Child Malnutrition in Pakistan: Evidence from Literature
Abstract
:1. Introduction
2. Aim and Objectives of the Review
- (i)
- to identify about the range of methodologies and methods to access the children malnutrition;
- (ii)
- to highlight the emerging themes to address the children malnutrition;
- (iii)
- to identify the geographical areas that are neglected in this research in Pakistan; and
- (iv)
- to provide recommendations for future work.
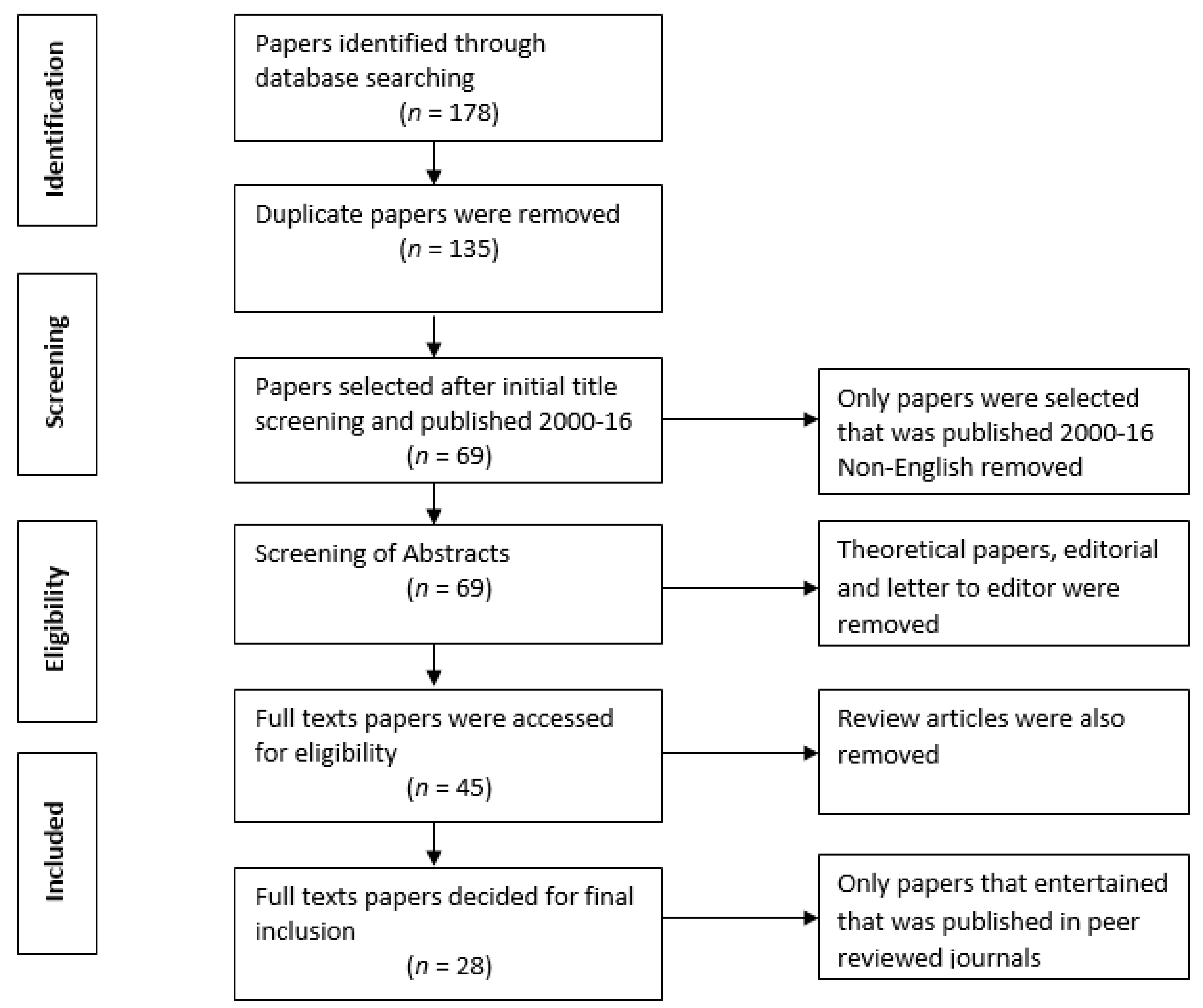
3. Methodology
Inclusion and Exclusion Criteria
4. Results
4.1. Methodological Findings
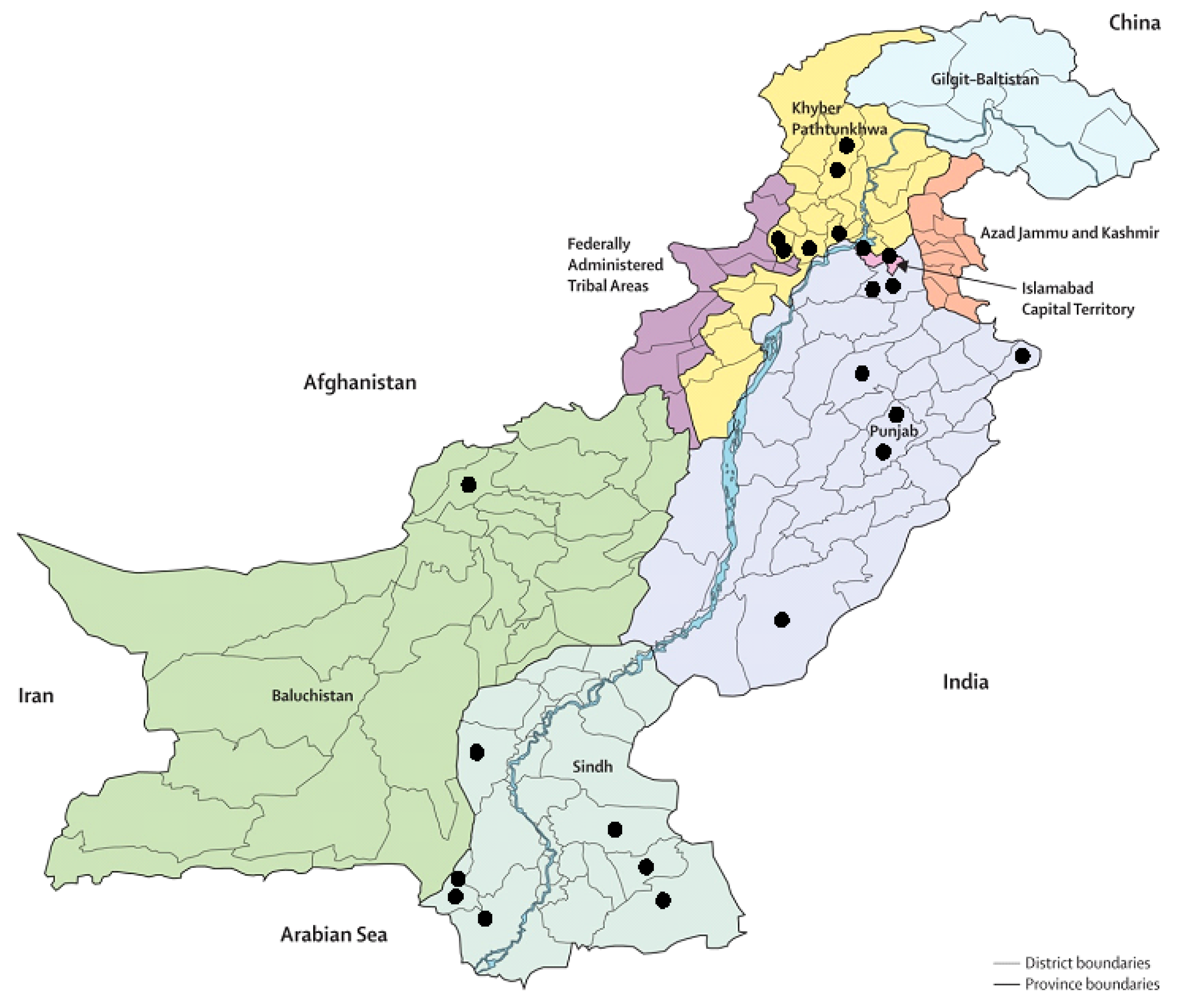
4.2. Coverage of Geographical Area
4.3. Child Age
4.4. Rural Urban Disparities
4.5. Gender
5. Discussion
5.1. Methodological Issues
5.2. Prevalence of Malnutrition among Children
5.3. Associated Factors with Malnutrition
5.4. Child Age
6. Conclusions
7. Strength and Limitation of Study
8. Recommendation for Future Studies
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Black, R.E.; Victora, C.G.; Walker, S.P.; Bhutta, Z.A.; Christian, P.; de Onis, M.; Ezzati, M.; Grantham-McGregor, S.; Katz, J.; Martorell, R.; et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 2013, 382, 427–451. [Google Scholar] [CrossRef]
- Meshram, I.I.; Arlappa, N.; Balakrishna, N.; Rao, K.M.; Laxmaiah, A.; Brahmam, G.N.V. Trends in the prevalence of undernutrition, nutrient and food intake and predictors of undernutrition among under five-year tribal children in India. Asia Pac. J. Clin. Nutr. 2012, 21, 568–576. [Google Scholar] [PubMed]
- Demissie, S.; Worku, A. Magnitude and factors associated with malnutrition in children 6–59 months of age in Pastoral community of Dollo Ado District, Somali Region, Ethiopia. Sci. J. Public Health 2013, 1, 175–183. [Google Scholar] [CrossRef]
- Müller, O.; Krawinkel, M. Malnutrition and health in developing countries. Can. Med. Assoc. J. 2005, 173, 279–286. [Google Scholar] [CrossRef] [PubMed]
- Bryce, J.; Boschi-Pinto, C.; Shibuya, K.; Black, R.E.; WHO Child Health Epidemiology Reference Group. WHO estimates of the causes of death in children. Lancet 2005, 365, 1147–1152. [Google Scholar] [CrossRef]
- World Health Organization. Children: Reducing Mortality. Available online: http://www.who.int/mediacentre/factsheets/fs178/en/ (accessed on 3 March 2018).
- Pelletier, D.L.; Olson, C.M.; Frongillo, E., Jr. Food insecurity, hunger, and under nutrition. In Present Knowledge in Nutrition, 8th ed.; Bowman, B.A., Russell, R.M., Eds.; ILSI Press: Washington, DC, USA, 2006; pp. 701–713. [Google Scholar]
- Asad, N.; Mushtaq, A. Malnutrition in Pakistani children, its causes, consequences and recommendations. J. Pak. Med. Assoc. 2012, 62, 311. [Google Scholar] [PubMed]
- Ali, S.S.; Karim, N.; Billoo, A.G.; Haider, S.S. Association of literacy of mothers with malnutrition among children under three years of age in rural area of district Malir, Karachi. J. Pak. Med. Assoc. 2005, 55, 550–553. [Google Scholar] [PubMed]
- Stevens, G.A.; Finucane, M.M.; Paciorek, C.J.; Flaxman, S.R.; White, R.A.; Donner, A.J.; Ezzati, M.; Nutrition Impact Model Study Group. Trends in mild, moderate, and severe stunting and underweight, and progress towards MDG 1 in 141 developing countries: A systematic analysis of population representative data. Lancet 2012, 380, 824–834. [Google Scholar] [CrossRef]
- United Nation International Children’s Emergency Fund (UNICEF). Levels and Trends in Child Malnutrition. 2014. Available online: http://www.unicef.org/media/files/Levels_and_Trends_in_Child_Mortality_2014.pdf (accessed on 25 November 2015).
- Di Cesare, M.; Bhatti, Z.; Soofi, S.B.; Fortunato, L.; Ezzati, M.; Bhutta, Z.A. Geographical and socioeconomic inequalities in women and children’s nutritional status in Pakistan in 2011: An analysis of data from a nationally representative survey. Lancet Glob. Health 2015, 3, e229–e239. [Google Scholar] [CrossRef]
- Planning Commission, Government of Pakistan, Pakistan Institute of Development Economics. National Nutrition Survey; Planning Commission, Government of Pakistan, Pakistan Institute of Development Economics: Islamabad, Pakistan, 2011.
- Masibo, P.K.; Makoka, D. Trends and determinants of undernutrition among young Kenyan children: Kenya Demographic and Health Survey; 1993, 1998, 2003 and 2008–2009. Public Health Nutr. 2012, 15, 1715–1727. [Google Scholar] [CrossRef] [PubMed]
- Pasricha, S.R.; Biggs, B.A. Undernutrition among children in South and South-East Asia. J. Paediatr. Child Health 2010, 46, 497–503. [Google Scholar] [CrossRef] [PubMed]
- Jesmin, A.; Yamamoto, S.S.; Malik, A.A.; Haque, A. Prevalence and determinants of chronic malnutrition among preschool children: A cross-sectional study in Dhaka City, Bangladesh. J. Health Popul. Nutr. 2011, 29, 494–499. [Google Scholar] [CrossRef] [PubMed]
- Lozano, R.; Naghavi, M.; Foreman, K.; Lim, K.; Shibuya, K.; Aboyans, V.; Abraham, J.; Adair, T.; Aggarwal, R.; Ahn, S.Y.; et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012, 380, 2095–2128. [Google Scholar] [CrossRef]
- Guerrant, R.L.; DeBoer, M.D.; Moore, S.R.; Scharf, R.J.; Lima, A.A.M. The impoverished gut—A triple burden of diarrhoea, stunting and chronic disease. Nat. Rev. Gastroenterol. Hepatol. 2013, 10, 220. [Google Scholar] [CrossRef] [PubMed]
- Wolf, J.; Prüss-Ustün, A.; Cumming, O.; Bartram, J.; Bonjour, S.; Cairncross, S.; Clasen, T.; Colford, J.M., Jr.; Curtis, V.; de France, J.; et al. Assessing the impact of drinking water and sanitation on diarrhoeal disease in low- and middle-income settings: Systematic review and meta-regression. Trop. Med. Int. Health. 2014, 19, 928–942. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Engell, R.E.; Lim, S.S. Does clean water matter? An updated analysis of water supply and sanitation interventions and diarrhoeal diseases. Lancet 2013, 381, 544. [Google Scholar] [CrossRef]
- Bhutta, Z.A.; Hafeez, A.; Rizvi, A.; Ali, N.; Khan, A.; Ahmad, F.; Bhutta, S.; Hazir, T.; Zaidi, A.; Jafarey, S.N. Reproductive, maternal, newborn, and child health in Pakistan: Challenges and opportunities. Lancet 2013, 381, 2207–2218. [Google Scholar] [CrossRef]
- Bhutta, Z.A.; Gazdar, H.; Haddad, L. Seeing the unseen: Breaking the logjam of undernutrition in Pakistan. IDS Bull. 2013, 44, 1–9. [Google Scholar] [CrossRef] [Green Version]
- Bhutta, Z.A.; Gupta, I.; de’Silva, H.; Manandhar, D.; Awasthi, S.; Hossain, S.M.M. Maternal and child health: Is South Asia ready for change? BMJ 2004, 328, 816–819. [Google Scholar] [CrossRef] [PubMed]
- Shetty, P. Malnutrition and undernutrition. Medicine 2006, 34, 524–529. [Google Scholar] [CrossRef]
- De Onis, M.; Onyango, A.W.; Borghi, E.; Garza, C.; Yang, H.; WHO Multicentre Growth Reference Study Group. Comparison of the World Health Organization (WHO) Child Growth Standards and the National Center for Health Statistics/WHO international growth reference: Implications for child health programmes. Public Health Nutr. 2006, 9, 942–947. [Google Scholar] [CrossRef] [PubMed]
- Wong, L.P. Summarizing research findings: Systematic review and meta-analysis. Malaysian family physician. Off. J. Acad. Fam. Physicians Malays. 2007, 2, 8. [Google Scholar]
- Beaton, G.H.; Martorell, R.; Aronson, K.A.; Edmonston, B.; Ross, G.M.A.C.; Harvey, B. Micronutrient deficiencies Vitamin A supplementation and child morbidity and mortality in developing countries (introductory text). Food Nutr. Bull. 1993, 15, 1994. [Google Scholar]
- Save the Children. Nutrition in the First 1000 Days: State of the World’s Mothers 2012; Save the Children: London, UK, 2012. [Google Scholar]
- United Nation International Children’s Emergency Fund (UNICEF). Improving Child Nutrition. The Achievable Imperative for Global Progress; United Nations Children’s Fund Google Scholar: New York, NY, USA, 2013. [Google Scholar]
- Ali, W.; Ayub, A.; Hussain, H. Prevalence and associated risk factors of under nutrition among children aged 6 to 59 months in internally displaced persons of jalozai camp, District Nowshera, Khyber Pakhtunkhwa. J. Ayub Med. Coll. Abbottabad 2015, 27, 556–559. [Google Scholar] [PubMed]
- Afridi, M.F.; Khushdil, A.; Riaz, S.; Ehsan, A. Nutritional status of pre-school children–A cross-sectional study in Mingora, Swat. J. Postgrad. Med. Inst. 2014, 28, 314–328. [Google Scholar]
- Achakzai, P.; Khan, R. Nutritional status and associated factors among children less than five years of age in tehsil Zarghoon town, District Quetta, Baluchistan. J. Ayub Med. Coll. Abbottabad 2016, 28, 146–151. [Google Scholar] [PubMed]
- Baig-Ansari, N.; Rahbar, M.H.; Bhutta, Z.A.; Badruddin, S.H. Child’s gender and household food insecurity are associated with stunting among young Pakistani children residing in urban squatter settlements. Food Nutr. Bull. 2006, 27, 114–127. [Google Scholar] [CrossRef] [PubMed]
- Batool, S.; Shaheen, A.; Rehman, R. To Assess the Nutritional Status of Primary School Children in an Urban School of Faisalabad. Pak. J. Med. Health Sci. A 2012, 4, 160. [Google Scholar]
- Nisar, Y.B.; Aurangzeb, B.; Hazir, T. Nutritional Status of Hospitalized Children with Nutritional Anaemia: A Cross Sectional Study. Ann. Pak. Inst. Med. Sci. 2013, 9, 122–125. [Google Scholar]
- Shah, S.M.; Selwyn, B.J.; Luby, S.; Merchant, A.; Bano, R. Prevalence and correlates of stunting among children in rural Pakistan. Pediatr. Int. 2003, 45, 49–53. [Google Scholar] [CrossRef] [PubMed]
- Laghari, Z.A.; Soomro, A.M.; Tunio, S.A.; Lashari, K.; Baloach, F.G.; Baig, N.M.; Bano, S. Malnutrition among children under five years in district Sanghar, Sindh, Pakistan. Gomal J. Med. Sci. 2015, 13, 314–318. [Google Scholar]
- Gul, R.; Kibria, Z. Prevalence and predeterminants of malnutrition in children under 3 years of age in the two rural communities of Peshawar. Khyber Med. Univ. J. 2013, 5, 190–194. [Google Scholar]
- District Government Tharparkar. Analysis of Nutritional Data Community-Based Management of Acute Malnutrition Project; District Government Tharparkar: Sindh, Pakistan, 2014.
- Nuruddin, R.; Lim, M.K.; Hadden, W.C.; Azam, I. Comparison of estimates of under-nutrition for pre-school rural Pakistani children based on the WHO standard and the National Center for Health Statistics (NCHS) reference. Public Health Nutr. 2009, 12, 716–722. [Google Scholar] [CrossRef] [PubMed]
- Mushtaq, M.U.; Gull, S.; Khurshid, U.; Shahid, U.; Shad, M.A.; Siddiqui, A.M. Prevalence and socio-demographic correlates of stunting and thinness among Pakistani primary school children. BMC Public Health 2011, 11, 790. [Google Scholar] [CrossRef] [PubMed]
- Anwer, I.; Awan, J.A. Nutritional status comparison of rural with urban school children in Faisalabad District, Pakistan. Rural Remote Health 2003, 3, 130. [Google Scholar] [PubMed]
- Khattak, K.M.M.; Shah, J.S. Malnutrition and associated risk factors in pre-school children (2–5 years) in district Swabi (NWFP)-Pakistan. J. Med. Sci. 2010, 10, 34–39. [Google Scholar]
- Khan, G.N.; Turab, A.; Khan, M.I.; Rizvi, A.; Shaheen, F.; Ullah, A.; Hussain, A.; Hussain, I.; Ahmed, I.; Yaqoob, M.; et al. Prevalence and associated factors of malnutrition among children under-five years in Sindh, Pakistan: A cross-sectional study. BMC Nutr. 2016, 2, 69. [Google Scholar] [CrossRef]
- Khuwaja, S.; Selwyn, B.J.; Shah, S.M. Prevalence and correlates of stunting among primary school children in rural areas of southern Pakistan. J. Trop. Pediatr. 2005, 51, 72–77. [Google Scholar] [CrossRef] [PubMed]
- Fryar, C.D.; Ogden, C.L. Prevalence of Underweight among Children and Adolescents Aged 2–19 Years: United States, 1963–1965 through 2011–2012; National Center for Health Statistics Health: Hyattsville, MD, USA, 2014. [Google Scholar]
- Hamad, N.; Sarwar, Z.; Ranjha, M.K.; Ahmad, I. Food utilization as anti-stunting intervention in Pakistan. Med. Channel 2016, 22, 80–87. [Google Scholar]
- National Institute of Population Studies. Pakistan Demographic and Health Survey 2012–2013; National Institute of Population Studies and ICF International: Islamabad, Pakistan; Calverton, MA, USA, 2013. [Google Scholar]
- Mahmood, S.; Nadeem, S.; Saif, T.; Mannan, M.; Arshad, U. Nutritional status and associated factors in under-five children of Rawalpindi. J. Ayub Med. Coll. Abbottabad 2016, 28, 67–71. [Google Scholar] [PubMed]
- SMART Survey Report, District Umarkot, Sindh, Pakistan. Available online: http://reliefweb.int/report/pakistan/smart-survey-report-taluka-district-umerkot-sindh-pakistan-january-2016 (accessed on 31 January 2016).
- Zainab, S.; Kadir, M. Nutritional status and physical abuse among the children involved in domestic labour in Karachi Pakistan: A cross-sectional survey. JPMA J. Pak. Med. Assoc. 2016, 66, 1243. [Google Scholar] [PubMed]
- Khan, T.; Khan, R.E.; Raza, M.A. Gender Analysis of Malnutrition: A Case Study of School-Going Children in Bahawalpur. Asian Dev. Policy Rev. 2015, 3, 29–48. [Google Scholar] [CrossRef]
- Ullah, H.; Ullah, B.; Karim, S.; Tariq, I.; Khan, A.K.; Mir, S.; Baseer, A.; Azhar, S.; Murtaza, G. Malnutrition amongst Under-Five Years Children in Swat, Pakistan: Prevalence and Risk Factors. Trop. J. Pharm. Res. 2014, 13, 1367–1370. [Google Scholar] [CrossRef]
- Rehman, Z.; Ishtiaq, M.; Naeem, M.; Gul, R.; Amjad, M.; Iftikhar, B. Prevalence of Malnutrition among School Going Children of University Campus Peshawar; Sadiu Medical College: Swat, Pakistan, 2013; Available online: http://www.smcswat.edu.pk/Vol-4-No-1/Dr%20Zai%20ur%20rehman.doc (accessed on 25 December 2017).
- Mushtaq, M.U.; Gull, S.; Mushtaq, K.; Abdullah, H.M.; Khurshid, U.; Shahid, U.; Shad, M.A.; Akram, J. Height, weight and BMI percentiles and nutritional status relative to the international growth references among Pakistani school-aged children. BMC Pediatr. 2012, 12, 31. [Google Scholar] [CrossRef] [PubMed]
- Farid-ul-Hasnain, S.; Sophie, R. Prevalence and risk factors for stunting among children under 5 years: A community-based study from Jhangara town, Dadu Sindh. JPMA J. Pak. Med. Assoc. 2010, 60, 41–44. [Google Scholar] [PubMed]
- Riaz, R.; Sultana, A.; Hameed, S.; Tehseen, I.; Sabir, S.A. Nutritional Status of School Going Children. J. Rawalpindi Med. Coll. 2010, 14, 51–54. [Google Scholar]
- Anwar, H.N.; Zafar, M.I.; Hussain, S. Health screening of primary school children—A case study of district Sargodha-Pakistan. Pak. J. Life Soc. Sci. 2006, 4, 40–47. [Google Scholar]
- Mian, R.M.; Ali, M.; Ferroni, P.A.; Underwood, P. The nutritional status of school-aged children in an urban squatter settlement in Pakistan. Pak. J. Nutr. 2002, 1, 121–123. [Google Scholar]
- Kroeger, A. Health interview Survey in developing countries: A review of methods and results. Int. J. Epidemiol. 1983, 12, 456–481. [Google Scholar] [CrossRef]
- Joseph, B.; Rebello, A.; Kullu, P.; Raj, V.D. Prevalence of malnutrition in rural Karnataka, South India: A comparison of anthropometric indicators. J. Health Popul. Nutr. 2002, 20, 239–244. [Google Scholar] [PubMed]
- World Health Organization. WHO Child Growth Standards: Length/Height-for-Age, Weight-for-Age, Weight for-Length, Weight-for-Height and Body Mass Index-Forage: Methods and Development; WHO: Geneva, Switzerland, 2006. [Google Scholar]
- De Onis, M. WHO Child Growth Standards: Length/Height-Forage, Weight-for-Age, Weight-for-Length, Weight-for-Height and Body Mass Index-for-Age; WHO: Geneva, Switzerland, 2006. [Google Scholar]
- Ratnu, A.N. Prevalence of Under Nutrition in 0–5 Year Children of Junagadh District, Gujarat; Achutha Menon Centre for Health Science Studies, Shree Chitra Tirunal Institute for Medical Sciences and Technology: Trivandrum, India, 2013; Volume 5. [Google Scholar]
- De Onis, M.; Garza, C.; Victora, C.G.; Onyango, A.W.; Frongillo, E.A.; Martines, J. The WHO Multicentre Growth Reference Study: Planning, study design, and methodology. Food Nutr. Bull. 2004, 25, S15–S26. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, T.; Hossain, M.; Mahfuz, M.; Choudhury, N.; Hossain, M.M.; Bhandari, N.; Lin, M.M.; Joshi, P.C.; Angdembe, M.R.; Wickramasinghe, V.P.; et al. Severe acute malnutrition in Asia. Food Nutr. Bull. 2014, 35, S14–S26. [Google Scholar] [CrossRef] [PubMed]
- Akram, D.S.; Bharmal, F.Y.; Hussain, T. PediaSure in the treatment of severe malnutrition in Pakistani children. J. Pak. Med. Assoc. 2000, 50, 377–380. [Google Scholar] [PubMed]
- Bhutta, Z.A. Addressing severe acute malnutrition where it matters. Lancet 2009, 374, 94–96. [Google Scholar] [CrossRef]
- Dairo, M.D.; Fatokun, M.E.; Kuti, M. Reliability of the Mid Upper Arm Circumference for the Assessment of Wasting among Children Aged 12–59 Months in Urban Ibadan, Nigeria. Int. J. Biomed. Sci. 2012, 8, 140–143. [Google Scholar] [PubMed]
- Martorell, R.; Ho, T.J. Malnutrition, morbidity, and mortality. Pop. Dev. Rev. 1984, 10, 49–68. [Google Scholar] [CrossRef]
- Svedberg, P. Poverty and Undernutrition: Theory, Measurement, and Policy; Oxford University Press for WIDER: Oxford, UK, 2000. [Google Scholar]
| Study | Type | Participant | Sample Size | Target Population | Malnutrition Assessment | Study Design | Rural/Urban | Human Development * | Geographical Area: Province (Village/Town/City) |
|---|---|---|---|---|---|---|---|---|---|
| Achakzai and Khan [32] (2016) | Community based | Children and mothers | 104 | Under five years | NCHS/WHO Z score | Cross-sectional | Rural | LHD | Baluchistan, Quetta |
| Hamad et al. [47] (2016) | Hospital based | Pregnant mothers | 200 | Not mention | NCHS/WHO Z score | Cross-sectional | Not mention | Not applicable | Pakistan, four provinces |
| Khan et al. [44] (2016) | Community based | Mothers and children | 3964 | Less than five years | NCHS/WHO Z score | Cross-sectional | Rural | LHD | Sindh, Thatta |
| Mahmood et al. [49] (2016) | Hospital based | Guardian | 100 | Under five years | NCHS/WHO Z score | Cross-sectional | Urban | MHD | Punjab, Rawalpindi |
| SMART, [50] (2016) | Community based | Mother-child | 415 | 6–59 Months | MUAC | Cross-sectional | Rural | LHD | Sindh, Umerkot |
| Zanib and Qadir [51] (2016) | Community based | Children | 385 | 10–14 years | BMI | Cross-sectional | Rural | MHD | Sindh, Karachi |
| Ali et al. [30] (2015) | Community based | Children and Parents | 446 | Child age 6–59 months | NCHS/WHO Z score | Cross-sectional Structured Questionnaire | Rural | LHD | KPK, Nowshera, Jalozai Camp |
| Khan et al. [52] (2015) | Schools | Children | 684 | 5–14 Years | NCHS/WHO Z score | Cross-sectional | Rural | LHD | Punjab, Bahwalpur |
| Laghari et al. [37] (2015) | Community based | Children | 511 | 6–59 Months | MUAC | Cross-sectional | Rural | LHD | Sindh, Sanghar |
| Afridi et al. [31] (2014) | Community based | Children | 550 | 2–5 years | NCHS/WHO Z score | Cross-sectional | Rural | LHD | KPK, Swat, Mangora |
| Anonymous [39] (2014) | Community bases | Mother-Child | 50,247 | Under five | MUAC | Cross-sectional | Rural | VLHD | Sindh, Tharparkar |
| Ullah et al. [53] (2014) | Hospital based | Children | 186 | Under five children | Gomez’s Classification | Cross-sectional | Rural | LHD | KPK, Swat |
| Gul and Kibria [38] (2013) | Community based | Children and mothers | 200 | Less than three years | Weight for age using Harvard standard | Cross-sectional | Rural | MHD | KPK, Peshwar—two rural communities |
| Nisar et al. [35] (2013) | Hospital based | Children | 116 | 6 months to 12 years | NCHS/WHO Z score and Hemoglobin level | Cross-sectional | Urban | VHHD | Islamabad |
| Rehman et al. [54] (2013) | Primary Schools | Children | 400 | 4–12 years | BMI | Cross sectional | Urban | MHD | KPK, Peshawar |
| Batool et al. [34] (2012) | Primary schools | Children | 432 | 4–12 years | Jelliffe | Cross-sectional | Rural | MHD | Punjab, Faisalabad |
| Mushtaq et al. [55] (2012) | Schools | Children | 1860 | 5–12 | NCHS/WHO Z score | Cross-sectional | Urban | HHD | Punjab, Lahore |
| Mushtaq et al. [41] (2011) | Primary schools | Children | 1860 | 5–12 years | BMI | Cross-sectional | Urban | MHD | Punjab, Lahore |
| Hasnain et al. [56] (2010) | Community based | Mother and child | 800 | Less than five years | NCHS/WHO Z score | Cross-sectional | Rural | LHD | Sindh, Dadu |
| Khattak and Ali [43] (2010) | Community based | Children | 140 | Child age 2–5 years | NCHS/WHO Z score | Cross-sectional Structured Interview | Rural | VLHD | KPK, Swabi |
| Riaz et al. [57] (2010) | Primary schools | Children | 344 | 5–10 years | BMI | Cross-sectional comparative study | Urban | MHD | Punjab, Rawalpindi |
| Nuruddin et al. [40] (2008) | Secondary data | Children and mothers | 1533 | Less than 35 months | NCHS/WHO Z score | Secondary data analysis | Rural | LHD | Thatta, Sindh |
| Ansari et al. [33] (2006) | Community based | Mothers | 420 | 6–18 Months | NCHS/WHO Z score | Cross-sectional | Urban | MHD | Sindh, Karachi |
| Anwar et al. [58] (2006) | Primary schools | Children | 1185 | 5–14 years | Weight and height using Jelliffe’s classification | Cross-sectional | Punjab, Sargodha | MHD | Punjab, Rural 5 villages |
| Khuwaja et al. [45] (2005) | Primary schools | Children | 1915 | 6–12 years | NCHS/WHO Z score | Cross-sectional | Rural | LHD | Sindh, Rural 4 Villages |
| Anwar and Awan [42] (2003) | Schools | Children | 2042 | 6–12 Years | NCHS/WHO Z score | Cross-sectional | Urban | MHD | Punjab, Faisalabad |
| Shah et al. [36] (2003) | Community based | Children and mothers | 1878 | Less than three years | NCHS/WHO Z score | Cross-sectional | Rural | LHD | Four rural districts, Sindh |
| Mian et al. [59] (2002) | Community based | Mothers and caretakers | 200 | 5–10 years | NCHS/WHO Z score | Cross-sectional Quantitative and Qualitative | Urban | VHHD | Islamabad |
| Study and Years | Associated Factors with Child Malnutrion |
|---|---|
| Achakzai and Khan [32] (2016) | Stunting and wasting in children were 48% and 10% respectively. Socio-demographic characteristics, maternal health, and child health indicators were significantly associated with stunting and wasting. |
| Hamad et al. [47] (2016) | There was a greater ratio of undernutrition in boys as compared to girls. |
| Khan et al. [44] (2016) | The prevalence of underweight, stunting, and wasting was 39%, 48%, and 16% respectively. Boys were found to be more stunned compare to girls. Children in the poorest households were two times more like to be stunted and wasted compared to wealthier households. Diarrhoea was associated with underweight. |
| Mahmood et al. [49] (2016) | 32% of children were malnourished. Study indicated malnutrition to be significantly associated with maternal illiteracy and presence of disabled family members in home. |
| SMART, [50] (2016) | 30% of children belonging to rural areas were malnourished compared to 19% in urban areas. Half of the children were stunned. Children belong to 6–17 month’s age were more stunned and wasted as compare to higher age group. |
| Zanib and Qadir [51] (2016) | Physical abuse among the domestic child labour was the major factor of malnutrition. |
| Ali et al. [30] (2015) | 9% of children were stunted, 11% were underweight, and 4% were wasted. Illiteracy, large family size, late and early weaning, lack of exclusive breast feeding, and poverty were the factors associated with malnutrition. |
| Khan et al. [52] (2015) | The childrenin nuclearfamilies have higher risk to be wasted and stunned. Mother’s education was found strong predicator of reducing the malnutrition burden in children. |
| Laghari et al. [37] (2015) | 66% children were affected by malnutrition. Severe malnutrition was significantly higher in female children. Malnutrition was significantly higher in youngerchildren 6–23 months than in older children 24–59 months. |
| Afridi et al. [31] (2014) | 14% were underweight; 8% of the children were wasted; while 8% were stunted. |
| Anonymous [39] (2014) | Girls were found to be more malnourishedcompared to boys and children in the younger age group were also severely malnourished as compare to older age group. |
| Ullah et al. [53] (2014) | 38% male and 32% female children were malnourished. Risk factors for child malnutrition were lack of education, lack of immunization, teenage pregnancy, and large family size. |
| Gul and Kibria [38] (2013) | 61% males and 40% females were found malnourished. 71% children less than two years were malnourished. Large family size, poor socioeconomic status, mother’s illiteracy, younger mothers, maternal anemia and multipleparities were the major causes of child malnutrition. |
| Nisar et al. [35] (2013) | Children admitted with nutritional anemia in children hospital, Islamabad were belonged to the less than two years of age and had very poor nutritional status. |
| Rehman et al. [54] (2013) | 30% children were undernourished. It was found that 18% children were slightly, 10% were moderately and 2% were severely underweight. |
| Batool et al. [34] (2012) | Stunting and underweightwas more common in boys as compared to the girls. Low socioeconomic status, large family size, low literacy ratewas associated with poor health and nutrition in children. |
| Mushtaq et al. [55] (2012) | Poverty, lower education, low income, and overcrowded houses were the associated factors of children malnutrition. |
| Mushtaq et al. [41] (2011) | 8% children were stunted and 10% children were wasted. Wasting and stunting were not significantly associated with gender. |
| Hasnain et al. [56] (2010) | 61% children were stunned. Stunting was associated with ethnicity and birth interval less than two years. |
| Khattak and Ali [43] (2010) | 50% of pre-school children were facing malnutrition. Strong association of child malnutriton was found with family size, household income, and number of children in family |
| Riaz et al. [57] (2010) | 24% and 11% children were found to be underweight and stunted respectively. Stunted growth was found in 13% males and 8% female children. |
| Nuruddin et al. [40] (2008) | Prevalence of wasting, stunting, and underweight were higher in less than two year of children. |
| Ansari et al. [33] (2006) | Female children were three times more likely to be stunted than male. Food insecurity, lack of child feeding knowledge, and child health care practices were the major causes of child malnutrition. |
| Anwar et al. [58] (2006) | 46% of school attending childrenwas malnourished. One fourth children were facing dental caries scabies and multiple boils are the common diseases of malnourished children. |
| Khuwaja et al. [45] (2005) | 16% children were stunted. Female children compared to males were more likely to be stunted. Fathers who were working as public servant, farmers and shopkeepers were more likely to have children who were stunted when compared to landlords. |
| Anwar and Awan [42] (2003) | 36% children were stunned and 45% were underweight. Female childrenin rural areas were found two times more malnourished as compare to females living in urban areas. |
| Shah et al. [36] (2003) | 26% children were wasted and 15% were stunted. Mother’s illiteracy, poverty, and overcrowded houses were more likely to have stunned children. |
| Mian et al. [59] (2002) | Overall 44% children were malnourished. Childreninhigher age group, large family size and poverty were the majoer factors of child malnutrition. |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Asim, M.; Nawaz, Y. Child Malnutrition in Pakistan: Evidence from Literature. Children 2018, 5, 60. https://doi.org/10.3390/children5050060
Asim M, Nawaz Y. Child Malnutrition in Pakistan: Evidence from Literature. Children. 2018; 5(5):60. https://doi.org/10.3390/children5050060
Chicago/Turabian StyleAsim, Muhammad, and Yasir Nawaz. 2018. "Child Malnutrition in Pakistan: Evidence from Literature" Children 5, no. 5: 60. https://doi.org/10.3390/children5050060
APA StyleAsim, M., & Nawaz, Y. (2018). Child Malnutrition in Pakistan: Evidence from Literature. Children, 5(5), 60. https://doi.org/10.3390/children5050060





