Designing a Mobile Health Solution to Facilitate the Transition from NICU to Home: A Qualitative Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Research Team and Reflexivity
2.2. Study Design and Framework
2.3. Participant Selection and Setting
2.4. Development of Interview Guide
2.5. Data Collection
2.6. Data Analysis
3. Results
3.1. Demographics
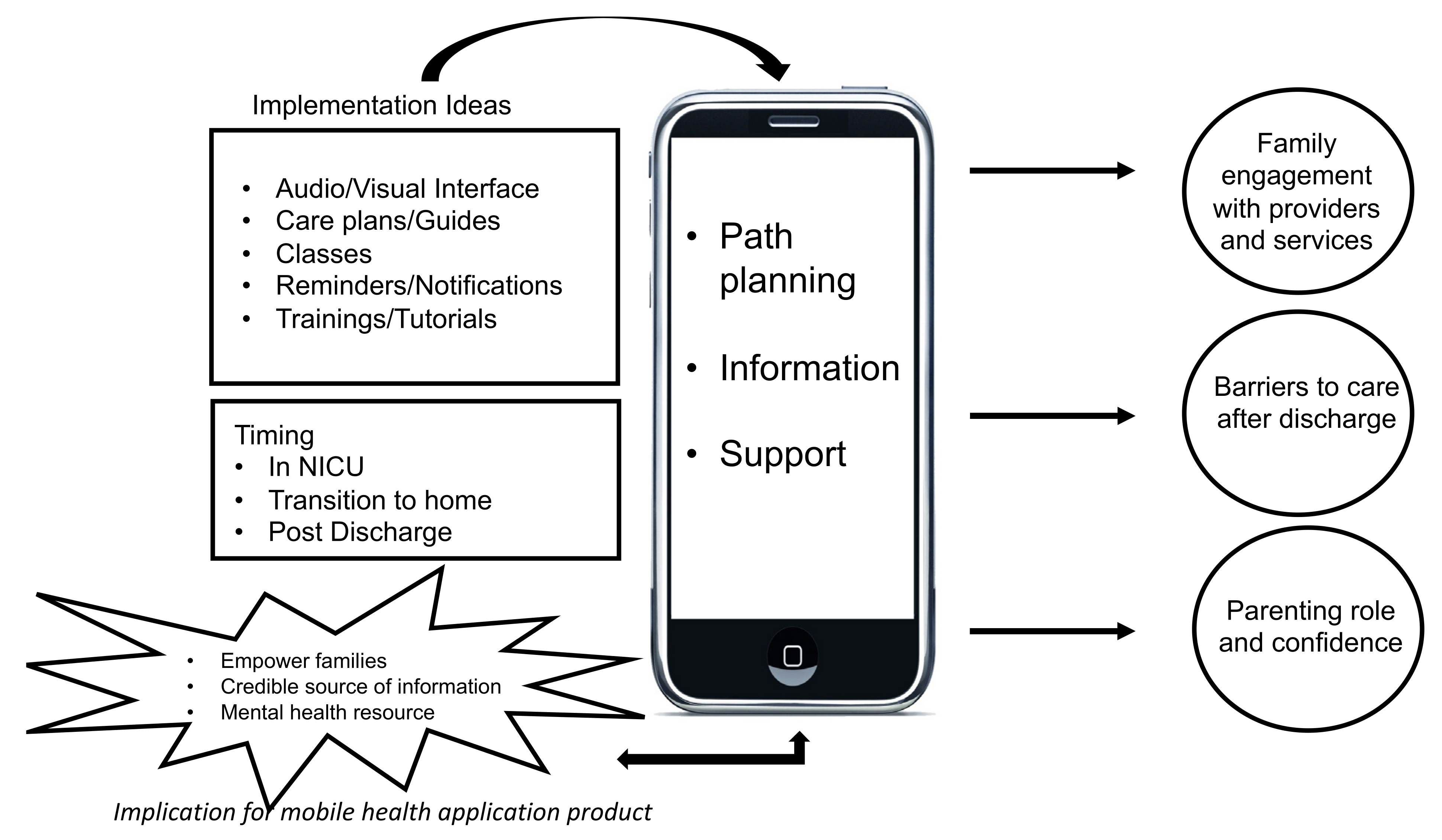
3.2. Conceptual Model
3.3. Domain 1: Ideas for Content Formats and User Interface
3.4. Domain 2: Timing of Events around Discharge
3.5. Domain 3: Path Planning
3.6. Domain 4: Provision of Information
3.7. Domain 5: Accessing Support
3.8. Domain 6: Engagement with Providers
3.9. Domain 7: Barriers to Care after Discharge
3.10. Domain 8: Parenting Role and Confidence
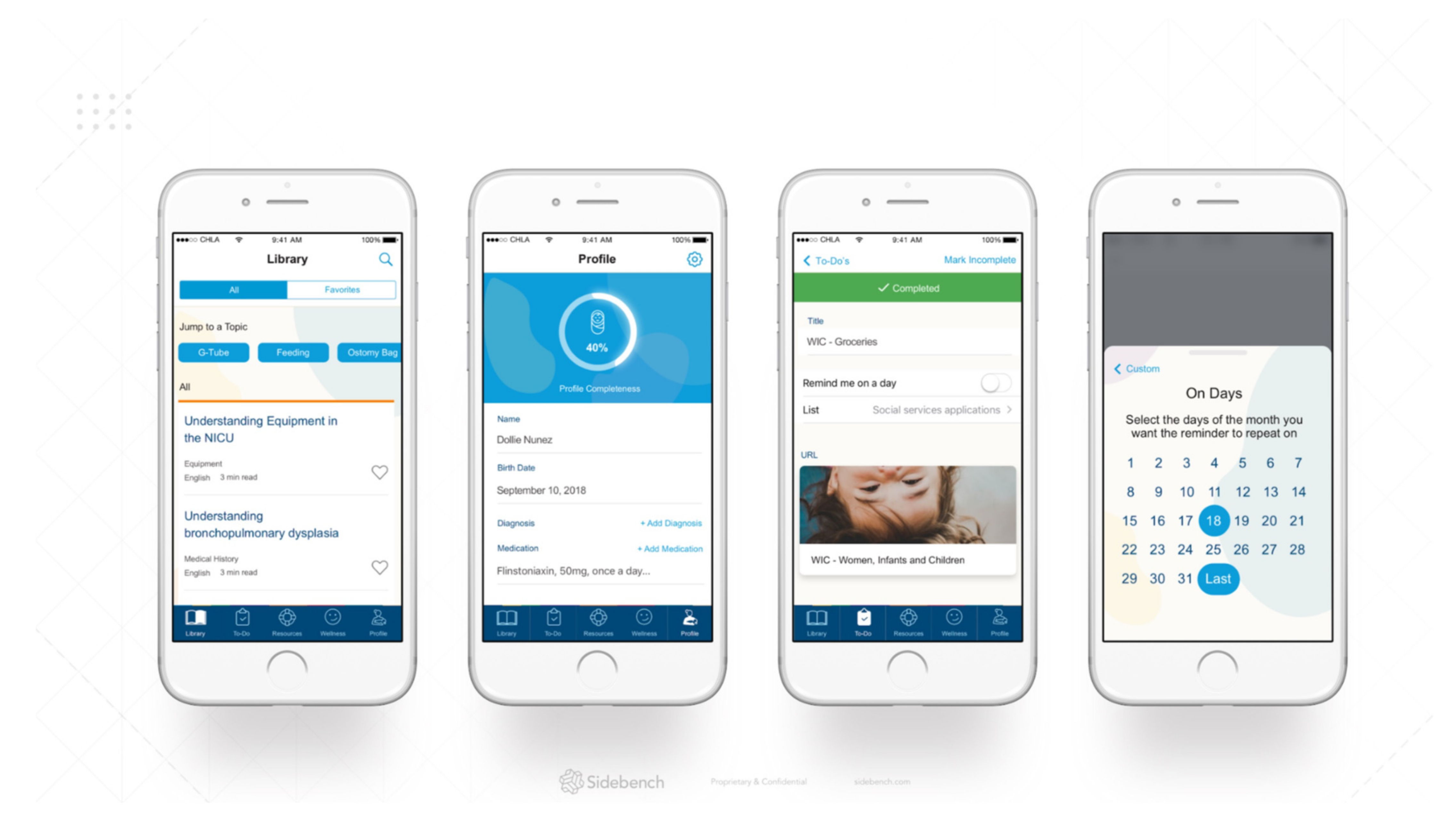
3.11. Implications for Product Development
4. Discussion
- (1)
- Consider the access to technology that families might have (type of smart device, carrier, etc.);
- (2)
- Integrate educational and path-planning resources into discharge planning using web-based tools such as a mobile health applications or websites;
- (3)
- Consider virtual support groups or structures to support families during the transition to home.
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Construct 1: Information | The first set of questions are about how you would like information presented to you on a web based application.
|
| Construct 2: Social Supports | Would you be interested in having a social support system via the web based platform?
|
| Construct 3: Community based services | How would a web based platform help you access community based services like:
|
| Construct 4: Mental Health | The next set of questions are about how you feel, your mental health-do you think a web based platform might be useful to you as a resource?
|
References
- Hebballi, N.B.; Kerl, C.G.; Garcia, E.I.; Ottosen, M.J.; Kelly, K.C.; Bartz-Kurycki, M.A.; Tang, B.; Hillman, E.A.; Aneji, C.U.; Tsao, K.; et al. Barriers to Transition to Home from the Neonatal Intensive Care Unit: A Qualitative Perspectives of Parents and Healthcare Providers. J. Perinat. Neonatal Nurs. 2021, 35, 340–349. [Google Scholar] [CrossRef] [PubMed]
- Berman, L.; Raval, M.; Ottosen, M.; Mackow, A.K.; Cho, M.; Goldin, A.B. Parent Perspectives on Readiness for Discharge Home after Neonatal Intensive Care Unit Admission. J. Pediatr. 2019, 205, 98–104. [Google Scholar] [CrossRef] [PubMed]
- Desai, A.D.; Durkin, L.K.; Jacob-Files, E.A.; Mangione-Smith, R. Caregiver Perceptions of Hospital to Home Transitions According to Medical Complexity: A Qualitative Study. Acad. Pediatr. 2016, 16, 136–144. [Google Scholar] [CrossRef] [PubMed]
- Enlow, E.; Herbert, S.L.; Jovel, I.J.; Lorch, S.A.; Anderson, C.; Chamberlain, L.J. Neonatal intensive care unit to home: The transition from parent and pediatrician perspectives, a prospective cohort study. J. Perinatol. 2014, 34, 761–766. [Google Scholar] [CrossRef] [PubMed]
- Horbar, J.D.; Edwards, E.M.; Greenberg, L.T.; Profit, J.; Draper, D.; Helkey, D.; Lorch, S.A.; Lee, H.C.; Phibbs, C.S.; Rogowski, J.; et al. Racial Segregation and Inequality in the Neonatal Intensive Care Unit for Very Low-Birth-Weight and Very Preterm Infants. JAMA Pediatr. 2019, 173, 455–461. [Google Scholar] [CrossRef]
- Lake, E.T.; Staiger, D.; Horbar, J.; Kenny, M.J.; Patrick, T.; Rogowski, J.A. Disparities in Perinatal Quality Outcomes for Very Low Birth Weight Infants in Neonatal Intensive Care. Health Serv. Res. 2014, 50, 374–397. [Google Scholar] [CrossRef]
- American Academy of Pediatrics Committee on Fetus and Newborn. Hospital discharge of the high-risk neonate. Pediatrics 2008, 122, 1119–1126. [Google Scholar] [CrossRef] [Green Version]
- Hannan, K.E.; Hwang, S.S.; Bourque, S.L. Readmissions among NICU graduates: Who, when and why? Semin. Perinatol. 2020, 44, 151245. [Google Scholar] [CrossRef]
- McManus, B.M.; Richardson, Z.; Schenkman, M.; Murphy, N.; Morrato, E.H. Timing and Intensity of Early Intervention Service Use and Outcomes Among a Safety-Net Population of Children. JAMA Netw. Open 2019, 2, 187529. [Google Scholar] [CrossRef] [Green Version]
- Lapcharoensap, W.; Lund, K.; Huynh, T. Telemedicine in neonatal medicine and resuscitation. Curr. Opin. Pediatr. 2021, 33, 203–208. [Google Scholar] [CrossRef]
- Davis, D.W.; Logsdon, M.C.; Vogt, K.; Rushton, J.; Myers, J.; Lauf, A.; Hogan, F. Parent Education is Changing: A Review of Smartphone Apps. MCN Am. J. Matern. Child Nurs. 2017, 42, 248–256. [Google Scholar] [CrossRef] [PubMed]
- Orr, T.; Campbell-Yeo, M.; Benoit, B.; Hewitt, B.; Stinson, J.; McGrath, P. Smartphone and Internet Preferences of Parents: Information Needs and Desired Involvement in Infant Care and Pain Management in the NICU. Adv. Neonatal Care 2017, 17, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Dol, J.; Richardson, B.; Boates, T.; Campbell-Yeo, M. Learning to parent from Google? Evaluation of available online health evidence for parents of preterm infants requiring neonatal intensive care. Health Inf. J. 2018, 25, 1265–1277. [Google Scholar] [CrossRef] [Green Version]
- Richardson, B.; Dol, J.; Rutledge, K.; Monaghan, J.; Orovec, A.; Howie, K.; Boates, T.; Smit, M.; Campbell-Yeo, M. Evaluation of Mobile Apps Targeted to Parents of Infants in the Neonatal Intensive Care Unit: Systematic App Review. JMIR mHealth uHealth 2019, 7, e11620. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Garfield, C.F.; Lee, Y.S.; Kim, H.N.; Rutsohn, J.; Kahn, J.Y.; Mustanski, B.; Mohr, D.C. Supporting Parents of Premature Infants Transitioning from the NICU to Home: A Pilot Randomized Control Trial of a Smartphone Application. Internet Interv. 2016, 4, 131–137. [Google Scholar] [CrossRef] [Green Version]
- Dedoose. Available online: https://www.dedoose.com/userguide/appendix#:~:text=Download-,Citing%20Dedoose,method%20research%20data%20(2018) (accessed on 10 February 2022).
- Simon, T.D.; Haaland, W.; Hawley, K.; Lambka, K.; Mangione-Smith, R. Development and Validation of the Pediatric Medical Complexity Algorithm (PMCA) Version 3.0. Acad. Pediatr. 2018, 18, 577–580. [Google Scholar] [CrossRef]
- Desai, A.D.; Jacob-Files, E.A.; Wignall, J.; Wang, G.; Pratt, W.; Mangione-Smith, R.; Britto, M.T. Caregiver and Health Care Provider Perspectives on Cloud-Based Shared Care Plans for Children With Medical Complexity. Hosp. Pediatr. 2018, 8, 394–403. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lakshmanan, A.; Sunshine, I.; Escobar, C.M.; Kipke, M.; Vanderbilt, D.; Friedlich, P.S.; Mirzaian, C.B. Connecting to Early Intervention Services After Neonatal Intensive Care Unit Discharge in a Medicaid Sample. Acad. Pediatr. 2021. [Google Scholar] [CrossRef]
- Baggett, K.M.; Davis, B.; Landry, S.H.; Feil, E.G.; Whaley, A.; Schnitz, A.; Leve, C. Understanding the Steps Toward Mobile Early Intervention for Mothers and Their Infants Exiting the Neonatal Intensive Care Unit: Descriptive Examination. J. Med. Internet Res. 2020, 22, e18519. [Google Scholar] [CrossRef]
- McGowan, E.C.; Du, N.; Hawes, K.; Tucker, R.; O’Donnell, M.; Vohr, B. Maternal Mental Health and Neonatal Intensive Care Unit Discharge Readiness in Mothers of Preterm Infants. J. Pediatr. 2017, 184, 68–74. [Google Scholar] [CrossRef]
- Franck, L.S.; McNulty, A.; Alderdice, F. The Perinatal-Neonatal Care Journey for Parents of Preterm Infants: What Is Working and What Can Be Improved. J Perinat. Neonatal Nurs. 2017, 31, 244–255. [Google Scholar] [CrossRef]
- Hall, S.L.; Ryan, D.J.; Beatty, J.; Grubbs, L. Recommendations for peer-to-peer support for NICU parents. J. Perinatol. 2015, 35 (Suppl. 1), S9–S13. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Enlow, E.; Faherty, L.J.; Wallace-Keeshen, S.; Martin, A.E.; Shea, J.A.; Lorch, S.A. Perspectives of Low Socioeconomic Status Mothers of Premature Infants. Pediatrics 2017, 139, e20162310. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- McGowan, E.C.; Abdulla, L.S.; Hawes, K.K.; Tucker, R.; Vohr, B.R. Maternal Immigrant Status and Readiness to Transition to Home From the NICU. Pediatrics 2019, 143. [Google Scholar] [CrossRef] [PubMed]
- Flores-Fenlon, N.; Song, A.Y.; Yeh, A.; Gateau, K.; Vanderbilt, D.L.; Kipke, M.; Friedlich, P.; Lakshmanan, A. Smartphones and Text Messaging are Associated With Higher Parent Quality of Life Scores and Enrollment in Early Intervention after NICU Discharge. Clin. Pediatr. 2019, 58, 903–911. [Google Scholar] [CrossRef] [PubMed]
| N (%) | Median (IQR) | |
|---|---|---|
| Infant and Parent Demographics (n = 11) | ||
| Infant demographics | ||
| Race/Ethnicity | ||
| Hispanic | 7 (63) | |
| Black non-Hispanic | 2 (19) | |
| White non-Hispanic | 1 (9) | |
| Other (Native American, Mixed) | 1 (9) | |
| Gestational age (weeks), median (IQR), if preterm | 29 (23, 34) | |
| Birth weight (grams), median (IQR) | 1365 (969, 2800) | |
| Neonatal diagnoses | ||
| Bronchopulmonary dysplasia | 5 (45) | |
| Retinopathy of prematurity requiring intervention | 3 (27) | |
| Necrotizing enterocolitis (surgical) | 1 (9) | |
| Intraventricular hemorrhage (Grade III/IV) | 2 (19) | |
| Infants with medical complexity (post-discharge) a | ||
| Complex Chronic Disease (C-CD) | 11 (100) | |
| Non-Complex Chronic Disease (NC-CD) | ||
| Non-Complex Non-Chronic Disease (NC-NCD) | ||
| Infants requiring prescription medications after discharge | 4 (36) | |
| Infants requiring durable medical equipment after discharge | 4 (36) | |
| Oxygen | 3 (27) | |
| Feeding tube (gastrostomy/jejunostomy) | 4 (36) | |
| Diagnosis of developmental issue after discharge (may have more than 1) | ||
| Language delay | 1 (9) | |
| Autism risk | 1 (9) | |
| Sensory issue | 5 (46) | |
| Global developmental delay | 5 (46) | |
| Cerebral palsy | 3 (27) | |
| Early intervention services received | 8 (73) | |
| Speech therapy | 3 (27) | |
| Occupational/Physical therapy | 5 (45) | |
| Vision | 1 (9) | |
| Maternal demographics | ||
| Primary Language | ||
| English | 9 (81) | |
| Spanish | 2 (19) | |
| Neighborhood equity b | ||
| Home zip code in service planning area (SPA) with 4th quartile economic hardship index | 7 (63) | |
| Medicaid/California Children’s Services | 11 (100) | |
| Distance to HRIF clinic from participants’ home, in miles, median (IQR) | 12.2 (5.8, 41.8) | |
| Distance to early intervention program from participants’ home, in miles, median (IQR) | 4.4 (1.7, 15.6) | |
| Provider Demographics (n = 11) | ||
| Provider type | ||
| Neonatology (physician) | 4 (37) | |
| Clinical care coordinator/Case Manager | 1 (9) | |
| Nursing | 3 (27) | |
| Social Work | 1 (9) | |
| Developmental behavioral specialist | 1 (9) | |
| General pediatrician | 1 (9) | |
| Years of practice | ||
| <5 years | 2 (18) | |
| 5–10 years | 3 (27) | |
| >10 years | 6 (55) | |
| Gender (female) | 10 (90) | |
| Participate in transition planning/discharge planning committees | 4 (37) | |
| Bilingual provider (English and Spanish) | 2 (18) |
| N | Patient | Provider | |||
|---|---|---|---|---|---|
| Domain/Theme | N | Illustrative Quotations | N | Illustrative Quotations | |
| Domain 1: Ideas for content formats and user interface | |||||
| (a) Provide audio/visual resources | 29 | 17 | “I’m a very visual person, I [want] to click right to that video, and after I’m done with it, I can also read an article” “Definitions, medical terminology, like little sketches or PowerPoint presentations or some type of thing where it shows you direct step by step on how to deal with certain procedures afterwards, like even if they’re just more like redo your information on how to, how to place a bag, or how to, correctly change out a G tube, whatever, or how to do a trach, anything, just like step by step, and, and like watching somebody actually do it. Yeah that would be awesome, and clicking on certain words for medical terminology, you get a better definition and understanding of it. Being able to talk at a medical professional with a click of a button if you have any other questions, that’s available to you 24/7.” | 12 | “[There is] an online, electronic, learning tool called the GetWellNetwork. The NICU doesn’t have it, and that’s a big setback for us. But that builds confidence in that they can watch a video, audiovisual, before they practice. Every nurse has a different style in how they teach. Some nurses will schedule a teaching, some nurses will turn around and say, hey, I’m about to do this, step right up. Not every family is comfortable doing something for the very first time on their child with the implications of risks and, and that kind of thing without having watched it first, maybe rewind, watch it again.” “We had an illiterate mom, so we allowed her to record [us] teaching her, so she would have that as her teaching because she would not be able to read the discharge instructions. And so, that’s a special circumstance and it wasn’t a fancy device, but it was us using technology in a way. We’d love to use it in the future, to teach.” |
| (b) Provide care plan/guides | 12 | 9 | “I’d love it if there was something like that in the NICU, [because] he was on so many more drugs then, and I had such a hard time keeping track of everything. I think for me having it like written down or even if they could kind of give you like printouts… it was kind of this blur for me.” “I would love it if there were some way to some sort of a simple like manual for our [oxygen] machine too… if the oxygen saturation is below like or hits 98% versus 100 then it starts beeping. I’m going, how do I stop this incessant beeping?” | 3 | “When when I was thinking through these things, we should consider providing a guide like there is the ‘100 Days of Autism.’ So it’s like day one, what are you supposed to be thinking of, day two. Like it’s a day by day thing that guides some, a parent through a first diagnosis of autism. And so something, like you’re saying, like a timeline or something with the NICU, like these are during the first week when you’re out of the NICU, consider these things. During the second week, consider these things, or the first month.” |
| (c) Consider providing classes around discharge/transition issues | 31 | 27 | “Being a first-time mom with a child with a disability, they gave me a lot of resources, but even with the resources… Like, seriously even though I took the CPR classes and everything I still panicked a couple of times. But eventually the older she got the more better I got. The more classes I went to, the more knowledge I got from other people, and resources, the better I became, and the easier it became.” “The parenting hour that they would have… I liked those so much because they would have different subjects that they would touch on in each class. And they would really give you some very vital information that you needed. They would even have other parents come in and talk to you. They would have different nurses come in and talk to the group. And it was really, really very helpful. I just wish, I honest to god wish that there was more of those classes every week, instead of just like one or two.” | 4 | “Wouldn’t it be great if a family who knew how to put a G-tube in could, could rotate around and could do classes or… [another provider} got a grant from the Regional Center to help bring in a family navigator to help families navigate the Regional Center with classes.” |
| (d) Reminders and notifications | 18 | 10 | “I think it’s very useful to remind you of any appointments or anything that you have to do at the clinic or hospital.” | 8 | “Maybe direct links, if you can attach ‘em on, instead of them having to go through, five different links in one website, have the direct form with reminders.” “Connection to updates from the medical team and therapy services. As in, they might get a message, ‘did you forget your refill?’ Or they might get a message ‘Follow up with surgery in two weeks,’ like a bulletin board I suppose.” |
| (e) Tutorials | 46 | 29 | “Actually, I like how you guys have tummy time tutorials… parents hours are absolutely amazing.” “Do they have an option for how to switch out the G-tube, like, step-by-step instructions?” | 17 | “I would imagine that [tutorials] would also help standardize discharge teaching too because we have wildly different teaching styles.” “Because you may not know how to fill out that information… And then there might even be a way to say if you don’t have this number, like this is how you would obtain it and have like side links off that, so that you don’t get stuck on one component of it and not be able to complete the rest of the form.” |
| Domain 2: Timing of events around discharge (In the NICU, around transition and post-discharge care) | 40 | 14 | “Well my fears when I left were being a first-time mom you’re kind of scared, especially with special needs children, because you wonder if she’s [the baby] is going to live to say am I doing it right...guiding first time moms is important.” “She has a lot of therapy. So, just trying to like, have a good schedule for her and figuring out when is what… somehow, someway, we’ve been pulling through good.” | 26 | “Like in our discharge [plan], I think we have different, time intervals, for what’s relevant in that time. So dividing it from like a timeframe to discharge, what would be in the most relevant at that point, so that they can focus their attention to that next step.” “I think setting up or educating the family on what is expected of them… what kind of tasks they need to learn as well as the timeline. And how to go about that. Because some families expect people just to come to them and teach. Whereas they have, it’s a give and take thing, you know, I’m here today, and I need to learn X, Y, and Z, or what do I need to learn.” |
| N | Patient | Provider | |||
|---|---|---|---|---|---|
| Domain/Theme | N | Illustrative Quotations | N | Illustrative Quotations | |
| Domain 3: Path planning | |||||
| (a) Providing a discharge summary embedded in application | 17 | 0 | 17 | “[We should include] an updated discharge summary. A lot of families read the summary, and they are either confused by the jargon because it’s, you know, physician to physician or sometimes they don’t remember that that child had this or that, or this diagnosis that completely resolved etcetera, etcetera.” | |
| (b) Embedded patient navigation assistance with parent navigators | 21 | 21 | “When my son had hearing loss, I don’t remember the name of the organization, but there was some organization that paired me up with a parent mentor that was super helpful. And I was just thinking, if there could be something like that [at our hospital]. Like my son’s primary need is in the pulmonary area. So if you could have like another parent of a kid with lung issues kind of partner up with you … I think that would’ve been massively helpful, and I mean, I’d totally be happy to do that with someone else. And explain all these different programs and insurance and how DNEs work and all that stuff. Like Regional and therapy. That was a lot to try and figure out, and took a long time to kind of navigate all of those. So I think something like that would be incredibly helpful, if there was like a volunteer system, you know, than they get pair you up with someone.” | 0 | |
| (c) Coordination with the medical home | 22 | 7 | “But it was quite a while before I even heard they had they had a medical home department. And I ended up working so much with our pulmonology care coordinator, nurse care coordinator. She’s done most of that stuff for me. But that would be super helpful to know, ‘cause I didn’t know they had that department for quite a while.” | 15 | “So, the, the medical home in [clinic] has sort of sheets on, like, okay, here’s your durable medical equipment, you know, until, so, sort of, putting it together, not, not just a, an electronic medical record but also one that’s parent-focused. So, it has everybody that I need to contact and, you know, the calendar and person, and what my insurance covers, and medications, and everything, just, we build that, it goes from our system to theirs and, and out to the community.” “And that’s what we see in the HRF [High Risk Infant Follow Up Program] environment… the breakdowns in that transition planning and the connections with the other services. So, sometimes they don’t have an appointment with pulmonology. They don’t have an appointment with cardiology, and then they’re, sort of, floating and then, that’s just increasing the anxiety around how do I care for my baby if I can get connected. And it is sort of, quarterbacking all that in the medical home. So, we, we often are failing primary care providers and walking them down to [clinic] because the community providers can’t manage some of the kids you guys are discharging. They can’t, they can’t connect them with the resources that can support them, so.” “Technically if they have a pediatrician, technically that pediatrician could be a medical home, if they’re, you know, supporting the family appropriately, right? Again it varies how how comfortable some of the community pediatricians feel connecting the family to, back to the specialist here, back to resources, when the, when there’s been those gaps. So that’s often an area that we are um intervening.” |
| (d) Facilitating appointment scheduling/referrals to specialists | 29 | 9 | “Sometimes I have personal things that I need to do. So, it’s a little hard trying to overlap that. They’re not, the therapies are not long it’s just they’re at the timing that like, most of the things that I need to take care of are the only available time. So, I try to make it as positive as I can.” | 20 | “And another part of the problem with accessing services and referrals outside is if we’re asking them to do so much, we’re asking them to make appointments with ten different specialists and call the Regional Center, and go to WIC, and call to get refills for your formula and your G-tube supplies, and they may, they may have 20 phone calls a month in that first two weeks to, to try to arrange all this in their life.” |
| Domain 4: Provision of information | |||||
| (a) Requested content area: accessing and using medications/durable medical equipment | 99 | 79 | “Going home … they teach you how to use everything, they show you how to do it. You have a good basic handle on how to use the machinery. But then it’s just using it by yourself, trying to make sure that you don’t do anything wrong that messes up and then end up sending your child back to the hospital. And if you accidentally miss this because you’re so worn out and tired, then you’re gonna mess up everything … it’s nerve-racking knowing that all of this is soon gonna be your, your issue, your things to deal with.” “feel like more than anything, like, the whole process of like, how the oxygen works … because obviously, they’re premature, so some babies de-sat … I feel like more of like, like, those, that kind of area, I would feel like it would be helpful if there would be more information.” “I mean I think all the equipment training was really helpful. Like the G-tube class was really helpful. But I had one nurse in particular who I remember really kind of like warned us how careful we needed to be and how easily he could end up back in the hospital. And most people didn’t really talk that way. So it was really helpful, some of her advice on how to keep your kid out of the hospital.” | 20 | “And this is, to build on that their medications and where they get them. And it’s an ongoing problem. Where, who refills my Albuterol? Who refills my Sildenafil? Because a pediatrician doesn’t refill all of those. And they could probably but sometimes, the CCS panel doctor and sometimes with the community pediatricians, they’re not going to touch the pulmonary meds, I don’t want you guys to do that, you check the electrolytes and you refill the sodium because I never give that. So, they don’t know where to get the refills.” |
| (b) Requested content area: community-based services | 72 | 34 | “And like she said, it’s hard, it’s hard. Like she said, her husband doesn’t even have a job. You know, and they just living and it’s hard. And a little help would do, like two times you could give us a food voucher, you know, when we go home, go here, here’s a, a gift certificate for some diapers, you know. Because I think it’s, it’s, it’s needed. You know? I’m, you know, I’m struggling.” | 38 | “I think you touched on the key point … when they do actually get the resources, it resonates with them. My last research was talking to these moms that were discharged. And the ones that said that the social workers offered it in the NICU, it helped them tremendously throughout … identifying them in the first place, to give them those resources are the hardest.” “Some of the units that I’ve been to, we do have weekly or monthly support group. And it’s family there discussing. And the topics may be different, and different things will come up, but, but things like doing the early intervention or regional center is really important, how do you get to it, how, what forms do you have to fill out, what are the shortcuts, you know. Those type of things can really come out in family support groups.” |
| (c) Requested content area: accessing mental health services | 35 | 14 | “I don’t remember being given anything. Unless I’m forgetting. I don’t think I was. I mean my OB would check in a tiny bit. I think I had one or two follow-ups with her. Like kind of just screening for post-, post-partum depression and things. I don’t think the NICU specifically did anything. But honestly, that would be super helpful. They could even just have like a counselor come and sit and offer their services, I would have loved that. Just, I like used to do that a little bit with a social worker and with some of the chaplains, and it was so helpful to have someone to talk to, but, yeah, I would love it if they had a counselor who was available to the parents. I wasn’t aware of it if they did.” | 21 | “The rates of postpartum depression that like we get from clinic are probably lower, that probably moms are maybe underreporting to the pediatrician. And then the big challenge then is linking them to community-based resources. One thing at least with the earlier postpartum moms that we see, they need to be depressed and need therapy, but they can’t get out of the house with the baby they don’t have a ride.” |
| Domain 5: Accessing support | |||||
| (a) Family support | 34 | 27 | “I just cheer her on. My mom, and my sister help me out a lot. We’re just like, cheering her on like, yes, you could do this. Like, she barely started walking. So, we just try to cheer her on in that, or we tell her oh, we’re going to go somewhere.” “I have support with my family. I will tell you that. I call my family for everything, okay, cause they’ve been there with kids. They have grown kids. So I try to basically call them and be like, hey, what do you do when this happens, or what happens when you do this? That’s what I do. I’m a crybaby to my family.” “I had a lot going on, you know, with my daughter and that really was my main focus and that really demanded all of my attention. But, you know, it wasn’t ‘til later that she was a lot stronger, and I could kind of sit there and relax a bit more. And then that’s kind of what I realized, you know, I am depressed. I do have a lot on my mind. I am almost at my breaking point emotionally, and it was just overwhelming and, you know, yeah, you can talk to your family, and you can talk to your spouse.” “Scared the hell outta me. But the person who watches him is his godmother. And she actually took G tube classes with me and everything like that. So she’s the only person that I can like legit trust to watch him and I don’t fear anything. And my job is in the same, you know, area, so I’m not too far away from him.” | 7 | “Social support is the same way … when I hear that ‘I’m living with my mother and my aunt helps,’ my stress level goes down because I know you have backups, and your other child can get cared for, and you can be here and if the dads not present, that’s a red flag.” |
| (b) Peer support | 78 | 60 | “You can talk to, you know, maybe other friends if you are to have children who may or may not have their issues and whatnot. But just somebody to listen, somebody you can just be privy to, somebody. I mean honestly even if it were Joe Schmo on the other end of an email, you know, just somebody you can even type a long 30-page novel to about how you feel and what you’re going through and how all that makes you feel and how your world really does feel like it got flipped upside down and inside out.” “She was saying, at first of course you’re scared because now you’re coming home with a baby that has a disability and you don’t know how you’re going to cope, and try to go with your everyday life too, but, it was a great experience because, they had already gone home. Unfortunately, their son had to come back to the hospital, but, it was a great learning experience for us because, like, that’s okay. This is what we did wrong. This is what you shouldn’t do wrong. So all the pointers that they gave us were very good.” | 18 | “Pairing somebody who’s gone through the process and knows what it takes, so maybe knows the next step like would be ideal a situation, like a mommy support group, you know, parent support group.” |
| (c) Religious support | 10 | 10 | “I don’t know if he was like a chaplain or a reverend, or I’m not sure. But, he came and kind of, you know, talked to me a little bit and told me about the prayer center.” “My family … But I also found, a lot of support through the church.” | 0 | |
| (d) Support group | 21 | 10 | “To be honest with you, people are all different. A section for both would be great. Like, if they wanted to go find a group that they can talk in, or if they were more, like me, not so apt to just finding a whole group of people you don’t know to spill your business in front of, and you just want to talk to like, one person, simple, just, straight to the point, having somebody do Facetime like this or just chatting with them would, would help a lot, an unbiased opinion to talk to, right then and there.” “Yes and then also maybe having like a little chat group with other parents and just talk about, you know, just everything that they went through, and just so I won’t feel alone. ‘Cause um sometimes like it’s really hard for me to talk to other people about what I went through because it’s just really traumatic for me.” | 11 | “I highlight what [other focus group participant] was saying about support groups because I also listed it as one of the things that we don’t have and would really be important for us to have because simply getting over the language barrier wouldn’t be enough I don’t think. The cultural barrier and having a support group that you know is non-judgmental—the support group would explain to you, this is my trick for having two kids and bringing them both to the appointment with my other kid to a therapy. And this is how I get around it. That support group might explain, this is the train I take, these are the days I make this appointment, this is when doctor so and so is in.” “Some of the units that I’ve been to, we do have weekly or monthly support groups. And it’s family there discussing. And the topics may be different, and different things will come up, but, things like doing the early intervention or regional center is really important, how do you get to it, what forms do you have to fill out, what are the shortcuts, you know. Those type of things can really come out in family support groups. So you’re gonna have family who’s been here longer period of time, have seen more things going on, and parents that are just here for like one week and still kind of wide-eyed and learning all of the resources that’s available to them.” |
| N | Patient | Provider | |||
|---|---|---|---|---|---|
| Domain/Theme | N | Illustrative Quotations | N | Illustrative Quotations | |
| Domain 6: Engagement with providers | |||||
| (a) Communication with pediatricians | 34 | 6 | “And, you know, I think a lot of it too was, again, feeling that she looked and seemed so healthy … And I felt for a long time that somehow I was being inadvertently blamed for her not gaining more quickly. Nobody told me about that. You know, when we are, they do the transition from being in the hospital to going home. But we basically even now, we still have, you know, pediatrician’s appointments and whatnot and I have to keep a food diary and, you know, it’s daunting, it’s just, it’s constant. I didn’t get that memo, apparently.” | 28 | “There’s a lot that we can do for that that we don’t …. I called your pediatrician last week, we’ve talked, they’ve asked a bunch of questions, I’m going to let them know, the day before, again, that you’re going home, and this is the final word, and if they have any more quest-, that would make them feel more confident if they had some of them don’t even know that we call their pediatrician at all, even if we have.” “Yeah. I know when I ask the front-line providers to call the pediatrician with an update, call them with a handoff and all that, there’s many times that I get pushback and say, well, give the parents the discharge summary, they’ll plan it out. And that really needs to be enforced from not just me, but from somebody higher up than me to call, even just, maybe not the simple ones, maybe have some guidelines. But I know on, on the complex kids, I’ll often call and deal them out. You know, this is baby with X, Y, Z, can you, do you have the resources to take of it in your clinic? sometimes they’ll say no, I’m the only pediatrician, I’m only here once a week and it’s nurse practitioners.” |
| (b) Communication and importance of clinical care coordinators | 21 | 9 | “I was thinking something that could be helpful at discharge is maybe giving you the contact info of like your nurse care coordinator or someone from the high-risk clinic. Those people have been amazingly helpful to me, but I didn’t have their contact info at the beginning, and I didn’t realize how much they could help me … They’ve advocated for me. They’ve told me what I can push for. ‘Cause I think at the beginning I didn’t understand how much you had to advocate for your kid, so I would be told no by insurance and didn’t realize I kind of just had to keep pushing and to get stuff. And so those people have done that for me.” | 12 | “Cause I literally did spend two hours trying to get to these clinics and get them numbers, and the dates and times.” “Yeah. I think the fact of the matter with regional center … we work with them continuously with all of our patients, is that advocating for your baby is number one. They are very impacted. They have too many patients, not enough therapists … so the ball often gets dropped. And I think part of the education piece should be you need to continually call, they are not going to call you.” |
| Domain 7: Barriers to care after discharge | |||||
| (a) Health literacy | 11 | 5 | “And it would’ve been so helpful, though, too, to understand more what tests were being done and for what reasons and what the results mean. And, okay, she had a blood gas number of X. Okay, well what does that mean? it’d be nice to have some sort of way to like decode all of this stuff. So, it’d be great if, you know, that was the case.” | 6 | “I think you know there’s a lot that … their baseline reading level may not be high, so the info we’re throwing is um really difficult to comprehend.” |
| (b) Language/cultural barriers | 13 | 0 | 13 | “I feel like sometimes there’s a language barrier because I feel families might not be familiar with all the different resources that are available, they might be scared that they don’t speak their language, that they won’t get the support that other families need.” “I highlight what [co participant} was saying about support groups because simply getting over the language barrier wouldn’t be enough I don’t think. The cultural barrier and having a support group that you know is non-judgmental um, that support group would explain to you, this is my trick for having two kids and bringing them both to the appointment with my other kid to a therapy. And this is what I, this is how I get around it.” | |
| (c) Transportation/housing | 21 | 14 | “You know, my biggest, my biggest thing is maybe … I know it’s probably far-fetched, but maybe you guys could have some transportation for people that really need [it] … Maybe people on the bus or, or walking, or that don’t have transportation, maybe we could have maybe a free shuttle.” | 7 | “And then, some of these parents don’t have, like, a car for example, and so, it’s public transportation to all the different, like, offices and Regional Centers and some specialist’s appointments can be also really hard for them too?” |
| Domain 8: Parenting role and confidence | |||||
| (a) Parenting confidence and parenting role | 20 | 14 | “I feel like the only thing that I do remember one of the nurses telling me that, she, that to not really like be scared but more like to see like, it’s really hard to explain because more than anything, I was just scared because I had never seen a premature baby.” “It’s for regular babies, that’s why I feel like it would be more difficult because, there was some moms that I could, like, relate to. Most of them never really had the experience of prematurity. So, I feel like that would be useful to like, have something more specifically to premature baby.” | 6 | “Parenting confidence is ironic in that first-time parents who deliver in a birthing center, take their kids home on day two will tell I do not know what I’m doing. It is the same lack of confidence that, that families in the NICU feel except for the fact that this child is more likely to have a big setback with their lack of confidence. And that is what drives the fear and the anxiety. Not that more so, that they don’t know what they’re doing like any other parent, but if another parent forgets to feed their kid they’ll just catch up on the next one, and in this one, this feeding was supposed to go over a pump, over two hours, this child has some insulin instability, glucose instability, and that, anxiety is definitely a big deal.” “Yeah. I think that, I don’t know, just going to what [participant] was saying which is about parents being at the bedside and just forming those bonds … I think that kind of fosters a lot awareness of the baby and builds their confidence that they know that they can provide for their baby, even if they’re not a doctor and they’re not a nurse, and they’re not a specialist, like, they can, they have the means to be able to provide for their baby and comfort their baby.” |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lakshmanan, A.; Sunshine, I.; Calvetti, S.; Espinoza, J.; Santoro, S.; Butala, S.; House, M.; Kipke, M. Designing a Mobile Health Solution to Facilitate the Transition from NICU to Home: A Qualitative Study. Children 2022, 9, 260. https://doi.org/10.3390/children9020260
Lakshmanan A, Sunshine I, Calvetti S, Espinoza J, Santoro S, Butala S, House M, Kipke M. Designing a Mobile Health Solution to Facilitate the Transition from NICU to Home: A Qualitative Study. Children. 2022; 9(2):260. https://doi.org/10.3390/children9020260
Chicago/Turabian StyleLakshmanan, Ashwini, Isabel Sunshine, Sam Calvetti, Juan Espinoza, Sofia Santoro, Saloni Butala, Madison House, and Michele Kipke. 2022. "Designing a Mobile Health Solution to Facilitate the Transition from NICU to Home: A Qualitative Study" Children 9, no. 2: 260. https://doi.org/10.3390/children9020260
APA StyleLakshmanan, A., Sunshine, I., Calvetti, S., Espinoza, J., Santoro, S., Butala, S., House, M., & Kipke, M. (2022). Designing a Mobile Health Solution to Facilitate the Transition from NICU to Home: A Qualitative Study. Children, 9(2), 260. https://doi.org/10.3390/children9020260






