Insights from Second-Line Treatments for Idiopathic Dilated Cardiomyopathy
Abstract
1. Introduction
2. Methods
3. Results
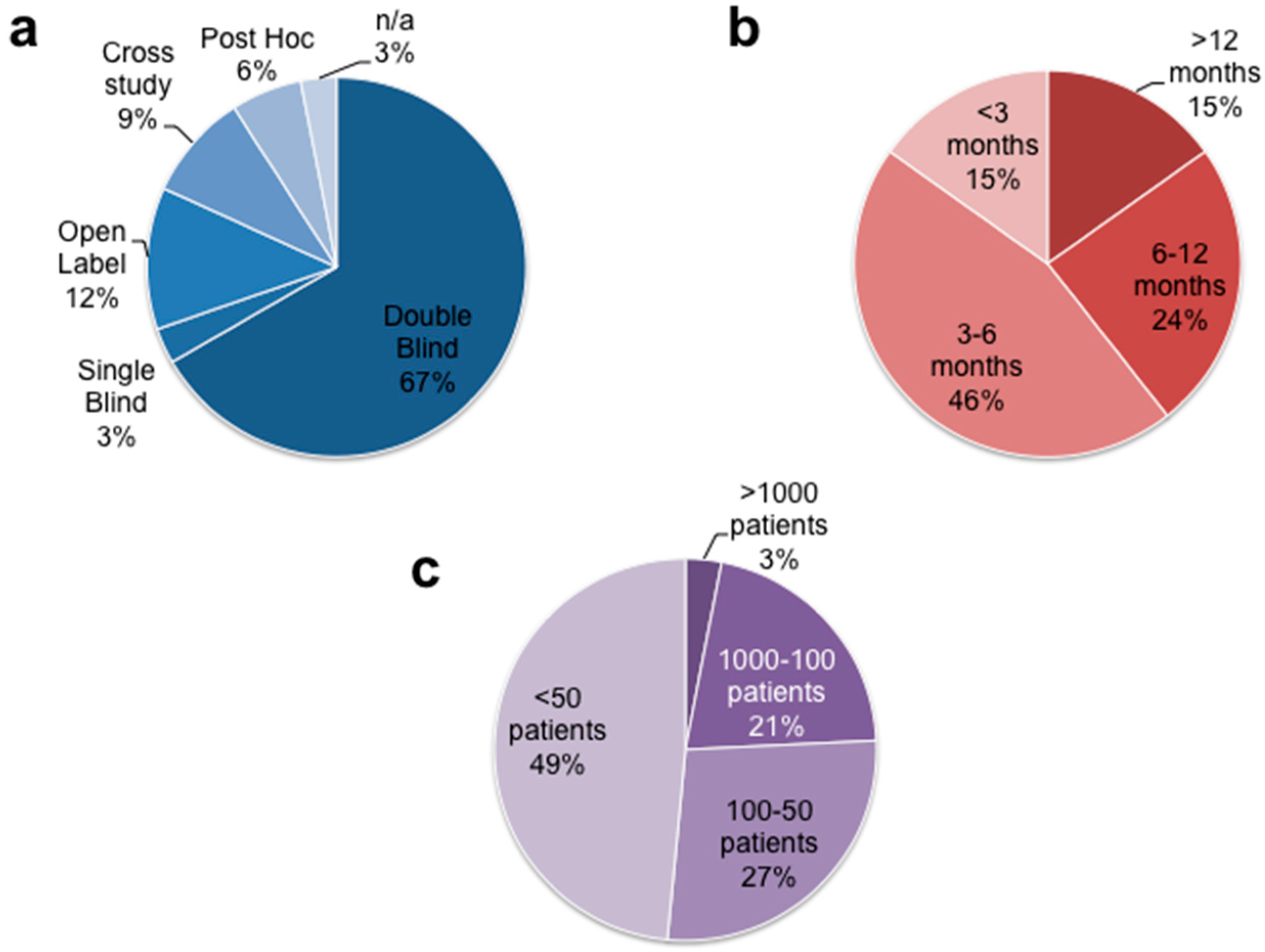
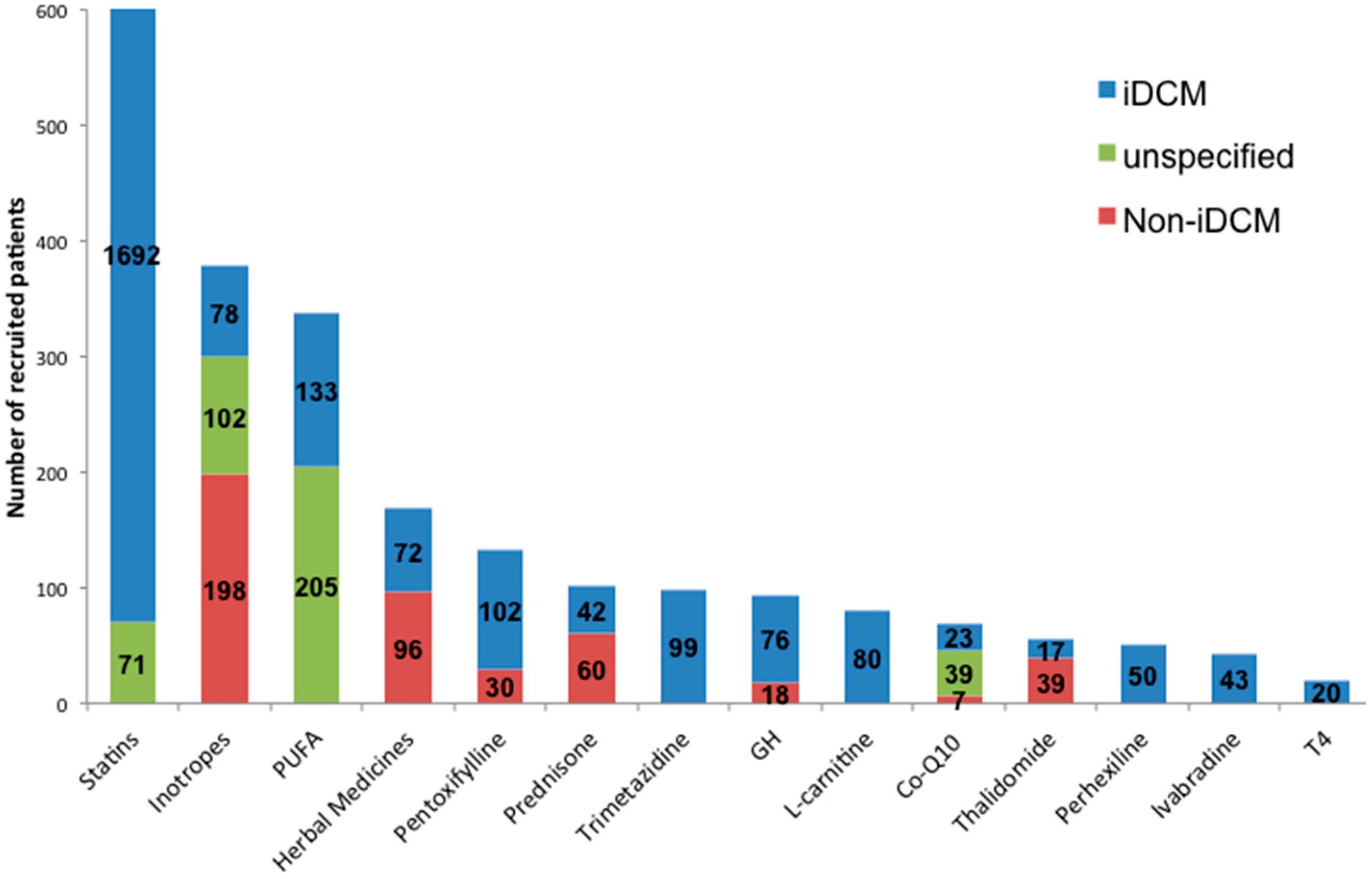
3.1. General Study Characteristics
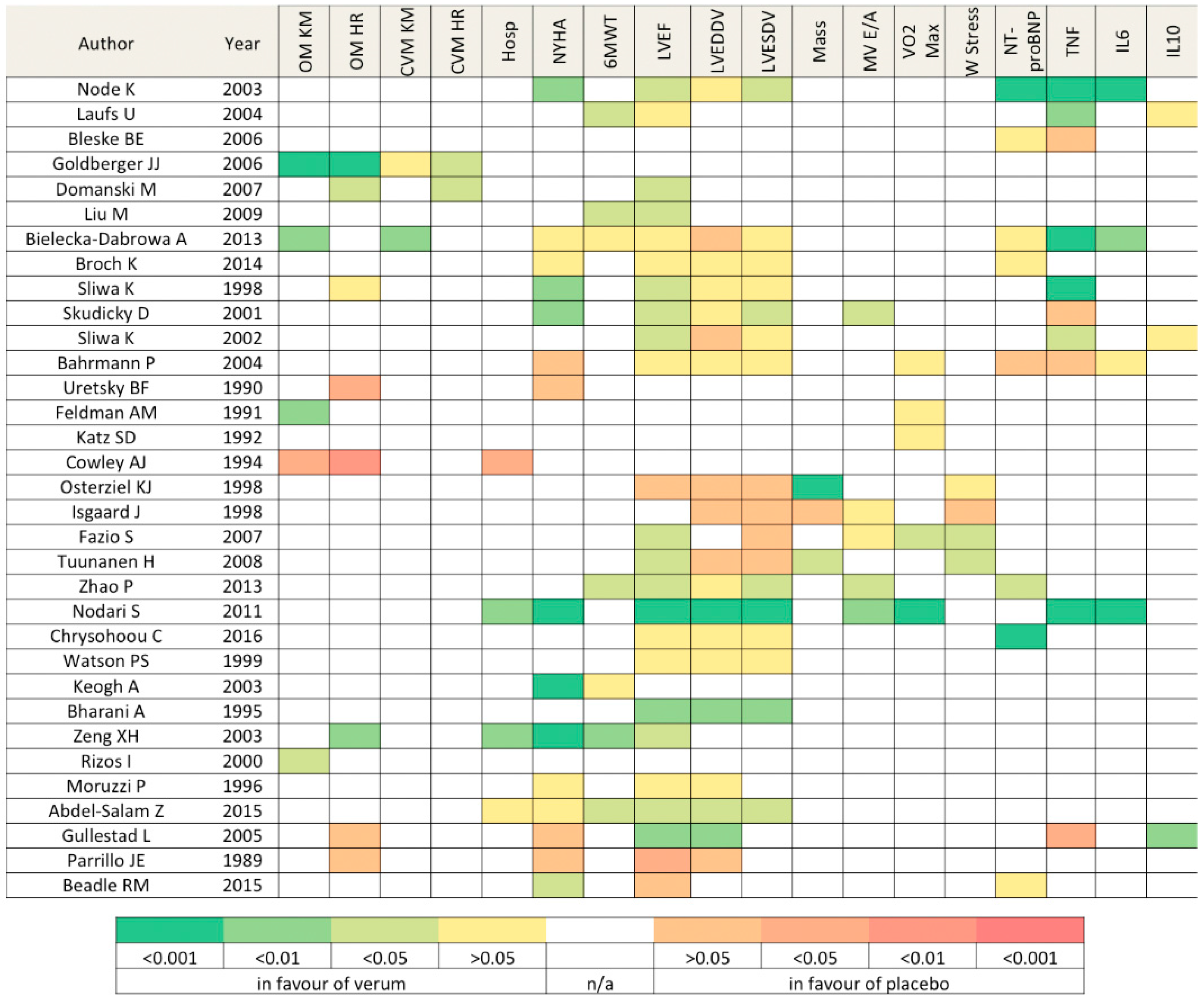
3.2. Overall Findings
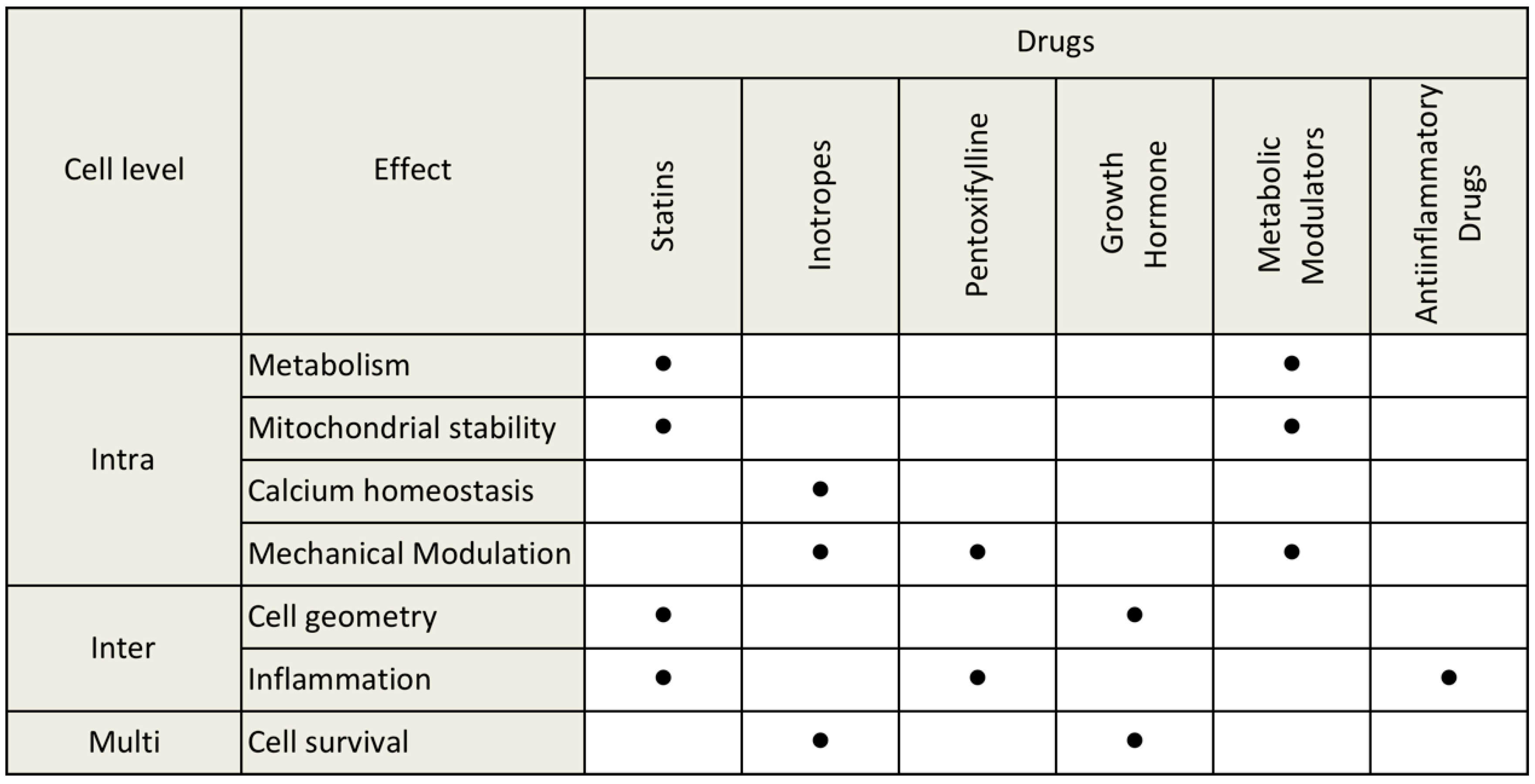
4. Discussion
4.1. Not All Statins Were Created Equal
4.2. Inflammation Resolution: Is It Worth?
4.3. Inotropism Manipulation: A Double-Edged Knife
4.4. Mitochondrion: A Hijacked Powerhouse
4.5. Growth Hormone: New Bricks for a Crumbling Heart?
4.6. A Challenging Equation
5. Conclusions
6. Limitations
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Elliott, P. Cardiomyopathy: Diagnosis and management of dilated cardiomyopathy. Heart 2000, 84, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Japp, A.G.; Gulati, A.; Cook, S.A.; Cowie, M.R.; Prasad, S.K. The Diagnosis and Evaluation of Dilated Cardiomyopathy. J. Am. Coll. Cardiol. 2016, 67, 2996–3010. [Google Scholar] [CrossRef] [PubMed]
- Pecini, R.; Moller, D.V.; Torp-Pedersen, C.; Hassager, C.; Kober, L. Heart failure etiology impacts survival of patients with heart failure. Int. J. Cardiol. 2011, 149, 211–215. [Google Scholar] [CrossRef] [PubMed]
- Kober, L.; Thune, J.J.; Nielsen, J.C.; Haarbo, J.; Videbæk, L.; Korup, E.; Jensen, G.; Hildebrandt, P.; Steffensen, F.H.; Bruun, N.E.; et al. Defibrillator Implantation in Patients with Nonischemic Systolic Heart Failure. N. Engl. J. Med. 2016, 375, 1221–1230. [Google Scholar] [CrossRef] [PubMed]
- Rose, E.A.; Gelijns, A.C.; Moskowitz, A.J.; Heitjan, D.F.; Stevenson, L.W.; Dembitsky, W.; Long, J.W.; Ascheim, D.D.; Tierney, A.R.; Levitan, R.G.; et al. Long-term use of a left ventricular assist device for end-stage heart failure. N. Engl. J. Med. 2001, 345, 1435–1443. [Google Scholar] [CrossRef] [PubMed]
- Slaughter, M.S.; Rogers, J.G.; Milano, C.A.; Russell, S.D.; Conte, J.V.; Feldman, D.; Sun, B.; Tatooles, A.J.; Delgado, R.M., 3rd; Long, J.W.; et al. Advanced heart failure treated with continuous-flow left ventricular assist device. N. Engl. J. Med. 2009, 361, 2241–2251. [Google Scholar] [CrossRef] [PubMed]
- Buckberg, G.; Athanasuleas, C.; Conte, J. Surgical ventricular restoration for the treatment of heart failure. Nat. Rev. Cardiol. 2012, 9, 703–716. [Google Scholar] [CrossRef] [PubMed]
- Bolli, R.; Ghafghazi, S. Current status of cell therapy for non-ischaemic cardiomyopathy: A brief overview. Eur. Heart J. 2015, 36, 2905–2908. [Google Scholar] [CrossRef] [PubMed]
- Weintraub, R.G.; Semsarian, C.; Macdonald, P. Dilated cardiomyopathy. Lancet 2017, 390, 400–414. [Google Scholar] [CrossRef]
- Node, K.; Fujita, M.; Kitakaze, M.; Hori, M.; Liao, J.K. Short-term statin therapy improves cardiac function and symptoms in patients with idiopathic dilated cardiomyopathy. Circulation 2003, 108, 839–843. [Google Scholar] [CrossRef] [PubMed]
- Laufs, U.; Wassmann, S.; Schackmann, S.; Heeschen, C.; Böhm, M.; Nickenig, G. Beneficial effects of statins in patients with non-ischemic heart failure. Z. Kardiol. 2004, 93, 103–108. [Google Scholar] [CrossRef] [PubMed]
- Bleske, B.E.; Nicklas, J.M.; Bard, R.L.; Brook, R.D.; Gurbel, P.A.; Bliden, K.P.; Rajagopalan, S.; Pitt, B. Neutral effect on markers of heart failure, inflammation, endothelial activation and function, and vagal tone after high-dose HMG-CoA reductase inhibition in non-diabetic patients with non-ischemic cardiomyopathy and average low-density lipoprotein level. J. Am. Coll. Cardiol. 2006, 47, 338–341. [Google Scholar] [CrossRef] [PubMed]
- Goldberger, J.J.; Subacius, H.; Schaechter, A.; Howard, A.; Berger, R.; Shalaby, A.; Levine, J.; Kadish, A.H.; DEFINITE Investigators. Effects of statin therapy on arrhythmic events and survival in patients with nonischemic dilated cardiomyopathy. J. Am. Coll. Cardiol. 2006, 48, 1228–1233. [Google Scholar] [CrossRef] [PubMed]
- Domanski, M.; Coady, S.; Fleg, J.; Tian, X.; Sachdev, V. Effect of statin therapy on survival in patients with nonischemic dilated cardiomyopathy (from the Beta-blocker Evaluation of Survival Trial [BEST]). Am. J. Cardiol. 2007, 99, 1448–1450. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.; Wang, F.; Wang, Y.; Jin, R. Atorvastatin improves endothelial function and cardiac performance in patients with dilated cardiomyopathy: The role of inflammation. Cardiovasc. Drugs Ther. 2009, 23, 369–376. [Google Scholar] [CrossRef] [PubMed]
- Bielecka-Dabrowa, A.; Mikhailidis, D.P.; Rizzo, M.; von Haeling, S.; Rysz, J.; Banach, M. The influence of atorvastatin on parameters of inflammation left ventricular function, hospitalizations and mortality in patients with dilated cardiomyopathy—5-year follow-up. Lipids Health Dis. 2013, 12, 47. [Google Scholar] [CrossRef] [PubMed]
- Broch, K.; Askevold, E.T.; Gjertsen, E.; Ueland, T.; Yndestad, A.; Godang, K.; Stueflotten, W.; Andreassen, J.; Svendsmark, R.; Smith, H.J.; et al. The effect of rosuvastatin on inflammation, matrix turnover and left ventricular remodeling in dilated cardiomyopathy: A randomized, controlled trial. PLoS ONE 2014, 9, e89732. [Google Scholar] [CrossRef] [PubMed]
- Sliwa, K.; Skudicky, D.; Candy, G.; Wisenbaugh, T.; Sareli, P. Randomised investigation of effects of pentoxifylline on left-ventricular performance in idiopathic dilated cardiomyopathy. Lancet 1998, 351, 1091–1093. [Google Scholar] [CrossRef]
- Skudicky, D.; Bergemann, A.; Sliwa, K.; Candy, G.; Sareli, P. Beneficial effects of pentoxifylline in patients with idiopathic dilated cardiomyopathy treated with angiotensin-converting enzyme inhibitors and carvedilol: Results of a randomized study. Circulation 2001, 103, 1083–1088. [Google Scholar] [CrossRef] [PubMed]
- Sliwa, K.; Woodwiss, A.; Candy, G.; Badenhorst, D.; Libhaber, C.; Norton, G.; Skudicky, D.; Sareli, P. Effects of pentoxifylline on cytokine profiles and left ventricular performance in patients with decompensated congestive heart failure secondary to idiopathic dilated cardiomyopathy. Am. J. Cardiol. 2002, 90, 1118–1122. [Google Scholar] [CrossRef]
- Bahrmann, P.; Hengst, U.M.; Richartz, B.M.; Figulla, H.R. Pentoxifylline in ischemic, hypertensive and idiopathic-dilated cardiomyopathy: Effects on left-ventricular function, inflammatory cytokines and symptoms. Eur. J. Heart Fail. 2004, 6, 195–201. [Google Scholar] [CrossRef] [PubMed]
- Uretsky, B.F.; Jessup, M.; Konstam, M.A.; Dec, W.; Leier, C.V.; Benotti, J.; Murali, S.; Herrman, H.C.; Sandberg, J.A. Multicenter trial of oral enoximone in patients with moderate to moderately severe congestive heart failure. Lack of benefit compared with placebo. Enoximone Multicenter Trial Group. Circulation 1990, 82, 774–780. [Google Scholar] [CrossRef] [PubMed]
- Feldman, A.M.; Baughman, K.L.; Lee, W.K.; Gottlieb, S.H.; Weiss, J.L.; Becker, L.C.; Strobeck, J.E. Usefulness of OPC-8212, a quinolinone derivative, for chronic congestive heart failure in patients with ischemic heart disease or idiopathic dilated cardiomyopathy. Am. J. Cardiol. 1991, 68, 1203–1210. [Google Scholar] [CrossRef]
- Katz, S.D.; Kubo, S.H.; Jessup, M.; Brozena, S.; Troha, J.M.; Wahl, J.; Cohn, J.N.; Sonnenblick, E.H.; LeJemtel, T.H. A multicenter, randomized, double-blind, placebo-controlled trial of pimobendan, a new cardiotonic and vasodilator agent, in patients with severe congestive heart failure. Am. Heart J. 1992, 123, 95–103. [Google Scholar] [CrossRef]
- Cowley, A.J.; Skene, A.M. Treatment of severe heart failure: Quantity or quality of life? A trial of enoximone. Enoximone Investigators. Br. Heart J. 1994, 72, 226–230. [Google Scholar] [CrossRef] [PubMed]
- Osterziel, K.J.; Strohm, O.; Schuler, J.; Friedrich, M.; Hänlein, D.; Willenbrock, R.; Anker, S.D.; Poole-Wilson, P.A.; Ranke, M.B.; Dietz, R. Randomised, double-blind, placebo-controlled trial of human recombinant growth hormone in patients with chronic heart failure due to dilated cardiomyopathy. Lancet 1998, 351, 1233–1237. [Google Scholar] [CrossRef]
- Isgaard, J.; Bergh, C.H.; Caidahl, K.; Lomsky, M.; Hjalmarson, A.; Bengtsson, B.A. A placebo-controlled study of growth hormone in patients with congestive heart failure. Eur. Heart J. 1998, 19, 1704–1711. [Google Scholar] [CrossRef] [PubMed]
- Fazio, S.; Palmieri, E.A.; Affuso, F.; Cittadini, A.; Castellano, G.; Russo, T.; Ruvolo, A.; Napoli, R.; Saccà, L. Effects of growth hormone on exercise capacity and cardiopulmonary performance in patients with chronic heart failure. J. Clin. Endocrinol. Metab. 2007, 92, 4218–4223. [Google Scholar] [CrossRef] [PubMed]
- Tuunanen, H.; Engblom, E.; Naum, A.; Nagren, K.; Scheinin, M.; Hesse, B.; Juhani Airaksinen, K.E.; Nuutila, P.; Iozzo, P.; Ukkonen, H.; et al. Trimetazidine, a metabolic modulator, has cardiac and extracardiac benefits in idiopathic dilated cardiomyopathy. Circulation 2008, 118, 1250–1258. [Google Scholar] [CrossRef] [PubMed]
- Zhao, P.; Zhang, J.; Yin, X.G.; Maharaj, P.; Narraindoo, P.; Cui, L.Q.; Tang, Y.S. The effect of trimetazidine on cardiac function in diabetic patients with idiopathic dilated cardiomyopathy. Life Sci. 2013, 92, 633–638. [Google Scholar] [CrossRef] [PubMed]
- Nodari, S.; Triggiani, M.; Campia, U.; Manerba, A.; Milesi, G.; Cesana, B.M.; Gheorghiade, M.; Dei Cas, L. Effects of n-3 polyunsaturated fatty acids on left ventricular function and functional capacity in patients with dilated cardiomyopathy. J. Am. Coll. Cardiol. 2011, 57, 870–879. [Google Scholar] [CrossRef] [PubMed]
- Chrysohoou, C.; Metallinos, G.; Georgiopoulos, G.; Mendrinos, D.; Papanikolaou, A.; Magkas, N.; Pitsavos, C.; Vyssoulis, G.; Stefanadis, G.; Tousoulis, D. Short term omega-3 polyunsaturated fatty acid supplementation induces favorable changes in right ventricle function and diastolic filling pressure in patients with chronic heart failure; A randomized clinical trial. Vascul. Pharmacol. 2016, 79, 43–50. [Google Scholar] [CrossRef] [PubMed]
- Watson, P.S.; Scalia, G.M.; Galbraith, A.; Burstow, D.J.; Bett, N.; Aroney, C.N. Lack of effect of coenzyme Q on left ventricular function in patients with congestive heart failure. J. Am. Coll. Cardiol. 1999, 33, 1549–1552. [Google Scholar] [CrossRef]
- Keogh, A.; Fenton, S.; Leslie, C.; Aboyoun, C.; Macdonald, P.; Zhao, Y.C.; Bailey, M.; Rosenfeldt, F. Randomised double-blind, placebo-controlled trial of coenzyme Q, therapy in class II and III systolic heart failure. Heart Lung Circ. 2003, 12, 135–141. [Google Scholar] [CrossRef] [PubMed]
- Zeng, X.H.; Zeng, X.J.; Li, Y.Y. Efficacy and safety of berberine for congestive heart failure secondary to ischemic or idiopathic dilated cardiomyopathy. Am. J. Cardiol. 2003, 92, 173–176. [Google Scholar] [CrossRef]
- Bharani, A.; Ganguly, A.; Bhargava, K.D. Salutary effect of Terminalia Arjuna in patients with severe refractory heart failure. Int. J. Cardiol. 1995, 49, 191–199. [Google Scholar] [CrossRef]
- Rizos, I. Three-year survival of patients with heart failure caused by dilated cardiomyopathy and l-carnitine administration. Am. Heart J. 2000, 139 Pt 3, S120–S123. [Google Scholar] [CrossRef] [PubMed]
- Moruzzi, P.; Doria, E.; Agostoni, P.G. Medium-term effectiveness of l-thyroxine treatment in idiopathic dilated cardiomyopathy. Am. J. Med. 1996, 101, 461–467. [Google Scholar] [CrossRef]
- Abdel-Salam, Z.; Rayan, M.; Saleh, A.; Abdel-Barr, M.G.; Hussain, M.; Nammas, W. I(f) current inhibitor ivabradine in patients with idiopathic dilated cardiomyopathy: Impact on the exercise tolerance and quality of life. Cardiol. J. 2015, 22, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Gullestad, L.; Ueland, T.; Fjeld, J.G.; Holt, E.; Gundersen, T.; Breivik, K.; Skardal, R.; Kjekshus, J.; Andreassen, A.; Kjekshus, E.; et al. Effect of thalidomide on cardiac remodeling in chronic heart failure: Results of a double-blind, placebo-controlled study. Circulation 2005, 112, 3408–3414. [Google Scholar] [CrossRef] [PubMed]
- Parrillo, J.E.; Cunnion, R.E.; Epstein, S.E.; Parker, M.M.; Suffredini, A.F.; Brenner, M.; Schaer, G.L.; Palmieri, S.T.; Cannon, R.O., 3rd; et al. A prospective, randomized, controlled trial of prednisone for dilated cardiomyopathy. N. Engl. J. Med. 1989, 321, 1061–1068. [Google Scholar] [CrossRef] [PubMed]
- Beadle, R.M.; Williams, L.K.; Kuehl, M.; Bowater, S.; Abozguia, K.; Leyva, F.; Yousef, Z.; Wagenmakers, A.; Thies, F.; Horowitz, J.; et al. Improvement in cardiac energetics by perhexiline in heart failure due to dilated cardiomyopathy. JACC Heart Fail. 2015, 3, 202–211. [Google Scholar] [CrossRef] [PubMed]
- Chien, K.R. Stress pathways and heart failure. Cell 1999, 98, 555–558. [Google Scholar] [CrossRef]
- Tsutamoto, T.; Sakai, H.; Ibe, K.; Yamaji, M.; Kawahara, C.; Nakae, I.; Fujii, M.; Yamamoto, T.; Horie, M. Effect of atorvastatin vs. rosuvastatin on cardiac sympathetic nerve activity in non-diabetic patients with dilated cardiomyopathy. Circ. J. 2011, 75, 2160–2166. [Google Scholar] [CrossRef] [PubMed]
- Oesterle, A.; Laufs, U.; Liao, J.K. Pleiotropic Effects of Statins on the Cardiovascular System. Circ. Res. 2017, 120, 229–243. [Google Scholar] [CrossRef] [PubMed]
- Sawada, N.; Li, Y.; Liao, J.K. Novel aspects of the roles of Rac1 GTPase in the cardiovascular system. Curr. Opin. Pharmacol. 2010, 10, 116–121. [Google Scholar] [CrossRef] [PubMed]
- Cho, K.J.; Hill, M.M.; Chigurupati, S.; Du, G.; Parton, R.G.; Hancock, J.F. Therapeutic levels of the hydroxmethylglutaryl-coenzyme A reductase inhibitor lovastatin activate ras signaling via phospholipase D2. Mol. Cell. Biol. 2011, 31, 1110–1120. [Google Scholar] [CrossRef] [PubMed]
- Noma, K.; Oyama, N.; Liao, J.K. Physiological role of ROCKs in the cardiovascular system. Am. J. Physiol. Cell Physiol. 2006, 290, C661–C668. [Google Scholar] [CrossRef] [PubMed]
- Takemoto, M.; Node, K.; Nakagami, H.; Liao, Y.; Grimm, M.; Takemoto, Y.; Kitakaze, M.; Liao, J.K. Statins as antioxidant therapy for preventing cardiac myocyte hypertrophy. J. Clin. Investig. 2001, 108, 1429–1437. [Google Scholar] [CrossRef] [PubMed]
- Yano, M.; Matsumura, T.; Senokuchi, T.; Ishii, N.; Murata, Y.; Taketa, K.; Motoshima, H.; Taguchi, T.; Sonoda, K.; Kukidome, D.; et al. Statins activate peroxisome proliferator-activated receptor gamma through extracellular signal-regulated kinase 1/2 and p38 mitogen-activated protein kinase-dependent cyclooxygenase-2 expression in macrophages. Circ. Res. 2007, 100, 1442–1451. [Google Scholar] [CrossRef] [PubMed]
- Feldman, A.M.; Combes, A.; Wagner, D.; Kadakomi, T.; Kubota, T.; Li, Y.Y.; McTiernan, C. The role of tumor necrosis factor in the pathophysiology of heart failure. J. Am. Coll. Cardiol. 2000, 35, 537–544. [Google Scholar] [CrossRef]
- Levine, B.; Kalman, J.; Mayer, L.; Fillit, H.M.; Packer, M. Elevated circulating levels of tumor necrosis factor in severe chronic heart failure. N. Engl. J. Med. 1990, 323, 236–241. [Google Scholar] [CrossRef] [PubMed]
- Habib, F.M.; Springall, D.R.; Davies, G.J.; Oakley, C.M.; Yacoub, M.H.; Polak, J.M. Tumour necrosis factor and inducible nitric oxide synthase in dilated cardiomyopathy. Lancet 1996, 347, 1151–1155. [Google Scholar] [CrossRef]
- Torre-Amione, G.; Kapadia, S.; Benedict, C.; Oral, H.; Young, J.B.; Mann, D.L. Proinflammatory cytokine levels in patients with depressed left ventricular ejection fraction: A report from the Studies of Left Ventricular Dysfunction (SOLVD). J. Am. Coll. Cardiol. 1996, 27, 1201–1206. [Google Scholar] [CrossRef]
- Torre-Amione, G.; Kapadia, S.; Lee, J.; Durand, J.B.; Bies, R.D.; Young, J.B.; Mann, D.L. Tumor necrosis factor-alpha and tumor necrosis factor receptors in the failing human heart. Circulation 1996, 93, 704–711. [Google Scholar] [CrossRef] [PubMed]
- Bristow, M.R. Tumor necrosis factor-alpha and cardiomyopathy. Circulation 1998, 97, 1340–1341. [Google Scholar] [CrossRef] [PubMed]
- Kubota, T.; McTiernan, C.F.; Frye, C.S.; Slawson, S.E.; Lemster, B.H.; Koretsky, A.P.; Demetris, A.J.; Feldman, A.J. Dilated cardiomyopathy in transgenic mice with cardiac-specific overexpression of tumor necrosis factor-alpha. Circ. Res. 1997, 81, 627–635. [Google Scholar] [CrossRef] [PubMed]
- Chung, E.S.; Packer, M.; Lo, K.H.; Fasanmade, A.A.; Willerson, J.T.; ATTACH Investigators. Randomized, double-blind, placebo-controlled, pilot trial of infliximab, a chimeric monoclonal antibody to tumor necrosis factor-alpha, in patients with moderate-to-severe heart failure: Results of the anti-TNF Therapy Against Congestive Heart Failure (ATTACH) trial. Circulation 2003, 107, 3133–3140. [Google Scholar] [PubMed]
- Mann, D.L.; McMurray, J.J.; Packer, M.; Swedberg, K.; Borer, J.S.; Colucci, W.S.; Djian, J.; Drexler, H.; Feldman, A.; Kober, L.; et al. Targeted anticytokine therapy in patients with chronic heart failure: Results of the Randomized Etanercept Worldwide Evaluation (RENEWAL). Circulation 2004, 109, 1594–1602. [Google Scholar] [CrossRef] [PubMed]
- Yndestad, A.; Damas, J.K.; Oie, E.; Ueland, T.; Gullestad, L.; Aukrust, P. Role of inflammation in the progression of heart failure. Curr. Cardiol. Rep. 2007, 9, 236–241. [Google Scholar] [CrossRef] [PubMed]
- Wojnicz, R.; Nowalany-Kozielska, E.; Wojciechowska, C.; Gianowska, G.; Wilczewski, P.; Niklewski, T.; Zembala, M.; Polonski, L.; Rozek, M.M.; Wodniecki, J. Randomized, placebo-controlled study for immunosuppressive treatment of inflammatory dilated cardiomyopathy: Two-year follow-up results. Circulation 2001, 104, 39–45. [Google Scholar] [CrossRef] [PubMed]
- Colucci, W.S.; Wright, R.F.; Braunwald, E. New positive inotropic agents in the treatment of congestive heart failure. Mechanisms of action and recent clinical developments. 1. N. Engl. J. Med. 1986, 314, 290–299. [Google Scholar] [CrossRef] [PubMed]
- Colucci, W.S.; Wright, R.F.; Braunwald, E. New positive inotropic agents in the treatment of congestive heart failure. Mechanisms of action and recent clinical developments. 2. N. Engl. J. Med. 1986, 314, 349–358. [Google Scholar] [CrossRef] [PubMed]
- Pollesello, P.; Papp, Z.; Papp, J.G. Calcium sensitizers: What have we learned over the last 25 years? Int. J. Cardiol. 2016, 203, 543–548. [Google Scholar] [CrossRef] [PubMed]
- Gwathmey, J.K.; Copelas, L.; MacKinnon, R.; Schoen, F.J.; Feldman, M.D.; Grossman, W.; Morgan, J.P. Abnormal intracellular calcium handling in myocardium from patients with end-stage heart failure. Circ. Res. 1987, 61, 70–76. [Google Scholar] [CrossRef] [PubMed]
- Mercadier, J.J.; Lompré, A.M.; Duc, P.; Boheler, K.R.; Fraysse, J.B.; Wisnewsky, C.; Allen, P.D.; Komajda, M.; Schwartz, K. Altered sarcoplasmic reticulum Ca2(+)-ATPase gene expression in the human ventricle during end-stage heart failure. J. Clin. Investig. 1990, 85, 305–309. [Google Scholar] [CrossRef] [PubMed]
- Hasenfuss, G.; Reinecke, H.; Studer, R.; Meyer, M.; Pieske, B.; Holtz, J.; Holubarsch, C.; Posival, H.; Just, H.; Drexler, H. Relation between myocardial function and expression of sarcoplasmic reticulum Ca(2+)-ATPase in failing and nonfailing human myocardium. Circ. Res. 1994, 75, 434–442. [Google Scholar] [CrossRef] [PubMed]
- Dec, G.W.; Fifer, M.A.; Herrmann, H.C.; Cocca-Spofford, D.; Semigran, M.J. Long-term outcome of enoximone therapy in patients with refractory heart failure. Am. Heart J. 1993, 125 Pt 1, 423–429. [Google Scholar] [CrossRef]
- Brown, D.A.; Perry, J.B.; Allen, M.E.; Sabbah, H.N.; Stauffer, B.L.; Shaikh, S.R.; Cleland, J.G.; Colucci, W.S.; Butler, J.; Voors, A.A.; et al. Expert consensus document: Mitochondrial function as a therapeutic target in heart failure. Nat. Rev. Cardiol. 2017, 14, 238–250. [Google Scholar] [CrossRef] [PubMed]
- Hershberger, R.E.; Hedges, D.J.; Morales, A. Dilated cardiomyopathy: The complexity of a diverse genetic architecture. Nat. Rev. Cardiol. 2013, 10, 531–547. [Google Scholar] [CrossRef] [PubMed]
- Bione, S.; D’Adamo, P.; Maestrini, E.; Gedeon, A.K.; Bolhuis, P.A.; Toniolo, D. A novel X-linked gene, G4.5. is responsible for Barth syndrome. Nat. Genet. 1996, 12, 385–389. [Google Scholar] [CrossRef] [PubMed]
- Davila-Roman, V.G.; Vedala, G.; Herrero, P.; de las Fuentes, L.; Rogers, J.G.; Kelly, D.P.; Gropler, R.J. Altered myocardial fatty acid and glucose metabolism in idiopathic dilated cardiomyopathy. J. Am. Coll. Cardiol. 2002, 40, 271–277. [Google Scholar] [CrossRef]
- Sack, M.N.; Rader, T.A.; Park, S.; Bastin, J.; McCune, S.A.; Kelly, D.P. Fatty acid oxidation enzyme gene expression is downregulated in the failing heart. Circulation 1996, 94, 2837–2842. [Google Scholar] [CrossRef] [PubMed]
- Witteles, R.M.; Tang, W.H.; Jamali, A.H.; Chu, J.W.; Reaven, G.M.; Fowler, M.B. Insulin resistance in idiopathic dilated cardiomyopathy: A possible etiologic link. J. Am. Coll. Cardiol. 2004, 44, 78–81. [Google Scholar] [CrossRef] [PubMed]
- Sharma, A.; Fonarow, G.C.; Butler, J.; Ezekowitz, J.A.; Felker, G.M. Coenzyme Q10 and Heart Failure: A State-of-the-Art Review. Circ. Heart Fail. 2016, 9, e002639. [Google Scholar] [CrossRef] [PubMed]
- Olivetti, G.; Abbi, R.; Quaini, F.; Kajstura, J.; Cheng, W.; Nitahara, J.A.; Quaini, E.; Di Loreto, C.; Beltrami, C.A.; Krajewski, S.; et al. Apoptosis in the failing human heart. N. Engl. J. Med. 1997, 336, 1131–1141. [Google Scholar] [CrossRef] [PubMed]
- Narula, J.; Haider, N.; Virmani, R.; DiSalvo, T.G.; Kolodgie, F.D.; Hajjar, R.J.; Schmidt, U.; Semigran, M.J.; Dec, G.W.; Khaw, B.A. Apoptosis in myocytes in end-stage heart failure. N. Engl. J. Med. 1996, 335, 1182–1189. [Google Scholar] [CrossRef] [PubMed]
- Pluess, M.; Daeubler, G.; Dos Remedios, C.G.; Ehler, E. Adaptations of cytoarchitecture in human dilated cardiomyopathy. Biophys. Rev. 2015, 7, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Stewart, C.E.; Rotwein, P. Growth, differentiation, and survival: Multiple physiological functions for insulin-like growth factors. Physiol. Rev. 1996, 76, 1005–1026. [Google Scholar] [PubMed]
- Fazio, S.; Sabatini, D.; Capaldo, B.; Vigorito, C.; Giordano, A.; Guida, R.; Pardo, F.; Biondi, B.; Saccà, L. A preliminary study of growth hormone in the treatment of dilated cardiomyopathy. N. Engl. J. Med. 1996, 334, 809–814. [Google Scholar] [CrossRef] [PubMed]
- Dreifuss, P. Growth hormone in dilated cardiomyopathy (advantages and disadvantages). Eur. Heart J. 1999, 20, 243–244. [Google Scholar] [PubMed]
- Maison, P.; Chanson, P. Cardiac effects of growth hormone in adults with growth hormone deficiency: A meta-analysis. Circulation 2003, 108, 2648–2652. [Google Scholar] [CrossRef] [PubMed]
- Eryol, N.K.; Güven, M.; Topsakal, R.; Sungur, M.; Ozdogru, I.; Inanç, T.; Oguzhan, A. The effects of octreotide in dilated cardiomyopathy: An open-label trial in 12 patients. Jpn. Heart J. 2004, 45, 613–621. [Google Scholar] [CrossRef] [PubMed]
- Lamberts, S.W.; van der Lely, A.J.; de Herder, W.W.; Hofland, L.J. Octreotide. N. Engl. J. Med. 1996, 334, 246–254. [Google Scholar] [CrossRef] [PubMed]
- Bierer, B.E.; Crosas, M.; Pierce, H.H. Data Authorship as an Incentive to Data Sharing. N. Engl. J. Med. 2017, 376, 1684–1687. [Google Scholar] [CrossRef] [PubMed]
- Braunwald, E. The war against heart failure: The Lancet lecture. Lancet 2015, 385, 812–824. [Google Scholar] [CrossRef]
| Author | Year | No. of Patients iDCM/Total (%) | Study Type and Design | Active Drug Target | Follow-up (Months) | LVEF % | |
|---|---|---|---|---|---|---|---|
| Threshold | Baseline Average | ||||||
| Statins | |||||||
| Node K [10] | 2003 | 48/48 (100%) | Double blind | Simvastatin (10 mg/day) | 3 | 40 | 34 |
| Laufs U [11] | 2004 | 15/15 (100%) | Double blind | Cerivastatin (0.4 mg/day) | 5 | n/a | 40 |
| Bleske BE [12] | 2006 | 15/15 (100%) | Crossed | Atorvastatin (80 mg/day) | 3 | 45 | 25 |
| Goldberger JJ [13] | 2006 | 458/458 (100%) | Post hoc analysis | Any statin at any dosage | 24 | 35 | 20 |
| Domanski M [14] | 2007 | 1024/1024 (100%) | Post hoc analysis | Any statin at any dosage | 24 | 35 | 25 |
| Liu M [15] | 2009 | 64/64 (100%) | Double blind | Atorvastatin (10mg/day) | 3 | 40 | 35 |
| Bielecka-Dabrowa A [16] | 2013 | 68/68 (100%) | Open | Atorvastatin (10 or 20 mg/day) | 60 | n/a | 32 |
| Broch K [17] | 2014 | 71 unspecified | Double blind | Rosuvastatin (10 mg/day) | 6 | 40 | 36 |
| Pentoxifylline | |||||||
| Sliwa K [18] | 1998 | 28/28 (100%) | Double blind | Pentoxifylline (400 mg/tid) | 6 | 40 | 22 |
| Skudicky D [19] | 2001 | 39/39 (100%) | Double blind | Pentoxifylline (400 mg/tid) | 6 | 40 | 24 |
| Sliwa K [20] | 2002 | 18/18 (100%) | Double blind | Pentoxifylline (400 mg/tid) | 1 | 40 | 16 |
| Bahrmann P [21] | 2004 | 17/47 (36.2%) | Double blind | Pentoxifylline (600 mg/bid) | 6 | 40 | 29 |
| Inotropes | |||||||
| Uretsky BF [22] | 1990 | 102 unspecified | Double blind | Enoximone (100 or 150 mg/tid) | 4 | n/a | 22 |
| Feldman AM [23] | 1991 | 38/76 (50%) | Double blind | Vesnarinone (60 mg/day) | 3 | n/a | 24 |
| Katz SD [24] | 1992 | 14/49 (28.6%) | Double blind | Pimobendan (5 or 10 mg/day) | 3 | n/a | 19 |
| Cowley AJ [25] | 1994 | 26/151 (16.6%) | Double blind | Enoximone (50 or 100 mg/tid) | 12 | n/a | n/a |
| Growth Hormone (GH) | |||||||
| Osterziel KJ [26] | 1998 | 50/50 (100%) | Double blind | rhGH subq (2 IU/qd) | 3 | 45 | 26 |
| Isgaard J [27] | 1998 | 13/22 (59.1%) | Double blind | rhGH subq (to 4 IU/qd) | 3 | 45 | 30 |
| Fazio S [28] | 2007 | 13/22 (59.1%) | Double blind | rhGH subq (to 4 IU/qod) | 3 | 40 | 32 |
| Trimetazidine | |||||||
| Tuunanen H [29] | 2008 | 19/19 (100%) | Single blind | Trimetazidine (35 mg/bid) | 3 | 47 | 31 |
| Zhao P [30] | 2013 | 80/80 (100%) | Double blind | Trimetazidine(20mg/tid) | 6 | 40 | 34 |
| Polyunsaturated Fatty Acids (PUFAs) | |||||||
| Nodari S [31] | 2011 | 133/133 (100%) | Double blind | EPA/DHA850 mg/bid | 12 | 45 | 36 |
| Chrysohoou C [32] | 2016 | 205 unspecified | Open | PUFA 1000 mg/day | 6 | 40 | 28 |
| CoQ10 | |||||||
| Watson PS [33] | 1999 | 23/30 (76.7%) | Cross | CoQ10 (33 mg/tid) | 3 | 35 | 26 |
| Keogh A [34] | 2003 | 39 unspecified | Double blind | CoQ10 (150 mg/day) | 3 | 40 | n/a |
| Herbal Medications | |||||||
| Bharani A [35] | 1995 | 10/12 (83.3%) | Cross | Terminalia Arjuna (500 mg/tid) | 0.5 | n/a | 30 |
| Zeng XH [36] | 2003 | 62/156 (39.8%) | Double blind | Berberine (up to 0.5 g/qid) | 2 | n/a | 22 |
| L-carnitine | |||||||
| Rizos I [37] | 2000 | 80/80 (100%) | Open | L-carnitine (2 g/day) | 34 | n/a | 27 |
| Levotyroxine (T4) | |||||||
| Moruzzi P [38] | 1996 | 20/20 (100%) | n/a | Levotyroxine (100 ug/day) | 3 | 40 | 30 |
| Ivabradine | |||||||
| Abdel-Salam Z [39] | 2015 | 43/43 (100%) | Double blind | Ivabradine(2.5 mg/tid) | 3 | 40 | 34 |
| Thalidomide | |||||||
| Gullestad L [40] | 2005 | 17/56 (30.4%) | Double blind | Thalidomide (200 mg/qd) | 3 | 40 | 24 |
| Steroids | |||||||
| Parrillo JE [41] | 1989 | 42/102 (41.2%) | Open | Prednisone (60 mg/day) for 3 months | 15 | 35 | 18 |
| Perhexelline | |||||||
| Beadle RM [42] | 2015 | 50/50 (100%) | Double blind | Perhexelline (200 mg/day) | 2 | 40 | 27 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Luciani, M.; Del Monte, F. Insights from Second-Line Treatments for Idiopathic Dilated Cardiomyopathy. J. Cardiovasc. Dev. Dis. 2017, 4, 12. https://doi.org/10.3390/jcdd4030012
Luciani M, Del Monte F. Insights from Second-Line Treatments for Idiopathic Dilated Cardiomyopathy. Journal of Cardiovascular Development and Disease. 2017; 4(3):12. https://doi.org/10.3390/jcdd4030012
Chicago/Turabian StyleLuciani, Marco, and Federica Del Monte. 2017. "Insights from Second-Line Treatments for Idiopathic Dilated Cardiomyopathy" Journal of Cardiovascular Development and Disease 4, no. 3: 12. https://doi.org/10.3390/jcdd4030012
APA StyleLuciani, M., & Del Monte, F. (2017). Insights from Second-Line Treatments for Idiopathic Dilated Cardiomyopathy. Journal of Cardiovascular Development and Disease, 4(3), 12. https://doi.org/10.3390/jcdd4030012




