Implementing an Oral Health Intervention for People Experiencing Homelessness in Scotland: A Participant Observation Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample and Recruitment
2.2. Ethical Considerations
2.3. Data Collection
2.4. Data Analysis
3. Results
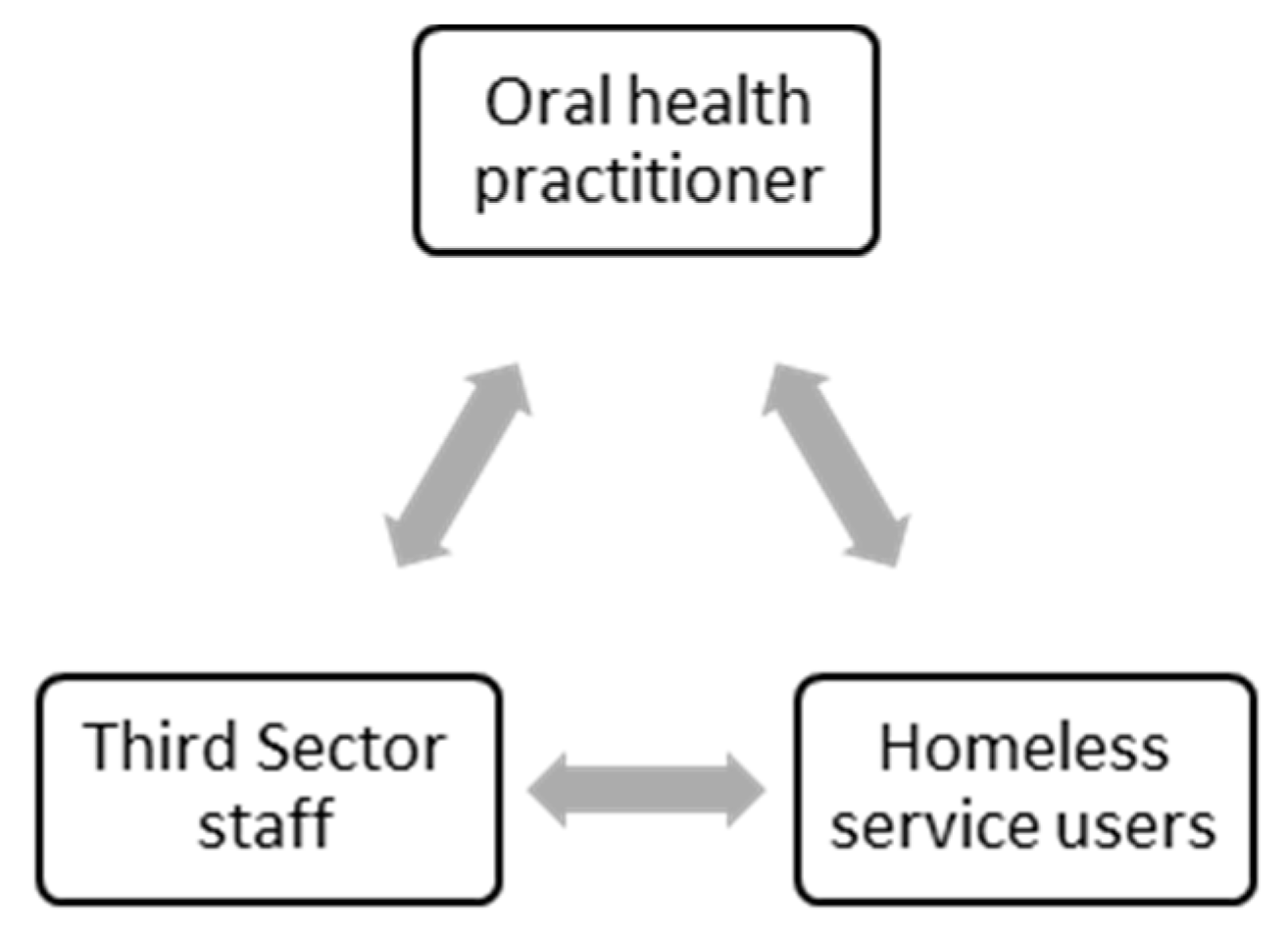
3.1. Alliance 1: Oral Health Practitioner and Service User
3.1.1. Barriers
“Practitioner 4 would go up to tables with men having breakfast and say who she was and why she was there, but just to make them aware—it was up to the individuals to approach her if they wanted to”(Observation 8)
“We were put in the medical room along the corridor from the office, but there was no opportunity for Practitioner 4 to approach any of the residents. We only saw service users if they specifically wanted to talk about their oral health or if they had walked past the room and wanted to see who we were.”(Observation 9)
“When I was there today two service users opened the MDU door from the outside and barged in”(Observation 3)
“When I arrived there were two women outside the front door (of the MDU) shouting.”(Observation 4)
3.1.2. Enablers
“Working in the mobile dental unit would not be for everyone—you need to be confident and thick-skinned”(Observation 3)
“Practitioner 1 is confident and appears quite fearless, putting up with language/behaviour that would not be tolerated in a normal clinic.”(Observation 6)
“I get the impression that Practitioner 4 and the other practitioners I have observed… do not see the risk involved in their job, or they just see it as part of the job… it is also possible that after a while doing this kind of work they stop seeing it as risky”(Observation 9)
“The dental team spoke about how they felt that working in the MDU would not suit everyone”(Observation 3)
“I believe that not everyone is suited to doing Practitioner 1’s job—personality aside, you need to be fast-thinking, tough-skinned, a bit fearless, and approachable.”(Observation 6)
“Practitioner 1 is very experienced and upfront with all service users—not visibly fazed by service users’ admissions or behaviours”(Observation 1)
“The MDU dentist admitted that she is aware that she acts differently with patients in the MDU than she would with regular patients—she is not as formal, more likely to speak to them in the same way they speak to her… she is quite matter-of-fact”(Observation 3)
“When a service user said he found it difficult to stop smoking, Practitioner 1 admitted that she was an ex-smoker, and explained that she still feels tempted”(Observation 1)
“To me it seems that Practitioner 4 goes above and beyond for the service users she sees. She will offer to phone and make appointments, sends them reminders the day before (even on her day off) and she will even take them to an appointment. It’s clear that she cares if they attend or not—she mentioned that she has asked some practices to waive fines, and clearly advocates for the service users when necessary.”(Observation 8)
“Practitioner 1 would take the time to find free samples that would be specific to the service user, e.g., Corsodyl toothpaste for people with bleeding gums, or denture care items”(Observation 1)
3.2. Alliance 2: Oral Health Practitioners and Third Sector Staff
3.2.1. Barriers
“Practitioner 3 did not really interact with service users beyond telling them if they can be seen by the dentist, or making general conversation. She would encourage people to wait in the drop-in rather than in the MDU before their treatment”(Observation 3)
“The oral health team do not seem bothered to recruit any patients, even if that means sitting waiting with nothing to do—the feeling seems to be that if a patient wants to be seen then they will come to the MDU.”(Observation 4)
“In all three establishments today, staff did not seem well prepared for Practitioner 2’s visit—her poster was only displayed in one of them, and they had not spoken to their service users about her visit…In one place, the room we were offered was in the staff area, so there would never be any passing service users”(Observation 2)
3.2.2. Enablers
“it is clear that Practitioner 1 works hard at maintaining strong relationships with staff at these locations… she makes a point of visiting every 6 weeks and reminds them the day before that she will be visiting.”(Observation 1)
“Practitioner 1 clearly has a good relationship with the staff… she told me that ‘keeping the staff sweet’ is a major part of her role and really helps with building rapport”(Observation 7)
3.3. Alliance 3: Third Sector Staff and Service Users
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Somerville, P. Understanding homelessness. Hous. Theory Soc. 2013, 30, 384–415. [Google Scholar] [CrossRef]
- Collins, J. Characterising Homeless People in Scotland: Can Oral Health, Health and Psychosocial Wellbeing Enhance the ETHOS Typology of Homelessness. Ph.D. Thesis, University of Dundee, Dundee, Scotland, 2012. [Google Scholar]
- Scottish Government. Homelessness in Scotland: 2015–16; Scottish Government: Edinburgh, Scotland, 2016.
- Fitzpatrick, S.; Johnsen, S.; White, M. Multiple Exclusion Homelessness in the UK: Key patterns and intersections. Soc. Policy Soc. 2011, 10, 501–512. [Google Scholar] [CrossRef]
- Collins, J.; Freeman, R. Homeless in North and West Belfast: An oral health needs assessment. Br. Dent. J. 2007, 202, E31. [Google Scholar] [CrossRef] [PubMed]
- Chi, D.; Milgrom, P. The oral health of homeless adolescents and young adults and determinants of oral health: Preliminary findings. Spec. Care Dent. 2008, 28, 237–242. [Google Scholar] [CrossRef] [PubMed]
- Figueiredo, R.L.F.; Hwang, S.W.; Quiñonez, C. Dental health of homeless adults in Toronto, Canada. J. Public Health Dent. 2013, 73, 74–78. [Google Scholar] [CrossRef] [PubMed]
- NHS Health Scotland. Inequality Briefing: Health and Homelessness; NHS Health Scotland: Edinburgh, Scotland, 2016. [Google Scholar]
- Groundswell. Healthy Mouths: A Peer-Led Health Audit on the Oral Health of People Experiencing Homelessness; Groundswell: London, UK, 2017. [Google Scholar]
- Scottish Executive. Health and Homelessness Standards; Scottish Executive: Edinburgh, Scotland, 2005. [Google Scholar]
- Scottish Executive. An Action Plan for Improving Oral Health and Modernising NHS Dental Services; Scottish Executive: Edinburgh, Scotland, 2005. [Google Scholar]
- NHS Principles and Values. Available online: https://www.nhs.uk/using-the-nhs/about-the-nhs/principles-and-values/ (accessed on 31 October 2018).
- Wanyonyi, K.L.; Themessl-Huber, M.; Humphris, G.; Freeman, R. A systematic review of meta-analysis of face-to-face communication of tailored health messages: Implications for practice. Patient Educ. Couns. 2011, 85, 348–355. [Google Scholar] [CrossRef] [PubMed]
- Scottish Government. National Oral Health Improvement Strategy for Priority Groups; Scottish Government: Edinburgh, Scotland, 2012.
- Coles, E.; Edwards, M.; Elliott, G.; Heffernan, A.; Moore, A.; Freeman, R. Smile4life: The Oral Health of Homeless People in Scotland; University of Dundee: Dundee, Scotland, 2011. [Google Scholar]
- Freeman, R.; Coles, E.; Watt, C.; Edwards, M.; Jones, C. Smile4life Guide for Trainers: Better Oral Care for Homeless People; NHS Health Scotland: Edinburgh, Scotland, 2012. [Google Scholar]
- Beaton, L.; Freeman, R. Oral health promotion and homelessness: A theory-based approach to understanding processes of implementation and adoption. Health Educ. J. 2016, 75, 184–197. [Google Scholar] [CrossRef]
- Mays, N.; Pope, C. Observational methods in health care settings. Br. Med. J. 1995, 311, 182–184. [Google Scholar] [CrossRef]
- Ekins, R. Male Femaling: A Grounded Theory Approach to Cross-Dressing and Sex Changing; Routledge: London, UK, 1997; ISBN 0415106249. [Google Scholar]
- Scottish Government. Operation of the Homeless Persons Legislation in Scotland; Scottish Government: Edinburgh, Scotland, 2015.
- Taylor-Powell, E.; Steele, S. Collecting Evaluation Data: Direct Observation. Programme Development and Evaluation; Cooperative Extension Publications: Madison, WI, USA, 1996. [Google Scholar]
- Zhao, M.; Ji, Y. Challenges of introducing participant observation to community health research. ISRN Nurs. 2014. [Google Scholar] [CrossRef] [PubMed]
- Jorgensen, D.L. Participant Observation: A methodology for Human Studies; SAGE Publications Inc.: Thousand Oaks, CA, USA, 1989; ISBN 0803928777. [Google Scholar]
- Elo, S.; Kyngäs, H. The qualitative content analysis process. J. Adv. Nurs. 2008, 62, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Silverman, D. Interpreting Qualitative Data, 4th ed.; SAGE Publications Ltd.: London, UK, 2011; ISBN 0857024213. [Google Scholar]
- Birks, M.; Chapman, Y.; Francis, K. Memoing in qualitative research: Probing data and processes. J. Res. Nurs. 2008, 13, 68–75. [Google Scholar] [CrossRef]
- Mayring, P. Qualitative Content Analysis. Forum Qual. Soc. Res. 2000, 1, 20. [Google Scholar]
- Bordin, E.S. The generalisability of the psychoanalytic concept of the working alliance. Psychother. Theory Res. Pract. 1979, 16, 252–260. [Google Scholar] [CrossRef]
- Hill, L.B.; McGrath, J.M. Communication within the triadic context: Intercultural prospects. Intercult. Commun. Stud. 2008, 17, 52–67. [Google Scholar]
- Simmel, G. The Sociology of Georg Simmel; Wolff, K.H., Translator; Wolff, K.H., Ed.; Free Press: New York, NY, USA, 1950; ISBN 1296031292. [Google Scholar]
- Caplow, T. Further development of a theory of coalitions in the triad. Am. J. Sociol. 1959, 64, 488–493. [Google Scholar] [CrossRef]
- Mills, T.M. Power relations in three-person groups. Am. Sociol. Rev. 1953, 18, 351–357. [Google Scholar] [CrossRef]
- Robinson, D.T.; Brown, D.G.; Parker, D.C.; Schreinemachers, P.; Janssen, M.A.; Huigen, M.; Wittmer, H.; Gotts, N.; Promburom, P.; Irwins, E.; et al. Comparison of empirical methods for building agent-based models in land use science. J. Land Use Sci. 2007, 2, 31–55. [Google Scholar] [CrossRef]
| Observation | Location | Services Visited | Setting |
|---|---|---|---|
| Observation 1 | Board 2 | 3 supported accommodation establishments (1 h each) | Shared living room Meeting room |
| Observation 2 | Board 2 | An accommodation for young men (1 h) A long-term accommodation for families and individuals (1 h) A short-term accommodation for young people (1 h) | Kitchen Meeting room Shared living room |
| Observation 3 | Board 1 | Mobile dental unit at a drop-in service (2 h) | Mobile dental unit waiting area |
| Observation 4 | Board 1 | Mobile dental unit at a harm reduction service for young people (1 h 30 min) | Mobile dental unit waiting area |
| Observation 5 | Board 1 | Mobile dental unit at a harm reduction service for young people (1 h 30 min) | Mobile dental unit waiting area |
| Observation 6 | Board 2 | Drop-in service providing hot meals (3 h) | Canteen |
| Observation 7 | Board 2 | A space for families and friend of prisoners to wait before entering the prison (4 h 30 min) | Visitor centre |
| Observation 8 | Board 3 | An emergency accommodation for women (1 h) A support and drop-in service (1 h 45 min) An emergency accommodation for men (2 h) | Canteen Reception area |
| Observation 9 | Board 3 | A homeless assessment centre and short-term accommodation (2 h) Supported long-term accommodation for women (1 h) | Medical room Service user’s flat |
| Practitioner Number | Board | Job Title | Gender |
|---|---|---|---|
| Practitioner 3 | Board 1 | Dental Health Support Worker | Female |
| Practitioner 1 | Board 2 | Oral Health Educator | Female |
| Practitioner 2 | Board 2 | Oral Health Educator | Female |
| Practitioner 4 | Board 3 | Dental Health Support Worker | Female |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Beaton, L.; Anderson, I.; Humphris, G.; Rodriguez, A.; Freeman, R. Implementing an Oral Health Intervention for People Experiencing Homelessness in Scotland: A Participant Observation Study. Dent. J. 2018, 6, 68. https://doi.org/10.3390/dj6040068
Beaton L, Anderson I, Humphris G, Rodriguez A, Freeman R. Implementing an Oral Health Intervention for People Experiencing Homelessness in Scotland: A Participant Observation Study. Dentistry Journal. 2018; 6(4):68. https://doi.org/10.3390/dj6040068
Chicago/Turabian StyleBeaton, Laura, Isobel Anderson, Gerry Humphris, Andrea Rodriguez, and Ruth Freeman. 2018. "Implementing an Oral Health Intervention for People Experiencing Homelessness in Scotland: A Participant Observation Study" Dentistry Journal 6, no. 4: 68. https://doi.org/10.3390/dj6040068
APA StyleBeaton, L., Anderson, I., Humphris, G., Rodriguez, A., & Freeman, R. (2018). Implementing an Oral Health Intervention for People Experiencing Homelessness in Scotland: A Participant Observation Study. Dentistry Journal, 6(4), 68. https://doi.org/10.3390/dj6040068






