Climate Change Perception and Mental Health. Results from a Systematic Review of the Literature
Abstract
1. Introduction
2. Materials and Methods
2.1. Literature Search
2.2. Inclusion/Exclusion Criteria and Selection Process
2.3. Data Extraction and Quality Assessment
3. Results
3.1. Literature Search
3.2. Main Characteristics of Included Studies
3.3. Main Characteristics of Included Population
3.4. Mental Health Outcomes
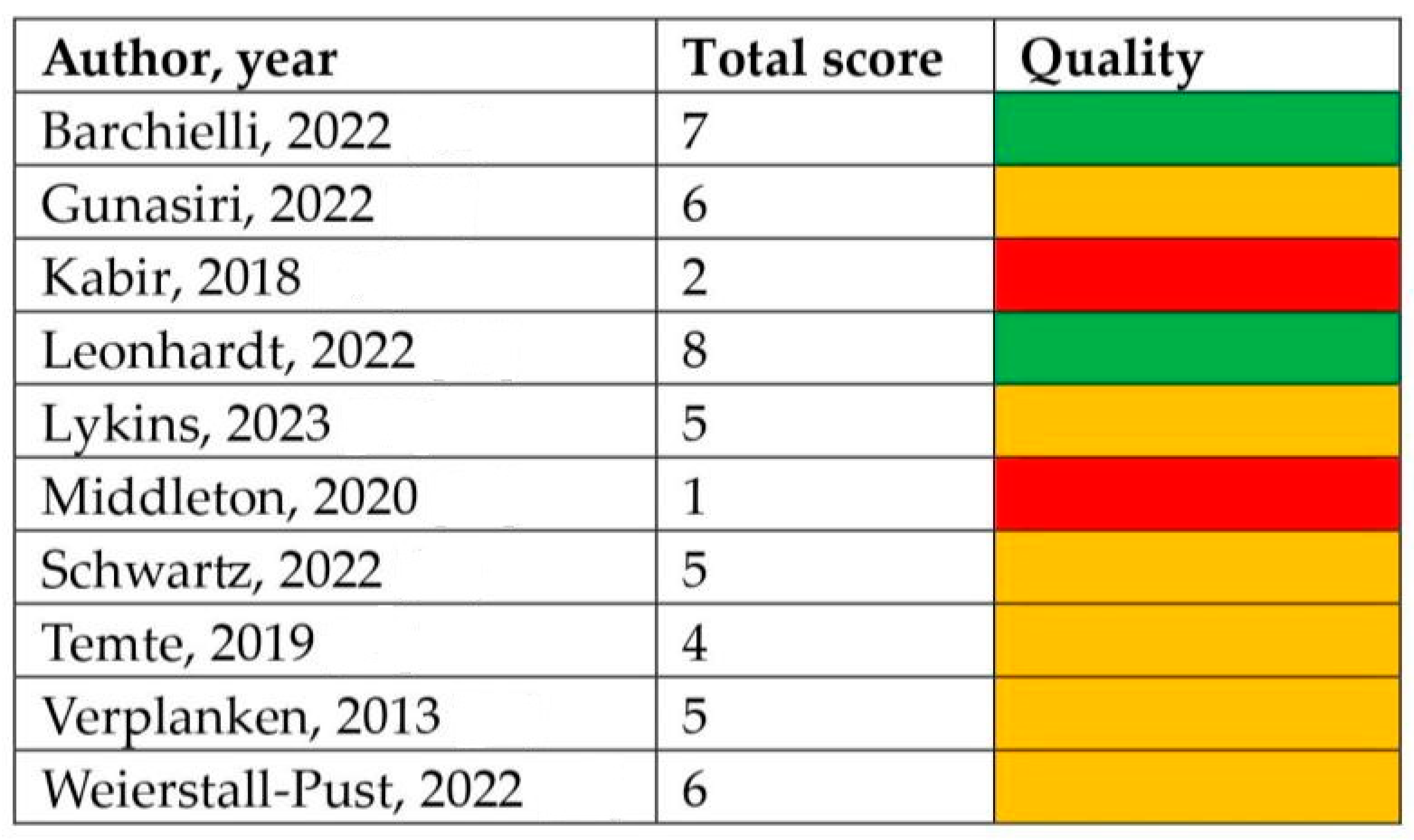
3.5. Quality Assessment of Included Studies
4. Discussion
4.1. Potential Biological Mechanisms
4.2. Limitations and Strengths
4.3. Implications for Public Health Policies and Future Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Barrett, B.; Charles, J.W.; Temte, J.L. Climate change, human health, and epidemiological transition. Prev. Med. 2015, 70, 69–75. [Google Scholar] [CrossRef]
- Neira, M.; Erguler, K.; Ahmady-Birgani, H.; Al-Hmoud, N.D.; Fears, R.; Gogos, C.; Hobbhahn, N.; Koliou, M.; Kostrikis, L.G.; Lelieveld, J.; et al. Climate change and human health in the Eastern Mediterranean and Middle East: Literature review, research priorities and policy suggestions. Environ. Res. 2023, 216 Pt 2, 114537. [Google Scholar] [CrossRef]
- Knowlton, K.; Rotkin-Ellman, M.; Geballe, L.; Max, W.; Solomon, G.M. Six climate change-related events in the United States accounted for about $14 billion in lost lives and health costs. Health Aff. 2011, 30, 2167–2176. [Google Scholar] [CrossRef] [PubMed]
- Ebi, K.L.; Hess, J.J.; Watkiss, P. Health Risks and Costs of Climate Variability and Change. In Injury Prevention and Environmental Health; Mock, C.N., Nugent, R., Kobusingye, O., Smith, K.R., Eds.; The International Bank for Reconstruction and Development/The World Bank: Washington, DC, USA, 2017. [Google Scholar]
- Panel on Climate Change. Sixth Assessment Report (AR6) on Climate Change. Interlaken, Switzerland 2023. Available online: https://www.ipcc.ch/report/sixth-assessment-report-cycle/ (accessed on 30 October 2023).
- Van de Vuurst, P.; Escobar, L.E. Climate change and infectious disease: A review of evidence and research trends. Infect. Dis. Poverty 2023, 12, 51. [Google Scholar] [CrossRef]
- Rupasinghe, R.; Chomel, B.B.; Martinez-Lopez, B. Climate change and zoonoses: A review of the current status, knowledge gaps, and future trends. Acta Trop. 2022, 226, 106225. [Google Scholar] [CrossRef] [PubMed]
- Myers, S.; Fanzo, J.; Wiebe, K.; Huybers, P.; Smith, M. Current guidance underestimates risk of global environmental change to food security. BMJ 2022, 378, e071533. [Google Scholar] [CrossRef] [PubMed]
- Duchenne-Moutien, R.A.; Neetoo, H. Climate Change and Emerging Food Safety Issues: A Review. J. Food Prot. 2021, 84, 1884–1897. [Google Scholar] [CrossRef]
- Klingelhofer, D.; Braun, M.; Bruggmann, D.; Groneberg, D.A. Heatwaves: Does global research reflect the growing threat in the light of climate change? Glob. Health 2023, 19, 56. [Google Scholar] [CrossRef]
- World Health Organization. Heatwaves. 2021. Available online: https://www.who.int/health-topics/heatwaves#tab=tab_1 (accessed on 1 September 2023).
- Li, Y.; Cao, G.Y.; Jing, W.Z.; Liu, J.; Liu, M. Global trends and regional differences in incidence and mortality of cardiovascular disease, 1990–2019: Findings from 2019 global burden of disease study. Eur. J. Prev. Cardiol. 2023, 30, 276–286. [Google Scholar] [CrossRef]
- Schwerdtle, P.; Bowen, K.; McMichael, C. The health impacts of climate-related migration. BMC Med. 2017, 16, 1. [Google Scholar] [CrossRef]
- Rory, W. Global warming is more harmful for people with respiratory problems, warns specialist society. BMJ 2009, 339, b3530. [Google Scholar] [CrossRef]
- Cianconi, P.; Hanife, B.; Hirsch, D.; Janiri, L. Is climate change affecting mental health of urban populations? Curr. Opin. Psychiatry 2023, 36, 213–218. [Google Scholar] [CrossRef] [PubMed]
- Crane, K.; Li, L.; Subramanian, P.; Rovit, E.; Liu, J. Climate Change and Mental Health: A Review of Empirical Evidence, Mechanisms and Implications. Atmosphere 2022, 13, 2096. [Google Scholar] [CrossRef] [PubMed]
- Galway, L.P.; Beery, T.; Jones-Casey, K.; Tasala, K. Mapping the Solastalgia Literature: A Scoping Review Study. Int. J. Environ. Res. Public Health 2019, 16, 2662. [Google Scholar] [CrossRef]
- Knight, V. ‘Climate Grief’: Fears about the Planet’s Future Weigh on Americans’ Mental Health. KFF Health News. 2019. Available online: https://kffhealthnews.org/news/climate-grief-fears-about-the-planets-future-weigh-on-americans-mental-health/ (accessed on 31 October 2023).
- White, B.P.; Breakey, S.; Brown, M.J.; Smith, J.R.; Tarbet, A.; Nicholas, P.K.; Ros, A.M.V. Mental Health Impacts of Climate Change Among Vulnerable Populations Globally: An Integrative Review. Ann. Glob. Health 2023, 89, 66. [Google Scholar] [CrossRef]
- Thompson, R.; Lawrance, E.L.; Roberts, L.F.; Grailey, K.; Ashrafian, H.; Maheswaran, H.; Toledano, M.B.; Darzi, A. Ambient temperature and mental health: A systematic review and meta-analysis. Lancet Planet. Health 2023, 7, e580–e589. [Google Scholar] [CrossRef]
- Higgins, J.P.; Altman, D.G.; Gotzsche, P.C.; Juni, P.; Moher, D.; Oxman, A.D.; Savovic, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.C.; et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, d5928. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Wells, G.A.; Shea, B.; O’Connell, D.; Paterson, J.; Welch, V.; Losos, M.P.T. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomised Studies in Meta-Analyses the Ottawa Hospital, Ottawa, Canada. 2014. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 15 November 2018).
- Herzog, R.; Alvarez-Pasquin, M.J.; Diaz, C.; Del Barrio, J.L.; Estrada, J.M.; Gil, A. Are healthcare workers’ intentions to vaccinate related to their knowledge, beliefs and attitudes? A systematic review. BMC Public Health 2013, 13, 154. [Google Scholar] [CrossRef]
- Nucci, D.; Nardi, M.; Cinnirella, A.; Campagnoli, E.; Maffeo, M.; Perrone, P.M.; Shishmintseva, V.; Grosso, F.M.; Castrofino, A.; Castaldi, S.; et al. Adherence to Mediterranean Diet and Risk of Pancreatic Cancer: Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2023, 20, 2403. [Google Scholar] [CrossRef]
- Verplanken, B.; Roy, D. “My Worries Are Rational, Climate Change Is Not”: Habitual Ecological Worrying Is an Adaptive Response. PLoS ONE 2013, 8, e74708. [Google Scholar] [CrossRef] [PubMed]
- Weierstall-Pust, R.; Schnell, T.; Heßmann, P.; Feld, M.; Höfer, M.; Plate, A.; Müller, M.J. Stressors related to the COVID-19 pandemic, climate change, and the Ukraine crisis, and their impact on stress symptoms in Germany: Analysis of cross-sectional survey data. BMC Public Health 2022, 22, 2233. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, S.E.O.; Benoit, L.; Clayton, S.; Parnes, M.F.; Swenson, L.; Lowe, S.R. Climate change anxiety and mental health: Environmental activism as buffer. Curr. Psychol. 2022, 42, 16708–16721. [Google Scholar] [CrossRef] [PubMed]
- Temte, J.L.; Holzhauer, J.R.; Kushner, K.P. Correlation between climate change and dysphoria in primary care. Wis. Med. J. 2019, 118, 71–74. [Google Scholar]
- Leonhardt, M.; Granrud, M.D.; Bonsaksen, T.; Lien, L. Associations between Mental Health, Lifestyle Factors and Worries about Climate Change in Norwegian Adolescents. Int. J. Environ. Res. Public Health 2022, 19, 12826. [Google Scholar] [CrossRef]
- Barchielli, B.; Cricenti, C.; Gallè, F.; Sabella, E.A.; Liguori, F.; Da Molin, G.; Liguori, G.; Orsi, G.B.; Giannini, A.M.; Ferracuti, S.; et al. Climate Changes, Natural Resources Depletion, COVID-19 Pandemic, and Russian-Ukrainian War: What Is the Impact on Habits Change and Mental Health? Int. J. Environ. Res. Public Health 2022, 19, 11929. [Google Scholar] [CrossRef] [PubMed]
- Gunasiri, H.; Wang, Y.; Watkins, E.M.; Capetola, T.; Henderson-Wilson, C.; Patrick, R. Hope, Coping and Eco-Anxiety: Young People’s Mental Health in a Climate-Impacted Australia. Int. J. Environ. Res. Public Health 2022, 19, 5528. [Google Scholar] [CrossRef]
- Lykins, A.D.; Parsons, M.; Craig, B.M.; Cosh, S.M.; Hine, D.W.; Murray, C. Australian Youth Mental Health and Climate Change Concern After the Black Summer Bushfires. EcoHealth 2023, 20, 3–8. [Google Scholar] [CrossRef]
- Middleton, J.; Cunsolo, A.; Jones-Bitton, A.; Shiwak, I.; Wood, M.; Pollock, N.; Flowers, C.; Harper, S.L. “We’re people of the snow”: Weather, climate change, and Inuit mental wellness. Soc. Sci. Med. 2020, 262, 113137. [Google Scholar] [CrossRef]
- Kabir, S.M.S. Psychological health challenges of the hill-tracts region for climate change in Bangladesh. Asian J. Psychiatry 2018, 34, 74–77. [Google Scholar] [CrossRef]
- World Health Organization. Climate Change and Health. 2023. Available online: https://www.who.int/news-room/fact-sheets/detail/climate-change-and-health (accessed on 29 September 2023).
- Kuehn, B.M. WHO: Pandemic Sparked a Push for Global Mental Health Transformation. JAMA 2022, 328, 5–7. [Google Scholar] [CrossRef] [PubMed]
- Coffey, Y.; Bhullar, N.; Durkin, J.; Islam, M.S.; Usher, K. Understanding Eco-anxiety: A Systematic Scoping Review of Current Literature and Identified Knowledge Gaps. J. Clim. Chang. Health 2021, 3, 100047. [Google Scholar] [CrossRef]
- Bourban, M. Eco-Anxiety and the Responses of Ecological Citizenship and Mindfulness. In The Palgrave Handbook of Environmental Politics and Theory; Kassiola, J.J., Luke, T.W., Eds.; Springer International Publishing: Cham, Switzerland, 2023; pp. 65–88. [Google Scholar]
- Hayes, K.; Poland, B. Addressing Mental Health in a Changing Climate: Incorporating Mental Health Indicators into Climate Change and Health Vulnerability and Adaptation Assessments. Int. J. Environ. Res. Public Health 2018, 15, 1806. [Google Scholar] [CrossRef]
- Cicchetti, D. Resilience under conditions of extreme stress: A multilevel perspective. World Psychiatry 2010, 9, 145–154. [Google Scholar] [CrossRef] [PubMed]
- Maibach, E.W.; Nisbet, M.; Baldwin, P.; Akerlof, K.; Diao, G. Reframing climate change as a public health issue: An exploratory study of public reactions. BMC Public Health 2010, 10, 299. [Google Scholar] [CrossRef] [PubMed]
- Jelin, E. Towards a Global Environmental Citizenship? Citizsh. Stud. 2000, 4, 47–63. [Google Scholar] [CrossRef]
- Doherty, T.J.; Clayton, S.J.A.P. The psychological impacts of global climate change. Am. Psychol. 2011, 66, 265. [Google Scholar] [CrossRef]
- Cianconi, P.; Betro, S.; Janiri, L. The Impact of Climate Change on Mental Health: A Systematic Descriptive Review. Front. Psychiatry 2020, 11, 74. [Google Scholar] [CrossRef]
- Hayes, K.; Blashki, G.; Wiseman, J.; Burke, S.; Reifels, L. Climate change and mental health: Risks, impacts and priority actions. Int. J. Ment. Health Syst. 2018, 12, 28. [Google Scholar] [CrossRef]
- Abbass, K.; Qasim, M.Z.; Song, H.; Murshed, M.; Mahmood, H.; Younis, I. A review of the global climate change impacts, adaptation, and sustainable mitigation measures. Environ. Sci. Pollut. Res. Int. 2022, 29, 42539–42559. [Google Scholar] [CrossRef]
- Gianfredi, V.; Buffoli, M.; Rebecchi, A.; Croci, R.; Oradini-Alacreu, A.; Stirparo, G.; Marino, A.; Odone, A.; Capolongo, S.; Signorelli, C. Association between Urban Greenspace and Health: A Systematic Review of Literature. Int. J. Environ. Res. Public Health 2021, 18, 5137. [Google Scholar] [CrossRef] [PubMed]

| Author, Year [Ref] | Country | Study Period | Study Design | Sample Size | Attrition | Population Characteristics | Climate Change Assessment | Validation | MH Outcome | Diagnostic Assessment | Effect Size (95% CI) p-Value |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Barchielli, 2022 [31] | IT | n.a. | C-S | 1831 | n.a. | Access to electronic devices and internet connection; age 47.71; F 61% | 4-item 5-point Likert scale of an ad hoc questionnaire | Yes | Dep, Anx, and stress | DASS-21 | Climate change preoccupation was correlated with Dep and Anx in all age groups and with Anx among young adults and adults (Pearson ranged between 0.100 and 0.391, p < 0.01.) |
| Gunasiri, 2022 [32] | AU | 13 July–3 August 2020 | C-S | 46 | 0 | Young people living in Australia; age 18–24; sex n.s. | Survey developed ad hoc | Yes | Worry about the future, eco-anxiety, stress, and Anx | Survey developed ad hoc | Worry about the future 93%; eco anxiety 89%; stress and anxiety 83% |
| Kabir, 2018 [35] | BD | January 2015–October 2016 | C-S | 125 | n.a. | High-variety background; age 10–70; F 75, M 50 | Semi-structured interview | No | Feelings of loss and feelings of suicide ideation | Semi-structured interview | 75% of participants stated that climate change impacted daily activities and led to feelings of loss, thereby increasing feelings of suicide ideation. |
| Leonhardt, 2022 [30] | NO | 2021 | C-S | 128,484 | 11,357 | Pupils; age 13–19; F: 60,959 | Single 5-point Likert scale questionnaire | No | DepSym and well-being | DMI derived from the HSCCW | DepSym: OR 1.71 (1.10–1.42) well-being: OR 0.91 (0.88–0.95) |
| Lykins, 2023 [33] | AU | March 2020 | C-S | 746 | n.a. | Adolescents, young adults; age 16–25; F: 584, M: 152, 10 others | ETSEAI | Yes | Dep, Anx, stress, adjustment disorder, substance use, resilience | DASS-21; ADNM8, UNCOPE, BRS | Dep (r = 0.15, p < 0.001); Anx (r = 0.11, p < 0.01); stress (r = 0.19, p < 0.001); adjustment disorder (r = 0.21, p < 0.001); substance use (r = 0.10, p > 0.05); resilience (r = −0.14, p < 0.001) |
| Middleton, 2020 [34] | CA | November 2012–May 2013 | C-S | 116 | n.a. | 96 community members + 20 health professionals; 68 F, 48 M | Semi-structured interview | No | Mental well-being | Semi-structured interview | Climate change impacts environmental conditions, which in turn determines daily activities, indirectly affecting mental well-being. |
| Schwartz, 2022 [28] | USA | October and December 2020 | C-S | 323 | 12% (284/323 provided completed data on all variables) | Students; age 18–35; F 78.9%; transgender, non-binary, or other 2.1% | 3-item 5-point Likert scale for climate change experience and 13-item Climate Change Anxiety Scale | Yes | Cognitive and functional impairment in CCA, MDD, GAD | PHQ-8 for MDD, GAD-7 | MDD β = 0.11 (0.36), p > 0.05; cognitive impairment β = 1.53 (0.76), p < 0.05; GAD β = 0.37 (0.34), p > 0.05; functional impairment β = 1.85 (0.72), p < 0.05 |
| Temte, 2019 [29] | USA | 2013 | C-S | 571 | n.a. | Adult primary care patients; age 18–96; M 183, F 357 | Climate change composite score | No | Dep, Anx, and dysphoria | PHQ-9, GAD-7, and a combination of PHQ-9 and GAD-7 | Dep (Chi-square = 0.178, n.s.) and Anx (Chi-square = 0.441, n.s.), dysphoria: r = 0.345, p < 0.001) |
| Verplanken, 2013 [26] | USA and EU | June 2012–July 2012 | C-S | 132 | n.a. | Students and non-students; age 26; 39 M, 78 F, 15 not declared | 5-item 5-point Likert scale | Yes | Ecological worries, including global warming, pollution, extinction of species, resource depletion, and deforestation | PSWQ for item “pathological worry,” B5I for item “big five personality traits,” EAI for item “enviromental attitudes” | Habitual ecological worry and environmental attitudes (r = 0.47; p < 0.001), pro-environmental behavior (r = 0.37; p < 0.001) |
| Weierstall-Pust, 2022 [27] | DE | April–May 2022 | C-S | 3094 | n.a. | Adults (≥ 18 years) with fluent German and access to internet; F = 1560 M = 1534 | 5 items 5-point Likert scale climate change stressors | Yes | Stress symptoms | SSQ-25 | β = 0.06 (0.03) p < 0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gianfredi, V.; Mazziotta, F.; Clerici, G.; Astorri, E.; Oliani, F.; Cappellina, M.; Catalini, A.; Dell’Osso, B.M.; Pregliasco, F.E.; Castaldi, S.; et al. Climate Change Perception and Mental Health. Results from a Systematic Review of the Literature. Eur. J. Investig. Health Psychol. Educ. 2024, 14, 215-229. https://doi.org/10.3390/ejihpe14010014
Gianfredi V, Mazziotta F, Clerici G, Astorri E, Oliani F, Cappellina M, Catalini A, Dell’Osso BM, Pregliasco FE, Castaldi S, et al. Climate Change Perception and Mental Health. Results from a Systematic Review of the Literature. European Journal of Investigation in Health, Psychology and Education. 2024; 14(1):215-229. https://doi.org/10.3390/ejihpe14010014
Chicago/Turabian StyleGianfredi, Vincenza, Francesco Mazziotta, Giovanna Clerici, Elisa Astorri, Francesco Oliani, Martina Cappellina, Alessandro Catalini, Bernardo Maria Dell’Osso, Fabrizio Ernesto Pregliasco, Silvana Castaldi, and et al. 2024. "Climate Change Perception and Mental Health. Results from a Systematic Review of the Literature" European Journal of Investigation in Health, Psychology and Education 14, no. 1: 215-229. https://doi.org/10.3390/ejihpe14010014
APA StyleGianfredi, V., Mazziotta, F., Clerici, G., Astorri, E., Oliani, F., Cappellina, M., Catalini, A., Dell’Osso, B. M., Pregliasco, F. E., Castaldi, S., & Benatti, B. (2024). Climate Change Perception and Mental Health. Results from a Systematic Review of the Literature. European Journal of Investigation in Health, Psychology and Education, 14(1), 215-229. https://doi.org/10.3390/ejihpe14010014







