Psychological Burden during the COVID-19 Pandemic in Female Caregivers of Preterm versus Term Born Children
Abstract
1. Introduction
2. Materials and Methods
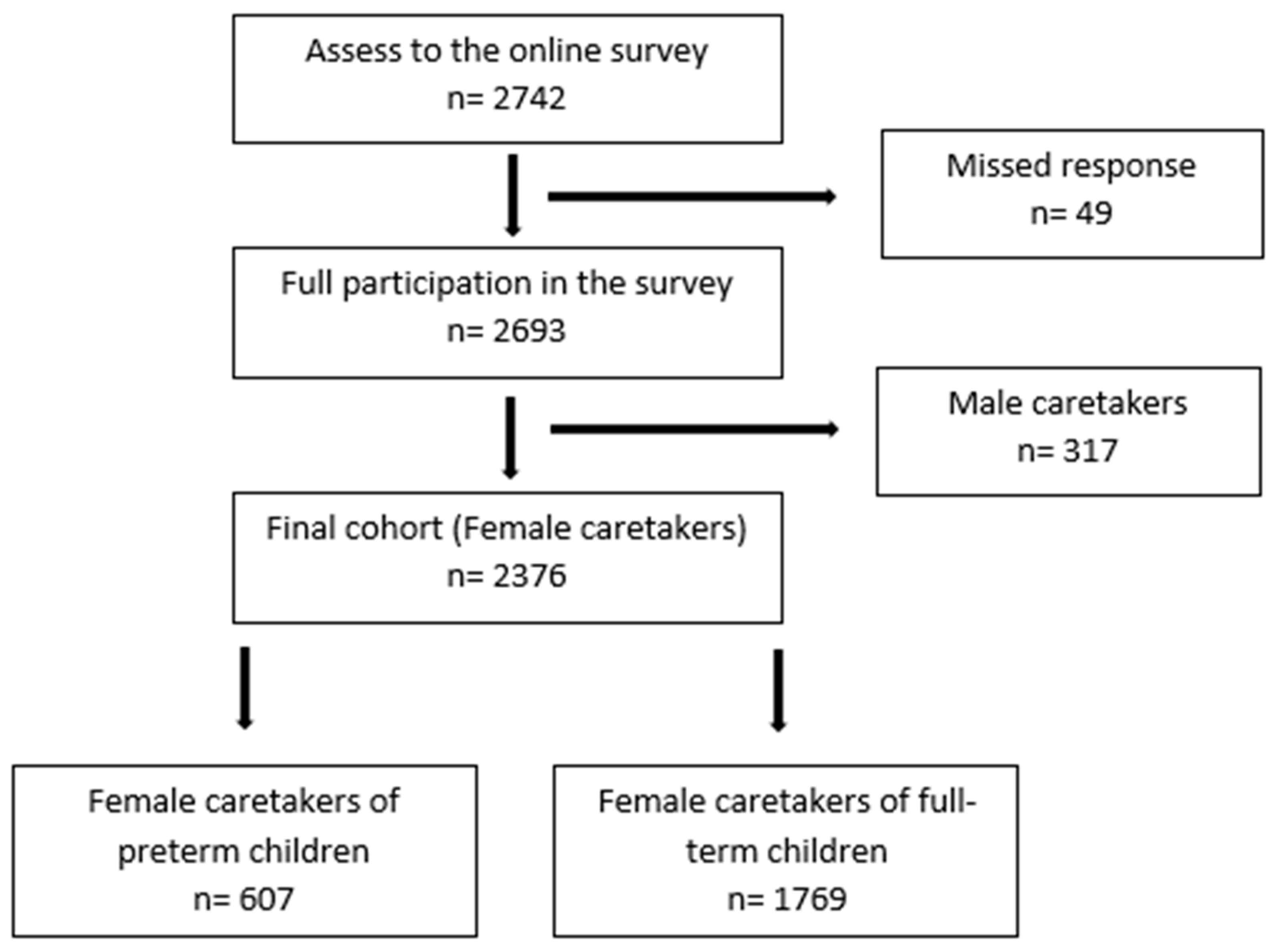
2.1. Study Design
2.2. Assessments
2.3. Statistical Analysis
3. Results
- Prevalence of generalized anxiety and depression symptoms and COVID-19 anxiety in female caregivers during the second lockdown in Germany
- Correlation of child protection behavior with generalized anxiety symptoms, depression symptoms and COVID-19 anxiety
- Multiple regression analysis
- Subgroup analysis
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| C-19-A | COVID-19-Anxiety Questionnaire |
| GAD-7 | generalized anxiety disorder-7 |
| PB | child protection behavior |
| PHQ-2 | patient health questionnaire-2 |
References
- Halligan, S.L.; Murray, L.; Martins, C.; Cooper, P.J. Maternal depression and psychiatric outcomes in adolescent offspring: A 13-year longitudinal study. J. Affect. Disord. 2007, 97, 145–154. [Google Scholar] [CrossRef] [PubMed]
- Conners-Burrow, N.A.; Bokony, P.; Whiteside-Mansell, L.; Jarrett, D.; Kraleti, S.; McKelvey, L.; Kyzer, A. Low-level depressive symptoms reduce maternal support for child cognitive development. J. Pediatr. Health Care 2014, 28, 404–412. [Google Scholar] [CrossRef] [PubMed]
- Poobalan, A.S.; Aucott, L.S.; Ross, L.; Smith, W.C.; Helms, P.J.; Williams, J.H. Effects of treating postnatal depression on mother-infant interaction and child development: Systematic review. Br. J. Psychiatry J. Ment. Sci. 2007, 191, 378–386. [Google Scholar] [CrossRef] [PubMed]
- Holditch-Davis, D.; Miles, M.S.; Weaver, M.A.; Black, B.; Beeber, L.; Thoyre, S.; Engelke, S. Patterns of distress in African-American mothers of preterm infants. J. Dev. Behav. Pediatr. 2009, 30, 193–205. [Google Scholar] [CrossRef]
- Greene, M.M.; Rossman, B.B.; Patra, K.; Kratovil, A.L.; Janes, J.E.; Meier, P.P. Depression, Anxiety, and Perinatal-Specific Posttraumatic Distress in Mothers of Very Low Birth Weight Infants in the Neonatal Intensive Care Unit. J. Dev. Behav. Pediatr. 2015, 36, 362–370. [Google Scholar] [CrossRef]
- Lasiuk, G.C.; Comeau, T.; Newburn-Cook, C. Unexpected: An interpretive description of parental traumas’ associated with preterm birth. BMC Pregnancy Childbirth 2013, 13 (Suppl. 1), S13. [Google Scholar] [CrossRef]
- Schappin, R.; Wijnroks, L.; Uniken Venema, M.M.; Jongmans, M.J. Rethinking stress in parents of preterm infants: A meta-analysis. PLoS ONE 2013, 8, e54992. [Google Scholar] [CrossRef]
- Brunson, E.; Thierry, A.; Ligier, F.; Vulliez-Coady, L.; Novo, A.; Rolland, A.C.; Eutrope, J. Prevalences and predictive factors of maternal trauma through 18 months after premature birth: A longitudinal, observational and descriptive study. PLoS ONE 2021, 16, e0246758. [Google Scholar] [CrossRef]
- Cohen, S.; Gianaros, P.J.; Manuck, S.B. A Stage Model of Stress and Disease. Perspect. Psychol. Sci. 2016, 11, 456–463. [Google Scholar] [CrossRef]
- Barra, S.M.M.; Baharudin, R.; Zulkefly, N.S.; Yahya, A.N.; Madon, Z. Understanding Sex Differences in Depressive Symptomatology Among Malaysian Adolescents. Recoletos Multidiscip. Res. J. 2019, 7, 63–79. [Google Scholar] [CrossRef]
- Herbison, C.; Allen, K.; Robinson, M.; Newnham, J.; Pennell, C. The impact of life stress on adult depression and anxiety is dependent on gender and timing of exposure. Dev. Psychopathol. 2017, 29, 1443–1454. [Google Scholar] [CrossRef]
- Cohen, S.; Murphy, M.L.M.; Prather, A.A. Ten Surprising Facts About Stressful Life Events and Disease Risk. Annu. Rev. Psychol. 2019, 70, 577–597. [Google Scholar] [CrossRef] [PubMed]
- Gloster, A.T.; Lamnisos, D.; Lubenko, J.; Presti, G.; Squatrito, V.; Constantinou, M.; Nicolaou, C.; Papacostas, S.; Aydin, G.; Chong, Y.Y.; et al. Impact of COVID-19 pandemic on mental health: An international study. PLoS ONE 2020, 15, e0244809. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [PubMed]
- Hetkamp, M.; Schweda, A.; Bäuerle, A.; Weismüller, B.; Kohler, H.; Musche, V.; Dörrie, N.; Schöbel, C.; Teufel, M.; Skoda, E.-M. Sleep disturbances, fear, and generalized anxiety during the COVID-19 shut down phase in Germany: Relation to infection rates, deaths, and German stock index DAX. Sleep Med. 2020, 75, 350–353. [Google Scholar] [CrossRef] [PubMed]
- Bäuerle, A.; Teufel, M.; Musche, V.; Weismüller, B.; Kohler, H.; Hetkamp, M.; Dörrie, N.; Schweda, A.; Skoda, E.-M. Increased generalized anxiety, depression and distress during the COVID-19 pandemic: A cross-sectional study in Germany. J. Public Health 2020, 42, 672–678. [Google Scholar] [CrossRef] [PubMed]
- Asmundson, G.J.G.; Taylor, S. Coronaphobia: Fear and the 2019-nCoV outbreak. J. Anxiety Disord. 2020, 70, 102196. [Google Scholar] [CrossRef]
- Huang, Y.; Zhao, N. Generalized anxiety disorder, depressive symptoms and sleep quality during COVID-19 outbreak in China: A web-based cross-sectional survey. Psychiatry Res. 2020, 288, 112954, Erratum in Psychiatry Res. 2021, 299, 113803. [Google Scholar] [CrossRef]
- Teufel, M.; Schweda, A.; Dörrie, N.; Musche, V.; Hetkamp, M.; Weismüller, B.; Lenzen, H.; Stettner, M.; Kohler, H.; Bäuerle, A.; et al. Not all world leaders use Twitter in response to the COVID-19 pandemic: Impact of the way of Angela Merkel on psychological distress, behaviour and risk perception. J. Public Health 2020, 42, 644–646. [Google Scholar] [CrossRef]
- Skoda, E.-M.; Bäuerle, A.; Schweda, A.; Dorrie, N.; Musche, V.; Hetkamp, M.; Kohler, H.; Teufel, M.; Weismuller, B. Severely increased generalized anxiety, but not COVID-19-related fear in individuals with mental illnesses: A population based cross-sectional study in Germany. Int. J. Soc. Psychiatry 2021, 67, 550–558. [Google Scholar] [CrossRef]
- Kohler, H.; Bäuerle, A.; Schweda, A.; Weismuller, B.; Fink, M.; Musche, V.; Robitzsch, A.; Pfeiffer, C.; Benecke, A.-V.; Dorrie, N.; et al. Increased COVID-19-related fear and subjective risk perception regarding COVID-19 affects behavior in individuals with internal high-risk diseases. J. Prim. Care Community Health 2021, 12. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Y.; Yang, Q.; Chi, J.; Dong, B.; Lv, W.; Shen, L.; Wang, Y. Comorbidities and the risk of severe or fatal outcomes associated with coronavirus disease 2019: A systematic review and meta-analysis. Int. J. Infect. Dis. 2020, 99, 47–56. [Google Scholar] [CrossRef] [PubMed]
- Petzold, M.B.; Bendau, A.; Plag, J.; Pyrkosch, L.; Maricic, L.M.; Rogoll, J.; Betzler, F.; Grosse, J.; Strohle, A. Development of the COVID-19-Anxiety Questionnaire and first psychometric testing. BJPsych Open 2020, 6, e91. [Google Scholar] [CrossRef] [PubMed]
- Musche, V.; Bäuerle, A.; Steinbach, J.; Schweda, A.; Hetkamp, M.; Weismüller, B.; Kohler, H.; Beckmann, M.; Herrmann, K.; Tewes, M.; et al. COVID-19-Related Fear and Health-Related Safety Behavior in Oncological Patients. Front. Psychol. 2020, 11, 1984. [Google Scholar] [CrossRef]
- Fink, M.; Bäuerle, A.; Schmidt, K.; Rheindorf, N.; Musche, V.; Dinse, H.; Geiger, S.; Weismüller, B.; Schweda, A.; Teufel, M.; et al. COVID-19-Fear Affects Current Safety Behavior Mediated by Neuroticism—Results of a Large Cross-Sectional Study in Germany. Front. Psychol. 2021, 12, 671768. [Google Scholar] [CrossRef]
- Garbe, L.; Rau, R.; Toppe, T. Influence of perceived threat of COVID-19 and HEXACO personality traits on toilet paper stockpiling. PLoS ONE 2020, 15, e0234232. [Google Scholar] [CrossRef] [PubMed]
- Weismüller, B.; Schweda, A.; Dörrie, N.; Musche, V.; Fink, M.; Kohler, H.; Skoda, E.-M.; Teufel, M.; Bäuerle, A. Different Correlates of COVID-19-Related Adherent and Dysfunctional Safety Behavior. Front. Public Health 2021, 8, 625664. [Google Scholar] [CrossRef]
- Schweda, A.; Weismüller, B.; Bäuerle, A.; Dörrie, N.; Musche, V.; Fink, M.; Kohler, H.; Teufel, M.; Skoda, E.-M. Phenotyping mental health: Age, community size, and depression differently modulate COVID-19-related fear and generalized anxiety. Compr. Psychiatry 2021, 104, 152218. [Google Scholar] [CrossRef]
- Flowers, P.; Davis, M.; Lohm, D.; Waller, E.; Stephenson, N. Understanding pandemic influenza behaviour: An exploratory biopsychosocial study. J. Health Psychol. 2016, 21, 759–769. [Google Scholar] [CrossRef]
- Calvano, C.; Engelke, L.; Di Bella, J.; Kindermann, J.; Renneberg, B.; Winter, S.M. Families in the COVID-19 pandemic: Parental stress, parent mental health and the occurrence of adverse childhood experiences—Results of a representative survey in Germany. Eur. Child. Adolesc. Psychiatry 2022, 31, 1–13. [Google Scholar] [CrossRef]
- Decker, O.; Müller, S.; Brahler, E.; Schellberg, D.; Herzog, W.; Herzberg, P.Y. Validation and standardization of the Generalized Anxiety Disorder Screener (GAD-7) in the general population. Med. Care 2008, 46, 266–274. [Google Scholar] [CrossRef]
- Löwe, B.; Kroenke, K.; Grafe, K. Detecting and monitoring depression with a two-item questionnaire (PHQ-2). J. Psychosom. Res. 2005, 58, 163–171. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.nimh.nih.gov/sites/default/files/documents/health/publications/generalized-anxiety-disorder-gad/generalized_anxiety_disorder.pdf (accessed on 27 March 2023).
- Diagnostisches und Statistisches Handbuch für Psychische Störungen: DSM-5, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013. [CrossRef]
- Available online: https://www.g-ba.de/downloads/62-492-2537/QFR-RL_2021-04-01_iK-2021-04-01.pdf (accessed on 25 September 2021).
- Available online: https://www.awmf.org/uploads/tx_szleitlinien/024-027l_S2k_Psychosoziale-Betreuung-Familien-Fruehgeborene-Neugeborenen_2018-11.pdf (accessed on 25 September 2021).
- Westrup, B.; Kuhn, P.; Daly, M.; Guerra, P.; Ahlqvist-Bjorkroth, S.; Bertoncelli, N.; Bergman, N.; Boukydis, Z.; Caballero, S.; Casper, C.; et al. European Standards of Care for Newborn Health: Family Support Services; EFCNI: Munchen, Germany, 2018. [Google Scholar]
- Ouyang, M.; Gui, D.; Cai, X.; Yin, Y.; Mao, X.; Huang, S.; Zeng, P.; Wang, P. Stressful Life Events and Subjective Well-Being in Vocational School Female Adolescents: The Mediating Role of Depression and the Moderating Role of Perceived Social Support. Front. Psychol. 2021, 11, 603511. [Google Scholar] [CrossRef]
- Kapti, R.E.; Yuni, S.A.; Mira, T.; Qori’ila, S.; Nurona, A.; Lilik, S. Maternal Coping Strategies for Premature Infant: A Systematic Review. Kesmas Natl. Public Health J. 2022, 17, 74–80. Available online: https://journal.fkm.ui.ac.id/kesmas/article/view/6059/1464 (accessed on 28 March 2023).
- Rossi, R.; Jannini, T.B.; Socci, V.; Pacitti, F.; Lorenzo, G.D. Stressful Life Events and Resilience During the COVID-19 Lockdown Measures in Italy: Association with Mental Health Outcomes and Age. Front. Psychiatry 2021, 12, 635832. [Google Scholar] [CrossRef]
- Kenntemich, L.; von Hülsen, L.; Schäfer, I.; Böttche, M.; Lotzin, A. Coping profiles and differences in well-being during the COVID-19 pandemic: A latent profile analysis. Stress Health 2022, 39, 460–473. [Google Scholar] [CrossRef]
- Adler, N.; Matthews, K. Health psychology: Why do some people get sick and some stay well? Annu. Rev. Psychol. 1994, 45, 229–259. [Google Scholar] [CrossRef]
- Bonanno, G.A.; Westphal, M.; Mancini, A.D. Resilience to loss and potential trauma. Annu. Rev. Clin. Psychol. 2011, 7, 511–535. [Google Scholar] [CrossRef]
- Davenport, M.H.; Meyer, S.; Meah, V.L.; Strynadka, M.C.; Khurana, R. Moms Are Not OK: COVID-19 and Maternal Mental Health. Front. Glob. Womens Health 2020, 1, 1. [Google Scholar] [CrossRef]
- Aydin, E.; Glasgow, K.A.; Weiss, S.M.; Khan, Z.; Austin, T.; Johnson, M.H.; Barlow, J.; Lloyd-Fox, S. Giving birth in a pandemic: Women’s birth experiences in England during COVID-19. BMC Pregnancy Childbirth 2022, 22, 304. [Google Scholar] [CrossRef]
- Available online: https://www.dw.com/en/covid-how-germany-battles-the-pandemic-a-chronology/a-58026877 (accessed on 27 March 2023).
- Available online: https://www.efcni.org/health-topics/going-home/hygiene-at-home/ (accessed on 25 September 2021).
- Arroyas, M.; Calvo, C.; Rueda, S.; Esquivias, M.; Gonzalez-Menchen, C.; Gonzalez-Carrasco, E.; Garcia-Garcia, M. Asthma prevalence, lung and cardiovascular function in adolescents born preterm. Sci. Rep. 2020, 10, 19616. [Google Scholar] [CrossRef]
- Jouni, J.K.; Jaakkola, M.D.; Ahmed, P.; Ieromnimon, A.; Laiou, E.; Quansah, R.; Jaakkola, M.S. Preterm delivery and asthma: A systematic review and meta-analysis. Asthma Diagn. Treat. 2006, 118, 823–830. [Google Scholar] [CrossRef]
- Silverstein, M.; Feinberg, E.; Young, R.; Sauder, S. Maternal depression, perceptions of children’s social aptitude and reported activity restriction among former very low birthweight infants. Arch. Dis. Child. 2010, 95, 521–525. [Google Scholar] [CrossRef] [PubMed]
- Greene, M.M.; Rossman, B.; Meier, P.; Patra, K. Parental perception of child vulnerability among mothers of very low birth weight infants: Psychological predictors and neurodevelopmental sequelae at 2 years. J. Perinatol. 2017, 37, 454–460. [Google Scholar] [CrossRef]
- Steinberg, L. Risk Taking in Adolescence: New Perspectives from Brain and Behavioral Science. Curr. Dir. Psychol. Sci. 2007, 16, 55–59. [Google Scholar] [CrossRef]
- Reyes, L.M.; Jaekel, J.; Wolke, D. Effects of Gestational Age and Early Parenting on Children’s Social Inhibition at 6 Years. Children 2019, 6, 81. [Google Scholar] [CrossRef] [PubMed]
- Heuser, K.M.; Jaekel, J.; Wolke, D. Origins and Predictors of Friendships in 6- to 8-Year-Old Children Born at Neonatal Risk. J. Pediatr. 2018, 193, 93–101.e5. [Google Scholar] [CrossRef] [PubMed]
- Siegenthaler, E.; Munder, T.; Egger, M. Effect of preventive interventions in mentally ill parents on the mental health of the offspring: Systematic review and meta-analysis. J. Am. Acad. Child Psychiatry 2012, 51, 8–17. [Google Scholar] [CrossRef]
- Verrocchio, M.C.; Ambrosini, A.; Fulcheri, M. Promotion of mental health in children of parents with a mental disorder. Ann. Ist. Super. Sanita 2013, 49, 406–411. [Google Scholar] [CrossRef]
- Patrick, S.W.; Henkhaus, L.E.; Zickafoose, J.S.; Lovell, K.; Halvorson, A.; Loch, S.; Letterie, M.; Davis, M.M. Well-being of parents and children during the COVID-19 pandemic: A national survey. Pediatrics 2020, 146, e2020016824. [Google Scholar] [CrossRef]
- Daig, I.; Herschbach, P.; Lehmann, A.; Knoll, N.; Decker, O. Gender and age differences in domain-specific life satisfaction and the impact of depressive and anxiety symptoms: A general population survey from Germany. Qual. Life Res. 2009, 18, 669–678. [Google Scholar] [CrossRef] [PubMed]
- Hinz, A.; Klein, A.M.; Brahler, E.; Glaesmer, H.; Luck, T.; Riedel-Heller, S.G.; Wirkner, K.; Hilbert, A. Psychometric evaluation of the generalized anxiety disorder screener GAD-7, based on a large German general population sample. J. Affect. Disord. 2017, 210, 338–344. [Google Scholar] [CrossRef] [PubMed]
- Hou, F.; Bi, F.; Jiao, R.; Luo, D.; Song, K. Gender differences of depression and anxiety among social media users during the COVID-19 outbreak in China: A cross-sectional study. BMC Public Health 2020, 20, 1648. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.researchgate.net/publication/355906636_Evaluation_of_the_E-Mental_Health_Mindfulness-Based_and_Skills-Based_CoPE_It_Intervention_to_Reduce_Psychological_Distress_in_Times_of_COVID-19_Results_of_a_Bicentre_Longitudinal_Study (accessed on 10 October 2021).
| N | % | |
|---|---|---|
| Age | ||
| 18–24 years | 168 | 6.2 |
| 25–34 years | 1736 | 64.5 |
| 35–44 years | 723 | 26.8 |
| 45–54 years | 63 | 2.3 |
| 55–74 years | 3 | 0.1 |
| Marital status | ||
| Single | 219 | 8.1 |
| Married | 1872 | 69.5 |
| In a relationship | 522 | 19.4 |
| Divorced/separated | 73 | 2.7 |
| Widowed | 3 | 0.1 |
| Other | 4 | 0.1 |
| Family role | ||
| Mother | 2657 | 98.7 |
| Foster mother | 7 | 0.3 |
| Others | 25 | 0.9 |
| Educational level | ||
| University education | 856 | 31.8 |
| Higher education entrance | ||
| Qualification | 854 | 31.7 |
| Secondary education | 827 | 30.7 |
| Lower secondary education | 136 | 5.1 |
| No qualification | 5 | 0.2 |
| Other | 15 | 0.6 |
| Occupation | ||
| Not employed | 609 | 22.6 |
| Child’s age (Medium age: 2, 6 years) | ||
| 0–3 years | 1726 | 64.1 |
| 4–6 years | 331 | 12.3 |
| 7–10 years | 190 | 7.1 |
| 11–17 years | 86 | 3.2 |
| Missing birth date | 360 | 13.4 |
| Childcare | ||
| Family | 1283 | 54.0 |
| Others | 1 | 0.0 |
| Preschool | 827 | 34.8 |
| School | 266 | 11.2 |
| Breast feeding last 8 month | ||
| Yes | 898 | 37.8 |
| Gestational age of preterm children | ||
| 32–36 weeks | 345 | 56.8 * |
| 28–32 weeks | 173 | 28.5 * |
| ≤28 weeks | 89 | 14.7 * |
| Child’s diseases | ||
| Bronchopulmonary Dysplasia | 55 | 9.1 * |
| Operation | 131 | 5.5 |
| Asthma | 74 | 3.1 |
| Total | 2693 | 100.0 |
| N | Generalized Anxiety (GAD-7) | Depression (PHQ-2) | COVID-19 Anxiety (C-19-A) | Child Protection Behavior (PB) | |
|---|---|---|---|---|---|
| Female caregivers of preterm children | 607 | 6.44 [0.0–21.0] | 1.70 [0.0–6.0] | 18.83 [9.0–39.0] | 31.65 [9.0–63.0] |
| 42.5% b 14% c 9.7% d | 22.1% e | ||||
| Female caregivers of full-term children | 1769 | 6.63 [0.0–21.0] | 1.89 [0.0–6.0] | 18.84 [1.0–43.0] | 30.48 [9.0–61.0] |
| 35.1% b 15.4% c 8.7% d | 27.8% e | ||||
| p (95% CI) a | 0.178 | ≤0.05 | 0.945 | ≤0.05 | |
| Z | −1.346 | −2.275 | −0.069 | −2.233 |
| Correlation of Child Protection Behavior with | Spearman-Rho | p | |
|---|---|---|---|
| Generalized anxiety (GAD-7) | 0.327 | ≤0.001 | |
| Depression (PHQ-2) | 0.237 | ≤0.001 | |
| COVID-19 Anxiety (C-19-A) | 0.422 | ≤0.001 | |
| Predictor | Β | Βse | T | p |
|---|---|---|---|---|
| Generalized anxiety (GAD-7) | 0.225 | 0.113 | 3.586 | ≤0.001 |
| Depression (PHQ-2) | −0.085 | −0.014 | −0.501 | 0.617 |
| COVID-19 anxiety | 0.635 | 0.380 | 14.775 | ≤0.001 |
| Female caregiver’ age | 0.804 | 0.049 | 2.303 | 0.021 |
| Child age | −0.000017 | 0.000 | −0.18 | 0.985 |
| Education level of female caregiver | 0.482 | 0.046 | 2.147 | 0.032 |
| Employer status | 0.142 | 0.011 | 0.515 | 0.606 |
| Number of siblings | 0.371 | 0.029 | 1.352 | 0.177 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brasseler, M.; Fink, M.; Mitschdörfer, B.; Reimann, M.; Skoda, E.-M.; Bäuerle, A.; Teufel, M.; Felderhoff-Müser, U.; Hüning, B. Psychological Burden during the COVID-19 Pandemic in Female Caregivers of Preterm versus Term Born Children. Children 2023, 10, 787. https://doi.org/10.3390/children10050787
Brasseler M, Fink M, Mitschdörfer B, Reimann M, Skoda E-M, Bäuerle A, Teufel M, Felderhoff-Müser U, Hüning B. Psychological Burden during the COVID-19 Pandemic in Female Caregivers of Preterm versus Term Born Children. Children. 2023; 10(5):787. https://doi.org/10.3390/children10050787
Chicago/Turabian StyleBrasseler, Maire, Madeleine Fink, Barbara Mitschdörfer, Margarete Reimann, Eva-Maria Skoda, Alexander Bäuerle, Martin Teufel, Ursula Felderhoff-Müser, and Britta Hüning. 2023. "Psychological Burden during the COVID-19 Pandemic in Female Caregivers of Preterm versus Term Born Children" Children 10, no. 5: 787. https://doi.org/10.3390/children10050787
APA StyleBrasseler, M., Fink, M., Mitschdörfer, B., Reimann, M., Skoda, E.-M., Bäuerle, A., Teufel, M., Felderhoff-Müser, U., & Hüning, B. (2023). Psychological Burden during the COVID-19 Pandemic in Female Caregivers of Preterm versus Term Born Children. Children, 10(5), 787. https://doi.org/10.3390/children10050787







