Applying a Health Access Framework to Understand and Address Food Insecurity
Abstract
:1. Introduction
1.1. Food Insecurity through the Lens of Access Barriers
1.2. Limitations of Food Insecurity Measures
1.3. Nonprofit Organizations’ Role in Addressing Social Needs including Food Insecurity
2. Methods
3. Results
4. Discussion
5. Conclusions
6. Limitations
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- U.S. Department of Agriculture. Food Security in the U.S. Available online: https://www.ers.usda.gov/topics/food-nutrition-assistance/food-security-in-the-us/ (accessed on 10 September 2021).
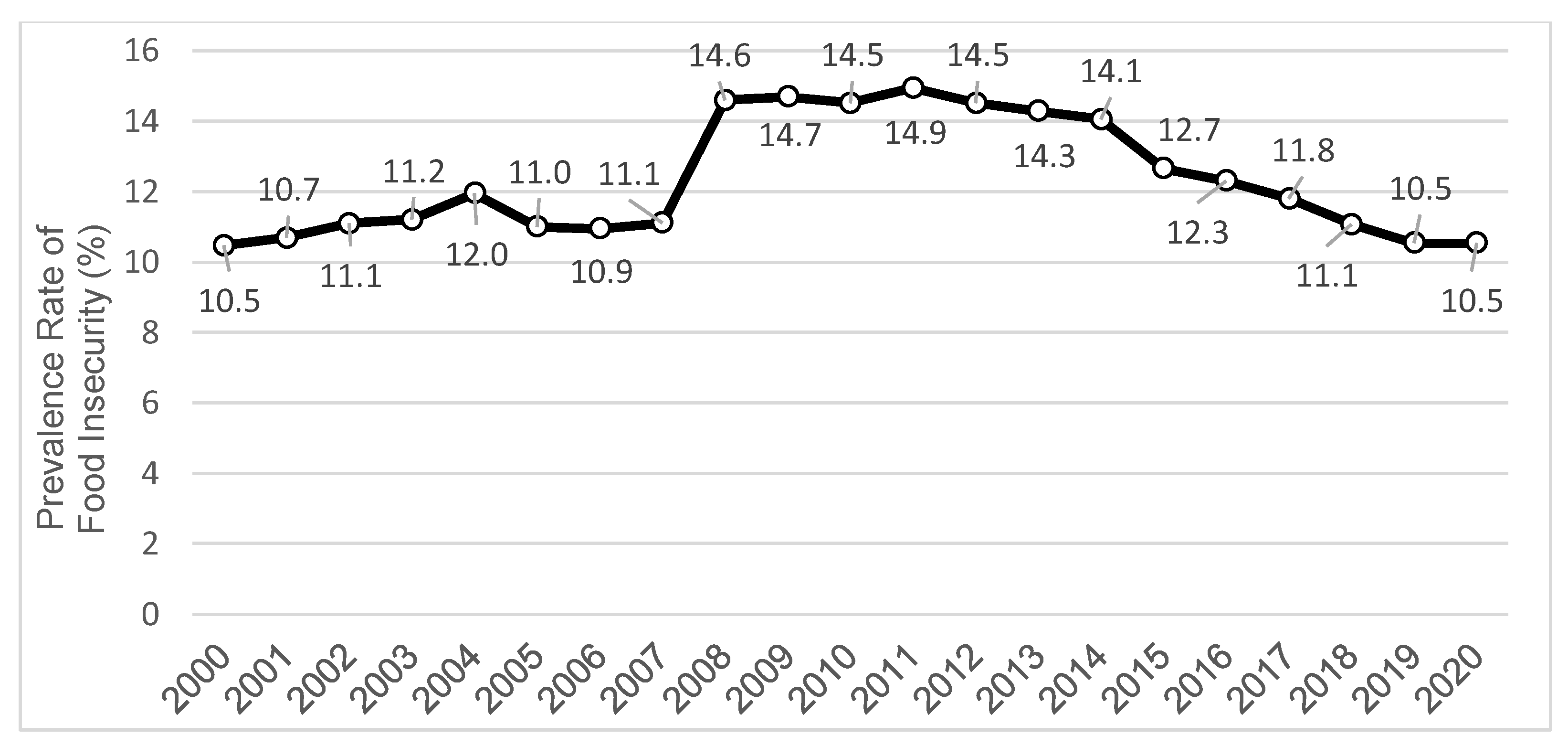
- U.S. Department of Agriculture. Trends in Prevalence Rates. Available online: https://www.ers.usda.gov/topics/food-nutrition-assistance/food-security-in-the-us/key-statistics-graphics/ (accessed on 10 September 2021).
- Gundersen, C.; Ziliak, J.P. Food insecurity and health outcomes. Health Aff. 2015, 34, 1830–1839. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ricks, J.L.; Cochran, S.D.; Arah, O.A.; Williams, J.K.; Seeman, T.E. Food insecurity and intimate partner violence against women: Results from the California Women’s Health Survey. Public Health Nutr. 2016, 19, 914–923. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Young, S.; Wheeler, A.C.; McCoy, S.I.; Weiser, S.D. A review of the role of food insecurity in adherence to care and treatment among adult and pediatric populations living with HIV and AIDS. AIDS Behav. 2014, 18, 505–515. [Google Scholar] [CrossRef] [Green Version]
- Chilton, M.M.; Rabinowich, J.R.; Woolf, N.H. Very low food security in the USA is linked with exposure to violence. Public Health Nutr. 2014, 17, 73–82. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Whittle, H.J.; Sheira, L.A.; Frongillo, E.A.; Palar, K.; Cohen, J.; Merenstein, D.; Wilson, T.E.; Adedimeji, A.; Cohen, M.H.; Adimora, A.A. Longitudinal associations between food insecurity and substance use in a cohort of women with or at risk for HIV in the United States. Addiction 2019, 114, 127–136. [Google Scholar] [CrossRef]
- Koyanagi, A.; Stubbs, B.; Oh, H.; Veronese, N.; Smith, L.; Haro, J.M.; Vancampfort, D. Food insecurity (hunger) and suicide attempts among 179,771 adolescents attending school from 9 high-income, 31 middle-income, and 4 low-income countries: A cross-sectional study. J. Affect. Disord. 2019, 248, 91–98. [Google Scholar] [CrossRef]
- Thomas, M.M.; Miller, D.P.; Morrissey, T.W. Food insecurity and child health. Pediatrics 2019, 144, e20190397. [Google Scholar] [CrossRef] [Green Version]
- Berkowitz, S.A.; Seligman, H.K.; Meigs, J.B.; Basu, S. Food insecurity, healthcare utilization, and high cost: A longitudinal cohort study. Am. J. Manag. Care 2018, 24, 399–404. [Google Scholar]
- Berkowitz, S.; Basu, S.; Gundersen, C.; Seligman, H. State-Level and County-Level Estimates of Health Care Costs Associated with Food Insecurity. Prev. Chronic Dis. 2019, 16, E90. [Google Scholar] [CrossRef]
- HealthyPeople. Reduce Household Food Insecurity and in Doing So Reduce Hunger. Available online: https://www.healthypeople.gov/node/4936/data_details#:~:text=The%20HP2010%20target%20of%20at,6%20percent%20experiencing%20food%20insecurity (accessed on 10 September 2021).
- HealthyPeople. Reduce Household Food Insecurity and Hunger—NWS-01. Available online: https://health.gov/healthypeople/objectives-and-data/browse-objectives/nutrition-and-healthy-eating/reduce-household-food-insecurity-and-hunger-nws-01 (accessed on 10 September 2021).
- Caswell, J.A.; Yaktine, A.L.; Council, N.R. History, background, and goals of the supplemental nutrition assistance program. In Supplemental Nutrition Assistance Program: Examining the Evidence to Define Benefit Adequacy; National Academies Press: Washington, DC, USA, 2013. [Google Scholar]
- Coleman-Jensen, A.; Rabbitt, M.P.; Gregory, C.A.; Singh, A. Household Food Security in the United States in 2018; U.S. Department of Agriculture: Washington, DC, USA, 2019.
- National Conference of State Legislatures (NCSL). Chart of Federal Nutrition Programs. Available online: https://www.ncsl.org/research/human-services/federal-nutrition-programs-chart.aspx (accessed on 5 October 2021).
- Schanzenbach, D.W.; Bauer, L.; Nantz, G. Twelve Facts about Food Insecurity and SNAP; Brookings Institution: Washington, DC, USA, 2016. [Google Scholar]
- Bleich, S.; Dunn, C.; Fleischhacker, S. The Impact of Increasing SNAP Benefits on Stabilizing the Economy, Reducing Poverty and Food Insecurity amid COVID-19 Pandemic. Available online: https://healthyeatingresearch.org/wp-content/uploads/2020/04/HER-SNAP-Brief-042220.pdf (accessed on 5 October 2021).
- Gaines-Turner, T.; Simmons, J.C.; Chilton, M. Recommendations From SNAP Participants to Improve Wages and End Stigma. Am. J. Public Health 2019, 109, 1664–1667. [Google Scholar] [CrossRef]
- National Research Council. Supplemental Nutrition Assistance Program: Examining the Evidence to Define Benefit Adequacy; National Academies Press: Washington, DC, USA, 2013. [Google Scholar]
- Community Tool Box. An overview of the Community Tool Box and Frameworks for Guiding, Supporting and Evaluating the Work of Community and System Change. 2021. Available online: https://ctb.ku.edu/en/table-of-contents (accessed on 10 September 2021).
- Ricketts, T.C.; Goldsmith, L.J. Access in health services research: The battle of the frameworks. Nurs. Outlook 2005, 53, 274–280. [Google Scholar] [CrossRef] [PubMed]
- Andersen, R.M. Revisiting the behavioral model and access to medical care: Does it matter? J. Health Soc. Behav. 1995, 36, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Penchansky, R.; Thomas, J.W. The concept of access: Definition and relationship to consumer satisfaction. Med. Care 1981, 19, 127–140. [Google Scholar] [CrossRef]
- Alexander, K.E.; Brijnath, B.; Mazza, D. Parents’ decision making and access to preventive healthcare for young children: Applying A ndersen’s M odel. Health Expect. 2015, 18, 1256–1269. [Google Scholar] [CrossRef] [Green Version]
- Miller, D.P.; Nepomnyaschy, L.; Ibarra, G.L.; Garasky, S. Family structure and child food insecurity. Am. J. Public Health 2014, 104, e70–e76. [Google Scholar] [CrossRef]
- Cui, S. Dynamics of Food Insecurity of Families with Children. Ph.D. Thesis, Iowa State University Digital Repository, Ames, IA, USA, 2007. [Google Scholar]
- Higashi, R.T.; Lee, S.C.; Pezzia, C.; Quirk, L.; Leonard, T.; Pruitt, S.L. Family and social context contributes to the interplay of economic insecurity, food insecurity, and health. Ann. Anthropol. Pract. 2017, 41, 67–77. [Google Scholar] [CrossRef]
- Manleey, J.; Neuberger, Z. Using Data Matching and Targeted Outreach to Enroll Families with Young Children in WIC—Lessons Learned from State Pilots. Available online: https://bdtrust.org/cbpp-bdt-case-study.pdf (accessed on 5 October 2021).
- Benefits Data Trust. Facilitating Remote Application Assistance for SNAP during COVID-19: Recommendations for States and Application Assisters. Available online: https://bdtrust.org/Brief-Remote_Application_Assistance_for_SNAP_During_COVID-19.pdf (accessed on 17 October 2021).
- Finkelstein, A.; Notowidigdo, M.J. Take-up and targeting: Experimental evidence from SNAP. Q. J. Econ. 2019, 134, 1505–1556. [Google Scholar] [CrossRef] [Green Version]
- United Way. United Way 211 Program. Available online: https://www.unitedway.org/our-impact/featured-programs/2-1-1 (accessed on 10 September 2021).
- Feeding America. Map the Meal Gap: Food Insecurity in The United States. Available online: https://map.feedingamerica.org/ (accessed on 10 September 2021).
- HealthyPeople. Food Insecurity. Available online: https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-health/interventions-resources/food-insecurity#:~:text=Low%20food%20security%3A%20%E2%80%9CReports%20of,patterns%20and%20reduced%20food%20intake.%E2%80%9D (accessed on 10 September 2021).
- Feeding America. What Are the Connections between Food Insecurity and Health? Available online: https://hungerandhealth.feedingamerica.org/understand-food-insecurity/hunger-health-101/ (accessed on 10 September 2021).
- U.S. Department of Agriculture. Go to the Atlas: Food Deserts. Available online: https://www.ers.usda.gov/data-products/food-access-research-atlas/go-to-the-atlas/ (accessed on 10 September 2021).
- Pinard, C.; Bertmann, F.; Byker Shanks, C.; Schober, D.; Smith, T.; Carpenter, L.; Yaroch, A. What factors influence SNAP participation? Literature reflecting enrollment in food assistance programs from a social and behavioral science perspective. J. Hunger. Environ. Nutr. 2017, 12, 151–168. [Google Scholar] [CrossRef]
- Algert, S.J.; Reibel, M.; Renvall, M.J. Barriers to participation in the food stamp program among food pantry clients in Los Angeles. Am. J. Public Health 2006, 96, 807–809. [Google Scholar] [CrossRef]
- Gundersen, C. Food assistance programs and child health. Future Child. 2015, 25, 91–109. [Google Scholar] [CrossRef]
- Pérez-Escamilla, R.; Segall-Corrêa, A.M. Food insecurity measurement and indicators. Revista Nutrição 2008, 21, 15s–26s. [Google Scholar] [CrossRef]
- National Research Council. Food Insecurity and Hunger in the United States: An Assessment of the Measure; National Academies Press: Washington, DC, USA, 2006. [Google Scholar]
- Bickel, G.; Nord, M.; Price, C.; Hamilton, W.; Cook, J. Guide to Measuring Household Food Security. Available online: https://naldc.nal.usda.gov/download/38369/PDF (accessed on 17 October 2021).
- Census. CPS Frequently Asked Questions. Available online: https://www.census.gov/programs-surveys/cps/about/faqs.html#Q3 (accessed on 10 September 2021).
- Torres, J.; De Marchis, E.; Fichtenberg, C.; Gottlieb, L. Identifying Food Insecurity in Health Care Settings: A Review of the Evidence. Available online: https://sirenetwork.ucsf.edu/sites/sirenetwork.ucsf.edu/files/SIREN_FoodInsecurity_Brief.pdf (accessed on 17 October 2021).
- Billioux, A.; Verlander, K.; Anthony, S.; Alley, D. Standardized screening for health-related social needs in clinical settings: The accountable health communities screening tool. NAM Perspect. Available online: https://nam.edu/standardized-screening-for-health-related-social-needs-in-clinical-settings-the-accountable-health-communities-screening-tool/ (accessed on 17 October 2021). [CrossRef] [Green Version]
- National Research Council. A Sustainability Challenge: Food Security for All: Report of Two Workshops; National Academies Press: Washington, DC, USA, 2012.
- Fraze, T.; Lewis, V.A.; Rodriguez, H.P.; Fisher, E.S. Housing, transportation, and food: How ACOs seek to improve population health by addressing nonmedical needs of patients. Health Aff. 2016, 35, 2109–2115. [Google Scholar] [CrossRef] [Green Version]
- American Hospital Association (AHA). Social Determinants of Health Series: Food Insecurity and the Role of Hospitals. Available online: https://www.aha.org/system/files/hpoe/Reports-HPOE/2017/determinants-health-food-insecurity-role-of-hospitals.pdf (accessed on 10 September 2021).
- Wallace, A.S.; Luther, B.L.; Sisler, S.M.; Wong, B.; Guo, J.-W. Integrating social determinants of health screening and referral during routine emergency department care: Evaluation of reach and implementation challenges. Implement. Sci. Commun. 2021, 2, 114. [Google Scholar] [CrossRef]
- Jiao, J.; Moudon, A.V.; Ulmer, J.; Hurvitz, P.M.; Drewnowski, A. How to identify food deserts: Measuring physical and economic access to supermarkets in King County, Washington. Am. J. Public Health 2012, 102, e32–e39. [Google Scholar] [CrossRef]
- Walker, R.E.; Keane, C.R.; Burke, J.G. Disparities and access to healthy food in the United States: A review of food deserts literature. Health Place 2010, 16, 876–884. [Google Scholar] [CrossRef]
- Meenar, M.R. Using participatory and mixed-methods approaches in GIS to develop a Place-Based Food Insecurity and Vulnerability Index. Environ. Plan. A 2017, 49, 1181–1205. [Google Scholar] [CrossRef]
- Sharareh, N.; Hess, R.; Wan, N.; Zick, C.D.; Wallace, A.S. Incorporation of Information-Seeking Behavior Into Food Insecurity Research. Am. J. Prev. Med. 2020, 58, 879–887. [Google Scholar] [CrossRef]
- 211. Utah 211 by the Numbers. Available online: https://uw.org/211/211-our-work/ (accessed on 17 October 2021).
- Benefits Data Trust (BDT). Available online: https://bdtrust.org/ (accessed on 17 October 2021).
- Metta, K.; Olabisi, L.; Wallace, R. A system dynamics approach to examining household food insecurity. J. Agric. Food Syst. Community Dev. 2021, 10, 455–472. [Google Scholar] [CrossRef]
- Sterman, J. Business Dynamics: Systems Thinking and Modeling for a Complex World (Irwin/McGr); McGraw-Hill Inc.: Boston, MA, USA, 2000. [Google Scholar]
- Kirkpatrick, S.I.; Tarasuk, V. Housing circumstances are associated with household food access among low-income urban families. J. Urban Health 2011, 88, 284–296. [Google Scholar] [CrossRef] [Green Version]
- Mui, Y.; Ballard, E.; Lopatin, E.; Thornton, R.L.; Pollack Porter, K.M.; Gittelsohn, J. A community-based system dynamics approach suggests solutions for improving healthy food access in a low-income urban environment. PLoS ONE 2019, 14, e0216985. [Google Scholar] [CrossRef]
- Gany, F.; Melnic, I.; Ramirez, J.; Wu, M.; Li, Y.; Paolantonio, L.; Smith, J.; Pan, S.; Roberts-Eversley, N.; Blinder, V. Food insecurity among cancer patients enrolled in the supplemental nutrition assistance program (SNAP). Nutr. Cancer 2021, 73, 206–214. [Google Scholar] [CrossRef]
- Hiller, M.B.; Winham, D.M.; Knoblauch, S.T.; Shelley, M.C. Food Security Characteristics Vary for Undergraduate and Graduate Students at a Midwest University. Int. J. Environ. Res. Public Health 2021, 18, 5730. [Google Scholar] [CrossRef]
- Niles, M.T.; Bertmann, F.; Belarmino, E.H.; Wentworth, T.; Biehl, E.; Neff, R. The early food insecurity impacts of COVID-19. Nutrients 2020, 12, 2096. [Google Scholar] [CrossRef]
- Yousefi-Rizi, L.; Baek, J.-D.; Blumenfeld, N.; Stoskopf, C. Impact of Housing Instability and Social Risk Factors on Food Insecurity Among Vulnerable Residents in San Diego County. J. Community Health 2021, 46, 1107–1114. [Google Scholar] [CrossRef]
- De Marchis, E.H.; de Cuba, S.A.E.; Chang, L.; Sheward, R.S.; Doran, K.M.; Gottlieb, L.M.; Cohen, A.J.; Fleegler, E.W.; Sandel, M.T. Screening Discordance and Characteristics of Patients With Housing-Related Social Risks. Am. J. Prev. Med. 2021, 61, e1–e12. [Google Scholar] [CrossRef]
| Predisposing Access Barriers | Enabling Access Barriers | |
|---|---|---|
| Societal-Level | Inequality in education and occupation, Informational barriers (lack of understanding about the need for specific resources) | Inequality in income, healthcare, and housing |
| Institutional-Level | Attitudes towards food providers (e.g., food pantries, soup kitchens) | Food prices, Eligibility and application process of federal nutrition assistance programs, Geographic barriers (lack of access to supermarkets, and food providers, transportation barriers), Food policies, Poor communications about available food resources |
| Individual-Level | Stigma, Beliefs, Informational barriers (lack of information about resources), healthcare comorbidities | Economic instability (income), Social relationships |
| Loop | Name—Explanation |
|---|---|
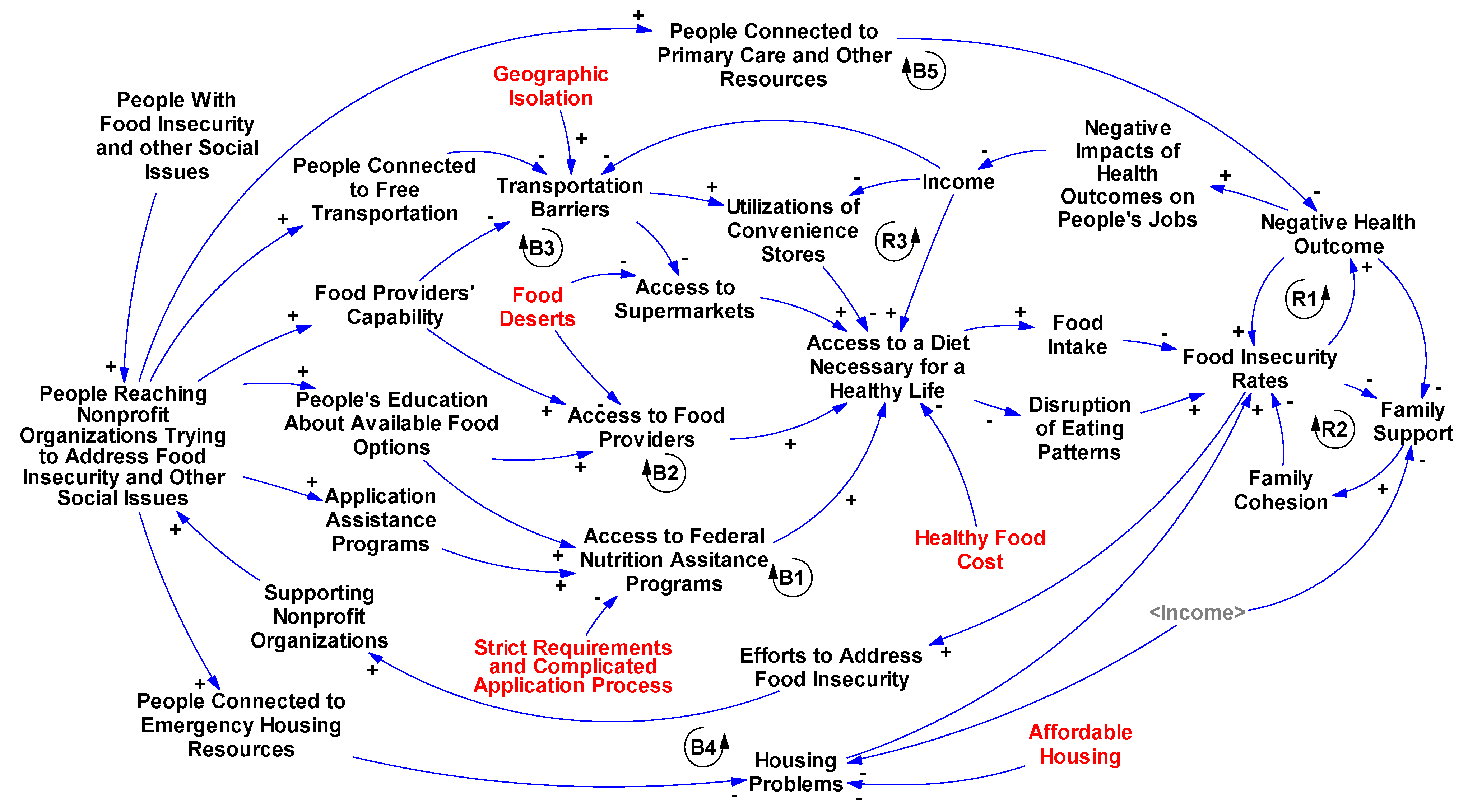
| R1 | Health loop: the causal link between FI and negative health outcomes such as obesity, depression, violence, etc. creates a reinforcing loop that increases FI and negative health outcomes |
| R2 | Family Structure loop: FI creates stress, disorganizes households, and impacts family cohesion which reinforces FI. |
| R3 | Unhealthy Food loop: Lack of income cause transportation barriers, which force people to acquire food from convenience stores with mostly unhealthy foods, and eventually lead to higher FI rates. Many other factors can also cause transportation barriers but we just illustrated the link between income, transportation, and FI in this loop. Additionally, economic instability impacts health and housing but the links are not shown. |
| B1 | Federal Nutrition Assistance Programs loop: increasing efforts to address FI could include supporting nonprofit organizations to connect people to federal nutrition assistance programs or enhancing these programs’ capabilities in which both will provide critical benefits to low-income people to meet their food needs |
| B2 | Food Providers loop: as the efforts to address FI increase, more nonprofit organizations assist food providers and will raise public awareness about these providers which will eventually raise access to food. |
| B3 | Balancing transportation loop: some nonprofit organizations assist people to get access to free transportation, hencepeople could shop from supermarkets that are far from their neighborhood, which will decrease FI. |
| B4 | Housing loop: nonprofit organizations can connect people to emergency housing resources, assisting people to overcome their housing problems, so that people will not need to choose between housing and food. |
| B5 | Primary Care loop: addressing healthcare issues provide the chance to people to better perform their job duties, improve their economic stability, choose better food, andmeet their food needs. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sharareh, N.; Wallace, A.S. Applying a Health Access Framework to Understand and Address Food Insecurity. Healthcare 2022, 10, 380. https://doi.org/10.3390/healthcare10020380
Sharareh N, Wallace AS. Applying a Health Access Framework to Understand and Address Food Insecurity. Healthcare. 2022; 10(2):380. https://doi.org/10.3390/healthcare10020380
Chicago/Turabian StyleSharareh, Nasser, and Andrea S. Wallace. 2022. "Applying a Health Access Framework to Understand and Address Food Insecurity" Healthcare 10, no. 2: 380. https://doi.org/10.3390/healthcare10020380
APA StyleSharareh, N., & Wallace, A. S. (2022). Applying a Health Access Framework to Understand and Address Food Insecurity. Healthcare, 10(2), 380. https://doi.org/10.3390/healthcare10020380






