Impacts of Climate Change on Inequities in Child Health
Abstract
:1. Introduction
2. Existing Inequities in Child Health
3. The Impact of Climate Change on Environmental Health Hazards in Childhood
4. Pathways between Inequities in Child Health Outcomes and the Impacts of Climate Change on Environmental Hazards
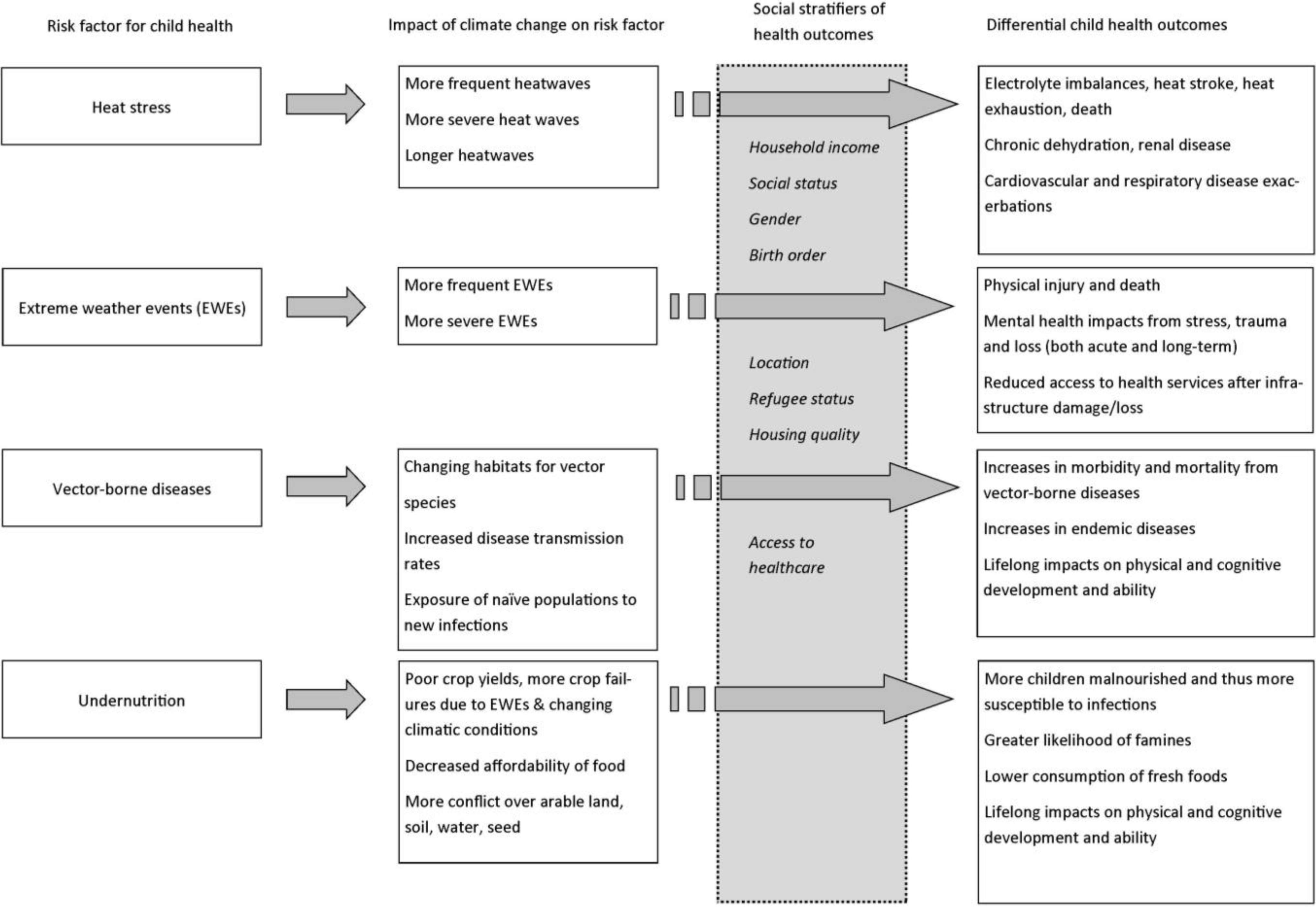
4.1. Heat Stress
4.2. Extreme Weather Events
4.3. Vector-Borne Diseases
4.4. Undernutrition
5. Conclusion: A Way Forward—Reducing Child Health Inequities to Reduce the Impacts of Climate Change on Child Health
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Caldwell, J.; McDonald, P. Influence of maternal education on infant and child mortality: Levels and causes. Health Policy Educ. 1982, 2, 251–267. [Google Scholar] [CrossRef] [PubMed]
- Kiros, G.-E.; Hogan, D.P. War, famine and excess child mortality in Africa: The role of parental education. Int. J. Epidemiol. 2001, 30, 447–455. [Google Scholar] [CrossRef] [PubMed]
- Grantham-McGregor, S.; Cheung, Y.B.; Cueto, S.; Glewwe, P.; Richter, L.; Strupp, B. Developmental potential in the first 5 years for children in developing countries. Lancet 2007, 369, 60–70. [Google Scholar] [CrossRef] [PubMed]
- Barros, F.C.; Victora, C.G.; Scherpbier, R.; Gwatkin, D. Socioeconomic inequities in the health and nutrition of children in low/middle income countries. Rev. Saude Publica 2010, 44, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Victora, C.G.; Wagstaff, A.; Schellenberg, J.A.; Gwatkin, D.; Claeson, M.; Habicht, J.-P. Applying an equity lens to child health and mortality: More of the same is not enough. Lancet 2003, 362, 233–241. [Google Scholar] [CrossRef] [PubMed]
- Fotso, J.-C.; Kuate-Defo, B. Socioeconomic inequalities in early childhood malnutrition and morbidity: Modification of the household-level effects by the community SES. Health Place 2005, 11, 205–225. [Google Scholar] [CrossRef] [PubMed]
- Xu, Z.; Sheffield, P.E.; Hu, W.; Su, H.; Yu, W.; Qi, X.; Tong, S. Climate change and children’s health—A call for research on what works to protect children. Int. J. Environ. Res. Public Health 2012, 9, 3298–3316. [Google Scholar] [CrossRef] [PubMed]
- Bartlett, S. Climate change and urban children: Impacts and implications for adaptation in low- and middle-income countries. Environ. Urban. 2008, 20, 501–519. [Google Scholar] [CrossRef]
- Bunyavanich, S.; Landrigan, C.P.; McMichael, A.J.; Epstein, P.R. The impact of climate change on child health. Ambul. Pediatr. 2003, 3, 44–52. [Google Scholar] [CrossRef] [PubMed]
- Pronczuk, J.; Surdu, S. Children’s environmental health in the twenty-first century: Challenges and solutions. Ann. N.Y. Acad. Sci. 2008, 1140, 143–154. [Google Scholar] [CrossRef] [PubMed]
- Ebi, K.; Paulson, J.A. Climate change and children. Pediatr. Clin. N. Am. 2007, 54, 213–226. [Google Scholar] [CrossRef]
- Voelker, R. Climate change puts children in jeopardy. JAMA 2009, 301, 2197–2199. [Google Scholar] [CrossRef] [PubMed]
- Walker, S.P.; Wachs, T.D.; Gardner, J.M.; Lozoff, B.; Wasserman, G.A.; Pollitt, E.; Carter, J.A. Child development: Risk factors for adverse outcomes in developing countries. Lancet 2007, 369, 145–157. [Google Scholar] [CrossRef] [PubMed]
- Shea, K.M. Global climate change and children’s health. Pediatrics 2007, 120, e1359–e1367. [Google Scholar] [CrossRef] [PubMed]
- Heat-related deaths—Four states, July–August 2001, and united states, 1979–1999. MMWR 2002, 51, 567–570.
- Knowlton, K.; Rotkin-Ellman, M.; King, G.; Margolis, H.G.; Smith, D.; Solomon, G.; Trent, R.; English, P. The 2006 california heat wave: Impacts on hospitalizations and emergency department visitis. Environ. Health Perspect. 2009, 117, 61–67. [Google Scholar] [PubMed]
- Lam, L.T. The association between climatic factors and childhood illnesses presented to hospital emergency among young children. Int. J. Environ. Health Res. 2007, 17, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Strand, L.B.; Barnett, A.G.; Tong, S. Maternal exposure to ambient temperature and the risks of preterm birth and stillbirth in brisbane, australia. Am. J. Epidemiol. 2012, 175, 99–107. [Google Scholar] [CrossRef] [PubMed]
- Basu, R.; Malig, B.; Ostro, B. High ambient temperature and the risk of preterm delivery. Am. J. Epidemiol. 2010, 172, 1108–1117. [Google Scholar] [PubMed]
- Kovats, S.; Akhtar, R. Climate, climate change and human health in asian cities. Environ. Urban. 2008, 20, 165–175. [Google Scholar] [CrossRef]
- Smit, W.; Parnell, S. Urban sustainability and human health: An african perspective. Curr. Opin. Environ. Sustain. 2012, 4, 443–450. [Google Scholar] [CrossRef]
- Sverdlik, A. Ill-health and poverty: A literature review on health in informal settlements. Environ. Urban. 2011, 23, 123–155. [Google Scholar] [CrossRef]
- Fussell, E.; Sastry, N.; VanLandingham, M. Race, socioeconomic status and return migration to new orleans after hurricane katrina. Popul. Environ. 2010, 31, 20–42. [Google Scholar] [CrossRef] [PubMed]
- Pradhan, E.K.; West, K.P.; Katz, J.; LeClerq, S.C.; Khatry, S.K.; Shrestha, S.R. Risk of flood-related mortality in nepal. Disasters 2007, 31, 57–70. [Google Scholar] [CrossRef] [PubMed]
- Paardekooper, B.; deJong, J.T.V.M.; Hermanns, J. The psychological impact of war and the refugee situation on south sudanese children in refugee camps in northern uganda: An exploratory study. J. Child Psychol. Psychiatry 1999, 40, 529–536. [Google Scholar] [CrossRef] [PubMed]
- McDermott, B.M.; Less, E.M.; Judd, M.; Gibbon, P. Posttraumatic stress disorder and general psychopathology in children and adolescents following a wildfire disaster. Can. J. Psychiatry 2005, 50, 137–143. [Google Scholar] [PubMed]
- Dean, J.; Stain, H.J. The impact of drought on the emotional well-being of children and adolescents in rural and remote new south wales. J. Rural Health 2007, 23, 356–364. [Google Scholar] [CrossRef] [PubMed]
- Dean, J.G.; Stain, H.J. Mental health impact for adolescents living with prolonged drought. Aust. J. Rural Health 2010, 18, 32–37. [Google Scholar] [CrossRef] [PubMed]
- Shaw, J.A.; Applegate, B.; Schorr, C. Twenty-one-month follow-up study of school-age children exposed to hurricane andrew. J. Am. Acad. Child Adolesc. Psychiatry 1996, 35, 359–364. [Google Scholar] [CrossRef] [PubMed]
- Mclaughlin, K.A.; Fairbank, J.A.; Gruber, M.J.; Jones, R.T.; Lakoma, M.D.; Pfefferbaum, B.; Sampson, N.A.; Kessler, R.C. Serious emotional disturbance among youths exposed to hurricane katrina 2 years postdisaster. J. Am. Acad. Child Adolesc. Psychiatry 2009, 48, 1069–1078. [Google Scholar] [CrossRef] [PubMed]
- Lustig, S.L.; Kia-Keating, M.; Knight, W.G.; Geltman, P.; Ellis, H.; Kinzie, D.; Keane, T.; Saxe, G.N. Review of child and adolescent refugee mental health. J. Am. Acad. Child Adolesc. Psychiatry 2004, 43, 24–36. [Google Scholar] [CrossRef] [PubMed]
- Leichenko, R.; Silva, J.A. Climate change and poverty: Vulnerability, impacts and alleviation strategies. Wiley Interdiscip. Rev. Clim. Change 2014, 5, 539–556. [Google Scholar] [CrossRef]
- Keenan, H.T.; Marshall, S.W.; Nocera, M.A.; Runyan, D.K. Increased incidence of inflicted traumatic brain injury in children after a natural disaster. Am. J. Prev. Med. 2004, 26, 189–193. [Google Scholar] [CrossRef] [PubMed]
- Curtis, T.; Miller, B.C.; Berry, E.H. Changes in reports and incidence of child abuse following natural disasters. Child Abuse Negl. 2000, 24, 1151–1162. [Google Scholar] [CrossRef] [PubMed]
- Patz, J.A.; Graczyk, T.K.; Geller, N.; Vittor, A.Y. Effects of environmental change on emerging parasitic diseases. Int. J. Parasitol. 2000, 30, 1395–1405. [Google Scholar] [CrossRef] [PubMed]
- Reiter, P. Climate change and mosquito-borne disease. Environ. Health Perspect 2001, 109 (Suppl. 1), 141–161. [Google Scholar] [CrossRef]
- Subak, S. Effects of climate on variability in lyme disease incidence in the northeastern united states. Am. J. Epidemiol. 2003, 157, 531–538. [Google Scholar] [CrossRef] [PubMed]
- Ogden, N.H.; Maarouf, A.; Barker, I.K.; Bigras-Poulin, M.; Lindsay, L.R.; Morshed, M.G.; O’Callaghan, C.J.; Ramay, F.; Waltner-Toews, D.; Charron, D.F. Climate change and the potential for range expansion of the lyme disease vector ixodes scapularis in canada. Int. J. Parasitol. 2006, 36, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Patz, J.A.; Reisen, W.K. Immunology, climate change and vector-borne diseases. Trends Immunol. 2001, 22, 171–172. [Google Scholar] [CrossRef] [PubMed]
- Bennett, C.M.; McMichael, A.J. Non-heat related impacts of climate change on working populations. Glob. Health Action 2010, 3. [Google Scholar] [CrossRef]
- Shears, P. Epidemiology and infection in famine and disasters. Epidemiol. Infect. 1991, 107, 241–251. [Google Scholar] [CrossRef] [PubMed]
- Boivin, M.J. Effects of early cerebral malaria on cognitive ability in senegalese children. Dev. Behav. Pediatr. 2002, 23, 353–364. [Google Scholar] [CrossRef]
- Carter, J.A.; Mung’ala-Odera, V.; Neville, B.G.R.; Murira, G.; Mturi, N.; Musumba, C.; Newton, C.R.J.C. Persistent neurocognitive impairments associated with severe falciparum malaria in kenyan children. J. Neurol. Neurosurg. Psychiatry 2005, 76, 476–481. [Google Scholar] [CrossRef] [PubMed]
- Kihara, M.; Carter, J.A.; Newton, C.R.J.C. The effect of plasmodium falciparum on cognition: A systematic review. Trop. Med. Int. Health 2006, 11, 386–397. [Google Scholar] [PubMed]
- Holding, P.A.; Snow, R.W. Impact of Plasmodium falciparum malaria on performance and learning: Review of the evidence. Am. J. Trop. Med. Hyg. 2001, 64, 68–75. [Google Scholar] [PubMed]
- Loevinsohn, M.E. Climatic warming and increased malaria incidence in Rwanda. Lancet 1994, 343, 714–718. [Google Scholar] [CrossRef] [PubMed]
- Kiszewski, A.E.; Teklehaimanot, A. A review of the clinical and epidemiologic burdens of epidemic malaria. Am. J. Trop. Med. Hyg. 2004, 71, 128–135. [Google Scholar] [PubMed]
- Checkley, W.; Epstein, L.D.; Gilman, R.H.; Figueroa, D.; Cama, R.I.; Patz, J.A.; Black, R.E. Effects of el niño and ambient temperature on hospital admissions for diarrhoeal diseases in peruvian children. Lancet 2000, 355, 442–450. [Google Scholar] [PubMed]
- Parry, M.; Rosenzweig, C.; Livermore, M. Climate change, global food supply and risk of hunger. Philos. Trans. R. Soc. Lond. B 2005, 360, 2125–2138. [Google Scholar] [CrossRef]
- Baker, L. Feeling the Heat: Child Survival in a Changing Climate; International Save the Children Alliance: London, UK, 2009; p. 22. [Google Scholar]
- Caulfield, L.E.; Richard, S.A.; Black, R.E. Undernutrition as an underlying cause of malaria morbidity and mortality in children less than five years old. Am. J. Trop. Med. Hyg. 2004, 71, 55–63. [Google Scholar] [PubMed]
- Black, R.; Allen, L.; Bhutta, Z.; Caulfield, L.; de Onis, M.; Ezzati, M.; Mathers, C.; Rivera, J. Maternal and child undernutrition: Global and regional exposures and health consequences. Lancet 2008, 371, 243–260. [Google Scholar] [CrossRef] [PubMed]
- Victora, C.G.; Adair, L.; Fall, C.; Hallal, P.C.; Martorell, R.; Richter, L.; Sachdev, H.S. Maternal and child undernutrition: Consequences for adult health and human capital. Lancet 2008, 371, 340–357. [Google Scholar] [CrossRef] [PubMed]
- Choudhury, K.K.; Hanifi, M.A.; Rasheed, S.; Bhuiya, A. Gender inequality and severe malnutrition among children in a remote rural area of bangladesh. J. Health Popul. Nutr. 2000, 18, 123–130. [Google Scholar] [PubMed]
- Gupta, M.D. Selective discrimination against female children in rural Punjab, India. Popul. Dev. Rev. 1987, 13, 77–100. [Google Scholar] [CrossRef]
- Pande, R.P. Selective gender differences in childhood nutrition and immunization in rural India: The role of siblings. Demography 2003, 40, 395–418. [Google Scholar] [CrossRef] [PubMed]
- Kishor, S. “May god give sons to all”: Gender and child mortality in India. Am. Sociol. Rev. 1993, 58, 247–265. [Google Scholar] [CrossRef]
- Behrman, J.R. Nutrition, health, birth order and seasonality: Intrahousehold allocation among children in india. J. Dev. Econ. 1988, 28, 43–62. [Google Scholar] [CrossRef] [PubMed]
- Friel, S.; Marmot, M.; McMichael, A.J.; Kjellstrom, T.; Vagero, D. Global health equity and climate stabilisation: A common agenda. Lancet 2008, 372, 1677–1683. [Google Scholar] [CrossRef] [PubMed]
- Urbano, M.; Maclellan, N.; Ruff, T.; Blashki, G. Climate Change and Children in the Pacific Islands; University of Melbourne: Melbourne, Austrilia, 2010; p. 89. [Google Scholar]
- UNICEF. The State of the World’s Children 2008: Child Survival; Hatteras Press: New York, NY, USA, 2008; pp. 1–164. [Google Scholar]
- Marmot, M.; Friel, S.; Bell, R.; Houweling, T.A.J.; Taylor, S. Closing the gap in a generation: Health equity through action on the social determinants of health. Lancet 2008, 372, 1661–1669. [Google Scholar] [CrossRef] [PubMed]
- Marmot, M. Fair Society, Healthy Lives: The Marmot Review. Available online: http://www.instituteofhealthequity.org (accessed on 2 March 2014).
- Series on Health and Climate Change: Public Health Benefits of Strategies to Reduce Greenhouse-gas Emissions. Available online: http://www.thelancet.com/series/health-and-climate-change (accessed on 2 March 2014).
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bennett, C.M.; Friel, S. Impacts of Climate Change on Inequities in Child Health. Children 2014, 1, 461-473. https://doi.org/10.3390/children1030461
Bennett CM, Friel S. Impacts of Climate Change on Inequities in Child Health. Children. 2014; 1(3):461-473. https://doi.org/10.3390/children1030461
Chicago/Turabian StyleBennett, Charmian M., and Sharon Friel. 2014. "Impacts of Climate Change on Inequities in Child Health" Children 1, no. 3: 461-473. https://doi.org/10.3390/children1030461
APA StyleBennett, C. M., & Friel, S. (2014). Impacts of Climate Change on Inequities in Child Health. Children, 1(3), 461-473. https://doi.org/10.3390/children1030461



