Ultrastructural Changes of Blood Cells in Children with Generalized Purulent Peritonitis: A Cross-Sectional and Prospective Study
Abstract
1. Introduction
2. Materials and Methods
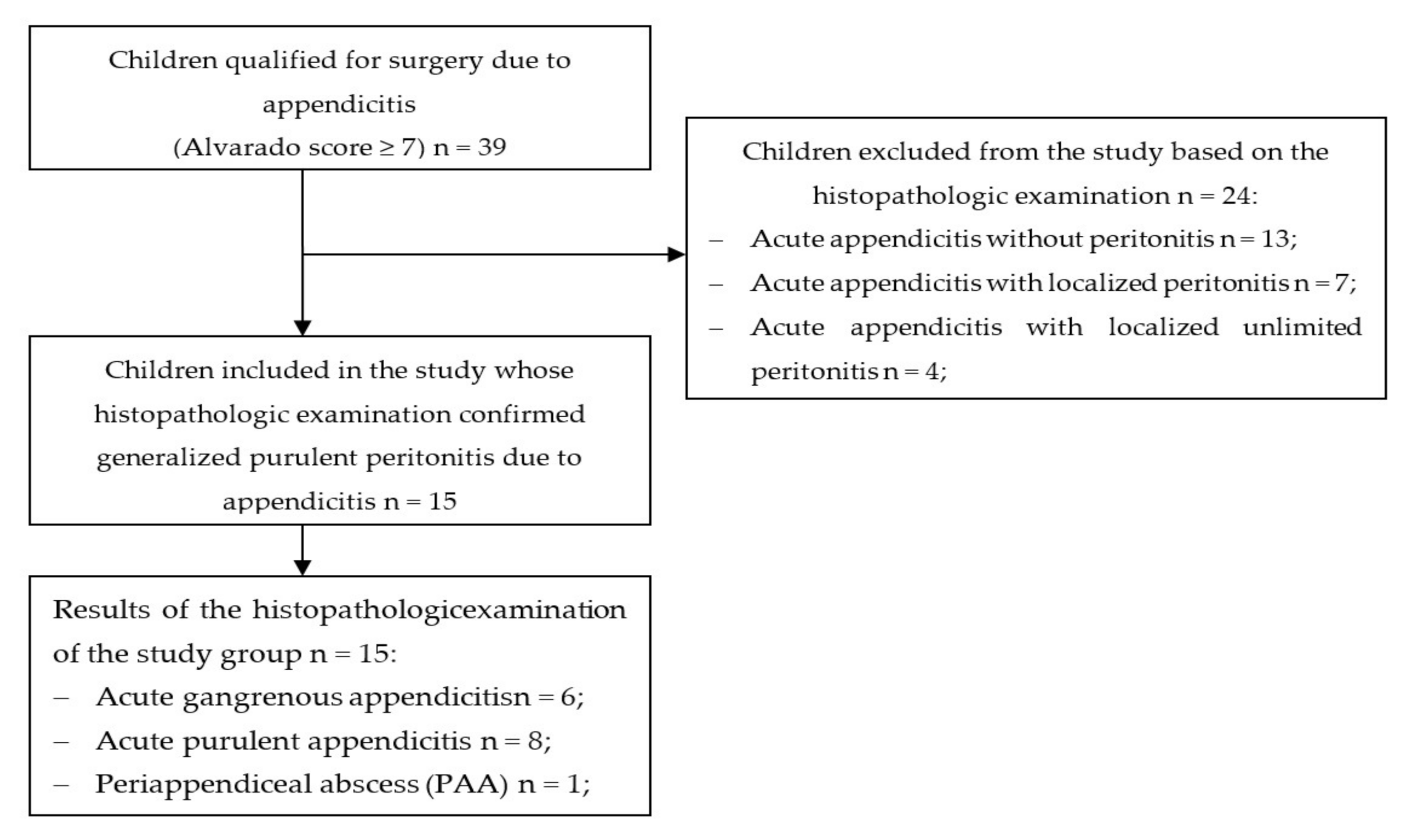
2.1. Study Desing and Population
2.2. Participants
2.3. Blood Sample
2.4. Other Data
2.5. Statistical Analysis
3. Results
3.1. Characteristics of Participants
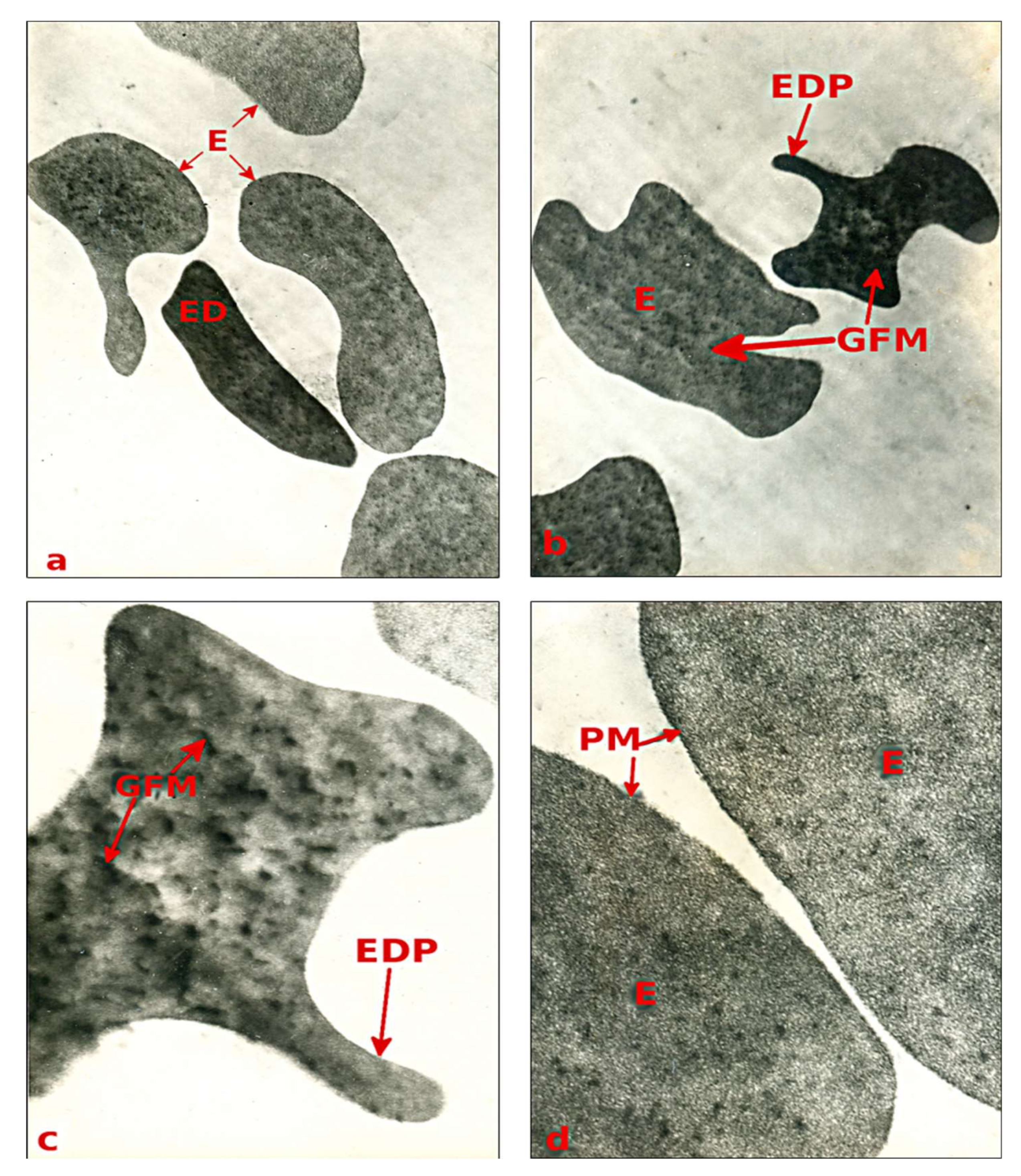
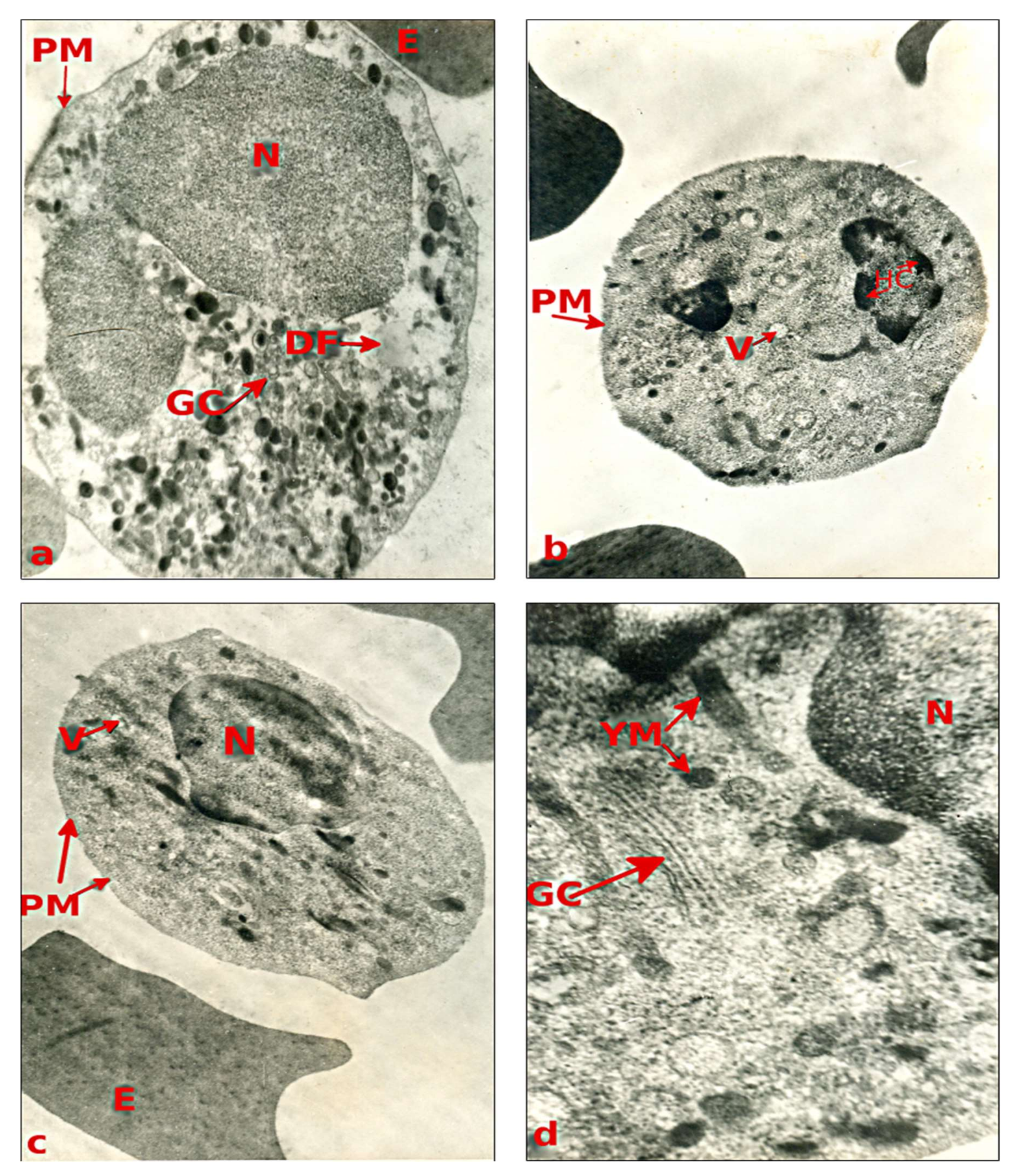
3.2. Results of the Electron Microscopy Analysis of Blood Sediment of the Examined Children in a State of Sepsis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- GlobalSurg. Collaborative Mortality of emergency abdominal surgery in high-, middle- and low-income countries. BJS 2016, 103, 971–988. [Google Scholar] [CrossRef] [PubMed]
- Bhangu, A.; Søreide, K.; Di Saverio, S.; Assarsson, J.H.; Drake, F.T. Acute appendicitis: Modern understanding of pathogenesis, diagnosis, and management. Lancet 2015, 386, 1278–1287. [Google Scholar] [CrossRef]
- Addiss, D.G.; Shaffer, N.; Fowler, B.S.; Tauxe, R.V. The epidemiology of appendicitis and appendectomy in the United States. Am. J. Epidemiol. 1990, 132, 910–925. [Google Scholar] [CrossRef] [PubMed]
- Omling, E.; Salö, M.; Saluja, S.; Bergbrant, S.; Olsson, L.; Persson, A.; Björk, J.; Hagander, L. Nationwide study of appendicitis in children. BJS 2019, 106, 1623–1631. [Google Scholar] [CrossRef]
- Lee, J.H.; Park, Y.S.; Choi, J.S. The Epidemiology of Appendicitis and Appendectomy in South Korea: National Registry Data. J. Epidemiol. 2010, 20, 97–105. [Google Scholar] [CrossRef]
- Ohene-Yeboah, M.; Abantanga, F.A. Incidence of acute appendicitis in Kumasi, Ghana. West Afr. J. Med. 2009, 28, 122–125. [Google Scholar]
- Lamps, L.W. Infectious Causes of Appendicitis. Infect. Dis. Clin. N. Am. 2010, 24, 995–1018. [Google Scholar] [CrossRef] [PubMed]
- Dzabic, M.; Boström, L.; Rahbar, A. High prevalence of an active cytomegalovirus infection in the appendix of immunocompetent patients with acute appendicitis. Inflamm. Bowel Dis. 2008, 14, 236–241. [Google Scholar] [CrossRef]
- Carr, N.J. The pathology of acute appendicitis. Ann. Diagn. Pathol. 2000, 4, 46–58. [Google Scholar] [CrossRef]
- Ergul, E. Heredity and familial tendency of acute appendicitis. Scand. J. Surg. 2007, 96, 290–292. [Google Scholar] [CrossRef]
- Wei, P.-L.; Chen, C.-S.; Keller, J.J.; Lin, H.-C. Monthly variation in acute appendicitis incidence: A 10-year nationwide population-based study. J. Surg. Res. 2012, 178, 670–676. [Google Scholar] [CrossRef] [PubMed]
- Zingone, F.; Sultan, A.A.; Humes, D.J.; West, J. Risk of Acute Appendicitis in and Around Pregnancy. Ann. Surg. 2015, 261, 332–337. [Google Scholar] [CrossRef] [PubMed]
- Saverio, D.; Birindelli, S.; Kelly, A.; Catena, M.; Weber, F.; Sartelli, D.G.; Sugrue, M.; de Moya, M.; Gomes, M.; Bhangu, C.A.; et al. WSES Jerusalem guidelines for diagnosis and treatment of acute appendicitis. World J. Emerg. Surg. 2016, 11, 34. [Google Scholar] [CrossRef] [PubMed]
- Bhangu, A. Evaluation of appendicitis risk prediction models in adults with suspected appendicitis. BJS 2019, 107, 73–86. [Google Scholar] [CrossRef] [PubMed]
- Hall, N.J.; Rahman, A.; Morini, F.; Prato, A.P.; Friedmacher, F.; Koivusalo, A.; Van Heurn, E.; Pierro, A.; Zani, A. European Paediatric Surgeons’ Association Survey on the Management of Pediatric Appendicitis. Eur. J. Pediatr. Surg. 2018, 29, 53–61. [Google Scholar] [CrossRef] [PubMed]
- Mureșan, M.G.; Balmoș, I.A.; Badea, I.; Santini, A. Abdominal Sepsis: An Update. J. Crit. Care Med. 2018, 4, 120–125. [Google Scholar] [CrossRef] [PubMed]
- Russo, A.; Falcone, M.; Gutiérrez-Gutiérrez, B.; Calbo, E.; Almirante, B.; Viale, P.; Oliver, A.; Ruiz-Garbajosa, P.; Gasch, O.; Gozalo, M.; et al. Predictors of outcome in patients with severe sepsis or septic shock due to extended-spectrum β-lactamase-producing Enterobacteriaceae. Int. J. Antimicrob. Agents 2018, 52, 577–585. [Google Scholar] [CrossRef]
- Singer, M.; Deutschman, C.S.; Seymour, C.W.; Shankar-Hari, M.; Annane, D.; Bauer, M.; Bellomo, R.; Bernard, G.R.; Chiche, J.-D.; Coopersmith, C.M.; et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016, 315, 801–810. [Google Scholar] [CrossRef]
- Cecconi, M.; De Backer, D.; Antonelli, M.; Baele, R.; Bakker, J.; Hofer, C.; Jaeschke, R.; Mebazza, A.; Pinsky, M.R.; Teboul, J.L.; et al. Consensus on circulatory shock and hemodynamic monitoring. Task Force of the European Society of Intensive Care Medicin. Intensive Care Med. 2014, 40, 1795–1815. [Google Scholar] [CrossRef]
- Brøchner, A.C.; Toft, P. Pathophysiology of the systemic inflammatory response after major accidental trauma. Scand. J. Trauma Resusc. Emerg. Med. 2009, 17, 43. [Google Scholar] [CrossRef]
- Sadaka, F.; O’Brien, J.; Prakash, S. Red Cell Distribution Width and Outcome in Patients with Septic Shock. J. Intensiv. Care Med. 2012, 28, 307–313. [Google Scholar] [CrossRef] [PubMed]
- Watkins, G.M.; Rabelo, A.; Plzak, L.F.; Sheldon, G.F. The Left Shifted Oxyhemoglobin Curve in Sepsis. Ann. Surg. 1974, 180, 213–220. [Google Scholar] [CrossRef] [PubMed]
- Reggiori, G.; Occhipinti, G.; De Gasperi, A.; Vincent, J.-L.; Piagnerelli, M. Early alterations of red blood cell rheology in critically ill patients*. Crit. Care Med. 2009, 37, 3041–3046. [Google Scholar] [CrossRef]
- Zhang, F.; Liu, A.-L.; Gao, S.; Ma, S.; Guo, S.-B. Neutrophil Dysfunction in Sepsis. Chin. Med. J. 2016, 129, 2741–2744. [Google Scholar] [CrossRef] [PubMed]
- Moroz, V.V.; Golubev, A.M.; Afanasyev, A.V.; Sergunova, V.A.; Gudkova, O.E.; Chernysh, A.M.; Kuzovlev, A. The Structure and Function of a Red Blood Cell in Health and Critical Conditions. Gen. Reanimatol. 2012, 8, 52. [Google Scholar] [CrossRef]
- Vincent, J.L.; Moreno, R.; Takala, J.; Willatts, S.; Mendonça, A.; Bruining, H.; Reinhart, C.K.; Suter, P.M.; Thijs, L.G. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med. 1996, 22, 707–710. [Google Scholar] [CrossRef]
- Ohle, R.; O’Reilly, F.; O’Brien, K.K.; Fahey, T.; Dimitrov, B.D. The Alvarado score for predicting acute appendicitis: A systematic review. BMC Med. 2011, 9, 139. [Google Scholar] [CrossRef]
- O’Connor, B.H. A Color Atlas and Instruction Manual of Peripheral Blood Cell Morphology; Lippincott Williams & Wilkins: Baltimore, MD, USA, 1984; Volume 316. [Google Scholar]
- Galankin, V.N.; Saprykin, V.P. Ultrastructural characterization of neutrophilic leukocytes in the blood of patients with sepsis. Patol. Fiziol. Eksp. Ter. 1996, 3, 13–18. [Google Scholar]
- Dupire, J.; Socol, M.; Viallat, A. Full dynamics of a red blood cell in shear flow. Proc. Natl. Acad. Sci. USA 2012, 109, 20808–20813. [Google Scholar] [CrossRef]
- De Oliveira, Y.P.A.; Pontes-De-Carvalho, L.C.; Couto, R.D.; Noronha-Dutra, A.A. Oxidative stress in sepsis. Possible production of free radicals through an erythrocyte-mediated positive feedback mechanism. Braz. J. Infect. Dis. 2017, 21, 19–26. [Google Scholar] [CrossRef] [PubMed]
- Piagnerelli, M.; Boudjeltia, K.Z.; Gulbis, B.; Vanhaeverbeek, M.; Vincent, J. Anemia in sepsis: The importance of red blood cell membrane changes. Transfus. Altern. Transfus. Med. 2007, 9, 143–149. [Google Scholar] [CrossRef]
- Yasui, K.; Ishiguro, S.; Komatsu, S.; Matsumura, T.; Komaya, K.; Saito, T.; Arikawa, T.; Kaneko, K.; Sano, T. Novel approach to intraoperative peritoneal lavage with an extracorporeal stirring method in laparoscopic surgery for generalized peritonitis: Preliminary results. Asian J. Endosc. Surg. 2019, 13, 89–94. [Google Scholar] [CrossRef]
- Yatsenko, O.V.; Yatsenko, V.P. Comparative analysis of characteristics of erythrocytes deformability in the Mother—Fetus system under gravity loading. Bullet. Prob. Biol. Med. 2014, 2, 215–219. [Google Scholar]
- Shylov, A.M.; Avshalumov, A.S.; Sinitsyna, E.N.; Markovsky, V.B.; Poleshchuk, O.I. Changes in the rheological properties of blood in patients with metabolic syndrome. Russ. Med. J. 2008, 16, 200–204. [Google Scholar]
- Kidalov, V.N.; Syasin, N.I.; Khadartsev, A.A. On the question concerning the physiological significance of changes of the form, ultrastructure and fluorescence of erythrocytes of peripheral blood during their transformation into echinocytes. J. Nucl. Med. Technol. 2005, 2, 6–10. [Google Scholar]
- Lang, K.S.; Lang, P.A.; Bauer, C.; Duranton, C.; Wieder, T.; Huber, S.M.; Lang, F. Mechanisms of Suicidal Erythrocyte Death. Cell. Physiol. Biochem. 2005, 15, 195–202. [Google Scholar] [CrossRef]
- Repsold, L.; Joubert, A.M. Eryptosis: An Erythrocyte’s Suicidal Type of Cell Death. BioMed Res. Int. 2018, 2018, 1–10. [Google Scholar] [CrossRef]
- Schultz, J.K.; Yaqub, S.; Wallon, C.; Blecic, L.; Forsmo, H.M.; Folkesson, J.; Buchwald, P.; Körner, H.; A Dahl, F.; Øresland, T. Laparoscopic Lavage vs Primary Resection for Acute Perforated Diverticulitis. JAMA 2015, 314, 1364–1375. [Google Scholar] [CrossRef]
| Variables | Study Group (n = 15) |
|---|---|
| Demographic data: | |
| Age [years] b | 9.07 ± 1.94 |
| Gender (male) a | 9 (60) |
| Disease duration [hours] b | 50.67 ± 18.6 |
| Blood count result: | |
| RBC [×1012/L] b | 3.69 ± 0.29 |
| HGB [g/dL] b | 12.73 ± 2.71 |
| HCT [%] b | 40 ± 0.5 |
| WBC [×109/L] b | 14.7 ± 2.86 |
| NLR c | 6.1, (4.7–8.85) |
| PLT [×109/L] c | 129, (90.5–140) |
| ESR [mm/h] b | 22.33 ± 5.37 |
| Biochemical parameters: | |
| Total bilirubin [mg/dL] c | 1.7, (1.4–3.55) |
| CRP [mg/L] b | 25.23 ± 11.34 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Halyuk, U.; Lychkovska, O.; Mota, O.; Kovalyshyn, V.; Kech, N.; Pokotylo, P.; Trutiak, O.; Zboina, B.; Nowicki, G.J.; Ślusarska, B. Ultrastructural Changes of Blood Cells in Children with Generalized Purulent Peritonitis: A Cross-Sectional and Prospective Study. Children 2020, 7, 189. https://doi.org/10.3390/children7100189
Halyuk U, Lychkovska O, Mota O, Kovalyshyn V, Kech N, Pokotylo P, Trutiak O, Zboina B, Nowicki GJ, Ślusarska B. Ultrastructural Changes of Blood Cells in Children with Generalized Purulent Peritonitis: A Cross-Sectional and Prospective Study. Children. 2020; 7(10):189. https://doi.org/10.3390/children7100189
Chicago/Turabian StyleHalyuk, Ulyana, Olena Lychkovska, Oksana Mota, Vasyl Kovalyshyn, Natalia Kech, Petro Pokotylo, Olena Trutiak, Bożena Zboina, Grzegorz Józef Nowicki, and Barbara Ślusarska. 2020. "Ultrastructural Changes of Blood Cells in Children with Generalized Purulent Peritonitis: A Cross-Sectional and Prospective Study" Children 7, no. 10: 189. https://doi.org/10.3390/children7100189
APA StyleHalyuk, U., Lychkovska, O., Mota, O., Kovalyshyn, V., Kech, N., Pokotylo, P., Trutiak, O., Zboina, B., Nowicki, G. J., & Ślusarska, B. (2020). Ultrastructural Changes of Blood Cells in Children with Generalized Purulent Peritonitis: A Cross-Sectional and Prospective Study. Children, 7(10), 189. https://doi.org/10.3390/children7100189










