Abstract
Caregivers of people with intellectual disabilities may feel overburdened in their work and experience negative psychological consequences. The purpose of this instrumental study was to determine the evidence of internal structure and reliability of the Zarit Caregiver Burden Interview scale. A total of 398 family caregivers, including women and men, participated (M = 47.33, SD = 10.44). The structure of the scale was evaluated by factor analysis and the McDonald Omega coefficient was used to estimate reliability. Sixteen models of the scale were tested, differing in number of items and factor structures. A model of 15 items and 4 dimensions (overload, competence, social relationship, and interpersonal relationship) obtained acceptable fit (χ2 = 184.72; p < 0.001; CFI = 0.95; TLI = 0.94; RMSEA = 0.055; SRMR = 0.05) and reliability coefficients above 0.70 in their dimensions. It is concluded that the Zarit scale is valid and reliable for use in caregivers of people with intellectual disabilities.
1. Introduction
Intellectual disability (ID) is characterized by cognitive and adaptive behavioral deficits that originate before the age of 18 years [1]. It is a lifelong condition that requires support from educational, health, and social institutions [2]. It is associated with other conditions such as autism, externalizing disorders, cerebral palsy, and compulsive/epileptic problems [3]. Studies indicate that people with ID are more likely to suffer from physical health problems, age faster [4,5], suffer from any psychiatric disorder [6], and have an increased risk of death [7].
COVID-19 has predicted an increased risk of mortality in people with ID [8,9]. In addition, it has harmed their mental health and that of caregivers due to changes in family routines and restrictions in health and social services [10,11], causing problematic behaviors and emotional instability [12]. Depending on the level of dependency, the person with ID requires the permanent support of a caregiver [13]. However, caring for a dependent may negatively impact mental health [14].
Family members, in fulfilling their caregiving role, suffer a significant impact on their lives, since work overload can generate marital, work, and emotional problems [15]. Evidence indicates that parents caring for children with ID present profound stress, anxiety and depression [16], sleep deprivation [15,17], lower quality of life [18], and they withdraw from their leisure activities or hobbies [19].
Caregiver overload is the level of stress experienced by the caregiver in caring for their family member or loved one for an extended period of time [20]. They have objective elements, such as the time of tasks dedicated to the person in need of care, where the responsibility for care is assumed by the caregiver. Subjective elements, on the other hand, are derived from the individual’s emotional, social, and role perceptions, such as fatigue, inequality, emotional distress, and stress [21].
Throughout the literature, different instruments have been designed to measure caregiver overload from both objective and subjective approaches. From the objective criteria, there is the six-item Caregiver Activity Survey (CAS) [22], designed to quantify the tasks associated with caregiving activities. Among the subjective scales, the Caregiver Burden Scale for Family Caregivers with Relatives in Nursing Homes (CBS-FNH) [23], with 16 items and made up of 4 dimensions (conflicts with care staff, caregiver restrictions, guilt and loss of care, and anticipated grief), stands out in a sample of family caregivers of older adults. Another measure is the Carers of Older People in Europe (COPE Index) [24], consisting of 17 items and 3 dimensions (positive overload, negative overload, and quality of support) obtained from an exploratory factor analysis through principal components.
One of the most popular instruments for measuring caregiver overload is the Zarit Burden Interview (ZBI). It was originally composed of 29 items assessing psychological well-being, financial situation, relationship of the caregiver and person with disability, and social life [21]; it was later reduced to 22 items [25]. This tool has been validated in caregivers of patients with dementia [26], schizophrenia [27], informal caregivers [28,29], older adults [30], and oncology patients [31].
It has been translated into different languages and validated in various countries such as Germany [31], Singapore [32], Thailand [33], Mongolia [34], and Brazil [30,35], among others. The Spanish version, conducted by Martín-Carrasco et al. [36], showed a factorial structure of three dimensions (overload, competence, and dependence), with adequate sensitivity and specificity with mental health.
The general use of the ZBI has fostered interest in studies that sought to simplify the 22-item scale in order to facilitate its administration and perform rapid detection of caregiver burden [37]. Whitlatch et al. [38] found the presence of 18 items and two factors: personal strain and role strain. For their part, Montorio et al. [39] found three factors: impact of care, interpersonal burden, and self-efficacy expectations. Another validation study of the ZBI identified 14 items and three factors (embarrassment/anger, patient dependence, and self-criticism) [40]. Later on, Hébert et al. [41] and Bédard et al. [42] obtained a reduced version of 12 items with two factors (personal strain and role strain), while Ballesteros et al. [43] kept the 12 items, but grouped them into a single factor. However, in other studies, the structure of 22 items and 3 factors has not been modified [44].
Validations of the ZBI have been developed in Latin America. In Brazil, work was conducted with a group of caregivers of older adults, where a 3-factor structure composed of 12 items was found [45]. In Argentina, Tartaglini et al. [46] considered a unifactorial model composed of 17 items. In Colombia, Albarracín et al. [47], by means of exploratory factor analysis, identified a 4-factor model (overload, competence, social relationship, and interpersonal relationship) with 14 items. Other studies have identified much shorter versions of the ZBI, such as the ZBI-3 items [48] and the ZBI-4 items that were developed in caregivers of older adults with dementia [49].
In Peru, Boluarte et al. [50], through a confirmatory factor analysis, demonstrated that the unidimensional model proposed by Rueda et al. [51] shows good fit across its 13 items. Likewise, factor loadings range from 0.332 to 0.788 in a sample of informal caregivers of people with ID.
Thus, the literature shows little consensus on the dimensionality of the instrument, making it difficult to evaluate its comparison and equivalence with the original version [52]. In addition, the cut-off points of the different variants of the ZBI may lack a meaningful outcome in the measurement of overload, and most studies have been developed in caregivers of older adult patients with degenerative problems and other diseases. For this reason, the main objective of the present study is to determine the evidence of internal structure, relationship with other variables, and reliability of the ZBI scale in caregivers of people with intellectual disabilities in the Peruvian context. The use of a valid and reliable instrument is important in psychological work for the detection and clinical intervention of caregivers.
2. Materials and Methods
2.1. Design and Procedure
The design was instrumental. This study followed the guidelines suggested by the Association of Psychologists of Peru [53] and the 2013 Declaration of Helsinki [54], and obtained the approval of the ethics committee of the Universidad Tecnológica del Perú (Technological University of Peru) with registration number 175-2021-CEI-UTP. Each participant was informed of the objective of the study, the confidentiality of the information and the anonymity of the data, and gave informed consent. Data collection was carried out between January and June 2022. Initially, we coordinated with the Municipal Offices for the Attention of Persons with Disabilities (OMAPED: from the Spanish abbreviation), obtaining the list of caregivers, who were contacted by telephone to explain the research objectives and their voluntary participation and the anonymity of the data; then, through instant messaging, they were sent an online form to fill out the questionnaires.
2.2. Participants
The participants were immediate family members of a person with intellectual disabilities who used the services of the Municipal Offices for the Attention of Persons with Disabilities (OMAPED) in Lima, Peru. For this study, only one caregiver was allowed to participate. Sample selection was by convenience sampling and was calculated using Soper’s statistical calculator (2022) [55]. For this purpose, the 22 observed variables (22 items of the ZBI), 1 latent variable (caregiver overload), an anticipated effect size (lambda = 0.1), probability (0.05), and a statistical power level (0.95) were considered.
The final number of the sample was higher than suggested. A total of 398 family caregivers (333 women and 65 men) between 24 and 65 years of age (Median = 47.33, SD = 10.44) participated. Regarding marital status, most were single (34.9%), had completed secondary education (52.8%), and were mothers (60.6%). Table 1 shows, in greater detail, the sociodemographic characteristics of the participants.

Table 1.
Sociodemographic data of the sample.
2.3. Instrument
The Zarit Caregiver Burden Interview (ZBI) was created by Zarit et al. in 1980 [21]. It is a self-administered instrument composed of 22 items scored on a Likert-type scale with 5 response options: never (0 points), rarely (1 point), sometimes (2 points), quite often (3 points), and almost always (4 points). Higher scores indicate greater caregiver burden. The Spanish translation of the ZBI by Martín-Carrasco et al. [36] was used for this study. The ZBI assesses the impact of psychological well-being, financial situation, relationship of the caregiver and person with disability, and social life. Proposals have generated different versions of the scale, which have varied in number of items and factor structure. Sufficient evidence of validity and reliability has been reported in different countries and languages.
2.4. Statistical Analysis
First, the descriptive analysis of the ZBI items was performed (mean, standard deviation, asymmetry coefficient, and kurtosis). Likewise, univariate normality was calculated by analysis of asymmetry and kurtosis, where the values should be between +/−1.5. For evidence based on internal structure, a confirmatory factor analysis (CFA) was performed for the 16 ZBI models, using the weighted least squares estimator with corrected mean and variance (WLSMV), due to the ordinal nature of the items.
The chi-square test (χ2), the root mean square error of approximation (RMSEA) with its 90% confidence intervals, the standardized root mean square residual (SRMR), the comparative fit index (CFI), and the Tucker–Lewis index (TLI) were used to evaluate the fit of the factorial models. For a good fit of the factorial model, values lower than 0.08 for RMSEA and SRMR, values higher than 0.90 for CFI and TLI [56,57], and values higher than 0.50 for factor loadings [58] were considered acceptable. Reliability was calculated using the McDonald Omega coefficient (ω) with its 95% confidence intervals, where values above 0.80 were considered sufficient [59].
For the item response theory model, the graded response model (GRM) was used by extending the 2-parameter logistic model (2-PLM) for ordered polytomous items [60]. Thus, two parameters are calculated for each item: discrimination (a) and difficulty (b). The discrimination parameter evaluates the slope at which item responses change as a function of the latent trait; the difficulty parameter determines the amount of latent trait required as a response to the item. Because the scale has five response options, four difficulty estimates per threshold were obtained. The estimates for each threshold indicate the level of the latent variable that the subject possesses at a 50% probability of scoring at or above a particular response category. Finally, item information curve (IIC) and test information curve graphs (TIC) were obtained.
Statistical analysis was carried out using the Rstudio environment version 4. 1. 2 [61,62], the “lavaan” libraries for the CFA, and “ltm” for the item response theory model, through the graded response model extension (GRM). In addition, the coding of the analysis is available upon request to the authors.
3. Results
3.1. Preliminary Analysis
Item 8 (“Do you feel that your relative depends on you?”) has the highest average (M = 3.81; SD = 1.22), while item 13 (“Do you feel uncomfortable inviting friends over because of your relative?”) obtained the lowest value (M = 1.45; SD = 0.88). In the univariate normality, most of the items show adequate values lower than +/−1.5; however, items 4, 5, and 13 present an asymmetric response behavior with a high concentration of scores in the first response options (Table 2).

Table 2.
Descriptive statistics of the ZBI.
3.2. Evidence Based on the Internal Structure
A CFA was performed by testing 16 models of the ZBI that differ in number of items and factor structure. The results show that the unidimensional models of Bédard et al. [42] (χ2 = 13.11; p < 0.001; CFI = 0.97; TLI = 0.91; RMSEA = 0.118; SRMR = 0.03) and Gort et al. (2005) [63] (χ2 = 77.54; p < 0.001; CFI = 0.93; TLI = 0.90; RMSEA = 0.107; SRMR = 0.04) obtained adequate fit indexes. However, the root mean squared error of approximation (RMSEA) was higher than the suggested criterion (<0.08) for both models; therefore, they were not satisfactory.
The 15-item model of Albarracín et al. [47] shows 4 dimensions: overload with 4 items (items 17, 18, 19, and 22), competence with 5 items (items 1, 9, 10, 15, and 16), social relationship with 3 items (items 6, 11, and 12), and interpersonal relationship with 3 items (items 4, 5, and 13), which fit correctly (χ2 = 184. 72; p < 0.001; CFI = 0.95; TLI = 0.94; RMSEA = 0.055; SRMR = 0.05) (Table 3). The factor loadings ranged from 0.34 (item 1) to 0.88 (item 12). Because of this, this model was considered in the following analyses.

Table 3.
ZBI goodness-of-fit indexes.
3.3. Reliability
The four-factor model obtained coefficients above 0.70 in its 4 dimensions: overload (α = 0.81, CI 95% [0.77–0.83]; ω = 0.74; CI 95% [0.68–0.79]), competence (α = 0.75, CI 95% [0.71–0.79]; ω = 0.76; CI 95% [0.72–0.80]), social relationship (α = 0.83, CI 95% [0.80–0.86]; ω = 0.84; CI 95% [0.80–0.87]), and interpersonal relationship (α = 0.77, CI 95% [0.73–0.80]; ω = 0.78; CI 95% [0.72- 0.84]).
3.4. Item Response Theory Model
Four Graded Response Models were used, in a two-parameter logistic model for each dimension (overload, competence, social relationship, and interpersonal relationship), due to the polytomous items of the ZBI. Table 4 shows column (a) of the discrimination items for each item, with values higher than 1, evidencing an acceptable level of discrimination between subjects. On the other hand, columns (b1) to (b4) show monotonically ordered estimates for the difficulty of the questionnaire.

Table 4.
Discrimination and difficulty parameters of the items by ZBI dimensions.
Figure 1 shows the test information curves for each dimension. The reliability (accuracy) of the overload dimension is between −1.8 and 3, the competence dimension between −1 and 3, the social relationship dimension between −1 and 3, and, finally, the interpersonal relationship dimension is between −1 and 3.5.
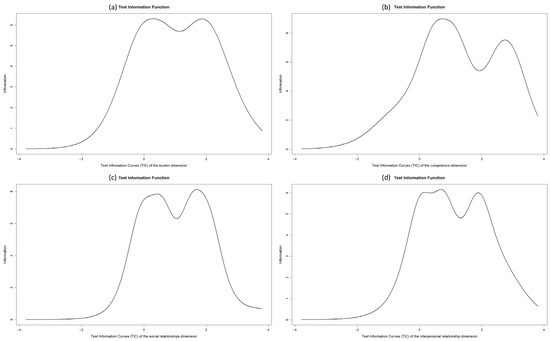
Figure 1.
Information curves by ZBI dimensions: overload (Panel (a)), competence (Panel (b)), social relationship (Panel (c)), interpersonal relationship (Panel (d)).
Figure 2 shows the information curves per item for each dimension. In the overload dimension, item 17 is the most accurate item for the evaluation of the latent trait. In the competence dimension, item 10 is the item that shows the greatest discriminatory capacity for the measurement of the variable. In the social relationship dimension, items 11 and 12 show the highest accuracy. Finally, in the interpersonal relationship dimension, item 4 shows the highest discrimination.
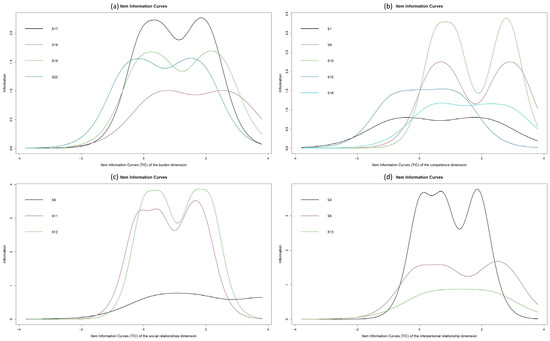
Figure 2.
Item information curves according to ZBI dimensions: overload (Panel (a)), competence (Panel (b)), social relationship (Panel (c)), interpersonal relationship (Panel (d)).
3.5. Association with Other Variables
Table 5 shows evidence of positive correlations between the ZBI factors, with values ranging from 0.44 to 0.68. Regarding gender, differences were obtained in all factors with small effect sizes: overload (rbis = 0.13, p = 0.02, CI 95% = 0.03, 0.23), competence (rbis = 0.14, p = 0.01, CI 95% = 0.05, 0.24), social relationship (rbis = 0.11, p = 0.03, CI 95% = 0.01, 0.21), and interpersonal relationship (rbis = 0.11, p = 0.03, CI 95% = 0.01, 0.21), with higher scores in females than in males. In relation to age, positive and small correlations were found with the factors of overload (rs = 0.12, p < 0.01, CI 95% = 0.02, 0.21) and competence (rs = 0.16, p < 0.01, CI 95% = 0.05, 0.24). However, no correlations were found with the social relationship and interpersonal relationship factors.

Table 5.
Association with other variables.
4. Discussion
Overload has a significant impact on the caregiver’s role, generating physical, emotional, cognitive and financial consequences [65]. The context of the coronavirus pandemic has not only brought negative consequences to the person with ID, but also to his or her caregiver [13]. This demonstrates the importance of having an instrument that measures caregiver overload with evidence of validity and reliability in the Peruvian context.
The dimensionality of 16 previous ZBI models was assessed by means of CFA, of which fifteen did not fit satisfactorily. Some of them had already been tested previously, showing similar results. For example, the two-dimensional 17-item structure of Whitlatch et al. [38], was not successful in the studies by Li et al. [66] and Landfeldt et al. [67]. Similarly, the model of Bianchi et al. [45] and Martín-Carrasco et al. [36] did not obtain an adequate fit in the study by Boluarte et al. [50].
The model of Albarracín et al. [47] had the best fit. In this version of the ZBI, 7 of the 22 items were eliminated because they did not load on any factor or were composed of two-item factors, which was not feasible. In this sense, in family caregivers of people with intellectual disabilities, a short version of 15 items and four dimensions (overload, competence, social relationship, and interpersonal relationship) is the most useful.
Despite the little consensus on the dimensionality of the instrument and its difficulty in comparing its dimensions with other groups, this study confirmed the 4-factor multidimensional model with 15 items of Albarracín et al. [47]. The factors of overload and competence are congruent with the factorial exploration in other psychometric validation studies in caregivers of older adults [68] with Alzheimer’s disease [36] and patients with cerebrovascular accident [69]. Although the research participants have different characteristics and come from different backgrounds, there is similarity in the factors measured through the ZBI. In this way, stress, lack of time for personal activities, health problems, and role capacity are indicators of overload and competence. On the other hand, social and interpersonal relationship factors are reported by other designations [70,71] such as: uncertainty and shame and guilt, as well as emotions experienced by the caregiver for his or her role and the person he or she cares for.
Overload, measured with the ZBI scale, converges with gender and age. In this regard, a systematic review study identified higher levels of overload in female caregivers, describing higher physical and emotional stress compared to men [71]. On the other hand, older caregivers experience higher caregiving overload, developing more symptoms of irritability and apathy [72].
In the analysis of the item response theory (IRT) model, the graded response model (GRM) was used. In all four dimensions, discrimination was adequate, showing that the items can clearly and efficiently differentiate between individuals who reach high and low levels in the four dimensions of caregiver overload. On the other hand, the estimates of the difficulty parameters for each item increased monotonically; therefore, the difficulty is acceptable. Items 4, 10, 11, 11, 12, and 17 have acceptable levels of discrimination for the evaluation of the latent trait in each of their dimensions. On the other hand, the total information curves show higher reliability for the precision of the four dimensions [59].
Regarding reliability, the model of Albarracín et al. [47] showed acceptable consistency indexes in the dimensions of the ZBI scale (>0.70). As for the finding, the four-factor model is the most accessible for use in family caregivers of people with ID. In addition, the reliability of the IRT through the total information curves (TIC) was acceptable. Thus, their values were among the acceptable parameters for item discrimination and difficulty.
This research is included within the growing area of study of the theoretical foundations of caregiver burden. Its relevance lies in the fact that it addresses the main problem of the family caregiver of the person with ID, which is to assume responsibilities for which they are not prepared, since the lack of information and training generate physical, economic, and emotional impacts. Likewise, it offers the validation of an instrument widely studied in different groups, contexts, and test variations, with an important usefulness in the health field in the Peruvian context.
For this reason, early detection of overload facilitates intervention and reduction of psychological distress in caregivers, and allows them to better cope with their work, with positive implications for them and for those they care for. On the other hand, the study contributes methodologically by applying IRT and classical test theory as part of the psychometric properties of the instrument. Finally, this psychometric validation will be useful to health professionals as they will be able to have an instrument that will contribute to the timely diagnosis of overload.
Among the limitations of the study is the absence of evidence of validity with instruments equivalent to overload and with other constructs such as stress, mental health, anxiety, depression, or coping strategies to obtain evidence of discriminant and convergent validity. On the other hand, the use of non-probability convenience sampling affects the external validity of the study. Finally, the previous contact by telephone call and the virtual evaluation could generate implications in the response process of the instruments. Therefore, it is suggested that future studies use some technique for randomizing the sample and collecting information in person.
5. Conclusions
The study finds evidence in favor of the ZBI presenting a multi-dimensional structure of four correlated factors in caregivers of people with ID in the Peruvian context. In addition, its factors converge with gender and age. On the other hand, the combination of the Item Response Theory (IRT) model allows for greater understanding of item difficulty and discrimination. In conclusion, the ZBI presents satisfactory results in terms of validity and reliability, making it a suitable instrument that can be used in future research as a tool for measuring caregiver overload in people with ID.
Author Contributions
Conceptualization, J.D.-V. and H.S.-C.-E.; methodology, J.D.-V. and H.S.-C.-E.; validation, J.D.-V. and H.S.-C.-E.; formal analysis J.D.-V.; investigation, J.D.-V. and H.S.-C.-E.; resources, J.D.-V. and H.S.-C.-E.; writing—original draft preparation, J.D.-V., H.S.-C.-E. and G.C.-V.; writing—review and editing, J.D.-V. and H.S.-C.-E. and G.C.-V.; visualization, J.D.-V., H.S.-C.-E. and G.C.-V.; project administration, J.D.-V.; funding acquisition, J.D.-V. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding and the APC was funded by Universidad Tecnológica del Perú.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki, and approved by the Ethics Committee of Universidad Tecnológica del Perú (protocol code 175-2021-CEI-UTP, 10 December 2021) for studies involving humans.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented are available upon request to the corresponding author for academic and research use.
Acknowledgments
The authors would like to thank Oscar Carrillo-Verástegui for translating the article from Spanish into English.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Patel, D.; Cabral, M.D.; Ho, A.; Merrick, J. A clinical primer on intellectual disability. Transl. Pediatr. 2020, 9, S23–S35. [Google Scholar] [CrossRef]
- Dunn, K.; Rydzewska, E.; Macintyre, C.; Rintoul, J.; Cooper, S.A. The prevalence and general health status of people with intellectual disabilities and autism co-occurring together: A total population study. J. Intellect. Disabil. Res. 2019, 63, 277–285. [Google Scholar] [CrossRef]
- Uzun, A.; Sarı, S.A.; Mercan Isık, C. Sociodemographic characteristics, risk factors, and prevalence of comorbidity among children and adolescents with intellectual disability: A cross-sectional study. J. Ment. Health Res. Intellect. Disabil. 2020, 13, 66–85. [Google Scholar] [CrossRef]
- Oppewal, A.; Schoufour, J.D.; Van der Maarl, H.J.; Evenhuis, H.M.; Hilgenkamp, T.I.; Festen, D.A. Causes of mortality in older people with intellectual disability: Results from the HA-ID study. Am. J. Intellect. Dev. Disabil. 2018, 123, 61–71. [Google Scholar] [CrossRef] [PubMed]
- Cuypers, M.; Schalk, B.W.M.; Koks-Leensen, M.C.J.; Nägele, M.E.; Bakker-van Gijssel, E.J.; Naaldenberg, J.; Leusink, G.L. Mortality of people with intellectual disabilities during the 2017/2018 influenza epidemic in the Netherlands: Potential implications for the COVID-19 pandemic. J. Intellect. Disabil. Res. 2020, 64, 482–488. [Google Scholar] [CrossRef]
- Apostolidis, K.; Mezaris, V.; Papadogiorgaki, M.; Bei, E.B.; Livanos, G.; Zervakis, M. Content and Other Resources Recommendations for Individuals with Intellectual Disability: A Review. Electronics 2022, 11, 3472. [Google Scholar] [CrossRef]
- Glover, G.; Williams, R.; Heslop, P.; Oyinlola, J.; Grey, J. Mortality in people with intellectual disabilities in England. J. Intellect. Disabil. Res. 2017, 61, 62–74. [Google Scholar] [CrossRef]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef] [PubMed]
- Fang, L.; Karakiulakis, G.; Roth, M. Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection? Lancet Respir. Med. 2020, 8, e21. [Google Scholar] [CrossRef] [PubMed]
- Courtenay, K.; Perera, B. COVID-19 and people with intellectual disability: Impacts of a pandemic. Ir. J. Psychol. Med. 2020, 37, 231–236. [Google Scholar] [CrossRef]
- Suarez-Balcazar, Y.; Mirza, M.; Errisuriz, V.L.; Zeng, W.; Brown, J.P.; Venegas, S.; Heydarian, N.; Parra-Medina, D.; Morales, P.; Torres, H.; et al. Impact of COVID-19 on the Mental Health and Well-Being of Latinx Caregivers of Children with Intellectual and Developmental Disabilities. Int. J. Environ. Res. Public Health 2021, 18, 7971. [Google Scholar] [CrossRef]
- Narzisi, A. Handle the autism spectrum condition during Coronavirus (COVID-19) stay at home period: Ten tips for helping parents and caregivers of young children. Brain Sci. 2020, 10, 207. [Google Scholar] [CrossRef]
- Kuijken, N.M.J.; Vlot-van Anrooij, K.; Van Schrojenstein Lantman-de Valk, H.M.J.; Leusink, G.; Naaldenberg, J.; Nijhuis-van der Sanden, M.W. Stakeholder expectations, roles and responsibilities in Dutch health promotion for people with intellectual disabilities. Health Promot. 2019, 34, e59–e70. [Google Scholar] [CrossRef]
- Flores, N.; Jenaro, C.; Moro, L.; Tomşa, R. Health and Quality of Life of Family and Professional Caregivers of Dependent Elderly: A Comparative Study. Eur. J. Investig. Health Psychol. Educ. 2014, 4, 79–88. [Google Scholar] [CrossRef]
- Kayadjanian, N.; Schwartz, L.; Farrar, E.; Comtois, K.A.; Strong, T.V. High levels of caregiver burden in Prader-Willi syndrome. PLoS ONE 2018, 13, e0194655. [Google Scholar] [CrossRef] [PubMed]
- Haider, S.; Ahmed, A. Caregiver burden among parents of hearing impaired and intellectually disabled children in Pakistan. Iran. J. Public Health 2020, 49, 249. [Google Scholar] [CrossRef]
- Wakimizu, R.; Fujioka, H.; Nishigaki, K.; Matsuzawa, A. Family empowerment and associated factors in Japanese families raising a child with severe motor and intellectual disabilities. Int. J. Nurs. Sci. 2018, 5, 370–376. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Ávalos, M.I.; Pérez-Marfil, M.N.; Ferrer-Cascales, R.; Cruz-Quintana, F.; Clement-Carbonell, V.; Fernández-Alcántara, M. Quality of Life and Concerns in Parent Caregivers of Adult Children Diagnosed with Intellectual Disability: A Qualitative Study. Int. J. Environ. Res. Public Health 2020, 17, 8690. [Google Scholar] [CrossRef] [PubMed]
- Vaz, S.; Thomson, A.; Cuomo, B.; Falkmer, T.; Chamberlain, A.; Black, M.H. Co-occurring intellectual disability and autism: Associations with stress, coping, time use, and quality of life in caregivers. Res. Autism. Spectr. Disord. 2021, 84, 101765. [Google Scholar] [CrossRef]
- Liu, Z.; Heffernan, C.; Tan, J. Caregiver burden: A concept analysis. Int. J. Nurs. Sci. 2020, 7, 438–445. [Google Scholar] [CrossRef]
- Zarit, S.H.; Reever, K.E.; Bach-Peterson, J. Relatives of the impaired elderly: Correlates of feelings of burden. Gerontologist 1980, 20, 649–655. [Google Scholar] [CrossRef] [PubMed]
- Davis, K.L.; Marin, D.B.; Kane, R.; Patrick, D.; Peskind, E.R.; Raskind, M.A.; Puder, K.L. The Caregiver Activity Survey (CAS): Development and validation of a new measure for caregivers of persons with Alzheimer’s disease. Int. J. Geriatr. Psychiatry 1997, 12, 978–988. [Google Scholar] [CrossRef]
- Fukahori, H.; Yamamoto-Mitani, N.; Sugiyama, T.; Sugai, Y.; Kai, I. Psychometric properties of the Caregiving Burden Scale for Family Caregivers with Relatives in Nursing Homes: Scale development. Jpn. J. Nurs. Sci. 2010, 7, 136–147. [Google Scholar] [CrossRef] [PubMed]
- McKee, K.; Philp, I.; Lamura, G.; Prouskas, C.; Oberg, B.; Krevers, B.; Szczerbinska, K. The COPE index: A First Stage assessment of Negative Impact, Positive Value and Quality of Support of Caregiving in Informal Carers of Older People. Aging Ment. Health 2003, 7, 39–52. [Google Scholar] [CrossRef]
- Zarit, S.H.; Orr, N.K.; Zarit, J.M. The Hidden Victims of Alzheimer’s Disease. Families under Stress; Nueva York University Press: New York, NY, USA, 1985. [Google Scholar]
- Ougjij, A.A.; Achbani, A.; Chigr, F. Cross-Cultural Adaptation and Psychometric Validation of the Moroccan Dialect Version of the Zarit Scale of Dementia Caregivers’ Burden. Electron. J. Gen. Med. 2022, 19. [Google Scholar] [CrossRef]
- Yu, Y.; Liu, Z.W.; Zhou, W.; Chen, X.C.; Zhang, X.Y.; Hu, M.; Xiao, S.Y. Assessment of burden among family caregivers of schizophrenia: Psychometric testing for short-form Zarit burden interviews. Front. Psychol. 2018, 9, 2539. [Google Scholar] [CrossRef]
- Ojifinni, O.O.; Uchendu, O.C. Validation and reliability of the 12-item Zarit Burden Interview among informal caregivers of elderly persons in Nigeria. Arch. Basic Appl. Med. 2018, 6, 45. [Google Scholar]
- Alves, S.; O’Caoimh, R.; Ribeiro, O.; Teixeira, L.; Molloy, D.W.; Paúl, C. Screening for caregiver burden in the community: Validation of the European Portuguese Screening Version of the Zarit Burden Interview (ZBI-4). Clin. Gerontol. 2022, 45, 525–537. [Google Scholar] [CrossRef]
- Gratão, A.C.; Brigola, A.G.; Ottaviani, A.C.; Luchesi, B.M.; Souza, É.N.; Rossetti, E.S.; de Oliveira, N.A.; Terassi, M.; Pavarini, S.C. Brief version of Zarit Burden Interview (ZBI) for burden assessment in older caregivers. Dement. Neuropsychol. 2019, 13, 122–129. [Google Scholar] [CrossRef]
- Kühnel, M.B.; Ramsenthaler, C.; Bausewein, C.; Fegg, M.; Hodiamont, F. Validation of two short versions of the Zarit Burden Interview in the palliative care setting: A questionnaire to assess the burden of informal caregivers. Support Care Cancer 2020, 28, 5185–5193. [Google Scholar] [CrossRef] [PubMed]
- Liew, T.M.; Yap, P. A 3-item screening scale for caregiver burden in dementia caregiving: Scale development and score mapping to the 22-item Zarit burden interview. J. Am. Med. Dir. Assoc. 2019, 20, 629–633. [Google Scholar] [CrossRef]
- Pinyopornpanish, K.; Pinyopornpanish, M.; Wongpakaran, N.; Wongpakaran, T.; Soontornpun, A.; Kuntawong, P. Investigating psychometric properties of the Thai version of the Zarit Burden Interview using rasch model and confirmatory factor analysis. BMC Res. Notes 2020, 13, 1–7. [Google Scholar] [CrossRef]
- Yamaguchi, M.; Uga, D.; Nakazawa, R.; Sakamoto, M. Reliability and validity of the Mongolian version of the Zarit Caregiver Burden Interview. J. Phys. Ther. Sci. 2020, 32, 449–453. [Google Scholar] [CrossRef]
- Queluz, F.N.; Ferreira Campos, C.R.; Santis, L.; de Isaac, L.; Barham, E.J. The Zarit Caregiver Burden Interview: Evidence of Validity for the Brazilian Population of Caregivers of the Elderly. Rev. Colomb. Psicol. 2019, 28, 99–114. [Google Scholar] [CrossRef]
- Martín-Carrasco, M.; Otermin, P.; Pérez-Camo, V.; Pujol, J.; Agüera, L.; Martín, M.J.; Gobartt, A.L.; Pons, S.; Balana, M. EDUCA study: Psychometric properties of the Spanish version of the Zarit Caregiver Burden Scale. Aging Ment Health 2010, 14, 705–711. [Google Scholar] [CrossRef]
- Lin, C.Y.; Wang, J.D.; Pai, M.C.; Ku, L.J. Measuring burden in dementia caregivers: Confirmatory factor analysis for short forms of the Zarit Burden Interview. Arch. Gerontol. Geriatr. 2017, 68, 8–13. [Google Scholar] [CrossRef]
- Whitlatch, C.J.; Zarit, S.H.; von Eye, A. Efficacy of interventions with caregivers: A reanalysis. Gerontologist 1991, 31, 9–14. [Google Scholar] [CrossRef] [PubMed]
- Montorio, I.; Fernández de Trocóniz, M.I.; López López, A.; Sánchez Colodrón, M. La entrevista de carga del cuidador. Utilidad y validez del concepto de carga. An. Psicol. 1998, 14, 229–248. [Google Scholar]
- Knight, B.G.; Fox, L.S.; Chou, C.P. Factor structure of the Burden Interview. J. Clin. Geropsychol. 2000, 6, 249–258. [Google Scholar] [CrossRef]
- Hébert, R.; Bravo, G.; Préville, M. Reliability, validity and reference values of the Zarit Burden Interview for assessing informal caregivers of community-dwelling older persons with dementia. Can. J. Aging 2000, 19, 494–507. [Google Scholar] [CrossRef]
- Bédard, M.; Molloy, D.W.; Squire, L.; Dubois, S.; Lever, J.Á.; O’Donnell, M. The Zarit Burden Interview: A new short version and screening version. Gerontologist 2001, 41, 652–657. [Google Scholar] [CrossRef]
- Ballesteros, J.; Santos, B.; González-Fraile, E.; Muñoz-Hermoso, P.; Domínguez-Panchón, A.I.; Martín-Carrasco, M. Unidimensional 12-item Zarit Caregiver Burden Interview for the assessment of dementia caregivers’ burden obtained by item response theory. Value Health 2012, 15, 1141–1147. [Google Scholar] [CrossRef]
- Oh, J.; Kim, J.A. Factor analysis of the Zarit Burden Interview in family caregivers of patients with amyotrophic lateral sclerosis. Amyotroph. Lateral Scler. Front. Degener. 2018, 19, 50–56. [Google Scholar] [CrossRef]
- Bianchi, M.; Flesch, L.D.; Alves, E.V.; Batistoni, S.S.; Neri, A.L. Zarit burden interview psychometric indicators applied in older people caregivers of other elderly. Rev. Lat. Am. Enfermagem. 2016, 24, e2835. [Google Scholar] [CrossRef]
- Tartaglini, M.F.; Feldberg, C.; Hermida, P.D.; Heisecke, S.L.; Dillon, C.; Ofman, S.D.; Nuñez, M.L.; Somale, V. Escala de sobrecarga del cuidador de Zarit: Análisis de sus propiedades psicométricas en cuidadores familiares residentes en Buenos Aires, Argentina. Neurol. Argentina 2020, 12, 27–35. [Google Scholar] [CrossRef]
- Albarracín, A.P.; Cerquera, A.M.; Pabón, D.K. Escala de sobrecarga del cuidador Zarit: Estructura factorial en cuidadores informales de Bucaramanga. Rev. Psicol. Univ. Antioquía 2016, 8, 87–99. [Google Scholar] [CrossRef]
- Higginson, I.J.; Gao, W.; Jackson, D.; Murray, J.; Harding, R. Short-form Zarit Caregiver Burden Interviews were valid in advanced conditions. J. Clin. Epidemiol. 2010, 63, 535–542. [Google Scholar] [CrossRef]
- Gort, A.M.; Mingot, M.; March, J.; Gómez, X.; Soler, T.; Nicolás, F. Utilidad de la escala de Zarit reducida en demencias. Med Clin. 2010, 135, 447–449. [Google Scholar] [CrossRef]
- Boluarte-Carbajal, A.; Paredes-Angeles, R.; Tafur-Mendoza, A.A. Psychometric Properties of the Zarit Burden Interview in Informal Caregivers of Persons with Intellectual Disabilities. Front. Psychol. 2022, 13. [Google Scholar] [CrossRef]
- Rueda, L.J.; Ramos, J.X.; Márquez, M. Análisis de Rasch de la Escala Burden Interview de Zarit Aplicada a Cuidadores Familiares en Bucaramanga, Colombia. Arch. Med. (Manizales) 2017, 17, 17–26. [Google Scholar]
- Monreal, A.; Prieto, G. Análisis del Test de Detección del Cuidador Quemado con el Modelo de Rasch. Escr. Psicología. 2017, 10, 116–125. [Google Scholar] [CrossRef]
- Colegio de Psicólogos del Perú. Código de ética y Deontología. 2017. Available online: https://www.cpsp.pe/documentos/marco_legal/codigo_de_etica_y_deontologia.pdf (accessed on 14 September 2022).
- Asociación Médica Mundial. Declaración de Helsinki de la AMM—Principios Éticos para las Investigaciones Médicas en seres Humanos; Fortaleza, Brazil, 2013. [Google Scholar]
- Soper, D.S. A-Priori Sample Size Calculator for Structural Equation Models [Software]. 2022. Available online: https://www.danielsoper.com/statcalc/calculator.aspx?id=89 (accessed on 14 September 2022).
- DiStefano, C.; Liu, J.; Jiang, N.; Shi, D. Examination of the weighted root mean square residual: Evidence for trustworthiness? Struct. Equ. Model. 2018, 25, 453–466. [Google Scholar] [CrossRef]
- Schumacker, R.E.; Lomax, R.G. A Beginner’s Guide to Structural Equation Modeling, 4th ed; Routledge: Reino Unido, UK, 2015. [Google Scholar]
- Domínguez-Lara, S. Proposal for cut-offs for factor loadings: A construct reliability perspective. Enferm. Clin. 2018, 28, 401–402. [Google Scholar] [CrossRef]
- Raykov, T.; Hancock, G.R. Examining change in maximal reliability for multiple-component measuring instruments. Br. J. Math. Stat. Psychol. 2005, 58, 65–82. [Google Scholar] [CrossRef]
- Hambleton, R.K.; van der Linden, W.J.; Wells, C.S. IRT models for the analysis of polytomously scored data: Brief and selected history of model building advances. In Handbook of Polytomous Item Response Models; Nering, M.L., Ostini, R., Eds.; Routledge: Reino Unido, UK, 2010; pp. 21–42. [Google Scholar]
- RStudio Team. RStudio: Integrated Development Environment for R; RStudio, Inc: 2018. Available online: https://www.rstudio.com (accessed on 3 October 2022).
- R Core Team. A Language and Environment for Statistical Computing; R version 3.6.1; R Foundation for Statistical Computing: 2019. Available online: http://www.r-project.org/ (accessed on 3 October 2022).
- Gort, A.M.; March, J.; Gómez, X.; de Miguel, M.; Mazarico, S.; Ballesté, J. Short Zarit scale in palliative care. Med. Clin. 2005, 124, 651–653. [Google Scholar] [CrossRef]
- Lucijanić, J.; Baždarić, K.; Librenjak, D.; Lucijanić, M.; Hanževački, M.; Jureša, V. A validation of the Croatian version of Zarit Burden Interview and clinical predictors of caregiver burden in informal caregivers of patients with dementia: A cross-sectional study. Croat. Med. J. 2020, 61, 527–537. [Google Scholar] [CrossRef] [PubMed]
- Martos, A.; Cadilla, F.; Barragán, A.B.; Pérez-Fuentes, M.C.; Molero, M.M.; Gázquez, J.J. Instruments for evaluating the burden of family caregivers of persons with dementia. Eur. J. Investig. Health Psychol. Educ. 2015, 5, 281–292. [Google Scholar] [CrossRef]
- Li, R.; Chong, M.S.; Chan, P.C.; Tay, B.G.; Ali, N.B.; Lim, W.S. Worry about caregiving Performance: A confirmatory Factor analysis. Front. Med. 2018, 5, 79. [Google Scholar] [CrossRef]
- Landfeldt, E.; Mayhew, A.; Straub, V.; Bushby, K.; Lochmüller, H.; Lindgren, P. Psychometric properties of the Zarit Caregiver Burden Interview administered to caregivers to patients with Duchenne muscular dystrophy: A Rasch analysis. Disabil. Rehabil. 2019, 41, 966–973. [Google Scholar] [CrossRef]
- Ferraresi, F.; Ferreira, C.; De Santis, L.; Isaac, L.; Barham, E. Zarit Caregiver Burden Interview: Evidências de Validade para a População Brasileira de Cuidadores de Idosos. Rev. Colomb. Psicología 2018, 28, 99. [Google Scholar] [CrossRef]
- Ferreira da Costa, T.; Pereira, K.; Alves, T.; Costa, S.; Lopes, C.; Freitas, C. Estrutura fatorial da Escala Zarit Burden Interview em cuidadores de pacientes com acidente vascular encefálico. Rev. Enferm. Atual. 2019, 87, 206. [Google Scholar] [CrossRef]
- Kenneth, J.; Chin-Bailey, C.; Holder-Nevins, D.; Thompson, C.; Donaldson-Davis, K.; Eldemire-Shearer, D. Zarit burden interview among caregivers of community-dwelling older adults in a caribbean setting (Jamaica): Reliability and factor structure. Health Soc. Care 2020, 29, e79–e88. [Google Scholar]
- Xiong, C.; Biscardi, M.; Astell, A.; Nalder, E.; Cameron, J.I.; Mihailidis, A.; Colantonio, A. Sex and gender differences in caregiving burden experienced by family caregivers of persons with dementia: A systematic review. PLoS ONE 2020, 15, e0231848. [Google Scholar] [CrossRef]
- Tsai, C.F.; Hwang, W.S.; Lee, J.J.; Wang, W.F.; Huang, L.C.; Huang, L.K.; Lee, W.J.; Sung, P.S.; Liu, Y.C.; Hsu, C.C.; et al. Predictors of caregiver burden in aged caregivers of demented older patients. BMC Geriatr. 2021, 21, 59. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).