Health Promotion Programs to Reduce Noncommunicable Diseases: A Call for Action in Kuwait
Abstract
1. Introduction
2. The Burden of Noncommunicable Diseases (NCDs)
3. Unhealthy Behaviours
3.1. Physical Inactivity
3.2. Obesity
3.3. Smoking
4. Current Efforts in Kuwait to Promote Health and to Address Noncommunicable Diseases (NCDs)
5. Moving Forward—Recommendations for Addressing NCDs in Kuwait through the Lens of Health Promotion and Socioecological Model (SEM)
6. Call for Actions: National-Level Actions for Health Promotion
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- World Health Organization. What Is Health Promotion? Available online: https://www.who.int/features/qa/health-promotion/en/ (accessed on 25 April 2020).
- Schroeder, S.A. We can do better—Improving the health of the American people. N. Engl. J. Med. 2007, 357, 1221–1228. [Google Scholar] [CrossRef] [PubMed]
- Nyberg, S.T.; Batty, G.D.; Pentti, J.; Virtanen, M.; Alfredsson, L.; Fransson, E.I.; Goldberg, M.; Heikkila, K.; Jokela, M.; Knutsson, A.; et al. Obesity and loss of disease-free years owing to major non-communicable diseases: A multicohort study. Lancet Public Health 2018, 3, e490–e497. [Google Scholar] [CrossRef]
- Webber, L.; Divajeva, D.; Marsh, T.; McPherson, K.; Brown, M.; Galea, G.; Breda, J. The future burden of obesity-related diseases in the 53 WHO European-Region countries and the impact of effective interventions: A modelling study. BMJ Open 2014, 4, e004787. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Promoting Health: Guide to National Implementation of the Shanghai Declaration; WHO: Geneva, Switzerland, 2017. [Google Scholar]
- The Public Authority for Civil Information. Kuwait Population Statistical Reports: Gender by Nationality and Age and Governorate. Available online: http://stat.paci.gov.kw/englishreports/ (accessed on 25 April 2020).
- Central Agency Intelligence. The World Factbook. Available online: https://www.cia.gov/library/publications/resources/the-world-factbook/geos/ku.html (accessed on 25 April 2020).
- Worldometer. Kuwait Population. Available online: https://www.worldometers.info/world-population/kuwait-population/ (accessed on 6 June 2020).
- World Health Organization. Kuwait Noncommunicable Diseases Profile. Available online: https://www.who.int/nmh/countries/kwt_en.pdf?ua=1 (accessed on 12 May 2020).
- National Centre for Health Information. Kuwait Health Annual Report; Ministry of Health in the State of Kuwait: Kuwait City, Kuwait, 2015.
- The World Bank Group. Diabetes Prevalence (% of Population Ages 20 to 79). Available online: https://data.worldbank.org/indicator/SH.STA.DIAB.ZS (accessed on 12 May 2020).
- Awad, A.; Al-Nafisi, H. Public knowledge of cardiovascular disease and its risk factors in Kuwait: A cross-sectional survey. BMC Public Health 2014, 14, 1131. [Google Scholar] [CrossRef] [PubMed]
- The World Bank Group. Life Expectancy at Birth. Available online: https://data.worldbank.org/indicator/SP.DYN.LE00.IN?year_low_desc=true (accessed on 19 July 2020).
- World Health Organization. Prevalence of Insufficient Physical Activity among Adults. Global Health Observatory Data Repository. Available online: https://apps.who.int/gho/data/view.main.2463?lang=en (accessed on 12 May 2020).
- Mossialos, E.; Cheatley, J.; Reka, H.; Alsabah, A.; Patel, N. Kuwait Health System Review; London School of Economics and Political Science: London, UK, 2018. [Google Scholar]
- Klautzer, L.; Becker, J.; Mattke, S. The curse of wealth—Middle Eastern countries need to address the rapidly rising burden of diabetes. Int. J. Health Policy Manag. 2014, 2, 109–114. [Google Scholar] [CrossRef][Green Version]
- Behbehani, K. Kuwait national programme for healthy living: First 5-year plan (2013–2017). Med. Princ. Pract. 2014, 23, 32–42. [Google Scholar] [CrossRef]
- World Atlas. The Most Obese Countries in the World. Available online: https://www.worldatlas.com/articles/29-most-obese-countries-in-the-world.html (accessed on 12 May 2020).
- World Health Organization. Mean Body Mass Index Trends among Adults. Global Health Observatory Data Repository. Available online: https://apps.who.int/gho/data/view.main.BMIMEANAREGv?lang=en (accessed on 12 May 2020).
- Global Nutrition Report. Kuwait Nutrition Profile. Available online: https://globalnutritionreport.org/resources/nutrition-profiles/asia/western-asia/kuwait/#profile (accessed on 12 May 2020).
- Al-Wotayan, R.; Sadek, A.; Annaka, M.; Al-Sarraf, A. Eastern Mediterranean Approach for Control of Non Communicable Diseases: Survey of Risk Factors for Chronic Non Communicable Diseases; Ministry of Health in the State of Kuwait: Kuwait City, Kuwait, 2015.
- World Health Organization. WHO Global Report on Trends in Prevalence of Tobacco Smoking 2000–2025; WHO: Geneva, Switzerland, 2018. [Google Scholar]
- WHO Report on the Global Tobacco Epidemic, 2019 Country Profile: Kuwait. Available online: https://www.who.int/tobacco/surveillance/policy/country_profile/kwt.pdf?ua=1 (accessed on 12 May 2020).
- Memon, A.; Moody, P.M.; Sugathan, T.N.; El-Gerges, N.; Al-Bustan, M.; Al-Shatti, A.; Al-Jazzaf, H. Epidemiology of smoking among Kuwaiti adults: Prevalence, characteristics, and attitudes. Bull. World Health Organ. 2000, 78, 1306–1315. [Google Scholar]
- Kuwaitis Lower Blood Pressure by Reducing Salt in Bread. Available online: https://www.who.int/features/2014/kuwait-blood-pressure/en/ (accessed on 28 May 2020).
- UNIATF. Joint Mission of the United Nations Interagency Task Force on the Prevention and Control of Noncommunicable Diseases, Cambodia, 7–11 August 2017; World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- World Health Organization. Development of a New Health Sector Strategy for the States of Kuwait; WHO Regional Office for the Eastern Mediterranean: Cairo, Egypt, 2017. [Google Scholar]
- World Health Organization. Health Promotion. Available online: https://www.who.int/healthpromotion/fact-sheet/en/ (accessed on 12 May 2020).
- Smith, B.J.; Tang, K.C.; Nutbeam, D. WHO health promotion glossary: New terms. Health Promot. Int. 2006, 21, 340–345. [Google Scholar] [CrossRef]
- DiClemente, R.; Nowara, A.; Shelton, R.; Wingood, G. Need for innovation in public health research. Am. J. Public Health 2019, 109, S117–S120. [Google Scholar] [CrossRef]
- Norton, B.; McLeroy, K.; Burdine, J.; Felix, R.; Dorsey, A. Community capacity: Concept, theory, and methods. In Emerging Theory in Health Promotion Practice and Research; Jossey-Bass: San Francisco, CA, USA, 2002; pp. 194–227. [Google Scholar]
- Minkler, M.; Pies, C.; Hyde, C.A. Ethical issues in community organizing and capacity building. In Community Organizing and Community Building for Health and Welfare; Rutgers University Press: New Brunswick, NJ, USA, 2019; pp. 110–129. [Google Scholar]
- Berkowitz, B.; Nicola, R.M. Public health infrastructure system change. J. Public Health Manag. Pract. 2003, 9, 224–227. [Google Scholar] [CrossRef]
- McDonald, M.; Catalani, C.; Minkler, M. 16. Using the arts and new media in community organizing and community building: An overview and case study from post-Katrina New Orleans. In Community Organizing and Community Building for Health and Welfare; Rutgers University Press: New Brunswick, NJ, USA, 2019; pp. 288–304. [Google Scholar]
- Chapman, L.S. Meta-evaluation of worksite health promotion economic return studies: 2005 update. Am. J. Health Promot. 2005, 19, 1–11. [Google Scholar] [CrossRef] [PubMed]
- The Center for Chronic Disease Prevention and Health Promotion. Certified Healthy Oklahoma. Available online: https://certifiedhealthyok.com/ (accessed on 19 July 2020).
- Butterfoss, F.D.; Kegler, M.C. A coalition model for community action. In Community Organizing and Community Building for Health and Welfare; Rutgers University Press: New Brunswick, NJ, USA, 2019; pp. 309–328. [Google Scholar]
- Butterfoss, F.D.; Kegler, M.C. The community coalition action theory. In Emerging Theories in Health Promotion Practice and Research; DiClemente, R., Crosby, R., Kegler, M.C., Eds.; Jossey-Bass: San Francisco, CA, USA, 2009. [Google Scholar]
- Gasana, J. Research and Development in Public Health—Priorities, Barriers and Solutions for Kuwait: A Stakeholder Consensus through a Modified Delphi Study; Faculty of Public Health, Kuwait University: Kuwait City, Kuwait, 2020. [Google Scholar]
- Bergeron, K.; Abdi, S.; DeCorby, K.; Mensah, G.; Rempel, B.; Manson, H. Theories, models and frameworks used in capacity building interventions relevant to public health: A systematic review. BMC Public Health 2017, 17, 914. [Google Scholar] [CrossRef] [PubMed]
- McLeroy, K.R.; Bibeau, D.L.; Steckler, A.; Glanz, K. An ecological perspective on health promotion programs. Health Educ. Q. 1988, 15, 351–377. [Google Scholar] [CrossRef] [PubMed]
- Max, J.L.; Sedivy, V.; Garrido, M. Increasing Our Impact by Using a Social-Ecological Approach; Administration on Children, Youth and Families, Family and Youth Services Bureau: Washington, DC, USA, 2015.
- Vo, L.; Albrecht, S.S.; Kershawd, K.N. Multilevel interventions to prevent and reduce obesity. Curr. Opin. Endocr. Metab. Res. 2019, 4, 62–69. [Google Scholar] [CrossRef]
- McLeroy, K.; Norton, B.L.; Kegler, M.C.; Burdine, J.N.; Sumaya, C.V. Community-based interventions. Am. J. Public Health 2003, 93, 529–533. [Google Scholar] [CrossRef]
- Golden, S.D.; Earp, J.A.L. Social ecological approaches to individuals and their contexts. Health Educ. Behav. 2012, 39, 364–372. [Google Scholar] [CrossRef]
- Vandenbroeck, I.P.; Goossens, J.; Clemens, M. Tackling Obesities: Future Choices—Obesity System Atlas; Department of Innovation Universities and Skills: London, UK, 2007.
- Laverack, G. The challenge of the ‘art and science’ of health promotion. Challenges 2017, 8, 22. [Google Scholar] [CrossRef]
- Verrotti, A.; Peñta, L.; Zenzeri, L.; Agostinelli, S.; De Feo, P. Childhood obesity: Prevention and strategies of intervention. A systematic review of school-based interventions in primary schools. J. Endocrinol. Investig. 2014, 37, 1155–1164. [Google Scholar] [CrossRef]
- Lambrinou, C.-P.; Androutsos, O.; Karaglani, E.; Cardon, G.; Huys, N.; Wikström, K.; Kivelä, J.; Ko, W.; Karuranga, E.; Tsochev, K.; et al. Effective strategies for childhood obesity prevention via school based, family involved interventions: A critical review for the development of the Feel4Diabetes-study school based component. BMC Endocr. Disord. 2020, 20, 20–52. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Components of the Whole School, Whole Community, Whole Child (WSCC). Available online: https://www.cdc.gov/healthyschools/wscc/components.htm (accessed on 12 May 2020).
- Trans Fat Free by 2023: Case Studies in Trans Fat Elimination; NCD Alliance: Geneva, Switzerland, 2019.
- Goldstein, G. Healthy cities: Overview of a who international program. Rev. Environ. Health 2000, 15, 207–214. [Google Scholar] [CrossRef]
- Ministry of Health. Healthy Cities Office. Available online: https://healthycities.moh.gov.kw/en/Pages/default.aspx (accessed on 19 July 2020).
- Bennett, H.; Coleman, E.A.; Parry, C.; Bodenheimer, T.; Chen, E.H. Health coaching for patients with chronic illness. Fam. Pract. Manag. 2010, 17, 24–29. [Google Scholar] [PubMed]
- Carter, A.; Tamkin, P.; Wilson, S.; Miller, L. The Case for Health Coaching: Lessons Learned from Implementing a Training and Development Intervention for Clinicians Across the East of England; Institute for Employment Studies: Brighton, UK, 2015. [Google Scholar]
- Green, L.; Kreuter, M. Health Program Planning: An Educational and Ecological Approach; McGraw-Hill: New York, NY, USA, 2005. [Google Scholar]
- Marmot, M.; Friel, S.; Bell, R.; Houweling, T.A.J.; Taylor, S. Closing the gap in a generation: Health equity through action on the social determinants of health. Lancet 2008, 372, 1661–1669. [Google Scholar] [CrossRef]
- Hillemeier, M.; Lynch, J.; Harper, S.; Casper, M. Data Set Directory of Social Determinants of Health at the Local Level; Department of Health and Human Services, Centers for Disease Control and Prevention: Atlanta, GA, USA, 2004.
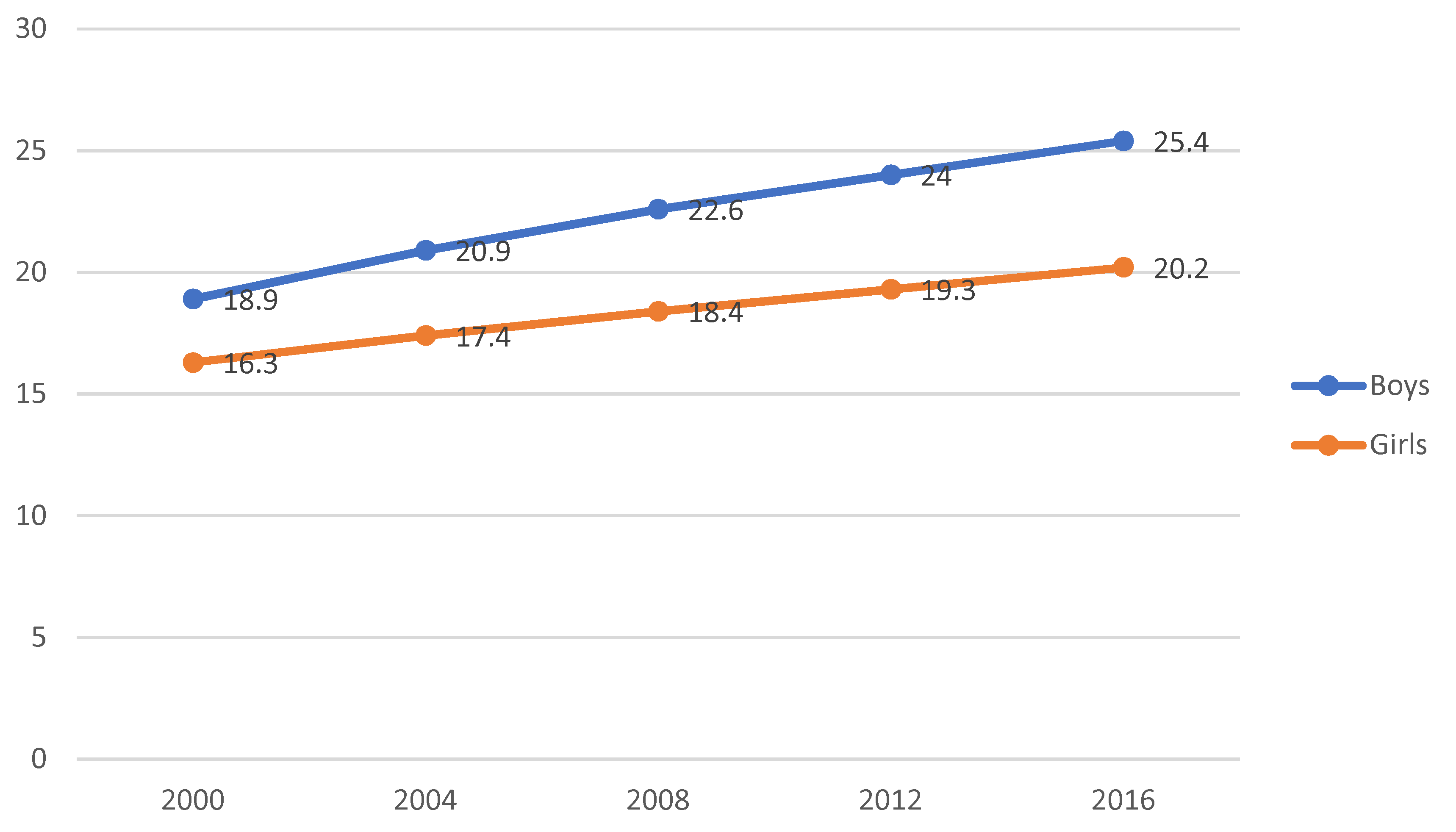
| Risk Factors | Male | Female | Total |
|---|---|---|---|
| Physical inactivity | 60.0 | 73.0 | 65.0 |
| Current tobacco smoking (aged 15+) | 40.0 | 3.0 | 24.0 |
| Obesity | 33.0 | 44.0 | 37.0 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Salman, A.; Tolma, E.; Chun, S.; Sigodo, K.O.; Al-Hunayan, A. Health Promotion Programs to Reduce Noncommunicable Diseases: A Call for Action in Kuwait. Healthcare 2020, 8, 251. https://doi.org/10.3390/healthcare8030251
Salman A, Tolma E, Chun S, Sigodo KO, Al-Hunayan A. Health Promotion Programs to Reduce Noncommunicable Diseases: A Call for Action in Kuwait. Healthcare. 2020; 8(3):251. https://doi.org/10.3390/healthcare8030251
Chicago/Turabian StyleSalman, Ahmad, Eleni Tolma, Sungsoo Chun, Kennedy O. Sigodo, and Adel Al-Hunayan. 2020. "Health Promotion Programs to Reduce Noncommunicable Diseases: A Call for Action in Kuwait" Healthcare 8, no. 3: 251. https://doi.org/10.3390/healthcare8030251
APA StyleSalman, A., Tolma, E., Chun, S., Sigodo, K. O., & Al-Hunayan, A. (2020). Health Promotion Programs to Reduce Noncommunicable Diseases: A Call for Action in Kuwait. Healthcare, 8(3), 251. https://doi.org/10.3390/healthcare8030251





