The Effect of High-Frequency Vibration on Tooth Movement and Alveolar Bone in Non-Growing Skeletal Class II High Angle Orthodontic Patients: Case Series
Abstract
1. Introduction
2. Materials and Methods
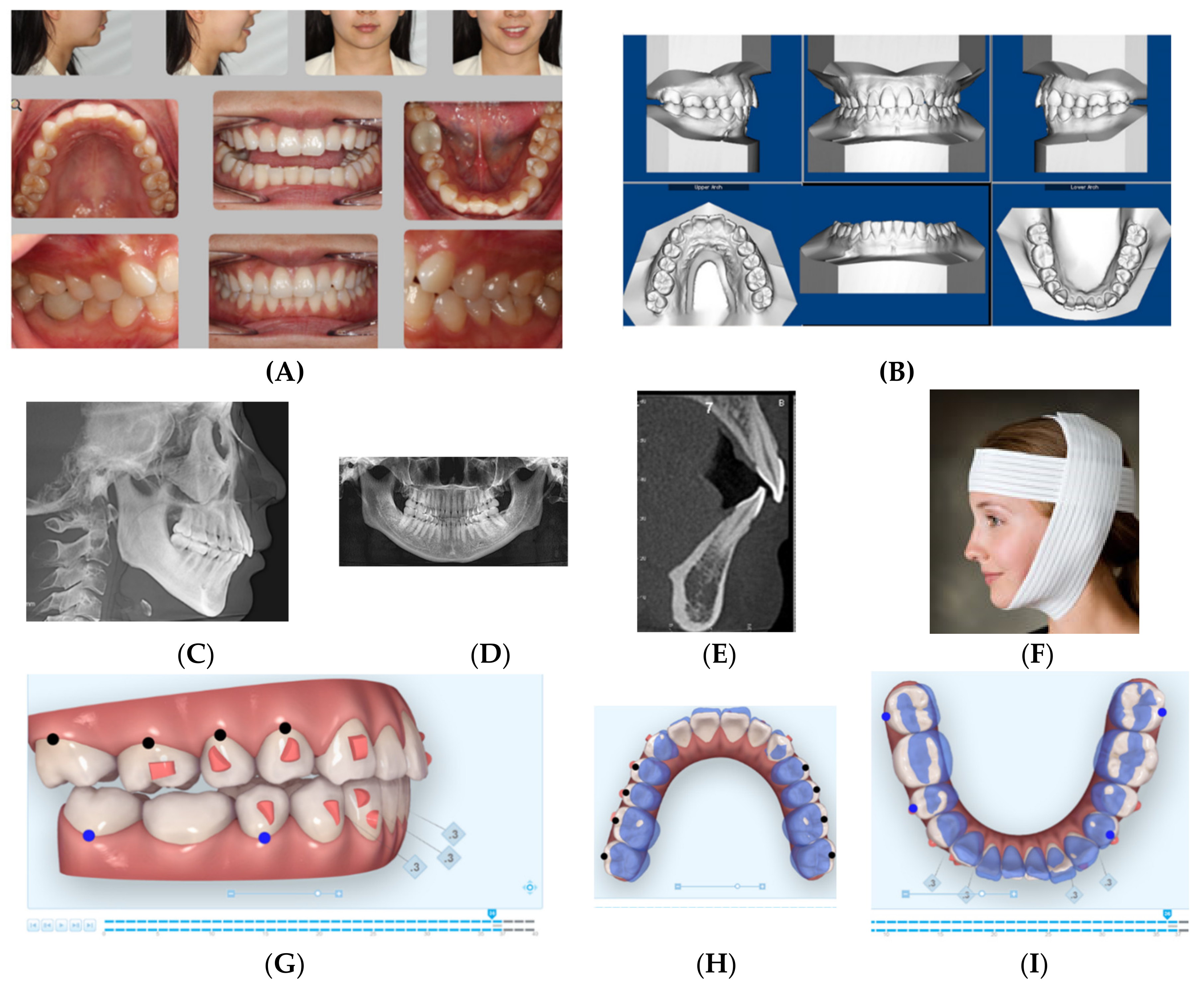
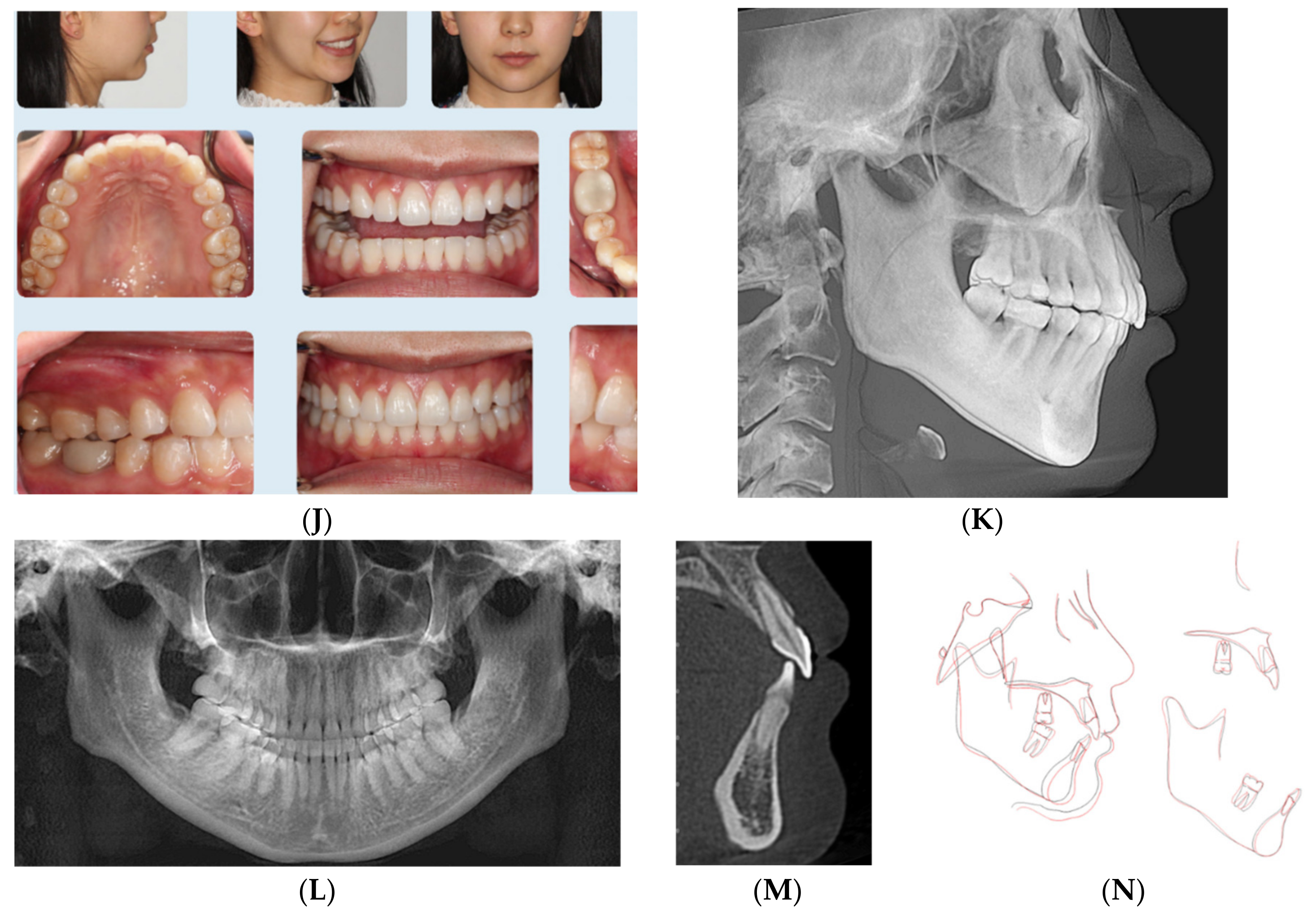
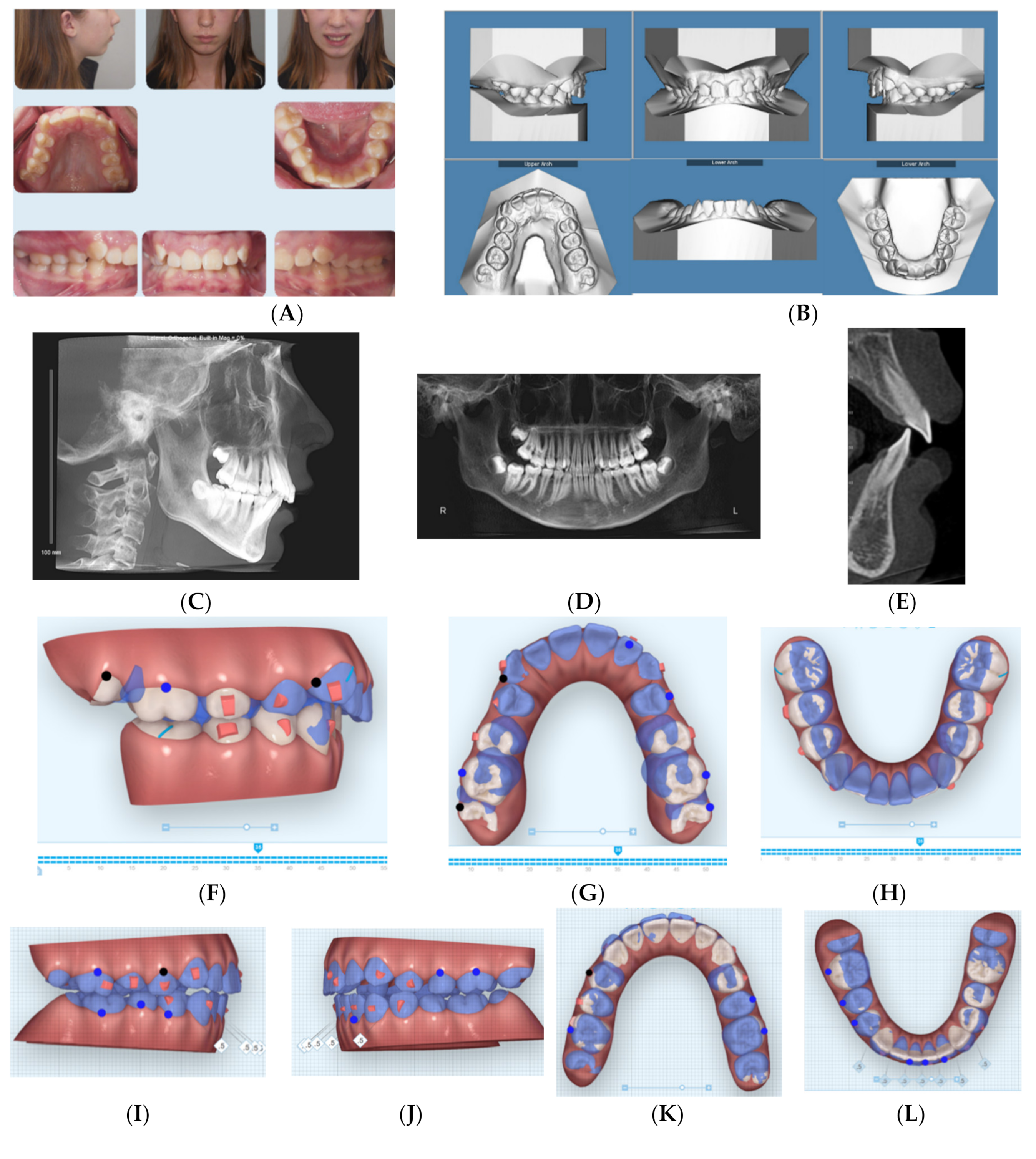
2.1. Case 1
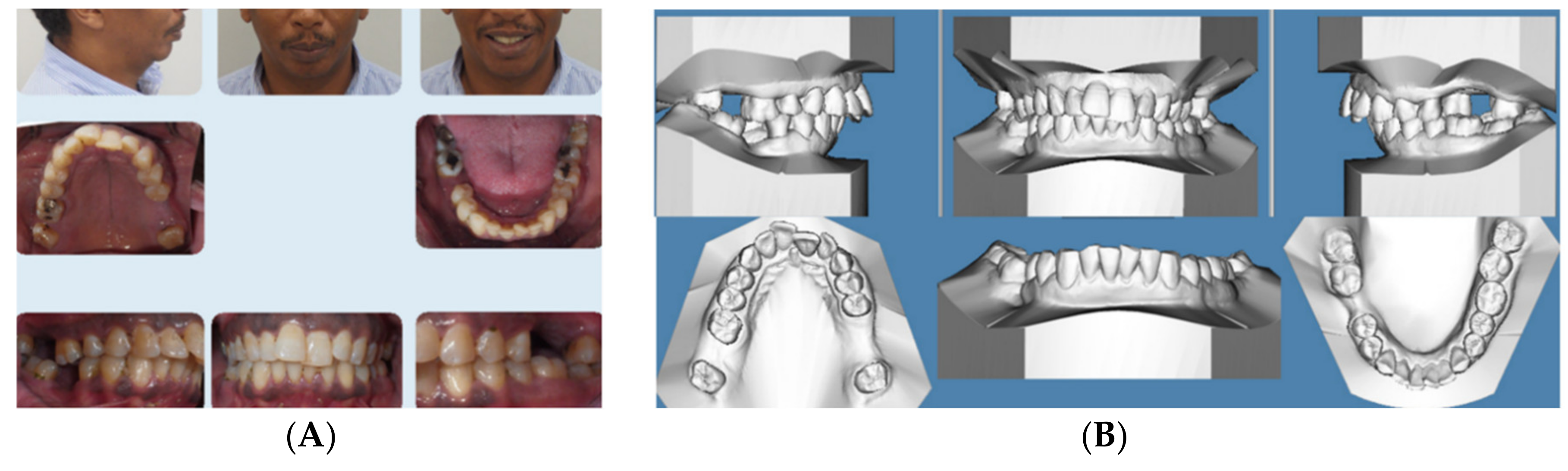
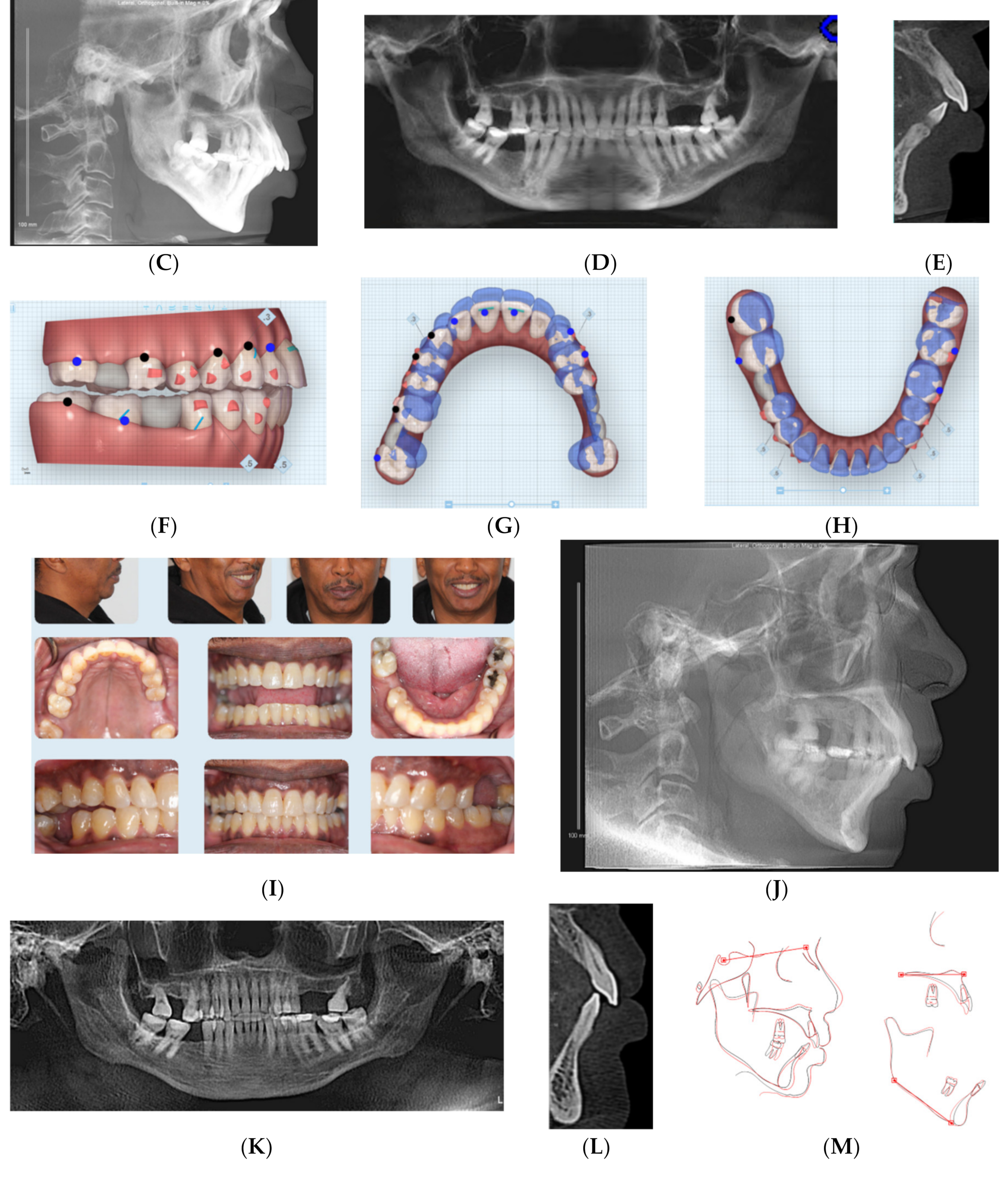
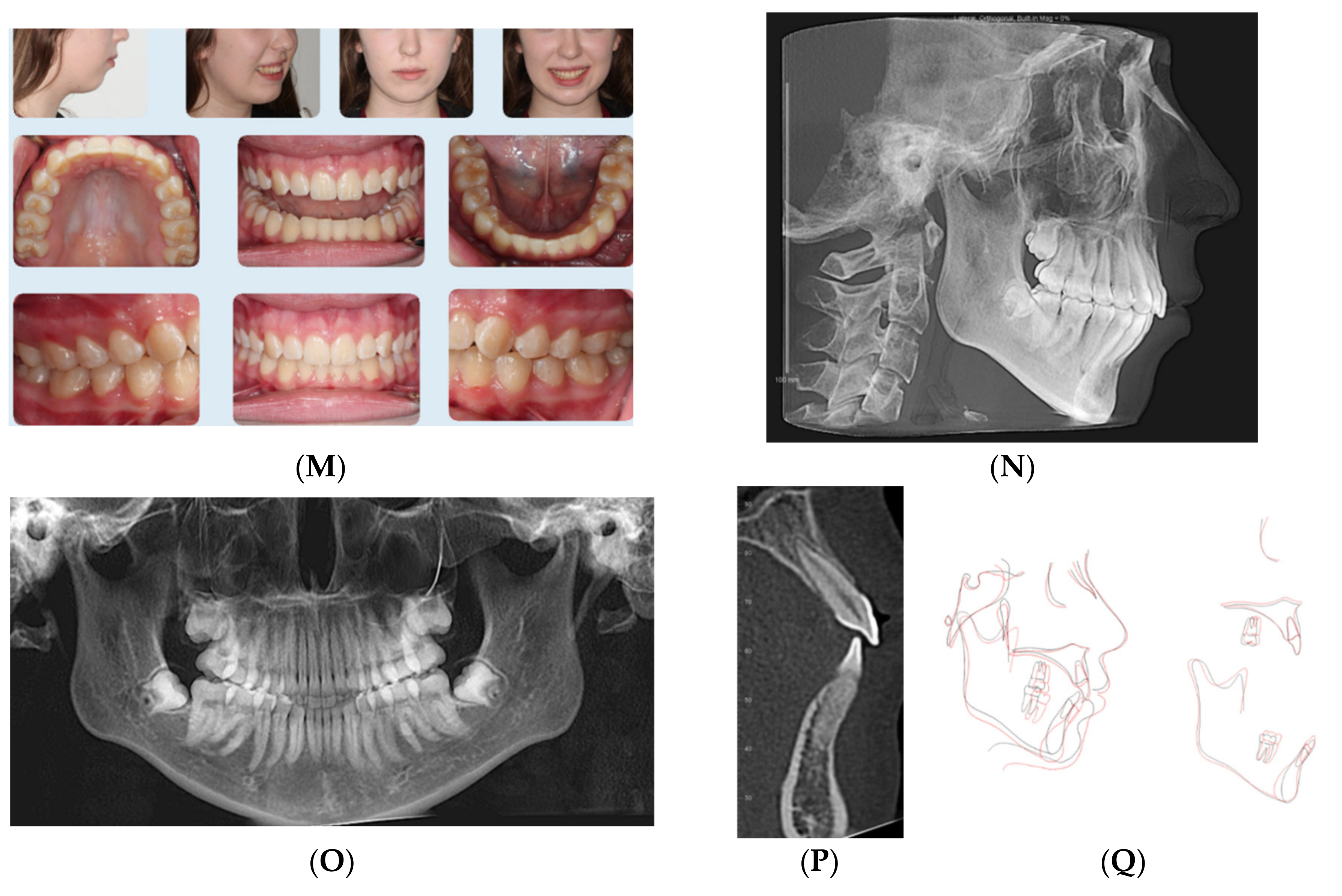
2.2. Case 2
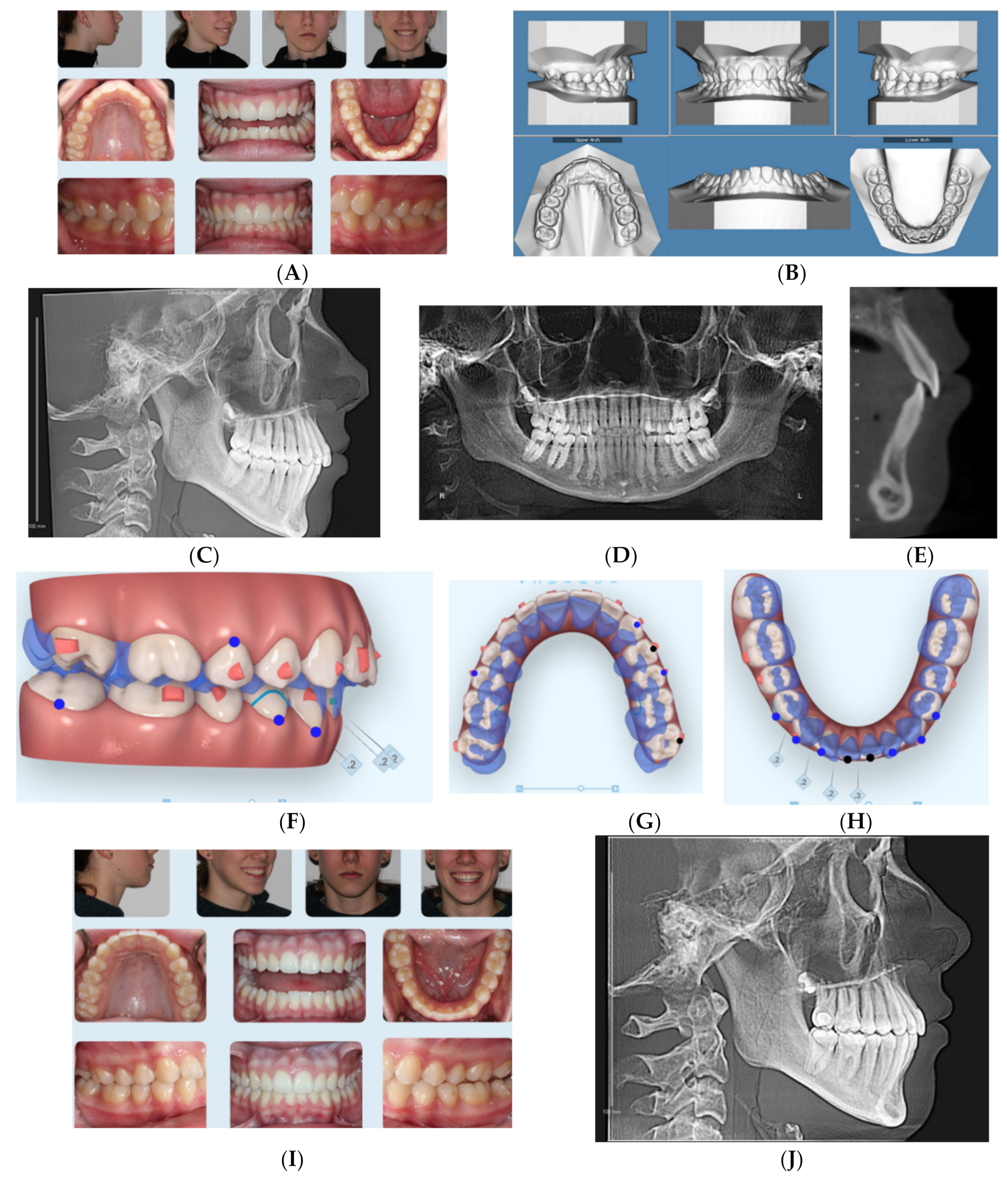
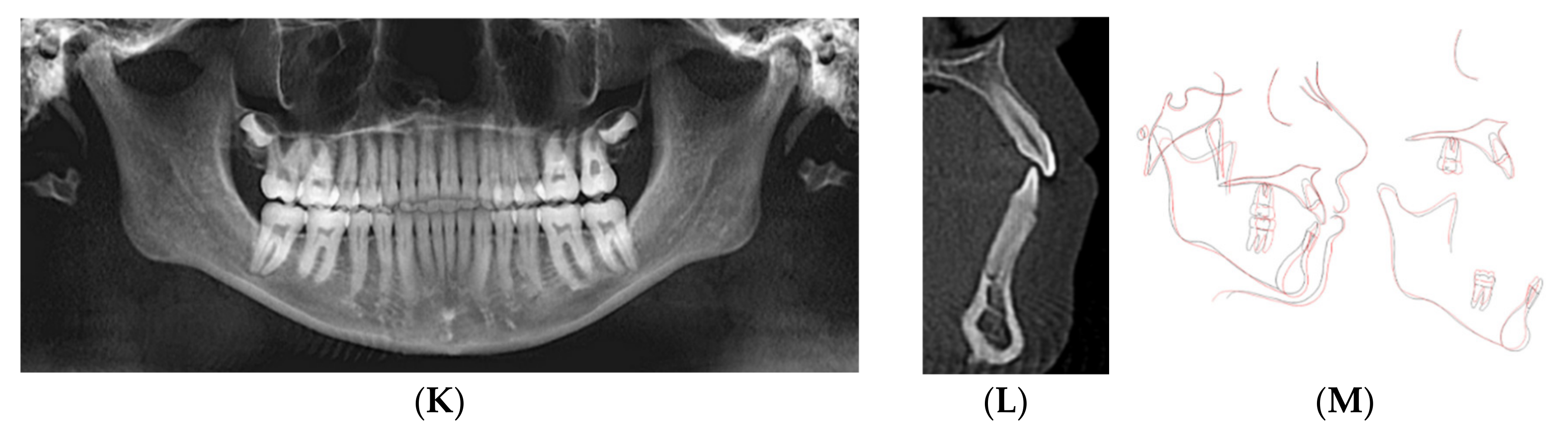
2.3. Case 3
2.4. Case 4
3. Results
4. Discussion
5. Conclusions
- The use of HFV concurrent with SmartTrack® Invisalign aligners and vertical-pull chin cup in this case series allowed achievement of complex tooth movement including posterior teeth intrusion and expansion simultaneously as well as forward mandibular rotation/projection in non-growing patients with a skeletal Class II relationship, which otherwise would have required surgery. These results should be confirmed with future larger samples size prospective controlled clinical trials.
- Although the improvement of patients’ profiles was not as ideal as could possibly achieved with surgical intervention, the achieved improvement was satisfactory to all patients/parents.
- The clinical impact and implications of this case series are that the use of HFV facilitates complex orthodontic tooth movement including posterior teeth intrusion and incisor decompensation in addition to increasing bone formation labial to lower incisors that may minimize future gum recession due to their labial inclination. Again, the presented results should be confirmed with future larger samples size prospective controlled clinical trials.
Funding
Acknowledgments
Conflicts of Interest
References
- Mummolo, S.; Nota, A.; Albani, F.; Marchetti, E.; Tecco, S. Salivary levels of Streptococcus mutans and Lactobacilli and other salivary indices in patients wearing clear aligners versus fixed orthodontic appliances: An observational study. PLoS ONE 2020, 15, e0228798. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Q.; Li, J.; Mei, L.; Du, J.; Li, H. Periodontal health during orthodontic treatment with clear aligners and fixed appliances: A meta-analysis. J. Am. Dent. Assoc. 2018, 149, 712–720. [Google Scholar]
- Wheeler, T.T.; Patel, N.; McGorray, S.P. Effect of aligner material on orthodontic tooth movement. J. Aligner. Orthod. 2017, 1, 21–27. [Google Scholar]
- Schott, T.C.; Göz, G. Color fading of the blue compliance indicator encapsulated in removable clear Invisalign Teen® aligners. Angle Orthod. 2011, 81, 185–191. [Google Scholar] [CrossRef] [PubMed]
- Crouse, J.M. Patient compliance with removable clear aligner therapy. J. Clin. Orthod. 2018, 52, 710–713. [Google Scholar] [PubMed]
- Giancotti, A.; Garino, F.; Mampieri, G. Use of clear aligners in open bite cases: An unexpected treatment option. J. Orthod. 2017, 44, 114–125. [Google Scholar] [CrossRef]
- Ojima, K.; Dan, C.; Kumagai, Y.; Schupp, W. Invisalign Treatment Accelerated by Photobiomodulation. J. Clin. Orthod. 2016, 50, 309–317. [Google Scholar]
- Ojima, K.; Dan, C.; Watanabe, H.; Kumagai, Y. Upper molar distalization with Invisalign treatment accelerated by photobiomodulation. J. Clin. Orthod. 2018, 52, 675–683. [Google Scholar]
- Taha, K.; Conley, R.S.; Arany, P.; Warunek, S.; Al-Jewair, T. Effects of mechanical vibrations on maxillary canine retraction and perceived pain: A pilot, single-center, randomized-controlled clinical trial. Odontology 2020, 108, 321–330. [Google Scholar] [CrossRef]
- Lo Giudice, A.; Nucera, R.; Perillo, L.; Paiusco, A.; Caccianiga, G. Is Low-Level Laser Therapy an Effective Method to Alleviate Pain Induced by Active Orthodontic Alignment Archwire? A Randomized Clinical Trial. J. Evid. Based Dent. Pract. 2019, 19, 71–78. [Google Scholar] [CrossRef]
- El-Bialy, T.; Farouk, K.; Carlyle, T.D.; Wiltshire, W.; Drummond, R.; Dumore, T.; Knowlton, K.; Tompson, B. Effect of Low Intensity Pulsed Ultrasound (LIPUS) on Tooth Movement and Root Resorption: A Prospective Multi-Center Randomized Controlled Trial. J. Clin. Med. 2020, 16, 804. [Google Scholar] [CrossRef]
- Yamaguchi, M.; Hayashi, M.; Fujita, S.; Yoshida, T.; Utsunomiya, T.; Yamamoto, H.; Kasai, K. Low-energy laser irradiation facilitates the velocity of tooth movement and the expressions of matrix metalloproteinase-9, cathepsin K, and alpha(v) beta(3) integrin in rats. Eur. J. Orthod. 2010, 32, 131–139. [Google Scholar] [CrossRef]
- Maurya, R.K.; Singh, H.; Kapoor, P.; Jain, U.; Mitra, R. Effects of low-level laser and low-intensity pulsed ultrasound therapy on treatment duration and pain perception. J. Clin. Orthod. 2019, 53, 154–162. [Google Scholar]
- Peter, M.; Nikolaos, P. AcceleDent Aura does not influence treatment duration or number of visits. Australas. Orthod. J. 2020, 36, 2–8. [Google Scholar]
- Alikhani, M.; Alansari, S.; Hamidaddin, M.A.; Sangsuwon, C.; Alyami, B.; Thirumoorthy, S.N.; Oliveira, S.M.; Nervina, J.M.; Teixeira, C.C. Vibration paradox in orthodontics: Anabolic and catabolic effects. PLoS ONE 2018, 13, e0196540. [Google Scholar] [CrossRef] [PubMed]
- Shipley, T. Effects of High Frequency Acceleration Device on Aligner Treatment—A Pilot Study. Dent. J. 2018, 6, 32. [Google Scholar] [CrossRef] [PubMed]
- Shipley, T.; Farouk, K.; El-Bialy, T. Effect of high-frequency vibration on orthodontic tooth movement and bone density. J. Orthod Sci. 2019, 8, 15. [Google Scholar] [PubMed]
- Alikhani, M.; Alikhani, M.; Alansari, S.; Almansour, A.; Hamidaddin, M.A.; Khoo, E.; Lopez, J.A.; Nervina, J.M.; Nho, J.Y.; Oliveira, S.M.; et al. Therapeutic effect of localized vibration on alveolar bone of osteoporotic rats. PLoS ONE 2019, 14, e0211004. [Google Scholar] [CrossRef] [PubMed]
- Alikhani, M.; Sangsuwon, C.; Alansari, S.; Nervina, J.M.; Teixeira, C.C. High Frequency Acceleration: A New Tool for Alveolar Bone Regeneration. JSM Dent. Surg. 2017, 2, 1026. [Google Scholar]
- Alikhani, M.; Lopez, J.A.; Alabdullah, H.; Vongthongleur, T.; Sangsuwon, C.; Alikhani, M.; Alansari, S.; Oliveira, S.M.; Nervina, J.M.; Teixeira, C.C. High-Frequency Acceleration: Therapeutic Tool to Preserve Bone following Tooth Extractions. J. Dent. Res. 2016, 95, 311–318. [Google Scholar] [CrossRef]
- Benjakul, S.; Jitpukdeebodintra, S.; Leethanakul, C. Effects of low magnitude high frequency mechanical vibration combined with compressive force on human periodontal ligament cells in vitro. Eur. J. Orthod. 2018, 40, 356–363. [Google Scholar] [CrossRef] [PubMed]
- Benjakul, S.; Leethanakul, C.; Jitpukdeebodintra, S. Low magnitude high frequency vibration induces RANKL via cyclooxygenase pathway in human periodontal ligament cells in vitro. J. Oral. Biol. Craniofac. Res. 2019, 9, 251–255. [Google Scholar] [CrossRef] [PubMed]
- Takano-Yamamoto, T.; Sasaki, K.; Fatemeh, G.; Fukunaga, T.; Seiryu, M.; Daimaruya, T.; Takeshita, N.; Kamioka, H.; Adachi, T.; Ida, H.; et al. Synergistic acceleration of experimental tooth movement by supplementary high-frequency vibration applied with a static force in rats. Sci. Rep. 2017, 7, 13969. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Li, J.; Zhang, L.; Zhou, Y.; Hou, W.; Quan, H.; Li, X.; Chen, Y.; Yu, H. Effects of mechanical vibration on proliferation and osteogenic differentiation of human periodontal ligament stem cells. Arch. Oral Biol. 2012, 57, 1395–1407. [Google Scholar] [CrossRef]
- Raposo, R.; Peleteiro, B.; Paço, M.; Pinho, T. Orthodontic camouflage versus orthodontic-orthognathic surgical treatment in class II malocclusion: A systematic review and meta-analysis. Int. J. Oral Maxillofac. Surg. 2018, 47, 445–455. [Google Scholar] [CrossRef]
- Daniels, S.; Brady, P.; Daniels, A.; Howes, S.; Shin, K.; Elangovan, S.; Allareddy, V. Comparison of surgical and non-surgical orthodontic treatment approaches on occlusal and cephalometric outcomes in patients with Class II Division I malocclusions. Prog. Orthod. 2017, 18, 16. [Google Scholar] [CrossRef]
- Schubert, A.; Jäger, F.; Maltha, J.C.; Bartzela, T.N. Age effect on orthodontic tooth movement rate and the composition of gingival crevicular fluid: A literature review. J. Orofac. Orthop. 2020, 81, 113–125. [Google Scholar] [CrossRef]
- El-Bialy, T. The Use of High Frequency Vibration and Clear Aligners in Management of an Adult Patient with Class III Skeletal Malocclusion with Open Bite and Severe Bimaxillary Protrusion: Case Report. Dent. J. 2020, 8, 75, Published 14 July 2020. [Google Scholar] [CrossRef]
- Pernet, F.; Vento, C.; Pandis, N.; Kiliaridis, S. Long-term evaluation of lower incisors gingival recessions after orthodontic treatment. Eur. J. Orthod. 2019, 15, 559–564. [Google Scholar] [CrossRef]
- Caruso, S.; Nota, A.; Ehsani, S.; Maddalone, E.; Ojima, K.; Tecco, S. Impact of molar teeth distalization with clear aligners on occlusal vertical dimension: A retrospective study. BMC Oral Health 2019, 13, 182. [Google Scholar] [CrossRef]
| Measurement | Initial | Final | Change/Variation from Initial Values | Normal |
|---|---|---|---|---|
| SNA (º) | 87.1 | 87.5 | 0.4 | 82 |
| SNB (º) | 79.3 | 82.5 | 3.2 | 80.9 |
| SN-MP (º) | 41.8 | 40 | −1.8 | 32.9 |
| FMA (MP-FH) (º) | 38.1 | 35.5 | −2.6 | 23.9 |
| ANB (º) | 7.9 | 5 | −2.9 | 1.6 |
| U1-NA (mm) | 0.5 | 1.3 | 0.8 | 4.3 |
| U1-SN (º) | 92 | 99 | 7 | 102.8 |
| L1-NB (mm) | 8.1 | 4.8 | −3.3 | 4 |
| L1-MP (º) | 90.4 | 88.6 | −1.8 | 95 |
| Lower Lip to E-Plane (mm) | 4.9 | 2.2 | −2.7 | −2 |
| Upper Lip to E-Plane (mm) | 4.3 | 0.7 | −3.6 | −6 |
| Nasolabial Angle (Col-Sn-UL) (º) | 107.4 | 109 | 1.6 | 102 |
| Facial Convexity (G’-Sn-Po’) (º) | 29.5 | 22.7 | −6.8 | 12 |
| Measurement | Initial | Final | Change/Variation from Initial Values | Norm |
|---|---|---|---|---|
| SNA (º) | 83.7 | 83.6 | −0.1 | 82 |
| SNB (º) | 74.7 | 76.3 | 2.4 | 80.9 |
| SN-MP (º) | 41.3 | 41 | 0.3 | 32.9 |
| FMA (MP-FH) (º) | 35.2 | 37.1 | 1.9 | 22.9 |
| ANB (º) | 9 | 7.3 | −1.7 | 1.6 |
| U1-NA (mm) | 5.9 | 3.5 | −2.4 | 4.3 |
| U1-SN (º) | 98.4 | 90.4 | 2 | 103.1 |
| L1-NB (mm) | 11.3 | 9.4 | −1.9 | 4 |
| L1-MP (º) | 99.2 | 88.2 | −11 | 95 |
| Lower Lip to E-Plane (mm) | 9.7 | 6.4 | −3.4 | -2 |
| Upper Lip to E-Plane (mm) | 7.1 | 3.2 | −3.9 | -8 |
| Nasolabial Angle (Col-Sn-UL) (º) | 104.3 | 107.2 | 2.9 | 102 |
| Facial Convexity (G’-Sn-Po’) (º) | 22.7 | 20.6 | −1.9 | 12 |
| Measurement | Initial | Final | Change/Variation from Initial Values | Norm |
|---|---|---|---|---|
| SNA (º) | 82.5 | 83.3 | 0.8 | 82 |
| SNB (º) | 74.1 | 76.7 | 1.4 | 80.9 |
| SN-GoGn (º) | 41.1 | 41.1 | 0 | 32.9 |
| FMA (MP-FH) (º) | 36.4 | 36.3 | −0.1 | 24.9 |
| ANB (º) | 8.4 | 6.7 | −1.4 | 1.6 |
| U1-NA (mm) | −1.8 | 0.7 | 2.5 | 4.3 |
| U1-SN (º) | 89.1 | 92.4 | 3.3 | 102.5 |
| L1-NB (mm) | 6.7 | 8.1 | 1.4 | 4 |
| L1-GoGn (º) | 95.2 | 87.5 | −7.7 | 93 |
| Lower Lip to E-Plane (mm) | 0.7 | 3.6 | 2.9 | -2 |
| Upper Lip to E-Plane (mm) | 0.8 | 0.8 | 0 | -3.9 |
| Nasolabial Angle (Col-Sn-UL) (º) | 105 | 105.6 | 0.6 | 102 |
| Facial Convexity (G’-Sn-Po’) (º) | 23.4 | 21.6 | −1.8 | 12 |
| Measurement | Initial | Final | Change/Variation from Initial Values | Norm |
|---|---|---|---|---|
| SNA (º) | 82.9 | 81.4 | −1.5 | 82 |
| SNB (º) | 78.5 | 79 | 0.5 | 80.9 |
| SN-MP (º) | 37.5 | 37.7 | 0.2 | 32.9 |
| FMA (MP-FH) (º) | 30.4 | 28.7 | −2.3 | 24 |
| ANB (º) | 4.5 | 2.4 | −2.1 | 1.6 |
| U1-NA (mm) | 4.2 | 5.7 | 1.5 | 4.3 |
| U1-SN (º) | 100.6 | 102.2 | 1.6 | 102.8 |
| L1-NB (mm) | 7.4 | 5.8 | −1.6 | 4 |
| L1-MP (º) | 84.9 | 81.8 | −3.1 | 95 |
| Lower Lip to E-Plane (mm) | 1.4 | 1 | −0.4 | −2 |
| Upper Lip to E-Plane (mm) | −2.7 | −0.9 | −1.6 | −5.7 |
| Nasolabial Angle (Col-Sn-UL) (º) | 111.2 | 107.2 | −3 | 102 |
| Facial Convexity (G’-Sn-Po’) (º) | 21.2 | 16.5 | −4.7 | 12 |
© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
El-Bialy, T. The Effect of High-Frequency Vibration on Tooth Movement and Alveolar Bone in Non-Growing Skeletal Class II High Angle Orthodontic Patients: Case Series. Dent. J. 2020, 8, 110. https://doi.org/10.3390/dj8040110
El-Bialy T. The Effect of High-Frequency Vibration on Tooth Movement and Alveolar Bone in Non-Growing Skeletal Class II High Angle Orthodontic Patients: Case Series. Dentistry Journal. 2020; 8(4):110. https://doi.org/10.3390/dj8040110
Chicago/Turabian StyleEl-Bialy, Tarek. 2020. "The Effect of High-Frequency Vibration on Tooth Movement and Alveolar Bone in Non-Growing Skeletal Class II High Angle Orthodontic Patients: Case Series" Dentistry Journal 8, no. 4: 110. https://doi.org/10.3390/dj8040110
APA StyleEl-Bialy, T. (2020). The Effect of High-Frequency Vibration on Tooth Movement and Alveolar Bone in Non-Growing Skeletal Class II High Angle Orthodontic Patients: Case Series. Dentistry Journal, 8(4), 110. https://doi.org/10.3390/dj8040110





