Variability in the Method of Gastrostomy Placement in Children
Abstract
1. Introduction
2. Methods
2.1. Data Source
2.2. Study Population
2.3. Statistical Analysis
3. Results
3.1. Study Population
3.2. Characteristics by Gastrostomy Placement Method
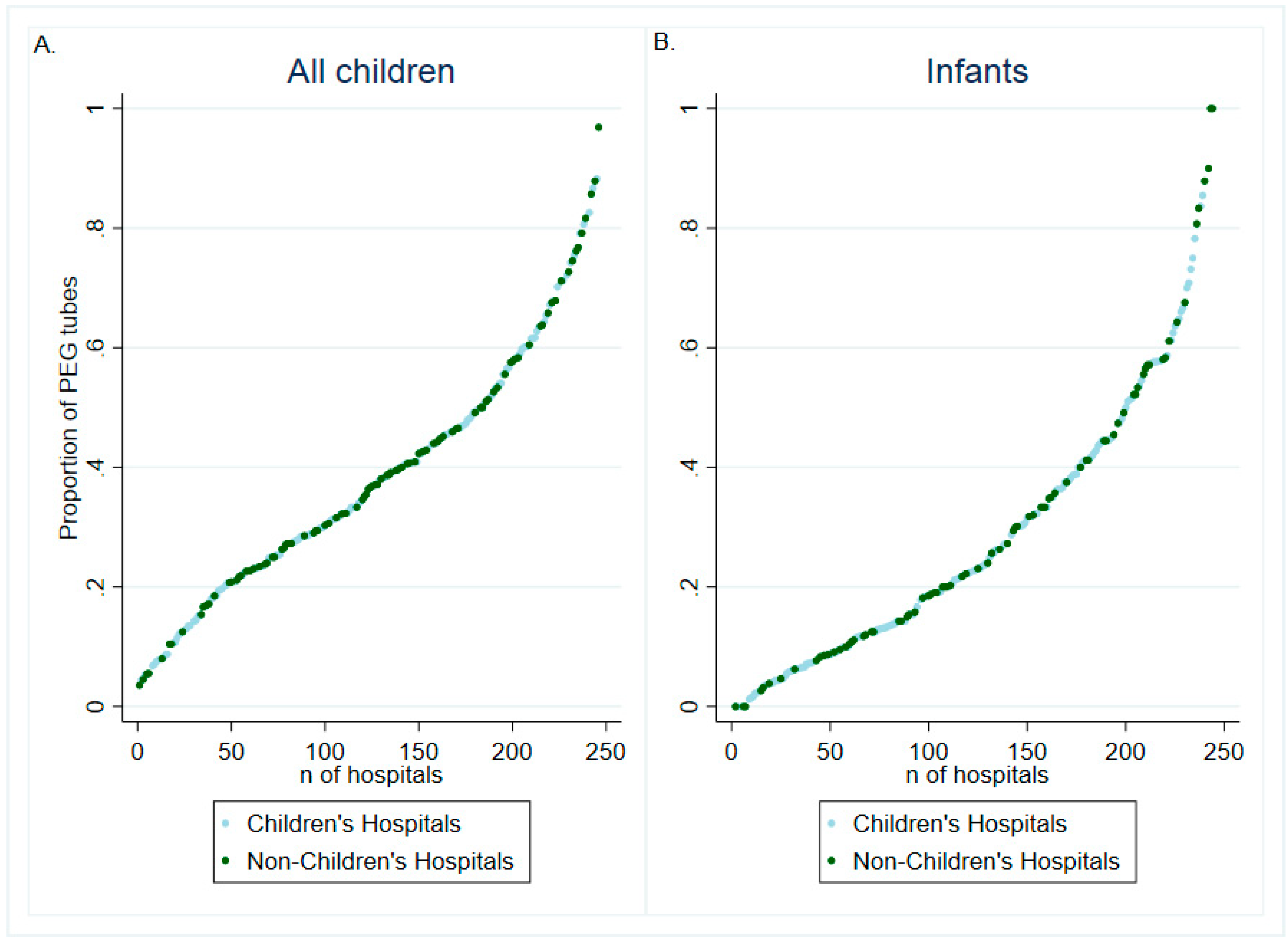
3.3. Center-Level Variability in Gastrostomy Placement
4. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Gauderer, M.W.; Ponsky, J.L.; Izant, R.J., Jr. Gastrostomy without laparotomy: A percutaneous endoscopic technique. J. Pediatr. Surg. 1980, 15, 872–875. [Google Scholar] [CrossRef]
- Sandberg, F.; Viktorsdottir, M.B.; Salo, M.; Stenstrom, P.; Arnbjornsson, E. Comparison of major complications in children after laparoscopy-assisted gastrostomy and percutaneous endoscopic gastrostomy placement: A meta-analysis. Pediatr. Surg. Int. 2018, 34, 1321–1327. [Google Scholar] [CrossRef] [PubMed]
- Baker, L.; Beres, A.L.; Baird, R. A systematic review and meta-analysis of gastrostomy insertion techniques in children. J. Pediatr. Surg. 2015, 50, 718–725. [Google Scholar] [CrossRef] [PubMed]
- Suksamanapun, N.; Mauritz, F.A.; Franken, J.; van der Zee, D.C.; van Herwaarden-Lindeboom, M.Y. Laparoscopic versus percutaneous endoscopic gastrostomy placement in children: Results of a systematic review and meta-analysis. J. Minim. Access. Surg. 2017, 13, 81–88. [Google Scholar] [CrossRef]
- Landisch, R.M.; Colwell, R.C.; Densmore, J.C. Infant gastrostomy outcomes: The cost of complications. J. Pediatr. Surg. 2016, 51, 1976–1982. [Google Scholar] [CrossRef]
- Petrosyan, M.; Khalafallah, A.M.; Franklin, A.L.; Doan, T.; Kane, T.D. Laparoscopic Gastrostomy Is Superior to Percutaneous Endoscopic Gastrostomy Tube Placement in Children Less Than 5 years of Age. J. Laparoendosc Adv. Surg. Tech. A 2016, 26, 570–573. [Google Scholar] [CrossRef]
- HCUP Databases. Available online: https://www.hcup-us.ahrq.gov/kidoverview.jsp (accessed on 31 March 2020).
- Haider, A.H.; Saleem, T.; Leow, J.J.; Villegas, C.V.; Kisat, M.; Schneider, E.B.; Haut, E.R.; Stevens, K.A.; Cornwell, E.E., 3rd; Mackenzie, E.J.; et al. Influence of the national trauma data bank on the study of trauma outcomes: Is it time to set research best practices to further enhance its impact? J. Am. Coll. Surg. 2012, 214, 756–768. [Google Scholar] [CrossRef]
- Brewster, B.D.; Weil, B.R.; Ladd, A.P. Prospective determination of percutaneous endoscopic gastrostomy complication rates in children: Still a safe procedure. Surgery 2012, 152, 714–719, discussion 719–721. [Google Scholar] [CrossRef]
- Miyata, S.; Dong, F.; Lebedevskiy, O.; Park, H.; Nguyen, N. Comparison of operative outcomes between surgical gastrostomy and percutaneous endoscopic gastrostomy in infants. J. Pediatr. Surg. 2017, 52, 1416–1420. [Google Scholar] [CrossRef]
- Merli, L.; De Marco, E.A.; Fedele, C.; Mason, E.J.; Taddei, A.; Paradiso, F.V.; Catania, V.D.; Nanni, L. Gastrostomy Placement in Children: Percutaneous Endoscopic Gastrostomy or Laparoscopic Gastrostomy? Surg. Laparosc. Endosc. Percutaneous Tech. 2016, 26, 381–384. [Google Scholar] [CrossRef]
- Zamakhshary, M.; Jamal, M.; Blair, G.K.; Murphy, J.J.; Webber, E.M.; Skarsgard, E.D. Laparoscopic vs percutaneous endoscopic gastrostomy tube insertion: A new pediatric gold standard? J. Pediatr. Surg. 2005, 40, 859–862. [Google Scholar] [CrossRef]
- Akay, B.; Capizzani, T.R.; Lee, A.M.; Drongowski, R.A.; Geiger, J.D.; Hirschl, R.B.; Mychaliska, G.B. Gastrostomy tube placement in infants and children: Is there a preferred technique? J. Pediatr. Surg. 2010, 45, 1147–1152. [Google Scholar] [CrossRef]
- Fascetti-Leon, F.; Gamba, P.; Dall’Oglio, L.; Pane, A.; de Angelis, G.L.; Bizzarri, B.; Fava, G.; Maestri, L.; Cheli, M.; Di Nardo, G.; et al. Complications of percutaneous endoscopic gastrostomy in children: Results of an Italian multicenter observational study. Dig. Liver Dis. 2012, 44, 655–659. [Google Scholar] [CrossRef] [PubMed]
- Vervloessem, D.; van Leersum, F.; Boer, D.; Hop, W.C.; Escher, J.C.; Madern, G.C.; de Ridder, L.; Bax, K.N. Percutaneous endoscopic gastrostomy (PEG) in children is not a minor procedure: Risk factors for major complications. Semin. Pediatr. Surg. 2009, 18, 93–97. [Google Scholar] [CrossRef] [PubMed]
- McSweeney, M.E.; Kerr, J.; Jiang, H.; Lightdale, J.R. Risk factors for complications in infants and children with percutaneous endoscopic gastrostomy tubes. J. Pediatr. 2015, 166, 1514–1519.e1. [Google Scholar] [CrossRef] [PubMed]
- Minar, P.; Garland, J.; Martinez, A.; Werlin, S. Safety of percutaneous endoscopic gastrostomy in medically complicated infants. J. Pediatr. Gastroenterol. Nutr. 2011, 53, 293–295. [Google Scholar] [CrossRef] [PubMed]
- Sutherland, C.; Carr, B.; Biddle, K.Z.; Jarboe, M.; Gadepalli, S.K. Pediatric gastrostomy tubes and techniques: Making safer and cleaner choices. J. Surg. Res. 2017, 220, 88–93. [Google Scholar] [CrossRef] [PubMed]
| SG (n = 42,980) | PEG (n = 24,831) | p-Value | |
|---|---|---|---|
| PATIENT DEMOGRAPHICS | |||
| Mean Age (± SD) (years) | 2.3 ±4.3 | 4.8 ±6.0 | <0.001 |
| Infants, n (%) | 25,679 (59.7) | 9620 (38.7) | <0.001 |
| 0–3 months | 9310 (63.3) | 2742 (49.7) | |
| 3–6 months | 2509 (17.0) | 1177 (21.3) | |
| 6–9 months | 1712 (11.6) | 873 (15.8) | |
| 9–12 months | 1189 (8.1) | 730 (13.2) | |
| Female Sex | 19,554 (45.5) | 11,126 (44.8) | 0.4 |
| Race/Ethnicity, n (%) | <0.001 | ||
| White | 18,479 (43.0) | 10,846 (43.7) | |
| Black | 5793 (13.5) | 3215 (12.9) | |
| Hispanic | 7919 (18.4) | 4112 (16.6) | |
| Other | 3832 (8.9) | 2355 (9.5) | |
| Unknown | 6957 (16.2) | 4304 (17.3) | |
| Insurance | <0.001 | ||
| Public | 23,654 (55.0) | 12,293 (49.5) | |
| Private | 16,684 (38.8) | 10,815 (43.6) | |
| Self-Pay | 503 (1.2) | 329 (1.3) | |
| Other/Unknown | 2140 (5.0) | 1394 (5.6) | |
| CENTER CHARACTERISTICS | |||
| Children’s Hospital | 24,362 (56.7) | 13,931 (56.1) | <0.001 |
| Urban Location | 30,766 (71.6) | 18,665 (75.2) | <0.001 |
| Teaching Hospital | 28,259 (65.7) | 17,230 (69.4) | <0.001 |
| Bed Size | <0.001 | ||
| Small | 4998 (11.6) | 3321 (13.4) | |
| Medium | 10,493 (24.4) | 5736 (23.1) | |
| Large | 25,097 (58.4) | 14,730 (59.3) | |
| Unknown | 2392 (5.6) | 1044 (4.2) | |
| Region | <0.001 | ||
| Northeast | 5786 (13.5) | 4443 (17.9) | |
| Midwest | 9019 (21.0) | 5963 (24.0) | |
| South | 16,775 (39.0) | 8120 (32.7) | |
| West | 11,400 (26.5) | 6305 (25.4) |
| OR * (95%CI) | p-Value | |
|---|---|---|
| Year (per 3 year increment) | 0.99 (0.98–1.00) | 0.1 |
| Infant | 0.30 (0.26–0.33) | <0.001 |
| Female Sex | 1.02 (0.97–1.08) | 0.6 |
| Race | ||
| White | Reference | |
| Black | 1.01 (0.91–1.11) | 0.9 |
| Hispanic | 1.01 (0.92–1.10) | 0.9 |
| Other | 1.06 (0.95–1.18) | 0.3 |
| Insurance | ||
| Public | Reference | |
| Private | 1.17 (1.09–1.25) | <0.001 |
| Self-Pay | 1.08 (0.80–1.47) | 0.6 |
| Other/Unknown | 1.14 (0.99–1.32) | 0.08 |
| Children’s Hospital | 0.57 (0.48–0.69) | <0.001 |
| Urban Location | 0.38 (0.18–0.82) | 0.01 |
| Teaching Hospital | 0.94 (0.76–1.17) | 0.6 |
| Bed Size | ||
| Small | Reference | |
| Medium | 0.92 (0.76–1.10) | 0.4 |
| Large | 0.88 (0.71–1.08) | 0.2 |
| Region | ||
| Northeast | Reference | |
| Midwest | 1.21 (0.85–1.73) | 0.3 |
| South | 0.88 (0.65–1.18) | 0.4 |
| West | 1.12 (0.82–1.55) | 0.5 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Salazar, J.H.; Spanbauer, C.; Sood, M.R.; Densmore, J.C.; Van Arendonk, K.J. Variability in the Method of Gastrostomy Placement in Children. Children 2020, 7, 53. https://doi.org/10.3390/children7060053
Salazar JH, Spanbauer C, Sood MR, Densmore JC, Van Arendonk KJ. Variability in the Method of Gastrostomy Placement in Children. Children. 2020; 7(6):53. https://doi.org/10.3390/children7060053
Chicago/Turabian StyleSalazar, Jose H., Charles Spanbauer, Manu R. Sood, John C. Densmore, and Kyle J. Van Arendonk. 2020. "Variability in the Method of Gastrostomy Placement in Children" Children 7, no. 6: 53. https://doi.org/10.3390/children7060053
APA StyleSalazar, J. H., Spanbauer, C., Sood, M. R., Densmore, J. C., & Van Arendonk, K. J. (2020). Variability in the Method of Gastrostomy Placement in Children. Children, 7(6), 53. https://doi.org/10.3390/children7060053






