Conversion of Cannabidiol (CBD) into Psychotropic Cannabinoids Including Tetrahydrocannabinol (THC): A Controversy in the Scientific Literature
Abstract
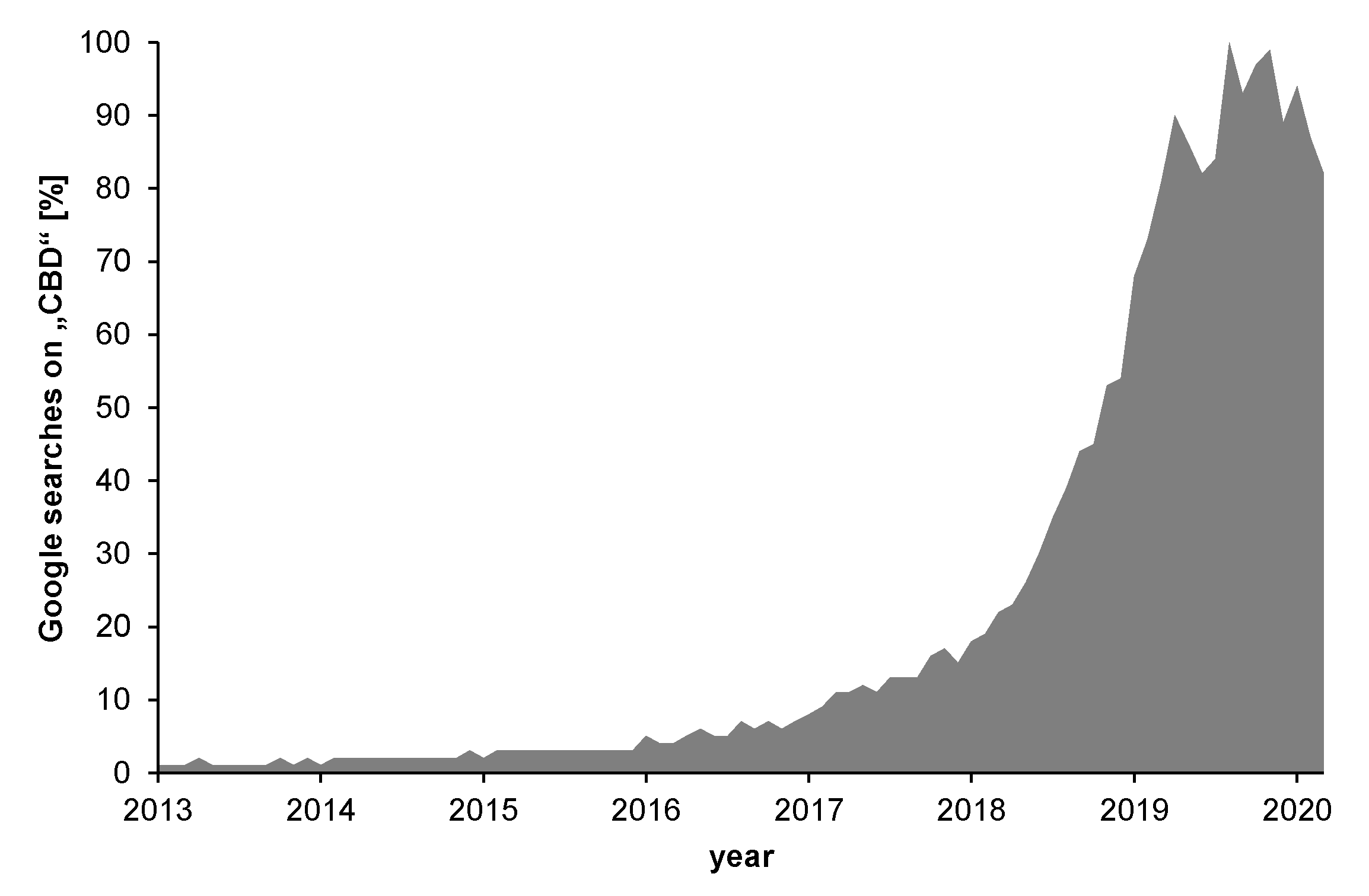
1. Introduction
2. Materials and Methods
3. Results and Discussion
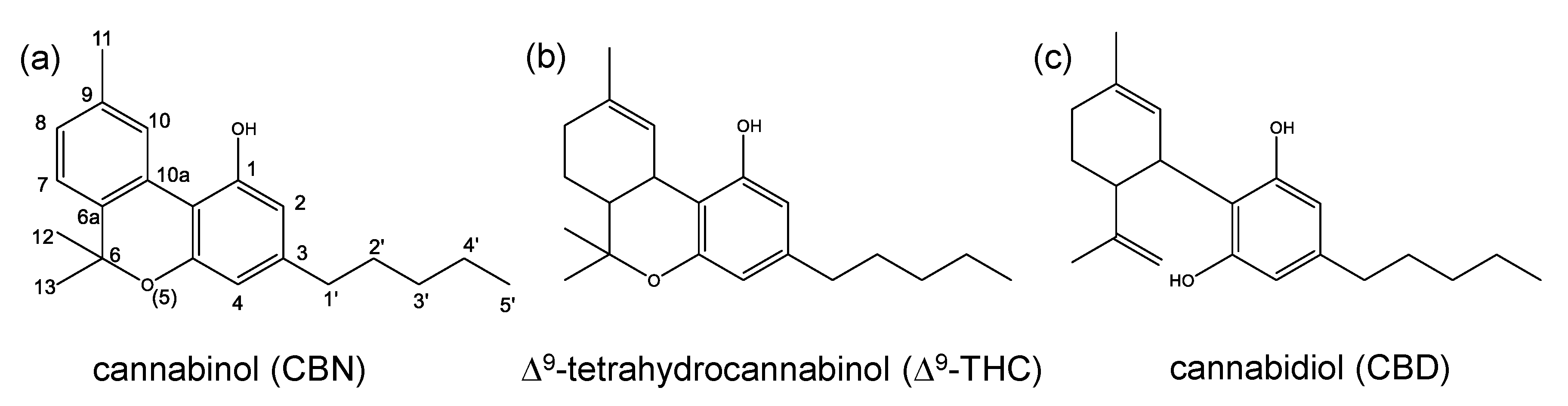
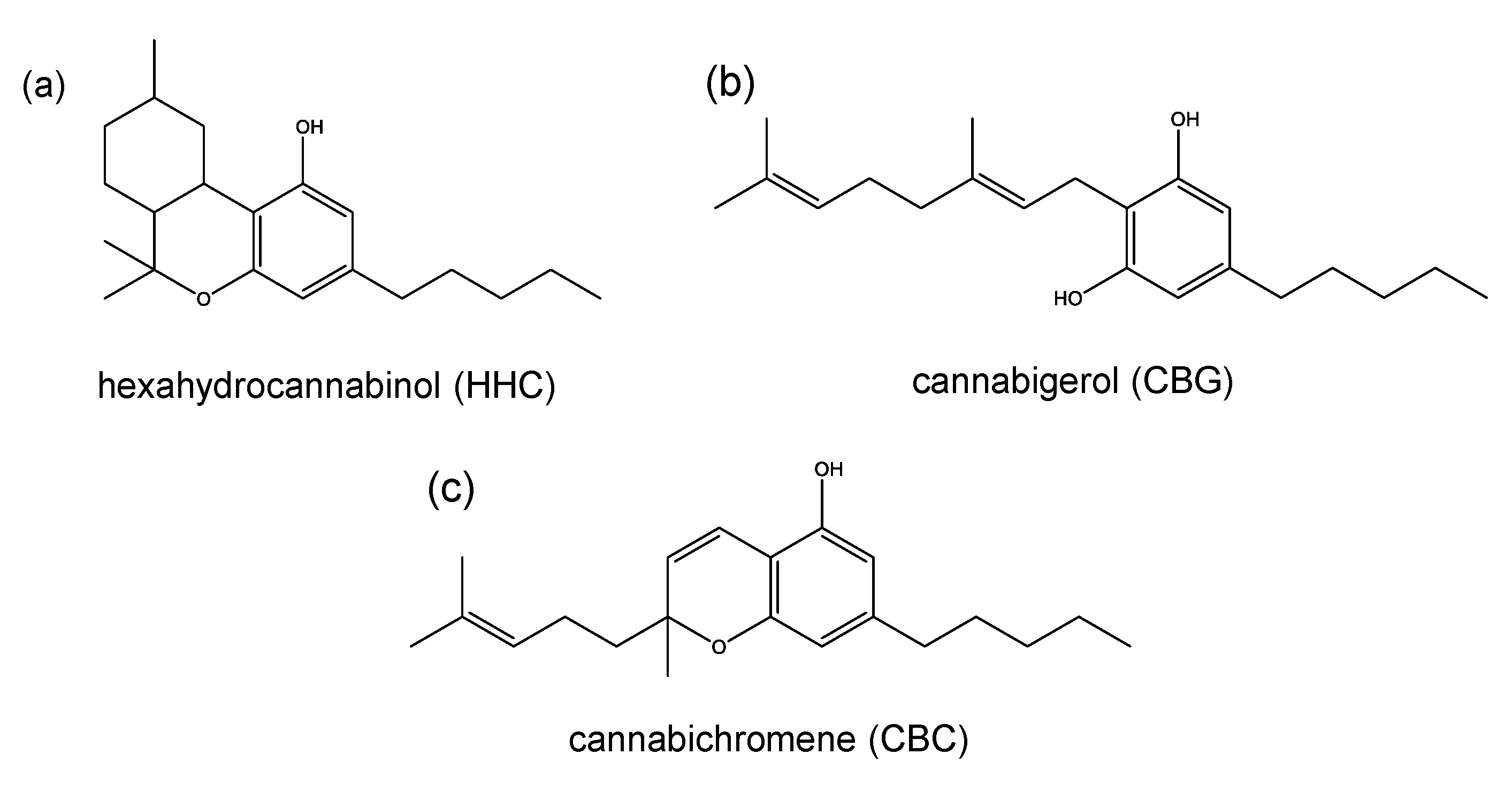
3.1. Psychotropicity of Cannabinoids
3.2. Conversion of Cannabidiol
3.2.1. Analytical Challenges in Detecting CBD, Its Degradation Products and Other Cannabinoids
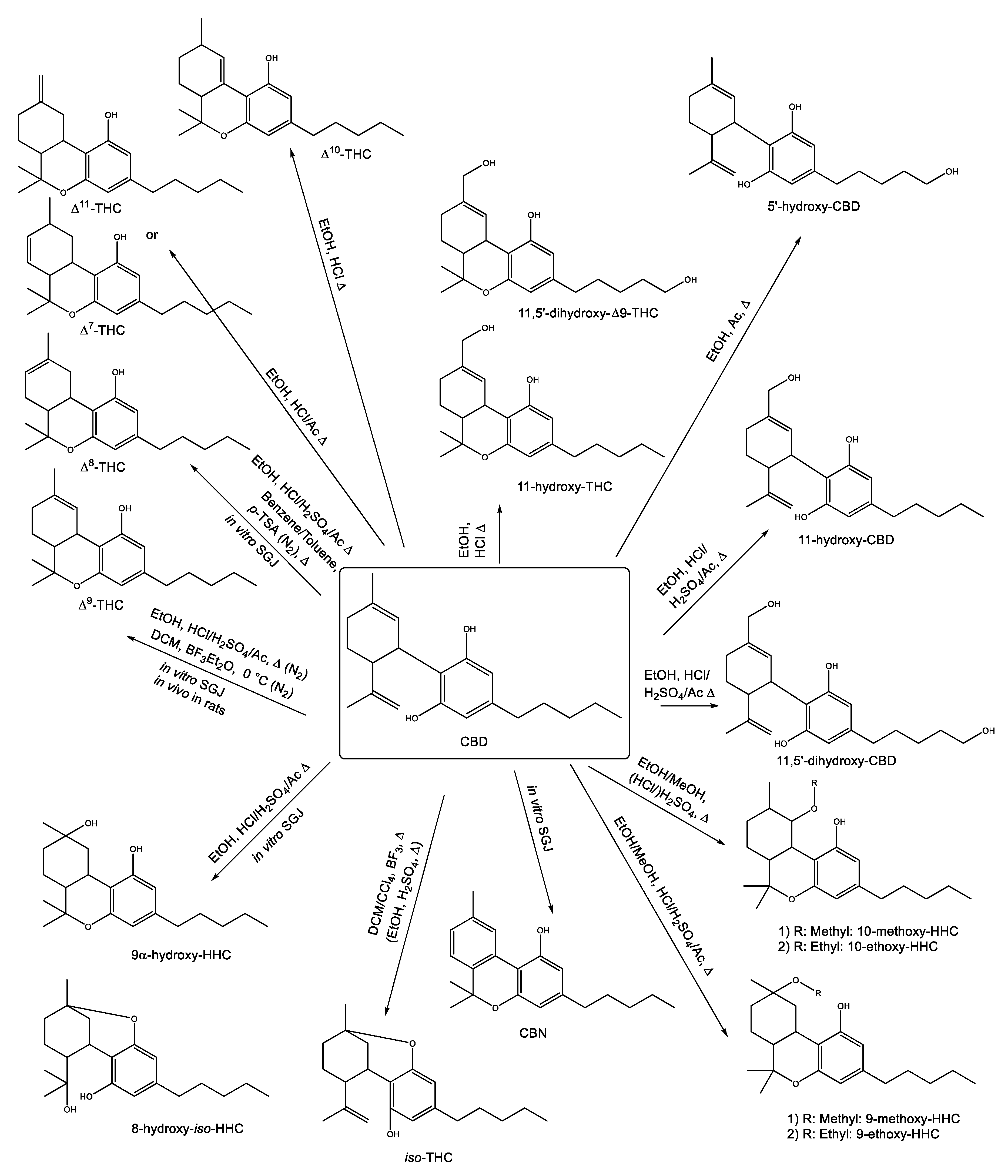
3.2.2. Conversion of CBD under Acidic Conditions
3.2.3. In Vitro Studies: Conversion of CBD in Artificial Gastric Juice and Other Model Systems
3.2.4. In Vivo Studies: Conversion of CBD in Animals and Humans
3.2.5. Conversion of CBD during the Storage of CBD Products
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| 5′-hydroxy-CBD | 5′-hydroxy-cannabidiol |
| CBD-ME | cannabidiol monomethyl ether |
| CBDA | cannabidiolic acid |
| CBG | cannabigerol |
| 5-acetyl-4-hydroxy-CBG | 5-acetyl-4-hydroxy-cannabigerol |
| CBN | cannabinol |
| 11-hydroxy-CBN | 11-hydroxy-cannabinol |
| TMCS | chlorotrimethylsilane |
| DCM | dichloromethane |
| ESI | electrospray ionization |
| EU | European Union |
| GC | gas chromatography |
| HEPES | 4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid |
| HHC | hexahydrocannabinol |
| 8-hydroxy-iso-HHC | 8-hydroxy-iso-hexahydrocannabinol |
| 9α-hydroxy-HHC | 9α-hydroxy-hexahydrocannabinol |
| HPLC | high performance liquid chromatography |
| HCl | hydrochloric acid |
| IR | infra-red |
| LC | liquid chromatography |
| MS | mass spectrometry |
| NMR | nuclear magnetic resonance |
| OTC | over the counter |
| RASFF | Rapid Alert System for Food and Feed |
| SDS | sodium dodecyl sulfate |
| NaOH | sodium hydroxide |
| THC | tetrahydrocannabinol |
| iso-THC | iso-tetrahydrocannabinol |
| Δ6a-THC | Δ6a-tetrahydrocannabinol |
| Δ7-THC | Δ7-tetrahydrocannabinol |
| Δ8-THC | Δ8-tetrahydrocannabinol |
| Δ8-iso-THC | Δ8-iso-tetrahydrocannabinol |
| Δ9-THC | Δ9-tetrahydrocannabinol |
| Δ10-THC | Δ10-tetrahydrocannabinol |
| Δ10a-THC | Δ10a-tetrahydrocannabinol |
| Δ11-THC | Δ11-tetrahydrocannabinol |
| Δ9-THCA | Δ9-tetrahydrocannabinolic acid |
| 10-methoxy-THC | 10-methoxy-tetrahydrocannabinol |
| 11,5′-dihydroxy-Δ9-THC | 11,5′-dihydroxy-Δ9-tetrahydrocannabinol |
| 11-hydroxy-THC | 11-hydroxy-tetrahydrocannabinol |
| 11-COOH-THC | 11-nor-9-carboxy-tetrahydrocannabinol |
| 6β-hydroxymethyl-Δ9-THC | 6β-hydroxymethyl-Δ9-tetrahydrocannabinol |
| 9-methoxy-THC | 9-methoxy-tetrahydrocannabinol |
| TLC | thin layer chromatography |
| UPLC | ultra-performance liquid chromatography |
| UV | ultra violet |
| UN | United Nations |
| USP | United States Pharmacopeia |
| WHO | World Health Organization |
Appendix A
| Compound | Abbreviation | Conditions Reported in Literature | Stereo- Isomers | Psycho- Tropicity |
|---|---|---|---|---|
| Cannabinol | CBN | in vitro (SGJ a) [39] | 1 | yes [43] |
| Cannabidiol | CBD | HCl/acetic acid in ethanol [54] (conversion was not complete) | 4 | no [45] |
| ∆9-Tetrahydrocannabinol | ∆9-THC | H2SO4/HCl/acetic acid in ethanol/methanol, refluxing (N2) [54,55,76]; BF3Et2O (N2), 0 °C [76]; acidic conditions (HCl) [74,75,78]; in vitro (SGJ a) [39,80]; in vivo (rats) [56] | 4 | yes [30] |
| ∆7-Tetrahydrocannabinol | ∆7-THC | HCl/acetic acid in ethanol [54] | 8 | unknown |
| ∆8-Tetrahydrocannabinol | ∆8-THC | H2SO4/HCl/acetic acid in ethanol [54]; p-TSA b in benzene/toluene, refluxing (N2) [53,55,76]; acidic conditions (H2SO4, p-TSA b) [74,75,78]; in vitro (SGJ a) [80] | 4 | yes [35] |
| ∆10-Tetrahydrocannabinol | ∆10-THC | HCl/acetic acid in ethanol [54] | 4 | no [35] |
| ∆11-Tetrahydrocannabinol | ∆11-THC | HCl/acetic acid in ethanol [54] | 4 | yes [35] |
| 11-Hydroxycannabidiol | 11- hydroxy-CBD | H2SO4/HCl/acetic acid in ethanol [54] | 4 | unknown |
| 5′-Hydroxycannabidiol | 5′-hydroxy-CBD | Acetic acid in ethanol [54] | 4 | unknown |
| 11,5′-Dihydroxycannabidiol | 11,5′-hydroxy-CBD | H2SO4/HCl/acetic acid in ethanol [54] | 4 | unknown |
| 11-Hydroxy-∆9-tetrahydrocannabinol | 11- hydroxy-THC | HCl in ethanol [54] | 4 | yes [36] |
| 11,5′-Dihydroxy-∆9-tetrahydrocannabinol | 11,5′-dihydroxy-THC | HCl in ethanol [54] | 4 | unknown |
| 8-Hydroxy-iso-hexahydrocannabinol | 8-hydroxy-iso-HHC | H2SO4/HCl/acetic acid in ethanol [54]; in vitro (SGJ a) [39] | - | yes [39] |
| 9α-Hydroxy-hexahydrocannabinol | 9α-hydroxy-HHC | H2SO4/HCl/acetic acid in ethanol [54]; in vitro (SGJ a) [39] | - | yes [39] |
| 9-Methoxy-hexahydrocannabinol | 9-methoxy-HHC | H2SO4/HCl/acetic acid in ethanol [54]; H2SO4 in methanol [53] | 8 | unknown |
| 10-Methoxy-hexahydrocannabinol | 10-methoxy-HHC | H2SO4 [10]; H2SO4 in methanol [53] | 16 | unknown |
| 9-Ethoxy-hexahydrocannabinol | 9-ethoxy-HHC | HCl/H2SO4 in ethanol [53,55] | 8 | unknown |
| 10-Ethoxy-hexahydrocannabinol | 10-ethoxy-HHC | HCl/H2SO4 in ethanol [53,55] | 16 | unknown |
| iso-Tetrahydrocannabinol | iso-THC | BF3 in DCM/CCl4 or HCl/H2SO4 in ethanol [53] | 4 | unknown |
References
- Turner, C.E.; Elsohly, M.A.; Boeren, E.G. Constituents of Cannabis sativa L. XVII. A review of the natural constituents. J. Nat. Prod. 1980, 43, 169–234. [Google Scholar] [CrossRef] [PubMed]
- Ameri, A. The effects of cannabinoids on the brain. Prog. Neurobiol. 1999, 58, 315–348. [Google Scholar] [CrossRef]
- Lachenmeier, D.W.; Rajcic de Rezende, T.; Habel, S.; Sproll, C.; Walch, S.G. Aktuelle Rechtsprechung bestätigt Novel-Food-Einstufung von Hanfextrakten und Cannabidiol (CBD) in Lebensmitteln—Betäubungsmitteleinstufung von Cannabislebensmitteln ist weiterhin unklar. Deut. Lebensm. Rundsch. 2020, 116, 111–119. [Google Scholar] [CrossRef]
- UN General Assembly. Protocol Amending the Single Convention on Narcotic Drugs, 1961; United Nations: New York, NY, USA, 1972. [Google Scholar]
- Lachenmeier, D.W. Hanfhaltige Lebensmittel—Ein Problem? Deut. Lebensm. Rundsch. 2004, 100, 481–490. [Google Scholar] [CrossRef]
- Lachenmeier, D.W.; Walch, S.G. Current status of THC in German hemp food products. J. Ind. Hemp. 2006, 10, 5–17. [Google Scholar] [CrossRef]
- Burstein, S. Cannabidiol (CBD) and its analogs: A review of their effects on inflammation. Bioorg. Med. Chem. 2015, 23, 1377–1385. [Google Scholar] [CrossRef]
- Zuardi, A.W. Cannabidiol: From an inactive cannabinoid to a drug with wide spectrum of action. Rev. Bras. de Psiquiatr. 2008, 30, 271–280. [Google Scholar] [CrossRef]
- Iffland, K.; Grotenhermen, F. An update on safety and side effects of cannabidiol: A review of clinical data and relevant animal studies. Cannabis Cannabinoid Res. 2017, 2, 139–154. [Google Scholar] [CrossRef]
- Mechoulam, R.; Parker, L.A.; Gallily, R. Cannabidiol: An overview of some pharmacological aspects. J. Clin. Pharmacol. 2002, 42, 11S–19S. [Google Scholar] [CrossRef]
- Zuardi, A.W.; Crippa, J.A.S.; Hallak, J.E.C.; Bhattacharyya, S.; Atakan, Z.; Martin-Santos, R.; McGuire, P.K.; Guimarães, F.S. A critical review of the antipsychotic effects of cannabidiol: 30 years of a translational investigation. Curr. Pharm. Des. 2012, 18, 5131–5140. [Google Scholar] [CrossRef]
- Iseger, T.A.; Bossong, M.G. A systematic review of the antipsychotic properties of cannabidiol in humans. Schizophr. Res. 2015, 162, 153–161. [Google Scholar] [CrossRef]
- Ben Amar, M. Cannabinoids in medicine: A review of their therapeutic potential. J. Ethnopharmacol. 2006, 105, 1–25. [Google Scholar] [CrossRef] [PubMed]
- Cerne, K. Toxicological properties of Δ9-tetrahydrocannabinol and cannabidiol. Arh. Hig. Rada Toksikol. 2020, 71, 1–11. [Google Scholar] [CrossRef]
- Chesney, E.; Oliver, D.; Green, A.; Sovi, S.; Wilson, J.; Englund, A.; Freeman, T.P.; McGuire, P. Adverse effects of cannabidiol: A systematic review and meta-analysis of randomized clinical trials. Neuropsychopharmacology 2020. [Google Scholar] [CrossRef] [PubMed]
- Perkins, D.; Butler, J.; Ong, K.; Nguyen, T.-H.; Cox, S.; Francis, B.; Mcintosh, M.; Lilley, B. A phase 1, randomised, placebo-controlled, dose escalation study to investigate the safety, tolerability and pharmacokinetics of cannabidiol in fed healthy volunteers. Eur. J. Drug Metab. Pharmacokinet. 2020. [Google Scholar] [CrossRef] [PubMed]
- Skinner, C.M.; Nookaew, I.; Ewing, L.E.; Wongsurawat, T.; Jenjaroenpun, P.; Quick, C.M.; Yee, E.U.; Piccolo, B.D.; ElSohly, M.; Walker, L.A.; et al. Potential probiotic or trigger of gut inflammation—The Janus-faced nature of cannabidiol-rich Cannabis extract. J. Diet. Suppl. 2020. [Google Scholar] [CrossRef] [PubMed]
- Spindle, T.R.; Cone, E.J.; Goffi, E.; Weerts, E.M.; Mitchell, J.M.; Winecker, R.E.; Bigelow, G.E.; Flegel, R.R.; Vandrey, R. Pharmacodynamic effects of vaporized and oral cannabidiol (CBD) and vaporized CBD-dominant cannabis in infrequent cannabis users. Drug Alcohol Depend. 2020, 211, 107937. [Google Scholar] [CrossRef]
- Lachenmeier, D.W.; Habel, S.; Fischer, B.; Herbi, F.; Zerbe, Y.; Bock, V.; Rajcic de Rezende, T.; Walch, S.G.; Sproll, C. Are side effects of cannabidiol (CBD) products caused by tetrahydrocannabinol (THC) contamination? F1000Res. 2020, 8, 1394. [Google Scholar] [CrossRef]
- Mazzetti, C.; Ferri, E.; Pozzi, M.; Labra, M. Quantification of the content of cannabinol in commercially available e-liquids and studies on their thermal and photo-stability. Sci. Rep. 2020, 10, 3697. [Google Scholar] [CrossRef]
- Lachenmeier, D.W.; Bock, V.; Deych, A.; Sproll, C.; Rajcic de Rezende, T.; Walch, S.G. Hanfhaltige Lebensmittel - ein Update. Deut. Lebensm. Rundsch. 2019, 115, 351–372. [Google Scholar] [CrossRef]
- Regulation (EU) 2015/2283 of the European Parliament and of the Council of 25 November 2015 on novel foods, amending Regulation (EU) No 1169/2011 of the European Parliament and of the Council and repealing Regulation (EC) No 258/97 of the European Parliament and of the Council and Commission Regulation (EC) No 1852/2001. Off. J. EU 2015, L 327, 1–22.
- Google Trends. Available online: https://trends.google.de/trends/explore?q=CBD&geo=DE&date=2013-01-01%202020-03-11#TIMESERIES (accessed on 13 March 2020).
- Food Safety Authority of Ireland. Available online: https://www.fsai.ie/news_centre/press_releases/cbd_food_supplement_survey_130220.html (accessed on 18 March 2020).
- Lachenmeier, D.W.; Walch, S.G. Cannabidiol (CBD): A strong plea for mandatory pre-marketing approval of food supplements. J. Consum. Prot. Food Saf. 2020, 5, 97–98. [Google Scholar] [CrossRef]
- Mechoulam, R. Cannabinoids as Therapeutic Agents; CRC Press: Boca Raton, FL, USA, 1986. [Google Scholar]
- Ashton, C.H. Pharmacology and effects of cannabis: A brief review. Br. J. Psychiatry 2001, 178, 101–106. [Google Scholar] [CrossRef]
- Gaoni, Y.; Mechoulam, R. Isolation, structure, and partial synthesis of an active constituent of hashish. J. Am. Chem. Soc. 1964, 86, 1646–1647. [Google Scholar] [CrossRef]
- Mechoulam, R.; Shvo, Y. Hashish—I: The structure of cannabidiol. Tetrahedron 1963, 19, 2073–2078. [Google Scholar] [CrossRef]
- Pertwee, R.G. Cannabinoid pharmacology: The first 66 years. Br. J. Pharmacol. 2006, 147, S163–S171. [Google Scholar] [CrossRef] [PubMed]
- Howlett, A.C.; Bidaut-Russell, M.; Devane, W.A.; Melvin, L.S.; Johnson, M.R.; Herkenham, M. The cannabinoid receptor: Biochemical, anatomical and behavioral characterization. Trends Neurosci. 1990, 13, 420–423. [Google Scholar] [CrossRef]
- Howlett, A.C.; Barth, F.; Bonner, T.I.; Cabral, G.; Casellas, P.; Devane, W.A.; Felder, C.C.; Herkenham, M.; Mackie, K.; Martin, B.R.; et al. International Union of Pharmacology. XXVII. Classification of cannabinoid receptors. Pharmacol. Rev. 2002, 54, 161–202. [Google Scholar] [CrossRef] [PubMed]
- Devane, W.A.; Hanus, L.; Breuer, A.; Pertwee, R.G.; Stevenson, L.A.; Griffin, G.; Gibson, D.; Mandelbaum, A.; Etinger, A.; Mechoulam, R. Isolation and structure of a brain constituent that binds to the cannabinoid receptor. Science 1992, 258, 1946–1949. [Google Scholar] [CrossRef]
- UN General Assembly. Convention on Psychotropic Substances; United Nations: New York, NY, USA, 1971. [Google Scholar]
- WHO Expert Committee on Drug Dependence. Isomers of THC, Critical Review; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Lemberger, L.; Martz, R.; Rodda, B.; Forney, R.; Rowe, H. Comparative pharmacology of Δ9-tetrahydrocannabinol and its metabolite, 11-OH-Δ9-tetrahydrocannabinol. J. Clin. Investig. 1973, 52, 2411–2417. [Google Scholar] [CrossRef]
- Watanabe, K.; Yamamoto, I.; Oguri, K.; Yoshimura, H. Comparison in mice of pharmacological effects of Δ8-tetrahydrocannabinol and its metabolites oxidized at 11-position. Eur. J. Pharmacol. 1980, 63, 1–6. [Google Scholar] [CrossRef]
- Järbe, T.U.C.; Hiltunen, A.J.; Lander, N.; Mechoulam, R. Cannabimimetic activity (Δ1-THC cue) of cannabidiol monomethyl ether and two stereoisomeric hexahydrocannabinols in rats and pigeons. Pharmacol. Biochem. Behav. 1986, 25, 393–399. [Google Scholar] [CrossRef]
- Watanabe, K.; Itokawa, Y.; Yamaori, S.; Funahashi, T.; Kimura, T.; Kaji, T.; Usami, N.; Yamamoto, I. Conversion of cannabidiol to Δ9-tetrahydrocannabinol and related cannabinoids in artificial gastric juice, and their pharmacological effects in mice. Forensic Toxicol. 2007, 25, 16–21. [Google Scholar] [CrossRef]
- Ujváry, I.; Grotenhermen, F. 11-Nor-9-carboxy-∆9-tetrahydrocannabinol – a ubiquitous yet underresearched cannabinoid. A review of the literature. Cannabinoids 2014, 9, 1–8. [Google Scholar]
- Moreno-Sanz, G. Can you pass the acid test? Critical review and novel therapeutic perspectives of Δ9-tetrahydrocannabinolic acid A. Cannabis Cannabinoid Res. 2016, 1, 124–130. [Google Scholar] [CrossRef]
- Yamamoto, I.; Watanabe, K.; Kuzuoka, K.; Narimatsu, S.; Yoshimura, H. The pharmacological activity of cannabinol and its major metabolite, 11-hydroxycannabinol. Chem. Pharm. Bull. 1987, 35, 2144–2147. [Google Scholar] [CrossRef]
- Järbe, T.U.C.; Hiltunen, A.J. Cannabimimetic activity of cannabinol in rats and pigeons. Neuropharmacology 1987, 26, 219–228. [Google Scholar] [CrossRef]
- Compton, D.R.; Rice, K.C.; de Costa, B.R.; Razdan, R.K.; Melvin, L.S.; Johnson, M.R.; Martin, B.R. Cannabinoid structure-activity relationships: Correlation of receptor binding and in vivo activities. J. Pharmacol. Exp. Ther. 1993, 265, 218–226. [Google Scholar]
- Hayakawa, K.; Mishima, K.; Fujiwara, M. Therapeutic potential of non-psychotropic cannabidiol in ischemic stroke. Pharmaceuticals 2010, 3, 2197–2212. [Google Scholar] [CrossRef]
- Mechoulam, R.; Shani, A.; Edery, H.; Grunfeld, Y. Chemical basis of hashish activity. Science 1970, 169, 611–612. [Google Scholar] [CrossRef]
- Pertwee, R.G. The diverse CB1 and CB2 receptor pharmacology of three plant cannabinoids: ∆9-tetrahydrocannabinol, cannabidiol and ∆9-tetrahydrocannabivarin. Br. J. Pharmacol. 2008, 153, 199–215. [Google Scholar] [CrossRef] [PubMed]
- Takeda, S.; Okazaki, H.; Ikeda, E.; Abe, S.; Yoshioka, Y.; Watanabe, K.; Aramaki, H. Down-regulation of cyclooxygenase-2 (COX-2) by cannabidiolic acid in human breast cancer cells. J. Toxicol. Sci. 2014, 39, 711–716. [Google Scholar] [CrossRef] [PubMed]
- Rock, E.M.; Limebeer, C.L.; Parker, L.A. Effect of cannabidiolic acid and ∆9-tetrahydrocannabinol on carrageenan-induced hyperalgesia and edema in a rodent model of inflammatory pain. Psychopharmacology 2018, 235, 3259–3271. [Google Scholar] [CrossRef] [PubMed]
- Navarro, G.; Varani, K.; Reyes-Resina, I.; Sánchez de Medina, V.; Rivas-Santisteban, R.; Sánchez-Carnerero, C.; Carolina, V.F.; Casano, S.; Ferreiro-Vera, C.; Canela, E.I.; et al. Cannabigerol action at cannabinoid CB1 and CB2 receptors and at CB1-CB2 heteroreceptor complexes. Front. Pharmacol. 2018, 9, 632. [Google Scholar] [CrossRef]
- Radwan, M.M.; Elsohly, M.A.; Slade, D.; Ahmed, S.A.; Khan, I.A.; Ross, S.A. Biologically active cannabinoids from high-potency Cannabis sativa. J. Nat. Prod. 2009, 72, 906–911. [Google Scholar] [CrossRef]
- Pollastro, F.; Caprioglio, D.; Del Prete, D.; Rogati, F.; Minassi, A.; Taglialatela-Scafati, O.; Munoz, E.; Appendino, G. Cannabichromene. Nat. Prod. Commun. 2018, 13, 1934578X1801300. [Google Scholar] [CrossRef]
- Gaoni, Y.; Mechoulam, R. The iso-tetrahydrocannabinols. Isr. J. Chem. 1968, 6, 679–690. [Google Scholar] [CrossRef]
- Kiselak, T.D.; Koerber, R.; Verbeck, G.F. Synthetic route sourcing of illicit at home cannabidiol (CBD) isomerization to psychoactive cannabinoids using ion mobility-coupled-LC-MS/MS. Forensic Sci. Int. 2020, 308, 110173. [Google Scholar] [CrossRef]
- Gaoni, Y.; Mechoulam, R. Hashish—VII. Tetrahedron 1966, 22, 1481–1488. [Google Scholar] [CrossRef]
- Hložek, T.; Uttl, L.; Kadeřábek, L.; Balíková, M.; Lhotková, E.; Horsley, R.R.; Nováková, P.; Šíchová, K.; Štefková, K.; Tylš, F.; et al. Pharmacokinetic and behavioural profile of THC, CBD, and THC+CBD combination after pulmonary, oral, and subcutaneous administration in rats and confirmation of conversion in vivo of CBD to THC. Eur. Neuropsychopharm. 2017, 27, 1223–1237. [Google Scholar] [CrossRef]
- Vollner, L.; Bieniek, D.; Korte, F. Review of analytical methods for identification and quantification of Cannabis products. Regul. Toxicol. Pharmacol. 1986, 6, 348–358. [Google Scholar] [CrossRef]
- Bartle, K.D.; Myers, P. History of gas chromatography. Trends Anal. Chem. 2002, 21, 547–557. [Google Scholar] [CrossRef]
- Farmilo, C.G.; Davis, T.W.M. Paper and gas chromatographic analysis of cannabis. J. Pharm. Pharmacol. 1961, 13, 767–768. [Google Scholar] [CrossRef] [PubMed]
- Davis, T.W.M.; Farmilo, C.G.; Osadchuk, M. Identification and origin determinations of cannabis by gas and paper chromatography. Anal. Chem. 1963, 35, 751–755. [Google Scholar] [CrossRef]
- Snyder, L.R. Modern practice of liquid chromatography: Before and after 1971. J. Chem. Educ. 1997, 74, 37. [Google Scholar] [CrossRef]
- Wheals, B.B.; Smith, R.N. Comparative cannabis analysis: A comparison of high-pressure liquid chromatography with other chromatographic techniques. J. Chromatogr. A 1975, 105, 396–400. [Google Scholar] [CrossRef]
- Smith, R.N. High-pressure liquid chromatography of cannabis. J. Chromatogr. A 1975, 115, 101–106. [Google Scholar] [CrossRef]
- Smith, R.N.; Vaughan, C.G. High-pressure liquid chromatography of cannabis. J. Chromatogr. A 1976, 129, 347–354. [Google Scholar] [CrossRef]
- Raharjo, T.J.; Verpoorte, R. Methods for the analysis of cannabinoids in biological materials: A review. Phytochem. Anal. 2004, 15, 79–94. [Google Scholar] [CrossRef]
- Citti, C.; Braghiroli, D.; Vandelli, M.A.; Cannazza, G. Pharmaceutical and biomedical analysis of cannabinoids: A critical review. J. Pharm. Biomed. Anal. 2018, 147, 565–579. [Google Scholar] [CrossRef]
- Dussy, F.E.; Hamberg, C.; Luginbühl, M.; Schwerzmann, T.; Briellmann, T.A. Isolation of ∆9-THCA-A from hemp and analytical aspects concerning the determination of ∆9-THC in cannabis products. Forensic Sci. Int. 2005, 149, 3–10. [Google Scholar] [CrossRef] [PubMed]
- Garcia, A.; Borchardt, D.; Chang, C.-E.A.; Marsella, M.J. Thermal isomerization of cannabinoid analogues. J. Am. Chem. Soc. 2009, 131, 16640–16641. [Google Scholar] [CrossRef] [PubMed]
- Harvey, D.J.; Mechoulam, R. Metabolites of cannabidiol identified in human urine. Xenobiotica 1990, 20, 303–320. [Google Scholar] [CrossRef] [PubMed]
- Harvey, D.J.; Samara, E.; Mechoulam, R. Urinary metabolites of cannabidiol in dog, rat and man and their identification by gas chromatography—Mass spectrometry. J. Chromatogr. B 1991, 562, 299–322. [Google Scholar] [CrossRef]
- Angeli, I.; Casati, S.; Ravelli, A.; Minoli, M.; Orioli, M. A novel single-step GC-MS/MS method for cannabinoids and 11-OH-THC metabolite analysis in hair. J. Pharm. Biomed. Anal. 2018, 155, 1–6. [Google Scholar] [CrossRef]
- Broecker, S.; Pragst, F. Isomerization of cannabidiol and Δ9-tetrahydrocannabinol during positive electrospray ionization. In-source hydrogen/deuterium exchange experiments by flow injection hybrid quadrupole-time-of-flight mass spectrometry. Rapid Commun. Mass Spectrom. 2012, 26, 1407–1414. [Google Scholar] [CrossRef]
- Gertsch, J. Analytical and pharmacological challenges in cannabis research. Planta Med. 2018, 84, 213. [Google Scholar] [CrossRef]
- Adams, R.; Pease, D.C.; Cain, C.K.; Clark, J.H. Structure of cannabidiol. VI. Isomerization of cannabidiol to tetrahydrocannabinol, a physiologically active product. Conversion of cannabidiol to cannabinol. J. Am. Chem. Soc. 1940, 62, 2402–2405. [Google Scholar] [CrossRef]
- Adams, R.; Cain, C.K.; McPhee, W.D.; Wearn, R.B. Structure of cannabidiol. XII. Isomerization to tetrahydrocannabinols. J. Am. Chem. Soc. 1941, 63, 2209–2213. [Google Scholar] [CrossRef]
- Webster, G.B.; Sarna, L.P.; Mechoulam, R. Conversion of CBD to Δ8-THC and Δ9-THC. Google Patents US20040143126A1, 25 June 2008. [Google Scholar]
- Mechoulam, R.; Gaoni, Y. Recent advances in the chemistry of hashish. In Progress in the Chemistry of Organic Natural Products; Zechmeister, L., Ed.; Springer: Vienna, Austria, 1967; Volume 25, pp. 175–213. [Google Scholar] [CrossRef]
- Layton, C.; Runco, J.; Aubin, A. Forced Degradation of Cannabidiol; Waters Corporation: Milford, MA, USA, 2016. [Google Scholar]
- Nagai, K.; Watanabe, K.; Narimatsu, S.; Gohda, H.; Matsunaga, T.; Yamamoto, I.; Yoshimura, H. In vitro metabolic formation of a new metabolite, 6β-hydroxymethyl-∆9-tetrahydrocannabinol from cannabidiol through an epoxide intermediate and its pharmacological effects on mice. Biol. Pharm. Bull. 1993, 16, 1008–1013. [Google Scholar] [CrossRef][Green Version]
- Merrick, J.; Lane, B.; Sebree, T.; Yaksh, T.; O’Neill, C.; Banks, S. Identification of psychoactive degradants of cannabidiol in simulated gastric and physiological fluid. Cannabis Cannabinoid Res. 2016, 1, 102–112. [Google Scholar] [CrossRef]
- Grotenhermen, F.; Russo, E.; Zuardi, A.W. Even high doses of oral cannabidiol do not cause THC-like effects in humans: Comment on Merrick et al. Cannabis Cannabinoid Res. 2017, 2, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Samara, E.; Bialer, M.; Harvey, D.J. Identification of glucose conjugates as major urinary metabolites of cannabidiol in the dog. Xenobiotica 1990, 20, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Samara, E.; Bialer, M.; Harvey, D.J. Identification of urinary metabolites of cannabidiol in the dog. Drug Metab. Dispos. 1990, 18, 571–579. [Google Scholar] [PubMed]
- Samara, E.; Bialer, M.; Harvey, D.J. Pharmacokinetics of urinary metabolites of cannabidiol in the dog. Biopharm. Drug Dispos. 1990, 11, 785–795. [Google Scholar] [CrossRef] [PubMed]
- Samara, E.; Bialer, M.; Harvey, D.J. Metabolism of cannabidiol by the rat. Eur. J. Drug Metab. Pharmacokinet. 1991, 16, 305–313. [Google Scholar] [CrossRef] [PubMed]
- Consroe, P.; Kennedy, K.; Schram, K. Assay of plasma cannabidiol by capillary gas chromatography/ion trap mass spectroscopy following high-dose repeated daily oral administration in humans. Pharmacol. Biochem. Behav. 1991, 40, 517–522. [Google Scholar] [CrossRef]
- Martin-Santos, R.; Crippa, J.A.; Batalla, A.; Bhattacharyya, S.; Atakan, Z.; Borgwardt, S.; Allen, P.; Seal, M.; Langohr, K.; Farré, M.; et al. Acute effects of a single, oral dose of Δ9-tetrahydrocannabinol (THC) and cannabidiol (CBD) administration in healthy volunteers. Curr. Pharm. Des. 2012, 18, 4966–4979. [Google Scholar] [CrossRef]
- Ujváry, I.; Hanuš, L. Human metabolites of cannabidiol: A review on their formation, biological activity, and relevance in therapy. Cannabis Cannabinoid Res. 2016, 1, 90–101. [Google Scholar] [CrossRef]
- Bonn-Miller, M.O.; Banks, S.L.; Sebree, T. Conversion of cannabidiol following oral administration: Authors’ response to Grotenhermen et al. Cannabis Cannabinoid Res. 2017, 2, 5–7. [Google Scholar] [CrossRef]
- Nahler, G.; Grotenhermen, F.; Zuardi, A.W.; Crippa, J.A.S. A conversion of oral cannabidiol to Δ9-tetrahydrocannabinol seems not to occur in humans. Cannabis Cannabinoid Res. 2017, 2, 81–86. [Google Scholar] [CrossRef] [PubMed]
- Palazzoli, F.; Citti, C.; Licata, M.; Vilella, A.; Manca, L.; Zoli, M.; Vandelli, M.A.; Forni, F.; Cannazza, G. Development of a simple and sensitive liquid chromatography triple quadrupole mass spectrometry (LC-MS/MS) method for the determination of cannabidiol (CBD), Δ9-tetrahydrocannabinol (THC) and its metabolites in rat whole blood after oral administration of a single high dose of CBD. J. Pharm. Biomed. Anal. 2018, 150, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Wray, L.; Stott, C.; Jones, N.; Wright, S. Cannabidiol does not convert to Δ9-tetrahydrocannabinol in an in vivo animal model. Cannabis Cannabinoid Res. 2017, 2, 282–287. [Google Scholar] [CrossRef] [PubMed]
- Crippa, J.A.S.; Zuardi, A.W.; Hallak, J.C.; Miyazawa, B.; Bernardo, S.A.; Donaduzzi, C.M.; Guzzi, S.; Favreto, W.A.J.; Campos, A.; Queiroz, M.E.C.; et al. Oral cannabidiol does not convert to Δ8-THC or Δ9-THC in humans: A pharmacokinetic study in healthy subjects. Cannabis Cannabinoid Res. 2020, 5, 89–98. [Google Scholar] [CrossRef] [PubMed]
- Crippa, J.A.S.; Crippa, A.C.S.; Hallak, J.E.C.; Martín-Santos, R.; Zuardi, A.W. Δ9-THC intoxication by cannabidiol-enriched cannabis extract in two children with refractory epilepsy: Full remission after switching to purified cannabidiol. Front. Pharmacol. 2016, 7, 359. [Google Scholar] [CrossRef] [PubMed]
- Liebling, J.P.; Clarkson, N.J.; Gibbs, B.W.; Yates, A.S.; O’Sullivan, S.E. An analysis of over-the-counter Cannabidiol products in the United Kingdom. Cannabis Cannabinoid Res. 2020. [Google Scholar] [CrossRef]
- Srebnik, M.; Lander, N.; Breuer, A.; Mechoulam, R. Base-catalysed double-bond isomerizations of cannabinoids: Structural and stereochemical aspects. J. Chem. Soc. 1984, 2881–2886. [Google Scholar] [CrossRef]
- Mechoulam, R.; Hanuš, L. Cannabidiol: An overview of some chemical and pharmacological aspects. Part I: Chemical aspects. Chem. Phys. Lipids 2002, 121, 35–43. [Google Scholar] [CrossRef]
- Bonn-Miller, M.O.; Loflin, M.J.E.; Thomas, B.F.; Marcu, J.P.; Hyke, T.; Vandrey, R. Labeling accuracy of cannabidiol extracts sold online. JAMA 2017, 318, 1708–1709. [Google Scholar] [CrossRef]
- Hazekamp, A. The trouble with CBD oil. Med. Cannabis Cannabinoids 2018, 1, 65–72. [Google Scholar] [CrossRef]
- Pavlovic, R.; Nenna, G.; Calvi, L.; Panseri, S.; Borgonovo, G.; Giupponi, L.; Cannazza, G.; Giorgi, A. Quality traits of “Cannabidiol Oils”: Cannabinoids content, terpene fingerprint and oxidation stability of European commercially available preparations. Molecules 2018, 23, 1230. [Google Scholar] [CrossRef] [PubMed]
- Turner, C.E.; Henry, J.T. Constituents of Cannabis sativa L. IX: Stability of synthetic and naturally occurring cannabinoids in chloroform. J. Pharm. Sci. 1975, 64, 357–359. [Google Scholar] [CrossRef] [PubMed]
- Fairbairn, J.W.; Liebmann, J.A. The extraction and estimation of the cannabinoids in Cannabis sativa L. and its products. J. Pharm. Pharmacol. 1973, 25, 150–155. [Google Scholar] [CrossRef] [PubMed]
- Parker, J.M.; Borke, M.L.; Block, L.H.; Cochran, T.G. Decomposition of cannabidiol in chloroform solution. J. Pharm. Sci. 1974, 63, 970–971. [Google Scholar] [CrossRef] [PubMed]
- Smith, R.N.; Vaughan, C.G. The decomposition of acidic and neutral cannabinoids in organic solvents. J. Pharm. Pharmacol. 1977, 29, 286–290. [Google Scholar] [CrossRef] [PubMed]
- Lydon, J.; Teramura, A.H. Photochemical decomposition of cannabidiol in its resin base. Phytochemistry 1987, 26, 1216–1217. [Google Scholar] [CrossRef]
- Turner, C.E.; Elsohly, M.A. Constituents of Cannabis sativa L. XVI. A possible decomposition pathway of Δ9-tetrahydrocannabinol to cannabinol. J. Heterocycl. Chem. 1979, 16, 1667–1668. [Google Scholar] [CrossRef]
- Harvey, D.J. Stability of cannabinoids in dried samples of cannabis dating from around 1896–1905. J. Ethnopharmacol. 1990, 28, 117–128. [Google Scholar] [CrossRef]
- Lindholst, C. Long term stability of cannabis resin and cannabis extracts. Aust. J. Forensic. Sci. 2010, 42, 181–190. [Google Scholar] [CrossRef]
- Trofin, I.G. Long term storage and cannabis oil stability. Rev. Chim. 2012, 63, 293–297. [Google Scholar] [CrossRef]
- Trofin, I.G.; Dabija, G.; Váireanu, D.-I.; Filipescu, L. The influence of long-term storage conditions on the stability of cannabinoids derived from cannabis resin. Rev. Chim. 2012, 63, 422–427. [Google Scholar]
- Skopp, G.; Pötsch, L.; Mauden, M. Stability of cannabinoids in hair samples exposed to sunlight. Clin. Chem. 2000, 46, 1846–1848. [Google Scholar] [CrossRef] [PubMed]
- Grafström, K.; Andersson, K.; Pettersson, N.; Dalgaard, J.; Dunne, S.J. Effects of long term storage on secondary metabolite profiles of cannabis resin. Forensic Sci. Int. 2019, 301, 331–340. [Google Scholar] [CrossRef]
- Deary, E.C.; Ross, J.S.; Nyhan, K.; Wallach, J.D. Conflicts of interest among authors of published cannabidiol articles, 2014–2019. Ann. Intern. Med. 2020, 172, 769–771. [Google Scholar] [CrossRef] [PubMed]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Golombek, P.; Müller, M.; Barthlott, I.; Sproll, C.; Lachenmeier, D.W. Conversion of Cannabidiol (CBD) into Psychotropic Cannabinoids Including Tetrahydrocannabinol (THC): A Controversy in the Scientific Literature. Toxics 2020, 8, 41. https://doi.org/10.3390/toxics8020041
Golombek P, Müller M, Barthlott I, Sproll C, Lachenmeier DW. Conversion of Cannabidiol (CBD) into Psychotropic Cannabinoids Including Tetrahydrocannabinol (THC): A Controversy in the Scientific Literature. Toxics. 2020; 8(2):41. https://doi.org/10.3390/toxics8020041
Chicago/Turabian StyleGolombek, Patricia, Marco Müller, Ines Barthlott, Constanze Sproll, and Dirk W. Lachenmeier. 2020. "Conversion of Cannabidiol (CBD) into Psychotropic Cannabinoids Including Tetrahydrocannabinol (THC): A Controversy in the Scientific Literature" Toxics 8, no. 2: 41. https://doi.org/10.3390/toxics8020041
APA StyleGolombek, P., Müller, M., Barthlott, I., Sproll, C., & Lachenmeier, D. W. (2020). Conversion of Cannabidiol (CBD) into Psychotropic Cannabinoids Including Tetrahydrocannabinol (THC): A Controversy in the Scientific Literature. Toxics, 8(2), 41. https://doi.org/10.3390/toxics8020041







