Extracts from Annona Muricata L. and Annona Reticulata L. (Annonaceae) Potently and Selectively Inhibit Plasmodium Falciparum
Abstract
:1. Introduction
2. Experimental Section
2.1. Plant Collection and Authentication
2.2. Preparation of Extracts and Fractionation
2.3. Evaluation of Biological Activities
2.3.1. Erythrocyte Susceptibility to Plant Extracts
2.3.2. Human Foreskin Fibroblast (HFF) Susceptibility to Plant Extracts
2.3.3. Antiplasmodial Activity
3. Results and Discussion
3.1. Plant Extraction and Fractionation
| Plant Species | Organ | Nature of Extract | Code | a Yield (%) | b IC50 (µg/mL) ± S.D. | c SI |
|---|---|---|---|---|---|---|
| Annona muricata | Pericarp | Crude ethanol extract | AMpEthOH | 5.68 | 1.01 ± 0.07 | ˃9.90 |
| H2O fraction | AMpH2O | 1.02 | >10 | ND | ||
| CH2Cl2 fraction | AMpCH2Cl2 | 3.54 | 0.94 ± 0.03 | ˃10.63 | ||
| Root | Crude ethanolic extract | AMrEthOH | 6.23 | 0.79 ± 0.14 | ˃12.65 | |
| H2O fraction | AMrH2O | 0.98 | >10 | ND | ||
| CH2Cl2 fraction | AMrCH2Cl2 | 4.18 | 0.19 ± 0.03 | ˃52.63 | ||
| Subfractions | AMrSF1 | 0.56 | 0.61 ± 0.04 | ˃16.39 | ||
| AMr SF2 | 0.33 | 0.22 ± 0.06 | ˃45.45 | |||
| AMrSF3 | 1.07 | 0.09 ± 0.003 | ˃111.11 | |||
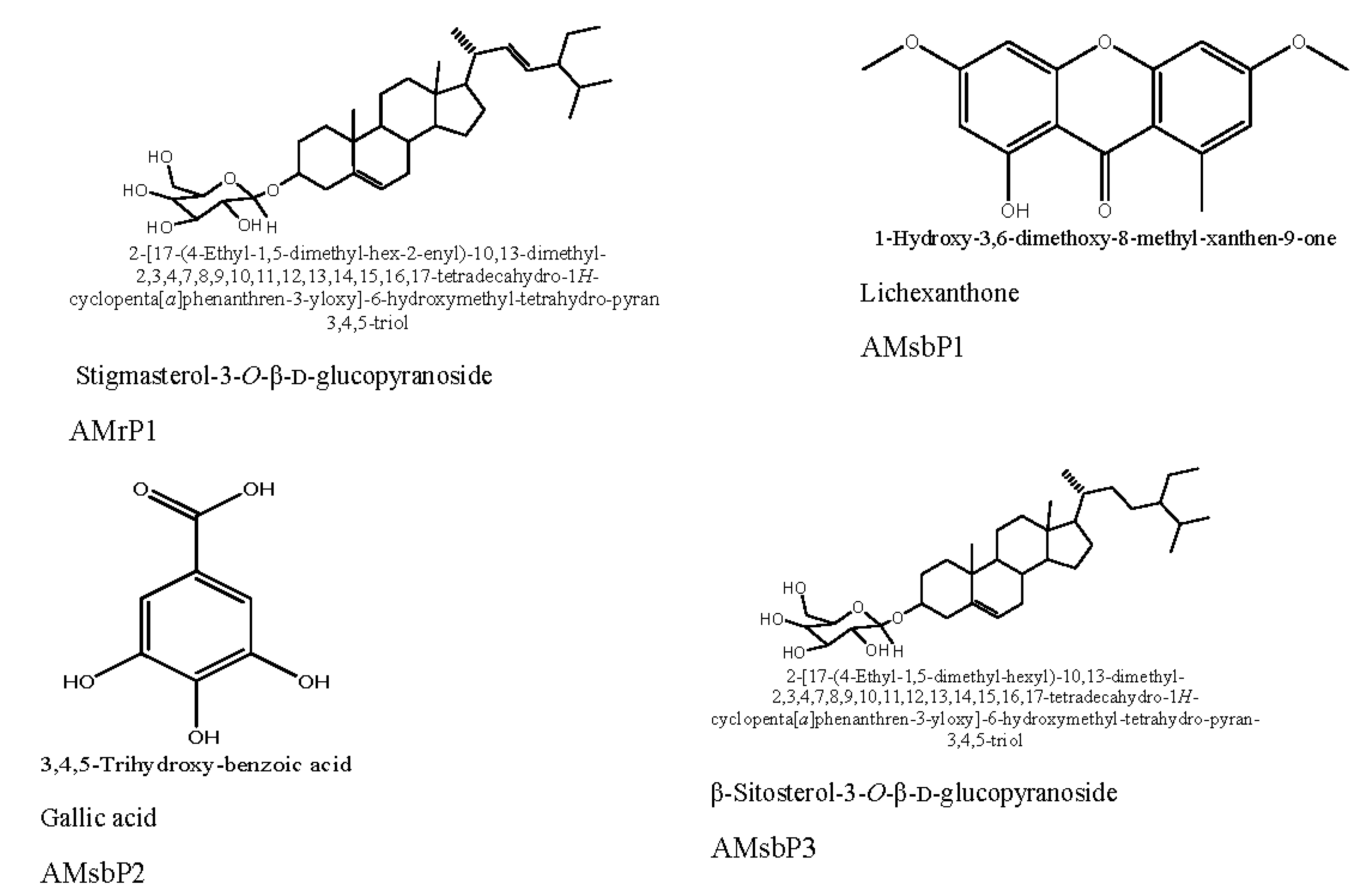
| Purified compound | Stigmasterol-3-O-β-d-glucopyranoside (AMrP1) | 0.016 | ˃10 | ND | ||
| Stem bark | Crude ethanolic extract | AMsb-EthOH | 5.91 | 1.45 ± 0.20 | ˃6.45 | |
| H2O fraction | AMsbH2O | 0.87 | >10 | ND | ||
| CH2Cl2 fraction | AMsbCH2Cl2 | 4.32 | 1.50 ± 0.07 | ˃6.66 | ||
| Subfractions | AMsbSF2 | 0.11 | 1.65 ± 1.58 | ˃6.06 | ||
| AMsbSF15 | 0.08 | 2.52 ± 1.41 | ˃3.96 | |||
| AMsbSF16 | 0.16 | 3.46 ± 0.98 | ˃2.89 | |||
| AMsbSF17 | 0.04 | 2.45 ± 1.77 | ˃3.92 | |||
| AMsbSF18 | 0.02 | 2.75 ± 1.86 | ˃3.63 | |||
| AMsbSF19 | 0.73 | 2.89 ± 0.55 | ˃3.46 | |||
| AMsbSF20 | 0.03 | 1.14 ± 0.22 | ˃8.77 | |||
| AMsbSF21 | 0.03 | 1.11 ± 0.34 | ˃9.00 | |||
| AMsbSF22 | 0.02 | 0.12 ± 0.03 | ˃83.3 | |||
| AMsbSF24 | 0.41 | 0.46 ± 0.04 | ˃21.7 | |||
| AMsbSF27 | 0.02 | 1.17 ± 0.16 | ˃8.54 | |||
| AMsbSF28 | 0.62 | 0.72 ± 0.07 | ˃13.88 | |||
| AMsbSF29 | 0.07 | 0.75 ± 0.13 | ˃13.33 | |||
| AMsbSF30 | 0.31 | 0.07 ± 0.009 | ˃142.3 | |||
| AMsbSF31 | 0.19 | 0.28 ± 0.05 | ˃35.7 | |||
| AMsbSF32 | 0.017 | 0.78 ± 0.43 | ˃12.8 | |||
| AMsbSF33 | 0.05 | 1.31 ± 0.19 | ˃7.63 | |||
| AMsbSF34 | 0.09 | 1.07 ± 0.36 | ˃9.34 | |||
| AMsbSF35 | 0.019 | 2.19 ± 0.47 | ˃4.56 | |||
| AMsbSF36 | 0.22 | 1.39 ± 0.33 | ˃7.19 | |||
| Purified compounds | Lichexanthone (AMsbP1) | 0.014 | ˃10 | ND | ||
| Gallic acid (AMsbP2) | 0.052 | 3.32 ± 1.49 | ˃3.01 | |||
| β-Sitosterol-3-O-β-D-glucopyranoside (AMsbP3) | 0.012 | ˃10 | ND | |||
| Annona reticulata | Leaf | Crude ethanolic extract | ARlEthOH | 10.46 | ˃ 10 | ND |
| H2O fraction | ARlH2O | 1.71 | >10 | ND | ||
| CH2Cl2 fractions | ARlCH2Cl2 | 9.93 | ˃ 10 | ND | ||
| Twig | Crude ethanolic extract | ARtwEthOH | 4.96 | ˃ 10 | ND | |
| H2O fraction | ARtwH2O | 0.53 | >10 | ND | ||
| CH2Cl2 fraction | ARtwCH2Cl2 | 1.78 | 0.88 ± 0.34 | ˃11.4 | ||
| Stem bark | Crude ethanolic extract | ARsbEthOH | 6.02 | 0.29 ± 0.02 | ˃34.5 | |
| H2O fraction | ARsbH2O | 1.04 | >10 | ND | ||
| CH2Cl2 fraction | ARsbCH2Cl2 | 3.71 | 0.82 ± 0.25 | ˃12.2 | ||
| Root | Crude ethanolic extract | ARrEthOH | 5.12 | 1.90 ± 0.008 | ˃5.26 | |
| H2O fraction | ARrH2O | 0.71 | >10 | ND | ||
| CH2Cl2 fraction | ARrCH2Cl2 | 4.54 | 0.38 ± 0.23 | ˃26.3 | ||
| Fruit | Crude ethanolic extract | ARfrEthOH | 5.14 | 0.67 ± 0.02 | ˃14.9 | |
| H2O fraction | ARfrH2O | 0.48 | >10 | ND | ||
| CH2Cl2 fraction | ARfrCH2Cl2 | 2.12 | 0.42 ± 0.009 | ˃23.8 | ||
| Positive control | Artemisinin | 0.005 ± 0.0008 | ND |
3.2. Susceptibility of Erythrocytes, HFF Cells, and P. Falciparum to Plant Extracts
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organization. Malaria Report; WHO: Geneva, Switzerland, 2014. [Google Scholar]
- World Health Organization. World Health Organization Treatment Recommendation; WHO: Geneva, Switzerland, 2010. [Google Scholar]
- Dondorp, A.M.; Nostern, F.; Yi, P.; Das, D.; Phyo, A.P.; Tarning, J.; Lwin, K.M.; Ariey, F.; Hanpithakpong, W.; Lee, S.J.; et al. Artemisinin-Resistant Plasmodium falciparum Malaria. N. Engl. J. Med. 2009, 361, 455–467. [Google Scholar] [CrossRef] [PubMed]
- Meshnick, S.R.; Taylor, T.E.; Kamchonwongpaisan, S. Artemisinin and the antimalarial endoperoxides: from herbal remedy to targeted chemotherapy. Microbiol. Rev. 1996, 60, 301–315. [Google Scholar] [PubMed]
- Tsabang, N.; Tsouh, F.P.V.; Yamthe, T.L.R.; Noguem, B.; Bakarnga-Via, I.; Dongmo, N.M.S.; Boyom, F.F. Ethnopharmacological survey of Annonaceae medicinal plants used to treat malaria in four areas of Cameroon. J. Ethnopharmacol. 2012, 139, 171–180. [Google Scholar] [CrossRef] [PubMed]
- Pinto, A.C.; Andrade, S.R.; Ferreira, F.R.; Kinpara, D.I. Annona species. In International Center for under Utilised Crops; University of Southampton: Southampton, UK, 2005; pp. 1–281. [Google Scholar]
- Boyom, F.F.; Tsouh, F.P.V.; Tchokouaha, Y.L.R.; Ngoutane, M.A.; Madiesse, K.A.E.; Mbacham, F.W.; Tsamo, E.; Amvam, Z.P.H.; Jiri, G.; Rosenthal, P.J. Potent antiplasmodial extracts from Cameroonian Annonaceae. J. Ethnopharmacol. 2011, 134, 717–724. [Google Scholar] [CrossRef] [PubMed]
- Bidla, G.; Titanji, V.P.K.; Joko, B.; Ghazali, G.E.; Bolad, A.; Berzins, K. Antiplasmodial activity of seven plants used in african folk medicine. Indian J. Pharmacol. 2004, 36, 245–246. [Google Scholar]
- Razak, M.A.; Adlin, A.; Rosnani, A.N.; Mohd, I.W.; Siti, H.S.; Noor, R.A.; Zakiah, I. Effect of selected local medicinal plants on the asexual blood stage of chloroquine resistant Plasmodium falciparum. BMC Comp. Altern. Med. 2014, 14, 492. [Google Scholar]
- Menan, H.; Banzouzi, J.T.; Hocquette, A.; Pelissier, Y.Y.; Blache, Y.; Kone, M.; Mallie, M.; Ake, A.L.; Valentin, A. Antiplasmodial activity and cytotoxicity of plants used in West African traditional medicine for the treatment of malaria. J. Ethnopharmacol. 2006, 105, 131–136. [Google Scholar] [CrossRef] [PubMed]
- Chavan, S.S.; Shamkuwar, P.B.; Damale, M.G.; Pawar, D.P. A comprehensive review on Annona reticulata. Int. J. Pharm. Sc. Res. 2014, 5, 45–50. [Google Scholar]
- Alali, F.Q.; Liu, X.X.; McLaughlin, J.L. Annonaceous acetogenins: Recent progress. J. Nat. Prod. 1999, 62, 504–540. [Google Scholar] [CrossRef] [PubMed]
- Cedillo-Rivera, R.; Ramfrez, A.; Munoz, O. A rapid colorimetric assay with the Tetrazolium salt MTT and Phenazine Methosulfate (PMS) for viability of Entamoeba histolytica. Arch. Med. Res. 1992, 23, 59–61. [Google Scholar] [PubMed]
- Boyom, F.F.; Madiesse, K.E.; Tepongning, R.; Ngouana, V.; Mbacham, W.F.; Tsamo, E.; Amvam Zollo, P.H.; Gut, J.; Rosenthal, P.J. Antiplasmodial activity of extracts from seven medicinal plants used in malaria treatment in Cameroon. J. Ethnopharmacol. 2009, 123, 483–488. [Google Scholar] [CrossRef] [PubMed]
- Boyom, F.F.; Tsouh, F.P.V.; Tchokouaha, Y.L.R.; Spangenberg, T.; Mfopa, N.A.; Kouipou, T.R.M.; Mbouna, J.C.; Donkeng, D.F.V.; Zollo, A.P.H. Repurposing the open access malaria box to discovery potent inhibitors of Toxoplasma gondii and Entamoeba histolytica. Antimicrob. Agents Chemother. 2014, 58, 5848. [Google Scholar] [CrossRef] [PubMed]
- Lambros, C.; Vanderberg, J.P. Synchronization of Plasmodium falciparum erythrocytic stages in culture. J. Parasitol. 1979, 65, 418–420. [Google Scholar] [CrossRef] [PubMed]
- Singh, A.; Rosenthal, P.J. Comparison of efficacies of cysteine protease inhibitors against five strains of Plasmodium falciparum. Antimicrob. Agents Chemother. 2001, 45, 949–951. [Google Scholar] [CrossRef] [PubMed]
- Wright, H.E.; Burton, W., Jr.; Berry, R.C. Identification of stigmasteryl d-glucoiside in aged burley tobacco. J. Org. Chem. 1962, 27, 918–920. [Google Scholar] [CrossRef]
- Mba’ning, B.M. Etude Phytochimique et Pharmacologique de SalaciacamerunensisLoes., Salaciadimidia Hall. (Celastraceae) et Crinumnatans Baker (Amaryllidaceae). Ph.D. Thesis, University of Yaoundé I, Yaoundé, Cameroon, 2012. [Google Scholar]
- Ruben, F.G.; Keith, S.B. Alkaloids of three Aspidosperma species. Phytochemistry 1976, 15, 1093–1095. [Google Scholar] [CrossRef]
- Buitrago, D.A.; Rojas, V.J.; Cote, V.; Bruno-Colmenárez, J.; de Delgado, G.D. NMR elucidation and crystal structure analysis of 1-hydroxy-3,6-dimethoxy-8-methyl-9h-xanthen-9-one (lichexanthone) isolated from Vismia baccifera (Guttiferae). Bol. Lat. Am. Caribe Plantas Med. Aromát. 2010, 9, 470–474. [Google Scholar]
- Eldahshan, O.A. Isolation and structure elucidation of phenolic compounds of Carob leaves grown in Egypt. Curr. Res. J. Biol. Sci. 2010, 3, 52–55. [Google Scholar]
- Zhang, H.M.; Wang, C.F.; Shen, S.M.; Wang, G.L.; Liu, Z.M.; Wang, Y.Y.; Du, S.S.; Liu, Z.L.; Liu, P.; Deng, Z.W. Antioxidant phenolic compounds from Pu-erh tea. Molecules 2012, 17, 14037–14045. [Google Scholar] [CrossRef] [PubMed]
- Ramiarantsoa, H.; Koffi, B.A.; Kouamé, M.A.; Djakouré, L.A. Le O-β-d-glucoside du β-sitostérol Isolé des feuilles de Ravenala madagascariensis. J. Soc. Ouest-Afr. Chim. 2008, 026, 99–103. [Google Scholar]
- Faizi, S.; Khan, R.A.; Azher, S.; Khan, S.A.; Tauseef, S.; Ahmad, A. New antimicrobial alkaloids from the roots of Polyalthia longifolia var pendula. Planta Medica 2003, 69, 350–355. [Google Scholar] [CrossRef] [PubMed]
- Arriaga, A.M.; Feitosa, E.M.; Lemos, T.L.; Santiago, G.M.; Lima, J.Q.; de Oliveira, M.C.; Vasconcelos, J.N.; Rodrigues, F.E.; Gomes, T.B.; Braz-Filho, R. Chemical constituents and insecticidal activity of Rollina leptopetala. Nat. Prod. Commun. 2008, 3, 1565–1688. [Google Scholar]
- Costa, E.V.; Assis, M.F.; Lucia, B.M.P.; Broga, R.M.; Delarmelina, C.; Duarte, T.C.M.; Ruiz, T.G.L.A.; Carvalho, J.E.; Maia, B.H. Chemical constituents isolated from the bark of Guatteria blepharophylla (Annonaceae) and their antiproliferative and antimicrobial activities. J. Braz. Chem. Soc. 2011, 22, S1–S15. [Google Scholar] [CrossRef]
- Sampath, M. Isolation and identification of gallic acid from Polyalthia longifolia (Sonn.) Thawaites. Int. J. Pharm. Biol. Sci. 2013, 4, 966–972. [Google Scholar]
- Dinesh, K.Y.; Neetu, S.; Shaima, R.; Mahendra, S.; Gautam, P.; Rakesh, M. Anti-ulcer constituents of Annona squamosa twigs. Fitoterapia 2011, 82, 666–675. [Google Scholar] [CrossRef] [PubMed]
- Nwaka, S.; Ramirez, B.; Reto, B.; Maes, L.; Douglas, F.; Ridley, R. Advancing drug innovation for negleted diseases. Critera for lead progression. PLoS Negl. Trop. Dis. 2009, 3, e440. [Google Scholar] [CrossRef] [PubMed]
- Weniger, B.; Robledo, S.; Arango, G.J.; Deharo, E.; Aragon, R.; Munoz, V.; Callapa, J.; Lobstein, A.; Anton, R. Antiprotozoal activities of Colombian plants. J. Ethnopharmacol. 2001, 78, 193–200. [Google Scholar] [CrossRef] [PubMed]
- Graziose, R.; Rathinasabapathy, T.; Lategan, C.; Poulev, A.; Smith, P.J.; Grace, M.; Lila, M.A.; Raskin, I. Antiplasmodial activity of aporphine alkaloids and sesquiterpene lactones from Liriodendron tulipifera L. J. Ethnopharmacol. 2011, 133, 26–30. [Google Scholar] [CrossRef] [PubMed]
- Ndjonka, D.; Bärbel, B.; Agyare, C.; Zimbres, F.M.; Lüersen, K.; Hensel, A.; Carsten, W.; Liebau, E. In vitro activity of extracts and isolated polyphenols from West African medicinal plants against Plasmodium falciparum. Parasitol. Res. 2012, 111, 827–834. [Google Scholar] [CrossRef] [PubMed]
- Zofou, D.; Tematio, E.L.; Ntie-Kang, F.; Tene, M.; Ngemenya, M.N.; Tane, P.; Titanji, V.P.K. New Antimalarial Hits from Dacryodes edulis (Burseraceae)—Part I: Isolation, In Vitro Activity, In Silico “drug-likeness” and Pharmacokinetic Profiles. PLoS One 2013, 8, e79544. [Google Scholar] [CrossRef] [PubMed]
- De Lima, J.P.S.; Pinheiro, M.L.B.; Santos, A.M.G.; Pereira, J.L.S.; Santos, D.M.F.; Barison, A.; Silva-Jardim, I.; Costa, E.V. In Vitro Atileishmanial and Cytotoxic Activities of Annona mucosa (Annonaceae). Rev. Virtual Quim. 2012, 4, 692–702. [Google Scholar]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yamthe, L.R.T.; Fokou, P.V.T.; Mbouna, C.D.J.; Keumoe, R.; Ndjakou, B.L.; Djouonzo, P.T.; Mfopa, A.N.; Legac, J.; Tsabang, N.; Gut, J.; et al. Extracts from Annona Muricata L. and Annona Reticulata L. (Annonaceae) Potently and Selectively Inhibit Plasmodium Falciparum. Medicines 2015, 2, 55-66. https://doi.org/10.3390/medicines2020055
Yamthe LRT, Fokou PVT, Mbouna CDJ, Keumoe R, Ndjakou BL, Djouonzo PT, Mfopa AN, Legac J, Tsabang N, Gut J, et al. Extracts from Annona Muricata L. and Annona Reticulata L. (Annonaceae) Potently and Selectively Inhibit Plasmodium Falciparum. Medicines. 2015; 2(2):55-66. https://doi.org/10.3390/medicines2020055
Chicago/Turabian StyleYamthe, Lauve Rachel Tchokouaha, Patrick Valere Tsouh Fokou, Cedric Derick Jiatsa Mbouna, Rodrigue Keumoe, Bruno Lenta Ndjakou, Paul Toukam Djouonzo, Alvine Ngoutane Mfopa, Jennifer Legac, Nole Tsabang, Jiri Gut, and et al. 2015. "Extracts from Annona Muricata L. and Annona Reticulata L. (Annonaceae) Potently and Selectively Inhibit Plasmodium Falciparum" Medicines 2, no. 2: 55-66. https://doi.org/10.3390/medicines2020055
APA StyleYamthe, L. R. T., Fokou, P. V. T., Mbouna, C. D. J., Keumoe, R., Ndjakou, B. L., Djouonzo, P. T., Mfopa, A. N., Legac, J., Tsabang, N., Gut, J., Rosenthal, P. J., & Boyom, F. F. (2015). Extracts from Annona Muricata L. and Annona Reticulata L. (Annonaceae) Potently and Selectively Inhibit Plasmodium Falciparum. Medicines, 2(2), 55-66. https://doi.org/10.3390/medicines2020055