Nursing Practice and Telehealth in School Health Services: A Scoping Review
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Eligibility Criteria
2.3. Search Strategy
2.4. Quality Assessment
2.5. Data Extraction
2.6. Analysis and Synthesis of Data
3. Results
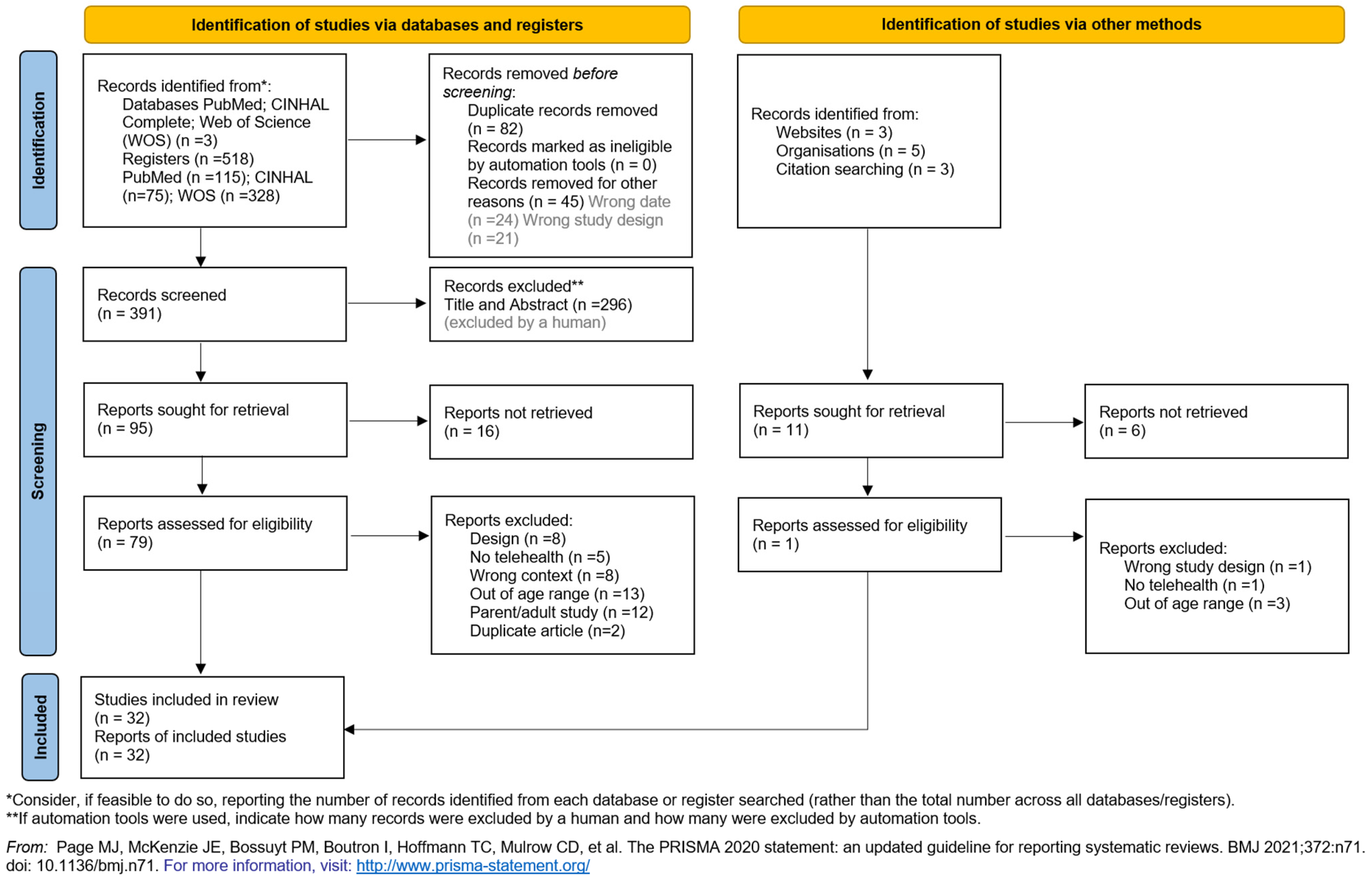
3.1. Search Outcomes
3.2. Characteristics of Studies
3.3. Purpose of Telehealth and Intervention Strategies
- (a)
- (b)
- (c)
- (d)
- (e)
- (f)
- (g)
- (h)
- (i)
- Care and behaviour in one study (3.12%) [68];
- (j)
- Prevention of psychosocial problems in one study (3.12%) [56];
- (k)
- Autism assessment in one study (3.12%) [47];
- (l)
- Diagnosis and management of skin scabies in one study (3.12%) [71];
- (m)
- Prevention of skin cancer and photoaging in one study (3.12%) [64];
- (n)
- Screening for metabolic syndrome in one study (3.12%) [58].
3.4. Role of Nursing in School-Based Telehealth Practice
- -
- Administration and monitoring of medical guidelines via teleconsultation to ensure efficient completion; support to school staff; and scheduling and monitoring attendance of telemedicine visits in the prevention and diagnosis of asthma [50,71]. In addition, the nurses helped ensure seamless communication with the physician during virtual visits; served as guardians of students’ health information; and operated as the primary interface between parents, students, paediatricians, and teachers on school health issues [67];
- -
- -
- Finally, nurses collaborated by conducting educational interventions via telemedicine and conducting comprehensive asthma education aimed at preventing crises, as well as assessing treatment efficacy and monitoring crises via teleconsultation [69]. In the detection and follow-up of hearing problems, they coordinated with primary care staff in the implementation of the Tele-Health-Kids (THK) programme and collaborated in follow-ups via telemedicine [74]. They coordinated and executed the biochemical analyses (blood draw) and anthropometric tests for metabolic syndrome screening via telemedicine [58].
3.5. Perceived Benefits and Limitations of School-Based Telehealth Studies
4. Discussion
4.1. Limitations and Strengths
4.2. Implications of Findings
4.2.1. Implications for Practice
4.2.2. Implications for Research
4.2.3. Implications for Policy
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Scott, R.; Mars, M. Here We Go again—“Digital Health”. J. Int. Soc. Telemed. eHealth 2019, 7, e1. Available online: https://journals.ukzn.ac.za/index.php/JISfTeH/article/view/976/1321 (accessed on 20 March 2023). [CrossRef]
- Camden, C.; Silva, M. Pediatric Teleheath: Opportunities Created by the COVID-19 and Suggestions to Sustain Its Use to Support Families of Children with Disabilities. Phys. Occup. Ther. Pediatr. 2021, 41, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Dorsey, E.; Topol, E. State of Telehealth. N. Engl. J. Med. 2016, 375, 154–161. [Google Scholar] [CrossRef]
- Stephens, J.; Greenberg, G. Asynchronous Telehealth. Prim. Care Clin. Off. Pract. 2022, 49, 531–541. [Google Scholar] [CrossRef] [PubMed]
- Fisher, K.; Davey, A.; Magin, P. Telehealth for Australian general practice: The present and the future. Aust. J. Gen. Pract. 2022, 51, 626–629. [Google Scholar] [CrossRef] [PubMed]
- Doraiswamy, S.; Abraham, A.; Mamtani, R.; Cheema, S. Use of Telehealth During the COVID-19 Pandemic: Scoping Review. J. Med. Internet Res. 2020, 22, e24087. [Google Scholar] [CrossRef]
- Esposito, S.; Rosafio, C.; Antodaro, F.; Argentiero, A.; Bassi, M.; Becherucci, P.; Bonsanto, F.; Cagliero, A.; Cannata, G.; Capello, F.; et al. Use of Telemedicine Healthcare Systems in Children and Adolescents with Chronic Disease or in Transition Stages of Life: Consensus Document of the Italian Society of Telemedicine (SIT), of the Italian Society of Preventive and Social Pediatrics (SIPPS), of the Italian Society of Pediatric Primary Care (SICuPP), of the Italian Federation of Pediatric Doctors (FIMP) and of the Syndicate of Family Pediatrician Doctors (SIMPeF). J. Pers. Med. 2023, 13, 235. [Google Scholar] [CrossRef]
- Savignano, M.; Kondratiuk, G.; Martínez, M.; Lechuga, P.; Ugo, F.; Della Corte, M.; Mato, A.; Luna, A. Telehealth for the Care of Complex Chronic Pediatric Patients in Latin America and the Caribbean: Narrative Review. Curr. Pediatr. Rep. 2021, 9, 167–170. [Google Scholar] [CrossRef]
- Bauer, E.; Bollig, G.; Dieperink, K. District nurses’ views on and experiences with a telemedicine educational programme in palliative care. Scand. J. Caring Sci. 2020, 34, 1083–1093. [Google Scholar] [CrossRef]
- James, S.; Ashley, C.; Williams, A.; Desborough, J.; Mcinnes, S.; Calma, K.; Mursa, R.; Stephen, C.; Halcomb, E. Experiences of Australian primary healthcare nurses in using telehealth during COVID-19: A qualitative study. BMJ Open 2021, 11, e049095. [Google Scholar] [CrossRef]
- National Association of School Nurses. Telehealth: Equitable Student Access to Health Services. [Position Statement]. NASN 2022, 38, 4. [Google Scholar] [CrossRef]
- Love, H.; Panchal, N.; Schlitt, J.; Behr, C.; Soleimanpour, S. The Use of Telehealth in School-Based Health Centers. Glob. Pediatr. Health 2019, 6, 2333794X1988419. [Google Scholar] [CrossRef] [PubMed]
- Martinsson, E.; Garmy, P.; Einberg, E. School Nurses’ Experience of Working in School Health Service during the COVID-19 Pandemic in Sweden. Int. J. Environ. Res. Public Health 2021, 18, 6713. [Google Scholar] [CrossRef] [PubMed]
- Lukas, H.; Xu, C.; Yu, Y.; Gao, W. Emerging Telemedicine Tools for Remote COVID-19 Diagnosis, Monitoring, and Management. ACS Nano 2020, 14, 16180–16193. [Google Scholar] [CrossRef] [PubMed]
- Marrapese, B.; Gormley, J.; Deschene, K. Reimagining School Nursing: Lessons Learned from a Virtual School Nurse. NASN Sch. Nurse 2021, 36, 218–225. [Google Scholar] [CrossRef] [PubMed]
- Cook, G.; Appleton, J.; Bekaert, S.; Harrold, T.; Taylor, J.; Sammut, D. School nursing: New ways of working with children and young people during the Covid-19 pandemic: A scoping review. J. Adv. Nurs. 2022, 79, 471–501. [Google Scholar] [CrossRef] [PubMed]
- Kang, H.; Jeong, D.; Suh, B.; Ahn, M. The Impact of the Coronavirus Disease-2019 Pandemic on Childhood Obesity and Vitamin D Status. J. Korean Med. Sci. 2021, 36, e21. [Google Scholar] [CrossRef] [PubMed]
- Dallolio, L.; Marini, S.; Masini, A.; Toselli, S.; Stagni, R.; Bisi, M.; Gori, D.; Tessari, A.; Sansavini, A.; Lanari, M.; et al. The impact of COVID-19 on physical activity behaviour in Italian primary school children: A comparison before and during pandemic considering gender differences. BMC Public Health 2022, 22, 52. [Google Scholar] [CrossRef]
- Elbarbary, N.; Dos Santos, T.; de Beaufort, C.; Agwu, J.; Calliari, L.; Scaramuzza, A. COVID-19 outbreak and pediatric diabetes: Perceptions of health care professionals worldwide. Pediatr. Diabetes 2020, 21, 1083–1092. [Google Scholar] [CrossRef]
- Sánchez-García, J.; Marín-Jiménez, A.; Tovar-Gálvez, M.; Cortés-Martín, J.; Montiel-Troya, M.; Menor-Rodríguez, M.; Rodríguez-Blanque, R. Evolution of the COVID-19 Pandemic after the Introduction of School Referral Nurses in the Province of Granada-A Descriptive Study. Children 2022, 9, 1646. [Google Scholar] [CrossRef]
- Maughan, E.; Johnson, K.; Gryfinski, J.; Lamparelli, W.; Chatham, S.; Lopez-Carrasco, J. Show Me the Evidence: COVID-19 and School Nursing in the 21st Century. NASN Sch. Nurse 2021, 36, 46–51. [Google Scholar] [CrossRef]
- McIntosh, C.; Brelage, P.; Thomas, C.; Wendel, J.; Phelps, B. School nurse and COVID-19 response. Psychol. Sch. 2022, 60, 1532–1543. [Google Scholar] [CrossRef] [PubMed]
- Galemore, C.; Marion, S.; Moran, K.; O’Toole, S.; Ragan, K.; Robertson, B. Leading During a Pandemic: A School Nurse Administrator Roundtable. NASN Sch. Nurse (Print) 2022, 37, 155–164. [Google Scholar] [CrossRef]
- Pennington, B. Changing Roles of the State School Nurse Consultants: How the Pandemic Has Accentuated Their Value and Visibility. NASN Sch. Nurse 2023, 38, 17–19. [Google Scholar] [CrossRef]
- Campbell, J.; Theodoros, D.; Russell, T.; Gillespie, N.; Hartley, N. Client, provider and community referrer perceptions of telehealth for the delivery of rural paediatric allied health services. Aust. J. Rural. Health 2019, 27, 419–426. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, R.; Dubey, M.; Chatterjee, S.; Dubey, S. Impact of COVID-19 on children: Special focus on the psychosocial aspect. Minerva Pediatr. 2020, 72. [Google Scholar] [CrossRef] [PubMed]
- Green, P. Risks to children and young people during COVID-19 pandemic. BMJ 2020, 369, m1669. [Google Scholar] [CrossRef]
- Okuyama, J.; Seto, S.; Fukuda, Y.; Funakoshi, S.; Amae, S.; Onobe, J.; Izumi, S.; Ito, K.; Imamura, F. Mental Health and Physical Activity among Children and Adolescents during the COVID-19 Pandemic. Tohoku J. Exp. Med. 2021, 253, 203–215. [Google Scholar] [CrossRef]
- Levitt, K.; Munzer, T.; Torres, C.; Schaller, A.; McCaffery, H.; Radesky, J. Remote and Hybrid Schooling During COVID-19: Associations with Child Behavior and Sleep. J. Dev. Behav. Pediatr. 2022, 43, e288–e295. [Google Scholar] [CrossRef]
- Costa, P.; Cruz, A.; Alves, A.; Rodrigues, M.; Ferguson, R. The impact of the COVID-19 pandemic on young children and their caregivers. Child Care Health Dev. 2022, 48, 1001–1007. [Google Scholar] [CrossRef]
- Lim, M.; Ramamurthy, M.; Aishworiya, R.; Rajgor, D.; Tran, A.; Hiriyur, P.; Kunaseelan, S.; Jabri, M.; Goh, D. School closure during the coronavirus disease 2019 (COVID-19) pandemic—Impact on children’s sleep. Sleep Med. 2021, 78, 108–114. [Google Scholar] [CrossRef] [PubMed]
- So, H.-K.; Chua, G.; Yip, K.-M.; Tung, K.; Wong, R.; Louie, L.; Tso, W.; Wong, I.; Yam, J.; Kwan, M.; et al. Impact of COVID-19 Pandemic on School-Aged Children’s Physical Activity, Screen Time, and Sleep in Hong Kong: A Cross-Sectional Repeated Measures Study. Int. J. Environ. Res. Public Health 2022, 19, 10539. [Google Scholar] [CrossRef] [PubMed]
- Vicari, S.; Pontillo, M. Developmental Psychopathology in the COVID-19 period. COVID-19 Pandemic Impact on Children and Adolescents’ Mental Health. Psychiatr. Danub. 2021, 33 (Suppl. S11), 33–35. Available online: https://www.psychiatria-danubina.com/UserDocsImages/pdf/dnb_vol33_noSuppl%2011/dnb_vol33_noSuppl%2011_33.pdf (accessed on 20 March 2023). [PubMed]
- Love, H.; Schlitt, J.; Soleimanpour, S.; Panchal, N.; Behr, C. Twenty years of school-based health care growth and expansion. Health Aff. 2019, 38, 55–64. [Google Scholar] [CrossRef] [PubMed]
- Williams, S.; Xie, L.; Hill, K.; Mathew, M.; Perry, T.; Wesley, D.; Messiah, S. Potential Utility of School-Based Telehealth in the Era of COVID-19. J. Sch. Health 2021, 91, 550–554. [Google Scholar] [CrossRef] [PubMed]
- Janjua, S.; Carter, D.; Threapleton, C.; Prigmore, S.; Disler, R. Telehealth interventions: Remote monitoring and consultations for people with chronic obstructive pulmonary disease (COPD). Cochrane Database Syst. Rev. 2021, CD013196. [Google Scholar] [CrossRef]
- Slater, H.; Briggs, A.; Stinson, J.; Campbell, J. End user and implementer experiences of mHealth technologies for noncommunicable chronic disease management in young adults: A qualitative systematic review protocol. JBI Database Syst. Rev. Implement. Rep. 2017, 15, 2047–2054. [Google Scholar] [CrossRef]
- Grant, M.; Booth, A. A typology of reviews: An analysis of 14 review types and associated methodologies. Health Inf. Libr. J. 2009, 26, 91–108. [Google Scholar] [CrossRef]
- Peters, M.; Godfrey, C.; Khalil, H.; McInerney, P.; Parker, D.; Soares, C. Guidance for conducting systematic scoping reviews. Int. J. Evid.-Based Healthc. 2015, 13, 141–146. [Google Scholar] [CrossRef]
- Page, M.; McKenzie, J.; Bossuyt, P.; Boutron, I.; Hoffmann, T.; Mulrow, C.; Shamseer, L.; Tetzlaff, J.; Akl, E.; Brennan, S.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Flagas, M.; Pitsouni, E.; Malietzis, G.; Pappas, G. Comparison of PubMed, Scopus, Web of Science, and Google Scholar: Strengths and weaknesses. FASEB J. 2008, 22, 338–342. [Google Scholar] [CrossRef] [PubMed]
- Hopia, H.; Heikkilä, J. Nursing research priorities based on CINAHL database: A scoping review. Nurs. Open 2019, 26, 483–494. [Google Scholar] [CrossRef] [PubMed]
- Khalil, H.; Peters, M.; Godfrey, C.; McInerney, P.; Soares, C.; Parker, D. An Evidence-Based Approach to Scoping Reviews. Worldviews Evid.-Based Nurs. 2016, 13, 118–123. [Google Scholar] [CrossRef]
- Joanna Briggs Institute Levels of Evidence and Grades of Recommendation Working Party. JBI Levels of Evidence. 2014. Available online: https://jbi.global/sites/default/files/2019-05/JBI-Levels-of-evidence_2014_0.pdf (accessed on 29 November 2023).
- Green, I.; Reardon, T.; Button, R.; Williamson, V.; Halliday, G.; Hill, C.; Larkin, M.; Sniehotta, F.F.; Ukoumunne, O.C.; Ford, T.; et al. Increasing access to evidence-based treatment for child anxiety problems: Online parent-led CBT for children identified via schools. Child Adolesc. Ment. Health 2023, 28, 48–51. [Google Scholar] [CrossRef] [PubMed]
- Martinez, W.; Patel, S.G.; Contreras, S.; Baquero-Devis, T.; Bouche, V.; Birman, D. “We could see our real selves”: The COVID-19 syndemic and the transition to telehealth for a school-based prevention program for newcomer Latinx immigrant youth. J. Community Psychol. 2023, 51, 2372–2389. [Google Scholar] [CrossRef]
- Shahidullah, J.; Brinster, M.; Patel, P.; Cannady, M.; Krishnan, A.; Talebi, H.; Mani, N. Increasing resources for autism evaluation and support for under-resourced schools through a state-wide school telehealth initiative. Phicology Sch. 2022, 59, 1295–1307. [Google Scholar] [CrossRef]
- Emmett, S.; Platt, A.; Turner, E.; Gallo, J.; Labrique, A.; Inglis, S.; Jenson, C.D.; E Parnell, H.; Wang, N.-Y.; Hicks, K.L.; et al. Mobile health school screening and telemedicine referral to improve access to specialty care in rural Alaska: A cluster- randomised controlled trial. Lancet Glob. Health 2022, 10, e1023–e1033. [Google Scholar] [CrossRef]
- Brown, A.; Sutherland, R.; Janssen, L.; Hudson, N.; Chooi, A.; Reynolds, R.; Walton, A.; Lecathelinais, C.; Reilly, K.; Nathan, N.; et al. Enhancing the potential effects of text messages delivered via an m-health intervention to improve packing of healthy school lunchboxes. Public Health Nutr. 2021, 24, 2867–2876. [Google Scholar] [CrossRef]
- Crabtree-Ide, C.; Lillvis, D.; Nie, J.; Fagnano, M.; Tajon, R.; Tremblay, P.; Halterman, J.S.; Noyes, K. Evaluating the Financial Sustainability of the School-Based Telemedicine Asthma Management Program. Popul. Health Manag. 2021, 24, 664–674. [Google Scholar] [CrossRef]
- Marshman, Z.; El-Yousfi, S.; Kellar, I.; Dey, D.; Robertson, M.; Day, P.; Chestnutt, I.; Pavitt, S.; de Araujo, M.; Innes, N. Development of a secondary school-based digital behaviour change intervention to improve tooth brushing. BMC Oral Health 2021, 21, 546. [Google Scholar] [CrossRef]
- Moltrecht, B.; Patalay, P.; Deighton, J.; Edbrooke-Childs, J. A School-Based Mobile App Intervention for Enhancing Emotion Regulation in Children: Exploratory Trial. JMIR mHealth uHealth 2021, 9, e21837. [Google Scholar] [CrossRef] [PubMed]
- Sutherland, R.; Brown, A.; Nathan, N.; Yoong, S.; Janssen, L.; Chooi, A.; Hudson, N.; Wiggers, J.; Kerr, N.; Evans, N.; et al. A Multicomponent mHealth-Based Intervention (SWAP IT) to Decrease the Consumption of Discretionary Foods Packed in School Lunchboxes: Type I Effectiveness-Implementation Hybrid Cluster Randomized Controlled Trial. J. Med. Internet Res. 2021, 24, e25256. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, T. Effect of mHealth tool on knowledge regarding reproductive health of school going adolescent girls: A before-after quasi-experimental study. BMJ Open 2020, 10, e036656. [Google Scholar] [CrossRef]
- Langlet, B.; Maramis, C.; Diou, C.; Maglaveras, N.; Fagerberg, P.; Heimeier, R.; Lekka, I.; Delopoulos, A.; Ioakimidis, I. Formative Evaluation of a Smartphone App for Monitoring Daily Meal Distribution and Food Selection in Adolescents: Acceptability and Usability Study. JMIR mHealth uHealth 2020, 8, e14778. [Google Scholar] [CrossRef]
- Thabrew, H.; Kumar, H.; Goldfinch, M.; Cavadino, A.; Goodyear-Smith, F. Repeated Psychosocial Screening of High School Students Using YouthCHAT: Cohort Study. JMIR Pediatr. Parent. 2020, 3, e20976. [Google Scholar] [CrossRef] [PubMed]
- Müssener, U.; Linderoth, C.; Thomas, K.; Bendtsen, M. mHealth smoking cessation intervention among high school students: 3-month primary outcome findings from a randomized controlled trial. PLoS ONE 2020, 15, e0229411. [Google Scholar] [CrossRef]
- Bacopoulou, F.; Efthymiou, V.; Palaiologos, G.; Tsarouhas, K.; Landis, G.; Fostiropoulos, I.; Kaklea, M.; Rentoumis, A.; Papassotiriou, I. Telemedicine screening adolescent metabolic syndrome in Greek schools. Eur. J. Clin. Investig. 2019, 49, e13075. [Google Scholar] [CrossRef]
- Bian, J.; Cristaldi, K.; Summer, A.; Su, Z.; Marsden, J.; Mauldin, P.; McElligott, J.T. Association of a School-Based, Asthma-Focused Telehealth Program With Emergency Department Visits Among Children Enrolled in South Carolina Medicaid. JAMA Pediatr. 2019, 173, 1041–1048. [Google Scholar] [CrossRef]
- Langbecker, D.; Caffery, L.; Taylor, M.; Theodoros, D.; Smith, A. Impact of school-based allied health therapy via telehealth on children’s speech and language, class participation and educational outcomes. J. Telemed. Telecare 2019, 25, 559–565. [Google Scholar] [CrossRef]
- Lau, P.; Pitkethly, A.; Leung, B.; Lau, E.; Wang, J. The Intervention Effect of SMS Delivery on Chinese Adolescent’s Physical Activity. Int. J. Environ. Res. Public Health 2019, 16, 787. [Google Scholar] [CrossRef]
- Marshman, Z.; Ainsworth, H.; Chestnutt, I.; Day, P.; Dey, D.; El Yousfi, S.; Fairhurst, C.; Gilchrist, F.; Hewitt, C.; Jones, C.; et al. Brushing RemInder 4 Good oral HealTh (BRIGHT) trial: Does an SMS behaviour change programme with a classroom-based session improve the oral health of young people living in deprived areas? A study protocol of a randomised controlled trial. Trials 2019, 20, 452. [Google Scholar] [CrossRef]
- Tebb, K.; Leng, S.; Rico, R.; Renteria, R.; Rodriguez, F.; Puffer, M. A Mobile Health Contraception Decision Support Intervention for Latina Adolescents: Implementation Evaluation for Use in School-Based Health Centers. JMIR mHealth uHealth 2019, 7, e11163. [Google Scholar] [CrossRef] [PubMed]
- Brinker, T.; Faria, B.; Gatzka, M.; de Faria, O.; Heppt, M.; Kirchberger, M.; Schadendorf, D.; Nakamura, Y.; Buslaff, F.; Lisboa, O.C.; et al. A skin cancer prevention photoageing intervention for secondary schools in Brazil delivered by medical students: Protocol for a randomised controlled trial. BMJ Open 2018, 8, e018299. [Google Scholar] [CrossRef] [PubMed]
- Estai, M.; Bunt, S.; Kanagasingam, Y.; Kruger, E.; Tennant, M. A resource reallocation model for school dental screening: Taking advantage of teledentistry in low-risk areas. Int. Dent. J. 2018, 68, 262–268. [Google Scholar] [CrossRef] [PubMed]
- Govender, S.; Mars, M. Assessing the efficacy of asynchronous telehealth-based hearing screening and diagnostic services using automated audiometry in a rural South African school. S. Afr. J. Commun. Disord. 2018, 65, e1–e9. [Google Scholar] [CrossRef]
- Halterman, J.; Fagnano, M.; Tajon, R.; Tremblay, P.; Wang, H.; Butz, A.; Perry, T.T.; McConnochie, K.M. Effect of the School-Based Telemedicine Enhanced Asthma Management (SB-TEAM) Program on Asthma Morbidity: A Randomized Clinical Trial. JAMA Pediatr. 2018, 172, e174938. [Google Scholar] [CrossRef] [PubMed]
- McLennan, J. Video-conferencing Telehealth Linkage attempts to Schools to Facilitate Mental Health Consultation. J. Can Acad. Child Adolesc. Psychiatry 2018, 27, 137–141. Available online: https://gallery.mailchimp.com/7277068e5c73e73e1fd465a54/files/e1bf42af-c273-4d4c-955b-62e7c579d405/Video_conferencing_Telehealth_Linkage_attempts_to_Schools.pdf (accessed on 20 March 2023).
- Perry, T.; Halterman, J.; Brown, R.; Luo, C.; Randle, S.; Hunter, C.; Rettiganti, M. Results of an asthma education program delivered via telemedicine in rural schools. Ann. Allergy Asthma Immunol. 2018, 120, 401–408. [Google Scholar] [CrossRef]
- Pradhan, T.; Six-Workman, E.; Law, K. An Innovative Approach to Care: Integrating Mental Health Services Through Telemedicine in Rural School-Based Health Centers. Psychiatr. Serv. 2019, 70, 239–242. [Google Scholar] [CrossRef]
- Zettler-Greeley, C. How Telehealth Stopped a Contagious Outbreak at a School. Health Aff. 2018, 37, 2092–2095. [Google Scholar] [CrossRef]
- Skarzyński, P.; Świerniak, W.; Piłka, A.; Skarżynska, M.; Włodarczyk, A.; Kholmatov, D.; Makhamadiev, A.; Hatzopoulos, S. Hearing Screening Program for Children in Primary Schools in Tajikistan: A Telemedicine Model. Med. Sci. Monit 2016, 22, 2424–2430. [Google Scholar] [CrossRef] [PubMed]
- Burckhardt, R.; Manicavasagar, V.; Batterham, P.; Miller, L.; Talbot, E.; Lum, A. A Web-Based Adolescent Positive Psychology Program in Schools: Randomized Controlled Trial. J. Med. Internet Res. 2015, 17, e187. [Google Scholar] [CrossRef] [PubMed]
- Langkamp, D.; McManus, M.; Blakemore, S. Telemedicine for children with developmental disabilities: A more effective clinical process than office-based care. Telemed. J. E Health 2015, 21, 110–114. [Google Scholar] [CrossRef] [PubMed]
- Bannink, R.; Broeren, S.; Joosten-van Zwanenburg, E.; van As, E.; van de Looij-Jansen, P.; Raat, H. Effectiveness of a Web-based tailored intervention (E-health4Uth) and consultation to promote adolescents’ health: Randomized controlled trial. J. Med. Internet Res. 2014, 16, e143. [Google Scholar] [CrossRef] [PubMed]
- Cremers, H.; Mercken, L.; Crutzen, R.; Willems, P.; de Vries, H.; Oenema, A. Do email and mobile phone prompts stimulate primary school children to reuse an Internet-delivered smoking prevention intervention? J. Med. Internet Res. 2014, 16, e86. [Google Scholar] [CrossRef] [PubMed]
- WHO. Global Strategic Directions for Nursing and Midwifery 2021–2025; World Health Organization: Geneva, Switzerland, 2021; Available online: https://apps.who.int/iris/bitstream/handle/10665/344562/9789240033863-eng.pdf (accessed on 20 March 2023).
- Hertz, M.; Barrios, L. Adolescent mental health, COVID-19, and the value of school-community partnerships. Inj. Prev. 2021, 27, 85–86. [Google Scholar] [CrossRef] [PubMed]
- Ziebold, C.; Silva-Ribeiro, W.; King, D.; McDaid, D.; Hoffmann, M.; Romeo, R.; Pan, P.; Miguel, E.; Bressan, R.; Rohde, L.; et al. Utilisation and costs of mental health-related service use among adolescents. PLoS ONE 2022, 17, e0273628. [Google Scholar] [CrossRef]
- MacGeorge, C.; King, K.; Andrews, A.; Sterba, K.; Johnson, E.; Brinton, D.; Teufel, R.; Kruis, R.; Ford, D. School nurse perception of asthma care in school-based telehealth. J. Asthma 2022, 59, 1248–1255. [Google Scholar] [CrossRef]
- Shdaifat, M.; Khasawneh, R.; Alefan, Q. Clinical and economic impact of telemedicine in the management of pediatric asthma in Jordan: A pharmacist-led intervention. J. Asthma 2022, 59, 1452–1462. [Google Scholar] [CrossRef]
- Shimasaki, S.; Brunner Nii, P.; Davis, L.; Bishop, E.; Berget, C.; Perreault, C.; Thomas, J. A School Nurse Application of the ECHO Model. J. Sch. Nurs. 2021, 37, 306–315. [Google Scholar] [CrossRef]
- Cantrell, M.; Ruble, K.; Mensinger, J.; Birkhoff, S.; Morris, A.; Griffith, P.; Adams, J. The Use and Effect of the Health Storylines mHealth App on Female Childhood Cancer Survivors’ Self-efficacy, Health-Related Quality of Life and Perceived Illness. Cancer Nurs. 2022, 45, 61–69. [Google Scholar] [CrossRef]
- Diane, G.; Ganga, M.; Patricia, P. Parents’ perception of the school nurse’s role. J. Adv. Pediatr. Child Health 2020, 3, 064–067. [Google Scholar] [CrossRef]
- Reynolds, C.; Maughan, E. Telehealth in the School Setting: An Integrative Review. J. Sch. Nurs. 2015, 31, 44–53. [Google Scholar] [CrossRef]
- Dhaliwal, J.; Hall, T.; LaRue, J.; Maynard, S.; Pierre, P.; Bransby, K. Expansion of telehealth in primary care during the COVID-19 pandemic: Benefits and barriers. J. Am. Assoc. Nurse Pract. 2022, 34, 224–229. [Google Scholar] [CrossRef] [PubMed]
- Gareev, I.; Gallyametdinov, A.; Beylerli, O.; Valitov, E.; Alyshov, A.; Pavlov, V.; Izmailov, A.; Zhao, S. The opportunities and challenges of telemedicine during COVID-19 pandemic. Front. Biosci. (Elite Ed.) 2021, 13, 291–298. [Google Scholar] [CrossRef] [PubMed]
- Curfman, A.; Hackell, J.; Herendeen, N.; Alexander, J.; Marcin, J.; Moskowitz, W.; Bodnar, C.; Simon, H.; McSwain, S. Telehealth: Improving Access to and Quality of Pediatric Health Care. Pediatrics 2021, 148, e2021053129. [Google Scholar] [CrossRef]
- Mens, M.; Keijsers, L.; Dietvorst, E.; Koval, S.; Legerstee, J.; Hillegers, M. Promoting Daily Well-being in Adolescents using mHealth. J. Youth Adolesc. 2022, 51, 2173–2189. [Google Scholar] [CrossRef] [PubMed]
- Pacheco-Vergara, M.; Cartes-Velásquez, R. mHealth para mejorar la higiene oral de niños. Revisión de literatura. Av. En Odontoestomatol. 2020, 36, 27–34. [Google Scholar] [CrossRef]
- King, I.; Heidler, P. Teleconsultation Services in Pediatric Primary Care in Austria: Upgrading Clinical Decision Support in Primary Health Care Settings. Telemed. E-Health 2022, 28, 1470–1478. [Google Scholar] [CrossRef] [PubMed]
- Macwilliam, J.; Hennessey, I.; Cleary, G. Telemedicine: Improving clinical care and medical education in paediatrics. Paediatr. Child Health 2021, 31, 388–396. [Google Scholar] [CrossRef]
- Buchi, A.; Langlois, D.; Northway, R. Use of Telehealth in Pediatrics. Prim. Care Clin. Off. Pract. 2022, 49, 585–596. [Google Scholar] [CrossRef] [PubMed]
- Sanchez, D.; Reiner, J.; Sadlon, R.; Price, O.; Long, M. Systematic Review of School Telehealth Evaluations. J. Sch. Nurs. 2019, 35, 61–76. [Google Scholar] [CrossRef] [PubMed]
- Benke, K.; Benke, G. Artificial Intelligence and Big Data in Public Health. Int. J. Environ. Res. Public Health 2018, 15, 2796. [Google Scholar] [CrossRef] [PubMed]
- Schwalbe, N.; Wahl, B. Artificial intelligence and the future of global health. Lancet 2020, 395, 1579–1586. [Google Scholar] [CrossRef] [PubMed]
- Haynie, K.; Lindahl, B.; Simons-Major, K.; Meadows, L.; Maughan, E. The Role of School Nursing in Telehealth [Position Statement]. NASN. 2022. Available online: https://www.nasn.org/advocacy/professional-practice-documents/position-statements/ps-telehealth (accessed on 20 May 2023).
- Mataxen, P.; Webb, L. Telehealth nursing. Nursing 2019, 49, 11–13. [Google Scholar] [CrossRef] [PubMed]
- Morse, B.; Anderson, L.; Combe, L.; Delack, S.; Ondeck, L.; Homme, C. U.S. School Nursing Job Analysis. J. Sch. Nurs. 2022, 38, 126–137. [Google Scholar] [CrossRef] [PubMed]
- Pollock, A.; Beaton, W.; Burgess, B.; Logel, S.; Wilson, L.; Ciha, J.; Allen, J. Diabetes in School Health (DiSH): Telementoring Collaboration between Pediatric Diabetes Specialists and School Nurses to Improve Care of Children with Diabetes. J. Sch. Nurs. 2023, in press. [Google Scholar] [CrossRef] [PubMed]
- Williams, M.; Morse, B.; DeGraffenried, W.; McAuliffe, D. Addressing Stress in High School Students during the COVID-19 Pandemic. NASN Sch. Nurse 2021, 36, 226–232. [Google Scholar] [CrossRef]
- Ouellette, C.; Bird, M.; Devereaux, P.; Lounsbury, J.; Djuric-Paulin, A.; LeBlanc, B.; Handsor, S.; DuMerton, D.; Deuchar, L.; Waggott, M.; et al. A Case Study of Two Emerging Nurse Leaders Specializing in Virtual Health during the COVID-19 Global Pandemic. Can. J. Nurs. Leadersh. 2021, 34, 30–37. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.; Horsley, T.; Weeks, L.; et al. PRISMA Extension for Scoping Reviews (PRISMAScR): Checklist and Explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef]
| Reference | Design and JBI Level of Evidence * | Data Sample | Purpose of Telehealth Use | Nursing Role | Benefits Perceived | Limitations Perceived |
|---|---|---|---|---|---|---|
| Green et al. (2023) [45] | Descriptive observational (uncontrolled case series). Level 4.c—Case series | UK. Children aged 8–9 | To provide a brief, therapist-guided treatment called Online Support and Intervention (OSI) to parents/carers of children identified through school-based screening as likely to have anxiety problems. Strategy: teleconsultation | N/A | Session-to-session improvements in all measures. The online platform was found to be more convenient and less stigmatising than traditional face-to-face clinic appointments | Difficulty of extrapolation and limitations of study design |
| Martinez et al. (2023) [46] | Qualitative method. N/A—No mention of qualitative method in JBI Levels of Evidence | USA. Immigrant youth aged 13–18 | To examine the impact that the transition to telehealth had on a school-based group prevention programme for immigrant youth, FUERTE Program. Strategy: tele-education through teleconference | N/A | Improved access to mental healthcare for immigrant youth using telehealth | Lack of representativeness of the population and difficulty in extrapolating the data |
| Shahidulla et al. (2022) [47] | Quasi-experimental. Level 2.c—Quasi-experimental prospectively controlled study | USA. School-aged youth (13–18) in under-resourced school systems in central Texas | To increase resources for autism evaluation and support for under-resourced schools through a state-wide school telehealth initiative. Strategy: teleconsultation | N/A | Increases access to timely autism spectrum disorder (ASD) assessments and support through a statewide school telehealth initiative | Not reported |
| Emmett et al. (2022) [48] | Randomised controlled trial. Level 1.c—RCT | Alaska (USA) aged 4–21. All children enrolled in the Bering Strait School District | Improve specialised follow-up time after positive school hearing tests (in possible hearing loss or ear disease). Strategy: telemonitoring through mHealth | None of the schools have school nurses | Improving early access to specialists for rural children, reducing health disparities | Short duration of the trial and small sample size due to age restrictions in school achievement tests and hearing-related quality of life questionnaires |
| Brown et al. (2021) [49] | Experimental design. Prospective impact assessment. Level 1.d—Pseudo-RCTs | Australia. Children aged 6–12 | To assess the impact of different lunchbox messages on parents’ intention to prepare a healthy lunchbox. Strategy: tele-education through mHealth—short message service (SMS) | N/A | Particularly strong effects on behavioural intentions in relation to messages related to other Health Belief Model (HBM) constructs | Technical limitations in the use of technology |
| Crabtree-Ide et al. (2021) [50] | Quasi-experimental. Level 2.c—Quasi-experimental prospectively controlled study | USA. Children aged 3–10 | To assess whether a telemedicine-based programme for enhanced asthma management (SB-TEAM), designed to overcome barriers to care for families of urban school-aged children, can be financially sustainable in urban school settings. Strategy: teleconsultation | Nurses oversaw the telehealth programme, assistants, and telemedicine visits programme. School nurses identified children with uncontrolled asthma at the beginning of the school year, administered daily preventive asthma medication, and monitored symptoms | The use of telemedicine to improve asthma control in underserved communities was shown to be highly effective | Economic limitations and lack of resources |
| Marshman et al. (2021) [51] | Observational action-research. Level 3.e—Observational study without a control group | UK. Students aged 11–16 | To describe the development process of a behaviour change intervention to improve the oral health of students. Strategy: tele-education through mHealth (SMS) | N/A | The intervention was needed to address the shortage of oral health promotion interventions for secondary school students and attempted to integrate a traditional classroom delivery method complemented with a newer mHealth technology solution. Parents and teachers were involved in the process | Restriction on the number of characters available; the need for basic literacy; and limited access to mobile phones for some young people |
| Moltrecht et al. (2021) [52] | Observational exploratory trial. Level 4—Not specified | UK. Children aged 10–12 | To explore the use of a new app-based intervention designed to support children’s emotion regulation in schools. Strategy: tele-education through mHealth—mobile application (app) | N/A | Using app improves emotion regulation; making app available improves access to teachers | Teachers report lack of content as one of the main obstacles to implementing the application |
| Sutherland et al. (2021) [53] | Cluster randomised controlled trial. Level 1.c—RCT | Australia. Children aged 7–12 | To assess the effectiveness of a multicomponent, mobile health-based intervention (SWAP IT) in reducing the energy contribution of discretionary foods and drinks packed for children to consume at school. Strategy: tele-education through mHealth (SMS/app) | N/A | There were no significant changes in pupils’ engagement in school | Technical problems were detected that could have reduced participation |
| Ahmed (2020) [54] | Quasi-experimental. Level 2.d—Pretest–post-test or historic/retrospective control group study | Bangladesh. Adolescent girls aged 14–19 | To assess the effect of an mHealth tool on knowledge regarding reproductive health. Strategy: tele-education through mHealth (SMS) | N/A | Knowledge score increased to 70.8% ± 9.7% after the 8-week SMS intervention on reproductive health knowledge | Difficult to extrapolate |
| Langlet et al. (2020) [55] | Descriptive observational acceptability–usability study. Level 3.e—Observational study without a control group | Sweden. Adolescents aged 13–18 | To conduct a formative evaluation of a smartphone app for monitoring daily meal distribution and food selection. Strategy: telediagnosis/telemonitoring through mHealth (app) | N/A | The smartphone application has a high acceptability and usability among students | Lack of resources (shortage of devices). Difficulty in extrapolating |
| Thabrew et al. (2020) [56] | Cluster randomised controlled trial. Level 1.c—RCT | New Zealand. Adolescents aged 14–15 | To assess the effectiveness of repeated psychosocial screening of high school students using the help assessment tool Please check the accuracy. Strategy: telediagnosis/telemonitoring through mHealth (app) | Conducting the YouthCHAT assessment and managing positive detection of analysed behaviour | Its availability in schools, with school nurses and counsellors, facilitates its application for opportunistic and routine psychosocial assessment, reducing costs compared to time-consuming face-to-face assessments | Difficult to generalise data. Lack of data on the satisfaction of participating nurses |
| Müssener et al. (2020) [57] | Randomised controlled trial. Level 1.c—RCT | Sweden. High school students aged 17 | To estimate the effectiveness of a novel mHealth intervention called NEXit Junior, which targets smoking cessation. Strategy: tele-education through mHealth (SMS) | N/A | The results of the NEXit junior trial demonstrated a positive effect on smoking cessation of a text messaging-only intervention | Follow-up was assessed by self-reported measures and was not biochemically verified |
| Bacopoulou et al. (2019) [58] | Descriptive observational study. Level 4—Not specified | Greece. Adolescents aged 12–17 | Detect MS (International Diabetes Federation criteria) and explore its associations with anthropometric, sociodemographic, and behavioural parameters using telemedicine in the school setting. Strategy: telediagnosis/telemonitoring | Coordinate and execute the biochemical analysis of the study (blood extraction), as well as the anthropometric tests | N/A | Difficulty in extrapolating data in different contexts |
| Bian et al. (2019) [59] | Randomised controlled trial. Level 1.c—RCT | USA. Children aged 3–17 enrolled in the Medicaid Statistical Information System | To examine the associations of a school-based telehealth programme with all-cause emergency department (ED) visits. Strategy: teleconsultation | N/A | 21% reduction in the likelihood of ED visits among a subsample of children with asthma; programme was associated with an overall reduction in ED visits of more than 20% | Limited generalisation and difficult extrapolation |
| Langbecker et al. (2019) [60] | Experimental prospective evaluation study. Level 1.d—Pseudo-RCTs | Australia. Children aged 3–12 in rural schools | To assess a service delivering speech and language therapy (SLT) and occupational therapy (OT) via videoconferencing. Strategy: teleconsultation | N/A | The majority of children who received telehealth services (SLT and OT) through the Health-e-Regions programme showed steady improvement over time | Limitations of the design (lack of validation strategies) |
| Lau et al. (2019) [61] | Cluster randomised controlled trial. Level 1.c—RCT | Hong Kong. Adolescents aged 12–16 | To assess the effectiveness of a short message service (SMS) intervention on promoting physical activity. Strategy: tele-education through mHealth (SMS) | N/A | El efecto recordatorio mediante SMS a los participantes es la función más obvia para lograr efectos significativos de la intervención y proporciona apoyo motivacional, interactivo y social | Difficulty to generalise due to small sample size |
| Marshman et al. (2019) [62] | Randomised controlled trial. Level 1.c—RCT | UK. Young people aged 11–13 from deprived areas | The Bringing Information and Guided Help Together (BRIGHT) trial assessed the clinical use and cost-effectiveness of a behaviour change intervention—classroom-based session (CBS) embedded in the curriculum and a series of SMS delivered to participants twice daily to remind them to brush their teeth—compared to usual curriculum and no SMS. Strategy: tele-education through mHealth (SMS) | N/A | Motivational SMS improved self-reported oral health | Contamination between participating groups |
| Tebb et al. (2019) [63] | Cluster randomised control trial. Level 1.c—RCT | USA. Latin adolescents aged 13–18 | To assess the implementation of a mobile health contraception decision support intervention in school-based health centres. Strategy: Tele-education through mHealth (app) | N/A | Preventing pregnancy in at-risk communities, facilitating access to contraceptive information through the Health-E You mobile digital tool | Difficulty in generalising to other environments. Limitations related to technological infrastructure (reliable connectivity, confidentiality assurance, communication required across multiple levels) |
| Brinker et al. (2018) [64] | Randomised controlled trial. Level 1.c—RCT | Brazil. Students in secondary schools aged 13–18 | To assess the effectiveness of a photoaging intervention for skin cancer prevention delivered by medical students in secondary schools. Strategy: tele-education through mHealth (app) | N/A | Raises awareness among future doctors about the importance of skin cancer prevention and influences the improvement of health behaviours in the prevention of photoaging | Difficulty in extrapolating data in different contexts |
| Estai et al. (2018) [65] | Cross-sectional study. Level 4.b—Cross-sectional study | Australia. Children and adolescents aged 5–14 from low-risk areas | To develop a resource reallocation model for school dental screening that takes advantage of teledentistry. Strategy: telediagnosis/telemonitoring | N/A | Telemedicine improves access to dental healthcare | Not reported |
| Govender et al. (2018) [66] | Randomised controlled trial. Level 1.c—RCT | South Africa. Children aged 6–12 | To assess the efficacy of an asynchronous telehealth-based service delivery model using automated technology for screening and diagnostic testing. Strategy: telediagnosis/telemonitoring | N/A | Automated asynchronous telehealth-based automated hearing tests in the school context can be used to facilitate early identification of hearing loss | Limitations related to “carry-over effects” where a participant’s performance in one test may influence his or her performance in the other test |
| Halterman et al. (2018) [67] | Randomised controlled trial. Level 1.c—RCT | USA. Children aged 3–10 | To assess the effect of the School-Based Telemedicine Enhanced Asthma Management (SB-TEAM) Program. Strategy: teleconsultation | Review telemedicine visits to ensure efficient completion of guideline-based care, including appropriate prescribing of preventive medications. Nurses do not receive additional compensation | Children in the SB-TEAM group had more symptom-free days every 2 weeks post intervention compared to children in the enhanced usual care group and were less likely to have an emergency department visit or hospitalisation for asthma | Difficulties in ensuring double-blinding and difficult extrapolation |
| McLennan (2018) [68] | Descriptive observational study. Level 4—Not specified | Canada. Children aged 6–12 | To assess the effectiveness of video-conferencing telehealth linkage attempts to schools to facilitate mental health consultations. Strategy: teleconsultation | N/A | Mental health consultations were successfully conducted through two different telehealth video conferencing links between a health centre and several schools in this pilot initiative. The linkage that was able to utilise existing hardware in both the health and school systems holds promise for scalability given the low equipment costs and minimal technical support required | Difficulty of extrapolation |
| Perry et al. (2018) [69] | Cluster randomised controlled trial. Level 1.c—RCT | USA. Children (aged 7–14) living in an impoverished rural region | To examine the effect of a school-based asthma education programme delivered by telemedicine. Strategy: tele-education through videoconference | Nursing is a component of the study, receiving telemedicine educational intervention, comprehensive asthma education, and interactive question and answer sessions aimed at preventing asthma attacks, assessing treatment efficacy, and managing attacks | Although some behavioural changes were observed among intervention participants, these were insufficient | Reluctance of primary care providers to change or initiate asthma medication according to recommendations without a formal referral to a clinical setting; possible lack of contact between families and primary care providers due to difficulty accessing care within the 3-month period in which the primary outcome was measured; low caregiver participation in educational sessions; low response rates to the survey |
| Pradhan et al. (2018) [70] | Descriptive observational study. Level 4—Not specified | USA. Vulnerable youth aged 12–17 | To describe a telehealth model for delivering integrated mental health services in a telemedicine-based school health clinic. Strategy: teleconsultation | N/A | Access to specialised care for the most vulnerable young people increased | Connected teams that maintain communication and facilitate follow-up to interventions and mitigate cultural and distance barriers |
| Zettler-Greeley et al. (2018) [71] (grey literature) | Descriptive observational study (individual case report). Level 4.d—Case study | USA. Students aged 6–12 | To describe how telehealth stopped a contagious outbreak at a school. Strategy: teleconsultation through telenursing | School nurses are positioned to triage complaints appropriately, reducing the potential for overuse, a common concern given the easy access to care offered by telehealth. The nurse ensures seamless communication with the physician during virtual visits; serves as a gatekeeper of students’ personal health information; and operates as the primary interface between parents, students, paediatricians, and teachers on school health issues | Telehealth visits are more cost-effective than an emergency room visit and can help prevent and contain public health problems. Telehealth in schools reduces absenteeism, increases instructional time, and offers benefits to underserved children in regions where access to healthcare is limited | Unresolved political issues related to licensing, jurisdiction, and reimbursement hinder the growth of paediatric telehealth |
| Skarzynski et al. (2016) [72] | Analytical observational study. Level 3.e—Observational study without a control group | Poland. Children aged 7–8 | To validate hearing screening procedures in young children and collect data using a telemedicine model. Strategy: telediagnosis/telemonitoring | N/A | Improved monitoring and control of hearing problems through telemedicine | Limitation in the collection of data through questionnaires |
| Burckhard et al. (2015) [73] | Randomised controlled trial. Level 1.c—RCT | Australia. Students aged 12–18 | To examine the feasibility of an online school-based positive psychology programme (Bite-Back) delivered in a structured format over a 6-week period utilising a workbook to guide students through website content and interactive exercises. Strategy: tele-education through interactive activities | N/A | No significant results were reported | Problems in the implementation of Bite Back in the school setting. |
| Langkamp et al. (2015) [74] | Descriptive study of a case series. Level 4.c—Case series | USA. Children and adolescents aged 3–21 | Detection of hearing problems through the Tele-Health-Kids (THK) telemedicine tool. Strategy: telediagnosis/telemonitoring | Performing nursing duties and coordinating with primary healthcare staff for the implementation of the THK programme | High level of parental satisfaction with the programme; increased adherence to treatment and cooperation from children; families felt more actively involved in their children’s healthcare; the familiar figure of the school nurse instils confidence and security in the family and children; reduced stress for the child and parents; increased likelihood of successful medical examination; superior and more effective clinical care than traditional office visits | Sample size too limited to make generalisations about telemedicine use |
| Bannink et al. (2014) [75] | Cluster randomised controlled trial. Level 1.c—RCT | Netherlands. Students aged 13–18 | To assess the effect of E-health4Uth and consultation on well-being (mental health status and health-related quality of life) and health behaviours (alcohol and drug use, smoking, safer sex). Strategy: tele-education through mHealth (SMS) | School nurses were trained to conduct motivational interviews with adolescents aged 15–16 years. During the consultation, they focused on specific risk areas and mental health. Adolescents were referred to another professional if deemed necessary | E-health4Uth allows the selection of vulnerable adolescents and provides nurses with information about the health of these adolescents. It contributes to the efficiency of face-to-face consultations | Abandonment and difficulty of extrapolation |
| Cremers et al. (2014) [76] | Cluster randomised controlled trial. Level 1.c—RCT | Netherlands. Children aged 10–11 | To assess whether email and mobile phone prompts stimulate primary school children to reuse an internet-delivered smoking prevention intervention. Strategy: tele-education through mHealth (SMS) | N/A | Prompts can encourage children to reuse an intervention website aimed at smoking prevention | Limited access to technology and tedious measures to ensure confidentiality that complicate participation |
| Purpose of Telehealth | N (%) |
|---|---|
| Hearing screenings and speech and communication problems | 5 (15.62%) |
| Promoting healthy habits and lifestyles (healthy eating and physical activity) | 4 (12.50%) |
| Promoting mental health and emotion management | 4 (12.50%) |
| Prevention and management of respiratory problems such as asthma | 4 (12.50%) |
| Oral health screening and hygiene | 3 (9.37%) |
| Prevention of tobacco, alcohol, and other substance use | 2 (6.25%) |
| Reproductive health and pregnancy prevention | 2 (6.25%) |
| Screening and monitoring of mental health problems | 2 (6.25%) |
| Prevention of psychosocial problems | 1 (3.12%) |
| Autism assessment | 1 (3.12%) |
| Diagnosis and management of skin scabies | 1 (3.12%) |
| Prevention of skin cancer and photoaging | 1 (3.12%) |
| Screening for metabolic syndrome | 1 (3.12%) |
| Intervention strategies | |
| Tele-education | 15 (46.87%) |
| Teleconsultation (telehealth) | 9 (28.12%) |
| Telediagnosis or telemonitoring | 8 (25%) |
| Nursing role | |
| Administration and monitoring of medical guidelines via teleconsultation; scheduling and monitoring of telemedicine visits; facilitating fluid communication in virtual visits; and mediating between different agents (family, teachers, paediatricians, and students). | 3 (9.37%) |
| Motivational interviews through teleconsultation on specific risk areas and mental health; behavioural assessment in the detection of psychosocial problems via YouthCHAT. | 2 (6.25%) |
| Comprehensive asthma education aimed at crisis prevention; evaluation and treatment of asthma crises; coordination with the primary care team for the application of the hearing problems detection programme; follow-up through telemedicine; and coordination and execution of anthropometric tests for the detection of metabolic syndrome. | 3 (9.37%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ayuso Margañon, R.; Llistosella, M.; Ayuso Margañon, S.; Rojano Navarro, M.; Bou Gràcia, N.; Sillero Sillero, A. Nursing Practice and Telehealth in School Health Services: A Scoping Review. Healthcare 2023, 11, 3124. https://doi.org/10.3390/healthcare11243124
Ayuso Margañon R, Llistosella M, Ayuso Margañon S, Rojano Navarro M, Bou Gràcia N, Sillero Sillero A. Nursing Practice and Telehealth in School Health Services: A Scoping Review. Healthcare. 2023; 11(24):3124. https://doi.org/10.3390/healthcare11243124
Chicago/Turabian StyleAyuso Margañon, Raquel, Maria Llistosella, Sonia Ayuso Margañon, Marta Rojano Navarro, Núria Bou Gràcia, and Amalia Sillero Sillero. 2023. "Nursing Practice and Telehealth in School Health Services: A Scoping Review" Healthcare 11, no. 24: 3124. https://doi.org/10.3390/healthcare11243124
APA StyleAyuso Margañon, R., Llistosella, M., Ayuso Margañon, S., Rojano Navarro, M., Bou Gràcia, N., & Sillero Sillero, A. (2023). Nursing Practice and Telehealth in School Health Services: A Scoping Review. Healthcare, 11(24), 3124. https://doi.org/10.3390/healthcare11243124






