Emotion Dysregulation as a Mediator of the Relationship between Anxiety, Compulsive Exercise and Eating Disorder Symptoms in Adolescents
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Instruments
2.3. Procedure
2.4. Statistical Analysis
3. Results
3.1. Sample Characteristics
3.2. Descriptive Statistics and Correlations
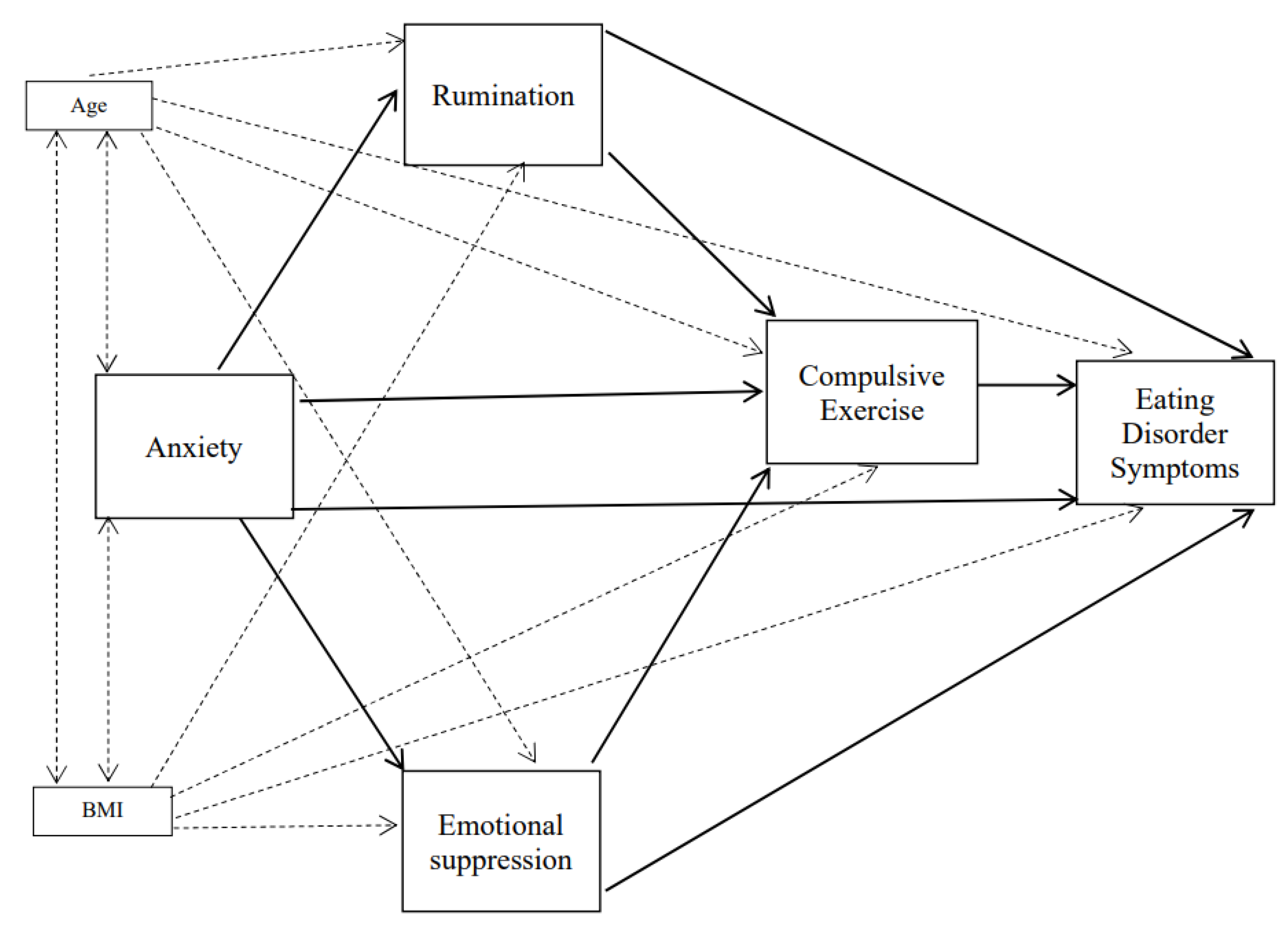
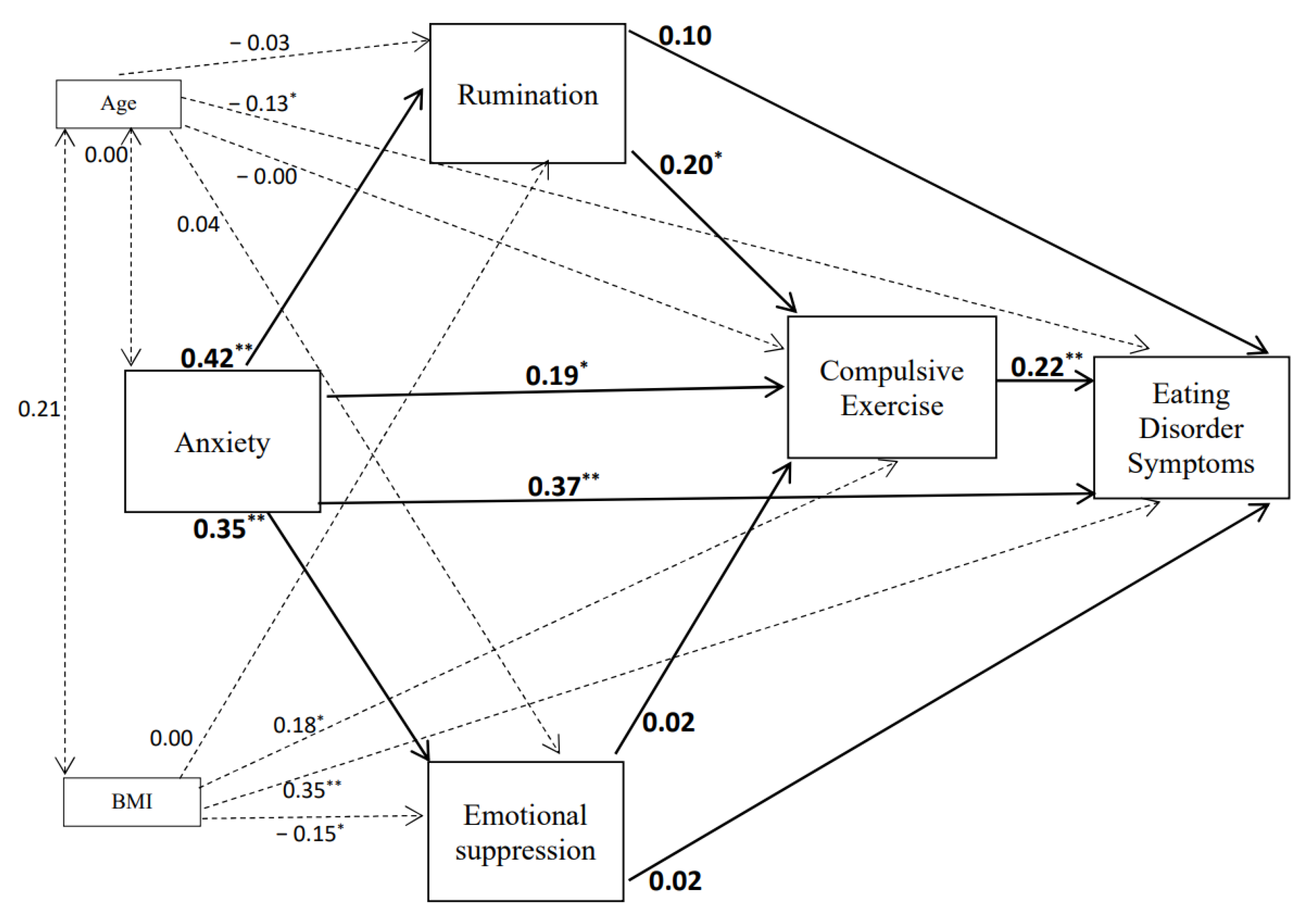
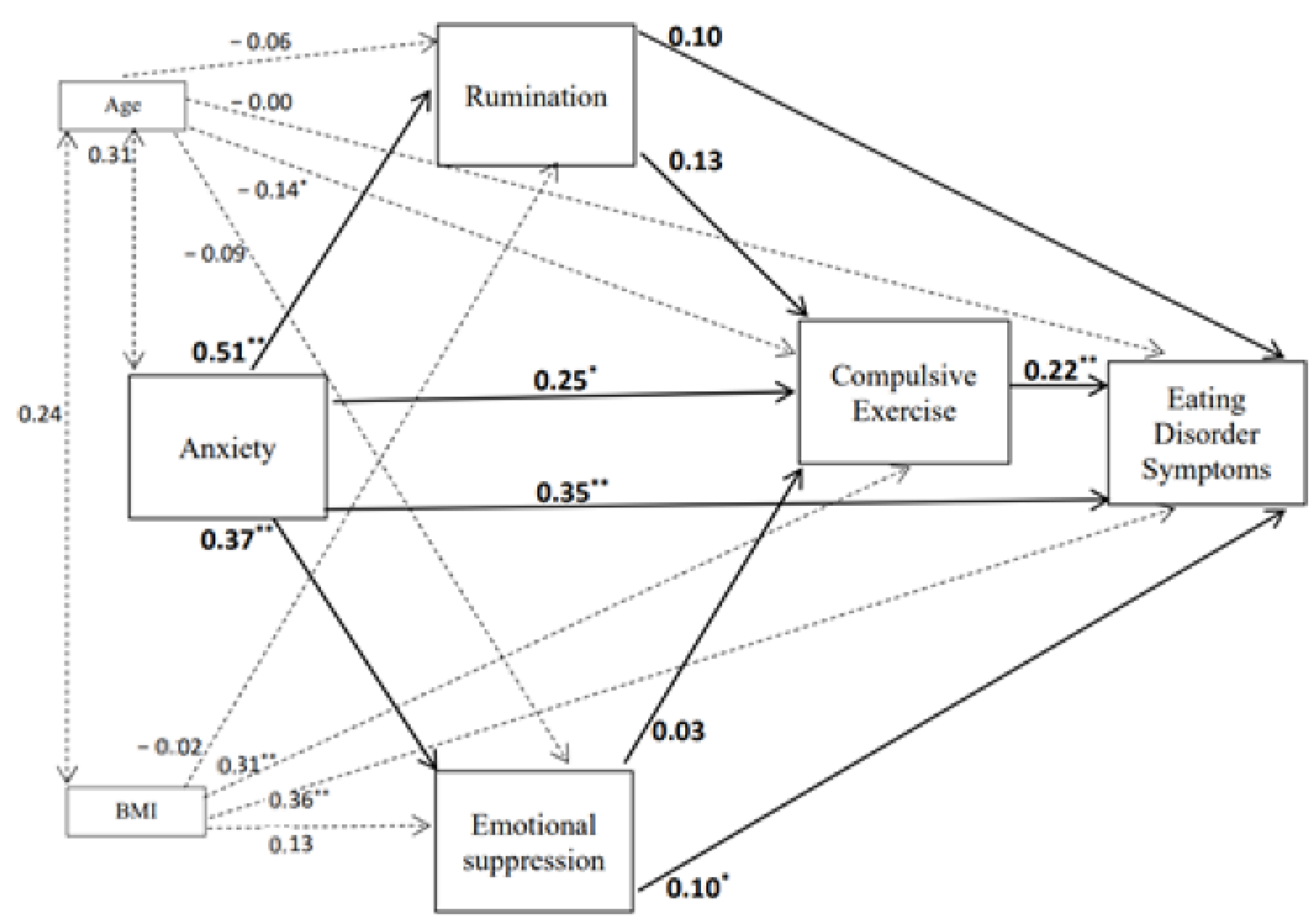
3.3. Structural Equation Models
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Meyer, C.; Taranis, L.; Goodwin, H.; Haycraft, E. Compulsive exercise and eating disorders. Eur. Eat. Disord. Rev. 2011, 19, 174–189. [Google Scholar] [CrossRef]
- Brewerton, T.D.; Stellefson, E.J.; Hibbs, N.; Hodges, E.L.; Cochrane, C.E. Comparison of eating disorder patients with and without compulsive exercising. Int. J. Eat. Disord. 1995, 17, 413–416. [Google Scholar] [CrossRef]
- Davis, C.; Katzman, D.K.; Kaptein, S.; Kirsh, C.; Brewer, H.; Kalmbach, K.; Kaplan, A.S. The prevalence of high-level exercise in the eating disorders: Etiological implications. Compr. Psychiatry 1997, 38, 323–326. [Google Scholar] [CrossRef]
- Bentley, C.; Gratwick-Sarll, K.; Harrison, C.; Mond, J. Sex differences in psychosocial impairment associated with eating disorder features in adolescents: A school-based study. Int. J. Eat. Disord. 2015, 48, 633–640. [Google Scholar] [CrossRef] [PubMed]
- Young, S.; Touyz, S.; Meyer, C.; Arcelus, J.; Rhodes, P.; Madden, S.; Pike, K.; Attia, E.; Crosby, R.D.; Hay, P. Relationships between compulsive exercise, quality of life, psychological distress and motivation to change in adults with anorexia nervosa. J. Eat. Disord. 2018, 6, 2. [Google Scholar] [CrossRef]
- Smith, A.R.; Fink, E.L.; Anestis, M.D.; Ribeiro, J.D.; Gordon, K.H.; Davis, H.; Joiner, T.E., Jr. Exercise caution: Over-exercise is associated with suicidality among individuals with disordered eating. Psychiatry Res. 2013, 206, 246–255. [Google Scholar] [CrossRef] [PubMed]
- Taliaferro, L.A.; Rienzo, B.A.; Miller, M.D.; Pigg, R.M.; Dodd, V.J. High School Youth and Suicide Risk: Exploring Protection Afforded Through Physical Activity and Sport Participation. J. Sch. Heal 2008, 78, 545–553. [Google Scholar] [CrossRef]
- Ganson, K.T.; Mitchison, D.; Rodgers, R.F.; Cunningham, M.L.; Murray, S.B.; Nagata, J.M. Compulsive exercise among college students: 5-year time trends in prevalence and demographic, substance use, and mental health correlates. Eat. Weight. Disord.-Stud. Anorexia Bulim. Obes. 2021, 1–12. [Google Scholar] [CrossRef]
- Bahji, A.; Mazhar, M.N.; Hudson, C.C.; Nadkarni, P.; MacNeil, B.A.; Hawken, E. Prevalence of substance use disorder comorbidity among individuals with eating disorders: A systematic review and meta-analysis. Psychiatry Res. 2019, 273, 58–66. [Google Scholar] [CrossRef] [PubMed]
- Heathers, J.; Nagata, J.; Murray, S. What’s at the heart of anorexia nervosa? Reconsidering the physiology of bradycardia in anorexia Nerovsa. PsyArXiV 2017. [Google Scholar] [CrossRef]
- Fietz, M.; Touyz, S.; Hay, P. A risk profile of compulsive exercise in adolescents with an eating disorder: A systematic review. Adv. Eat. Disord. 2014, 2, 241–263. [Google Scholar] [CrossRef]
- Carpine, L.; Charvin, I.; Da Fonseca, D.; Bat-pitault, F. Clinical features of children and adolescents with anorexia nervosa and problematic physical activity. Eat. Weight. Disord.-Stud. Anorex. Bulim. Obes. 2021, 1–11. [Google Scholar] [CrossRef]
- Renz, J.A.; Fisher, M.; Vidair, H.B.; Hirsch, D.; Malizio, J.; Barger, H.; Fornari, V. Excessive exercise among adolescents with eating disorders: Examination of psychological and demographic variables. Int. J. Adolesc. Med. Health 2019, 31, 20170032. [Google Scholar] [CrossRef]
- McCabe, M.P.; Ricciardelli, L.A. Extreme weight change behaviours: Are overweight and normal weight adolescents different, and does this vary over time? Eur. Eat. Disord. Rev. 2009, 17, 301–314. [Google Scholar] [CrossRef]
- Goodwin, H.; Haycraft, E.; Willis, A.-M.; Meyer, C. Compulsive exercise: The role of personality, psychological morbidity, and disordered eating. Int. J. Eat. Disord. 2011, 44, 655–660. [Google Scholar] [CrossRef] [PubMed]
- Goodwin, H.; Haycraft, E.; Meyer, C. Psychological risk factors for compulsive exercise: A longitudinal investigation of adolescent boys and girls. Personal. Individ. Differ. 2014, 68, 83–86. [Google Scholar] [CrossRef]
- Selby, E.A.; Anestis, M.D.; Joiner, T.E. Understanding the relationship between emotional and behavioral dysregulation: Emotional cascades. Behav. Res. Ther. 2008, 46, 593–611. [Google Scholar] [CrossRef]
- Selby, E.A.; Franklin, J.; Carson-Wong, A.; Rizvi, S.L. Emotional Cascades and Self-Injury: Investigating Instability of Rumination and Negative Emotion. J. Clin. Psychol. 2013, 69, 1213–1227. [Google Scholar] [CrossRef] [PubMed]
- Arbuthnott, A.E.; Lewis, S.P.; Bailey, H.N. Rumination and Emotions in Nonsuicidal Self-Injury and Eating Disorder Behaviors: A Preliminary Test of the Emotional Cascade Model. J. Clin. Psychol. 2015, 71, 62–71. [Google Scholar] [CrossRef] [PubMed]
- Tuna, E.; Bozo, Ö. Exploring the Link Between Emotional and Behavioral Dysregulation: A Test of the Emotional Cascade Model. J. Gen. Psychol. 2014, 141, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Nolen-Hoeksema, S. Emotion Regulation and Psychopathology: The Role of Gender. Annu. Rev. Clin. Psychol. 2012, 8, 161–187. [Google Scholar] [CrossRef] [PubMed]
- Rivière, J.; Rousseau, A.; Douilliez, C. Effects of induced rumination on body dissatisfaction: Is there any difference between men and women? J. Behav. Ther. Exp. Psychiatry 2018, 61, 1–6. [Google Scholar] [CrossRef]
- Naumann, E.; Tuschen-Caffier, B.; Voderholzer, U.; Schäfer, J.; Svaldi, J. Effects of emotional acceptance and rumination on media-induced body dissatisfaction in anorexia and bulimia nervosa. J. Psychiatr. Res. 2016, 82, 119–125. [Google Scholar] [CrossRef]
- Naumann, E.; Tuschen-Caffier, B.; Voderholzer, U.; Caffier, D.; Svaldi, J. Rumination but not distraction increases eating-related symptoms in anorexia and bulimia nervosa. J. Abnorm. Psychol. 2015, 124, 412–420. [Google Scholar] [CrossRef]
- Goossens, L.; Van Malderen, E.; Van Durme, K.; Braet, C. Loss of control eating in adolescents: Associations with adaptive and maladaptive emotion regulation strategies. Eat. Behav. 2016, 22, 156–163. [Google Scholar] [CrossRef]
- Nolen-Hoeksema, S.; Stice, E.; Wade, E.; Bohon, C. Reciprocal relations between rumination and bulimic, substance abuse, and depressive symptoms in female adolescents. J. Abnorm. Psychol. 2007, 116, 198–207. [Google Scholar] [CrossRef] [PubMed]
- McLaughlin, K.A.; Nolen-Hoeksema, S. Rumination as a transdiagnostic factor in depression and anxiety. Behav. Res. Ther. 2011, 49, 186–193. [Google Scholar] [CrossRef]
- Dondzilo, L.; Rieger, E.; Palermo, R.; Byrne, S.; Bell, J. Association between rumination factors and eating disorder behaviours in young women. Adv. Eat. Disord. 2016, 4, 84–98. [Google Scholar] [CrossRef]
- Smith, K.E.; Mason, T.B.; Lavender, J.M. Rumination and eating disorder psychopathology: A meta-analysis. Clin. Psychol. Rev. 2018, 61, 9–23. [Google Scholar] [CrossRef]
- Xie, Y.; Kong, Y.; Yang, J.; Chen, F. Perfectionism, worry, rumination, and distress: A meta-analysis of the evidence for the perfectionism cognition theory. Personal. Individ. Differ. 2019, 139, 301–312. [Google Scholar] [CrossRef]
- Wahl, K.; Ertle, A.; Bohne, A.; Zurowski, B.; Kordon, A. Relations between a ruminative thinking style and obsessive–compulsive symptoms in non-clinical samples. Anxiety Stress Coping 2011, 24, 217–225. [Google Scholar] [CrossRef]
- Smith, K.E.; Mason, T.B.; Anderson, N.L.; Lavender, J.M. Unpacking cognitive emotion regulation in eating disorder psychopathology: The differential relationships between rumination, thought suppression, and eating disorder symptoms among men and women. Eat. Behav. 2019, 32, 95–100. [Google Scholar] [CrossRef] [PubMed]
- Fisher, M.; Schneider, M.; Burns, J.; Symons, H.; Mandel, F.S. Differences between adolescents and young adults at presentation to an eating disorders program. J. Adolesc. Health 2001, 28, 222–227. [Google Scholar] [CrossRef]
- Gross, J.J. The Emerging Field of Emotion Regulation: An Integrative Review. Rev. Gen. Psychol. 1998, 2, 271–299. [Google Scholar] [CrossRef]
- Geller, J.; Cockell, S.J.; Hewitt, P.L.; Goldner, E.M.; Flett, G.L. Inhibited expression of negative emotions and interpersonal orientation in anorexia nervosa. Int. J. Eat. Disord. 2000, 28, 8–19. [Google Scholar] [CrossRef]
- Hayaki, J.; Friedman, M.A.; Brownell, K.D. Emotional expression and body dissatisfaction. Int. J. Eat. Disord. 2002, 31, 57–62. [Google Scholar] [CrossRef] [PubMed]
- Fox, J.R.E.; Smithson, E.; Baillie, S.; Ferreira, N.; Mayr, I.; Power, M.J. Emotion Coupling and Regulation in Anorexia Nervosa. Clin. Psychol. Psychother. 2013, 20, 319–333. [Google Scholar] [CrossRef]
- Brownstone, L.M.; Fitzsimmons-Craft, E.E.; Wonderlich, S.A.; Joiner, T.E.; Le Grange, D.; Mitchell, J.E.; Crow, S.J.; Peterson, C.B.; Crosby, R.D.; Klein, M.H.; et al. Hard exercise, affect lability, and personality among individuals with bulimia nervosa. Eat. Behav. 2013, 14, 413–419. [Google Scholar] [CrossRef][Green Version]
- Wegner, D.M. White Bears and Other Unwanted Thoughts: Suppression, Obsession, and the Psychology of Mental Control; Penguin Press: New York, NY, USA, 1989. [Google Scholar]
- Goodwin, H.; Haycraft, E.; Meyer, C. The relationship between compulsive exercise and emotion regulation in adolescents. Br. J. Health Psychol. 2012, 17, 699–710. [Google Scholar] [CrossRef] [PubMed]
- Goodwin, H.; Haycraft, E.; Meyer, C. Emotion regulation styles as longitudinal predictors of compulsive exercise: A twelve month prospective study. J. Adolesc. 2014, 37, 1399–1404. [Google Scholar] [CrossRef]
- Johnson, D.P.; Whisman, M.A. Gender differences in rumination: A meta-analysis. Personal. Individ. Differ. 2013, 55, 367–374. [Google Scholar] [CrossRef] [PubMed]
- Opwis, M.; Schmidt, J.; Martin, A.; Salewski, C. Gender differences in eating behavior and eating pathology: The mediating role of rumination. Appetite 2017, 110, 103–107. [Google Scholar] [CrossRef]
- Cai, A.; Lou, Y.; Long, Q.; Yuan, J. The Sex Differences in Regulating Unpleasant Emotion by Expressive Suppression: Extraversion Matters. Front. Psychol. 2016, 7, 1011. [Google Scholar] [CrossRef]
- Wang, K.; Huang, H.; Chen, L.; Hou, X.; Zhang, Y.; Yang, J.; Hao, X.; Qiu, J. MRI correlates of interaction between gender and expressive suppression among the Chinese population. Neuroscience 2017, 347, 76–84. [Google Scholar] [CrossRef]
- Sharp, C.W.; Clark, S.A.; Dunan, J.R.; Blackwood, D.H.R.; Shapiro, C.M. Clinical presentation of anorexia nervosa in males: 24 new cases. Int. J. Eat. Disord. 1994, 15, 125–134. [Google Scholar] [CrossRef]
- Margo, J.L. Anorexia Nervosa in Males. Br. J. Psychiatry 1987, 151, 80–83. [Google Scholar] [CrossRef]
- Lewinsohn, P.M.; Seeley, J.R.; Moerk, K.C.; Striegel-Moore, R.H. Gender differences in eating disorder symptoms in young adults. Int. J. Eat. Disord. 2002, 32, 426–440. [Google Scholar] [CrossRef]
- Murray, S.B.; Griffiths, S.; Rieger, E.; Touyz, S. A comparison of compulsive exercise in male and female presentations of anorexia nervosa: What is the difference? Adv. Eat. Disord. 2014, 2, 65–70. [Google Scholar] [CrossRef]
- Anderson, C.B.; Bulik, C.M. Gender differences in compensatory behaviors, weight and shape salience, and drive for thinness. Eat. Behav. 2004, 5, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Stice, E.; Gau, J.M.; Rohde, P.; Shaw, H. Risk factors that predict future onset of each DSM–5 eating disorder: Predictive specificity in high-risk adolescent females. J. Abnorm. Psychol. 2017, 126, 38–51. [Google Scholar] [CrossRef] [PubMed]
- Allen, K.L.; Byrne, S.M.; Crosby, R.D.; Stice, E. Testing for interactive and non-linear effects of risk factors for binge eating and purging eating disorders. Behav. Res. Ther. 2016, 87, 40–47. [Google Scholar] [CrossRef]
- Elosua, P.; López-Jáuregui, A.; Sánchez-Sánchez, F. EDI-3, Inventario de Trastornos de la Conducta Alimentaria-3, Manual; TEA Ediciones: Madrid, Spain, 2010. [Google Scholar]
- Garner, D.M. Eating Disorder Inventory-3 (EDI-3). Professional Manual; Psychological Assessment Resources: Odessa, TX, USA, 2004. [Google Scholar]
- Bieling, P.J.; Antony, M.M.; Swinson, R.P. The State--Trait Anxiety Inventory, Trait version: Structure and content re-examined. Behav. Res. Ther. 1998, 36, 777–788. [Google Scholar] [CrossRef]
- Spielberger, C.D.; Gorsuch, R.L.; Lushene, R.; Vagg, P.R.; Jacobs, G.A. Manual for the State-Trait Anxiety Inventory; Consulting Psychologists Press: Palo Alto, CA, USA, 1983. [Google Scholar]
- Sauchelli, S.; Arcelus, J.; Granero, R.; Jiménez-Murcia, S.; Agüera, Z.; Del Pino-Gutiérrez, A.; Fernández-Aranda, F. Dimensions of Compulsive Exercise across Eating Disorder Diagnostic Subtypes and the Validation of the Spanish Version of the Compulsive Exercise Test. Front. Psychol. 2016, 7, 1852. [Google Scholar] [CrossRef]
- Taranis, L.; Touyz, S.; Meyer, C. Disordered eating and exercise: Development and preliminary validation of the compulsive exercise test (CET). Eur. Eat. Disord. Rev. 2011, 19, 256–268. [Google Scholar] [CrossRef]
- Cuesta-Zamora, C. El Papel Del Ejercicio Compulsivo Y La Inteligencia Emocional En Los Síntomas De Trastorno De La Conducta Alimentaria En Preadolescentes Y Adolescentes; University of Castilla-La Mancha: Albacete, Spain, 2019. [Google Scholar]
- Ricarte, J.J.; Aizpurúa, E.; Ros, L.; Latorre, J.M.; Raes, F. Psychometric Properties of the Spanish Short Depressive Rumination Scale in a Nonclinical Sample. Span. J. Psychol. 2018, 21, E34. [Google Scholar] [CrossRef]
- Raes, F.; Hermans, D.; Williams, J.M.G.; Eelen, P. A sentence completion procedure as an alternative to the Autobiographical Memory Test for assessing overgeneral memory in non-clinical populations. Memory 2007, 15, 495–507. [Google Scholar] [CrossRef] [PubMed]
- Raes, F.; Hermans, D.; Williams, J.M.G.; Bijttebier, P.; Eelen, P. A “Triple W”-Model of Rumination on Sadness: Why Am I Feeling Sad, What’s the Meaning of My Sadness, and Wish I Could Stop Thinking About my Sadness (But I Can’t!). Cogn. Ther. Res. 2008, 32, 526–541. [Google Scholar] [CrossRef]
- Gross, J.J.; John, O.P. Individual differences in two emotion regulation processes: Implications for affect, relationships, and well-being. J. Personal. Soc. Psychol. 2003, 85, 348–362. [Google Scholar] [CrossRef] [PubMed]
- Cabello, R.; Salguero, J.M.; Fernández-Berrocal, P.; Gross, J.J. A Spanish Adaptation of the Emotion Regulation Questionnaire. Eur. J. Psychol. Assess. 2013, 29, 234–240. [Google Scholar] [CrossRef]
- Gómez-Ortiz, O.; Romera, E.M.; Ortega-Ruiz, R.; Cabello, R.; Fernández-Berrocal, P. Analysis of Emotion Regulation in Spanish Adolescents: Validation of the Emotion Regulation Questionnaire. Front. Psychol. 2016, 6, 1959. [Google Scholar] [CrossRef]
- Marfell-Jones, M.J.; Stewart, A.D.; de Ridder, J.H. International Standards for Anthropometric Assessment; International Society for the Advancement of Kinanthropometry: Portsmouth, UK, 2012. [Google Scholar]
- Bentler, P.M. On the fit of models to covariances and methodology to the bulletin. Psychol. Bull. 1992, 112, 400–404. [Google Scholar] [CrossRef] [PubMed]
- Hu, L.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Modeling A Multidiscip. J. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Browne, M.W.; Cudeck, R. Alternative ways of assessing model fit. In Testing Structural Models; Bollen, K.A., Long, J.S., Eds.; Sage: Newbury Park, CA, USA, 1993; pp. 136–162. [Google Scholar]
- Byrne, B.M. Structural Equation Modeling with AMOS: Basic Concepts, Applications, and Programming; Lawrence Erlbaum Associates: Mahwah, NJ, USA, 2001. [Google Scholar]
- Preacher, K.J.; Hayes, A.F. Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behav. Res. Methods 2008, 40, 879–891. [Google Scholar] [CrossRef]
- Jobst, L.J.; Bader, M.; Moshagen, M. A tutorial on assessing statistical power and determining sample size for structural equation models. Psychol. Methods 2021, in press. [Google Scholar] [CrossRef]
- Moshagen, M.; Erdfelder, E. A New Strategy for Testing Structural Equation Models. Struct. Equ. Modeling A Multidiscip. J. 2016, 23, 54–60. [Google Scholar] [CrossRef]
- Boyes, M.E.; Hasking, P.A.; Martin, G. Adverse Life Experience and Psychological Distress in Adolescence: Moderating and Mediating Effects of Emotion Regulation and Rumination. Stress Health 2016, 32, 402–410. [Google Scholar] [CrossRef] [PubMed]
- McEvoy, P.M.; Watson, H.; Watkins, E.R.; Nathan, P. The relationship between worry, rumination, and comorbidity: Evidence for repetitive negative thinking as a transdiagnostic construct. J. Affect. Disord. 2013, 151, 313–320. [Google Scholar] [CrossRef] [PubMed]
- Epling, W.F.; Pierce, W.D. Activity Anorexia: Theory, Research, and Treatment; Lawrence Earlbaum: Mahwah, NJ, USA, 1996. [Google Scholar]
- Lobera, J.I.; Humanes, S.E.; Santiago-Fernández, M.J. Ejercicio físico, conducta alimentaria y patología [Physical activity, eating behavior and pathology]. Arch. Latinoam. De Nutr. 2008, 58, 280–285. [Google Scholar]
- Stiles-Shields, C.E.; Labuschagne, Z.; Goldschmidt, A.B.; Doyle, A.C.; Grange, D. Le. The use of multiple methods of compensatory behaviors as an indicator of eating disorder severity in treatment-seeking youth. Int. J. Eat. Disord. 2012, 45, 704–710. [Google Scholar] [CrossRef]
- Park, R.J.; Dunn, B.D.; Barnard, P.J. Schematic Models and Modes of Mind in Anorexia Nervosa I: A Novel Process Account. Int. J. Cogn. Ther. 2011, 4, 415–437. [Google Scholar] [CrossRef]
- Cowdrey, F.A.; Park, R.J. Assessing rumination in eating disorders: Principal component analysis of a minimally modified ruminative response scale. Eat. Behav. 2011, 12, 321–324. [Google Scholar] [CrossRef] [PubMed]
- Nolen-Hoeksema, S.; Aldao, A. Gender and age differences in emotion regulation strategies and their relationship to depressive symptoms. Personal. Individ. Differ. 2011, 51, 704–708. [Google Scholar] [CrossRef]
- Cook, L.; Mostazir, M.; Watkins, E. Reducing Stress and Preventing Depression (RESPOND): Randomized Controlled Trial of Web-Based Rumination-Focused Cognitive Behavioral Therapy for High-Ruminating University Students. J. Med. Internet Res. 2019, 21, e11349. [Google Scholar] [CrossRef] [PubMed]
- Topper, M.; Emmelkamp, P.M.G.; Watkins, E.; Ehring, T. Prevention of anxiety disorders and depression by targeting excessive worry and rumination in adolescents and young adults: A randomized controlled trial. Behav. Res. Ther. 2017, 90, 123–136. [Google Scholar] [CrossRef] [PubMed]
- Noetel, M.; Dawson, L.; Hay, P.; Touyz, S. The assessment and treatment of unhealthy exercise in adolescents with anorexia nervosa: A Delphi study to synthesize clinical knowledge. Int. J. Eat. Disord. 2017, 50, 378–388. [Google Scholar] [CrossRef]
- Ackard, D.; Brehm, B.; Steffen, J. Exercise and Eating Disorders in College-Aged Women: Profiling Excessive Exercisers. Eat. Disord. 2002, 10, 31–47. [Google Scholar] [CrossRef]
- Adkins, E.C.; Keel, P.K. Does “excessive” or “compulsive” best describe exercise as a symptom of bulimia nervosa? Int. J. Eat. Disord. 2005, 38, 24–29. [Google Scholar] [CrossRef]
- Danielsen, M.; Bjørnelv, S.; Bratberg, G.H.; Rø, Ø. Validation of the exercise and eating disorder questionnaire in males with and without eating disorders. Int. J. Eat. Disord. 2018, 51, 429–438. [Google Scholar] [CrossRef]
| (1) | (2) | (3) | (4) | (5) | (6) | (7) | M (Males) | SD (Males) | U | |
|---|---|---|---|---|---|---|---|---|---|---|
| (1) STAI-A 1 | 0.41 ** | 0.34 ** | 0.29 ** | 0.49 ** | 0.04 | 0.05 | 70.21 | 30.86 | 14,144 ** | |
| (2) SDRS 2 | 0.48 ** | 0.27 ** | 0.26 ** | 0.34 ** | −0.00 | 0.02 | 140.28 | 90.40 | 14,012 ** | |
| (3) ES-ERQ 3 | 0.36 ** | 0.21 ** | 0.11 | 0.20 ** | 0.02 | −0.09 | 130.84 | 50.46 | 19,785 | |
| (4) Total CET 4 | 0.30 ** | 0.21 ** | 0.18 * | 0.41 ** | 0.05 | 0.19 ** | 100.09 | 30.57 | 18,720 | |
| (5) Total EDI-3 5 | 0.51 ** | 0.35 ** | 0.33 ** | 0.52 ** | −0.00 | 0.33 ** | 150.31 | 120.88 | 15,641 | |
| (6) Age | 0.34 ** | 0.09 | 0.08 | 0.03 | 0.23 ** | 0.25 ** | 130.39 | 10.22 | 17,914 ** | |
| (7) BMI 6 | 0.11 | −0.01 | 0.10 | 0.33 ** | 0.51 ** | 0.24 ** | 200.61 | 30.28 | 19,298 | |
| M (females) | 90.60 | 190.23 | 140.07 | 90.67 | 210.43 | 130.64 | 200.52 | |||
| SD (females) | 40.76 | 90.59 | 50.41 | 30.58 | 160.74 | 10.29 | 30.66 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cuesta-Zamora, C.; González-Martí, I.; García-López, L.M.; Ros, L.; Plateau, C.R.; Ricarte, J.J. Emotion Dysregulation as a Mediator of the Relationship between Anxiety, Compulsive Exercise and Eating Disorder Symptoms in Adolescents. Children 2021, 8, 1088. https://doi.org/10.3390/children8121088
Cuesta-Zamora C, González-Martí I, García-López LM, Ros L, Plateau CR, Ricarte JJ. Emotion Dysregulation as a Mediator of the Relationship between Anxiety, Compulsive Exercise and Eating Disorder Symptoms in Adolescents. Children. 2021; 8(12):1088. https://doi.org/10.3390/children8121088
Chicago/Turabian StyleCuesta-Zamora, Cristina, Irene González-Martí, Luis Miguel García-López, Laura Ros, Carolyn R. Plateau, and Jorge Javier Ricarte. 2021. "Emotion Dysregulation as a Mediator of the Relationship between Anxiety, Compulsive Exercise and Eating Disorder Symptoms in Adolescents" Children 8, no. 12: 1088. https://doi.org/10.3390/children8121088
APA StyleCuesta-Zamora, C., González-Martí, I., García-López, L. M., Ros, L., Plateau, C. R., & Ricarte, J. J. (2021). Emotion Dysregulation as a Mediator of the Relationship between Anxiety, Compulsive Exercise and Eating Disorder Symptoms in Adolescents. Children, 8(12), 1088. https://doi.org/10.3390/children8121088







