Figure 1.
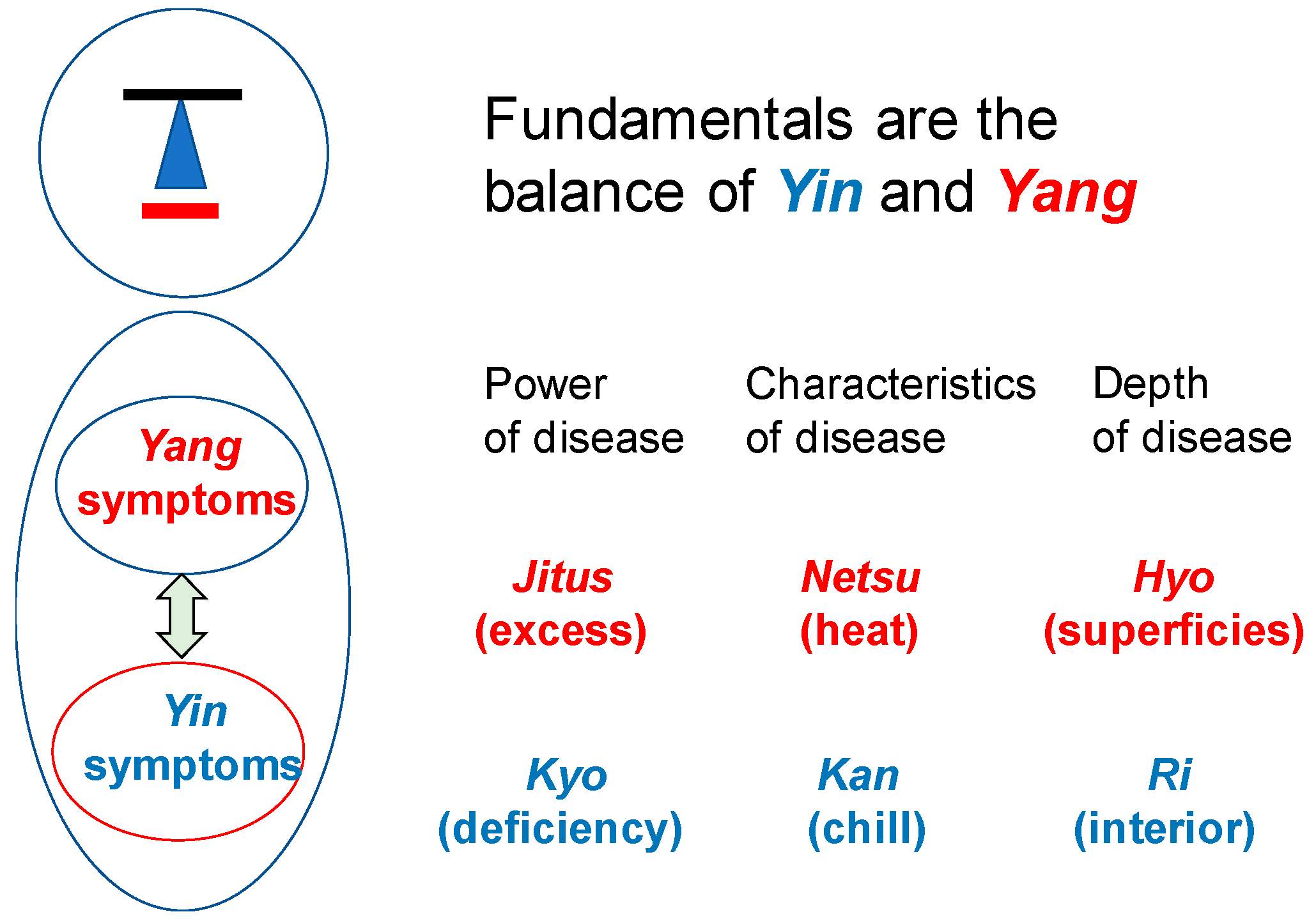
Concepts of Kampo therapy. Kampo therapy begins with the knowledge of constitutional characteristics of patient’s body. In-Yo or Yin-Yang: When the switch-over between two representative autonomic nerves, the sympathetic nerves (yang) and the parasympathetic nerves (yin), is good, the yin-yang balance is kept well. Kyo-Jits or asthenia and sthenia show physical strength, constitutional characteristics of body and the strength of resistance against disease. The reaction differs, depending on their Kyo-Sho or Jitsu-Sho. It is categorized into Jitsu-Sho (excess symptom), Kyo-Sho (deficiency symptom) and Chukan-Sho (symptom in-between the two). Kan-Netsu or chills and fever: Kan is Yin while Netsu is Yang. They are always in a relative relation. When Yin deteriorates, Yang predominates, called Netsu-sho (heat syndrome).
Figure 1.
Concepts of Kampo therapy. Kampo therapy begins with the knowledge of constitutional characteristics of patient’s body. In-Yo or Yin-Yang: When the switch-over between two representative autonomic nerves, the sympathetic nerves (yang) and the parasympathetic nerves (yin), is good, the yin-yang balance is kept well. Kyo-Jits or asthenia and sthenia show physical strength, constitutional characteristics of body and the strength of resistance against disease. The reaction differs, depending on their Kyo-Sho or Jitsu-Sho. It is categorized into Jitsu-Sho (excess symptom), Kyo-Sho (deficiency symptom) and Chukan-Sho (symptom in-between the two). Kan-Netsu or chills and fever: Kan is Yin while Netsu is Yang. They are always in a relative relation. When Yin deteriorates, Yang predominates, called Netsu-sho (heat syndrome).
Figure 2.
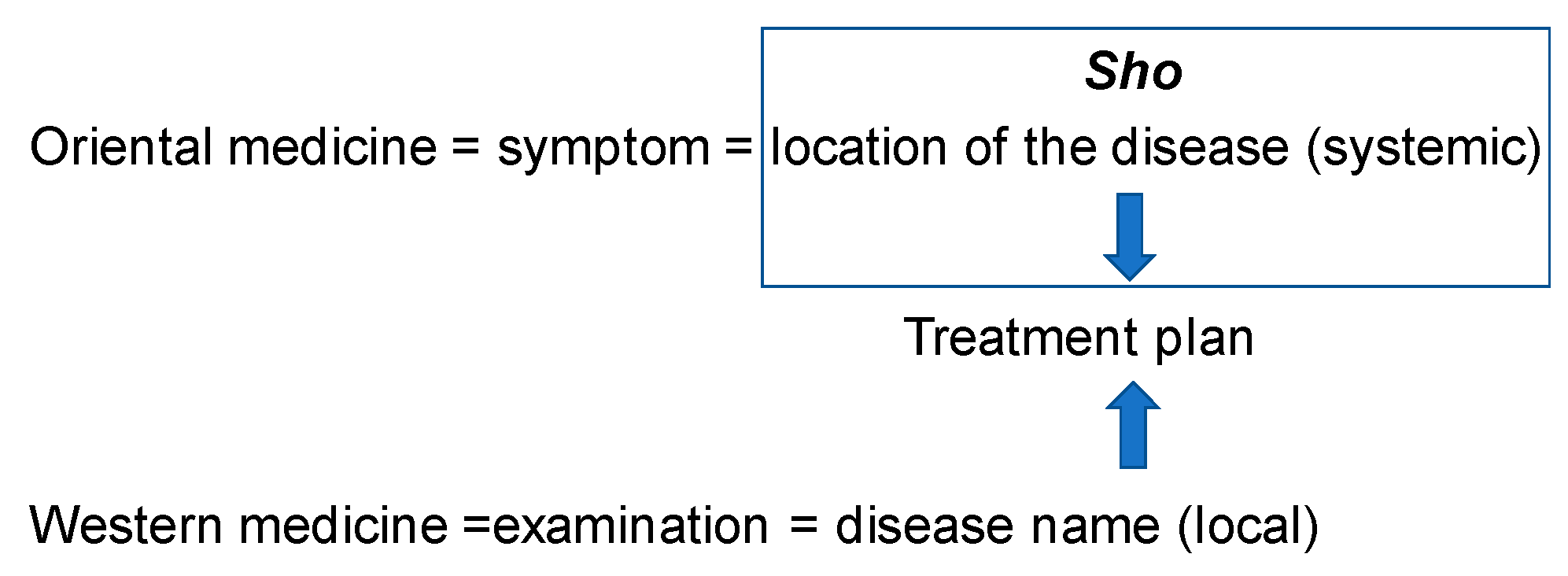
Characteristics of Oriental medicine and Western medicine therapy. Sho (Kampo Diagnosis): Capturing the Shoko (yin-yang, Kyo-Jitsu or deficiency and excess, Kan-Netsu or chills and fever, Hyo-Ri or superficies and interior) as the holistic symptom caused by the pathological condition and it shows the condition of the patient at the time of diagnosis. Sho changes depending on the bodily sensation.
Figure 2.
Characteristics of Oriental medicine and Western medicine therapy. Sho (Kampo Diagnosis): Capturing the Shoko (yin-yang, Kyo-Jitsu or deficiency and excess, Kan-Netsu or chills and fever, Hyo-Ri or superficies and interior) as the holistic symptom caused by the pathological condition and it shows the condition of the patient at the time of diagnosis. Sho changes depending on the bodily sensation.
Figure 3.
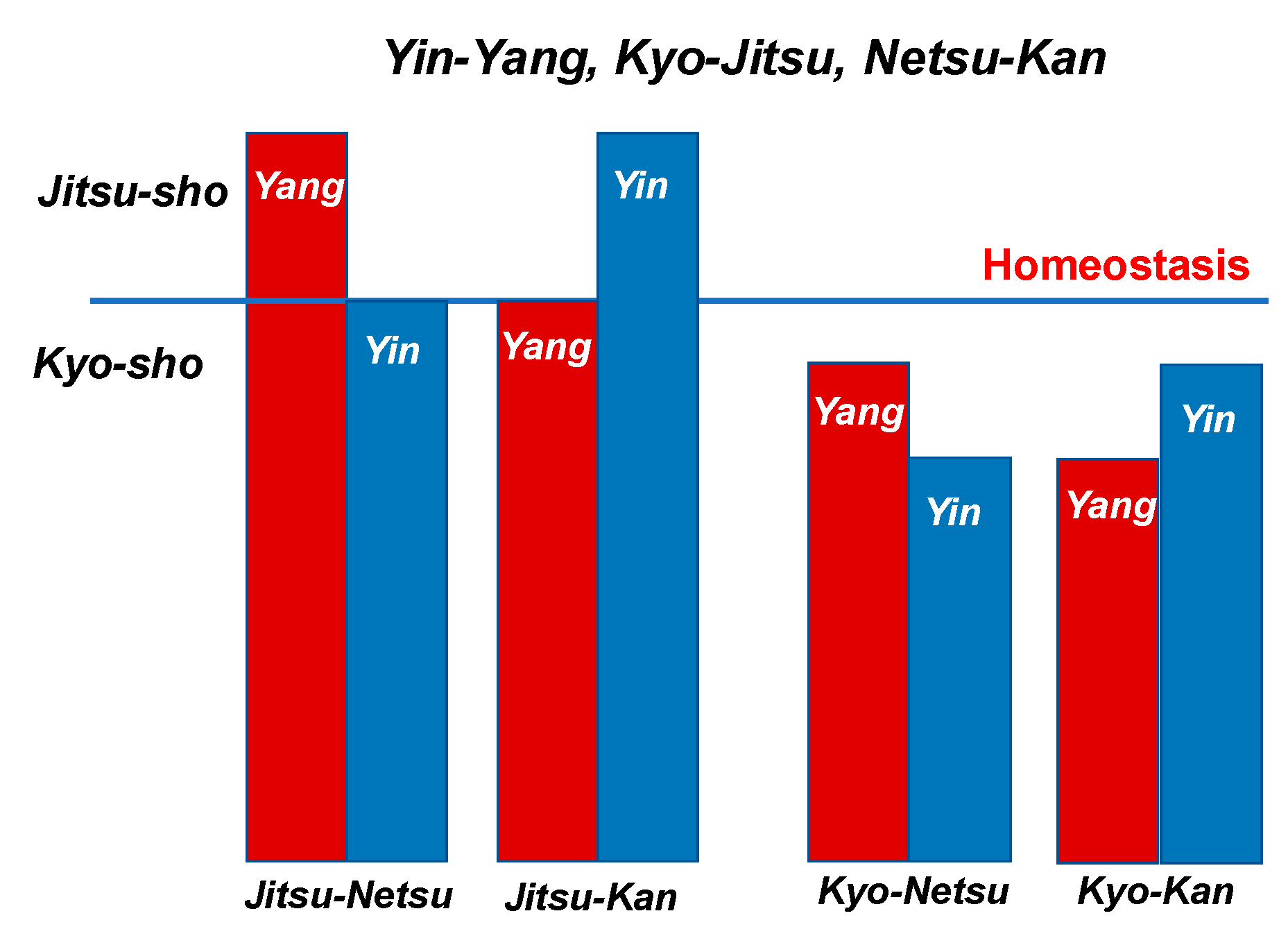
Condition categories of Yin-Yang, Kyo-sho and Netsu-Kan in the body.
Figure 3.
Condition categories of Yin-Yang, Kyo-sho and Netsu-Kan in the body.
Figure 4.
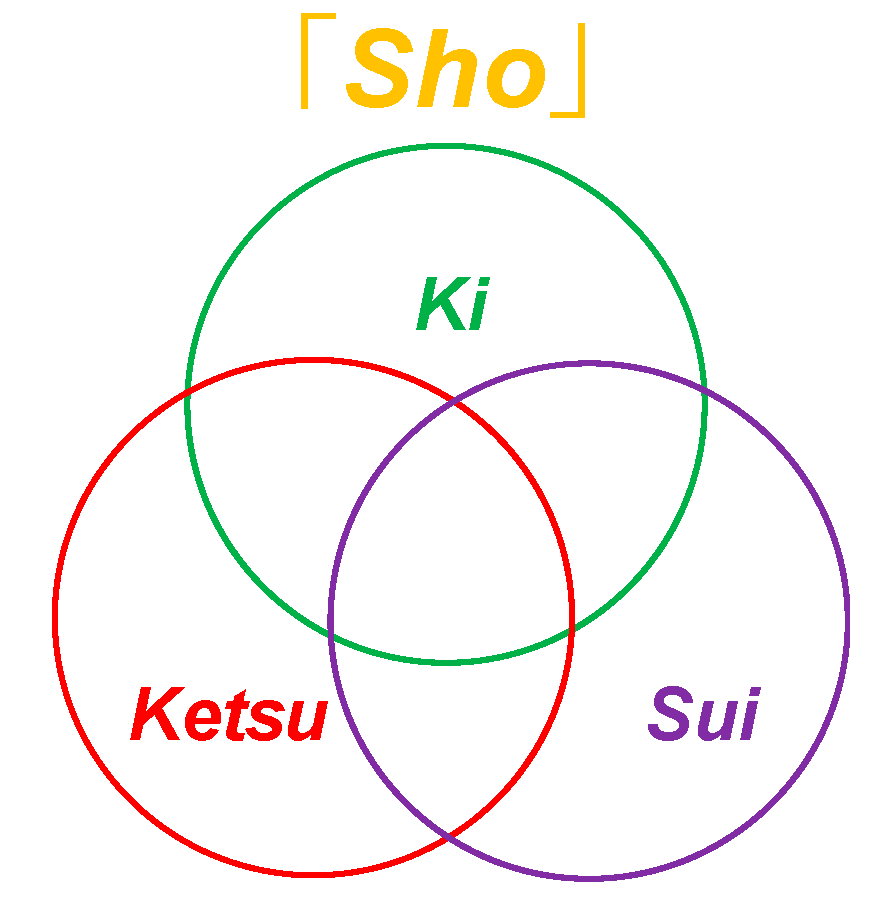
Diagrams of biological factors in Sho.
Figure 4.
Diagrams of biological factors in Sho.
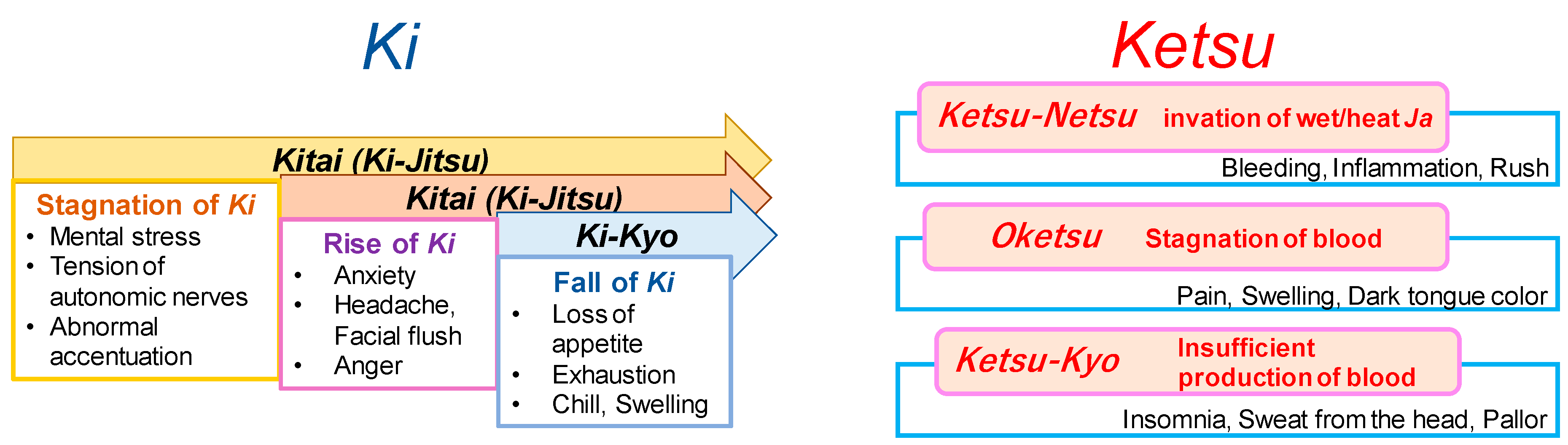
Figure 5.
The concepts of Ki and Ketsu.
Figure 5.
The concepts of Ki and Ketsu.
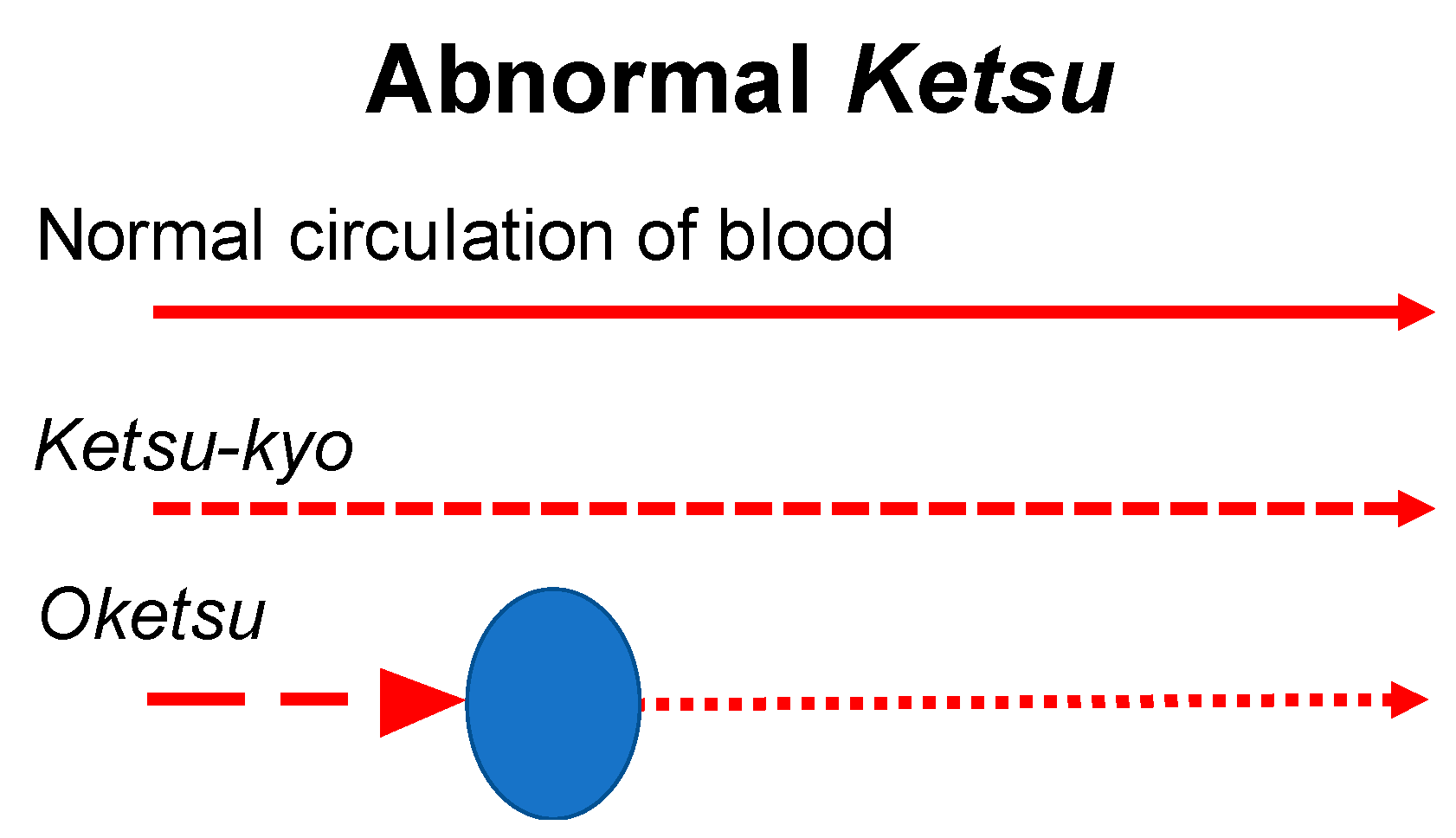
Figure 6.
The Symptoms of Oketsu, in blood stagnation.
Figure 6.
The Symptoms of Oketsu, in blood stagnation.
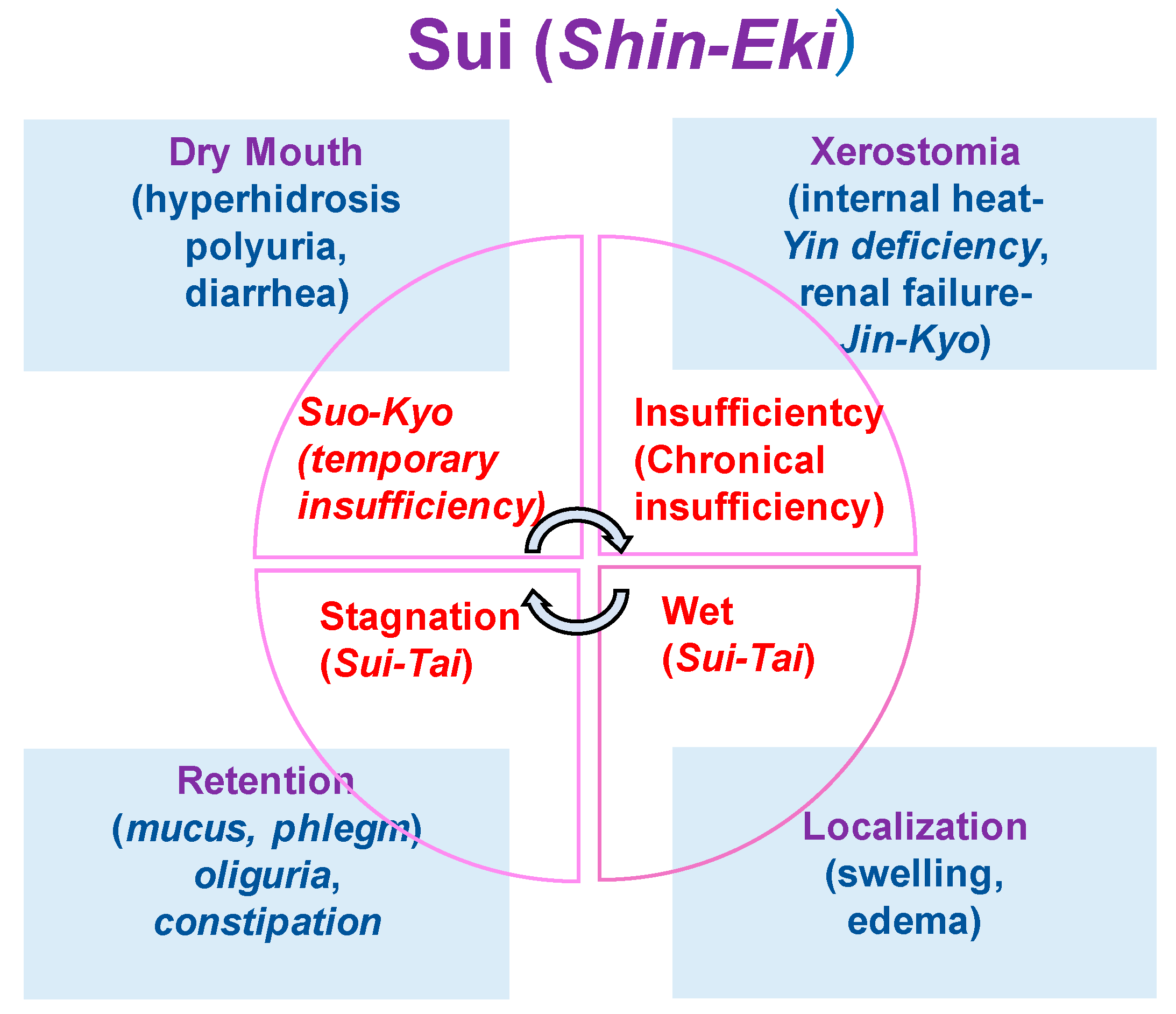
Figure 7.
The concepts of Sui (Shin-Eki).
Figure 7.
The concepts of Sui (Shin-Eki).
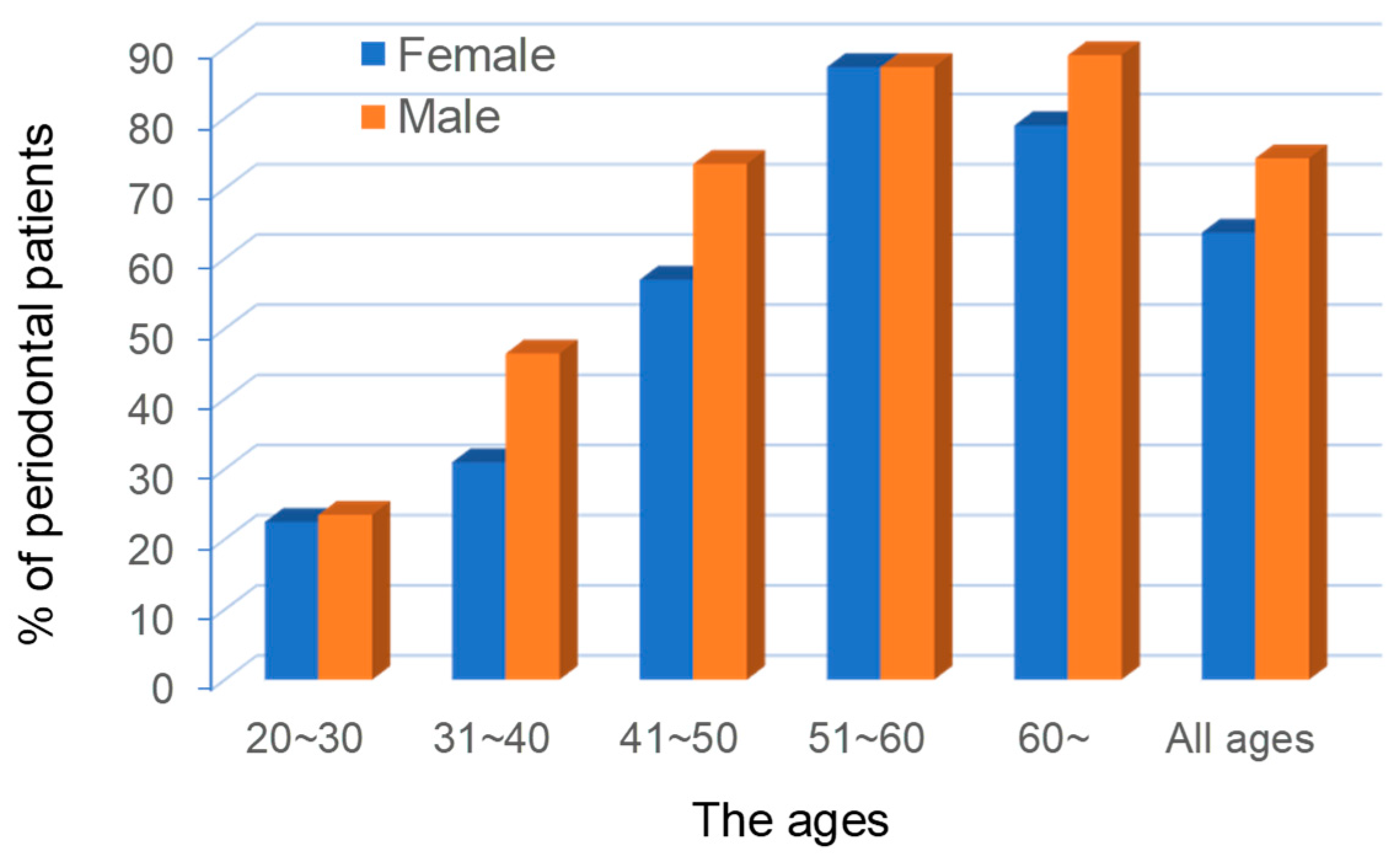
Figure 8.
The proportions of poor blood circulation (
Oketu) in the ages of the periodontal patients. Cited from [
9] with permission.
Figure 8.
The proportions of poor blood circulation (
Oketu) in the ages of the periodontal patients. Cited from [
9] with permission.
Figure 9.
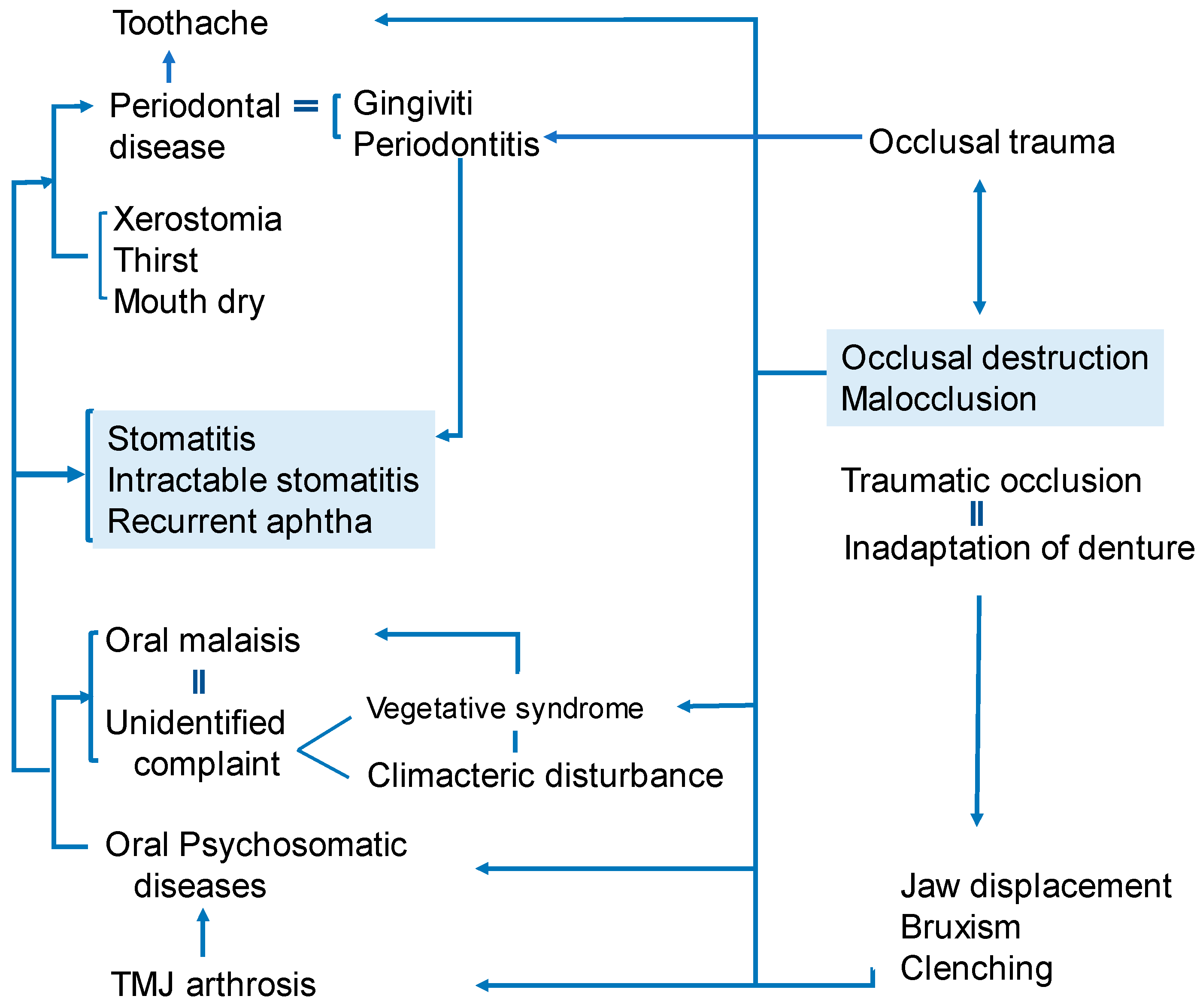
The correlations between occlusal-related troubles and oral diseases. (Watanabe S, unpublished data)
Figure 9.
The correlations between occlusal-related troubles and oral diseases. (Watanabe S, unpublished data)
Figure 10.
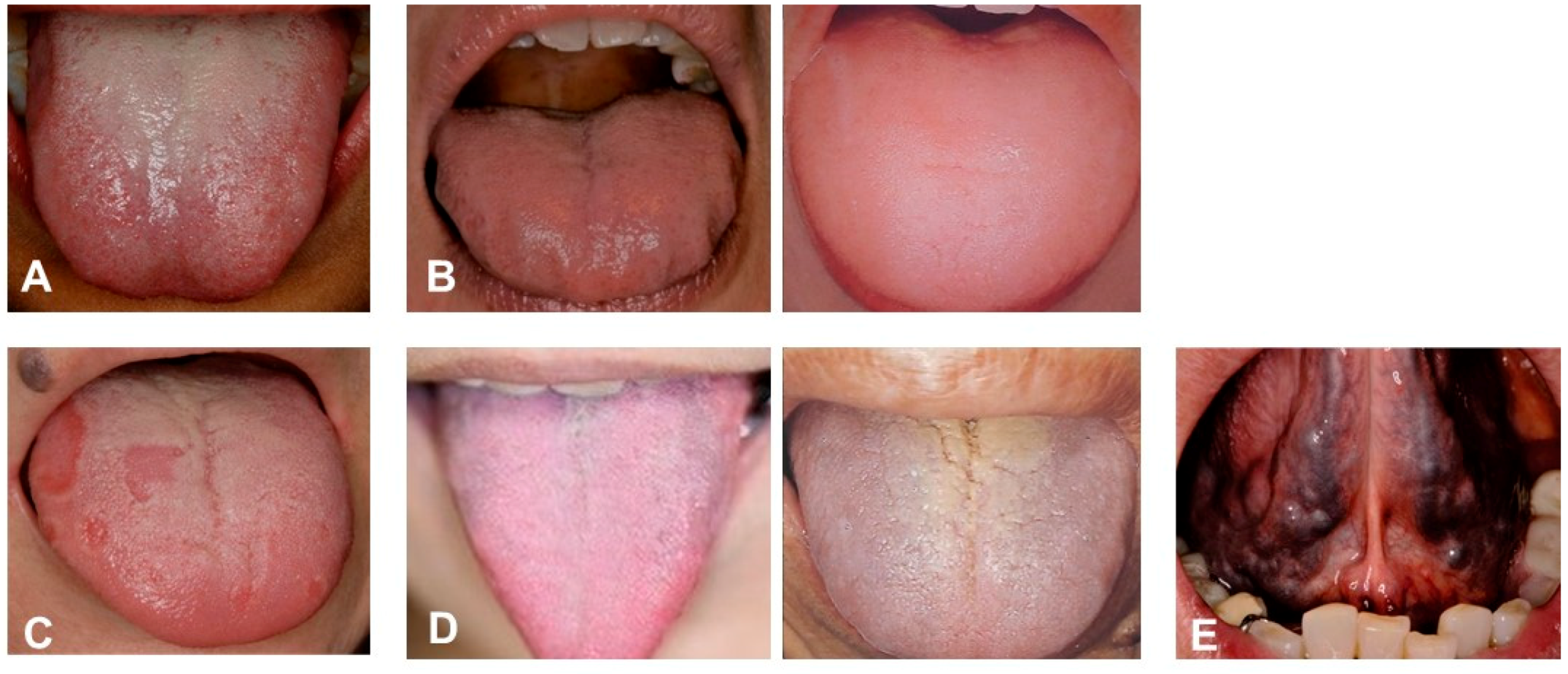
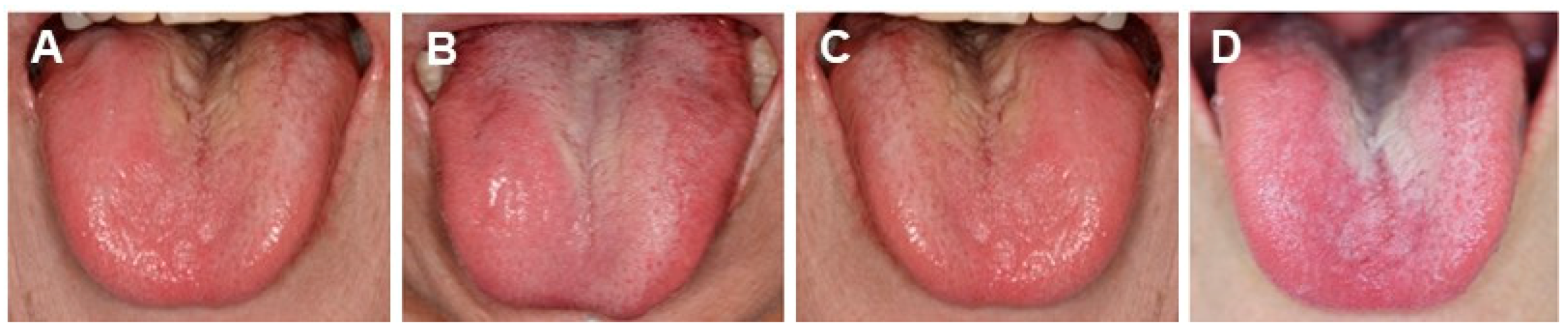
Tongue diagnosis of patients. (A) Clinical observation of Healthy tongue. Properly moistened: tongue coating white colour, thinly spread across the tongue. Light pink colour, Shape: fitting within the mouth. Back of tongue: sublingual vein is not over swelling. (B) Abnormal tongue (Sui). Tongue peripheral impression, swelling tongue (oedema). Left: Sui-Tai or water stagnationis oedema, tongue peripheral impression. Pressure impression by the teeth on the edge of the tongue where water is sustained. Right: Sui-Kyo (insufficient water): oedema, water is not flowing well; big and swollen. (C) Abnormal Ki (vital energy). Map-like tongue, insufficient Ki, slow circulation of Ki. Warming: Workings of warm-up and circulation; central of Ki. Defence: Workings to promote natural healing; protects skin and membrane and defends the body from the cause of disease. (D) Abnormal tongue (Ketsu-Kyo and Kyo-Netsu). Ketsu (blood circulation) indicate the body of the tongue and sublingual vein that are in reddish purple, colour change of the tongue coating (Ketsu-Kyo, Kyo-Netsu). Left: Ketsu-Kyo: Tongue is thin and lean; Nutrition, water and blood circulation were insufficient. Right: Kyo-Netsu: Sticky blood; stagnated; Nutrition. water and blood body fluids were insufficient. Body is dry, since the heat remains to circulate internally. (E) Abnormal tongue (Okesu). Blood heat condition in tongue. Ischemia (tongue: cyanosis) and over-swelling of sublingual veins. Systemically impaired flow of blood. These photos were taken, after obtaining the informed consent from the patients, under the condition that the patients are not identified. (Watanabe S, unpublished data)
Figure 10.
Tongue diagnosis of patients. (A) Clinical observation of Healthy tongue. Properly moistened: tongue coating white colour, thinly spread across the tongue. Light pink colour, Shape: fitting within the mouth. Back of tongue: sublingual vein is not over swelling. (B) Abnormal tongue (Sui). Tongue peripheral impression, swelling tongue (oedema). Left: Sui-Tai or water stagnationis oedema, tongue peripheral impression. Pressure impression by the teeth on the edge of the tongue where water is sustained. Right: Sui-Kyo (insufficient water): oedema, water is not flowing well; big and swollen. (C) Abnormal Ki (vital energy). Map-like tongue, insufficient Ki, slow circulation of Ki. Warming: Workings of warm-up and circulation; central of Ki. Defence: Workings to promote natural healing; protects skin and membrane and defends the body from the cause of disease. (D) Abnormal tongue (Ketsu-Kyo and Kyo-Netsu). Ketsu (blood circulation) indicate the body of the tongue and sublingual vein that are in reddish purple, colour change of the tongue coating (Ketsu-Kyo, Kyo-Netsu). Left: Ketsu-Kyo: Tongue is thin and lean; Nutrition, water and blood circulation were insufficient. Right: Kyo-Netsu: Sticky blood; stagnated; Nutrition. water and blood body fluids were insufficient. Body is dry, since the heat remains to circulate internally. (E) Abnormal tongue (Okesu). Blood heat condition in tongue. Ischemia (tongue: cyanosis) and over-swelling of sublingual veins. Systemically impaired flow of blood. These photos were taken, after obtaining the informed consent from the patients, under the condition that the patients are not identified. (Watanabe S, unpublished data)
![Medicines 06 00034 g010 Medicines 06 00034 g010]()
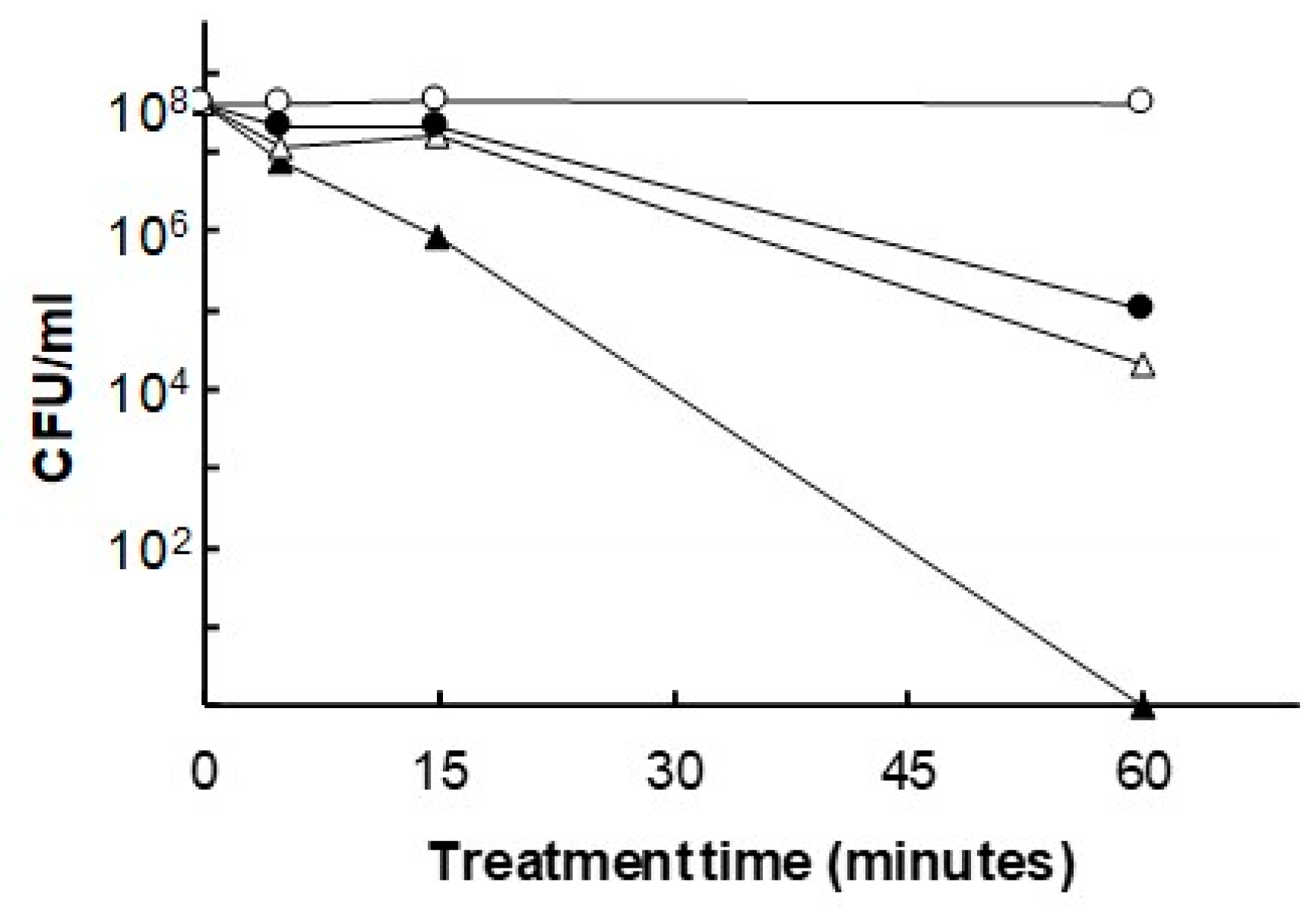
Figure 11.
Antibacterial effect of JTT on
P. gingivalis. Bacterial cells were treated with 10 mg/mL (▲), 1 mg/mL (△) or 0.1 mg/mL of JTT (●) or 0 mg/mL of JTT (〇) for the indicated period. At the end of the incubation period, a 10-fold serial dilution was performed in phosphate-buffered saline (PBS; pH 7.4) and spread onto a BHI blood agar plate broth supplemented with hemin (5 µg/mL), vitamin K
1 (0.2 µg/mL) and yeast extract (5 mg/mL). The number of CFU (colony forming unit) was determined after 7 days of incubation under anaerobic conditions (CO
2: 10%, H
2: 10%, N
2: 80%) at 37°C. Cited from [
14] with permission.
Figure 11.
Antibacterial effect of JTT on
P. gingivalis. Bacterial cells were treated with 10 mg/mL (▲), 1 mg/mL (△) or 0.1 mg/mL of JTT (●) or 0 mg/mL of JTT (〇) for the indicated period. At the end of the incubation period, a 10-fold serial dilution was performed in phosphate-buffered saline (PBS; pH 7.4) and spread onto a BHI blood agar plate broth supplemented with hemin (5 µg/mL), vitamin K
1 (0.2 µg/mL) and yeast extract (5 mg/mL). The number of CFU (colony forming unit) was determined after 7 days of incubation under anaerobic conditions (CO
2: 10%, H
2: 10%, N
2: 80%) at 37°C. Cited from [
14] with permission.
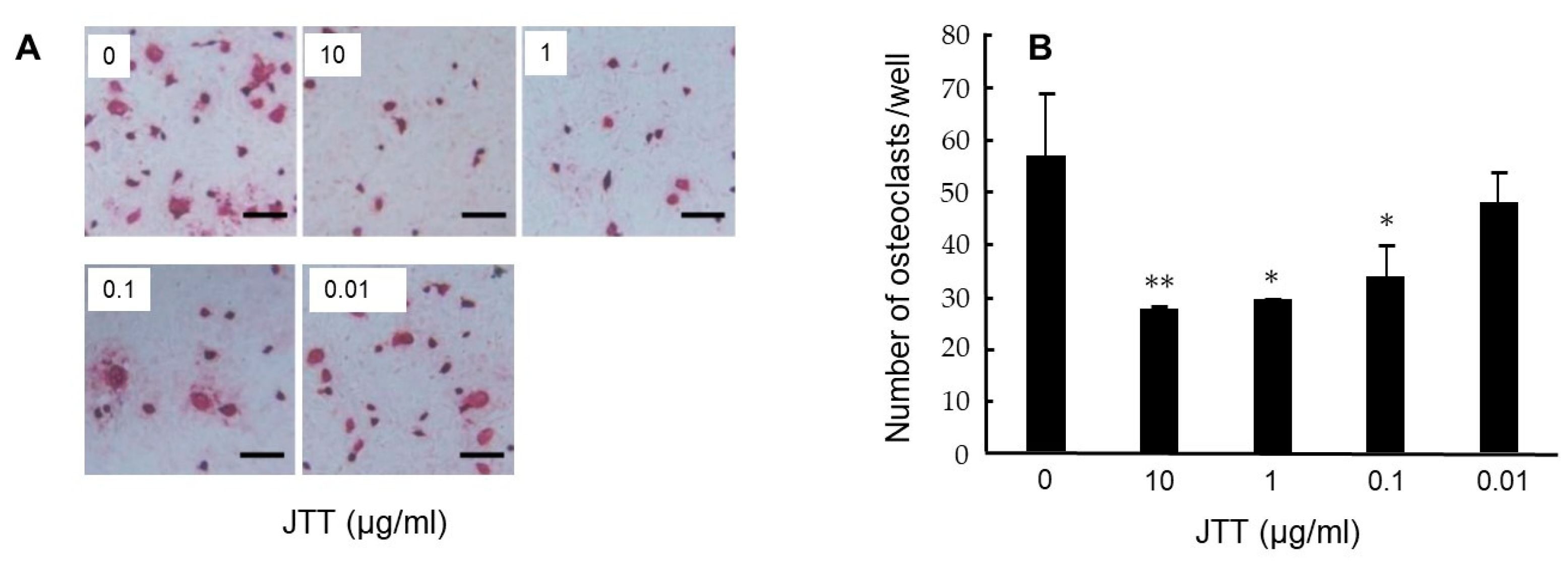
Figure 12.
JTT inhibits osteoclast differentiation of BALB/c mouse bone marrow cells co-cultured with MC3T3-G2/PA6 cells. After incubation for 7 days, co-cultured cells were stained for TRAP (
A) and determination of TRAP-positive multinucleated cells containing three or more nuclei (
B). Results are expressed as the mean ±SD of triplicate cultures. **
p < 0.01, *
p < 0.05. Cited from [
14] with permission.
Figure 12.
JTT inhibits osteoclast differentiation of BALB/c mouse bone marrow cells co-cultured with MC3T3-G2/PA6 cells. After incubation for 7 days, co-cultured cells were stained for TRAP (
A) and determination of TRAP-positive multinucleated cells containing three or more nuclei (
B). Results are expressed as the mean ±SD of triplicate cultures. **
p < 0.01, *
p < 0.05. Cited from [
14] with permission.
Figure 13.
Changes of the tongue surfaces at 1 (A), 4 (B), 8 (C) or 12 (D) months after GRS + JTT treatment. (Presented in Kanagawa Dental College Society 53rd General Assembly: A case in which Kampo and denture adjustment was successful for patients complaining of denture). Photos were taken, after obtaining the informed consent from the patient. (Watanabe S, unpublished data)
Figure 13.
Changes of the tongue surfaces at 1 (A), 4 (B), 8 (C) or 12 (D) months after GRS + JTT treatment. (Presented in Kanagawa Dental College Society 53rd General Assembly: A case in which Kampo and denture adjustment was successful for patients complaining of denture). Photos were taken, after obtaining the informed consent from the patient. (Watanabe S, unpublished data)
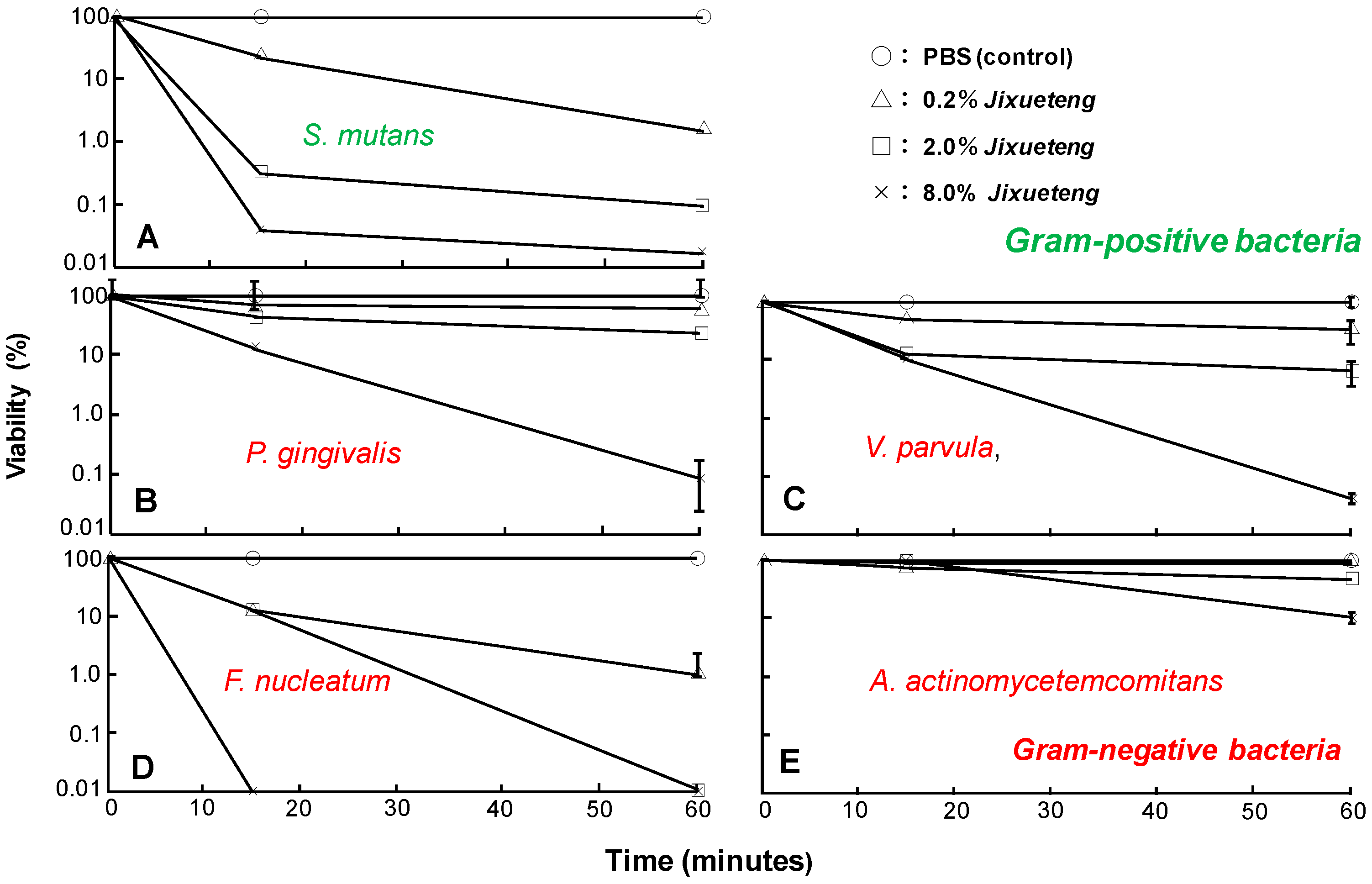
Figure 14.
Bactericidal effect of
Jixueteng against Gram-positive and -negative bacteria. Gram-positive bacteria (
S. mutans) (
A) and gram-negative bacteria (
B:
P. gingivalis,
C:
V. parvula,
D:
F. nucleatum,
E:
A. actinomycetemcomitans.) were treated by 0.2, 2 and 8% of the
Jixueteng extract for 1, 15 or 60 min. The suspensions were treated by PBS as a control. Cell viability was expressed as a percentage relative to control. Cited from [
23] with permission.
Figure 14.
Bactericidal effect of
Jixueteng against Gram-positive and -negative bacteria. Gram-positive bacteria (
S. mutans) (
A) and gram-negative bacteria (
B:
P. gingivalis,
C:
V. parvula,
D:
F. nucleatum,
E:
A. actinomycetemcomitans.) were treated by 0.2, 2 and 8% of the
Jixueteng extract for 1, 15 or 60 min. The suspensions were treated by PBS as a control. Cell viability was expressed as a percentage relative to control. Cited from [
23] with permission.
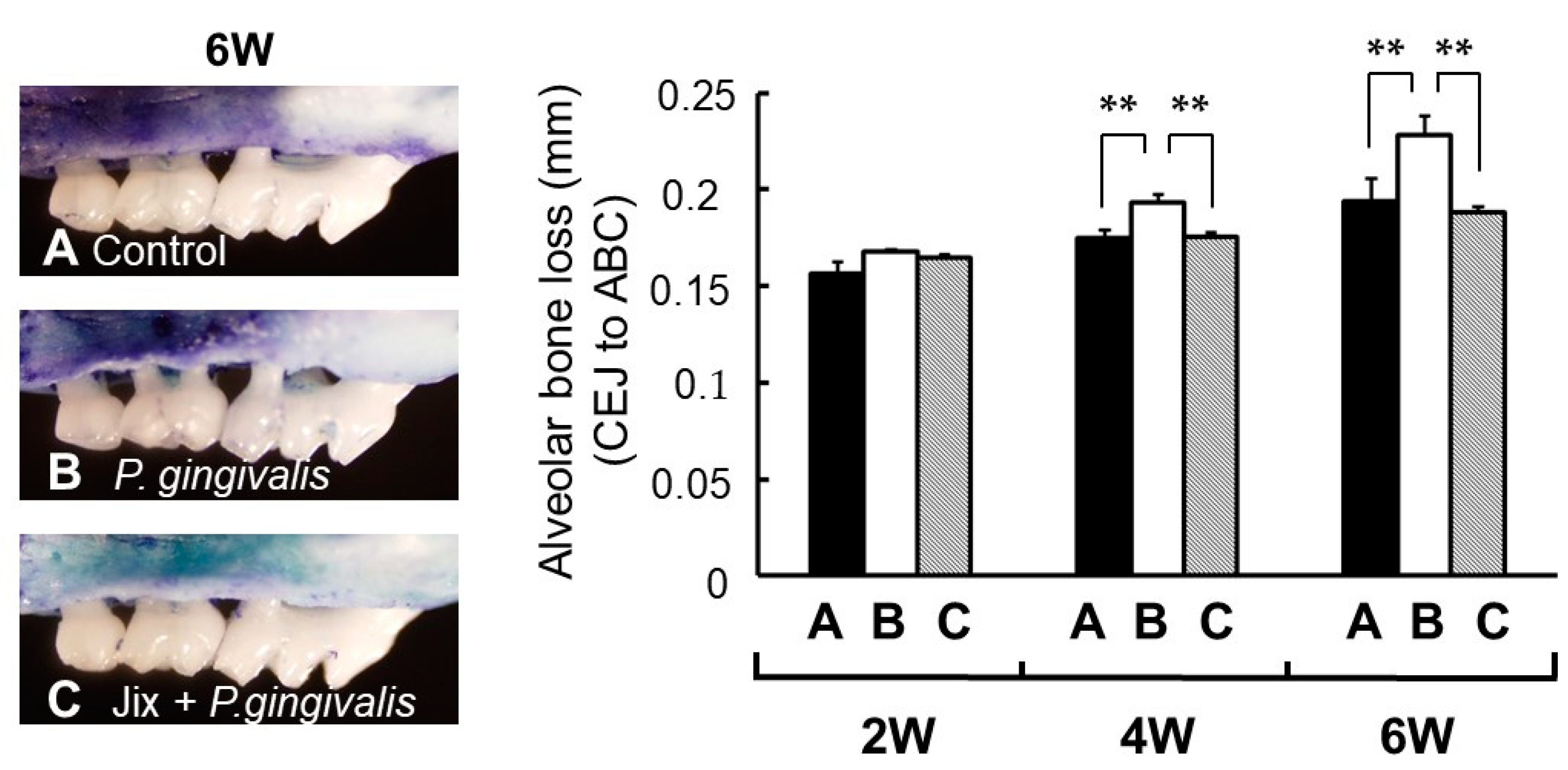
Figure 15.
Morphometric bone levels of 6 week after
P. gingivalis infection (left) and alveolar bone levels at 2, 4 and 6 weeks after
P. gingivalis infection (right).
A, non-infected control;
B, infected with
P. gingivalis;
C, Jixueteng administered group along with
P. gingivalis infection. Bone levels were evaluated by measuring the distance from the cemento-enamel junction (CEJ) to the alveolar bone crest (ABC) at seven palatal sites per mouse. Values indicate the mean bone loss levels ± standard error of the mean (n = 6/group). **: significantly different (
p < 0.01). Cited from [
28] with permission.
Figure 15.
Morphometric bone levels of 6 week after
P. gingivalis infection (left) and alveolar bone levels at 2, 4 and 6 weeks after
P. gingivalis infection (right).
A, non-infected control;
B, infected with
P. gingivalis;
C, Jixueteng administered group along with
P. gingivalis infection. Bone levels were evaluated by measuring the distance from the cemento-enamel junction (CEJ) to the alveolar bone crest (ABC) at seven palatal sites per mouse. Values indicate the mean bone loss levels ± standard error of the mean (n = 6/group). **: significantly different (
p < 0.01). Cited from [
28] with permission.
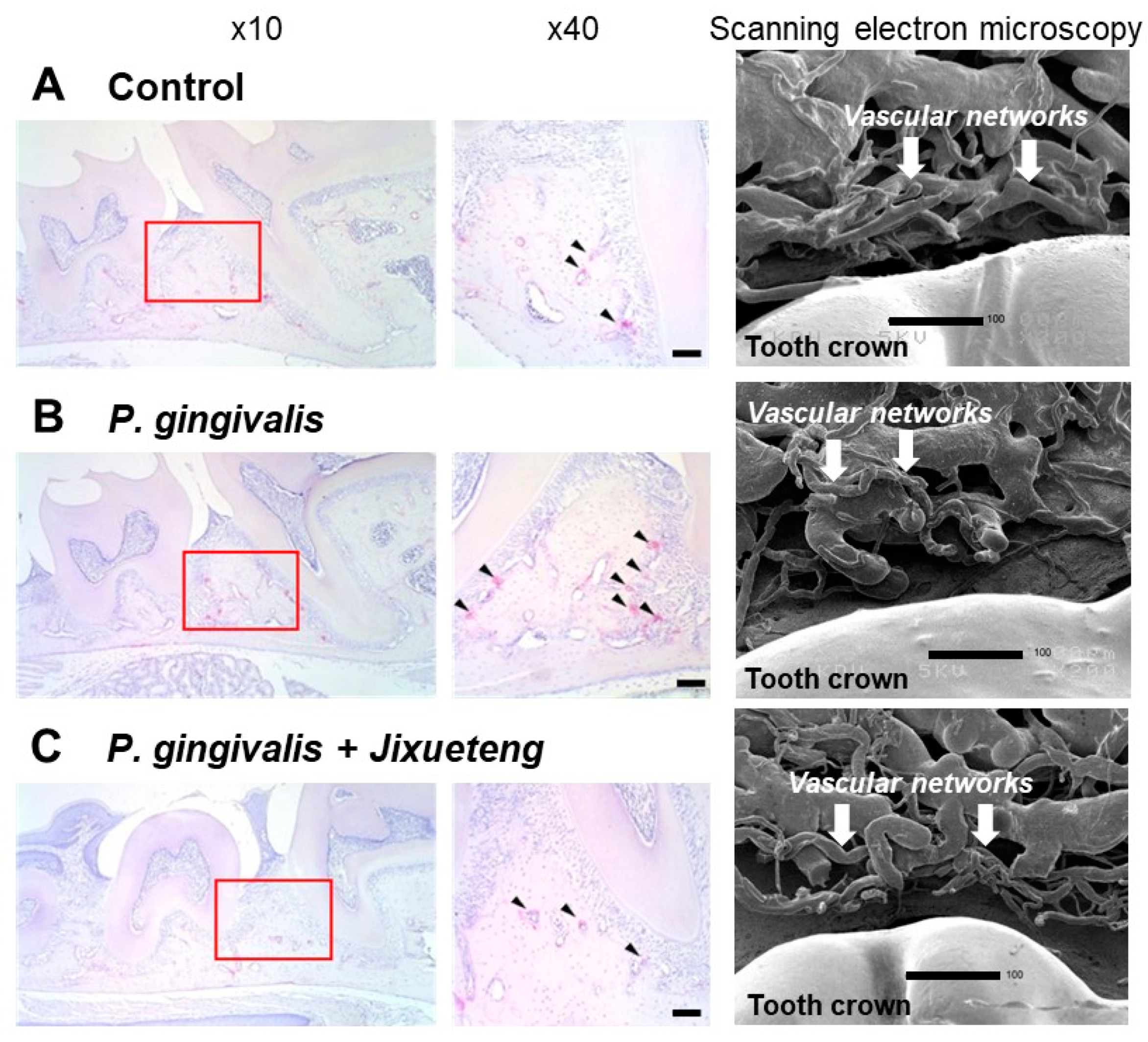
Figure 16.
Histopathological examination of mice periodontal tissues. Specimens obtained from the maxillary bone of mice were evaluated with TRAP staining. Osteoclasts (arrows) were observed along the alveolar septum of the maxillary molars.
A, con-infected control;
B, infected with
P. gingivalis;
C, administered
Jixueteng and infected with
P. gingivalis. Original magnification: × 10 and × 40. Bars: 100 μm. Scanning electron microscopy shows that compared to the normal group (
A), morphological degeneration of vessels in vascular networks and abnormality of the vascular lumen caused by
P. gingivalis infection were observed (
B). However, improvement in degeneration of these vascular networks and prolongation of the vascular plexus were observed by administration of
Jixueteng (
C). Cited from [
28] with permission.
Figure 16.
Histopathological examination of mice periodontal tissues. Specimens obtained from the maxillary bone of mice were evaluated with TRAP staining. Osteoclasts (arrows) were observed along the alveolar septum of the maxillary molars.
A, con-infected control;
B, infected with
P. gingivalis;
C, administered
Jixueteng and infected with
P. gingivalis. Original magnification: × 10 and × 40. Bars: 100 μm. Scanning electron microscopy shows that compared to the normal group (
A), morphological degeneration of vessels in vascular networks and abnormality of the vascular lumen caused by
P. gingivalis infection were observed (
B). However, improvement in degeneration of these vascular networks and prolongation of the vascular plexus were observed by administration of
Jixueteng (
C). Cited from [
28] with permission.
Figure 17.
Mastic tree (Pistacia lentiscus). (photos taken at Chios island, Greece, 2007)
Figure 17.
Mastic tree (Pistacia lentiscus). (photos taken at Chios island, Greece, 2007)
Figure 18.
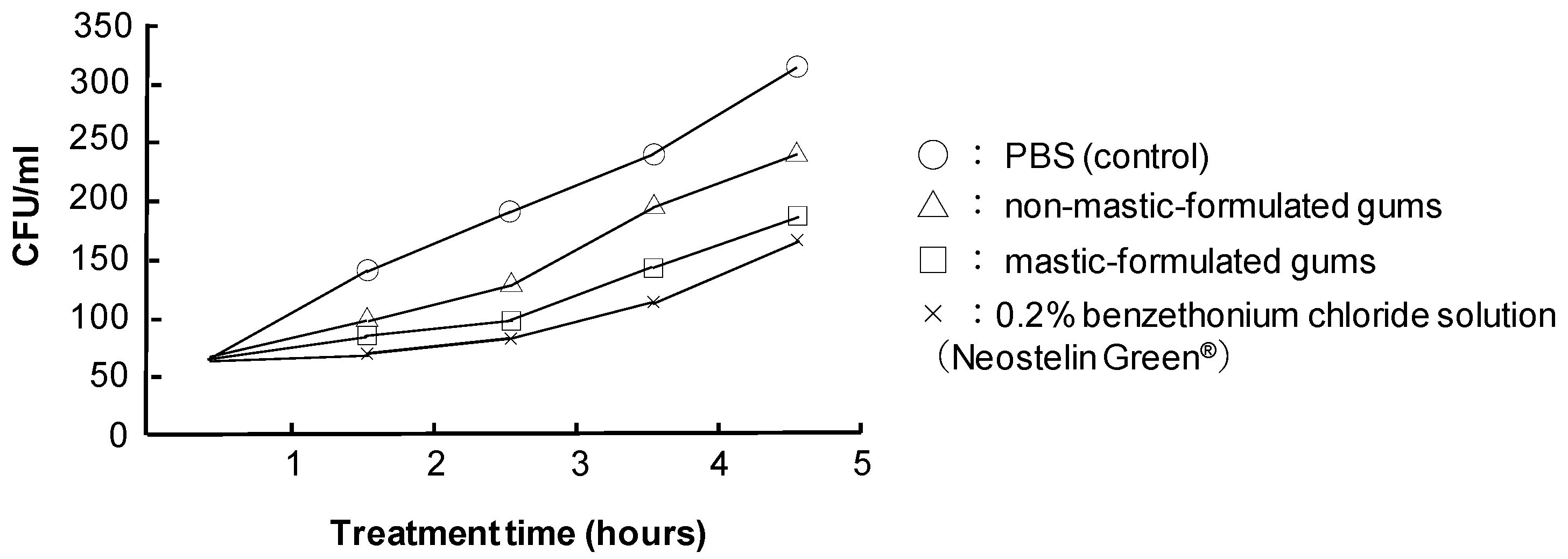
Bactericidal effect of mastic gum against oral bacteria. (Hamada N, unpublished data)
Figure 18.
Bactericidal effect of mastic gum against oral bacteria. (Hamada N, unpublished data)
Figure 19.
Toothpaste and mouth-rinse including mastic and IMPLA CARE. (unpublished data)
Figure 19.
Toothpaste and mouth-rinse including mastic and IMPLA CARE. (unpublished data)
Figure 20.
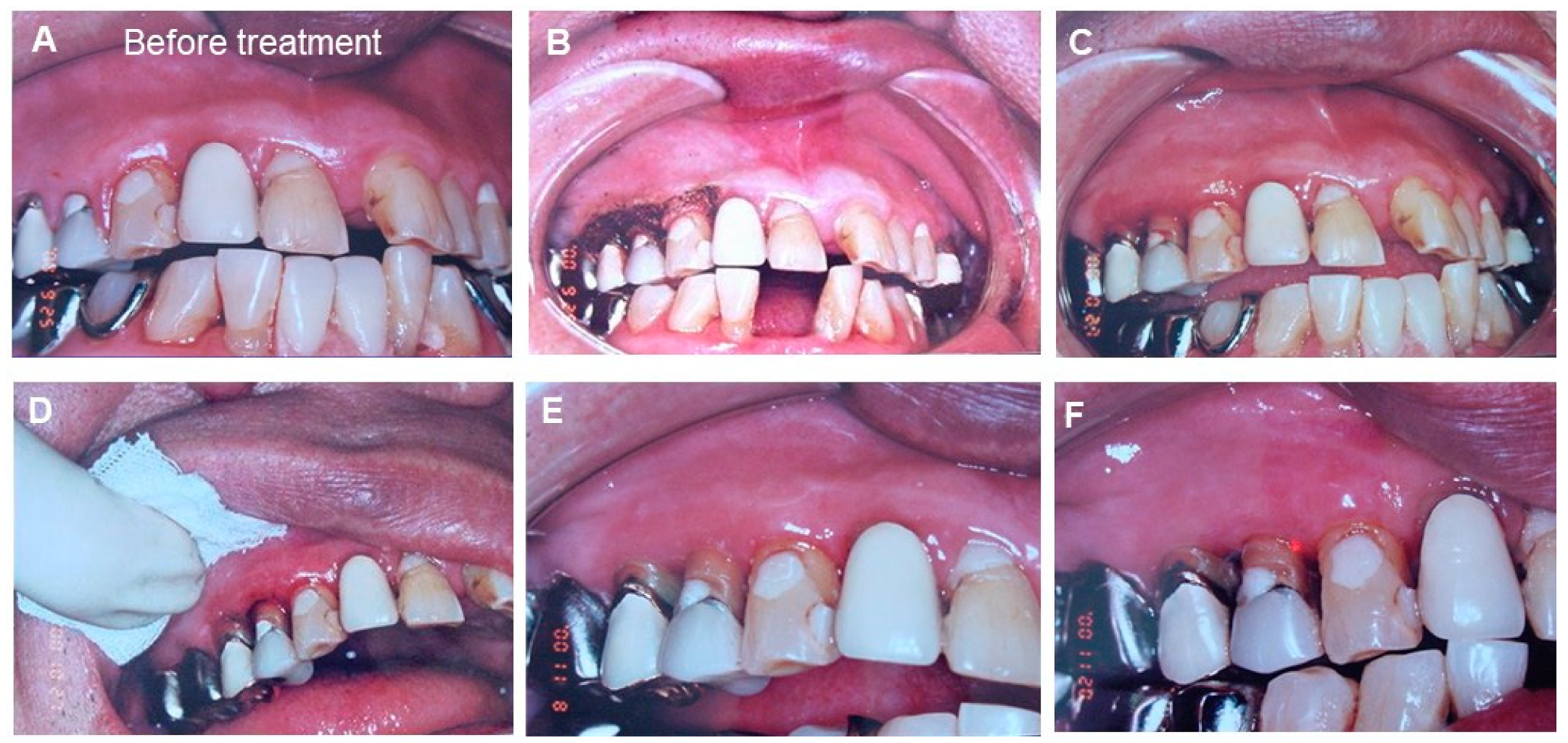
The clinical observation of periodontal tissue around the upper 4th and 5th teeth before and after treatment with laser and mastic gel. (A) Before treatment (at the first visited time); (B) First time after the laser treatment. Mastic gel was applied after carbonized laser treatment. (C) Second times after the laser treatment. After the laser treatment, chlorhexidine was used to prevent bacterial infection and mastic gel was applied at the gingiva. (D) Third times after the laser treatment. Mastic gel was applied after light coagulation layer was added by laser. (E) Fourth times after the laser treatment. Mastic gel was applied around the inflammatory gingival area. (F) Inflammatory gingival area between upper 4th and 5th are improved by using the mastic gel. Photos were taken, after obtaining the informed consent from the patient. (Watanabe S, unpublished data)
Figure 20.
The clinical observation of periodontal tissue around the upper 4th and 5th teeth before and after treatment with laser and mastic gel. (A) Before treatment (at the first visited time); (B) First time after the laser treatment. Mastic gel was applied after carbonized laser treatment. (C) Second times after the laser treatment. After the laser treatment, chlorhexidine was used to prevent bacterial infection and mastic gel was applied at the gingiva. (D) Third times after the laser treatment. Mastic gel was applied after light coagulation layer was added by laser. (E) Fourth times after the laser treatment. Mastic gel was applied around the inflammatory gingival area. (F) Inflammatory gingival area between upper 4th and 5th are improved by using the mastic gel. Photos were taken, after obtaining the informed consent from the patient. (Watanabe S, unpublished data)
Figure 21.
Effects of the IMPLA CARE. (Watanabe S, unpublished data)
Figure 21.
Effects of the IMPLA CARE. (Watanabe S, unpublished data)
Figure 22.
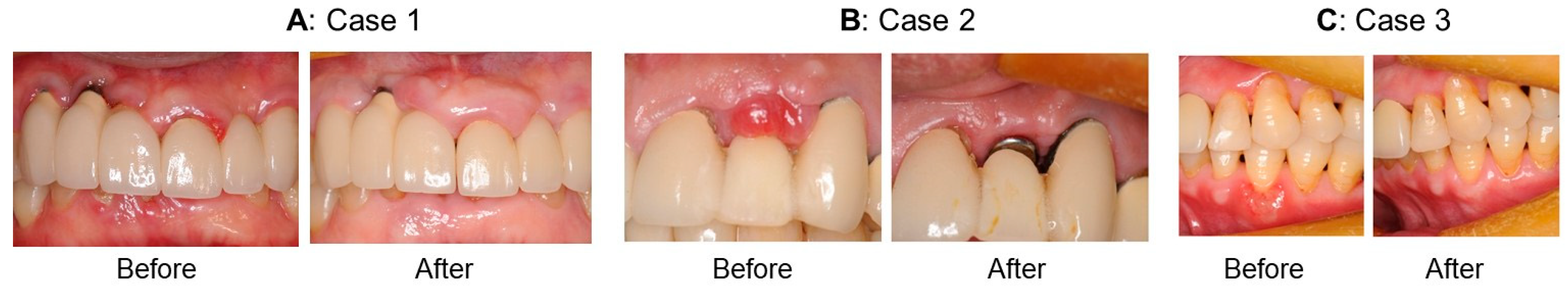
Case 1: A patient who was developing diabetes and hypertension (A), Case 2: A patient with peri-implantitis (B), Case3: A patient with an ulcer from sleep deprivation and work stress (C). (Suzuki M, unpublished data)
Figure 22.
Case 1: A patient who was developing diabetes and hypertension (A), Case 2: A patient with peri-implantitis (B), Case3: A patient with an ulcer from sleep deprivation and work stress (C). (Suzuki M, unpublished data)
Figure 23.
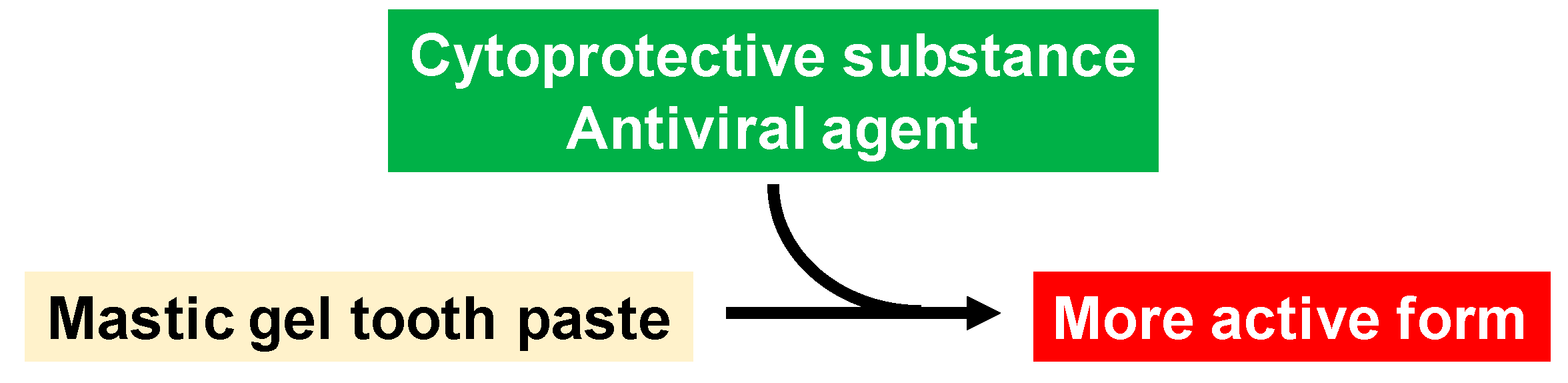
Manufacturing of advanced mastic gel tooth paste.
Figure 23.
Manufacturing of advanced mastic gel tooth paste.
Table 1.
Definitions and classifications of Yin-Yong, Kyo-Jitsu and Kan-Netsu.
Table 1.
Definitions and classifications of Yin-Yong, Kyo-Jitsu and Kan-Netsu.
| Categories | Yin-Yang | Kyo-Jitsu (Asthenia and Sthenia) | Kan-Netsu (Chills and Fever) |
|---|
| Definitions | Ability to resist the disease. The treatment differs, depending on whether the sho is yang and yin.
Yin disease: The resistant power against the disease is weak. Treatment is given to recover the exhaustion of the body. It is called honchi or the systemic meridian treatment | The state of deficiency is kyo-sho or asthenia and excess is jitsu-sho or sthenia.
Kyo (Asthenia): Deficiency of what is required for the body and shows the sho of Yin-kyo syndrome or yang-kyo syndrome | Actual feeling of chill and heat
Kyo-netsu (asthenic heat): Heat coming from poor metabolism and retained inside the body, slight fever, internal fever, showing yin-syndrome. |
Classification
(According to the Orthodox Theory) | Yang disease: The resistant power against the disease is strong. Treatment which positivity attacks the disease is effective. It is called hyochi or local and symptomatic treatment. | Jitsu (Sthenia): Low metabolic rate due to the accumulation of toxic substance in the body and shows the sho of yin-jitsu or yang-jitsu. | Jitsu-netsu (sthenic heat): Chills that occurs by increasing the heat in the body. Observes pyrexia and showing Yang-syndrome. |
Table 2.
Definitions of Yin-Kyo, Yo-Kyo, Yin-Jitsu and Yo-Jitsu.
Table 2.
Definitions of Yin-Kyo, Yo-Kyo, Yin-Jitsu and Yo-Jitsu.
| Categories | Yin-Kyo (yin deficiency) | Yo-Kyo (yang deficiency) | Yin-Jitsu (Yin excess) | Yo-Jitsu (Yang excess) |
|---|
| Definitions | Yin is insufficient and yan becomes relatively overactive; shows fever called asthenic fever; feverish symptom. | Yang is insufficient and yin relatively becomes overactive; asthenia cold; feeling chills. | Coldness comes from outside to constantly maintain the homeostasis of yin and yang and shows the state of chills, called Jitsu-Kan or sthenic cold; body is chilled and feeling cold. | Heat comes from outside to constantly maintain the homeostasis of yin and yang; and shows the state of heat, called Jitsu-Netsu or sthenic heat; feeling hot and excessive sw eating. |
Table 3.
Classifications of Ki, Ketsu and Sui.
Table 3.
Classifications of Ki, Ketsu and Sui.
Table 4.
The correlations between the colours and shapes in tongue.
Table 4.
The correlations between the colours and shapes in tongue.
| Colour Tone | Pale tongue: Paler colour than normal tongue; showing deficiency of Ki and Ketsu. Reddish tongue:Netsu-Sho (heat) symptom; redder than normal tongue colour and often shows dryness of mouth and lips. Purplish tongue: Systemic Oketsu due to stagnation of Ki and Ketsu; especially it is very likely when the dorsal lingual veins are over swelling. If the tongue is wet, it is Kan-Sho (cold) symptom and the body is chilled. If dry, it shows Netsu-Sho.
|
| Shape | Swelled tongue: Tongue is swollen and shows tooth marks on peripheral; showing Ki-Kyo and Sui-Tai (deficiency of Ki and fluid stagnation). Thin tongue: Tongue is dry and in deep purple colour; shows Sui-Kyo, Yin-Yo-Kyo (deficiency of Sui, Kyo of both Yin and Yang. Trembling tongue: When moving the tongue, it trembles; it vibrates; showing Netsu-Sho and Ki-Kyo (Ki deficiency).
|
Table 5.
The correlations between the colours and volumes in tongue.
Table 5.
The correlations between the colours and volumes in tongue.
| Colour Tone | White tongue coating: Pale white colour is considered normal but shows the changes in body condition, depending on the wetness Yellow tongue coating: Shows stomach/intestine function deficiency; fever; lack of water due to fever Greyish black tongue coating: Yellow tongue coating symptom progressed and disease worsened; related to infectious disease, high fever, dehydration
|
| Volume | Thin tongue coating: Normal No tongue coating: Abnormal; chronical disease; protracted illness Thick tongue coating: Abnormal; exacerbation of disease, growth of bacteria due to defective metabolism of tongue coating
|
Table 6.
Effects of Jixueteng on osteoclast formation in periodontal tissues.
Table 6.
Effects of Jixueteng on osteoclast formation in periodontal tissues.
| Groups | Number of Osteoclasts |
|---|
| 2W | 4W | 6W |
|---|
| Control | 14.25 ± 1.71 | 16.00 ± 1.00 | 10.33 ± 0.58 |
| P. gingivalis | 18.50 ± 5.45 | 29.00 ± 8.25 ** | 23.33 ±1.53 ** |
| Jixueteng + P. gingivalis | 15.75 ± 7.41 | 17.00 ± 2.94 | 12.33 ± 3.21 |
Table 7.
Minimum inhibitory concentration (MIC) of mastic resin oil. (Hamada N, unpublished data).
Table 7.
Minimum inhibitory concentration (MIC) of mastic resin oil. (Hamada N, unpublished data).
| Oral Bacteria | MIC (%) |
|---|
| Streptococcus mutans | 0.4 |
| Streptococcus sanguinis | 0.4 |
| Streptococcus mitis | 0.4 |
| Lactobacillus species | 0.2 |
| Staphylococcus aureus | 0.8 |
| Bacillus species | 0.2 |
| Actinomyces species | 0.2 |
| Porphyromonas gingivalis | < 0.05 |
| Porphyromonas endodontalis | 1.6 |
| Prevotella intermedia | 1.6 |
| Fusobacterium nucleatum | < 0.05 |
| Aggregatibacter actinomycetemcomitans | 0.2 |
Table 8.
Plaque formation on the tooth surface and effect of inhibition of gingivitis of mastic gums. (Hamada N, unpublished data).
Table 8.
Plaque formation on the tooth surface and effect of inhibition of gingivitis of mastic gums. (Hamada N, unpublished data).
| Group | Plaque Index | Gingivitis Index |
|---|
| Baseline | 1 week | Baseline | 1 week |
|---|
| Mastic gum (n = 10) | 1.06 ± 0.29 | 2.69 ± 0.29 ** | 0 | 0.44 ± 0.15* |
| Placebo gum (n = 10) | 1.19 ± 0.19 | 3.15 ± 0.24 ** | 0 | 0.66 ± 0.23* |
Table 9.
Minimum inhibitory concentration (MIC) of five natural products. (Hamada N, unpublished data).
Table 9.
Minimum inhibitory concentration (MIC) of five natural products. (Hamada N, unpublished data).
| Tested bacteria | Jixueteng | Sasa Veitchii | Grapefruit | Propolis | Lotus |
|---|
| Streptococcus mutans | 4 | > 8192 | 512 | 256 | 8192 |
| Streptococcus gordonii | 8 | 4 | 2048 | 8192 | > 8192 |
| Lactobacillus casei | 4 | > 8192 | 512 | 256 | 8192 |
| Staphylococcus aureus | 32 | > 8192 | 4096 | > 8192 | > 8192 |
| Actinomyces viscosus | 32 | 4 | 4096 | 256 | 8192 |
| Porphyromonas gingivalis | > 8192 | 512 | 4096 | > 8192 | > 8192 |
| Prevotella nigresecens | > 8192 | 128 | > 8192 | > 8192 | > 8192 |
| Fusobacterium nucleatum | 16 | 8 | 4096 | 2048 | > 8192 |
| Escherichia coli | > 8192 | > 8192 | 1024 | 16 | 8192 |
| Candida albicans | 64 | 8 | 8192 | 2048 | > 8192 |
Table 10.
Scores showing the progress of periodontal disease.
Table 10.
Scores showing the progress of periodontal disease.
| Examination Criteria |
|---|
| Score | Swollen Pus | Redness | Bleeding | Pus Discharge | Gingival Colour | Mobility | Patient’s Opinion |
|---|
| 5 | Papilla and adhering to gingiva | Extending to the papilla and gingival gums | Naturally bleeding | Naturally draining | Dark red purple | Upper and lower lip and tongue immobile | No change |
| 3 | Papilla and extending to the gingival margin | Papilla and tooth inflammation | Bleeding by acupressure | Acupressure-induced draining | Dark red | Strongly immobile | Improved a little |
| 1 | Part of the papilla | Part of the papilla | Slight bleeding with acupressure | Slight draining with acupressure | Brilliant | Slightly immobile | Tightened |
| 0 | None at all | No redness | None at all | No discharge at all | Light pink | Within a physiological range | Improved a lot |
Table 11.
Improvement of periodontal disease after administration of the IMPLA CARE. (Watanabe S, unpublished data).
Table 11.
Improvement of periodontal disease after administration of the IMPLA CARE. (Watanabe S, unpublished data).
| Examination Items | Scores at 0, 1, 2 or 3 Months Later |
|---|
| Patient A | Patient B | Patient C | Patient D | Patient E | Patient F |
|---|
| 0 | 1 | 2 | 3 | 0 | 1 | 2 | 3 | 0 | 1 | 2 | 3 | 0 | 1 | 2 | 3 | 0 | 1 | 2 | 3 | 0 | 1 | 2 | 3 |
|---|
| Swollen pus | 1 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 3 | 2 | 1 | 0 | 3 | 0 | 0 | 0 | 5 | 3 | 0 | 0 | 1 | 1 | 0 | 0 |
| Redness | 5 | 3 | 1 | 0 | 3 | 2 | 1 | 0 | 3 | 2 | 1 | 0 | 3 | 0 | 0 | 0 | 3 | 1 | 0 | 0 | 3 | 1 | 1 | 0 |
| Bleeding | 5 | 3 | 1 | 0 | 3 | 2 | 1 | 0 | 2 | 1 | 1 | 0 | 2 | 0 | 0 | 0 | 3 | 0 | 0 | 0 | 1 | 0 | 0 | 0 |
| Pus discharge | 1 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 3 | 2 | 1 | 0 | 3 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 1 | 0 | 0 | 0 |
| Gingival colour | 3 | 1 | 0 | 0 | 3 | 2 | 1 | 0 | 2 | 1 | 1 | 0 | 2 | 3 | 0 | 0 | 3 | 1 | 0 | 0 | 3 | 1 | 1 | 0 |
| Mobility | 3 | 1 | 0 | 0 | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 1 | 1 | 1 | 0 |
| Patient’s opinion | | 3 | 1 | 0 | | 3 | 1 | 0 | | 1 | 0 | 0 | | 0 | 0 | 0 | | 1 | 0 | 0 | | 1 | 0 | 0 |
| Total score | 18 | 11 | 3 | 0 | 12 | 9 | 4 | 0 | 13 | 9 | 5 | 0 | 14 | 3 | 0 | 0 | 16 | 6 | 0 | 0 | 10 | 5 | 3 | 0 |