An Exercise Program Designed for Children with Attention Deficit/Hyperactivity Disorder for Use in School Physical Education: Feasibility and Utility
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Procedure
2.3. Measures
2.4. Statistical Analysis
3. Results
4. Discussion
Limitations and Future Directions
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A

References
- Polanczyk, G.V.; Willcutt, E.G.; Salum, G.A.; Kieling, C.; Rohde, L.A. ADHD prevalence estimates across three decades: An updated systematic review and meta-regression analysis. Int. J. Epidemiol. 2014, 3, 434–442. [Google Scholar] [CrossRef] [PubMed]
- Thomas, R.; Sanders, S.; Doust, J.; Beller, E.; Glasziou, P. Prevalence of attention-deficit/hyperactivity disorder: A systematic review and meta-analysis. Pediatrics 2015, 135, e994–e1001. [Google Scholar] [CrossRef] [PubMed]
- Bunford, N.; Evans, S.W.; Langberg, J.M. Emotion dysregulation is associated with social impairment among young adolescents with ADHD. J. Atten. Disord. 2014, 1, 68–82. [Google Scholar] [CrossRef] [PubMed]
- Cordier, R.; Bundy, A.; Hocking, C.; Einfeld, S. Empathy in the play of children with attention deficit hyperactivity disorder. OTJR 2010, 30, 122–132. [Google Scholar] [CrossRef]
- Ronk, M.J.; Hund, A.M.; Landau, S. Assessment of social competence of boys with attention-deficit/hyperactivity disorder: Problematic peer entry, host responses, and evaluations. J. Abnorm. Child Psychol. 2011, 39, 829–840. [Google Scholar] [CrossRef]
- Laugesen, B.; Groenkjaer, M. Parenting experiences of living with a child with attention deficit hyperactivity disorder: A systematic review of qualitative evidence. JBI Database Syst. Rev. Implement. Rep. 2015, 13, 169–234. [Google Scholar] [CrossRef] [PubMed]
- DuPaul, G.J.; Weyandt, L.L.; Janusis, G.M. ADHD in the classroom: Effective intervention strategies. Theor. Pract. 2011, 50, 35–42. [Google Scholar] [CrossRef]
- Zaretskii, V.K. The zone of proximal development: What Vygotsky did not have time to write. J. Russ. East Eur. Psychol. 2009, 47, 70–93. [Google Scholar] [CrossRef]
- Verret, C.; Guay, M.C.; Berthiaume, C.; Gardiner, P.; Béliveau, L. A physical activity program improves behavior and cognitive functions in children with ADHD: An exploratory study. J Atten. Disord. 2012, 16, 71–80. [Google Scholar] [CrossRef]
- Choi, J.W.; Han, D.H.; Kang, K.D.; Jung, H.Y.; Renshaw, P.F. Aerobic exercise and attention deficit hyperactivity disorder: Brain research. Med. Sci. Sports Exerc. 2015, 47, 33–39. [Google Scholar] [CrossRef]
- Hoza, B.; Smith, A.L.; Shoulberg, E.K.; Linnea, K.S.; Dorsch, T.E.; Blazo, J.A.; McCabe, G.P. A randomized trial examining the effects of aerobic physical activity on attention-deficit/hyperactivity disorder symptoms in young children. J. Abnorm. Child Psychol. 2015, 43, 655–667. [Google Scholar] [CrossRef] [PubMed]
- Cerrillo-Urbina, A.J.; García-Hermoso, A.; Sánchez-López, M.; Pardo-Guijarro, M.J.; Santos Gómez, J.L.; Martínez-Vizcaíno, V. The effects of physical exercise in children with attention deficit hyperactivity disorder: A systematic review and meta-analysis of randomized control trials. Child Care Health Dev. 2015, 41, 779–788. [Google Scholar] [CrossRef] [PubMed]
- Ng, Q.X.; Ho, C.Y.X.; Chan, H.W.; Yong, B.Z.J.; Yeo, W.S. Managing childhood and adolescent attention-deficit/hyperactivity disorder (ADHD) with exercise: A systematic review. Complement. Ther. Med. 2017, 34, 123–128. [Google Scholar] [CrossRef] [PubMed]
- Vysniauske, R.; Verburgh, L.; Oosterlaan, J.; Molendijk, M.L. The effects of physical exercise on functional outcomes in the treatment of ADHD: A meta-analysis. J. Atten. Disord. 2016. [Google Scholar] [CrossRef] [PubMed]
- Ahn, S.; Fedewa, A.L. A meta-analysis of the relationship between children’s physical activity and mental health. J. Pediatr. Psychol. 2011, 36, 385–397. [Google Scholar] [CrossRef] [PubMed]
- Christiansen, L.; Beck, M.M.; Bilenberg, N.; Wienecke, J.; Astrup, A.; Lundbye-Jensen, J. Effects of Exercise on Cognitive Performance in Children and Adolescents with ADHD: Potential Mechanisms and Evidence-based Recommendations. J. Clin. Med. 2019, 8, 841. [Google Scholar] [CrossRef]
- Halperin, J.M.; Healey, D.M. The influences of environmental enrichment, cognitive enhancement, and physical exercise on brain development: Can we alter the developmental trajectory of ADHD? Neurosci. Biobehav. Rev. 2012, 35, 621–634. [Google Scholar] [CrossRef]
- Makris, N.; Biederman, J.; Monuteaux, M.C.; Seidman, L.J. Towards conceptualizing a neural systems-based anatomy of attention-deficit/hyperactivity disorder. Dev. Neurosci. 2009, 31, 36–49. [Google Scholar] [CrossRef]
- Epstein, J.N.; Casey, B.J.; Tonev, S.T.; Davidson, M.C.; Reiss, A.L.; Garrett, A.; Vitolo, A. ADHD-and medication-related brain activation effects in concordantly affected parent–child dyads with ADHD. J. Child Psychol. Psychiatry 2007, 48, 899–913. [Google Scholar] [CrossRef]
- Stahl, S.M. Mechanism of action of stimulants in attention-deficit/hyperactivity disorder. J. Clin. Psychiatry 2010, 71, 12–13. [Google Scholar] [CrossRef]
- Mulrine, C.F.; Prater, M.A.; Jenkins, A. The active classroom: Supporting students with attention deficit hyperactivity disorder through exercise. Teach. Except. Child. 2008, 40, 16–22. [Google Scholar] [CrossRef]
- ADDitude. Quiet Ways for Fidgety Kids to Release Energy at School. Available online: https://www.additudemag.com/fidgeting/ (accessed on 5 February 2019).
- ADHD Foundation. Primary School Classroom Strategies. Available online: https://www.adhdfoundation.org.uk/information/schools/ (accessed on 5 February 2019).
- Taylor, A.; Foreman, D. Maximising engagement by design: Collaborative development of therapeutic exercise for children with ADHD in schools. J. Sports Sci. 2018, 36, 73–74. [Google Scholar] [CrossRef]
- Kennedy, E.-K. The revised SEND code of practice 0–25: Effective practice in engaging children and young people in decision-making about interventions for social, emotional and mental health needs. Support Learn. 2015, 30, 364–380. [Google Scholar] [CrossRef]
- American College of Sports Medicine. ACSM’s Guidelines for Exercise Testing and Prescription, 10th ed.; Riebe, D., Ehrman, J.K., Liguori, G., Magal, M., Eds.; Wolters Kluwer: Philadelphia, PA, USA, 2018; pp. 1–468. [Google Scholar]
- DuPaul, G.J.; Stoner, G. ADHD in the Schools: Assessment and Intervention Strategies, 3rd ed.; The Guildford Press: New York, NY, USA, 2014; pp. 1–366. [Google Scholar]
- DuPaul, G.J. Parent and teacher ratings of ADHD symptoms: Psychometric properties in a community-based sample. J. Clin. Child Adolesc. Psychol. 1991, 20, 245–253. [Google Scholar] [CrossRef]
- DuPaul, G.J.; Power, T.J.; McGoey, K.E.; Ikeda, M.J.; Anastopoulos, A.D. Reliability and validity of parent and teacher ratings of attention-deficit/hyperactivity disorder symptoms. J. Psychoeduc. Assess. 1998, 16, 55–68. [Google Scholar] [CrossRef]
- Ludyga, S.; Brand, S.; Gerber, M.; Weber, P.; Brotzmann, M.; Habibifar, F.; Pühse, U. An event-related potential investigation of the acute effects of aerobic and coordinative exercise on inhibitory control in children with ADHD. Dev. Cognit. Neurosci. 2017, 28, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Ziereis, S.; Jansen, P. Effects of physical activity on executive function and motor performance in children with ADHD. Res. Dev. Disabil. 2015, 38, 181–191. [Google Scholar] [CrossRef]
- Bustamante, E.E.; Davis, C.L.; Frazier, S.L.; Rusch, D.; Fogg, L.F.; Atkins, M.S.; Marquez, D.X. Randomized controlled trial of exercise for ADHD and disruptive behavior disorders. Med. Sci. Sports Exerc. 2016, 48, 1397–1407. [Google Scholar] [CrossRef]
- Moore, D.A.; Russell, A.E.; Arnell, S.; Ford, T.J. Educators’ experiences of managing students with ADHD: A qualitative study. Child Care Health Dev. 2017, 43, 489–498. [Google Scholar] [CrossRef]
- Florian, L. Inclusive Pedagogy: A transformative approach to individual differences but can it help reduce educational inequalities. Scott. Edu. Rev. 2015, 47, 5–14. [Google Scholar] [CrossRef]
- Petrie, K.; Devcich, J.; Fitzgerald, H. Working towards inclusive physical education in a primary school: ‘Some days I just don’t get it right’. Phys. Educ. Sport Pedagogy 2018, 23, 345–357. [Google Scholar] [CrossRef]
| Pre-Intervention Median (Range) | Week 6 Median (Range) | Week 11 Median (Range) | |
|---|---|---|---|
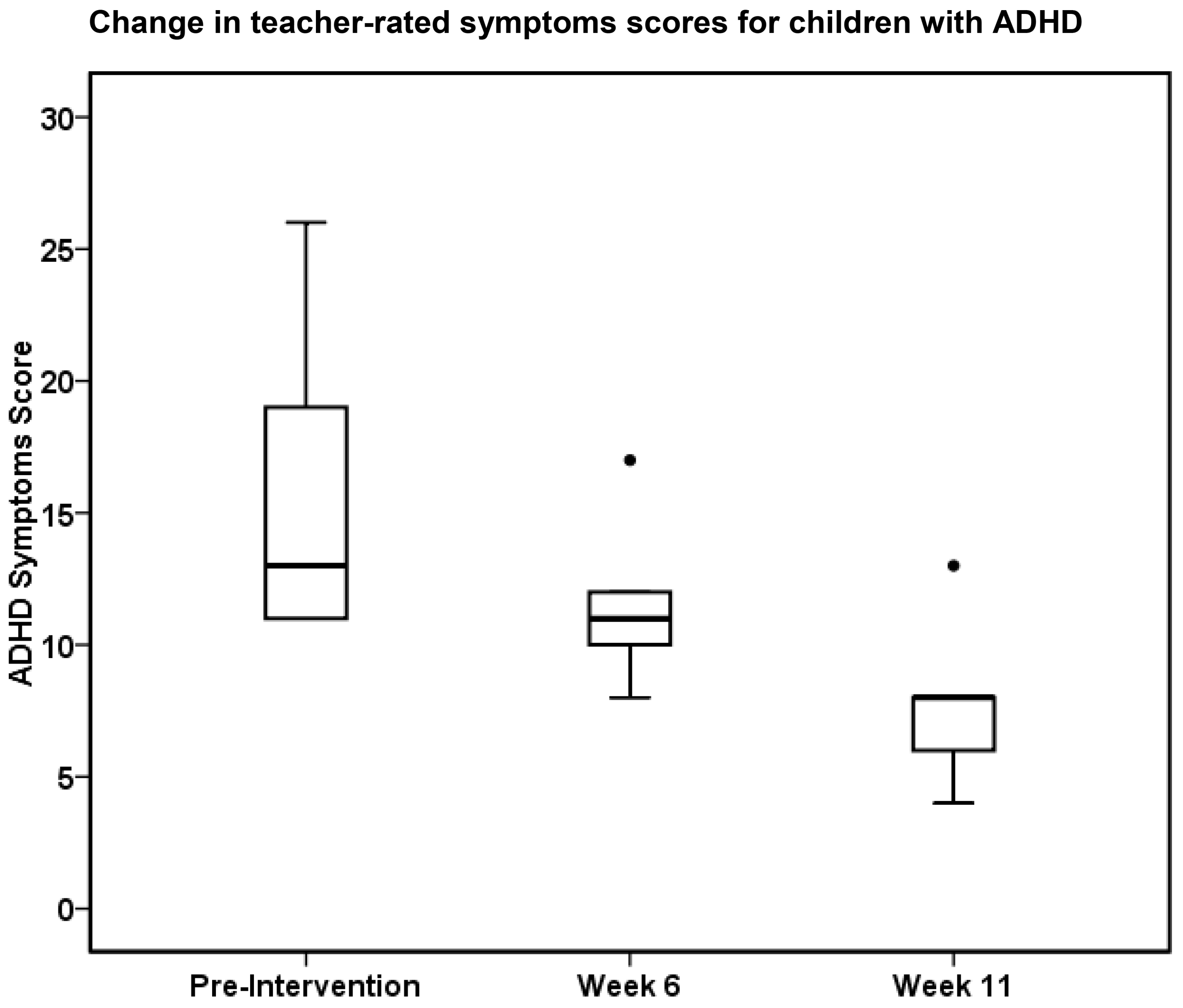
| Teacher-rated ADHD scores | 13 (11–26) | 11 (8–17) | 8 (4–13) * |
| Parent-rated ADHD scores | 9 (8–17) | 4 (0–12) | 3.5 (0–26) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Taylor, A.; Novo, D.; Foreman, D. An Exercise Program Designed for Children with Attention Deficit/Hyperactivity Disorder for Use in School Physical Education: Feasibility and Utility. Healthcare 2019, 7, 102. https://doi.org/10.3390/healthcare7030102
Taylor A, Novo D, Foreman D. An Exercise Program Designed for Children with Attention Deficit/Hyperactivity Disorder for Use in School Physical Education: Feasibility and Utility. Healthcare. 2019; 7(3):102. https://doi.org/10.3390/healthcare7030102
Chicago/Turabian StyleTaylor, Alyx, Dario Novo, and David Foreman. 2019. "An Exercise Program Designed for Children with Attention Deficit/Hyperactivity Disorder for Use in School Physical Education: Feasibility and Utility" Healthcare 7, no. 3: 102. https://doi.org/10.3390/healthcare7030102
APA StyleTaylor, A., Novo, D., & Foreman, D. (2019). An Exercise Program Designed for Children with Attention Deficit/Hyperactivity Disorder for Use in School Physical Education: Feasibility and Utility. Healthcare, 7(3), 102. https://doi.org/10.3390/healthcare7030102






