Lyme Disease Patient Outcomes and Experiences; A Retrospective Cohort Study
Abstract
1. Introduction
2. Materials and Methods
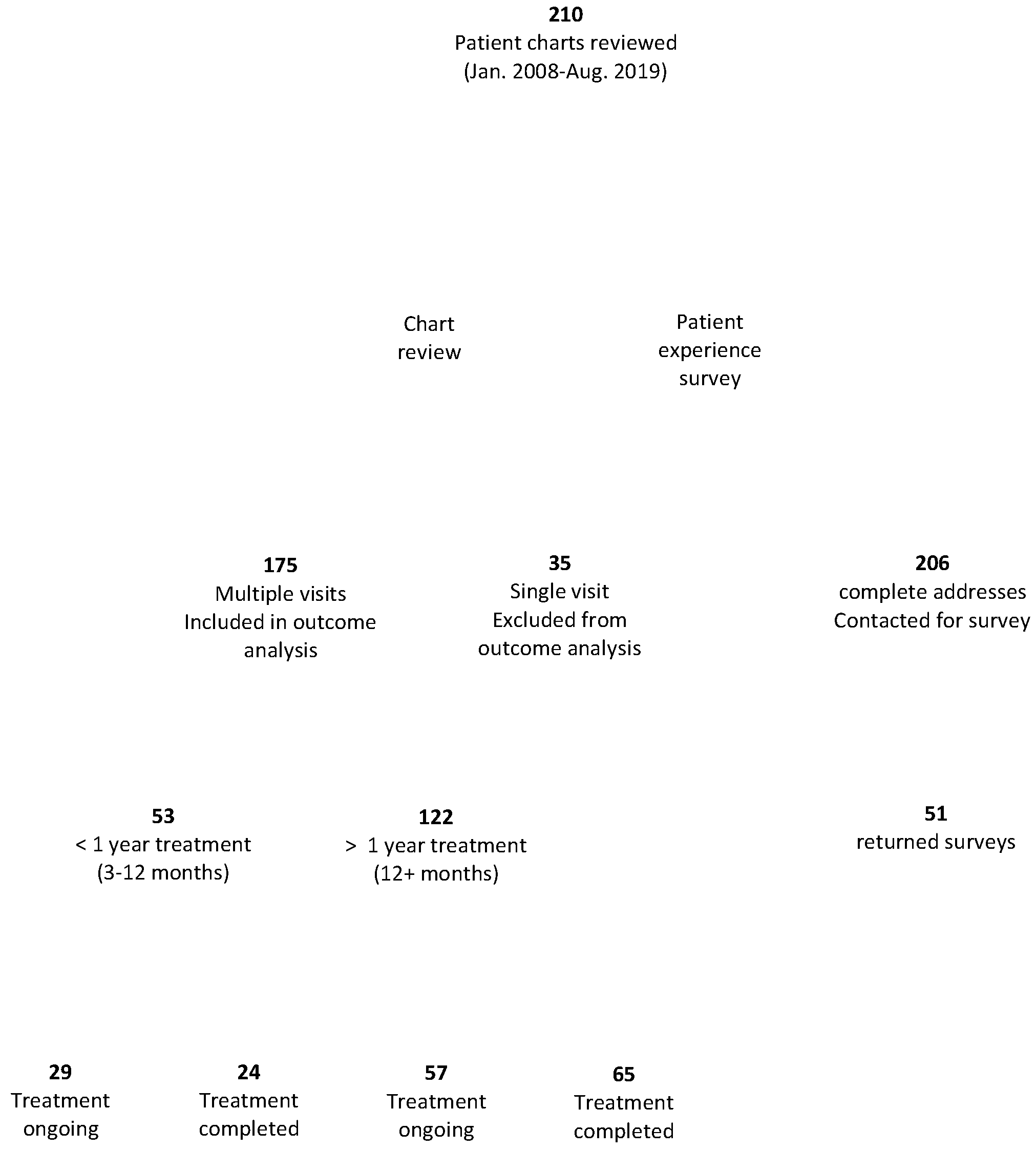
2.1. Participants and Setting
2.2. Study Design
- (a)
- Patients completed treatment in less than a year. This subset of patients had either two or three consultations at the clinic before ceasing visits. This group had no consultations at the clinic for at least one year prior to data collection.
- (b)
- Patients with ongoing treatment <1 year. This subset of patients had either two or three consultations at the clinic with their most recent consultation within one year prior to data collection.
- (c)
- Patients completed treatment >1 year. These patients were those who had had treatment regimens lasting more than 1 year but had no consultations at the clinic for at least one year prior to data collection.
- (d)
- Patients with ongoing treatment >1 year. This subset of patients was at the clinic for more than one year with their most recent consultation at the clinic within one year prior to data collection.
2.3. Statistical Analysis
3. Results
3.1. Patient Demographics
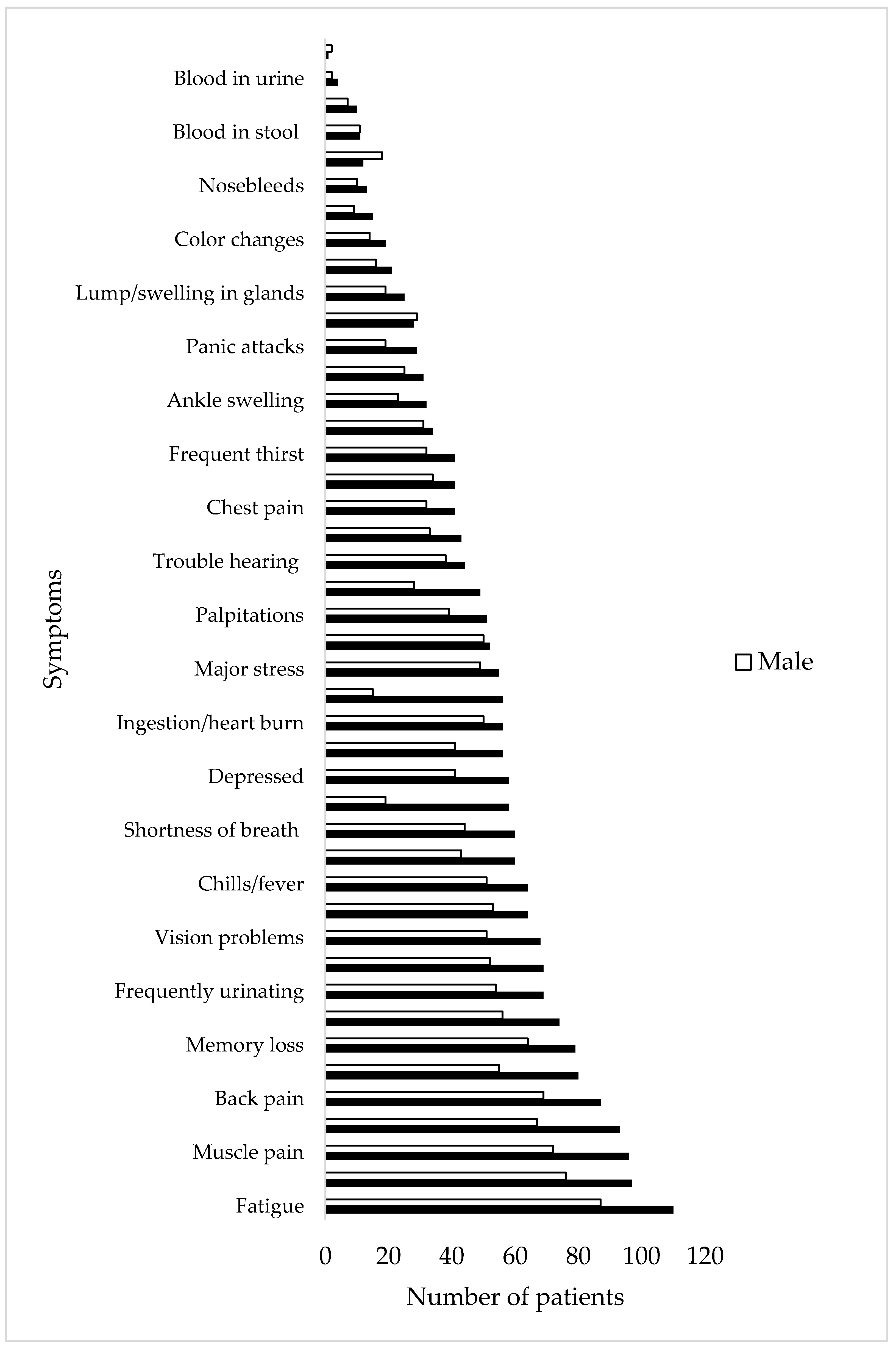
3.2. Symptoms Reported
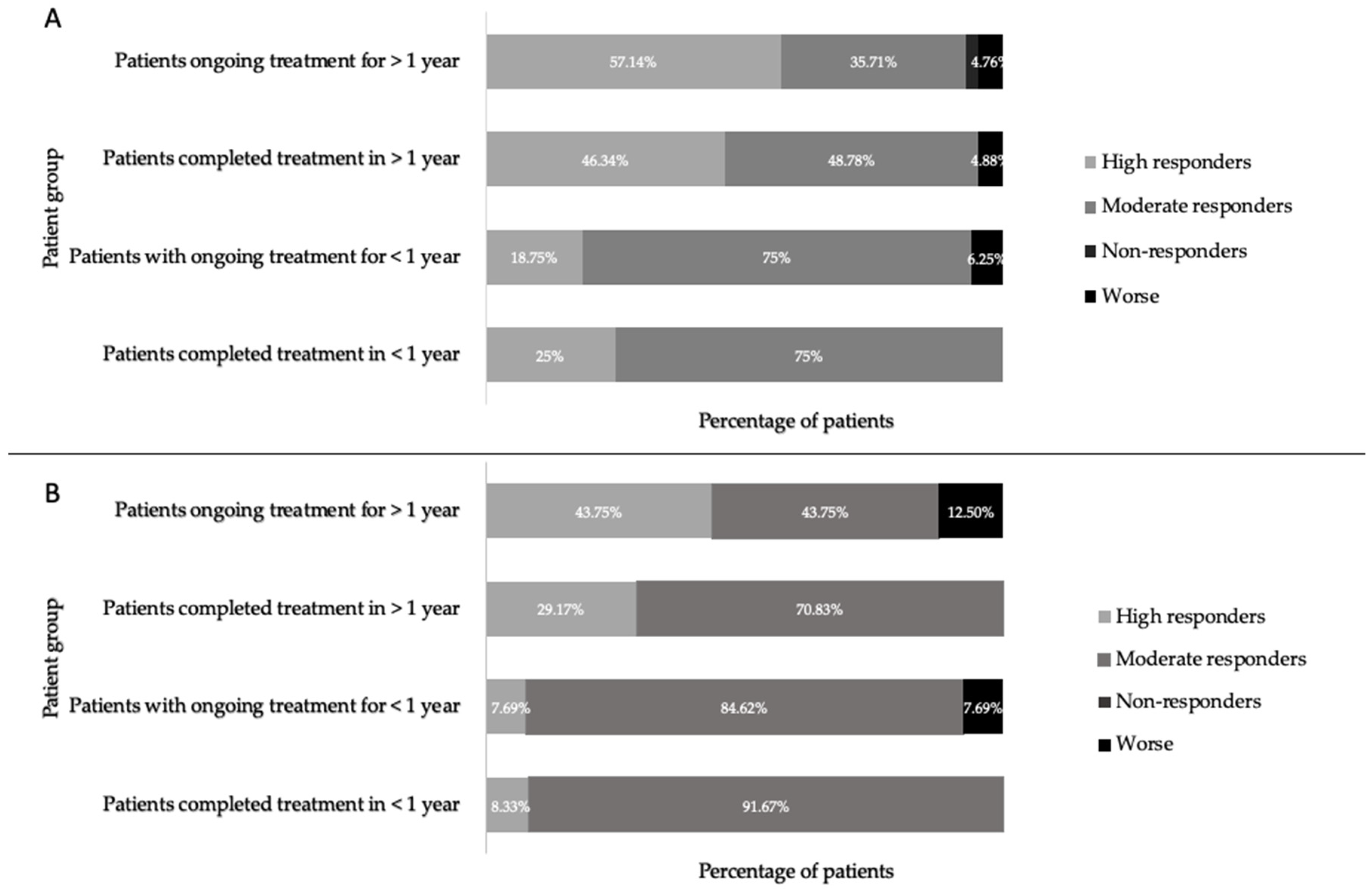
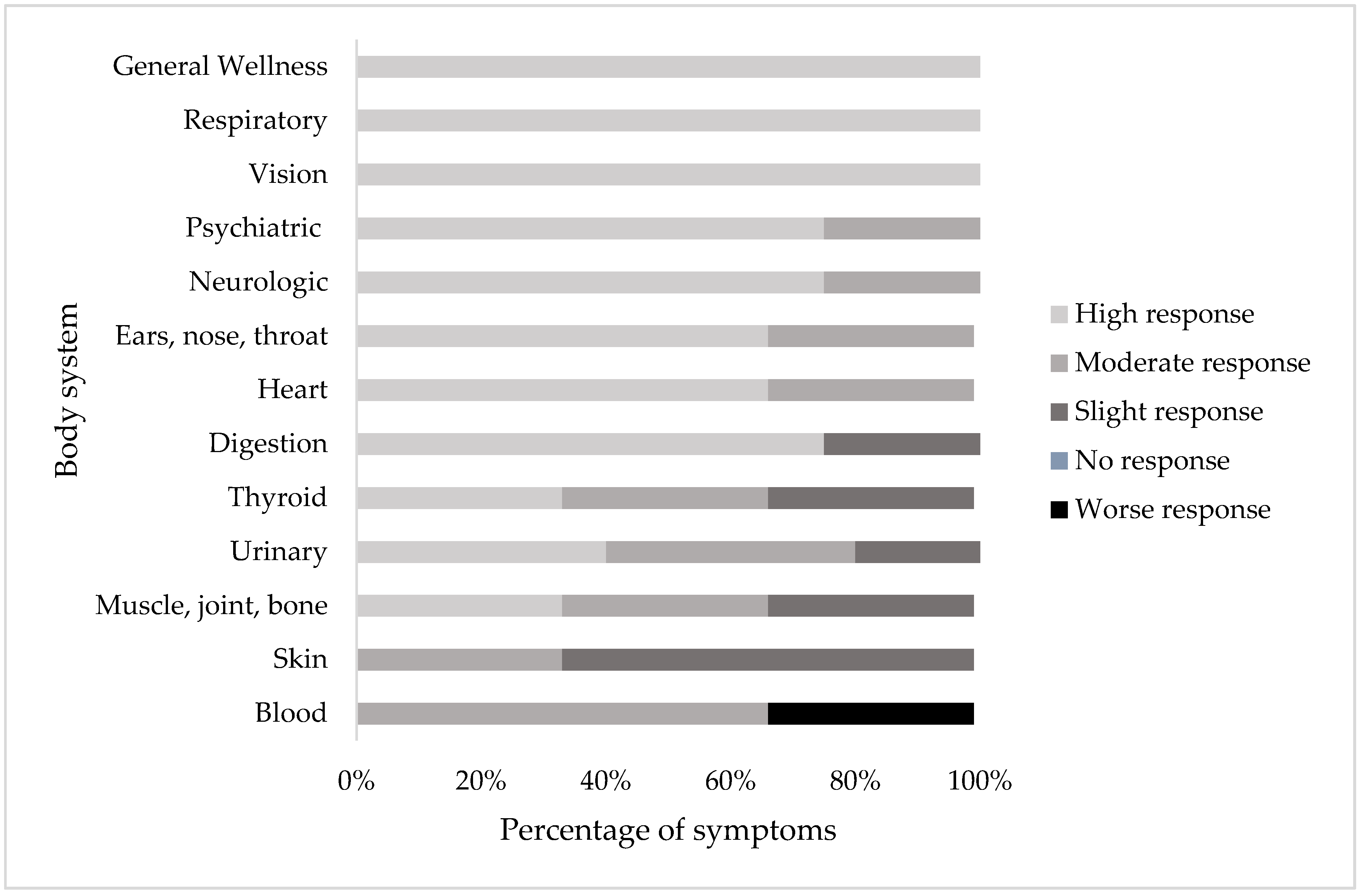
3.3. Determination of Patient Response to Treatment
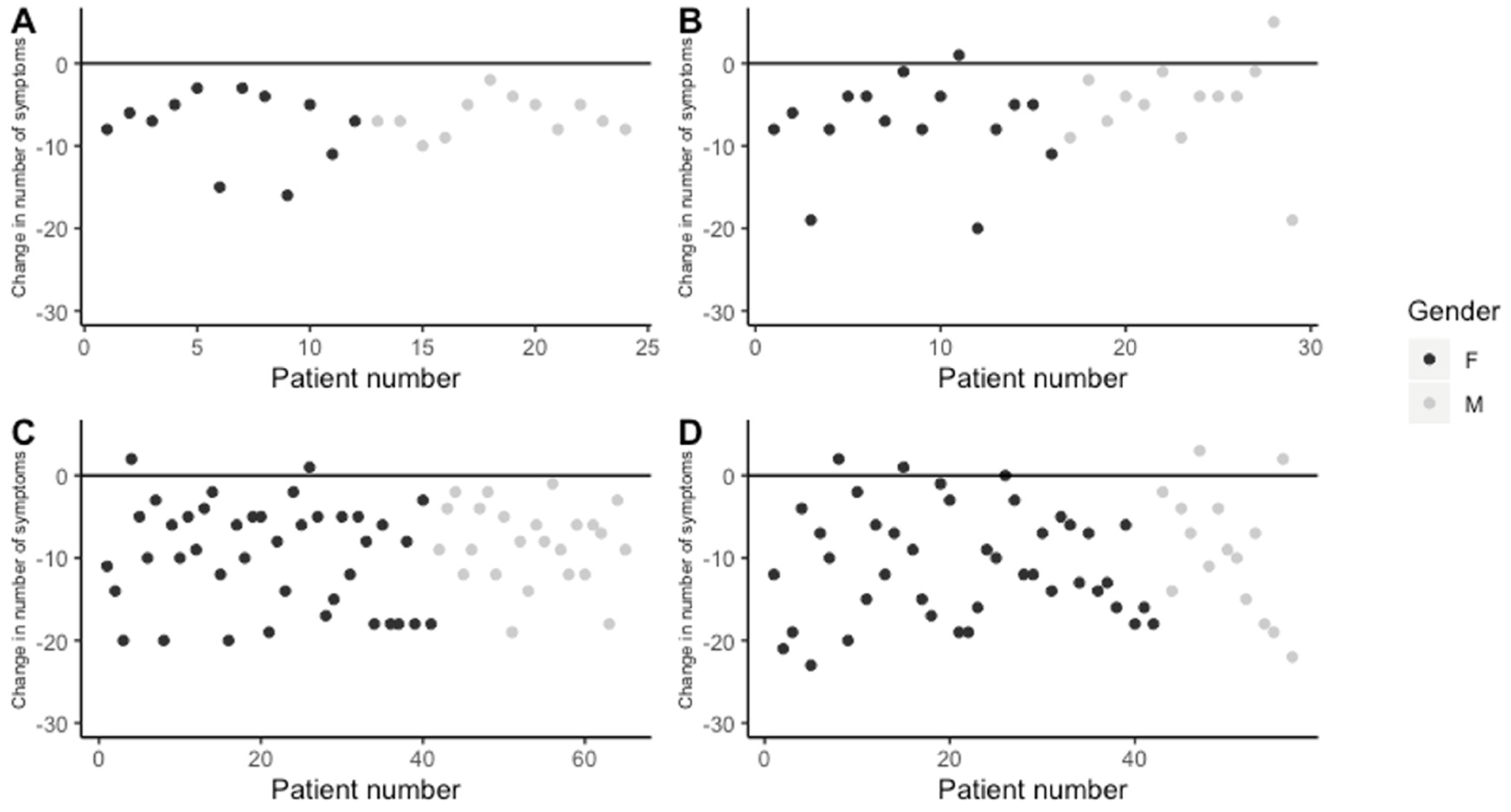
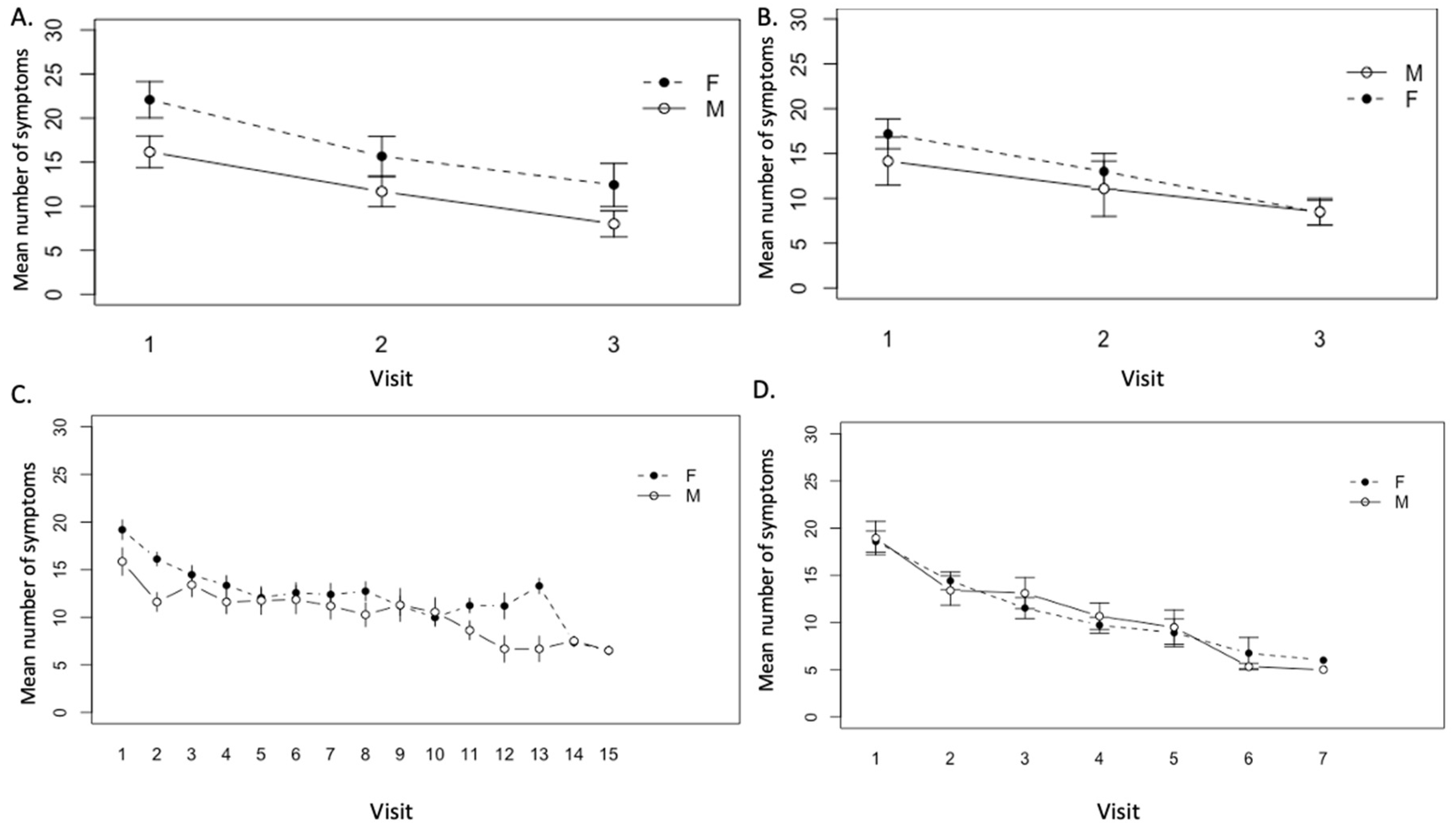
3.4. Determination of Average Change in Symptom Number over Time
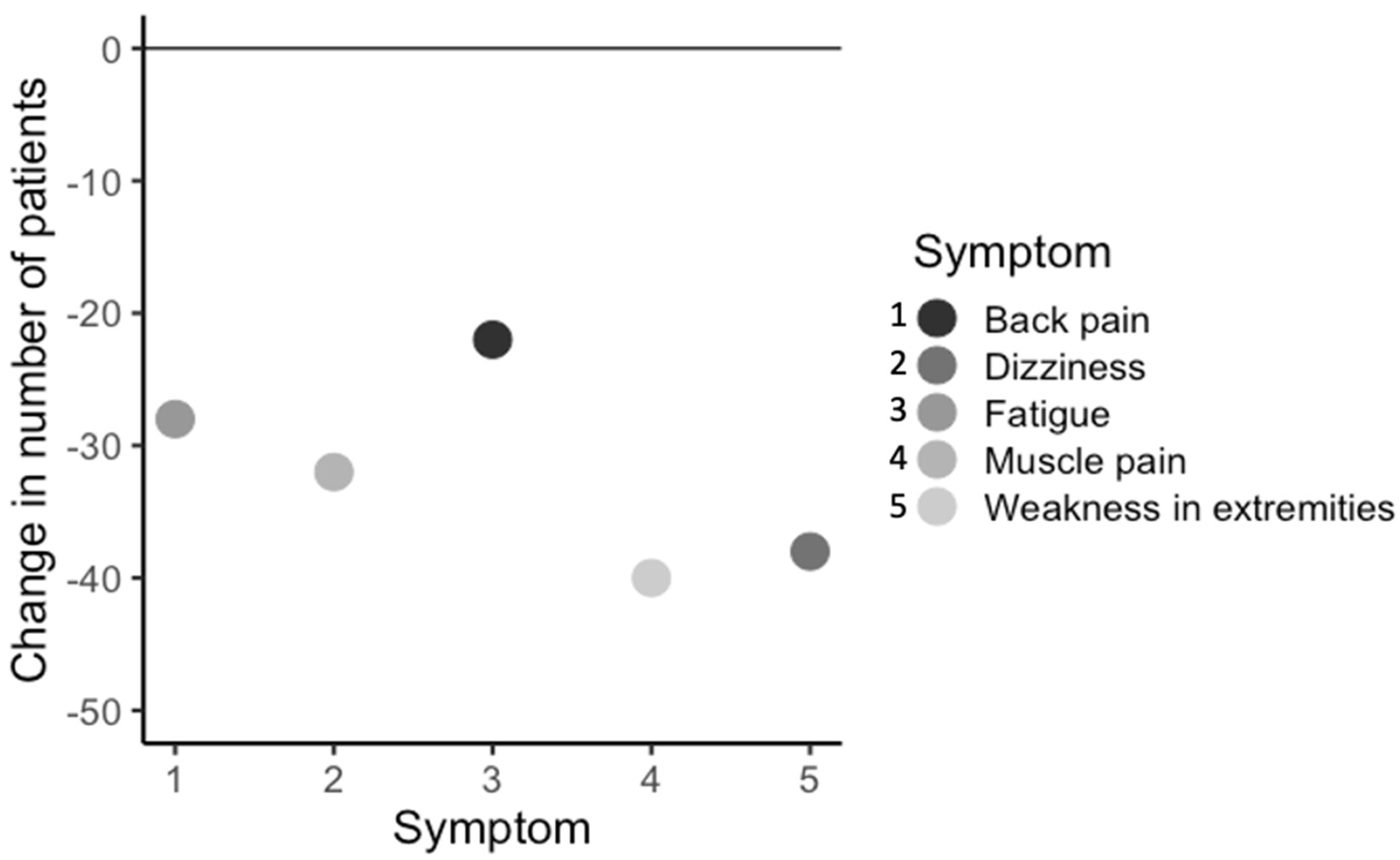
3.5. Effect of Treatment on Specific Symptoms
4. Discussion
4.1. Patients’ Response to Treatment
4.2. Gender-Based Differences in Presentation and Recovery
4.3. Response to Treatment at the Body Systems Level
4.4. Limitations of the Study
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Rudenko, N.; Golovchenko, M.; Grubhoffer, L.; Oliver, J.H. Updates on Borrelia burgdorferi sensu lato complex with respect to public health. Ticks Tick Borne Dis. 2011, 2, 123–128. [Google Scholar] [CrossRef]
- Sperling, J.L.H.; Sperling, F.A.H. Lyme borreliosis in Canada: Biological diversity and diagnostic complexity from an entomological perspective. Can. Entomol. 2009, 141, 521–549. [Google Scholar] [CrossRef]
- Tilly, K.; Rosa, P.A.; Stewart, P.E. Biology of Infection with Borrelia burgdorferi. Infect Dis. Clin. N. Am. 2008, 22, 217–234. [Google Scholar] [CrossRef] [PubMed]
- Stricker, R.B.; Middelveen, M.J. Sexual transmission of Lyme disease: Challenging the tickborne disease paradigm. Expert Rev. Anti-Infect. Ther. 2015, 13, 1303–1306. [Google Scholar] [CrossRef] [PubMed]
- Waddell, L.A.; Greig, J.; Lindsay, L.R.; Hinckley, A.F.; Ogden, N.H. A systematic review on the impact of gestational Lyme disease in humans on the fetus and newborn. PLoS ONE 2018, 43, 132–147. [Google Scholar] [CrossRef]
- Aoki, S.K.; Holland, P.V. Lyme disease—Another transfusion risk? Transfusion 1989, 29, 646–650. [Google Scholar] [CrossRef]
- Gasmi, S.; Ogden, N.; Lindsay, L.; Burns, S.; Fleming, S.; Badcock, J.; Hanan, S.; Gaulin, C.; Leblanc, M.; Russell, C.; et al. Surveillance for Lyme disease in Canada: 2009–2015. Can. Commun. Dis. Rep. 2017, 43, 194–199. [Google Scholar] [CrossRef] [PubMed]
- Public Health Agency of Canada—Surveillance of Lyme Disease. Available online: https://www.canada.ca/en/public-health/services/diseases/lyme-disease/surveillance-lyme-disease.html (accessed on 23 July 2020).
- Lloyd, V.K.; Hawkins, R.G. Under-detection of Lyme disease in Canada. Healthcare (Basel) 2018, 6, 25. [Google Scholar] [CrossRef]
- Cameron, D.J.; Johnson, L.B.; Maloney, E.L. Evidence assessments and guideline recommendations in Lyme disease: The clinical management of known tick bites, erythema migrans rashes and persistent disease. Expert Rev. Anti-Infect. Ther. 2014, 12, 1103–1135. [Google Scholar] [CrossRef]
- Steere, A.C.; Coburn, J.; Glickstein, L. The emergence of Lyme disease. J. Clin. Investig. 2004, 113, 1093–1101. [Google Scholar] [CrossRef]
- Asbrink, E.; Hovmark, A. Early and late cutaneous manifestations in Ixodes-born borreliosis (erythema migrans borreliosis, Lyme borreliosis). Ann. N. Y. Acad. Sci. 1988, 539, 4–15. [Google Scholar] [CrossRef] [PubMed]
- Dammin, G.J. Erythema migrans: A Chronicle. Rev. Infect Dis. 1989, 11, 142–151. [Google Scholar] [CrossRef] [PubMed]
- Boltri, J.M.; Hash, R.B.; Vogel, R.L. Patterns of Lyme disease diagnosis and treatment by family physicians in a southeastern state. J. Commun. Health 2002, 27, 395–402. [Google Scholar] [CrossRef] [PubMed]
- Steere, A.C. The clinical evolution of Lyme arthritis. Ann. Int. Med. 1987, 107, 725. [Google Scholar] [CrossRef] [PubMed]
- Johnson, L.; Shapiro, M.; Mankoff, J. Removing the mask of average treatment effects in chronic Lyme disease research using big data and subgroup analysis. Healthcare (Basel) 2018, 35, 124. [Google Scholar] [CrossRef]
- Cairns, V.; Godwin, J. Post-Lyme borreliosis syndrome: A meta-analysis of reported symptoms. Int. J. Epidemiol. 2005, 34, 1340–1345. [Google Scholar] [CrossRef]
- Rudenko, N.; Golovchenko, M.; Kybicova, K.; Vancova, M. Metamorphoses of Lyme disease spirochetes: Phenomenon of Borrelia persisters. Parasit. Vectors 2019, 34, 120–142. [Google Scholar] [CrossRef]
- Stricker, R. Counterpoint: Long-term antibiotic therapy improves persistent symptoms associated with Lyme disease. Clin. Infect. Dis. 2007, 45, 149–157. [Google Scholar] [CrossRef]
- Hodzic, E.; Imai, D.; Feng, S.; Barthold, S.W. Resurgence of persisting non-cultivable Borrelia burgdorferi following antibiotic treatment in mice. PLoS ONE 2014, 9, e86907. [Google Scholar] [CrossRef]
- Priem, S.; Burmester, G.R.; Kamradt, T.; Wolbart, K.; Rittig, M.G.; Krause, A. Detection of Borrelia burgdorferi by polymerase chain reaction in synovial membrane, but not in synovial fluid from patients with persisting Lyme arthritis after antibiotic therapy. Ann. Rheum. Dis. 1998, 57, 118–121. [Google Scholar] [CrossRef]
- Breier, F.; Khanakah, G.; Stanek, G.; Kunz, G.; Aberer, E.; Schmidt, B.; Tappeiner, G. Isolation and polymerase chain reaction typing of Borrelia afzelii from a skin lesion in a seronegative patient with generalized ulcerating bullous lichen sclerosus et atrophicus. Br. J. Dermatol. 2001, 144, 387–392. [Google Scholar] [CrossRef] [PubMed]
- Berglund, J.; Stjernberg, L.; Ornstein, K.; Tykesson-Joelsson, K.; Walter, H. 5-y Follow up study of patients with neuroborreliosis. Scand. J. Infect. Dis. 2002, 34, 421–425. [Google Scholar] [CrossRef] [PubMed]
- Asch, E.S.; Bujak, D.I.; Weiss, M.; Peterson, M.G.; Weinstein, A. Lyme disease: An infectious and postinfectious syndrome. J. Rheumatol. 1994, 21, 454–461. [Google Scholar] [PubMed]
- Middelveen, M.J.; Sapi, E.; Burke, J.; Filush, K.R.; Franco, A.; Fesler, M.C.; Stricker, R.B. Persistent Borrelia infection in patients with ongoing symptoms of Lyme disease. Healthcare (Basel) 2018, 84, 33. [Google Scholar] [CrossRef]
- Honegr, K.; Hulínská, D.; Beran, J.; Dostál, V.; Havlasová, J.; Cermáková, Z. Long term and repeated electron microscopy and PCR detection of Borrelia burgdorferi sensu lato after an antibiotic treatment. Cent. Eur. J. Public Health 2004, 12, 6–11. [Google Scholar]
- Marques, A.; Telford, S.R., 3rd; Turk, S.P.; Chung, E.; Williams, C.; Dardick, K.; Krause, P.J.; Brandeburg, C.; Crowder, C.D.; Carolan, H.E.; et al. Xenodiagnosis to detect Borrelia burgdorferi infection: A first-in-human study. Clin. Infect. Dis. 2014, 58, 937–945. [Google Scholar] [CrossRef]
- Li, X.; McHugh, G.A.; Damle, N.; Sikand, V.K.; Glickstein, L.; Steere, A.C. Burden and viability of Borrelia burgdorferi in skin and joints of patients with erythema migrans or Lyme arthritis. Arthritis Rheum. 2011, 63, 2238–2247. [Google Scholar] [CrossRef]
- Cameron, D.J. Insufficient evidence to deny antibiotic treatment to chronic Lyme disease patients. Med. Hypotheses 2009, 72, 688–691. [Google Scholar] [CrossRef]
- Wormser, G.P.; Dattwyler, R.J.; Shapiro, E.D.; Halperin, J.J.; Steere, A.C.; Klempner, M.S.; Krause, P.J.; Bakken, J.S.; Strle, F.; Stanek, G.; et al. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: Clinical practice guidelines by the Infectious Diseases Society of America. Clin. Infect. Dis. 2006, 43, 1089–1134. [Google Scholar] [CrossRef]
- Auwaerter, P.G. Point: Antibiotic therapy is not the answer for patients with persisting symptoms attributable to Lyme disease. Clin. Infect. Dis. 2007, 45, 143–148. [Google Scholar] [CrossRef]
- Boudreau, C.R.; Lloyd, V.K.; Gould, O.N. Motivations and experiences of Canadians seeking treatment for Lyme disease outside of the conventional Canadian health-care system. J. Patient Exp. 2018, 5, 120–126. [Google Scholar] [CrossRef] [PubMed]
- Cnaan, A.; Laird, N.M.; Slasor, P. Using the general linear mixed model to analyse unbalanced repeated measures and longitudinal data. Stat. Med. 1997, 16, 2349–2380. [Google Scholar] [CrossRef]
- Zeileis, A.; Kleiber, C.; Jackman, S. Regression models for count data in R. J. Stat. Softw. 2008, 19, 2–25. [Google Scholar]
- British Columbia Renal Agency—Patient Assessment of Chronic Illness Care (PACIC) 2016 Provincial Results: Hemodialysis. Available online: http://www.bcrenalagency.ca/resource-gallery/Documents/PACIC_BC%20Report%202016.HD.pdf7/2018 (accessed on 25 August 2020).
- Donta, S.T. Tetracycline therapy for chronic Lyme disease. Clin. Infect. Dis. 1997, 25, S52–S56. [Google Scholar] [CrossRef] [PubMed]
- Oksi, J.; Nikoskelainen, J.; Viljanen, M.K. Comparison of oral cefixime and intravenous ceftriaxone followed by oral amoxicillin in disseminated Lyme borreliosis. Eur. J. Clin. Microbiol. Infect. Dis. 1998, 17, 715–719. [Google Scholar] [CrossRef]
- Klempner, M.S.; Hu, L.T.; Evans, J.; Schmid, C.H.; Johnson, G.M.; Trevino, R.P.; Norton, D.; Levy, L.; Wall, D.; McCall, J.; et al. Two controlled trials of antibiotic treatment in patients with persistent symptoms and a history of Lyme disease. N. Eng. J. Med. 2001, 345, 85–92. [Google Scholar] [CrossRef]
- Kaplan, R.F.; Trevino, R.P.; Trevino, G.M.; Johnson, L.; Levy, R.; Dornbush, L.T.; Hu, J.; Evans, A.; Weinstein, C.H.; Schmid, M.S.; et al. Cognitive function in post-treatment Lyme disease: Do additional antibiotics help? Neurology 2003, 60, 1916–1922. [Google Scholar] [CrossRef]
- Berende, A.; ter Hofstede, H.J.; Vos, F.J.; Van Middendorp, H.; Vogelaar, M.L.; Tromp, M.; Hoogen, F.H.V.D.; Donders, A.R.T.; Evers, A.W.M.; Kullberg, B.-J. Randomized trial of longer-term therapy for symptoms attributed to Lyme disease. N. Eng. J. Med. 2016, 374, 1209–1220. [Google Scholar] [CrossRef]
- Krupp, L.B.; Hyman, L.G.; Grimson, R.; Coyle, P.K.; Melville, P.; Ahnn, S.; Dattwyler, R.; Chandler, B. Study and treatment of post Lyme disease (STOP-LD): A randomized double masked clinical trial. Neurology 2003, 60, 1923–1930. [Google Scholar] [CrossRef]
- Fallon, B.A.; Keilp, J.G.; Corbera, K.M.; Petkova, E.; Britton, C.B.; Dwyer, E.; Slavov, I.; Cheng, J.; Dobkin, J.; Nelson, D.R.; et al. A randomized, placebo-controlled trial of repeated IV antibiotic therapy for Lyme encephalopathy. Neurology 2008, 70, 992–1003. [Google Scholar] [CrossRef]
- Lee-Lewandrowski, E.; Chen, Z.; Branda, J.; Baron, J.; Kaufman, H.W. Laboratory blood-based testing for Lyme disease at a national reference laboratory. A 7-year experience (2010–2016). Am. J. Clin. Pathol. 2019, 152, 91–96. [Google Scholar] [CrossRef] [PubMed]
- Jarefors, S.; Bennet, L.; You, E.; Forsberg, P.; Ekerfelt, C.; Berglund, J.; Ernerudh, J. Lyme borreliosis reinfection: Might it be explained by a gender difference in immune response? Immunology 2006, 118, 224–235. [Google Scholar] [CrossRef] [PubMed]
- Aucott, J.N.; Seifter, A.; Rebman, A.W. Probable late Lyme disease: A variant manifestation of untreated Borrelia burgdorferi infection. BMC Infect. Dis. 2012, 12, 173. [Google Scholar] [CrossRef] [PubMed]
- Wills, A.B.; Spaulding, A.B.; Adjemian, J.; Prevots, D.R.; Turk, S.-P.; Williams, C.; Marques, A. Long-term follow-up of patients with Lyme disease: Longitudinal analysis of clinical and quality-of-life measures. Clin. Infect. Dis. 2016, 62, 1546–1551. [Google Scholar] [CrossRef] [PubMed]
- Rebman, A.W.; Aucott, J.N. Post-treatment Lyme disease as a model for persistent symptoms in Lyme disease. Front. Med. (Lausanne) 2020, 51, 23–51. [Google Scholar] [CrossRef] [PubMed]
- Rebman, A.W.; Bechtold, K.T.; Yang, T.; Mihm, E.A.; Soloski, M.J.; Novak, C.B.; Aucott, J.N. The clinical, symptom, and quality-of-life characterization of a well-defined group of patients with posttreatment Lyme disease syndrome. Front. Med. (Lausanne) 2017, 4, 224. [Google Scholar] [CrossRef]
- Moore, K.S. Lyme disease: Diagnosis, treatment guidelines, and controversy. J. Nurse Pract. 2015, 11, 64–69. [Google Scholar] [CrossRef]
- Sedgwick, P. Retrospective cohort studies: Advantages and disadvantages. BMJ 2014, 53, 12–25. [Google Scholar] [CrossRef]
- Hess, D.R. Retrospective studies and chart reviews. Respir. Care 2004, 49, 1171–1174. [Google Scholar]
| Category | Symptoms |
|---|---|
| General wellness | weight fluctuations, night sweats, fatigue, Chills |
| Vision | vision problems, eye pain |
| Digestion | ingestion/heart burn, nausea/vomiting, vomiting blood, blood in stool |
| Heart/Circulation | chest pain, palpitations, ankle swelling |
| Urinary | blood in urine, pain when urinating, weak urine flow, frequent urination, urinary leaking |
| Thyroid/Endocrine | hot flashes, frequent thirst, hair changes |
| Skin | lesions, itching/rash, color changes |
| Lungs/Breathing | shortness of breath, wheezing, frequent cough |
| Blood/Lymph | bruising easily, protracted bleeding |
| Neurological | weakness in extremities, dizziness, difficulty with balance, memory loss |
| Ear, Nose, Throat (ENT) | trouble hearing, sinus trouble, nosebleed |
| Muscles, Joints, Bones | joint pain, muscle pain, back pain |
| Psychiatric | panic attacks, anxious, depressed, feeling major stress |
| Patient Characteristic | Number | Percentage (%) |
|---|---|---|
| Age, years | ||
| <60 | 116 | 55.2 |
| >60 | 94 | 44.8 |
| Sex | ||
| Male | 86 | 41.0 |
| Female | 124 | 59.0 |
| Presence of comorbidity | ||
| Anemia | 40 | 19.0 |
| High blood pressure | 52 | 24.8 |
| Heart murmur | 23 | 11.0 |
| Asthma | 24 | 11.4 |
| Diabetes | 15 | 7.14 |
| Irritable bowel syndrome | 78 | 37.1 |
| Yellow jaundice | 9 | 4.29 |
| Seizures | 13 | 6.19 |
| Nervous condition | 28 | 13.3 |
| Gout | 9 | 4.29 |
| Arthritis | 64 | 30.4 |
| Migraines | 96 | 45.7 |
| History of health | ||
| Heart attack | 11 | 5.23 |
| Stroke | 7 | 3.33 |
| Pneumonia | 47 | 22.4 |
| Ulcer | 18 | 8.57 |
| Hernia | 19 | 9.05 |
| Cancer | 27 | 12.4 |
| Blood clot | 9 | 4.29 |
| Kidney infection | 47 | 22.4 |
| Kidney stones | 42 | 20.0 |
| Fractures | 63 | 30.0 |
| Tick exposure history | ||
| Known tick bite | 56 | 26.7 |
| erythema migrans (EM) rash | 46 | 21.9 |
| Patient Group | Patients | ||
|---|---|---|---|
| Female Number | Male Number | Total Percentage (%) | |
| Only one consultation (excluded from chart review) | 20 | 15 | 17% |
| Patients who completed treatment in <1 year (3–12 months) | 12 | 12 | 11% |
| Patients with ongoing treatment for <1 year (3–12 months) | 16 | 13 | 14% |
| Patients who completed treatment >1 year (12+ months) | 41 | 24 | 31% |
| Patients with ongoing treatment for >1 year (12+ months) | 42 | 15 | 27% |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rogerson, A.G.; Lloyd, V.K. Lyme Disease Patient Outcomes and Experiences; A Retrospective Cohort Study. Healthcare 2020, 8, 322. https://doi.org/10.3390/healthcare8030322
Rogerson AG, Lloyd VK. Lyme Disease Patient Outcomes and Experiences; A Retrospective Cohort Study. Healthcare. 2020; 8(3):322. https://doi.org/10.3390/healthcare8030322
Chicago/Turabian StyleRogerson, Ally G., and Vett K. Lloyd. 2020. "Lyme Disease Patient Outcomes and Experiences; A Retrospective Cohort Study" Healthcare 8, no. 3: 322. https://doi.org/10.3390/healthcare8030322
APA StyleRogerson, A. G., & Lloyd, V. K. (2020). Lyme Disease Patient Outcomes and Experiences; A Retrospective Cohort Study. Healthcare, 8(3), 322. https://doi.org/10.3390/healthcare8030322




