3.1. Structural Equation Model
To study the above questions and conjectures, the choice of SEM was guided by the several advantages that this technique presents. Health is a difficult concept to quantify and is oftentimes estimated by its outcomes, namely chronic disease occurrence or mortality rates. This method, however, does not provide a complete, nor a sufficient picture of the individual’s state of physical and mental well-being. In view of these elements, in our SEM model, we let health be a latent variable, influenced by the lifestyle. Doing so, we avoided at the same time any reporting bias and measurement errors of health-related variables (on which
Crossley and Kennedy (
2002) shed light). Indeed, some authors used the self-assessed health of the individual as a proxy for the unobserved health, especially in the labor market field (see
Haan and Myck 2009;
Strully 2009;
Böckerman and Ilmakunnas 2009, for a few examples). The issue in this procedure lies in the unobserved characteristics such as risk aversion, which may, for instance, affect both one’s own health perception and health insurance demand. Solely relying on the self-reported health at face value is also prone to severe measurement biases highlighted in the literature (mostly attributed to social desirability, discussed in
Huang et al. 1998 and
Van de Mortel et al. 2008). In an SEM setting, on the contrary, health can be captured by several more objective measures called manifest variables and, by this means, minimize the bias. The same rationale applies to the latent variable of health care seeking. Like health, the unobservable variable of the demand of health care services is a difficult notion to grasp by a single variable or even a set (as for instance in
Bourne et al. 2009) and may be subject to omitted variables’ bias. Again, SEM is well suited for using several variables at once to define the concept.
Additionally, in dealing with the above issues, SEM can indicate simultaneous direct relationships called paths. These paths can be specified as well between exogenous as between endogenous variables, thus allowing for a more thorough and exhaustive analysis. Because of this convenient ability of the model to assess the simultaneous relationship between multiple unobserved variables and observed outcomes, SEM frameworks have been widely used in the sociology- and psychology-related literature (
Sobel 1987;
Cuttance and Ecob 2009;
MacCallum and Austin 2000;
Martens 2005). Moreover, we note that usual econometric methodologies like fixed effects regressions cannot be applied in our context due to the cross-sectional nature of data from surveys. In an SEM, the estimation of the parameters comes from a maximization of likelihood between the actual covariance matrices of the relationships between variables and the estimated covariance matrices of the model (for more information, see
Bollen 1989).
Our research aims to assess the relationship between lifestyle and health insurance decisions.
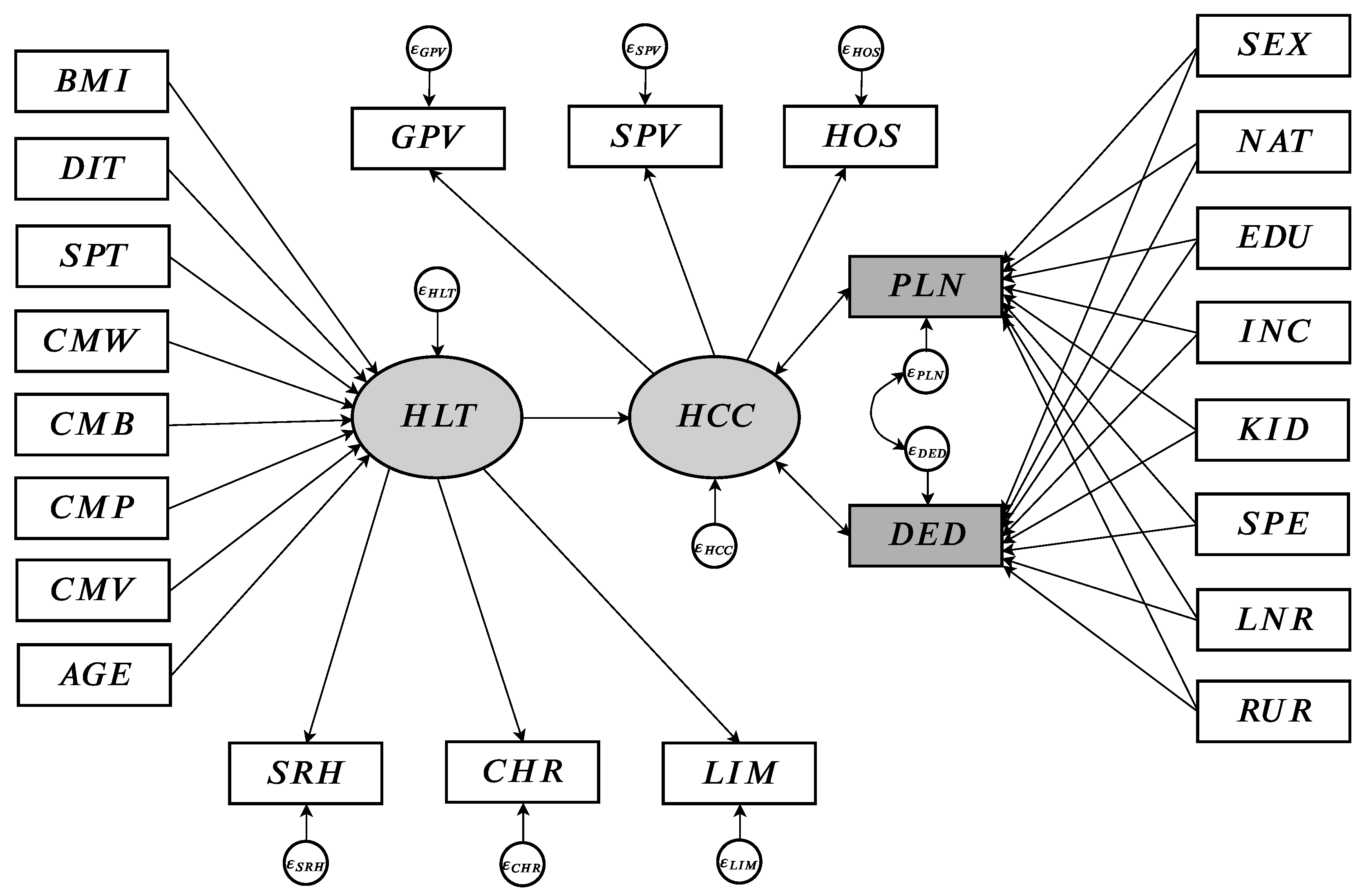
Figure 1 gives a graphical representation of the model that we employed. We measured lifestyle from four behaviors, namely BMI (
), diet (
), sports (
), and commuting modes (
,
,
,
), while we controlled for age (
). In our model, however, lifestyle was not assumed to have a direct effect on insurance decisions (insurance plan
and deductible
), but rather an indirect one mediated via health (
) and health care consumption (
). Health was hypothesized to play a role in health care usage, which in turn was conjectured to drive health insurance decisions, thus creating a bridge to lifestyle. Finally, the health insurance choice was controlled by socio-demographic characteristics (gender
, nationality
, education
and income
levels, number of children in the household
, freedom of choice for specialist doctors
, language region
, and urbanicity
). Further, health was measured using information on self-reported health
, chronic health conditions
, and limiting health conditions
, while health care consumption was evaluated from GP visits (
), specialist and gynecologist visits (
), and hospital stays (
). In
Table 1, we summarize and describe the variables that we used.
3.1.1. Measurement of Health
To run the analysis, we designed our model with health (
) as a latent variable. This latent variable was measured by three observed variables: the self-rated health (
), having or having had a chronic health condition lasting at least six months (
), and having health conditions limiting daily activities during the past six months (
). These three indicators were assumed to correlate perfectly with the unobserved health variable. We considered the following set of equations:
In the system of Equation (
1),
,
, and
are the loading factors.
are the error terms for the individual
i linked to each of the indicator variables. For our modeling, we assumed the error terms to be uncorrelated with each other and with the latent variable
, as well as having an expectation value of zero.
3.1.2. Regression Model for Health
The following Equation (
2) describes the regression of health on the lifestyle variables including a control for age as depicted in the left-hand part of the graph in
Figure 1.
The respective and coefficients correspond to the baseline, respectively the regression coefficients linked to the variables. The error term was assumed to have a zero expected value and to be uncorrelated with the error terms in the other submodels.
3.1.3. Measurement of Health Care Consumption
Our second latent variable was the individual’s inherent health care consumption (
). Three variables were used to approximate this behavior: the number of GP or family doctor visits (
), the number of specialists visits (
), and whether the respondent had an inpatient hospitalization (
). All three variables were accounted for during the past 12 months and were assumed to correlate perfectly with our unobserved health variable.
In the system of Equation (
3),
,
, and
are the loading factors.
denote the error terms for the individual
i in each indicator variable. The errors were assumed to be uncorrelated with each other and with the latent variable
. Errors were supposed to have an expected value of zero.
3.1.4. Regression Model for Health Care Consumption
The following Equation (
4) is the regression of health care consumption on health (
) and the insurance characteristics (plan
and deductible
):
The respective and coefficients correspond to the baseline, respectively the variables’ regression coefficients. The error term was assumed to have a zero expected value and to be uncorrelated with other error terms.
3.1.5. Regression Models for Health Insurance Decisions
The two following regressions express the choice of the insurance plan (
) and deductible level (
) according to health care consumption and socio-demographic characteristics. The variable
takes the value of one if the respondent chooses an alternative plan (HMO, family doctor, telmed, other) and zero for the standard plan. Concerning the deductible levels
, if the individual has opted for a yearly deductible of CHF 300, the variable takes the value of zero. The value is one if the chosen deductible is CHF 2500. Here, we built a simple model by selecting only the two extreme values because we considered that they unveiled a clear choice towards the highest versus the lowest coverage. We disregarded all individuals with other choices. The resulting respective probit models (choices 0 and 1) were modeled through latent variables. Indeed, for our SEM, we supposed there existed auxiliary random variables
and
such that:
and:
for which we had
and
variables acting as indicators:
and:
The values and , respectively and , follow the standard notations for regression coefficients. Further, the error terms and were assumed to come from a standard normal distribution and were allowed to correlate with each other.
3.2. Swiss Health Survey Data
We based our study on data obtained from the Swiss Health Survey, a cross-sectional nation-wide survey (
Swiss Federal Statistical Office 2019;
Swiss Federal Statistical Office 2018).
1 The survey was carried out by the Swiss Federal Statistical Office on behalf of the Federal Council every five years since 1992. In the following, we used the wave of 2017, which was the sixth and most recent one. The survey responses were firstly collected via computer-assisted telephone interviews and followed up by an additional written questionnaire available in the three official Swiss languages (German, French, and Italian). The included population was aged 15 years or over and lived in Switzerland in a private household. The total sample of 2017 included 22,134 telephone interviews and 18,832 subsequently completed and returned questionnaires. The information collected concerned the state of health of each individual (e.g., physical and mental well-being, health conditions, health limitations), the use of health care (e.g., doctor consultations, hospitalization, use of drugs), the health insurance status (e.g., insurance plan, deductible, purchase of complementary insurance), behaviors susceptible to have an influence on health (e.g., alcohol intake, drug consumption), and socio-demographic characteristics (e.g., employment status, income, nationality).
To conduct our empirical analysis, we extracted a sample of “complete” answers comprising 9301 observations. The completeness of an observation was defined by the absence of entries that were not available (NA). We could consider that the NAs were distributed randomly across the original data since our extracted sample was not markedly different from the original one. Regrading the lifestyle indicators, our final sample had a slightly higher median age, i.e., 52 versus 49 years. As concerned the BMI, the diet (number of portions of fruits and vegetables eaten per day) or the frequency of physical activity
2, and commuting, the average values and shares were very close. Regarding the other exogenous variables, the original sample displayed the same level of self-rated health (good), and a smaller percentage had health conditions limiting daily activities, which was most probably due to a lower proportion of individuals aged over 50 years; our final sample contained a higher number of individuals with chronic health conditions. Overall, we considered that our extracted sample did not present any selection bias thanks to the sampling performed beforehand by the Swiss Federal Statistical Office and the relatively large sample size when compared to other surveys (where the number of observations is often considerably smaller).
3.3. Descriptive Statistics
3.3.1. Exogenous Characteristics Affecting Health
In
Table 2, we present some descriptive statistics based on our data along with the variables appearing in our hypotheses. The lifestyle was conjectured to have an effect on health, which was defined in our model by the self-rated health (
), the past or ongoing existence of a chronic disease lasting for six months or more (
), and a health condition coming with a limitation in daily activities (
). Subsequently, through health, they impacted health care consumption, gauged in our model by the number of GP visits (
), the number of specialists visits (
, gynecologists excluded, to avoid pregnancy-related bias), and the individual’s hospital stays of one night or over (
). The first column in
Table 2 counts the number of observations
N per category in each variable, while the second represents the corresponding share from the whole sample of 9301 observations (total
N). The other six columns display the mean for each manifest variable. Over the total sample (cf. the last row of the table), the mean self-rated health was at 0.81, that is good health on average; 35% of the sample’s population reported chronic, and 21% health conditions limiting daily activities. Alongside this, the average number of GP visits was 2.27, and the number of visits to specialists was 1.99. Finally, 18% of the sampled individuals stayed in a hospital for more than one night during the 12 months preceding the survey.
Concerning the lifestyle variables, when grouping individuals by BMI categories, we deciphered the pattern that was documented in the literature, i.e., respondents with a BMI comprised between 18.5 and 24.9 declared the highest self-rated health (0.84) and the lowest propensity of having a chronic or a limiting health condition (0.31 and 0.18). Additionally, as the BMI increased, the
decreased (from 0.84 to 0.72 for the category with highest BMI), and the proportion of individuals having chronic or limiting health conditions increased (moving from 0.31 and 0.18 to 0.50 and 0.30 for
, respectively
, in the group with the highest BMI), thus matching observations from the literature (cf.
Section 2.2). An increase in BMI was also positively associated with health care services’ utilization. According to our descriptive statistics, the effect of the diet on the health and health care usage proxies was mitigated. Two associations could be made: an increase in the number of fruits and vegetables eaten on average per day came with an increase in self-rated health (0.80 to 0.83), but also with an increase of visits to specialists (1.33 to 1.66). Further analysis, including the study of significance, was performed in our SEM. When it came to physical activity, however, the relationship seemed indisputable. As the frequency of sports activities increased, the data presented a clear increase in the self-rated health variable (0.74 to 0.85), coupled with a decrease in the occurrence of health conditions (0.42 to 0.30 for
and 0.26 to 0.18 for
). This beneficial association continued on health care seeking through all indicators where we observed declining consumption. Concerning the effect on the commuting mode, we observed that it largely depended on the type. Biking as a means of transportation exhibited the most notable link to our indicators: individuals who bike reported a higher self-rated health (0.85 against 0.80) and a lower in-group propensity to have a chronic or limiting health condition (0.33 versus 0.36 for
and 0.19 versus 0.21 for
). By the same token, the number of GP visits dropped from 2.42 to 1.82 on average, the number of visits to specialists from 1.48 to 1.32, and the inpatient stays going down by three percentage points. Finally, age displayed the expected effect, that is as age increased, the self-rated health decreased, and the propensity in each category of having a chronic or a limiting health condition increased, along with the frequency of all medical visits. Finally, to supplement our descriptive statistics, we document in
Table 3 the correlation coefficients between our proxy variables, as well as their standard deviations.
3.3.2. Exogenous Characteristics Affecting Health Insurance Decisions
In the following
Table 4, we provide an overview of the distribution of the observations along the second set of exogenous variables, i.e., the socio-demographic characteristics, linked to insurance decisions. We provide the shares of individuals along the insurance plan and deductible choices. In addition to the control variables, we present the distribution along the health and health care utilization indicator variables.
Firstly, when comparing the statistics of health insurance decisions based on socio-demographic variables, we observed several trends. Between both genders, we noted one important difference with women being more likely to choose a lower deductible when compared to men (65.9% of the women, 52.2% of the men). Regarding the nationality, Swiss nationals tended to opt more often for an alternative plan, whereas non-Swiss individuals rather went for the standard one. Education, income, and the number of children in the household seemed to demonstrate differences. As the level of education, income, or the number of children increased, the majority switched from the low to the high level of deductible. Moreover, increasing education levels came along with a favor for alternative insurance plans. Along the two other variables, the majority already favored alternative plans with a slight increase in the share as income and number of children became higher. Finally, the last markedly different result with respect to the socio-demographic variables was the specificity of German-speaking respondents regarding the choice of the insurance plan: most individuals from the German-speaking language area tended towards alternative models, which was not the case in the French- and Italian-speaking regions.
Secondly, when focusing on health-related variables, we observed that higher levels of self-rated health went along with individuals that had chosen the high level deductible, as well as an alternative insurance plan. This observation was not at odds with economic logic as an individual with a lower self-rated health may expect to have higher yearly expenses and hence would prefer to pick a model with a higher coverage. The same observation could be drawn for individuals disclosing chronic or other limiting health conditions. The distribution of individuals who did not report having or having had any chronic health conditions was fairly even among both models (43.3% standard) and deductible levels (49.7% low). For individuals with a limiting health condition, the figures were still very similar. When focusing on people reporting any chronic or limiting health conditions, the shares regarding the model choices remained in fact relatively stable, but presented a strong increase in the share opting for the low deductible, i.e., 77.8% for and 78.5% for .
Finally, concerning our manifest variables accounting for health care consumption, the observations met the economic intuition. Regarding the models, the relationship was constant: as the number of visits, disregarding the type of doctor, increased, health care consumption did as well. Respondents typically favor an alternative insurance plan. Strong differences appeared with regard to the deductible. As an example, individuals not reporting any visits to a GP were 36.6% in the low deductible category; this percentage rose to 84.4% for those reporting four visits or more during the past 12 months. The same pattern could be observed throughout all three variables.