The Role of Selenium in Atherosclerosis Development, Progression, Prevention and Treatment
Abstract
1. Introduction
2. Molecular Basis of the Se-Mediated Athero-Protective Activities
2.1. Oxidative Stress and Se
2.2. Inflammation and Se
2.2.1. Se and Eicosanoid Metabolism
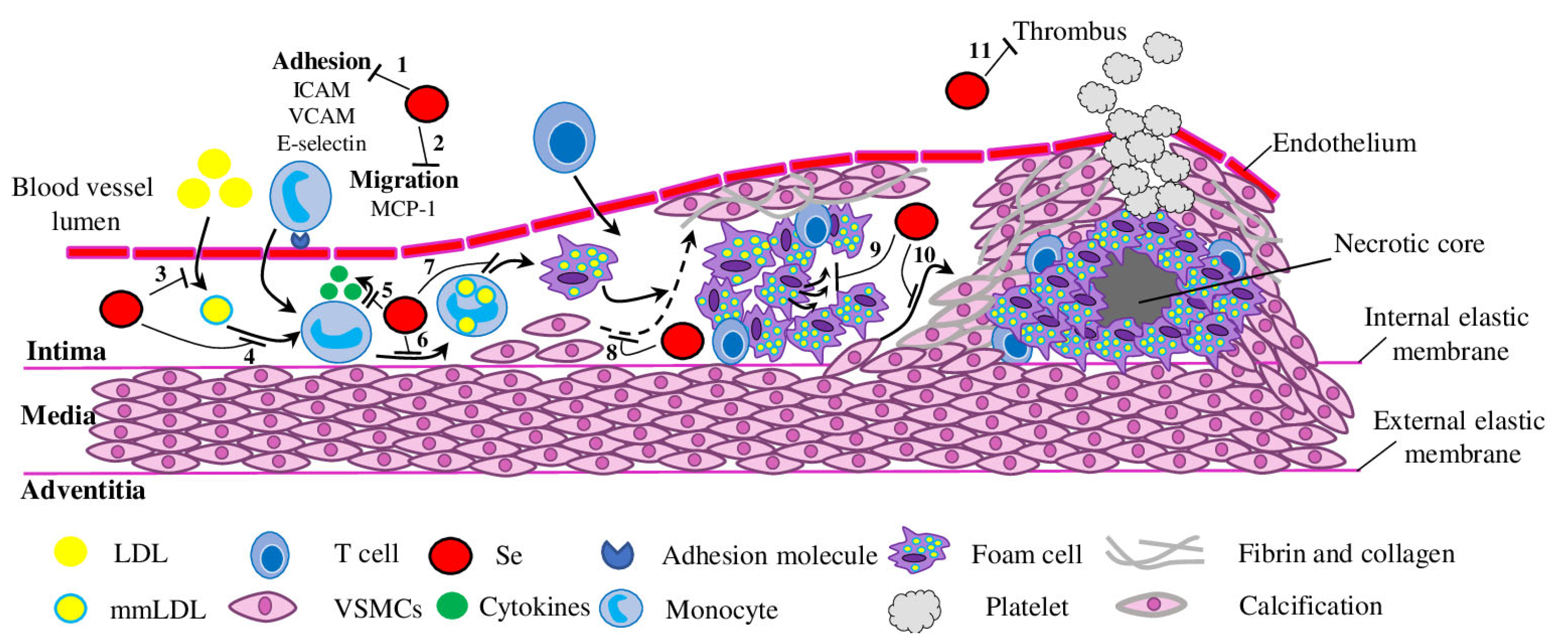
2.2.2. Se and Leukocyte Recruitment and Migration
2.2.3. Reduction of Foam Cell Formation by Se
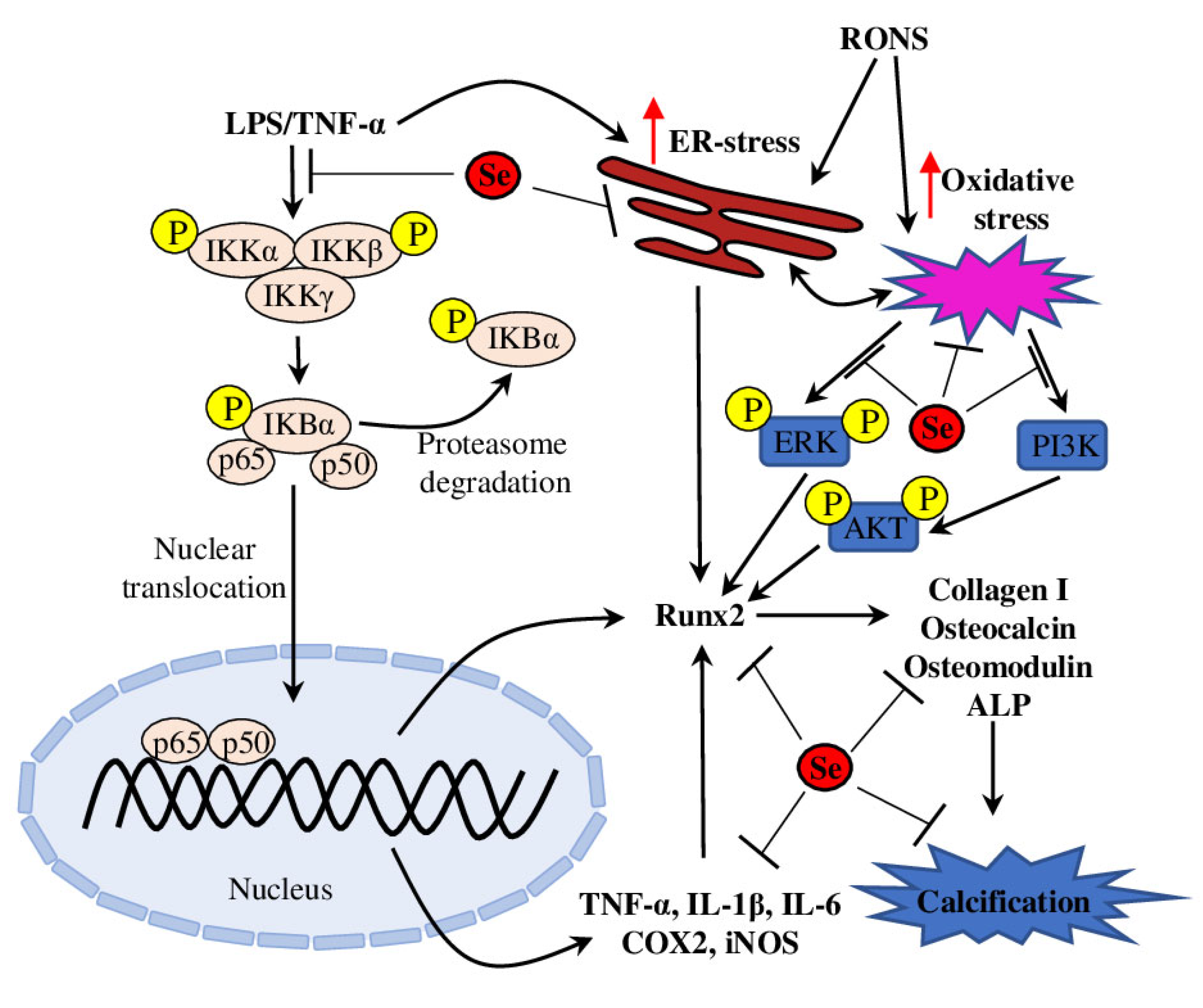
3. Se and Vascular Calcification
4. Se and Vascular Cell Apoptosis and Autophagy
4.1. Anti-Apoptotic Properties of Se
4.2. Se in Regulation of Apoptosis/Autophagy Balance
5. Se and Endothelial Dysfunction
6. Human Studies of Se Supplementation to Treat Cardiovascular Diseases
6.1. Human Studies with Se+Coenzyme Q10 Supplementation
6.2. Human Studies with Se Supplementation in CAD Treatment
6.3. Human Studies with Se Supplementation in Atherosclerosis Treatment
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kieliszek, M. Selenium–Fascinating Microelement, Properties and Sources in Food. Molecules 2019, 24, 1298. [Google Scholar] [CrossRef]
- Peng, J.-J.; Yue, S.-Y.; Fang, Y.-H.; Liu, X.-L.; Wang, C.-H. Mechanisms Affecting the Biosynthesis and Incorporation Rate of Selenocysteine. Molecules 2021, 26, 7120. [Google Scholar] [CrossRef] [PubMed]
- Cockman, E.M.; Narayan, V.; Willard, B.; Shetty, S.P.; Copeland, P.R.; Driscoll, D.M. Identification of the Selenoprotein S Positive UGA Recoding (SPUR) Element and Its Position-Dependent Activity. RNA Biol. 2019, 16, 1682–1696. [Google Scholar] [CrossRef]
- Incalza, M.A.; D’Oria, R.; Natalicchio, A.; Perrini, S.; Laviola, L.; Giorgino, F. Oxidative Stress and Reactive Oxygen Species in Endothelial Dysfunction Associated with Cardiovascular and Metabolic Diseases. Vasc. Pharmacol. 2018, 100, 1–19. [Google Scholar] [CrossRef]
- Wang, K.; Chen, X.-Z.; Wang, Y.-H.; Cheng, X.-L.; Zhao, Y.; Zhou, L.-Y.; Wang, K. Emerging Roles of Ferroptosis in Cardiovascular Diseases. Cell Death Discov. 2022, 8, 394. [Google Scholar] [CrossRef] [PubMed]
- McClung, J.P.; Roneker, C.A.; Mu, W.; Lisk, D.J.; Langlais, P.; Liu, F.; Lei, X.G. Development of Insulin Resistance and Obesity in Mice Overexpressing Cellular Glutathione Peroxidase. Proc. Natl. Acad. Sci. USA 2004, 101, 8852–8857. [Google Scholar] [CrossRef]
- Handy, D.E.; Loscalzo, J. Responses to Reductive Stress in the Cardiovascular System. Free Radic. Biol. Med. 2017, 109, 114–124. [Google Scholar] [CrossRef]
- Merry, T.L.; Tran, M.; Dodd, G.T.; Mangiafico, S.P.; Wiede, F.; Kaur, S.; McLean, C.L.; Andrikopoulos, S.; Tiganis, T. Hepatocyte Glutathione Peroxidase-1 Deficiency Improves Hepatic Glucose Metabolism and Decreases Steatohepatitis in Mice. Diabetologia 2016, 59, 2632–2644. [Google Scholar] [CrossRef]
- Kryukov, G.V.; Castellano, S.; Novoselov, S.V.; Lobanov, A.V.; Zehtab, O.; Guigó, R.; Gladyshev, V.N. Characterization of Mammalian Selenoproteomes. Science 2003, 300, 1439–1443. [Google Scholar] [CrossRef]
- Al-Mubarak, A.A.; Grote Beverborg, N.; Anker, S.D.; Samani, N.J.; Dickstein, K.; Filippatos, G.; Van Veldhuisen, D.J.; Voors, A.A.; Bomer, N.; Van Der Meer, P. A Clinical Tool to Predict Low Serum Selenium in Patients with Worsening Heart Failure. Nutrients 2020, 12, 2541. [Google Scholar] [CrossRef]
- Shimada, B.K.; Alfulaij, N.; Seale, L.A. The Impact of Selenium Deficiency on Cardiovascular Function. Int. J. Mol. Sci. 2021, 22, 10713. [Google Scholar] [CrossRef] [PubMed]
- Handy, D.E.; Joseph, J.; Loscalzo, J. Selenium, a Micronutrient That Modulates Cardiovascular Health via Redox Enzymology. Nutrients 2021, 13, 3238. [Google Scholar] [CrossRef] [PubMed]
- Glanz, V.; Bezsonov, E.E.; Soldatov, V.; Orekhov, A.N. Thirty-Five-Year History of Desialylated Lipoproteins Discovered by Vladimir Tertov. Biomedicines 2022, 10, 1174. [Google Scholar] [CrossRef]
- Xu, S.; Ilyas, I.; Little, P.J.; Li, H.; Kamato, D.; Zheng, X.; Luo, S.; Li, Z.; Liu, P.; Han, J.; et al. Endothelial Dysfunction in Atherosclerotic Cardiovascular Diseases and Beyond: From Mechanism to Pharmacotherapies. Pharmacol. Rev. 2021, 73, 924–967. [Google Scholar] [CrossRef]
- Soehnlein, O.; Libby, P. Targeting Inflammation in Atherosclerosis—From Experimental Insights to the Clinic. Nat. Rev. Drug Discov. 2021, 20, 589–610. [Google Scholar] [CrossRef] [PubMed]
- Batty, M.; Bennett, M.R.; Yu, E. The Role of Oxidative Stress in Atherosclerosis. Cells 2022, 11, 3843. [Google Scholar] [CrossRef]
- WHO CVDs Fact Sheets Cardiovascular Diseases (CVDs). Available online: https://www.who.int/health-topics/cardiovascular-diseases#tab=tab_1 (accessed on 11 June 2023).
- Liu, H.; Xu, H.; Huang, K. Selenium in the Prevention of Atherosclerosis and Its Underlying Mechanisms. Metallomics 2017, 9, 21–37. [Google Scholar] [CrossRef]
- Niki, E. Oxidant-Specific Biomarkers of Oxidative Stress. Association with Atherosclerosis and Implication for Antioxidant Effects. Free Radic. Biol. Med. 2018, 120, 425–440. [Google Scholar] [CrossRef]
- Tardif, J.-C.; McMurray, J.J.; Klug, E.; Small, R.; Schumi, J.; Choi, J.; Cooper, J.; Scott, R.; Lewis, E.F.; L’Allier, P.L.; et al. Effects of Succinobucol (AGI-1067) after an Acute Coronary Syndrome: A Randomised, Double-Blind, Placebo-Controlled Trial. Lancet 2008, 371, 1761–1768. [Google Scholar] [CrossRef]
- Toledo-Ibelles, P.; Mas-Oliva, J. Antioxidants in the Fight Against Atherosclerosis: Is This a Dead End? Curr. Atheroscler. Rep. 2018, 20, 36. [Google Scholar] [CrossRef]
- Poznyak, A.V.; Nikiforov, N.G.; Markin, A.M.; Kashirskikh, D.A.; Myasoedova, V.A.; Gerasimova, E.V.; Orekhov, A.N. Overview of OxLDL and Its Impact on Cardiovascular Health: Focus on Atherosclerosis. Front. Pharmacol. 2021, 11, 613780. [Google Scholar] [CrossRef] [PubMed]
- Khera, A.; Vanderlelie, J.J.; Holland, O.; Perkins, A.V. Overexpression of Endogenous Anti-Oxidants with Selenium Supplementation Protects Trophoblast Cells from Reactive Oxygen Species-Induced Apoptosis in a Bcl-2-Dependent Manner. Biol. Trace Elem. Res. 2017, 177, 394–403. [Google Scholar] [CrossRef] [PubMed]
- Ren, Z.; Chen, C.; Fan, Y.; Chen, C.; He, H.; Wang, X.; Zhang, Z.; Zuo, Z.; Peng, G.; Hu, Y.; et al. Toxicity of DON on GPx1-Overexpressed or Knockdown Porcine Splenic Lymphocytes In Vitro and Protective Effects of Sodium Selenite. Oxidative Med. Cell. Longev. 2019, 2019, 5769752. [Google Scholar] [CrossRef]
- Zheng, X.; Hu, X.; Ge, T.; Li, M.; Shi, M.; Luo, J.; Lai, H.; Nie, T.; Li, F.; Li, H. MicroRNA-328 Is Involved in the Effect of Selenium on Hydrogen Peroxide-Induced Injury in H9c2 Cells. J. Biochem. Mol. Toxicol. 2017, 31, e21920. [Google Scholar] [CrossRef]
- Ruseva, B.; Atanasova, M.; Tsvetkova, R.; Betova, T.; Mollova, M.; Alexandrova, M.; Laleva, P.; Dimitrova, A. Effect of Selenium Supplementation on Redox Status of the Aortic Wall in Young Spontaneously Hypertensive Rats. Oxidative Med. Cell. Longev. 2015, 2015, 609053. [Google Scholar] [CrossRef]
- Hamza, R.Z.; AL-Harbi, M.S.; El-Shenawy, N.S. Ameliorative Effect of Vitamin E and Selenium against Oxidative Stress Induced by Sodium Azide in Liver, Kidney, Testis and Heart of Male Mice. Biomed. Pharmacother. 2017, 91, 602–610. [Google Scholar] [CrossRef]
- Feriani, A.; Hachani, R.; Tir, M.; Ghazouani, L.; Mufti, A.; Borgi, M.A.; Allagui, M.S. Bifenthrin Exerts Proatherogenic Effects via Arterial Accumulation of Native and Oxidized LDL in Rats: The Beneficial Role of Vitamin E and Selenium. Environ. Sci. Pollut. Res. 2020, 27, 5651–5660. [Google Scholar] [CrossRef]
- Yamaguchi, A.; Botta, E.; Holinstat, M. Eicosanoids in Inflammation in the Blood and the Vessel. Front. Pharmacol. 2022, 13, 997403. [Google Scholar] [CrossRef]
- Piper, K.; Garelnabi, M. Eicosanoids: Atherosclerosis and Cardiometabolic Health. J. Clin. Transl. Endocrinol. 2020, 19, 100216. [Google Scholar] [CrossRef]
- Schrör, K. Prostaglandins, Other Eicosanoids and Endothelial Cells. Basic Res. Cardiol. 1985, 80, 502–514. [Google Scholar] [CrossRef]
- Nelson, J.R.; Raskin, S. The Eicosapentaenoic Acid:Arachidonic Acid Ratio and Its Clinical Utility in Cardiovascular Disease. Postgrad. Med. 2019, 131, 268–277. [Google Scholar] [CrossRef] [PubMed]
- Dhanjal, N.I.K.; Sharma, S.; Prabhu, K.S.; Tejo Prakash, N. Selenium Supplementation through Se-Rich Dietary Matrices Can Upregulate the Anti-Inflammatory Responses in Lipopolysaccharide-Stimulated Murine Macrophages. Food Agric. Immunol. 2017, 28, 1374–1392. [Google Scholar] [CrossRef] [PubMed]
- Dhanjal, N.I.; Sharma, S.; Skalny, A.V.; Skalnaya, M.G.; Ajsuvakova, O.P.; Tinkov, A.A.; Zhang, F.; Guo, X.; Prabhu, K.S.; Tejo Prakash, N. Selenium-Rich Maize Modulates the Expression of Prostaglandin Genes in Lipopolysaccharide-Stimulated RAW264.7 Macrophages. Food Funct. 2019, 10, 2839–2846. [Google Scholar] [CrossRef]
- Wolfram, T.; Weidenbach, L.M.; Adolf, J.; Schwarz, M.; Schädel, P.; Gollowitzer, A.; Werz, O.; Koeberle, A.; Kipp, A.P.; Koeberle, S.C. The Trace Element Selenium Is Important for Redox Signaling in Phorbol Ester-Differentiated THP-1 Macrophages. Int. J. Mol. Sci. 2021, 22, 11060. [Google Scholar] [CrossRef]
- Mavangira, V.; Sordillo, L.M. Role of Lipid Mediators in the Regulation of Oxidative Stress and Inflammatory Responses in Dairy Cattle. Res. Vet. Sci. 2018, 116, 4–14. [Google Scholar] [CrossRef] [PubMed]
- Mavangira, V.; Brown, J.; Gandy, J.C.; Sordillo, L.M. 20-Hydroxyeicosatetraenoic Acid Alters Endothelial Cell Barrier Integrity Independent of Oxidative Stress and Cell Death. Prostaglandins Other Lipid Mediat. 2020, 149, 106425. [Google Scholar] [CrossRef]
- Mauersberger, C.; Hinterdobler, J.; Schunkert, H.; Kessler, T.; Sager, H.B. Where the Action Is—Leukocyte Recruitment in Atherosclerosis. Front. Cardiovasc. Med. 2022, 8, 813984. [Google Scholar] [CrossRef]
- Zhang, F.; Yu, W.; Hargrove, J.L.; Greenspan, P.; Dean, R.G.; Taylor, E.W.; Hartle, D.K. Inhibition of TNF-α Induced ICAM-1, VCAM-1 and E-Selectin Expression by Selenium. Atherosclerosis 2002, 161, 381–386. [Google Scholar] [CrossRef]
- Zhang, Y.; Cartland, S.P.; Henriquez, R.; Patel, S.; Gammelgaard, B.; Flouda, K.; Hawkins, C.L.; Rayner, B.S. Selenomethionine Supplementation Reduces Lesion Burden, Improves Vessel Function and Modulates the Inflammatory Response within the Setting of Atherosclerosis. Redox Biol. 2020, 29, 101409. [Google Scholar] [CrossRef]
- Maddox, J.F.; Aherne, K.M.; Reddy, C.C.; Sordillo, L.M. Increased Neutrophil Adherence and Adhesion Molecule MRNA Expression in Endothelial Cells during Selenium Deficiency. J. Leukoc. Biol. 1999, 65, 658–664. [Google Scholar] [CrossRef]
- Lubos, E.; Kelly, N.J.; Oldebeken, S.R.; Leopold, J.A.; Zhang, Y.-Y.; Loscalzo, J.; Handy, D.E. Glutathione Peroxidase-1 Deficiency Augments Proinflammatory Cytokine-Induced Redox Signaling and Human Endothelial Cell Activation. J. Biol. Chem. 2011, 286, 35407–35417. [Google Scholar] [CrossRef]
- Handy, D.E.; Loscalzo, J. The Role of Glutathione Peroxidase-1 in Health and Disease. Free Radic. Biol. Med. 2022, 188, 146–161. [Google Scholar] [CrossRef]
- Sharma, A.; Yuen, D.; Huet, O.; Pickering, R.; Stefanovic, N.; Bernatchez, P.; De Haan, J.B. Lack of Glutathione Peroxidase-1 Facilitates a pro-Inflammatory and Activated Vascular Endothelium. Vasc. Pharmacol. 2016, 79, 32–42. [Google Scholar] [CrossRef] [PubMed]
- Broman, M.; Lindfors, M.; Norberg, Å.; Hebert, C.; Rooyackers, O.; Wernerman, J.; Fläring, U. Low Serum Selenium Is Associated with the Severity of Organ Failure in Critically Ill Children. Clin. Nutr. 2018, 37, 1399–1405. [Google Scholar] [CrossRef] [PubMed]
- De Almeida, C.B.; Leite, H.P.; Lopes Junior, E.; Konstantyner, T.; Franco, M.D.C.P. Erythrocyte and Plasma Selenium in Children with Acute Inflammatory Response. J. Trace Elem. Med. Biol. 2022, 74, 127068. [Google Scholar] [CrossRef] [PubMed]
- Lopes Júnior, E.; Leite, H.P.; Pinho Franco, M.D.C.; Konstantyner, T. Association of Selenium Status with Endothelial Activation during Acute Systemic Inflammation in Children. Clin. Nutr. ESPEN 2022, 47, 367–374. [Google Scholar] [CrossRef] [PubMed]
- Holley, A.; Pitman, J.; Miller, J.; Harding, S.; Larsen, P. Glutathione Peroxidase Activity and Expression Levels Are Significantly Increased in Acute Coronary Syndromes. J. Investig. Med. 2017, 65, 919–925. [Google Scholar] [CrossRef]
- Cheng, F.; Torzewski, M.; Degreif, A.; Rossmann, H.; Canisius, A.; Lackner, K.J. Impact of Glutathione Peroxidase-1 Deficiency on Macrophage Foam Cell Formation and Proliferation: Implications for Atherogenesis. PLoS ONE 2013, 8, e72063. [Google Scholar] [CrossRef]
- Kader, T.; Porteous, C.M.; Williams, M.J.A.; Gieseg, S.P.; McCormick, S.P.A. Ribose-Cysteine Increases Glutathione-Based Antioxidant Status and Reduces LDL in Human Lipoprotein(a) Mice. Atherosclerosis 2014, 237, 725–733. [Google Scholar] [CrossRef]
- Kader, T.; Porteous, C.M.; Jones, G.T.; Dickerhof, N.; Narayana, V.K.; Tull, D.; Taraknath, S.; McCormick, S.P.A. Ribose-Cysteine Protects against the Development of Atherosclerosis in ApoE-Deficient Mice. PLoS ONE 2020, 15, e0228415. [Google Scholar] [CrossRef]
- Oliveira, J.D.; Straliotto, M.R.; Mancini, G.; Figueiredo, C.P.; Braga, A.L.; Teixeira, J.B.R.; Bem, A.F. Atheroprotective Action of a Modified Organoselenium Compound: In Vitro Evidence. An. Acad. Bras. Ciências 2016, 88, 1953–1965. [Google Scholar] [CrossRef] [PubMed]
- Jinnouchi, H.; Sato, Y.; Sakamoto, A.; Cornelissen, A.; Mori, M.; Kawakami, R.; Gadhoke, N.V.; Kolodgie, F.D.; Virmani, R.; Finn, A.V. Calcium Deposition within Coronary Atherosclerotic Lesion: Implications for Plaque Stability. Atherosclerosis 2020, 306, 85–95. [Google Scholar] [CrossRef] [PubMed]
- Skenteris, N.T.; Seime, T.; Witasp, A.; Karlöf, E.; Wasilewski, G.B.; Heuschkel, M.A.; Jaminon, A.M.G.; Oduor, L.; Dzhanaev, R.; Kronqvist, M.; et al. Osteomodulin Attenuates Smooth Muscle Cell Osteogenic Transition in Vascular Calcification. Clin. Transl. Med. 2022, 12, e682. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Wang, C.; Chen, H. MicroRNAs Are Critical in Regulating Smooth Muscle Cell Mineralization and Apoptosis during Vascular Calcification. J. Cell. Mol. Med. 2020, 24, 13564–13572. [Google Scholar] [CrossRef]
- Chen, Y.; Zhao, X.; Wu, H. Arterial Stiffness: A Focus on Vascular Calcification and Its Link to Bone Mineralization. Arterioscler. Thromb. Vasc. Biol. 2020, 40, 1078–1093. [Google Scholar] [CrossRef]
- Liu, H.; Li, X.; Qin, F.; Huang, K. Selenium Suppresses Oxidative-Stress-Enhanced Vascular Smooth Muscle Cell Calcification by Inhibiting the Activation of the PI3K/AKT and ERK Signaling Pathways and Endoplasmic Reticulum Stress. J. Biol. Inorg. Chem. 2014, 19, 375–388. [Google Scholar] [CrossRef]
- Ye, Y.; Bian, W.; Fu, F.; Hu, J.; Liu, H. Selenoprotein S Inhibits Inflammation-Induced Vascular Smooth Muscle Cell Calcification. J. Biol. Inorg. Chem. 2018, 23, 739–751. [Google Scholar] [CrossRef]
- Lin, C.; Zhang, L.; Li, B.; Zhang, F.; Shen, Q.; Kong, G.; Wang, X.; Cui, S.; Dai, R.; Cao, W.; et al. Selenium-Containing Protein from Selenium-Enriched Spirulina Platensis Attenuates High Glucose-Induced Calcification of MOVAS Cells by Inhibiting ROS-Mediated DNA Damage and Regulating MAPK and PI3K/AKT Pathways. Front. Physiol. 2020, 11, 791. [Google Scholar] [CrossRef]
- Grootaert, M.O.J.; Moulis, M.; Roth, L.; Martinet, W.; Vindis, C.; Bennett, M.R.; De Meyer, G.R.Y. Vascular Smooth Muscle Cell Death, Autophagy and Senescence in Atherosclerosis. Cardiovasc. Res. 2018, 114, 622–634. [Google Scholar] [CrossRef]
- Ye, Y.; Fu, F.; Li, X.; Yang, J.; Liu, H. Selenoprotein S Is Highly Expressed in the Blood Vessels and Prevents Vascular Smooth Muscle Cells from Apoptosis: S Elenoprotein sp. Revents Vsmcs from a Poptosis. J. Cell. Biochem. 2016, 117, 106–117. [Google Scholar] [CrossRef]
- Zhang, S.; Liu, X.; Bawa-Khalfe, T.; Lu, L.-S.; Lyu, Y.L.; Liu, L.F.; Yeh, E.T.H. Identification of the Molecular Basis of Doxorubicin-Induced Cardiotoxicity. Nat. Med. 2012, 18, 1639–1642. [Google Scholar] [CrossRef] [PubMed]
- Doroshow, J.H.; Esworthy, R.S.; Chu, F.-F. Control of Doxorubicin-Induced, Reactive Oxygen-Related Apoptosis by Glutathione Peroxidase 1 in Cardiac Fibroblasts. Biochem. Biophys. Rep. 2020, 21, 100709. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Yang, M.; Ai, F.; Huang, C. Cardioprotective Effect of Aloe Vera Biomacromolecules Conjugated with Selenium Trace Element on Myocardial Ischemia-Reperfusion Injury in Rats. Biol. Trace Elem. Res. 2017, 177, 345–352. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Yang, B.; Cao, H.-L.; Wang, R.-Y.; Lu, Z.-Y.; Chi, R.-F.; Li, B. Selenium Supplementation Protects against Lipopolysaccharide-Induced Heart Injury via Sting Pathway in Mice. Biol. Trace Elem. Res. 2021, 199, 1885–1892. [Google Scholar] [CrossRef]
- Li, N.; Zhou, H.; Wu, H.; Wu, Q.; Duan, M.; Deng, W.; Tang, Q. STING-IRF3 Contributes to Lipopolysaccharide-Induced Cardiac Dysfunction, Inflammation, Apoptosis and Pyroptosis by Activating NLRP3. Redox Biol. 2019, 24, 101215. [Google Scholar] [CrossRef] [PubMed]
- Yu, S.; Liu, X.; Men, L.; Yao, J.; Xing, Q.; Du, J. Selenoprotein S Protects against High Glucose-induced Vascular Endothelial Apoptosis through the PKCβII/JNK/Bcl-2 Pathway. J. Cell. Biochem. 2019, 120, 8661–8675. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Virgilio, L.; Silva-Lucero, M.-C.; Flores-Morelos, D.-S.; Gallardo-Nieto, J.; Lopez-Toledo, G.; Abarca-Fernandez, A.-M.; Zacapala-Gómez, A.-E.; Luna-Muñoz, J.; Montiel-Sosa, F.; Soto-Rojas, L.O.; et al. Autophagy: A Key Regulator of Homeostasis and Disease: An Overview of Molecular Mechanisms and Modulators. Cells 2022, 11, 2262. [Google Scholar] [CrossRef]
- Yang, J.; Zhang, Y.; Hamid, S.; Cai, J.; Liu, Q.; Li, H.; Zhao, R.; Wang, H.; Xu, S.; Zhang, Z. Interplay between Autophagy and Apoptosis in Selenium Deficient Cardiomyocytes in Chicken. J. Inorg. Biochem. 2017, 170, 17–25. [Google Scholar] [CrossRef]
- Çakmak, H.A.; Demir, M. MicroRNA and Cardiovascular Diseases. Balk. Med J. 2020, 37, 60–71. [Google Scholar] [CrossRef]
- Liu, Q.; Cai, J.; Gao, Y.; Yang, J.; Gong, Y.; Zhang, Z. MiR-2954 Inhibits PI3K Signaling and Induces Autophagy and Apoptosis in Myocardium Selenium Deficiency. Cell. Physiol. Biochem. 2018, 51, 778–792. [Google Scholar] [CrossRef]
- Yang, T.; Cao, C.; Yang, J.; Liu, T.; Lei, X.G.; Zhang, Z.; Xu, S. MiR-200a-5p Regulates Myocardial Necroptosis Induced by Se Deficiency via Targeting RNF11. Redox Biol. 2018, 15, 159–169. [Google Scholar] [CrossRef] [PubMed]
- Qiao, S.; Hong, L.; Zhu, Y.; Zha, J.; Wang, A.; Qiu, J.; Li, W.; Wang, C.; An, J.; Zhang, H. RIPK1-RIPK3 Mediates Myocardial Fibrosis in Type 2 Diabetes Mellitus by Impairing Autophagic Flux of Cardiac Fibroblasts. Cell Death Dis. 2022, 13, 147. [Google Scholar] [CrossRef]
- Shengyu, C.; Yinhua, L.; Yuanhong, L.; Jinbo, Z.; Can, F.; Hao, X.; Changjiang, Z. Selenium Alleviates Heart Remodeling through Sirt1/AKT/GSK-3β Pathway. Int. Immunopharmacol. 2022, 111, 109158. [Google Scholar] [CrossRef]
- Luo, G.; Jian, Z.; Zhu, Y.; Zhu, Y.; Chen, B.; Ma, R.; Tang, F.; Xiao, Y. Sirt1 Promotes Autophagy and Inhibits Apoptosis to Protect Cardiomyocytes from Hypoxic Stress. Int. J. Mol. Med. 2019, 43, 2033–2043. [Google Scholar] [CrossRef] [PubMed]
- Infante, T.; Costa, D.; Napoli, C. Novel Insights Regarding Nitric Oxide and Cardiovascular Diseases. Angiology 2021, 72, 411–425. [Google Scholar] [CrossRef]
- Shaito, A.; Aramouni, K.; Assaf, R.; Parenti, A.; Orekhov, A.; Yazbi, A.E.; Pintus, G.; Eid, A.H. Oxidative Stress-Induced Endothelial Dysfunction in Cardiovascular Diseases. Front. Biosci. (Landmark Ed.) 2022, 27, 0105. [Google Scholar] [CrossRef]
- Ng, H.H.; Leo, C.H.; O’Sullivan, K.; Alexander, S.-A.; Davies, M.J.; Schiesser, C.H.; Parry, L.J. 1,4-Anhydro-4-Seleno-d-Talitol (SeTal) Protects Endothelial Function in the Mouse Aorta by Scavenging Superoxide Radicals under Conditions of Acute Oxidative Stress. Biochem. Pharmacol. 2017, 128, 34–45. [Google Scholar] [CrossRef]
- Cui, S.; Men, L.; Li, Y.; Zhong, Y.; Yu, S.; Li, F.; Du, J. Selenoprotein S Attenuates Tumor Necrosis Factor- α -Induced Dysfunction in Endothelial Cells. Mediat. Inflamm. 2018, 2018, 1625414. [Google Scholar] [CrossRef]
- Ren, H.; Mu, J.; Ma, J.; Gong, J.; Li, J.; Wang, J.; Gao, T.; Zhu, P.; Zheng, S.; Xie, J.; et al. Selenium Inhibits Homocysteine-Induced Endothelial Dysfunction and Apoptosis via Activation of AKT. Cell. Physiol. Biochem. 2016, 38, 871–882. [Google Scholar] [CrossRef]
- Zhong, Y.; Yu, S.; Yu, H.; Yao, J.; Men, L.; Li, Y.; Wang, Q.; Du, J. Selenoprotein S Attenuates Endothelial Dysfunction in a Diabetic Vascular Chip. Exp. Gerontol. 2020, 137, 110963. [Google Scholar] [CrossRef]
- Wang, Z.; Li, Y.; Yao, J.; Yu, S.; Yu, H.; Men, L.; Du, J. Selenoprotein S Attenuates High Glucose and/or Ox-LDL-Induced Endothelium Injury by Regulating Akt/MTOR Signaling and Autophagy. Int. J. Biochem. Cell Biol. 2021, 141, 106111. [Google Scholar] [CrossRef]
- Keshan Disease Research Group of the Chinese Academy of Medical Sciences, Beijing; Antiepidemic Station of Sichuan Province, Chengdu; Antiepidemic Station of Xichang District, Sichuan; Antiepidemic Station of Mianning County, Sichuan. Observations on Effect of Sodium Selenite in Prevention of Keshan Disease. Chin. Med. J. 1979, 92, 471–476. [Google Scholar]
- Navas-Acien, A.; Bleys, J.; Guallar, E. Selenium Intake and Cardiovascular Risk: What Is New? Curr. Opin. Lipidol. 2008, 19, 43–49. [Google Scholar] [CrossRef] [PubMed]
- Benstoem, C.; Goetzenich, A.; Kraemer, S.; Borosch, S.; Manzanares, W.; Hardy, G.; Stoppe, C. Selenium and Its Supplementation in Cardiovascular Disease—What Do We Know? Nutrients 2015, 7, 3094–3118. [Google Scholar] [CrossRef] [PubMed]
- Kuria, A.; Tian, H.; Li, M.; Wang, Y.; Aaseth, J.O.; Zang, J.; Cao, Y. Selenium Status in the Body and Cardiovascular Disease: A Systematic Review and Meta-Analysis. Crit. Rev. Food Sci. Nutr. 2021, 61, 3616–3625. [Google Scholar] [CrossRef]
- Flores-Mateo, G.; Navas-Acien, A.; Pastor-Barriuso, R.; Guallar, E. Selenium and Coronary Heart Disease: A Meta-Analysis. Am. J. Clin. Nutr. 2006, 84, 762–773. [Google Scholar] [CrossRef]
- Zhang, X.; Liu, C.; Guo, J.; Song, Y. Selenium Status and Cardiovascular Diseases: Meta-Analysis of Prospective Observational Studies and Randomized Controlled Trials. Eur. J. Clin. Nutr. 2016, 70, 162–169. [Google Scholar] [CrossRef]
- Ju, W.; Li, X.; Li, Z.; Wu, G.R.; Fu, X.F.; Yang, X.M.; Zhang, X.Q.; Gao, X.B. The Effect of Selenium Supplementation on Coronary Heart Disease: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. J. Trace Elem. Med. Biol. 2017, 44, 8–16. [Google Scholar] [CrossRef]
- Jenkins, D.J.; Kitts, D.; Giovannucci, E.L.; Sahye-Pudaruth, S.; Paquette, M.; Blanco Mejia, S.; Patel, D.; Kavanagh, M.; Tsirakis, T.; Kendall, C.W.; et al. Selenium, Antioxidants, Cardiovascular Disease, and All-Cause Mortality: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Am. J. Clin. Nutr. 2020, 112, 1642–1652. [Google Scholar] [CrossRef]
- Zachariah, M.; Maamoun, H.; Milano, L.; Rayman, M.P.; Meira, L.B.; Agouni, A. Endoplasmic Reticulum Stress and Oxidative Stress Drive Endothelial Dysfunction Induced by High Selenium. J. Cell. Physiol. 2021, 236, 4348–4359. [Google Scholar] [CrossRef]
- Alehagen, U.; Aaseth, J. Selenium and Coenzyme Q10 Interrelationship in Cardiovascular Diseases—A Clinician’s Point of View. J. Trace Elem. Med. Biol. 2015, 31, 157–162. [Google Scholar] [CrossRef]
- Alehagen, U.; Johansson, P.; Björnstedt, M.; Rosén, A.; Dahlström, U. Cardiovascular Mortality and N-Terminal-ProBNP Reduced after Combined Selenium and Coenzyme Q10 Supplementation: A 5-Year Prospective Randomized Double-Blind Placebo-Controlled Trial among Elderly Swedish Citizens. Int. J. Cardiol. 2013, 167, 1860–1866. [Google Scholar] [CrossRef]
- Alehagen, U.; Lindahl, T.L.; Aaseth, J.; Svensson, E.; Johansson, P. Levels of SP-Selectin and Hs-CRP Decrease with Dietary Intervention with Selenium and Coenzyme Q10 Combined: A Secondary Analysis of a Randomized Clinical Trial. PLoS ONE 2015, 10, e0137680. [Google Scholar] [CrossRef] [PubMed]
- Alehagen, U.; Johansson, P.; Svensson, E.; Aaseth, J.; Alexander, J. Improved Cardiovascular Health by Supplementation with Selenium and Coenzyme Q10: Applying Structural Equation Modelling (SEM) to Clinical Outcomes and Biomarkers to Explore Underlying Mechanisms in a Prospective Randomized Double-Blind Placebo-Controlled Intervention Project in Sweden. Eur. J. Nutr. 2022, 61, 3135–3148. [Google Scholar] [CrossRef]
- Alehagen, U.; Aaseth, J.; Johansson, P. Reduced Cardiovascular Mortality 10 Years after Supplementation with Selenium and Coenzyme Q10 for Four Years: Follow-Up Results of a Prospective Randomized Double-Blind Placebo-Controlled Trial in Elderly Citizens. PLoS ONE 2015, 10, e0141641. [Google Scholar] [CrossRef] [PubMed]
- Alehagen, U.; Aaseth, J.; Alexander, J.; Johansson, P. Still Reduced Cardiovascular Mortality 12 Years after Supplementation with Selenium and Coenzyme Q10 for Four Years: A Validation of Previous 10-Year Follow-up Results of a Prospective Randomized Double-Blind Placebo-Controlled Trial in Elderly. PLoS ONE 2018, 13, e0193120. [Google Scholar] [CrossRef]
- Alehagen, U.; Alexander, J.; Aaseth, J.; Larsson, A.; Lindahl, T.L. Significant Decrease of von Willebrand Factor and Plasminogen Activator Inhibitor-1 by Providing Supplementation with Selenium and Coenzyme Q10 to an Elderly Population with a Low Selenium Status. Eur. J. Nutr. 2020, 59, 3581–3590. [Google Scholar] [CrossRef]
- Shimizu, T.; Uematsu, M.; Yoshizaki, T.; Obata, J.; Nakamura, T.; Fujioka, D.; Watanabe, K.; Watanabe, Y.; Kugiyama, K. Myocardial Production of Plasminogen Activator Inhibitor-1 Is Associated with Coronary Endothelial and Ventricular Dysfunction after Acute Myocardial Infarction. J. Atheroscler. Thromb. 2016, 23, 557–566. [Google Scholar] [CrossRef]
- Rutten, B.; Maseri, A.; Cianflone, D.; Laricchia, A.; Cristell, N.; Durante, A.; Spartera, M.; Ancona, F.; Limite, L.; Hu, D.; et al. Plasma Levels of Active Von Willebrand Factor Are Increased in Patients with First ST-Segment Elevation Myocardial Infarction: A Multicenter and Multiethnic Study. Eur. Heart J. Acute Cardiovasc. Care 2015, 4, 64–74. [Google Scholar] [CrossRef] [PubMed]
- Alehagen, U.; Johansson, P.; Aaseth, J.; Alexander, J.; Surowiec, I.; Lundstedt-Enkel, K.; Lundstedt, T. Significant Changes in Metabolic Profiles after Intervention with Selenium and Coenzyme Q10 in an Elderly Population. Biomolecules 2019, 9, 553. [Google Scholar] [CrossRef]
- Opstad, T.B.; Kalstad, A.A.; Pettersen, A.Å.; Arnesen, H.; Seljeflot, I. Novel Biomolecules of Ageing, Sex Differences and Potential Underlying Mechanisms of Telomere Shortening in Coronary Artery Disease. Exp. Gerontol. 2019, 119, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Alehagen, U.; Aaseth, J.; Alexander, J.; Johansson, P.; Larsson, A. Supplemental Selenium and Coenzyme Q10 Reduce Glycation along with Cardiovascular Mortality in an Elderly Population with Low Selenium Status—A Four-Year, Prospective, Randomised, Double-Blind Placebo-Controlled Trial. J. Trace Elem. Med. Biol. 2020, 61, 126541. [Google Scholar] [CrossRef] [PubMed]
- Selvin, E.; Rawlings, A.M.; Lutsey, P.L.; Maruthur, N.; Pankow, J.S.; Steffes, M.; Coresh, J. Fructosamine and Glycated Albumin and the Risk of Cardiovascular Outcomes and Death. Circulation 2015, 132, 269–277. [Google Scholar] [CrossRef] [PubMed]
- Opstad, T.B.; Alexander, J.; Aaseth, J.O.; Larsson, A.; Seljeflot, I.; Alehagen, U. Selenium and Coenzyme Q10 Intervention Prevents Telomere Attrition, with Association to Reduced Cardiovascular Mortality—Sub-Study of a Randomized Clinical Trial. Nutrients 2022, 14, 3346. [Google Scholar] [CrossRef] [PubMed]
- Mirmohammadsadeghi, A.; Gharipour, M.; Roohafza, H.; Dianatkhah, M.; Sadeghi, M. Effects of Selenium Supplementation on Paraoxonase-1 and Myeloperoxidase Activity in Subjects with Cardiovascular Disease: The Selenegene Study, a Double-Blind Randomized Controlled Trial. Arch. Med. Sci. Atheroscler. Dis. 2018, 3, 112–118. [Google Scholar] [CrossRef]
- Kunutsor, S.K.; Bakker, S.J.L.; James, R.W.; Dullaart, R.P.F. Serum Paraoxonase-1 Activity and Risk of Incident Cardiovascular Disease: The PREVEND Study and Meta-Analysis of Prospective Population Studies. Atherosclerosis 2016, 245, 143–154. [Google Scholar] [CrossRef]
- Gharipour, M.; Ouguerram, K.; Nazih, E.; Salehi, M.; Behmanesh, M.; Roohafza, H.; Hosseini, S.M.; Nezafati, P.; Dianatkhah, M.; Gharipour, A.; et al. Effects of Selenium Supplementation on Expression of SEPP1 in MRNA and Protein Levels in Subjects with and without Metabolic Syndrome Suffering from Coronary Artery Disease: Selenegene Study a Double-blind Randomized Controlled Trial. J. Cell. Biochem. 2018, 119, 8282–8289. [Google Scholar] [CrossRef]
- Gharipour, M.; Sadeghi, M.; Haghjooy-Javanmard, S.; Hamledari, H.; Khosravi, E.; Dianatkhah, M.; Vaseghi, G. Effects of Selenium Intake on the Expression of Prostaglandin-Endoperoxide Synthase 2 (Cyclooxygenase-2) and Matrix Metallopeptidase-9 Genes in the Coronary Artery Disease: Selenegene Study, a Double-Blind Randomized Controlled Trial. ARYA Atheroscler. J. 2021, 17, 1–7. [Google Scholar] [CrossRef]
- Khabbaz Koche Ghazi, M.; Ghaffari, S.; Naemi, M.; Salehi, R.; Taban Sadeghi, M.; Barati, M.; Namazi Shabestari, A.; Kafil, B.; Mesri Alamdari, N.; Soleimanzadeh, H.; et al. Effects of Sodium Selenite and Selenium-Enriched Yeast on Cardiometabolic Indices of Patients with Atherosclerosis: A Double-Blind Randomized Clinical Trial Study. J. Cardiovasc. Thorac. Res. 2021, 13, 314–319. [Google Scholar] [CrossRef]
- Roshanravan, N.; Koche Ghazi, M.K.; Ghaffari, S.; Naemi, M.; Alamdari, N.M.; Shabestari, A.N.; Mosharkesh, E.; Soleimanzadeh, H.; Sadeghi, M.T.; Alipour, S.; et al. Sodium Selenite and Se-Enriched Yeast Supplementation in Atherosclerotic Patients: Effects on the Expression of Pyroptosis-Related Genes and Oxidative Stress Status. Nutr. Metab. Cardiovasc. Dis. 2022, 32, 1528–1537. [Google Scholar] [CrossRef]
- Liang, Y.; Pan, Z.; Zhu, M.; Gao, R.; Wang, Y.; Cheng, Y.; Zhang, N. Exposure to Essential and Non-Essential Trace Elements and Risks of Congenital Heart Defects: A Narrative Review. Front. Nutr. 2023, 10, 1121826. [Google Scholar] [CrossRef] [PubMed]
- Dabravolski, S.A.; Sadykhov, N.K.; Kartuesov, A.G.; Borisov, E.E.; Sukhorukov, V.N.; Orekhov, A.N. Interplay between Zn2+ Homeostasis and Mitochondrial Functions in Cardiovascular Diseases and Heart Ageing. Int. J. Mol. Sci. 2022, 23, 6890. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Wang, Q.; Luo, W.; Jia, S.; Liu, D.; Ma, W.; Gu, H.; Wei, X.; He, Y.; Cao, S.; et al. Relationship between Maternal Heavy Metal Exposure and Congenital Heart Defects: A Systematic Review and Meta-Analysis. Environ. Sci. Pollut. Res. 2022, 29, 55348–55366. [Google Scholar] [CrossRef]
- Rahman, M.M.; Hossain, K.F.B.; Banik, S.; Sikder, M.T.; Akter, M.; Bondad, S.E.C.; Rahaman, M.S.; Hosokawa, T.; Saito, T.; Kurasaki, M. Selenium and Zinc Protections against Metal-(Loids)-Induced Toxicity and Disease Manifestations: A Review. Ecotoxicol. Environ. Saf. 2019, 168, 146–163. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dabravolski, S.A.; Sukhorukov, V.N.; Melnichenko, A.A.; Khotina, V.A.; Orekhov, A.N. The Role of Selenium in Atherosclerosis Development, Progression, Prevention and Treatment. Biomedicines 2023, 11, 2010. https://doi.org/10.3390/biomedicines11072010
Dabravolski SA, Sukhorukov VN, Melnichenko AA, Khotina VA, Orekhov AN. The Role of Selenium in Atherosclerosis Development, Progression, Prevention and Treatment. Biomedicines. 2023; 11(7):2010. https://doi.org/10.3390/biomedicines11072010
Chicago/Turabian StyleDabravolski, Siarhei A., Vasily N. Sukhorukov, Alexandra A. Melnichenko, Victoria A. Khotina, and Alexander N. Orekhov. 2023. "The Role of Selenium in Atherosclerosis Development, Progression, Prevention and Treatment" Biomedicines 11, no. 7: 2010. https://doi.org/10.3390/biomedicines11072010
APA StyleDabravolski, S. A., Sukhorukov, V. N., Melnichenko, A. A., Khotina, V. A., & Orekhov, A. N. (2023). The Role of Selenium in Atherosclerosis Development, Progression, Prevention and Treatment. Biomedicines, 11(7), 2010. https://doi.org/10.3390/biomedicines11072010








