Frequency and Clinical Impact of Family History of Coronary Artery Disease in Patients with Vasospastic Angina
Abstract
1. Introduction
2. Materials and Methods
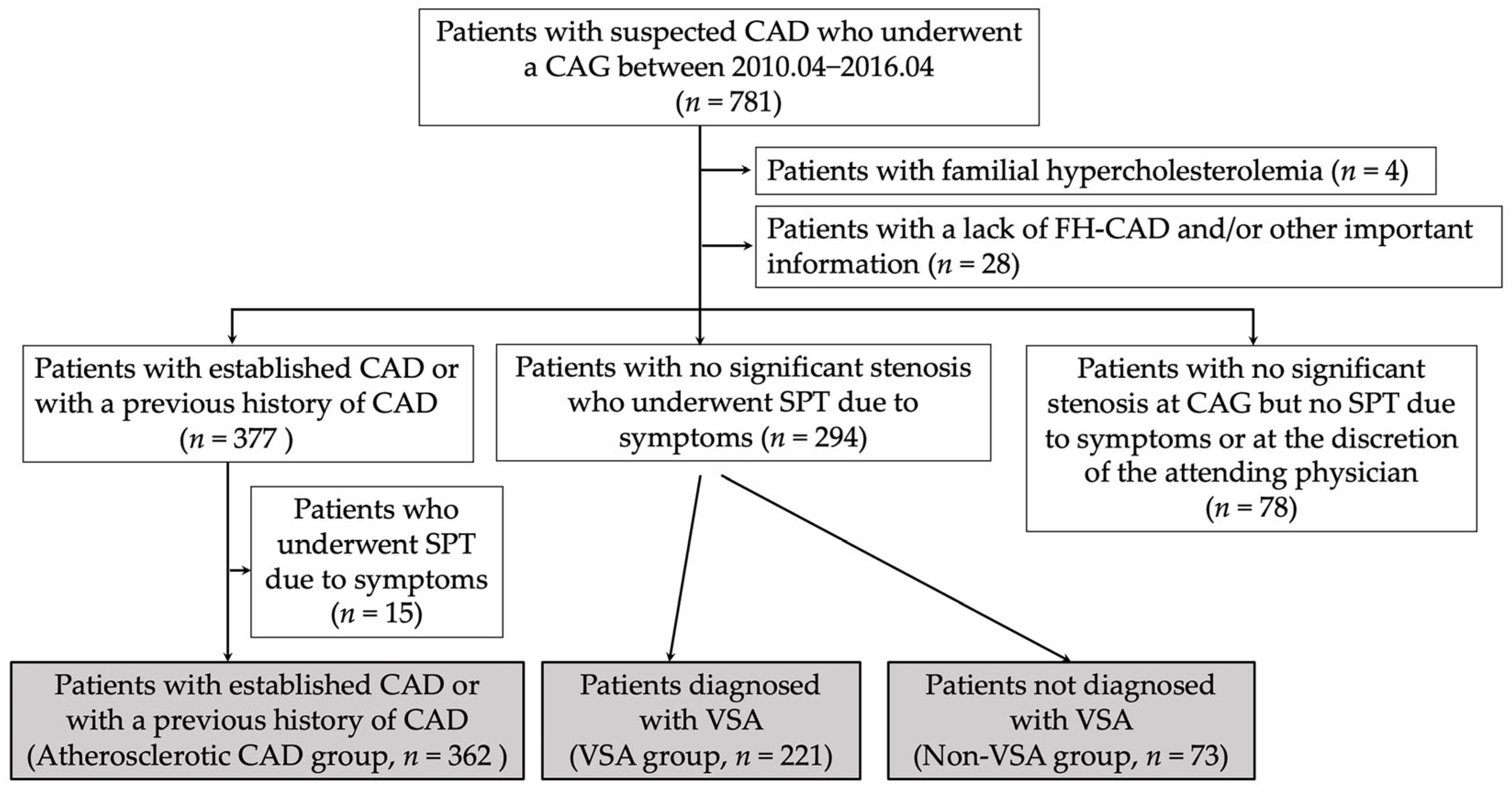
2.1. Study Population
2.2. Coronary Angiography (CAG) and Spasm Provocation Test (SPT)
2.3. Definition of CAG and Coronary Spasm-Related Factors
2.4. Definitions of FH-CAD
2.5. Parameters
2.6. Statistical Analyses
3. Results
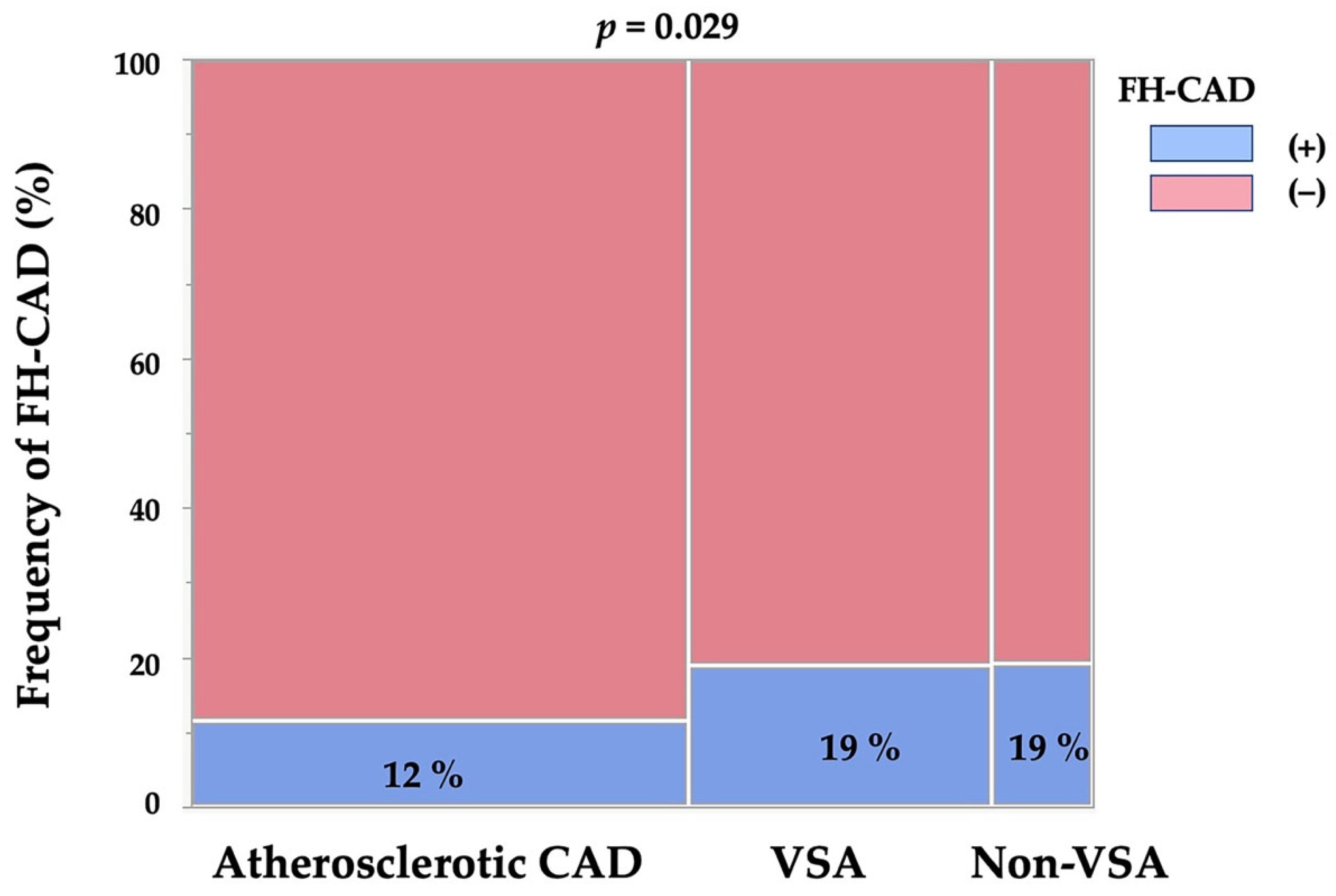
3.1. Patients’ Characteristics and Frequency of FH-CAD of the Three Groups
3.2. Clinical Characteristics and Prognosis in VSA Patients Based on the Presence of FH-CAD
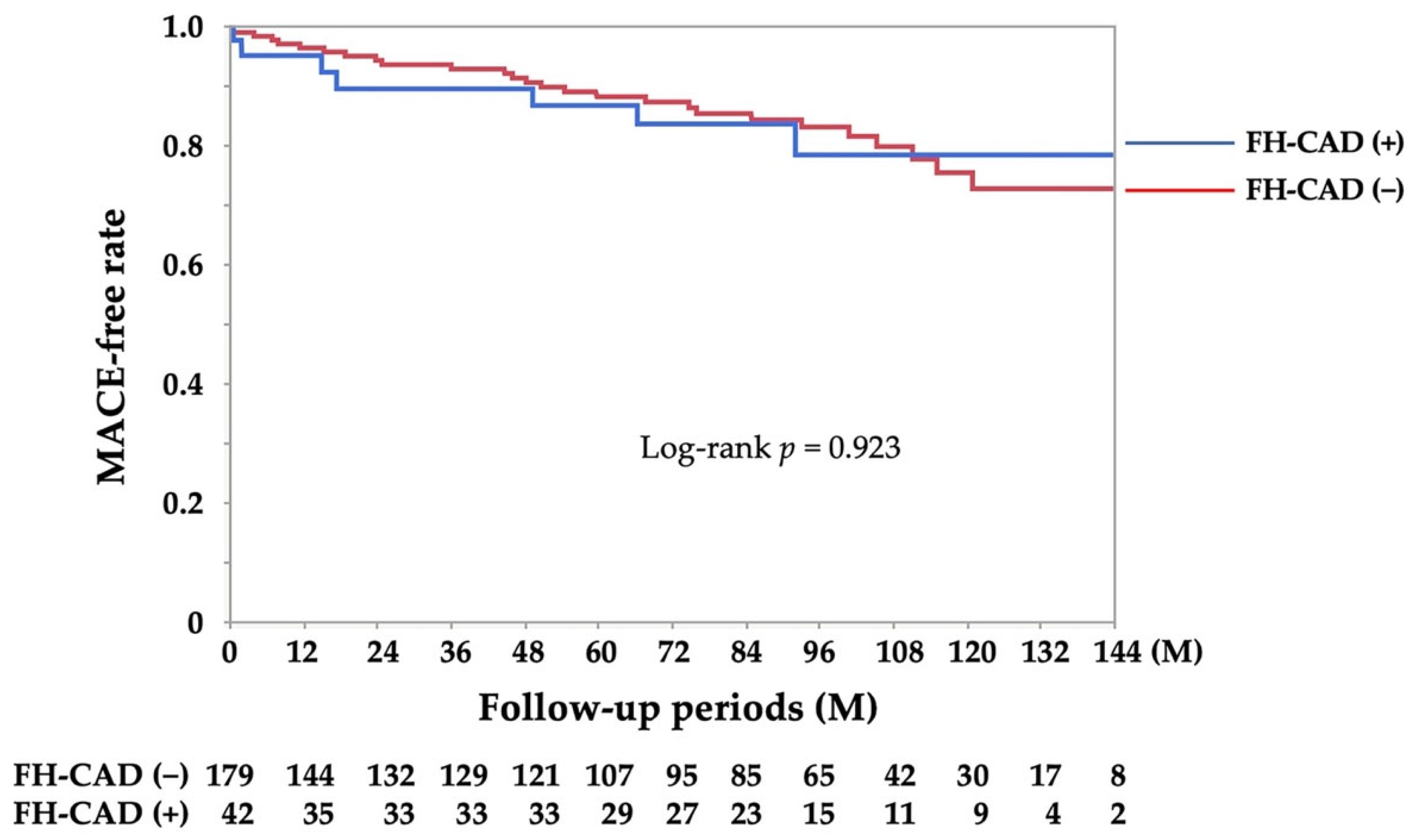
3.3. Prognosis in VSA Patients Based on FH-CAD
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Yasue, H.; Kugiyama, K. Coronary spasm: Clinical features and pathogenesis. Intern. Med 1997, 36, 760–765. [Google Scholar] [CrossRef] [PubMed]
- Yasue, H.; Nakagawa, H.; Itoh, T.; Harada, E.; Mizuno, Y. Coronary artery spasm--clinical features, diagnosis, pathogenesis, and treatment. J. Cardiol. 2008, 51, 2–17. [Google Scholar] [CrossRef] [PubMed]
- Group, J.C.S.J.W. Guidelines for diagnosis and treatment of patients with vasospastic angina (Coronary Spastic Angina) (JCS 2013). Circ. J. 2014, 78, 2779–2801. [Google Scholar] [CrossRef] [PubMed]
- Jewulski, J.; Khanal, S.; Dahal, K. Coronary vasospasm: A narrative review. World J. Cardiol. 2021, 13, 456–463. [Google Scholar] [CrossRef] [PubMed]
- Rehan, R.; Weaver, J.; Yong, A. Coronary Vasospastic Angina: A Review of the Pathogenesis, Diagnosis, and Management. Life 2022, 12, 1124. [Google Scholar] [CrossRef]
- Li, L.; Shen, Y.; Yu, B.; Xu, C.; Zhao, X.; Lin, X.; Lin, Z. Coronary Artery Spasm: Risk Factors, Pathophysiological Mechanisms and Novel Diagnostic Approaches. Rev. Cardiovasc. Med. 2022, 23, 175. [Google Scholar] [CrossRef]
- Watanabe, K.; Shishido, T.; Otaki, Y.; Watanabe, T.; Sugai, T.; Toshima, T.; Takahashi, T.; Yokoyama, M.; Kinoshita, D.; Murase, T.; et al. Increased plasma xanthine oxidoreductase activity deteriorates coronary artery spasm. Heart Vessel. 2019, 34, 1–8. [Google Scholar] [CrossRef]
- Lin, X.; Lin, Z.; Zhao, X.; Liu, Z.; Xu, C.; Yu, B.; Gao, P.; Wang, Z.; Ge, J.; Shen, Y.; et al. Serum SELENBP1 and VCL Are Effective Biomarkers for Clinical and Forensic Diagnosis of Coronary Artery Spasm. Int. J. Mol. Sci. 2022, 23, 13266. [Google Scholar] [CrossRef]
- Yu, B.; Xu, C.; Tang, X.; Liu, Z.; Lin, X.; Meng, H.; Shi, C.; Ma, K.; Xiao, B.; Li, L. Endoplasmic reticulum stress-related secretory proteins as biomarkers of early myocardial ischemia-induced sudden cardiac deaths. Int. J. Legal. Med. 2022, 136, 159–168. [Google Scholar] [CrossRef]
- Nobuyoshi, M.; Abe, M.; Nosaka, H.; Kimura, T.; Yokoi, H.; Hamasaki, N.; Shindo, T.; Kimura, K.; Nakamura, T.; Nakagawa, Y.; et al. Statistical analysis of clinical risk factors for coronary artery spasm: Identification of the most important determinant. Am. Heart J. 1992, 124, 32–38. [Google Scholar] [CrossRef]
- Sugiishi, M.; Takatsu, F. Cigarette smoking is a major risk factor for coronary spasm. Circulation 1993, 87, 76–79. [Google Scholar] [CrossRef] [PubMed]
- Kannel, W.B.; Feinleib, M.; McNamara, P.M.; Garrison, R.J.; Castelli, W.P. An investigation of coronary heart disease in families. The Framingham offspring study. Am. J. Epidemiol. 1979, 110, 281–290. [Google Scholar] [CrossRef]
- Shea, S.; Ottman, R.; Gabrieli, C.; Stein, Z.; Nichols, A. Family history as an independent risk factor for coronary artery disease. J. Am. Coll. Cardiol. 1984, 4, 793–801. [Google Scholar] [CrossRef] [PubMed]
- Hopkins, P.N.; Williams, R.R.; Kuida, H.; Stults, B.M.; Hunt, S.C.; Barlow, G.K.; Ash, K.O. Family history as an independent risk factor for incident coronary artery disease in a high-risk cohort in Utah. Am. J. Cardiol. 1988, 62, 703–707. [Google Scholar] [CrossRef] [PubMed]
- Jorde, L.B.; Williams, R.R. Relation between family history of coronary artery disease and coronary risk variables. Am. J. Cardiol. 1988, 62, 708–713. [Google Scholar] [CrossRef]
- Myers, R.H.; Kiely, D.K.; Cupples, L.A.; Kannel, W.B. Parental history is an independent risk factor for coronary artery disease: The Framingham Study. Am. Heart J. 1990, 120, 963–969. [Google Scholar] [CrossRef]
- Patel, J.; Al Rifai, M.; Scheuner, M.T.; Shea, S.; Blumenthal, R.S.; Nasir, K.; Blaha, M.J.; McEvoy, J.W. Basic vs More Complex Definitions of Family History in the Prediction of Coronary Heart Disease: The Multi-Ethnic Study of Atherosclerosis. Mayo Clin. Proc. 2018, 93, 1213–1223. [Google Scholar] [CrossRef]
- Takagi, Y.; Yasuda, S.; Tsunoda, R.; Ogata, Y.; Seki, A.; Sumiyoshi, T.; Matsui, M.; Goto, T.; Tanabe, Y.; Sueda, S.; et al. Clinical characteristics and long-term prognosis of vasospastic angina patients who survived out-of-hospital cardiac arrest: Multicenter registry study of the Japanese Coronary Spasm Association. Circ. Arrhythmia Electrophysiol. 2011, 4, 295–302. [Google Scholar] [CrossRef]
- Kawana, A.; Takahashi, J.; Takagi, Y.; Yasuda, S.; Sakata, Y.; Tsunoda, R.; Ogata, Y.; Seki, A.; Sumiyoshi, T.; Matsui, M.; et al. Gender differences in the clinical characteristics and outcomes of patients with vasospastic angina—A report from the Japanese Coronary Spasm Association. Circ. J. 2013, 77, 1267–1274. [Google Scholar] [CrossRef]
- Ong, P.; Pirozzolo, G.; Athanasiadis, A.; Sechtem, U. Epicardial Coronary Spasm in Women With Angina Pectoris and Unobstructed Coronary Arteries Is Linked With a Positive Family History: An Observational Study. Clin. Ther. 2018, 40, 1584–1590. [Google Scholar] [CrossRef]
- Teragawa, H.; Oshita, C.; Ueda, T. History of gastroesophageal reflux disease in patients with suspected coronary artery disease. Heart Vessel. 2019, 34, 1631–1638. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, S.; Kaikita, K.; Yamamoto, E.; Jinnouchi, H.; Tsujita, K. Role of acetylcholine spasm provocation test as a pathophysiological assessment in nonobstructive coronary artery disease. Cardiovasc. Interv. Ther. 2021, 36, 39–51. [Google Scholar] [CrossRef] [PubMed]
- Teragawa, H.; Oshita, C.; Orita, Y. Clinical significance of prolonged chest pain in vasospastic angina. World J. Cardiol. 2020, 12, 450–459. [Google Scholar] [CrossRef]
- Teragawa, H.; Oshita, C.; Uchimura, Y. Clinical Characteristics and Prognosis of Patients with Multi-Vessel Coronary Spasm in Comparison with Those in Patients with Single-Vessel Coronary Spasm. J. Cardiovasc. Dev. Dis. 2022, 9, 204. [Google Scholar] [CrossRef]
- Teragawa, H.; Oshita, C.; Ueda, T. The Myocardial Bridge: Potential Influences on the Coronary Artery Vasculature. Clin. Med. Insights Cardiol. 2019, 13, 1179546819846493. [Google Scholar] [CrossRef] [PubMed]
- Teragawa, H.; Oshita, C.; Uchimura, Y. The Impact of Myocardial Bridging on the Coronary Functional Test in Patients with Ischaemia with Non-Obstructive Coronary Artery Disease. Life 2022, 12, 1560. [Google Scholar] [CrossRef] [PubMed]
- Teragawa, H.; Fukuda, Y.; Matsuda, K.; Hirao, H.; Higashi, Y.; Yamagata, T.; Oshima, T.; Matsuura, H.; Chayama, K. Myocardial bridging increases the risk of coronary spasm. Clin. Cardiol. 2003, 26, 377–383. [Google Scholar] [CrossRef] [PubMed]
- Hokimoto, S.; Kaikita, K.; Yasuda, S.; Tsujita, K.; Ishihara, M.; Matoba, T.; Matsuzawa, Y.; Mitsutake, Y.; Mitani, Y.; Murohara, T.; et al. JCS/CVIT/JCC 2023 Guideline Focused Update on Diagnosis and Treatment of Vasospastic Angina (Coronary Spastic Angina) and Coronary Microvascular Dysfunction. Circ. J. 2023, 87, 879–936. [Google Scholar] [CrossRef]
- Sato, K.; Kaikita, K.; Nakayama, N.; Horio, E.; Yoshimura, H.; Ono, T.; Ohba, K.; Tsujita, K.; Kojima, S.; Tayama, S.; et al. Coronary vasomotor response to intracoronary acetylcholine injection, clinical features, and long-term prognosis in 873 consecutive patients with coronary spasm: Analysis of a single-center study over 20 years. J. Am. Heart Assoc. 2013, 2, e000227. [Google Scholar] [CrossRef]
- Nishimiya, K.; Suda, A.; Fukui, K.; Hao, K.; Takahashi, J.; Matsumoto, Y.; Mitsuishi, K.; Watanabe, T.; Ohyama, K.; Sugisawa, J.; et al. Prognostic Links Between OCT-Delineated Coronary Morphologies and Coronary Functional Abnormalities in Patients With INOCA. JACC Cardiovasc. Interv. 2021, 14, 606–618. [Google Scholar] [CrossRef]
- Teragawa, H.; Fukuda, Y.; Matsuda, K.; Higashi, Y.; Yamagata, T.; Matsuura, H.; Chayama, K. Effect of alcohol consumption on endothelial function in men with coronary artery disease. Atherosclerosis 2002, 165, 145–152. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, S.; Imai, E.; Horio, M.; Yasuda, Y.; Tomita, K.; Nitta, K.; Yamagata, K.; Tomino, Y.; Yokoyama, H.; Hishida, A.; et al. Revised equations for estimated GFR from serum creatinine in Japan. Am. J. Kidney Dis. 2009, 53, 982–992. [Google Scholar] [CrossRef] [PubMed]
- Teragawa, H.; Oshita, C.; Uchimura, Y. Clinical Characteristics and Prognosis of Patients with Vasospastic Angina Subjected to the Spasm Provocation Test and the Unavoidable Use of Nitroglycerin. J. Cardiovasc. Dev. Dis. 2023, 10, 16. [Google Scholar] [CrossRef]
- Teragawa, H.; Oshita, C.; Uchimura, Y. Vasospastic angina in women: Clinical backgrounds and prognoses of patients younger than and older than 60 years. World J. Cardiol. 2023, 15, 154–164. [Google Scholar] [CrossRef]
- Benjamin, E.J.; Blaha, M.J.; Chiuve, S.E.; Cushman, M.; Das, S.R.; Deo, R.; de Ferranti, S.D.; Floyd, J.; Fornage, M.; Gillespie, C.; et al. Heart Disease and Stroke Statistics-2017 Update: A Report From the American Heart Association. Circulation 2017, 135, e146–e603. [Google Scholar] [CrossRef] [PubMed]
- Pohjola-Sintonen, S.; Rissanen, A.; Liskola, P.; Luomanmaki, K. Family history as a risk factor of coronary heart disease in patients under 60 years of age. Eur. Heart J. 1998, 19, 235–239. [Google Scholar] [CrossRef]
- Ishii, M.; Kaikita, K.; Sato, K.; Tanaka, T.; Sugamura, K.; Sakamoto, K.; Izumiya, Y.; Yamamoto, E.; Tsujita, K.; Yamamuro, M.; et al. Acetylcholine-Provoked Coronary Spasm at Site of Significant Organic Stenosis Predicts Poor Prognosis in Patients With Coronary Vasospastic Angina. J. Am. Coll Cardiol. 2015, 66, 1105–1115. [Google Scholar] [CrossRef]
- Yoshimura, M.; Yasue, H.; Nakayama, M.; Shimasaki, Y.; Sumida, H.; Sugiyama, S.; Kugiyama, K.; Ogawa, H.; Ogawa, Y.; Saito, Y.; et al. A missense Glu298Asp variant in the endothelial nitric oxide synthase gene is associated with coronary spasm in the Japanese. Hum. Genet. 1998, 103, 65–69. [Google Scholar] [CrossRef]
- Yoshimura, M.; Nakayama, M.; Shimasaki, Y.; Ogawa, H.; Kugiyama, K.; Nakamura, S.; Ito, T.; Mizuno, Y.; Harada, E.; Yasue, H.; et al. A T-786-->C mutation in the 5’-flanking region of the endothelial nitric oxide synthase gene and coronary arterial vasomotility. Am. J. Cardiol. 2000, 85, 710–714. [Google Scholar] [CrossRef]
- Mizuno, Y.; Harada, E.; Morita, S.; Kinoshita, K.; Hayashida, M.; Shono, M.; Morikawa, Y.; Murohara, T.; Nakayama, M.; Yoshimura, M.; et al. East asian variant of aldehyde dehydrogenase 2 is associated with coronary spastic angina: Possible roles of reactive aldehydes and implications of alcohol flushing syndrome. Circulation 2015, 131, 1665–1673. [Google Scholar] [CrossRef]
- Mizuno, Y.; Harada, E.; Kugimiya, F.; Shono, M.; Kusumegi, I.; Yoshimura, M.; Kinoshita, K.; Yasue, H. East Asians Variant Mitochondrial Aldehyde Dehydrogenase 2 Genotype Exacerbates Nitrate Tolerance in Patients With Coronary Spastic Angina. Circ. J. 2020, 84, 479–486. [Google Scholar] [CrossRef]
- Takagi, Y.; Takahashi, J.; Yasuda, S.; Miyata, S.; Tsunoda, R.; Ogata, Y.; Seki, A.; Sumiyoshi, T.; Matsui, M.; Goto, T.; et al. Prognostic stratification of patients with vasospastic angina: A comprehensive clinical risk score developed by the Japanese Coronary Spasm Association. J. Am. Coll. Cardiol. 2013, 62, 1144–1153. [Google Scholar] [CrossRef]
- Pirozzolo, G.; Seitz, A.; Athanasiadis, A.; Bekeredjian, R.; Sechtem, U.; Ong, P. Microvascular spasm in non-ST-segment elevation myocardial infarction without culprit lesion (MINOCA). Clin. Res. Cardiol. 2020, 109, 246–254. [Google Scholar] [CrossRef]
- Teragawa, H.; Oshita, C.; Uchimura, Y.; Akazawa, R.; Orita, Y. Coronary Microvascular Vasodilatory Function: Related Clinical Features and Differences According to the Different Coronary Arteries and Types of Coronary Spasm. J. Clin. Med. 2021, 11, 130. [Google Scholar] [CrossRef]
- Kunadian, V.; Chieffo, A.; Camici, P.G.; Berry, C.; Escaned, J.; Maas, A.; Prescott, E.; Karam, N.; Appelman, Y.; Fraccaro, C.; et al. An EAPCI Expert Consensus Document on Ischaemia with Non-Obstructive Coronary Arteries in Collaboration with European Society of Cardiology Working Group on Coronary Pathophysiology & Microcirculation Endorsed by Coronary Vasomotor Disorders International Study Group. Eur. Heart J. 2020, 41, 3504–3520. [Google Scholar] [CrossRef] [PubMed]
- Schachinger, V.; Britten, M.B.; Elsner, M.; Walter, D.H.; Scharrer, I.; Zeiher, A.M. A positive family history of premature coronary artery disease is associated with impaired endothelium-dependent coronary blood flow regulation. Circulation 1999, 100, 1502–1508. [Google Scholar] [CrossRef]
- Berg, A.O.; Baird, M.A.; Botkin, J.R.; Driscoll, D.A.; Fishman, P.A.; Guarino, P.D.; Hiatt, R.A.; Jarvik, G.P.; Millon-Underwood, S.; Morgan, T.M.; et al. National Institutes of Health State-of-the-Science Conference Statement: Family History and Improving Health: 24–26 August 2009. NIH Consens. State Sci. Statements 2009, 26, 1–19. [Google Scholar]
- Teragawa, H.; Oshita, C.; Ueda, T. Coronary spasm: It’s common, but it’s still unsolved. World J. Cardiol. 2018, 10, 201–209. [Google Scholar] [CrossRef] [PubMed]
- Hokimoto, S.; Mizuno, Y.; Sueta, D.; Morita, S.; Akasaka, T.; Tabata, N.; Harada, E.; Arima, Y.; Yamamuro, M.; Tanaka, T.; et al. High incidence of coronary spasm after percutaneous coronary interventions: Comparison between new generation drug-eluting stent and bare-metal stent. Int. J. Cardiol. 2015, 182, 171–173. [Google Scholar] [CrossRef] [PubMed]
| Atherosclerotic CAD | VSA | Non-VSA | p Value | ||
|---|---|---|---|---|---|
| No. | 362 | 221 | 73 | ||
| Age (years) | 69 ± 11 | 67± 11 | 66 ± 13 | 0.004 | |
| Male/Female | 270/92 | 114/107 | 24/49 | <0.001 | |
| Body mass index | 24.2 ± 4.7 | 24.2 ± 4.2 | 24.4 ± 3.8 | 0.933 | |
| Coronary risk factors (%) | |||||
| Active smoker | 86 (24) | 47 (21) | 6 (8) | 0.012 | |
| Hypertension | 264 (73) | 158 (71) | 50 (68) | 0.731 | |
| Dyslipidaemia | 294 (81) | 138 (62) | 42 (58) | <0.001 | |
| Diabetes mellitus | 159 (45) | 49 (22) | 15 (21) | <0.001 | |
| CKD (%) | 188 (53) | 66 (30) | 25 (35) | <0.001 | |
| LVEF on UCG (%) | 62 ± 12 | 66 ± 9 | 68 ± 6 | <0.001 | |
| Atherosclerotic CAD | VSA | Non-VSA | p Value | ||
|---|---|---|---|---|---|
| FH-CAD (No., %) | 42 (362,12) | 42 (221, 19) | 14 (73, 19) | 0.029 | |
| Male patients (No., %) | 33 (270, 12) | 16 (114, 14) | 4 (24, 17) | 0.764 | |
| Female patients (No., %) | 9 (92, 10) | 26 (107, 24) | 10 (49, 20) | 0.027 | |
| Patients with FH-CAD | |||||
| No. | 42 | 42 | 14 | ||
| Male/Female | 33/9 | 16/26 | 4/10 | <0.001 | |
| First-degree relative (%) | 31 (74) | 31 (74) | 10 (71) | 0.983 | |
| Only second-degree relative (%) | 11 (26) | 11 (26) | 4 (29) | 0.983 | |
| Non-pharmacological therapy for CAD (%) | 24 (52) | 12 (29) | 4 (29) | 0.017 | |
| Probable sudden cardiac death (%) | 7 (17) | 11 (26) | 1 (7) | 0.248 | |
| FH-CAD (−) VSA Group | FH-CAD (+) VSA Group | p Value | ||
|---|---|---|---|---|
| No. (%) | 179 (81) | 42 (19) | ||
| Age (years) | 68 ± 11 | 65 ± 12 | 0.178 | |
| Male/Female | 98/81 | 16/26 | 0.052 | |
| Body mass index | 22.4 ± 4.1 | 24.2 ± 4.5 | 0.978 | |
| Coronary risk factors (%) | ||||
| Active smoker | 39 (22) | 8 (19) | 0.696 | |
| Hypertension | 128 (72) | 30 (31) | 0.992 | |
| Dyslipidaemia | 112 (63) | 26 (62) | 0.936 | |
| Diabetes mellitus | 40 (22) | 9 (21) | 0.898 | |
| Alcoholic drinker (%) | 73 (41) | 11 (26) | 0.080 | |
| CKD (%) | 51 (28) | 15 (36) | 0.357 | |
| LVEF on UCG (%) | 66 ± 10 | 68 ± 6 | 0.364 | |
| FH-CAD (−) VSA Group | FH-CAD (+) VSA Group | p Value | ||
|---|---|---|---|---|
| Brachial ultrasonography | ||||
| No. | 152 | 40 | ||
| Brachial artery diameter at baseline (mm) | 3.9 ± 0.6 | 3.7 ± 0.7 | 0.073 | |
| FMD (%) | 3.9 ± 3.1 | 3.4 ± 3.0 | 0.384 | |
| NID (%) | 14.0 ± 6.0 | 16.7 ± 8.4 | 0.023 | |
| VSA-related symptoms | ||||
| At rest/on exercise/both | 146/18/15 | 34/6/2 | 0.554 | |
| Estimated diseased period (M) | 6 (2, 20) | 5 (2, 36) | 0.518 | |
| No. of anginal attack/M | 4 (2, 10) | 5 (2, 10) | 0.321 | |
| VA (%) | 6 (4) | 0 (0) | 0.229 | |
| CAG | ||||
| Atherosclerosis (%) | 109 (61) | 23 (55) | 0.476 | |
| MB (%) | 24 (13) | 8 (14) | 0.350 | |
| SPT | ||||
| L-ACh-induced spasms (%) | 43 (24) | 12 (29) | 0.539 | |
| TOC (%) | 15 (8) | 5 (12) | 0.474 | |
| Focal spasms (%) | 51 (28) | 14 (33) | 0.533 | |
| MVS (No, %) | 98 (152, 64) | 28 (38, 74) | 0.283 | |
| ST elevation during SPT (%) | 29 (16) | 5 (12) | 0.487 | |
| Unavoidable use of NTG (%) | 50 (32) | 11 (27) | 0.551 | |
| Follow-up | ||||
| Follow-up period (M) | 89 (38, 113) | 87 (55, 108) | 0.843 | |
| No. of anginal attack/M | 0 (0, 1) (No. = 135) | 0 (0, 1) (No. = 35) | 0.864 | |
| No. coronary vasodilators | 1.4 ± 0.9 (No. = 135) | 1.6 ± 1.1 (No. = 35) | 0.266 | |
| Cardiac death (%) | 1 (0.6) | 0 (0) | 0.622 | |
| Readmission for heart (%) | 26 (15) | 7 (15) | 0.726 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Teragawa, H.; Uchimura, Y.; Oshita, C.; Hashimoto, Y.; Nomura, S. Frequency and Clinical Impact of Family History of Coronary Artery Disease in Patients with Vasospastic Angina. J. Cardiovasc. Dev. Dis. 2023, 10, 249. https://doi.org/10.3390/jcdd10060249
Teragawa H, Uchimura Y, Oshita C, Hashimoto Y, Nomura S. Frequency and Clinical Impact of Family History of Coronary Artery Disease in Patients with Vasospastic Angina. Journal of Cardiovascular Development and Disease. 2023; 10(6):249. https://doi.org/10.3390/jcdd10060249
Chicago/Turabian StyleTeragawa, Hiroki, Yuko Uchimura, Chikage Oshita, Yu Hashimoto, and Shuichi Nomura. 2023. "Frequency and Clinical Impact of Family History of Coronary Artery Disease in Patients with Vasospastic Angina" Journal of Cardiovascular Development and Disease 10, no. 6: 249. https://doi.org/10.3390/jcdd10060249
APA StyleTeragawa, H., Uchimura, Y., Oshita, C., Hashimoto, Y., & Nomura, S. (2023). Frequency and Clinical Impact of Family History of Coronary Artery Disease in Patients with Vasospastic Angina. Journal of Cardiovascular Development and Disease, 10(6), 249. https://doi.org/10.3390/jcdd10060249







