Differences in and Prognostic Value of Quality of Life Data in Rectal Cancer Patients with and without Distant Metastases
Abstract
1. Introduction
2. Materials and Methods
2.1. Patients
2.2. Treatment
2.3. Quality of Life
2.4. Statistics
2.5. Survival Analysis
3. Results
3.1. Baseline Characteristics
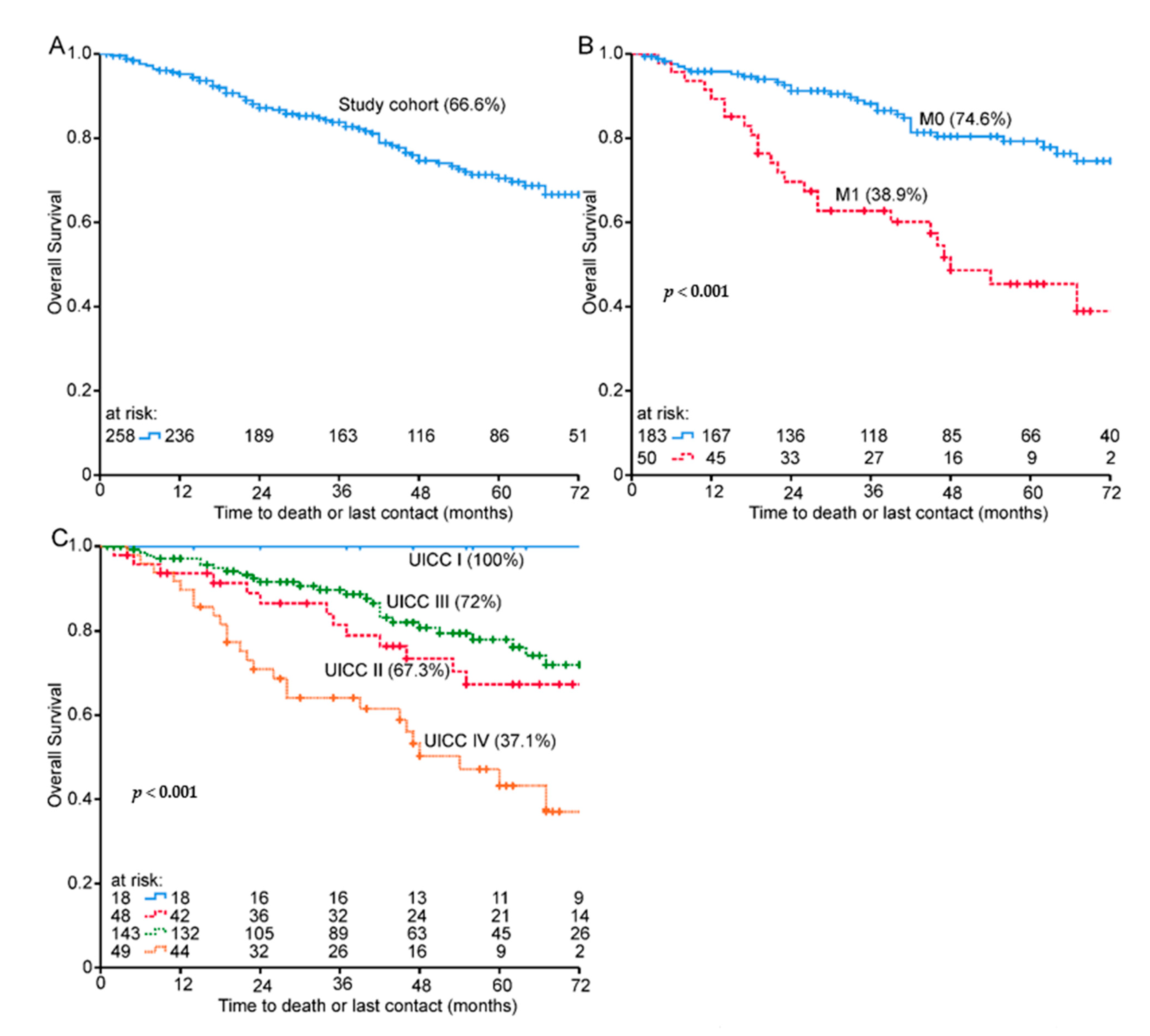
3.2. Patients Suffering from Metastases
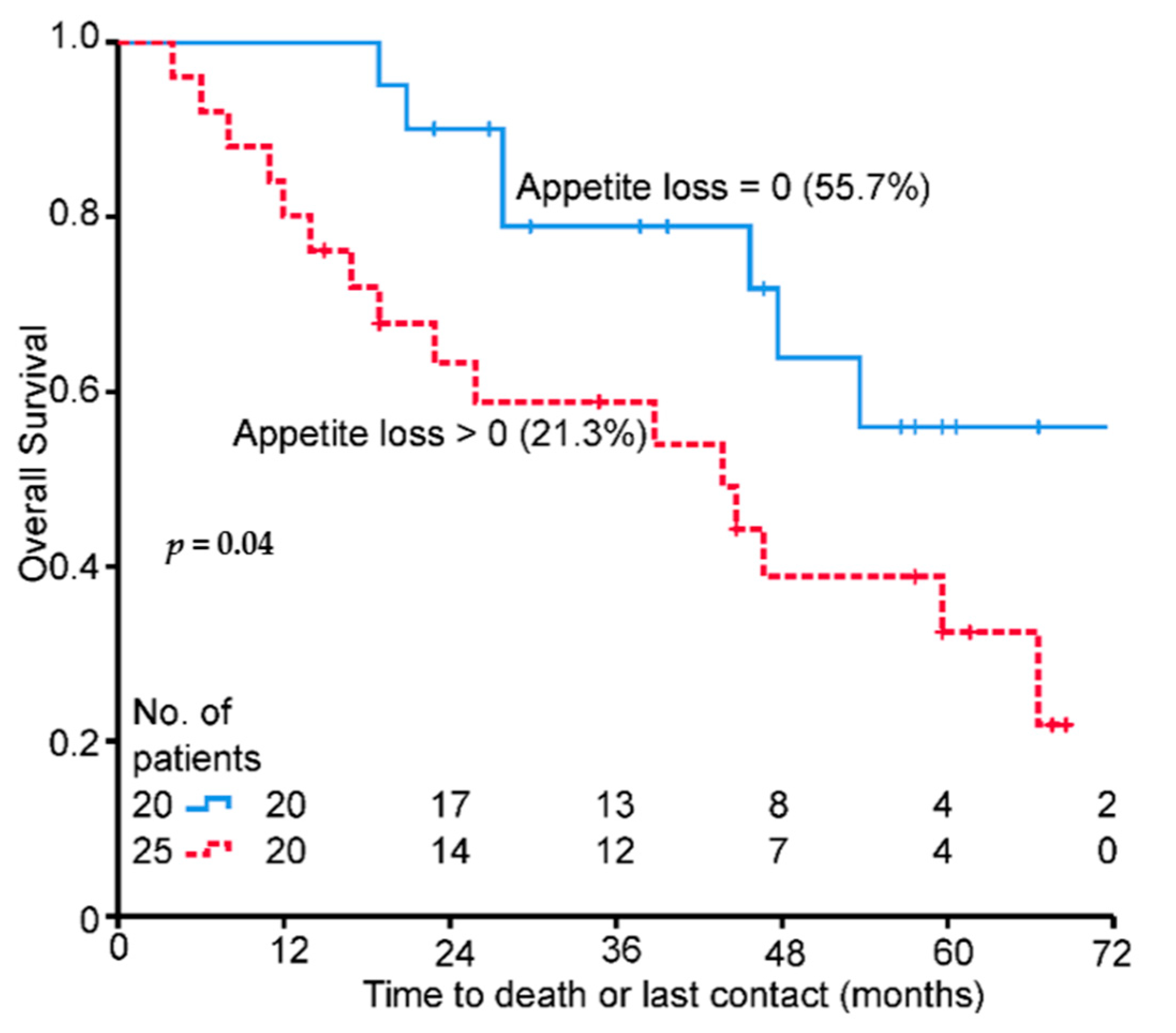
3.3. Prognostic Value of Baseline EORTC QLQ C30 and CR38 Data in the Whole Cohort
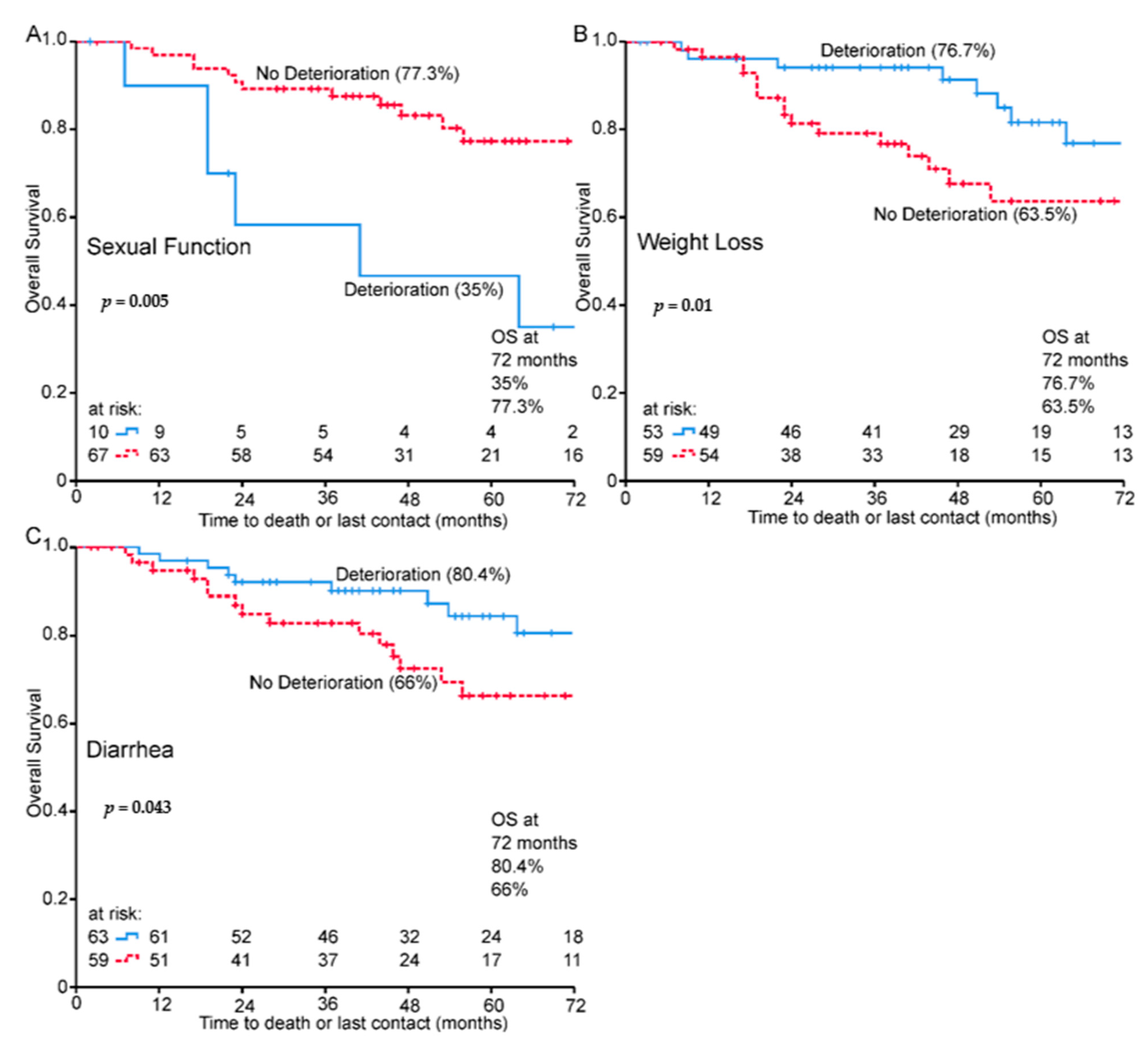
3.4. Prognostic Value of Change EORTC QLQ C30 and CR38 Data in the Whole Cohort
4. Discussion
4.1. Strengths and Weaknesses
4.2. Comparability
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Disclosure
Abbreviations
| PROs | patient reported outcomes |
| HRQoL | health related quality of life |
| QoL | quality of life |
| OS | overall survival |
| EORTC | European organization for research and treatment of cancer |
| QLQ | quality of life questionnaire |
References
- Byrne, C.; Griffin, A.; Blazeby, J.; Conroy, T.; Efficace, F. Health-related quality of life as a valid outcome in the treatment of advanced colorectal cancer. Eur. J. Surg. Oncol. 2007, 33 (Suppl. 2), S95–S104. [Google Scholar] [CrossRef] [PubMed]
- Haussmann, J.; Nestle-Kraemling, C.; Bolke, E.; Wollandt, S.; Speer, V.; Djiepmo Njanang, F.J.; Tamaskovics, B.; Gerber, P.A.; Orth, K.; Ruckhaeberle, E.; et al. Long-term quality of life after preoperative radiochemotherapy in patients with localized and locally advanced breast cancer. Strahlenther. Onkol. 2020, 196, 386–397. [Google Scholar] [CrossRef]
- Steinmann, D.; Vordermark, D.; Gerstenberg, W.; Aschoff, R.; Gharbi, N.; Muller, A.; Schafer, C.; Theodorou, M.; Wypior, H.J.; Geinitz, H.; et al. Quality of life in patients with limited (1–3) brain metastases undergoing stereotactic or whole brain radiotherapy: A prospective study of the degro qol working group. Strahlenther. Onkol. 2020, 196, 48–57. [Google Scholar] [CrossRef] [PubMed]
- Maisey, N.R.; Norman, A.; Watson, M.; Allen, M.J.; Hill, M.E.; Cunningham, D. Baseline quality of life predicts survival in patients with advanced colorectal cancer. Eur. J. Cancer 2002, 38, 1351–1357. [Google Scholar] [CrossRef]
- Efficace, F.; Bottomley, A.; Coens, C.; Van Steen, K.; Conroy, T.; Schoffski, P.; Schmoll, H.; Van Cutsem, E.; Kohne, C.H. Does a patient’s self-reported health-related quality of life predict survival beyond key biomedical data in advanced colorectal cancer? Eur. J. Cancer 2006, 42, 42–49. [Google Scholar] [CrossRef]
- Jörling, M.; Rutzner, S.; Hecht, M.; Fietkau, R.; Distel, L. Deterioration of health-related quality of life scores under treatment predicts longer survival. BioMed Res. Int. 2020, 2020, 1–10. [Google Scholar] [CrossRef]
- Bonnetain, F.; Borg, C.; Adams, R.R.; Ajani, J.A.; Benson, A.; Bleiberg, H.; Chibaudel, B.; Diaz-Rubio, E.; Douillard, J.Y.; Fuchs, C.S.; et al. How health-related quality of life assessment should be used in advanced colorectal cancer clinical trials. Ann. Oncol. 2017, 28, 2077–2085. [Google Scholar] [CrossRef]
- Gotay, C.C.; Kawamoto, C.T.; Bottomley, A.; Efficace, F. The prognostic significance of patient-reported outcomes in cancer clinical trials. J. Clin. Oncol. 2008, 26, 1355–1363. [Google Scholar] [CrossRef]
- Grande, G.E.; Farquhar, M.C.; Barclay, S.I.; Todd, C.J. Quality of life measures (eortc qlq-c30 and sf-36) as predictors of survival in palliative colorectal and lung cancer patients. Palliat. Support. Care 2009, 7, 289–297. [Google Scholar] [CrossRef]
- Wong, C.K.; Law, W.L.; Wan, Y.F.; Poon, J.T.; Lam, C.L. Health-related quality of life and risk of colorectal cancer recurrence and all-cause death among advanced stages of colorectal cancer 1-year after diagnosis. BMC Cancer 2014, 14, 337. [Google Scholar] [CrossRef]
- Fournier, E.; Jooste, V.; Woronoff, A.S.; Quipourt, V.; Bouvier, A.M.; Mercier, M. Health-related quality of life is a prognostic factor for survival in older patients after colorectal cancer diagnosis: A population-based study. Dig. Liver Dis. 2016, 48, 87–93. [Google Scholar] [CrossRef] [PubMed]
- Osthus, A.A.; Aarstad, A.K.; Olofsson, J.; Aarstad, H.J. Health-related quality of life scores in long-term head and neck cancer survivors predict subsequent survival: A prospective cohort study. Clin. Otolaryngol. 2011, 36, 361–368. [Google Scholar] [CrossRef] [PubMed]
- Coates, A.S.; Hurny, C.; Peterson, H.F.; Bernhard, J.; Castiglione-Gertsch, M.; Gelber, R.D.; Goldhirsch, A. Quality-of-life scores predict outcome in metastatic but not early breast cancer. International breast cancer study group. J. Clin. Oncol. 2000, 18, 3768–3774. [Google Scholar] [CrossRef] [PubMed]
- Efficace, F.; Biganzoli, L.; Piccart, M.; Coens, C.; Van Steen, K.; Cufer, T.; Coleman, R.E.; Calvert, H.A.; Gamucci, T.; Twelves, C.; et al. Baseline health-related quality-of-life data as prognostic factors in a phase iii multicentre study of women with metastatic breast cancer. Eur. J. Cancer 2004, 40, 1021–1030. [Google Scholar] [CrossRef]
- Lee, C.K.; Stockler, M.R.; Coates, A.S.; Gebski, V.; Lord, S.J.; Simes, R.J.; Australian New Zealand Breast Cancer Trials, G. Self-reported health-related quality of life is an independent predictor of chemotherapy treatment benefit and toxicity in women with advanced breast cancer. Br. J. Cancer 2010, 102, 1341–1347. [Google Scholar] [CrossRef] [PubMed]
- Haraldseide, L.M.; Jakola, A.S.; Solheim, O.; Sagberg, L.M. Does preoperative health-related quality of life predict survival in high-grade glioma patients?—A prospective study. Br. J. Neurosurg. 2019, 34, 28–34. [Google Scholar] [CrossRef]
- Sauer, R.; Becker, H.; Hohenberger, W.; Rodel, C.; Wittekind, C.; Fietkau, R.; Martus, P.; Tschmelitsch, J.; Hager, E.; Hess, C.F.; et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N. Engl. J. Med. 2004, 351, 1731–1740. [Google Scholar] [CrossRef]
- Li, Y.; Wang, J.; Ma, X.; Tan, L.; Yan, Y.; Xue, C.; Hui, B.; Liu, R.; Ma, H.; Ren, J. A review of neoadjuvant chemoradiotherapy for locally advanced rectal cancer. Int. J. Biol. Sci. 2016, 12, 1022–1031. [Google Scholar] [CrossRef]
- van der Geest, L.G.; Lam-Boer, J.; Koopman, M.; Verhoef, C.; Elferink, M.A.; de Wilt, J.H. Nationwide trends in incidence, treatment and survival of colorectal cancer patients with synchronous metastases. Clin. Exp. Metastasis 2015, 32, 457–465. [Google Scholar] [CrossRef]
- Folprecht, G.; Grothey, A.; Alberts, S.; Raab, H.R.; Kohne, C.H. Neoadjuvant treatment of unresectable colorectal liver metastases: Correlation between tumour response and resection rates. Ann. Oncol. 2005, 16, 1311–1319. [Google Scholar] [CrossRef]
- Field, K.; Lipton, L. Metastatic colorectal cancer-past, progress and future. World J. Gastroenterol. 2007, 13, 3806–3815. [Google Scholar] [CrossRef] [PubMed]
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2015. CA Cancer J. Clin. 2015, 65, 5–29. [Google Scholar] [CrossRef] [PubMed]
- Aaronson, N.K.; Ahmedzai, S.; Bergman, B.; Bullinger, M.; Cull, A.; Duez, N.J.; Filiberti, A.; Flechtner, H.; Fleishman, S.B.; de Haes, J.C.; et al. The european organization for research and treatment of cancer qlq-c30: A quality-of-life instrument for use in international clinical trials in oncology. J. Natl. Cancer Inst. 1993, 85, 365–376. [Google Scholar] [CrossRef]
- Sprangers, M.A.; te Velde, A.; Aaronson, N.K. The construction and testing of the eortc colorectal cancer-specific quality of life questionnaire module (qlq-cr38). European organization for research and treatment of cancer study group on quality of life. Eur. J. Cancer 1999, 35, 238–247. [Google Scholar] [CrossRef]
- Sternby Eilard, M.; Hagstrom, H.; Mortensen, K.E.; Wilsgaard, T.; Vagnildhaug, O.M.; Dajani, O.; Stal, P.; Rizell, M. Quality of life as a prognostic factor for survival in hepatocellular carcinoma. Liver Int. 2017, 38, 885–894. [Google Scholar] [CrossRef]
- Krebs in Deutschland Für 2015/2016, 12th ed.; Robert Koch-Institut (Hrsg) und Die Gesellschaft der Epidemiologischen Krebsregister in Deutschland e.V. Publisher: Berlin, Germany, 2019.
- Hamer, J.; McDonald, R.; Zhang, L.; Verma, S.; Leahey, A.; Ecclestone, C.; Bedard, G.; Pulenzas, N.; Bhatia, A.; Chow, R.; et al. Quality of life (qol) and symptom burden (sb) in patients with breast cancer. Support. Care Cancer 2017, 25, 409–419. [Google Scholar] [CrossRef] [PubMed]
- Picozzi, V.; Narayanan, S.; Henry Hu, X.; Vacirca, J. Health-related quality of life in patients with metastatic pancreatic cancer. J. Gastrointest. Cancer 2017, 48, 103–109. [Google Scholar] [CrossRef]
- Williams, K.; Jackson, S.E.; Beeken, R.J.; Steptoe, A.; Wardle, J. The impact of a cancer diagnosis on health and well-being: A prospective, population-based study. Psychooncology 2016, 25, 626–632. [Google Scholar] [CrossRef]
- Vickers, M.M.; Lee, C.; Tu, D.; Wheatley-Price, P.; Parulekar, W.; Brundage, M.D.; Moore, M.J.; Au, H.; O’Callaghan, C.J.; Jonker, D.J.; et al. Significance of baseline and change in quality of life scores in predicting clinical outcomes in an international phase iii trial of advanced pancreatic cancer: Ncic ctg pa.3. Pancreatology 2016, 16, 1106–1112. [Google Scholar] [CrossRef]
- Brierley, J.; Gospodarowicz, M.K.; Wittekind, C. Tnm Classification of Malignant Tumours, 8th ed.; John Wiley & Sons, Inc.: Chichester, UK; Hoboken, NJ, USA, 2017. [Google Scholar]
- Alberts, S.R. Update on the optimal management of patients with colorectal liver metastases. Crit. Rev. Oncol. Hematol. 2012, 84, 59–70. [Google Scholar] [CrossRef]
- Efficace, F.; Innominato, P.F.; Bjarnason, G.; Coens, C.; Humblet, Y.; Tumolo, S.; Genet, D.; Tampellini, M.; Bottomley, A.; Garufi, C.; et al. Validation of patient’s self-reported social functioning as an independent prognostic factor for survival in metastatic colorectal cancer patients: Results of an international study by the chronotherapy group of the european organisation for research and treatment of cancer. J. Clin. Oncol. 2008, 26, 2020–2026. [Google Scholar] [PubMed]
- Braun, D.P.; Gupta, D.; Grutsch, J.F.; Staren, E.D. Can changes in health related quality of life scores predict survival in stages iii and iv colorectal cancer? Health Qual. Life Outcomes 2011, 9, 62. [Google Scholar] [CrossRef]
- Osthus, A.A.; Aarstad, A.K.; Olofsson, J.; Aarstad, H.J. Prediction of survival by pretreatment health-related quality-of-life scores in a prospective cohort of patients with head and neck squamous cell carcinoma. JAMA Otolaryngol. Head Neck Surg. 2013, 139, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Efficace, F.; Bottomley, A.; Smit, E.F.; Lianes, P.; Legrand, C.; Debruyne, C.; Schramel, F.; Smit, H.J.; Gaafar, R.; Biesma, B.; et al. Is a patient’s self-reported health-related quality of life a prognostic factor for survival in non-small-cell lung cancer patients? A multivariate analysis of prognostic factors of eortc study 08975. Ann. Oncol. 2006, 17, 1698–1704. [Google Scholar] [CrossRef] [PubMed]
- Camilleri-Brennan, J.; Steele, R.J. Prospective analysis of quality of life and survival following mesorectal excision for rectal cancer. Br. J. Surg. 2001, 88, 1617–1622. [Google Scholar] [CrossRef] [PubMed]
- Coates, A.; Porzsolt, F.; Osoba, D. Quality of life in oncology practice: Prognostic value of eortc qlq-c30 scores in patients with advanced malignancy. Eur. J. Cancer 1997, 33, 1025–1030. [Google Scholar] [CrossRef]
- Quinten, C.; Martinelli, F.; Coens, C.; Sprangers, M.A.; Ringash, J.; Gotay, C.; Bjordal, K.; Greimel, E.; Reeve, B.B.; Maringwa, J.; et al. A global analysis of multitrial data investigating quality of life and symptoms as prognostic factors for survival in different tumor sites. Cancer 2014, 120, 302–311. [Google Scholar] [CrossRef]
- Osoba, D. Health-related quality of life and cancer clinical trials. Ther. Adv. Med. Oncol. 2011, 3, 57–71. [Google Scholar] [CrossRef]


| Risk Factor | Total No. | No. (%) |
|---|---|---|
| Age (years) 1 | 258 | 67.4 (11.6) |
| Gender | 258 | |
| Male | 191 (74) | |
| Female | 67 (26) | |
| Status | 258 | |
| Alive | 184 (71.3) | |
| UICC | 258 | |
| I | 21 (8.1) | |
| II | 49 (19) | |
| III | 141 (54.7) | |
| IV | 47 (18.2) | |
| TNM: cT | 258 | |
| 1 | 6 (2.3) | |
| 2 | 30 (11.6) | |
| 3 | 162 (62.8) | |
| 4 | 60 (23.3) | |
| TNM: cN | 255 | |
| X | 3 (1.2) | |
| 0 | 70 (27.1) | |
| 1 | 135 (52.3) | |
| 2 | 50 (19.4) | |
| TNM: cM | 233 | |
| X | 25 (9.7) | |
| 0 | 183 (70.9) | |
| 1 | 50 (19.4) | |
| TNM: pL | 214 | |
| X | 44 (17.1) | |
| 0 | 172 (66.7) | |
| 1 | 42 (16.3) | |
| TNM: pV | 212 | |
| X | 46 (17.8) | |
| 0 | 202 (78.3) | |
| 1 | 10 (3.9) |
| Risk Factor 1 | p-Value (2-Tailed) | Mean Difference | 95% CI | Cohen’s d |
|---|---|---|---|---|
| Baseline | ||||
| Physical function | 0.036 | 7.78 | 0.51–15.05 | 0.286 |
| Appetite loss | 0.008 | −15.35 | −26.62–4.09 | 0.716 |
| Chemotherapy Side Effects | 0.015 | −4.66 | −8.37–0.95 | 0.657 |
| change | ||||
| Weight loss | 0.008 | 18.33 | 4.91–31.75 | 0.797 |
| Univariate | Multivariate | ||||
|---|---|---|---|---|---|
| Risk Factor 1 | Deterioration | HR (95% CI) | p-Value | HR (95% CI) | p-Value |
| Baseline2 | |||||
| Physical function | 0.70 (0.49–1.01) | 0.055 | |||
| Appetite loss | 1.30 (1.01–1.66) | 0.043 | 1.30 (1.01–1.66) | 0.043 | |
| Chemotherapy side effects | 1.15 (0.51–2.60) | 0.739 | |||
| Change | |||||
| Weight loss | No Yes | 2.67 (0.46, 15.28) | 0.272 |
| Univariate | Multivariate | ||||
|---|---|---|---|---|---|
| Risk Factor 1 | Mean (SD) | HR (95% CI) | p-Value | HR (95% CI) | p-Value |
| Gender QLQ C30 | 1.19 (0.91–1.56) | 0.208 | 1.46 (1.07–2.01) | 0.011 | |
| Physical function | 79.67 (22.30) | 0.70 (0.59-0.84) | <0.001 | 0.71 (0.57-0.88) | 0.002 |
| Role function | 69.26 (30.33) | 0.83 (0.71–0.97) | 0.02 | 1.13 (0.86–1.48) | 0.375 |
| Emotional function | 64.02 (25.95) | 0.96 (0.79–1.16) | 0.669 | ||
| Cognitive function | 84.30 (21.71) | 0.84 (0.67–1.06) | 0.15 | ||
| Social function | 66.32 (30.38) | 1.02 (0.85–1.21) | 0.863 | ||
| Global health | 58.95 (22.30) | 0.89 (0.73–1.09) | 0.248 | ||
| Fatigue | 36.29 (27.74) | 1.32 (1.10–1.58) | 0.003 | 0.84 (0.58–1.21) | 0.351 |
| Nausea and vomiting | 6.30 (15.61) | 1.36 (1.04–1.76) | 0.024 | 1.07 (0.73–1.58) | 0.732 |
| Pain | 24.79 (29.37) | 1.26 (1.07–1.50) | 0.004 | 1.11 (0.89–1.39) | 0.369 |
| Dyspnea | 18.67 (27.33) | 1.24 (1.03–1.50) | 0.021 | 1.23 (0.99–1.53) | 0.068 |
| Insomnia | 33.61 (33.20) | 1.12 (0.95–1.32) | 0.194 | ||
| Appetite loss | 19.08 (28.79) | 1.34 (1.14–1.58) | <0.001 | 1.18 (0.93–1.50) | 0.171 |
| Constipation | 14.70 (28.29) | 0.86 (0.68–1.10) | 0.225 | ||
| Diarrhea | 34.45 (36.01) | 1.15 (0.97–1.34) | 0.078 | ||
| Financial difficulties | 21.52 (31.61) | 0.99 (0.82–1.20) | 0.944 | ||
| QLQ CR38 | |||||
| Body Image | 77.81 (25.78) | 0.85 (0.69–1.05) | 0.125 | ||
| Sexual function | 71.72 (29.36) | 1.11 (0.88–1.41) | 0.369 | ||
| Future prospects | 34.18 (33.75) | 1.01 (0.85–1.18) | 0.949 | ||
| Micturition problems | 15.75 (10.86) | 1.33 (0.83–2.13) | 0.241 | ||
| Chemotherapy side effects | 7.61 (9.52) | 1.48 (0.79–2.79) | 0.221 | ||
| Gastrointestinal problems | 10.93 (9.55) | 0.90 (0.44–1.82) | 0.769 | ||
| Male sexual problems 2 | 18.77 (19.31) | 1.60 (1.07–2.40) | 0.021 | ||
| Defecation problems | 16.13 (10.83) | 0.85 (0.48–1.51) | 0.583 | ||
| Weight loss | 21.48 (29.85) | 1.22 (1.02–1.47) | 0.033 | 1.04 (0.81–1.34) | 0.756 |
| Univariate | Multivariate | ||||
|---|---|---|---|---|---|
| Risk Factor 1 | Deterioration | HR (95% CI) | p-Value | HR (95% CI) | p-Value |
| QLQ C30 | |||||
| Physical function | No Yes | 1.09 (0.33–3.64) | 0.883 | ||
| Role function | No Yes | 0.78 (0.23–2.60) | 0.682 | ||
| Emotional function | No Yes | 0.95 (0.40–2.23) | 0.902 | ||
| Cognitive function | No Yes | 0.54 (0.22–1.34) | 0.185 | ||
| Social function | No Yes | 0.61 (0.27–1.40) | 0.246 | ||
| Global health | No Yes | 1.40 (0.66–2.97) | 0.376 | ||
| Fatigue | No Yes | 0.52 (0.24–1.11) | 0.09 | ||
| Nausea and vomiting | No Yes | 0.90 (0.39–2.08) | 0.801 | ||
| Pain | No Yes | 0.82 (0.38–1.73) | 0.593 | ||
| Dyspnea | No Yes | 0.64 (0.25–1.64) | 0.35 | ||
| Insomnia | No Yes | 0.93 (0.43–2.02) | 0.857 | ||
| Appetite loss | No Yes | 0.53 (0.24–1.17) | 0.115 | ||
| Constipation | No Yes | 1.85 (0.81–4.21) | 0.144 | ||
| Diarrhea | No Yes | 0.44 (0.20–0.98) | 0.044 | 0.34 (0.13–0.93) | 0.035 |
| Financial difficulties | No Yes | 1.50 (0.69–3.29) | 0.309 | ||
| QLQ CR38 | |||||
| Body Image | No Yes | 0.56 (0.26–1.19) | 0.13 | ||
| Sexual function | No Yes | 3.60 (1.36–9.57) | 0.01 | 4.05 (1.47–11.11) | 0.007 |
| Future prospects | No Yes | 0.60 (0.18–2.02) | 0.41 | ||
| Micturition problems | No Yes | 1.04 (0.48–2.26) | 0.923 | ||
| Chemo side effects | No Yes | 0.83 (0.39–1.80) | 0.642 | ||
| Gastrointestinal problems | No Yes | 0.56 (0.26–1.20) | 0.133 | ||
| Male sexual problems1 | No Yes | 0.82 (0.27–2.52) | 0.733 | ||
| Defecation problems | No Yes | 1.84 (0.57–5.88) | 0.307 | ||
| Weight loss | No Yes | 0.33 (0.14–0.77) | 0.01 | 0.32 (0.10–0.97) | 0.044 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Frank, F.; Hecht, M.; Loy, F.; Rutzner, S.; Fietkau, R.; Distel, L. Differences in and Prognostic Value of Quality of Life Data in Rectal Cancer Patients with and without Distant Metastases. Healthcare 2021, 9, 1. https://doi.org/10.3390/healthcare9010001
Frank F, Hecht M, Loy F, Rutzner S, Fietkau R, Distel L. Differences in and Prognostic Value of Quality of Life Data in Rectal Cancer Patients with and without Distant Metastases. Healthcare. 2021; 9(1):1. https://doi.org/10.3390/healthcare9010001
Chicago/Turabian StyleFrank, Fabian, Markus Hecht, Florian Loy, Sandra Rutzner, Rainer Fietkau, and Luitpold Distel. 2021. "Differences in and Prognostic Value of Quality of Life Data in Rectal Cancer Patients with and without Distant Metastases" Healthcare 9, no. 1: 1. https://doi.org/10.3390/healthcare9010001
APA StyleFrank, F., Hecht, M., Loy, F., Rutzner, S., Fietkau, R., & Distel, L. (2021). Differences in and Prognostic Value of Quality of Life Data in Rectal Cancer Patients with and without Distant Metastases. Healthcare, 9(1), 1. https://doi.org/10.3390/healthcare9010001







