AI in Dentistry: Innovations, Ethical Considerations, and Integration Barriers
Abstract
1. Introduction
- (1)
- to delineate the current landscape of AI integration in dental diagnostic imaging and workflow automation;
- (2)
- to identify and critically analyze significant ethical, regulatory, and technical obstacles to clinical adoption; and
- (3)
- to propose evidence-based strategies for future research, standardization, and interdisciplinary collaboration.
2. Current AI Applications in Oral Medicine
2.1. Diagnostic Imaging and Analysis
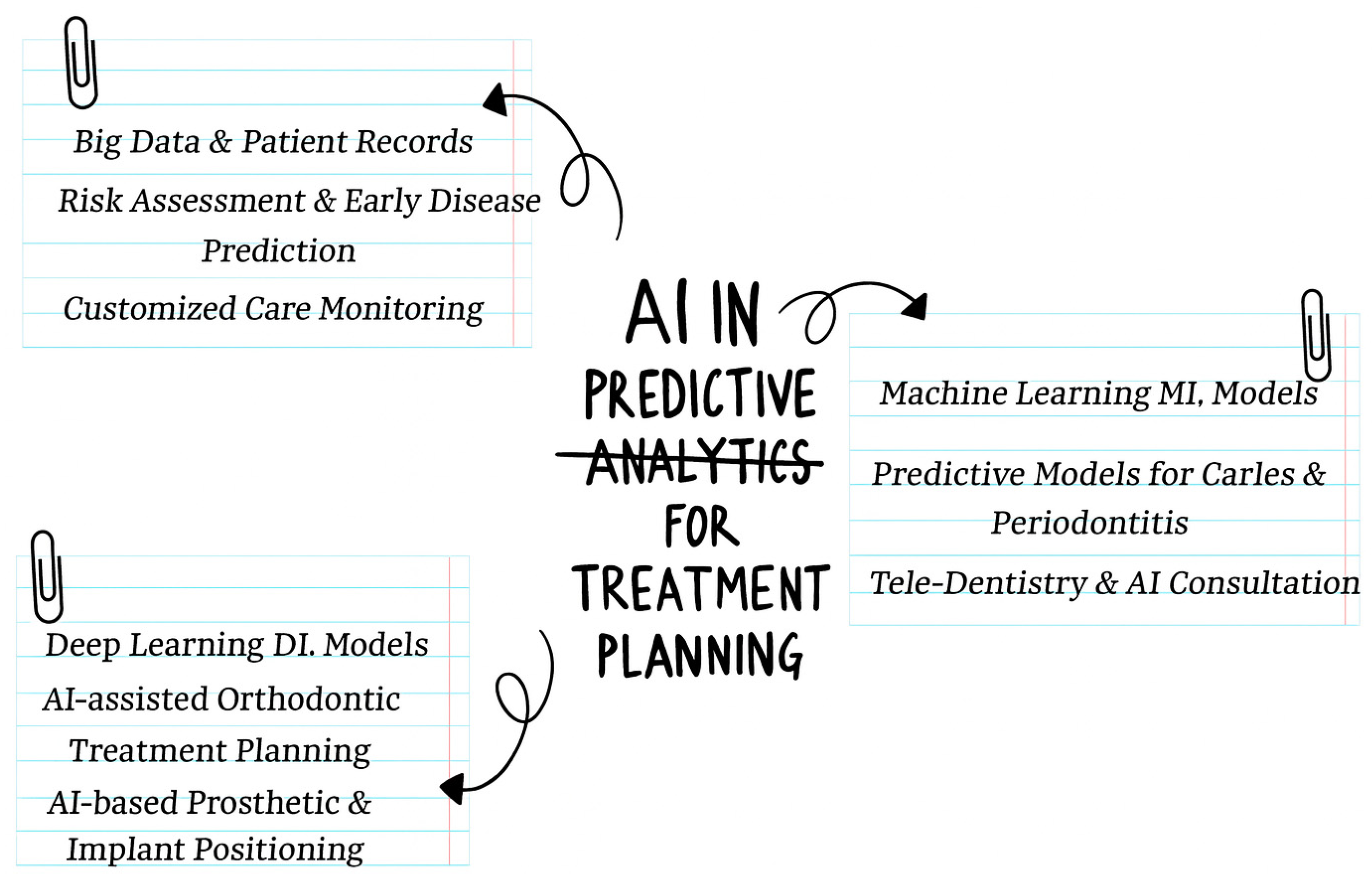
2.2. Predictive Analytics for Treatment Planning
2.3. AI in Real-Time Documentation and Workflow Automation
3. Technological Advancements in AI Models
4. Challenges and Limitations
4.1. Ethical and Legal Concerns
4.2. Integration Barriers
5. Future Perspective and Research Directions
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Deshmukh, S.V. Artificial Intelligence in Dentistry; Medknow: Ghatkopar Mumbai, India, 2018; pp. 47–48. [Google Scholar]
- Ahmed, N.; Abbasi, M.S.; Zuberi, F.; Qamar, W.; Halim, M.S.B.; Maqsood, A.; Alam, M.K. Artificial intelligence techniques: Analysis, application, and outcome in dentistry—A systematic review. BioMed Res. Int. 2021, 2021, 9751564. [Google Scholar] [CrossRef]
- Thurzo, A.; Urbanová, W.; Novák, B.; Czako, L.; Siebert, T.; Stano, P.; Mareková, S.; Fountoulaki, G.; Kosnáčová, H.; Varga, I. Where is the artificial intelligence applied in dentistry? Systematic review and literature analysis. Healthcare 2022, 10, 1269. [Google Scholar] [CrossRef]
- Carrillo-Perez, F.; Pecho, O.E.; Morales, J.C.; Paravina, R.D.; Della Bona, A.; Ghinea, R.; Pulgar, R.; Pérez, M.D.M.; Herrera, L.J. Applications of artificial intelligence in dentistry: A comprehensive review. J. Esthet. Restor. Dent. 2022, 34, 259–280. [Google Scholar] [CrossRef] [PubMed]
- Ding, H.; Wu, J.; Zhao, W.; Matinlinna, J.P.; Burrow, M.F.; Tsoi, J.K. Artificial intelligence in dentistry—A review. Front. Dent. Med. 2023, 4, 1085251. [Google Scholar] [CrossRef]
- Chen, Y.-W.; Stanley, K.; Att, W. Artificial intelligence in dentistry: Current applications and future perspectives. Quintessence Int. 2020, 51, 248–257. [Google Scholar] [PubMed]
- Meghil, M.M.; Rajpurohit, P.; Awad, M.E.; McKee, J.; Shahoumi, L.A.; Ghaly, M. Artificial intelligence in dentistry. Dent. Rev. 2022, 2, 100009. [Google Scholar] [CrossRef]
- Tandon, D.; Rajawat, J.; Banerjee, M. Present and future of artificial intelligence in dentistry. J. Oral Biol. Craniofacial Res. 2020, 10, 391–396. [Google Scholar] [CrossRef]
- Wang, L.; Xu, Y.; Wang, W.; Lu, Y. Application of machine learning in dentistry: Insights, prospects and challenges. Acta Odontol. Scand. 2025, 84, 43345. [Google Scholar] [CrossRef]
- Surdu, A.; Budala, D.G.; Luchian, I.; Foia, L.G.; Botnariu, G.E.; Scutariu, M.M. Using AI in optimizing oral and dental diagnoses—A narrative review. Diagnostics 2024, 14, 2804. [Google Scholar] [CrossRef]
- Alghamdi, S.N.; Alghamdi, M.A.; Miswak, A.A.; Simsim, O.A.A.; Wasli, A.; Refaei, H.T.A.; Batt, K.H.; Ajeebi, W.M.Y.; Almosa, A.I.; Abdullah, M.M. Advancements in Dental Care: Shaping the Future of Oral Health. J. Int. Crisis Risk Commun. Res. 2024, 7, 830. [Google Scholar]
- Putra, R.H.; Doi, C.; Yoda, N.; Astuti, E.R.; Sasaki, K. Current applications and development of artificial intelligence for digital dental radiography. Dentomaxillofac. Radiol. 2022, 51, 20210197. [Google Scholar] [CrossRef]
- Nooraldaim, A.; Saed, A. Artificial Intelligence for Caries and Tooth Detection in Dental Imaging: A Review. Indones. J. Comput. Sci. 2023, 12. [Google Scholar] [CrossRef]
- Cui, Z.; Fang, Y.; Mei, L.; Zhang, B.; Yu, B.; Liu, J.; Jiang, C.; Sun, Y.; Ma, L.; Huang, J. A fully automatic AI system for tooth and alveolar bone segmentation from cone-beam CT images. Nat. Commun. 2022, 13, 2096. [Google Scholar] [CrossRef]
- Lahoud, P.; EzEldeen, M.; Beznik, T.; Willems, H.; Leite, A.; Van Gerven, A.; Jacobs, R. Artificial intelligence for fast and accurate 3-dimensional tooth segmentation on cone-beam computed tomography. J. Endod. 2021, 47, 827–835. [Google Scholar] [CrossRef]
- Alharbi, S.S.; Alhasson, H.F. Exploring the Applications of Artificial Intelligence in Dental Image Detection: A Systematic Review. Diagnostics 2024, 14, 2442. [Google Scholar] [CrossRef]
- Ji, Y.; Chen, Y.; Liu, G.; Long, Z.; Gao, Y.; Huang, D.; Zhang, L. Construction and evaluation of an AI-based CBCT resolution optimization technique for extracted teeth. J. Endod. 2024, 50, 1298–1306. [Google Scholar] [CrossRef]
- Pauwels, R. A brief introduction to concepts and applications of artificial intelligence in dental imaging. Oral Radiol. 2021, 37, 153–160. [Google Scholar] [CrossRef]
- Prados-Privado, M.; Villalón, J.G.; Martínez-Martínez, C.H.; Ivorra, C. Dental images recognition technology and applications: A literature review. Appl. Sci. 2020, 10, 2856. [Google Scholar] [CrossRef]
- Katsumata, A. Deep learning and artificial intelligence in dental diagnostic imaging. Jpn. Dent. Sci. Rev. 2023, 59, 329–333. [Google Scholar] [CrossRef] [PubMed]
- Ezhov, M.; Gusarev, M.; Golitsyna, M.; Yates, J.M.; Kushnerev, E.; Tamimi, D.; Aksoy, S.; Shumilov, E.; Sanders, A.; Orhan, K. Clinically applicable artificial intelligence system for dental diagnosis with CBCT. Sci. Rep. 2021, 11, 15006. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.-H.; Kim, K.B.; Choo, H. New frontier in advanced dentistry: CBCT, intraoral scanner, sensors, and artificial intelligence in dentistry. Sensors 2022, 22, 2942. [Google Scholar] [CrossRef]
- Bonny, T.; Al Nassan, W.; Obaideen, K.; Rabie, T.; AlMallahi, M.N.; Gupta, S. Primary Methods and Algorithms in Artificial-Intelligence-Based Dental Image Analysis: A Systematic Review. Algorithms 2024, 17, 567. [Google Scholar] [CrossRef]
- Chauhan, R.B.; Shah, T.V.; Shah, D.H.; Gohil, T.J.; Oza, A.D.; Jajal, B.; Saxena, K.K. An overview of image processing for dental diagnosis. Innov. Emerg. Technol. 2023, 10, 2330001. [Google Scholar] [CrossRef]
- Mureșanu, S.; Almășan, O.; Hedeșiu, M.; Dioșan, L.; Dinu, C.; Jacobs, R. Artificial intelligence models for clinical usage in dentistry with a focus on dentomaxillofacial CBCT: A systematic review. Oral Radiol. 2023, 39, 18–40. [Google Scholar] [CrossRef] [PubMed]
- Pappireddy, A.R. Predictive Analytics in Dental Health: Leveraging Data for Early Detection and Prevention. J. Sci. Technol. 2024, 5, 121–137. [Google Scholar]
- Batra, A.M.; Reche, A. A new era of dental care: Harnessing artificial intelligence for better diagnosis and treatment. Cureus 2023, 15, e49319. [Google Scholar] [CrossRef]
- Sharma, S.; Kumari, P.; Sabira, K.; Parihar, A.S.; Rani, P.D.; Roy, A.; Surana, P. Revolutionizing dentistry: The applications of artificial intelligence in dental health care. J. Pharm. Bioallied Sci. 2024, 16 (Suppl. 3), S1910–S1912. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W. Machine Learning-Based Predictive Analytics for Dental Practice Management. Aust. J. Mach. Learn. Res. Appl. 2023, 3, 151. Available online: https://sydneyacademics.com/index.php/ajmlra/article/view/5 (accessed on 5 July 2025).
- Krupa, C.S. Tele-dentistry and Data Science: Enhancing Access and Quality of Dental Care. J. Sci. Technol. 2024, 5, 137–149. [Google Scholar]
- Tanaka, H. Machine Learning-Based Predictive Analytics for Early Disease Diagnosis. In Orthodontics Unveiled: Exploring Emerging Trends in Dental Alignment; Inkbound Publishers: Ahmedabad, India, 2021; p. 178. [Google Scholar]
- Khorshidi, F.; Esmaeilyfard, R.; Paknahad, M. Enhancing predictive analytics in mandibular third molar extraction using artificial intelligence: A CBCT-Based study. Saudi Dent. J. 2024, 36, 1582–1587. [Google Scholar] [CrossRef]
- Kim, S. Personalized Dental Treatment Planning Using AI-Powered Algorithms. Afr. J. Artif. Intell. Sustain. Dev. 2023, 3, 12–20. [Google Scholar]
- Bhat, N.; Kukreja, B.J.; Kukreja, P.; Bagde, H. Efficient Treatment Planning on Optimization Techniques Empowered by AI in Dentistry. In Optimizing Intelligent Systems for Cross-Industry Application; IGI Global: Hershey, PA, USA, 2024; pp. 239–266. [Google Scholar]
- Adekugbe, A.P.; Ibeh, C.V. Optimizing dental health equity: Integrating business analytics and program management for underserved populations in the US. Int. J. Front. Life Sci. Res. 2024, 6, 011–020. [Google Scholar] [CrossRef]
- Aziz, S.; Adnan, K.; Fatemah, H.; Farrukh, U.; Rathore, E.; Umer, M. Automated diagnosis and treatment planning in dentistry. Int. J. Health Sci. 2023, 7, 1166–1179. [Google Scholar] [CrossRef]
- Schwendicke, F.; Krois, J. Precision dentistry—What it is, where it fails (yet), and how to get there. Clin. Oral Investig. 2022, 26, 3395–3403. [Google Scholar] [CrossRef] [PubMed]
- Mueller, K. AI-Enabled Decision Support for Dental Professionals. J. Bioinform. Artif. Intell. 2024, 4, 12. Available online: https://biotechjournal.org/index.php/jbai/article/view/4Nambiar (accessed on 5 July 2025).
- Nambiar, R.; Nanjundegowda, R. A comprehensive review of ai and deep learning applications in dentistry: From image segmentation to treatment planning. J. Robot. Control (JRC) 2024, 5, 1744–1752. [Google Scholar]
- Hashem, M.; Youssef, A.E. Teeth infection and fatigue prediction using optimized neural networks and big data analytic tool. Clust. Comput. 2020, 23, 1669–1682. [Google Scholar] [CrossRef]
- Dhopte, A.; Bagde, H. Smart smile: Revolutionizing dentistry with artificial intelligence. Cureus 2023, 15, e41227. [Google Scholar] [CrossRef]
- Thunki, P.; Kukalakunta, Y.; Yellu, R.R. Autonomous Dental Healthcare Systems-A Review of AI and Robotics Integration. J. Mach. Learn. Pharm. Res. 2024, 4, 38–49. [Google Scholar]
- Shujaat, S. Automated machine learning in dentistry: A narrative review of applications, challenges, and future directions. Diagnostics 2025, 15, 273. [Google Scholar] [CrossRef]
- Schwendicke, F.; Krois, J. Data dentistry: How data are changing clinical care and research. J. Dent. Res. 2022, 101, 21–29. [Google Scholar] [CrossRef]
- Thorat, V.; Rao, P.; Joshi, N.; Talreja, P.; Shetty, A.R. Role of Artificial Intelligence (AI) in Patient Education and Communication in Dentistry. Cureus 2024, 16, e59799. [Google Scholar] [CrossRef]
- Jain, P.; Wynne, C. Artificial Intelligence and Big Data in Dentistry. In Digitization in Dentistry; Springer: Cham, Switzerland, 2021; pp. 1–28. [Google Scholar]
- Raparthi, M. Robotic Process Automation in Healthcare-Streamlining Precision Medicine Workflows with AI. J. Sci. Technol. 2020, 1, 91–99. [Google Scholar]
- Juluru, K.; Shih, H.-H.; Keshava Murthy, K.N.; Elnajjar, P.; El-Rowmeim, A.; Roth, C.; Genereaux, B.; Fox, J.; Siegel, E.; Rubin, D.L. Integrating Al algorithms into the clinical workflow. Radiol. Artif. Intell. 2021, 3, e210013. [Google Scholar] [CrossRef]
- Afrin, S.; Roksana, S.; Akram, R. AI-Enhanced Robotic Process Automation: A Review of Intelligent Automation Innovations. IEEE Access 2024, 13, 173–197. [Google Scholar] [CrossRef]
- Ogunsakin, O.L.; Anwansedo, S. Leveraging AI for Healthcare Administration: Streamlining Operations and Reducing Costs. IRE J. 2024, 7, 235–244. [Google Scholar]
- Marescotti, D.; Narayanamoorthy, C.; Bonjour, F.; Kuwae, K.; Graber, L.; Calvino-Martin, F.; Ghosh, S.; Hoeng, J. AI-driven laboratory workflows enable operation in the age of social distancing. SLAS Technol. 2022, 27, 195–203. [Google Scholar] [CrossRef]
- Baviskar, D.; Ahirrao, S.; Potdar, V.; Kotecha, K. Efficient automated processing of the unstructured documents using artificial intelligence: A systematic literature review and future directions. IEEE Access 2021, 9, 72894–72936. [Google Scholar] [CrossRef]
- Eziefule, A.O.; Adelakun, B.O.; Okoye, I.N.; Attieku, J.S. The Role of AI in Automating Routine Accounting Tasks: Efficiency Gains and Workforce Implications. Eur. J. Account. Audit. Financ. Res. 2022, 10, 109–134. [Google Scholar]
- Machireddy, J.R. Revolutionizing Claims Processing in the Healthcare Industry: The Expanding Role of Automation and AI. Hong Kong J. AI Med. 2022, 2, 10–36. [Google Scholar]
- Ronak, B. AI-Driven Project Management Revolutionizing Workflow Optimization and Decision-Making. Int. J. Trend Sci. Res. Dev. 2024, 8, 325–338. [Google Scholar]
- Khankhoje, R. The Power of AI Driven Reporting in Test Automation. Int. J. Sci. Res. (IJSR) 2018, 7, 1956–1959. [Google Scholar] [CrossRef]
- Pasupuleti, M.K.; Salwaji, S.; Dantuluri, M.; Raju, M.; Ramaraju, A.V.; Marrapodi, M.M.; Cicciù, M.; Minervini, G. Newer technological advances: A step towards better dental care: A systematic review. Open Dent. J. 2024, 18, e18742106320205. [Google Scholar] [CrossRef]
- Farhadi Nia, M.; Ahmadi, M.; Irankhah, E. Transforming dental diagnostics with artificial intelligence: Advanced integration of ChatGPT and large language models for patient care. Front. Dent. Med. 2025, 5, 1456208. [Google Scholar] [CrossRef]
- Rahim, A.; Khatoon, R.; Khan, T.A.; Syed, K.; Khan, I.; Khalid, T.; Khalid, B. Artificial intelligence-powered dentistry: Probing the potential, challenges, and ethicality of artificial intelligence in dentistry. Digit. Health 2024, 10, 20552076241291345. [Google Scholar] [CrossRef]
- Safitra, M.F.; Lubis, M.; Kusumasari, T.F.; Putri, D.P. Advancements in Artificial Intelligence and Data Science: Models, Applications, and Challenges. Procedia Comput. Sci. 2024, 234, 381–388. [Google Scholar] [CrossRef]
- Shafi, I.; Fatima, A.; Afzal, H.; Díez, I.d.l.T.; Lipari, V.; Breñosa, J.; Ashraf, I. A comprehensive review of recent advances in artificial intelligence for dentistry e-health. Diagnostics 2023, 13, 2196. [Google Scholar] [CrossRef]
- Alqutaibi, A.Y.; Algabri, R.S.; Alamri, A.S.; Alhazmi, L.S.; Almadani, S.M.; Alturkistani, A.M.; Almutairi, A.G. Advancements of artificial intelligence algorithms in predicting dental implant prognosis from radiographic images: A systematic review. J. Prosthet. Dent. 2024; Online ahead of print. [Google Scholar]
- Hassani, H.; Amiri Andi, P.; Ghodsi, A.; Norouzi, K.; Komendantova, N.; Unger, S. Shaping the future of smart dentistry: From Artificial Intelligence (AI) to Intelligence Augmentation (IA). IoT 2021, 2, 510–523. [Google Scholar] [CrossRef]
- Ossowska, A.; Kusiak, A.; Świetlik, D. Artificial intelligence in dentistry—Narrative review. Int. J. Environ. Res. Public Health 2022, 19, 3449. [Google Scholar] [CrossRef]
- Claman, D.; Sezgin, E. Artificial intelligence in dental education: Opportunities and challenges of large language models and multimodal foundation models. JMIR Med. Educ. 2024, 10, e52346. [Google Scholar] [CrossRef] [PubMed]
- Familoni, B.T.; Onyebuchi, N.C. Advancements and challenges in AI integration for technical literacy: A systematic review. Eng. Sci. Technol. J. 2024, 5, 1415–1430. [Google Scholar] [CrossRef]
- Alzaid, N.; Ghulam, O.; Albani, M.; Alharbi, R.; Othman, M.; Taher, H.; Albaradie, S.; Ahmed, S. Revolutionizing Dental Care: A Comprehensive Review of Artificial Intelligence Applications Among Various Dental Specialties. Cureus 2023, 15, e47033. [Google Scholar] [CrossRef]
- Bharadwaj, R.S.; Kalgeri, S.H.; Shivakumar, A.T.; Doddawad, V.; Shankar, P.M.; BB, S.K. Revolutionizing Dental Health Care: An In-Depth Exploration of Technological Advancements. Eur. J. Gen. Dent. 2024, 13, 001–014. [Google Scholar] [CrossRef]
- Surlari, Z.; Budală, D.G.; Lupu, C.I.; Stelea, C.G.; Butnaru, O.M.; Luchian, I. Current Progress and challenges of using artificial intelligence in clinical dentistry—A Narrative review. J. Clin. Med. 2023, 12, 7378. [Google Scholar] [CrossRef]
- Vinothkumar, J.; Karunamurthy, A. Recent Advancements in Artificial Intelligence Technology: Trends and Implications. Quing Int. J. Multidiscip. Sci. Res. Dev. 2023, 2, 1–11. [Google Scholar] [CrossRef]
- Musleh, D.; Almossaeed, H.; Balhareth, F.; Alqahtani, G.; Alobaidan, N.; Altalag, J.; Aldossary, M.I. Advancing Dental Diagnostics: A Review of Artificial Intelligence Applications and Challenges in Dentistry. Big Data Cogn. Comput. 2024, 8, 66. [Google Scholar] [CrossRef]
- Mishra, S.; Abbas, M.; Jindal, K.; Narayan, J.; Dwivedy, S.K. Artificial intelligence-based technological advancements in clinical healthcare applications: A systematic review. In Revolutions in Product Design for Healthcare, Design Science and Innovation; Springer: Singapore, 2022; pp. 207–227. [Google Scholar]
- Taherdoost, H.; Madanchian, M. AI Advancements: Comparison of Innovative Techniques. AI 2023, 5, 38–54. [Google Scholar] [CrossRef]
- Malik, A. The Future of AI: Predicting Technological Advancements and Their Societal Impact. Front. Artif. Intell. Res. 2024, 1, 467–493. [Google Scholar]
- Da Silva, M.; Horsley, T.; Singh, D.; Da Silva, E.; Ly, V.; Thomas, B.; Daniel, R.C.; Chagal-Feferkorn, K.A.; Iantomasi, S.; White, K. Legal concerns in health-related artificial intelligence: A scoping review protocol. Syst. Rev. 2022, 11, 123. [Google Scholar] [CrossRef]
- Naeem, M.M.; Sarwar, H.; Hassan, M.T.; Balouch, N.M.; Singh, S.P.; Essrani, P.D.; Rajper, P. Exploring the ethical and privacy implications of artificial intelligence in dentistry. Int. J. Health Sci. 2023, 7, 904–915. [Google Scholar] [CrossRef]
- Roganović, J.; Radenković, M. Ethical Use of Artificial Intelligence in Dentistry. In Ethics-Scientific Research, Ethical Issues, Artificial Intelligence and Education; IntechOpen: London, UK, 2023. [Google Scholar]
- Cristache, C.M.; Mihut, T.; Burlacu-Vatamanu, O.-E.; Sgiea, E.-D. Exploring the Ethical and Legal Aspects of Digital Innovations in Preventive Dentistry. Leveraging Digit. Technol. Prev. Dent. 2024, 30, 109–138. [Google Scholar]
- Mörch, C.; Atsu, S.; Cai, W.; Li, X.; Madathil, S.; Liu, X.; Mai, V.; Tamimi, F.; Dilhac, M.; Ducret, M. Artificial intelligence and ethics in dentistry: A scoping review. J. Dent. Res. 2021, 100, 1452–1460. [Google Scholar] [CrossRef]
- Rokhshad, R.; Ducret, M.; Chaurasia, A.; Karteva, T.; Radenkovic, M.; Roganovic, J.; Hamdan, M.; Mohammad-Rahimi, H.; Krois, J.; Lahoud, P. Ethical considerations on artificial intelligence in dentistry: A framework and checklist. J. Dent. 2023, 135, 104593. [Google Scholar] [CrossRef] [PubMed]
- Maart, R.; Mulder, R. Ethical considerations for artificial intelligence in dentistry. S. Afr. Dent. J. 2024, 79, 260–262. [Google Scholar] [CrossRef]
- Patcas, R.; Bornstein, M.M.; Schätzle, M.A.; Timofte, R. Artificial intelligence in medico-dental diagnostics of the face: A narrative review of opportunities and challenges. Clin. Oral Investig. 2022, 26, 6871–6879. [Google Scholar] [CrossRef]
- Duggal, I.; Tripathi, T. Ethical principles in dental healthcare: Relevance in the current technological era of artificial intelligence. J. Oral Biol. Craniofacial Res. 2024, 14, 317–321. [Google Scholar] [CrossRef] [PubMed]
- Lin, G.S.S.; Foo, J.Y.; Goh, S.M.; Alam, M.K. Exploring the Ethical Dimensions of Artificial Intelligence and Robotics in Dental Education. Bangladesh J. Med. Sci. 2024, 23, 999–1007. [Google Scholar]
- Minssen, T.; Solaiman, B.; Köttering, L.; Wested, J.; Malik, A. Governing AI in the European Union: Emerging infrastructures and regulatory ecosystems in health 1. Res. Handb. Health AI Law 2024, 311–331. [Google Scholar]
- Singh, V.; Cheng, S.; Kwan, A.C.; Ebinger, J. United States Food and Drug Administration Regulation of Clinical Software in the Era of Artificial Intelligence and Machine Learning. Mayo Clin. Proc. Digit. Health 2025, 3, 100231. [Google Scholar] [CrossRef]
- Ivanišević, A.; Tadin, A. Artificial Intelligence and Modern Technology in Dentistry: Attitudes, Knowledge, Use, and Barriers Among Dentists in Croatia—A Survey-Based Study. Clin. Pract. 2024, 14, 2623–2636. [Google Scholar] [CrossRef]
- Singh, N.; Pandey, A.; Tikku, A.P.; Verma, P.; Singh, B.P. Attitude, perception and barriers of dental professionals towards artificial intelligence. J. Oral Biol. Craniofacial Res. 2023, 13, 584–588. [Google Scholar] [CrossRef]
- Müller, A.; Mertens, S.M.; Göstemeyer, G.; Krois, J.; Schwendicke, F. Barriers and enablers for artificial intelligence in dental diagnostics: A qualitative study. J. Clin. Med. 2021, 10, 1612. [Google Scholar] [CrossRef]
- Lin, G.S.S.; Ng, Y.S.; Ghani, N.R.N.A.; Chua, K.H. Revolutionising dental technologies: A qualitative study on dental technicians’ perceptions of Artificial intelligence integration. BMC Oral Health 2023, 23, 690. [Google Scholar] [CrossRef] [PubMed]
- Adnan, K.; Khan, M.K.; Umar, M.; Umair, M. A Systematic Analysis of Artificial Intelligence in Dentistry. J. Comput. Biomed. Inform. 2023, 5, 74–81. [Google Scholar]
- Grischke, J.; Johannsmeier, L.; Eich, L.; Griga, L.; Haddadin, S. Dentronics: Towards robotics and artificial intelligence in dentistry. Dent. Mater. 2020, 36, 765–778. [Google Scholar] [CrossRef] [PubMed]
- Alsharari, M.O.; Aldahabani, S.H.; Alsharari, F.M.; Alsharari, A.M. The future of dental prosthetics: Artificial Intelligence and Machine Learning applications. Afr. J. Biomed. Res. 2024, 27, 1063–1070. [Google Scholar]



| Imaging Modality | Diagnostic Task | Common AI Models | Performance Metrics (Generalized) | Clinical Validation Level |
|---|---|---|---|---|
| Cone-Beam Computed Tomography (CBCT) | Anatomical segmentation, lesion detection | U-Net, Mask R-CNN, ResNet-based CNNs | High accuracy (>90%), strong lesion detection (AUC ~0.90) | Validated via prospective clinical and multi-center studies |
| Intraoral Photography | Caries detection, periodontal classification | VGG16, ResNet50, DenseNet | Accuracy (~90–95%), high clinician correlation | Pilot studies, clinician correlation studies |
| Digital Radiography | Periapical lesion identification | YOLOv8, Faster R-CNN | High sensitivity (~90%), specificity (~85–90%) | Retrospective dataset validations across multiple clinics |
| Predictive Application | Clinical Status | Example Use-Cases | Validation and Impact |
|---|---|---|---|
| Periodontal Disease Progression | Clinically Implemented | Routine risk assessments, preventive care | Validated via longitudinal clinical trials; widely adopted |
| Orthodontic Treatment Outcomes | Clinically Implemented | Treatment duration, personalized planning | Prospective studies confirming predictive accuracy in clinics |
| Implant Success Prediction | Emerging/Theoretical | Implant planning, personalized risk analysis | Early-stage retrospective analyses; ongoing clinical validation needed |
| Oral Cancer Prognostics | Emerging/Theoretical | Cancer progression prediction, precision care | Promising preliminary results; awaiting larger clinical trials |
| AI Tool/Technology | Key Applications | Clinical Benefits |
|---|---|---|
| Automated Machine Learning (AutoML) | Sorting and classifying dental data (EHRs) | Reduced documentation workload, improved data management |
| Robotic Process Automation (RPA) | Billing, scheduling, claims processing | Reduced clerical errors, improved operational effectiveness |
| AI-enhanced Patient Communication Tools | Interactive patient inquiry, virtual consultations, language translation | Enhanced patient engagement and satisfaction |
| CAD-CAM and Virtual Simulations | Computerized impressions, treatment planning | Streamlined clinical and laboratory workflows |
| AI-powered Scheduling & Predictive Analysis | Appointment optimization, resource allocation | Enhanced resource use, reduced administrative costs |
| Laboratory Automation Platforms | Remote lab operations, task management | Improved productivity, minimized manual intervention |
| AI Document Processing | Processing unstructured documentation, recordkeeping | Increased efficiency, improved information retrieval |
| AI Claims Processing Software | Reimbursement management | Reduced errors and delays, faster claims processing |
| XAI | Improved transparency and interpretability of AI decisions | Enhanced clinician trust and adoption |
| Federated Learning | Decentralized AI model training, data privacy preservation | Improved data security, ethical AI integration |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, T.-Y.; Lee, K.-H.; Mukundan, A.; Karmakar, R.; Dhiman, H.; Wang, H.-C. AI in Dentistry: Innovations, Ethical Considerations, and Integration Barriers. Bioengineering 2025, 12, 928. https://doi.org/10.3390/bioengineering12090928
Liu T-Y, Lee K-H, Mukundan A, Karmakar R, Dhiman H, Wang H-C. AI in Dentistry: Innovations, Ethical Considerations, and Integration Barriers. Bioengineering. 2025; 12(9):928. https://doi.org/10.3390/bioengineering12090928
Chicago/Turabian StyleLiu, Tao-Yuan, Kun-Hua Lee, Arvind Mukundan, Riya Karmakar, Hardik Dhiman, and Hsiang-Chen Wang. 2025. "AI in Dentistry: Innovations, Ethical Considerations, and Integration Barriers" Bioengineering 12, no. 9: 928. https://doi.org/10.3390/bioengineering12090928
APA StyleLiu, T.-Y., Lee, K.-H., Mukundan, A., Karmakar, R., Dhiman, H., & Wang, H.-C. (2025). AI in Dentistry: Innovations, Ethical Considerations, and Integration Barriers. Bioengineering, 12(9), 928. https://doi.org/10.3390/bioengineering12090928









