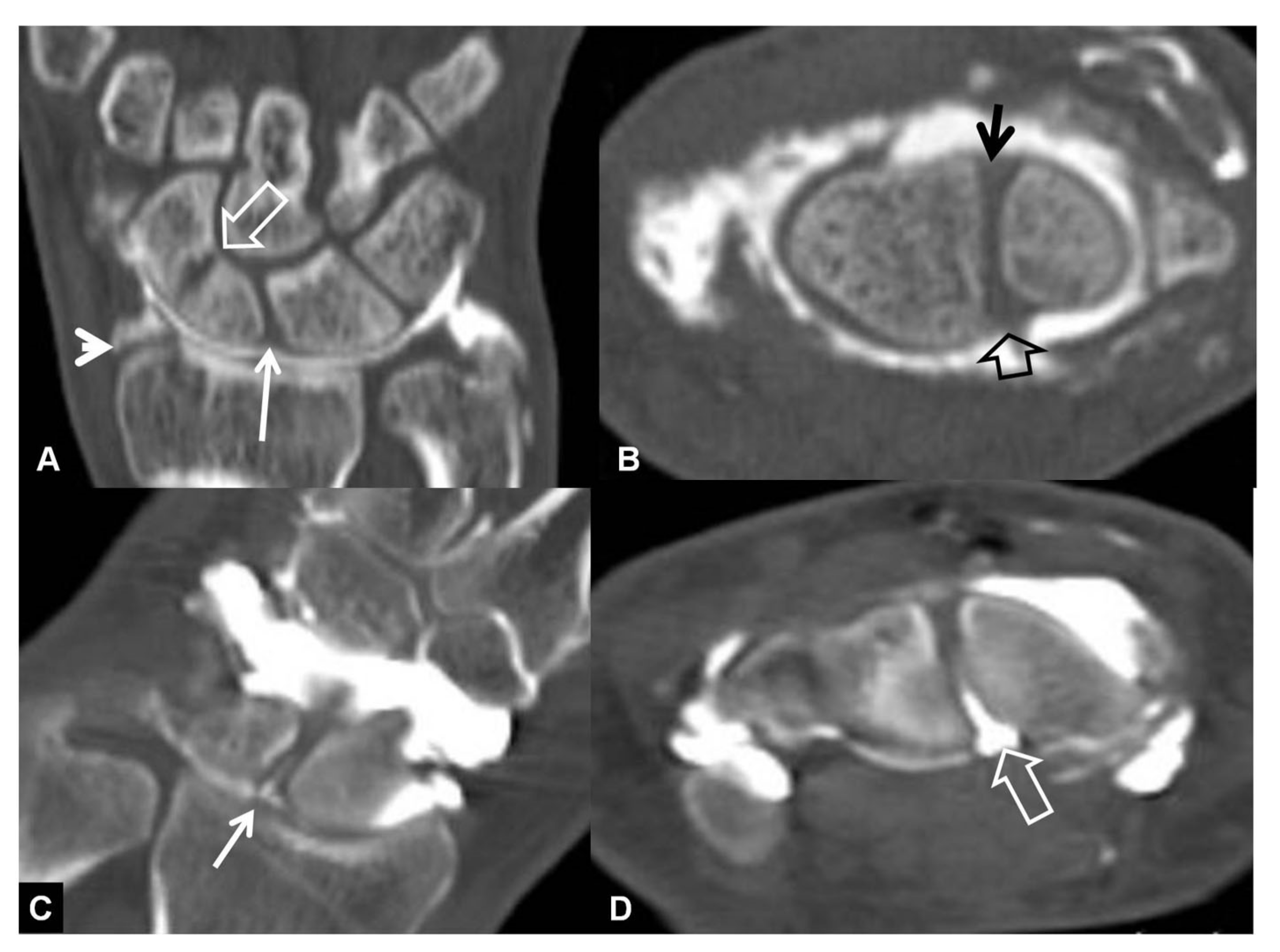
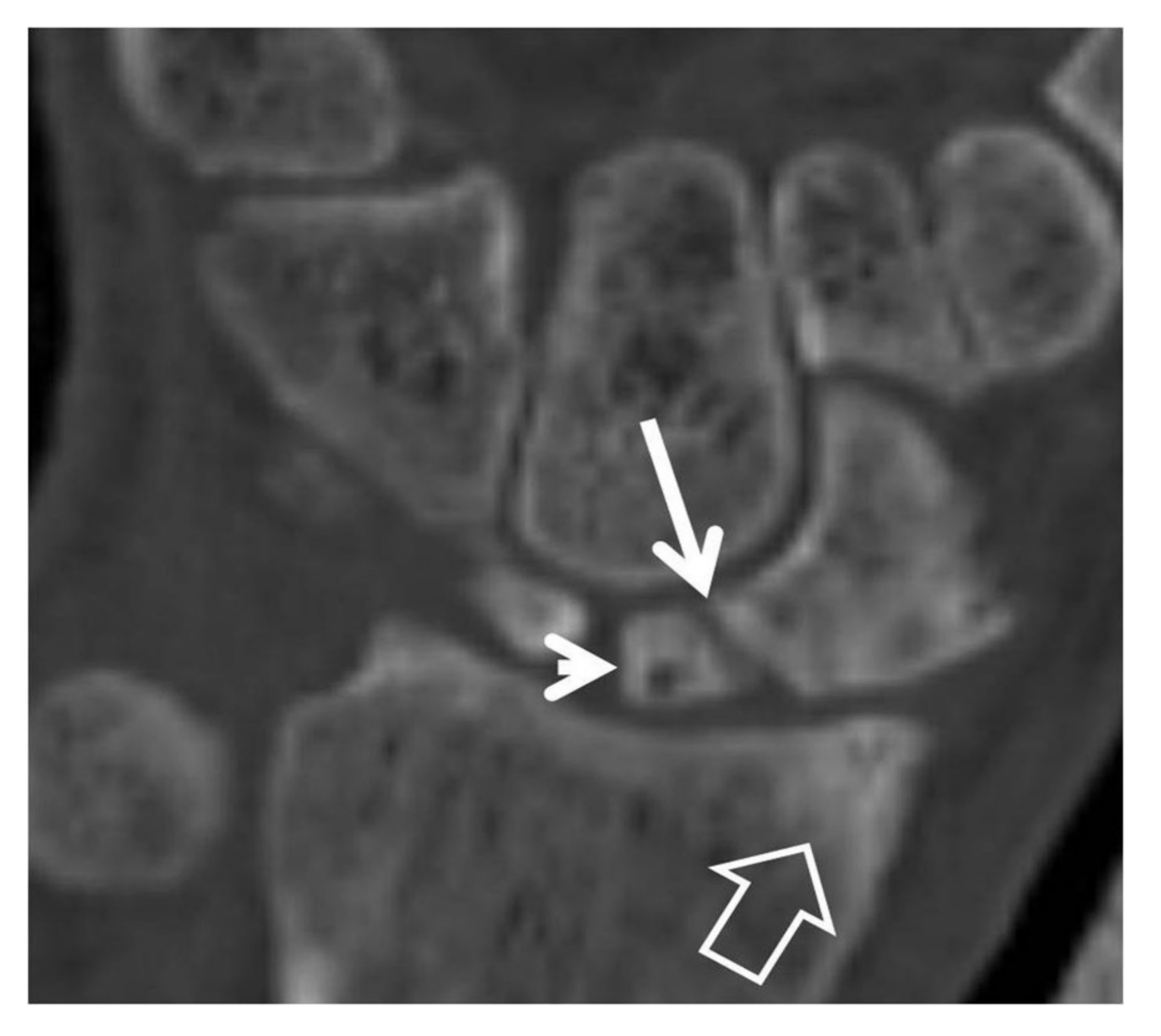
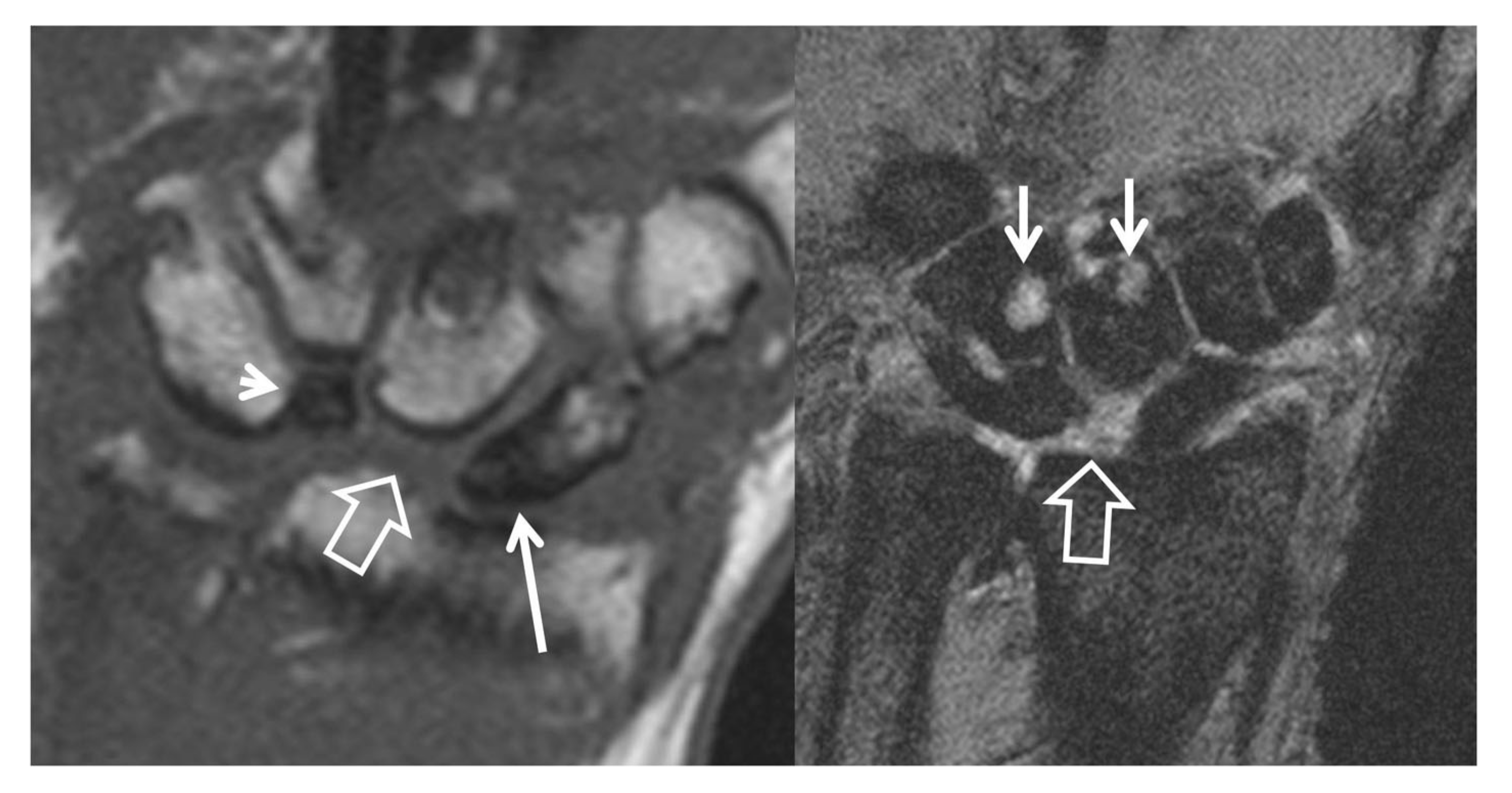
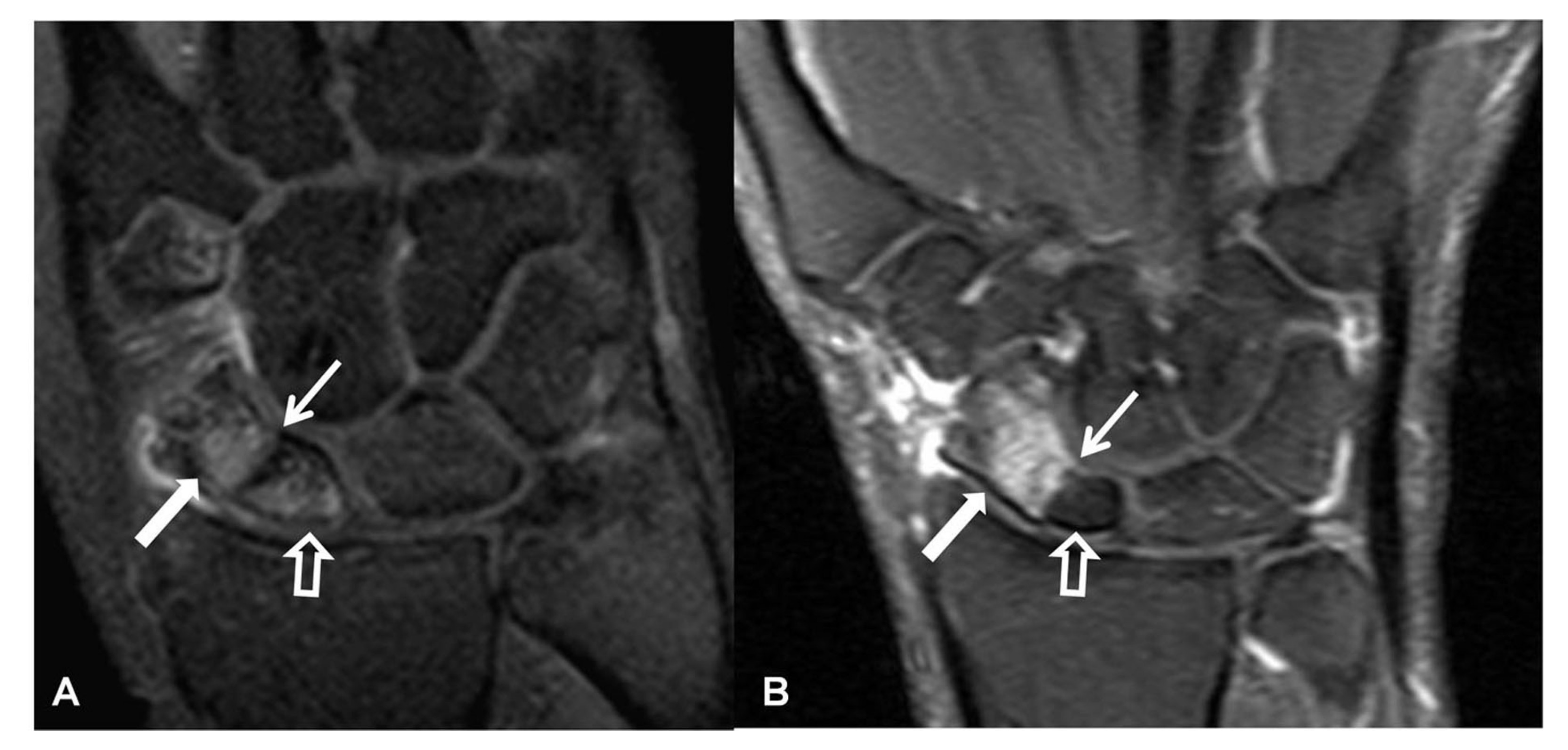
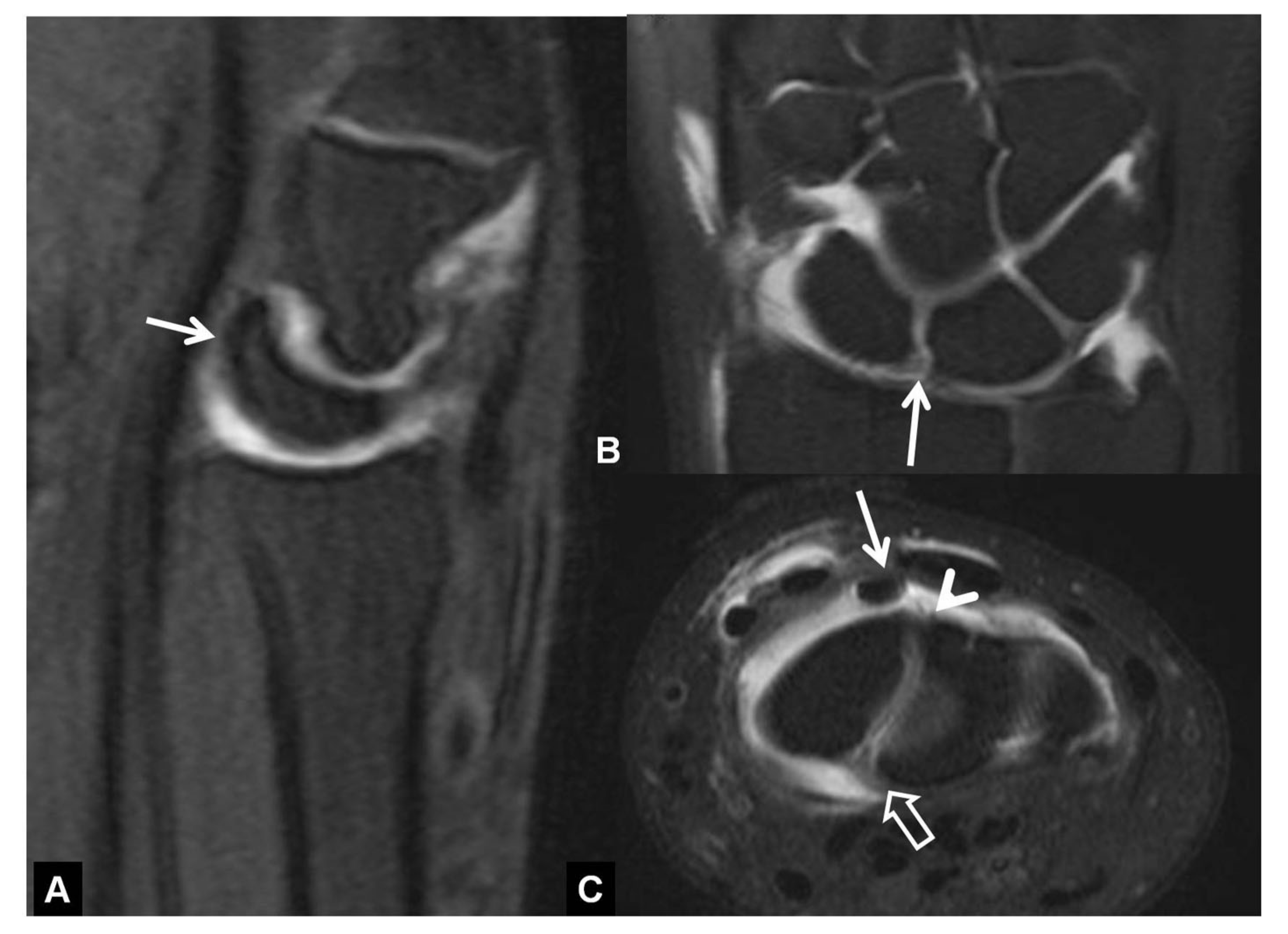
2.3.2. Computed Tomography/CT-Arthrography
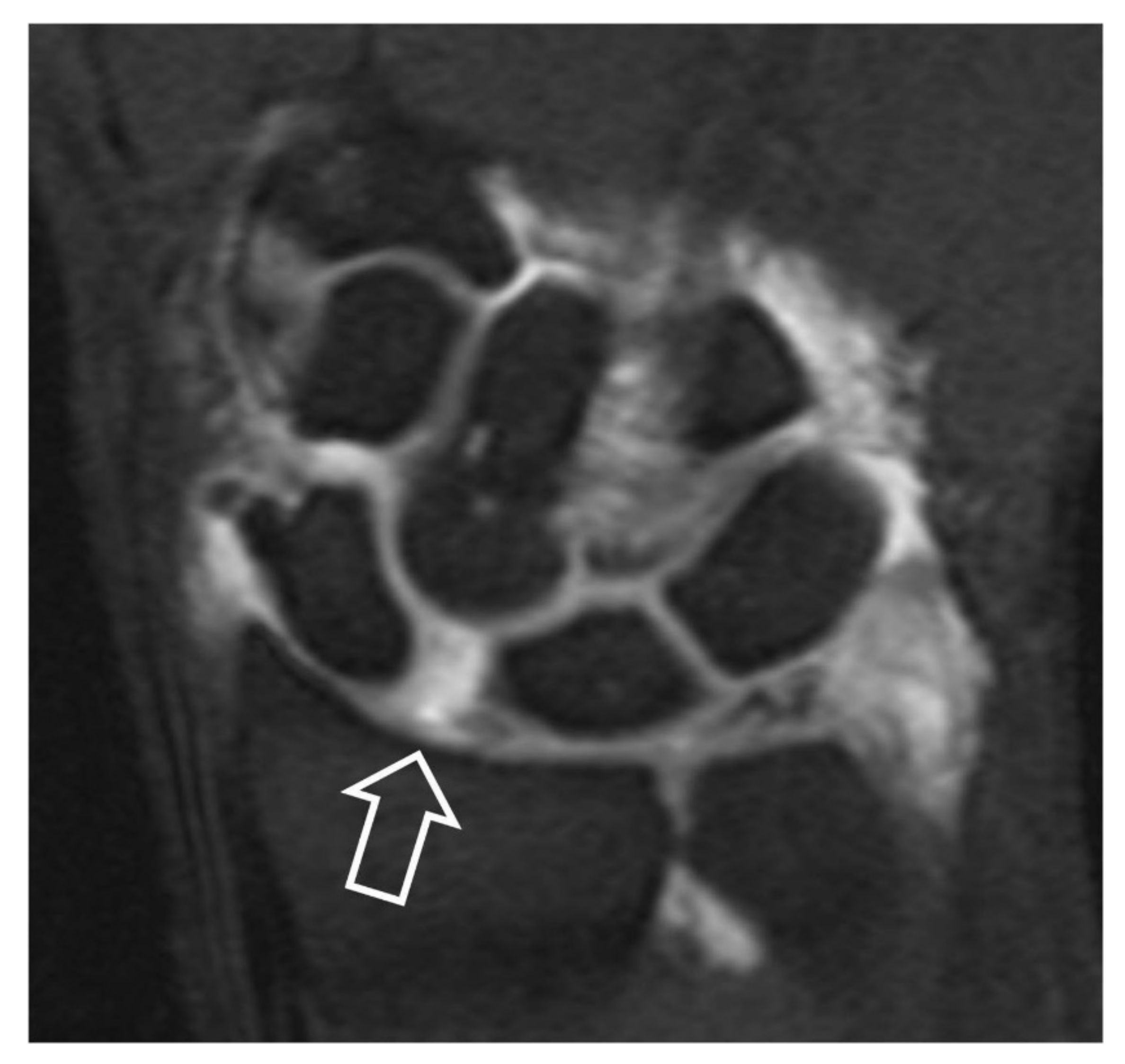
2.3.3. Magnetic Resonance Imaging/MRI-Arthrography
2.4. Differential Diagnosis
2.5. Treatment
3. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Tischler, B.T.; Diaz, L.E.; Murakami, A.M.; Roemer, F.W.; Goud, A.R.; Arndt, W.F., 3rd; Guermazi, A. Scapholunate advanced collapse: A pictorial review. Insights Imaging 2014, 5, 407–417. [Google Scholar] [CrossRef] [PubMed]
- Vender, M.I.; Watson, H.K.; Wiener, B.D.; Black, D.M. Degenerative change in symptomatic scaphoid nonunion. J. Hand Surg. 1987, 12, 514–519. [Google Scholar] [CrossRef]
- Trehan, S.K.; Lee, S.K.; Wolfe, S.W. Scapholunate advanced collapse: Nomenclature and differential diagnosis. J. Hand Surg. 2015, 40, 2085–2089. [Google Scholar] [CrossRef] [PubMed]
- Brenner, L.H. Degenerative disorders of the wrist. J. Hand Surg. 1985, 10, 1002–1006. [Google Scholar]
- Laulan, J.; Marteau, E.; Bacle, G. Wrist osteoarthritis. Orthop. Traumatol. Surg. Res. 2015, 101, S1–S9. [Google Scholar] [CrossRef]
- Belhaouane, R.; Lebeau, N.; Maes-Clavier, C.; Hustin, C.; Krief, E.; Bonnaire, B.; Warin, M.; Rotari, V.; David, E. Reproducibility of X-rays and CT arthrography in SLAC, SNAC, SCAC wrists. Hand Surg. Rehabil. 2016, 35, 393–400. [Google Scholar] [CrossRef]
- Li, A.; Lee, S.; Rancy, S.; Burge, A.; Potter, H.G.; Wolfe, S.W. Comparison of magnetic resonance imaging and radiographs for evaluation of carpal osteoarthritis. J. Wrist Surg. 2016, 6, 120–125. [Google Scholar] [CrossRef]
- Goldfarb, C.A.; Yin, Y.; Gilula, L.A.; Fisher, A.J.; Boyer, M.I. Wrist fractures: What the clinician wants to know. Radiology 2001, 219, 11–28. [Google Scholar] [CrossRef]
- Crema, M.D.; Phan, C.; Miquel, A.; Quach, C.; Arrive, L.; Menu, Y. MDCT arthrography assessment of scaphoid nonunion advanced collapse: Distribution of cartilage damage and relationship with scaphoid nonunion features. Skelet. Radiol. 2018, 47, 1157–1165. [Google Scholar] [CrossRef]
- Crema, M.D.; Zentner, J.; Guermazi, A.; Jomaah, N.; Marra, M.D.; Roemer, F. Scapholunate advanced collapse and scaphoid nonunion advanced collapse: MDCT arthrography features. AJR Am. J. Roentgenol. 2012, 199, 202–207. [Google Scholar] [CrossRef] [PubMed]
- Maizlin, Z.V.; Brown, J.A.; Clement, J.J.; Brown, J.A. MR arthrography of the wrist: Controversies and concepts. Hand 2009, 4, 66–73. [Google Scholar] [CrossRef]
- Johnson, D.; Stevens, K.J.; Riley, G.; Shapiro, L.; Yoshioka, H.; Gold, G.E. Approach to MR Imaging of the Elbow and Wrist. Magn. Reason. Imaging Clin. 2015, 23, 355–366. [Google Scholar] [CrossRef] [PubMed]
- Cerezal, L.; Abascal, F.; García-Valtuille, R.; Del Pinal, F. Wrist MR arthrography: How, why, when. Radiol. Clin. 2005, 43, 709–731. [Google Scholar] [CrossRef]
- Romano, S. Arthrose non traumatique du poignet: La chondrocalcinose. Chir. Main 2003, 22, 285–292. [Google Scholar] [CrossRef]
- Kahloune, M.; Libouton, X.; Omoumi, P.; Larbi, A. Osteoarthritis and scapholunate instability in chondrocalcinosis. Diagn. Interv. Imaging 2015, 96, 115–119. [Google Scholar] [CrossRef]
- Taniguchi, Y.; Tamaki, T.; Honda, T.; Yoshida, M. Rotatory subluxation of the scaphoid in Kienböck’s disease is not a cause of scapholunate advanced collapse (SLAC) in the wrist. J. Bone Jt. Surg. Br. Vol. 2002, 84, 684–687. [Google Scholar] [CrossRef]
- Kim, S.R. Successful treatment of scapholunate advanced collapse: A case report. Clin. Case Rep. 2019, 7, 1230–1232. [Google Scholar] [CrossRef]
- Mayoly, A.; Iniesta, A.; Curvale, C.; Kachouh, N.; Jaloux, C.; Eraud, J.; Vogtensperger, M.; Veran, J.; Grimaud, F.; Jouve, E.; et al. Development of autologous platelet-rich plasma mixed-microfat as an advanced therapy medicinal product for intra-articular injection of radio-carpal osteoarthritis: From validation data to preliminary clinical results. Int. J. Mol. Sci. 2019, 20, 1111. [Google Scholar] [CrossRef]
- Strauch, R.J. Scapholunate advanced collapse and scaphoid nonunion advanced collapse arthritis: Update on evaluation and treatment. J. Hand Surg. 2011, 36, 729–735. [Google Scholar] [CrossRef] [PubMed]
- Purnell, A.C.; Wollstein, R. Treatment of Stage I and II scapholunate advanced collapse (SLAC) wrist. Curr. Rheumatol. Rev. 2013, 8, 258–260. [Google Scholar] [CrossRef]
- Dacho, A.K.; Baumeister, S.; Germann, G.; Sauerbier, M. Comparison of proximal row carpectomy and midcarpal arthrodesis for the treatment of scaphoid nonunion advanced collapse (SNAC-wrist) and scapholunate advanced collapse (SLAC-wrist) in stage II. J. Plast. Reconstr. Aesthetic Surg. 2008, 61, 1210–1218. [Google Scholar] [CrossRef] [PubMed]
- Siegel, J.M.; Ruby, L.K. Midcarpal arthrodesis. J. Hand Surg. 1996, 21, 179–182. [Google Scholar] [CrossRef]
- Odella, S.; Querenghi, A.M.; Locatelli, F.M.; Dacatra, U.; Creta, E.; Pierluigi, T. Locking dorsal plate in four-bone arthrodesis in SLAC and SNAC 3 wrist. Joints 2018, 6, 37–41. [Google Scholar] [CrossRef]
- Wei, D.H.; Tang, P. The treatment of wrist osteoarthritis, SLAC wrist Grade 3-4. Curr. Rheumatol. Rev. 2013, 8, 261–265. [Google Scholar] [CrossRef]
- Rimokh, J.; Benazech, B.; Lebeau, N.; Haddad, B.; Moughabghab, M.; David, E. Clinical and radiological outcomes of 40 cases of SLAC and SNAC wrist treated by four-corner arthrodesis with locking plate. Hand Surg. Rehabil. 2020, 39, 36–40. [Google Scholar] [CrossRef]
| Scapholunate ligament rupture |
| Pyrophosphate leading to SLL 1 tear |
| Idiopathic avascular scaphoid necrosis |
| Avascular necrosis of the lunate |
| Involving the radioscaphoid or capitolunate joint |
| Stages | Vender et al. on SNAC | Watson and Ballet on SNAC and SLAC |
|---|---|---|
| Stage I | Involvement of the joint between radial styloid and distal scaphoid fragment | Articulation between radial styloid and scaphoid is involved |
| Stage II | Involvement of the joint among proximal scaphoid fragment and capitate data | Plus, proximal radioscaphoid joint |
| Stage III | Radioscaphoid, scaphoid-capitate and capitolunate articulation is affected | Plus, capitolunate articulation |
| Comparison | Radiographs | CT-CTA | MRI-MRa |
|---|---|---|---|
| PROS | Widely available | Evaluates cartilage, ligament lesions | Depicts osseous/soft |
| Low-cost | Spatial ability | Evaluates bone marrow | |
| Quick-minimal motion artifacts | Estimates fracture time | ||
| Detects established osteoarthritis | Post-operative monitoring | Assesses ligaments, cartilage and sub- chondral lesions | |
| Estimates bone fractures | |||
| CONS | Dorsal displacement of the scaphoid is difficult to assess | No standardized interpretation | Time-consuming/ motion artifacts |
| Osteoarthritic changes are obvious only when they are well established | Partial tear of SLL not well detected | ||
| Only indirectly detects cartilage damage via space joint narrowing | Radiation | Not feasible in the presence of metallic objects |
| Stage I | Stage II | Stage III |
|---|---|---|
| Radial styloidectomy | Proximal row carpectomy | Proximal row carpectomy |
| Scapholunate reconstruction | Midcarpal arthrodesis | Four corner arthrodesis |
| Distal scaphoid excision | Total wrist denervation |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kompoliti, E.; Prodromou, M.; Karantanas, A.H. SLAC and SNAC Wrist: The Top Five Things That General Radiologists Need to Know. Tomography 2021, 7, 488-503. https://doi.org/10.3390/tomography7040042
Kompoliti E, Prodromou M, Karantanas AH. SLAC and SNAC Wrist: The Top Five Things That General Radiologists Need to Know. Tomography. 2021; 7(4):488-503. https://doi.org/10.3390/tomography7040042
Chicago/Turabian StyleKompoliti, Eliza, Mikaella Prodromou, and Apostolos H. Karantanas. 2021. "SLAC and SNAC Wrist: The Top Five Things That General Radiologists Need to Know" Tomography 7, no. 4: 488-503. https://doi.org/10.3390/tomography7040042
APA StyleKompoliti, E., Prodromou, M., & Karantanas, A. H. (2021). SLAC and SNAC Wrist: The Top Five Things That General Radiologists Need to Know. Tomography, 7(4), 488-503. https://doi.org/10.3390/tomography7040042







