1. Introduction
The objectives of this article are to investigate the incidence rate of Lyme disease in the USA and Europe, to investigate the financial cost of chronic Lyme disease and to find the most cost-efficient way for the governments to solve the current chronic Lyme disease pandemic [
1]. Very few studies exist that calculate the economic impact of chronic Lyme disease [
2]. According to the European Centre for Disease Prevention and Control (ECDC), Lyme disease—also known as Borreliosis—is caused by a spirochete bacteria called
Borrelia burgdorferi [
3]. An early stage
Borrelia infection is known as acute Lyme disease and a late stage
Borrelia infection is known as chronic Lyme disease. A Lyme disease “war” has been going for a long time [
4,
5] between two doctors’ associations regarding the most appropriate way to diagnose and treat Lyme disease. The two doctors associations are the Infectious Diseases Society of America (IDSA) [
6] and International Lyme and Associated Diseases Society (ILADS) [
7]. IDSA represents infectious disease doctors that firmly believe that all Lyme disease infections, regardless of whether the infection is acute or chronic, can successfully and easily be treated with three weeks of oral antibiotic [
8] despite the fact that no scientific studies currently exist that support the claim that three weeks of oral antibiotics can always cure acute or chronic Lyme disease [
9] and there exist many scientific studies that have shown that the
Borrelia bacteria can survive three weeks of oral antibiotics in vitro [
10,
11] and in vivo, in mice [
12,
13,
14,
15], dogs [
16], horses [
17], monkeys [
18] and in humans [
19,
20,
21,
22,
23,
24,
25,
26,
27,
28,
29,
30,
31,
32,
33,
34,
35,
36]. The in vivo references have mostly been extracted from [
37,
38,
39]. Alive
Borrelia bacteria has been found in 7 out of 8 patients with chronic Lyme disease [
40]. The immune system by itself can never eradicate a
Borrelia infection [
41,
42,
43,
44] and no scientific studies exist that show that bacterial infections can simply disappear. Approximately 63% [
45,
46] of people today that are infected with
Borrelia, unfortunately, develop chronic Lyme disease. Most Lyme disease patients today either do not receive any antibiotic treatment at all or they receive an insufficient amount of antibiotic treatment. The IDSA does not recognize chronic Lyme disease, nor do they recommend antibiotic treatment for chronic Lyme disease. The IDSA calls chronic Lyme disease post-treatment Lyme disease syndrome (PTLDS) [
47] but it has been suggested that this term is a misnomer and should not be used [
48]. Because chronic Lyme disease is classified as a syndrome instead of an infection, the IDSA therefore does not recommend antibiotic treatment for chronic Lyme disease.
In 2006, the IDSA treatment guidelines development process was subjected to an antitrust investigation by the Connecticut Attorney General [
49], which found that many IDSA treatment panel members had conflicts of interest [
50]. In November 2017, another antitrust lawsuit (Civil Action No 17-cv-190) [
51,
52] was directed at the IDSA along with several large insurance companies in the USA and several IDSA medical doctors, in a federal court in Texarkana, Texas in the USA. The allegations concern violations of the Racketeer Influenced and Corrupt Organizations (RICO) Act and the Sherman Antitrust Act. According to the Agency for Healthcare Research and Quality (AHRQ), which is part of the U.S. Department of Health and Human Services, 86% of health care costs in 2010 in the USA came from patients with one or more chronic conditions [
53]. The concern is that because Intravenous (IV) antibiotic treatment for people with chronic Lyme disease costs so much money, insurance companies in the USA may gain by colluding with the IDSA to ensure chronic Lyme disease is not classified as a real disease caused by bacteria, so that IV antibiotic treatment can be denied.
The scientific process fails if it can be controlled by a group or groups with a particular agenda [
54]. The IDSA’s treatment guidelines for Lyme disease are problematic in the following ways: (A) They do not follow The National Academies of Sciences, Engineering and Medicine recommendations on how to develop treatment guidelines [
55] because the IDSA treatment guideline panel did not consist of a diversified and balanced group of doctors nor did the panel include patient representatives; (B) More than 50% of IDSAs treatment guidelines are based only on “expert opinion” [
56]; (C) The IDSA’s treatment guidelines for Lyme disease do reflect the fact that, according to the CDC, Lyme disease can lead to death if not treated with antibiotics [
57]. The CDC has, however, significantly underestimated the number of deaths caused by
chronic Lyme disease. One study estimates that chronic Lyme disease and associated diseases could be the cause of over 1200 suicides per year in the USA [
58].
The International Lyme and Associated Diseases Society (ILADS) represents Lyme Literate Medical Doctors (LLMDs) from around the world who recognize that chronic Lyme disease is a real and serious disease that must be treated with long-term antibiotics [
59]. ILADS’ treatment guidelines for Lyme disease can be found on the National Guidelines Clearinghouse (NGC) web page [
60]. According to ILADS, Lyme disease is a clinical diagnosis that is based on the symptoms a patient presents. LLMDs prefer to treat chronic Lyme disease patients with IV antibiotics because IV antibiotics are more effective than oral antibiotics [
61]. However, oral antibiotics are much easier to administer, and they are not as expensive as IV antibiotics. Hence, in a situation where a patient cannot afford IV antibiotics, or if a patient has difficulties finding someone to administer IV antibiotics, then oral antibiotics are always preferred over no antibiotics. LLMDs can, if necessary, treat a patient with chronic Lyme disease with oral antibiotics for the rest of the patient’s life. Thus, similarities exist between chronic Lyme disease and the Human Immunodeficiency Virus (HIV) that also cannot be eradicated with oral medication.
Up until December 2017, the Centers for Disease Control and Prevention (CDC) in the USA officially endorsed the IDSA treatment guidelines for Lyme disease. What the CDC’s view on treatment for chronic Lyme disease is today is unclear [
62]. The CDC still uses the IDSA terminology ‘post-treatment Lyme disease syndrome’ (PTLDS) [
63]. It is unlikely that the IDSA’s lack of medical ethics when it comes to Lyme disease [
64] was the reason why the CDC stopped officially endorsing IDSA treatment guidelines for Lyme disease, because in 2016 an anonymous whistleblower group of scientists from within the CDC, calling themselves CDC Scientists Preserving Integrity, Diligence and Ethics in Research (CDC SPIDER), raised concerns about the CDC’s lack of independence and ethics [
65], stating, “We are a group of scientists at CDC that are very concerned about the current state of ethics at our agency. It appears that our mission is being influenced and shaped by outside parties and rogue interests”. The CDC therefore most likely stopped endorsing the IDSA treatment guidelines because legal and public pressure was building up. Today people are becoming more aware of chronic Lyme disease. The conflict over what the best ways are to diagnose and treat Lyme disease have gone so far that a Tick-Borne Disease Working Group was created when the 21st-century cures act became law in the USA in December 2016 [
66]. The objective of the working group is to review the scientific literature, regarding for example causes, prevention, diagnosis, duration, surveillance and treatment for Lyme disease and associated diseases.
The genus
Borrelia was named in honor of the French bacteriologist Amédée Borrel in 1907 [
67]. The name Lyme comes from the name of the town in Connecticut in the USA where the disease was ”first” observed in 1977 [
68] this despite the fact that the German physician Alfred Buchwald published the first case of atrophy of the skin already in 1883 [
69]. In 1902 Herxheimer and Hartmann named such atrophy of the skin Acrodermatitis Chronica Atrophicans (ACA) [
70] which is why ACA, which is dermatological disorder mostly associated with chronic Lyme disease in Europe [
71], sometimes is called Herxheimer disease. ACA presents its self as a red-bluish discoloration of the extremities [
72]. The link between Lyme disease and the bacteria that cause it was first discovered by the medical entomologist Dr. Willy Burgdorfer in 1982 [
73]. The bacteria, therefore, took the name after its discoverer
Borrelia Burgdorferi. It was first in 1929 when the serendipitous discovery of penicillin was made by scientist Alexander Fleming [
74] that treatment for Lyme disease became available. Penicillin was originally produced from mold. Naturally occurring antibiotics can also be produced by fermentation, an old technique that can be traced back almost 8000 years [
75]. The genes that convey antibiotic resistance to bacteria have been around for at least 30,000 years [
76], which means that antibiotic resistance to a large part has not been developed during the last 88 years humankind has known about antibiotics which is a fact that we rarely hear about though.
One of the first people to treat chronic Lyme, or more specifically ACA, with penicillin in 1949 was Nils Thyresson [
77] who was a Swedish medical doctor and professor of Dermatology and Venereology. The first human believed to have been infected with Lyme disease was Ötzi the Iceman [
78]. This 5300 years old naturally preserved mummy was discovered in 1991 in the Ötztal Alps on the border between Austria and Italy. Spirochete bacteria are believed to be much older this though. Spirochetes similar to
Borrelia has been found in a 15 million years old tick preserved in amber in the Dominican Republic [
79] which means that the spirochete bacteria that causes Lyme disease is much older than humankind. The complete
Borrelia genome was first sequenced in 1997 [
80]. The
Borrelia bacteria has the most complex genomic architecture among known prokaryotes [
81].
Borrelia bacteria are also very genetically diversified [
82,
83]. Different Borrelia strains have different antigens [
84] which means that different
Borrelia strains will produce different immune system responses in the form of antibodies in an infected host. A blood test that only test for one specific antibody cannot detect antibodies from different Borrelia strains. A person that is infected with one type of Borrelia strain will also have different symptoms compared to a person that is infected with a different Borrelia strain [
85]. For example, arthritis is usually not seen in European Lyme disease patients [
86] due to the different
Borrelia strains that exist in Europe compared to the USA which means that the lack of arthritis in a patient should not be interpreted as the patient not having Lyme disease. Lyme disease diagnosis and treatment are further complicated by the fact that
Borrelia also has many different co-infections [
87] such as Babesia, Bartonella, Ehrlichia, etc. It is believed that a vector such as a tick can spread at least 237 different types of bacteria [
88] and many types of viruses [
89] which means that many chronic Lyme patients might be infected with many different types of microbes at the same time.
In the Lyme disease documentary Under Our Skin, Dr. Burgdorfer says: “The controversy in the Lyme disease research is a shameful affair and I say this because the whole thing is politically tainted. Money goes to the same people who have for the last thirty years produced the same thing. Nothing”. [
90]. The
Borrelia bacteria has at least three different morphological forms. (1) A spirochete form [
91]. (2) A round body form that is also known as cyst form [
92]. (3) A biofilm form [
93]. The
Borrelia bacteria evade the immune system by for example changing morphology [
94] and by changing its outer surface proteins (Osp) also known as antigens [
95,
96,
97,
98]. When the bacteria change its antigens all the time, the specific antibodies that are produced by the immune system to try to eradicate the infection becomes useless. The DNA structure that is believed to be responsible for the bacteria’s antigenic variation ability is called G-quadruplex (G4) [
99]. Immune system evasion by other diseases such as Amyotrophic Lateral Sclerosis (ALS) [
100] and cancer [
101] is also believed to be connected to G4. Exciting research is being done that is trying to find medications that block G4 for the
Borrelia bacteria [
102]. If the researchers are successful, it could mean an end to chronic Lyme disease but also to other diseases. If the immune system in combination with some drug could eradicate the
Borrelia bacteria that would be a superior solution compared to a possible lifetime of oral antibiotics. The bacteria evade being killed by broad-spectrum antibiotics by changing morphology [
103]. Note that the bacteria ability to evade broad-spectrum antibiotics should not be interpreted as antibiotic resistant. Metronidazole/Tinidazole forces the bacteria to take a spirochete form [
104,
105] where other broad-spectrum antibiotics such as Azithromycin can kill it off. When chronic Lyme patients are treated with a macrolide antibiotic such as Azithromycin in combination with Metronidazole/Tinidazole, then the physician can also give Plaquenil which is an anti-malaria medication. Plaquenil raises the PH level in cells so that macrolide antibiotics can work more effectively [
106]. Unfortunately, Plaquenil does not work for tetracycline antibiotics [
107]. It is, however, important to note that Plaquenil can cause eye problems [
108] which means that not all patients can tolerate this medication.
Because different combinations of antibiotics have different effects on the different morphological forms of the
Borrelia bacteria [
109], ILADS treatment guidelines recommend combination therapy with two different types antibiotics for chronic Lyme disease [
110] for example metronidazole/tinidazole in combination with azithromycin/doxycycline. The recommended treatment for chronic Lyme disease is therefore different from the recommended treatment for acute Lyme by the IDSA which is, monotherapy with one antibiotic for example doxycycline. Again, similarities exist between HIV and chronic Lyme disease because both are treated with combination therapy. The reason for combination therapy for HIV and chronic Lyme disease is however different. Combination therapy in HIV is motivated by the fact that the virus develops resistance to the medication if you only treat with one antiviral medication. For chronic Lyme disease, this is not the cases. Combination therapy for chronic Lyme disease is motivated by the fact that
the Borrelia bacteria changes morphology which means that monotherapy is not an effective treatment for Lyme disease.
A common mistake is to describe the symptoms of Lyme disease as “flu-like”. A serious Lyme disease infection should not be reduced to a simple cold. A better screening symptom for Lyme disease is paresthesia. Paresthesia manifests itself as vibrating sensation under the skin. One study estimates that 53% of patients with chronic Lyme disease develop paresthesia [
111]. A second study estimates that 70% of patients with chronic Lyme disease develop paresthesia [
112]. The good thing is that the paresthesia stops when antibiotics have killed off the infection [
113] but also during treatment with antibiotics such as Metronidazole or Tinidazole. There are three main questions that need to be answered to justify treatment for chronic Lyme disease. (1) Do chronic Lyme disease patients without treatment suffer from a low Quality of Life (QOL) than the general population? Four National Institute of Health (NIH) studies have shown that the answer to that question is yes [
114]. (2) Are the symptoms of chronic Lyme disease patients reduced because of antibiotic treatment? The answer to that question is yes [
115,
116,
117,
118,
119]. (3) Can an untreated chronic Lyme disease lead to premature death? The answer to that question is yes according to our previous CDC reference. There exist a few studies that show that the symptoms of chronic Lyme patients do not improve with antibiotics treatment. There exist at least two problems with these studies. (1) They usually treat chronic Lyme patients with monotherapy which again is not a recommended treatment. (2) They have used flawed statistical methods [
120]. Medical doctors should be able to use their professional expertise and in consultation with their patients determine the most appropriate treatment for patients.
A European study [
121] estimates the sensitivity of the Lyme disease test to 44%. Such number was found by analyzing the performance of eight different Lyme disease tests. 89 different blood samples were tested for each test manufacturer. The sample also included healthy controls. Another study [
122] that conducted a meta-analysis of the American scientific literature (eight scientific articles) regarding the performance of the Lyme disease test estimates the sensitivity of the Lyme disease test to 46% and the specificity to 99%. Because the blood tests that are used today by government health agencies to detect the human body’s production of antibodies against the
Borrelia bacteria’s antigens are so insensitive Lyme disease, today must be defined as a clinical diagnosis as correctly advocated by ILADS. If a patient has had a blood test that suggests a Lyme disease infection that is fine, but a positive blood test should not be a requirement for a diagnosis. A person that suspect a Lyme disease infection is today, unfortunately, better of tossing a coin and diagnosing themselves because the blood tests for Lyme disease today will miss most infections. Specific antibodies often cannot be found in patients with Lyme disease because of the bacteria ability to shift its antigens.
Testing cerebrospinal fluid instead of blood will not improve test sensitivity because the bacteria can still shift its antigens in cerebrospinal fluid which means that the probability of detecting specific antibodies in cerebrospinal fluid is not larger than in blood. Moreover, cerebrospinal fluid causes the bacteria to change its morphology from a spirochete form to a cyst from [
123]. If you only diagnose Lyme disease in patients that have specific antibodies in their blood or cerebrospinal fluid, you will miss most cases. To better understand Lyme disease testing let’s look at the confusion matrix [
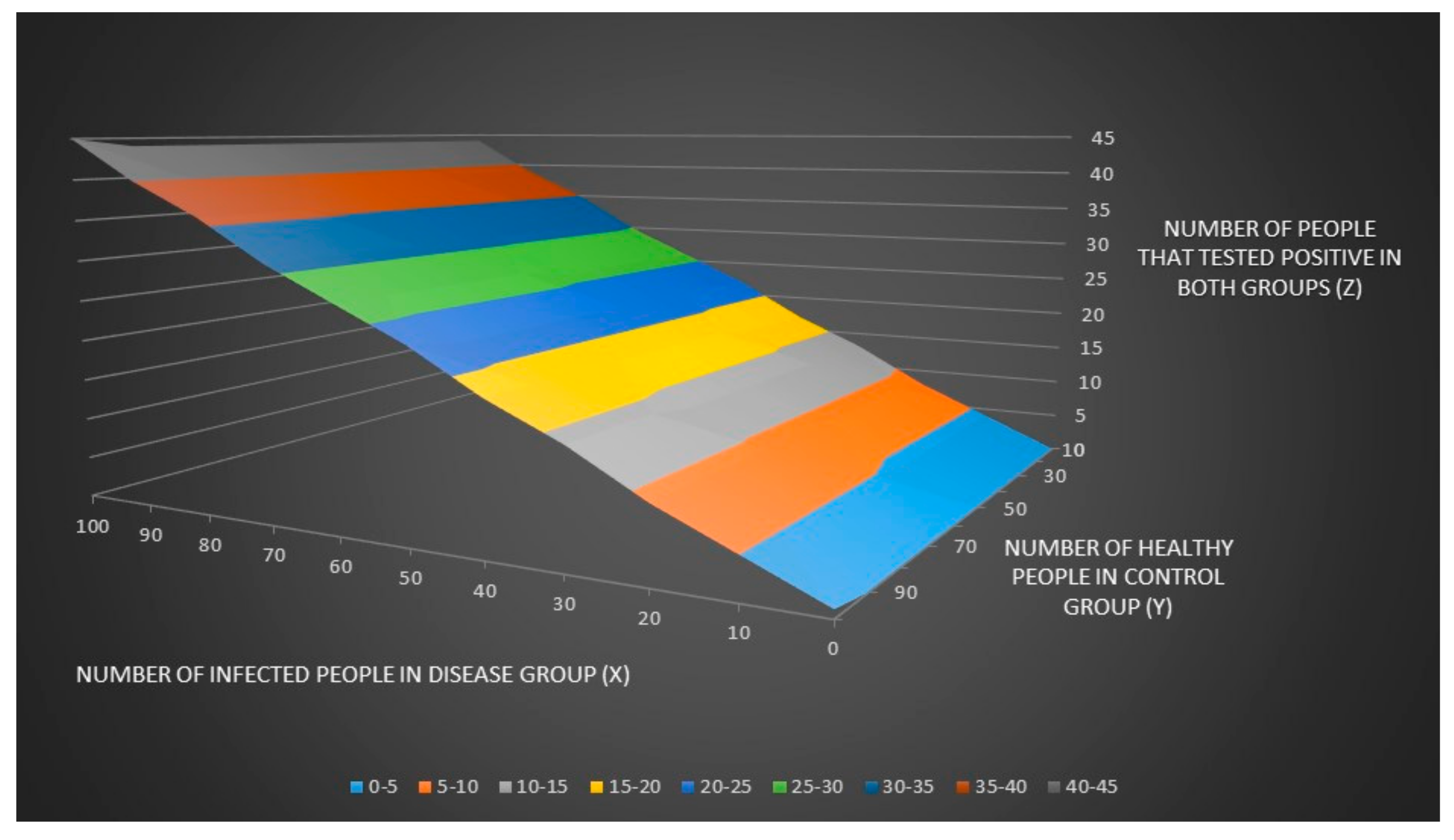
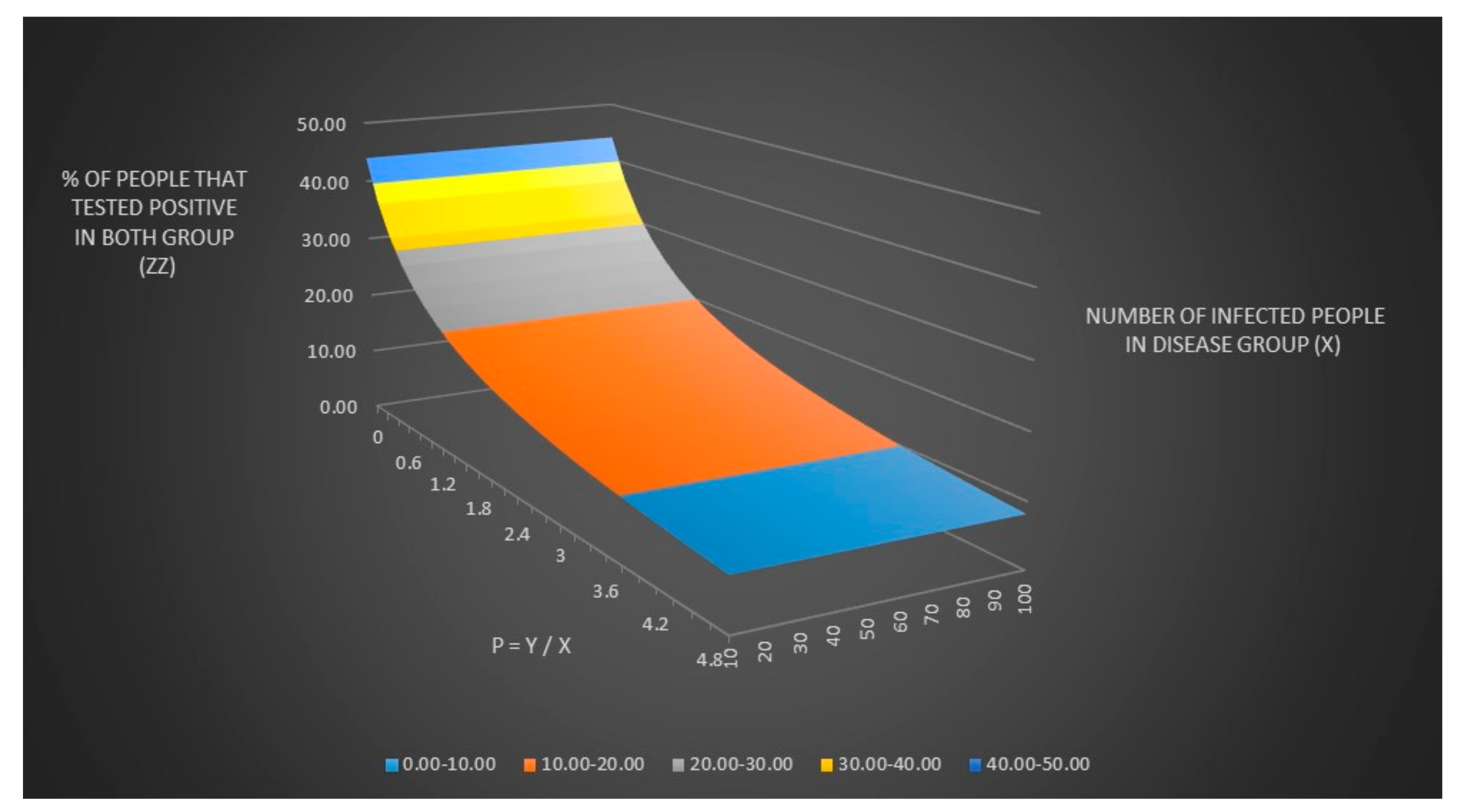
124]. All calculations can be found in the macro-enabled excel file “Lyme disease model.xlsm”. We assume in
Table 1 that the number of people in the disease and control groups are known and equal. In real life, however, we do not know the number of people in the disease and control group. We can only observe the total number of people that tested positive in both groups.
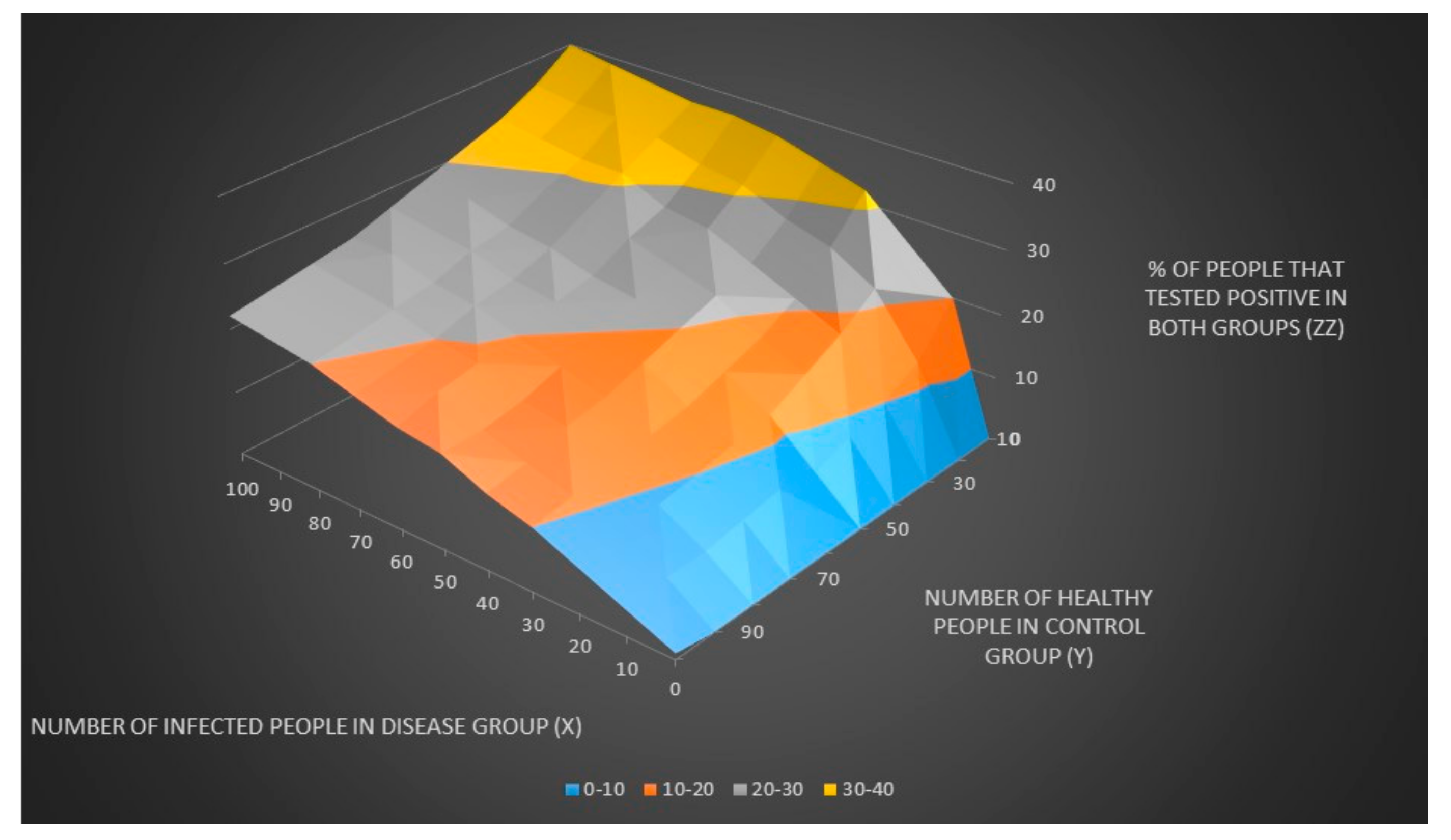
We can now plot the number of people that tested positive in both groups (z) and the % number of people that tested positive in both groups (zz) when the number of infected people in the disease group (x) and the number of healthy people in control groups (y) are unknown as seen in
Figure 1 and
Figure 2.
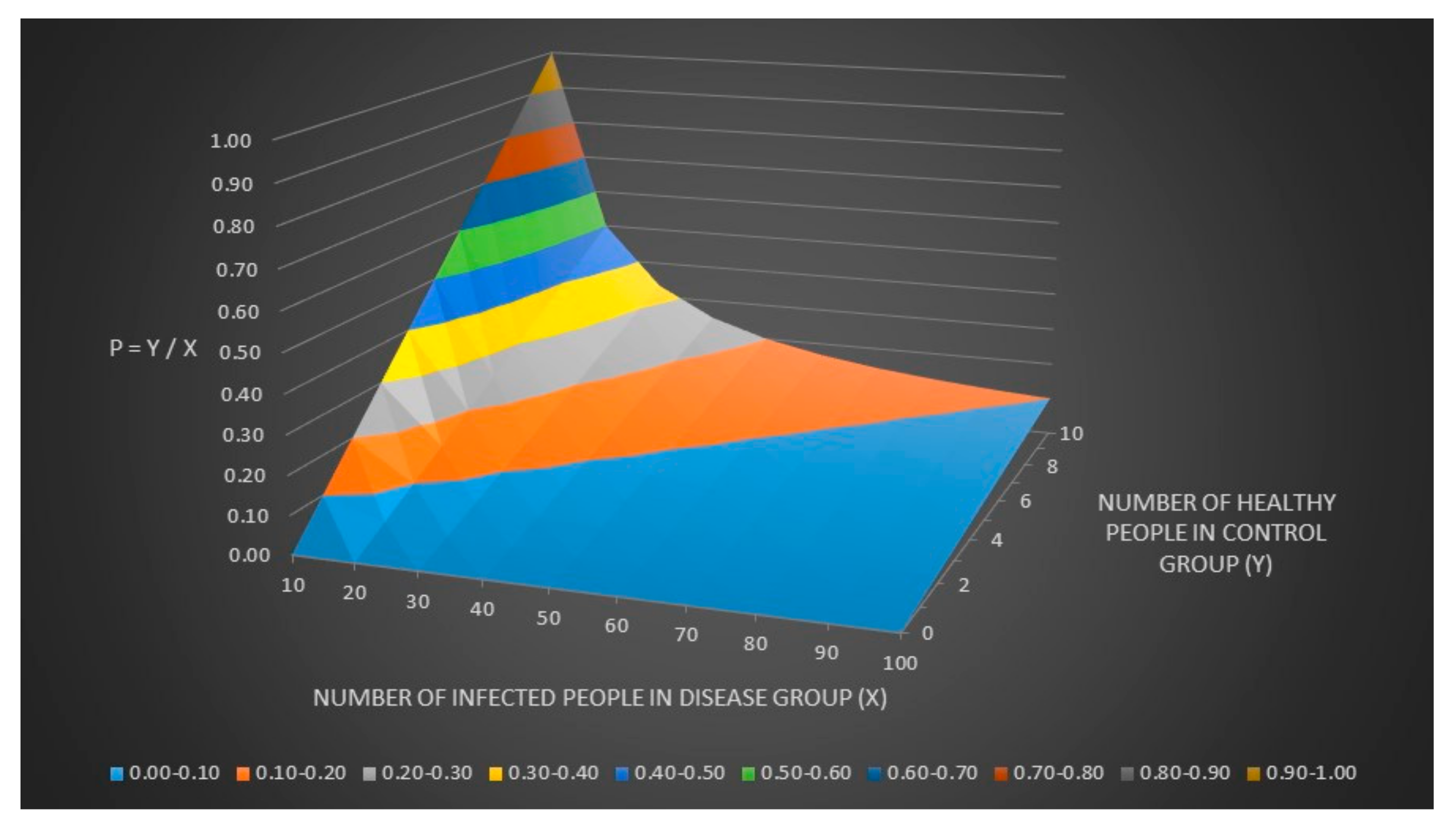
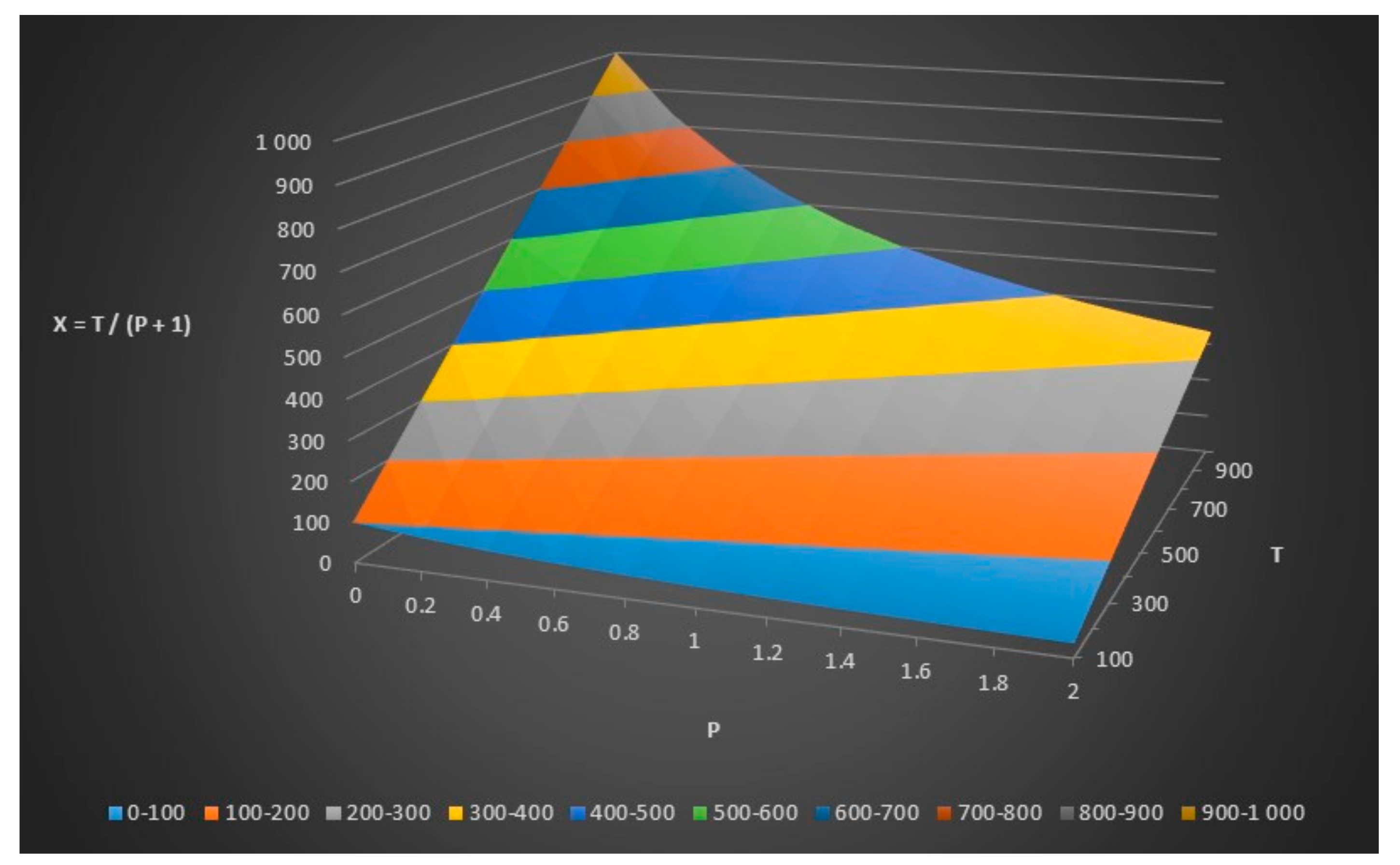
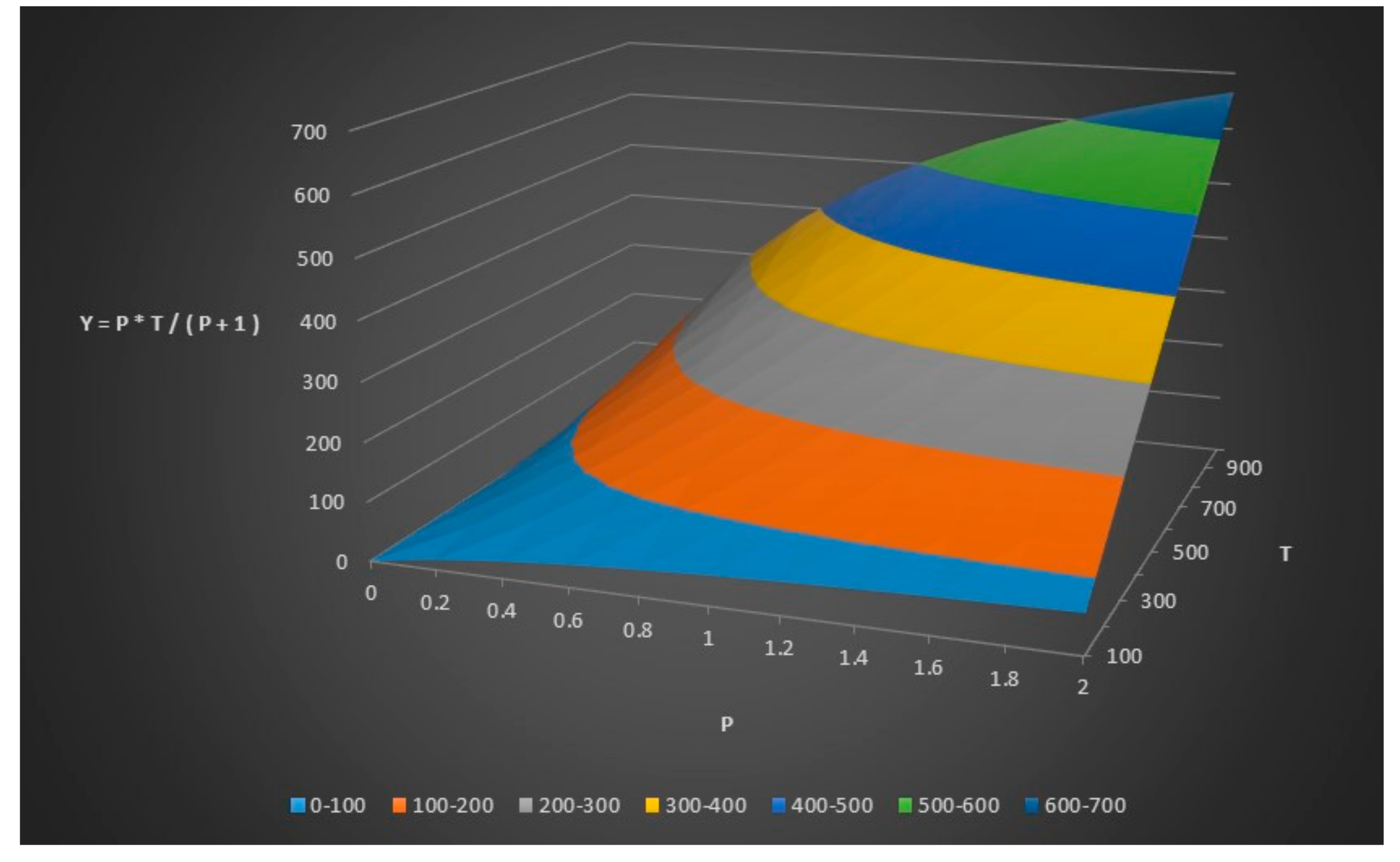
We can now assume that the number of healthy people in the control group (y) = p × the number of sick people in the disease group (x). The relationship between y, x and p can be seen in
Figure 3.
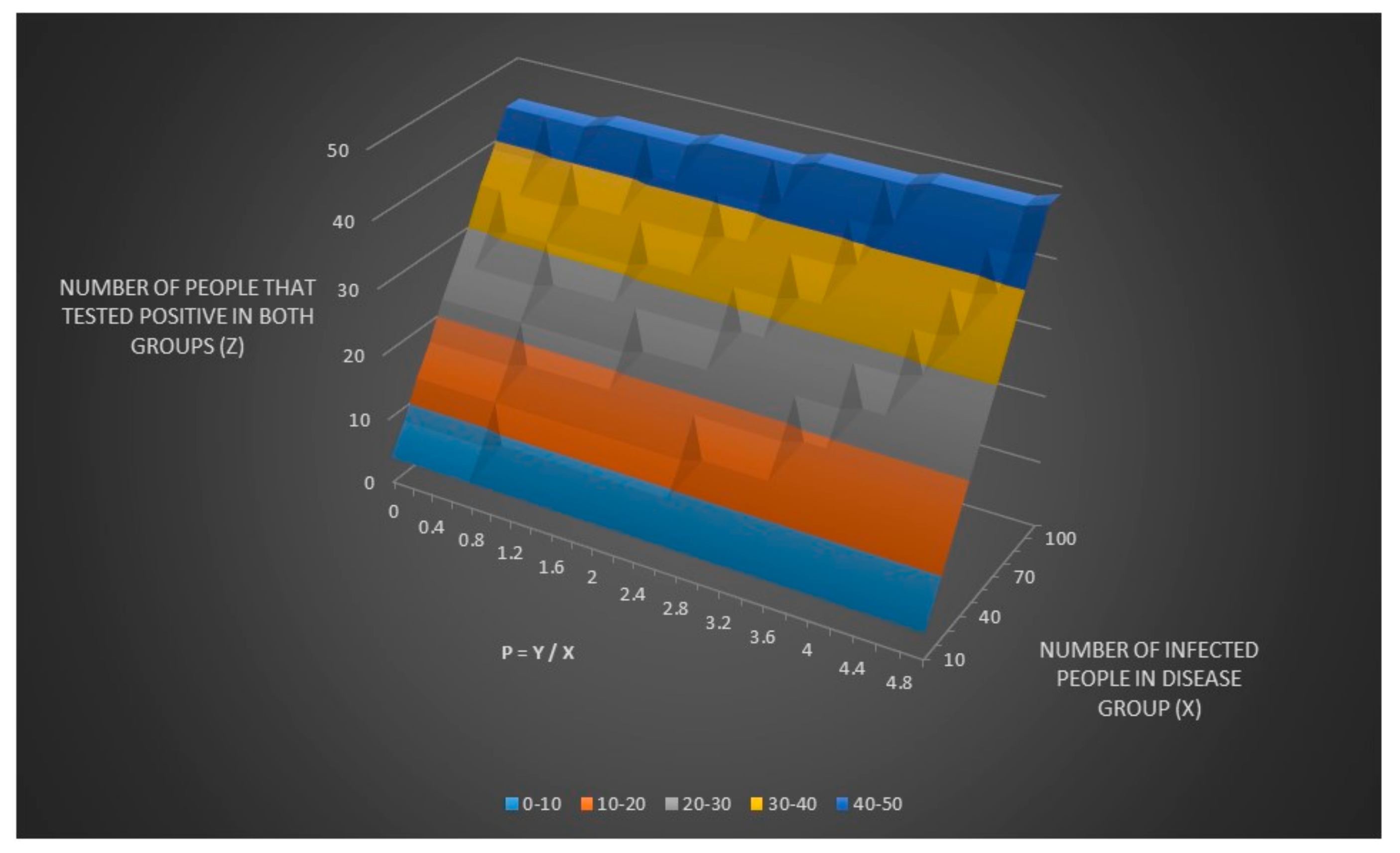
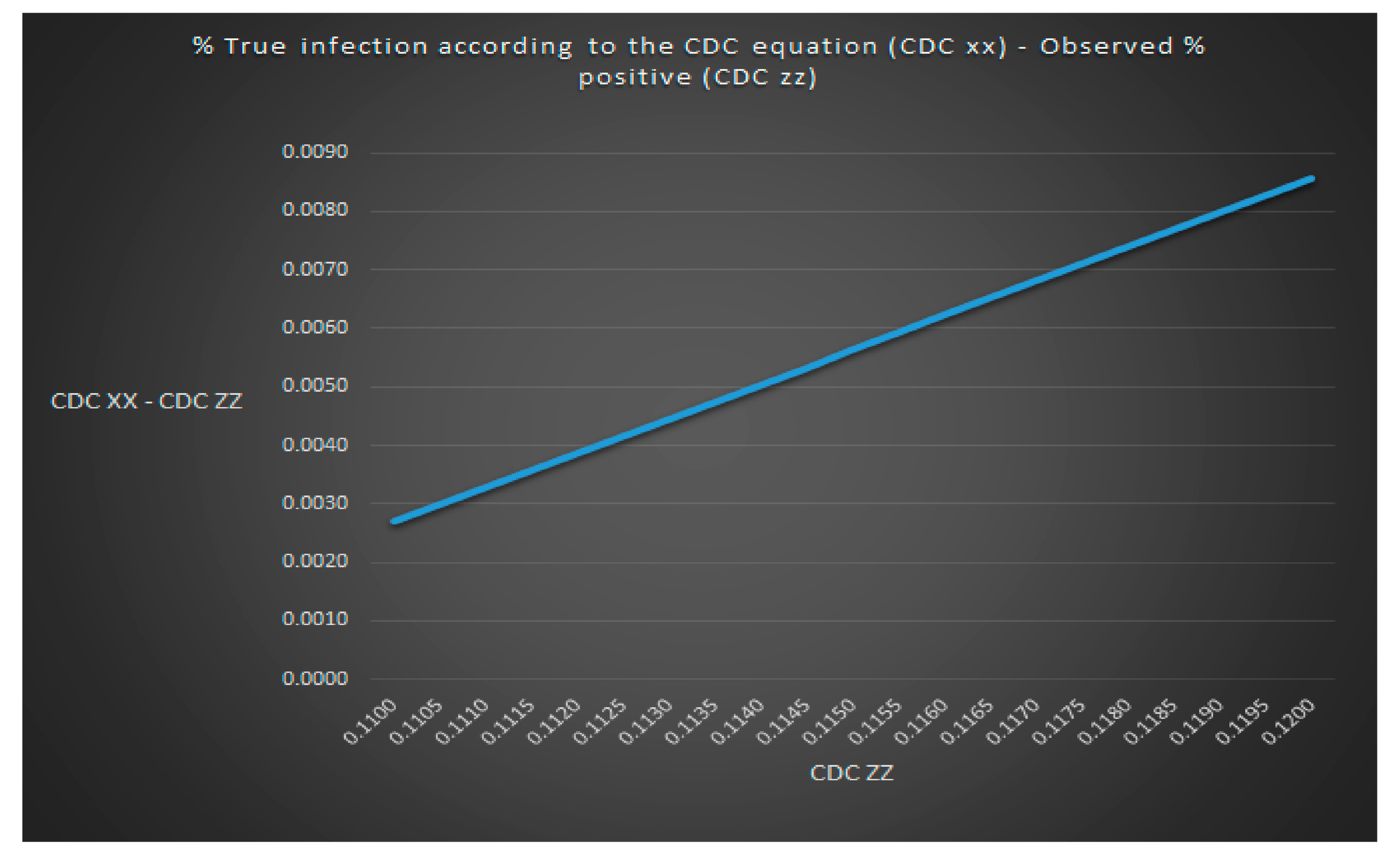
We now can adjust the equation for z and zz to include p as seen in
Figure 4 and
Figure 5. It can be hard to see in
Figure 5 (it is better to look in the excel file directly) but zz has the same value for all x values for any given value of p which means that you can never find a value for x (and a value for y thanks to y = x × p) only given values for se, sp, p and zz. I have also written a sub procedure in VBA called zzz() that also can be found in the excel file “Lyme disease model.xlsm” that can be called by simply pressing a button that calculates zz given a Lyme disease test sensitivity (se) equal to 0.44 and a Lyme disease test specificity of (sp) equal to 0.99.
We can now solve for the number of infected people in the disease group (x) and the number of healthy people in the control group (y) when they are unknown given a value for z with matrix algebra as seen in
Table 2.
We can algebraically manipulate the previous equations further as seen in
Table 3.
3. Results
According to one scientific study [
128], that can be found on the CDC website and published in
Clinical Infectious Diseases which is a “scientific” journal issued by the IDSA 2.4 million individual Lyme disease blood tests were done in the USA 2008. That number comes from a survey that was sent to seven of the largest commercial laboratories in the USA. The most interesting part of such publication an equation was not included in the article itself but was present in the supplementary data [
129]. The equation that the entire paper is based on is:
If we multiply the above equation by the number of individual Lyme disease blood tests that were performed in 2008 in the USA, then we get the observed number of Lyme disease infections in the USA in 2008 by the CDC.
We solve the first equation for % True infection.
If we multiply the above equation by the number of individual Lyme disease blood tests that were performed in 2008 in the USA, then we get CDC’s predicted number of Lyme disease infections in the USA in 2008.
The CDC study estimated three different scenarios: high, low and average with an assumed test sensitivity of 66.9% and assumed specificity of 96.1%. Unfortunately, the only value for observed % positive that the CDC provides was 11.89%, which was the average scenario. The other two are not reported in the paper and need to be calculated. Why is the observed % positive variable so important for our calculations later? The observed % positive value has not been adjusted for the sensitivity and specificity of the Lyme disease blood test. Therefore, we can use our values for sensitivity and specificity. The observed % positive values do also not include any assumptions about the relationship between the number of sick people in the disease group (x) and the number of healthy people in the control group (y) that we previously defined as p. The CDC calculations can be found in
Table 6.
We can see that the CDC has unrealistically and secretly assumed without motivation or explanation that the size of the control group with healthy people is 9 (low scenario), 8.5 (average scenario) and 4.4 (high scenario) times the size of the disease group with infected people (
p = 9,
p = 8.5 and
p = 4.4). These assumed
p-values cannot be empirically observed because it is impossible to know the value of p by simply looking at the total number of people that test positive in the control and disease group (z). It would be more realistic to assume that the size of the control group with healthy people is the same size as the disease group with infected people (
p = 1). Because blood testing today is so primitive (you can more or less only test for one pathogen at the time) and because the blood tests for Lyme disease are so insensitive most people today will only test to get a confirmation that they are infected. Hence, many people will only test if they are infected. It is therefore unrealistic to expect that a lot of people without an infection will demand to get tested just for “fun” because there is also a personal financial cost involved. The CDC also claims in their paper that the value of the variable observed % positive was the same as the value for the variable predicted % positive for the average scenario which is mathematically impossible as seen in
Figure 8 using the same assumptions regarding Lyme disease test sensitivity and specificity as the CDC. Such claim by the CDC, therefore, does not make any sense.
We can now evaluate whether the CDC equation is correct and compare the CDC model with my model as seen in
Table 7.
Given the CDC unrealistic assumptions regarding se, sp and p, it appears that the equation is more or less correct. There is, however, an unexplained difference of +418 infections for the high scenario. We can also see that if the CDC had assumed that
p = 1 in combination with the CDC assumptions se = 0.669, sp = 0.961, then the number of Lyme disease infections in the USA for 2008 for the high scenario would have been 527,288 instead of 444,000. We can also see that the difference between the CDC model with CDC assumptions of se = 0.669, sp = 0.961, p(low) = 9, p(average) = 8.5 and p(high) = 4.4 and my model with my assumptions of se = 0.44, sp = 0.99 and
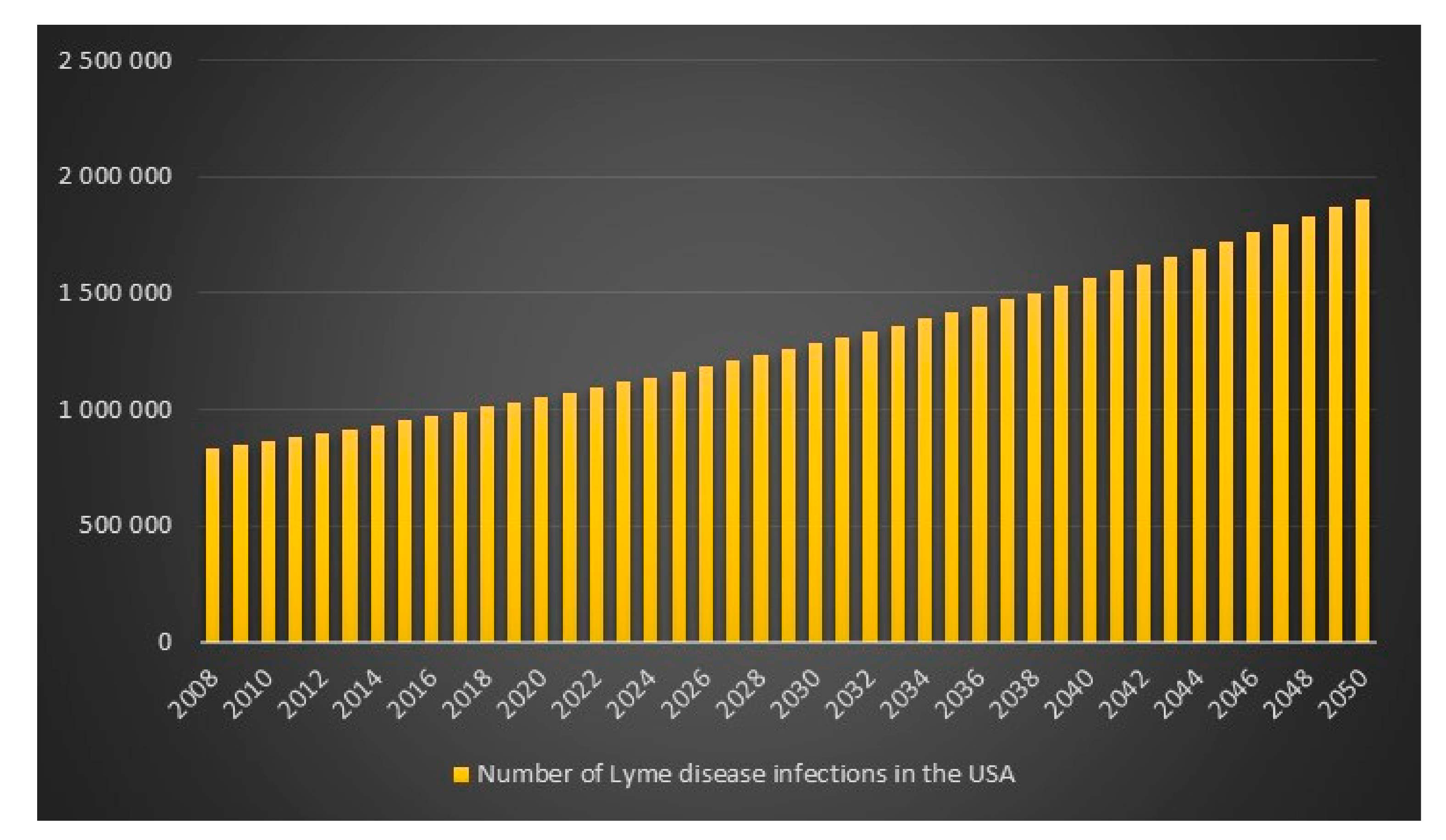
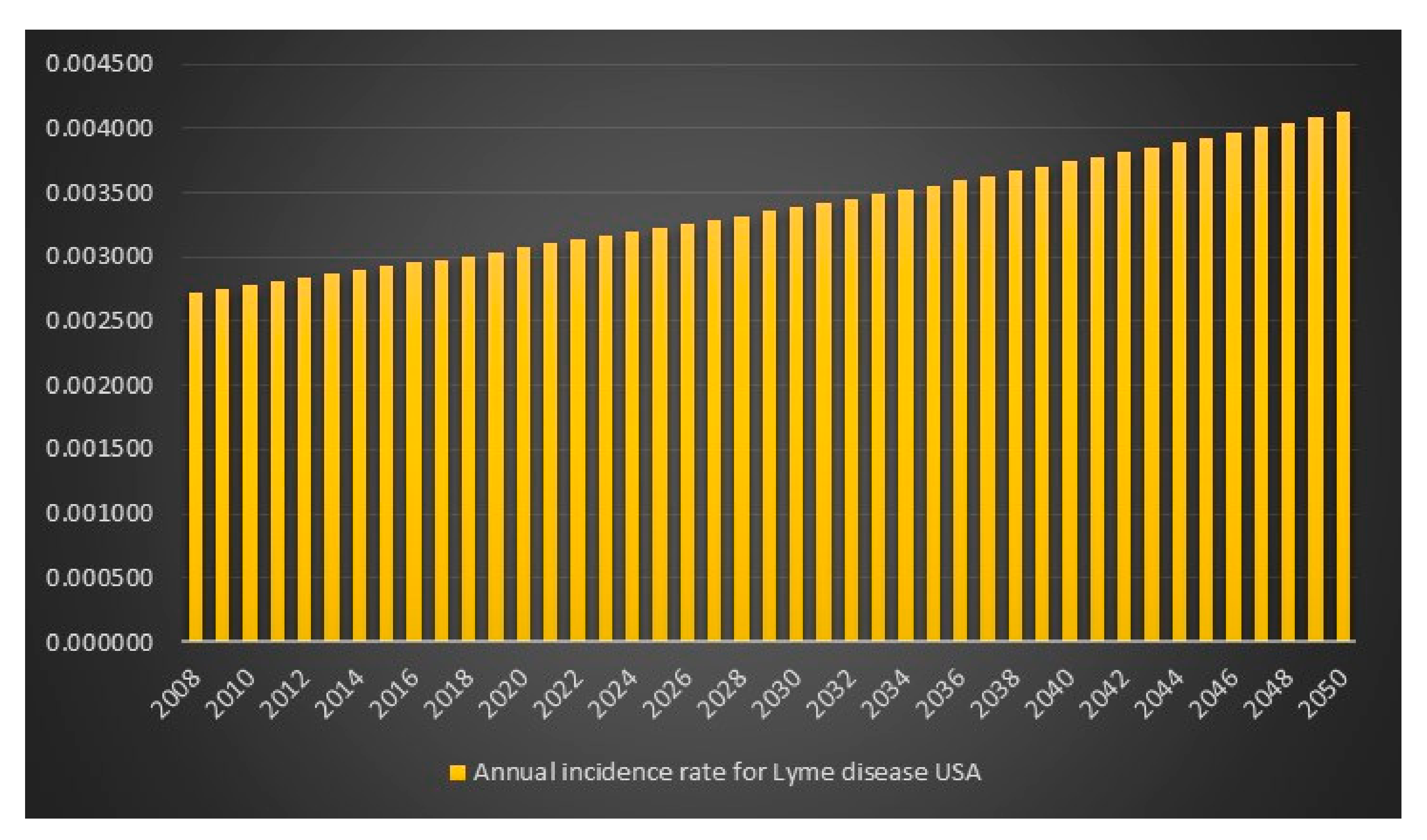
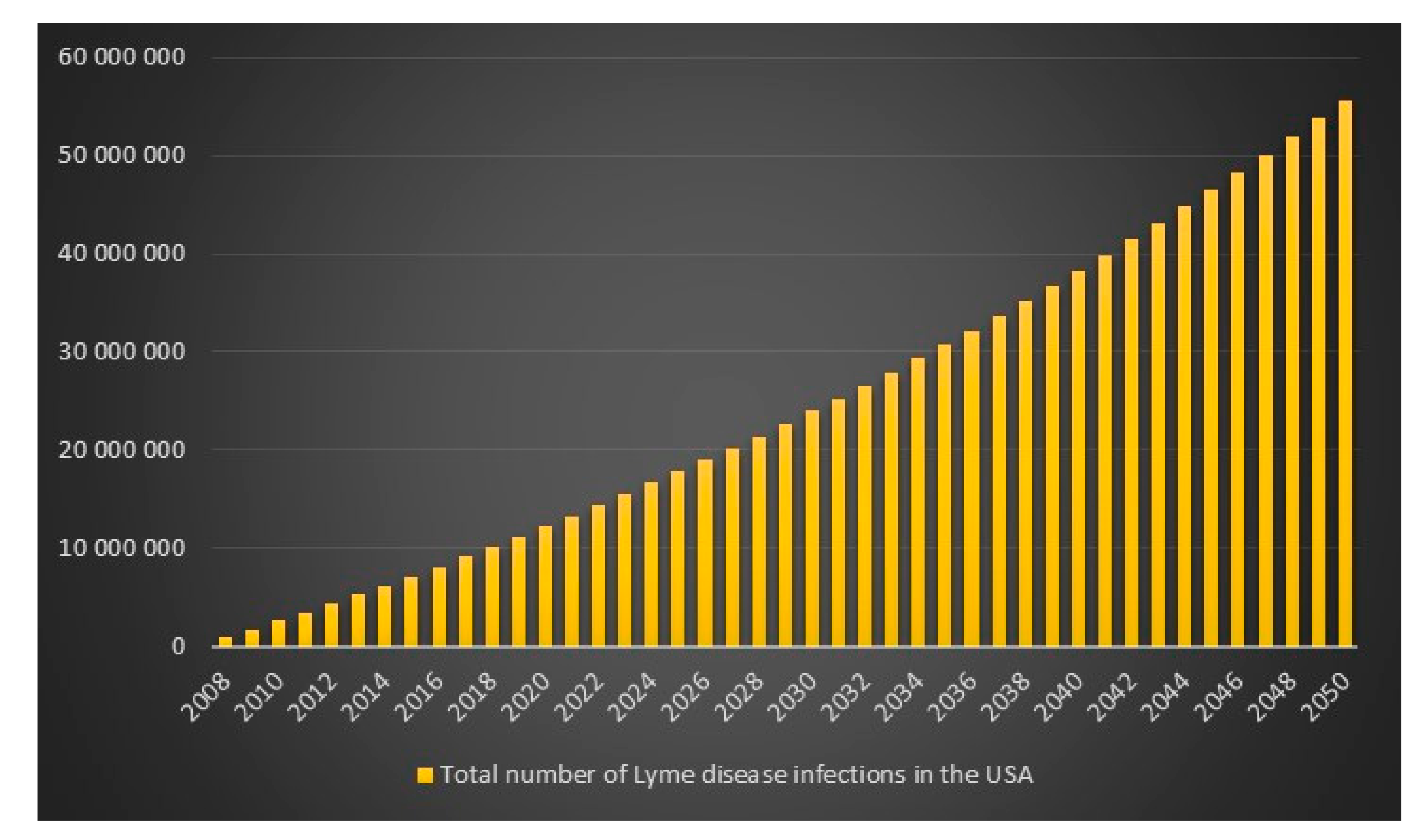
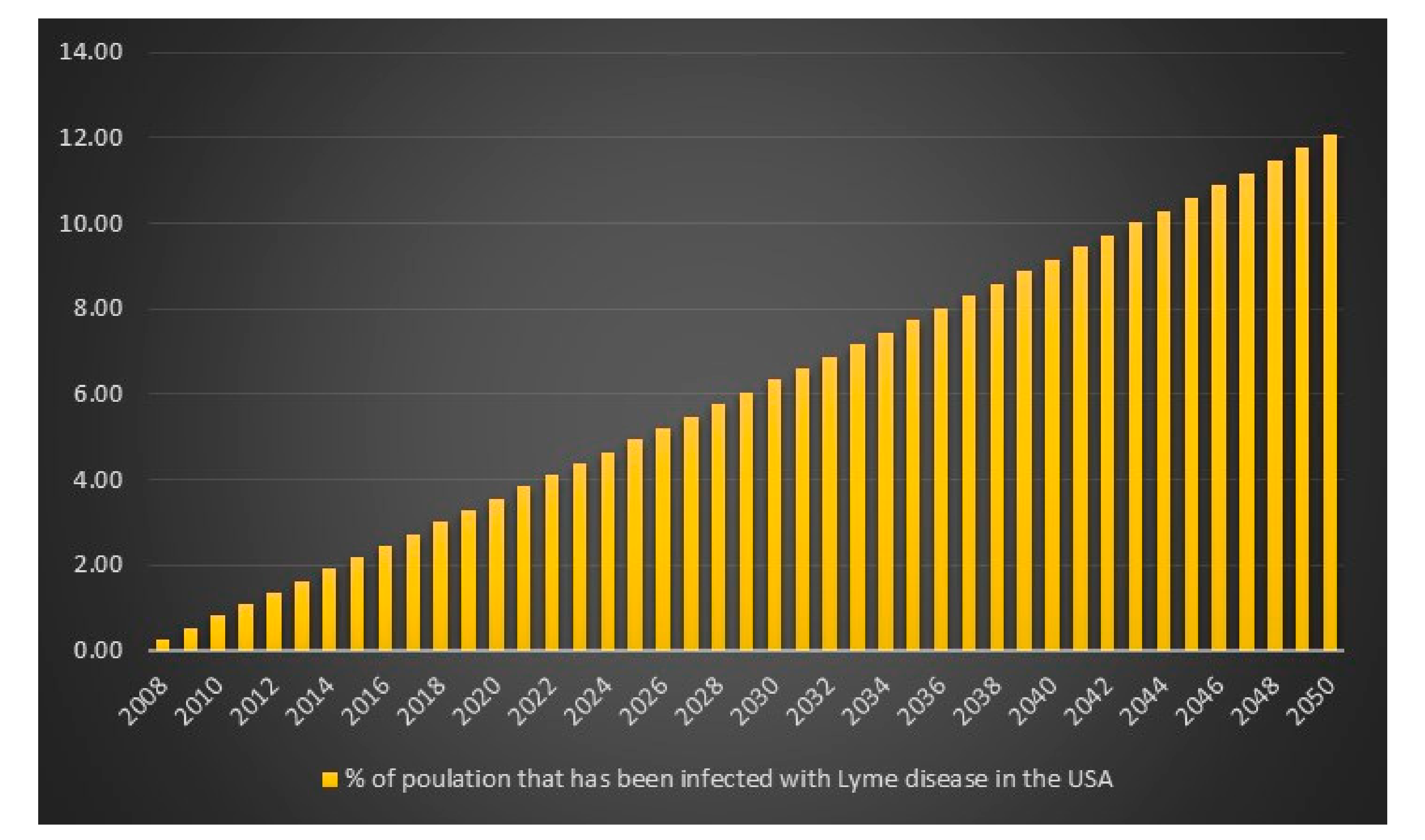
p = 1 is lowest for the CDC high scenario hence I will report that in 2008 in the USA the estimated number of Lyme disease infections is 829,600. The data and calculations that I will present now can be found in the excel file “Lyme disease calculations.xlsx”. Given 829,600 Lyme disease infections in 2008 in the USA and an assumed annual infection growth rate of 2% then in 2018 in the USA approximately 1 million people will get infected with Lyme disease. The total number of Lyme disease infections that we can expect in the USA from 2008 to 2050 is 55.7 million. Given an annual population growth rate in the USA of 1% and given that everyone that is infected from 2008 to 2050 is still alive than 12% of the population in the USA will have been infected with Lyme disease in 2050. The plots are presented in
Figure 9,
Figure 10,
Figure 11 and
Figure 12.
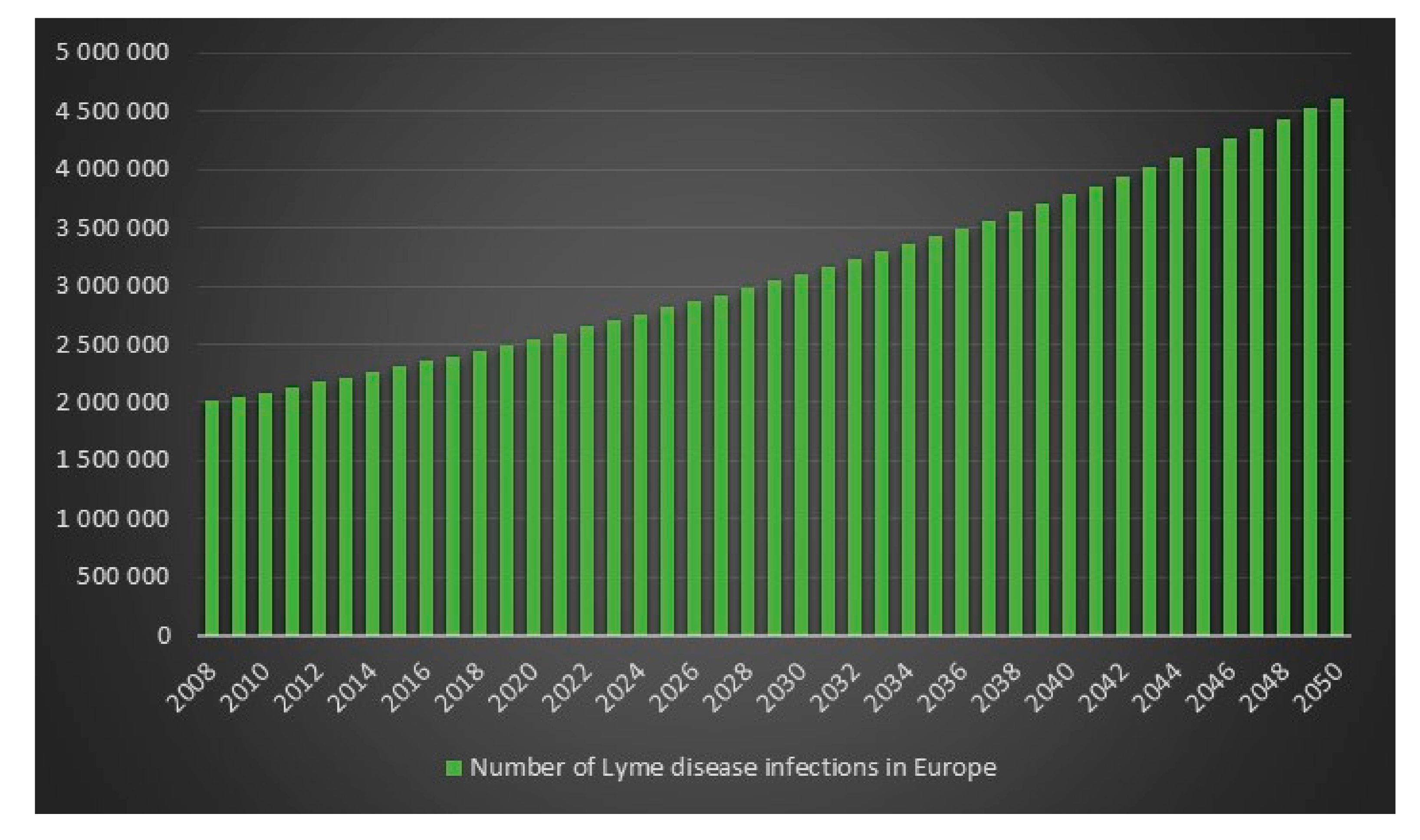
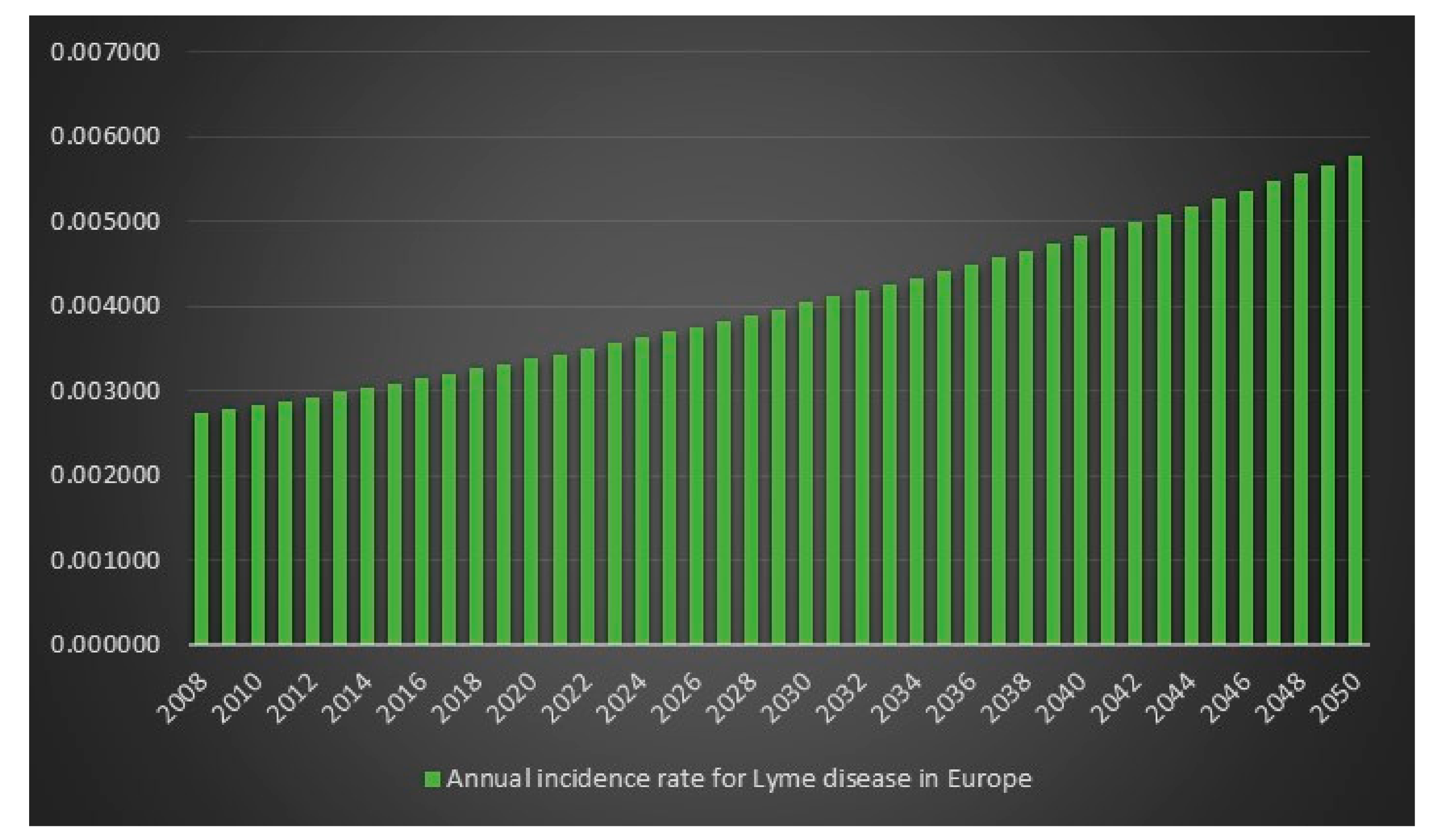
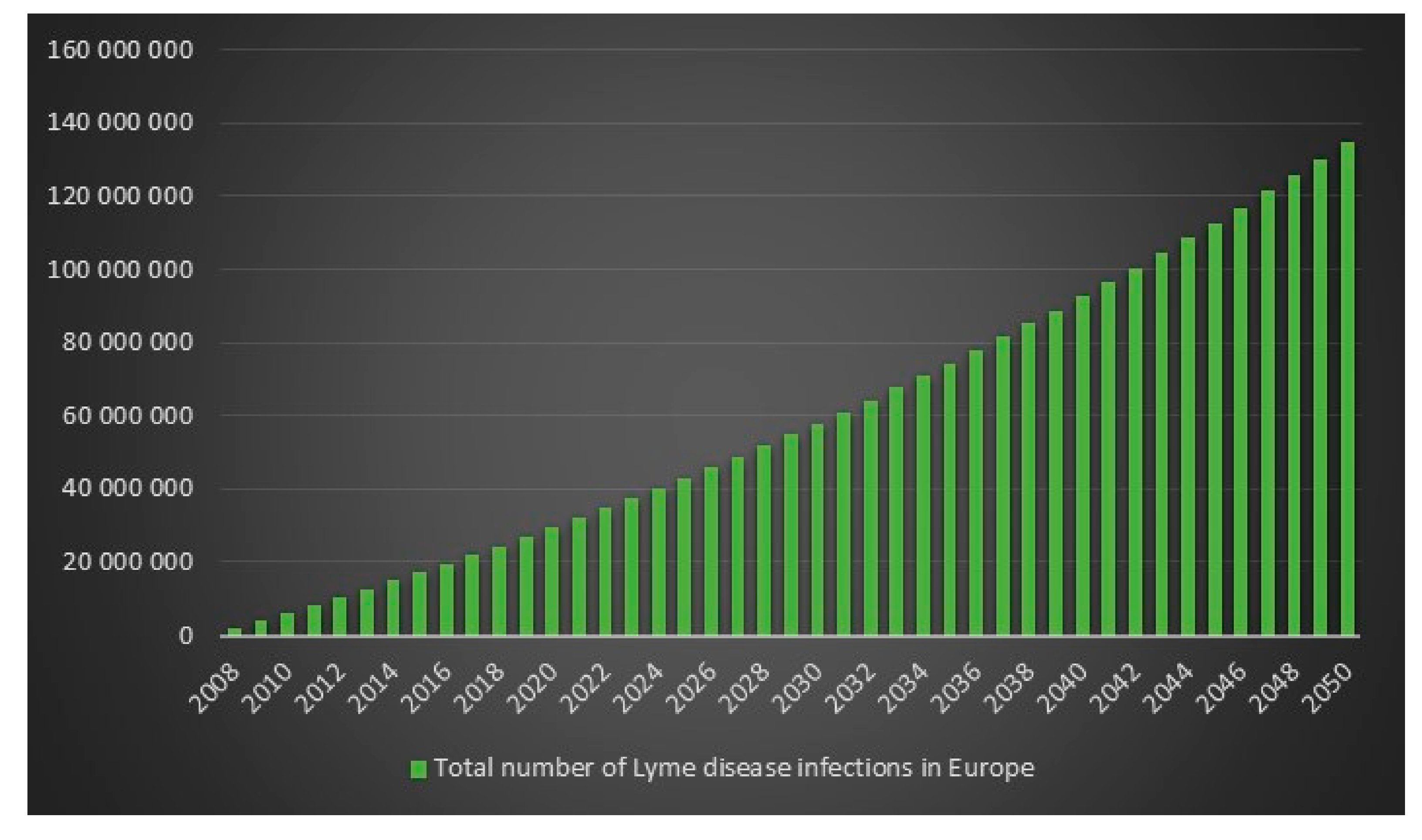
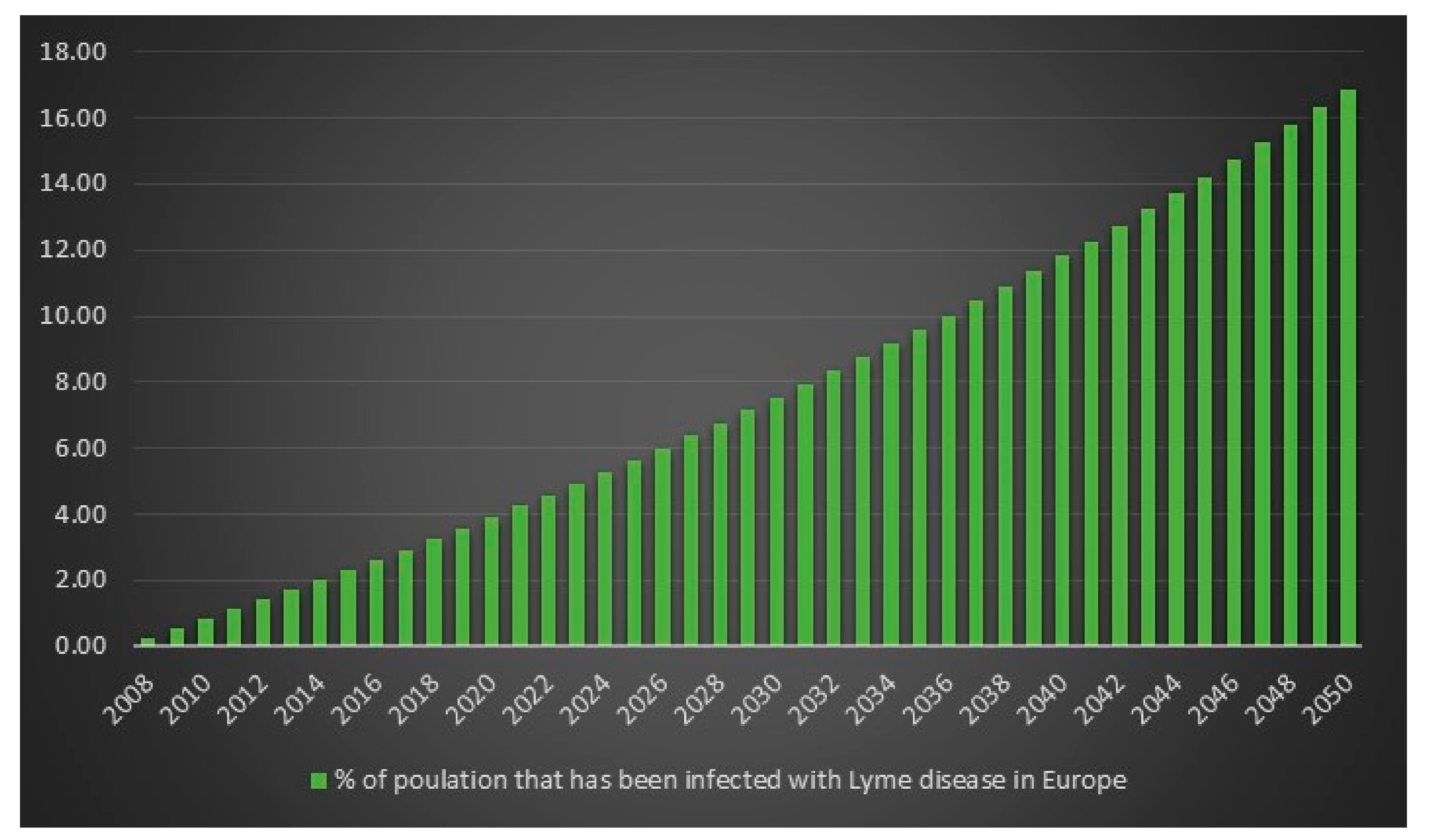
Since the ECDC does not have any statistics on how frequent Lyme disease is in Europe, it is difficult to determine an exact figure for the number of Lyme disease cases in Europe in 2008. However, we can use the incidence rate (frequency) from the USA for 2008 on Europe’s population for 2008 to get an estimate. The estimated number of Lyme disease infections in Europe in 2008 is 2,008,505. Given 2,008,505 Lyme disease infections in 2008 in Europe and an assumed annual infection growth rate of 2% then in 2018 in Europe approximately 2.4 million people will get infected with Lyme disease. The total number of Lyme disease infections that we can expect in Europe from 2008 to 2050 is 134.9 million. Given an annual population growth rate in Europe of 0.2% and given that everyone that is infected from 2008 to 2050 is still alive than 17% of the population of Europe will have been infected with Lyme disease in 2050. The plots are presented in
Figure 13,
Figure 14,
Figure 15 and
Figure 16.
According to our previous scientific reference, 63% of people that are infected with
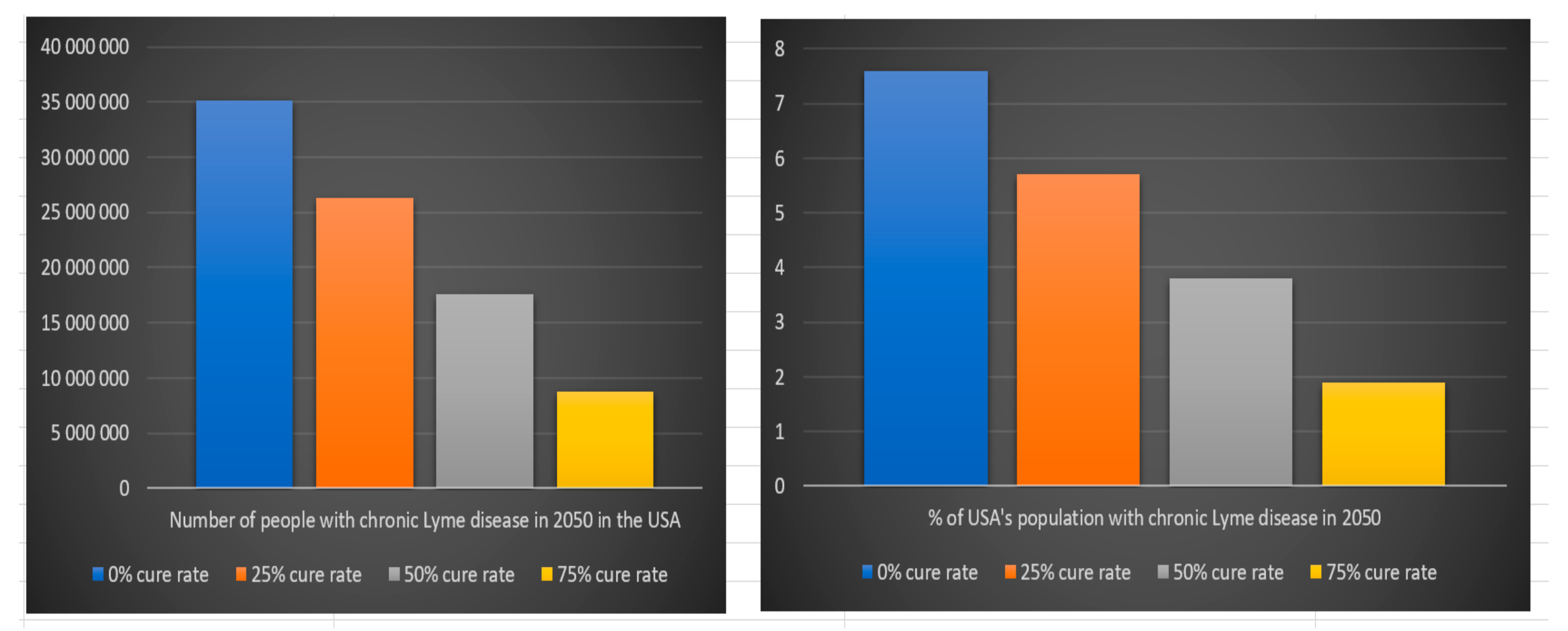
Borrelia develop chronic Lyme disease. The estimated number of people suffering from chronic Lyme disease in 2050 in the USA and Europe depend on the assumption we make regarding the estimated cure rate for chronic Lyme disease treatment and on the assumption that everyone that develop chronic Lyme disease from 2008 to 2050 is still alive. The last assumption is very uncertain because of how difficult it is today for chronic Lyme patients to get treatment. We can see in
Table 8 and
Figure 17 that the number of people that will suffer from chronic Lyme disease in 2050 in the USA with a 0% cure rate is approximately 35 million (8% of the USA population in 2050), with a 25% cure rate 26 million (6% of the USA population in 2050), with a 50% cure rate 18 million (4% of the USA population in 2050), with a 75% cure rate 9 million (2% of the USA population in 2050) and with a 100% cure rate zero (0% of the USA population in 2050).
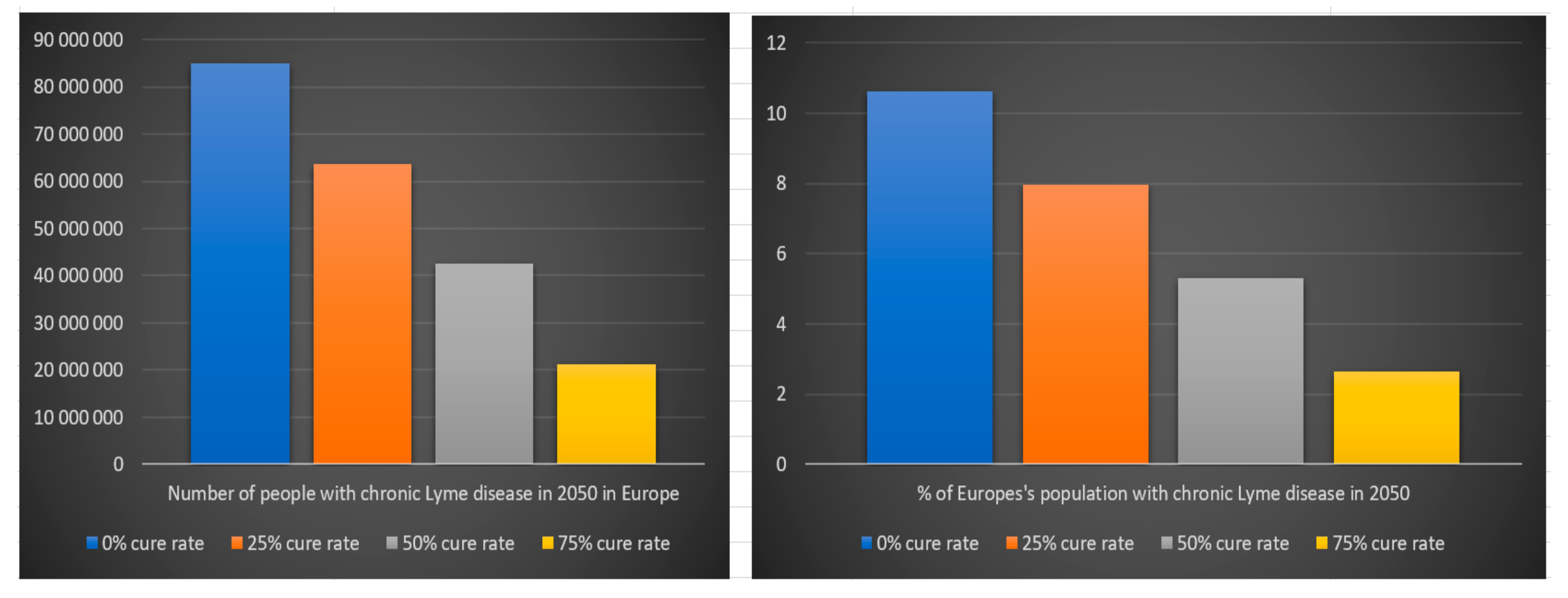
We can see in
Table 9 and
Figure 18 that the number of people that will suffer from chronic Lyme disease in 2050 in Europe with a 0% cure rate is approximately 85 million (11% of Europe’s population in 2050), with a 25% cure rate 64 million (8% of Europe’s population in 2050), with a 50% cure rate 42 million (5% of Europe’s population in 2050), with a 75% cure rate 21 million (3% of the Europe’s population in 2050) and with a 100% cure rate zero (0% of Europe’s population in 2050).
If 2,008,505 people were infected with Lyme disease in Europe in 2008 and go undetected by the non-exist statistics what types of illnesses can Lyme disease patients be misdiagnosed with? It is therefore not unrealistic to assume that some Lyme disease patients are misdiagnosed with illnesses such as for example fibromyalgia, chronic fatigue syndrome (CFS), heart arrhythmia, multiple sclerosis (MS), restless legs syndrome (RLS), amyotrophic lateral sclerosis (ALS), Parkinson disease, systemic lupus erythematosus (SLE), Gulf War Syndrome (GWS) or Alzheimer’s disease. The commonality between these diseases is that there is currently no known cure. Before we can start to estimate costs for Lyme disease, we need to discuss the tax on disability benefits. The tax rate on disabilities benefits is approximately 50% of the tax rate on income from work [
130,
131]. However, the tax on disability benefits is irrelevant to the government because assuming the government keeps the amount of disability benefit after tax fixed an increased tax rate on disability benefits will not increase the government’s financial balance (government revenues + government costs) as seen in
Table 10. If a government raises the tax rate on a person’s disability benefit, then the increased tax revenues from such tax raise are completely offset by the larger government cost for the disability benefit.
We can now estimate the costs for Lyme disease treatment in the USA and Europe for the year 2018. We have previously estimated that the number of infections in the USA for 2018 is approximately 1 million. In Europe, that number is approximately 2.4 million. Let’s assume that in the USA for 2018 the annual cost for oral antibiotics is 1400 USD and the annual cost for IV antibiotics is 15,000 USD. In Europe, the estimated annual cost for oral antibiotics is 1200 EUR and the annual cost for IV antibiotics is 13,000 EUR. Currently, the treatment cost for IV antibiotics for chronic Lyme disease are paid by the individual and not by the government or insurance companies. Note that the cost of IV treatment for chronic Lyme disease can be different in the USA and Europe because in the USA a peripherally inserted central catheter (PICC) is preferred while in Europe an IV drip is preferred. The cost for IV treatment in Europe could easily be twice as large because patients must travel a long way and stay at a hotel close to a specialized chronic Lyme disease clinic to get daily IV treatments with a butterfly needle. Sometimes people are even forced to sell their house to afford treatment. We assume that acute Lyme disease is treated with oral antibiotics for one month and that chronic Lyme disease is treated with IV antibiotics for six months or one year. Chronic Lyme disease can also be treated with oral antibiotics but then the patient runs the risk of having to take oral antibiotics for the rest of his/her life. I have therefore not calculated the cost of treating chronic Lyme with oral antibiotics since its more realistic to assume that all chronic Lyme patients want to treat with IV antibiotics because then they will at least have a chance of getting cured of their “chronic” infection. We can see in
Table 11 and
Table 12 that the estimated treatment cost for Lyme disease for 2018 for the USA is somewhere between 4.8 billion USD and 9.6 billion USD and for Europe somewhere between 10.1 billion EUR and 20.1 billion EUR depending on the assumptions we make regarding the length of treatment with IV antibiotics (six months vs. one year). We can also see that the cost of treating acute Lyme disease with oral antibiotics for one month only represents 0.6% of the average treatment cost for IV antibiotics. The cost of treating acute Lyme disease with oral antibiotics is so small that it barely has an impact on total treatment costs.
We have so far only looked at treatment cost. Many people are forced to leave their jobs due to the infection. So, the cost of lost personal income is also high. According to one study, approximately 42% of chronic Lyme disease patients cannot work [
132]. I believe that the number is even higher but 42% is reasonable enough. The financial cost for both the individual (lost earnings from not working due to chronic Lyme disease) and for the government (lost tax revenues because chronic Lyme patients are not working and disability benefits for chronic Lyme disease patients) are therefore significant. We can now calculate the government cost for chronic Lyme disease for the USA and Europe for 2018 if governments do not finance treatment. According to the Organisation for Economic Co-Operation and Development (OECD) the average annual wage rate before tax for 2016 for the USA was 60 154 USD and for Germany 38,302 EUR [
133]. The average annual wage rate in Germany represents the average annual wage rate for Europe. The global accounting firm KPMG states that the income tax rate for 2016 for the USA is 39.6% and for Germany 45% [
134]. A website called disabilitysecrets.com [
135] claims that the average monthly Social Security Disability Insurance (SSDI) payment after tax for the USA for 2017 is 1171 USD which means that the average annual disability benefit after tax for the USA for 2017 is 14,052 USD. This amount is on par with the lowest monthly disability payment after taxed paid in Sweden which is 11,000 Swedish kroner [
136] which means that the minimum annual disability benefit after tax for Sweden is 132,000 Swedish kroner which as of October 2017 is approximately 13,778 EUR. We will use the monthly Swedish disability payment to represent the disability payment in Europe.
We can see in
Table 13 and
Table 14 that the estimated lost personal income for chronic Lyme patients that are not working for 2018 for the USA is 16.1 billion USD and in Europe 24.8 billion EUR. If the governments in the USA and Europe do not finance IV treatment with antibiotics for chronic Lyme disease, then the estimated government costs for chronic Lyme disease (lost tax revenues because some chronic Lyme patients are not working plus disability benefits for chronic Lyme patients that not working) for 2018 for the USA is 10.1 billion USD and for Europe 20.1 billion EUR. We can also see that the government cost for chronic Lyme disease for 2018 (which does not include treatment costs) in the USA is 2.1 times larger than the cost for 6 months of IV treatment with antibiotics in the USA for 2018 and 1.1 times larger than the cost for 1 year of IV treatment with antibiotics in the USA for 2018. In Europe, the government cost for chronic Lyme disease for 2018 is two times larger than the cost for six months of IV treatment in Europe for 2018 and the government cost is on par with the cost for one year of IV treatment in Europe for 2018.
Today’s and future government revenues and costs for chronic Lyme disease are however much more important to look at than historical annual cost. We will again treat the cure rate for IV antibiotics for chronic Lyme disease as an unknown. We will calculate variables for five different scenarios: A cure rate of 0%, a cure rate 25%, a cure rate of 50%, a cure rate of 75% and a cure rate of 100%. The number of chronic Lyme patients that are cured with treatment/not cured with treatment and are working/not working can be seen in
Table 15.
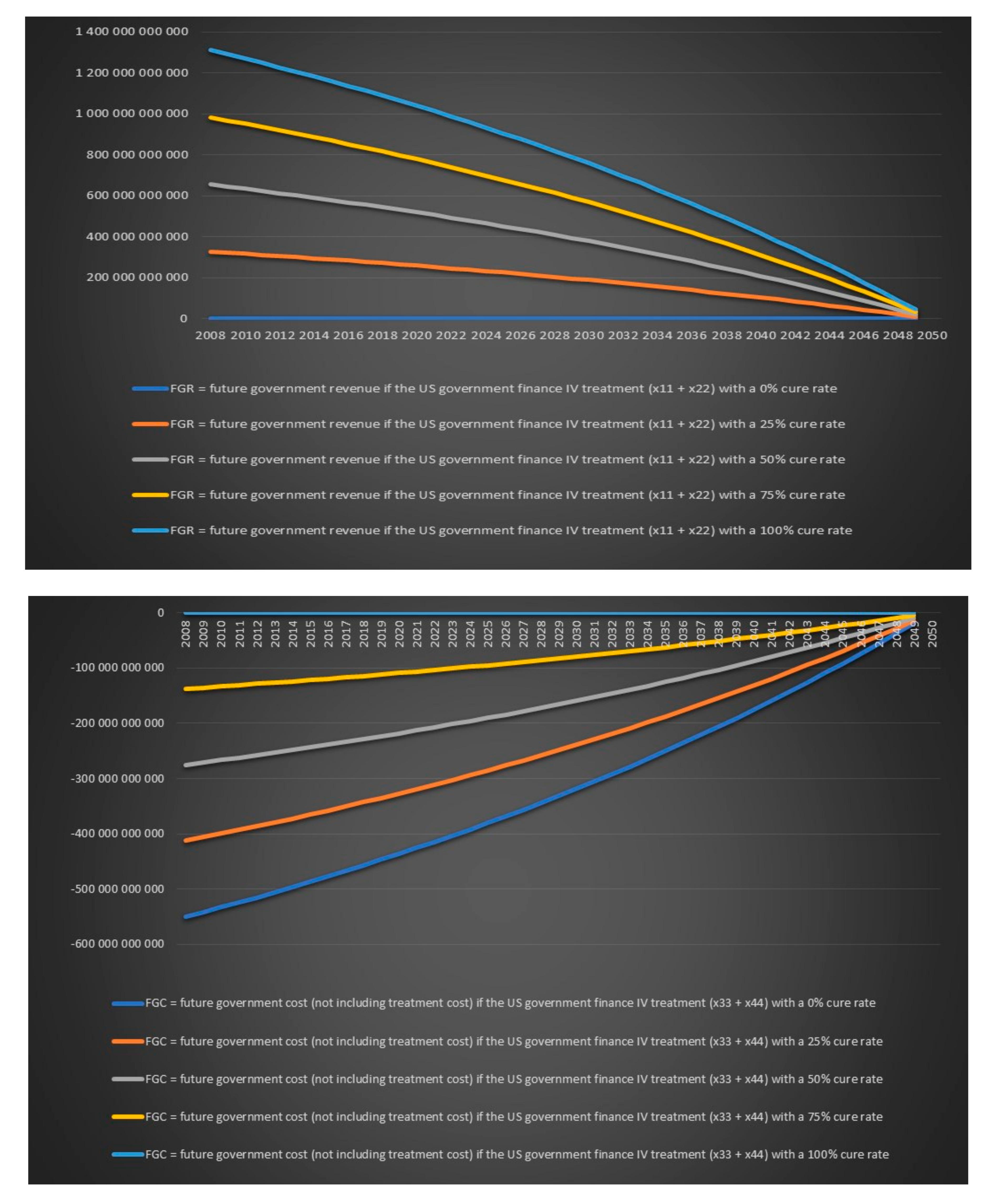
Now we need to answer the important question: should a government pay for IV treatment for chronic Lyme disease? From a purely economic and financial perspective which excludes any ethical aspect of not offering antibiotics treatment to patients that suffer from a bacterial infection that can lead to death a government should finance treatment with IV antibiotics for chronic Lyme disease if
where government revenues are positive values and government costs are negative values. Such governments’ financial chronic Lyme disease balance sheet is presented in
Table 16.
Note also that the previous equation become less reliable over time. The closer we get to our endpoint which is 2050 the less impact the future government revenues and future government expenditures will have on a government's financial balance. Note that tax revenues from chronic Lyme patients that are not cured with treatment and working, saved disability benefits from chronic Lyme patients that are not cured with treatment and working, tax revenues from chronic Lyme patients that are sick and have not received treatment and are working and saved disability benefits from chronic Lyme patients that are sick and have not received treatment and are working are not included in the above government financial chronic Lyme disease balance sheet because they will be the same regardless of if the government choose to treat or not. The government’s purely financial treatment decision regarding chronic Lyme disease is further illustrated in
Table 17.
We now again assume that the annual growth rate of the infection is 2% per year, the annual population growth rate in the USA is assumed to be 1% and the annual population growth rate in Europe is assumed to be 0.2%. We assume that we treat all chronic Lyme patients with IV antibiotics for either six months or one year and we again look at the value for different variables for five different cure rates 0%, 25%, 50%, 75% and 100%. All charts in this section and more can be found in the Excel file “Lyme disease calculations.xlsx”. There will be only four individual group captions in this section: today’s government costs and revenues in the USA over time, future government costs and revenues in the USA over time, today’s government costs and revenues in Europe over time and future government costs and revenues in Europe over time. There is no point in including a caption for each chart when the same text can be found in the chart’s legend. We can see in
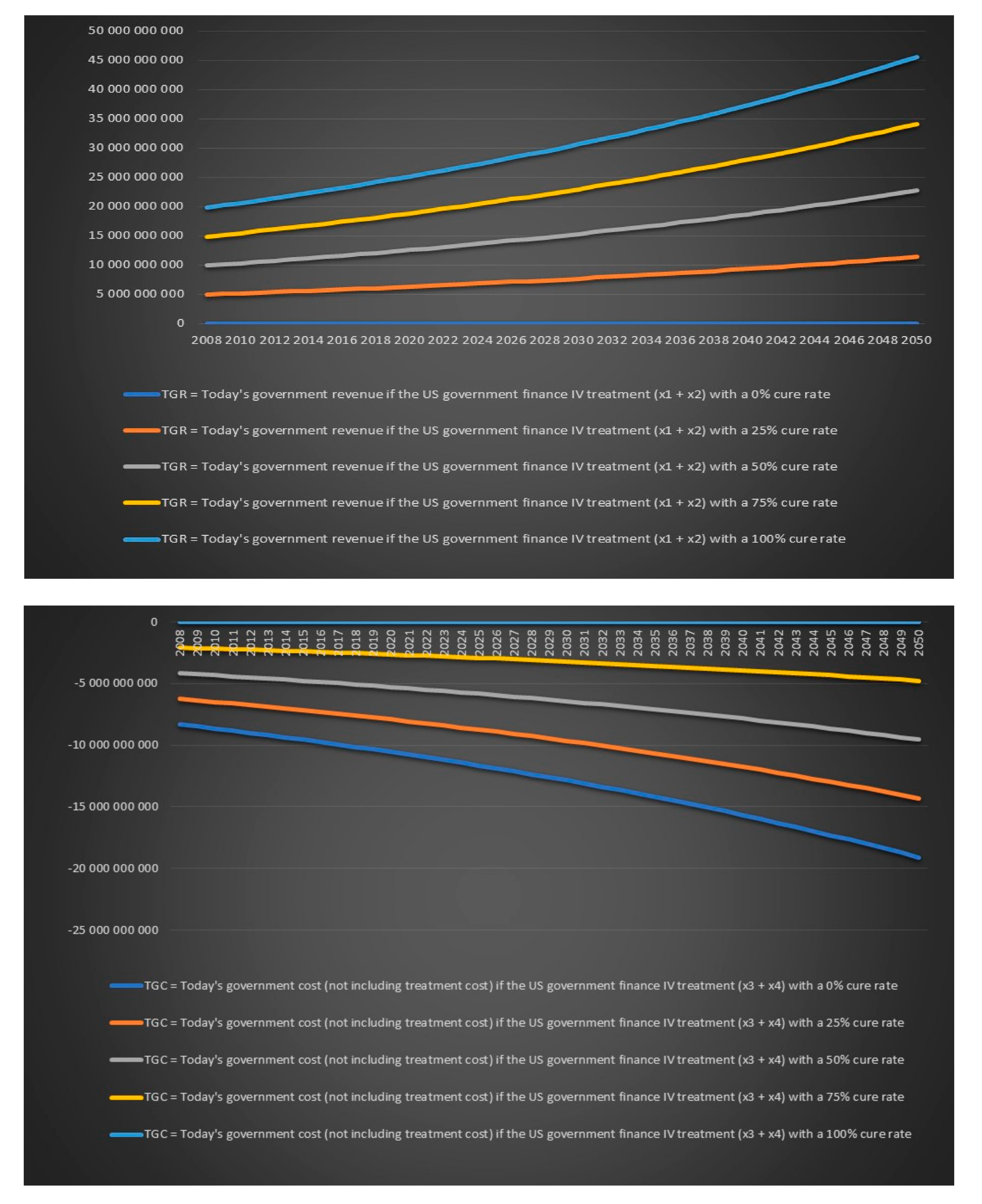
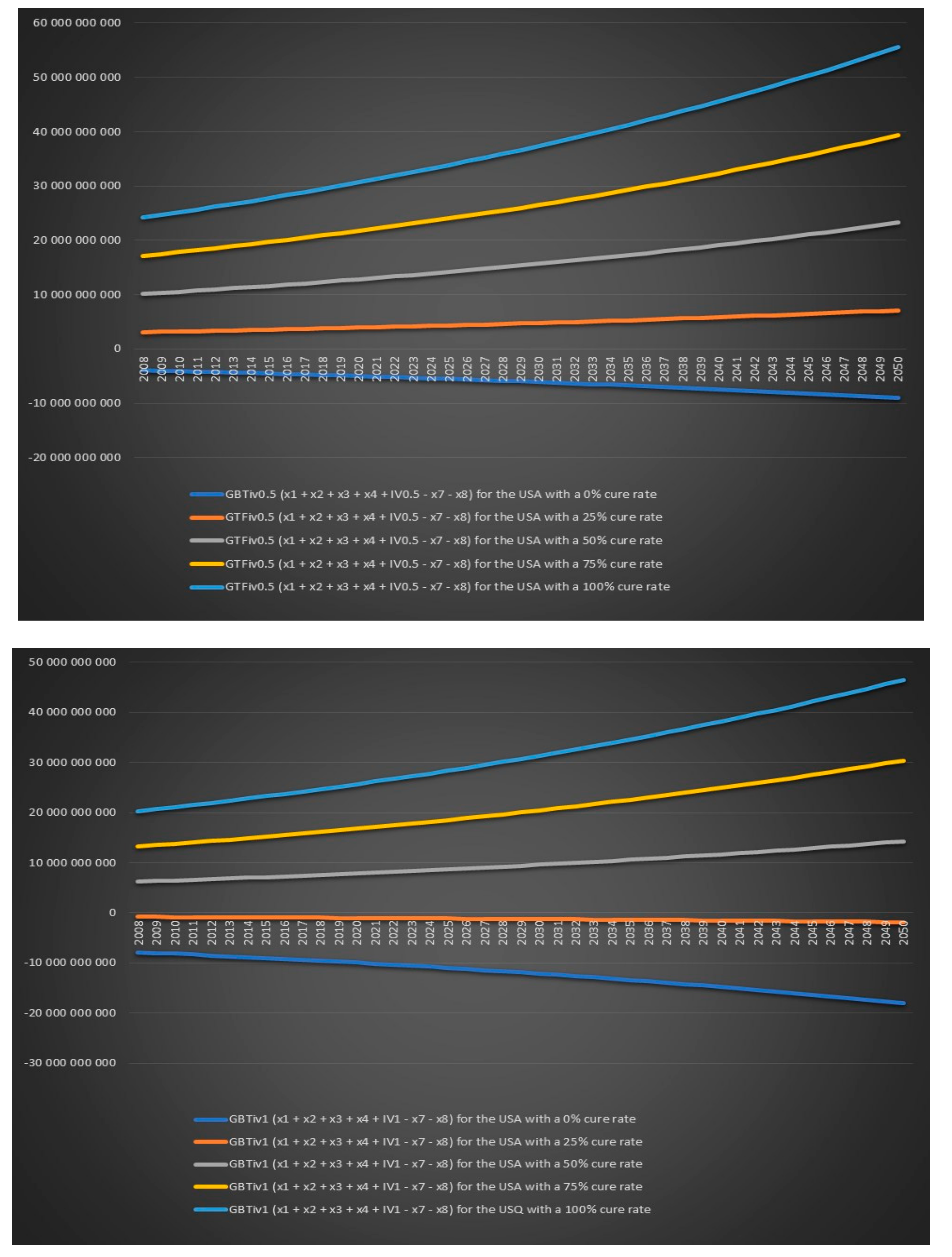
Figure 19 that the US government’s financial balance based on today’s cost and revenues for antibiotic IV treatment for 6 months for chronic Lyme disease GBTiv0.5 is positive for an assumed cure rate of 25% and above and for 1 year of IV treatment with antibiotics GBTiv1 is positive for an assumed cure rate of 50% and above. We can see in
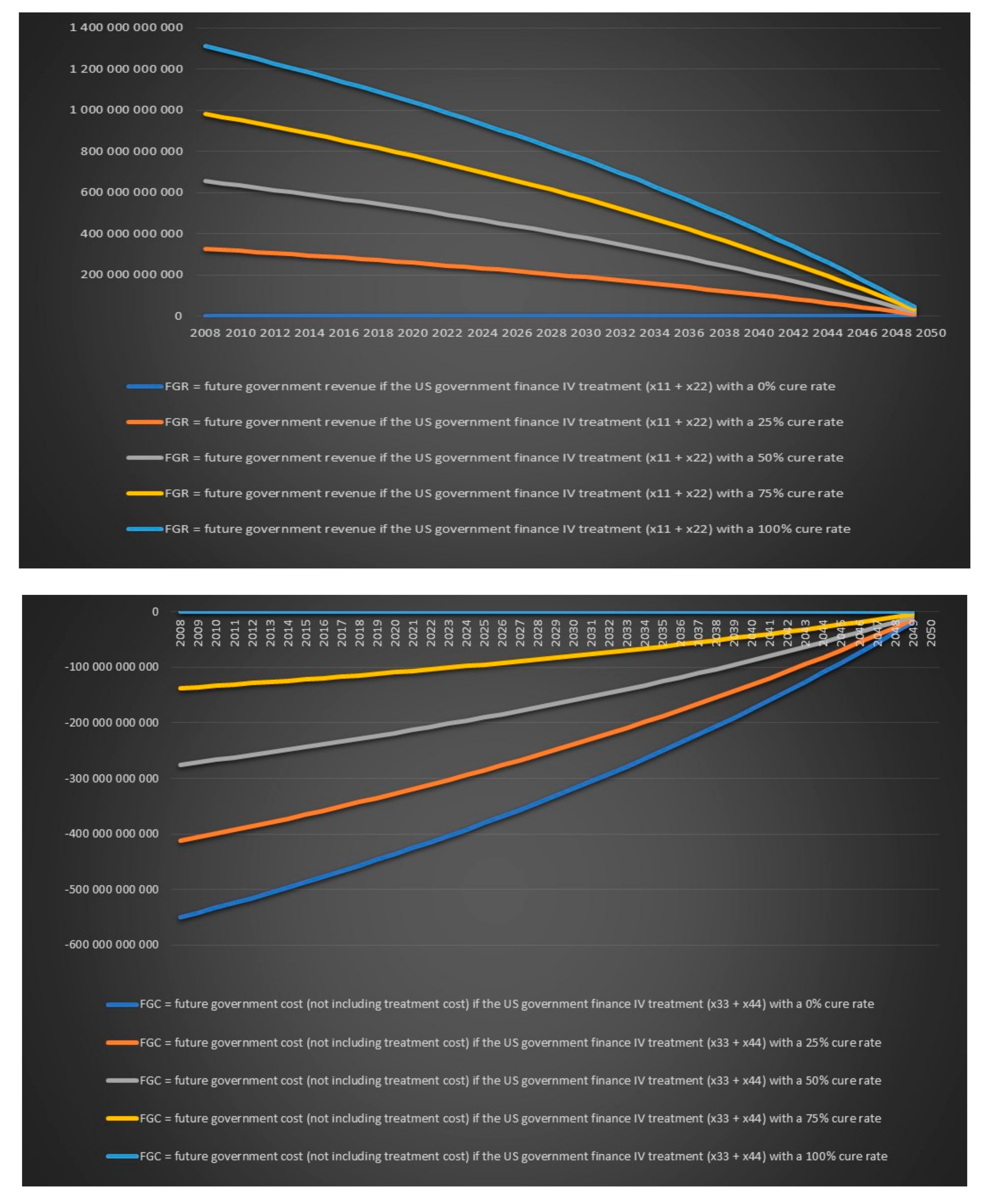
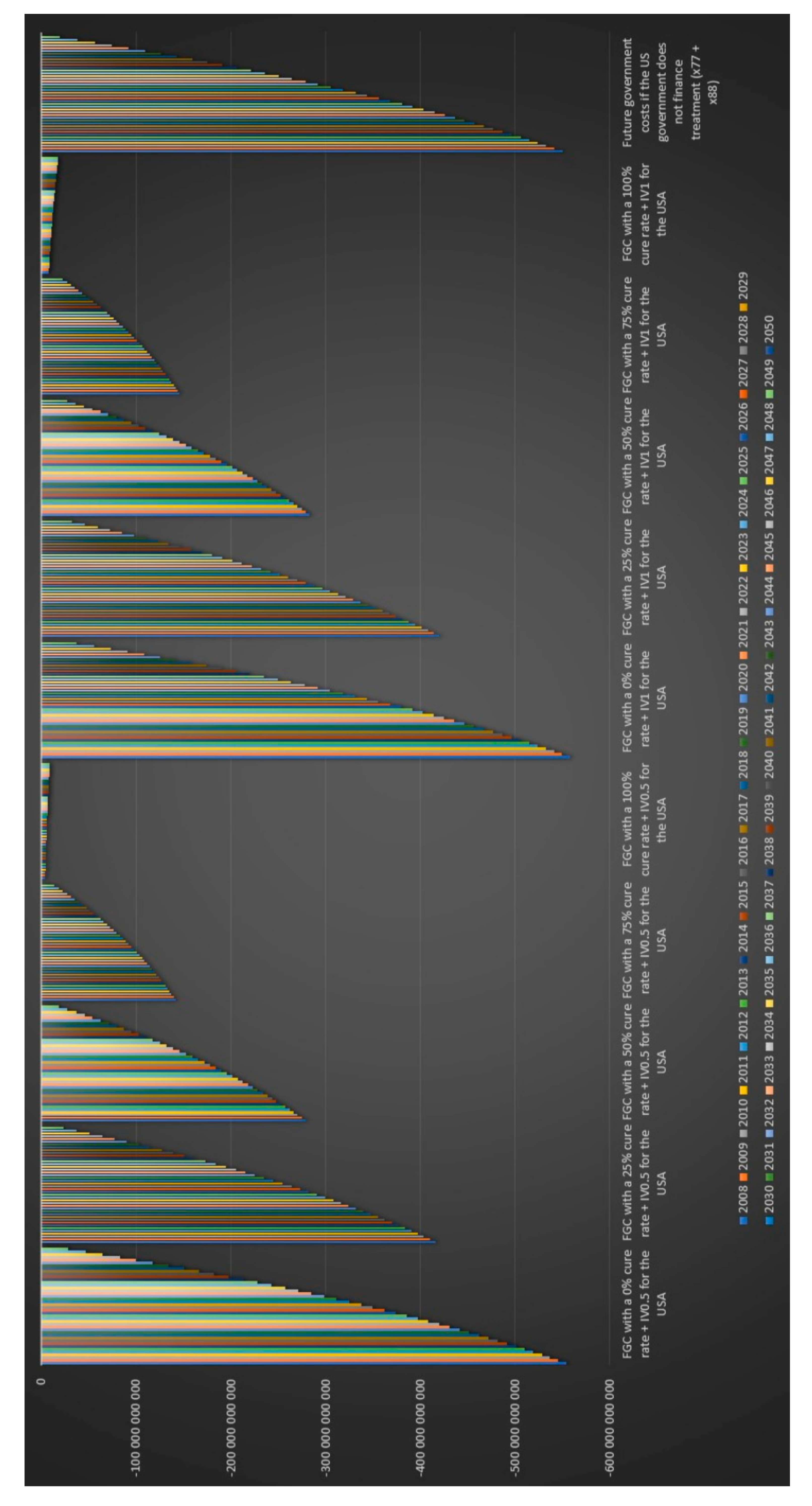
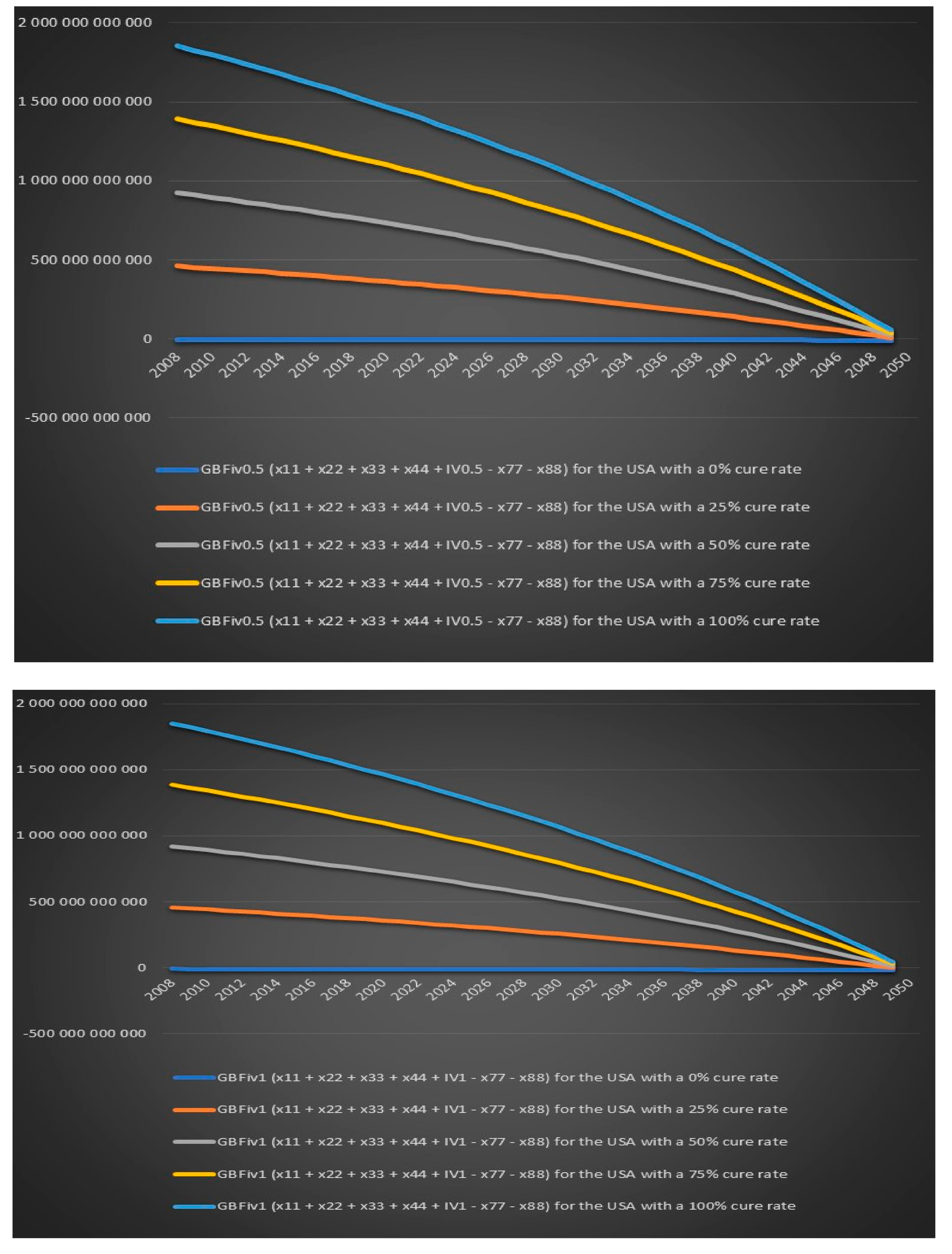
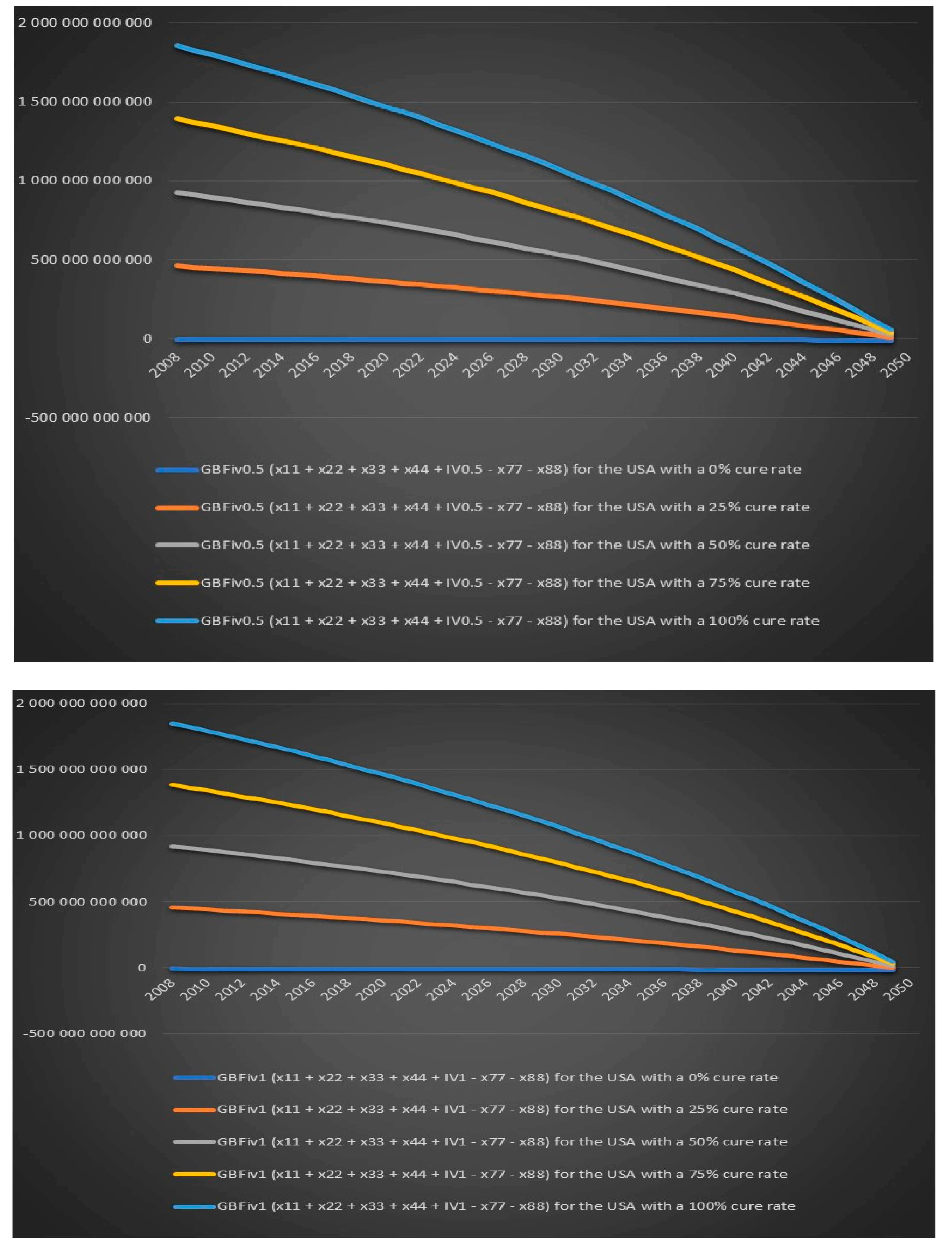
Figure 20 that the US government’s financial balance based on future cost and revenues for antibiotic IV treatment for 6 months for chronic Lyme disease GBFiv0.5 is positive for an assumed cure rate of 25% and above and for 1 year of IV treatment GBFiv1 is also positive for an assumed cure rate of 25% and above. We can see in
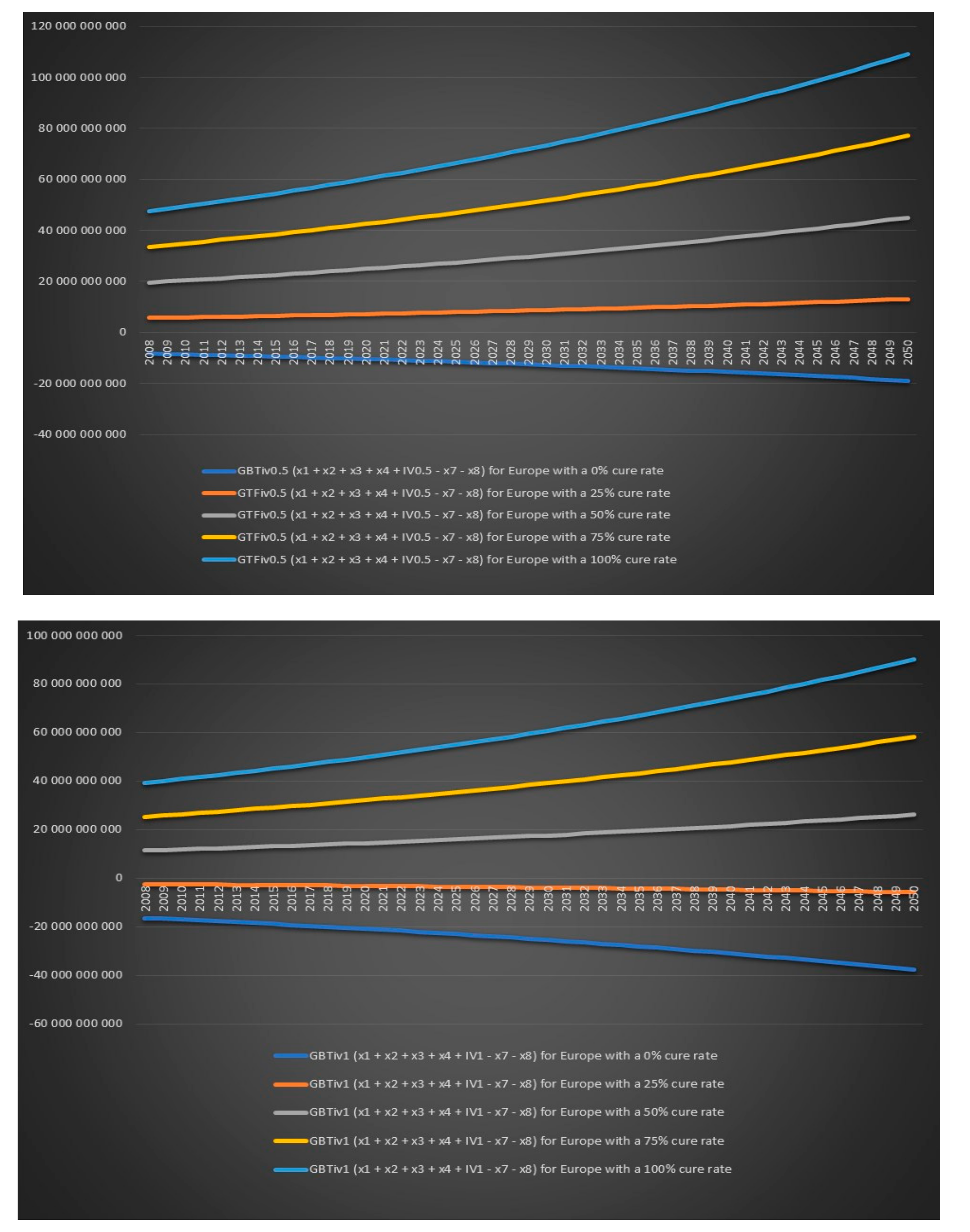
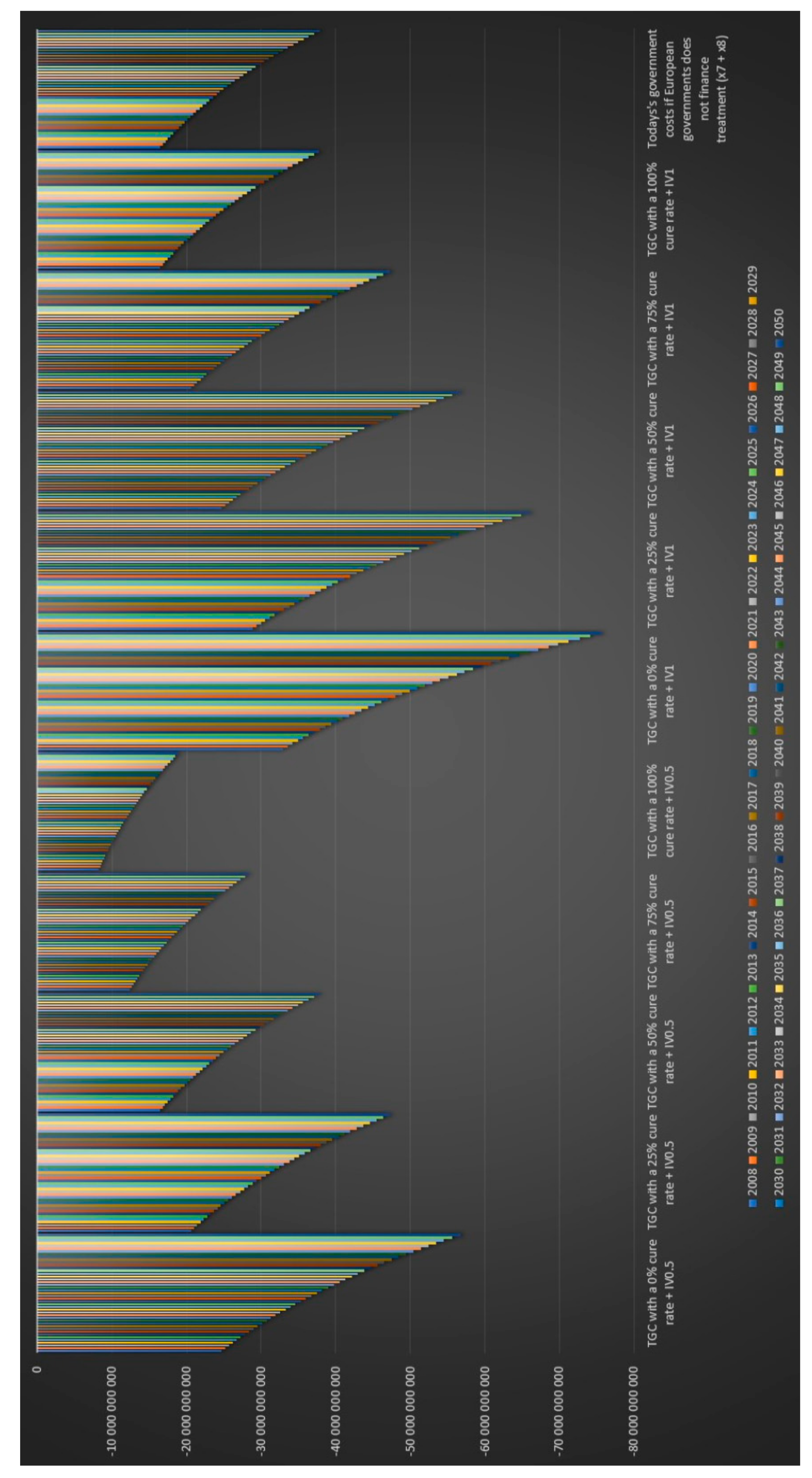
Figure 21 that the European governments’ financial balance based on today’s cost and revenues for antibiotic IV treatment for 6 months for chronic Lyme disease GBTiv0.5 is positive for an assumed cure rate of 25% and above and for 1 year of IV treatment with antibiotic GBTiv1 is positive for an assumed cure rate of 50% and above. We can see in
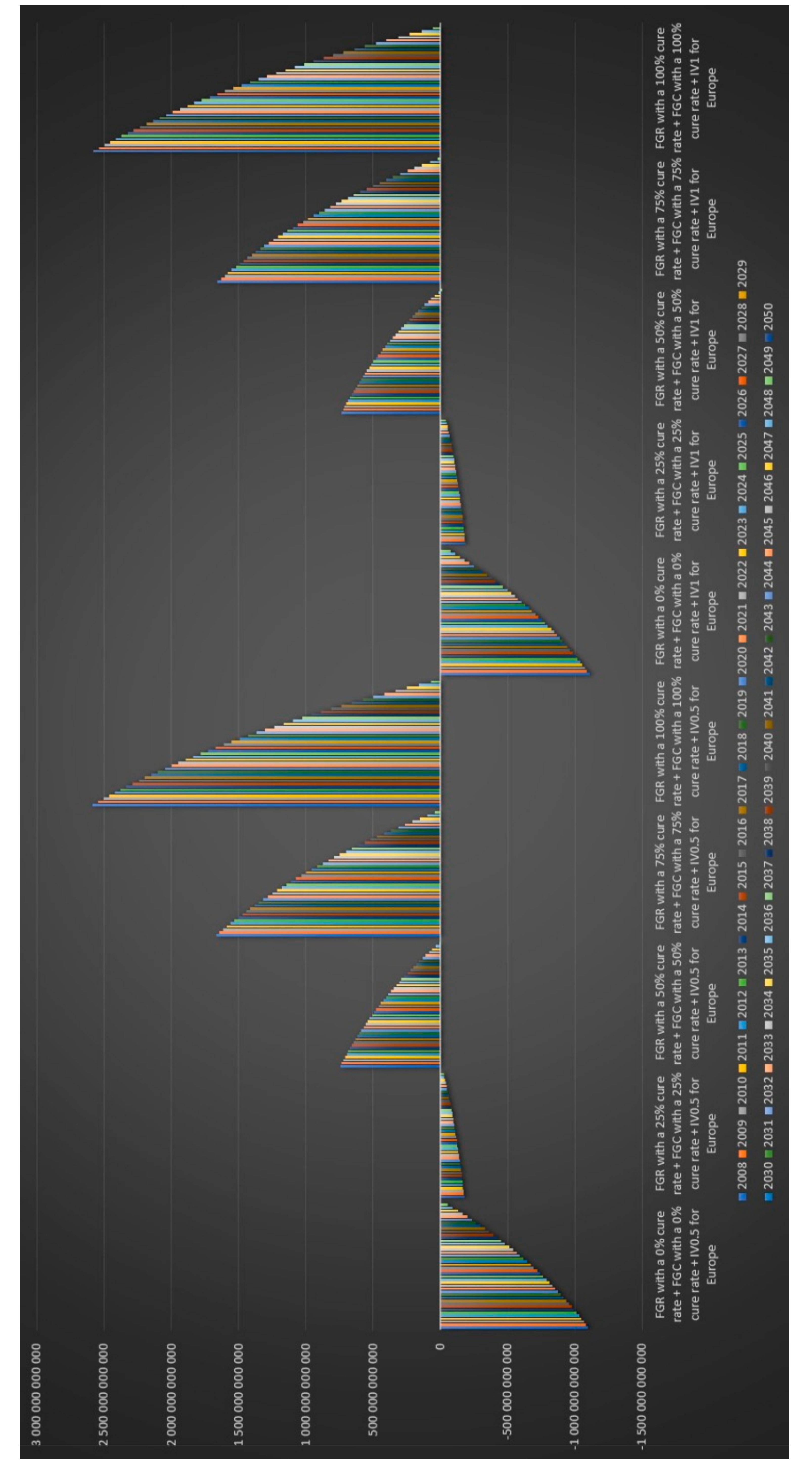
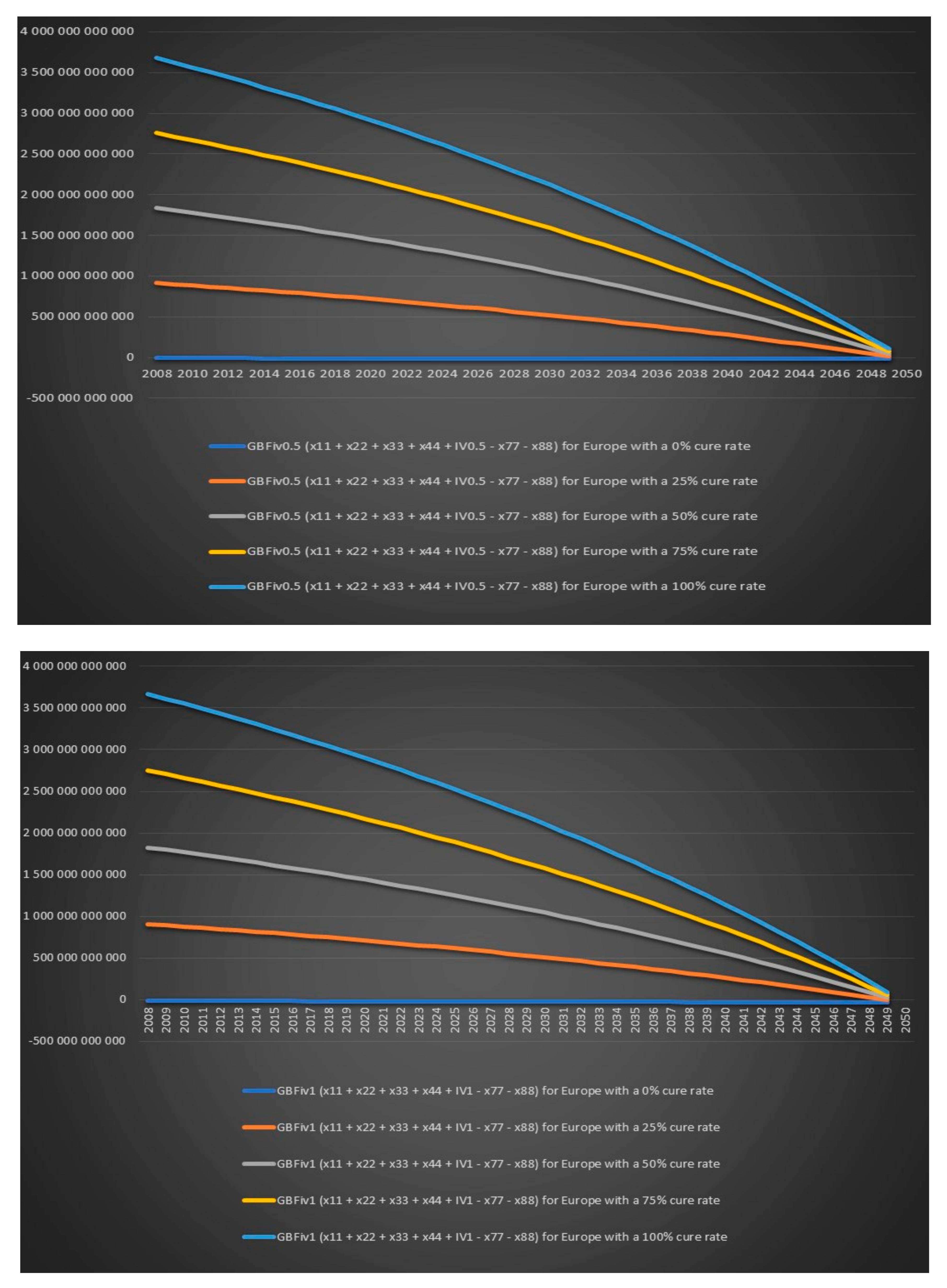
Figure 22 that the European governments’ financial balance based on future cost and revenues for IV antibiotic treatment for 6 months for chronic Lyme disease GBFiv0.5 is positive for an assumed cure rate of 25% and above and for 1 year of IV antibiotic treatment GBFiv1 is also positive for an assumed cure rate of 25% and above.