Minimally-Invasive Definitive Treatment of Recurrent Sialadenitis Due to Obstructive Sialolithiasis—A Case Report
Abstract
Introduction
Case report
Discussion
Conclusions
Author Contributions
Funding
Conflicts of Interest
Consent
References
- Adhikari, R.; Soni, A. Submandibular sialadenitis and sialadenosis. StatPearls Publishing: StatPearls. Treasure Island (FL), 2022. [Google Scholar]
- Chandak, R.; Degwekar, S.; Chandak, M.; Rawlani, S. Acute submandibular sialadenitis-a case report. Case Rep Dent. 2012, 2012, 615375. [Google Scholar] [CrossRef] [PubMed]
- Chow, A. Suppurative parotitis in adults. Post, TE, Ed.; UpToDate: Waltham, MA:, 2023. [Google Scholar]
- Hoffmann, H. Salivary gland swelling: Evaluation and diagnostic approach. Post, TE, Ed.; UpToDate: Waltham, MA, 2023. [Google Scholar]
- Al-Dajani, N.; Wootton, S.H. Cervical lymphadenitis, suppurative parotitis, thyroiditis, and infected cysts. Infect Dis Clin North Am. 2007, 21, 523–541, viii. [Google Scholar] [CrossRef] [PubMed]
- Brook, I.; Frazier, E.H.; Thompson, D.H. Aerobic and anaerobic microbiology of acute suppurative parotitis. Laryngoscope. 1991, 101, 170–172. [Google Scholar] [CrossRef] [PubMed]
- Brook, I. Aerobic and anaerobic microbiology of suppurative sialadenitis. J Med Microbiol. 2002, 51, 526-9. [Google Scholar] [CrossRef] [PubMed]
- Dangore-Khasbage, S.; Bhowate, R.R.; Degwekar, S.S.; Bhake, A.S.; Lohe, V.K. Tuberculosis of parotid gland: a rare clinical entity. Pediatr Dent. 2015, 37, 70–74. [Google Scholar] [PubMed]
- Poisbleau, D.; Ducroz, C.; Siest, R.; Giot, J.P.; Fabre, C. Bilateral candidal abscess of the parotid gland: a case report and literature review. J Stomatol Oral Maxillofac Surg. 2023, 124, 101355. [Google Scholar] [CrossRef] [PubMed]
- Paouris, D.; Dallos, T.; Pitiriga, V. Polymicrobial acute suppurative parotitis in a 33-day-old infant: a case report and review of the literature. Clin Pediatr (Phila). 2022, 61, 802–807. [Google Scholar] [CrossRef] [PubMed]
- Carta, F.; Farneti, P.; Cantore, S.; et al. Sialendoscopy for salivary stones: principles, technical skills and therapeutic experience. Acta Otorhinolaryngol Ital. 2017, 37, 102–112. [Google Scholar] [CrossRef] [PubMed]
- Kopec, T.; Wierzbicka, M.; Kaluzny, J.; Mlodkowska, A.; Szyfter, W. Sialendoscopy and sialendoscopically-assisted operations in the treatment of lithiasis of the submandibular and parotid glands: our experience of 239 cases. Br J Oral Maxillofac Surg. 2016, 54, 767–771. [Google Scholar] [CrossRef] [PubMed]
- Koch, M.; Mantsopoulos, K.; Muller, S.; Sievert, M.; Iro, H. Treatment of sialolithiasis: What has changed? An update of the treatment algorithms and a review of the literature. J Clin Med 2021, 11, 231. [Google Scholar] [CrossRef] [PubMed]
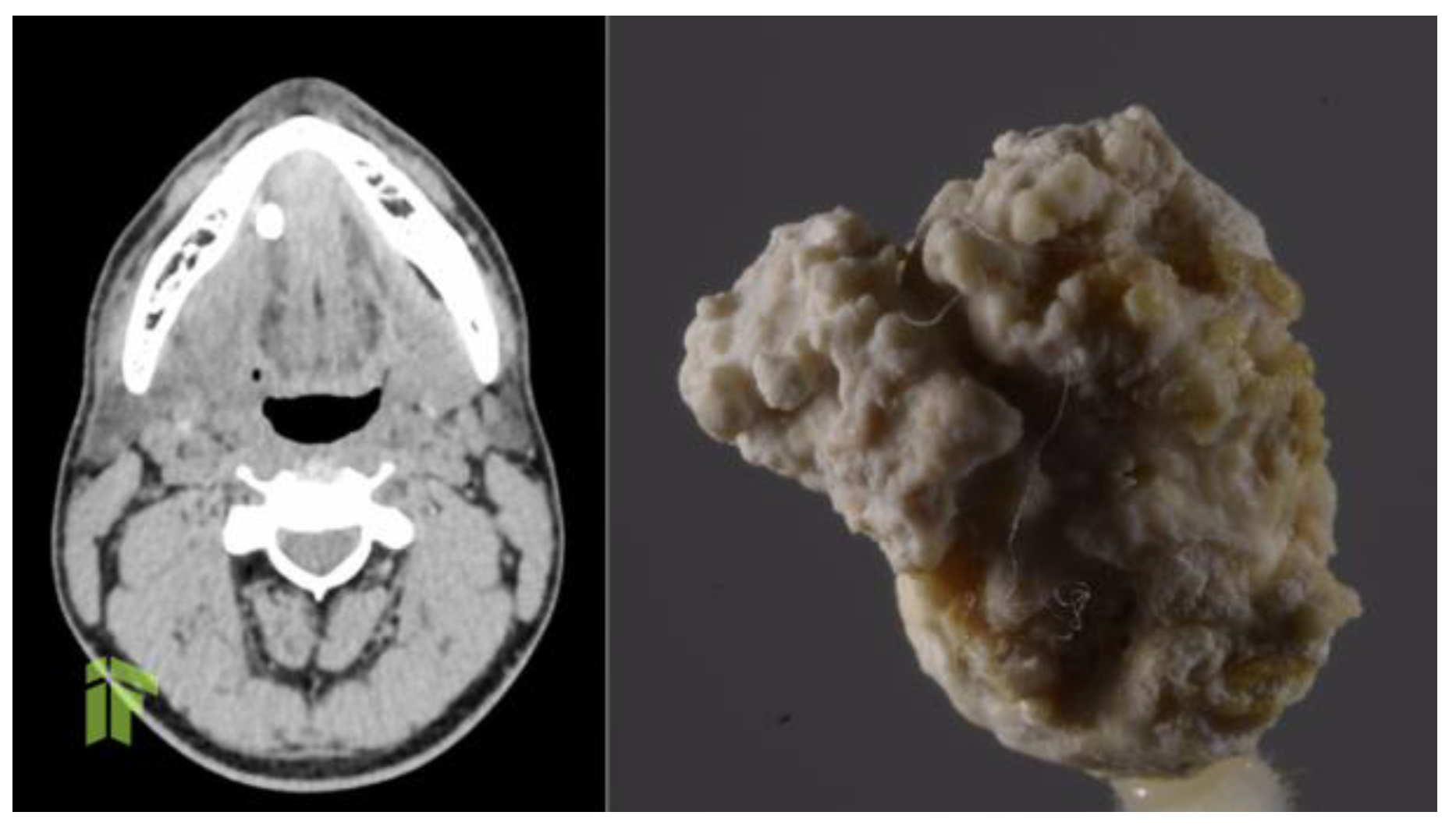
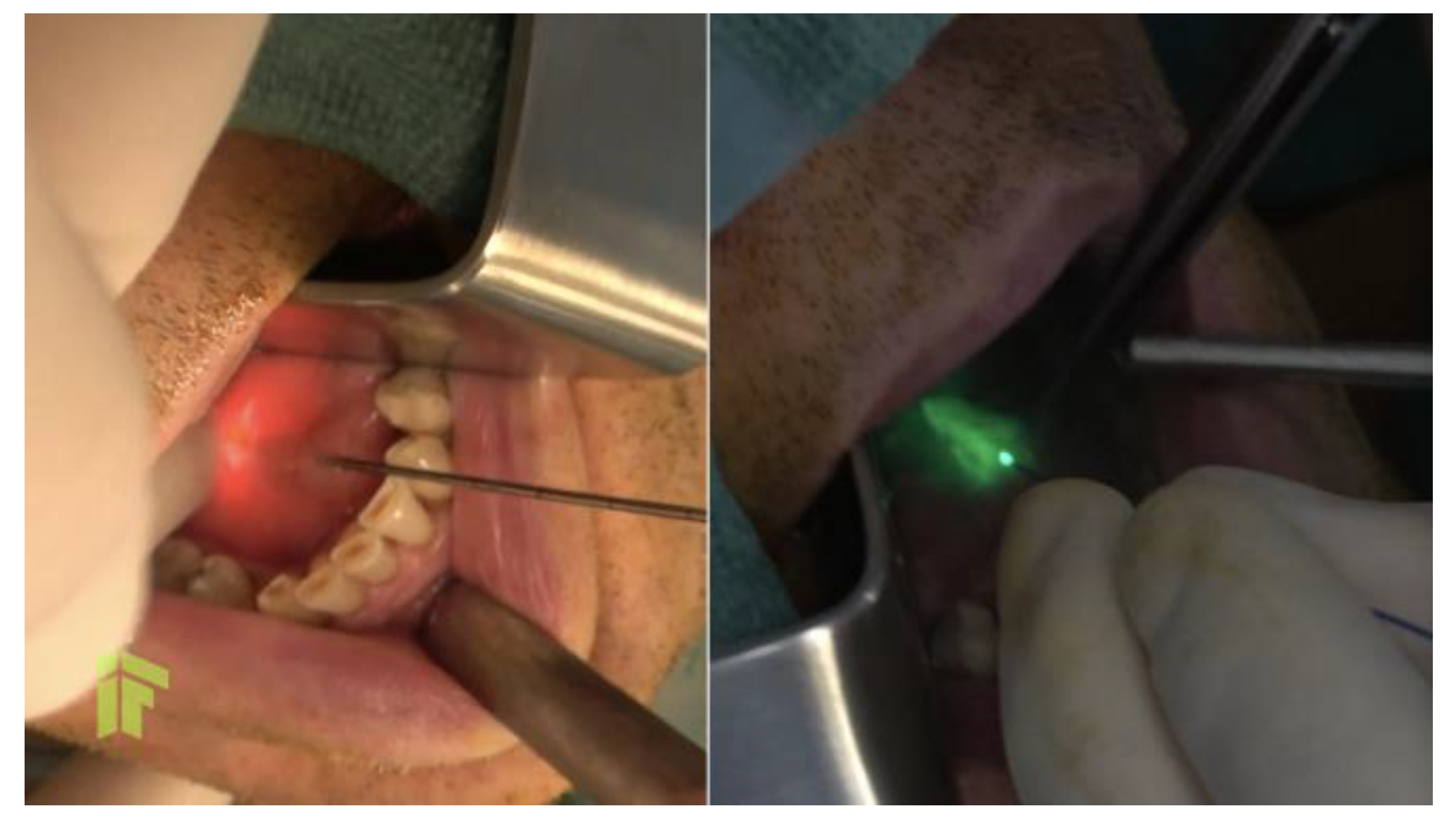
© GERMS 2023.
Share and Cite
Filipov, I.; Cristache, C.M.; Săndulescu, M. Minimally-Invasive Definitive Treatment of Recurrent Sialadenitis Due to Obstructive Sialolithiasis—A Case Report. Germs 2023, 13, 288-291. https://doi.org/10.18683/germs.2023.1397
Filipov I, Cristache CM, Săndulescu M. Minimally-Invasive Definitive Treatment of Recurrent Sialadenitis Due to Obstructive Sialolithiasis—A Case Report. Germs. 2023; 13(3):288-291. https://doi.org/10.18683/germs.2023.1397
Chicago/Turabian StyleFilipov, Iulian, Corina Marilena Cristache, and Mihai Săndulescu. 2023. "Minimally-Invasive Definitive Treatment of Recurrent Sialadenitis Due to Obstructive Sialolithiasis—A Case Report" Germs 13, no. 3: 288-291. https://doi.org/10.18683/germs.2023.1397
APA StyleFilipov, I., Cristache, C. M., & Săndulescu, M. (2023). Minimally-Invasive Definitive Treatment of Recurrent Sialadenitis Due to Obstructive Sialolithiasis—A Case Report. Germs, 13(3), 288-291. https://doi.org/10.18683/germs.2023.1397



