Spray Drying for the Preparation of Nanoparticle-Based Drug Formulations as Dry Powders for Inhalation
Abstract
1. Introduction
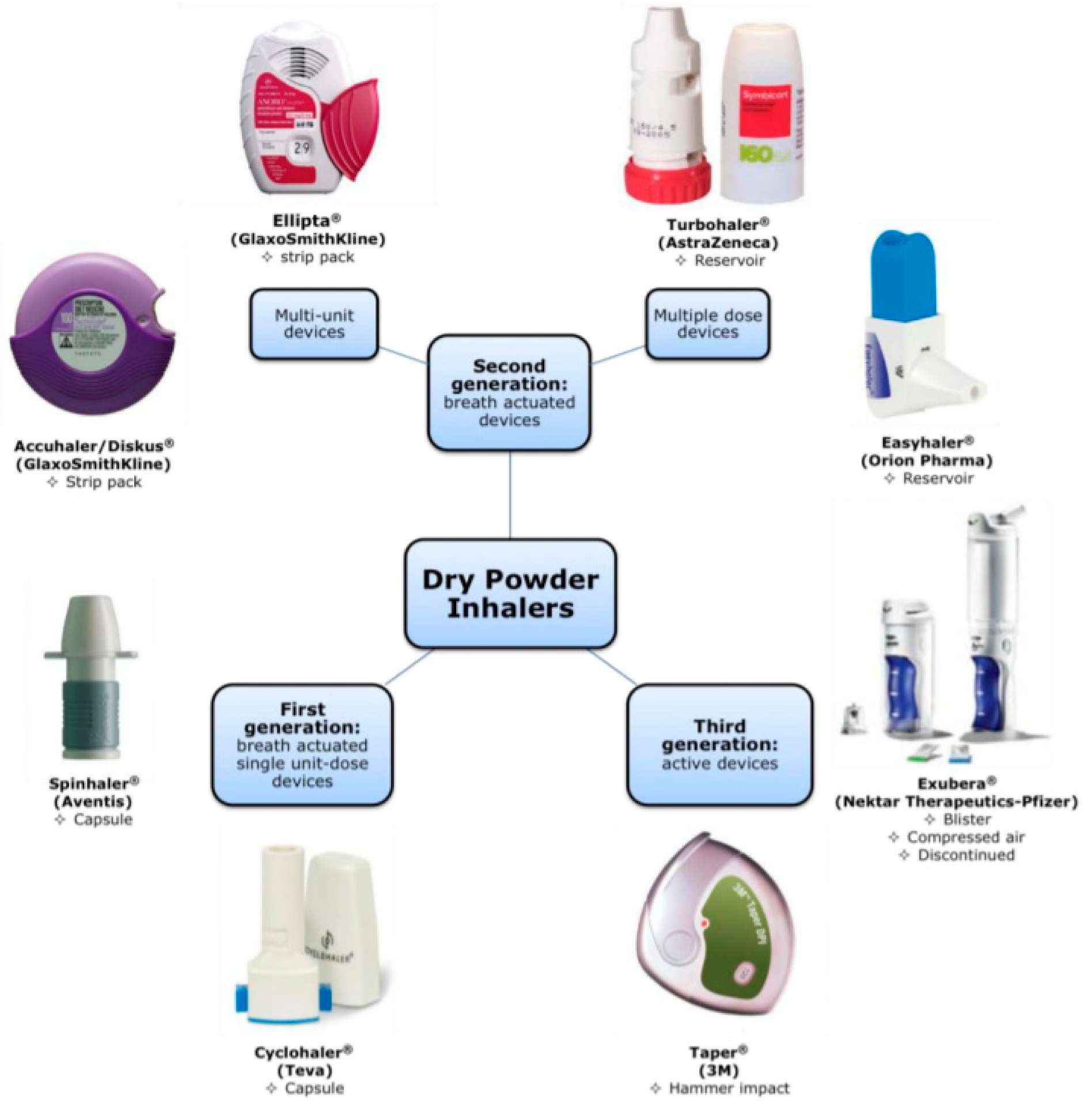
Pulmonary Drug Delivery Using Dry Powder Inhalers
2. Formulations for DPIs Based on Nanoparticle Engineering
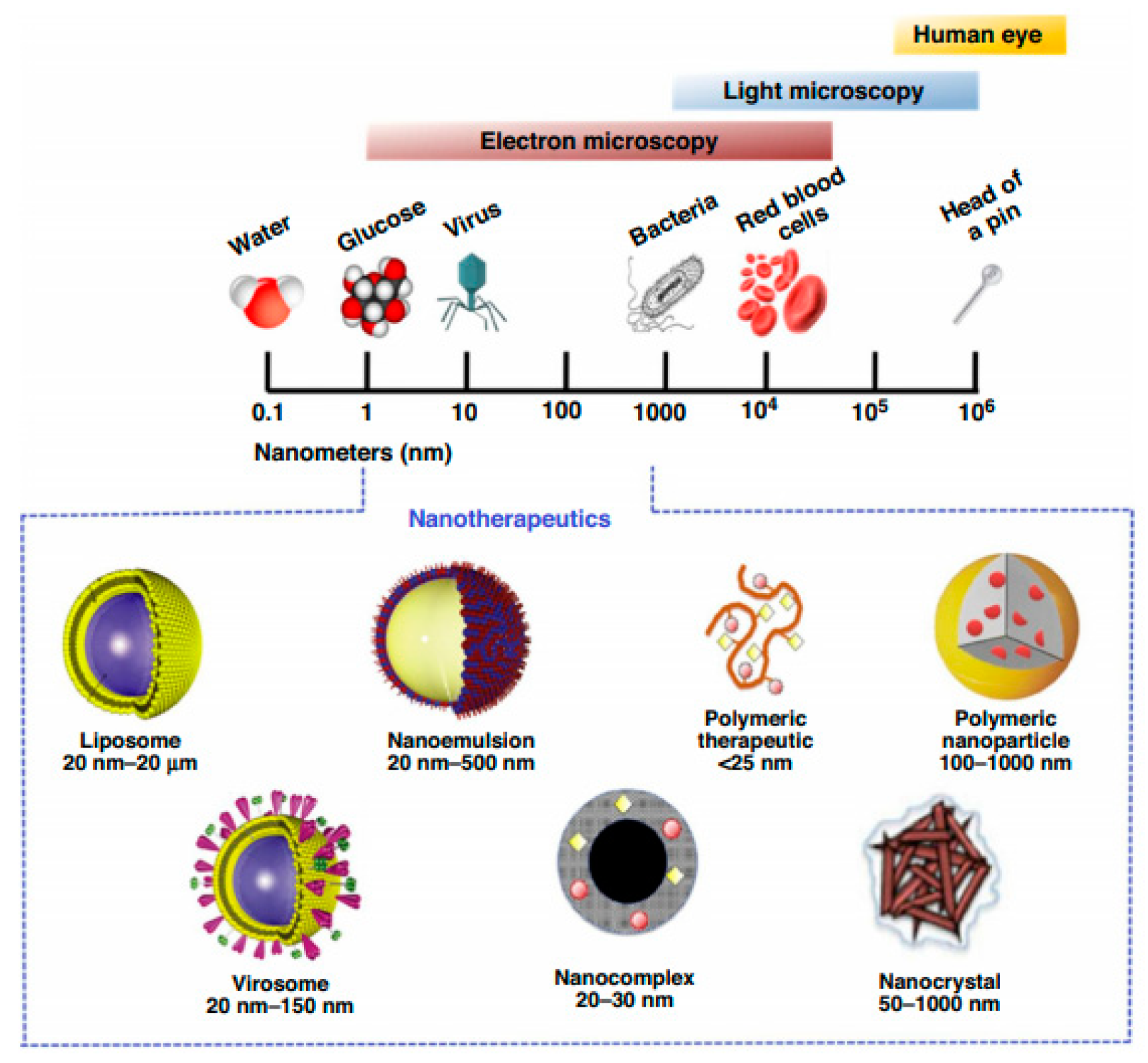
2.1. Nanoparticles in Pulmonary Drug Delivery
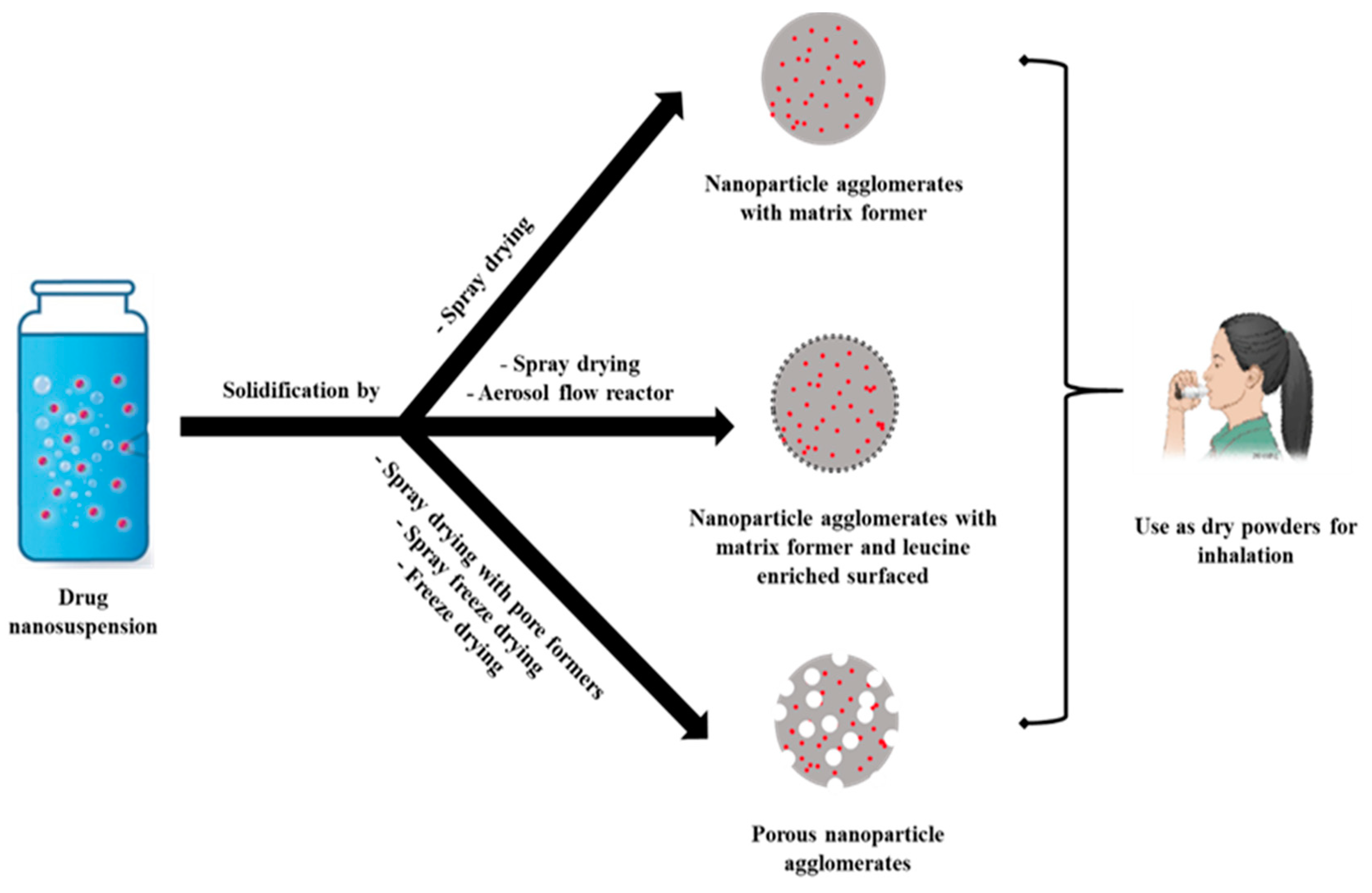
2.2. Nanoparticle-Based Dry Powders for Inhalation
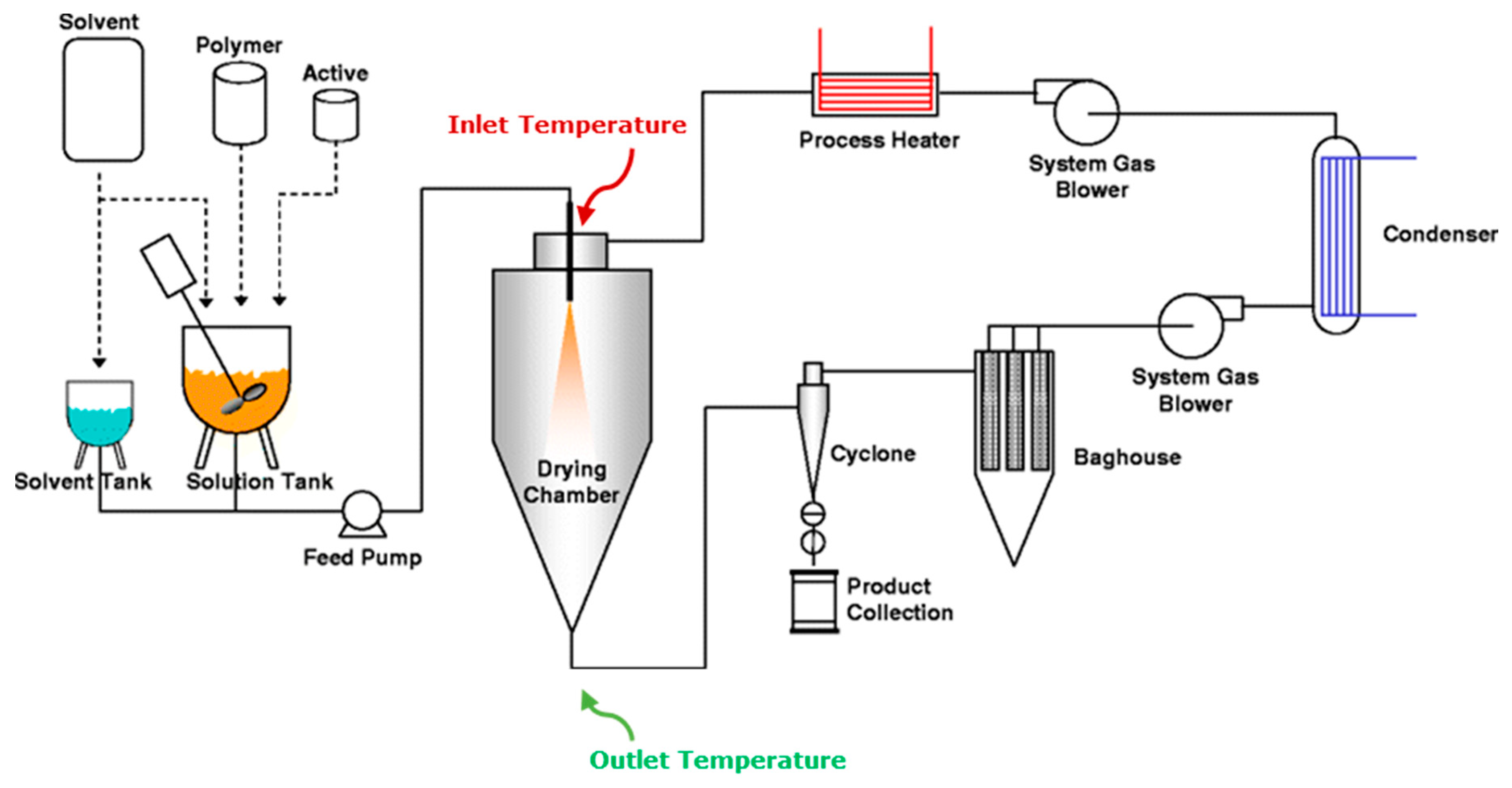
3. Particle Engineering Using Spray Drying
3.1. Liquid Feedstock Preparation
3.2. Atomisation
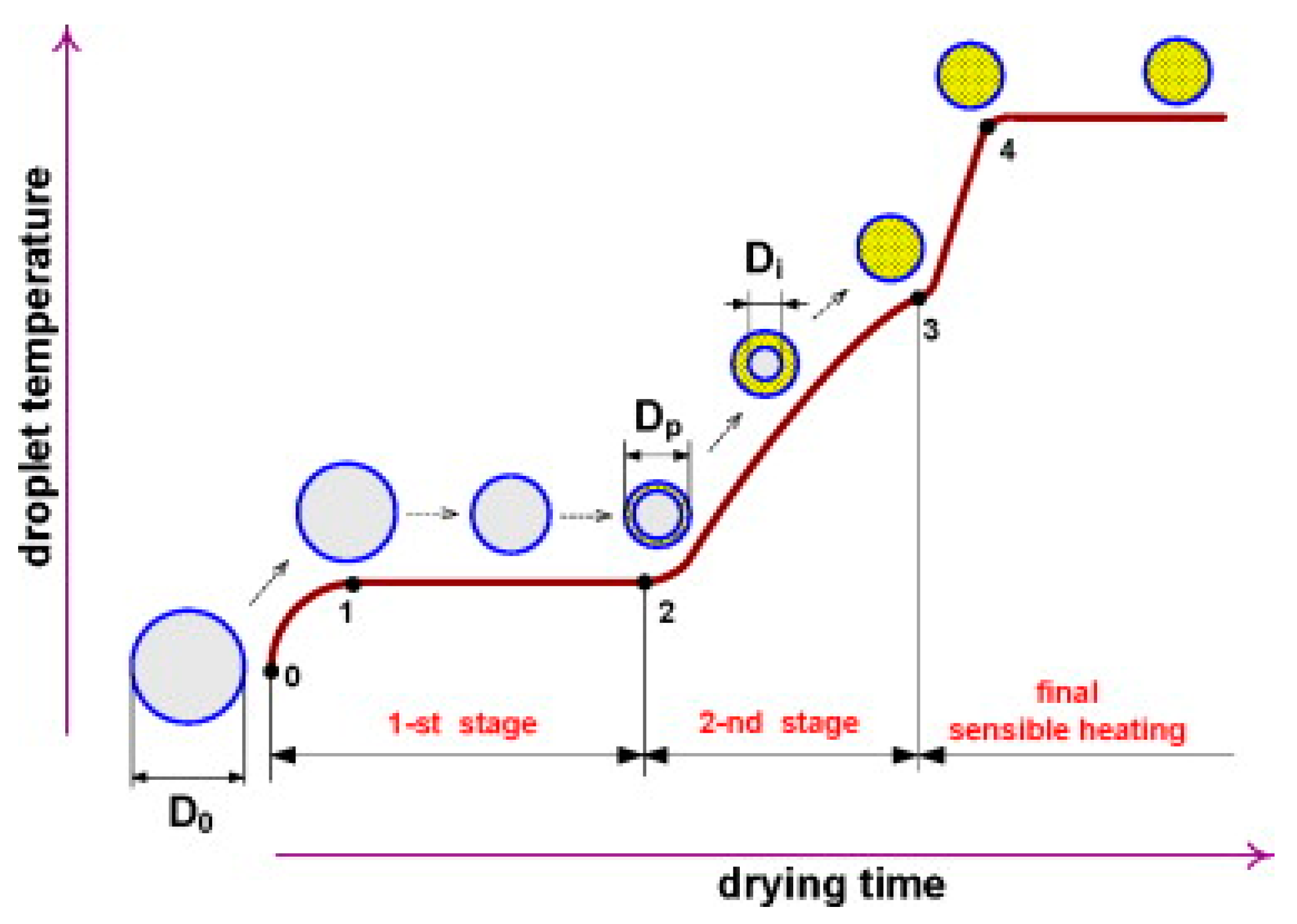
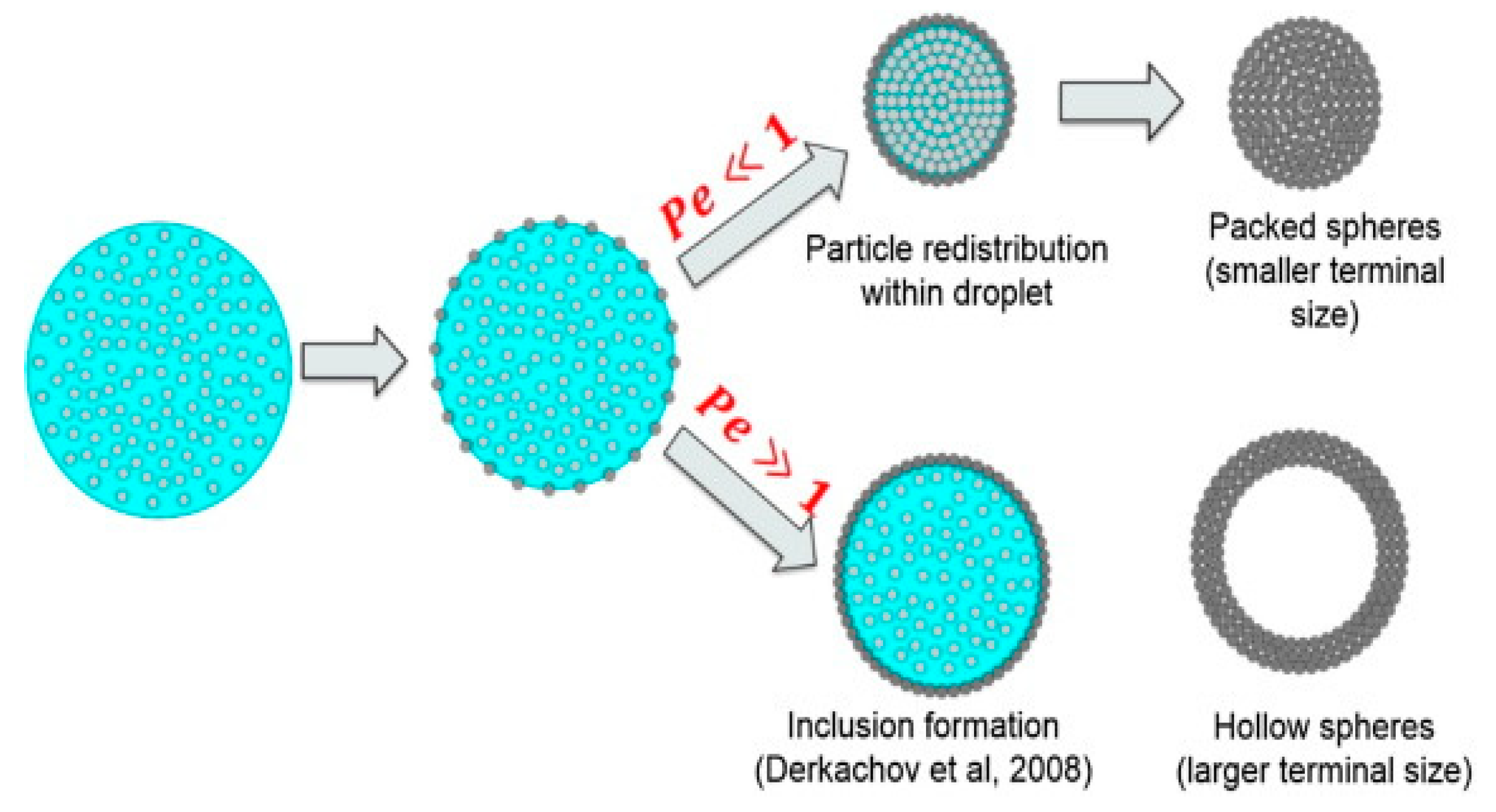
3.3. Drying
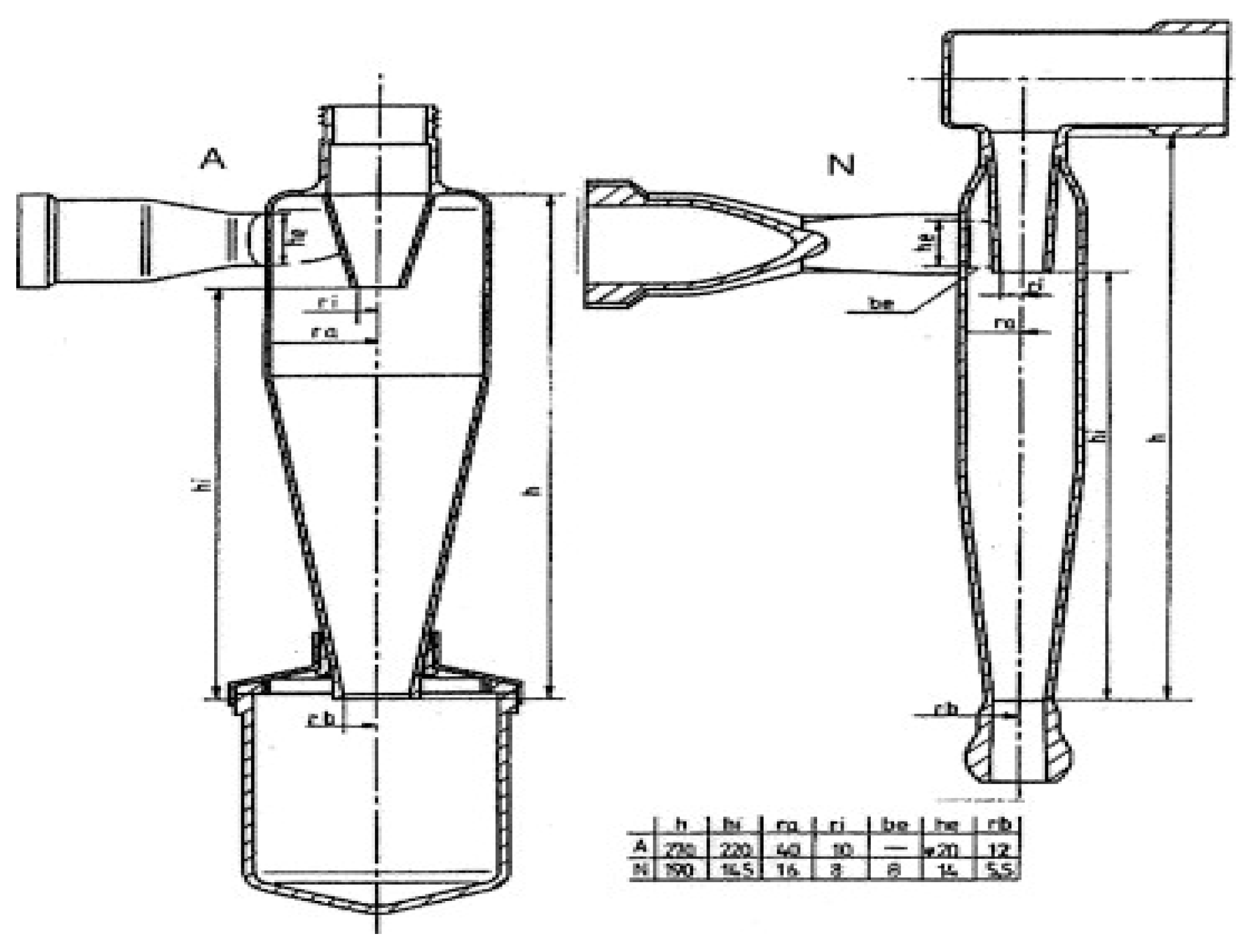
3.4. Separation
4. Studies on Inhalable Nanoparticle-Based Drug Formulations Produced by Spray Drying
4.1. Nanoporous Microparticles (NPMPs)
4.2. Nanocrystalline Agglomerates
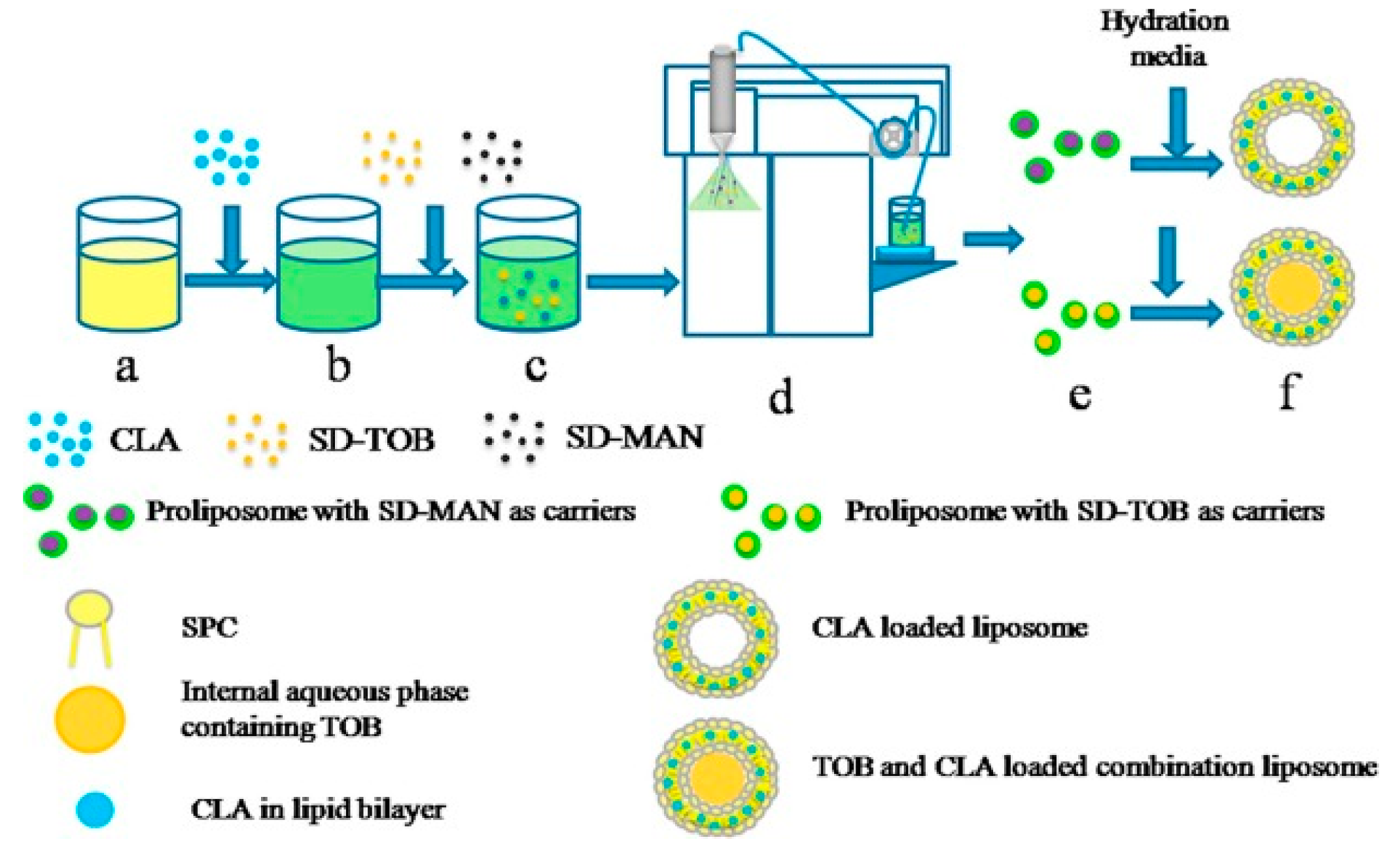
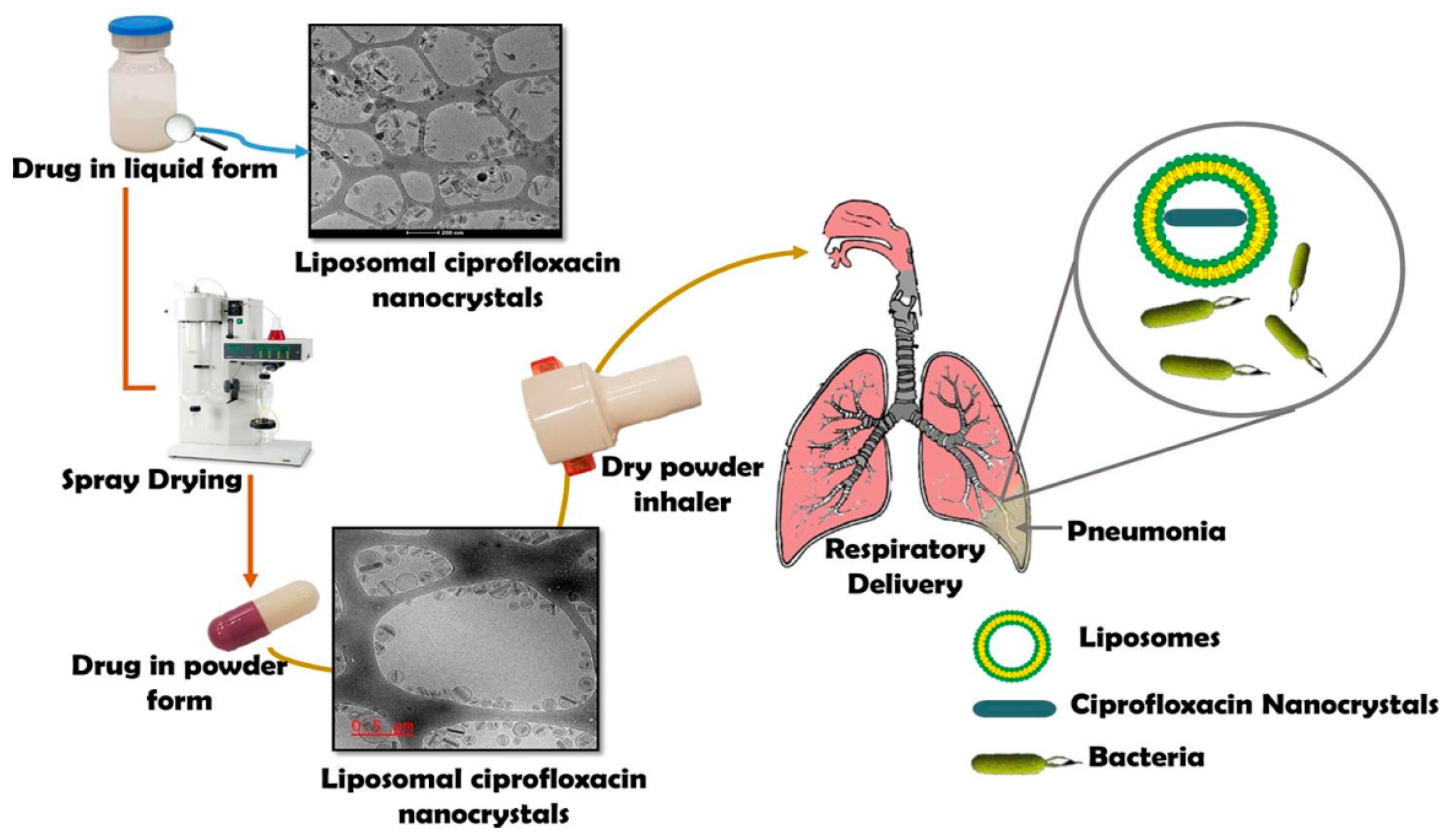
4.3. Proliposomes, Solid Lipid Nanoparticles and Nanocrystal Liposomal Powders
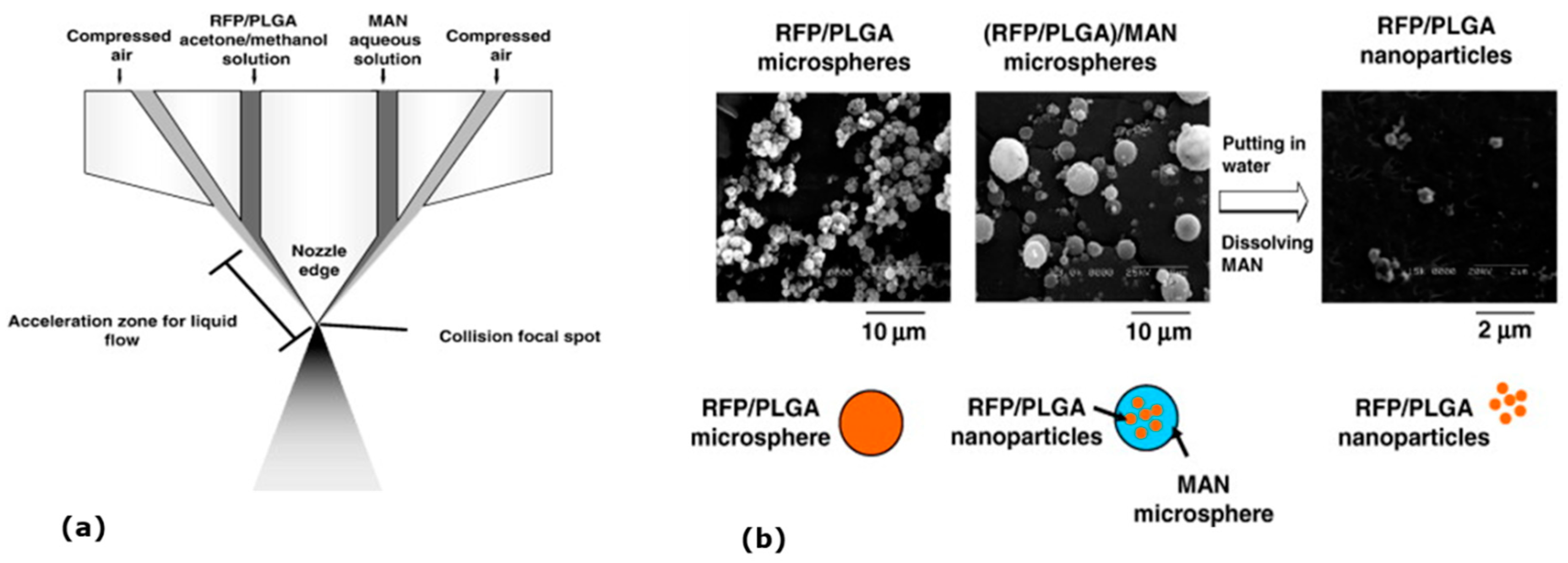
4.4. Polymeric Nanoparticles
5. Application of Alternative Spray-Drying Techniques
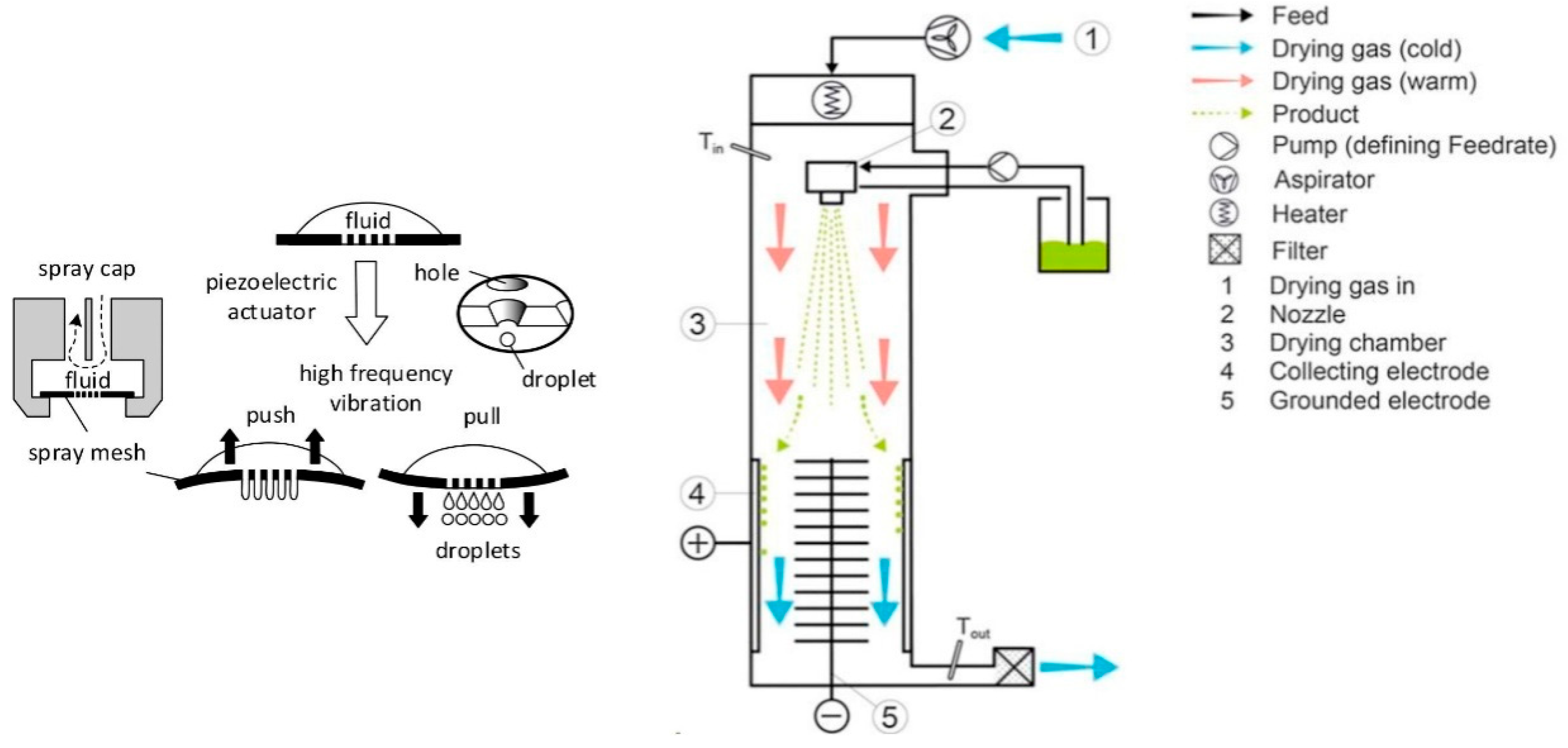
5.1. Nano Spray Drying
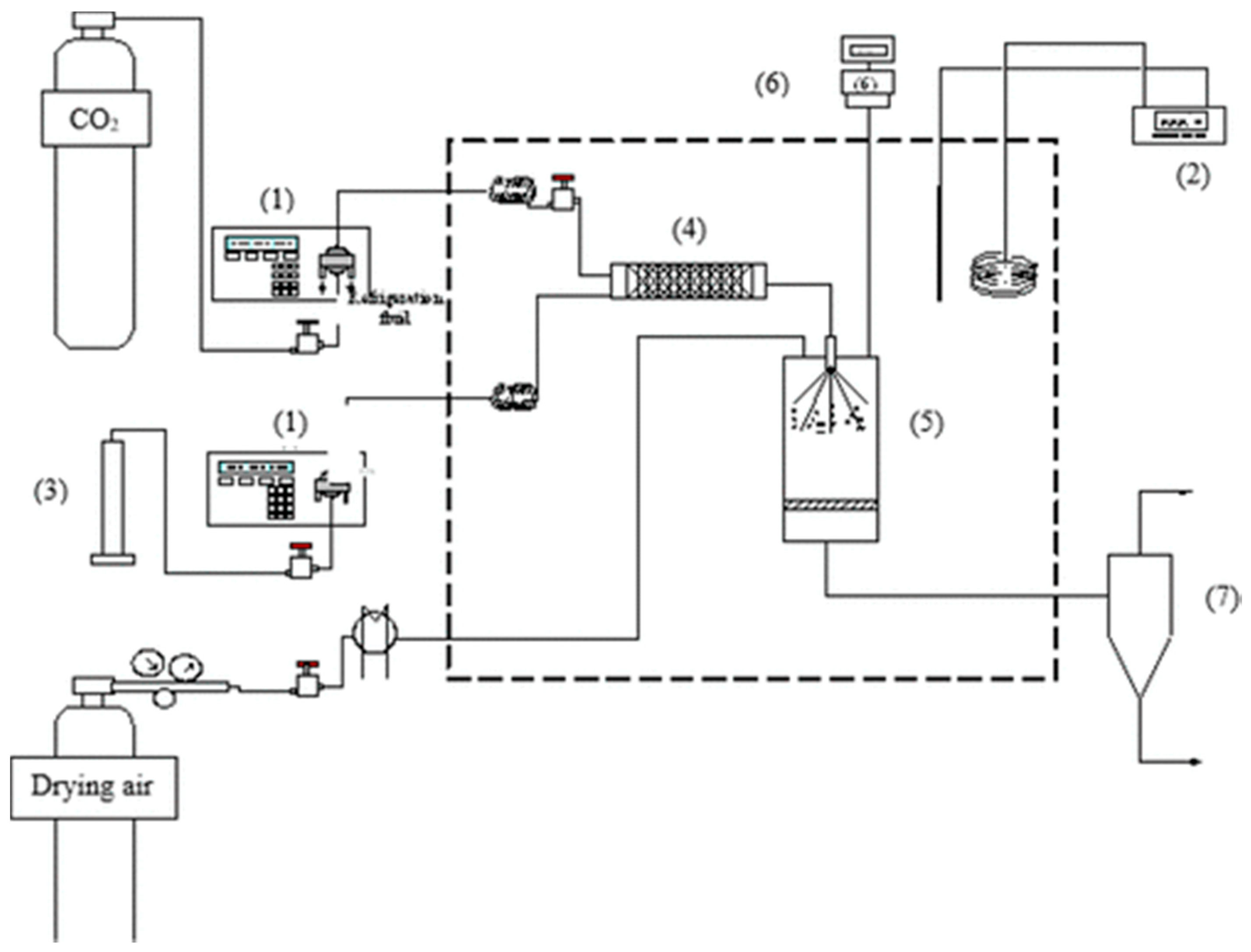
5.2. Supercritical CO2-Assisted Spray Drying
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Anselmo, A.C.; Gokarn, Y.; Mitragotri, S. Non-invasive delivery strategies for biologics. Nat. Rev. Drug Discov. 2019, 18, 19–40. [Google Scholar] [CrossRef]
- Murnane, D.; Hutter, V.; Harang, M. Pharmaceutical aerosols and pulmonary drug delivery. In Aerosol Science: Technology and Applications, 1st ed.; Coldbeck, I., Lazaridis, M., Eds.; John Wiley and Sons: Hoboken, NJ, USA, 2014; pp. 221–269. [Google Scholar]
- Jabbal, S.; Poli, G.; Lipworth, B. Does size really matter? Relationship of particle size to lung deposition and exhaled fraction. J. Allergy Clin. Immunol. 2017, 139, 2013–2014.e2011. [Google Scholar] [CrossRef] [PubMed]
- Heyder, J. Deposition of inhaled particles in the human respiratory tract and consequences for regional targeting in respiratory drug delivery. Proc. Am. Thorac. Soc. 2004, 1, 315–320. [Google Scholar] [CrossRef] [PubMed]
- Tatkare, D. Copd and Asthma Devices Market by Inhalers Type (Drug Powder, Metered Dose, Soft Mist), Nebulizers (Compressor, Ultrasonic, Mesh). Available online: https://www.alliedmarketresearch.com/COPD-asthma-devices-market (accessed on 21 May 2020).
- Malamatari, M. Engineering Nanoparticle Agglomerates as Dry Powders for Pulmonary Drug Delivery; UCL (University College London): London, UK, 2016. [Google Scholar]
- Darquenne, C. Aerosol Deposition in health and disease. J. Aerosol Med. Pulm. Drug Deliv. 2012, 25, 140–147. [Google Scholar] [CrossRef] [PubMed]
- Kourmatzis, A.; Cheng, S.; Chan, H.K. Airway geometry, airway flow, and particle measurement methods: Implications on pulmonary drug delivery. Expert Opin. Drug Deliv. 2018, 15, 271–282. [Google Scholar] [CrossRef]
- Martin, R.A.; Moore, C.P.; Finlay, W.H. Models of deposition, pharmacokinetics, and intersubject variability in respiratory drug delivery. Expert Opin. Drug Deliv. 2018, 15, 1175–1188. [Google Scholar] [CrossRef]
- He, Y.; Liang, Y.; Han, R.; Lu, W.L.; Wo Mak, J.C.; Zheng, Y. Rational particle design to overcome pulmonary barriers for obstructive lung diseases therapy. J. Control. Release 2019, 314, 48–61. [Google Scholar] [CrossRef]
- Islam, N.; Gladki, E. Dry powder inhalers (DPIs)—A review of device reliability and innovation. Int. J. Pharm. 2018, 360, 1–11. [Google Scholar] [CrossRef]
- Islam, N.; Cleary, M.J. Developing an efficient and reliable dry powder inhaler for pulmonary drug delivery—A review for multidisciplinary researchers. Med. Eng. Phys. 2012, 34, 409–427. [Google Scholar] [CrossRef]
- Hoppentocht, M.; Hagedoorn, P.; Frijlink, H.W.; de Boer, A.H. Technological and practical challenges of dry powder inhalers and formulations. Adv. Drug Deliv. Rev. 2014, 75, 18–31. [Google Scholar] [CrossRef]
- De Boer, A.H.; Hagedoorn, P.; Hoppentocht, M.; Buttini, F.; Grasmeijer, F.; Frinjlink, H.W. Dry Powder Inhalation: Past, Present and Future. Expert Opin. Drug Deliv. 2017, 14, 499–512. [Google Scholar] [CrossRef] [PubMed]
- Buttini, F.; Rozou, S.; Rossi, A.; Zoumpliou, V.; Rekkas, D.M. The application of Quality by Design framework in the pharmaceutical development of dry powder inhalers. Eur. J. Pharm. Sci. 2018, 13, 64–76. [Google Scholar] [CrossRef] [PubMed]
- Levy, M.L.; Carroll, W.; Izquierdo Alonso, J.L.; Keller, C.; Lavorini, F.; Lehtimaki, L. Understanding Dry Powder Inhalers: Key Technical and Patient Preference Attributes. Adv. Ther. 2019, 36, 2547–2557. [Google Scholar] [CrossRef] [PubMed]
- Pilcer, G.; Amighi, K. Formulation strategy and use of excipients in pulmonary drug delivery. Int. J. Pharm. 2010, 392, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Al-Hallak, M.H.D.K.; Sarfaz, M.K.; Azarmi, S.; Roa, W.H.; Finlay, W.H.; Lobenberg, R. Pulmonary delivery of inhalable nanoparticles: Dry powder inhalers. Ther. Deliv. 2011, 2, 1313–1324. [Google Scholar] [CrossRef] [PubMed]
- Healy, A.M.; Amaro, M.I.; Paluch, K.J.; Tajber, L. Dry powders for oral inhalation free of lactose carrier particles. Adv. Drug Deliv. Rev. 2014, 75, 32–52. [Google Scholar] [CrossRef] [PubMed]
- Gradon, L.; Sosnowski, T.R. Formation of particles for dry powder inhalers. Adv. Powder Technol. 2014, 25, 43–55. [Google Scholar] [CrossRef]
- Brunaugh, A.D.; Smyth, H.D.C. Formulation Techniques for High Dose Dry Powders. Int. J. Pharm. 2018, 25, 489–498. [Google Scholar] [CrossRef]
- Hadiwinoto, G.D.; Kwok, P.C.L.; Lakerveld, R. A Review on Recent Technologies for the Manufacture of Pulmonary Drugs. Ther. Deliv. 2018, 9, 47–70. [Google Scholar] [CrossRef]
- Nikolakakis, I.; Newton, J.M. Solid state adsorption of antibiotics onto sorbitol. J. Pharm. Pharmacol. 1989, 41, 145–148. [Google Scholar] [CrossRef]
- Nikolakakis, I.; Newton, J.M.; Malamataris, S. Solid state ‘adsorption’ of fine antibiotic powders onto sorbitol: Effects of particle size, state of sorbed water and surface free energy characteristics. Eur. J. Pharm. Sci. Offic. J. Eur. Fed. Pharm. Sci. 2002, 17, 229–238. [Google Scholar] [CrossRef]
- Grasmeijer, F.; Grasmeijer, N.; Hagedoorn, P.; Frijlink, H.W.; Haaije de Boer, A. Recent advances in the fundamental understanding of adhesive mixtures for inhalation. Curr. Pharm. Des. 2015, 21, 5900–5914. [Google Scholar] [CrossRef] [PubMed]
- Keck, C.M.; Müller, R.H. Drug nanocrystals of poorly soluble drugs produced by high pressure homogenisation. Eur. J. Pharm. Biopharm. Offic. J. Arb. Fur Pharm. Verfahr. E.V 2006, 62, 3–16. [Google Scholar] [CrossRef] [PubMed]
- Nikolakakis, I.; Pilpel, N. Effect of particle shape on the tensile strengths of powders. Powder Technol. 1985, 42, 279–283. [Google Scholar] [CrossRef]
- Florence, A.T.; Attwood, D. Physicochemical principles of pharmacy. In Manufacture, Formulation and Clinical Use; Pharmaceutical Press: London, UK, 2015. [Google Scholar]
- Buckton, G.; Beezer, A.E. The relationship between particle size and solubility. Int. J. Pharm. 1992, 82, R7–R10. [Google Scholar] [CrossRef]
- Williams, H.D.; Trevaskis, N.L.; Charman, S.A.; Shanker, R.M.; Charman, W.N.; Pouton, C.W.; Porter, C.J.H. Strategies to address low drug solubility in discovery and development. Pharmacol. Rev. 2013, 65, 315–499. [Google Scholar] [CrossRef]
- Malamatari, M.; Taylor, K.M.G.; Malamataris, S.; Douroumis, D.; Kachrimanis, K. Pharmaceutical nanocrystals: Production by wet milling and applications. Drug Discov. Today 2018, 23, 534–547. [Google Scholar] [CrossRef]
- Iyer, R.; Hsia, C.C.; Nguyen, K.T. Nano-therapeutics for the lung: State-of-the-art and future perspectives. Curr. Pharm. Des. 2015, 21, 5233–5244. [Google Scholar] [CrossRef]
- Tolman, J.A.; Williams, R.O. Advances in the pulmonary delivery of poorly water-soluble drugs: Influence of solubilization on pharmacokinetic properties. Drug Dev. Ind. Pharm. 2010, 36, 1–30. [Google Scholar] [CrossRef]
- Wu, L.; Zhang, J.; Watanabe, W. Physical and chemical stability of drug nanoparticles. Adv. Drug Deliv. Rev. 2011, 63, 456–469. [Google Scholar] [CrossRef]
- Rogueda, P.G.A.; Traini, D. The nanoscale in pulmonary delivery. Part 1: Deposition, fate, toxicology and effects. Expert Opin. Drug Deliv. 2007, 4, 595–606. [Google Scholar] [CrossRef] [PubMed]
- Watts, A.; Williams, R. Nanoparticles for pulmonary delivery. In Controlled Pulmonary Drug Delivery; Springer: Berlin/Heidelberg, Germany, 2011; pp. 335–366. [Google Scholar]
- El-Gendy, N.; Gorman, E.M.; Munson, E.J.; Berkland, C. Budesonide nanoparticle agglomerates as dry powder aerosols with rapid dissolution. J. Pharm. Sci. 2009, 98, 2731–2746. [Google Scholar] [CrossRef]
- Muralidharan, P.; Malapit, M.; Mallory, E.; Hayes, D., Jr.; Mansour, H.M. Inhalable nanoparticulate powders for respiratory delivery. Nanomed. Nanotechnol. Biol. Med. 2015, 11, 1189–1199. [Google Scholar] [CrossRef]
- Malamatari, M.; Somavarapu, S.; Taylor, K.M.G.; Buckton, G. Solidification of nanosuspensions for the production of solid oral dosage forms and inhalable dry powders. Expert Opin. Dry Deliv. 2016, 13, 435–450. [Google Scholar] [CrossRef] [PubMed]
- Silva, A.S.; Tavares, M.T.; Aguiar-Ricardo, A. Sustainable strategies for nano-in-micro particle engineering for pulmonary delivery. J. Nanoparticle Res. 2014, 16, 2602. [Google Scholar] [CrossRef]
- Vehring, R.; Snyder, H.; Lechuga-Ballesteros, D. Spray drying. In Drying Technologies for Biotechnology and Pharmaceutical Applications, 1st ed.; Ohtake, S., Izutsu, K., Lechuga-Ballesteros, D., Eds.; Wiley-VCH Verlag GmbH: Weinheim, Germany, 2020; pp. 179–216. [Google Scholar]
- Partheniadis, I.; Karakasidou, P.; Vergkizi, S.; Nikolakakis, I. Spectroscopic examination and release of microencapsulated oregano essential oil. Admet Dmpk 2017, 5, 224–233. [Google Scholar] [CrossRef]
- Vehring, R. Pharmaceutical particle engineering via spray drying. Pharm. Res. 2008, 25, 999–1022. [Google Scholar] [CrossRef]
- Masters, K. The Spray Drying Handbook; Longman Scientific Publication: New York, NY, USA, 1991; pp. 329–556. [Google Scholar]
- Dobry, D.E.; Settell, D.M.; Baumann, J.M.; Ray, R.J.; Graham, L.J.; Beyerinck, R.A. A model-based methodology for spray-drying process development. J. Pharm. Innov. 2009, 4, 133–142. [Google Scholar] [CrossRef] [PubMed]
- Elversson, J.; Millqvist-Fureby, A. Particle size and density in spray drying—Effects of carbohydrate properties. J. Pharm. Sci. 2015, 94, 2049–2060. [Google Scholar] [CrossRef] [PubMed]
- Cheow, W.S.; Li, S.; Hadinoto, K. Spray drying formulation of hollow spherical aggregates of silica nanoparticles by experimental design. Chem. Eng. Res. Des. 2010, 88, 673–685. [Google Scholar] [CrossRef]
- Kemp, I.C.; Wadley, R.; Hartwig, T.; Cocchini, U.; See-Toh, Y.; Gorringe, L.; Fordham, K.; Ricard, F. Experimental study of spray drying and atomization with a two-fluid nozzle to produce inhalable particles. Dry. Technol. 2013, 31, 930–941. [Google Scholar] [CrossRef]
- Mezhericher, M.; Levy, A.; Borde, I. Spray drying modelling based on advanced droplet drying kinetics. Chem. Eng. Process. Process Intensif. 2010, 49, 1205–1213. [Google Scholar] [CrossRef]
- Osman, A.; Goehring, L.; Patti, A.; Stitt, H.; Shokri, N. Fundamental investigation of the drying of solid suspensions. Ind. Eng. Chem. Res. 2017, 56, 10506–10513. [Google Scholar] [CrossRef]
- Tsapis, N.; Bennett, D.; Jackson, B.; Weitz, D.A.; Edwards, D.A. Trojan particles: Large porous carriers of nanoparticles for drug delivery. Proc. Natl. Acad. Sci. USA 2002, 99, 12001–12005. [Google Scholar] [CrossRef] [PubMed]
- Wei, Y.; Deng, W.; Chen, R.-H. Effects of insoluble nano-particles on nanofluid droplet evaporation. Int. J. Heat Mass Transf. 2016, 97, 725–734. [Google Scholar] [CrossRef]
- Torge, A.; Grützmacher, P.; Mücklich, F.; Schneider, M. The influence of mannitol on morphology and disintegration of spray-dried nano-embedded microparticles. Eur. J. Pharm. Sci. 2017, 104, 171–179. [Google Scholar] [CrossRef] [PubMed]
- Maa, Y.F.; Nguyen, P.A.; Sit, K.; Hsu, C.C. Spray-drying performance of a bench-top spray dryer for protein aerosol powder preparation. Biotechnol. Bioeng. 1998, 60, 301–309. [Google Scholar] [CrossRef]
- Maury, M.; Murphy, K.; Kumar, S.; Shi, L.; Lee, G. Effects of process variables on the powder yield of spray-dried trehalose on a laboratory spray-dryer. Eur. J. Pharm. Biopharm. 2005, 59, 565–573. [Google Scholar] [CrossRef] [PubMed]
- Kemp, I.C.; Hartwig, T.; Herdman, R.; Hamilton, P.; Bisten, A.; Bermingham, S. Spray drying with a two-fluid nozzle to produce fine particles: Atomization, scale-up, and modeling. Dry. Technol. 2016, 34, 1243–1252. [Google Scholar] [CrossRef]
- Edwards, D.A.; Hanes, J.; Caponetti, G.; Hrkach, J.; Ben-Jebria, A.; Eskew, M.L.; Mintzes, J.; Deaver, D.; Lotan, N.; Langer, R. Large porous particles for pulmonary drug delivery. Science 1997, 276, 1868–1871. [Google Scholar] [CrossRef]
- Healy, A.M.; McDonald, B.F.; Tajber, L.; Corrigan, O.I. Characterisation of excipient-free nanoporous microparticles (npmps) of bendroflumethiazide. Eur. J. Pharm. Biopharm. 2008, 69, 1182–1186. [Google Scholar] [CrossRef] [PubMed]
- Nolan, L.M.; Tajber, L.; McDonald, B.F.; Barham, A.S.; Corrigan, O.I.; Healy, A.M. Excipient-free nanoporous microparticles of budesonide for pulmonary delivery. Eur. J. Pharm. Sci. 2009, 37, 593–602. [Google Scholar] [CrossRef]
- Paluch, K.J.; Tajber, L.; Corrigan, O.I.; Healy, A.M. Impact of process variables on the micromeritic and physicochemical properties of spray-dried porous microparticles, part i: Introduction of a new morphology classification system. J. Pharm. Pharmacol. 2012, 64, 1570–1582. [Google Scholar] [CrossRef] [PubMed]
- Ógáin, O.N.; Li, J.; Tajber, L.; Corrigan, O.I.; Healy, A.M. Particle engineering of materials for oral inhalation by dry powder inhalers. I—Particles of sugar excipients (trehalose and raffinose) for protein delivery. Int. J. Pharm. 2011, 405, 23–35. [Google Scholar]
- NíÓgáin, O.; Tajber, L.; Corrigan, O.I.; Healy, A.M. Spray drying from organic solvents to prepare nanoporous/nanoparticulate microparticles of protein: Excipient composites designed for oral inhalation. J. Pharm. Pharmacol. 2012, 64, 1275–1290. [Google Scholar]
- Amaro, M.I.; Tajber, L.; Corrigan, O.I.; Healy, A.M. Optimisation of spray drying process conditions for sugar nanoporous microparticles (NPMPs) intended for inhalation. Int. J. Pharm. 2011, 421, 99–109. [Google Scholar] [CrossRef]
- Amaro, M.I.; Tewes, F.; Gobbo, O.; Tajber, L.; Corrigan, O.I.; Ehrhardt, C.; Healy, A.M. Formulation, stability and pharmacokinetics of sugar-based salmon calcitonin-loaded nanoporous/nanoparticulate microparticles (npmps) for inhalation. Int. J. Pharm. 2015, 483, 6–18. [Google Scholar] [CrossRef]
- Nolan, L.M.; Li, J.; Tajber, L.; Corrigan, O.I.; Healy, A.M. Particle engineering of materials for oral inhalation by dry powder inhalers. II—Sodium cromoglicate. Int. J. Pharm. 2011, 405, 36–46. [Google Scholar] [CrossRef]
- Gad, S.; Tajber, L.; Corrigan, O.I.; Healy, A.M. Preparation and characterisation of novel spray-dried nano-structured para-aminosalicylic acid particulates for pulmonary delivery: Impact of ammonium carbonate on morphology, chemical composition and solid state. J. Pharm. Pharmacol. 2012, 64, 1264–1274. [Google Scholar] [CrossRef]
- Tewes, F.; Paluch, K.J.; Tajber, L.; Gulati, K.; Kalantri, D.; Ehrhardt, C.; Healy, A.M. Steroid/mucokinetic hybrid nanoporous microparticles for pulmonary drug delivery. Eur. J. Pharm. Biopharm. Offic. J. Arb. Fur Pharm. Verfahr. E.V 2013, 85, 604–613. [Google Scholar] [CrossRef]
- Yamasaki, K.; Kwok, P.C.; Fukushige, K.; Prud’homme, R.K.; Chan, H.K. Enhanced dissolution of inhalable cyclosporine nano-matrix particles with mannitol as matrix former. Int. J. Pharm. 2011, 420, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Duret, C.; Wauthoz, N.; Sebti, T.; Vanderbist, F.; Amighi, K. New inhalation-optimized itraconazole nanoparticle-based dry powders for the treatment of invasive pulmonary aspergillosis. Int. J. Nanomed. 2012, 7, 5475–5489. [Google Scholar] [CrossRef] [PubMed]
- Pomázi, A.; Buttini, F.; Ambrus, R.; Colombo, P.; Szabó-Révész, P. Effect of polymers for aerolization properties of mannitol-based microcomposites containing meloxicam. Eur. Polym. J. 2013, 49, 2518–2527. [Google Scholar] [CrossRef]
- Malamatari, M.; Somavarapu, S.; Bloxham, M.; Buckton, G. Nanoparticle agglomerates of indomethacin: The role of poloxamers and matrix former on their dissolution and aerosolisation efficiency. Int. J. Pharm. 2015, 495, 516–526. [Google Scholar] [CrossRef]
- Malamatari, M.; Somavarapu, S.; Kachrimanis, K.; Bloxham, M.; Taylor, K.M.G.; Buckton, G. Preparation of theophylline inhalable microcomposite particles by wet milling and spray drying: The influence of mannitol as a co-milling agent. Int. J. Pharm. 2016, 514, 200–211. [Google Scholar] [CrossRef]
- Malamatari, M.; Somavarapu, S.; Kachrimanis, K.; Buckton, G.; Taylor, K.M.G. Preparation of respirable nanoparticle agglomerates of the low melting and ductile drug ibuprofen: Impact of formulation parameters. Powder Technol. 2017, 308, 123–134. [Google Scholar] [CrossRef]
- Liu, Q.; Guan, J.; Sun, Z.; Shen, X.; Li, L.; Jin, L.; Mao, S. Influence of stabilizer type and concentration on the lung deposition and retention of resveratrol nanosuspension-in-microparticles. Int. J. Pharm. 2019, 569, 118562. [Google Scholar] [CrossRef]
- Teymouri Rad, R.; Dadashzadeh, S.; Vatanara, A.; Alavi, S.; Ghasemian, E.; Mortazavi, S.A. Tadalafil nanocomposites as a dry powder formulation for inhalation, a new strategy for pulmonary arterial hypertension treatment. Eur. J. Pharm. Sci. 2019, 133, 275–286. [Google Scholar] [CrossRef]
- Šimková, K.; Joost, B.; Imanidis, G. Production of fast-dissolving low-density powders for improved lung deposition by spray drying of a nanosuspension. Eur. J. Pharm. Biopharm. 2020, 146, 19–31. [Google Scholar] [CrossRef]
- Pilcer, G.; Rosière, R.; Traina, K.; Sebti, T.; Vanderbist, F.; Amighi, K. New co-spray-dried tobramycin nanoparticles-clarithromycin inhaled powder systems for lung infection therapy in cystic fibrosis patients. J. Pharm. Sci. 2013, 102, 1836–1846. [Google Scholar] [CrossRef]
- Leng, D.; Kissi, E.O.; Löbmann, K.; Thanki, K.; Fattal, E.; Rades, T.; Foged, C.; Yang, M. Design of inhalable solid dosage forms of budesonide and theophylline for pulmonary combination therapy. Aaps Pharmscitech 2019, 20, 137. [Google Scholar] [CrossRef]
- Leng, D.; Thanki, K.; Foged, C.; Yang, M. Formulating inhalable dry powder using two-fluid and three-fluid nozzle spray drying. Pharm. Res. 2018, 35, 247. [Google Scholar] [CrossRef]
- Cipolla, D.; Shekunov, B.; Blanchard, J.; Hickey, A. Lipid-based carriers for pulmonary products: Preclinical development and case studies in humans. Adv. Drug Deliv. Rev. 2014, 75, 53–80. [Google Scholar] [CrossRef]
- Ngan, C.L.; Asmawi, A.A. Lipid-based pulmonary delivery system: A review and future considerations of formulation strategies and limitations. Drug Deliv. Transl. Res. 2018, 8, 1527–1544. [Google Scholar] [CrossRef] [PubMed]
- Storm, G.; Crommelin, D.J.A. Liposomes: Quo vadis? Pharm. Sci. Technol. Today 1998, 1, 19–31. [Google Scholar] [CrossRef]
- Payne, N.I.; Timmins, P.; Ambrose, C.V.; Ward, M.D.; Ridgway, F. Proliposomes: A novel solution to an old problem. J. Pharm. Sci. 1986, 75, 325–329. [Google Scholar] [CrossRef] [PubMed]
- Rojanarat, W.; Changsan, N.; Tawithong, E.; Pinsuwan, S.; Chan, H.-K.; Srichana, T. Isoniazid proliposome powders for inhalation-preparation, characterization and cell culture studies. Int. J. Mol. Sci. 2011, 12, 4414–4434. [Google Scholar] [CrossRef]
- Patil-Gadhe, A.A.; Kyadarkunte, A.Y.; Pereira, M.; Jejurikar, G.; Patole, M.S.; Risbud, A.; Pokharkar, V.B. Rifapentine-proliposomes for inhalation: In vitro and in vivo toxicity. Toxicol. Int. 2014, 21, 275–282. [Google Scholar]
- Ye, T.; Sun, S.; Sugianto, T.D.; Tang, P.; Parumasivam, T.; Chang, Y.K.; Astudillo, A.; Wang, S.; Chan, H.K. Novel combination proliposomes containing tobramycin and clarithromycin effective against pseudomonas aeruginosa biofilms. Int. J. Pharm. 2018, 552, 130–138. [Google Scholar] [CrossRef]
- Weber, S.; Zimmer, A.; Pardeike, J. Solid lipid nanoparticles (sln) and nanostructured lipid carriers (nlc) for pulmonary application: A review of the state of the art. Eur. J. Pharm. Biopharm. 2014, 86, 7–22. [Google Scholar] [CrossRef]
- Gaspar, D.P.; Faria, V.; Gonçalves, L.M.D.; Taboada, P.; Remuñán-López, C.; Almeida, A.J. Rifabutin-loaded solid lipid nanoparticles for inhaled antitubercular therapy: Physicochemical and in vitro studies. Int. J. Pharm. 2016, 497, 199–209. [Google Scholar] [CrossRef] [PubMed]
- Honmane, S.; Hajare, A.; More, H.; Osmani, R.A.M.; Salunkhe, S. Lung delivery of nanoliposomal salbutamol sulfate dry powder inhalation for facilitated asthma therapy. J. Liposome Res. 2019, 29, 332–342. [Google Scholar] [CrossRef]
- Cipolla, D.; Wu, H.; Salentinig, S.; Boyd, B.; Rades, T.; Vanhecke, D.; Petri-Fink, A.; Rothin-Rutishauser, B.; Eastman, S.; Redelmeier, T.; et al. Formation of drug nanocrystals under nanoconfinement afforded by liposomes. RSC Adv. 2016, 6, 6223–6233. [Google Scholar] [CrossRef][Green Version]
- Khatib, I.; Khanal, D.; Ruan, J.; Cipolla, D.; Dayton, F.; Blanchard, J.D.; Chan, H.K. Ciprofloxacin nanocrystals liposomal powders for controlled drug release via inhalation. Int. J. Pharm. 2019, 566, 641–651. [Google Scholar] [CrossRef]
- Sur, S.; Rathore, A.; Dave, V.; Reddy, K.R.; Chouhan, R.S.; Sadhu, V. Recent developments in functionalized polymer nanoparticles for efficient drug delivery system. Nano Struct. Nano Obj. 2019, 20, 100397. [Google Scholar] [CrossRef]
- Lebhardt, T.; Roesler, S.; Beck-Broichsitter, M.; Kissel, T. Polymeric nanocarriers for drug delivery to the lung. J. Drug Deliv. Sci. Technol. 2010, 20, 171–180. [Google Scholar] [CrossRef]
- Ohashi, K.; Kabasawa, T.; Ozeki, T.; Okada, H. One-step preparation of rifampicin/poly(lactic-co-glycolic acid) nanoparticle-containing mannitol microspheres using a four-fluid nozzle spray drier for inhalation therapy of tuberculosis. J. Control. Release 2009, 135, 19–24. [Google Scholar] [CrossRef]
- Wang, Z.; Cuddigan, J.L.; Gupta, S.K.; Meenach, S.A. Nanocomposite microparticles (ncmp) for the delivery of tacrolimus in the treatment of pulmonary arterial hypertension. Int. J. Pharm. 2016, 512, 305–313. [Google Scholar] [CrossRef]
- Wang, Z.; Gupta, S.K.; Meenach, S.A. Development and physicochemical characterization of acetalated dextran aerosol particle systems for deep lung delivery. Int. J. Pharm. 2017, 525, 264–274. [Google Scholar] [CrossRef]
- Wang, Z.; Meenach, S.A. Optimization of acetalated dextran–based nanocomposite microparticles for deep lung delivery of therapeutics via spray-drying. J. Pharm. Sci. 2017, 106, 3539–3547. [Google Scholar] [CrossRef]
- Rezazadeh, M.; Davatsaz, Z.; Emami, J.; Hasanzadeh, F.; Jahanian-Najafabadi, A. Preparation and characterization of spray-dried inhalable powders containing polymeric micelles for pulmonary delivery of paclitaxel in lung cancer. J. Pharm. Pharm. Sci. A Publ. Can. Soc. Pharm. Sci. Soc. Can. Des Sci. Pharm. 2018, 21, 200s–214s. [Google Scholar] [CrossRef]
- Farhangi, M.; Mahboubi, A.; Kobarfard, F.; Vatanara, A.; Mortazavi, S.A. Optimization of a dry powder inhaler of ciprofloxacin-loaded polymeric nanomicelles by spray drying process. Pharm. Dev. Technol. 2019, 24, 584–592. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Anton, N.; Arpagaus, C.; Belleteix, F.; Vandamme, T.F. Nanoparticles by spray drying using innovative new technology: The büchi nano spray dryer b-90. J. Control Release 2010, 147, 304–310. [Google Scholar] [CrossRef] [PubMed]
- Arpagaus, C.; Collenberg, A.; Rütti, D.; Assadpour, E.; Jafari, S.M. Nano spray drying for encapsulation of pharmaceuticals. Int. J. Pharm. 2018, 546, 194–214. [Google Scholar] [CrossRef] [PubMed]
- Chan, H.K.; Kwok, P.C. Production methods for nanodrug particles using the bottom-up approach. Adv. Drug Deliv. Rev. 2011, 63, 406–416. [Google Scholar] [CrossRef]
- Bürki, K.; Jeon, I.; Arpagaus, C.; Betz, G. New insights into respirable protein powder preparation using a nano spray dryer. Int. J. Pharm. 2011, 408, 248–256. [Google Scholar] [CrossRef]
- Schoubben, A.; Giovagnoli, S.; Tiralti, M.C.; Blasi, P.; Ricci, M. Capreomycin inhalable powders prepared with an innovative spray-drying technique. Int. J. Pharm. 2014, 469, 132–139. [Google Scholar] [CrossRef]
- Merchant, Z.; Taylor, K.M.; Stapleton, P.; Razak, S.A.; Kunda, N.; Alfagih, I.; Sheikh, K.; Saleem, I.Y.; Somavarapu, S. Engineering hydrophobically modified chitosan for enhancing the dispersion of respirable microparticles of levofloxacin. Eur. J. Pharm. Biopharm. Offic. J. Arb. Fur Pharm. Verfahr. E.V 2014, 88, 816–829. [Google Scholar] [CrossRef]
- Kaewjan, K.; Srichana, T. Nano spray-dried pyrazinamide-l-leucine dry powders, physical properties and feasibility used as dry powder aerosols. Pharm. Dev. Technol. 2016, 21, 68–75. [Google Scholar] [CrossRef]
- Tabernero, A.; Martín del Valle, E.M.; Galán, M.A. Supercritical fluids for pharmaceutical particle engineering: Methods, basic fundamentals and modelling. Chem. Eng. Process. Process Intensif. 2012, 60, 9–25. [Google Scholar] [CrossRef]
- Aguiar-Ricardo, A. Building dry powder formulations using supercritical co2 spray drying. Curr. Opin. Green Sustain. Chem. 2017, 5, 12–16. [Google Scholar] [CrossRef]
- Costa, C.; Casimiro, T.; Aguiar-Ricardo, A. Optimization of supercritical co2-assisted atomization: Phase behavior and design of experiments. J. Chem. Eng. Data 2018, 63, 885–896. [Google Scholar] [CrossRef]
- Silva, A.S.; Sousa, A.M.; Cabral, R.P.; Silva, M.C.; Costa, C.; Miguel, S.P.; Bonifácio, V.D.B.; Casimiro, T.; Correia, I.J.; Aguiar-Ricardo, A. Aerosolizable gold nano-in-micro dry powder formulations for theragnosis and lung delivery. Int. J. Pharm. 2017, 519, 240–249. [Google Scholar] [CrossRef] [PubMed]
- Silva, M.C.; Silva, A.S.; Fernandez-Lodeiro, J.; Casimiro, T.; Lodeiro, C.; Aguiar-Ricardo, A. Supercritical CO2-assisted spray drying of strawberry-like gold-coated magnetite nanocomposites in chitosan powders for inhalation. Materials 2017, 10, 74. [Google Scholar] [CrossRef]
- Restani, R.B.; Conde, J.; Pires, R.F.; Martins, P.; Fernandes, A.R.; Baptista, P.V.; Bonifácio, V.D.; Aguiar-Ricardo, A. Poxylated polyurea dendrimers: Smart core-shell vectors with ic50 lowering capacity. Macromol. Biosci. 2015, 15, 1045–1051. [Google Scholar] [CrossRef] [PubMed]


| Author(s) | Reference | Topics Covered |
|---|---|---|
| Pulmonary particle deposition | ||
| Darquenne (2012) | [7] |
|
| Kourmatzis et al. (2018) | [8] |
|
| Martin et al. (2018) | [9] |
|
| He et al. (2019) | [10] |
|
| Development of DPIs | ||
| Islam and Gladki (2008) | [11] |
|
| Islam and Clearly (2012) | [12] |
|
| Hoppentocht et al. (2014) | [13] |
|
| de Boer et al. (2017) | [14] |
|
| Buttini et al. (2018) | [15] |
|
| Levy et al. (2019) | [16] |
|
| Formulations for DPIs | ||
| Pilcer and Amighi (2010) | [17] |
|
| Al-Hallak et al. (2011) | [18] |
|
| Healy et al. (2014) | [19] |
|
| Gradon and Sosnowski (2014) | [20] |
|
| Brunaugh and Smyth (2018) | [21] |
|
| Hadiwinoto et al. (2018) | [22] |
|
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Malamatari, M.; Charisi, A.; Malamataris, S.; Kachrimanis, K.; Nikolakakis, I. Spray Drying for the Preparation of Nanoparticle-Based Drug Formulations as Dry Powders for Inhalation. Processes 2020, 8, 788. https://doi.org/10.3390/pr8070788
Malamatari M, Charisi A, Malamataris S, Kachrimanis K, Nikolakakis I. Spray Drying for the Preparation of Nanoparticle-Based Drug Formulations as Dry Powders for Inhalation. Processes. 2020; 8(7):788. https://doi.org/10.3390/pr8070788
Chicago/Turabian StyleMalamatari, Maria, Anastasia Charisi, Stavros Malamataris, Kyriakos Kachrimanis, and Ioannis Nikolakakis. 2020. "Spray Drying for the Preparation of Nanoparticle-Based Drug Formulations as Dry Powders for Inhalation" Processes 8, no. 7: 788. https://doi.org/10.3390/pr8070788
APA StyleMalamatari, M., Charisi, A., Malamataris, S., Kachrimanis, K., & Nikolakakis, I. (2020). Spray Drying for the Preparation of Nanoparticle-Based Drug Formulations as Dry Powders for Inhalation. Processes, 8(7), 788. https://doi.org/10.3390/pr8070788








