Evaluation of Antifungal Activity by Mixed Oxide Metallic Nanocomposite against Candida spp.
Abstract
1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Methods
2.2.1. Synthesis of Zirconia Nanoparticles
2.2.2. Synthesis of Ag2O Nanoparticles
2.2.3. Synthesis of ZrO2-Ag2O Nanoparticles
2.3. Characterization
2.4. Antifungal Study
2.4.1. Disc Diffusion Method
2.4.2. Antifungal Susceptibility Testing
2.5. Oxidative Effects on Mononuclear Cells
2.5.1. Blood Collection
2.5.2. Cell Viability
2.6. Statistical Analyses
3. Results
3.1. XRD, IR Analysis, and Zeta Potential Measurement
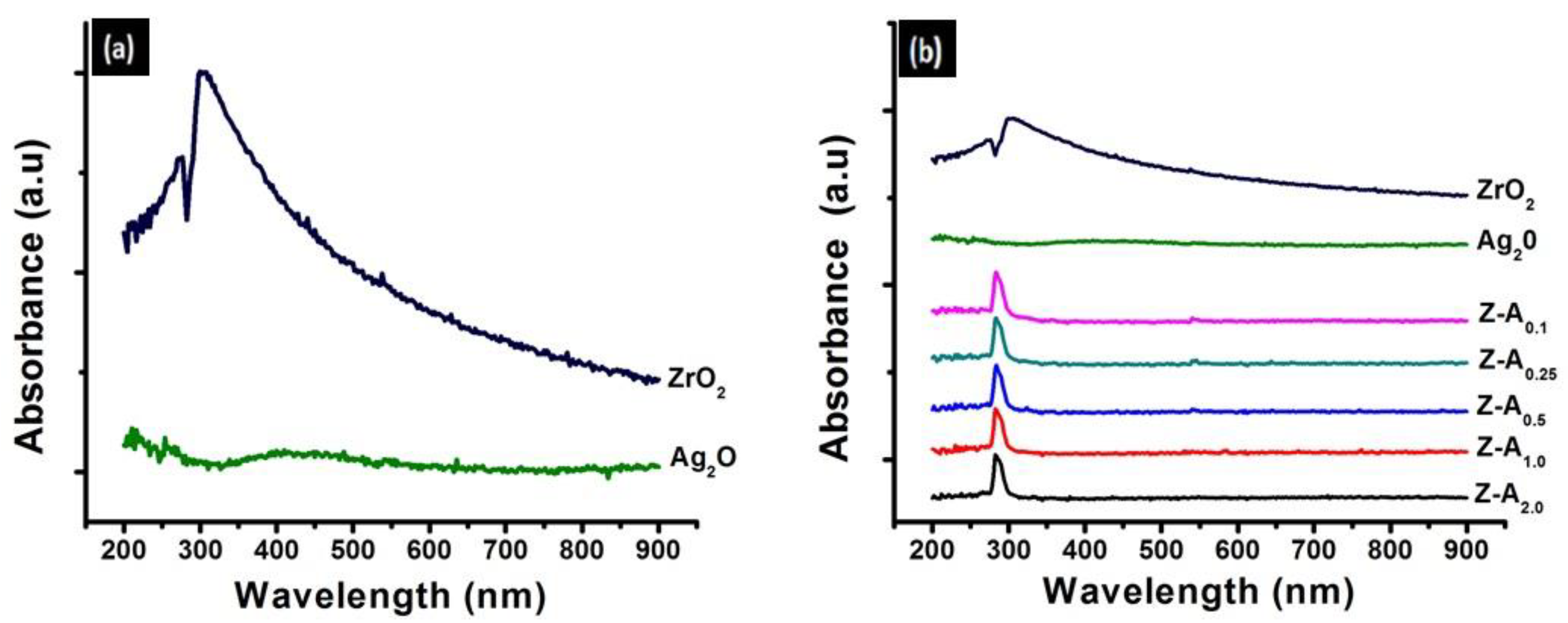
3.2. UV-Visible Absorption Analysis
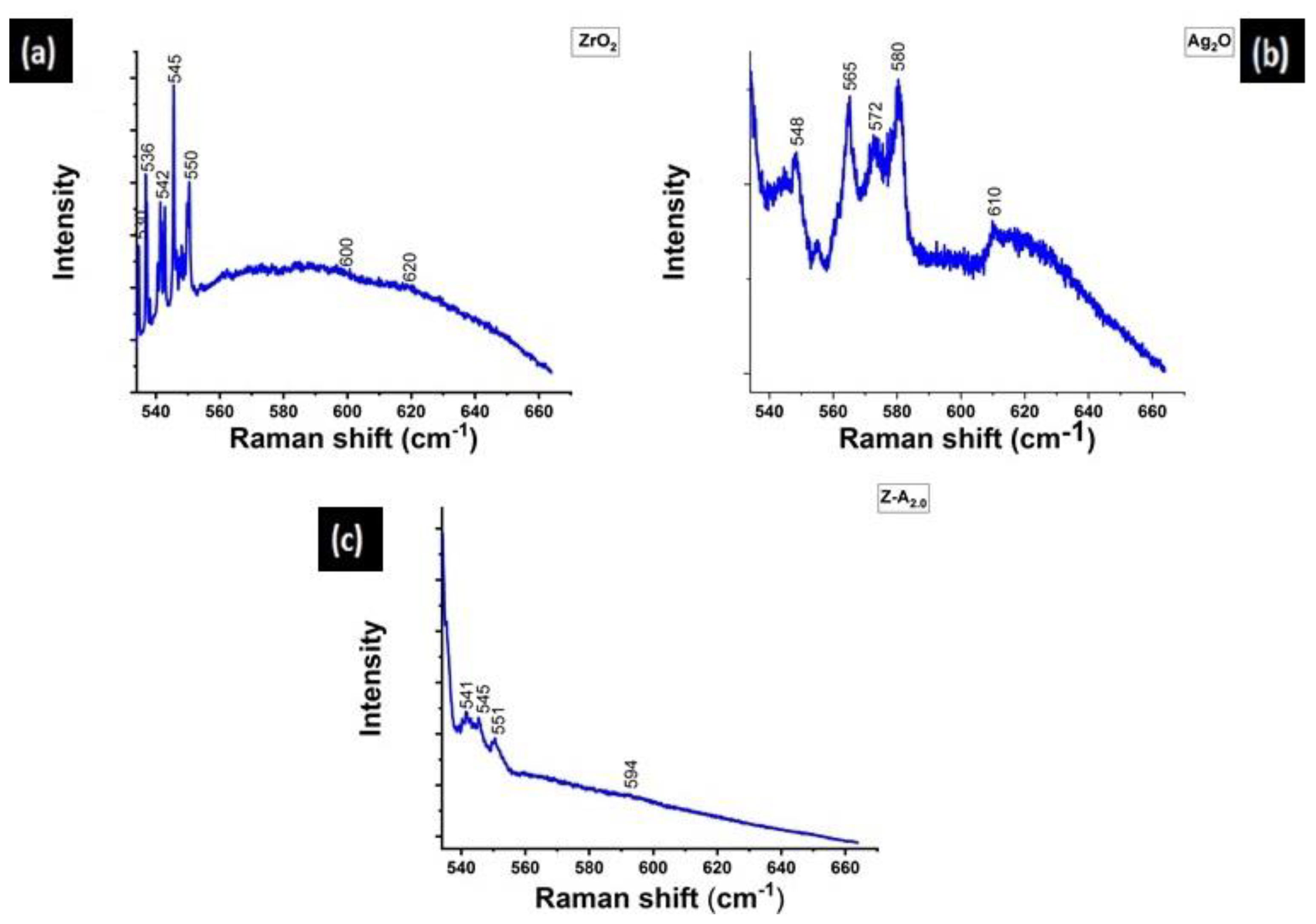
3.3. Raman Spectroscopy
3.4. Dynamic Light Scattering Analysis
3.5. Scanning Transmission Electron Microscopy
3.6. Antifungal Activity of Z-A Nanoparticles on Candida spp.
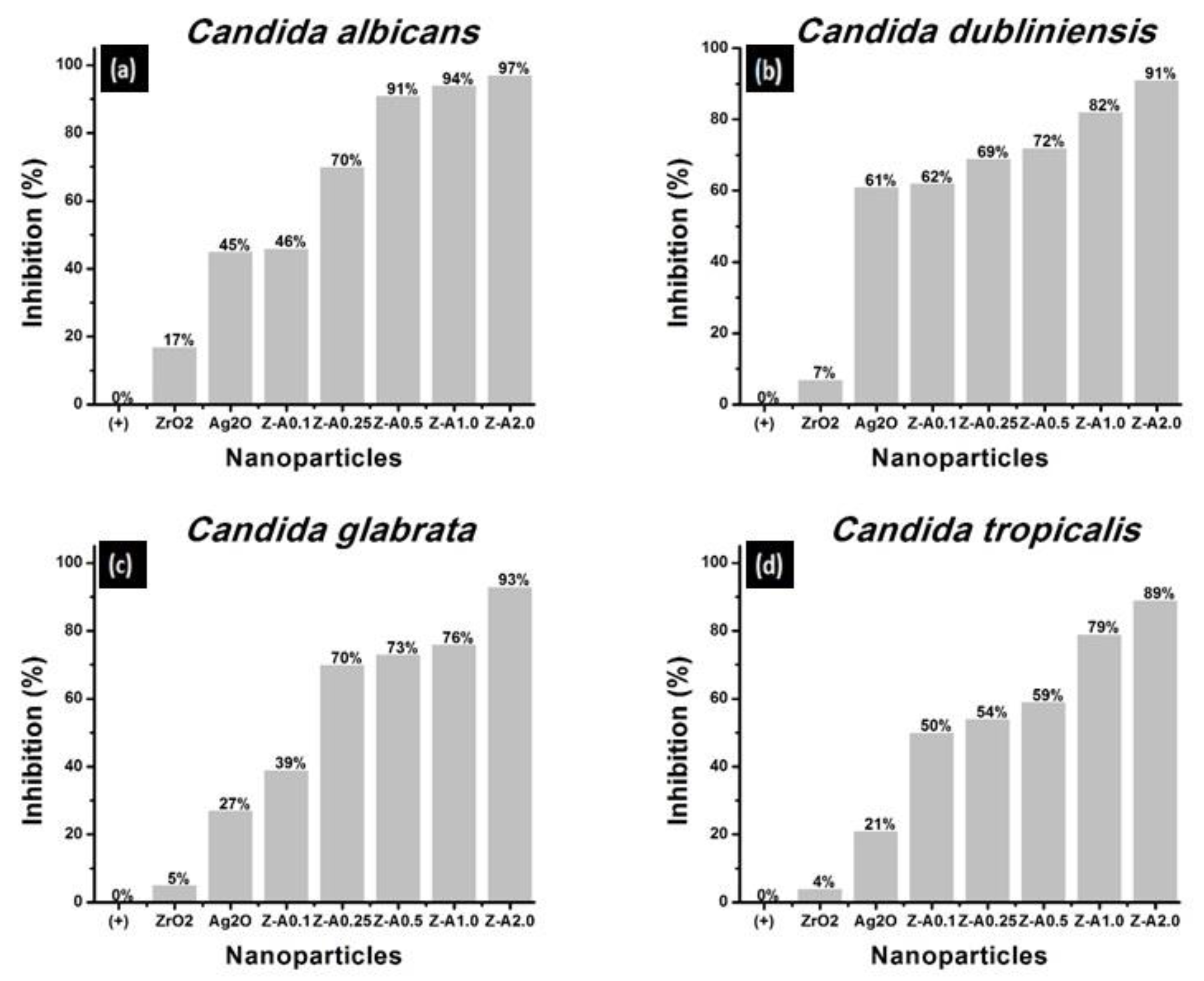
3.7. Evaluation of the Growth Inhibition of Candida spp.
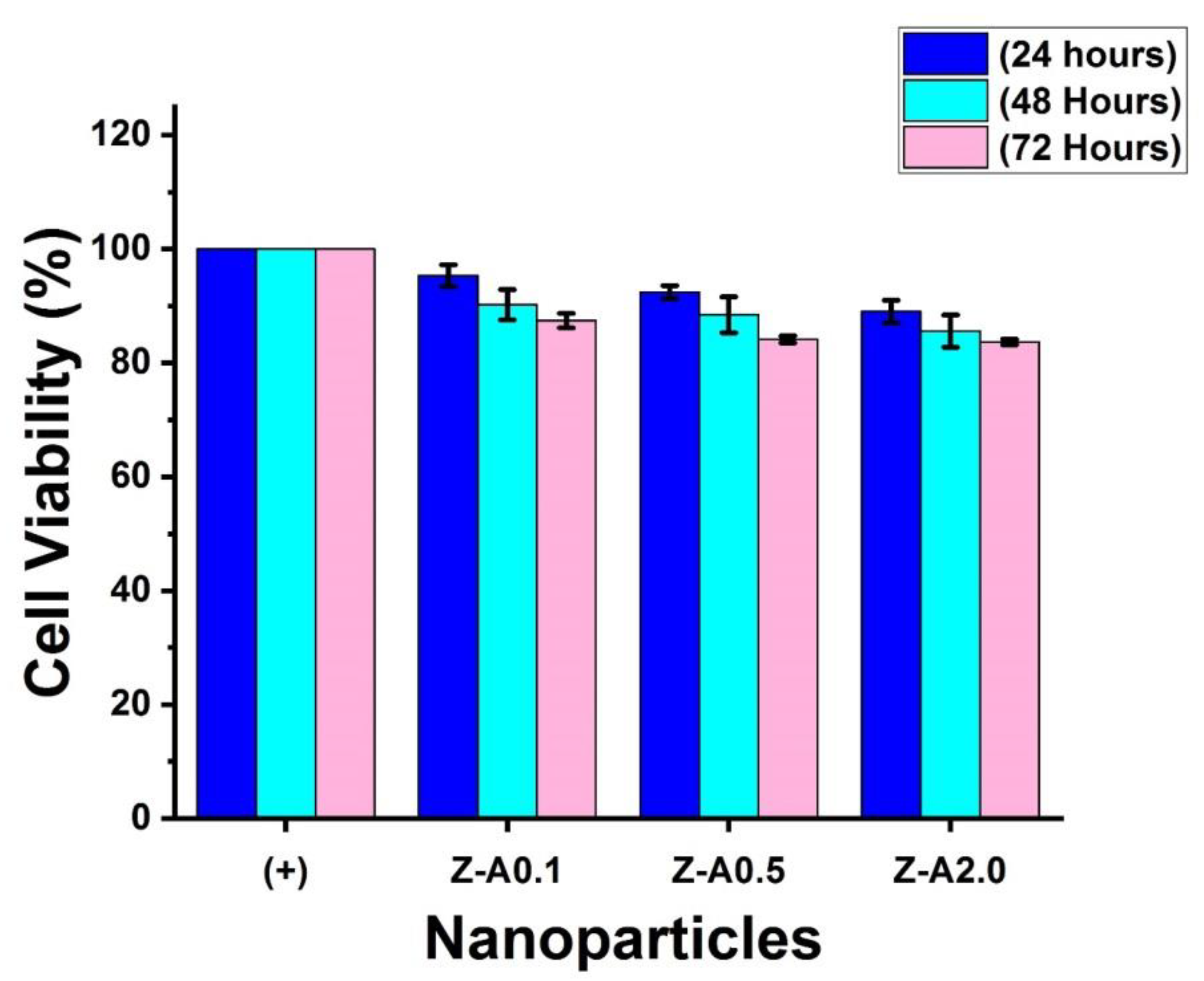
3.8. Effect of Z-A Nanoparticle on Cell Viability
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Artunduaga Bonilla, J.J.; Paredes Guerrero, D.J.; Sánchez Suárez, C.I.; Ortiz López, C.C.; Torres Sáez, R.G. In vitro antifungal activity of silver nanoparticles against fluconazole-resistant Candida species. World J. Microbiol. Biotechnol. 2015, 31, 1801–1809. [Google Scholar] [CrossRef]
- Owaid, M.N.; Raman, J.; Lakshmanan, H.; Al-Saeedi, S.S.S.; Sabaratnam, V.; Ali Abed, I. Mycosynthesis of silver nanoparticles by Pleurotus cornucopiae var. citrinopileatus and its inhibitory effects against Candida sp. Mater. Lett. 2015, 153, 186–190. [Google Scholar] [CrossRef]
- De Castro, R.D.; de Souza, T.M.P.A.; Bezerra, L.M.D.; Ferreira, G.L.S.; de Brito Costa, E.M.M.; Cavalcanti, A.L. Antifungal activity and mode of action of thymol and its synergism with nystatin against Candida species involved with infections in the oral cavity: An in vitro study. BMC Complement. Altern. Med. 2015, 15, 1–7. [Google Scholar] [CrossRef]
- Naglik, J.R.; Moyes, D.L.; Wächtler, B.; Hube, B. Candida albicans interactions with epithelial cells and mucosal immunity. Microbes Infect. 2011, 13, 963–976. [Google Scholar] [CrossRef]
- Bondaryk, M.; Kurzątkowski, W.; Staniszewska, M. Antifungal agents commonly used in the superficial and mucosal candidiasis treatment: Mode of action and resistance development. Postep. Dermatol. Alergol. 2013, 30, 293–301. [Google Scholar] [CrossRef]
- Perween, N.; Khan, H.M.; Fatima, N. Silver nanoparticles: An upcoming therapeutic agent for the resistant Candida infections. J. Microbiol. Exp. 2019, 7, 49–54. [Google Scholar] [CrossRef]
- Brayner, R.; Dahoumane, S.A.; Yéprémian, C.; Djediat, C.; Meyer, M.; Couté, A.; Fiévet, F. ZnO nanoparticles: Synthesis, characterization, and ecotoxicological studies. Langmuir 2010, 26, 6522–6528. [Google Scholar] [CrossRef]
- Gutiérrez, J.A.; Caballero, S.; Díaz, L.A.; Guerrero, M.A.; Ruiz, J.; Ortiz, C.C. High Antifungal Activity against Candida Species of Monometallic and Bimetallic Nanoparticles Synthesized in Nanoreactors. ACS Biomater. Sci. Eng. 2018, 4, 647–653. [Google Scholar] [CrossRef] [PubMed]
- Vivekanandhan, S.; Christensen, L.; Misra, M.; Kumar Mohanty, A. Green Process for Impregnation of Silver Nanoparticles into Microcrystalline Cellulose and Their Antimicrobial Bionanocomposite Films. J. Biomater. Nanobiotechnol. 2012, 3, 371–376. [Google Scholar] [CrossRef]
- Sundeep, D.; Vijaya Kumar, T.; Rao, P.S.S.; Ravikumar, R.V.S.S.N.; Gopala Krishna, A. Green synthesis and characterization of Ag nanoparticles from Mangifera indica leaves for dental restoration and antibacterial applications. Prog. Biomater. 2017, 6, 57–66. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.P.; Bhargava, C.S.; Dubey, V.; Mishra, A.; Singh, Y. Silver nanoparticles: Biomedical applications, toxicity, and safety issues. Int. J. Res. Pharm. Pharm. Sci. 2017, 2, 2455–2698. [Google Scholar]
- Gowri, S.; Rajiv Gandhi, R.; Sundrarajan, M. Structural, optical, antibacterial and antifungal properties of zirconia nanoparticles by biobased protocol. J. Mater. Sci. Technol. 2014, 30, 782–790. [Google Scholar] [CrossRef]
- Ayanwale, A.P.; Cornejo, A.D.; González, J.C.C.; Cristóbal, L.F.E.; López, S.Y.R. Review of the Synthesis, Characterization and Application of Zirconia Mixed Metal Oxide Nanoparticles. Int. J. Res. Granthaalayah 2018, 6, 136–145. [Google Scholar] [CrossRef]
- Karn-Orachai, K.; Sakamoto, K.; Laocharoensuk, R.; Bamrungsap, S.; Dharakul, T.; Miki, K. SERS-based immunoassay on 2D-arrays of Au@Ag core-shell nanoparticles: Influence of the sizes of the SERS probe and sandwich immunocomplex on the sensitivity. RSC Adv. 2017, 7, 14099–14106. [Google Scholar] [CrossRef]
- Panáček, A.; Kolář, M.; Večeřová, R.; Prucek, R.; Soukupová, J.; Kryštof, V.; Hamal, P.; Zbořil, R.; Kvítek, L. Antifungal activity of silver nanoparticles against Candida spp. Biomaterials 2009, 30, 6333–6340. [Google Scholar] [CrossRef] [PubMed]
- Precious Ayanwale, A.; Reyes-López, S.Y. ZrO2-ZnO Nanoparticles as Antibacterial Agents. ACS Omega 2019, 4, 19216–19224. [Google Scholar] [CrossRef]
- Ayanwale, A.P.; Ruíz-Baltazar, A. de J.; Espinoza-Cristóbal, L.; Reyes-López, S.Y. Bactericidal Activity Study of ZrO2-Ag2O Nanoparticles. Dose-Response 2020, 18, 1–13. [Google Scholar] [CrossRef]
- Muñoz-Escobar, A.; Reyes-López, S.Y. Antifungal susceptibility of Candida species to copper oxide nanoparticles on polycaprolactone fibers (PCL-CuONPs). PLoS ONE 2020, 15, e0228864. [Google Scholar] [CrossRef]
- Mota Ferreira, L.; Gehrcke, M.; Ferrari Cervi, V.; Eliete Rodrigues Bitencourt, P.; Ferreira da Silveira, E.; Hofstatter Azambuja, J.; Prates Ramos, A.; Nascimento, K.; Beatriz Moretto, M.; Braganhol, E.; et al. Pomegranate seed oil nanoemulsions with selective antiglioma activity: Optimization and evaluation of cytotoxicity, genotoxicity and oxidative effects on mononuclear cells. Pharm. Biol. 2016, 54, 2968–2977. [Google Scholar] [CrossRef]
- Mendoza, A.; Torres-Hernandez, J.A.; Ault, J.G.; Pedersen-Lane, J.H.; Gao, D.; Lawrence, D.A. Silica nanoparticles induce oxidative stress and inflammation of human peripheral blood mononuclear cells. Cell Stress Chaperones 2014, 19, 777–790. [Google Scholar] [CrossRef]
- Kumaresan, M.; Vijai Anand, K.; Govindaraju, K.; Tamilselvan, S.; Ganesh Kumar, V. Seaweed Sargassum wightii mediated preparation of zirconia (ZrO2) nanoparticles and their antibacterial activity against gram positive and gram negative bacteria. Microb. Pathog. 2018, 124, 311–315. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Liu, H.; Ma, Z. Flower-like Ag2O/Bi2MoO6 p-n heterojunction with enhanced photocatalytic activity under visible light irradiation. J. Mol. Catal. A Chem. 2016, 424, 37–44. [Google Scholar] [CrossRef]
- Negahdary, M.; Habibi-Tamijani, A.; Asadi, A.; Ayati, S. Synthesis of zirconia nanoparticles and their ameliorative roles as additives concrete structures. J. Chem. 2013, 2013, 314862. [Google Scholar] [CrossRef]
- Rani, S.; Aggarwal, M.; Kumar, M.; Sharma, S.; Kumar, D. Removal of methylene blue and rhodamine B from water by zirconium oxide/graphene. Water Sci. 2016, 30, 51–60. [Google Scholar] [CrossRef]
- Waterhouse, G.I.N.; Bowmaker, G.A.; Metson, J.B. The thermal decomposition of silver (I, III) oxide: A combined XRD, FT-IR and Raman spectroscopic study. Phys. Chem. Chem. Phys. 2001, 3, 3838–3845. [Google Scholar] [CrossRef]
- Gurunathan, S.; Jeong, J.K.; Han, J.W.; Zhang, X.F.; Park, J.H.; Kim, J.H. Multidimensional effects of biologically synthesized silver nanoparticles in Helicobacter pylori, Helicobacter felis, and human lung (L132) and lung carcinoma A549 cells. Nanoscale Res. Lett. 2015, 10, 1–17. [Google Scholar] [CrossRef]
- Kumari, M.; Giri, V.P.; Pandey, S.; Kumar, M.; Katiyar, R.; Nautiyal, C.S.; Mishra, A. An insight into the mechanism of antifungal activity of biogenic nanoparticles than their chemical counterparts. Pestic. Biochem. Physiol. 2019, 157, 45–52. [Google Scholar] [CrossRef]
- Kim, K.J.; Sung, W.S.; Suh, B.K.; Moon, S.K.; Choi, J.S.; Kim, J.G.; Lee, D.G. Antifungal activity and mode of action of silver nano-particles on Candida albicans. Biometals 2009, 22, 235–242. [Google Scholar] [CrossRef]
- Stankic, S.; Suman, S.; Haque, F.; Vidic, J. Pure and multi metal oxide nanoparticles: Synthesis, antibacterial and cytotoxic properties. J. Nanobiotechnol. 2016, 14, 73. [Google Scholar] [CrossRef]
- Sahu, D.; Kannan, G.M.; Tailang, M.; Vijayaraghavan, R. In Vitro Cytotoxicity of Nanoparticles: A Comparison between Particle Size and Cell Type. J. Nanosci. 2016, 2016, 1–9. [Google Scholar] [CrossRef]
- Babu, M.M.; Prasad, P.S.; Bindu, S.H.; Venkateswara Rao, P.; Govindan, N.P.; Veeraiah, N.; Özcan, M. Bioactivity, antibacterial activity and functionality of zirconia doped zinc phosphate bioglasses for application in dentistry. Mater. Sci. Eng. C 2020, 114, 111052. [Google Scholar] [CrossRef]
- El-Baz, A.F.; El-Batal, A.I.; Abomosalam, F.M.; Tayel, A.A.; Shetaia, Y.M.; Yang, S.T. Extracellular biosynthesis of anti-Candida silver nanoparticles using Monascus purpureus. J. Basic Microbiol. 2016, 56, 531–540. [Google Scholar] [CrossRef]
- Zielińska, A.; Kowalska, E.; Sobczak, J.W.; Łacka, I.; Gazda, M.; Ohtani, B.; Hupka, J.; Zaleska, A. Silver-doped TiO2 prepared by microemulsion method: Surface properties, bio- and photoactivity. Sep. Purif. Technol. 2010, 72, 309–318. [Google Scholar] [CrossRef]
- Rajamanickam, K.; Sudha, S.S.; Francis, M.; Sowmya, T.; Rengaramanujam, J.; Sivalingam, P.; Prabakar, K. Microalgae associated Brevundimonas sp. MSK 4 as the nano particle synthesizing unit to produce antimicrobial silver nanoparticles. Spectrochim. Acta Part A Mol. Biomol. Spectrosc. 2013, 113, 10–14. [Google Scholar] [CrossRef] [PubMed]
- Khan, N.T.; Mushtaq, M. Determination of Antifungal Activity of Silver Nanoparticles Produced from Aspergillus niger. Biol. Med. 2016, 9, 1–4. [Google Scholar] [CrossRef]
- Fernández, E.; Benito, J.M.; Pazos, C.; Coca, J. Ceramic membrane ultrafiltration of anionic and nonionic surfactant solutions. J. Memb. Sci. 2005, 246, 1–6. [Google Scholar] [CrossRef]
- Kvitek, L.; Vanickova, M.; Panacek, A.; Soukupov, J.; Dittrich, M.; Valentova, E.; Prucek, R.; Bancirova, M.; Milde, D.; Zboril, R. Initial study on the toxicity of silver nanoparticles (NPs) against Paramecium caudatum. J. Phys. Chem. C 2009, 113, 4296–4300. [Google Scholar] [CrossRef]


| Materials | C. albicans | C. dubliniensis | C. glabrata | C. tropicalis |
|---|---|---|---|---|
| ZrO2 | 0 | 0 | 0 | 0 |
| Ag2O | 8.7 ± 0.6 | 6.3 ± 0.6 | 6.0 ± 1.0 | 8.0 ± 1.0 |
| Z-A0.1 | 9.0 ± 1.0 | 6.6 ± 1.0 | 6.3 ± 1.5 | 8.2 ± 1.5 |
| Z-A0.25 | 12.3 ± 0.6 | 7.3 ± 0.6 | 8.7 ± 2.5 | 8.7 ± 1.2 |
| Z-A0.5 | 13.3 ± 0.6 | 9.0 ± 1.0 | 10.3 ± 2.5 | 10.3 ± 0.6 |
| Z-A1.0 | 14.0 ± 1.0 | 10.7 ± 0.6 | 14.3 ± 1.5 | 13.7 ± 0.6 |
| Z-A2.0 | 18.3 ± 0.6 | 13.7 ± 1.5 | 17.0 ± 1.0 | 16.7 ± 0.6 |
| Fungi | Material | Conc. | Inhibition Zone | References |
|---|---|---|---|---|
| C. albicans | Ag + M. purpureus | 1 mM | 16.7 ± 0.25 | [32] |
| C. albicans | Ag-TiO2 | 8.5% Ag | 11 | [33] |
| C. albicans | Ag | 1 mM | 10 | [34] |
| C. albicans | Ag | 80 µL | 10 | [35] |
| C. albicans | Z-A2.0 | 1:2 | 18.3 ± 0.6 | Present work |
| C. glabrata | Ag + M. purpureus | 1 mM | 18.7 ± 0.37 | [32] |
| C. glabrata | Ag-TiO2 | 8.5% Ag | 15 | [33] |
| C. glabrata | Ag | 80 µL | 9 | [34] |
| C. glabrata | Z-A2.0 | 1:2 | 17 ± 1.0 | Present work |
| C. tropicalis | Ag + M. purpureus | 1 mM | 16.0 ± 0.44 | [32] |
| C. tropicalis | Ag-TiO2 | 8.5% Ag | 15 | [33] |
| C. tropicalis | Ag | 1 mM | 9 | [34] |
| C. tropicalis | Ag | 80 µL | 9 | [35] |
| C. tropicalis | Z-A2.0 | 1:2 | 16.7 ± 0.6 | Present work |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ayanwale, A.P.; Estrada-Capetillo, B.L.; Reyes-López, S.Y. Evaluation of Antifungal Activity by Mixed Oxide Metallic Nanocomposite against Candida spp. Processes 2021, 9, 773. https://doi.org/10.3390/pr9050773
Ayanwale AP, Estrada-Capetillo BL, Reyes-López SY. Evaluation of Antifungal Activity by Mixed Oxide Metallic Nanocomposite against Candida spp. Processes. 2021; 9(5):773. https://doi.org/10.3390/pr9050773
Chicago/Turabian StyleAyanwale, Ayodeji Precious, Brenda Lizbeth Estrada-Capetillo, and Simón Yobanny Reyes-López. 2021. "Evaluation of Antifungal Activity by Mixed Oxide Metallic Nanocomposite against Candida spp." Processes 9, no. 5: 773. https://doi.org/10.3390/pr9050773
APA StyleAyanwale, A. P., Estrada-Capetillo, B. L., & Reyes-López, S. Y. (2021). Evaluation of Antifungal Activity by Mixed Oxide Metallic Nanocomposite against Candida spp. Processes, 9(5), 773. https://doi.org/10.3390/pr9050773







